Académique Documents
Professionnel Documents
Culture Documents
Radical Cystectomy: History of The Procedure
Transféré par
Ivy MinaTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Radical Cystectomy: History of The Procedure
Transféré par
Ivy MinaDroits d'auteur :
Formats disponibles
Radical Cystectomy
A radical cystectomy is done to treat bladder cancer. This means the surgeon removes the bladder, uterus, ovaries, fallopian tubes, cervix, front wall of the vagina, and the urethra. Although women who have this surgery are often past the age of menopause, many still have active sex lives.
History of the Procedure
The first record of a radical cystectomy dates to the late 1800s. In 1949, Marshall and Whitmore described the basic surgical principles of radical cystoprostatectomy. In 1987, following the neuroanatomic mapping of the pelvic plexus by Schlegel and Walsh, nerve-sparing cystectomy became a surgical option that allowed for preservation of sexual function.[1] For many years, radical cystectomy carried a significant perioperative mortality rate (5%-10%). However, presumably because of improvements in surgical technique, the evolution of intensive care medicine, and the availability of new antibiotics, radical cystectomy is now a common procedure in major medical centers and carries a perioperative mortality rate of approximately 1%-2%.[2] At high-volume centers with postoperative pathway care programs, an ICU stay is no longer routine and the median hospital stay is approximately 7 days.
Problem
Bladder cancer can be axiomatically subdivided into nonmuscle invasive and muscle-invasive disease. This article focuses primarily on the management of muscle-invasive transitional cell carcinoma (TCC) and the role of radical cystectomy.
Epidemiology
Frequency United States More than 90% of bladder cancers are TCC. Bladder cancer diagnoses increased by 36% from 1984-1993. In the United States, up to 600,000 people have bladder cancer. In 2008, an estimated 68,000 new cases of bladder cancer were diagnosed, and 14,000 persons died of the disease.[3] In 2008, the male-to-female incidence ratio was 2.9:1, and the male-to-female mortality ratio is 2.4:1.[3] Bladder cancer is more common in whites than in African Americans. The average age at diagnosis is 65 years. Screening of asymptomatic individuals is not currently recommended. International In 1996, an estimated 310,000 new cases of bladder cancer were diagnosed worldwide. The incidence rate in Western Europe and North America is higher than in East Asian countries. In developing countries, many bladder cancers are SCCs caused by the parasiteSchistosoma haematobium. In high-prevalence regions, SCC of the bladder has enormous health implications (eg, SCC is the most common solid tumor in Egyptian men).
Etiology
Environmental risk factors
Smoking Exposure to aromatic amines found in some dyes, paints, solvents, leather dust, inks, combustion products, rubbers, and textiles Prior radiation therapy. Women who have undergone pelvic radiation (eg, for cervical cancer) have a 2- to 4-fold increased incidence rate; survival rates are poorer in men who
have undergone radiation for prostate cancer than in men of similar age and stage who have not undergone radiation. Low daily fluid intake may be a contributing factor. Schistosomiasis caused by the parasite S haematobium can cause SCC; this is common in Egypt and the Nile River Valley. Long-term phenacetin use Long-term placement of indwelling catheters is a risk factor; patients who have indwelling catheters for longer than 10 years should undergo bladder surveillance via cytology and cystoscopy. Artificial sweeteners (saccharin, cyclamate), when administered in high doses to laboratory animals, are risk factors for bladder cancer; no similar evidence has been shown in humans. The use of Aristolochia fangchi, a Chinese herb, has been implicated as a risk factor for both upper and lower tract TCC. Coffee and tea are not risk factors for bladder cancer.
Pathophysiology
As with most neoplasms, bladder carcinogenesis is a complex multistep process that is not fully understood. Activation of proto-oncogenes, loss or inactivation of tumor suppressor genes, and abnormal growth factor or receptor expression have been implicated. Multiple mutations of chromosome 9 have been identified in superficial bladder cancer cells. Increased expression of the epidermal growth factor receptor and increased mutations of tumor suppressor genes (eg, TP53 and Rb) are common in patients with advanced bladder cancer. Mutations and nuclear accumulation ofTP53 have been correlated with an increased grade, stage, and recurrence risk. The risk of progression to muscle-invasive disease is associated with tumor grade, stage (Ta vs T1), size, number of lesions (solitary vs multiple lesions), previous tumor recurrence, and presence of CIS.
Presentation
Gross or microscopic hematuria is the initial presenting sign in 80%-90% of patients. Approximately 20% of patients have irritative symptoms such as urinary urgency, dysuria, or frequency. This presentation is typical in patients with diffuse CIS, which can be confused with a urinary tract infection and can result in a delayed diagnosis. With the more routine use of crosssectional imaging, many bladder lesions are incidentally diagnosed. Patients with muscleinvasive disease can present with incidental or symptomatic obstructive hydroureteronephrosis or, less commonly, with metastatic deposits. These factors make bladder cancer a very uncommon incidental finding on autopsy.
Indications
Indications for radical cystectomy include the following: Infiltrating muscle-invasive bladder cancer without evidence of metastasis or with lowvolume, resectable locoregional metastases (stage T2-T3b) Superficial bladder tumors characterized by any of the following: o Refractory to cystoscopic resection and intravesical chemotherapy or immunotherapy (Up to 71% of these patients may progress to stage T2 within 5 years of initial recurrence.) o Extensive disease not amenable to cystoscopic resection o Invasive prostatic urethral involvement Stage-pT1, grade-3 tumors unresponsive to intravesical BCG vaccine therapy CIS refractory to intravesical immunotherapy or chemotherapy Palliation for pain, bleeding, or urinary frequency Primary adenocarcinoma, SCC, or sarcoma
Indications for urethrectomy include the following: Tumor in the anterior urethra Prostatic stromal invasion that is noncontiguous with the primary Positive urethral margin during radical cystectomy Diffuse CIS of bladder, prostatic ducts, or prostatic urethra (a relative indication)
Anatomy and Physiology
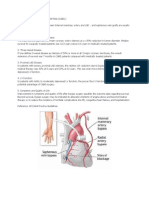
The anatomy of the bladder forms an extraperitoneal muscular urine reservoir that lies behind the pubic symphysis in the pelvis. A normal bladder functions through a complex coordination of musculoskeletal, neurologic, and psychological functions that allow filling and emptying of the bladder contents. The prime effector of continence is the synergic relaxation of detrusor muscles and contraction of the bladder neck and pelvic floor muscles.
Gross anatomy of the bladder.
The normal adult bladder accommodates 300600 mL of urine; a central nervous system (CNS) response is usually triggered when the volume reaches 400 mL. However, urination can be prevented by cortical suppression of the peripheral nervous system or by voluntary contraction of the external urethral sphincter.
Contraindications
Contraindications to radical cystectomy include (1) bleeding diathesis, (2) evidence of gross, unresectable metastatic disease (unless performed for palliation), and (3) medical comorbidities that preclude operative intervention (eg, advanced heart disease, poor pulmonary mechanics, advanced age).
Treatment
Medical Therapy
Alternative therapy for mscle-invasive disease Transurethral resection of bladder tumor (TURBT) alone: Risks include incomplete resection, a high rate of disease recurrence, and the potential for disease progression. Systemic chemotherapy in combination with TURBT This regimen has historically included methotrexate, vinblastine, doxorubicin (Adriamycin), and cisplatin (MVAC). A doublet of gemcitabine and cisplatin has shown similar response rates to MVAC in the metastatic setting and is easier to tolerate; therefore, this regimen is often considered the first-line therapy. Primary radiation therapy: This therapy is more commonly used in countries outside the United States for patients with T2 and T3 cancer. The 5-year survival rate is 20%-40% (less than radical cystectomy). Bladder-sparing multimodality therapy Transurethral resection plus radiation therapy and concomitant cisplatin-based chemotherapy carries a 3- to 5-year estimated survival rate of 45%-64%. Delayed cystectomy is often required for palliation of symptoms or for recurrent disease. At 5 years following treatment, approximately 40% of patients are disease-free with their native bladder. No significant improvement over up-front cystectomy has been shown, and the burden of therapy is often greater in patients who undergo multimodal therapy. This therapy is considered only in patients who are highly motivated to preserve their bladder and reliably adhere to the rigorous surveillance protocol required.
Partial cystectomy: Partial cystectomy is for highly selected patients with a single tumor at a single point in time in a surgically amenable location who have no associated CIS and a bladder volume capable of tolerating a partial resection. Patients must be willing to accept the risk of local recurrence within the retained bladder and the risk of disease progression.
Surgical Therapy
Patients who undergo radical cystectomy may benefit from a cancer-specific survival advantage when neoadjuvant chemotherapy is given prior to surgery. The rationale of preoperative chemotherapy includes treatment of micrometastatic disease and pathologic downstaging. However, some patients with node-negative disease are needlessly treated with chemotherapy; in addition, surgery is significantly delayed. A recent meta-analysis of 11 trials showed an overall survival rate benefit of 6.5% among patients who received neoadjuvant chemotherapy. If locally advanced TCC is suspected based on clinical staging, the rationale for neoadjuvant chemotherapy prior to cystectomy is even stronger.
Preoperative Details
Prehospital Consideration of neoadjuvant chemotherapy for stage pT2 disease or higher: Adequate renal function (estimated glomerular filtration rate >60 mL/min) is required to administer cisplatinbased regimens (MVAC or gemcitabine/cisplatin). Cisplatin-based neoadjuvant chemotherapy is the preferred standard when possible, as it has been shown to improve survival rates. Neoadjuvant chemotherapy is preferred over adjuvant chemotherapy because of improved patient tolerance. Evaluation and optimization of cardiopulmonary disease Stoma marking and counseling, if necessary Autologous blood donation, if desired Bowel preparation, with surgeon's choice of clear-liquid diet, magnesium citrate, Phosphosoda, GoLYTELY, or enemas Confirmation of urine sterility Smoking cessation In-hospital Adequate intravenous hydration Nasogastric tube placed intraoperatively (Many centers remove gastric suction at the end of surgery.) Antibiotics with bowel flora coverage Subcutaneous heparin or pneumatic compression stockings Operating room Paralytic anesthetic agent Long, curved, and angled instruments; self-retaining retractor Supine position in men (For concomitant urethrectomy, lithotomy is needed.) Modified lithotomy position with Allen or Lloyd-Davies stirrups in women Sterile preparation and drape from mid chest to mid thigh, including the genitalia and perineum Bladder catheter
Intraoperative Details
Continent cutaneous urinary diversions In 1987, Rowland and associates introduced the Indiana pouch, which is the most commonly used continent cutaneous diversion technique. Approximately 30-40 cm of cecum and ascending colon are isolated with approximately 10 cm of terminal ileum. The colon is detubularized. The terminal ileum is plicated to the size of a 14F catheter with a GIA stapler. The ileocecal valve is buttressed and imbricated as a continence mechanism. The cecum is folded down, shaped into a spherical
reservoir, and closed with 2-0 running absorbable suture. The ureterointestinal anastomoses are placed on the posterior colonic wall and stented perioperatively. A cecostomy tube is placed to drain the pouch and to provide for postoperative irrigation, as needed. The estimated rate of daytime continence is 93% and nocturnal continence, 76%.
Postoperative Details
Optional use of nasogastric suction and stress gastritis prophylaxis Bowel-spectrum antibiotics for 1-2 days Deep vein thrombosis (DVT) prophylaxis - Includes serial compression devices, subcutaneous unfractionated heparin, or low molecular weight heparin Incentive spirometry and chest physiotherapy Removal of Jackson-Pratt drains when less than 150 mL per day accumulates
Complications
Common complications include ileus, atelectasis, DVT, and wound infection. Less common complications include rectal injury, ureteroileal anastomotic leaks, and bowel obstruction.
Nursing Care
Potential long-term sequela and complications for these surgically unique patients do not differ based on approach, robotic versus open. There are several potential complications and issues as a result of cystectomy with urinary diversion. The potential of ureteral anastomosis stricture, urethral stricture (with neobladder), and reservoir rupture (neobladder or Indiana pouch) are rare but must be discussed pre-operatively and taken into account as patient and surgeon discuss options for urinary diversion (personal communication, D. Theodorescu, May 2005). Metabolic complications are monitored with regular lab work and are managed with medications as appropriate. If the patient is undergoing surgery for cancer, the potential for recurrence must be monitored vigilantly. Ideally, this should be by the urologist who performed the surgery for continuity. In continence, as a result of a failed pouch sphincter or neobladder sphincter, can be an outcome that is frustrating for patients and caregivers. Often incontinence can be addressed surgically but must be evaluated carefully. If the incontinence arises in the face of an intact sphincter with poor pouch emptying, then the urologist may implement a regimen of clean intermittent catheterization to allow for consistent reservoir decompression and hopefully return of reservoir tone (personal communication, D. Theodorescu, May 2005). Sexuality for both men and women is often affected with cystectomy surgery. For women, it can affect sexual function since usually the uterus and ovaries are removed with cystectomy. This may lead to menopausal symptoms such as hot flashes or vaginal dryness. If part of the vagina is removed during surgery, then sexual intercourse may be difficult. For men, surgery may damage the nerves that control erections resulting in erectile dysfunction. Fortunately, there are treatments available to address these problems. Patients should be encouraged to discuss their feelings and explore available options with their health care providers. Skin issues are rare but bothersome for patients with an ileal conduit, ileocecal, or Indiana pouch. With the ileal conduit, pouch changes can lead to skin excoriation and tears. Education about proper skin care regimens is important pre and postoperatively, and on return clinic visits. This is
often done by the nurse practitioner or WOC nurse. Since the ileocecal pouch may produce a small amount of mucous at the exit site, a small adhesive bandage or gauze dressing can be placed over the stoma to prevent leakage on clothing. Many patients use mineral oil to keep the stoma moist between catheterizations. Signs and symptoms of urinary tract infection should be taught to patients and caregivers. These are rare but can occur. Fevers and flank pain can be signs of pyelonephritis or pouchitis. Abdominal pain can indicate a sign of infection that may or may not be localized to the urinary reservoir. Urine collected for laboratory assessment will have bacterial colonization due to the use of bowel for reservoir construction. If urine is needed, a double catheterization method can be used to secure a more accurate upstream specimen that can have culture and sensitivity evaluated. Treatment should be guided by culture and sensitivity results.
Vous aimerez peut-être aussi
- ACLS Drug TherapyDocument8 pagesACLS Drug TherapySahrensPas encore d'évaluation
- Pawanmuktasana Series (Part 2)Document20 pagesPawanmuktasana Series (Part 2)bhavna M100% (1)
- Wound AssessmentDocument19 pagesWound Assessmentdrsonuchawla100% (1)
- Assertive Community Treatment TreatmentOptions 2018Document2 pagesAssertive Community Treatment TreatmentOptions 2018titik dyahPas encore d'évaluation
- Pearson Vue 200 QuestionsDocument40 pagesPearson Vue 200 QuestionsdrhirasalmanPas encore d'évaluation
- Oral Squamous Cell Carcinoma (OSCC) : Homam Mansour Abo Orabi 201814250Document15 pagesOral Squamous Cell Carcinoma (OSCC) : Homam Mansour Abo Orabi 201814250Homam MAPas encore d'évaluation
- Ways of Knowing in A Clinical CaseDocument8 pagesWays of Knowing in A Clinical CaseAntonioPas encore d'évaluation
- Trauma and Emergency NursingDocument9 pagesTrauma and Emergency Nursingchinthaka18389021Pas encore d'évaluation
- Diabetes and CancerDocument15 pagesDiabetes and CancerAriHendraWijayanti100% (1)
- Actual SpendingDocument3 pagesActual SpendingPislaru Veaceslav100% (1)
- How To Write An Ethics Paper Mackinnon Fiala 8edDocument13 pagesHow To Write An Ethics Paper Mackinnon Fiala 8edLetYoMama Proud100% (1)
- Surgical Treatment For BREAST CANCERDocument5 pagesSurgical Treatment For BREAST CANCERJericho James TopacioPas encore d'évaluation
- DRUG STUDY: Fenofibrate - TricorDocument2 pagesDRUG STUDY: Fenofibrate - TricorYum CPas encore d'évaluation
- On Floating and Flying WindmillDocument33 pagesOn Floating and Flying WindmillTANISHK JHARWAL100% (1)
- Hypoglycemia: Presented by Farse GhabayenDocument11 pagesHypoglycemia: Presented by Farse GhabayenFares G. Ghabayen100% (2)
- Screening - 2012Document51 pagesScreening - 2012Tin Wann100% (2)
- Pain Management: Lecture Note Powerpoint PresentationDocument48 pagesPain Management: Lecture Note Powerpoint PresentationTobiDaPas encore d'évaluation
- Nursing Diagnosis and Nursing Interventions For Dengue Hemorrhagic FeverDocument2 pagesNursing Diagnosis and Nursing Interventions For Dengue Hemorrhagic FeverThirdy Aquino82% (28)
- Abo Blood Group System GeneticsDocument17 pagesAbo Blood Group System GeneticsSYED MUHAMMAD ALI100% (1)
- Unit 9. Epidemic InvestigationDocument57 pagesUnit 9. Epidemic Investigationbereket gashuPas encore d'évaluation
- Neonatal HypertensionDocument21 pagesNeonatal HypertensionMuhammad Ammar Abdul WahabPas encore d'évaluation
- Post Op Assessment SurgeryDocument20 pagesPost Op Assessment SurgeryAbdullah MatarPas encore d'évaluation
- Practice Essentials of Pulmonary ThromboembolismDocument39 pagesPractice Essentials of Pulmonary ThromboembolismEzzat Abdelhafeez SalemPas encore d'évaluation
- Total Knee Replacement Assignment-Documentation and Clinical Decision Making AssignmentDocument2 pagesTotal Knee Replacement Assignment-Documentation and Clinical Decision Making AssignmentMartin Avilanes Jr.Pas encore d'évaluation
- Coronary Artery Bypass Graft Report NCM 118Document23 pagesCoronary Artery Bypass Graft Report NCM 118Vhince Norben PiscoPas encore d'évaluation
- Zamora - Colon Cancer 2Document25 pagesZamora - Colon Cancer 2Kristel PunoPas encore d'évaluation
- CNUR303 Final NotesDocument30 pagesCNUR303 Final NotesMSPas encore d'évaluation
- EbpDocument21 pagesEbpapi-356303021Pas encore d'évaluation
- The Community Client: Assessment Diagnosis: As andDocument43 pagesThe Community Client: Assessment Diagnosis: As andAbid HussainPas encore d'évaluation
- Of Client Having A Nephrectomy: Nursing CareDocument1 pageOf Client Having A Nephrectomy: Nursing CareJayshree ParmarPas encore d'évaluation
- Coronary Artery Bypass SurgeryDocument12 pagesCoronary Artery Bypass SurgeryCarlos Eduardo Quisse SánchezPas encore d'évaluation
- IMEI Renal DiseaseDocument4 pagesIMEI Renal DiseaseRahadiyan HadinataPas encore d'évaluation
- Needs Assessment Cover PageDocument3 pagesNeeds Assessment Cover Pageapi-291660325Pas encore d'évaluation
- Observation Report - Hemodialysis - Kit P. RoaquinDocument15 pagesObservation Report - Hemodialysis - Kit P. Roaquineljhayar_18Pas encore d'évaluation
- Fluid Management and Shock ResuscitationDocument35 pagesFluid Management and Shock ResuscitationAsrarudin HamidPas encore d'évaluation
- Contemporary ImageDocument43 pagesContemporary ImageProf. L100% (1)
- Syndrome of Inapropriate Antidiuretic Hormone (SIADH)Document15 pagesSyndrome of Inapropriate Antidiuretic Hormone (SIADH)Asrul Rahim100% (1)
- Omaha System Journal ReadingDocument4 pagesOmaha System Journal ReadingAya PaquitPas encore d'évaluation
- Coronary Artery Bypass Grafting (CABG)Document1 pageCoronary Artery Bypass Grafting (CABG)I.m. DanielPas encore d'évaluation
- Cushings SyndromeDocument51 pagesCushings SyndromeTina TalmadgePas encore d'évaluation
- Cardiac TestsDocument17 pagesCardiac TestsGiorgiana pPas encore d'évaluation
- 3112 MultisystemcasestudyDocument9 pages3112 Multisystemcasestudyapi-306118308Pas encore d'évaluation
- C NUR 850 2019 2020 SyllabusDocument14 pagesC NUR 850 2019 2020 SyllabusaamenaPas encore d'évaluation
- Think Nursing! ReportDocument20 pagesThink Nursing! ReportRobert Fraser RNPas encore d'évaluation
- A Care Bundle Approach For Prevention of Ventilator-AssociatedDocument7 pagesA Care Bundle Approach For Prevention of Ventilator-AssociatedRestu Kusuma NingtyasPas encore d'évaluation
- CVPDocument25 pagesCVPNikhil YadavPas encore d'évaluation
- Overview of Acute Pulmonary Embolism in AdultsDocument9 pagesOverview of Acute Pulmonary Embolism in AdultsnathanaelandryPas encore d'évaluation
- Pleural Fluid AnalysisDocument15 pagesPleural Fluid AnalysisNatalie Sarah MoonPas encore d'évaluation
- Blood SugarDocument18 pagesBlood Sugarlaloo01Pas encore d'évaluation
- Emphysematous Pyelonephritis (EPN)Document31 pagesEmphysematous Pyelonephritis (EPN)HardiTariqHammaPas encore d'évaluation
- Case Study HemodialysisDocument5 pagesCase Study HemodialysisCharmaine del RosarioPas encore d'évaluation
- NANDA DefinitionDocument3 pagesNANDA DefinitionDeology JuaninoPas encore d'évaluation
- Nursing Care PlanDocument4 pagesNursing Care PlanPutra AginaPas encore d'évaluation
- Group 5 - Hemodialysis - Chronic Kidney FailureDocument31 pagesGroup 5 - Hemodialysis - Chronic Kidney FailureKimberly Abella CabreraPas encore d'évaluation
- Gastric CarcinomaDocument21 pagesGastric CarcinomaAli Abbas100% (2)
- Fluid and ElectrolytesDocument29 pagesFluid and ElectrolytesLinh Tra100% (1)
- Windshield Survey ComponentDocument1 pageWindshield Survey ComponentMavi RomadaniPas encore d'évaluation
- Acute Respiratory InfectionsDocument18 pagesAcute Respiratory InfectionsEmilyRose17Pas encore d'évaluation
- Concept Map 9 GradedDocument14 pagesConcept Map 9 GradedJen CareyPas encore d'évaluation
- Digital Rectal ExaminationDocument21 pagesDigital Rectal Examinationmegahed7320000Pas encore d'évaluation
- Sexual Dysfunctions Self StudyDocument6 pagesSexual Dysfunctions Self StudymelissagoldenPas encore d'évaluation
- High Sensitivity TroponinsDocument6 pagesHigh Sensitivity TroponinsPhilip ChiangPas encore d'évaluation
- Cancer NursingDocument53 pagesCancer Nursingfairwoods100% (1)
- Colonic Carcinoma Case StudyDocument23 pagesColonic Carcinoma Case StudyGlaiza Claire Am-amlan OlayanPas encore d'évaluation
- Flucloxacillin AFTcapssolnDocument6 pagesFlucloxacillin AFTcapssolnEliza ArmanPas encore d'évaluation
- COMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuideD'EverandCOMPREHENSIVE NURSING ACHIEVEMENT TEST (RN): Passbooks Study GuidePas encore d'évaluation
- What Is High Blood PressureDocument2 pagesWhat Is High Blood PressureTariqPas encore d'évaluation
- Pediatrics, Geriatrics and Clinical MicrobiologyDocument15 pagesPediatrics, Geriatrics and Clinical MicrobiologySelvakumardxbPas encore d'évaluation
- Zabrina Joana DDocument4 pagesZabrina Joana DEmman BalidoPas encore d'évaluation
- Cataracts The Mayo ClinicDocument6 pagesCataracts The Mayo ClinicJandz MNPas encore d'évaluation
- Cause and Effect EssayDocument10 pagesCause and Effect EssayМолдабекова АйсулуPas encore d'évaluation
- Spinal Tumors Intra-Extra (Turgut Tali)Document92 pagesSpinal Tumors Intra-Extra (Turgut Tali)Drbaddireddy RayuduPas encore d'évaluation
- Campy Lo Bacterio SisDocument14 pagesCampy Lo Bacterio SisHarikrishnan NamPas encore d'évaluation
- FHP SampleDocument8 pagesFHP SampleJade GordoncilloPas encore d'évaluation
- Psychosurgery, Epilepsy Surgery, or Surgical Psychiatry: The Tangled Web of Epilepsy and Psychiatry As Revealed by Surgical OutcomesDocument2 pagesPsychosurgery, Epilepsy Surgery, or Surgical Psychiatry: The Tangled Web of Epilepsy and Psychiatry As Revealed by Surgical Outcomesximena sanchezPas encore d'évaluation
- The Lymphatic SystemDocument6 pagesThe Lymphatic SystemErica SharonPas encore d'évaluation
- Oncology NCLEX Questions Flashcards - QuizletDocument50 pagesOncology NCLEX Questions Flashcards - QuizletGLORY MI SHANLEY CARUMBAPas encore d'évaluation
- Treatment: Guillain-Barré Syndrome (GBS) (Document15 pagesTreatment: Guillain-Barré Syndrome (GBS) (akku_m1991Pas encore d'évaluation
- Phototherapy: Prepared By: DR/ Lamiaa Ahmed ElsayedDocument36 pagesPhototherapy: Prepared By: DR/ Lamiaa Ahmed Elsayedngocbienk56Pas encore d'évaluation
- Jonathan C. Lubag Unintentional Injuries Q3M1 W1-3Document26 pagesJonathan C. Lubag Unintentional Injuries Q3M1 W1-3Jonathan LubagPas encore d'évaluation
- Breast CancerDocument129 pagesBreast CancerHope LeePas encore d'évaluation
- How We Conquered SmallpoxDocument4 pagesHow We Conquered SmallpoxNadir BaghdadPas encore d'évaluation
- A Case Report On Symptomatic Primary Herpetic Gingivostomatitis (New)Document4 pagesA Case Report On Symptomatic Primary Herpetic Gingivostomatitis (New)Annisa MardhatillahPas encore d'évaluation
- Demystifying The Diagnosis and Classification of Lymphoma - Gabriel C. Caponetti, Adam BaggDocument6 pagesDemystifying The Diagnosis and Classification of Lymphoma - Gabriel C. Caponetti, Adam BaggEddie CaptainPas encore d'évaluation
- Stages of Gingival InflammationDocument13 pagesStages of Gingival Inflammationvisi thiriyanPas encore d'évaluation
- Panc Adenocarcinoma Recent Data and Perspective JR Delpero HPB Course 2022 V4-NuoveDocument176 pagesPanc Adenocarcinoma Recent Data and Perspective JR Delpero HPB Course 2022 V4-NuoveDiana MitreaPas encore d'évaluation
- 5BBK Lec5 - Other Blood Groups MQA 2019-09-26 08-14-44Document37 pages5BBK Lec5 - Other Blood Groups MQA 2019-09-26 08-14-44gothai sivapragasamPas encore d'évaluation
- SpermatoceleDocument2 pagesSpermatocelemrizkidm2301Pas encore d'évaluation
- Classification of Acute Pancreatitis-2012 - Revision of The Atlanta Classification and Definitions by International ConsensusDocument12 pagesClassification of Acute Pancreatitis-2012 - Revision of The Atlanta Classification and Definitions by International ConsensusRichard CuevasPas encore d'évaluation