Académique Documents
Professionnel Documents
Culture Documents
Molluscum Contagiosum Andrew N Pitzpatrick
Transféré par
Hel Da0 évaluation0% ont trouvé ce document utile (0 vote)
65 vues5 pagesMolluscum contagiosum is caused by a poxvirus that infects young children, sexually active adults, and immunosuppressed individuals like those with HIV. It presents as small, smooth, dome-shaped papules with a central indentation. Treatment involves removing the core of the lesions by curettage, cryotherapy, or topical medications. For immunosuppressed patients, resolving the underlying condition often leads to clearance of molluscum lesions.
Description originale:
wewe
Titre original
Molluscum Contagiosum Andrew n Pitzpatrick
Copyright
© © All Rights Reserved
Formats disponibles
DOCX, PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentMolluscum contagiosum is caused by a poxvirus that infects young children, sexually active adults, and immunosuppressed individuals like those with HIV. It presents as small, smooth, dome-shaped papules with a central indentation. Treatment involves removing the core of the lesions by curettage, cryotherapy, or topical medications. For immunosuppressed patients, resolving the underlying condition often leads to clearance of molluscum lesions.
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
65 vues5 pagesMolluscum Contagiosum Andrew N Pitzpatrick
Transféré par
Hel DaMolluscum contagiosum is caused by a poxvirus that infects young children, sexually active adults, and immunosuppressed individuals like those with HIV. It presents as small, smooth, dome-shaped papules with a central indentation. Treatment involves removing the core of the lesions by curettage, cryotherapy, or topical medications. For immunosuppressed patients, resolving the underlying condition often leads to clearance of molluscum lesions.
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 5
Molluscum contagiosum
Molluscum contagiosum is caused by up to four closely related
types of poxvirus, MCV-1 to 4 and their variants. Although
the proportion of infection caused by the various types varies
geographically, throughout the world MCV-1 infections are
most common. In small children virtually all infections are
caused by MCV-1. There is no difference in the anatomic
region of isolation with regard to infecting type (as opposed
to HSV, for example). In patients infected with HIV, however,
MCV-2 causes the majority of infections (60%), suggesting that
HIV infection-associated molluscum does not represent recrudescence
of childhood molluscum.
Infection with MCV is worldwide. Three groups are primarily
affected: young children, sexually active adults, and
immunosuppressed persons, especially those with HIV infection.
Molluscum is most easily transmitted by direct skin-toskin
contact, especially if the skin is wet. Swimming pools
have been associated with infection.
In all forms of infection, the lesions are relatively similar.
Individual lesions are smooth-surfaced, firm, dome-shaped,
pearly papules, averaging 35 mm in diameter (Fig. 19-32).
Giant lesions may be up to 1.5 cm in diameter. A central
umbilication is characteristic. Irritated lesions may become
crusted and even pustular, simulating secondary bacterial
infection. This may precede spontaneous resolution. Lesions
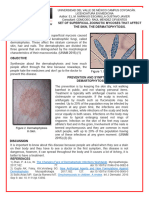
Fig. 19-34 Molluscum contagiosum, child with atopic dermatitis.
that rupture into the dermis may elicit a marked suppurative
inflammatory reaction that resembles an abscess.
The clinical pattern depends on the risk group affected. In
young children the lesions are usually generalized and number
from a few to more than 100. Dermatitis surrounding a lesion
usually heralds the resolution of that lesion. Lesions tend to
be on the face, trunk, and extremities. Genital lesions occurring
as part of a wider distribution occur in 10% of childhood cases.
When molluscum is restricted to the genital area in a child, the
possibility of sexual abuse must be considered.
In adults, molluscum is sexually transmitted and other
STDs may coexist. There are usually fewer than 20 lesions;
these favor the lower abdomen, upper thighs, and the penile
shaft in men (Fig. 19-33). Mucosal involvement is very
uncommon.
Immunosuppression, either systemic T-cell immunosuppression
(usually HIV, but also sarcoidosis and malignancies)
or abnormal cutaneous immunity (as in atopic dermatitis or
topical steroid use), predisposes the individual to infection. In
atopic dermatitis, lesions tend to be confined to dermatitic skin
(Fig. 19-34).
Secondary infection may occur. In addition, in about 10% of
lesions, a surrounding eczematous reaction is present (molluscum
dermatitis). Rarely, erythema annulare centrifugum
may be associated. Lesions on the eyelid margin or conjunctiva
may be associated with a conjunctivitis or keratitis. Rarely, the
molluscum lesions may present as a cutaneous horn (molluscum
contagiosum cornuatum).
Between 10 and 30% of AIDS patients not receiving antiretroviral
therapy have molluscum contagiosum. Virtually all
Fig. 19-33 Molluscum contagiosum of the penis.
Fig. 19-34 Molluscum contagiosum, child with atopic dermatitis.
HIV-infected patients with molluscum contagiosum already
have an AIDS diagnosis and a helper T-cell count of less than
100. In untreated HIV disease, lesions favor the face (especially
the cheeks, neck, and eyelids) and genitalia. They may be few
or numerous, forming confluent plaques. Giant lesions are not
uncommon and may be confused with a basal cell carcinoma.
Involvement of the oral and genital mucosa may occur, virtually
always indicative of advanced AIDS (helper T-cell count
less than 50). Facial disfigurement with numerous lesions can
occur.
Molluscum contagiosum has a characteristic histopathology.
Lesions primarily affect the follicular epithelium. The lesion is
acanthotic and cup-shaped. In the cytoplasm of the prickle
cells, numerous small eosinophilic and later basophilic inclusion
bodies, called molluscum bodies or HendersonPaterson
bodies, are formed. Eventually, their bulk compresses the
nucleus to the side of the cell. In the fully developed lesion
each lobule empties into a central crater. Inflammatory changes
are slight or absent. Characteristic brick-shaped poxvirus particles
are seen on electron microscopy in the epidermis. Latent
infection has not been found, except in untreated AIDS
patients, in whom even normal-appearing skin may contain
viral particles. Molluscum contagiosum virus contains an
IL-18 binding protein gene it apparently acquired from
humans. This blocks the hosts initial effective Th1 immune
response against the virus by reducing local IFN-
production.
The diagnosis is easily established in most instances because
of the distinctive central umbilication of the dome-shaped
lesion. This may be enhanced by light cryotherapy that leaves
the umbilication appearing clear against a white (frozen) background.
For confirmation, express the pasty core of a lesion,
squash it between two microscope slides (or a slide and a cover
glass) and stain it with Wright, Giemsa, or Gram stains. Firm
compression between the slides is required.
Treatment is determined by the clinical setting. In young
immunocompetent children, especially those with numerous
lesions, the most practical course may be not to treat or
to use only topical tretinoin. Aggressive treatment may be
emotionally traumatic and can cause scarring. Spontaneous
resolution is virtually a certainty in this setting, avoiding
these sequelae. Individual lesions last 24 months each;
the duration of infection is about 2 years. Continuous application
of surgical tape to each lesion daily after bathing for
16 weeks led to cure in 90% of children so treated. Topical
cantharidin, applied for 46 h to approximately 20 lesions per
setting, led to resolution in 90% of patients and 8% of patients
improved. This therapy is well tolerated, has a very high
satisfaction rate for patients and their parents, and has rare
complications. If lesions are limited and the child is cooperative,
nicking the lesions with a blade to express the core (with
or without the use of a comedo extractor), light cryotherapy,
application of trichloroacetic acid (35100%), or removal by
curettage are all alternatives. The application of EMLA cream
for 1 h before any painful treatments has made the management
of molluscum in children much easier. Topical 5%
sodium nitrite with 5% salicylic acid cures about 75% of
patients. No controlled trials have confirmed the efficacy of
imiquimod and it cannot be recommended for the treatment
of molluscum.
In adults with genital molluscum, removal by cryotherapy
or curettage is very effective. Neither imiquimod nor podophyllotoxin
has been demonstrated to be effective. In fact, the
failure of these agents to improve genital warts suggests the
diagnosis of genital molluscum contagiosum. Sexual partners
should be examined; screening for other coexistent STDs is
mandatory.
In patients with atopic dermatitis, application of EMLA followed
by curettage or cryotherapy is most practical. Caustic
chemicals should not be used on atopic skin. Topical steroid
application to the area should be reduced to the minimum
strength possible. A brief course of antibiotic therapy should
be considered after initial treatment, since dermatitic skin is
frequently colonized with S. aureus.
In immunosuppressed patients, especially those with AIDS,
management of molluscum can be very difficult. Aggressive
treatment of the HIV infection with HAART, if it leads to
improvement of the helper T-cell count, is predictably associated
with a dramatic resolution of the lesions. This response
is delayed 68 months from the institution of the treatment.
Molluscum occurs frequently in the beard area, so shaving
with a blade razor should be discontinued to prevent its
spread. If lesions are few, curettage or core removal with a
blade and comedo extractor is most effective. EMLA application
may permit treatment without local anesthesia. Cantharone
or 100% trichloroacetic acid may be applied to individual
lesions. Temporary dyspigmentation and slight surface irregularities
may occur. Cryotherapy may be effective but must be
used with caution in persons of pigment. When lesions are
numerous or confluent, treatment of the whole affected area
may be required because of the possibility of latent infection.
Trichloroacetic acid peels above 35% concentration (medium
depth) or daily applications of 5-fluorouracil (5-FU) to the
point of skin erosion may eradicate lesions, at least temporarily.
At times, removal by curette is required. In patients with
HIV infection, continuous application of tretinoin cream once
nightly at the highest concentration tolerated seems to reduce
the rate of appearance of new lesions. Topical 13% cidofovir
application and systemic infusion of this agent have been
reported to lead to dramatic resolution of molluscum in
patients with AIDS.
The curette has long been a standard tool in the dermatologists
surgical management of neoplasm. This round, semisharp
knife is available in sizes from 0.5 to 10 mm, allowing
for the removal of a variety of lesions. Since it is not as sharp
as a scalpel, the curette does not easily cut through normal
skin. Therefore, it is best suited for use on soft or friable lesions,
such as warts, seborrheic and actinic keratoses, the papules of
molluscum contagiosum, or selected basal and squamous cell
carcinomas. The proper selection of lesion, location, and the
size of the curette, combined with the surgeons technique, all
play a role in both the therapeutic and cosmetic outcome.
The skin should be stabilized with the nondominant hand
while the curette is held like a pencil. Curettage should be
performed in a centripetal manner (from the outside in) to
avoid stripping sun-damaged skin and creating a larger
wound. To ensure complete destruction, curettage should be
performed in multiple directions to produce symmetrical
wound margins. A large curette is used for initial debulking,
followed by a smaller curette to remove any residual foci
or extensions. Curettage is complete when the gritty, firm
sensation of normal dermis is felt and slight punctate dermal
bleeding occurs.
Curettage, combined with electrodesiccation (C&E), is
widely used for the treatment of BCC and squamous cell carcinomas
(SCC) (Fig. 37-15). Silverman et al reviewed the cure
rates of primary BCC treated with C&E over a 27-year period
at New York University. The result of the study stratified low-,
middle-, and high-risk anatomic locations and the risk of
recurrence following C&E of primary BCC. Low-risk anatomic
sites (neck, trunk, and four extremities) had a 5-year recurrence
rate of 3.3%. Middle-risk sites (scalp, forehead, pre- and
post-auricular, and malar areas) had an overall recurrence
rate of 12.9%, but this was reduced to 5% when limited to
noninfiltrative carcinomas of less than 1 cm. High-risk sites
(nose, paranasal, nasolabial groove, ear, chin, mandibular,
perioral, periocular areas) had an overall recurrence rate of
17.5%, but a more acceptable 5% recurrence rate was achieved
when treatment was limited to lesions of less than 6 mm.
In addition to size and anatomic location, the histologic
subtype is an important factor in the effectiveness of C&E.
Infiltrative and micronodular BCC are not appropriate for
C&E, while it can be considered a therapeutic option in superficial
and nodular subtypes. SCC in situ may be appropriately
treated with C&E, while in most circumstances invasive SCC
would not typically be amenable to this modality
Vous aimerez peut-être aussi
- Epidemiology: Aureus and GABHS 10% of The Time. Methicillin-Resistant S Aureus (MRSA) HasDocument8 pagesEpidemiology: Aureus and GABHS 10% of The Time. Methicillin-Resistant S Aureus (MRSA) HasPutra YdpaPas encore d'évaluation
- Skin and Soft Tissue Infection InfoDocument4 pagesSkin and Soft Tissue Infection InfoPresura Andreea IulianaPas encore d'évaluation
- Tubkut Srilanka JournalDocument7 pagesTubkut Srilanka JournalMusdalifah MimousPas encore d'évaluation
- Molluscum Contagiosum and WartsDocument8 pagesMolluscum Contagiosum and WartscefalalgiaPas encore d'évaluation
- Herpes Zoster Ophthalmicus-Diagnosis and ManagementDocument6 pagesHerpes Zoster Ophthalmicus-Diagnosis and ManagementseptynePas encore d'évaluation
- Tom Son 2007Document7 pagesTom Son 2007riedha_chanzPas encore d'évaluation
- MolluscumDocument11 pagesMolluscumAstari Pratiwi NuhrintamaPas encore d'évaluation
- Candidiasis (Candidosis)Document17 pagesCandidiasis (Candidosis)h8j5fnyh7dPas encore d'évaluation
- Molluscum MedscapeDocument35 pagesMolluscum MedscapeAninditaPas encore d'évaluation
- Viral Skin Infections: Verrucae ValgarusDocument14 pagesViral Skin Infections: Verrucae Valgarusمسلم هاشم منافPas encore d'évaluation
- Reaction (PCR) Dan Hibridisasi. Penularan Kutil Terjadi Langsung Dari Hubungan Langsung AtauDocument5 pagesReaction (PCR) Dan Hibridisasi. Penularan Kutil Terjadi Langsung Dari Hubungan Langsung AtauJo MahameruPas encore d'évaluation
- Fungal InfectionsDocument9 pagesFungal InfectionsCoral Srinivasa RamaluPas encore d'évaluation
- DR - Ali's Uworld Notes For Step 2 CKDocument19 pagesDR - Ali's Uworld Notes For Step 2 CKuyesPas encore d'évaluation
- Diagnosis, Prevention, and Treatment of ScabiesDocument5 pagesDiagnosis, Prevention, and Treatment of ScabiesSince Ivanna RumbiakPas encore d'évaluation
- Molluscum Contagiosum (EScholarship)Document7 pagesMolluscum Contagiosum (EScholarship)Try Wahyudi Jeremi LoLyPas encore d'évaluation
- Acs Skabies InternationalDocument3 pagesAcs Skabies InternationalChandra AnggaraPas encore d'évaluation
- Pathophysiology ImpetigoDocument3 pagesPathophysiology ImpetigoAnne de VeraPas encore d'évaluation
- Epidemiology: FilariasisDocument10 pagesEpidemiology: Filariasisketty putriPas encore d'évaluation
- Impetigo in Children: A Clinical Guide and Treatment OptionsDocument2 pagesImpetigo in Children: A Clinical Guide and Treatment OptionsBeuty SavitriPas encore d'évaluation
- Annular LesionsDocument8 pagesAnnular LesionshpmcentrePas encore d'évaluation
- Psoriasis: Posted: 02 Aug 2010 11:18 PM PDTDocument5 pagesPsoriasis: Posted: 02 Aug 2010 11:18 PM PDTScamb TrekPas encore d'évaluation
- Molluscum ContagiosumDocument1 pageMolluscum Contagiosumshailesh284Pas encore d'évaluation
- Skin Diseases Affecting The VulvaDocument7 pagesSkin Diseases Affecting The VulvaNoraPas encore d'évaluation
- Skin InfectionsDocument22 pagesSkin InfectionsoktafPas encore d'évaluation
- Toxoplasmosis AaoDocument28 pagesToxoplasmosis AaoUNHAS OphthalmologyPas encore d'évaluation
- Bacterial Infections of The Skin, Soft TissuesDocument27 pagesBacterial Infections of The Skin, Soft TissuesSHIHAB UDDIN KAZI100% (1)
- SOFIA SALSABILA Rangkuman On ProgressDocument10 pagesSOFIA SALSABILA Rangkuman On ProgressSofia SalsabilaPas encore d'évaluation
- YAWS: Elimination To EradicationDocument5 pagesYAWS: Elimination To EradicationShrutiPas encore d'évaluation
- TRACHOMA and YAWS-1Document19 pagesTRACHOMA and YAWS-1Aadil AminPas encore d'évaluation
- Tinea Capitis in AdultsDocument7 pagesTinea Capitis in Adultsdimasarya671Pas encore d'évaluation
- Leishmaniasis: Dr. Kazi Shihab Uddin Mbbs MRCP (Uk) Associate Professor & HOD Department of Internal MedicineDocument20 pagesLeishmaniasis: Dr. Kazi Shihab Uddin Mbbs MRCP (Uk) Associate Professor & HOD Department of Internal MedicineSHIHAB UDDIN KAZIPas encore d'évaluation
- Molluscum Contagiosum - An Update: ReviewDocument3 pagesMolluscum Contagiosum - An Update: ReviewArdi WidiatmikaPas encore d'évaluation
- Jurnal Reading KulitDocument26 pagesJurnal Reading KulitKeyko SeptiyantiPas encore d'évaluation
- 3.bacterial Infection-2Document146 pages3.bacterial Infection-2Biruk WorkuPas encore d'évaluation
- Integumen Viral InfectionDocument34 pagesIntegumen Viral InfectionNissa KeyssaPas encore d'évaluation
- Etiology and Epidemiology: Eroded As The Overlying Epidermis SloughsDocument3 pagesEtiology and Epidemiology: Eroded As The Overlying Epidermis SloughsUlul Azmi Rumalutur NeinaPas encore d'évaluation
- C R o W E, M A R K A - Moluscum Contagiosum. Diakses Dari: - Pada Tanggal 27 Desember 2016Document22 pagesC R o W E, M A R K A - Moluscum Contagiosum. Diakses Dari: - Pada Tanggal 27 Desember 201679lalalaPas encore d'évaluation
- Cartel MejoradoDocument1 pageCartel MejoradoGustavo NaranjoPas encore d'évaluation
- ScabiesDocument16 pagesScabiescarla_sarmiento4847Pas encore d'évaluation
- Impetigo: Author: Sadegh Amini, MD, Senior Clinical Research Fellow, Skin Research GroupDocument12 pagesImpetigo: Author: Sadegh Amini, MD, Senior Clinical Research Fellow, Skin Research GroupDanoe Setyo SPas encore d'évaluation
- Dermatology For The General SurgeonDocument24 pagesDermatology For The General SurgeonAnita HerreraPas encore d'évaluation
- 0 - Skin Conditions in SportsDocument28 pages0 - Skin Conditions in SportsAndroid HomePas encore d'évaluation
- Superficial Skin Infections and The Use of Topical and Systemic Antibiotics in General PracticeDocument4 pagesSuperficial Skin Infections and The Use of Topical and Systemic Antibiotics in General Practicepeter_mrPas encore d'évaluation
- A. Introduction of Skin and Soft Tissue InfectionsDocument10 pagesA. Introduction of Skin and Soft Tissue InfectionsChristin alexaPas encore d'évaluation
- Kondilomata AkuminataDocument6 pagesKondilomata AkuminataChristy BradyPas encore d'évaluation
- RF2 Tabal JDocument2 pagesRF2 Tabal JRamses ParconPas encore d'évaluation
- Reactive Inflammatory ErythemasDocument71 pagesReactive Inflammatory ErythemasYasir Saleem KhanPas encore d'évaluation
- C Professor of Pediatrics, Medical Microbiology andDocument20 pagesC Professor of Pediatrics, Medical Microbiology andB'durPas encore d'évaluation
- Jur DingDocument6 pagesJur DingRund Van EarghPas encore d'évaluation
- Molluscum ContagiosumDocument2 pagesMolluscum ContagiosumMalueth AnguiPas encore d'évaluation
- Tinea FasialisDocument8 pagesTinea FasialisFelix Tortora SekaiPas encore d'évaluation
- 14 - Bacterial InfectionsDocument43 pages14 - Bacterial Infectionseagame gamersPas encore d'évaluation
- Viral Skin InfectionsDocument9 pagesViral Skin InfectionsMa Sul JudayaPas encore d'évaluation
- Congenital Toxoplasmosis: Clinical Features and Diagnosis - UpToDateDocument33 pagesCongenital Toxoplasmosis: Clinical Features and Diagnosis - UpToDateMARIA EMILIA ORTEGA ABADPas encore d'évaluation
- Cap 16 Schwatz - Pyoderma Gangrenosum (PG) : SummaryDocument2 pagesCap 16 Schwatz - Pyoderma Gangrenosum (PG) : SummaryLuca VaccaroPas encore d'évaluation
- Ulcers and Vesicles2Document24 pagesUlcers and Vesicles2Kelly MayerPas encore d'évaluation
- TrachomaDocument6 pagesTrachomaSpislgal PhilipPas encore d'évaluation
- Herpes Zoster (Shingles) : Jessie Mccary, MDDocument5 pagesHerpes Zoster (Shingles) : Jessie Mccary, MDtejinderatwork100% (2)
- AxnldhwDocument18 pagesAxnldhwHel DaPas encore d'évaluation
- Daftar PustakaDocument1 pageDaftar PustakaHel DaPas encore d'évaluation
- Print 2Document44 pagesPrint 2Hel DaPas encore d'évaluation
- AbstractDocument1 pageAbstractHel DaPas encore d'évaluation
- Classification and External Resources: Neurological ExaminationDocument40 pagesClassification and External Resources: Neurological ExaminationHel DaPas encore d'évaluation
- Draft: The Principles of Infection Prevention and ControlDocument36 pagesDraft: The Principles of Infection Prevention and Controlandrel davidPas encore d'évaluation
- Uterine Prolapse in A Primigravid Woman JournalDocument13 pagesUterine Prolapse in A Primigravid Woman JournalFadhlyanyPas encore d'évaluation
- Brochure Medicine PDFDocument12 pagesBrochure Medicine PDFJacklinePas encore d'évaluation
- II. Task 2: Write An Analytical Exposition TextDocument2 pagesII. Task 2: Write An Analytical Exposition TextYunika VandiaPas encore d'évaluation
- Preventing and Treating Bronchitis HDocument2 pagesPreventing and Treating Bronchitis HSinbad Alfin PelautPas encore d'évaluation
- Multimorbidity and Its Associated Risk Factors Among Adults in Northern Sudan: A Community-Based Cross-Sectional StudyDocument7 pagesMultimorbidity and Its Associated Risk Factors Among Adults in Northern Sudan: A Community-Based Cross-Sectional StudyOwais SaeedPas encore d'évaluation
- 2020 ESC Guidelines On Sports Cardiology and Exercise in Patients With Cardiovascular DiseaseDocument80 pages2020 ESC Guidelines On Sports Cardiology and Exercise in Patients With Cardiovascular DiseaseKlaraPas encore d'évaluation
- Eeg, PSG, Sleep DisordersDocument48 pagesEeg, PSG, Sleep DisordersIoana MunteanuPas encore d'évaluation
- Dialog Present Continous TenseDocument2 pagesDialog Present Continous TenseMessy100% (1)
- Ultimate MJDF Part 1Document89 pagesUltimate MJDF Part 1SueChen Tan75% (4)
- Tips To Increase Speed of AssessmentDocument6 pagesTips To Increase Speed of AssessmentEsmareldah Henry SiruePas encore d'évaluation
- Asthma Fullguideline 2009Document132 pagesAsthma Fullguideline 2009Lajwanti DesignersPas encore d'évaluation
- Diabetes Home Health RubricDocument13 pagesDiabetes Home Health Rubricapi-372924050Pas encore d'évaluation
- Craniectomia 3Document8 pagesCraniectomia 3Vlady78Pas encore d'évaluation
- Medtronic Earnings Presentation FY16Q4 FINALDocument21 pagesMedtronic Earnings Presentation FY16Q4 FINALmedtechyPas encore d'évaluation
- Holding Health Care AccountableDocument37 pagesHolding Health Care AccountableGulalayPas encore d'évaluation
- 1 - Introduction of CytopathologyDocument41 pages1 - Introduction of CytopathologyAyu Rizky Fitriawan AyuPas encore d'évaluation
- Concepts of DiseaseDocument55 pagesConcepts of DiseaseKailash NagarPas encore d'évaluation
- BCS Guidance On Workload For Cardiologists - Final March 2010Document9 pagesBCS Guidance On Workload For Cardiologists - Final March 2010Narendra KumarPas encore d'évaluation
- MEDS 1. Diabetic Retinopathy: Practice Essentials, Pathophysiology, EtiologyDocument14 pagesMEDS 1. Diabetic Retinopathy: Practice Essentials, Pathophysiology, EtiologyVivi DeviyanaPas encore d'évaluation
- PP-MIR-US-0477-1 Mirena Patient Brochure DigitalDocument13 pagesPP-MIR-US-0477-1 Mirena Patient Brochure DigitalimtariquePas encore d'évaluation
- Methodology and Project Design 4Document4 pagesMethodology and Project Design 4api-706947027Pas encore d'évaluation
- Management of A Case of Ventricular Bigeminy UsingDocument2 pagesManagement of A Case of Ventricular Bigeminy UsingAlfian AlfianPas encore d'évaluation
- Acute Viral Hepatitis: Jonathan WalaDocument49 pagesAcute Viral Hepatitis: Jonathan WalaAntony WaithakaPas encore d'évaluation
- LaQshya Quality Improvement Cycles Resource MaterialDocument344 pagesLaQshya Quality Improvement Cycles Resource Materialkparasher100% (1)
- Cellulitis CaseDocument15 pagesCellulitis CaseHarshini DonepudiPas encore d'évaluation
- Colonoscopy Instructions Using PegLyteDocument2 pagesColonoscopy Instructions Using PegLyteRomelia CampuzanoPas encore d'évaluation
- Patient Positioning (Sims, Orthopneic, Dorsal Recumbent) Guide (2020)Document28 pagesPatient Positioning (Sims, Orthopneic, Dorsal Recumbent) Guide (2020)JOSHUA DICHOSO100% (1)
- 09.Project-Hospital Management SystemDocument37 pages09.Project-Hospital Management Systemzahidrafique0% (1)
- BAB I SomatoformDocument3 pagesBAB I SomatoformDewiRekmawatiPradaswariPas encore d'évaluation