Académique Documents
Professionnel Documents
Culture Documents
Appendectomy
Transféré par
Roseben SomidoDescription originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Appendectomy
Transféré par
Roseben SomidoDroits d'auteur :
Formats disponibles
A laparotomy is a surgical procedure involving a large incision through the abdominal wall to gain access into the abdominal
cavity. It is also known as coeliotomy. Terminology In diagnostic laparotomy (most often referred to as an exploratory laparotomy and abbreviated Ex-Lap), the nature of the disease is unknown, and laparotomy is deemed the best way to identify the cause. In therapeutic laparotomy, a cause has been identified (e.g. peptic ulcer, colon cancer) and laparotomy is required for its therapy. Usually, only exploratory laparotomy is considered a stand-alone surgical operation. When a specific operation is already planned, laparotomy is considered merely the first step of the procedure. Spaces accessed Depending on incision placement, laparotomy may give access to any abdominal organ or space, and is the first step in any major diagnostic or therapeutic surgical procedure of these organs, which include:
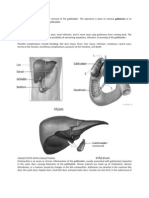
the lower part of the digestive tract (the stomach, duodenum, jejunum, ileum and colon) the liver, pancreas and spleen the bladder the female reproductive organs (the uterus and ovaries) the retroperitoneum (the kidneys, the aorta, abdominal lymph nodes) the appendix
Types of incisions Midline The most common incision for laparotomy is the midline incision, a vertical incision which follows the lineaalba.
The upper midline incision usually extends from the xiphoid process to the umbilicus. A typical lower midline incision is limited by the umbilicus superiorly and by the pubic symphysis inferiorly.
Sometimes a single incision extending from xiphoid process to pubic symphysis is employed, especially in trauma surgery.
Midline incisions are particularly favoured in diagnostic laparotomy, as they allow wide access to most of the abdominal cavity. Other Other common laparotomy incisions include: TheKocher (right subcostal) incision (after Emil Theodor Kocher); appropriate for certain operations on the liver, gallbladder and biliary tract. This shares a name with the Kocher incision used for thyroid surgery: a transverse, slightly curved incision about 2 cm above the sternoclavicular joints; the Davis or Rockey-Davis "muscle-splitting" right lower quadrant incision for appendectomy; the Pfannenstiel incision, a transverse incision below the umbilicus and just above the pubic symphysis. In the classic Pfannenstiel incision, the skin and subcutaneous tissue are incised transversally, but the lineaalba is opened vertically. It is the incision of choice for Cesarean section and for abdominal hysterectomy for benign disease. A variation of this incision is the Maylard incision in which the rectus abdominis muscles are sectioned transversally to permit wider access to the pelvis.
Lumbotomy consists of a lumbar incision which permits access to the kidneys (which are retroperitoneal) without entering the peritoneal cavity. It is typically used only for benign renal lesions. It has also been proposed for surgery of the upper urological tract. Related procedures A related procedure is laparoscopy, where cameras and other instruments are inserted into the peritoneal cavity via small holes in the abdomen. For example, an appendectomy can be done either by a laparotomy or by a laparoscopic approach.
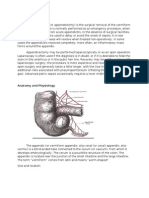
An appendectomy (sometimes called appendisectomy or appendicectomy) is the surgical removal of the vermiform appendix. This procedure is normally performed as an emergency procedure, when the patient is suffering from acute appendicitis. In the absence of surgical facilities, intravenous antibiotics are used to delay or avoid the onset of sepsis; it is now recognized that many cases will resolve when treated perioperatively. In some cases the appendicitis resolves completely; more often, an inflammatory mass forms around the appendix, causing transruptural flotation. This is a relative contraindication to surgery. Appendectomy may be performed laparoscopically (this is called minimally invasive surgery) or as an open operation. Laparoscopy is often used if the diagnosis is in doubt, or if it is desirable to hide the scars in the umbilicus or in the pubic hair line. Recovery may be a little quicker with laparoscopic surgery; the procedure is more expensive and resource-intensive than open surgery and generally takes a little longer, with the (low in most patients) additional risks associated with pneumoperitoneum (inflating the abdomen with gas). Advanced pelvic sepsis occasionally requires a lower midline laparotomy. There have been some cases of auto-appendectomies, i.e. operating on yourself. One was performed by Dr Kane in 1921, but the operation was completed by his assistants. Another case is Leonid Rogozov who had to perform the operation on himself as he was the only surgeon on a remote Arctic base.
Procedure
In general terms, the procedure for an open appendectomy is as follows. 1. Antibiotics are given immediately if there are signs of sepsis, otherwise a single dose of prophylactic intravenous antibiotics is given immediately prior to surgery. 2. General anaesthesia is induced, with endotracheal intubation and full muscle relaxation, and the patient is positioned supine. 3. The abdomen is prepared and draped and is examined under anesthesia.
4. If a mass is present, the incision is made over the mass; otherwise, the incision is made over McBurney's point, one third of the way from the anterior superior iliac spine (ASIS) and the umbilicus; this represents the position of the base of the appendix (the position of the tip is variable). 5. The various layers of the abdominal wall are then opened. 6. The effort is always to preserve the integrity of abdominal wall. Therefore, the External Oblique Aponeurosis is slitted along its fiber, and the internal oblique muscle is split along its length, not cut. As the two run at right angles to each other, this prevents later Incisional hernia. 7. On entering the peritoneum, the appendix is identified, mobilized and then ligated and divided at its base. 8. Some surgeons choose to bury the stump of the appendix by inverting it so it points into the caecum. 9. Each layer of the abdominal wall is then closed in turn. 10. The skin may be closed with staples or stitches. 11. The wound is dressed. 12. The patient will be brought to the recovery room.
NURSING MANAGEMENT: Assess the severity and location of pain. If client presents with board-like rigidity and severe pain, suspect for peritonitis. Administer analgesics after a diagnosis is made. Assess the effectiveness of the analgesic given. Position client in a supine position with thighs slightly flexed.
Preoperative care It is important to prepare a patient several hours pre-surgery. The patient may be dehydrated due to symptoms such as vomiting. It may be necessary to administer IV fluids. The patient's vital signs should be recorded every 2-4 hours. The nurse should not apply any heat over the area of pain while the patient is awaiting diagnosis as this could cause the appendix to rupture (Box 2). Analgesia should not be administered before examination because this can lead to an inaccurate diagnosis as the pain may subside and the examination will be ineffective. Aperients should also be avoided as induced peristalsis may cause perforation. If appendicitis has been diagnosed regular analgesia, usually an opioid depending on pain severity, should be given to make the patient comfortable before treatment. They may feel anxious so the nurse or surgical team should fully explain the procedure to them and answer any questions. The operation site will be washed and shaved before surgery, depending on local procedures. Postoperative care The severity of the patient's pain needs to be assessed with the use of a pain scale. Appropriate pain relief can then be administered. Vital signs should be regularly monitored at half-hourly intervals for two hours postoperatively, hourly for two hours and, if stable, every four hours while the patient is recovering in hospital. If the patient has had a straightforward appendectomy the surgical team should review the patient on recovery and decide when they may eat and drink. A drain may have been inserted during surgery. If so, the output of the drain should be recorded every 24 hours. The drain can be removed when there is minimal drainage - usually 50ml or less. The wound should be managed aseptically. If the wound is covered with a dry dressing then it should be changed every 1-2 days. Clips/stitches should be removed 10 days postoperatively. The patient can go home with these in place and the district or practice nurse can remove them. If dissolvable stitches have been used this is unnecessary, although a visit to check the wound will reduce anxiety. Before discharge, the patient must be confident in how to manage their wound and have details of who they should contact in case of concern. The patient should be encouraged to get up and out of bed as soon as possible to prevent the formation of emboli. Anticoagulants are usually administered in the form of subcutaneous injections before surgery and postoperatively. Antiembolism stockings should be worn. If peritonitis has developed, the patient's postoperative management will be over a longer period but will follow the same principles. The patient will not be able to commence food and fluids for a few days, this is to enable the bowel to regain normal function. The convalescence period is almost invariably smooth and the patient recovers rapidly (Colmer, 1986). The hospital stay for patients who have undergone an uncomplicated appendectomy is usually 2-3 days. In most cases the patient will be discharged when their temperature is normal and their bowels have started to function again (Peterson, 2002). People can live a full life without their appendix. Changes in diet, exercise or other lifestyle factors are not necessary (NDDIC, 2004).
Vous aimerez peut-être aussi
- Opd Meds JgejDocument4 pagesOpd Meds JgejDinen Dot100% (5)
- List of Surgical ProceduresDocument6 pagesList of Surgical ProceduresMatin Ahmad KhanPas encore d'évaluation
- CraniotomyDocument10 pagesCraniotomyUzma KhanPas encore d'évaluation
- 38 - PC - 1 - 1 - Jul - Sep - 2011Document108 pages38 - PC - 1 - 1 - Jul - Sep - 2011Rosales Rosales Jesús100% (1)
- HerniaDocument11 pagesHerniaHapsari Wibawani 'winda'100% (1)
- TIROIDECTOMIIDocument66 pagesTIROIDECTOMIIThoreEPas encore d'évaluation
- School Age ChildDocument26 pagesSchool Age ChildRoseben SomidoPas encore d'évaluation
- Preschooler: From 3-5 Years OldDocument44 pagesPreschooler: From 3-5 Years OldRoseben Somido100% (2)
- Types of AnesthesiaDocument3 pagesTypes of AnesthesiaAudrey LeonarPas encore d'évaluation
- HERNIORRHAPHYDocument2 pagesHERNIORRHAPHYSheldon Deypalubos Jr.Pas encore d'évaluation
- CellulitisDocument15 pagesCellulitisSujatha J JayabalPas encore d'évaluation
- Pendekatan Kaunseling Dalam Rawatan & Pemulihan Penagihan DadahDocument23 pagesPendekatan Kaunseling Dalam Rawatan & Pemulihan Penagihan Dadahadib emirPas encore d'évaluation
- NCP - Disturbed Body ImageDocument3 pagesNCP - Disturbed Body ImageRoseben Somido100% (1)
- Pa Tho Physiology of Ectopic PregnancyDocument2 pagesPa Tho Physiology of Ectopic Pregnancythediaber60% (5)
- Appendicitis & Appendectomy: Jenny Juniora AjocDocument31 pagesAppendicitis & Appendectomy: Jenny Juniora AjocJenny AjocPas encore d'évaluation
- NPD Elsa RonningstamDocument15 pagesNPD Elsa RonningstamFrancescaPas encore d'évaluation
- Theraputic Alliance EssayDocument15 pagesTheraputic Alliance Essaymiimii33100% (1)
- AppendectomyDocument37 pagesAppendectomyRaquid MariaPas encore d'évaluation
- Hiatal Hernia AchalasiaDocument22 pagesHiatal Hernia AchalasiaDhen MarcPas encore d'évaluation
- Penetrating Abdominal Trauma Emergency ManagementDocument29 pagesPenetrating Abdominal Trauma Emergency Managementanjali singhPas encore d'évaluation
- LaparotomyDocument36 pagesLaparotomydenekePas encore d'évaluation
- Breast Self ExamDocument3 pagesBreast Self ExamLoveSheryPas encore d'évaluation
- Hirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsD'EverandHirschsprung’s Disease, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsPas encore d'évaluation
- The Psychodynamic Diagnostic ManualDocument6 pagesThe Psychodynamic Diagnostic ManuallukasPas encore d'évaluation
- MastectomyDocument6 pagesMastectomyJustinAlmedaPas encore d'évaluation
- Cardiac MonitoringDocument19 pagesCardiac MonitoringYaska Musa100% (1)
- Mastectomy: Prepared By: Hilario, Eunice Lamoste, Jenebelle Lopez, Maria SofiaDocument34 pagesMastectomy: Prepared By: Hilario, Eunice Lamoste, Jenebelle Lopez, Maria SofiaSofia LopezPas encore d'évaluation
- Intestinal Obstruction 4Document25 pagesIntestinal Obstruction 4Muvenn KannanPas encore d'évaluation
- A Case Presentation On AppendecitisDocument30 pagesA Case Presentation On AppendecitisrodericpalanasPas encore d'évaluation
- Surya NamaskarDocument12 pagesSurya NamaskarBaskaran SowrirajuluPas encore d'évaluation
- Vethathiri - Holistic HealthDocument19 pagesVethathiri - Holistic HealthProf. Madhavan100% (2)
- Drug StudyDocument14 pagesDrug Studysyd1975% (8)
- Case Study Presented by Group 22 BSN 206: In-Depth View On CholecystectomyDocument46 pagesCase Study Presented by Group 22 BSN 206: In-Depth View On CholecystectomyAjiMary M. DomingoPas encore d'évaluation
- NLE Reviewer Q and ADocument11 pagesNLE Reviewer Q and ARoseben Somido100% (1)
- 8 Irrigating A ColostomyDocument5 pages8 Irrigating A ColostomyAnn Jalover PerezPas encore d'évaluation
- Ethico - Moral Aspect of NursingDocument37 pagesEthico - Moral Aspect of NursingMarichu Bajado100% (1)
- CholecystitisDocument27 pagesCholecystitisKadek Ariarta MahartamaPas encore d'évaluation
- OstomyDocument22 pagesOstomyJosiah VillacampaPas encore d'évaluation
- Sigmoidoscopy: Presented by Kriti Adhikari Roll No: 17Document38 pagesSigmoidoscopy: Presented by Kriti Adhikari Roll No: 17sushma shresthaPas encore d'évaluation
- NCLEX Questions 96-105Document3 pagesNCLEX Questions 96-105kxviperPas encore d'évaluation
- Hemangioma PresentationDocument18 pagesHemangioma Presentationplastic guardiansPas encore d'évaluation
- Pregabalin Drug by IvanDocument3 pagesPregabalin Drug by IvanRoseben Somido100% (1)
- NCP Hypertension 2Document3 pagesNCP Hypertension 2Roseben Somido50% (2)
- NCP ConstipationDocument2 pagesNCP ConstipationRoseben Somido100% (1)
- Common Surgical Procedures TerminologyDocument10 pagesCommon Surgical Procedures TerminologySara Tongcua TacsagonPas encore d'évaluation
- Nle Tips MS PDFDocument11 pagesNle Tips MS PDFjthsPas encore d'évaluation
- 2010 - Hoffman - The Effect of Mindfulness Based Therapy On Anxiety and DepressionDocument15 pages2010 - Hoffman - The Effect of Mindfulness Based Therapy On Anxiety and DepressionFabián MaeroPas encore d'évaluation
- Drug Study - Paracetamol Ambroxol, Ascorbic Acid, CefuroximeDocument4 pagesDrug Study - Paracetamol Ambroxol, Ascorbic Acid, Cefuroximeapi-3701489100% (12)
- AppendectomyDocument35 pagesAppendectomyleighjagPas encore d'évaluation
- Gastric Outlet Obstruction, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsD'EverandGastric Outlet Obstruction, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsPas encore d'évaluation
- Preoperative Preparation of The Surgical PatientDocument33 pagesPreoperative Preparation of The Surgical PatientPrincewill SeiyefaPas encore d'évaluation
- Compartment SyndromeDocument3 pagesCompartment SyndromeTantyo Adi P100% (2)
- AppendectomyDocument5 pagesAppendectomyCris EstoniloPas encore d'évaluation
- Appendicitis: I. Signs and SymptomsDocument3 pagesAppendicitis: I. Signs and Symptomsslimescared01Pas encore d'évaluation
- Cholelithiasis GallstoneDocument22 pagesCholelithiasis GallstoneBheru LalPas encore d'évaluation
- Intestinal ObstructionDocument35 pagesIntestinal Obstructionwht89100% (1)
- CholecystectomyDocument6 pagesCholecystectomyTom Bayubs-tucsPas encore d'évaluation
- Activity IntoleranceDocument6 pagesActivity IntoleranceRaidis PangilinanPas encore d'évaluation
- NCM 112: Care of Clients With Inflammatory and Immunologic Response Maricris B. Florendo/Constantino Y. Mendoza/Sandra Layne G. Luczon/Rhizza AbinsayDocument23 pagesNCM 112: Care of Clients With Inflammatory and Immunologic Response Maricris B. Florendo/Constantino Y. Mendoza/Sandra Layne G. Luczon/Rhizza AbinsayRyrey Abraham PacamanaPas encore d'évaluation
- ClubfootDocument22 pagesClubfootJhong Xyrus100% (3)
- Transcult - Nursing PPT Nurs 450 FinalDocument32 pagesTranscult - Nursing PPT Nurs 450 FinalJuan Cruz100% (1)
- The Neonatal Period (N2)Document25 pagesThe Neonatal Period (N2)api-3721542100% (1)
- Uterine Rupture: Mariano Marcos StateDocument10 pagesUterine Rupture: Mariano Marcos StateSalvaje CaballeroPas encore d'évaluation
- Operating Room Nurses Knowledge and Practice of Sterile Technique 2167 1168.1000113Document5 pagesOperating Room Nurses Knowledge and Practice of Sterile Technique 2167 1168.1000113mlbrown8Pas encore d'évaluation
- Operating Room InstrumentsDocument8 pagesOperating Room InstrumentsVictoria Castillo TamayoPas encore d'évaluation
- CraniotomyDocument6 pagesCraniotomychaSephPas encore d'évaluation
- Patient Positioning During SurgeryDocument30 pagesPatient Positioning During SurgeryKristine AlejandroPas encore d'évaluation
- ATELECTASISDocument4 pagesATELECTASISAshley Jane MacapayadPas encore d'évaluation
- Postoperative Nursing CareDocument2 pagesPostoperative Nursing CareYeana AlonPas encore d'évaluation
- THORACOTOMYDocument3 pagesTHORACOTOMYConnie May Fernando Evangelio100% (1)
- CHOLELITHIASISSDocument29 pagesCHOLELITHIASISSAngelica Mercado SirotPas encore d'évaluation
- Case UreterolithiasisDocument26 pagesCase UreterolithiasisPutri Dwi Kartini0% (1)
- Clinical Guidelines (Nursing) - Indwelling Urinary Catheter - Insertion and Ongoing CareDocument8 pagesClinical Guidelines (Nursing) - Indwelling Urinary Catheter - Insertion and Ongoing CareLeePas encore d'évaluation
- Thromboltic TherapyDocument19 pagesThromboltic Therapyhanimozaghi100% (1)
- Surgical TeamDocument9 pagesSurgical Teamkarenkaren09Pas encore d'évaluation
- OsteomyelitisDocument7 pagesOsteomyelitis4kscribd100% (1)
- Wound Healing and Wound CareDocument15 pagesWound Healing and Wound CareNinaPas encore d'évaluation
- OMCDocument37 pagesOMCyurie_ameliaPas encore d'évaluation
- Patient Positioning: Complete Guide For Nurses: Marjo S. Malabanan, R.N.,M.NDocument43 pagesPatient Positioning: Complete Guide For Nurses: Marjo S. Malabanan, R.N.,M.NMercy Anne EcatPas encore d'évaluation
- Dermoid CystDocument8 pagesDermoid CystMohamed Hazem ElfollPas encore d'évaluation
- Fistula in AnoDocument3 pagesFistula in Anokhadzx80% (5)
- Abdominal Compartment SyndromeDocument23 pagesAbdominal Compartment SyndromeUmar Farooq GondalPas encore d'évaluation
- nLE rEVIEWER 2Document1 pagenLE rEVIEWER 2Roseben SomidoPas encore d'évaluation
- DKADocument5 pagesDKARoseben SomidoPas encore d'évaluation
- Baptism of JesusDocument3 pagesBaptism of JesusRoseben SomidoPas encore d'évaluation
- Medical PrefixesDocument6 pagesMedical PrefixesRoseben SomidoPas encore d'évaluation
- Funda Q and ADocument4 pagesFunda Q and ARoseben SomidoPas encore d'évaluation
- Funda Q and ADocument4 pagesFunda Q and ARoseben SomidoPas encore d'évaluation
- PhynetoinDocument3 pagesPhynetoinRoseben SomidoPas encore d'évaluation
- Ferrous SulfateDocument2 pagesFerrous SulfateRoseben SomidoPas encore d'évaluation
- Vitamin CDocument3 pagesVitamin CRoseben SomidoPas encore d'évaluation
- MethergineDocument2 pagesMethergineRoseben SomidoPas encore d'évaluation
- A Research: Perpetual Help College of Manila V.Conception ST., Sampaloc, Manila Bachelor of Science in NursingDocument8 pagesA Research: Perpetual Help College of Manila V.Conception ST., Sampaloc, Manila Bachelor of Science in NursingRoseben SomidoPas encore d'évaluation
- Altered Cerebral PerfusionDocument3 pagesAltered Cerebral PerfusionRoseben SomidoPas encore d'évaluation
- DKADocument5 pagesDKARoseben SomidoPas encore d'évaluation
- Medical PrefixesDocument6 pagesMedical PrefixesRoseben SomidoPas encore d'évaluation
- Impaired Physical MobilityDocument2 pagesImpaired Physical MobilityRoseben SomidoPas encore d'évaluation
- Roseben R. Somido: PATIENT: Mitra Michelle, 8 Years Old CASE: Enteric FeverDocument2 pagesRoseben R. Somido: PATIENT: Mitra Michelle, 8 Years Old CASE: Enteric FeverRoseben SomidoPas encore d'évaluation
- Roseben R. Somido: PATIENT: Delos Reyes, Lloyd: 2mos - Old CASE: Pneumonia SevereDocument2 pagesRoseben R. Somido: PATIENT: Delos Reyes, Lloyd: 2mos - Old CASE: Pneumonia SevereRoseben SomidoPas encore d'évaluation
- Vulvitis Power Point NewDocument22 pagesVulvitis Power Point NewRoseben Somido75% (4)
- Vulvitis Power Point NewDocument22 pagesVulvitis Power Point NewRoseben Somido75% (4)
- Wound DebridementDocument3 pagesWound DebridementRoseben SomidoPas encore d'évaluation
- Reishimax GLP Us PipDocument3 pagesReishimax GLP Us PipKeith KingPas encore d'évaluation
- HSDC QuintesenceDocument6 pagesHSDC QuintesenceDavid CasaverdePas encore d'évaluation
- 1955 Ball LauraDocument55 pages1955 Ball LauraBene BeanPas encore d'évaluation
- Efficacy of HA PDFDocument4 pagesEfficacy of HA PDFARPas encore d'évaluation
- Nursing Skills ChecklistDocument6 pagesNursing Skills Checklistapi-433700464Pas encore d'évaluation
- Machine LearningDocument14 pagesMachine LearningKantapon DissaneewatePas encore d'évaluation
- SMF Orthopaedi Dan Traumatologi RSU DR Saiful Anwar Malang: Thomas Erwin C J HuwaeDocument58 pagesSMF Orthopaedi Dan Traumatologi RSU DR Saiful Anwar Malang: Thomas Erwin C J Huwaeyulia manaweanPas encore d'évaluation
- Arum Hastuti Dwi Sofiati Jurnal Persalinan B.inggrisDocument5 pagesArum Hastuti Dwi Sofiati Jurnal Persalinan B.inggrisArum HastutiPas encore d'évaluation
- BBC Open Minds ArticleDocument3 pagesBBC Open Minds ArticlebrainbalancePas encore d'évaluation
- Grievance Status RMLDocument1 pageGrievance Status RMLMayankPas encore d'évaluation
- Medwatch 1Document26 pagesMedwatch 1Swaralipi GhoshPas encore d'évaluation
- AcknowledgementDocument6 pagesAcknowledgementJustin VarghesePas encore d'évaluation
- Targeted Therapy in CancerDocument51 pagesTargeted Therapy in CancerSatya WangsaPas encore d'évaluation
- Protein Synthesis Inhibitors 2Document25 pagesProtein Synthesis Inhibitors 2AliImadAlKhasakiPas encore d'évaluation
- Grilly1980 PDFDocument5 pagesGrilly1980 PDFAliPas encore d'évaluation
- Pubh 7420 Supplemental Notes: Endpoints Supplemental Reading ReferencesDocument7 pagesPubh 7420 Supplemental Notes: Endpoints Supplemental Reading ReferencesVaishnavi SoundarPas encore d'évaluation
- DR Wilfredo Stokes Pain Related With Spine (DRCV) and More Information For All Guatemala Junio 2010Document10 pagesDR Wilfredo Stokes Pain Related With Spine (DRCV) and More Information For All Guatemala Junio 2010drwstokes100% (1)
- Left Thigh Pain: I. Chief Complaint/ Other ComplaintsDocument9 pagesLeft Thigh Pain: I. Chief Complaint/ Other ComplaintsDominic BristolPas encore d'évaluation