Académique Documents
Professionnel Documents
Culture Documents
Traumatic Oral Lesions: A Review
Transféré par
Auliapratiwi13Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Traumatic Oral Lesions: A Review
Transféré par
Auliapratiwi13Droits d'auteur :
Formats disponibles
Traumatic Oral Mucosal Lesions: A Mini Review and Clinical Update
Ariyawardana Anura
School of Medicine and Dentistry, James Cook University, McGregor Road, Smithfield, QLD 4878 Australia.
Abstract
Oral mucosal lesions are a common occurrence and very often dentists are called upon to see such patients. Among many causes
trauma is one of the leading for oral mucosal diseases. Oral traumatic lesions are diverse in which some present as acute lesions while
the majority are chronic lesions. Clinical presentation of traumatic lesions vary significantly and most of the occasions the cause and
the effect can be established with thorough history and clinical examination. Although, biopsy of such lesions are not required in
most of the occasions some may warrant histological investigations to exclude conditions which clinically mimic traumatic lesions.
This paper provides an overview of common and some rare traumatic conditions of the oral mucosa.
Introduction
raised white line on the buccal mucosae extending from the
commissure to the last molar teeth along their occlusal line
[1]. In a Turkish study among adolescents (13-16 years of age)
linea alba was the second commonest finding which accounts
for 5.3% of the total [2]. It is believed that parakeratosis occur
along the line of the occlusal plane as the cheeks sucks in due
to the negative pressure [1]. Linea alba is asymptomatic and
generally considered a normal variation than pathological [3]
and therefore, no treatment is required.
Oral lesions associated with trauma are a relatively common
finding in dental practice. A diverse array of oral mucosal
disorders caused by acute and chronic trauma exists. They
manifest in the oral mucosa as acute or chronic ulcers, white
or red lesions, mucositis, and reactive hyperplasia or even as
bone exposures with sequestration. Such lesions may also
impair oral functions to a significant extent and also pose some
difficulties in arriving at a diagnosis especially the chronic
lesions. However, prompt diagnosis and elimination of the
causative factor ensure cure. Injury of the oral mucosa could
result from physical, chemical or thermal trauma. They could
be originated from accidental dental biting, sharp or pointing
food stuff, sharp edges of teeth, hot food or overzealous tooth
brushing. Some injuries also could result from iatrogenic
damage during dental treatment or other procedures involving
oral cavity such as intubation during general anaesthesia.
Similarly chemical or physical injury could result from undue
or careless handling of chemicals and dental instruments
during dental treatment procedures. This paper reviews some
common causes of traumatic injuries, their diagnosis and
management (Table 1).
Mucosal Biting
Accidental mucosal biting is a common occurrence which
eventually leads to mucosal bleeding and painful ulceration.
Such lesions generally heal in a few days time with no
complications. However, chronic habitual biting of the oral
mucosa may lead to transient or persistent white patches.
Chronic biting (nibbling) of the buccal mucosa often leads
to produce loose thread like keratin shreds, tissue tags or
desquamative areas on the mucosal surface [4]. Such lesions
have been referred to as morsicatio buccarum when occurs
on the buccal mucosa (Figure 1) and morsicatio labiorum
and morsicatio linguarum when occur on labial mucosa and
lateral borders of the tongue, respectively [5].
In a retrospective study of 584 patients Woo and Lin [4]
Linea Alba
Linea alba is a common finding which is described as a bilateral
Table 1. Summary of oral mucosal traumatic lesions and their management.
Condition
Diagnosis
Linea Alba
Clinical
Mucosal Biting
Clinical
Riga-Fede disease
Eosinophilic ulcer
Ulcers caused by self-mutilation or self-injury
Ulcers due to oral trauma in patients with
congenital insensitivity to pain
Electrical and Thermal Burns
Trauma associated with sexual practices
Denture associated hyper keratosis
Denture associated ulcers
Inflammatory papillary hyperplasia
Epulis fissuratum
Clinical
Biopsy
Clinical
Clinical
Clinical
Clinical
Clinical
Clinical
Clinical
Clinical
Common sites of occurrence
Management
Explanation and reassurance, no specific
Buccal mucosa
treatment required
Buccal mucosa, lip and lateral border Explanation and reassurance, advice on
of the tongue
habitual biting
Tip or ventral surface of the tongue
Extraction of neonatal teeth
Gingiva
Spontaneous healing
Gingiva
Psychological assessment and counselling
Symptomatic treatment, prevent trauma
Lips and tongue
from sharp edges of teeth
Lips and tongue
Surgical excision and reconstruction
Soft palate, lips
Symptomatic management
Alveolar ridge
Elimination of irritation from the denture
Buccal and lingual sulci
Trim the denture to eliminate trauma
Palate
Anti-fungal treatment, surgical excision
Buccal sulcus
Surgical excision and vestibuloplasty
Corresponding author: Ariyawardana Anura, School of Medicine and Dentistry, James Cook University, McGregor Road, Smithfield,
QLD 4878, Australia, Tel: +647-4232-1248; e-mail: anura.ariyawardana@jcu.edu.au
254
OHDM - Vol. 13 - No. 2 - June, 2014
Traumatic Ulceration
reported a prevalence of 9.0% of such lesions where they refer
as morsicatio mucosa oris. Although, buccal mucosa is the
most commonly affected site [5], this study found lateral
border of the tongue as the commonest site accounting for
53.6% and followed by buccal mucosa (32.1%) and labial
mucosa (9%). These lesions can be found between 3rd to 6th
decades of life and it is generally resulted from deliberate
act of habitual biting or even subconsciously though many
patients deny their habit [4,5].
In most cases clinical presentation is sufficient to arrive
at the diagnosis and often does not require histological
investigation. Oral hairy leukoplakia, uremic stomatitis
and chewers mucosa are important differential diagnosis.
Therefore, if the lesions are seen on the lateral border of the
tongue in a patient with high risk of HIV infection further
investigations are required to rule out HIV associated hairy
leukoplakia [5]. In general no treatment is required and patient
education and counseling may often resolve the problem.
However, for some patients the use of acrylic shield to cover
the facial surfaces of teeth may be used to eliminate the lesion
by restricting the access to the lesion sites (lips and buccal
mucosa) [5].
Traumatic ulcers could result from physical, thermal or
chemical injuries. Ulcers resulting from traumatic injuries
are probably the most common types of ulcers encountered
in clinical practice (Figures 2 and 3). Accidental biting
during mastication, sharp pointy food may cause acute
traumatic ulceration. Such ulcers generally heal within few
days without complications. However, chronic trauma from
sharp edges of teeth, restorations and appliances particularly
ill-fitting dentures may cause chronic ulcers. The majority of
such injuries are unintentional however, self-inflicted injuries
also can frequently be found. In most occasions the cause and
effect relationship can be established.
From two cohorts of patients in Thailand and Malaysia
reported prevalence of traumatic ulcers 13.2% and 12.4%
from Thailand and Malaysia, respectively [6]. Similarly in
another study on elderly Thai patents also reported traumatic
ulcers in 15.6% of their study population out of which the
majority were due to poor dentures, fractured restorations
and sharp edges of teeth [7]. Slightly lower prevalence of
traumatic ulcers has been reported from Spain (7.1%) [8],
Denmark (4.4%) [9] and Chile (3.5%) [10]. In a large group of
Saudi dental patients over the age of 15 years Al-Mobeeriek
and Al Dosari (2009) found a prevalence of 1.9% accounting
for the third most common oral mucosal disease in that cohort
of patients [11].
Chronic traumatic ulcers are commonly found on the
mucosa that is subjected to trauma from dentition such as
buccal mucosa, lateral border of the tongue or lips. Lesions
on other areas including mucobuccal folds and gingivae are
associated with other sources of irritation such as trauma from
tooth brush or food.
Chronic traumatic ulcers generally present as a solitary
shallow or deep discontinuation of epithelium with varying
degrees of peripheral keratosis (Figure 4). Floor of the ulcer
is covered by a white or yellowish fibrin clot. Ulcer resulted
from repeated trauma may be symptomatic or asymptomatic,
often exhibits an elevated border which is firm on palpation.
Upon elimination of the causative factor often ulcer heals
with or without scar depending on the extent of the damage
occurred.
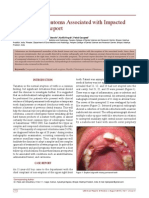
Figure 1. Cheek biting: A 30 year old male patient with a white
patch on both sides of his cheek. Note irregular shaggy surface
typical of cheek biting.
Figure 2. Traumatic ulcer: A 14 year old male patient with an
ulcer on his right lower lip after 2 days of a tooth extraction.
Traumatic ulcer due to lip biting after inferior dental nerve block
was diagnosed on clinical grounds: Note the irregular margin with
slough and exudate on flow of the ulcer.
255
Figure 3. Traumatic ulcer: A 13 year old male patent with an
ulcer on the ventral surface of the tongue for a period of 3 moths.
Traumatic ulcer on the ventral surface of the tongue was caused by
lingually erupted mandibular central incisor.
OHDM - Vol. 13 - No. 2 - June, 2014
lesion which is usually manifested on the lateral border of
the tongue [14,15]. However, this has also been reported
to occur in the gingiva and rarely on other sites [15,16].
Since its first description it has been descried in a number of
different names: traumatic granuloma, Traumatic Ulcerative
Granuloma with Stromal Eosinophilia (TUGSE), atypical
histiocytic granuloma [5,14-18]. When it occurs in infants
and children in association with natal, neonatal or primary
teeth it has been termed as Riga-Fede disease [12].
Lesions are commonly seen among individuals of 4th to 5th
decades of life with equal sex distribution. Eosinophilic ulcer
commonly presents as solitary indurated or granulomatous
ulcer which may sometime mimic a malignant lesion [15].
Therefore, confirmation of the diagnosis may need an
incisional biopsy. Generally ulcers tend to heal spontaneously
but slowly over a period of 3-10 weeks. Some lesions heal
promptly after carrying out a biopsy [15,19].
Figure 4. Traumatic ulcer: A 60 year old man with a chronic
ulcer on the left posterior lateral border of the tongue caused by
lingually tilted mandibular 3rd molar. Note central ulceration with
peripheral keratosis.
Necrotizing Sialometaplasia
Necrotizing Sialometaplasia (NS) is first described by
Abrams et al. as an uncommon inflammatory necrotizing
process involving minor salivary glands predominantly
affecting the hard palate [20]. Although the exact aetiology
is not known, the mostly suspected and generally accepted
underlying mechanism is ischaemia of minor salivary gland
tissues [20-22]. Several predisposing factors which lead to
ischaemia have been proposed by these authors. Brannon
and coworkers reported that they observed after NS 8 days
on average following a surgical procedure in 36% of their
case series. Other traumatic episodes such as dental injection
and wearing ill-fitting dentures were also been implicated in
some cases [21]. In addition to trauma, smoking and alcohol
consumption, allergy and upper respiratory tract infections
were also considered as predisposing to NS [21].
Clinically NS presents as a solitary unilateral ulcer on the
hard palate (Figure 5) [20-22]. However, a number of cases
were also reported as non-ulcerated swelling or mass [21].
Lesions could accompany with pain or numbness while some
may be asymptomatic [5,21-23]. Although a wide variation of
Riga-Fede Disease
Riga-Fede disease is a reactive traumatic ulcerative disorder
with benign course often seen on tip or ventral surface of the
tongue [5,12,13]. Lesions tend to occur after the eruption
of neonatal, natal or primary incisors. They are commonly
observed in relation to the lower incisors believed to be
caused by repetitive trauma associated with back and forward
movement of the tongue against them. Although rare, they
can also been reported on the dorsal surface of the tongue and
the lower lip.
A number of terms have been used to describe these
lesions including traumatic lingual ulceration, eosinophilic
granuloma, traumatic eosinophilic ulceration of the tongue
and traumatic granuloma of the tongue [12,13].
van der Meij et al. [13] in a review summarized 34 cases
(age range 0.3-24 months) that they found since 1902. Of
them 82% of the lesions were found on the ventral surface of
the tongue while rest of the lesions was equally distributed on
the dorsum of the tongue and the lower lip. Only seven lesions
(20.5%) were associated with neonatal teeth while the rest of
the lesions were caused by primary teeth with a mean age of
onset at 10 months. Overall, lesions were more commonly
found among males with a male to female ratio of 1.8:1 [13].
Clinically these lesions appear as ulcerated area with
fibrinous exudate with varying degrees of raised margins
depending on the duration and frequency of trauma [12,13].
Generally the diagnosis is established clinically alone and
rarely biopsy is required. Several treatment options have
been described which principally aiming at elimination of the
causative factor. The treatment of choice for lesions associated
with neonatal teeth is extractions of such teeth. Contrary to
this, more conservative approaches such as placement of
a protective barrier or grinding of the sharp edges of teeth
have also been attempted. However, in some intractable cases
extraction of causative teeth is the only option [13].
Figure 5. Necrotizing sialometaplasia: A 55 year old male with an
ulcer on his left side of the palate. Clinical diagnosis of necrotizing
sialometaplasia was made and the lesion healed in 14 days after
the diagnosis. These ulcers may mimic squamous cell carcinoma
clinically as well as histologically.
Eosinophilic Ulcer
Eosinophilic ulcer is a chronic, often self-limiting benign
256
OHDM - Vol. 13 - No. 2 - June, 2014
age of onset had been reported, NS is more commonly seen
in adults with the mean age of 46 years and more commonly
affecting males [21]. The most important clinical significance
is that the lesion mimics malignancy clinically as well as
histologically; squamous cell carcinoma and mucoepidermoid
carcinoma in particular [5,23]. Although history of traumatic
event could be of importance in arriving at diagnosis, due to
the worrisome appearance of the lesion it is recommended
to carry out an incisional biopsy. Lesions generally heal
spontaneously in an average period of 5-6 weeks [5].
occur in young children. Such injuries often lead to
disfigurement and functional disabilities [5,33]. There are two
types of electrical burns; contact and arc types. Contact type
require a good ground and electrical current passes through
the body from the site of contact to the ground where as in
arc type burns saliva act as a conducting medium and current
flows between the source and the mouth. The resultant high
temperature causes electrical burn leading to severe destruction
of oral tissues [33]. Most of the electrical injuries occur as a
result of sucking or chewing of live electrical wires, extension
cords, plugs or power outlets. Hence, they most commonly
occur in toddlers or preschool children. Such injuries in adults
are extremely rare [34]. Electrical trauma most commonly
affects the lips, and present as painless, charred yellowish
area with little or no bleeding followed by significant oedema
within few hours [5]. Necrosed tissues slough and heal with
scarring leading to significant disfigurement [33].
Thermal injuries to oral soft tissues most commonly occur
due to accidental ingestion of hot food or beverages. Food
associated thermal injuries generally occur in the palate or
the posterior buccal mucosa. They appear as sloughy necrotic
tissue surrounded by erythema [5].
Management of electrical burn injuries are difficult and
often challenging due to extreme contractions leading to
disfigurement and functional disability. Several methods have
been attempted including excision and reconstruction and use
of burn appliances [33]. Management of thermal burns is not
as complicated as electrical burns and generally heals with
fewer complications [5,35].
Factitious Disorders and Trauma
Factitious mucosal lesions are not uncommon. Selfmutilation or self-injury is a behavioural disturbance
that leads to deliberate harm to own body tissues and not
associated with intention to commit suicide [24]. Although
the exact prevalence in the world population is not known,
it affects people regardless of their age, sex or ethnicity [25].
The aetiology can be of two fold; organic and functional.
Organic self-mutilation injuries include injuries in comatose
patients, patients with some syndromes such as Lesch-Nyhan
syndrome, De Lange syndrome, Tourette syndrome, Leigh
syndrome, patients with autism spectrum disorders and
familial dysautonomia [26-30]. Functional self-mutilation
refers to intentional self-injuring in physically healthy
patients without detectable genetic disorders [25]. Oral selfmutilation injuries are commonly seen among children than
adolescents or adults. In a recent review Hilderbrand et al.
[25] reported 15 cases including their case among children
with an age range of 3-13 years. Among them over 90% of the
lesions were observed in the gingivae. Clinically such lesions
appear as ulcers on the gingiva or as gingival recession [25].
Diagnosis and management of self-mutilation injuries are
generally difficult and thorough medical history and physical
examinations are of utmost importance in arriving at correct
diagnosis. Patients psychological assessment is mandatory
and multidisciplinary approach helps to carry out overall
management of the affected individual.
Chemical Injuries
A wide array of chemicals and drugs come into contact with
oral mucosa and some of them may cause direct mucosal
trauma due to their caustic nature. Some people tend to apply
certain chemicals as a remedy for their oral problems such
as application of aspirin to ease toothache [19]. Health care
practitioners are also responsible in applying certain chemicals
in the mouth for treatment or investigative procedures. Some
of such chemicals if used inadvertently can be potentially
injurious. However, such injuries are not very common since
the introduction of rubber dam in dental practice.
Oral Trauma due to Congenital Insensitivity to
Pain
Familial insensitivity to pain is a rare clinical syndrome
in which affected individuals pain sensation is impaired.
Individuals affected by this syndrome are generally normal
in terms of their physical and mental health and with normal
perception of other sensations [31]. This condition is generally
present at birth and the majority of cases are diagnosed at
early stages of life. Due to lack of pain sensation, self-inflicted
and unintentional oral injuries are common especially to lips
and tongue. Injuries to dental hard tissues are also common
[32]. Oral mucosal lesions are generally observed when
primary teeth erupt. Lips and tongue are the commonest sites
to be injured. No specific management strategy is available
to date however, preventive measures such as grinding and
smoothening sharp edges of teeth may help prevent the
injuries.
Sexual Practices and Oral Mucosal Trauma
Oro-genital stimulation has become a popular practice
during the last few decades and this is more common among
homosexual males and females [5,36]. It has been reported
that 90% of the married heterosexual couples under the age
of 25 years also practice oro-genital sex [36]. However,
the prevalence of trauma related to oro-genital stimulation
is surprisingly low [5]. Despite this it is imperative for the
dental practitioners to be familiar with the cause and the oral
manifestations of lesions associated with oro-genital sex.
Fellatio is the commonest among oro-genital sexual practices
that causes oral trauma. This generally manifests as erythema,
ecchymosis or petechiae in the soft palate [5]. These lesions
may be noticed during routine oral examinations and the
lesions are generally asymptomatic and heal within 7-10 days.
It is also of utmost importance for the dentists to be vigilant of
child abuse if such lesions are found in children.
Electrical and Thermal Burns
Oral electrical burns are relatively common and predominantly
257
OHDM - Vol. 13 - No. 2 - June, 2014
exposure to masticatory forces oral mucosa shows acanthosis,
rete hyperplasia and parakeratosis [37]. Hyperkeratosis is
regarded as a normal adaptation to function and resolve once
the irritation is removed. Traumatic ulcers generally occur
soon after the insertion of new dentures. They often appear
over the sharp bony ridges where the mucosa is sandwiched
between the denture and bone, under spicules or high spots
of dentures. Such trauma produces erythema, oedema and
subsequently ulceration which generally produce soreness or
pain preventing patients a comfortable mastication. Careful
elimination of such trauma leads to complete resolution of
the problem.
Inflammatory Papillary Hyperplasia (IPH) is a reactive
form of tissue overgrowth clinically present as a nodular or
papillary surface covering completely or partially the area of
the palate covered by the denture (Figure 6) [37-39]. Although
the exact aetiology is unknown, the condition is most often
suspected to be related to; continuous wearing of ill-fitting
dentures with poor hygiene that often causing trauma together
with predisposition to Candidal infection [5,40]. Lesions are
directly related to age of the patient and the length of denture
usage [41]. IPH is usually asymptomatic and often identified
during routine clinical examination. Very early lesions may
subside once the irritation is eliminated together with the
use of antifungal agents. However, more established lesions
may need surgical removal, curettage, electrosurgery or
cryotherapy [5].
Epulis fissuratum (inflammatory fibrous hyperplasia) is a
tumour like fibrous connective tissue lesion that develops as
a result of ill-fitting denture flange. Clinically, it presents as
a sessile mass in the sulcus with smooth surface and normal
mucosal colour and also may be erythematous and ulcerated
(Figure 7) [5,42]. This is most often seen among middle aged
and older adults occurring either in relation to the mandible or
maxilla and shows a female predilection. Treatment is often
involved with excision of the lesion with vestibuloplasty and
correction of the denture.
Figure 6. Papillary hyperplasia of the palate: A 70 year old female
with papillary hyperplasia of the palate; this lesion is localized to
the area of retention device. However, in most of the cases lesion
could be widespread in the palate.
Figure 7. Epulis fissuratum (inflammatory fibrous hyperplasia) in
a 70 year old female denture wearer: Note the tumour like fibrous
connective tissue on the alveolar ridge and extending to the labial
sulcus. Lesion develops as a result of chronic irritation due to illfitting denture.
Denture Associated Mucosal Trauma
Denture wearing can cause a number of acute or chronic oral
mucosal problems ranging from histological to gross clinical
changes [37]. Gross clinical changes include keratotic,
hyperplastic, inflammatory and ulcerative lesions [38]. In
a retrospective clinical study using 200 denture wearing
patients Dorey et al. [38] reported a positive relationship
of oral mucosal abnormalities and denture wearing in 60%
of their cohort of patients. Of these, chronic trauma from
denture was the most common cause accounting for 17% and
presented in the form of stomatitis with or without candida
infection. Other problems encountered were; hyperkeratosis
(12%), ulceration (8%), inflammatory papillary hyperplasia
(6%) and epulis fissurata (2%).
In response to chronic irritation from dentures particularly
Summary
References
2. Parlak AH, Koybasi S, Yavuz T, Yesildal N, Aydogan I, et
al. Prevalence of oral lesions in 13 to 16 year old students in Duzce,
Turkey. Oral Diseases. 2006; 12: 552-558.
3. Bhattacharyya I, Chehal HK. White lesions. Otolaryngologic
Clinics of North America. 2011; 44: 109-131.
This paper gives an overview of traumatic lesions of the oral
mucosa. The paper summarizes the common to rare disorders
causing traumatic lesions. Diverse array of causative factors
can be identified. Commonly encountered lesions are generally
straightforward to diagnose and hence easy to manage by
elimination of the causative factor and enhancing the healing
of the lesion. If chronic ulcer persists after the elimination
of the suspected causative factor within a reasonable time
limit (2-3 weeks) a biopsy should be considered to confirm
the diagnosis. Thorough clinical examination and attention
to all possible aspects of causative factors are mandatory for
complete resolution of the lesion.
1. Seoane LJM, Aguado SA, Varela-Centelles PI, Vazquez GJ,
Romero MA, et al. Oral Mucosa: variations from normalcy, part I.
Cutis. 2002; 69: 131-131.
258
OHDM - Vol. 13 - No. 2 - June, 2014
24. Favazza AR. Why patients mutilate themselves. Hospital
and Community Psychiatry. 1989; 40: 137-145.
25. Hilderbrand LC, Carvalho AL, da Rosa EM, Martins MD,
Filho MS. Functional oral self-mutilation in physically healthy
pediatric patients: Case report and analysis of 27 literature cases.
International Journal of Pediatric Otorhinolaryngology. 2011; 75:
880-883.
26. Kobayashi T, Ghanem H, Umezawa K, Mega J, Kawara M,
et al. Treatment of self-inflicted oral trauma in a comatose patient:
A case report. Journal of Canadian Dental Association. 2005; 71:
661-664.
27. Shimoyama T, Horie N, Kato T, Nasu D, Kaneko T.
Tourettes syndrome with rapid deterioration by self-mutilation of
the upper lip. Journal of Clinical Pediatric Dentistry. 2003; 27: 117-180.
28. Cauwels RGEC, Martens LC. Self-mutilation behavior in
Lesch-Nyhan Syndrome. Journal of Oral Pathology and Medicine.
2005; 34: 573-575.
29. Medina AC, Sogbe R, Gomez-Rey AM, Mata M. Factitial
oral lesions in an autistic pediatric patient. International Journal of
Pediatric Dentistry. 2003; 13: 130-137.
30. Mass E, Gadoth N. Oro-dental self-mutilation in familial
dysautonomia. Journal of Oral Pathology and Medicine. 1994; 23:
273-276.
31. Thompson CC, Park RI, Prescott GH. Oral manifestations
of congenital insensitivity to pain syndrome. Oral Surgery Oral
Medicine Oral Pathology Oral Radiology and Endodontics. 1980;
50: 220-205.
32. Butler J, Felming P, Webb D. Congenital insensitivity to
pain-review and report of a case with dental implications. Oral
Surgery Oral Medicine Oral Pathology Oral Radiology and
Endodontics. 2006; 101: 58-62.
33. Linebaugh ML, Koka S. Oral electrical burns: Etiology,
Histopathology and Prosthetic treatment. Journal of Prosthodontics.
1993; 2: 136-141.
34. Shimoyama T, Kaneko T, Nasu D, Suzuki T, Horie N. A
case of an electrical burn in the oral cavity of an adult. Journal of
Oral Science. 1999; 41: 127-128.
35. Baruchin AM, Lustig JP, Nahlieli O, Amos N. Burns of the
oral mucosa: Report of 6 cases. Journal of Cranio-Maxillofacial
Surgery. 1991; 19: 94-96.
36. Damm DD, White DK, Brinker M. Variations of palatal
erythema secondary to fellatio. Oral Surgery Oral Medicine Oral
Pathology. 1981; 52: 417-421.
37. Cook RJ. Response of the oral mucosa to denture wearing.
Journal of Dentistry. 1991; 19: 135-147.
38. Dorey JL, Blasberg B, McEntee MI, Conklin RJ. Oral
mucosal disorders in denture wearers. Journal of Prosthetic
Dentistry. 1985; 53: 210-213.
39. Budtz-Jorgensen E. Oral mucosal lesions associated with the
wearing of removable dentures. Journal of Oral Pathology. 1981;
10: 65-80.
40. Poulopoulos A, Belazi M, Epivatianos A, Velegraki A,
Antoniades D. The role of candida in inflammatory papillary
hyperplasia of the palate. Journal of Oral Rehabilitation. 2007; 34:
685-692.
41. Turker SB, Sener ID, Koak A, Yilmaz S, zkan YK.
Factors triggering the oral mucosal lesions by complete dentures.
Archives of Gerontology and Geriatrics. 2010; 51: 100-104.
42. Niccolo-Filho W, Neves ACC, Penna LAP, Seraidarian PI,
Riva R. Removal of epulis fissuratum associated to vestibuloplasty
with carbon dioxide laser. Lasers in Medical Science. 1999; 14:
203-206.
4. Woo SB, Lin D. Morsicatio Mucosae Oris-A chronic
oral frictional Keratosis, Not a Leukoplakia. Journal of Oral and
Maxillofacial Surgery. 2009; 67: 140-142.
5. Neville BW, Damm DD, Allen CM, Bouquot JE. Oral and
Maxillofacial Pathology. (3rd edn.) Philadelphia: Saunders. 2009;
pp. 285-329.
6. Axll T, Zain RB, Siwamogstham P, Tantiniran D, Thampipit
J. Prevalence of oral soft tissue lesions in out-patients at two
Malaysian and Thai dental schools. Community Dentistry and Oral
Epidemiology. 1990; 18: 95-99.
7. Jainkittivosng A, Aneksuk V, Langlias RP. Oral mucosal
conditions in elderly dental patients. Oral Diseases. 2002; 8: 218-223.
8. Garca-Pola VMJ, Martnez DCAI, Garca MJM, Gonzlez
GM. Risk factors for oral soft tissue lesions in and adult Spanish
population. Community Dentistry and Oral Epidemiology. 2002; 30:
277-285.
9. Vigild M. Oral mucosal lesions among institutionalized
elderly in Denmark. Community Dentistry and Oral Epidemiology
1987; 15: 309-313.
10. Espinoza I, Rojas R, Aranda W, Gamonal J. Prevalence of
oral mucosal lesions in elderly people in Santiago, Chile. Journal of
Oral Pathology and Medicine. 2003; 32: 571-575.
11. Al-Mobeeriek A, Al-Dosari AM. Prevalence of oral lesions
among Saudi Dental Patients. Annals of Saudi Medicine. 2009; 29:
365-368.
12. Ceyhan AM, Yildirim M, Basak PY, Akkaya VB, Ayata A.
Traumatic lingual ulcer in a child: Riga Fede disease. Clinical and
Experimental Dermatology. 2009; 34: 186-188.
13. van der Meij E, de Vries, Eggink HF, de Visscher JGAM.
Traumatic lingual ulceration in a new born: Riga-Fede disease.
Italian Journal of Pediatrics. 2012; 38: 20.
14. Compilato D, Cirillo N, Termine N, Kerr AR, Paderni C, et al.
Long-standing oral ulcers: proposal for a new S-C-D classification
system. Journal of Oral Pathology and Medicine. 2009; 38: 241253.
15. Horie N, Shimoyama T, Kato T, Ide F. Eosinophilic ulcer
of the tongue: a case report with immune-histochemical study. Oral
Medicine and Pathology. 1999; 4: 25-29.
16. Tornes K, Bang G. Traumatic eosinophilic granuloma of
gingiva. Oral Surgery. 1974; 38: 99-102.
17. Regezi JA. Oral traumatic granuloma: characterization of
the cellular infiltrate. Oral Surgery Oral Medicine Oral Pathology.
1993; 75: 723-727.
18. Hirshberg A, Amariglo N, Akrish S, Yahalom R, Rosenbaum
H, et al. Traumatic ulcerative granuloma with stromal eosinophilia:
A reactive lesion of the oralmucosa. American Journal of Clinical
Pathology. 2006; 126: 522-529.
19. Cawson RA, Odell EW. Cawsons Essentials of Oral
Pathology and Oral Medicine. (8th edn) Edinburgh: Elsevier. 2008;
pp. 237-238.
20. Abrams AM, Melrose RJ, Howell FV. Necrotizing
sialometaplasia: a disease simulating malignancy. Cancer. 1973; 32:
130-135.
21. Brannon RB, Fowler CB, Hartman KS. Necrotizing
sialometaplasia: A clinicopathological study of sixty nine cases and
review of literature. Oral Surgery Oral Medicine Oral Pathology.
1991; 72: 317-325.
22. Anneroth G, Hansen L. Necrotizing sialometaplasia:
the relationship of its pathogenesis to its clinical characteristics.
International Journal of Oral Surgery. 1982; 11: 283-291.
23. Carlson DL. Necrotizing sialometaplasia: A practical
approach to diagnosis. Archives of Pathology and Laboratory
Medicine. 2009; 133: 692-698.
259
Vous aimerez peut-être aussi
- Traumatic Oral Mucosal Lesions A Mini Review and Clinical Update 2247 2452.1000573Document7 pagesTraumatic Oral Mucosal Lesions A Mini Review and Clinical Update 2247 2452.1000573hokoPas encore d'évaluation
- Lip PiercingDocument5 pagesLip PiercingDana PopaPas encore d'évaluation
- Oral Frictional HyperkeratosisDocument5 pagesOral Frictional Hyperkeratosisahmedstar162000Pas encore d'évaluation
- Traumatic Oral Ulcers: Causes, Presentation and ManagementDocument7 pagesTraumatic Oral Ulcers: Causes, Presentation and ManagementamilaPas encore d'évaluation
- FistulaDocument5 pagesFistulaNurkamila SariPas encore d'évaluation
- Variasi Normal Rongga MulutDocument18 pagesVariasi Normal Rongga MulutRafi Kusuma Ramdhan SukonoPas encore d'évaluation
- Articol 1 ParoDocument7 pagesArticol 1 ParoRoxanaAnaHociungPas encore d'évaluation
- Dental and Oral Complications of Lip and Tongue Piercings: PracticeDocument4 pagesDental and Oral Complications of Lip and Tongue Piercings: Practiceshawn mary abrahamPas encore d'évaluation
- Odontogenic Maxillary Sinusitis - Need For Multidisciplinary Approach - A ReviewDocument6 pagesOdontogenic Maxillary Sinusitis - Need For Multidisciplinary Approach - A ReviewInternational Organization of Scientific Research (IOSR)Pas encore d'évaluation
- Malignant Vs Traumatic Tongue Ulcer A Clinical AppDocument6 pagesMalignant Vs Traumatic Tongue Ulcer A Clinical Appvivi hutabaratPas encore d'évaluation
- Median Rhomboid Glossitis in A Patient Undergoing Orthodontic TreatmentDocument4 pagesMedian Rhomboid Glossitis in A Patient Undergoing Orthodontic Treatmentandreia ichimPas encore d'évaluation
- Angular Cheilitis Guide: Causes, Symptoms & TreatmentDocument3 pagesAngular Cheilitis Guide: Causes, Symptoms & TreatmentNur Sita DewiPas encore d'évaluation
- Pattern of Dental Caries in Mulago Dental School Clinic, UgandaDocument4 pagesPattern of Dental Caries in Mulago Dental School Clinic, UgandaNeil DolendoPas encore d'évaluation
- Oral Frictional HyperkeratosisDocument15 pagesOral Frictional HyperkeratosisFajarRahmantiyoPas encore d'évaluation
- Journal of Advanced Clinical and Research InsightsDocument3 pagesJournal of Advanced Clinical and Research InsightsAninda Wulan PradaniPas encore d'évaluation
- Oral Pemphigus Vulgaris: A Case Report With Review of The LiteratureDocument4 pagesOral Pemphigus Vulgaris: A Case Report With Review of The LiteratureDhilah Harfadhilah FakhirahPas encore d'évaluation
- Long-Standing Oral Ulcers: Proposal For A New S-C-D Classification System'Document14 pagesLong-Standing Oral Ulcers: Proposal For A New S-C-D Classification System'Tegar Subeqi MochammadPas encore d'évaluation
- LabiopalatoschisisDocument21 pagesLabiopalatoschisisOna AkyuwenPas encore d'évaluation
- Ndodontic Iagnosis: by Clifford J. Ruddle, D.D.SDocument10 pagesNdodontic Iagnosis: by Clifford J. Ruddle, D.D.Srojek63Pas encore d'évaluation
- Candida-Associateddenturestomatitis - Aetiologyand Management: Areview - Part2.Oraldiseasescausedby Candida SpeciesDocument7 pagesCandida-Associateddenturestomatitis - Aetiologyand Management: Areview - Part2.Oraldiseasescausedby Candida SpeciesDentist HerePas encore d'évaluation
- Oral Ulcer Diseases DDDocument7 pagesOral Ulcer Diseases DDAmbar ZenPas encore d'évaluation
- Noma امجد حمزة عبد حسينDocument8 pagesNoma امجد حمزة عبد حسينSaif HaiderPas encore d'évaluation
- CleftLip-StatPearls-NCBIBookshelfDocument6 pagesCleftLip-StatPearls-NCBIBookshelfDébora QuagliatoPas encore d'évaluation
- Ijgmp - Assessment of Complications Occurring After Third Molar Removal in Specialized Dental Centre, KFH, Medina, Ksa A Retrospective StudyDocument8 pagesIjgmp - Assessment of Complications Occurring After Third Molar Removal in Specialized Dental Centre, KFH, Medina, Ksa A Retrospective Studyiaset123Pas encore d'évaluation
- 20231126-17335-15l8m04Document4 pages20231126-17335-15l8m04chd9r5hr5kPas encore d'évaluation
- Dental TrumaDocument26 pagesDental TrumaAseelPas encore d'évaluation
- Covid-19 Impact An Oral Health With A Focus On Temporomandibular Joint DisordersDocument5 pagesCovid-19 Impact An Oral Health With A Focus On Temporomandibular Joint Disordersbotak berjamaahPas encore d'évaluation
- Applied Sciences: The Pseudolesions of The Oral Mucosa: Di Diagnosis and Related Systemic ConditionsDocument8 pagesApplied Sciences: The Pseudolesions of The Oral Mucosa: Di Diagnosis and Related Systemic Conditionssiti baiq gadishaPas encore d'évaluation
- Compound Odontoma Associated With Impacted Teeth: A Case ReportDocument4 pagesCompound Odontoma Associated With Impacted Teeth: A Case ReportayuandraniPas encore d'évaluation
- Squamous Cell Carcinoma of The Mandibular Gingiva: Pei-Yu Li, DDS Ling Auyeung, DDS, MS Shun-Chen Huang, MDDocument5 pagesSquamous Cell Carcinoma of The Mandibular Gingiva: Pei-Yu Li, DDS Ling Auyeung, DDS, MS Shun-Chen Huang, MDtsntiPas encore d'évaluation
- Dental Trauma Due To Intubating During General Anaesthesia Incidencerisks Factors and PreventionDocument5 pagesDental Trauma Due To Intubating During General Anaesthesia Incidencerisks Factors and PreventionAnaPas encore d'évaluation
- Frictional Keratoses On The Facial Attached Gingiva Are Rare Clinical Findings and Do Not Belong To The Category of LeukoplakiaDocument8 pagesFrictional Keratoses On The Facial Attached Gingiva Are Rare Clinical Findings and Do Not Belong To The Category of LeukoplakiaShinta PurnamasariPas encore d'évaluation
- Ped. Dent, Pub. Health (2) - 6 - Management of Traumatic Dental InjuriesDocument30 pagesPed. Dent, Pub. Health (2) - 6 - Management of Traumatic Dental InjuriesEslam HafezPas encore d'évaluation
- Meta-Analisis of The Etiology of Odontogenic Maxillary SinusitisDocument4 pagesMeta-Analisis of The Etiology of Odontogenic Maxillary SinusitisSari Yanti MatsyahPas encore d'évaluation
- Care Plan Michael ValenciaDocument9 pagesCare Plan Michael Valenciaapi-643725836Pas encore d'évaluation
- Management of Third Molar Surgery in HIV Positive PatientsDocument4 pagesManagement of Third Molar Surgery in HIV Positive Patientskiara wardanaPas encore d'évaluation
- Flaitz11 00Document2 pagesFlaitz11 00caduceus001Pas encore d'évaluation
- Tongue Piercing and Associated Oral and Dental ComplicationsDocument6 pagesTongue Piercing and Associated Oral and Dental ComplicationsJihan_Johari_8053Pas encore d'évaluation
- 7 L0910 - ENG - 4year - VIIISemester - VNicolaiciucDocument16 pages7 L0910 - ENG - 4year - VIIISemester - VNicolaiciucShany SchwarzwaldPas encore d'évaluation
- Multidisciplinary Treatment in Cleft Lip and Palate PatientsDocument13 pagesMultidisciplinary Treatment in Cleft Lip and Palate PatientsDiana PredaPas encore d'évaluation
- Denture Stomatitis CausesDocument4 pagesDenture Stomatitis CausesDentist HerePas encore d'évaluation
- Oral Squamous Cell Carcinoma Clinical Aspects: March 2012Document27 pagesOral Squamous Cell Carcinoma Clinical Aspects: March 2012Anh TranPas encore d'évaluation
- Macroglossia PDFDocument7 pagesMacroglossia PDFpaolaPas encore d'évaluation
- Oralfistulasintech PDFDocument30 pagesOralfistulasintech PDFAndra MahyuzaPas encore d'évaluation
- Handbook of Oral Diseases 1 Edition PDFDocument449 pagesHandbook of Oral Diseases 1 Edition PDFEdgar Trujillo Benítez88% (8)
- Dentigerous Cyst: A Retrospective Study of 20 Cases in S. S. Medical College Rewa, Madhya PradeshDocument4 pagesDentigerous Cyst: A Retrospective Study of 20 Cases in S. S. Medical College Rewa, Madhya PradeshnjmdrPas encore d'évaluation
- Treatment of Lingual Traumatic Ulcer Accompanied With Fungal InfectionsDocument5 pagesTreatment of Lingual Traumatic Ulcer Accompanied With Fungal InfectionsYuganya SriPas encore d'évaluation
- L T O P: Eukemia: He Ral ErspectiveDocument2 pagesL T O P: Eukemia: He Ral ErspectiveLiana OpriţăPas encore d'évaluation
- Etiology and Occurrence of Gingival Recession - An Epidemiological Study - ScienceOpenDocument13 pagesEtiology and Occurrence of Gingival Recession - An Epidemiological Study - ScienceOpen61msdcPas encore d'évaluation
- Primary Gingival Squamous Cell CarcinomaDocument7 pagesPrimary Gingival Squamous Cell CarcinomaMandyWilsonPas encore d'évaluation
- Maxillofacial Trauma: Child DevelopmentDocument8 pagesMaxillofacial Trauma: Child DevelopmentAchmadArifinPas encore d'évaluation
- Oral Health in Children With Leukemia: Review ArticleDocument8 pagesOral Health in Children With Leukemia: Review ArticleNindy TweelingenPas encore d'évaluation
- Endo-Perio LesionsDocument16 pagesEndo-Perio LesionsFathima ShaminPas encore d'évaluation
- Open Bite: A Review of Etiology and Management: Peter Ngan, DMD Henry W. Fields, DDS, MS, MSDDocument8 pagesOpen Bite: A Review of Etiology and Management: Peter Ngan, DMD Henry W. Fields, DDS, MS, MSDAzi Pertiwi HussainPas encore d'évaluation
- Zabokova Bilbilova2014Document8 pagesZabokova Bilbilova2014Mairen RamirezPas encore d'évaluation
- Prevalence and Sex Distribution of Oral Lesions in Patients Attending an Oral Diagnosis ClinicDocument7 pagesPrevalence and Sex Distribution of Oral Lesions in Patients Attending an Oral Diagnosis ClinicDimaz ImanPas encore d'évaluation
- Periodontal Root Coverage: An Evidence-Based Guide to Prognosis and TreatmentD'EverandPeriodontal Root Coverage: An Evidence-Based Guide to Prognosis and TreatmentPas encore d'évaluation
- Traumatic Oral Lesions: A ReviewDocument6 pagesTraumatic Oral Lesions: A ReviewAuliapratiwi13Pas encore d'évaluation
- 1.POWDER-CAIR RASIO DAN SIFAT DUA RestoratifDocument5 pages1.POWDER-CAIR RASIO DAN SIFAT DUA RestoratifAuliapratiwi13Pas encore d'évaluation
- 1.POWDER-CAIR RASIO DAN SIFAT DUA RestoratifDocument5 pages1.POWDER-CAIR RASIO DAN SIFAT DUA RestoratifAuliapratiwi13Pas encore d'évaluation
- 5035 9731 1 SMDocument8 pages5035 9731 1 SMAuliapratiwi13Pas encore d'évaluation
- 1409576673037Document85 pages1409576673037Auliapratiwi13Pas encore d'évaluation
- 1409576673037Document85 pages1409576673037Auliapratiwi13Pas encore d'évaluation
- 1409576673037Document85 pages1409576673037Auliapratiwi13Pas encore d'évaluation
- 1409576673037Document85 pages1409576673037Auliapratiwi13Pas encore d'évaluation
- 1409576673037Document85 pages1409576673037Auliapratiwi13Pas encore d'évaluation
- 1409576673037Document85 pages1409576673037Auliapratiwi13Pas encore d'évaluation
- 1409576673037Document85 pages1409576673037Auliapratiwi13Pas encore d'évaluation
- Hypodontia Classification, Prevalence, and TreatmentDocument9 pagesHypodontia Classification, Prevalence, and TreatmentViral Parekh100% (1)
- Lived Experiences of Elementary Teachers in A Remote School in Samar, PhilippinesDocument14 pagesLived Experiences of Elementary Teachers in A Remote School in Samar, Philippinesルイス ジャンPas encore d'évaluation
- The Human Element is Critical in Personal SellingDocument18 pagesThe Human Element is Critical in Personal SellingArsalan AhmedPas encore d'évaluation
- GSM ZTE Paging Feature GuideDocument17 pagesGSM ZTE Paging Feature Guidemikepadilla82100% (1)
- Bible Study RisksDocument6 pagesBible Study RisksVincentPas encore d'évaluation
- Sengoku WakthroughDocument139 pagesSengoku WakthroughferdinanadPas encore d'évaluation
- ET's and Aliens: Problems of Exopolitics - Dec 2009Document8 pagesET's and Aliens: Problems of Exopolitics - Dec 2009Alex KochkinPas encore d'évaluation
- Bruno Latour: What Is Iconoclash?Document3 pagesBruno Latour: What Is Iconoclash?Clara HabibPas encore d'évaluation
- TOS and CID FORM-TLE 8 ANIMATIONDocument80 pagesTOS and CID FORM-TLE 8 ANIMATIONAriel AntaboPas encore d'évaluation
- Christian Appraisal of Feminist Ideologies Among Nigerian Women 2020Document78 pagesChristian Appraisal of Feminist Ideologies Among Nigerian Women 2020Nwaozuru JOHNMAJOR ChinecheremPas encore d'évaluation
- Soal Paket 1Document10 pagesSoal Paket 1Nurul HayatiPas encore d'évaluation
- APCHG 2019 ProceedingsDocument69 pagesAPCHG 2019 ProceedingsEnrico SocoPas encore d'évaluation
- Liquid Hydrogen As A Propulsion Fuel, 1945-1959Document341 pagesLiquid Hydrogen As A Propulsion Fuel, 1945-1959Bob AndrepontPas encore d'évaluation
- Policy Guidelines On Classroom Assessment K12Document88 pagesPolicy Guidelines On Classroom Assessment K12Jardo de la PeñaPas encore d'évaluation
- Fractional GradingDocument7 pagesFractional Gradingapi-355619062Pas encore d'évaluation
- Futurology and EducationDocument32 pagesFuturology and EducationMuhammad Abubakar100% (1)
- CHEST 6. Chest Trauma 2022 YismawDocument61 pagesCHEST 6. Chest Trauma 2022 YismawrobelPas encore d'évaluation
- 2018 World Traumatic Dental Injury Prevalence and IncidenceDocument16 pages2018 World Traumatic Dental Injury Prevalence and IncidencebaridinoPas encore d'évaluation
- Chapter 11, 12 Curve Tracing and EnvelopeDocument37 pagesChapter 11, 12 Curve Tracing and EnvelopeNitish PokhrelPas encore d'évaluation
- Readingdev 7Document2 pagesReadingdev 7api-190328610Pas encore d'évaluation
- Longman - New Total English Elementary Video BankDocument26 pagesLongman - New Total English Elementary Video Bankyuli100% (1)
- Due process violation in granting relief beyond what was prayed forDocument2 pagesDue process violation in granting relief beyond what was prayed forSam LeynesPas encore d'évaluation
- Muhammad v. Hall, 10th Cir. (2017)Document12 pagesMuhammad v. Hall, 10th Cir. (2017)Scribd Government DocsPas encore d'évaluation
- Physical Education For Class - 11thDocument19 pagesPhysical Education For Class - 11thdjjagu908Pas encore d'évaluation
- Silvianita - LK 0.1 Modul 2 English For Personal CommunicationDocument3 pagesSilvianita - LK 0.1 Modul 2 English For Personal CommunicationSilvianita RetnaningtyasPas encore d'évaluation
- EY The Cfo Perspective at A Glance Profit or LoseDocument2 pagesEY The Cfo Perspective at A Glance Profit or LoseAayushi AroraPas encore d'évaluation
- Contemporary Philippine Arts From The RegionsDocument29 pagesContemporary Philippine Arts From The RegionsDina Ilagan50% (2)
- Three Phase Transformer Model For TransientsDocument10 pagesThree Phase Transformer Model For TransientsYeissonSanabriaPas encore d'évaluation
- Philhis Handouts Week 1Document5 pagesPhilhis Handouts Week 1Jeen JeenPas encore d'évaluation
- 6 Strategies For Effective Financial Management Trends in K12 SchoolsDocument16 pages6 Strategies For Effective Financial Management Trends in K12 SchoolsRainiel Victor M. CrisologoPas encore d'évaluation