Académique Documents
Professionnel Documents
Culture Documents
Jurnal Pediatri
Transféré par
Aprilian Ayu Sita0 évaluation0% ont trouvé ce document utile (0 vote)
17 vues6 pagesJurnal dari paediatricaindonesiana.org
Copyright
© © All Rights Reserved
Formats disponibles
PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentJurnal dari paediatricaindonesiana.org
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
17 vues6 pagesJurnal Pediatri
Transféré par
Aprilian Ayu SitaJurnal dari paediatricaindonesiana.org
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 6
Paediatrica Indonesiana
VOLUME 54 NUMBER 2 March 2O11
Original Article
Paediatr Indones, Vol. 54, No. 2, March 2014 67
Nutritional status and physical activity of
childhood leukemia survivors
Conny Tanjung, Johannes Bondan Lukito, Prima Dyarti Meylani
Abstract
Background Acute lymphoblastic leukemia (ALL), the most
common malignancy of childhood, has an overall cure rate of
approximatelv oO'. lon,-term survivors of childhood All are
at increased risk for obesity and physical inactivity that may lead
to the development of diabetes, dyslipidemia, metabolic syndrome,
as well as cardiovascular diseases, and related mortality in the
vears followin, treatment.
Objective To evaluate the physical activity and the propensity
for developin, obesitv lon,er term in All survivors.
Methods This retrospective cohort study included all ALL
survivors from Pantai lndah Kapuk (PlK) Hospital. We assessed
their physical activity and nutritional status at the first time of
All dia,nosis and at the time of interview.
Results Subjects were 15 All survivors a,ed 7 to 21 vears. 1he
median follow up time was 6.1 vears (ran,e 3 to 1O vears). nlv
2 out of 15 survivors were overwei,ht and none were obese.
All survivors led a sedentarv lifestvle. Most female subjects
had increased BMl, thou,h most were not overwei,ht/obese.
Steroid therapy in the induction phase did not increase the risk
of developin, obesitv in All survivors.
Conclusion lon,-term survivors of childhood All do not meet
physical activity recommendations according to the CDC(Centers
for Disease Control). However, steroid therapv do not seem to
lead to overwei,ht/obesitv in All survivors. [Paediatr Indones.
2014;54:67-72.].
Keywords: acute lymphoblastic leukemia, survivors,
obesity, physical inactivity
From the Department of Pediatrics, Pantai Indah Kapuk Hospital, Jakarta,
lndonesia.
Reprint requests to: dr. Connv 1anjun,, Sp.A. RS Pantai lndah Kapuk.
Phone 6221.5ooO.911. lmail address: mfconnvtanjun,_vahoo.com.
T
he number of survivors of childhood
acute lymphoblastic leukemia (ALL) has
been steadily increasing with progressive
improvements in therapv. 1his expandin,
population of survivors mandates better characteriza-
tion of the lon,-term complications of treatment to
improve our understandin, of their future health risks.
Recent studies suggest that ALL survivors have an
increased prevalence of obesity and physical inactivity
and may be at risk of developing diabetes, dyslipidemia,
and metabolic syndrome that may contribute to the
development of cardiovascular diseases. 1hus it is
imperative to further studv this population.
1-1
Until now, there has been little data on the
nutritional and physical activity status of ALL
survivors in lndonesia. We aimed to evaluate the
physical activity of ALL survivors, their nutritional
status and assess for possible lon,-term effects of
steroid therapv as a potential cause of obesitv.
Methods
We conducted a retrospective cohort studv in the
Pediatric Ward of Pantai lndah Kapuk (PlK) Hospital,
Conny Tanjung et al: Nutritional status and physical activity of leukemia survivors
68 Paediatr Indones, Vol. 54, No. 2, March 2014
Jakarta from April to Julv 2O12 to evaluate the current
nutritional status, physical activity and the effect of
steroids as a potential cause of obesitv on All survivors.
All patients were treated between 2OOO - 2O1O, accordin,
to the All '97 Hon, Kon, (HK All 97) Protocol.
Wei,ht in kilo,rams was measured bv electronic
scale (SECA 727). Hei,ht in centimeters was
measured with a wall-mounted stadiometer. 1hese
two parameters were measured at the time of diagnosis,
during treatment, at the end of therapy, and at the time
of this studv. We used the CDC 2OOO ,rowth charts
for children over 5-vear-old. Nutritional status was
determined based on bodv wei,ht (BW) in relation
to body height (BH) and categorized according to
the Waterlow criteria for children over 5 vears old.
lor children under 5 vears of a,e, we used the cut-
off z-score from WH 2OO6. lf the result showed
overwei,ht (>1 SD) or BW/BH >1OO', we used
the bodv mass index (BMl) ,raphs for their a,e and sex.
Body mass index (BMI, kg/m
2
), was used as an indicator
of obesity according to Centers for Disease Control
(CDC) charts. 1hese patients were cate,orized as
overweight when BMI was above 85
th
- 91
th
percentile,
or obese if BMI 95
th
percentile.
5
For adult patients
(a,e >1o vears), the BMl was used to define wei,ht
cate,ories as follows: underwei,ht (BMl 1o.5),
normal wei,ht (BMl 1o.5 to 21.9), overwei,ht (BMl
25.O to 29.9), or obese (BMl ~3O).
1
Physical activity was assessed by asking, During
the past month, did you participate in any physical
activities or exercises such as running, calisthenics,
golf, gardening, bicycling, swimming, wheelchair
basketball, or walking for exercise? Participants
were then asked a series of six questions to quantify
the amount of time (number of days per week and
number of minutes per day) spent in moderate
or vi,orous phvsical activitv durin, a usual week.
Vigorous activities were defined as any activity causing
a lar,e increase in breathin, or heart rate. lxamples
provided by the surveyors included running, aerobics,
wheelchair basketball, and heavv vard work. Moderate
activities were defined as any activity causing small
increases in breathing or heart rate, including brisk
walking, bicycling, vacuuming, gardening, and manual
wheelchair operation. Participants were considered
to not meet CDC recommendations if they did not
report moderate-intensitv phvsical activities for at
least 3O min, ~5 davs in a week or vi,orous-intensitv
phvsical activitv for ~2O minutes per occasion ~3
davs per week.
4
Results
There were 42 children admitted to PIK Hospital with
a dia,nosis of acute lvmphoblastic leukemia (All).
f these, 2O children did not receive further therapv
because of parent refusal (15 patients) or failure to
achieve remission (5 patients). ne patient died one
vear after completin, the re,imen. 1he final studv
sample consisted of 21 All survivors, but six All
subjects were excluded because of incomplete data.
1he remainin, subjects consisted of 7 females and
o males. 1he median a,e at dia,nosis was 6.7 vears
(ran,e 2 to 15 vears) and the median a,e at the time
of interview was 13.1 vears (ran,e 7 to 21 vears). 1he
median time from dia,nosis to last assessment was 6.1
vears (ran,e 3 to 1O vears).
These subjects started induction chemotherapy
comprised of vincristine, ara C, leunase, daunorubicin,
cvclophosphamide, and hi,h-dose of intrathecal
methotrexate (M1X). All patients received intrave-
nous hi,h-dose M1X (5 ,/m
2
), prednisolone (6O m,/
m
2
/dav for 2o davs) in the induction phase 1 and
dexamethasone (1O m,/m
2
/dav for 21 davs) in the
re-induction phase. None of the subjects received
cranial irradiation. ln the maintenance phase,
subjects received mercaptopurine, methotrexate, and
dexamethasone orallv.
Subjects' nutritional status at the time of dia,-
nosis and at the time of study are summarized in Table
1. At diagnosis, five patients were underweight, two
patients were obese and three were overwei,ht. At
the time of this studv, this proportion chan,ed. At
the last assessment almost all survivors had good
nutritional status, none were obese, and onlv 2/15
patients fulfilled the criteria for overwei,ht.
None of the ALL survivors met the CDC
recommendations for physical activity, as no patients
regularly exercised 5 times per week or engaged
in vi,orous activitv 3 times per week. 1he a,e at
cancer dia,nosis did not modifv outcomes. Subjects
spent more than two hours in front of the television,
plavin, ,ames or surfin, the internet. nlv 5 survivors
en,a,ed in re,ular exercise for 3O minutes one or two
times per week (Table 2).
Conny Tanjung et al: Nutritional status and physical activity of leukemia survivors
Paediatr Indones, Vol. 54, No. 2, March 2014 69
have been proposed for this effect, including cranial
radiotherapy, growth hormone insufficiency, use of
corticosteroids and reduced energy expenditure.
6-9
1his sin,le-institution studv provides lon,itudi-
nal follow-up observations of wei,ht and hei,ht. We
observed that children who were younger at diagnosis
did not have greater likelihood of becoming over-
weight at the interview assessment (a median time of
6.1 vears after dia,nosis). ln contrast, Razzouk et al.
1
found a correlation of younger age to the likelihood of
becomin, obese. Patients who were underwei,ht at the
time of diagnosis had the largest increase in BMI, as
would have been expected with improvement in their
nutritional status after achieving complete remission
of their leukemia.
1
Figure 1. shows about the differences of BMI in the
boys and the girls survivors that were evaluated at the first
time of All dia,nosis and the last interview. 1he fi,ure
also shows the increasing trend of BMI among the girls,
that linked to the fat composition in the bodv.
Discussion
Acute lymphoblastic leukemia (ALL) is the most
common malignancy of childhood, accounting for
approximatelv 25' of all childhood cancers.
6
Since
the 196Os, the All cure rate in children has improved
dramaticallv, from less than 3O' toa current estimated
5-vear overall survival of oO-o6'. Reports on lon,-
term childhood ALL survivors have claimed that
obesitv is a common findin,.
7,o
Several explanations
Table 1. Subjects nutritional status
Nutritional status at study time
Number of
patients
Under weight Normal Over weight Obese
Age at study time, years
18
10 - 14
5 9
Gender
Female
Male
Nutritional status at diagnosis
Underweight
Normal
Overweight
Obese
2
8
5
7
8
5
5
3
2
1
-
-
-
1
-
1
-
-
1
8
3
6
6
5
3
3
1
-
-
2
1
1
-
1
-
1
-
-
-
-
-
-
-
-
-
Table 2. Subjects physical activity (according to CDC recommendation criteria)
Physical activity study time
Number of patients Moderate physical activity
(> 30 min for 5 days a
week)
Vigorous physical activity
(> 30 min for 3 days a
week)
Sedentary lifestyle
(watching TV/
computer for 2
hours)
Age at study time , years
18
1014
59
Gender
Female
Male
Nutritional status at
assessment
Underweight
Normal weight
Overweight
Obese
2
8
5
7
8
5
5
3
2
-
-
-
-
-
-
-
-
-
-
-
-
-
-
-
-
-
-
2
8
5
7
8
5
5
3
2
Conny Tanjung et al: Nutritional status and physical activity of leukemia survivors
70 Paediatr Indones, Vol. 54, No. 2, March 2014
Based on BW/BH assessments, we found that no
survivors fulfilled the criteria for obesitv. lurthermore,
onlv two survivors were overwei,ht. Similarlv, Jarfelt et
al. found no obese survivors in their study, but in their
studv 12/35 patients were overwei,ht.
7
Although we
found that almost all survivors had good nutritional
status, changes in BMI were evident in our study
population (Figure 1). The BMI is a potential clinical
marker for metabolic abnormalities. lnterpretation
of BMI in childhood and adolescents is not as
straightforward as in adults because of progressive
chan,es with ,rowth. lncreased total fat mass with
or without increased BMI has been described after
recoverv from mali,nancv.
7
Our results were contrary
to the findings of Nysom et al. who found a high BMI
at the follow up of Danish children and young adults
at a median time of 1O vears after dia,nosis.
1O
Other
studies have reported on the changes of body fat
composition after completion of therapv. 1he amount
of fat, fat-free mass, and fat distribution are more
important risk factors for predicting cardiovascular
diseases and non-insulin dependent diabetes mellitus
(NlDDM).
11
Unlike our male subjects, almost all females had
increased BMI, similar to the findings of Murphy et al.
who showed a tendency of increased fat mass in female
subjects.
3
Warner et al. also found that only female
survivors tended to be obese,
12
and Odame et al.
reported that female ALL survivors had significantly
higher BMI standard deviation scores than did other
patients who had been treated with chemotherapv.
13
It is unclear how gender affects the body composition
of children in remission from All.
Some reports have shown a correlation between
obesity and corticosteroid treatment applied during
the induction of remission. ne theorv is that durin,
glucocorticoid treatment, ALL patients have increased
energy intake and reduced energy expenditure while
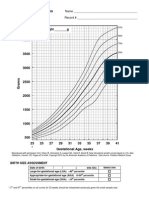
Figure 1. The BMI changes in ALL survivors (the BMI differences measured at the ALL diagnosis and at the
time of interview)
NAME
RECORD #
2 5 4 3 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20
26
24
22
20
18
16
14
12
kg/m
2
28
26
24
22
20
18
16
14
12
kg/m
2
30
32
34
BMI
BMI
AGE (YEARS)
13
15
17
19
21
23
25
27
13
15
17
19
21
23
25
27
29
31
33
35
Date Age Weight Stature BMI* Comments
95
90
85
75
50
10
25
5
2 5 4 3 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20
26
24
22
20
18
16
14
12
kg/m
2
28
26
24
22
20
18
16
14
12
kg/m
2
30
32
34
BMI
BMI
AGE (YEARS)
13
15
17
19
21
23
25
27
13
15
17
19
21
23
25
27
29
31
33
35
95
90
75
50
25
10
5
85
NAME
RECORD #
Date Age Weight Stature BMI* Comments
2 to 20 years: Boys
Body mass index-for-age percentiles
2 to 20 years: Girls
Body mass index-for-age percentiles
Published May 30, 2000 (modifed 10/16/00).
SOURCE: Developed by the National Centerfor Health Statistics in collaboration with
the National Center for Chronic Disease Prevention and Health Promotion (2000).
http://www.cdc.gov/growthcharts
Published May 30, 2000 (modifed 10/16/00).
SOURCE: Developed by the National Centerfor Health Statistics in collaboration with
the National Center for Chronic Disease Prevention and Health Promotion (2000).
http://www.cdc.gov/growthcharts
Conny Tanjung et al: Nutritional status and physical activity of leukemia survivors
Paediatr Indones, Vol. 54, No. 2, March 2014 71
continuing on their baseline physical activity and
that this effect continues after treatment ceases.
Other theories are that glucocorticoid treatment
causes increased adiposity by suppressing growth
hormone secretion or that it causes resistance to
leptin. Dexamethasone and prednisolone are two
,lucocorticoids usuallv used in All treatment.
Ahmed et al. reported that dexamethasone was 1o
times as potent as prednisolone in suppressin, short-
term growth and in increasin, bodv wei,ht.
11
After
adjustment for differences in dose, dexamethasone was
more potent thanprednisolone in increasing leptin, an
indicator of percenta,e of fat mass.
15
Unfortunately
we did not observe this correlation in our study, as a
longer follow up time would be required in order to
track subjects' final hei,ht. ur findin,s suggest that
further studies are needed to examine the longer term
effects of glucocorticoids on body composition in a
lar,er cohort for a lon,er time of observation.
Cranial irradiation, especiallv at doses of 2O
Gray or higher, has been reported to be a significant
predictor of risk for overweight/obesity in previous
investigations of childhood ALL, especially in females
treated before 5 vears of a,e.
2
Since none of our
subjects underwent cranial radiation, it may be one
reason whv none of our subjects was obese.
Although we had a relatively small number of
patients, this studv has several stren,ths. lirst, all
patients were treated at a single institution, using the
same treatment protocol, with a duration of follow up of
3 - 1O vears (mean 6.1 vears) permittin, us to determine
chan,es in BMl over time. Second, all hei,ht and
weight values used in the BMI determinations were
measured durin, routine clinic visits.
The second aim of this study was to evaluate the
phvsical activitv in our All survivors. ln the ,eneral
population, regular moderate intensity physical
activity has been shown to be protective against
osteoporosis, hvpertension, non-insulin dependent
diabetes mellitus, and cardiovascular diseases.
However, in 2OO1, onlv 15.1' of the All patients
were reported meeting the CDC recommendation
of ~ 3O min of moderate intensitv phvsical activitv
for ~ 5 davs per week or ~ 2O minutes of vi,orous
intensitv activitv for ~ 3 davs per week. Oiven that
ALL survivors are at higher risk than the general
population for several modifiable health problems, the
importance of participating in regular physical activity
is even ,reater for this ,roup.
17-19
The study of Florin et al. shows that ALL
survivors were more likely to not meet CDC
recommendations for physical activity [odds ratio
(R) 1.11, 95' Cl 1.32 to 1.57] and more likelv to
be inactive (R 1.71, 95' Cl 1.56 to 1.91) compared
to the ,eneral population.
4
A systematic review shows
that the physical fitness (as reflected by peak oxygen
uptake/VO
2
peak levels) of ALL survivors tend to
be reduced compared to healthv children. lmpaired
physical fitness leads to early fatigue dur ing physical
activities and can severely diminish the quality of
life of ALL survivors, which suggests the need for
these children to en,a,e in re,ular phvsical activities.
Furthermore, there are scientific indications that
exercise training improves the function of several
anti-cancer immune svstem components and can
attenuate tumor development.
16
In conclusion, we find no obesity in the childhood
All survivors in our institution. Steroid therapv in
the intensification phase seems to not increase the risk
of obesitv in All survivors. However, all survivors
are phvsicallv inactive. 1his level of inactivitv
likely increases their risk of cardiovascular diseases,
osteoporosis, and metabolic svndrome. lurther studies
of longer duration are needed to assess the factors
contributin, to these findin,s.
References
1. Razzouk Bl, Rose SR, Hon,en, S, Wallace D, Smeltzer MP,
Zacher M, et al. besitv in survivors of childhood acute
lvmphoblastic leukemia and lvmphoma. J Clin ncol. 2OO7,
25:11o3-9.
2. effin,er KC, Adams-Huet B, Victor RO, Church 1S, Snell
PG, Dunn AL, et al. lnsulin resistance and risk factors for
cardiovascular disease in young adult survivors of childhood
acute lvmphoblastic leukemia. J Clin ncol. 2OO9,27:369o-
7O1.
3. Murphv AJ, Wells JC, Williams Jl, lewtrell MS, Davies PS,
Webb DK. Bodv composition in children in remission from
acute lvmphoblastic leukemia. Am J Clin Nutr. 2OO6,o3:7O-
71.
1. llorin 1A, lrver Ol, Mivoshi 1, Weitzman M, Mertens AC,
Hudson MM, et al. Physical inactivity in adult survivors
of childhood acute lvmphoblastic leukemia: a report from
the Childhood Cancer Survivor Studv. Cancer lpidemiol
Conny Tanjung et al: Nutritional status and physical activity of leukemia survivors
72 Paediatr Indones, Vol. 54, No. 2, March 2014
Biomarkers Prev. 2OO7,16:1356-63.
5. Sjarif DR, Nasar SS, Devaera Y, 1anjun, C. Rekomendasi
lkatan Dokter Anak lndonesia. Asuhan Nutrisi Pediatrik.
BP lDAl, Jakarta, 2O11.
6. Modv R, li S, Dover DC, Sallan S, leisenrin, W, effun,er
KC, et al. 1wentv-five-vear follow-up amon, survivors of child-
hood acute lvmphoblastic leukemia: a report from the Child-
hood Cancer Survivor Studv. Blood. 2OOo,111:5515-23.
7. Jarfelt M, lannerin, B, Bosaeus l, Johannsson O, Bjarnason R.
Body composition in young adult survivors of childhood acute
lvmphoblastic leukaemia. lur J lndocrinol. 2OO5:153:o1-9.
o. Janiszewski PM, effin,er KC, Church 1S, Dunn Al,
Eshelman DA, Victor RG, et al. Abdominal obesity, liver
fat, and muscle composition in survivors of childhood
acute lvmphoblastic leukemia. J Clin lndocrinol Metab.
2OO7,92:3o16-21.
9. Ro,ers PC, Meacham lR, effin,er KC, Henrv DW, lan,e
BJ. besitv in pediatric oncolo,v. Pediatr Blood Cancer.
2OO5,15:oo1-91.
1O. Nvsom K, Holm K, Michaelsen Kl, Hertz H, Muller J,
Mol,aard C. De,ree of fatness after treatment for acute
lvmphoblastic leukemia in childhood. J Clin lndocrinol
Metab. 1999,o1:1591-6.
11. Neville KA, Cohn RJ, Steinbeck KS, Johnston K, Walker Jl.
Hyperinsulinemia, impaired glucose tolerance, and diabetes
mellitus in survivors of childhood cancer: prevalence and
risk factors. J Clin lndocrinol Metab. 2OO6,91:11O1-7.
12. Warner J1, lvans WD, Webb DK, Ore,orv JW. Bodv
composition of lon,-term survivors of acute lvmphoblastic
leukemia. Med Pediatr ncol. 2OO2,3o:165-72.
13. dame l, Reillv JJ, Oibson Bl, Donaldson MD. Patterns
of obesity in boys and girls after treatment for acute
lvmphoblastic leukaemia. Arch Dis Child. 1991,71:117-9.
11. Ahmed Sl, 1ucker P, Mushtaq 1, Wallace AM, Williams DM,
Hu,hes lA. Short-term effects on linear ,rowth and bone
turnover in children randomized to receive prednisolone or
dexamethasone. Clin lndocrinol (xf). 2OO2,57:1o5-91.
15. Wallace AM, 1ucker P, Williams DM, Hu,hes lA, Ahmed
Sl. Short-term effects of prednisolone and dexamethasone on
circulatin, concentrations of leptin and sex hormone-bindin,
globulin in children being treated for acute lymphoblastic
leukaemia. Clin lndocrinol (xf) 2OO3,5o:77O-6.
16. van Brussel M, 1akken 1, lucia A, van der Net J, Helders
PJ. ls phvsical fitness decreased in survivors of childhood
leukemia' A svstematic review. leukemia. 2OO5,19:13-7.
17. World Cancer Research lund/American lnstitute for
Cancer Research. lood, Nutrition, Phvsical Activitv, and
the Prevention of Cancer: a Olobal Perspective. AlCR,
Washin,ton, DC: 2OO7.
1o. Centers for Disease Control and Prevention. Phvsical activitv
for evervone. |cited June o 2O12]. Available from: http://
www.cdc.,ov/phvsicalactivitv/evervone/,uidelines.
19. U.S. Department of Health c Human Services. Active
children and adolescents. Phvsical activitv ,uidelines for
Americans. |cited June o 2O12]. Available from: http://www.
health.,ov/pa,uidelines/,uidelines.
Vous aimerez peut-être aussi
- Print Jurnal 1Document1 pagePrint Jurnal 1fadhlialbaniPas encore d'évaluation
- Tumor Lysis Syndrome OLDocument37 pagesTumor Lysis Syndrome OLfadhlialbaniPas encore d'évaluation
- 0-DM Problem Chart 2Document1 page0-DM Problem Chart 2fadhlialbaniPas encore d'évaluation
- Mellits and Cheek FormulaDocument5 pagesMellits and Cheek FormulafadhlialbaniPas encore d'évaluation
- Pathophysiology of Tethered Cord Syndrome and SimilarDocument10 pagesPathophysiology of Tethered Cord Syndrome and SimilarfadhlialbaniPas encore d'évaluation
- MRI CorrelateDocument7 pagesMRI CorrelatefadhlialbaniPas encore d'évaluation
- Altered Iron Metabolism in HIV Infection - Mechanisms, Possible Consequences, and Proposals For Management.Document1 pageAltered Iron Metabolism in HIV Infection - Mechanisms, Possible Consequences, and Proposals For Management.fadhlialbaniPas encore d'évaluation
- 7 - Quality of Life, Depressed Mood, and Self-Esteem in Adolescents WithDocument6 pages7 - Quality of Life, Depressed Mood, and Self-Esteem in Adolescents WithfadhlialbaniPas encore d'évaluation
- Infantile Spasm - EmedicineDocument13 pagesInfantile Spasm - EmedicinefadhlialbaniPas encore d'évaluation
- Pediatrics-2008-Inattention, Hyperactivity, and School Performance in School Age Children With Complex CHDDocument11 pagesPediatrics-2008-Inattention, Hyperactivity, and School Performance in School Age Children With Complex CHDfadhlialbaniPas encore d'évaluation
- 1 - Psychological Aspects in Children and Adolescent With Congenital Heart Disease and Their ParentsDocument18 pages1 - Psychological Aspects in Children and Adolescent With Congenital Heart Disease and Their ParentsfadhlialbaniPas encore d'évaluation
- Infantile Spasms - Pediatric NeurolDocument1 pageInfantile Spasms - Pediatric NeurolfadhlialbaniPas encore d'évaluation
- Pediatrics-1993 - Psychosocial Risks of Chronic Health Conditions in Childhoentod and AdolescDocument5 pagesPediatrics-1993 - Psychosocial Risks of Chronic Health Conditions in Childhoentod and AdolescfadhlialbaniPas encore d'évaluation
- The Impact of Severe Congenital Heart Disease On Physical and Psychosocial Functioning in AdolescentsDocument7 pagesThe Impact of Severe Congenital Heart Disease On Physical and Psychosocial Functioning in AdolescentsfadhlialbaniPas encore d'évaluation
- Transposition of The Great Arteries: What Is It?Document3 pagesTransposition of The Great Arteries: What Is It?fadhlialbaniPas encore d'évaluation
- Evaluasi Anak Dengan Ambigous GenitaliaDocument12 pagesEvaluasi Anak Dengan Ambigous GenitaliafadhlialbaniPas encore d'évaluation
- Pathogenesis of Encephalitis BookDocument19 pagesPathogenesis of Encephalitis BookfadhlialbaniPas encore d'évaluation
- Infantile Spasms - MenkesDocument4 pagesInfantile Spasms - MenkesfadhlialbaniPas encore d'évaluation
- Management of Elevated Serum Ferritin LevelsDocument2 pagesManagement of Elevated Serum Ferritin LevelsfadhlialbaniPas encore d'évaluation
- Infantile Spasm - EmedicineDocument13 pagesInfantile Spasm - EmedicinefadhlialbaniPas encore d'évaluation
- Evaluation of Risk Factors For Severe PneumoniaDocument8 pagesEvaluation of Risk Factors For Severe PneumoniafadhlialbaniPas encore d'évaluation
- Early Developmental Delays - A Cross Validation StudyDocument5 pagesEarly Developmental Delays - A Cross Validation StudyfadhlialbaniPas encore d'évaluation
- WHO HIV Clinical Staging GuidelinesDocument49 pagesWHO HIV Clinical Staging Guidelinesdonovandube8235Pas encore d'évaluation
- Growthcurves Gestational AgeDocument4 pagesGrowthcurves Gestational AgefadhlialbaniPas encore d'évaluation
- Guidelines American Academy of Neurology 2011Document4 pagesGuidelines American Academy of Neurology 2011fadhlialbaniPas encore d'évaluation
- Treatment Guidelines For GuillainDocument15 pagesTreatment Guidelines For GuillainfadhlialbaniPas encore d'évaluation
- Etiology Malnutrisi HIVDocument8 pagesEtiology Malnutrisi HIVfadhlialbaniPas encore d'évaluation
- Prevalence of Undetected Developmental Delays in Iranian ChildrenDocument10 pagesPrevalence of Undetected Developmental Delays in Iranian ChildrenfadhlialbaniPas encore d'évaluation
- Altered Iron Metabolism in HIV Infection - Mechanisms, Possible Consequences, and Proposals For Management.Document1 pageAltered Iron Metabolism in HIV Infection - Mechanisms, Possible Consequences, and Proposals For Management.fadhlialbaniPas encore d'évaluation
- Royals - LordeDocument14 pagesRoyals - LordefadhlialbaniPas encore d'évaluation
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (890)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (587)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (265)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2219)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (119)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)