Académique Documents
Professionnel Documents
Culture Documents
Obstruction. Return of Bowel Sounds - Not Effective To Judges Post Op Ileus
Transféré par
justin_saneTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Obstruction. Return of Bowel Sounds - Not Effective To Judges Post Op Ileus
Transféré par
justin_saneDroits d'auteur :
Formats disponibles
Research for Practice
Return of Bowel Sounds Indicating An End of Postoperative Ileus: Is it Time to Cease this Long-Standing Nursing Tradition?
Robert L. Massey
phenomenon commonly known as postoperative ileus (POI) occurs almost universally among the millions of patients worldwide who undergo abdominal surgery. POI is a form of gastrointestinal (GI) dysmotility causing a build-up of gas and fluid within the GI tract lasting 3-5 days after abdominal surgery (Maron & Fry, 2008; Massey, 2010; Person & Wexner, 2006). Historically, nurses and physicians have been trained to ascultate daily for at least 5 minutes in each of the four abdominal quadrants (20 minutes total) for the return of bowel sounds after abdominal surgery (Madsen et al., 2005). Over time, this has evolved as an indicator of the resolution of POI. However, the efficacy of auscultation for return of bowel sounds as an indicator for the resolution of POI has been questioned through evidence-based inquiry. Using the Iowa Model of EvidenceBased Practice (Titler et al., 2001), Madsen and colleagues (2005) explored the evidence and actual clinical practice to determine if auscultation of the abdomen for the return of bowel sounds was a reliable indicator of the return of GI motility and thus an end to POI in patients recovering from abdominal surgery. Determination of the primary endpoint indicator for an end to POI (return of bowel sounds, first flatus and/or bowel movement after surgery, tolerating a diet) remains controversial (Delaney et al., 2010; Huge
Evidence and rationale supporting return of bowel sounds as an unreliable indicator of the end of postoperative ileus after abdominal surgery are provided.
Introduction A loss of gastrointestinal motility, commonly known as postoperative ileus (POI), occurs after abdominal surgery. Since the 1900s, nurses and other clinicians have been taught to listen for return of bowel sounds to indicate the end of POI. Evidence-based nursing literature has challenged this long-standing traditional nursing practice. Purpose The purpose of this study was to provide evidence from a randomized clinical trial and rationale supporting evidence-based inquiry concerning return of bowel sounds as an unreliable indicator of the end of POI after abdominal surgery. Method Time (days) of return of bowel sounds after abdominal surgery was compared to the time (days) of first postoperative flatus, an indicator of the end of POI, in 66 patients recovering from abdominal surgery randomized to receive standard care compared to those who received standard care plus a rocking chair intervention. Findings Pearsons correlation between time to first flatus and return of bowel sounds for combined groups was not significant (r=0.231, p=0.062, p<0.05) indicating that time to return of bowel sounds and time to first flatus were not associated. Conclusions The results of this study provide support to evidence-based inquiry that questions the relevance of traditional nursing practice activities such as listening to bowel sounds as an indicator of the end of POI.
Robert L. Massey, PhD, RN, NEA-BC, is Assistant Professor and Director, Clinical Nursing, The University of Texas M.D. Anderson Cancer Center, Houston, TX.
146
May-June 2012 Vol. 21/No. 3
Return of Bowel Sounds Indicating an End of Postoperative Ileus: Is it Time to Cease this Long-Standing Nursing Tradition?
et al., 2000; Person & Wexner, 2006; Prasad & Matthews, 1999; Stewart & Waxman, 2007; Thomas, Ptak, Giddings, Moore, & Oppermann, 1990; Waldhausen, Shaffrey, Skenderis, Jones, & Schirmer, 1990). Previous research has questioned the reliability of return of bowel sounds as an indicator for the end of POI, supporting Madsen and colleagues (2005) evidence-based inquiry versus multiple indicators (first flatus and/or bowel movement) for the end of POI (Huge et al., 2000; Waldhausen & Schirmer, 1990). However, previous research did not compare return of bowel sounds to a specific indicator, such as first postoperative flatus, for the end of POI. Therefore, design of the randomized trial of rocking chair therapy included measuring the date and time of return of bowel sounds as the primary indicator for the end of POI, date and time of passage of first postoperative flatus, and determining if there was an association. In this article the results of the study are reported and rationale is presented for why return of bowel sounds is probably not an indicator for return of POI.
use; however, more research is required to validate their contributions (Kehlet, 2008; Maron & Fry, 2008). The duration of POI is in part related to the degree of surgical trauma and appears to be most severe following extensive surgeries of the colon, especially those requiring reanastomosis (Huge et al., 2000; Kehlet, 2008; Maron & Fry, 2008; Person & Wexner, 2006). POI, one of the most significant side effects of abdominal surgery, can last 3-5 days and result in an average hospital stay of 7-8 days. It adds billions of dollars to health care costs annually (Miedema & Johnson, 2003; Person & Wexner, 2006). Patients often describe the period immediately after surgery, until the resolution of POI, as the most uncomfortable part of their abdominal surgery recovery experience (Massey, 2010; Moore, Shannon, Richard, & Vacca, 1995; Thomas et al., 1990).
Literature Review
Review of the literature for this article included MEDLINE, SCOPUS, and CINHAL searches plus a snowball method due to alterations in bowel motility being first identified in the 1890s and Cannon proposing auscultation for return of bowel sounds in 1905 (Greenhalgh, Robert, Macfarlane, Bate, & Kyriakidou, 2004; Nachlas, Younis, Roda, & Wityk, 1972). Nursing research regarding correlations between auscultation of bowel sounds and resolution of POI are limited although there have been case studies reported in the literature (Kirton, 1997; Mehta, 2003); therefore, the reliance on the surgical literature. Clinical standards for determining the prevention, treatment, and end of POI continue to be as confounding as the multiple combinations of contributing factors that cause it (Huge et al., 2000; Kehlet, 2008; Maron & Fry, 2008; Person & Wexner, 2006). Current clinical practice protocols include daily auscultation of the patients abdomen for the return of bowel sounds plus monitoring the patient for the passage of flatus, a phenomenon traditionally called surgeons music (Prasad &
Background
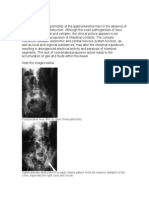
Postoperative ileus occurs universally after abdominal surgery (open and laparoscopic), resulting in absent or delayed gastrointestinal motility that causes gas and fluid retention within the GI tract (Delaney, 2004; Kehlet, 2008; Maron & Fry, 2008; Person & Wexner, 2006; Stewart & Waxman, 2007). Patients experience a symptom cluster that includes nausea, vomiting, abdominal distention, diet intolerance, pain, and is generally a self-resolving phenomenon complicating a full and timely recovery of the postabdominal surgery patient (Delaney et al., 2010; Massey, 2010). Abdominal incisions, manipulation of the bowel, and extensive dissection required to remove abdominal lesions initiate a surgical-induced stress response believed to be the primary cause of POI (Desborough, 2000; Person & Wexner, 2006). Other causes may include inflammation, hormonal effects, and opioid
Matthews, 1999, p. 489) and/or passage of stool. Postoperative return of bowel function within the GI tract varies by location. The return of function appears to occur first in the small intestine within 24 hours after surgery, the stomach in 24-48 hours, and the colon within 3-5 days (Huge et al., 2000; Stewart & Waxman, 2007; Waldhausen & Schirmer, 1990; Waldhausen et al., 1990) Waldhausen and colleagues (1990) first indicated the passage of flatus usually preceded the first bowel movement, and the two events generally occur with 24 hours of each other. The first bowel movements after abdominal surgery are liquid in nature, a phenomenon supporting POIs link to a build-up of gas and fluid within the bowel rather than the hard, dry stool common with constipation. Evidence supports the use of passage of first flatus after surgery as the indicator to define the return of GI motility (Madsen et al., 2005; Maron & Fry, 2008; Massey, 2010; Person & Wexner, 2006; Prasad & Matthews, 1999; Waldhausen et al., 1990). Other parameters may include absence of a symptom cluster that includes abdominal distention, nausea, vomiting, pain, and the inability to tolerate a diet until the resolution of POI (Delaney, 2004; Delaney et al., 2010; Madsen et al., 2005; Maron & Fry, 2008; Person & Wexner, 2006). More studies are required to determine the reliability and validity of passage of first postoperative flatus and absence of abdominal distention, nausea vomiting, and tolerance of diet to indicate a return of GI motility or the end of POI.
Bowel Sounds
Findings from seminal studies involving electrode implantation during laparotomy supported suspicions that bowel function may never cease fully during or after abdominal surgery and created further doubt regarding the reliability of using presence of bowel sounds as an indicator of POI resolution (Huge et al., 2000; Waldhausen & Schirmer, 1990; Waldhausen et al., 1990). Past research also has failed to find any positive correlations between bowel sounds and actual propulsive bowel
May-June 2012 Vol. 21/No. 3
147
Research for Practice
TABLE 1. Time to Return of Bowel Sounds
Mean Time to Bowel Sounds (Days) Day 1 Day 1 Day 2 Day 3 Rocking Non-Rocking
such as reduced pulmonary complications, deep vein thrombosis, and other negative physiological changes associated with bed rest.
p
n
1 25 8
% 2.9 75.3 23.5
n
1 22 9
% 3.1 68.8 28.1
Rocking Chair Intervention
A rocking motion delivered using a rocking chair is a relatively new nursing-derived noninvasive procedure believed to reduce the duration and effects of POI. Findings of three nursing studies demonstrated efficacy of rocking chair motion in reducing POI duration in patients after abdominal surgery and cesarean section (Massey, 2010; Moore et al., 1995; Thomas et al., 1990). Rocking motion has also been used by nurses to calm infants and symptoms of dementia in older adults (Bonadonna, 1981; Houston, 1993; Vrugt & Pederson, 1973). The gentle rhythmic rocking chair motion is thought to modulate the surgical stress response through vestibular nerve stimulation of the reticular activating system, thus mitigating the effects of POI. The rationale for this study was to evaluate the efficacy of rocking chair motion on the duration of POI in patients recovering from abdominal surgery. A secondary aim was to compare the return of bowel sounds with an indicator of the end of POI. Previous research reported a lack of association in randomized trials with design limitations, and studies that compared multiple therapies to rocking chair motion or lacked a specific indicator for the resolution of POI (Huge et al., 2000; Moore et al., 1995; Thomas et al., 1990; Waldhausen & Schirmer, 1990; Waldhausen et al., 1990). A gap existed in the literature regarding an association between return of bowel sounds and a specific indicator for the resolution of POI.
0.909
functioning, thereby lending even more doubt to the reliability of bowel sounds as an indicator of the resolution of POI. In a study of 44 patients undergoing laparotomy, bowel sounds returned on day 2.4 (0.4 days) and passage of flatus and stool occurred on day 5.1 (0.2 days), indicating no correlation between onset of bowel sounds and the resolution of POI (Waldhausen et al., 1990). Also complicating the assessment and treatment of POI after abdominal surgery are other findings that suggest some postoperative patients with normal active bowel sounds continue to suffer from symptoms indicating a lack of GI motility (Huge et al., 2000; Waldhausen et al., 1990). In these studies, patients with normal, active postoperative bowel sounds continued to experience the symptom cluster associated with POI that included abdominal distention, nausea, vomiting, and diet intolerance.
Common Clinical Practice
Despite a lack of compelling evidence, clinical practice continues to promote daily auscultation of the abdomen for a minimum of 5 minutes in each quadrant to determine the return of bowel sounds as an indicator for resolution of POI. In the practice evaluation conducted by Madsen and co-authors (2005) (N=82), 54 advanced practice nurses, 19 staff nurse experts, and 9 surgeons responded to a questionnaire of current practice. Of the 54 advanced practice respondents, 60% (n=32) and 90% (n=17) of the clinical nurses reported they ascultate in four quadrants every 4-8 hours. However, less than 10% (n=5) of the APNs and none of the clinical nurses
reported listening for the recommended 5 minutes in each quadrant of the abdomen. Almost 50% (n=27) of the advanced practice nurses and at least 40% (n= 8) of staff nurses indicated they listen for 30-60 seconds in each quadrant rather than 5 minutes as stipulated in clinical practice guidelines at the institution. Of surgeons, 78% (n=7) reported little benefit from nurses assessing and reporting bowel sounds indicating resolution of POI. Instead, they identified return of flatus (89%, n=8), bowel movement (44%, n=4), and return of appetite (44%, n=4) as primary parameters to indicate POI resolution. They concluded passage of first postoperative flatus, bowel movement, and the concurrent resolution of a symptom cluster (abdominal distention, nausea, vomiting, and diet tolerance) were more reliable indicators for return of GI motility and resolution of POI. As a result of the evidence-based review, the assessment of bowel sounds as a primary indicator of the resolution of POI was discontinued.
Standard Postoperative Care
One noninvasive, postoperative standard of care intervention that is believed to resolve POI is to have the patient get out of bed, sit in a chair, and walk beginning the first postoperative day, increasing the duration each day until passage of flatus or stool occurs (Brieger, 1983; Luckey, Livingston, & Tache, 2003; Waldhausen & Schirmer, 1990; Waldhausen et al., 1990). Evidence that these activities effectively reduce the duration of POI remain unconvincing. However, consensus indicates the postoperative patient experiences other positive benefits,
Methods
Guided by previous evidence, evaluation of the association between onset of bowel sounds and time to first flatus to indicate the resolution of POI was included in a randomized clinical study comparing the effect of rocking chair motion and standard care on postoperative ileus duration in patients with can-
148
May-June 2012 Vol. 21/No. 3
Return of Bowel Sounds Indicating an End of Postoperative Ileus: Is it Time to Cease this Long-Standing Nursing Tradition?
cer recovering from abdominal surgery (Massey, 2010).
Design
A two-group, post-test only, randomly assigned study completed in 2007 at a major Southwestern cancer center compared the effect of rocking chair motion and standard care on POI duration. This post-test design was chosen because measurement for resolution of POI could occur only after abdominal surgery. The studys primary aim was to examine differences in the duration of POI as indicated by time to passage of first flatus in days between two groups of patients recovering from surgery performed to remove cancerous gastrointestinal tumors (standard care or standard care plus the rocking intervention). Standard postoperative care involved having the patient out of bed sitting in a non-rocking chair and ambulating beginning the first postoperative day, with care continuing until resolution of POI indicated by passage of first postoperative flatus. Care for the intervention group care involved having the patient out of bed rocking in a rocking chair in 10-20 minute increments for at least 1 hour per day, ambulating beginning the first postoperative day, and continuing until passage of first postoperative flatus. There were no significant differences in time rocking in rocking chairs, time sitting in nonrocking chairs, and distances ambulated between the two groups. A secondary aim of the study was to determine if there was an association between the time (day) bowel sounds first were heard with the time (day) passage of first flatus, the indicator used in the study, to indicate the resolution of POI.
patients with digestive system cancers scheduled to undergo abdominal surgery, English speaking, cognitively intact, able to ambulate and sit in a chair or rocking chair, and able to receive patient-controlled intravenous or epidural analgesia. Research team members interviewed patients during their preoperative evaluation in a private room in the Anesthesia Assessment Center. After patients received an explanation of the studys purpose and were allowed to ask questions, they signed a consent form if they desired to participate. Those agreeing to participate were randomized to receive either the standard care (non-rocking) or standard care plus the rocking intervention. Beginning the first postoperative day, the primary investigator assessed the patients at the same time each morning for return of bowel sounds and passage of first flatus. A review of the patients medical record was completed each day after surgery to identify any documentation (date/time) of a return of bowel sounds and/or passage of first flatus by nurses and/or surgeons. Auscultation of all quadrants of the abdomen for 5 minutes was performed by the primary investigator for the presence of bowel sounds regardless of any documentation of bowel sounds in the medical record. All data were documented on a study data sheet by the primary investigator.
not significant (r=0.231, p=0.062), indicating return of bowel sounds and time to first flatus were not associated. Findings from the Massey study support results reported by Madsen and colleagues (2005) for the evidence-based project challenging the auscultation of bowels as a reliable indicator for the end of POI. No association existed between the return of bowel sounds and the end of POI, supporting past evidence and a physiological basis for use of bowel sounds as most likely a poor indicator for the end of POI (Huge et al., 2000; Maron & Fry, 2008; Person & Wexner, 2006; Stewart & Waxman, 2007; Waldhausen & Schirmer, 1990; Waldhausen et al., 1990). Gastrointestinal motility returns in a specific sequence: small bowel within 24 hours, stomach 24-48 hours, and colon 72-120 hours after abdominal surgery. The resolution of POI is also dependent upon return of colon function, the last segment of the GI tract to experience return of motility after abdominal surgery (Delaney, 2004; Kehlet, 2008; Maron & Fry, 2008; Miedema & Johnson, 2003; Person & Wexner, 2006; Stewart & Waxman, 2007). Therefore, nurses should approach the use of return of bowel sounds with caution as an indicator of the end of POI in surgical patients after abdominal surgery.
Results
Sixty-six patients were enrolled in the study, and randomized either to the control (non-rocking) group (n=32) or rocking group (n=34) prior to surgery. Time to first bowel sounds and time to first flatus data were distributed normally, homogeneous for both groups, and indicated no significant differences between the rocking and non-rocking groups (see Table 1). No statistically significant differences were found in time to first bowel sounds between the non-rocking (M=2.25, SD=0.50) and rocking (M=2.21, SD=0.48) groups (t (64)=0.363, p=0.718, p<0.05). Pearsons correlation between time to first flatus and return of bowel sounds for combined groups was
Implications for Nursing
The auscultation for the return of bowel sounds to indicate return of GI motility and/or resolution of POI after abdominal surgery may be a practice tradition that should be used with caution and possibly replaced with other, more reliable indicators for the end of POI after abdominal surgery. Passage of first postoperative flatus, elimination of abdominal distention, nausea, vomiting, and tolerance of diet are indicators that appear to be more reliable indicators for the end of POI (Delaney et al., 2010; Kehlet, 2008; Maron & Fry, 2008; Person & Wexner, 2006; Stewart & Waxman, 2007). Future research and evidencebased evaluation of the passage of
149
Procedures
Approval was obtained from the University of Texas MD Anderson Cancer Center Institutional Review Board prior to implementation of the study. Informed consent was obtained prior to surgery from patients who met eligibility criteria. Participant inclusion criteria were all
May-June 2012 Vol. 21/No. 3
Research for Practice
first flatus, elimination of abdominal distention, nausea, vomiting, and tolerance of diet is needed and their roles in the resolution of POI is needed. In the meantime, nurses should use the return of bowel sounds with caution as an indicator of the resolution of POI in patients recovering from abdominal surgery.
REFERENCES Bonadonna, P . (1981). Effects of a vestibular stimulation program on stereotypic rocking behavior. [Clinical Trial Controlled Clinical Trial]. The American Journal of Occupational Therapy, 35(12), 775-781. Brieger, G.H. (1983). Early ambulation. A study in the history of surgery. [Case Reports Historical Article]. Annals of Surgery, 197(4), 443-449. Delaney, C.P . (2004). Clinical perspective on postoperative ileus and the effect of opiates. Neurogastroenterology Motilility, 16 (Suppl. 2), 61-66. doi:10.1111/j.17433150.2004.00559.x NMO559 [pii] Delaney, C.P ., Marcello, P .W., Sonoda, T., Wise, P ., Bauer, J., & Techner, L. (2010). Gastrointestinal recovery after laparoscopic colectomy: Results of a prospective, observational, multicenter study. [Multicenter Study Research Support, Non-U.S. Govt]. Surgical Endoscopy, 24(3), 653-661. doi:10.1007/s00464009-0652-7 Desborough, J. P . (2000). The stress response to trauma and surgery. British Journal of Anaesthesia, 85(1), 109-117. Greenhalgh, T., Robert, G., Macfarlane, F., Bate, P., & Kyriakidou, O. (2004). Diffusion of innovations in service organizations: Systematic review and recommendations. The Milbank Quarterly, 82(4), 581-629. doi: MILQ325 [pii]10.1111/j.0887-378X.2004.00325.x Houston, K.A. (1993). An investigation of rocking as relaxation for the elderly. Does rocking elicit in the elderly the physiologic changes of the relaxation response? Geriatric Nursing, 14(4), 186-189. Huge, A., Kreis, M.E., Zittel, T.T., Becker, H.D., Starlinger, M.J., & Jehle, E.C. (2000). Postoperative colonic motility and tone in patients after colorectal surgery. Diseases of the Colon and Rectum, 43(7), 932-939. Kehlet, H. (2008). Postoperative ileus an update on preventive techniques. Natational Clininical Practice Gastroenterolology and Hepatolology, 5(10), 552558. doi:ncpgasthep1230 [pii]10.1038/ ncpgasthep1230 Kirton, C. A. (1997). Assessing bowel sounds. Nursing, 27(3), 64. Luckey, A., Livingston, E., & Tache, Y. (2003). Mechanisms and treatment of postoperative ileus. Archives of Surgery, 138(2), 206-214. doi:srv2005[pii] Madsen, D., Sebolt, T., Cullen, L., Folkedahl, B., Mueller, T., Richardson, C., & Titler, M. (2005). Listening to bowel sounds: An evidence-based practice project: Nurses find that a traditional practice isnt the best indicator of returning gastrointestinal motility in patients whove undergone abdominal surgery. American Journal of Nursing, 105(12), 40-49; quiz 49-50. doi:00000446-200512000-00029 [pii] Maron, D.J., & Fry, R.D. (2008). New therapies in the treatment of postoperative ileus after gastrointestinal surgery. American Journal of Therapeutics, 15(1), 59-65. doi:10.1097/MJT.0b013e31804c6f37000 45391-200801000-00011 [pii] Massey, R.L. (2010). A randomized trial of rocking-chair motion on the effect of postoperative ileus duration in patients with cancer recovering from abdominal surgery. Applied Nursing Research, 23(2), 59-64. doi:S0897-1897(08)000499 [pii]10.1016/j.apnr.2008.06.001 Mehta, M. (2003). Assessing the abdomen. Nursing, 33(5), 54-55. Miedema, B.W., & Johnson, J.O. (2003). Methods for decreasing postoperative gut dysmotility. Lancet Oncolology, 4(6), 365-372. doi:S1470204503011185 [pii] Moore, L., Shannon, M.L., Richard, P ., & Vacca, G.R. (1995). Investigation of rocking as a postoperative intervention to promote gastrointestinal motility. Gastroenterology Nursing, 18(3), 86-91. Nachlas, M.M., Younis, M.T., Roda, C.P ., & Wityk, J.J. (1972). Gastrointestinal motility studies as a guide to postoperative management. Annals of Surgergy, 175(4), 510-522. Person, B., & Wexner, S. D. (2006). The management of postoperative ileus. Current Problems in Surgery, 43(1), 6-65. doi: S0011-3840(05)00138-3[pii]10.1067/ j.cpsurg.2005.10.004 Prasad, M., & Matthews, J. B. (1999). Deflating postoperative ileus. Gastroenterology, 117(2), 489-492. doi:S0016508599001 791 [pii] Stewart, D., & Waxman, K. (2007). Management of postoperative ileus. American Journal of Therapeutics, 14(6), 561-566. doi: 10.1097/MJT.0b013e 31804bdf5400045391-20071100000009 [pii] Thomas, L., Ptak, H., Giddings, L.S., Moore, L., & Oppermann, C. (1990). The effects of rocking, diet modifications, and antiflatulent medication on postcesarean section gas pain. Journal of Perinatolgy and Neonatal Nursing, 4(3), 12-24. Titler, M.G., Kleiber, C., Steelman, V.J., Rakel, B.A., Budreau, G., Everett, L.Q., ... Goode, C.J. (2001). The Iowa model of evidence-based practice to promote quality care. Critical Care Nursing Clinics of North America, 13(4), 497-509. Vrugt, D.T., & Pederson, D.R. (1973). The effects of vertical rocking frequencies on the arousal level in two-month-old infants. Child Development, 44(1), 205209. Waldhausen, J.H., & Schirmer, B.D. (1990). The effect of ambulation on recovery from postoperative ileus. Annals of Surgery, 212(6), 671-677. Waldhausen, J.H., Shaffrey, M.E., Skenderis, B.S., Jones, R.S., & Schirmer, B.D. (1990). Gastrointestinal myoelectric and clinical patterns of recovery after laparotomy. Annals of Surgery, 211(6), 777784; discussion 785.
150
May-June 2012 Vol. 21/No. 3
Copyright of MEDSURG Nursing is the property of Jannetti Publications, Inc. and its content may not be copied or emailed to multiple sites or posted to a listserv without the copyright holder's express written permission. However, users may print, download, or email articles for individual use.
Vous aimerez peut-être aussi
- Periop UrologyKoubaartikelDocument4 pagesPeriop UrologyKoubaartikeljustin_sanePas encore d'évaluation
- Postoperative Paralytic IleusDocument9 pagesPostoperative Paralytic IleusazisaaiPas encore d'évaluation
- Pre-Op NPO and Traditional Post-Op Diet Advancement: Time To Move OnDocument7 pagesPre-Op NPO and Traditional Post-Op Diet Advancement: Time To Move OnDaru KristiyonoPas encore d'évaluation
- NZJP Volume 47 Number 2 02Document10 pagesNZJP Volume 47 Number 2 02Suman DeyPas encore d'évaluation
- Iccn 042Document14 pagesIccn 042Seftiana WahyuniPas encore d'évaluation
- Respiratory Physiology & NeurobiologyDocument5 pagesRespiratory Physiology & NeurobiologynimaaandmPas encore d'évaluation
- Pain Medication Aute Abdominal PainDocument4 pagesPain Medication Aute Abdominal PainPanca SapriawanPas encore d'évaluation
- Daftar Pustaka AMDocument6 pagesDaftar Pustaka AMaichikaraiPas encore d'évaluation
- Faktor2 Operasi LaparatomiDocument11 pagesFaktor2 Operasi LaparatomiUmi FazaPas encore d'évaluation
- Postoperative Oral Feeding After Cesarean Section-Early Versus Late Initiation: A Prospective Randomized TrialDocument5 pagesPostoperative Oral Feeding After Cesarean Section-Early Versus Late Initiation: A Prospective Randomized Trialjustin_sanePas encore d'évaluation
- Ejercicios Masticacion 1989Document7 pagesEjercicios Masticacion 1989Estaf EmkeyzPas encore d'évaluation
- Jurnal Konstipasi 1Document10 pagesJurnal Konstipasi 1Intan DwiPas encore d'évaluation
- Lang 2011Document14 pagesLang 2011aungmyintkyawdrPas encore d'évaluation
- EBP Article IOWA ModelDocument10 pagesEBP Article IOWA ModelZACKDOUBLEDAYPas encore d'évaluation
- Articulo 2 Fisiologia RectalDocument6 pagesArticulo 2 Fisiologia RectalIsraael JuuareezPas encore d'évaluation
- Effect of I Love You (ILU) Massage On Rehabilitation of Children Digestive Function Postoperative StomachDocument7 pagesEffect of I Love You (ILU) Massage On Rehabilitation of Children Digestive Function Postoperative StomachSufi NurkhairunnisaPas encore d'évaluation
- Effect of I Love You (ILU) Massage On Rehabilitation of Children Digestive Function Postoperative StomachDocument7 pagesEffect of I Love You (ILU) Massage On Rehabilitation of Children Digestive Function Postoperative StomachYustian PaleriPas encore d'évaluation
- Imaging LGEADocument10 pagesImaging LGEANuanSyafrinaPas encore d'évaluation
- Pattern of Acute Intestinal Obstruction: Is There A Change in The Underlying Etiology?Document4 pagesPattern of Acute Intestinal Obstruction: Is There A Change in The Underlying Etiology?neildamiPas encore d'évaluation
- Novel Approaches in The Treatment of Fecal IncontinenceDocument18 pagesNovel Approaches in The Treatment of Fecal IncontinenceprivedPas encore d'évaluation
- Pain Medication Aute Abdominal PainDocument4 pagesPain Medication Aute Abdominal PainruthPas encore d'évaluation
- Sinclair2011 PDFDocument10 pagesSinclair2011 PDFAulia ZahraniPas encore d'évaluation
- Postoperative Ileus: Cristina R. Harnsberger, MD Justin A. Maykel, MD Karim Alavi, MD, MPHDocument5 pagesPostoperative Ileus: Cristina R. Harnsberger, MD Justin A. Maykel, MD Karim Alavi, MD, MPHfatima chrystelle nuñalPas encore d'évaluation
- 5 CResearch 5 CThe 20 Effects 20 of 20 Foot 20 Reflexology 20 On 20 Anxiety 20 and 20 PainDocument12 pages5 CResearch 5 CThe 20 Effects 20 of 20 Foot 20 Reflexology 20 On 20 Anxiety 20 and 20 PainAnnisa Aulia TenryPas encore d'évaluation
- Effectiveness of Standard Nursing Care With Gum Chewing To Reduce Bowel Ileus in Post-Operative Gynecologic Patients Randomized Controlled TrialsDocument8 pagesEffectiveness of Standard Nursing Care With Gum Chewing To Reduce Bowel Ileus in Post-Operative Gynecologic Patients Randomized Controlled TrialsdetrikaPas encore d'évaluation
- The Pathophysiology of Chemotherapy-Induced Nausea and VomitingDocument13 pagesThe Pathophysiology of Chemotherapy-Induced Nausea and VomitingLeoberto Batista Pereira SobrinhoPas encore d'évaluation
- 2009 A Critical Review of AuscultatingDocument6 pages2009 A Critical Review of AuscultatingaubinloPas encore d'évaluation
- Assessing Progress in LabourDocument9 pagesAssessing Progress in LabourPujianti LestarinaPas encore d'évaluation
- Pelvic FloorDocument10 pagesPelvic FloorAline Costales TafoyaPas encore d'évaluation
- (2021) Effects of Swallowing Training and Follow-Up On The Problems Associated WithDocument13 pages(2021) Effects of Swallowing Training and Follow-Up On The Problems Associated With王宇萱Pas encore d'évaluation
- W H D S D P F ?: Hat Arm Oes A Econd Elivery To The Elvic LoorDocument5 pagesW H D S D P F ?: Hat Arm Oes A Econd Elivery To The Elvic LoorRadis Virna Da GustaPas encore d'évaluation
- A Meta-Analysis of Passive Descent Versus Immediate Pushing in NulliparousDocument10 pagesA Meta-Analysis of Passive Descent Versus Immediate Pushing in NulliparousNoraPas encore d'évaluation
- Chapter No# 1: Definition of Cesarean SectionDocument27 pagesChapter No# 1: Definition of Cesarean SectionRabiaPas encore d'évaluation
- International Journal of Surgery: Emma J. Noble, Ros Harris, Ken B. Hosie, Steve Thomas, Stephen J. LewisDocument6 pagesInternational Journal of Surgery: Emma J. Noble, Ros Harris, Ken B. Hosie, Steve Thomas, Stephen J. LewisChristopher AdhisasmitaPas encore d'évaluation
- A Myth About Anastomotic LeakDocument3 pagesA Myth About Anastomotic LeakAvinash RoyPas encore d'évaluation
- Malnutrition in Hip Fracture Patients: An Intervention StudyDocument13 pagesMalnutrition in Hip Fracture Patients: An Intervention Studydahlia4Pas encore d'évaluation
- Fecal Incontinence As Consequence of Anorectal Surgery and The Physiotherapeutic ApproachDocument9 pagesFecal Incontinence As Consequence of Anorectal Surgery and The Physiotherapeutic ApproachSarah MendonçaPas encore d'évaluation
- Retraining Diaphragm and Core Muscles May Improve Urinary IncontinenceDocument7 pagesRetraining Diaphragm and Core Muscles May Improve Urinary IncontinenceSara AguiarPas encore d'évaluation
- IJNER - 597 - 27 07 2018 Paper - R - 21Document7 pagesIJNER - 597 - 27 07 2018 Paper - R - 21Yuning tyas Nursyah FitriPas encore d'évaluation
- Oakley 2016Document9 pagesOakley 2016JAZH EDREY LOZANOPas encore d'évaluation
- Chronic Gastric Dilatation in Horses Diagnosis, Treatment and Feeding Management A Survey of 20 Clinical CasesDocument8 pagesChronic Gastric Dilatation in Horses Diagnosis, Treatment and Feeding Management A Survey of 20 Clinical CasesXp Julieth HernandezPas encore d'évaluation
- Risk of Failure in Pediatric Ventriculoperitoneal Shunts Placed After Abdominal SurgeryDocument31 pagesRisk of Failure in Pediatric Ventriculoperitoneal Shunts Placed After Abdominal SurgeryWielda VeramitaPas encore d'évaluation
- Perioperative Fasting: A Time To Relook: Guest EditorialDocument2 pagesPerioperative Fasting: A Time To Relook: Guest EditorialIbraim CervantesPas encore d'évaluation
- Regular Stretch Does Not Increase Muscle ExtensibilityDocument9 pagesRegular Stretch Does Not Increase Muscle ExtensibilityAnonymPas encore d'évaluation
- Shift Work Ups IBS RiskDocument4 pagesShift Work Ups IBS RiskmkhoPas encore d'évaluation
- Postoperative Ileus Strategies For ReductionDocument6 pagesPostoperative Ileus Strategies For Reductionon miniPas encore d'évaluation
- DeLancey AUGS Pres 2008Document129 pagesDeLancey AUGS Pres 2008blackanddeckerjoePas encore d'évaluation
- TRADUCIRDocument9 pagesTRADUCIRNatalia Gonzalez GalvisPas encore d'évaluation
- Advances in Surgical NutritionDocument10 pagesAdvances in Surgical NutritionAndyPas encore d'évaluation
- A Review of Pain Management Interventions in Bone Marrow BiopsyDocument9 pagesA Review of Pain Management Interventions in Bone Marrow BiopsyFikriPas encore d'évaluation
- Pengaruh Mobilisasi Dini Terhadap Waktu Pemulihan Peristaltik Usus Pada Pasien Pasca Operasi Abdomen Di Ruang Icu Bprsud Labuang Baji Makassar Stefanus Mendes KiikDocument8 pagesPengaruh Mobilisasi Dini Terhadap Waktu Pemulihan Peristaltik Usus Pada Pasien Pasca Operasi Abdomen Di Ruang Icu Bprsud Labuang Baji Makassar Stefanus Mendes KiikWahyu WijayaPas encore d'évaluation
- Constiopation With OpiatesDocument14 pagesConstiopation With OpiatesAnonymous ZUaUz1wwPas encore d'évaluation
- Background: Postoperative Ileus After An Open CholecystectomyDocument9 pagesBackground: Postoperative Ileus After An Open CholecystectomyYostesara Maurena SantosaPas encore d'évaluation
- Functional and Motility Disorders of the Gastrointestinal Tract: A Case Study ApproachD'EverandFunctional and Motility Disorders of the Gastrointestinal Tract: A Case Study ApproachPas encore d'évaluation
- The ASMBS Textbook of Bariatric Surgery: Volume 1: Bariatric SurgeryD'EverandThe ASMBS Textbook of Bariatric Surgery: Volume 1: Bariatric SurgeryPas encore d'évaluation
- Nutritional Support after Gastrointestinal SurgeryD'EverandNutritional Support after Gastrointestinal SurgeryDonato Francesco AltomarePas encore d'évaluation
- Surgical Management of Benign Esophageal Disorders: The ”Chicago Approach”D'EverandSurgical Management of Benign Esophageal Disorders: The ”Chicago Approach”P. Marco FisichellaPas encore d'évaluation
- Obesity and Esophageal DisordersD'EverandObesity and Esophageal DisordersDhyanesh PatelPas encore d'évaluation
- Esophageal Preservation and Replacement in ChildrenD'EverandEsophageal Preservation and Replacement in ChildrenAshwin PimpalwarPas encore d'évaluation
- Heart Dysrhythmias Cheat Sheet PDFDocument5 pagesHeart Dysrhythmias Cheat Sheet PDFbarbaraPas encore d'évaluation
- Common Drug Stems Cheat SheetDocument2 pagesCommon Drug Stems Cheat SheetCharis Mae DimaculanganPas encore d'évaluation
- IV GaugesDocument1 pageIV Gaugesjustin_sanePas encore d'évaluation
- Review The Acute Respiratory Management of Cervical Spinal Cord Injury in The First 6 Weeks After Injury: A Systematic ReviewDocument14 pagesReview The Acute Respiratory Management of Cervical Spinal Cord Injury in The First 6 Weeks After Injury: A Systematic Reviewjustin_sanePas encore d'évaluation
- DM NephroDocument4 pagesDM Nephrojustin_sanePas encore d'évaluation
- Injection Site Cheat Sheet PDFDocument2 pagesInjection Site Cheat Sheet PDFjustin_sane100% (2)
- Cranial Nerves FormDocument2 pagesCranial Nerves FormbarbaraPas encore d'évaluation
- LISDocument7 pagesLISjustin_sanePas encore d'évaluation
- Insulin Cheat SheetDocument1 pageInsulin Cheat Sheetjustin_sanePas encore d'évaluation
- 2004 ConceptsDocument19 pages2004 Conceptsjustin_sanePas encore d'évaluation
- 2012 English Language TestsDocument1 page2012 English Language Testsjustin_sanePas encore d'évaluation
- Applications of Telecounselling in Spinal Cord Injury Rehabilitation: A Systematic Review With Effect SizesDocument13 pagesApplications of Telecounselling in Spinal Cord Injury Rehabilitation: A Systematic Review With Effect Sizesjustin_sanePas encore d'évaluation
- Improving Postoperative Pain Management What Are.40Document6 pagesImproving Postoperative Pain Management What Are.40Luz Adriana Flores PalafoxPas encore d'évaluation
- PDFDocument17 pagesPDFOkri PernandoPas encore d'évaluation
- Applications of Telecounselling in Spinal Cord Injury Rehabilitation: A Systematic Review With Effect SizesDocument13 pagesApplications of Telecounselling in Spinal Cord Injury Rehabilitation: A Systematic Review With Effect Sizesjustin_sanePas encore d'évaluation
- Assessment Nursing Diagnosis Scientific Explanation Planning Interventions Rationale EvaluationDocument2 pagesAssessment Nursing Diagnosis Scientific Explanation Planning Interventions Rationale Evaluationjustin_sanePas encore d'évaluation
- Peptic UlcerrDocument3 pagesPeptic Ulcerrjustin_sanePas encore d'évaluation
- AssessmentDocument10 pagesAssessmentjustin_sanePas encore d'évaluation
- HieDocument24 pagesHiejustin_sanePas encore d'évaluation
- PostOp IlleusDocument8 pagesPostOp Illeusjustin_sanePas encore d'évaluation
- DiagnosticDocument5 pagesDiagnosticjustin_sanePas encore d'évaluation
- DM NephroDocument4 pagesDM Nephrojustin_sanePas encore d'évaluation
- Microsoft Word - Pneumonia Education EnglishDocument9 pagesMicrosoft Word - Pneumonia Education Englishjustin_sanePas encore d'évaluation
- Risk For Infection Pneumonia Nursing Care PlanDocument1 pageRisk For Infection Pneumonia Nursing Care Planjustin_sane100% (1)
- Jurnal HipertensiDocument17 pagesJurnal HipertensiWiny Ch'amhada TtarudaPas encore d'évaluation
- Hyperthermia Pneumonia Nursing Care PlanDocument1 pageHyperthermia Pneumonia Nursing Care Planjustin_sanePas encore d'évaluation
- UlcerDocument24 pagesUlcerjustin_sanePas encore d'évaluation
- DMDocument10 pagesDMjustin_sanePas encore d'évaluation
- 2 Acute Pain Chronic Renal Failure Nursing Care PlansDocument5 pages2 Acute Pain Chronic Renal Failure Nursing Care Plansjustin_sanePas encore d'évaluation
- Physical AssessmentDocument29 pagesPhysical Assessmentjustin_sanePas encore d'évaluation
- Medical Gas Pipeline SystemsDocument218 pagesMedical Gas Pipeline Systemsmedo2005100% (10)
- Research ProposalDocument3 pagesResearch Proposalapi-345809869Pas encore d'évaluation
- Recognized Ho So ListDocument36 pagesRecognized Ho So Listpavan0% (1)
- Basic Foundation of Iv TherapyDocument10 pagesBasic Foundation of Iv Therapyjanna mae patriarcaPas encore d'évaluation
- 1 5053054235202027721Document175 pages1 5053054235202027721andifa aziz satriawanPas encore d'évaluation
- Dietary Counseling - PPT 1Document1 pageDietary Counseling - PPT 1AlexandraPas encore d'évaluation
- Circulating Nurse ResponsibilitiesDocument2 pagesCirculating Nurse ResponsibilitiesLouthor Zyver TanPas encore d'évaluation
- Knowledge, Attitudes and Practices of Caregivers in Relation To Oral Health of Preschool ChildrenDocument6 pagesKnowledge, Attitudes and Practices of Caregivers in Relation To Oral Health of Preschool ChildrenYayas Qori AwwaliPas encore d'évaluation
- Lecture Notes For Chapter 14 (Autonomic Nervous System) PDFDocument60 pagesLecture Notes For Chapter 14 (Autonomic Nervous System) PDFdwataPas encore d'évaluation
- COVID 19 Bharat India Report November09 2022 DailyCases 1116 Deaths 5 Based 781 DaysAnalysis Fbclid IwAR2orDocument225 pagesCOVID 19 Bharat India Report November09 2022 DailyCases 1116 Deaths 5 Based 781 DaysAnalysis Fbclid IwAR2orP Eng Suraj SinghPas encore d'évaluation
- Caries Risk Assessment, Cariogram, Caries VaccineDocument35 pagesCaries Risk Assessment, Cariogram, Caries VaccineUmaima Khan0% (3)
- Cdbb-Guide Vocal-Techniques EN PDFDocument17 pagesCdbb-Guide Vocal-Techniques EN PDFrox100% (1)
- Drug Study Amphotericin B, Meropenem, Furosemide, Ciprofloxacin, Pentoxifylline, Pip-Tazo, Midazolam, VecuroniumDocument12 pagesDrug Study Amphotericin B, Meropenem, Furosemide, Ciprofloxacin, Pentoxifylline, Pip-Tazo, Midazolam, Vecuroniumpaupaulala100% (4)
- A Components' Model of Addiction Within A Biopsychosocial FrameworkDocument8 pagesA Components' Model of Addiction Within A Biopsychosocial FrameworkBognár ErzsébetPas encore d'évaluation
- Verb Surgical - Surgery in The Digital AgeDocument15 pagesVerb Surgical - Surgery in The Digital AgemedtechyPas encore d'évaluation
- Phimosis 5 PDFDocument4 pagesPhimosis 5 PDFNurul YaqinPas encore d'évaluation
- Pure Tone AudiometryDocument8 pagesPure Tone AudiometrySuhaimi RostiPas encore d'évaluation
- Hempalin Enamel 5214000030 En-UsDocument9 pagesHempalin Enamel 5214000030 En-UszayzanPas encore d'évaluation
- Clinical Practice 3 Reflective JournalDocument13 pagesClinical Practice 3 Reflective JournalMimiUjang Corner BizzPas encore d'évaluation
- Training Programs in LCPDocument6 pagesTraining Programs in LCPHarbyPas encore d'évaluation
- PETUNJUK KHUSUS PILIHAN GANDADocument12 pagesPETUNJUK KHUSUS PILIHAN GANDARindah Tiara SariPas encore d'évaluation
- Oci R PDFDocument2 pagesOci R PDFAngelicaPas encore d'évaluation
- Facts About The Hand-Off Communications ProjectDocument2 pagesFacts About The Hand-Off Communications ProjectMukhlish MudaPas encore d'évaluation
- Polycystic Ovary SyndromeDocument19 pagesPolycystic Ovary SyndromeJalal AlbadriPas encore d'évaluation
- Bladder Training and Pelvic Floor Exercises Manage Urinary IncontinenceDocument21 pagesBladder Training and Pelvic Floor Exercises Manage Urinary IncontinenceRakhmad HidayatPas encore d'évaluation
- History TakingDocument67 pagesHistory TakingOluremi KehindePas encore d'évaluation
- A Rat Model For Oral Mucositis Induced byDocument7 pagesA Rat Model For Oral Mucositis Induced byYanski DarmantoPas encore d'évaluation
- Ironman April 2005Document119 pagesIronman April 2005bamabob1100% (1)
- Smiths Pneupac Ventipac OperatorDocument66 pagesSmiths Pneupac Ventipac Operatorzebubu1Pas encore d'évaluation
- Assessment KD 3.1Document5 pagesAssessment KD 3.1Ika NurjanahPas encore d'évaluation