Académique Documents
Professionnel Documents
Culture Documents
DP26 Girolami Gay DP26
Transféré par
equalbenDescription originale:
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
DP26 Girolami Gay DP26
Transféré par
equalbenDroits d'auteur :
Formats disponibles
A Physical Therapy Protocol to Enhance Anticipatory Postural Control and Standing Balance in an Adult with CP: A Case Report
Gay L. Girolami, PT, PhD
Introduction
Individuals with cerebral palsy have impaired balance and anticipatory postural adjustments (APAs), which interfere with their ability to prepare for postural perturbations and sustain independent sitting and standing balance [1]. There are studies which report on compensatory postural adjustments (CPAs) and standing balance training in individuals with cerebral palsy [2, 3]. There is seminal research on APAs in children with typical development, hemiplegia and diplegia [4,5], but no research describing how to train APAs in individuals with cerebral palsy. The purpose of this case report was to examine the effectiveness of an intensive physical therapy program to improve balance and APAs in an adult with cerebral palsy.
Methods
PARTICIPANT A 31 year old male with spastic quadriplegia (GMFCS III), who participates in multiple weekly physical, occupational and speech therapy sessions, consented to participate in the intervention as part of an intensive PT treatment program. Goal: transition to forearm crutches in the home. Reverse walker for community ambulation Wears AFOs Prior surgical lengthenings: bilateral hip flexor, hamstring and gastrocnemius Works outside the home/active in the community Participates in sports (swimming/horseback riding) INTERVENTION 60 minute physical therapy sessions were provided four days per week in two 8 week phases for a total of 39 sessions (Tables 1 and 2)
Total
Results
Table 3. GAS Scores - Phase I
Phase I: February 22 April 8, 2010 Baseline Goal 1. Standing Balance: Support from Ball 2. Standing Balance: Trapeze Support GAS 2 seconds 3 seconds -2 -2 40 sec 20 sec 21 sessions April 8 GAS 0 -1
Results
Goal Attainment Scaling (Tables 3 and 4) Timed Standing (2 sec to 90 sec ); Standing Balance/Unstable Support (3 sec to 38 sec) Standing Reaching (2 reaches to 7 reaches). Pediatric Reach Test 4.4 inch improvement - Left sideways reach (the more involved side) No change - sitting forward reach No change - right sideways reach. EMG: (Figs 3 and 4) Pre-test EMGs - no APAs in the trunk or upper leg prior to perturbations in sitting and standing, Post-test EMGs - APAs documented in trunk and upper leg Video Documentation/Photos Improved alignment Improved ability to sustain sitting posture during upper extremity abduction movements Fig 3 Stand: Pre-test (L) and Post-test (R): RA and ES
Conclusion
Positive functional and EMG changes were found following this intensive physical therapy program using these outcome measures Goal Attainment Scaling Pediatric Reach Test EMG Video Documentation This intensive physical therapy protocol appears to be an effective intervention to improve sitting and standing balance as well as anticipatory postural adjustments. This protocol merits further investigation. Enrolling a larger group of participants would create more robust data to determine whether this protocol can be effectively applied as a therapy intervention. A larger data set would also be beneficial to determine the efficacy of the Goal Attainment Scale to assess changes in balance and APAs. EMG and force platform data can be effectively used as objective measure of change in anticipatory postural control.
Table 4. GAS Scores - Phase II
Phase II: April 12 May 19, 2010 April 12 Goals 1. Standing Balance: Support from Ball 2. Standing Balance: Trapeze Support 3. Standing Reach: 4. Independent Sitting 5. Bench Sit: Throw Ball GAS 40 sec 14 sec Right = 0 Left = 1 2 seconds 3 catch/ throw 0 -1 -2 -2 -2 90 sec 38 sec Right = 2 Left = 9 58 seconds 23 catch/ throw 18 sessions May 19 GAS +2 0 -2 -1 +1 +2
Intervention/Testing
Table 1. Therapy Sessions
Phase I February March April Total Sessions 2 15 4 21/28 April May Total 8 10 18/23 39 Phase II Sessions
Perturbations and mobile supports were used to effect changes in trunk posture, balance and APAs in sitting and standing. (Figs 1 and 2) External perturbations Mobile support Verbal and sensory cues Guided facilitation PRE, MID AND POST TESTING Goal Attainment Scale (GAS) measures individualized goal achievement of functional tasks based on a 5 point scale Pediatric Reach Test (PRT) - a measure of sitting and standing balance (administered in sitting) Electromyography (EMG) - documents timing, sequencing and magnitude of muscle activity Video documentation/Photos - an objective tool to assess changes in performance and alignment
Table 2. Testing Schedule Baseline
Video Documentation February 2, 2010 Goal Attainment Scale February 22, 2010 X EMG February 15, 2010
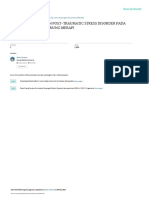
Fig 1. Externally initiated perturbations in sitting designed to train APAs
References
1. Bax, M., et al., Proposed definition and classification of cerebral palsy. Dev Med Child Neurol. 2005; 47(8): 571-6. 2. Shumway-Cook, A., et al., Effect of balance training on recovery of stability in children with cerebral palsy. Dev Med Child Neurol. 2003; 45(9): 591-602.
Test Session 1
Video Documentation April 12, 2010 Goal Attainment Scale April 12, 2010 Pediatric Reach Test April 12, 2010 X
Test Session 2
Video Documentation May 17, 2010 Goal Attainment Scale May 19, 2010 Pediatric Reach Test May 19, 2010 EMG May 7, 2010
Fig 4 Stand: Pre-test (L) and Post-test (R): RF and BF
3. Woollacott, M., et al., Effect of balance training on muscle activity used in recovery of stability in children with cerebral palsy: a pilot study. Dev Med Child Neurol. 2005; 47(7): 455-61. 4. Girolami GL, Shiratori T, Aruin AS. Anticipatory postural adjustments in children with typical motor development. Exp Brain Research. 2010; 205(2):153-165. 5. Girolami GL, Shiratori T, Aruin AS. Anticipatory postural adjustments in children with hemiplegia and diplegia. J Electromyogr Kinesiol. 2011. in press.
Fig 2 Standing balance practice using a mobile surface
This study was supported in part by Pathways Foundation and the Knecht Movement Science Laboratory, UIC.
Vous aimerez peut-être aussi
- The Effects of Pilates Based Exercise On Dynamic Balance in Healthy AdultsDocument5 pagesThe Effects of Pilates Based Exercise On Dynamic Balance in Healthy AdultsIka Nindyas RanitadewiPas encore d'évaluation
- Effect of Task-Oriented Training and Neurodevelopmental Treatment On The Sitting Posture in Children With Cerebral PalsyDocument3 pagesEffect of Task-Oriented Training and Neurodevelopmental Treatment On The Sitting Posture in Children With Cerebral PalsyPhysio SauravPas encore d'évaluation
- Effects of Two Types of Trunk Exercises OnDocument11 pagesEffects of Two Types of Trunk Exercises OnFrancisco Maldonado WilliamsPas encore d'évaluation
- Strengthening Versus Stabilisation Exercise Programmes for Preventing and Reducing Low Back Pain in FemalesD'EverandStrengthening Versus Stabilisation Exercise Programmes for Preventing and Reducing Low Back Pain in FemalesPas encore d'évaluation
- Exercisecommitment ResearchDocument14 pagesExercisecommitment Researchapi-282525755Pas encore d'évaluation
- Dilpreet Kaur Dr. Ravi Gupta Dr. Shikha: BackgroundDocument6 pagesDilpreet Kaur Dr. Ravi Gupta Dr. Shikha: BackgroundSiti Chodijah SyPas encore d'évaluation
- Yoga Therapy and Ambulatory Multiple Sclerosis Assessment of Gait Analysis Parameters, Fatigue and BalanceDocument10 pagesYoga Therapy and Ambulatory Multiple Sclerosis Assessment of Gait Analysis Parameters, Fatigue and BalancefranpmcPas encore d'évaluation
- Reseach Paper - Edited 1Document14 pagesReseach Paper - Edited 1api-238703581Pas encore d'évaluation
- Reseach PaperDocument12 pagesReseach Paperapi-238169773Pas encore d'évaluation
- Pilatesmakale PDFDocument9 pagesPilatesmakale PDFOzkan AltunPas encore d'évaluation
- Ansiedade e Treino Combinado PDFDocument8 pagesAnsiedade e Treino Combinado PDFPaulo AfonsoPas encore d'évaluation
- Scapula Setting AnaIsabel AlmeidaDocument1 pageScapula Setting AnaIsabel AlmeidaPeter ZachPas encore d'évaluation
- Wa0001.Document31 pagesWa0001.Moin RashidPas encore d'évaluation
- Amplitude-Oriented Exercise in Parkinson's Disease: A Randomized Study Comparing LSVT-BIG and A Short Training ProtocolDocument4 pagesAmplitude-Oriented Exercise in Parkinson's Disease: A Randomized Study Comparing LSVT-BIG and A Short Training ProtocolcaroPas encore d'évaluation
- Effect of Yoga On Selected Physical and Physiological Variables of Physical Education StudentsDocument7 pagesEffect of Yoga On Selected Physical and Physiological Variables of Physical Education StudentsIOSRjournalPas encore d'évaluation
- Cjbas 14 02 01 01Document8 pagesCjbas 14 02 01 01CJBAS ManagerPas encore d'évaluation
- Geiger RDocument2 pagesGeiger Rprajaktab_14thseptbrPas encore d'évaluation
- Effects of A 16-Week Pilates Exercises Training Program For Isometric Trunk Extension and Flexion StrengthDocument9 pagesEffects of A 16-Week Pilates Exercises Training Program For Isometric Trunk Extension and Flexion StrengthDiana Magnavita MouraPas encore d'évaluation
- A Study of Core Muscle Electromyographic Activity During Physical ConditionsDocument7 pagesA Study of Core Muscle Electromyographic Activity During Physical ConditionsEsteban AmayaPas encore d'évaluation
- Forward Head Posture Correction Versus Shoulder Stabilization Exercises Effect On Scapular Dyskinesia and Shoulder Proprioception in Athletes An Experimental StudyDocument7 pagesForward Head Posture Correction Versus Shoulder Stabilization Exercises Effect On Scapular Dyskinesia and Shoulder Proprioception in Athletes An Experimental StudyInternational Journal of PhysiotherapyPas encore d'évaluation
- BestDocument3 pagesBestRitika JangraPas encore d'évaluation
- Center Physiotherapy and Rehabilitation Sciences - CPRS: Effect of Plyometric Training On Functional Ankle InstabilityDocument42 pagesCenter Physiotherapy and Rehabilitation Sciences - CPRS: Effect of Plyometric Training On Functional Ankle InstabilityMoin RashidPas encore d'évaluation
- Medicina: Ffect of Functional Electrical Stimulation andDocument12 pagesMedicina: Ffect of Functional Electrical Stimulation andVizaPas encore d'évaluation
- Scapular Muscle Rehabilitation Exercises in Overhead Athletes With Impingement SymptomsDocument10 pagesScapular Muscle Rehabilitation Exercises in Overhead Athletes With Impingement SymptomsTheologos PardalidisPas encore d'évaluation
- The Effect of A Qualitative Training Program With Supplements On Some Physiological, Physical Variables & Skill Performance in FootballDocument5 pagesThe Effect of A Qualitative Training Program With Supplements On Some Physiological, Physical Variables & Skill Performance in FootballThe Swedish Journal of Scientific Research (SJSR) ISSN: 2001-9211Pas encore d'évaluation
- Bailey 2018Document12 pagesBailey 2018壮Pas encore d'évaluation
- Effect of Graded Plank Protocol On Core Stability in Sedentary DentistsDocument5 pagesEffect of Graded Plank Protocol On Core Stability in Sedentary DentistsVizaPas encore d'évaluation
- Ajustes Posturales Anticipatorios y Compensatorios en PCDocument10 pagesAjustes Posturales Anticipatorios y Compensatorios en PCPamela DíazPas encore d'évaluation
- Neuromuscular Training Improves Performance On The Star Excursion Balance Test in Young Female AthletesDocument8 pagesNeuromuscular Training Improves Performance On The Star Excursion Balance Test in Young Female Athletesrduran621679Pas encore d'évaluation
- 28 - Jpts 2015 650Document7 pages28 - Jpts 2015 650Mahmoud A KhatabPas encore d'évaluation
- Accepted Manuscript: 10.1016/j.jbmt.2014.05.011Document16 pagesAccepted Manuscript: 10.1016/j.jbmt.2014.05.011Diana Magnavita MouraPas encore d'évaluation
- Soap Note ExampleDocument3 pagesSoap Note ExampleJosh KuntzPas encore d'évaluation
- Lumbar Herniation Case StudyDocument1 pageLumbar Herniation Case Studyapi-238652699Pas encore d'évaluation
- Electromyographic Activity of Rectus Abdominis Muscles During Dynamic Pilates Abdominal ExercisesDocument8 pagesElectromyographic Activity of Rectus Abdominis Muscles During Dynamic Pilates Abdominal ExercisesNuno RodolfoPas encore d'évaluation
- OsjcbdgsnDocument3 pagesOsjcbdgsnpriesha aprilia03Pas encore d'évaluation
- 5-4-26 1 IjyppeDocument7 pages5-4-26 1 IjyppeMansi ParmarPas encore d'évaluation
- Ultrasound Evaluation of The Abdominal Wall and Lumbar Multifidus Muscles in Participants Who Practice Pilates: A 1-Year Follow-Up Case SeriesDocument11 pagesUltrasound Evaluation of The Abdominal Wall and Lumbar Multifidus Muscles in Participants Who Practice Pilates: A 1-Year Follow-Up Case SeriesDiana Magnavita MouraPas encore d'évaluation
- Scapular Bracing and Alteration of PostureDocument3 pagesScapular Bracing and Alteration of PostureMaximiliano Alejandro MPas encore d'évaluation
- Effects of Pilates Exercise On Trunk STRDocument9 pagesEffects of Pilates Exercise On Trunk STRyuliana fatmalaPas encore d'évaluation
- 23 247Document4 pages23 247Ita MagdalenaPas encore d'évaluation
- Effects of Caffeine On Session Ratings of Perceived ExertionDocument7 pagesEffects of Caffeine On Session Ratings of Perceived ExertionJackson PiercePas encore d'évaluation
- Sample TemplatesDocument153 pagesSample TemplatesRusty Kuule50% (2)
- Pilates Aumeto de Força em Idosos 2017Document32 pagesPilates Aumeto de Força em Idosos 2017Lex MHZPas encore d'évaluation
- Effect of Isometric Quadriceps Exercise On Muscle StrengthDocument7 pagesEffect of Isometric Quadriceps Exercise On Muscle StrengthAyu RosePas encore d'évaluation
- Balance & Mobility Following Stroke: Effects of Physical Therapy Interventions With & WithoutDocument38 pagesBalance & Mobility Following Stroke: Effects of Physical Therapy Interventions With & WithoutJen PassilanPas encore d'évaluation
- Art 63, PP 407 - 412Document6 pagesArt 63, PP 407 - 412Yusuf WildanPas encore d'évaluation
- Assessment of Motion and Muscle Activation Impacts On Low Back Pain During Pregnancy Using An Inertial Measurement UnitDocument14 pagesAssessment of Motion and Muscle Activation Impacts On Low Back Pain During Pregnancy Using An Inertial Measurement UnitNuno RobertoPas encore d'évaluation
- Final Ppt-VarshuDocument13 pagesFinal Ppt-Varshuzamren kafelaPas encore d'évaluation
- Lab Report Sps 477 Physiology of Sport and Exercise Group Sr243S1Document10 pagesLab Report Sps 477 Physiology of Sport and Exercise Group Sr243S1Titis Retno Sawitri SawitriPas encore d'évaluation
- Effectiveness of Antenatal Motor Relearning Approach of Diaphragm, Deep Abdominal and Pelvic Floor Muscles Versus Kegels Exercises On Postpartum Pelvic Floor Muscle StrengthDocument6 pagesEffectiveness of Antenatal Motor Relearning Approach of Diaphragm, Deep Abdominal and Pelvic Floor Muscles Versus Kegels Exercises On Postpartum Pelvic Floor Muscle StrengthRira Fauziah IPas encore d'évaluation
- Single Set Vs Multiple Sets 2004Document6 pagesSingle Set Vs Multiple Sets 2004turbobrikPas encore d'évaluation
- InserviceDocument16 pagesInserviceapi-550726251Pas encore d'évaluation
- Coursework FinalDocument1 pageCoursework FinalEmma NewberryPas encore d'évaluation
- Dr. G K Dhokrat 1Document4 pagesDr. G K Dhokrat 1Anonymous CwJeBCAXpPas encore d'évaluation
- 1.research PaperDocument18 pages1.research PaperbinPas encore d'évaluation
- Final Research Proposal-Evidence-Based PracticeDocument19 pagesFinal Research Proposal-Evidence-Based Practiceapi-677775315Pas encore d'évaluation
- Dr. G K Dhokrat 2Document5 pagesDr. G K Dhokrat 2Anonymous CwJeBCAXpPas encore d'évaluation
- Effectiveness of Home Exercise On Pain andDocument34 pagesEffectiveness of Home Exercise On Pain andsendilcoumarv83Pas encore d'évaluation
- Effects of Stabilization Exercise Using Flexi-Bar OnDocument5 pagesEffects of Stabilization Exercise Using Flexi-Bar OnYoh ChenPas encore d'évaluation
- Managing Tic and Habit Disorders: A Cognitive Psychophysiological Treatment Approach with Acceptance StrategiesD'EverandManaging Tic and Habit Disorders: A Cognitive Psychophysiological Treatment Approach with Acceptance StrategiesPas encore d'évaluation
- Range of Joint Evaluation ChartDocument2 pagesRange of Joint Evaluation ChartSyafiq Ishak100% (2)
- Normal Gait Mechanics: Weight UnloadingDocument3 pagesNormal Gait Mechanics: Weight UnloadingequalbenPas encore d'évaluation
- 17277561Document13 pages17277561equalbenPas encore d'évaluation
- Effect of Functional Electrical Stimulation On Asymmetries in Gait of Children With Hemiplegic Cerebral PalsyDocument9 pagesEffect of Functional Electrical Stimulation On Asymmetries in Gait of Children With Hemiplegic Cerebral PalsyequalbenPas encore d'évaluation
- Stimulation With High-Frequency TENS - Effects On Lower Limb Spasticity After StrokeDocument6 pagesStimulation With High-Frequency TENS - Effects On Lower Limb Spasticity After StrokeequalbenPas encore d'évaluation
- ICF Parental Consent-ClinicalstudiesDocument10 pagesICF Parental Consent-ClinicalstudiesequalbenPas encore d'évaluation
- T Tens A: Echniques OF PplicationDocument3 pagesT Tens A: Echniques OF PplicationequalbenPas encore d'évaluation
- The Effect of Physiotherapy On Sit-To-Stand Movements in A Child With Spastic DiplegiaDocument9 pagesThe Effect of Physiotherapy On Sit-To-Stand Movements in A Child With Spastic DiplegiaequalbenPas encore d'évaluation
- Who Boys Z Score PDFDocument15 pagesWho Boys Z Score PDFRizky Indah SorayaPas encore d'évaluation
- Speech SkincareDocument2 pagesSpeech SkincarePI40621 Fatin Alyaa Binti Abdullah ZawawiPas encore d'évaluation
- WECOC Final Announcement 29th CompressedDocument32 pagesWECOC Final Announcement 29th CompressedChristabella Natalia WijayaPas encore d'évaluation
- Inglés 8-2 AnexoDocument38 pagesInglés 8-2 AnexoEsperanza RiverosPas encore d'évaluation
- AmoebiasisDocument54 pagesAmoebiasistummalapalli venkateswara rao0% (1)
- 2017 Coca Cola Foundation GrantsDocument51 pages2017 Coca Cola Foundation GrantsPrincess PatagocPas encore d'évaluation
- Advanced Cardiovascular Life Support in Adults (ACLS) : SubtitleDocument30 pagesAdvanced Cardiovascular Life Support in Adults (ACLS) : SubtitleMohamad El SharPas encore d'évaluation
- Astm A 10.11Document13 pagesAstm A 10.11edu_canetePas encore d'évaluation
- Nursing TheoryDocument13 pagesNursing TheoryYana VictyPas encore d'évaluation
- Attitude of EMPLOYEES in Terms of Compliance of Health and SafetyDocument6 pagesAttitude of EMPLOYEES in Terms of Compliance of Health and SafetyJanice KimPas encore d'évaluation
- Fiscal Year 2014 BUDGET of The United States GovernmentDocument244 pagesFiscal Year 2014 BUDGET of The United States GovernmentAlex Tango FuegoPas encore d'évaluation
- Dukungan Sosial Dan Post-Traumatic Stress DisorderDocument7 pagesDukungan Sosial Dan Post-Traumatic Stress DisordercholiidPas encore d'évaluation
- Wintrobe Anemia On Chronic DiseaseDocument31 pagesWintrobe Anemia On Chronic DiseaseDistro ThedocsPas encore d'évaluation
- Lockout/Tagout (Loto) Checklist: 1. Scope of WorkDocument3 pagesLockout/Tagout (Loto) Checklist: 1. Scope of WorkPutri UnaPas encore d'évaluation
- Global Mental Health StudyDocument37 pagesGlobal Mental Health StudyAustin DeneanPas encore d'évaluation
- Nurses Role in Drug Therapy: BY Puan Haslinda Binti Dan NURSING BLOCK 2008/2009Document40 pagesNurses Role in Drug Therapy: BY Puan Haslinda Binti Dan NURSING BLOCK 2008/2009Rhomizal MazaliPas encore d'évaluation
- Characterization of Glaucoma Medication Adherence in Kaiser Permanente Southern CaliforniaDocument5 pagesCharacterization of Glaucoma Medication Adherence in Kaiser Permanente Southern CaliforniaAu ZouPas encore d'évaluation
- PRC-BON Resolution No. 17 Series of 2010Document2 pagesPRC-BON Resolution No. 17 Series of 2010PhilippineNursingDirectory.comPas encore d'évaluation
- Self-Esteem Moderates The Associations Between Body-Related Self-Conscious Emotions and Depressive SymptomsDocument11 pagesSelf-Esteem Moderates The Associations Between Body-Related Self-Conscious Emotions and Depressive SymptomsAlliyah Roma CadaPas encore d'évaluation
- Kertas Trial English Perlis K1 Set B 2021Document13 pagesKertas Trial English Perlis K1 Set B 2021darwish erfanPas encore d'évaluation
- Draft LKPDDocument34 pagesDraft LKPDaliPas encore d'évaluation
- Rewire Your BrainDocument0 pageRewire Your BrainJohn Bates100% (1)
- Jadual Respiro 2021Document16 pagesJadual Respiro 2021yayayayayayayaPas encore d'évaluation
- Mirena BrochureDocument24 pagesMirena BrochureNamrata HarishPas encore d'évaluation
- SPA vs. GPADocument24 pagesSPA vs. GPAYabb TabianPas encore d'évaluation
- Beyond OralityDocument27 pagesBeyond OralityYnon WeismanPas encore d'évaluation
- El Gran Libro de HTML5 CSS3 y JavascriptDocument303 pagesEl Gran Libro de HTML5 CSS3 y JavascriptHeriberto Aguirre MenesesPas encore d'évaluation
- TRAINING WORKSHOP FOR TRADITIONAL HERBAL MEDICAL PRACTIONERS Ode OmuDocument2 pagesTRAINING WORKSHOP FOR TRADITIONAL HERBAL MEDICAL PRACTIONERS Ode OmuOlatunji Adebisi TundePas encore d'évaluation
- Evs 3Document22 pagesEvs 3Shillin KsPas encore d'évaluation
- 1 s2.0 S187878861000086X MainDocument12 pages1 s2.0 S187878861000086X MainAngeel GomezPas encore d'évaluation