Académique Documents
Professionnel Documents
Culture Documents
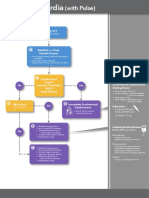
Tachycardia Algorythm
Transféré par
UZNAPM0 évaluation0% ont trouvé ce document utile (0 vote)
214 vues1 pageAlgorythm detailing step by step the management of tachycardia
Copyright
© Attribution Non-Commercial (BY-NC)
Formats disponibles
PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentAlgorythm detailing step by step the management of tachycardia
Droits d'auteur :
Attribution Non-Commercial (BY-NC)
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
214 vues1 pageTachycardia Algorythm
Transféré par
UZNAPMAlgorythm detailing step by step the management of tachycardia
Droits d'auteur :
Attribution Non-Commercial (BY-NC)
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 1
Resuscitation Council (UK)
• Support ABCs: give oxygen; cannulate a vein
• Monitor ECG, BP, SpO2
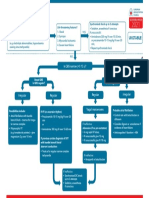
Adult tachycardia algorithm • Record 12-lead ECG if possible; if not, record rhythm strip
(with pulse) • Identify and treat reversible causes (e.g. electrolyte abnormalities)
Synchronised DC Shock * Unstable
Is patient stable?
Up to 3 attempts
Signs of instability include:
1. Reduced conscious level 2. Chest pain
3. Systolic BP < 90 mmHg 4. Heart failure
• Amiodarone 300 mg IV over 10-20 min (Rate-related symptoms uncommon at less than 150 beats min-1)
and repeat shock; followed by:
• Amiodarone 900 mg over 24 h Stable
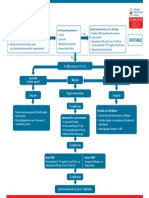
Is QRS narrow (< 0.12 sec)?
Broad Narrow
Broad QRS Narrow QRS
Is QRS regular? Is rhythm regular?
Regular Irregular
Irregular Regular • Use vagal manoeuvres Irregular Narrow Complex
• Adenosine 6 mg rapid IV bolus; Tachycardia
Seek expert help if unsuccessful give 12 mg;
Probable atrial fibrillation
if unsuccessful give further 12 mg.
Control rate with:
• Monitor ECG continuously
Possibilities include: If Ventricular Tachycardia • β-Blocker IV or digoxin IV
• AF with bundle branch block (or uncertain rhythm): If onset < 48 h consider:
treat as for narrow complex • Amiodarone 300 mg IV • Amiodarone 300 mg IV 20-60 min;
• Pre-excited AF over 20-60 min; Normal sinus rhythm restored? then 900 mg over 24 h
consider amiodarone then 900 mg over 24 h
• Polymorphic VT (e.g.
torsade de pointes - give
If previously confirmed SVT Yes No
with bundle branch block:
magnesium 2 g over 10 min)
• Give adenosine as for regular Probable re-entry PSVT:
narrow complex tachycardia Seek expert help
* Attempted electrical cardioversion is
• Record 12-lead ECG in sinus
always undertaken under sedation
rhythm
or general anaesthesia • If recurs, give adenosine again &
consider choice of anti-arrhythmic Possible atrial flutter
prophylaxis • Control rate (e.g. β-Blocker)
Vous aimerez peut-être aussi
- ALS Algorithms LS Tachycardia 2.0Document1 pageALS Algorithms LS Tachycardia 2.0Lucian Alin DinuPas encore d'évaluation
- 5.ALS Algorithms TachycardiaDocument1 page5.ALS Algorithms TachycardiaMassimo Di BenedettoPas encore d'évaluation
- Adult Tachycardia (With Pulse) AlgorithmDocument1 pageAdult Tachycardia (With Pulse) AlgorithmJames ChoiPas encore d'évaluation
- Ecgs and Acute Cardiac Events: Yuniardi Alriyanto, MD Doris Sylvanus Hospital PalangkarayaDocument47 pagesEcgs and Acute Cardiac Events: Yuniardi Alriyanto, MD Doris Sylvanus Hospital PalangkarayaAuliaRusdiAllmuttaqienPas encore d'évaluation
- G2015 Adult Tachycardia PDFDocument1 pageG2015 Adult Tachycardia PDFibbs91Pas encore d'évaluation
- G2015 Adult Tachycardia PDFDocument1 pageG2015 Adult Tachycardia PDFPlabber JunePas encore d'évaluation
- Tachycardia Algorithm 2021Document1 pageTachycardia Algorithm 2021Ravin DebiePas encore d'évaluation
- Managemen Disritmia: Dr. Rofika Hanifa, SPPDDocument20 pagesManagemen Disritmia: Dr. Rofika Hanifa, SPPDavivlabirdPas encore d'évaluation
- 2010 Integrated Updated Circulation ACLS Tachycardia AlgorithmDocument1 page2010 Integrated Updated Circulation ACLS Tachycardia AlgorithmRyggie ComelonPas encore d'évaluation
- Algo Tachycardia PDFDocument1 pageAlgo Tachycardia PDFYudhistira AdiPas encore d'évaluation
- Assess Appropriateness For Clinical Condition. Heart Rate Typically 150/min If TachyarrhythmiaDocument1 pageAssess Appropriateness For Clinical Condition. Heart Rate Typically 150/min If TachyarrhythmiaSiti Nur R Firda FauziyahPas encore d'évaluation
- AdultTachycardiaWithPulse AlgorithmDocument1 pageAdultTachycardiaWithPulse AlgorithmIsmail SlimPas encore d'évaluation
- Adult Tachycardia Algorithm: (With Pulse)Document1 pageAdult Tachycardia Algorithm: (With Pulse)ITSimplyPas encore d'évaluation
- AlgorithmACLS Tachycardia 200612Document1 pageAlgorithmACLS Tachycardia 200612must dietPas encore d'évaluation
- Adult Tachycardia With A Pulse Algorithm: Doses/DetailsDocument1 pageAdult Tachycardia With A Pulse Algorithm: Doses/DetailsAlexis HospitalPas encore d'évaluation
- Adult Tachycardia With A Pulse Algorithm: Doses/DetailsDocument1 pageAdult Tachycardia With A Pulse Algorithm: Doses/DetailsZakiyahulfahdwPas encore d'évaluation
- Advanced Cardiac Life SupportDocument37 pagesAdvanced Cardiac Life SupportRoy Acosta GumbanPas encore d'évaluation
- Website Tachycardia Algorithm DiagramDocument1 pageWebsite Tachycardia Algorithm Diagramcolette zgheibPas encore d'évaluation
- .JPG 958×1,280 PixelsDocument1 page.JPG 958×1,280 Pixelsyordanos getachewPas encore d'évaluation
- Tachycardia With A Pulse Algorithm: Assess Appropriateness For Clinical ConditionDocument1 pageTachycardia With A Pulse Algorithm: Assess Appropriateness For Clinical ConditionDendy Frannuzul RamadhanPas encore d'évaluation
- AlgorithmACLStachycardiawithapulse PDFDocument1 pageAlgorithmACLStachycardiawithapulse PDFDendy Frannuzul RamadhanPas encore d'évaluation
- AlgorithmACLS Tachycardia 200612Document1 pageAlgorithmACLS Tachycardia 200612YassarPas encore d'évaluation
- Pediatric Tachycardia With A Pulse Algorithm: Yes NoDocument1 pagePediatric Tachycardia With A Pulse Algorithm: Yes NoRatna TambaPas encore d'évaluation
- Peri-Arrest ArrythmiaDocument14 pagesPeri-Arrest Arrythmiamohamed mowafeyPas encore d'évaluation
- Adult Tachycardia Algorithm: (With Pulse)Document1 pageAdult Tachycardia Algorithm: (With Pulse)ITSimplyPas encore d'évaluation
- Bra Dal GoDocument1 pageBra Dal Gozacklim_2000Pas encore d'évaluation
- Pals TachycardiaDocument1 pagePals TachycardiadarlingcarvajalduquePas encore d'évaluation
- Arrhythmias: - Finot D., MD, MSC, Emergency Physician, CC FellowDocument43 pagesArrhythmias: - Finot D., MD, MSC, Emergency Physician, CC FellowKaleb DemissePas encore d'évaluation
- TachycardiaDocument7 pagesTachycardiaArvind SahniPas encore d'évaluation
- ACLS Tachycardia Algorithm For Managing Stable TachycardiaDocument4 pagesACLS Tachycardia Algorithm For Managing Stable TachycardiaLady MuffinsPas encore d'évaluation
- Acute Coronary SyndromeDocument7 pagesAcute Coronary SyndromePuskesmas Pinang JayaPas encore d'évaluation
- EKG StripsDocument10 pagesEKG StripsSaidel ElizondoPas encore d'évaluation
- Hippo EM Board Review - Bradycardia - A Simplified Approach Written Summary 2Document10 pagesHippo EM Board Review - Bradycardia - A Simplified Approach Written Summary 2alexandertorresreyPas encore d'évaluation
- Tachycardia AlgorithmDocument1 pageTachycardia AlgorithmGideon BahulePas encore d'évaluation
- Bradycardia and TachycardiaDocument66 pagesBradycardia and TachycardiaKarissaPas encore d'évaluation
- Algo Pals TachycardiaDocument1 pageAlgo Pals TachycardiaArdie FratamaPas encore d'évaluation
- Acls Study Guide 2016Document2 pagesAcls Study Guide 2016nova939100% (2)
- MCEM B CVS TachycardiaDocument12 pagesMCEM B CVS TachycardiaRajin MaahiPas encore d'évaluation
- Med II-LE1-1.03 Arrhythmia NotesDocument14 pagesMed II-LE1-1.03 Arrhythmia NotesAbigael SantosPas encore d'évaluation
- Algoritmos AHA ACLS AdultoDocument4 pagesAlgoritmos AHA ACLS AdultoChristianFelipePorrasCastroPas encore d'évaluation
- Periarestne AritmijeDocument10 pagesPeriarestne AritmijeMustafa ŠabićPas encore d'évaluation
- Onlinemeded Notes CardioDocument1 pageOnlinemeded Notes CardioCourtney HolbrookPas encore d'évaluation
- Obat-Obatan Dalam Bantuan Hidup LanjutDocument16 pagesObat-Obatan Dalam Bantuan Hidup LanjutTheresia SihotangPas encore d'évaluation
- Nursing CS Treatment-Of-Atrial-Dysrhythmias 02Document1 pageNursing CS Treatment-Of-Atrial-Dysrhythmias 02frankshro156Pas encore d'évaluation
- TachycardiaDocument12 pagesTachycardiaPuskesmas Pinang JayaPas encore d'évaluation
- Antiarrythmic Agents: Antiarrythmic Drugs For HorsesDocument3 pagesAntiarrythmic Agents: Antiarrythmic Drugs For HorsesMageja TatendaPas encore d'évaluation
- AlgorithmsDocument16 pagesAlgorithmsirish laglevaPas encore d'évaluation
- 26) Approach To Pediatric ArrhythmiasDocument44 pages26) Approach To Pediatric ArrhythmiasJude AlyousefPas encore d'évaluation
- Tatalaksana ArrthytmiaDocument55 pagesTatalaksana ArrthytmiaJanstine FirstiandyPas encore d'évaluation
- K31a - Electrophysiology and Cardiac Arrhytmia EmergencyDocument46 pagesK31a - Electrophysiology and Cardiac Arrhytmia EmergencyXeniel AlastairPas encore d'évaluation
- Arrhythmias EmergencyDocument10 pagesArrhythmias EmergencyNITACORDEIROPas encore d'évaluation
- U.M.F. "Gr. T. Popa" Ia Ş IDocument37 pagesU.M.F. "Gr. T. Popa" Ia Ş Ij.doe.hex_87Pas encore d'évaluation
- STEMI Algorithm Poster 18x24Document1 pageSTEMI Algorithm Poster 18x24OgizWaraPas encore d'évaluation
- Arrhythmias: Clinical DiagnosisDocument4 pagesArrhythmias: Clinical DiagnosispaveethrahPas encore d'évaluation
- Cardiology Notes USMLE Step CKDocument135 pagesCardiology Notes USMLE Step CKArianna BetancourtPas encore d'évaluation
- New S-MAX EbrochureDocument26 pagesNew S-MAX EbrochureshuusakuPas encore d'évaluation
- Cla Class PDFDocument68 pagesCla Class PDFUZNAPMPas encore d'évaluation
- Kuga EBrochureDocument33 pagesKuga EBrochureUZNAPMPas encore d'évaluation
- Renault TwizyDocument16 pagesRenault TwizyUZNAPMPas encore d'évaluation
- Nuevo Mapa Del MundoDocument1 pageNuevo Mapa Del MundoverarexPas encore d'évaluation
- Renault ZoeDocument16 pagesRenault ZoeUZNAPM100% (2)
- Scenic Family RenaultDocument20 pagesScenic Family RenaultUZNAPMPas encore d'évaluation
- Mercedes ClassDocument57 pagesMercedes ClassDejanPrckovicPas encore d'évaluation
- Renault SportDocument32 pagesRenault SportUZNAPMPas encore d'évaluation
- DrawCalendar2013 AsAt 12092013Document2 pagesDrawCalendar2013 AsAt 12092013UZNAPMPas encore d'évaluation
- Peugeot Roland Garros Range BrochureDocument6 pagesPeugeot Roland Garros Range BrochureUZNAPMPas encore d'évaluation
- Mercedes CLS Class CoupeDocument83 pagesMercedes CLS Class CoupeUZNAPMPas encore d'évaluation
- Peugeot RCZ Prices and Specifications BrochureDocument11 pagesPeugeot RCZ Prices and Specifications BrochureUZNAPMPas encore d'évaluation
- Application LetterDocument1 pageApplication LetterNina SatimbrePas encore d'évaluation
- Hosanna Complexe de Sante KolloDocument3 pagesHosanna Complexe de Sante Kolloapi-26180856Pas encore d'évaluation
- PEDIA - 1st Sem Prelims FeedbackDocument3 pagesPEDIA - 1st Sem Prelims FeedbackEricPas encore d'évaluation
- The Rochester Diabetic Neuropathy StudyDocument10 pagesThe Rochester Diabetic Neuropathy StudyMonica ViverosPas encore d'évaluation
- Inseparable - Prospectus With 2021 BudgetDocument9 pagesInseparable - Prospectus With 2021 BudgetAralee HenighanPas encore d'évaluation
- Ichroma II Test Panels 210331 104829Document2 pagesIchroma II Test Panels 210331 104829Sinergy DiagnosticPas encore d'évaluation
- Trichomonas Rapid Test: CLIA Complexity: WaivedDocument8 pagesTrichomonas Rapid Test: CLIA Complexity: WaivedRabecca TobingPas encore d'évaluation
- Kesehatan Indonesia. 2016.: Daftar PustakaDocument2 pagesKesehatan Indonesia. 2016.: Daftar PustakaSiti Raudatus SolihahPas encore d'évaluation
- CHAPTER 8. AdmissionsDocument9 pagesCHAPTER 8. AdmissionsKumala MadurahayunirwanaPas encore d'évaluation
- Spiritual Healing Chants - Opt PDFDocument11 pagesSpiritual Healing Chants - Opt PDFAmit Govilkar100% (1)
- Communicable Disease SurveillanceDocument60 pagesCommunicable Disease SurveillanceAmeer MuhammadPas encore d'évaluation
- Client Intake FormDocument1 pageClient Intake Formapi-162312216Pas encore d'évaluation
- LESSON 2-3 HealthDocument20 pagesLESSON 2-3 HealthKalabit PengePas encore d'évaluation
- GDMDocument30 pagesGDMCharlz ZipaganPas encore d'évaluation
- Nursing Pharmacology Immunity Study GuideDocument18 pagesNursing Pharmacology Immunity Study GuideChelsea SmithPas encore d'évaluation
- Health Care Law OutlineDocument17 pagesHealth Care Law OutlineMegan Lindsay Ruffin100% (1)
- Complete Blood Picture: Test Name Value Units Reference Range 3.44 7.4 76 22 28.5Document107 pagesComplete Blood Picture: Test Name Value Units Reference Range 3.44 7.4 76 22 28.5anil tanankiPas encore d'évaluation
- City of Batac, Ilocos Norte, Philippines Contact Details: Direct Line: (077) 6000105 Trunk Line: (077) 7923133 Loc. 102Document1 pageCity of Batac, Ilocos Norte, Philippines Contact Details: Direct Line: (077) 6000105 Trunk Line: (077) 7923133 Loc. 102LexiePascuaSantosPas encore d'évaluation
- Prescribing For The ElderlyDocument8 pagesPrescribing For The ElderlykarladeyPas encore d'évaluation
- Torn Meniscus A Sports InjuryDocument35 pagesTorn Meniscus A Sports InjuryPradeep RajPas encore d'évaluation
- Highly Agressive Multiple Sclerosis PDFDocument26 pagesHighly Agressive Multiple Sclerosis PDFnight.shadowPas encore d'évaluation
- Placenta PreviaDocument2 pagesPlacenta PreviaIrish Joy S. DecrepitoPas encore d'évaluation
- Schedule For Full Preparation NEET 2020 B 001Document3 pagesSchedule For Full Preparation NEET 2020 B 001goyal RPas encore d'évaluation
- Sana Mayar - Careers ExplorationDocument14 pagesSana Mayar - Careers Explorationapi-626536214Pas encore d'évaluation
- Definition of Deviated Nasal SeptumDocument3 pagesDefinition of Deviated Nasal SeptumMank BayuPas encore d'évaluation
- Homeopathic First Aid For Infants and Children PDFDocument3 pagesHomeopathic First Aid For Infants and Children PDFRamesh Shah100% (1)
- Quality Issu in Midwifery ICM PDFDocument9 pagesQuality Issu in Midwifery ICM PDFFarhatiPas encore d'évaluation
- Coma StimulationDocument18 pagesComa StimulationDarshika Vyas Mohan88% (17)
- Health & Family Welfare Department: Government of West BengalDocument2 pagesHealth & Family Welfare Department: Government of West BengalAnkit JhaPas encore d'évaluation
- Poison and Antidote ChartDocument5 pagesPoison and Antidote ChartSusanne Mae Gonzales50% (2)