Académique Documents
Professionnel Documents
Culture Documents
How Do The Kidneys Control Things?: Why Do We Need To Maintain It?
Transféré par
api-246259817Description originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
How Do The Kidneys Control Things?: Why Do We Need To Maintain It?
Transféré par
api-246259817Droits d'auteur :
Formats disponibles
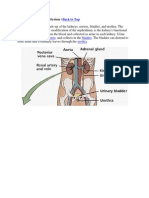
How do the kidneys control things?
The kidneys are responsible for the composition of the blood. This includes electrolyte balance, pH, osmolality, volume, waste and erythrocytes. Furthermore, the kidneys are capable of gluconeogenesis as glucose in important in the blood.
Water- maintaining osmolality
Why do we need to maintain it?
Like most things in biology the blood is mostly water, so lets first consider how the kidneys maintain the levels of water. If the extracellular fluid is hypotonic water will move into the cells. The kidneys need to remove water, to make the extracellular fluid more concentrated and back to normal. If the extracellular fluid is hypertonic water will move out of the cells, the ECF has a lower water potential because of its concentration.
How do we gain and loose water?
Gain through drinking and food- oxidative metabolism. Loss through lungs, skin, faeces and kidney- of these only the kidney can adjust. We have an obligatory water loss of .5 L per day, this is the minimum needed to dissolve stuff.
The potential to concentrate (urine)
The loop of henle produces dilute fluid- Na+ is actively reabsorbed in the ascending limb. The loop also creates conditions of high osmolality in the medulla. The distal tubule and collecting duct always have higher osmolarities outside of them compared to inside. There is always the potential for water to move from the filtrate outwards. Whether this occurs or not depends on their permeability to water. Their permeability to water depends on Antidiuretic Hormone, ADH increases the permeability causing water to move out of the urine reducing the volume of urine produced. ADH production is in the hypothalamus and secreted in the posterior pituitary gland. osmoreceptors detect hyper/hypotonic plasma and secrete ADH accordingly.
A negative feedback loop?
High plasma osmolality Eg Dehydration Osmoregulator cells in the hypothalamus shrink Increased secretion of ADH form posterior pituitary Increased aquaporins in Late Distal Tubule and Collecting duct Water leaves filtrate, removed by vasa recta More concentrated urine, lower volume of urine. More water retention, more water in plasma, lower osmolality. Low plasma osmolality Eg over hyration Osmoregulator cells in the hypothalamus swell Decreased secretion of ADH from the posterior pituitary Decreased aquaporins in Late Distal Tubule and Collecting duct Less water leaves filtrate Urine produced is dilute and of a high volume. Less water retention, less water in plasma, higher osmolality
What if you want really really concentrated urine?
Urea is reabsorbed by facilitated diffusion in the intrameduallary collecting duct. The basolateral membrane contains urea transporters that are constantly active but the apical membrane contains transporters which are minimally active except in the presents of ADH in the circulating vasculature. Through this ADH creates a pathway for urea to leave the filtrate into the medulla. This urea can be reabsorbed into earlier tubular segments or carried away in the circulation. o o It can re-enter the tubule via facilitated transport across the epithelia of the descending and ascending limbs If it is carried away in the circulation it is beneficial as it increases the osmolality of the blood passing through medulla allowing it to carry more water away. The urea will enter the cortex as it passes through.
The prevalence of urea in the medulla depends on the levels of ADH, high plasma levels of ADH yield more urea recycling. When water conservation is the most important aim urea recycling increases the conservation of water which is advantageous. As well as urea recycling ADH has another way of losing less water: ADH increases the reabsorption of sodium ions in the think ascending limb of the Loop of Henle (increasing the single effect).
Diabetes insipidus
Diabetes- too much urine, insipidus- very week. This condition comes from having insufficient ADH. Causes: 2
o o o
Idiopathic Trauma or surgery Familial
Alternatively it can be failure to respond to ADH. Urine output can be up to 18 L per day.
Sodium balance: control of blood volume
So far we have said how we can maintain the osmolality of the blood by increasing or decreasing the water that is reabsorbed in the distal tubule and collecting duct. Controlling the osmolality of the blood is only one roll of the kidneys, only controlling concentration would be useless unless you can control volume and composition as well. Lets look at how volume is controlled
Basics
o Sodium ions are the most abundant cation in the extracellular fluid. Changes in sodium ion content of the ECF leads to changes in water content.
Normally sodium ion intake is matched by kidney excretion. Increases in sodium ion concentration will lead to increases in osmolality leading to less ADH, see above. o Effective circulating volume o It is a virtual volume o Just the circulating volume- not the venous reservoir o Reflects the perfusion of tissue
Negative feedback system
In order to control volume we have a negative feedback system. This requires a sensor and an 3
effector. . For volume we have four effectors and three receptors. Next we look at them and how they interact.
The four effectors
The volume receptors will activate certain effectors, see diagram for which affects which. Firstly you need to get your head around what the effectors and receptors are.
Renal sympathetic nerves
Sympathetic nerves are for fight or flight. You do not want to have a full bladder when youre running from a bear, furthermore youll be sweating a lot take home message is sympathetic is for water retention. High effective circulating volume leads to increased renal sympathetic activity resulting in increased sodium reabsorption- where sodium goes water goes. Low effective circulating volume leads to decreased renal sympathetic activity resulting in decreased sodium reabsorption- where sodium goes water goes. Lead to: this is the role of the volume sensor which well talk about in a bit How? o Renal sympathetic activity causes constriction of the afferent and efferent arterioles. The afferent is constricted more than the efferent. There is a decrease in the hydrostatic pressure in the glomerular capillaries, this is a decrease in starlings forces favouring filtration. GFR will thus decrease and therefore the filtered load of sodium ions will decrease. Renal sympathetic activity directly stimulates sodium ion reabsorption in the thick ascending limb of the Loop of Henle Renal sympathetic activity increases the secretion of renin, and thus the renin-agniotensinaldosterone system. Also, renin, angiotensin is a vasoconstrictor which is what you want when youve got a bear up your arse!
o o
Renin-angiotensin-aldosterone system
Renin is secreted from the juxtaglomerular granular cells of the afferent arterial.
Some revision: o o o GFR must remain constant despite changes in blood pressure. There is autoregulation which maintains this Myogenic: smooth muscle in afferent arteriole contain Ca2+ permeant mechanosensory channels i.e. they constrict when stretched Tubuloglomerular feedback. This negative feedback mechanism relies on filtered load of sodium ions being a proxy measure of GFR and signals (using renin and adenosine) to constrict or dilate the afferent and efferent arterioles to maintain GFR.
In action: o Low blood volume would lead to a decrease in GFR. The juxtaglomerular feedback will cause an increase in GFR. Under normal circumstances this is beneficial, but in the case of low blood volume increasing GFR (to the same level) is a disadvantage Why do you not want a (relatively) high GFR in the case of low blood volume? With low blood volume you need to conserve sodium ion as water follows sodium. A greater GFR is equivalent to a greater filtered load of sodium, i.e. more that needs reabsorbing. Solution: renal sympathetic activity will override the effects of the juxtaglomerular feedback and constrict the afferent arteriole.
What does renin do??? Renin is an enzyme which converts angiotensinogen (from the liver) to angiotensin 1, then the enzyme we all know and love, ACE, converts angiotensin 1 to angiotensin 2. Angiotensin 2 has a whole host of effects: o o o o Arteriolar vasoconstriction Increased ADH secretion Increased sodium ion reabsorption in the proximal tubule. Increase in aldosterone secretion from the adrenal cortex (you see where this reninangiotensin-aldosterone systems coming from now erh)
Aldosterone is a steroid that simulates the synthesis of sodium ion and potassium ion channels on the apical membrane and sodium/potassium pumps on the basolatteral membrane of the distal tubule and collecting duct. The synthesis of these increases the reabsorption of sodium ions from the filtrate.
Atrial natriuretic peptide
Natriuretics cause sodium salts in the urine (natri, think Na). How can we get as much sodium ions into the urine as possible? o decrease reabsorption 5
Decrease renin secretion. An increase in the Na+ content of the filtrate is detected by the Tubuloglomerular feedback. Na+ is usually used as a proxy measure of GFR, high GFR results in increased sodium chloride delivered to the macula densa. For higher levels of sodium, usually indicative of a higher GFR, result in the inhibition of renin secretion. It is thought this is how ABP reduces renin secretion. Renin constricts the efferent arteriole increasing the hydrostatic pressure in the glomerular capillaries. Decreasing renin secretion decreases GFR. This causes a decrease in the filtered load of sodium which is counter intuitive but is an important effect of ANP. There are also other mechanisms which compensate for the reduced GFR and filtered load
Decrease aldosterone. Aldosterone as mentioned above increases the reabsorption of Na+ through increasing the synthesis of proteins mentioned above. This is through decreasing the renin secretion And a direct effect on the adrenal cortex Deceased reabsorption by collecting duct Again two causes, through the decreased aldosterone And direct inhibition of Na+ channels Decrease ADH secretion ADH increases the reabsorption of sodium ion in the thick ascending limb, by decreasing ADH secretion more sodium ions are being left in the filtrate.
ADH
ADH increases reabsorption of sodium ion in the think ascending limb and increase permeability of the late distal tubule and collecting duct to water.
The Three Volume Sensors
Now we have our mechanism to maintain blood volume lets have a look at the guys who inform them
Arterial (low pressure) Baroreceptors
These receptors are found in the atria and great veins. They are stretch receptors 6
Their afferent pathway is the vagus nerve Increased stretch means an increased effective circulatory volume, this causes: o Decrease in renal sympathetic activity Sympathetic works conserve water and sodium High effective circulatory volume (because the arterial baroreceptors are being stretched) needs a decrease in water content of the plasma thus a decrease in sympathetic activity We have a decrease in sympathetic activity as we aim to loose water and sodium Increase in Atrial Natriuretic Peptide Loose water, but also loose the sodium so its permanently lost
Arterial (high pressure) baroreceptors
These are the baroreceptors are the senors involved in the moment to moment control of blood pressure. They are found it the carotid sinus and the aortic arch. They are stimulated by stretch. Their afferent pathways are the vagus nerve and sinus nerve. Increased stretch means and increase in effective circulatory volume: o o Decrease heart rate (decrease sympathetic nerve activity) Decrease ADH Less water will be reabsorbed High volume of dilute urine Loss of water in urine will lead to a decrease in water component of plasma Decrease in renal sympathetic activity Renal sympathetic activitys role in decreasing blood water volume through reducing its activity is explained above
Renal baroreceptors Juxtaglomerular apparatus.
These are receptors in the afferent arterioles. They respond to stretch. Increase in stretch: o Decrease in renin secretion Renin is a sympathetic hormone, little stretch means little effective circulatory volume and thus a sympathetic response is appropriate The renin-angiotensin-aldosterone system does not pass go and does not collect 200
Potassium Ion Balance
Sodium ions were of particular importance because they are the most abundant ion in the Extracelluar Fluid, potassium ions are the most abundant in the Intracelluar Fluid. They are also extremely important in maintaining the resting potential.
Basics
98 % of potassium ions are intracellular Intracelluar fluid concentration is about 150mM Extracelluar fluid concentration must be between 3.5 and 5.0 mM It is really dangerous to not be in the range, you must know this range.
Dangers of not being in the range
Hypokalaemia (hypo, too little; kal, potassium; aemia in the blood) Less potassium ions on the outside of the cell than inside. There is a greater concentration gradient between the inside and the outside. Hypokalaemia is equivalent to a loss of positive charge outside of the cell. The cell is now relatively more negative than the outside. For excitable cells this causes them to be further away from their threshold. In severe cases: paralysis, cardiac arrhythmia, metabolic alkalosis. Hyperkalaemia More potassium ions on the outside of the cell than inside. There is a smaller concentration gradient. Smaller difference between the inside and out leads to a less negative resting potential. For excitable cells this means they will be closer to their threshold. Twitching, cardiac arrhythmia and arrest. In cases of trauma hyperkalaemia is common as you destroy cells allowing mixing of some intracellular fluid with extracelluar fluid. Either of these states can kill.
Controlling potassium quickly
Evidently having an increases or decreases is not good. The kidneys are in charge of controlling the concentration of potassium ions in the blood. However, it takes them a couple of hours to do this. Therefore we need other ways of controlling potassium over shorter periods of time. We use three hormones to stimulate the sodium potassium pumps to move potassium ions into cells, out of the extracellular fluid into the cells. In the cells it is not dangerous but over the long term still needs removing. This is the equivalent of moving the potassium from one pocket to another. The long term regulation is by the kidneys. Lets first look at these hormones Insulin Most important hormone in postprandial control (postprandial=after meal) In hyperkalaemia you can give insulin as (emergency) treatment as it will reduce the potassium levels to normal. However this requires strict monitoring of glucose levels. Another, slightly indirect, method is to give glucose which will stimulate insulin. This is used in trauma victims to treat hyperkalaemia Adrenaline Adrenaline has a bigger effect on beta receptors. Beta receptors stimulates potassium uptake into cells from the extracellular fluid. If a patient is on beta blockers, like propranolol, and are a victim of trauma they will be less able to prevent hyperkalaemia using adrenaline. Aldosterone Hyperkalaemia always stimulates the release of aldosterone.
Aldosterone works on both the short term control of potassium balance and long term renal control of it.
Longer term renal control of potassium levels
First well look at how the kidney handles potassium, then at how it controls potassium levels. Proximal tubule Two thirds of potassium, all of which is filtered at the glomerulus, is reabsorbed. Paracellular pathway by solvent drag. Solvent moves because of reabsorption of sodium. Ultimately this is linked so the sodium potassium pump. Loop of Henle 20% is reabsorbed here. Transcellular through the sodium, chloride, potassium symporter and paracelluar. Distal tubule and collecting duct This is where reabsorption can be controlled. Two types of cells: principal and intercalated. o Principal cells have Na/K pumps on the basolatteral side which create an electrochemical gradient for potassium from inside the cell to the filtrate. The apical membrane is permeable to potassium. This allows for potassium secretion.
What determines secretion?
The long term control of potassium needs controlling: o Plasma potassium ion concentration Higher concentrations of extracelluar potassium ions stimulate the sodium potassium ATPase pump. It also increases the permeability of the apical membrane to potassium Hyperkalaemia always stimulates the secretion of aldosterone (negative feedback) Aldosterone Increases activity of sodium potassium pump Short term solution to too much potassium Acts on distal tubule and collecting duct Also increase permeability of the apical membrane I hour lag before affect Increasing the flow of filtrate maintains the concentration gradient for potassium and leads to greater secretion- this is important when youre giving diuretics. Increased tubular sodium concentration
o o
10
More sodium ions move into cells Stimulate sodium potassium pump Greater pumping of potassium into cell- thus greater secretion. ADH ADH stimulates the sodium potassium pump to work harder and secrete more potassium However, ADH is increased at times when water content is high (ADH opens aquarpores allowing the reabsorption of water and the concentration of urine) If water content is high, flow of filtrate will be high. As discussed above the flow of filtrate leads to greater secretion. These two effects balance each other out.
Acidosis and alkalosis
Acidosis causes hyperkalaemia, and alkalosis causes hypokalaemia. How? o Protons can move from the extracelluar fluid to the intracellular fluid. This increases the number of intracellular cations. The cell responds by potassium exflux to the extracelluar fluid, thus maintaining the resting potential. This increases the extracelluar potassium ion concentration raises- hyperkalaemia. o This also works in reverse. Protons will inhibit the sodium potassium ATPase pump in the distal tubule, reducing potassium uptake from the blood and thus potassium excretion. This results in hyperkalaemia
Control of pH
Why is it important?
pH is an extremely important measurement of the blood. It is important in the structure and function of proteins, and thus the enzymes which control all of the biochemical reactions. They are also important in the voltage difference between the inside and out of cells and thus cell excitability. pH should be 7.4 at 37 degrees, concentration of H+ should be 35 to 45 nmol /L Remember pH is the minus log to the base ten of hydrogen ion concentration measured in moles per litre, not nanomoles etc. Tenth Hundredth 0.1 0.01 DeciCenti10-1 10-2
11
Thousandth Millionth Billionth
0.001 0.000001 0.000000001
MilliMicroNano-
10-3 10-6 10-9
Venous blood has a lower pH than arteriole o Venous blood has gained carbon dioxide from tissues (venous pH is 7.35)
What changes it?
All sorts of things can cause changes in pH of the blood, these changes can be dangerous if you dont do something about them. What are these things? o o o o o o o Respiratory depression (opiate use) Poor lung function Hyperventilation Prolonged vomiting (loss of acid, but also loss of chloride causing a change in strong ion difference, Steward approach) Prolonged diarrhoea (loss of bicarbonate) shock following trauma o Oxygen delivery is not good enough so you get anaerobic respiration All the tissues in your body are producing carbon dioxide o Producing 15 to 20 moles per day, you measure normal range in nmol o Can be excreted via lungs Its volatile! You also produce non-volatile acids o Sulphuric acid Cysteine, methionine o Hydrochloric Lysine, arginine o Phosphoric acid Phospholipids and phosphorylated amino acids o Organic acids Lactic acid Diabetic ketosis
How do we control it?
So far weve said why its important we maintain pH at a constant value. Weve also looked at some ways pH can be changed. Now lets think about how pH is maintained constant. There are three ways pH is maintained: o o Buffer systems Immediate Respiratory changes 12
o Renal
Changing PCO2 Over minutes Over hours to days
Buffers Different body fluids have different buffers: o Blood o Bicarbonate o Protein o Haemoglobin Interstitial o Bicarbonate Intracellular o Protein o Phosphoric acid
o o
Respiratory control How well the respiratory system is functioning effects PCO2, which in turn effects the equilibrium below.
H2O + CO2 H2CO3 H + HCO3
Another way of looking at it is how changes in PCO2 affect the Henderson-Hasselbalch equation.
13
Renal Control The kidney reabsorbs all HCO3- in health, it can add new HCO3- in acidosis and excrete HCO3- in alkalosis.
14
Vous aimerez peut-être aussi
- 201 - The Saggy Baggy Elephant - See, Hear, ReadDocument28 pages201 - The Saggy Baggy Elephant - See, Hear, ReadAndrew RukinPas encore d'évaluation
- Ascites, A Simple Guide To The Condition, Treatment And Related ConditionsD'EverandAscites, A Simple Guide To The Condition, Treatment And Related ConditionsPas encore d'évaluation
- A Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsD'EverandA Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsPas encore d'évaluation
- Histopathology ETASDocument89 pagesHistopathology ETASDr.Tawheed75% (4)
- Pharyngeal Arch Derivatives Chart!Document5 pagesPharyngeal Arch Derivatives Chart!Suphadetch Leung100% (1)
- GeneticsDocument13 pagesGeneticsNina SapphirePas encore d'évaluation
- Dictionary of Plant Biology En-SpDocument654 pagesDictionary of Plant Biology En-SpMelo2008100% (1)
- HEMODIALYSISDocument108 pagesHEMODIALYSISDan™100% (2)
- Hemodialysis: Carina Joane Villareal-Barroso, R.N.,M.NDocument108 pagesHemodialysis: Carina Joane Villareal-Barroso, R.N.,M.NJune BarsPas encore d'évaluation
- Acute Glomerulonephritis Case StudyDocument12 pagesAcute Glomerulonephritis Case StudyPrincess Tindugan100% (1)
- Under The Guidance Of: Dr. B.Shashidharan. Professor and Chief Unit-III By, Dr. Henley Punnen AndrewsDocument63 pagesUnder The Guidance Of: Dr. B.Shashidharan. Professor and Chief Unit-III By, Dr. Henley Punnen AndrewsHenley AndrewsPas encore d'évaluation
- Rembrandt BugattiDocument70 pagesRembrandt Bugattialdoremo1965100% (3)
- The Ontogenetic Basic of Human AnatomyDocument18 pagesThe Ontogenetic Basic of Human AnatomymeseniaPas encore d'évaluation
- Reproductive Biology and Phylogeny of SnakesDocument705 pagesReproductive Biology and Phylogeny of SnakesOscar David Ríos100% (2)
- ExcretionDocument17 pagesExcretionsmbdy tbhhhPas encore d'évaluation
- Urinalysis and Body FluidsDocument54 pagesUrinalysis and Body FluidsabdishakurPas encore d'évaluation
- Fluid and Electrolyte BalanceDocument3 pagesFluid and Electrolyte BalancejalajaraniPas encore d'évaluation
- A Share WATER & ELECTROLYTE BALANCEDocument14 pagesA Share WATER & ELECTROLYTE BALANCENaaz creates creativePas encore d'évaluation
- 25.9 Regulation of Fluid Volume and Composition - Anatomy and Physiology 2e - OpenStaxDocument4 pages25.9 Regulation of Fluid Volume and Composition - Anatomy and Physiology 2e - OpenStaxMarlene AngwaforPas encore d'évaluation
- 1.4 Virtual Patient - Elizabeth Harding: Describe The Structure of The NephronDocument7 pages1.4 Virtual Patient - Elizabeth Harding: Describe The Structure of The NephronAbdullah RajaPas encore d'évaluation
- Physio B 1.2 Renal Physiology Pt. 4 (Dr. Vila) : Because of Increase Water ReabsorptionDocument5 pagesPhysio B 1.2 Renal Physiology Pt. 4 (Dr. Vila) : Because of Increase Water ReabsorptionAnny AlvrzPas encore d'évaluation
- Biology Class NotesDocument11 pagesBiology Class NotessnnvcqzgnbPas encore d'évaluation
- Biology 7C 1Document4 pagesBiology 7C 1Abdullayev KamranPas encore d'évaluation
- 12.1 Waste Excretion and Equilibrium: Anatomy of The Urinary SystemDocument4 pages12.1 Waste Excretion and Equilibrium: Anatomy of The Urinary SystemVivian TangPas encore d'évaluation
- Excretion ExcretionDocument7 pagesExcretion ExcretionWaleed Bin KhalidPas encore d'évaluation
- Diagram of The KidneyDocument3 pagesDiagram of The KidneyElienai de LeonPas encore d'évaluation
- Test 4 Renal Gi Met DM AgingDocument9 pagesTest 4 Renal Gi Met DM AgingmeganPas encore d'évaluation
- THE URINARY SYSTEM Anatomy and PhysiologyDocument29 pagesTHE URINARY SYSTEM Anatomy and PhysiologyYatuwa LydiaPas encore d'évaluation
- Excretion (Continued)Document9 pagesExcretion (Continued)t0000123Pas encore d'évaluation
- Urinary Sys@completeDocument48 pagesUrinary Sys@completeGhina MengalPas encore d'évaluation
- The Renal SystemDocument10 pagesThe Renal SystemWahyu Purbo PangestiPas encore d'évaluation
- Basic of Fluid Therapy ImaDocument69 pagesBasic of Fluid Therapy Imal Made ArtawanPas encore d'évaluation
- PP24 Functioning of The KidneyDocument81 pagesPP24 Functioning of The KidneyLeloPas encore d'évaluation
- Chapter 16 ReviewDocument21 pagesChapter 16 Reviewjenn1722Pas encore d'évaluation
- The Human Excretory SystemDocument7 pagesThe Human Excretory Systemdonnah_veraPas encore d'évaluation
- KidneysDocument23 pagesKidneysshaliniPas encore d'évaluation
- Lecture 20 Notes 2018Document6 pagesLecture 20 Notes 2018Omed ZarifiPas encore d'évaluation
- FLG 332 Renal Physiology - 1 (2019)Document58 pagesFLG 332 Renal Physiology - 1 (2019)Huzaifa KhanPas encore d'évaluation
- 4 2 HomeworkDocument8 pages4 2 HomeworkShawntel IsordiaPas encore d'évaluation
- CairanDocument60 pagesCairanHanum HanattaPas encore d'évaluation
- Proximal Tubule Distal Tubule: Nutrients Nacl Hco H O K Nacl H O HcoDocument18 pagesProximal Tubule Distal Tubule: Nutrients Nacl Hco H O K Nacl H O HcogajenraoPas encore d'évaluation
- AP Biology Regulation Test ReviewDocument4 pagesAP Biology Regulation Test ReviewborntobewilderPas encore d'évaluation
- Chapter 19 Excretory Products and Their EliminationDocument27 pagesChapter 19 Excretory Products and Their Eliminationamit lakraPas encore d'évaluation
- Case AbstractDocument8 pagesCase AbstractRj DimaandalPas encore d'évaluation
- Fluid & Electrolyte Balance: Part 4: Regulation & MaintenanceDocument40 pagesFluid & Electrolyte Balance: Part 4: Regulation & MaintenanceMy MusicPas encore d'évaluation
- Endocrine Physiology: Dale Buchanan Hales, PHD Department of Physiology & BiophysicsDocument67 pagesEndocrine Physiology: Dale Buchanan Hales, PHD Department of Physiology & BiophysicsSourabh NandaPas encore d'évaluation
- PDF DocumentDocument86 pagesPDF DocumentRo-Anne LozadaPas encore d'évaluation
- Control of Extracellular Fluid Volume by The KidneyppDocument28 pagesControl of Extracellular Fluid Volume by The KidneyppLilian EdeniPas encore d'évaluation
- General Biology PPT Darryl Arcillas & Dency TuastumbanDocument14 pagesGeneral Biology PPT Darryl Arcillas & Dency TuastumbanApril Rose Caquilala GalauraPas encore d'évaluation
- AssignmentDocument6 pagesAssignmentleone shikukuPas encore d'évaluation
- JGLG TLA2 Refelective WritingDocument3 pagesJGLG TLA2 Refelective WritingJunnin Gay GarayPas encore d'évaluation
- The Renal SystemDocument53 pagesThe Renal SystemDarvey LongaraPas encore d'évaluation
- Renal Physiology 1Document9 pagesRenal Physiology 1Anny AlvrzPas encore d'évaluation
- Acute Glomerulonephritis Case StudyDocument12 pagesAcute Glomerulonephritis Case StudyPrincess Tindugan100% (1)
- Excretion and HomeostasisDocument11 pagesExcretion and HomeostasisstarcandypricessPas encore d'évaluation
- Chapter 25Document55 pagesChapter 25Chuy Cantu RdzPas encore d'évaluation
- I.Inroduction: Sign and SymptomsDocument7 pagesI.Inroduction: Sign and SymptomsMae Anne Cañas100% (1)
- 2d) Patofisiologi Sesak Napas by Dr. AminuddinDocument39 pages2d) Patofisiologi Sesak Napas by Dr. AminuddinMUHAMMAD BAGIR ALJUFRIPas encore d'évaluation
- Study Guide 2Document34 pagesStudy Guide 2api-260095216Pas encore d'évaluation
- Ii. Hydroelectrolytic Imbalance PDFDocument30 pagesIi. Hydroelectrolytic Imbalance PDFIvanes IgorPas encore d'évaluation
- Renal Physiology 5Document38 pagesRenal Physiology 5Hema KamatPas encore d'évaluation
- Physiology of Urine Formation: Submitted To - Mr. Pankaj Gupta Sir Department of ZoologyDocument15 pagesPhysiology of Urine Formation: Submitted To - Mr. Pankaj Gupta Sir Department of ZoologyRajeshwer duttPas encore d'évaluation
- The Urinary System: Pembentukan Urin Dan Peran Ginjal Dalam Keseimbangan Cairan TubuhDocument64 pagesThe Urinary System: Pembentukan Urin Dan Peran Ginjal Dalam Keseimbangan Cairan TubuhYunan Syahban MaskatPas encore d'évaluation
- SiadhDocument16 pagesSiadhGokul Rajan100% (1)
- 11.3 - The KidneyDocument7 pages11.3 - The KidneyraghadPas encore d'évaluation
- Clinical Disorder of Water 1Document7 pagesClinical Disorder of Water 1lovekhessyPas encore d'évaluation
- Renal Structure and Function: Dr. Catherine McdermottDocument38 pagesRenal Structure and Function: Dr. Catherine McdermottChrisPas encore d'évaluation
- Endocrine SystemDocument22 pagesEndocrine Systemmaxwell MutarePas encore d'évaluation
- Lower Limb Anatomy Quiz: Questions AnswersDocument3 pagesLower Limb Anatomy Quiz: Questions Answersapi-246259817Pas encore d'évaluation
- Upper Limb Anatomy Quiz: Questions AnswersDocument5 pagesUpper Limb Anatomy Quiz: Questions Answersapi-246259817Pas encore d'évaluation
- Year 1 Worksheet Wednesday 7Document1 pageYear 1 Worksheet Wednesday 7api-246259817Pas encore d'évaluation
- Head and Neck Quiz: Questions Answers My Answer Correct?Document6 pagesHead and Neck Quiz: Questions Answers My Answer Correct?api-246259817Pas encore d'évaluation
- Year 1 Worksheet Wednesday 8: CVRR Questions Are in RedDocument1 pageYear 1 Worksheet Wednesday 8: CVRR Questions Are in Redapi-246259817Pas encore d'évaluation
- Year 2 Worksheet Wednesday 6: 1. What Are The Three Parts of The Uterus?Document1 pageYear 2 Worksheet Wednesday 6: 1. What Are The Three Parts of The Uterus?api-246259817Pas encore d'évaluation
- Hi If Information On Potassium Levels Is Also Available Then You Should Use This in Your Calculation As Well. MarinaDocument1 pageHi If Information On Potassium Levels Is Also Available Then You Should Use This in Your Calculation As Well. Marinaapi-246259817Pas encore d'évaluation
- Year 1 Worksheet Wednesday 5: CVRR Questions Are in RedDocument2 pagesYear 1 Worksheet Wednesday 5: CVRR Questions Are in Redapi-246259817Pas encore d'évaluation
- Year 2 Worksheet Wednesday 5: CSIM Questions Are in BlueDocument1 pageYear 2 Worksheet Wednesday 5: CSIM Questions Are in Blueapi-246259817Pas encore d'évaluation
- UntitledDocument1 pageUntitledapi-246259817Pas encore d'évaluation
- Year 1 Worksheet Wednesday 2: CVRR Questions Are in RedDocument1 pageYear 1 Worksheet Wednesday 2: CVRR Questions Are in Redapi-246259817Pas encore d'évaluation
- Year 1 Worksheet Wednesday 6: CVRR Questions Are in RedDocument1 pageYear 1 Worksheet Wednesday 6: CVRR Questions Are in Redapi-246259817Pas encore d'évaluation
- Intro To Mic/ PPDDocument4 pagesIntro To Mic/ PPDapi-246259817Pas encore d'évaluation
- Year 1 Worksheet Wednesday 4: CVRR Questions Are in RedDocument1 pageYear 1 Worksheet Wednesday 4: CVRR Questions Are in Redapi-246259817Pas encore d'évaluation
- Shoulder Anatomy SummaryDocument4 pagesShoulder Anatomy Summaryapi-246259817Pas encore d'évaluation
- Year 2 Worksheet Wednesday 2: What Are The Different Categories of Differentiation of Malignant Neoplasms?Document1 pageYear 2 Worksheet Wednesday 2: What Are The Different Categories of Differentiation of Malignant Neoplasms?api-246259817Pas encore d'évaluation
- Year 1 Worksheet Wednesday 3: CVRR Questions Are in RedDocument1 pageYear 1 Worksheet Wednesday 3: CVRR Questions Are in Redapi-246259817Pas encore d'évaluation
- Introduction To FCDocument3 pagesIntroduction To FCapi-246259817Pas encore d'évaluation
- Year 2 Worksheet Wednesday 3: CSIM Questions Are in BlueDocument1 pageYear 2 Worksheet Wednesday 3: CSIM Questions Are in Blueapi-246259817Pas encore d'évaluation
- Year 1 Worksheet 1 AnswersDocument1 pageYear 1 Worksheet 1 Answersapi-246259817Pas encore d'évaluation
- Year 2 Worksheet Wednesday 1: CSIM Questions Are in BlueDocument1 pageYear 2 Worksheet Wednesday 1: CSIM Questions Are in Blueapi-246259817Pas encore d'évaluation
- Year 2 Worksheet 1 AnswersDocument1 pageYear 2 Worksheet 1 Answersapi-246259817Pas encore d'évaluation
- Year 1 Worksheet Wednesday 1: CVRR Questions Are in RedDocument1 pageYear 1 Worksheet Wednesday 1: CVRR Questions Are in Redapi-246259817Pas encore d'évaluation
- Reliability Theory of Aging and Longevity: Dr. Leonid A. Gavrilov, Ph.D. Dr. Natalia S. Gavrilova, PH.DDocument67 pagesReliability Theory of Aging and Longevity: Dr. Leonid A. Gavrilov, Ph.D. Dr. Natalia S. Gavrilova, PH.DUpendra KachruPas encore d'évaluation
- Altruism and Social TheoryDocument34 pagesAltruism and Social TheorySvetlanaPas encore d'évaluation
- Sri Chaitanya ZoologyDocument3 pagesSri Chaitanya ZoologypullaiPas encore d'évaluation
- MLTDocument20 pagesMLTSai SridharPas encore d'évaluation
- Wiki JellyfishDocument1 pageWiki Jellyfishwdm00Pas encore d'évaluation
- Cnidaria - Radiate Animals: HydrozoaDocument6 pagesCnidaria - Radiate Animals: Hydrozoafitness finessePas encore d'évaluation
- Animal ClassificationDocument18 pagesAnimal ClassificationPratham KhairnarPas encore d'évaluation
- EntomologyDocument50 pagesEntomologyapi-19960301100% (1)
- Biology Paper2 Form 4Document12 pagesBiology Paper2 Form 4hqbehPas encore d'évaluation
- Extinct Animals in India: Indian ChitaDocument4 pagesExtinct Animals in India: Indian ChitaHafizuddin SyedPas encore d'évaluation
- Hazel Rhs Horticulture Level 2 Essay 1Document24 pagesHazel Rhs Horticulture Level 2 Essay 1hazeldwyerPas encore d'évaluation
- Richard Dawkins in Furious Row With EO Wilson Over Theory of Evolution - Science - The GuardianDocument3 pagesRichard Dawkins in Furious Row With EO Wilson Over Theory of Evolution - Science - The GuardianrobiePas encore d'évaluation
- Examen - Unit 1 - Present SimpleDocument11 pagesExamen - Unit 1 - Present SimpleMary SalazarPas encore d'évaluation
- Work Sheet Animal Systematic I - Activity 2 - 20202021-1Document3 pagesWork Sheet Animal Systematic I - Activity 2 - 20202021-1Anang Yanuar RamadhanPas encore d'évaluation
- Rodriguez-Ferreretal - 2017 Marine RecorsDocument4 pagesRodriguez-Ferreretal - 2017 Marine Recorsalyman_bPas encore d'évaluation
- Migration in BirdsDocument29 pagesMigration in BirdsGEETA MOHAN100% (1)
- Z14 - Characteristics - Phylum Porifera & CnidariaDocument2 pagesZ14 - Characteristics - Phylum Porifera & CnidariaMilvy Faith C. SyjongtianPas encore d'évaluation
- Palaeoniscoid Remains From The Lower Permian Pedra de Fogo Formation Parna Ba Basin Insights From General Morphology and HistologyDocument12 pagesPalaeoniscoid Remains From The Lower Permian Pedra de Fogo Formation Parna Ba Basin Insights From General Morphology and HistologyVictor FontesPas encore d'évaluation
- Bingo สัตว์ 24คำDocument24 pagesBingo สัตว์ 24คำsatanghisoPas encore d'évaluation
- Skeleton Male or FemaleDocument5 pagesSkeleton Male or FemaleNaru DesuPas encore d'évaluation
- Chapter 18Document10 pagesChapter 18Aeriel Venice VergaraPas encore d'évaluation
- Bio205 Lab Report PDFDocument8 pagesBio205 Lab Report PDFjonahbsPas encore d'évaluation