Académique Documents
Professionnel Documents
Culture Documents
Cancer 2001 Hoos 869 74
Transféré par
Charles J. DiComo, PhDTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Cancer 2001 Hoos 869 74
Transféré par
Charles J. DiComo, PhDDroits d'auteur :
Formats disponibles
869
High Ki-67 Proliferative Index Predicts Disease Specic Survival in Patients with High-Risk Soft Tissue Sarcomas
Axel Hoos, M.D., Ph.D.1 Alexander Stojadinovic, M.D.1 Stephen Mastorides, M.D.2 Marshall J. Urist, B.S.2 David Polsky, M.D., Ph.D.2 Charles J. Di Como, Ph.D.2 Murray F. Brennan, M.D.1 Carlos Cordon-Cardo, M.D., Ph.D.2
1
Department of Surgery, Memorial Sloan-Kettering Cancer Center, New York, New York. Department of Pathology, Memorial Sloan-Kettering Cancer Center, New York, New York.
Supported by National Institutes of Health Grant CA-47179. The authors thank the following collaborators for their continuous support: Denis H. Y. Leung, Ph.D. for statistical analyses, Maria E. Dudas for immunohistochemistry, James D. Woodruff, M.D., and Cristina R. Antonescu, M.D. for conrmation of histopathologic diagnoses. Stephen Mastoridess current address: Department of Pathology, James Haley Veterans Hospital, Tampa, Florida. Address for reprints: Carlos Cordon-Cardo, M.D., Ph.D., Department of Pathology, Memorial SloanKettering Cancer Center, New York, NY 10021; Fax: (212)794-3186; E-mail: cordon-c@mskcc.org Received February 26, 2001; revision received May 8, 2001; accepted May 14, 2001. 2001 American Cancer Society
BACKGROUND. Soft tissue sarcomas (STSs) are heterogeneous neoplasms that have variable clinical outcome. Several clinical parameters and few molecular markers, including Ki-67 proliferative index, have been shown to correlate with patient prognosis. To the authors knowledge, no denitive report exists to identify one molecular marker that can be analyzed easily in a clinical setting and that predicts survival in a cohort of patients with high-risk STS of identical clinical characteristics but variable outcome. METHODS. The inuence of clinical prognostic factors was eliminated by selecting two patient groups with identical high-risk characteristics: large ( 10 cm), highgrade, deep, completely resected primary extremity STS (n 47). Patients in the rst group remained disease free (no evidence of disease [NED]) after primary tumor treatment (n 19), whereas patients in the second group subsequently died of disease (DOD; n 28). Triplicate 0.6-mm core biopsies from dened morphologic areas of parafn embedded primary tumors were assembled on a tissue microarray and analyzed by immunohistochemistry with the MIB-1 antibody, and Ki-67 proliferative indices were correlated with patient outcome. RESULTS. High Ki-67 proliferative index, dened as greater than 30% tumor cells showing nuclear immunoreactivity, was signicantly more frequent in the DOD group than in the NED group and was associated with tumor-related mortality (P 0.02). This marker identies an especially aggressive malignant phenotype within a cohort of high-risk tumors that is based on well established clinical and pathologic parameters alone and is easy to use in a clinical setting. CONCLUSIONS. On the basis of these data and previous reports, high Ki-67 proliferative index is suggested as a signicant factor for predicting the prognosis of patients with high-risk STS and should be evaluated prospectively based on clinical trials. Cancer 2001;92:869 74. 2001 American Cancer Society. KEYWORDS: immunohistochemistry, Ki-67, MIB-1, sarcoma, survival, prognosis.
oft tissue sarcomas (STSs) are a heterogeneous group of mesenchymal neoplasms with variable biologic behavior. Histologic grade, tumor size, depth, and status of surgical resection margins have been identied as clinical prognostic factors for STS.13 Because of their clinical relevance, grade, size, and depth form the basis for the clinical staging system of the American Joint Committee on Cancer (AJCC) of STS4 and can be used to identify patients at high risk to die of sarcoma. However, these prognostic variables do not explain the biologic differences in aggressiveness between STS of similar size, grade, and depth after complete tumor resection. Few molecular factors have been identied to correlate with prognosis of patients with STS, including Ki-67, among others.59
870
CANCER August 15, 2001 / Volume 92 / Number 4
Moreover, Ki-67 has been found to be associated with prognosis in STS in several independent studies.5,8,10 12 The Ki-67 antigen was rst described in 1983 as a nuclear protein associated with cellular proliferation.13 Further studies have shown that Ki-67 is expressed from early entrance into G1-phase throughout the cell cycle and that immunohistochemical staining correlates with the growth fraction of tumors.10,14,15 However, its functional signicance still remains unclear. Recent studies suggest Ki-67 to be involved in control and timing of mitosis.15,16 The monoclonal antibody MIB-1 frequently is used to detect Ki-67 in the nuclei of tumor cells on the basis of well established protocols.8,17 High Ki-67 proliferative index, the fraction of tumor cell nuclei above a dened threshold being positive for Ki-67, has been reported to correlate with prognosis of patients with various cancers.18 24 Despite promising results with Ki-67 proliferative index in sarcoma,5,8,11,12 no denitive study to our knowledge has validated the clinical relevance of Ki-67 for survival in a cohort of patients with high-risk STS of identical clinical characteristics but variable outcome. The main goal of the current study was to characterize the potential of Ki-67 proliferative index to discriminate patient survival in a cohort of clinical high-risk STSs. Specically, we analyzed two groups of carefully selected patients with large ( 10 cm), highgrade, deep, primary extremity sarcomas that have been completely resected and compared Ki-67 proliferative indices of patients who remained free of disease after treatment with those of patients who subsequently died of their disease.
disease. The rst group comprised 19 patients that remained free of disease (no evidence of disease [NED]) after primary treatment. The second group contained 28 patients that developed local recurrence and/or metastatic disease and subsequently died of their disease (died of disease [DOD]). All patients presented to MSKCC with primary disease only. All patients received surgical resection of the primary tumor. Some received neoadjuvant/ adjuvant chemotherapy/radiation at the discretion of the Multidisciplinary Soft Tissue Sarcoma Group or as part of clinical trials. Patients were treated according to the standard of care at MSKCC. Disease specic survival was dened as time from primary tumor resection to death from disease. Local recurrence was dened as recurrence occurring more than 3 months after complete resection.
Tissues, Array Construction, and Immunohistochemistry
We performed analysis on formalin xed, parafn embedded tissue. Tissue sections of each specimen were stained with hematoxylin and eosin and evaluated by a reference pathologist (S.M.). All cases were reviewed to conrm the diagnosis of sarcoma, tumor grade, and quality of the tissue and to identify a representative area of the specimen. From these dened areas, core biopsies were taken with a precision instrument (Beecher Instruments, Silver Spring, MD), as previously described.27 Tissue cores with a dimension of 0.6 mm from each specimen were punched and arrayed in triplicate on a recipient parafn block.17 The tissue microarray technique was chosen because it allows for efcient analysis of multiple tumors and normal tissue controls on one parafn block and preserves a large portion of the tumor block for further analysis. As previously shown by us, triplicate 0.6-mm core biopsies from STS parafn embedded tissues for the construction of tissue microarrays has a 96% concordance rate between MIB-1 immunohistochemistry performed on sections from tissue microarrays and on standard full tissue sections.17 This makes the technique feasible for the described analysis. Five-micrometer sections of the tissue array block were cut and placed on charged polylysine coated slides. These sections were used for immunohistochemical analysis.28 Sarcomas known to be strongly positive for Ki-67 were used as positive controls. Arrayed normal tissues served as negative controls. Sections from tissue arrays were deparafnized, rehydrated in graded alcohols, and processed using the avidin-biotin immunoperoxidase method. Briey, sections were incubated in preheated 0.05% trypsin, 0.05% CaCl2 in 0.05M Tris-HCl (pH 7.6) for 5 minutes at 37 C and then submitted
PATIENTS AND METHODS
Patients, Clinical, and Pathologic Parameters
The cohort analyzed consisted of two clinically well characterized, matched groups of patients (n 47) with large ( 10 cm), high-grade, deep primary extremity STSs that were completely resected. Histologic grade was dened based on the degree of tumor differentiation, cellularity, stroma, vascularity, necrosis, and mitoses.25,26 All patients were treated as inpatients at Memorial Sloan-Kettering Cancer Center (MSKCC) between January 1982 and January 1998 and were observed prospectively and entered into our sarcoma database. Median age of the patient cohort was 64 years (range, 27 87 years). Twenty-seven patients (57%) were male, and 20 were female (43%). Median follow-up for the patient cohort was 39 months (range, 7129 months). On the basis of their clinical characteristics, all patients in this study were at high risk to die of their
Ki-67 Proliferative Index in High-Risk Sarcoma/Hoos et al.
871
to antigen retrieval by microwave oven treatment for 15 minutes in 0.01 mM citrate buffer at pH 6.0. Slides subsequently were incubated in 5% normal horse serum for 30 minutes followed by MIB-1 antibody incubation overnight at 4 C (1:50; Immunotech, Marseille, France). Samples then were incubated with biotinylated anti-mouse immunoglobulins at 1:500 dilution (Vector Laboratories, Inc., Burlingame, CA) followed by avidinbiotin peroxidase complexes (1:25; Vector Laboratories, Inc.) for 30 minutes. Diaminobenzidine was used as the chromogen and hematoxylin as the nuclear counterstain. Immunoreactivity was classied as a continuum data (undetectable levels or 0% to homogeneous staining or 100%). Slides were reviewed by several investigators (C.C.-C., A.H., M.J.U.), and results were scored by estimating the percentage of tumor cells showing characteristic staining. The cutoff value used in this study was dened as follows: high proliferative Ki-67 index if greater than 30% tumor nuclei stained and low Ki-67 proliferative index if less than 30% tumor nuclei stained.
TABLE 1 Clinicopathologic Features of High-Risk Extremity Sarcoma (n 47) with P Values Demonstrating No Signicant Differences between the Two Groups
Variable Male gender 9 Age hrs, median 64 Presentation Bx/Inc. Exc. No prior Tx Site (extremity) Lower Upper Histopathology MFH LMS Lipo Fibro Size ( 10 cm) High grade 19 Deep depth 19 28 28 N/A 13 6 16 3 9 3 3 4 19 65 0.78 19 9 0.89 24 4 0.65 16 4 6 2 N/A 28 N/A 18 0.86 NED (n 19) DOD (n 28) P value 0.25
Statistical Analysis
Associations between clinicopathologic parameters and laboratory data were studied using Fisher exact test or chi-square test where appropriate.29 Survival analysis was performed by the method of Kaplan Meier30 and statistical signicance (P 0.05) evaluated by log-rank testing.31
Bx/Inc. Exc.: prior biopsy or incomplete excision; MFH: malignant brous histiocytoma; LMS: leiomyosarcoma; Lipo: liposarcoma; Fibro: brosarcoma.
TABLE 2 Treatment Characteristics of High-Risk Extremity Sarcoma (n 47), Demonstrating No Differences between the DOD and NED Group
Variable Primary procedure Resection Amputation Complete resection (yes) Adjuvant radiotherapy (yes) Adjuvant chemotherapy (yes)
N/A: not applicable.
RESULTS
Clinical and Pathologic Analyses
Median age of the patient cohort was 64 years (range, 27 87 years). Twenty-seven (57%) of patients were males, and 20 were females (43%). Samples were analyzed from 47 primary tumors. All lesions were large ( 10 cm), deep, high-grade extremity sarcomas that were completely resected at the time of primary surgery. Patients were grouped into two categories based on outcome alone. The rst group contained 19 patients that had no evidence of disease (NED) at last follow-up. The second group included 28 patients that died of disease (DOD). Patients with NED did not have any recurrences. There were no signicant differences between the study groups in terms of age, gender, primary presentation, site, histopathology, tumor size, grade, and depth. Table 1 shows the comparison between NED and DOD patients according to clinical and pathologic variables. All patients underwent complete tumor resection at time of primary surgery. Most (94%) of patients underwent limb-sparing resection; amputation was required in 3 (6%) cases on the basis of signicant
NED (n 19)
DOD (n 28)
P value 0.33
18 1 19 14 7
26 2 28 19 11
N/A 0.88 0.87
bone or neurovascular involvement by tumor that precluded complete functional limb-preserving resection. The proportion of patients receiving primary adjuvant chemoradiation therapy was similar between the two groups (Table 2). Median follow-up for the entire group at time of correlating laboratory results and clinicopathologic data was 39 months (range, 7129 months). The 3-year disease specic survival (DSS) rate of the entire cohort was 46%. Actuarial 5-year DSS rate was 35%. Median disease specic survival of patients in the NED group
872
CANCER August 15, 2001 / Volume 92 / Number 4
FIGURE 1. Representative photomicrograph of the immunophenotypes of a high-risk soft tissue sarcoma showing high Ki-67 proliferative index (quarter core from tissue array depicted in 400 magnication).
was 39.1 months and of patients in the DOD group was 17.8 months.
Ki-67 Proliferative Index and Survival in High-Risk Soft Tissue Sarcomas
Immunohistochemical staining showed high Ki-67 proliferative index in 4 tumors (21%) of patients that are free of disease (NED, n 19) as compared with 14 tumors (50%) of patients that died of disease (DOD, n 28). Low or no Ki-67 activity was observed in 15 sarcomas (79%) in the NED group and in 14 sarcomas (50%) in the DOD group. Most negative cases expressed Ki-67 below the cutoff value of 30%, and only 2 cases were truly negative, 1 in the DOD and 1 in the NED group. These two cases most likely expressed some low level Ki-67 ( 30%) that was not detected here because of the use of tissue microarrays.17 A representative immunophenotype of a sarcoma from the DOD patient group showing high nuclear expression of the Ki-67 antigen is shown in Figure 1. Patients who suffered tumor-related deaths had a signicantly higher proportion of tumor cell immunostaining for Ki-67 (50% DOD vs. 21% NED) than those who remain NED (P 0.04). Analysis of DSS revealed high Ki-67 proliferative index to be a signicant predictor of tumor-related mortality by univariate analysis (P 0.02). The 3-year DSS rate for patients with high Ki-67 proliferative index and low or no Ki-67 expression was 18% and 58%, respectively (Fig. 2).
FIGURE 2. KaplanMeier curve for disease specic survival of patients with
high-risk soft tissue sarcoma by Ki-67 proliferative index. High Ki-67 proliferative index was signicantly associated (P 0.02) with patients who had died of disease as compared with patients who have no evidence of disease at last follow-up.
DISCUSSION
Despite various efforts to improve treatment for human STSs, a subset of patients with this disease remains at high risk for tumor-related mortality. The main reason for this is the heterogeneity of STS as reected by variable biologic behavior. Clinical prognostic factors such as histologic grade, size, depth, and
status of surgical resection margins have been identied to better dene the risk of patients to die of disease and have been included in the AJCC classication of STS.1 4 However, within the high-risk group of patients with high-grade, large, deep sarcomas of the extremity that are completely resected clinically unpredictable differences in terms of patient outcome exist. Of the molecular markers that were analyzed with regard to their potential to predict outcome of sarcoma patients, the nuclear proliferation antigen Ki-67 has been suggested by several studies to be a promising candidate.5,8,10 12,3234 Initial reports on 34 and 46 cases showed a correlation between Ki-67 index, mitotic count, cellularity, and histologic grade of STS, suggesting it to be useful for grading and prognostication in this disease.10,11 In two studies from our institution on larger series of patients with STS that
Ki-67 Proliferative Index in High-Risk Sarcoma/Hoos et al.
873
were not matched with regard to clinical high-risk parameters (n 121 and 174), the prognostic implications of Ki-67 proliferative index were investigated. This showed a correlation between high Ki-67 proliferative index, occurrence of distant metastasis, and tumor-related mortality.5,8 This observation was conrmed by another report on 65 patients with STS showing the association of high Ki-67 proliferative index with poor overall survival.12 In these studies, Ki-67 proliferative index was dened as the percentage of tumor cell nuclei being positive for Ki-67 in relation to a cutoff value of 20 40%. To further characterize the clinical potential of Ki-67 as a molecular marker for disease specic survival in patients with high-risk STS, we selected a group of patients that remained free of disease (NED, n 19) after primary tumor treatment and compared the Ki-67 proliferative indices in these tumors with those of patients who subsequently died of their disease (DOD, n 28). The relatively small sample size of the two study groups (n 47), attributable to the few long-term disease free survivors with high-risk STS, is offset by the elimination of clinically relevant prognostic factors from the analysis, because both groups were matched for these critical clinicopathologic variables (Table 1). This allows for outcome analysis on the basis of Ki-67 proliferative index alone. This analysis was based on the tissue microarray technique for efcient evaluation of immunophenotypes in cancer tissues.27 We previously have validated this technique for its use in STS. This showed 96 98% concordance between triplicate core tissue array and full section immunohistochemistry (IHC) analyses and showed no signicant differences between survival analyses based on arrayderived data compared with regular full section IHCderived data.17 Expression of the Ki-67 antigen in tumor nuclei in our cohort of 47 high-risk STS showed high Ki-67 proliferative index to be a signicantly more frequent event in the DOD patient group. Clinicopathologic analyses revealed a signicant correlation between DSS and high Ki-67 proliferative index (P 0.02) (Fig. 2). The cutoff value in our study was 30% as suggested by the previous reports.5,8,12 This conrms the described relevance of Ki-67 for prediction of patient prognosis in STS and adds the important notion that high Ki-67 proliferative index allows for identication of patients with an especially aggressive tumor phenotype who cannot be identied based on well established clinical parameters alone. This suggests that high Ki-67 proliferative index may allow us to select patients with high-risk sarcomas for systemic adjuvant therapies and, more impor-
tantly, to avoid overtreatment of patients with less aggressive tumors within the high-risk patient group, reected by low Ki-67 proliferative index, and spare them from the side effects of aggressive, often not benecial, adjuvant therapy. In summary, this study further validates that high Ki-67 proliferative index is an independent prognostic marker for high-risk soft tissue sarcomas that identies patients with an especially aggressive tumor phenotype who cannot be identied based on well established clinical parameters alone. On the basis of our data and previous reports, high Ki-67 proliferative index may have potential for predicting the prognosis of patients with high-risk STS in a clinical routine setting and may be a useful addition to AJCC staging criteria for STS. This needs to be prospectively conrmed on the basis of clinical trials.
REFERENCES
1. Lewis JJ, Leung DHY, Casper ES, Woodruff J, Hajdu SI, Brennan MF. Multifactorial analysis of long-term follow-up (more than 5 years) of primary extremity sarcoma. Arch Surg 1999;134:190 4. 2. Brennan MF, Lewis JJ. Soft tissue sarcomas. In: Sabiston DC, editor. Textbook of surgerythe biological basis of modern surgical practice. 15th ed. New York: Saunders, 1996:528. 3. Levine EA. Prognostic factors in soft tissue sarcoma. Semin Surg Oncol 1999;17:2332. 4. Soft tissue sarcoma. AJCC cancer staging manual. 5th ed. Philadelphia: Lippincott, Williams & Wilkins, 1998:140 6. 5. Drobnjak M, Latres E, Pollack D, Karpeh M, Dudas M, Woodruff JM, et al. Prognostic implications of p53 nuclear overexpression and high proliferation index of Ki-67 in adult soft tissue sarcomas. J Natl Cancer Inst 1994;86:549 54. 6. Cordon-Cardo C, Latres E, Drobnjak M, Olivia MR, Pollack D, Woodruff JM, et al. Molecular abnormalities of mdm2 and p53 genes in adult soft tissue sarcoma. Cancer Res 1994;54:794 9. 7. Kim SH, Lewis JJ, Brennan MF, Woodruff JM, Dudas M, Cordon-Cardo C. Overexpression of cyclin D1 is associated with poor prognosis in extremity soft tissue sarcomas. Clin Cancer Res 1998;4:2377 82. 8. Heslin MJ, Cordon-Cardo C, Lewis JJ, Woodruff JM, Brennan MF. Ki-67 detected by MIB-1 predicts distant metastasis and tumor mortality in primary, high grade extremity soft tissue sarcoma. Cancer 1998;83:490 7. 9. Cance WG, Brennan MF, Dudas ME, Huang CM, CordonCrado C. Altered expression of the retinoblastoma gene product in human sarcomas. N Engl J Med 1990;323:1457 62. 10. Kroese MC, Rutgers DH, Wils IS, Van Unnik JA, Roholl PJ. The relevance of the DNA index and proliferation rate in the grading of benign and malignant soft tissue tumors. Cancer 1990;65:1782 8. 11. Ueda T, Aozasa K, Tsujimoto M, Ohsawa M, Uchida A, Aoki Y, et al. Prognostic signicance of Ki-67 reactivity in soft tissue sarcomas. Cancer 1989;63:1607-11. 12. Levine EA, Holzmayer T, Bacus S, Mechetner E, Mera R, Bollinger C, et al. Evaluation of newer prognostic markers for adult soft tissue sarcoma. J Clin Oncol 1997;15:3249 57.
874
CANCER August 15, 2001 / Volume 92 / Number 4
24. Jensen V, Ladekarl M, Holm-Nielsen P, Melsen F, Soerensen FB. The prognostic value of oncogenic antigen 519 (OA-519) expression and proliferative activity detected by antibody MIB-1 in node-negative breast cancer. J Pathol 1995;176: 34352. 25. Hajdu SI, Shiu MH, Brennan MF. The role of the pathologist in the management of soft tissue sarcomas. World J Surg 1988;12:326 31 26. Wunder JS, Healey JH, Davis AM, Brennan MF. A comparison of staging systems for localized extremity soft tissue sarcoma. Cancer 2000;88:272130 27. Kononen J, Bubendorf L, Kallioniemi A, Barlund M, Schraml P, Leighton S, et al. Tissue microarrays for high-throughput molecular proling of tumor specimens. Nat Med 1998;14: 844 7. 28. Cordon-Cardo C, Richon VM. Expression of the retinoblastoma protein is regulated in normal human tissues. Am J Pathol 1994;144:500 10. 29. Mehta C, Patel N. A network algorithm for performing Fishers exact test in rXc contingency tables. J Am Stat Assoc 1983;78:42734. 30. Kaplan E, Meier P. Nonparametric estimation from incomplete observations. J Am Stat 1958;53:457 81. 31. Peto R, Peto J. Asymptotically efcient rank invariant procedures. J R Stat Soc A 1972;135:185207. 32. Hoos A, Lewis JJ, Antonescu CR, Dudas ME, Leon L, Woodruff JM, et al. Characterization of molecular abnormalities in human broblastic neoplasmsa model for genotypephenotype association in soft tissue tumors. Cancer Res 2001;61:31715. 33. Hasegawa T, Yokoyama R, Lee YH, Shimoda T, Beppu Y, Hirohashi S. Prognostic relevance of a histological grading system using MIB-1 for adult soft tissue sarcoma. Oncology 2000;58:66 74. 34. Choong PF, Akerman M, Willen H, Andersson C, Gustafson P, Baldetorp B, et al. Prognostic value of Ki-67 expression in 182 soft tissue sarcomas. Proliferationa marker of metastasis? APMIS 1994;102:91524.
13. Gerdes J, Schwab U, Lemke H, Stein H. Production of a mouse monoclonal antibody reactive with a human nuclear antigen associated with cell proliferation. Int J Cancer 1983; 31:1320. 14. Gerdes J, Lemke H, Baisch H, Wacker H-H, Schwab U, Stein H. Cell cycle analysis of a cell proliferation-associated human nuclear antigen dened by the monoclonal antibody Ki-67. J Immunol 1984;133:1710 5. 15. Scholzen T, Gerdes J. The Ki-67 protein: from the known and the unknown. J Cell Physiol 2000;182:31122. 16. Endl E, Gerdes J. Posttranslational modications of the Ki-67 protein coincide with two major checkpoints during mitosis. J Cell Physiol 2000;182:371 80. 17. Hoos A, Urist MJ, Stojadinovic A, Mastorides S, Dudas ME, Kuo D, et al. Validation of tissue microarrays for immunohistochemical proling of cancer specimens using the example of human broblastic tumors. Am J Pathol 2001;158:124551. 18. Molino A, Micciolo R, Turazza M, Bonetti F, Piubello Q, Bonetti A, et al. Ki-67 immunostaining in 322 primary breast cancers: associations with clinical and pathological variables and prognosis. Int J Cancer 1997;74:4337. 19. Chowdhury GM, Kojima K, KanayamaH, Tsuji M, Kurokawa Y, Kagawa S. The proliferation index of MIB-1 as a prognostic factor for patients with transitional cell carcinoma of the upper urinary tract. Cancer 1996;78:82733. 20. Kros JM, Hop WCJ, Godschalk JJCJ, Krishnadath KK. Prognostic value of the proliferation-related antigen Ki-67 in oligodendrogliomas. Cancer 1996;78:110713. 21. Borre M, Bentzen SM, Nerstrom B, Overgaard J. Tumor cell proliferation and survival in patients with prostate cancer followed expectantly. J Urol 1998;159:1609 14. 22. Bubendorf L, Sauter G, Moch H, Schmid HG, Gasser TC, Jordan P, et al. Ki-67 labelling index: an independent predictor of progression in prostate cancer treated by radical prostatectomy. J Pathol 1996;178:437 41. 23. Jansen RL, Hupperets PS, Arends JW, Joosten-Achjanie SR, Vollovics A, Schouten HC, et al. MIB-1 labelling index is an independent prognostic marker in primary breast cancer. Br J Cancer 1998;78:460 5.
Vous aimerez peut-être aussi
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Mol. Cell. Biol.-1999-Di Como-1438-49Document13 pagesMol. Cell. Biol.-1999-Di Como-1438-49Charles J. DiComo, PhDPas encore d'évaluation
- Mol. Cell. Biol.-1995-Di Como-1835-46Document12 pagesMol. Cell. Biol.-1995-Di Como-1835-46Charles J. DiComo, PhDPas encore d'évaluation
- Exp. Derm.-2008-Di Como-405-11Document7 pagesExp. Derm.-2008-Di Como-405-11Charles J. DiComo, PhDPas encore d'évaluation
- Amer. J. Pathol.-2002-Urist-1199-1206Document8 pagesAmer. J. Pathol.-2002-Urist-1199-1206Charles J. DiComo, PhDPas encore d'évaluation
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5795)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (74)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1091)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Caderno de Questões - TwentyFour Dia 2Document2 pagesCaderno de Questões - TwentyFour Dia 2Guilherme MacedoPas encore d'évaluation
- Ovarian Cancer. Case ReportDocument18 pagesOvarian Cancer. Case ReportToby MarshallPas encore d'évaluation
- WJNM 17 151Document6 pagesWJNM 17 151Fadhil Muhammad A.Pas encore d'évaluation
- Canine Mast Cell TumorsDocument5 pagesCanine Mast Cell TumorsCarol LesliePas encore d'évaluation
- ASCCP Colposcopy Standards Role of Colposcopy,.3Document7 pagesASCCP Colposcopy Standards Role of Colposcopy,.3Laura Milagros Apóstol A.Pas encore d'évaluation
- Bonesarcomasand Desmoids: Jeremy M. Brownstein,, Thomas F. DelaneyDocument12 pagesBonesarcomasand Desmoids: Jeremy M. Brownstein,, Thomas F. DelaneyMed MedPas encore d'évaluation
- Cystosarcoma PhyllodesDocument3 pagesCystosarcoma PhyllodesrahadianharyantoPas encore d'évaluation
- PancreasDocument7 pagesPancreasMiguel Cuevas DolotPas encore d'évaluation
- Clinical Aspects of NeoplasiaDocument23 pagesClinical Aspects of NeoplasiaJahanzaib BashirPas encore d'évaluation
- Our R&D - Zai LabDocument12 pagesOur R&D - Zai LabKarina HonórioPas encore d'évaluation
- Trends in The Global Immuno-Oncology Landscape: From The Analyst'S CouchDocument2 pagesTrends in The Global Immuno-Oncology Landscape: From The Analyst'S CouchnagarajharishPas encore d'évaluation
- Supply Chain Management of Shifa International HospitalDocument10 pagesSupply Chain Management of Shifa International HospitalZarmeenaGauharPas encore d'évaluation
- Bronchogenic Carcinoma: Dr. Vineet ChauhanDocument49 pagesBronchogenic Carcinoma: Dr. Vineet ChauhanRaviPas encore d'évaluation
- Cancer in Thailand - VII PDFDocument232 pagesCancer in Thailand - VII PDFPonlapat YonglitthipagonPas encore d'évaluation
- CA Exam UndergraduateDocument3 pagesCA Exam UndergraduateMilagros Fuertes YosoresPas encore d'évaluation
- Leiomyoma - What Is It? Pathogenesis, Clinical Presentation, Diagnosis, HysterectomyDocument10 pagesLeiomyoma - What Is It? Pathogenesis, Clinical Presentation, Diagnosis, HysterectomyRida ArifPas encore d'évaluation
- Lung Cancer Report Sample High enDocument1 pageLung Cancer Report Sample High enBantiPas encore d'évaluation
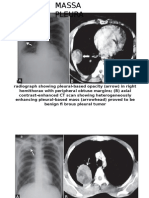
- Massa PleuraDocument4 pagesMassa PleuraPrayogi KramyPas encore d'évaluation
- Breast Absite QuestionsDocument18 pagesBreast Absite QuestionsGeshabelle ApuraPas encore d'évaluation
- Bi-Rads: (Breast Imaging-Reporting and Data System)Document30 pagesBi-Rads: (Breast Imaging-Reporting and Data System)Siti NirwanahPas encore d'évaluation
- Prostate Cancer ThesisDocument5 pagesProstate Cancer Thesisaflozmfxxranis100% (2)
- OF BLADDER CANCER" For M.Ch. Urology, Session 2020-2023Document24 pagesOF BLADDER CANCER" For M.Ch. Urology, Session 2020-2023flammator100% (1)
- Breast Cancer WHODocument104 pagesBreast Cancer WHOGoh Dody100% (2)
- KSC WSSforKSCCQIDocument34 pagesKSC WSSforKSCCQILệnhHồXungPas encore d'évaluation
- Brain TumorDocument10 pagesBrain TumorBakary BadjiePas encore d'évaluation
- Oncology Nursing NotesDocument12 pagesOncology Nursing Notesjoyrena ochondra100% (6)
- Newest Breast CancerDocument27 pagesNewest Breast CancerSAMMYPas encore d'évaluation
- Meigs Syndrome: Background: Meigs Syndrome Is Defined As The Triad of Benign OvarianDocument8 pagesMeigs Syndrome: Background: Meigs Syndrome Is Defined As The Triad of Benign OvarianRizki Amaliah100% (1)
- CH62 Management of Differentiated Thyroid CancerDocument52 pagesCH62 Management of Differentiated Thyroid Cancer許懷朔Pas encore d'évaluation
- Multidisciplinary Management of Prostate CancerDocument158 pagesMultidisciplinary Management of Prostate CancersuckafuckPas encore d'évaluation