Académique Documents
Professionnel Documents
Culture Documents
Concept Map Care Plan Kvalen2
Transféré par
api-302336744Description originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Concept Map Care Plan Kvalen2
Transféré par
api-302336744Droits d'auteur :
Formats disponibles
Kristina Valenzuela
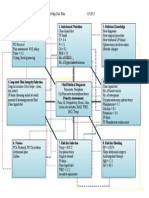
Concept Map Care Plan
Desired Outcomes
Pain
1. Patient reports satisfactory pain
control at a level less than 3/10 by
end of shift.
11/13/15
Interventions
Pain
1. Complete a pain assessment.
Assessment revealed patient stating
pain level 6/10, sharp to surgical
incision, crying and grimacing,
This outcome was met because the
made worse by deep breathing
patient's pain was well-controlled
2. Monitor possible PCA
during the shift and reported at a level
complications.
of 2/10 after all interventions were
Patient showed no signs of
implemented.
excessive sedation, respiratory
distress or urinary retention. Patient
did experience nausea.
3. Provide rest periods to facilitate
comfort, sleep and relaxation.
Patient care was grouped in the AM
in order to allow for adequate rest.
Patient was able to take a nap
during the clinical shift.
4. Administer PO opioid analgesics if
PCA ineffective.
PO Percocet was given to patient.
5. Evaluate effectiveness of pain
medication.
Medication was effective in
relieving pain to 2/10 as stated by
the patient.
6. Educate patient on s/s of PCA
complications.
Patient was able to verbalize
understanding of teaching.
Imbalanced Nutrition
Imbalanced Nutrition
1. Patient weighs within 10% of
1. Monitor lab values that indicate
admission weight by discharge.
nutritional well-being or
deterioration.
This outcome was partially met because
Lab values showed decreased
lab values improved (although still
potassium, calcium and
below expected limits) and patient was
phosphorous levels.
increasing intake, but I was unable to
2. Consult a dietitian for assessment
determine whether her current weight
and recommendations regarding
was within 10% of her admission
nutritional support.
weight.
A dietary consult was performed
and the patient's diet was changed
from NPO to Clear Liquids to Soft
Foods.
3. Encourage PO intake.
Kristina Valenzuela
Concept Map Care Plan
Deficient Knowledge
1. Patient verbalizes understanding of
desired content and ability to
perform home care by end of shift.
This outcome was met because the
patient was able to verbalize
understanding of specific discharge
instructions related to a splenectomy
and pancreatectomy.
11/13/15
With each subsequent meal, the
patient was able to consume a
greater amount
4. Administer antiemetic if needed.
The patient did not want to eat
breakfast because she was feeling
nauseous, so the RN administered
an antiemetic to make her feel
better.
5. Provide education on food choices
to increase electrolyte levels.
Patient verbalized understanding of
teaching and demonstrated
appropriate food choices to increase
electrolyte levels such as a banana
and milk.
6. Measure weight and height.
I was unable to obtain current
weight and height measurements
for this patient.
Deficient Knowledge
1. Assess the patient's understanding
of the procedure and implications
on health care.
The patient demonstrated some
knowledge about the surgical
procedure and lifestyle changes
needed after discharge.
2. Assess the motivation and
willingness of the patient and
caregivers to learn.
The patient and a family member
were present for the teaching and
were very attentive and interested to
learn.
3. Provide a quiet atmosphere without
interruption.
While I provided my own
education, and while the nurse
provided her discharge teaching and
the dietitian his dietary consult, the
patient's door remained closed to
ensure privacy and a calm, quiet
environment.
4. Provide information using various
media.
Kristina Valenzuela
Concept Map Care Plan
11/13/15
In addition to verbal instruction,
printed instructions were given to
the patient.
5. Use the teach-back technique to
determine the patient's
understanding of what was taught.
The patient was able to rephrase the
information accurately (ex. she
repeated food items that she was
restricted from eating, stated the s/s
of infection to report in relation to
splenectomy).
6. Teach the patient home care
instructions after splenectomy and
pancreatectomy: consuming a lowfat diet, how to perform wound
care, no lifting more than 10 lbs for
6 weeks, showering is acceptable,
bowel function should return in 1-2
days, seek medical attention for any
s/s of infection (fever, wound
drainage, redness in incision,
unusual pain in incision, absence of
bowel movements).
The patient verbalized
understanding of all teaching.
Impaired Skin Integrity
1. Patient shows no signs of skin
breakdown by end of shift.
This outcome was met because the
patient showed no signs of skin
breakdown during my shift.
Impaired Skin Integrity/Infection
1. Assess the general condition of the
skin.
Patient's skin had good turgor, was
warm and dry to touch, had quick
cap refill, and revealed no s/s of
infection to surgical site, skin wellapproximated and covered with
Steri-strips
2. Assess the patient's ability to move.
The patient is able to independently
turn in bed and can ambulate
without assistance.
3. Encourage ambulation if able.
The patient is ambulatory and walks
through the hall several times a day.
4. Ensure adequate nutrition and
hydration.
The patient was originally on NPO
Kristina Valenzuela
Concept Map Care Plan
11/13/15
status, then changed to Clear liquids
and Soft food diet during the 2 days
I provided care. During that time, I
encourage PO intake, and the
patient was able to eat consume
larger portions with each
subsequent meal.
5. Provide wound care.
The RN performed dressing
changes per facility protocol in
order to decrease the risk of
infection.
6. Educate patient on s/s of infection.
The patient verbalized
understanding of the teaching.
Fluid/Electrolyte Imbalance
Fluid/Electrolyte Imbalance
1. Patient will maintain normal serum
1. Assess for clinical conditions or
electrolyte balance as evidenced by
situations associated with
electrolyte levels within expected
electrolyte imbalances.
ranges by discharge.
Patient was on an NPO, then clear
liquid diet. She also had a JP drain,
This outcome was partially met because
history of cancer and s/p
only potassium levels had normalized
splenectomy and pancreatectomy.
prior to discharge.
2. Monitor serum electrolyte levels.
The patient's potassium (3.4),
phosphorous (2.1) and calcium
(8.1) were decreased.
3. Administer balanced electrolyte IV
solutions as prescribed.
In the days prior to my date of care,
the patient was on continuous IV
infusion of NS.
4. Administer electrolyte replacements
as prescribed.
RN administered an IV
phosphorous replacement x2.
5. Teach the patient about dietary
sources of electrolytes.
I provided suggestions on foods to
eat containing the deficient
electrolytes such as green, leafy
vegetables and bananas.
6. Teach the patient to report s/s of
hypokalemia: dysrhythmias,
weakness, fatigue, muscle cramps.
Patient verbalized understanding of
Kristina Valenzuela
Concept Map Care Plan
Nausea
1. Patient does not experience any
episodes of nausea by end of shift.
This outcome was met because the
patient did not experience any further
episodes of nausea after all
interventions were implemented.
Risk for Infection
1. Patient remains free of infection by
end of shift.
This outcome was met because the
patient remained free of any s/s of
infection during my shift.
11/13/15
teaching.
Nausea
1. Assess for the cause of nausea.
Patient had PCA Fentanyl and
taking PO Percocet, two
medications that could cause
nausea.
2. Assess the patient's hydration status
since dehydration can cause nausea.
The patient's BP was within normal
limits, intake was less than output at
this time, and skin turgor was
normal.
3. Administer antiemetics as ordered.
RN administered Zofran IV push.
4. Keep an emesis basin within easy
reach of the patient.
Emesis basin was placed on the
patient's bedside table.
5. Offer cold water or ice chips.
Patient accepted offer of ice chips.
6. Evaluate the patient's reponse to
antiemetics and interventions to
alleviate nausea.
Patient's nausea was resolved after
administration of medication.
Risk for Infection
1. Monitor the patient's temperature.
The patient's temperature remained
within normal limits.
2. Assess the surgical incision and
drain site for s/s of infection.
There was no redness, swelling,
drainage around the surgical
incision or drain site.
3. Assess the stability of tubes and
drains.
The patient's JP drain was patent
and properly secured and covered
with a dressing.
4. Wash hands before contact with the
postoperative patient.
I washed hands every time before
entering the patient's room.
5. Maintain aseptic technique during
dressing changes, wound care and
Kristina Valenzuela
Concept Map Care Plan
Risk for Bleeding
1. Patient does not experience
bleeding by end of shift.
This outcome was met because the
patient did not experience any bleeding
during my shift as evidenced by stable
H&H, BP and HR within normal limits,
and no physical evidence of bleeding.
11/13/15
manipulating the tubes.
I observed the RN who emptied the
drain maintain aseptic technique.
6. Teach patient s/s of infection: fever,
pain/redness/swelling/drainage at
incision or drain site.
Risk for Bleeding
1. Assess the patient's health history
for indications of conditions that
contribute to a risk for bleeding.
The patient had no relevant health
conditions that put her at risk for
bleeding.
2. Assess the patient's use of any
medications that can interfere with
hemostasis.
This patient was receiving Lovenox
injections as prophylaxis for DVT.
3. Monitor BP and HR. Observe for
signs of orthostatic hypotension.
The patient's BP and HR were
within normal limits. The patient
did not experience any
lightheadedness when changing
positions.
4. Assess skin and mucous
membranes for evidence of
bleeding.
The patient did not have any
petechiae, bruising, hematoma
formation or oozing of blood from
incision sites.
5. Monitor H&H.
The patient's H&H were within
normal limits.
6. Teach patient s/s of bleeding that
need to be reported: tachycardia,
hypotension, lightheadedness,
bruising, hematoma formation,
oozing of blood from incision site,
and saturated dressing.
Patient verbalized understanding of
teaching.
Kristina Valenzuela
Concept Map Care Plan
11/13/15
Discharge Plan/Patient Teaching
You will be discharged home.
You underwent a pancreatectomy, in which a portion of your pancreas was removed. Your
pancreas secretes enzymes that help with the digestion of food. It may function properly
since part of it has been removed so you will need to make changes to your diet.
You also underwent a splenectomy, in which your entire spleen was removed. Your
spleen acted as a filter for blood and helped your body fight infection. Now that it has
been removed, you are at greater risk for infection.
Activity should be limited for the first 6 weeks. Do not lift anything heavier than 10
pounds. Ensure adequate rest periods and gradually increase activity and ambulation each
day.
Steri-strips have been placed over your surgical incision. It is ok to shower and cleanse
with mild soap but do not soak incision in the tub. The strips will fall off as your incision
heals (within 5-7 days). Avoid applying creams, lotions or powder to the incision. Your
drain site has been covered with a dry dressing. You need to change the dressing once a
day or if it becomes loose or soiled. When changing the dressing, cleanse with mild soap
and water, dry, then apply the dry dressing and secure with tape. If you notice any
redness, swelling or drainage around the incision, notify your doctor immediately.
You will need to restrict your diet to a low-sugar, low-fat diet. Refer to the dietary
handout given to you by the dietitian for a list of foods you can and cannot eat.
You will be given a stool softener commonly known as Colace. Take 1 cap by mouth
once a day to help with constipation, which is common for several days following
surgery. You will also be given a pain medication commonly known as Percocet. Take as
prescribed. Take 2 tabs by mouth every 6 hours as needed for pain.
Follow up with your doctor in 1 week. Since you are at greater risk for infection, seek
medical attention even for mild illnesses such as colds and sinus problems. Talk to your
doctor about the types of vaccinations you should receive. Be sure to tell all your
healthcare providers that you do not have a spleen. Consider getting a medical
identification bracelet stating you do not have a spleen.
Seek immediate medical attention if you have a fever greater than 100.4 degrees
Fahrenheit, signs and symptoms of incisional infection, bleeding, worsening or
uncontrolled abdominal pain, dizziness or lightheadedness, or an incision site that opens
up or pulls apart.
Vous aimerez peut-être aussi
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- Ingredients: Ep 18 - Rhubarb Trifle With Champagne Jelly and MascarponeDocument6 pagesIngredients: Ep 18 - Rhubarb Trifle With Champagne Jelly and Mascarponegrupo077Pas encore d'évaluation
- Christians, Let Us Love One AnotherDocument2 pagesChristians, Let Us Love One AnotherGillie Caparas100% (1)
- The Spirit of Christmas Cookbook PDFDocument178 pagesThe Spirit of Christmas Cookbook PDFAna OmicevicPas encore d'évaluation
- EF3e Elem Progresstest 7 12 AnswerkeyDocument8 pagesEF3e Elem Progresstest 7 12 AnswerkeyCarlos Júlio92% (13)
- Management Style AssessmentDocument3 pagesManagement Style Assessmentapi-302336744Pas encore d'évaluation
- Tcs Ninja NQT Previous Year PapersDocument210 pagesTcs Ninja NQT Previous Year PapersVellasamy karthickPas encore d'évaluation
- Inverse VariationDocument4 pagesInverse Variationrotshen casilac100% (1)
- Common Mistakes in English GrammarDocument12 pagesCommon Mistakes in English GrammarSaid Halilovic50% (2)
- RUSAYL TenantDirectory Eng 02-12-2022Document41 pagesRUSAYL TenantDirectory Eng 02-12-2022Joseph AugustinePas encore d'évaluation
- n320 GDM Teaching BrochureDocument2 pagesn320 GDM Teaching Brochureapi-302336744Pas encore d'évaluation
- Detailed Lesson Plan in Tle Kitchen Utensils and EquipmentDocument7 pagesDetailed Lesson Plan in Tle Kitchen Utensils and EquipmentAprildhee Del Mundo Peña81% (88)
- Kvalenzuela ResumeDocument2 pagesKvalenzuela Resumeapi-302336744Pas encore d'évaluation
- Wse Week5Document4 pagesWse Week5api-302336744Pas encore d'évaluation
- n360 PR KvalenDocument10 pagesn360 PR Kvalenapi-302336744Pas encore d'évaluation
- Kristina VDocument1 pageKristina Vapi-302336744Pas encore d'évaluation
- Kvalen Leadership DiscussionDocument3 pagesKvalen Leadership Discussionapi-302336744Pas encore d'évaluation
- Community Case Study 3Document2 pagesCommunity Case Study 3api-302336744Pas encore d'évaluation
- Community Case StudyDocument9 pagesCommunity Case Studyapi-302336744Pas encore d'évaluation
- Bristol Hospice Elearner TranscriptDocument1 pageBristol Hospice Elearner Transcriptapi-302336744Pas encore d'évaluation
- Ethics PresentationDocument12 pagesEthics Presentationapi-285033848Pas encore d'évaluation
- n320 Kvalen Community ResourceDocument5 pagesn320 Kvalen Community Resourceapi-302336744Pas encore d'évaluation
- Kvalen QipresentationDocument9 pagesKvalen Qipresentationapi-302336744Pas encore d'évaluation
- Concept Map Care Plan Kvalen3Document1 pageConcept Map Care Plan Kvalen3api-302336744Pas encore d'évaluation
- PDP KvalenDocument3 pagesPDP Kvalenapi-302336744Pas encore d'évaluation
- Eloor Industrial Health Study - Research Adviser-Dr. Rajan R PatilDocument27 pagesEloor Industrial Health Study - Research Adviser-Dr. Rajan R PatilDr. Rajan R PatilPas encore d'évaluation
- Anemia: Dr. Tutik Harjianti, SP PDDocument47 pagesAnemia: Dr. Tutik Harjianti, SP PDsujidahPas encore d'évaluation
- Here, There and Everywhere: Unit 5Document10 pagesHere, There and Everywhere: Unit 5Bernabé Hernández MoguelPas encore d'évaluation
- Periodical Test English 6Document3 pagesPeriodical Test English 6Clifton MillerPas encore d'évaluation
- Finalprogram V4Document4 pagesFinalprogram V4MarkYamaPas encore d'évaluation
- The Fruit of Ancient PersiaDocument12 pagesThe Fruit of Ancient PersiaRafael Esteban Benitez AvendanoPas encore d'évaluation
- MicroPro Grill Recipes 2020Document85 pagesMicroPro Grill Recipes 2020Jayme-Lea VanderschootPas encore d'évaluation
- Mapping of Significant Natural Resources: Category: Plants (Flora)Document5 pagesMapping of Significant Natural Resources: Category: Plants (Flora)Dei HernandezPas encore d'évaluation
- Perten Falling Number FN SeriesDocument28 pagesPerten Falling Number FN SeriesOSMANPas encore d'évaluation
- PHE Preparation of Samples and Dilutions Plating and Sub-Culture PDFDocument21 pagesPHE Preparation of Samples and Dilutions Plating and Sub-Culture PDFdr Alex stanPas encore d'évaluation
- D7024 Completo EspañolDocument80 pagesD7024 Completo Españolluisruizch100% (4)
- Zdocs - Ro - Marine Exporters List India DirectoryxlsxDocument408 pagesZdocs - Ro - Marine Exporters List India DirectoryxlsxKRA SCS IndiaPas encore d'évaluation
- Design and Fabrication of Paddy Cleaning MachineDocument5 pagesDesign and Fabrication of Paddy Cleaning MachineDave RonePas encore d'évaluation
- DLL - Mapeh 3 - Q1 - W9Document2 pagesDLL - Mapeh 3 - Q1 - W9Rucelle Mae Fernandez ArbolerasPas encore d'évaluation
- Aloo GobiDocument2 pagesAloo GobiimyashPas encore d'évaluation
- OIV Annual Assessment-2023Document30 pagesOIV Annual Assessment-2023fanghao19980816Pas encore d'évaluation
- Preparation of Buffer Solutions - Pharmaceutical GuidelinesDocument3 pagesPreparation of Buffer Solutions - Pharmaceutical GuidelinesRavi RamgarhiaaPas encore d'évaluation
- 4ds0315e P2 (F)Document1 page4ds0315e P2 (F)nagravPas encore d'évaluation
- A Study On The Demographic Profile of The Fast Food Consumers in IndiaDocument4 pagesA Study On The Demographic Profile of The Fast Food Consumers in IndiaMadMix NBPas encore d'évaluation
- Jalgaon IIDocument9 pagesJalgaon IIRam K YadavPas encore d'évaluation
- Menu DietDocument11 pagesMenu DietKrisnaPas encore d'évaluation