Académique Documents
Professionnel Documents
Culture Documents
The Bridge Program Facilitating The Graduate Nurse's Transition Into The Profession
Transféré par
kitsil0 évaluation0% ont trouvé ce document utile (0 vote)
36 vues4 pagesThe Bridge program is an educational partnership between the nursing school and the hospital. Students can choose to earn 1, 2, or 3 hours of credit and are graded on a pass / fail basis. The hospital hopes to increase its ability to hire the best-qualified graduating nurses.
Description originale:
Titre original
The Bridge Program Facilitating the Graduate Nurse's Transition Into the Profession
Copyright
© © All Rights Reserved
Formats disponibles
PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentThe Bridge program is an educational partnership between the nursing school and the hospital. Students can choose to earn 1, 2, or 3 hours of credit and are graded on a pass / fail basis. The hospital hopes to increase its ability to hire the best-qualified graduating nurses.
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
36 vues4 pagesThe Bridge Program Facilitating The Graduate Nurse's Transition Into The Profession
Transféré par
kitsilThe Bridge program is an educational partnership between the nursing school and the hospital. Students can choose to earn 1, 2, or 3 hours of credit and are graded on a pass / fail basis. The hospital hopes to increase its ability to hire the best-qualified graduating nurses.
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 4
50 Nurse Leader February 2005
February 2005 Nurse Leader 51
Michelle Denyer, MSN, APRNBC, GNP;
Nancy Girard, PhD, RN, FAAN;
Nancy Ray, MA, RN; and
Kathleen Reeves, MSN, RN, CNS
Facilitating the
Graduate Nurses
Transition into the
Profession
The Bridge Program:
The Bridge Program is an educational partnership between the
University Healthcare System (UHS) in San Antonio, Texas, and the
University of Texas Health Science Center at San Antonio (UTHSCSA)
School of Nursing. The program consists of three undergraduate elec-
tives that are offered every semester, including summer, and is coordi-
nated and implemented by the department of acute nursing care faculty.
Initially developed in 1995, the Bridge Program was
designed as a training program and partially funded by
UHS. Mutually agreed upon goals by the nursing
school and the hospital were to provide students an
opportunity to get additional clinical experience to
increase their confidence and competency, prepare
them to better assume the role of the professional
nurse after graduation, and decrease orientation time
of the newly hired graduate. Additionally, the hospital
hoped to increase its ability to hire the best-qualified
graduating nurses.
Since its inception in 1995, the program has under-
52 Nurse Leader February 2005
gone several revisions. These changes have always been
based on formal and informal suggestions, feedback, and
evaluations received from the students, their preceptors,
and hospital administrators. Although the early years were
effective, few students were willing to make the commit-
ment to complete clinical hours that were not required.
An effort to improve the experience for the students and
staff was initiated. The Bridge courses were reorganized
and approved as undergraduate electives in 1998; students
could choose to earn 1, 2, or 3 hours of credit and would
be graded on a pass/fail basis. This method proved suc-
cessful and continues today. Students choosing to earn 1
hour of credit must complete 45 clock hours. Students
choosing to earn 2 hours of credit must complete 90 clock
hours, and students earning 3 hours of credit must com-
plete a project along with the 90 clock hours.
Bridge electives are best described as a clinical precep-
torship program. The student is allowed to choose a spe-
cific unit or area that reflects his or her interests. It is an
intense, hands-on clinical experience and is unique in its
true partnership nature. The nursing administration, along
with specific units of the hospital, commits to consistently
provide the students with qualified preceptors. The avail-
ability of a dedicated, primary preceptor is mandatory for
the student to participate in this program. The philosophy
of the program strongly and clearly reflects the School of
Nursings community-based partnership curriculum of the
baccalaureate program.
1
A student must be enrolled in his or her final year of the
undergraduate bachelor of science in nursing generic or
registered nurse completion program and be in good aca-
demic standing. After an interview with the faculty coordi-
nator to determine clinical area of interest, the student
must meet with the director of that unit or his or her des-
ignated representative. Almost all units of the hospital are
available, including the emergency center, critical care
units, medical/surgical units, labor and delivery, pediatrics,
and newborn services. The student approaches the meet-
ing with the unit director as if it were an interview for a
position as a graduate nurse. The student is not guaran-
teed a position after graduation, so he or she is not
required to commit to work at the hospital after gradua-
tion.
Once accepted into the program and assigned a pre-
ceptor, the student is responsible for arranging clinical
hours. The student may schedule clinicals on any day or
time that coincides with the preceptors schedule and
complements his or her academic schedule, whether
weekends, days, evenings, or nights. The faculty member
coordinates the clinical practicum, evaluates students
when they are in clinics to ensure that goals and objec-
tives are being met, counsels students, and grades the
course.
As a clinical experience, the program is considerably
different from the core courses students must complete.
There are no mandatory written nursing processes, care
plans, or examinations. However, students are evaluated
on their abilities to document, according to hospital poli-
cy, all aspects of the care they deliver. They are held
accountable for the application of the nursing process, as
opposed to submitting a written process. This is the pri-
mary component of the program that students have over-
whelmingly enjoyed and to which they have positively
responded.
Students earning 3 hours of elective credit are given
several options regarding the method in which they com-
plete the project requirement. Most students opt to pre-
pare a poster presentation on a topic of interest to their
unit. Preceptors often play an integral part in the choice of
topics as they help the student identify the learning needs
of the unit and staff. Students also may become involved
in developing or revising specific unit policies and proce-
dures or patient education material. Whatever strategy the
student chooses, creativity, enthusiasm for the topic, and
fun are encouraged.
On completion of the program, students are asked to
evaluate their experiences by completing two question-
naires. As outlined in Table 1, the first form consists of
four brief, open-ended questions that assess the students
sense of their own capabilities, their impressions of their
preceptors support, and whether they would recommend
the program to other students. The last item requests any
I What has this program enabled you to accomplish?
I Describe your relationship with your preceptor.
I Would you recommend the program to other students?
I Do you have any suggestions or comments?
Table 1. Evaluation of Bridge Program
February 2005 Nurse Leader 53
provided to students. The programs design helps students
be the adult learners they were meant to be. The nursing
faculty and hospital staff know each other well and can
depend on well-established channels of communication
that are always open. This allows for changes and adjust-
ments that might not be possible in a more structured
course format. Last, but certainly not least, the faculty and
staff are very comfortable with the inherent flexibility of the
program.
Reference
1. Staats CR. The development of a community-based baccalaureate
model in a culturally diverse health care delivery area. Nursing
Education Perspectives 2003;24(2):94-7.
Michelle Denyer, MSN, RN, GNP, is an assistant clinical professor
in the department of acute nursing care at the University of
Texas Health Science Center in San Antonio. She can be reached
at denyer@uthscsa.edu. Nancy Girard, PhD, RN, FAAN, is an
associate professor and chairwoman of the department;
Kathleen Reeves, MSN, RN, CNS, is also an assistant clinical pro-
fessor. Nancy Ray, MA, RN, is the CNO and associate administra-
tor of University Hospital in San Antonio.
1541-4612/2005/$ - see front matter
Copyright 2005 by Elsevier Inc.
doi:10.1016/j.mnl.2004.10.001
comments or suggestions, and students are encouraged to
write what they truly believe.
The second evaluation tool, outlined in Table 2, is a
more structured self-assessment tool that asks the stu-
dents to evaluate how they addressed each program
objective. They may choose ratings of satisfactory, unsatis-
factory, or not applicable and are asked for examples or
comments. This form also provides the opportunity for
faculty and preceptors to comment.
Student and hospital staff evaluations of the Bridge
Program have consistently been strongly positive.
Students have unanimously said that they would recom-
mend the program to other students. The numerous
opportunities to improve critical thinking skills, along with
the ability to successfully demonstrate assessment and
psychomotor skills, have been cited by students as the fac-
tors that create a meaningful experience.
At the completion of the program, students also report
an increase in confidence and appreciation for their cho-
sen profession. Comments have included:
This program was definitely the closest experience
to real nursing that I participated in while in nursing
school.
For the first time, I know what it is to be mentored,
and I deeply appreciated it.
This was a rewarding experience, and I want to do it
again.
I have gained more confidence in my ability to be a
professional nurse.
To date, approximately 200 students have completed
the Bridge, and approximately 60% have been hired by the
hospital. Students who accept a position with the hospital
after graduation are highly regarded by staff and are hired
at a slightly higher monetary rate.
The success of the program has been attributed to sev-
eral factors. Although student and staff feedback has
shaped the program, strong support and guidance are
I Identify the roles of the professional staff nurse in the unit.
I Demonstrate effective time management and organizational skills.
I Recognize and appropriately use the various members of the health care team in accordance with the Texas Nursing Practice Act.
I Demonstrate basic medical/surgical competencies safely.
I Demonstrate specific competencies unique to the assigned unit as identified by the preceptor.
I Demonstrate proficiency with the computer or hard copy charting system.
I Demonstrate the ability to make decisions, problem solve, think critically, and prioritize in a fast-paced, potentially high-stress
environment.
I Demonstrate the ability to provide and direct nursing care for at least ___ (patients) in the ______ (unit).
(The number varies depending on the type of unit.)
Table 2. Self-Evaluation Tool
Vous aimerez peut-être aussi
- Managing Chronic Heart FailureDocument51 pagesManaging Chronic Heart FailurekitsilPas encore d'évaluation
- GM HFIT Primary Care Heart Failure Project Full ReportDocument56 pagesGM HFIT Primary Care Heart Failure Project Full ReportkitsilPas encore d'évaluation
- Nurse Education in Practice (2004) 4, 100-106Document7 pagesNurse Education in Practice (2004) 4, 100-106kitsilPas encore d'évaluation
- g235 Heart Failure Nurse Services in England Executive Summary 0908Document27 pagesg235 Heart Failure Nurse Services in England Executive Summary 0908kitsilPas encore d'évaluation
- HF Network 051612 McKeeDocument38 pagesHF Network 051612 McKeekitsilPas encore d'évaluation
- z812 Role of The BHF Heart Failure Palliative Care Specialist Nurse A Retrospective Evaluation 0111Document65 pagesz812 Role of The BHF Heart Failure Palliative Care Specialist Nurse A Retrospective Evaluation 0111kitsilPas encore d'évaluation
- Disease Management For Heart FailureDocument84 pagesDisease Management For Heart FailureNational Pharmaceutical Council100% (7)
- Enhancing Transition: An Enhanced Model of Clinical Placement For Final Year Nursing StudentsDocument9 pagesEnhancing Transition: An Enhanced Model of Clinical Placement For Final Year Nursing StudentskitsilPas encore d'évaluation
- 1 s2.0 S0099176707004485 MainDocument6 pages1 s2.0 S0099176707004485 MainkitsilPas encore d'évaluation
- The NATURE and IMPLICATIONS of Support in Graduate Nurse TRansition Programs - An Australian StudyDocument8 pagesThe NATURE and IMPLICATIONS of Support in Graduate Nurse TRansition Programs - An Australian StudykitsilPas encore d'évaluation
- 1 s2.0 S0260691707001141 MainDocument10 pages1 s2.0 S0260691707001141 MainkitsilPas encore d'évaluation
- Transition Within A Graduate Nurse Residency ProgramDocument10 pagesTransition Within A Graduate Nurse Residency ProgramkitsilPas encore d'évaluation
- Successful Strategies For New Graduates: Beth Ulrich, Edd, RN, CheDocument3 pagesSuccessful Strategies For New Graduates: Beth Ulrich, Edd, RN, ChekitsilPas encore d'évaluation
- Graduate-Only Pre-Registration Mental Health Nursing ProgrammesDocument6 pagesGraduate-Only Pre-Registration Mental Health Nursing ProgrammeskitsilPas encore d'évaluation
- Stresses and Challenges For New Graduates in HospitalsDocument6 pagesStresses and Challenges For New Graduates in HospitalskitsilPas encore d'évaluation
- Expectations and Perceptions of Graduates' Performance at The Start and at The End of Their Graduate YearDocument6 pagesExpectations and Perceptions of Graduates' Performance at The Start and at The End of Their Graduate YearkitsilPas encore d'évaluation
- The Transitional Journey Through The Graduate Year A Focus Group StudyDocument7 pagesThe Transitional Journey Through The Graduate Year A Focus Group StudykitsilPas encore d'évaluation
- The Professional Self-Concept of New Graduate NursesDocument6 pagesThe Professional Self-Concept of New Graduate NurseskitsilPas encore d'évaluation
- Best Practice Principles For The Transition From Student To Registered NurseDocument7 pagesBest Practice Principles For The Transition From Student To Registered NursekitsilPas encore d'évaluation
- Experiences and Learning During A Graduate Nurse ProgramDocument6 pagesExperiences and Learning During A Graduate Nurse ProgramkitsilPas encore d'évaluation
- New Graduate Nurse Transitioning Necessary or NiceDocument9 pagesNew Graduate Nurse Transitioning Necessary or NicekitsilPas encore d'évaluation
- The Educational Preparation of Undergraduate Nursing Students in Pharmacology Clinical Nurses' Perceptions and Experiences of Graduate Nurses' Medication KnowledgeDocument12 pagesThe Educational Preparation of Undergraduate Nursing Students in Pharmacology Clinical Nurses' Perceptions and Experiences of Graduate Nurses' Medication KnowledgekitsilPas encore d'évaluation
- New Graduate Nurse Practice Readiness Perspectives On The Context Shaping Our Understanding and ExpectationsDocument5 pagesNew Graduate Nurse Practice Readiness Perspectives On The Context Shaping Our Understanding and ExpectationskitsilPas encore d'évaluation
- Facing Registration The Expectations and The Unexpected Original Research ArticleDocument8 pagesFacing Registration The Expectations and The Unexpected Original Research ArticlekitsilPas encore d'évaluation
- 2014new Graduate Nurses' Experiences in Their First Year of PracticeDocument7 pages2014new Graduate Nurses' Experiences in Their First Year of PracticekitsilPas encore d'évaluation
- Graduate Nurse Transition ProgramDocument5 pagesGraduate Nurse Transition ProgramkitsilPas encore d'évaluation
- The Learning Process of Recently Graduated Nurses in Professional Situations - Experiences of An Introduction ProgramDocument5 pagesThe Learning Process of Recently Graduated Nurses in Professional Situations - Experiences of An Introduction ProgramkitsilPas encore d'évaluation
- Fitting in A Pervasive New Graduate Nurse NeedDocument6 pagesFitting in A Pervasive New Graduate Nurse NeedkitsilPas encore d'évaluation
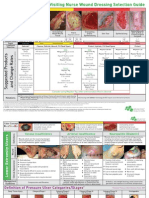
- Wound Dressing GuideDocument2 pagesWound Dressing Guidekitsil100% (7)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Gcu Student Teaching Evaluation of Performance Step Standard 1 Part I - SignedDocument4 pagesGcu Student Teaching Evaluation of Performance Step Standard 1 Part I - Signedapi-434580279100% (1)
- Daily Lesson Plan Date Subject Class Day Time Enrolment Level Theme Topic Focused Skill Integrated Skill Content StandardsDocument13 pagesDaily Lesson Plan Date Subject Class Day Time Enrolment Level Theme Topic Focused Skill Integrated Skill Content StandardsMohamad ShafeeqPas encore d'évaluation
- Courses After DegreeDocument7 pagesCourses After DegreeJitendra KumarPas encore d'évaluation
- Lesson 2Document3 pagesLesson 2Amanda WeyhingPas encore d'évaluation
- The Liar Paradox As A Reductio Ad Absurdum ArgumentDocument47 pagesThe Liar Paradox As A Reductio Ad Absurdum ArgumentHenrique AlmeidaPas encore d'évaluation
- RPMS Label TabbingDocument3 pagesRPMS Label TabbingKimberly Cler SuarezPas encore d'évaluation
- Student Teaching HandbookDocument42 pagesStudent Teaching HandbookNcup OkePas encore d'évaluation
- Student Application Form For The Masters Program In: Mechanical and Process EngineeringDocument5 pagesStudent Application Form For The Masters Program In: Mechanical and Process EngineeringMukeshPas encore d'évaluation
- Moorestown - 0831Document36 pagesMoorestown - 0831elauwitPas encore d'évaluation
- STP CurriculumDocument208 pagesSTP Curriculumapi-299089301Pas encore d'évaluation
- AcknowledgementDocument31 pagesAcknowledgementLuzille Anne Cordova AlertaPas encore d'évaluation
- Past Simple VsDocument3 pagesPast Simple VsBibi PetkoskaPas encore d'évaluation
- Module 1 - Lesson 1.1Document14 pagesModule 1 - Lesson 1.1Angelica TalastasinPas encore d'évaluation
- Book 1Document6 pagesBook 1manishaPas encore d'évaluation
- Private High School Entrance Exams PREPDocument3 pagesPrivate High School Entrance Exams PREPNathaniel Haynesworth0% (1)
- The New MethodologyDocument39 pagesThe New MethodologySabitha BanuPas encore d'évaluation
- Introduction LetterDocument1 pageIntroduction Letterapi-537851264Pas encore d'évaluation
- Rutherford: Contact Number: 0912-345-6789Document4 pagesRutherford: Contact Number: 0912-345-6789Franz Angelo Del RosarioPas encore d'évaluation
- Steps To Apply - UTech, JaDocument1 pageSteps To Apply - UTech, JaDamario berryPas encore d'évaluation
- Sergei Korsakoff PDFDocument2 pagesSergei Korsakoff PDFDipaziaPas encore d'évaluation
- Issue 6, Volume 46Document8 pagesIssue 6, Volume 46sisttonlPas encore d'évaluation
- Leanza Altenderfer: Student, University of Central FloridaDocument4 pagesLeanza Altenderfer: Student, University of Central FloridaJulie AebersoldPas encore d'évaluation
- The Impact of Physical Education Activities On: Student Academic PerformanceDocument10 pagesThe Impact of Physical Education Activities On: Student Academic PerformanceTariq RahimPas encore d'évaluation
- Pros and Cons of The Big CampusDocument3 pagesPros and Cons of The Big CampusClairePas encore d'évaluation
- Land of The White PeopleDocument124 pagesLand of The White PeoplejaygalePas encore d'évaluation
- A Study of Teaching Speaking Techniques Ecf83713Document15 pagesA Study of Teaching Speaking Techniques Ecf83713Kyla Mariz Layones RecioPas encore d'évaluation
- Report of School ProfileDocument24 pagesReport of School ProfileDinithi SnehaPas encore d'évaluation
- Capital Letters and Comma Study GuideDocument4 pagesCapital Letters and Comma Study GuideVictor Rafael Mejía Zepeda EDUCPas encore d'évaluation
- Role of Technology in Teaching and Learning English A Perspective of The Higher Secondary Level in BangladeshDocument3 pagesRole of Technology in Teaching and Learning English A Perspective of The Higher Secondary Level in BangladeshSharifMahmudPas encore d'évaluation
- Long CV Beer 130712Document29 pagesLong CV Beer 130712sarakhan0622Pas encore d'évaluation