Académique Documents
Professionnel Documents
Culture Documents
Brachial Plexus
Transféré par
Tuğcan YüksekDescription originale:
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Brachial Plexus
Transféré par
Tuğcan YüksekDroits d'auteur :
Formats disponibles
BRACHIAL PLEXUS
Specific branches
Bold indicates primary spinal root component of nerve. Italics indicate spinal roots that frequently, but not always, contribute to the nerve.
[2]
From
Nerve
Roots
Muscles
Cutaneous
roots
dorsal scapular nerve
C4, C5
rhomboid muscles and levator scapulae -
roots
long thoracic nerve C5, C6,C7 serratus anterior
upper trunk
nerve to the subclavius
C5, C6
subclavius muscle
upper trunk
suprascapular nerve
C5, C6
supraspinatus and infraspinatus
lateral cord
lateral pectoral nerve
C5, C6, C7
pectoralis major and pectoralis minor (by communicating with the medial pectoral nerve)
lateral cord
musculocutaneous C5, C6, nerve C7
coracobrachialis, brachialis and biceps brachii
becomes the lateral cutaneous nerve of the forearm
lateral cord
lateral root of the median nerve
C5, C6, C7
fibres to the median nerve
posterior upper subscapular C5, C6 cord nerve
subscapularis (upper part)
thoracodorsal C6, C7, posterior nerve(middle cord C8 subscapular nerve)
latissimus dorsi
posterior lower subscapular cord nerve
C5, C6
subscapularis (lower part ) and teres major
posterior axillary nerve cord
C5, C6
anterior branch: deltoid and a small area of overlying skin posterior branch: teres minor and deltoid muscles
posterior branch becomes upper lateral cutaneous nerve of the arm
posterior radial nerve cord
C5, C6, C7, C8, T1
triceps brachii, supinator, anconeus, the extensor muscles of the forearm, andbrachioradialis
skin of the posterior arm as the posterior cutaneous nerve of the arm
medial cord
medial pectoral nerve
C8, T1
pectoralis major and pectoralis minor
medial cord
medial root of themedian nerve
C8, T1
fibres to the median nerve
portions of hand not served by ulnar or radial
medial cord
medial cutaneous nerve of the arm
C8, T1
front and medial skin of the arm
medial cord
medial cutaneous nerve of the forearm
C8, T1
medial skin of the forearm
medial cord
ulnar nerve
C8, T1
flexor carpi ulnaris, the medial two bellies of flexor digitorum profundus, the intrinsic hand muscles except the thenar muscles and the two most lateral lumbricals
the skin of the medial side of the hand and medial one and a half fingers on the palmar side and medial two and a half fingers on the dorsal side
Posterior cord branches
STAR - subscapular (upper and lower), thoracodorsal, axillary, radial RATS- Radial nerve, Axillary nerve, Thoracodorsal nerve, Subscapular (Upper & Lower)nerve. ULTRA - upper subscapular, lower subscapular, thoracodorsal, radial, axillary ULNAR- Upper subscapular nerve, Lower subscapular nerve,Nerve to lattissimus dorsi, Axillary nerve, Radial nerve.
Lateral Cord Branches
LLM "Lucy Loves Me" - lateral pectoral, lateral root of the median nerve, musculocutaneous Love Me Latha (LML) - Lateral pectoral nerve, Musculocutaneous nerve, Lateral root of Median Nerve.
Medial Cord Branches MMMUM "Most Medical Men Use Morphine" - medial pectoral, medial cutaneous nerve of arm, medial cutaneous nerve of forearm, ulnar, medial root of the median nerve
Union of 4 Medials - Ulnar nerve, Medial cutaneous nerve of arm, Medial cutaneous nerve of forearm, Medial pectoral nerve, Medial root of Median Nerve.
5 main nerves of brachial plexus, in order laterally to medially
"My Aunty Raped My Uncle" - Musculocutaneous, axillary, radial, median, ulnar
Injuries to the brachial plexus affect cutaneous sensations and movements in the upper limb. They can be caused by stretching, diseases, and wounds to the lateral cervical region (posterior triangle) of the neck or the axilla. Depending on the location of the injury, the signs and symptoms can range from complete paralysis to anesthesia. Testing the patient's ability to perform movements and comparing it to their normal side is a method to assess the degree of paralysis. A common brachial plexus injury is from a hard landing where the shoulder widely separates from the neck (such as in the case of motorcycle accidents or falling from a tree). These stretches can cause ruptures to the superior portions of the brachial plexus or avulse the roots from the spinal cord. Upper brachial plexus injuries are frequent in newborns when excessive stretching of the neck occurs during delivery. Studies have shown a relationship between birth weight and brachial plexus injuries; however, the [3] number of cesarean deliveries necessary to prevent a single injury is high at most birth weights. For the upper brachial plexus injuries, paralysis occurs in those muscles supplied by C5 and C6 like the deltoid, biceps, brachialis, and brachioradialis. A loss of sensation in the lateral aspect of the upper limb is also common with such injuries. An inferior brachial plexus injury is far less common, but can occur when a person grasps something to break a fall or a baby's upper limb is pulled excessively during delivery. In this case, the short muscles of the hand would be affected and cause the inability [4] to form a full fist position. Acute brachial plexus neuritis is a neurological disorder that is characterized by the onset of severe pain in the shoulder region. Additionally, the compression of cords can cause pain radiating down the arm, numbness, paresthesia, erythema, and weakness of the hands. This kind of injury is common for people who have prolonged hyperabduction of the arm when they are performing tasks above their head.
Injuries During Birth
Brachial Plexus injuries also become an issue during the delivery of newborns. there were 80 [8] brachial plexus injuries identified, for an incidence of 1.03 per 1000 live birth. Nerve damage has been connected to birth weight with larger newborns being more susceptible to the injury but it also has to do with the delivery methods. Although very hard to prevent during live birth, doctors must be able to deliver a newborn with precise and gentle movements in order to decrease chances of injuring the child.
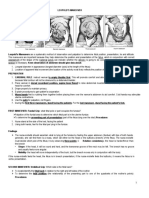
A pregnancy that has progressed without any apparent hitch can still give way to complications during delivery. Here are some of the most common concerns: Preterm Labor and Premature Delivery One of the greatest dangers a baby faces is being born too early, before his or her body systems are mature enough to ensure survival. The lungs, for example, may not be able to breathe air, or the baby's body may not generate enough heat to keep warm. A full-term pregnancy normally lasts about 38 to 40 weeks. Having labor contractions before 37 weeks of pregnancy is called preterm labor. A baby born before 37 weeks of pregnancy is considered a premature baby who is at risk of complications of prematurity, such as immature lungs, respiratory distress, and digestive problems. Prolonged Labor (Failure to Progress) A small percentage of women, mostly first-time mothers, may experience a labor that lasts too long, sometimes called "failure to progress." Both the mother and the baby are at risk for several complications, including infections, if the amniotic sac ruptures and the birth doesn't follow. Abnormal Presentation "Presentation" refers to the part of the baby that will appear first from the birth canal. In the weeks before your due date, the fetus usually drops lower in the uterus. Ideally, for labor, the baby is positioned head-down, facing the mother's back, with its chin tucked to its chest and the back of the head ready to enter the pelvis. That way, the smallest possible part of the baby's head leads the way through the cervix and into the birth canal. This normal presentation is called vertex (head down). Because the head is the largest and least flexible part of the baby, it's best for the head to lead the way into the birth canal. That way, there's little risk that the baby's body will make it through the birth canal, but the head will get hung up. Some fetuses present with their buttocks or feet pointed down toward the birth canal. This is called a breech presentation. Breech presentations are commonly observed during an ultrasound exam far before the due date, but most babies will turn to the normal head-down presentation as they get closer to the due date. Frank breech. In a frank breech, the baby's buttocks lead the way into the pelvis; the hips are flexed, the knee extended. Complete breech. In a complete breech, both knees and hips are flexed, and the baby's buttocks or feet may enter the birth canal first. Incomplete breech. In an incomplete or footling or breech, one or both feet lead the way. Transverse lie. A few babies lie horizontally in the uterus, called a transverse lie, which usually means the baby's shoulder will lead the way into the birth canal rather than the head. Umbilical Cord Compression Because the fetus moves and kicks inside the uterus, the umbilical cord can wrap and unwrap itself around the baby many times throughout pregnancy. While there are "cord accidents" in which the cord gets twisted around and harms the baby, this is extremely rare and usually can't be prevented. Sometimes the umbilical cord gets stretched and compressed during labor, leading to a brief decrease in blood flow to the fetus. This can cause sudden, short drops in fetal heart rate, called variable decelerations, which are usually picked up by monitors during labor. Cord compression happens in about one in 10 deliveries. In most cases, these heart rate changes are of no major concern, and the birth proceeds normally. But a cesarean delivery may be necessary if the baby's heart rate worsens or the fetus shows other signs of distress, such as a decrease of fetal blood pH
Electromyography (EMG) is a technique for evaluating and recording the electrical activity produced [1] by skeletal muscles. EMG is performed using an instrumentcalled an electromyograph, to produce a record called an electromyogram. An electromyograph detects the electrical potential generated by [2] muscle cells when these cells are electrically or neurologically activated. The signals can be analyzed to detect medical abnormalities, activation level, recruitment order or to analyze the biomechanics of human movement.
The Moro reflex is an infantile reflex normally present in all infants/newborns up to 4 or 5 months of age as a response to a sudden loss of support, when the infant feels as if it is falling. It involves 3 distinct components: 1. spreading out the arms (abduction) 2. unspreading the arms (adduction) 3. crying (usually) The primary significance of the Moro reflex is in evaluating integration of the central nervous system. [1] It is distinct from the startle reflex, and is believed to be the only unlearned fear in human newborns The Moro reflex may be observed in incomplete form in premature birth after the 28th week of gestation, and is usually present in complete form by week 34 (third trimester). Absence or asymmetry of either abduction or adduction is abnormal, as is persistence of the reflex in older infants, children and adults. Absence indicates a profound disorder of the motor system. An absent or inadequate Moro response on one side is found in infants with hemiplegia, brachial plexus palsy, or a fractured clavicle.
The palmar grasp reflex appears at birth and persists until five or six months of age. When an object is placed in the infant's hand and strokes their palm, the fingers will close and they will grasp it with a palmar grasp. The grip is strong but unpredictable; though it may be able to support the child's weight, they may also release their grip suddenly and without warning. The reverse motion can be induced by stroking the back or side of the hand.
Vous aimerez peut-être aussi
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Will Obstetri 2-8 Maret 2018Document16 pagesWill Obstetri 2-8 Maret 2018Shandy Suwanto Putra100% (2)
- Problems With The PassengerDocument65 pagesProblems With The Passengermark Orpilla100% (1)
- Compensatory MechanismDocument30 pagesCompensatory MechanismSenthil Kumar Elumalai100% (1)
- Multiple Pregnancy LectureDocument33 pagesMultiple Pregnancy Lecturefarid_nchep100% (1)
- Quiz RenalDocument81 pagesQuiz RenalMedShare86% (14)
- QuestionsDocument23 pagesQuestionsTuğcan YüksekPas encore d'évaluation
- Quiz Anatomy Part 3 of 3Document56 pagesQuiz Anatomy Part 3 of 3MedShare75% (4)
- QuestionsDocument23 pagesQuestionsTuğcan YüksekPas encore d'évaluation
- Quiz Anatomy Part 3 of 3Document56 pagesQuiz Anatomy Part 3 of 3Tuğcan YüksekPas encore d'évaluation
- Anato Qiuestions 1Document5 pagesAnato Qiuestions 1Tuğcan YüksekPas encore d'évaluation
- Anato Qiuestions 1Document5 pagesAnato Qiuestions 1Tuğcan YüksekPas encore d'évaluation
- Anato Qiuestions 1Document5 pagesAnato Qiuestions 1Tuğcan YüksekPas encore d'évaluation
- Breech PresentationDocument18 pagesBreech PresentationironPas encore d'évaluation
- Preterm BreechDocument38 pagesPreterm Breechorin78Pas encore d'évaluation
- Skill Lab SpecificationsDocument17 pagesSkill Lab Specificationssrboghe651665Pas encore d'évaluation
- OB Normal Labor and Delivery 1Document6 pagesOB Normal Labor and Delivery 1Rea Dominique CabanillaPas encore d'évaluation
- Beaulé, P. E. (Ed.) - (2020) - Hip DysplasiaDocument247 pagesBeaulé, P. E. (Ed.) - (2020) - Hip DysplasiaWilson A. Quintero100% (1)
- Emergencydelivery: Michele CallahanDocument14 pagesEmergencydelivery: Michele CallahanSandra Díaz MercadoPas encore d'évaluation
- A Proposal For A'new Method of Evaluation - of The Newborn Infant PDFDocument8 pagesA Proposal For A'new Method of Evaluation - of The Newborn Infant PDFcbac1990Pas encore d'évaluation
- Transverse Fetal LieDocument6 pagesTransverse Fetal LieJenny WoodruffPas encore d'évaluation
- Malpresentation and Malposition - ShoulderDocument5 pagesMalpresentation and Malposition - ShoulderNishaThakuri100% (1)
- OR Write Up - Repeat LSCSDocument2 pagesOR Write Up - Repeat LSCSWyen CabatbatPas encore d'évaluation
- NCM 107maternal FinalsDocument84 pagesNCM 107maternal FinalsFranz goPas encore d'évaluation
- SMLE TOP Gs - September 2023 (Part 1)Document589 pagesSMLE TOP Gs - September 2023 (Part 1)zzmmaallqqpp911Pas encore d'évaluation
- Obstetric History & Examination SheetDocument8 pagesObstetric History & Examination SheetVaibhav BhatiaPas encore d'évaluation
- Transverse LieDocument7 pagesTransverse LieKezia JessicaPas encore d'évaluation
- Leopolds and FetalDocument7 pagesLeopolds and Fetaltyche100% (1)
- Seminar On Obstructed LabourDocument98 pagesSeminar On Obstructed Labourtesfahuntekletilahun80% (5)
- OBS Oral Sheet Not AnsweredDocument5 pagesOBS Oral Sheet Not AnsweredMuhammed MostafaPas encore d'évaluation
- Plab 2 Recall 5Document137 pagesPlab 2 Recall 5Sadiya IslamPas encore d'évaluation
- Ncma 217 Week 7: Intrapartal CareDocument11 pagesNcma 217 Week 7: Intrapartal CareABEGAIL BALLORANPas encore d'évaluation
- MK Fetal Lie and Presentation (OBGY)Document9 pagesMK Fetal Lie and Presentation (OBGY)Moses Jr KazevuPas encore d'évaluation
- Complicated Labor and DeliveryDocument226 pagesComplicated Labor and Deliveryrhimineecat71100% (1)
- Multiple PregnancyDocument39 pagesMultiple PregnancyNoahPas encore d'évaluation
- Gauss Without AnswersDocument115 pagesGauss Without AnswersAshish R. JadhavPas encore d'évaluation
- Compound PresentationDocument10 pagesCompound PresentationmaezuPas encore d'évaluation
- Normal Labor and DeliveryDocument61 pagesNormal Labor and DeliverySulistianto TianPas encore d'évaluation
- Anatomy and Physiology of Breech PresentationDocument2 pagesAnatomy and Physiology of Breech Presentationeskempertus0% (2)