Académique Documents
Professionnel Documents
Culture Documents
Agenesis Vagina
Transféré par
i305Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Agenesis Vagina
Transféré par
i305Droits d'auteur :
Formats disponibles
Vaginal Agenesis/MRKH
Vaginal agenesis is a congenital disorder of the reproductive system in females that affects approximately 1 in 5,000 females. In this disorder, the uterus and the vaginal canal do not develop properly during the pregnancy and the female is born with a very short vaginal canal or no vagina at all (in most cases there is a dimple present between the labia where the vaginal opening should be). The condition is typically not detected until puberty when the teenage female is delayed in getting her menses or it may be discovered with first attempts at having sex. Most patients with this abnormality have Mayer-Rokitansky-Kuster-Hauser syndrome (MRKH). In this syndrome the vagina is absent (or very short) and the uterus is absent or extremely rudimentary (ie if it is present it is non-functioning and a very small remnant). The ovarian function is normal, the endocrine function is normal, the chromosomes are a normal 46 XX female and the secondary sexual characteristics are normal and that of a female. The patients is a normal female (ie appears female with normal breast development and the outside of the vagina appears normal as well), however she just does not have a vaginal canal, nor a functioning uterus at the top of the vagina. The cause of the syndrome remains unclear, however a multifactorial mode of inheritance, including genetic and environmental factors, seems to be the most likely explanation.
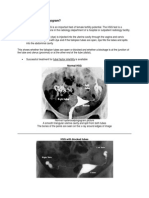
The picture on the left shows normal female development with normal uterus and full length vagina. The picture on the right demonstrates a patient with MRKH in the fact that the uterus does not fully develop nor does the vagina canal. There is a very short vaginal opening and sometimes just a "dimple" and beyond that the bladder and the rectum are fused together with no intervening vaginal canal.
Figure demonstrates a patient with MRKH and the fact that there is no uterus and no vaginal canal where it typically should develop between the bladder and the rectum.
Criteria for diagnosis- MRKH
Normal female appearance Normal external genitalia (ie Breasts, Vulva) Absence of vaginal canal Absent or rudimentary Uterus Normal functioning female ovaries
MRKH Diagnosis
Diagnosis of the condition includes a genetic evaluation including a chromosomal analysis to confirm a normal 46 XX female chromosomes. Additional studies will include a hormonal evaluation (however if the patient has normal breast development and other normal female appearance this typically means the ovaries are functioning and producing normal female hormones) as well as an Ultrasound of the pelvis and the kidneys (or an IVP which is a dye test with x-rays to evaluate the kidneys) and/or an MRI of the pelvis and abdomen. MRKH syndrome is often associated with urinary tract, skeletal and auditory anomalies. The incidence of urinary tract anomalies is as high as 40% of cases and can involve just having one kidney, having a pelvic kidney (one kidney is displaced down in the pelvis but may still function normally), and having duplication of the renal pelvis or ureters (ie having two tubes instead of one bringing urine from the kidney to the bladder). Skeletal
anomalies are found in 10-12% of cases and can involve abnormalities of the spine or vertebrae, ribs or limbs. Finally, middle ear anomalies including hearing loss can also be associated. None of these conditions is life threatening, however it is important to evaluate and be aware of any of these anomalies.
MRKH Diagnostic Evaluation
Chromosome analysis Ultrasound of pelvis and kidneys IVP (kidney dye test) and spine X-ray MRI of pelvis and abdomen (may replace some of above tests)
Diagnosis is usually delayed until adolescence when the young woman does not have her period. The confirmation of the diagnosis is inevitably a psychological shock for the patient and her family. The absence of a vagina has a profound impact on the young womans sense of feminity and her future sexuality, thoughts about her future ability to bear children and have a family and the immediate feelings and shock of being told she does not have a normal vagina or uterus. She inevitably will feel as if she is not normal and is typically at a very fragile age emotionally, ie her teen years and certainly will be concerned with how others will feel about her (if they know or would find out) or look at her. Counseling and support during this time frame will be crucial and there are support groups and psychologists/psychiatrists that are trained to assist during this time frame and help the patient cope and understand her condition. Helpful support information about the condition is also available through www.MRKH.org. Typically, vaginal agenesis patients do not have a functioning uterus and cannot become pregnant. However, most have normal functioning ovaries and can become biologic parents through in-vitro fertilization of their own eggs with the pregnancy carried by a surrogate mother.
Treatment options for creation of vaginal canal (Neovagina)
Patients with vaginal agenesis will need treatment to become sexualy active and therefore will need creation of a neovagina. Timing of this will depend on the patient and her family and the surgeon feel she is emotionally and physically mature enough to undergo the procedure or surgery. Ideally, in the past it was felt that the patient should be ready to be sexually active shortly after any surgical procedure to create a vagina, however many patients and families opt for treatment prior to this as the young woman desires a vaginal canal at a younger age as she wants to feel normal and doesnt want to wait until she is ready to be active. This is certainly understandable and why many young women undergo the procedure in their late teens. In this case, if the young woman is not planning on sexual activity for a period of time (and this could be years) after the surgery, then she will need to be prepared to use dilators to maintain the vaginal canal until she is having intercourse on a regular basis.
There are excellent treatment options available to create a functioning vagina. Some older techniques are much more invasive than others and require large abdominal incisions with major surgery, extensive recovery and very large abdominal wall scars while others require skin grafts, muscle flaps taken from the legs or other areas which are also very invasive with extensive recovery time. Drs. Miklos and Moore utilize a modification of an abdominal technique that utilizes the patients own peritoneum, requires no grafts or implants and has excellent success rates, however they utilize a laparoscopic approach with mini-incisions that enables the procedure to be completed on an outpatient basis with a very rapid recovery. Details of this procedure are listed below.
Non-surgical Neovaginal Treatment
Self-dilation Is sometimes used as a first attempt to create or lengthen the very short or non-existent vagina. In this treatment, the patient presses (or eventually sits on) a small rod (dilator) against the skin or the small vagina for 15-20 minutes a day. Progressively larger dilators are used to expand and lengthen the vagina. Several months may be required to obtain the needed length. It is recommended that the vagina be at least 2.5 cm in length to start (ie prior to dilating) otherwise the success rates are not adequate.
Surgical Neovaginal Techniques
There have been many different surgical techniques describe to create a neovagina and most have been very invasive large surgeries with variable success rates. Some of the most common ones described are below: McIndoe Vaginoplasty: A complicated procedure that requires skin grafts and/or muscle grafts from the thigh or leg and requires and implant in the vagina for up to 3 mos after surgery and then dilator use following this. Vecchietti Procedure: This utilizes an acrylic olive shape apparatus that is applied under tension (via threads that are brought up through the abdominal wall via incision in the abdomen) against the vaginal dimple. A traction device is then used on the threads on the abdominal wall and tightened over time that draws the olive upward and stretches the skin, thus creating a neovagina. This can take up to 3 months to accomplish and then requires dilators after. Bowel vaginoplasty:
The sigmoid colon or other loop of intestinal bowel can be transposed down into the pelvis and utilized as a new vagina. This is a major abdominal surgery that requires bowel resection and carries major risks and complications. Davydov Procedure: Utilizes the patients own peritoneum (the cellular layer that lines the walls of the pelvis and the abdominal cavity) as the new vaginal canal. Traditionally completed via open abdominal incision, the laparoscopic approach was developed in Russia in the late 1990s and early 2000s. The advantage of this procedure is that it utilizes the pelvic peritoneum as the lining of the new vagina, which has been shown to transform into histologic vaginal epithelium in approximately 6 months time. That means if one biopsies the new vagina 6 months after it was created, the skin appears as normal vaginal skin under the microscope! Additionally, it creates more length than any of the other procedures and is one of the least invasive techniques available, has a very quick recovery, has minimal risk of scarring down and typically requires very little dilating after surgery.
Laparoscopic Creation of a Neovagina
Drs Moore and Miklos utilize a laparoscopic modification of the Davydov procedure. This makes it even more minimally invasive than the original procedure. The doctors travelled to Russia and were trained by Dr L.V. Adamyan, who developed this original technique. They have used their laparoscopic expertise and suturing skills to modify the procedure even more and to do more of it laparoscopically (it is a combined laparoscopic and vaginal procedure) as they do most of the suturing required through the miniincisions in the belly button and abdomen while working off of High-Definition large screen TVs. In a recent study the procedure had a 96% functional success rate with sexual function scores in the good to very good rate. Typically, patients are able to have normal sexual function including arousal, lubrication, orgasm and satisfaction. The procedure itself is much less invasive than most of the alternative surgical options and achieves better length with less risk of scarring down. The procedure usually takes between 1 and 2 hours and is completed in an outpatient surgical setting (or a 23 hour stay facility). Recovery is rapid and intercourse is able to be achieved in as little as 2 weeks post-operatively. A vaginal pack is typically left in for just 36-48 hours (in some other procedures that may require skin grafting of the vagina, the pack has to be left in for up to 1-2 months), however in some cases it may need to be changed and left in for approximately a week. Pain is usually minimal and return to normal activities such as school is usually very rapid. Dr Miklos and Moore have utilized this laparoscopic technique on women throughout the US, including many young women that have had attempts of neovagina by other techniques and other surgeons and have failed. They are still able to utilize their laparoscopic skills even in this more complicated subset of patients to create a neovagina with the pelvic peritoneum and still operate through mini-incisions and give the patient the benefit of very minimally invasive surgery. Patients that have had previous surgery
cannot believe how much easier the approach was with Dr Moore and Miklos and the results they achieved after the procedure resulting in a normal, full length, functioning vagina! Drs. Moore and Miklos are considered world leaders in the laparoscopic approach to create a neovagina and are asked from experts throughout the world to come and lecture and teach on the subject. They just returned from Dubai where they taught surgeons from throughout Europe and the Middle East their laparoscopic techniques.
Vous aimerez peut-être aussi
- Gynecology: Three Minimally Invasive Procedures You Need to Know About For: Permanent Birth Control, Heavy Menstrual Periods, Accidental Loss of Urine Plus: Modern Hormone Therapy for the Post Menopausal WomenD'EverandGynecology: Three Minimally Invasive Procedures You Need to Know About For: Permanent Birth Control, Heavy Menstrual Periods, Accidental Loss of Urine Plus: Modern Hormone Therapy for the Post Menopausal WomenPas encore d'évaluation
- Vaginal Agenesis PDFDocument4 pagesVaginal Agenesis PDFBill HarmanPas encore d'évaluation
- Tinjauan Pustaka Agenesis UteriDocument2 pagesTinjauan Pustaka Agenesis UteriMaulana DimasPas encore d'évaluation
- Anorectal Malformations HandoutDocument4 pagesAnorectal Malformations HandoutShikha Acharya100% (1)
- Cervical IncompetenceDocument28 pagesCervical IncompetenceHoney May Rollan Vicente100% (1)
- Dr. Ahlam Al-Kharabsheh: Assistant Professor, OBS & GYN Department Mu'tah UniversityDocument36 pagesDr. Ahlam Al-Kharabsheh: Assistant Professor, OBS & GYN Department Mu'tah Universityraed faisalPas encore d'évaluation
- Midwifery - SterlizationDocument39 pagesMidwifery - SterlizationEsha KuttiPas encore d'évaluation
- What Is Microsurgical Tubal Ligation Reversal?Document2 pagesWhat Is Microsurgical Tubal Ligation Reversal?Andy WijayaPas encore d'évaluation
- Cervical Cancer ScreeningDocument25 pagesCervical Cancer Screening6ixSideCreate MPas encore d'évaluation
- HSG 6th Year StudentsDocument115 pagesHSG 6th Year StudentsYulita MustikasariPas encore d'évaluation
- VasectomyDocument20 pagesVasectomyAngelica MaePas encore d'évaluation
- ColposDocument41 pagesColposjumgzb 10Pas encore d'évaluation
- Incompetent CervixDocument4 pagesIncompetent CervixjastinmoralesPas encore d'évaluation
- Government College of Nursing Jodhpur (Raj.)Document5 pagesGovernment College of Nursing Jodhpur (Raj.)priyankaPas encore d'évaluation
- 2 2017 03 26!08 03 00 PMDocument10 pages2 2017 03 26!08 03 00 PManakayamPas encore d'évaluation
- Vaginal Agenesis or HypoplasiaDocument18 pagesVaginal Agenesis or Hypoplasianikd_6Pas encore d'évaluation
- CASE ANALYSIS Ectopic Pregnancy Part 1Document10 pagesCASE ANALYSIS Ectopic Pregnancy Part 1Diane Celine SantianoPas encore d'évaluation
- Cervical IncompetenceDocument30 pagesCervical IncompetenceSignor ArasPas encore d'évaluation
- Exploratory LaparotomyDocument25 pagesExploratory Laparotomywinai13Pas encore d'évaluation
- $RVQJ2N8Document35 pages$RVQJ2N8Elon EthereumPas encore d'évaluation
- Handout and Questions of HysterosalpingDocument12 pagesHandout and Questions of Hysterosalpingahmad shaltout100% (2)
- MRKH SundromeDocument37 pagesMRKH SundromeBudi Iman SantosoPas encore d'évaluation
- Hys Tero Salpingo GramDocument5 pagesHys Tero Salpingo GramShreMulyanaRahimPas encore d'évaluation
- HidroceleDocument4 pagesHidroceleAnshy V. FreirePas encore d'évaluation
- Journal of Medical Case ReportsDocument4 pagesJournal of Medical Case ReportsAna Di JayaPas encore d'évaluation
- Permanent Methods of Contraception (Surgical Sterilization) : VasectomyDocument7 pagesPermanent Methods of Contraception (Surgical Sterilization) : VasectomyEmAr ExPas encore d'évaluation
- Laparoscopy: Women's Health Information For PatientsDocument8 pagesLaparoscopy: Women's Health Information For PatientsKamran AfzalPas encore d'évaluation
- SCP BSUG July 2017Document15 pagesSCP BSUG July 2017Yasir K. HaniPas encore d'évaluation
- Pelvic Organ ProlapseDocument9 pagesPelvic Organ ProlapseSonny Dizon PareñasPas encore d'évaluation
- Hymen ImperforataDocument16 pagesHymen ImperforataImanuella KairupanPas encore d'évaluation
- Permanent Family PlanningDocument36 pagesPermanent Family PlanningNilakshi Barik MandalPas encore d'évaluation
- Imperforate AnusDocument8 pagesImperforate AnusBâchtyăr Đ'jâckêrsPas encore d'évaluation
- Infertility - Definition, Causes, Diagnostic Procedures AND CouncellingDocument37 pagesInfertility - Definition, Causes, Diagnostic Procedures AND CouncellingvincentsharonPas encore d'évaluation
- Figure 3: Missed Miscarriage by US.: Review of The LiteratureDocument5 pagesFigure 3: Missed Miscarriage by US.: Review of The LiteratureMenaKamelPas encore d'évaluation
- Anorectal MalformationsDocument19 pagesAnorectal MalformationsJumrotun Ni'mahPas encore d'évaluation
- O&G Counselling - TSPDocument6 pagesO&G Counselling - TSPTarran PhagooPas encore d'évaluation
- MRKH DissertationDocument4 pagesMRKH DissertationWriteMyPaperForCheapUK100% (1)
- Ruiz, P. - SGD and NCP On Imperforate AnusDocument8 pagesRuiz, P. - SGD and NCP On Imperforate AnusPatricia Dianne RuizPas encore d'évaluation
- Anorectal Malformations in Children - A Review: Amrish Vaidya, Kishore AdyanthayaDocument4 pagesAnorectal Malformations in Children - A Review: Amrish Vaidya, Kishore Adyanthayasangvi_tvPas encore d'évaluation
- Ovarian Cysts Treatment & Management - Approach Considerations, Fetal and Neonatal Cysts, Ovarian Cysts in PregnancyDocument6 pagesOvarian Cysts Treatment & Management - Approach Considerations, Fetal and Neonatal Cysts, Ovarian Cysts in PregnancyTrần Hà TrangPas encore d'évaluation
- Diagnostic LaparosDocument8 pagesDiagnostic Laparosdrhiwaomer100% (3)
- TotalAbdomHysterBilateralSalpingoOophorectPelvicNodeDissection EndometrialCancer TH PD9300Document36 pagesTotalAbdomHysterBilateralSalpingoOophorectPelvicNodeDissection EndometrialCancer TH PD9300Red StohlPas encore d'évaluation
- Ectopic PregnancyDocument8 pagesEctopic PregnancylaurelwingPas encore d'évaluation
- What Is Bilateral Tubal LigationDocument42 pagesWhat Is Bilateral Tubal LigationAldrich ArquizaPas encore d'évaluation
- Ob GynDocument13 pagesOb GynDianne Geremy RojoPas encore d'évaluation
- Incompetent CervixDocument29 pagesIncompetent CervixCyrelle Jen TorresPas encore d'évaluation
- Assisting With Gynecological ProceduresDocument12 pagesAssisting With Gynecological ProceduresVismayamaliekalPas encore d'évaluation
- Gynecologic Examination - StatPearls - NCBI BookshelfDocument6 pagesGynecologic Examination - StatPearls - NCBI BookshelfNot DeyvPas encore d'évaluation
- Sterilization Fertilization Isth Mic Portion of The Fallopian TubeDocument3 pagesSterilization Fertilization Isth Mic Portion of The Fallopian TubeRj FloresPas encore d'évaluation
- Day Case Vaginal Pomeroy Tubectomy A Simplified TechniqueDocument11 pagesDay Case Vaginal Pomeroy Tubectomy A Simplified TechniqueedelinPas encore d'évaluation
- Permanent ContraceptionDocument33 pagesPermanent Contraceptionshyama seerviPas encore d'évaluation
- Anorectal MalformationDocument28 pagesAnorectal MalformationJaya Prabha50% (2)
- Grand Case Pres - Transverse Vaginal Septum..Document32 pagesGrand Case Pres - Transverse Vaginal Septum..Gio LlanosPas encore d'évaluation
- Advanced Laparoscopic Hysterectomy SurgeryDocument2 pagesAdvanced Laparoscopic Hysterectomy SurgeryManu GynecologyPas encore d'évaluation
- Diagnostic Procedures of PregnancyDocument7 pagesDiagnostic Procedures of PregnancyRuth Anne Zonio DamasoPas encore d'évaluation
- GynecologyDocument18 pagesGynecologyLuai Tuma KhouryPas encore d'évaluation
- Cloacal MalformationsDocument6 pagesCloacal MalformationsRayhanun MardhatillahPas encore d'évaluation
- MRKH Sundrome PPTDocument37 pagesMRKH Sundrome PPTleenarobin100% (2)
- Abstract and IntroductionDocument10 pagesAbstract and Introductioni305Pas encore d'évaluation
- Figo Staging CA EndometriumDocument9 pagesFigo Staging CA Endometriumi305Pas encore d'évaluation
- Hipertensi Dalam KehamilanDocument47 pagesHipertensi Dalam KehamilanTommy NainggolanPas encore d'évaluation
- Infertility Treatment and Assisted ReproductionDocument30 pagesInfertility Treatment and Assisted ReproductionSumit RoyPas encore d'évaluation
- CA Ovarium DR deDocument50 pagesCA Ovarium DR dei305Pas encore d'évaluation
- Figo Staging CA EndometriumDocument9 pagesFigo Staging CA Endometriumi305Pas encore d'évaluation
- Figo Staging CA EndometriumDocument9 pagesFigo Staging CA Endometriumi305Pas encore d'évaluation
- StudyDocument6 pagesStudyi305Pas encore d'évaluation
- RelaksinDocument3 pagesRelaksini305Pas encore d'évaluation
- General FinalDocument4 pagesGeneral Finali305Pas encore d'évaluation
- Calcium and Vitamin D Intake and Risk of Incident Premenstrual SyndromeDocument7 pagesCalcium and Vitamin D Intake and Risk of Incident Premenstrual Syndromei305Pas encore d'évaluation
- VecchiettiDocument5 pagesVecchiettii305Pas encore d'évaluation
- Ogl 322 FinalDocument2 pagesOgl 322 Finalapi-538747121100% (1)
- Republic Act 7610Document44 pagesRepublic Act 7610Dawn Novera100% (4)
- Toxoplasmosis Serologic Testing AlgorithmDocument1 pageToxoplasmosis Serologic Testing AlgorithmHanny Prasetiana YuriantiPas encore d'évaluation
- Effectivity: SY 2016-2017 Document Code: QR - AAD - 001 Revision No.: 00 Issue No.: 01 Date Issued: March 2015Document7 pagesEffectivity: SY 2016-2017 Document Code: QR - AAD - 001 Revision No.: 00 Issue No.: 01 Date Issued: March 2015Sandre WaldenPas encore d'évaluation
- Treinamento Sensório MotorDocument8 pagesTreinamento Sensório MotorDébora SouzaPas encore d'évaluation
- UV 365 Disinfection of Drinking Water Tanks: A Product by Expert 365 Pty LTD.Document5 pagesUV 365 Disinfection of Drinking Water Tanks: A Product by Expert 365 Pty LTD.Faisal Ridho SaktiPas encore d'évaluation
- Shalkya TantraDocument3 pagesShalkya Tantratejpat2k7Pas encore d'évaluation
- Arena - Experimental Homeopathic Research On Opuntia Ficus IndicaDocument8 pagesArena - Experimental Homeopathic Research On Opuntia Ficus IndicaAnny Kelly VasconcelosPas encore d'évaluation
- Antimicrobial Products-Test For Antimicrobial Activity and EfficacyDocument14 pagesAntimicrobial Products-Test For Antimicrobial Activity and EfficacyherfuentesPas encore d'évaluation
- Bethesda Thyroid 2017Document6 pagesBethesda Thyroid 2017Ladipo Temitope AyodejiPas encore d'évaluation
- Genflex Roofing Systems, LLC Material Safety Data SheetDocument4 pagesGenflex Roofing Systems, LLC Material Safety Data SheetgjroddyPas encore d'évaluation
- POCSODocument15 pagesPOCSOThakur Avnish Singh100% (1)
- X120MN12Document6 pagesX120MN12mini p shendePas encore d'évaluation
- Ethiopia - Design Gudeline Final - OromiaDocument71 pagesEthiopia - Design Gudeline Final - OromiaEphrem Gizachew100% (15)
- Rigging TechniquesDocument27 pagesRigging TechniquesDeepak ShettyPas encore d'évaluation
- BT RA 01 WeldingDocument6 pagesBT RA 01 Weldingnandha gopalPas encore d'évaluation
- Product PlanDocument19 pagesProduct Planlily30109150% (2)
- Human Condition Before Common EraDocument2 pagesHuman Condition Before Common EraACM23Pas encore d'évaluation
- SF2 Aquarius Set BDocument2 pagesSF2 Aquarius Set BXyzaPas encore d'évaluation
- K3 Bidang Pertanian ILO PDFDocument350 pagesK3 Bidang Pertanian ILO PDFSufyan StauriPas encore d'évaluation
- No Sweat - Chapter 2: Escape The Vicious Cycle of FailureDocument27 pagesNo Sweat - Chapter 2: Escape The Vicious Cycle of FailureAMACOM, Publishing Division of the American Management AssociationPas encore d'évaluation
- Chapter 7 CapsulesDocument87 pagesChapter 7 CapsulesTeresa Saylo92% (26)
- Clinical Gaze Through The Prism of LiteratureDocument10 pagesClinical Gaze Through The Prism of LiteratureZedarPas encore d'évaluation
- Aris Wand Brochure (39555 V1)Document4 pagesAris Wand Brochure (39555 V1)mohitpriyank2003Pas encore d'évaluation
- Root Caries: A Periodontal Perspective: Review ArticleDocument21 pagesRoot Caries: A Periodontal Perspective: Review ArticleIlmia AmaliaPas encore d'évaluation
- TDR Business Plan 2008-2013: Robert RidleyDocument43 pagesTDR Business Plan 2008-2013: Robert RidleySripal JainPas encore d'évaluation
- PD 1067 Water Code of The Philippines and Clean Water ActDocument44 pagesPD 1067 Water Code of The Philippines and Clean Water ActNovy Jamboy Ragmac100% (2)
- Yaourt Foodand Health 2016Document10 pagesYaourt Foodand Health 2016Patrick ParraPas encore d'évaluation
- Max Bupa Claim Form NewDocument9 pagesMax Bupa Claim Form NewViral ShuklaPas encore d'évaluation
- Walk or Cycle For 'A Happier Commute': BBC Learning English Words in The NewsDocument2 pagesWalk or Cycle For 'A Happier Commute': BBC Learning English Words in The NewsCaio Augusto Takaki UechiPas encore d'évaluation