Académique Documents
Professionnel Documents
Culture Documents
P CPL
Transféré par
Jean Florencondia0 évaluation0% ont trouvé ce document utile (0 vote)
462 vues10 pagesThis document discusses three case histories related to glaucoma treatment and medication side effects:
1. A man being treated for glaucoma with pilocarpine drops experienced a drop in eye pressure but also initial brow aches and dimmed vision as side effects.
2. A man being treated for glaucoma with echothiophate drops developed diarrhea as a side effect. He later died from accidental organophosphate poisoning from pesticide exposure, which may have had additive effects due to his glaucoma medication.
3. A man being treated for glaucoma with timolol and echothiophate experienced asthma attacks as a possible side effect. During later surgery, he
Description originale:
asd
Titre original
p.cpl
Copyright
© © All Rights Reserved
Formats disponibles
PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentThis document discusses three case histories related to glaucoma treatment and medication side effects:
1. A man being treated for glaucoma with pilocarpine drops experienced a drop in eye pressure but also initial brow aches and dimmed vision as side effects.
2. A man being treated for glaucoma with echothiophate drops developed diarrhea as a side effect. He later died from accidental organophosphate poisoning from pesticide exposure, which may have had additive effects due to his glaucoma medication.
3. A man being treated for glaucoma with timolol and echothiophate experienced asthma attacks as a possible side effect. During later surgery, he
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
462 vues10 pagesP CPL
Transféré par
Jean FlorencondiaThis document discusses three case histories related to glaucoma treatment and medication side effects:
1. A man being treated for glaucoma with pilocarpine drops experienced a drop in eye pressure but also initial brow aches and dimmed vision as side effects.
2. A man being treated for glaucoma with echothiophate drops developed diarrhea as a side effect. He later died from accidental organophosphate poisoning from pesticide exposure, which may have had additive effects due to his glaucoma medication.
3. A man being treated for glaucoma with timolol and echothiophate experienced asthma attacks as a possible side effect. During later surgery, he
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 10
Case History #1: Pilocarpine
Local 1% pilocarpine was ordered by instillation
every six hours for a 64 year old man with chronic,
open-angle glaucoma. His vision had been declining
for a number of years, although he was not really
aware of it. The intraocular pressure (IOP) dropped
from 35 mm Hg to 18 mm Hg (normal pressure limits
are 10 to 22 mm Hg) following instillation. He
complained of brow ache for the first few days and
some dimness of vision, although visual acuity was
not altered. He also wonders why he should use the
drug now as he has already lost a lot of sight.
Questions:
Why (and how) does pilocarpine lower the IOP?
Why are there side effects of brow ache and dimness of
vision?
What other side effects may be associated with
pilocarpine?
How [and why] would you encourage compliance?
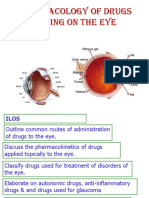
What is glaucoma?
BLOCKED
OR FAULTY
Open-angle Glaucoma
Mechanism of action pilocarpine in OAG
Pilocarpine lowers IOP
by increasing the fluid
outflow
Pilocarpine 1% solution
Well absorbed by the cornea and released slowly in to
the aqueous humor
Applied topically in the eye
Produces a reduction in IOP that starts after one hour
and lasts for 4 - 8 hours.
Administered every 6 hours to ensure good reduction
in IOP
Increases outflow by stimulating the ciliary muscles,
pulling traction on the scleral spur and the trabecular
mesh work
Side effects:
Temporary irritation/burning/stinging of the eye
temporary blurred vision
poor vision in dim light
headache, or brow ache
Diarrhea
Diaphoresis
Miosis
Nausea
Urinary urgency
Other side effects
Case History #2:Organophosphates
A forty-eight year old man required the use of
echothiophate by instillation twice daily for the
control of his glaucoma. After about two weeks on the
drops he developed a definite change in bowel habits
consisting of a mild diarrhea. He consulted his
internist about this, who, after a presumably thorough
history, ordered a complete GI series which was
negative. He then did a proctoscopy, a sigmoidoscopy,
a test for occult blood in the stools, stool cultures, and
stool smears. All were negative.
Case History #2:Organophosphates
About one month later the patient went out to
spray his orchard with parathion. He was found dead
two hours later by his wife under a peach tree in full
bloom. The death was said to be due to the careless
handling of a dangerous insecticide.
Questions:
What is echothiophate?
What about the diarrhea? What other problems
may he have experienced?
What factors may have been responsible for the
patient's death?
Explain how parathion poisoning should be
treated.
Echothiophate iodide
A long-acting cholinesterase inhibitor for
topical use
Approx.100 hours duration of action
Depresses both plasma and erythrocyte
cholinesterase levels in most patients
after a few weeks of eyedrop therapy
Echothiophate iodide
for ophthalmic solution
enhances the effect of endogenously liberated Ach in
iris, ciliary muscle, and other parasympathetically
innervated structures of the eye causing;
Miosis
increase in facility of outflow of aqueous humor
fall in intraocular pressure, and
potentiation of accommodation
Adverse effects of ophthalmic
solution of echothiophate
Stinging, burning
Lacrimation
Lid muscle twitching
Conjunctival and ciliary redness
Browache
Induced myopia with visual blurring
Iritis or uveitis
GI effects of Echothiophate
Attributed to muscarinic effects in the GIT
Increases secretory and motor activity in the gut
Increased peristaltic activity
diarrhea
To avoid systemic effects;
Digital compression of the
nasolacrimal ducts for a
minute or two following
instillation to minimize
drainage into the nasal
chamber
Hands should be washed
following instillation
Other problems related to
muscarinic toxicity
Miosis
Salivation
Sweating
Bronchial constriction
Cognitive disturbances
Convulsions
Coma
Echothiophate and Parathion
Both are cholinesterase inhibitors
Additive systemic effects of both drugs could have
been the cause of patients death
Possibly from absorption of the pesticide through the
respiratory tract or skin
Precaution
During periods of exposure to such pesticides, advise
patient to;
wear respiratory masks
wash hand frequently
change clothing
Treatment of organophosphate
poisoning
Airway control and adequate oxygenation
Remove all clothing and gently cleanse patients
suspected of organophosphate exposure with soap and
water
organophosphates are hydrolyzed readily in aqueous
solutions with a high pH
Irrigate the eyes of patients
isotonic sodium chloride solution or lactated Ringer's
solution
For health care worker
In decontaminating the patient;
Use personal protective equipment such as neoprene
gloves and gowns because hydrocarbons can penetrate
nonpolar substances such as latex and vinyl
Use charcoal cartridge masks for respiratory protection
Drugs for organophosphate poisoning
Atropine IV/IM
Competitive inhibitor at autonomic postganglionic
cholinergic receptors, including receptors found in GI
and pulmonary smooth muscle, exocrine glands, heart,
and eye
Purpose: reduce respiratory secretion, thus improve
oxygenation
Pralidoxime (2-PAM)
Benzodiazepines
Pralidoxime (2-PAM)
2-PAM (2-pyridine aldoxime methyl chloride)
Antidote for OP poisoning by reactivating the
phosphorylated AChE
2-PAM attaches to the site where the cholinesterase
inhibitor has attached to and blocked cholinesterase
2-PAM then attaches to the cholinesterase inhibitor and
removes it from cholinesterase, allowing the enzyme to
work normally again
sometimes referred to as regeneration of cholinesterase
AchE action
AchE inhibitors action
Organophosphate
Possibilities after cholinesterase inhibition
1.Hydrolyze to
original state (slow)
reversibility of
enzyme inhibition
2. Regenerate with an oxime (fast)
3. Age (cannot regenerate)
How 2-PAM works?
Pralidoxime (2-PAM)
Prevent aging of AChE and reverse muscle paralysis
with OP poisoning
Not effective once the OP compound has bound AChE
irreversibly (aged)
Should be administered within 48 h of OP poisoning
Pralidoxime (2-PAM)
Does not significantly relieve depression of respiratory
center or decrease muscarinic effects of AChE
poisoning
administer atropine concomitantly to block these effects
Signs of atropinization might occur earlier with
addition of 2-PAM to treatment regimen
2-PAM administration is not indicated for carbamate
exposure since no aging occurs
Case History #3:
Timolol and EchothiophateIodide
Two severe episodes of acute asthma prompted
evaluation of a 63-year old man in the pulmonary clinic.
The patient had had symptoms of atopic asthma up to the
age of 20 but had remained asymptomatic since. Three
weeks before he experienced the first asthmatic attack, he
had begun using Timoptic (timolol) eye drops, O.5%
solution, gtts i o.u., bid, for treatment of open-angle
glaucoma. Phospholine iodide (Echothiophate iodide),
0.05% solution, gtts i o.u., bid, was substituted for timolol
resulting in adequate control of the glaucoma but the
patient suffered another asthmatic attack 6 weeks later.
Case History #3:
Timolol and Echothiophate Iodide
On the day following this last asthmatic attack he was
involved in an auto accident and went into shock from
blood loss. He was hospitalized and taken to surgery for
wound repair. After anesthesia was instituted,
succinylcholine was administered intravenously to secure
relaxation of the laryngeal and pharyngeal muscles for
intubation. The patient become apneic and remained so
for the next eight hours. The anesthetist noted this
promptly and instituted artificial respiration which he
continued for the rest of the day. In the meantime, the
wounds were repaired and the surgical shock was
effectively treated by appropriate measures. Recovery was
uneventful.
Questions
1. What is timolol and what is it's mechanism of action?
2. Could the asthmatic attacks be associated with the use
of either of the ophthalmic solutions used by the
patient?
3. Why the prolonged apnea in this case?
4.Could the apnea have been treated more
expeditiously?
Timolol
A non-selective beta-receptor blocker
No partial agonist activity
No local anesthetic action
Elimination half-life is 4-5 hours
Applied topically in the eye for the treatment of
glaucoma
Lowers IOP by decreasing aqueous secretion from the
ciliary epithelium
Secretion of the aqueous humor
Mode of Action of Timolol in Medical
Treatment of Glaucoma
This invention demonstrates that in contrast to
previously believed c-AMP-mediated mechanism,
timolol, the widely-used therapeutic agent for
glaucoma, acts by specifically blocking either the
sodium-proton or the bicarbonate-chloride
exchanger. Both of these mechanisms are considered
critical in supporting the formation of aqueous humor
of the eye.
http://upenn.technologypublisher.com/technology/3995
Strategies for the treatment of
Glaucoma
Reduction of aqueous humor production
Beta blockers such as timolol, betaxolol, carteolol,
levobunolol, metipranol
Alpha-2 selective agonist apraclonidine, brimonidine
Diuretics CAIs (oral/topical)
Acetazolamide. Dichlorphenamide, methazolamide (oral)
Dorzolamide, brinzolamide (topical)
Enhancement of aqueous humor outflow
Strategies for the treatment of
Glaucoma
Reduction of aqueous humor production
Enhancement of aqueous humor outflow
Cholinergics pilocarpine, carbachol, physostigmine,
echothiophate, demecarium
Non-selective alpha agonist epinephrine, dipiverin
Prostaglandins latanaprost, bimatoprost, travaprost,
unoprostone
Immunohistochemical data have shown that the
IOP reduction with topical PGF2-alpha is associated
with a reduction of collagens within the
uveoscleral outflow pathway. The ciliary body
contains several prostaglandin receptors (mainly FP
and EP2 receptors), whose activation seems to
stimulate a second messenger cascade for
metalloproteinases synthesis (metalloproteinases are
enzymes involved in extracellular matrix remodeling).
Latanoprost ophthalmic solution in the treatment of open angle
glaucoma or raised intraocular pressure: a review
EFFECTS OF BETA BLOCKERS
In the eye
Reduce intraocular pressure
Used therapeutically in glaucoma
In the respiratory tract
Increase airway resistance (beta-2)
Selective beta-1 blockers do not exhibit this effect
Atenolol is the prototype drug of selective beta-1 blockers
Should be avoided by patients with COPD/asthma
Endocrine effects Beta blockers
Non-selective beta blockers are contraindicated in
diabetic patients
This is because catecholamines utilize the beta
2
receptor to
promote glycogenolysis and mobilize glucose
Selective beta
1
blockers should be used with caution
in patients with diabetes
In addition all beta blockers mask the tachycardia
associated with hypoglycemia
As a result, the diabetic patient is deprived of one of the
earliest physiologic responses to hypoglycemia
EFFECTS OF BETA BLOCKERS
Not related to beta blockade
Intrinsic sympathomimetic activity
Observed in partial beta agonist (e.g. Pindolol)
Sometimes desired to prevent the untoward effects like
exacerbation of asthma or excessive bradycardia
Local anesthetic action (membrane-stabilizing action)
Due to blockade of sodium channel
Not used topically in the eye
Sotalol (non-selective beta blocker) lacks local anesthetic
action
Prolonged Apnea.
Echothiophate potentiated the effects of
succinylcholine
Relaxation of the respiratory muscle
Respiratory failure
Deficiency in plasma cholinesterase due to blood loss
Case Study # 4
A 46-year-old woman sees her physician because
of palpitations and headaches. She enjoyed good
health until 1 year ago when spells of cardiac
palpitations began. These became more severe and
were eventually accompanied by throbbing headaches
and drenching sweats. Physical examination reveals a
blood pressure of 150/90 mm Hg and heart rate of 88
bpm.
During the physical examination, palpation of the
abdomen elicits a sudden and typical episode, with a
rise in blood pressure to 210/120 mm Hg, heart rate to
122 bpm, and facial pallor. This is accompanied by
severe headache and profuse sweating.
What is the likely cause of her episodes?
What caused the blood pressure and heart rate to rise
so high during the examination?
What treatments might help this patient?
Pheochromocytoma
A tumor of the adrenal medulla or sympathetic
ganglion cells
Tumor secretes catecholamines especially NE and EPI
Diagnosis:
Elevated plasma and urinary level of catecholamines
Imaging CT scan and MRI using radiomarkers such as
MIBG (
131
I-meta-iodobenzylguanidine)
Release of stored catecholamines may be spontaneous,
but it can be triggered by physical pressure, chemical
stimulation
Common symptoms in
pheochromocytoma
Hypertension
Headache
Sweating
Other symptoms include;
heart palpitations
Pallor
shortness of breath
Weakness
symptoms that resemble panic attacks
Treatment
Nitroprusside and alpha blockers
For hypertension during operative manipulation of
pheochromocytoma
Phenoxybenzamine
Clinically useful in the management of
pheochromocytoma
Useful in the chronic treatment of inoperable or
metastatic pheochromocytoma
Metyrosine
Inhibits tyrosine hydroxylase
SELECTIVE ALPHA
1
-ANTAGONISTS
Prazosin and Prazosin analogs
Terazosin, Doxazosin, Trimazosin
Reversible antagonists
CARDIOVASCULAR EFFECTS
Relaxes arterial and venous smooth muscle as
well as nonvascular smooth muscle.
Decreases peripheral vascular resistance and
venous return.
Decreases systemic arterial blood pressure
without a significant increase in heart rate.
SELECTIVE ALPHA
1
-ANTAGONISTS
OTHER EFFECTS
Miosis and nasal stuffiness
Decrease resistance to the flow of urine
SELECTIVE ALPHA
1
-ANTAGONISTS
CLINICAL USES
Treatment of Hypertension
Treatment of urinary retention due to
prostatic hyperplasia (Benign prostatic
hypertrophy)
SIDE EFFECTS
Orthostatic hypotension
Nasal stuffiness
Inhibition of ejaculation
Syncope - Prazosin
SELECTIVE ALPHA
1
-ANTAGONISTS
Prazosin and Prazosin analogs (terazosin, doxazosin,
trimazosin)
NON-SELECTIVE ALPHA BLOCKERS
Phentolamine
Competitive antagonist
Used in erectile dysfunction in combination
with papaverine (a non-specific smooth muscle
relaxant)
Phenoxybenzamine
Irreversibly blocks alpha receptors
Blocks H1, Ach, and SE receptors as well as alpha
receptors
Used clinically in pheochromocytoma
Other uses of alpha blockers
In peripheral vascular disease
Ocassionally , in Raynauds phenomenon
Chronic hypertension*
Hypertensive emergencies
Prazosin family
* With limited application
SOME ADVERSE EFFECTS COMMONLY
OBSERVED WITH ALPHA BLOCKERS
Orthostatic hypotension
Tachycardia
Vertigo
Sexual dysfunction
Vous aimerez peut-être aussi
- Case History 3Document10 pagesCase History 3Faith Dy NavalesPas encore d'évaluation
- Induction AgentsDocument100 pagesInduction AgentsSulfikar TknPas encore d'évaluation
- AEA - Ambulance Emergency Assistant - ProtocolsDocument12 pagesAEA - Ambulance Emergency Assistant - ProtocolsM Gavin100% (4)
- Tablet FriabilityDocument25 pagesTablet FriabilityJean Florencondia67% (3)
- Design 7 Research - Industrial ParkDocument41 pagesDesign 7 Research - Industrial ParkNur Sittie RufaidahPas encore d'évaluation
- Introduction To Electricity & Magnetism: QHSE-HIV-Level 2 Rev. Date: 30 Jan 2007Document30 pagesIntroduction To Electricity & Magnetism: QHSE-HIV-Level 2 Rev. Date: 30 Jan 2007Schields PedroPas encore d'évaluation
- General Radiotelephony Operator's Certificate ExaminationDocument5 pagesGeneral Radiotelephony Operator's Certificate Examinationjanine Goncalves100% (1)
- Case Study - Parkinson'S Disease: Clinical Pharmacy & Therapeutics 1Document13 pagesCase Study - Parkinson'S Disease: Clinical Pharmacy & Therapeutics 1Jenesis Cairo CuaresmaPas encore d'évaluation
- Pilot - PPL To CPL (155 Hours)Document1 pagePilot - PPL To CPL (155 Hours)Erwin Dave M. DahaoPas encore d'évaluation
- Introduction To Electricity and MagnetismDocument34 pagesIntroduction To Electricity and MagnetismFaraiFrancisZawairaPas encore d'évaluation
- CS3 Ocular PharmacologyDocument47 pagesCS3 Ocular PharmacologyؤيؤييسيPas encore d'évaluation
- EchothiophateDocument5 pagesEchothiophaterarasPas encore d'évaluation
- Anti GlaucomadrugsDocument31 pagesAnti GlaucomadrugsAshu KhanPas encore d'évaluation
- 1 Drugs Acting On The Eye - OkeDocument42 pages1 Drugs Acting On The Eye - OkeSintia AyuningsihPas encore d'évaluation
- Cholinergic Antagonists: DR - Ch. Shanmukha Sai RaghavDocument12 pagesCholinergic Antagonists: DR - Ch. Shanmukha Sai RaghavShanmukh SaiPas encore d'évaluation
- Dr. Ita - Farmakologi 1Document54 pagesDr. Ita - Farmakologi 1Ivo AfianiPas encore d'évaluation
- Topical Medication For GlaucomaDocument2 pagesTopical Medication For GlaucomaEddie LimPas encore d'évaluation
- Anti-Glaucoma Drugs (Ocular Hypotensive Drugs)Document24 pagesAnti-Glaucoma Drugs (Ocular Hypotensive Drugs)aamer niaziPas encore d'évaluation
- Emergency Room DrugsDocument20 pagesEmergency Room DrugstsikiPas encore d'évaluation
- BNS 200 Drugs and The EyeDocument36 pagesBNS 200 Drugs and The EyeAnthony MoepengPas encore d'évaluation
- Mydrin - P Ophthalmic SolutionDocument4 pagesMydrin - P Ophthalmic SolutionWu KathyPas encore d'évaluation
- Cases: Patient HistoryDocument8 pagesCases: Patient HistoryMohd HarizPas encore d'évaluation
- Case Studies PharmacologyDocument6 pagesCase Studies PharmacologyZaigham HammadPas encore d'évaluation
- Glaucoma and CataractDocument30 pagesGlaucoma and CataractJayselle ArviePas encore d'évaluation
- Local Anesthesia and Concious SedationDocument43 pagesLocal Anesthesia and Concious Sedationpawi18Pas encore d'évaluation
- GLUACOMADocument43 pagesGLUACOMAJoanna RachelPas encore d'évaluation
- Drug Therapy of Glaucoma 21.4.21Document29 pagesDrug Therapy of Glaucoma 21.4.21Beena ShajimonPas encore d'évaluation
- Medical Management - Glaucoma AppraochDocument73 pagesMedical Management - Glaucoma AppraochChickooTinaPas encore d'évaluation
- Guia Pequeños ArtesanalesDocument20 pagesGuia Pequeños ArtesanalesLaura TapiaPas encore d'évaluation
- Sialogogues & Anti SailogoguesDocument43 pagesSialogogues & Anti SailogoguesTavleen KaurPas encore d'évaluation
- Management Guidelines of Common PoisioningDocument52 pagesManagement Guidelines of Common PoisioningshravaniPas encore d'évaluation
- Organophosphate Poisoning 2Document12 pagesOrganophosphate Poisoning 2Diana MurguiaPas encore d'évaluation
- Hesi RN Med Surg 2020 Study Guide Review and Test BankDocument5 pagesHesi RN Med Surg 2020 Study Guide Review and Test BankJoseph Post100% (30)
- Pharmacotherapy of GlaucomaDocument15 pagesPharmacotherapy of Glaucomaمحمد فضل Fadhol Romdhoni100% (1)
- Drugs Used For GlaucomaDocument40 pagesDrugs Used For GlaucomaAgust SalimPas encore d'évaluation
- GLAUCOMA FinalDocument3 pagesGLAUCOMA FinalplethoraldorkPas encore d'évaluation
- Glaucoma 17.04.2021Document34 pagesGlaucoma 17.04.2021rufino tonyPas encore d'évaluation
- About 70% of All Sensory Information Reaches The Brain Through The EyesDocument127 pagesAbout 70% of All Sensory Information Reaches The Brain Through The Eyesjoan olantePas encore d'évaluation
- Glaucoma Medications: What We Have, Where We'Re GoingDocument65 pagesGlaucoma Medications: What We Have, Where We'Re Goingmero1983Pas encore d'évaluation
- Cycloplegic Drugs - Copy-1Document33 pagesCycloplegic Drugs - Copy-1devPas encore d'évaluation
- GlaucomeaDocument21 pagesGlaucomeamalathiPas encore d'évaluation
- Anaesthesia For Eye Surgery 1208455650159329 8 (2) .PPTDSDDocument32 pagesAnaesthesia For Eye Surgery 1208455650159329 8 (2) .PPTDSDfariz_maulana88_9890Pas encore d'évaluation
- 100 - Glaucoma - PharmacologyDocument17 pages100 - Glaucoma - PharmacologywidyastutiPas encore d'évaluation
- Study Guide Ch.14Document6 pagesStudy Guide Ch.14Draquillany ShieldsPas encore d'évaluation
- лекция №3Document88 pagesлекция №3THE TOXICPas encore d'évaluation
- Case ReportDocument7 pagesCase ReportJeel GaralaPas encore d'évaluation
- Welcome: Khartoum Eye Teaching HospitalDocument31 pagesWelcome: Khartoum Eye Teaching HospitalDoaa SaifPas encore d'évaluation
- Articaine (Septocaine) : Mu-Opioid Receptors Are in A Family of G-Protein Coupled ReceptorsDocument30 pagesArticaine (Septocaine) : Mu-Opioid Receptors Are in A Family of G-Protein Coupled ReceptorsphamnhuchauphuongPas encore d'évaluation
- Glaucoma 191024141130Document25 pagesGlaucoma 191024141130Broz100% (1)
- AnticholinergicsDocument33 pagesAnticholinergicspramod bhaleraoPas encore d'évaluation
- Primary Angle Closure GlaucomaDocument39 pagesPrimary Angle Closure GlaucomaMaria ShafiqPas encore d'évaluation
- Current Management Guidline in Organophosphors Poisoning: DR - Surendra Khosya Guided by Dr. S.R Meena Dr. Meenaxi ShardaDocument28 pagesCurrent Management Guidline in Organophosphors Poisoning: DR - Surendra Khosya Guided by Dr. S.R Meena Dr. Meenaxi ShardasurendrakhosyaPas encore d'évaluation
- ETHAMBUTOLDocument11 pagesETHAMBUTOLIrbasMantiniSyaifulPas encore d'évaluation
- 9 Glaucoma ManagementDocument44 pages9 Glaucoma ManagementMarshet GetePas encore d'évaluation
- Licence PA1339-017-002 01052020123923Document9 pagesLicence PA1339-017-002 01052020123923doctorsteve212Pas encore d'évaluation
- Recent Advances Glaucoma ImplantsDocument5 pagesRecent Advances Glaucoma ImplantsAnumeha JindalPas encore d'évaluation
- Balanced Salt SolutionDocument36 pagesBalanced Salt Solutionnaili nsnPas encore d'évaluation
- Timolol Maleate Pilocarpine HCLDocument21 pagesTimolol Maleate Pilocarpine HCLapi-414913553100% (1)
- Diclofenac Sodium Ophthalmic Solution, 0.1%: CL NaocchDocument2 pagesDiclofenac Sodium Ophthalmic Solution, 0.1%: CL NaocchBechchar HichamPas encore d'évaluation
- Acute Angle-Closure Glaucoma Treatment & ManagementDocument4 pagesAcute Angle-Closure Glaucoma Treatment & ManagementGhary HandojoPas encore d'évaluation
- Reveiwer 1st PDocument7 pagesReveiwer 1st PJean FlorencondiaPas encore d'évaluation
- Toxi-Ex 333Document51 pagesToxi-Ex 333Jean FlorencondiaPas encore d'évaluation
- Chapter 16: Histamine, Serotonin and Ergot Alkaloids Generic Name Brand Name Dosage Form Dosage Strength Manufactu RERDocument3 pagesChapter 16: Histamine, Serotonin and Ergot Alkaloids Generic Name Brand Name Dosage Form Dosage Strength Manufactu RERJean FlorencondiaPas encore d'évaluation
- Sonnet XxviiDocument2 pagesSonnet XxviiJean FlorencondiaPas encore d'évaluation
- Molecular Mechanism of Phenylhydrazine Induced Haematotoxicity: A ReviewDocument5 pagesMolecular Mechanism of Phenylhydrazine Induced Haematotoxicity: A ReviewJean FlorencondiaPas encore d'évaluation
- 18880Document9 pages18880Sundar RameshPas encore d'évaluation
- Related LiteratureDocument6 pagesRelated LiteratureJean FlorencondiaPas encore d'évaluation
- BN GN Therapeutic Category/ Indications Dosag E Form Dosage Strength DoseDocument2 pagesBN GN Therapeutic Category/ Indications Dosag E Form Dosage Strength DoseJean FlorencondiaPas encore d'évaluation
- International Journal of PharmtechDocument5 pagesInternational Journal of PharmtechJean FlorencondiaPas encore d'évaluation
- The Legend of OedipusDocument4 pagesThe Legend of OedipusJean FlorencondiaPas encore d'évaluation
- Bignay Local LitDocument8 pagesBignay Local LitJean FlorencondiaPas encore d'évaluation
- Pills For Type 2 Diabetes: A Guide For AdultsDocument16 pagesPills For Type 2 Diabetes: A Guide For AdultsJean FlorencondiaPas encore d'évaluation
- Cholesterol - Medicines To Help You Rev. 8-09Document20 pagesCholesterol - Medicines To Help You Rev. 8-09Jean FlorencondiaPas encore d'évaluation
- Greek and Roman Mythology LessonDocument35 pagesGreek and Roman Mythology LessonJean FlorencondiaPas encore d'évaluation
- AlbinoDocument7 pagesAlbinoJean FlorencondiaPas encore d'évaluation
- Filter MachinesDocument2 pagesFilter MachinesJean FlorencondiaPas encore d'évaluation
- Sedatives and Hypnotics - pdf1 PDFDocument30 pagesSedatives and Hypnotics - pdf1 PDFRamling PatrakarPas encore d'évaluation
- ManufacturingpharmacyDocument5 pagesManufacturingpharmacyJean FlorencondiaPas encore d'évaluation
- Pharmacology. Sedative HypnoticDocument16 pagesPharmacology. Sedative HypnoticJean FlorencondiaPas encore d'évaluation
- MLP by StateDocument12 pagesMLP by StateFlor OMPas encore d'évaluation
- Daftar ObatDocument1 pageDaftar ObatPramukadua DepokPas encore d'évaluation
- John Kerr BDocument3 pagesJohn Kerr BRex Loren de LeonPas encore d'évaluation
- VA DoD Management of Concussion Mild Traumatic Brain InjuryDocument112 pagesVA DoD Management of Concussion Mild Traumatic Brain InjurycirtestPas encore d'évaluation
- NTU Cat Management Network Annual General Report For Academic Year 2016/2017Document42 pagesNTU Cat Management Network Annual General Report For Academic Year 2016/2017Cat Management NetworkPas encore d'évaluation
- Instant Healing Meditation (Basic) - David Alan RamsdaleDocument31 pagesInstant Healing Meditation (Basic) - David Alan Ramsdaledeichem88% (8)
- 10 - Cognitive TherapyDocument32 pages10 - Cognitive TherapymartinjeanellPas encore d'évaluation
- Parts of A Tracheostomy TubeDocument3 pagesParts of A Tracheostomy TubeBal GiePas encore d'évaluation
- Alternative Treatment Strategies For Pseudo-Class III Malocclusion With Mild AsymmetryDocument17 pagesAlternative Treatment Strategies For Pseudo-Class III Malocclusion With Mild AsymmetrySchwan AbdulkareemPas encore d'évaluation
- Alat Alat MedisDocument6 pagesAlat Alat MedisDiasTikaPas encore d'évaluation
- Bronchogenic Carcinoma: DR Ayman El-DibDocument40 pagesBronchogenic Carcinoma: DR Ayman El-DibMuhdZaeedPas encore d'évaluation
- Liver Complications - SLEDocument5 pagesLiver Complications - SLEFanny PritaningrumPas encore d'évaluation
- Zambia Medicines Regulatory AuthorityDocument5 pagesZambia Medicines Regulatory AuthoritydaviesPas encore d'évaluation
- PMJJBYDocument1 pagePMJJBYArun PaiPas encore d'évaluation
- Coliform Analysis in Wastewater 2012Document24 pagesColiform Analysis in Wastewater 2012engrbvgPas encore d'évaluation
- ChoreaDocument4 pagesChoreaapi-19973386Pas encore d'évaluation
- HHS Public AccessDocument16 pagesHHS Public AccessintanPas encore d'évaluation
- Kansas Foodborne Illness ManualDocument186 pagesKansas Foodborne Illness ManualLeo M. Pedro Jr.Pas encore d'évaluation
- An Analytical Study of Euthanasia in India With - Rucha Kulkarni PDFDocument150 pagesAn Analytical Study of Euthanasia in India With - Rucha Kulkarni PDFDazzler AshishPas encore d'évaluation
- Oplan Kalusugan Sa DepEd SY 2019Document4 pagesOplan Kalusugan Sa DepEd SY 2019Klaribelle Villaceran100% (1)
- 香港脊醫 Hong Kong Chiropractors Dec 2017Document10 pages香港脊醫 Hong Kong Chiropractors Dec 2017CDAHKPas encore d'évaluation
- 4th Regional Pneumococcal Symposium - DownloadableDocument64 pages4th Regional Pneumococcal Symposium - DownloadablesabinvaccinePas encore d'évaluation
- عملیات شفاء امراض Amliyat Shifa Amraz 0091-33-23607502 - DIL KE AMRAZ KA RUHANI ELAJ (Spiritual Treatment of Heart Diseases)Document4 pagesعملیات شفاء امراض Amliyat Shifa Amraz 0091-33-23607502 - DIL KE AMRAZ KA RUHANI ELAJ (Spiritual Treatment of Heart Diseases)msmpaki@yahoo.comPas encore d'évaluation
- Instructor Clinical Evaluation ToolsDocument11 pagesInstructor Clinical Evaluation ToolsJoric MagusaraPas encore d'évaluation
- Orthodontic Appliances: General Requirements of An Orthodontic ApplianceDocument20 pagesOrthodontic Appliances: General Requirements of An Orthodontic ApplianceSafaa GhobPas encore d'évaluation
- Daftar Pustaka OaDocument2 pagesDaftar Pustaka OaCut Naja SoviaPas encore d'évaluation
- Communication Boards in Critical CareDocument9 pagesCommunication Boards in Critical CareSeresolPas encore d'évaluation
- Drugs and BruxismDocument14 pagesDrugs and BruxismAnthony HartonoPas encore d'évaluation
- Ssa 827Document2 pagesSsa 827joshud7264100% (2)
- Headline Magazine: Summer 2013Document24 pagesHeadline Magazine: Summer 2013BrainstreamsPas encore d'évaluation