Académique Documents
Professionnel Documents
Culture Documents
Decompression Sickness - DR Guritno
Transféré par
captaincandy0 évaluation0% ont trouvé ce document utile (0 vote)
150 vues34 pagesEmergency
Titre original
Decompression Sickness - Dr Guritno
Copyright
© © All Rights Reserved
Formats disponibles
PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentEmergency
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
150 vues34 pagesDecompression Sickness - DR Guritno
Transféré par
captaincandyEmergency
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 34
DLCCMkLSSICN SICkNLSS AND GAS LM8CLISM
Mohammad Gur|tno SUkCkUSUMC
Ketua Program Studi Kedokteran Hiperbarik
Program Pascasarjana Fakultas Kedokteran
Unversitas Indonesia, Jakarta
email: mguritno@yahoo.com
DLCCMkLSSICN SICkNLSS
Decompression sickness (DCS) refers to the clinical
syndrome of neurological deficits, pain, or other clinical
disorders resulting from the body tissues being
supersaturated with inert gas after a reduction in the
ambient pressure.
Ak1LkIAL GAS LM8CLISM
Arterial Gas Embolism (AGE) refers to gas bubbles in
the systemic arterial system resulting from pulmonary
barotrauma, iatrogenic entry of gas into the arterial
system, or arterialized venous gas emboli.
Classification of DI
1. The traditional or
Golding Classification
2. The descriptive or
Francis & Smith Classification
3. The ICD-10 Classification
Modified Golding Classification for DI
Arter|a| Gas Lmbo||sm
Decompress|on S|ckness
1. 1ype I : Muscu|oske|eta| a|n, Sk|n,
Lymphanc, Lxtreme Iangue,
er|phera| Nervous Symptoms
2. 1ype II : Neuro|og|c, Card|oresp|ratory,
Aud|o-vesnbu|ar, Shock
3. 1ype III : Comb|ned Decompress|on S|ckness
and Arter|a| Gas Lmbo||sm
Table The Francis & Smith Classification
for Dysbaric Illness
Evolution
o Spontaneously Recovery (Clinical improvement is
evident)
o Static (No change in clinical condition)
o Relapsing (Relapsing symptoms after initial recovery)
Progressive (Increasing number or severity
of signs)
Organ System:
o Neurological
o Cardiopulmonary
o Limb pain exclusively
o Skin
o Lymphatic
o Vestibular
Table The Francis & Smith Classification
for Dysbaric Illness
Time of onset:
o Time before surfacing
o Time after surfacing (or estimate)
Gas Burden
o Low (e.g., within NDL)
o Medium (e.g., Decompression Dive)
o High (e.g., Violation of Dive Table)
Evidence of Barotrauma
o Pulmonary (Yes / No)
o Ears
o Sinuses
Other Comments
The ICD-10 Classification
The ICD-10 codes most frequently used are:
o T70 (Effects of air pressure and water
pressure)
o T70.0 (Otitic barotrauma)
o T70.1 (Sinus barotrauma)
o T70.3 (Caissons disease)
o T70.4 (Effects of high-pressure fluids)
o T70.8 (Other effects of air pressure and water
pressure)
o T79.0 (Traumatic air embolism)
o T79.7 (Traumatic subcutaneous emphysema)
o M90.3 (Osteonecrosis in caisson disease
T70.3+)
Clinical Setting
1. Diving
2. Flying
3. HBOT
PATHOGENESIS OF DCS
Denaturation of Plasma Proteins
Endothelial Damage
Interaction of Bubbles with the Blood
Coagulation System
General Aspect :
Most of the clinical manifestations of DCS are
thought to result from tissue distortion of vascular
obstruction produced by bubbles
Presenting Symptoms Type Cases (%)
Local Pain
Arm
Leg
Vertigo (staggers)
Paralysis
Shortness of breath (chokes)
Extreme fatigue with pain
Collapse + unconsciousness
Type I
Type 2
89
30
70
5.3
2.3
1.6
1.3
0.5
Frequency of Various Symptoms of DCS
The time of onset of
symptoms after surfacing
30 % occurred < 30 minutes
85 % occurred < 1 hour
95 % occurred < 3 hours
1 % Delayed more than 6
hours
Predisposing Factors
Exercise
Injury
Cold
Obesity
Increased Fractional
Concentration of CO2 to
inspired Gas
Age
Ingestion of Alcohol
Dehydration
Fatigue
1reatment of DCS
re-kecompress|on
Cxygen 13 L/M wlLh reservolr mask or demand valve
auenL ln suplne posluon (noL head down)
Conunuous monlLorlng
Alr LransporL :
As low as safely posslble.
referably lower Lhan 1000
ressurlze alrcra cabln Lo 1 A1A lf posslble
Conslder Lmergency Lvacuauon Pyperbarlc SLreLcher
8ecompress even lf slgns/sympLoms resolve prlor Lo
recompresslon
Treatment of DCS
Type I Treatment Table 5 (TT5)
Musculoskeletal pain
Skin bends
Lymphatic bends
Type II Treatment Table 6 (TT6)
Includes all other manifestations of DCS
Recompress to 60 FSW on 100% O2 and begin TT6
Diving Medical Officer (DMO) has option to go to 165 early if
patient has unsatisfactory response at 60 FSW
*Note: Severe Type II signs/symptoms warrant full extensions of 60 FSW
oxygen breathing periods even if S/S resolve during the first oxygen
breathing period
Deep Uncontrolled Ascents Treatment Table 8 (TT8) 225 FSW
table for treating deep, uncontrolled ascents when more than 60
minutes of decompression have been missed.
Treatment of DCS
Persistent Symptoms at 60 FSW
Extend TT6 for two 25-minute periods at 60 FSW
Extend TT6 for two 75-minute periods at 30 FSW
DMO may recommend customized treatment
Stay at 60 FSW for 12 hours or longer come out on TT7
kecurrence of Ser|ous Symptoms dur|ng
Decompress|on
If shallower than 60 FSW go to 60 FSW
If deeper than 60 FSW go to 165 FSW
Treatment of DCS
Persistent Symptoms at 60 FSW
Extend TT6 for two 25-minute periods at 60 FSW
Extend TT6 for two 75-minute periods at 30 FSW
DMO may recommend customized treatment
Stay at 60 FSW for 12 hours or longer come out on TT7
kecurrence of Ser|ous Symptoms dur|ng
Decompress|on
If shallower than 60 FSW go to 60 FSW
If deeper than 60 FSW go to 165 FSW
Treatment of DCS
In-Water Recompression
Only when:
No recompression facility on site
Significant signs/symptoms
No prospect of reaching chamber in 12-24 hrs
No improvement after 30 min of 100% oxygen on
surface
Thermal conditions are favorable
Not for unconsciousness, paralysis, respiratory
distress, or shock
Keep these individuals on the surface with 100% O2
Treatment of DCS
In-Water Recompression
Only when:
In-Water Recompression with oxygen preferred
Purge rebreather 3 times with oxygen
30 FSW with stand-by diver
60 min at rest for Type 1
90 min at rest for Type II
20 FSW for 60 min
10 FSW for 60 min
100% O2 for additional 3 hours on the surface
Treatment of DCS
In-Water Recompression with air (if no oxygen
available)
Follow TT1A
Full face mask or surface-supplied helmet preferred
SCUBA used only as last resort
Stand-by diver required
* Note: In divers with severe Type II symptoms or symptoms of
arterial gas embolism (e.g. unconsciousness, paralysis, vertigo,
respiratory distress (chokes), shock, etc), the risk of increased
harm to the diver from in-water recompression probably
outweighs any anticipated benefit.
DCS kLVLN1ICN
1. D|ver Se|ecnon
Screening for Patent Foramen Ovale (PFO)
History of DCS Disqualifying for diving duty
Deselection of divers for repeated episodes of DCS Not
recommended
2. re-D|ve DCS revennon
re-dlve exerclse, no recommendation
Table modifications based on water temp No recommendation
Hydration (in warm water diving)
Dive depth limits: For SCUBA dives maximum depth of 130 ft
(on-site chamber recommended for military diving if dive depth is
greater than100 ft)
Clean times: Surface interval required for the diver to be
considered clean for the next dive: 2 hours 20 minutes for
repetitive group Alpha 15 hours 50 minutes for repetitive group
Zulu
DCS PREVENTION
3. DCS Prevention (During the Dive)
Ascent Rate 30 feet per minute
4. DCS Prevention (Post-Dive)
Exercise restrictions Both aerobic (e.g. running) and
anaerobic (e.g. weight lifting) exercise performed
within 4 hours after a compressed gas dive with
significant decompression stress may be associated
with an increased risk of DCS
Ascent to altitude restrictions (Up to 10,000 ft) Time/
ascent Table - up to 29:15 for Repet Group Zulu 48
hours for Exceptional Exposure Dives
Manifestations of AGE
Loss of consciousness
Confusion
Focal neurological deficits
Cardiac arrhythmias or ischemia
Cardiac arrest and death 4%
Causes of AGE
Pulmonary barotrauma
Iatrogenic events (radiologic
procedures and cardiac bypass
surgery)
Right-to-left shunt
Sma|| embo|| |n the vesse|s of the ske|eta|
musc|es or v|scera are we|| to|erated, but
embo||zanon to the cerebra| (CAGL) or
coronary c|rcu|anon may resu|t |n severe
morb|d|ty or death
Treatment of AGE
The primary goal of treatment is the
protection and maintenance of vital
functions
Pre-hospital
100% oxygen by rebreathing face mask
Supine position
Maintain hydration
HBO is the treatment of choice
Adjunctive therapy: lidocaine,
anticoagulant, corticosteroid
Benefits of HBOT
1. Compression of existing gas bubbles
2. Establishment of a high diffusion gradient to
speed dissolution of existing bubbles
3. Improved oxygenation of ischemic tissues
and lowered intracranial pressure
4. Reduction of ischemic-reperfusion injury
Treatment table selection
Initial treatment USNTT6 extend Table 6 or
UNSTT6A
Follow-up treatments
Daily or twice daily
Until complete relief of symptoms or until there is
no further clinical improvement after 2 consecutive
treatments
Until complete relief of symptoms or until there is
no further clinical improvement after 2 consecutive
treatments
No consensus: table 5, 6 and 9
1er|makas|h
Vous aimerez peut-être aussi
- Shock & Fluid TherapyDocument57 pagesShock & Fluid Therapyarnol3090Pas encore d'évaluation
- Status Asthmaticus: Triwahju AstutiDocument41 pagesStatus Asthmaticus: Triwahju AstutirianiPas encore d'évaluation
- 01 Enteral and Parenteral Nutrition Support PSIK UMMDocument68 pages01 Enteral and Parenteral Nutrition Support PSIK UMMSri YulianaPas encore d'évaluation
- Diabetic Foot: by Myrna Rita PMRDocument33 pagesDiabetic Foot: by Myrna Rita PMRDianNurlitaAnggrainiPas encore d'évaluation
- Gastric Carcinoma: Professor Ravi KantDocument44 pagesGastric Carcinoma: Professor Ravi KantAna Quintana100% (1)
- Intermediate UveitisDocument33 pagesIntermediate UveitismitaamayPas encore d'évaluation
- 1 Principles of First Aid and Its PracticeDocument118 pages1 Principles of First Aid and Its PracticeMohamed SamyPas encore d'évaluation
- 22ca ColonDocument21 pages22ca ColonDrVishal BhattPas encore d'évaluation
- Universal Safety (Health) PrecautionsDocument37 pagesUniversal Safety (Health) PrecautionsElizabeth Catharine Sianipar100% (1)
- Stoma Management: Shankar ZanwarDocument33 pagesStoma Management: Shankar Zanwarpradeep nairPas encore d'évaluation
- Thyroid Function TestsDocument25 pagesThyroid Function TestsEva SinghPas encore d'évaluation
- SnakebiteDocument4 pagesSnakebiteallenininiPas encore d'évaluation
- 2020 4 - Principles-of-Sterilization-and-DisinfectionDocument41 pages2020 4 - Principles-of-Sterilization-and-DisinfectionMely Kartikasari100% (1)
- Management of Patients With Burn InjuryDocument36 pagesManagement of Patients With Burn Injuryraghad awwad100% (1)
- Peptic UlcerDocument31 pagesPeptic UlcerHarpal Bajwa0% (1)
- 24 05 2021 Floroquinolones DR - Syeda ZainDocument46 pages24 05 2021 Floroquinolones DR - Syeda ZaintehreemPas encore d'évaluation
- Basic Physical Assessment Procedures - PowerpointDocument38 pagesBasic Physical Assessment Procedures - PowerpointWeng Ramojal100% (1)
- Abc of Burns: Kanwal Khan Lecturer ZCPTDocument35 pagesAbc of Burns: Kanwal Khan Lecturer ZCPTKanwal KhanPas encore d'évaluation
- Insect Bite ReactionDocument21 pagesInsect Bite ReactionSiska TeurupunPas encore d'évaluation
- Gastric Carcinoma: H. Pylori InfectionDocument7 pagesGastric Carcinoma: H. Pylori InfectionMuvenn KannanPas encore d'évaluation
- Allergic Reaction - RefDocument16 pagesAllergic Reaction - RefprimaPas encore d'évaluation
- Insertion and Confirmation of Position of Nasogastric Tubes For Adults and ChildrenDocument28 pagesInsertion and Confirmation of Position of Nasogastric Tubes For Adults and ChildrenMatt Q0% (1)
- Gastrointestinal Fistula: DR Vihar Kotecha M.D, M.MED Gen Surg (Nbi), FCS Gen Surg (ECSA) Lecturer CUHASDocument60 pagesGastrointestinal Fistula: DR Vihar Kotecha M.D, M.MED Gen Surg (Nbi), FCS Gen Surg (ECSA) Lecturer CUHASSangija kamataPas encore d'évaluation
- Aqueous HumorDocument46 pagesAqueous HumorJ NATASHA MARIAPas encore d'évaluation
- SnakebiteDocument54 pagesSnakebiteDimas Satrio BPas encore d'évaluation
- Diarrhea PPTDocument82 pagesDiarrhea PPTIshwar HavaragiPas encore d'évaluation
- OsteomielitisDocument28 pagesOsteomielitismaulidaangraini100% (1)
- Pneumothorax: DR - Naveen Vennilavan R Pg-IiiDocument95 pagesPneumothorax: DR - Naveen Vennilavan R Pg-Iiinaveen vennilavanPas encore d'évaluation
- Management of Pregnancy JaundiceDocument28 pagesManagement of Pregnancy JaundiceShailani Thakur100% (1)
- Refkas CondylomaAccuminataDocument18 pagesRefkas CondylomaAccuminatamichelle1945Pas encore d'évaluation
- Acute Diffuse Otitis ExternaDocument36 pagesAcute Diffuse Otitis ExternaIlham Isnin Dolyanov HasibuanPas encore d'évaluation
- Pancreatic Cancer (Cancer of The Pancreas) : Patient Discussions: FindDocument13 pagesPancreatic Cancer (Cancer of The Pancreas) : Patient Discussions: FindMoses ZainaPas encore d'évaluation
- Infection Control in Surgical PracticeDocument41 pagesInfection Control in Surgical PracticeMuhammad Azeem KhanPas encore d'évaluation
- WK13 CDN - Meningitis, Poliomyelitis, Leprosy, Tetanus, Red TideDocument43 pagesWK13 CDN - Meningitis, Poliomyelitis, Leprosy, Tetanus, Red TidePotato PceePas encore d'évaluation
- Ostomy Care in Home Health1Document39 pagesOstomy Care in Home Health1api-315120220100% (1)
- Burn NotesDocument5 pagesBurn NotespaulineorrPas encore d'évaluation
- Neurological Manifestations of HIVDocument34 pagesNeurological Manifestations of HIVashuPas encore d'évaluation
- SyphilisDocument54 pagesSyphilisYeyeh SantosPas encore d'évaluation
- Pediatric BurnsDocument22 pagesPediatric BurnsdrsdineshPas encore d'évaluation
- Oral Cavity NeoplasmaDocument42 pagesOral Cavity NeoplasmaWidya AdiartiPas encore d'évaluation
- Acute Diarrheal Disease Profound Secretory Diarrhoea Dehydration Hypovolemic Shock Native To The Ganges DeltaDocument24 pagesAcute Diarrheal Disease Profound Secretory Diarrhoea Dehydration Hypovolemic Shock Native To The Ganges DeltacipacipaaPas encore d'évaluation
- TetanusDocument102 pagesTetanusMo Oo MooPas encore d'évaluation
- Asthma (Reactive Airway Disease)Document33 pagesAsthma (Reactive Airway Disease)anwar jabariPas encore d'évaluation
- Stoma Types PDFDocument1 pageStoma Types PDFUmi Kalsum100% (1)
- Oncology NursingDocument15 pagesOncology NursingArdrina Sappari100% (1)
- CHAPTER TWO Communicable DssDocument36 pagesCHAPTER TWO Communicable DssAyro Business CenterPas encore d'évaluation
- Sterilization & DisinfectionDocument52 pagesSterilization & DisinfectionKabir RajputPas encore d'évaluation
- Diarrhea: ChildrenDocument16 pagesDiarrhea: ChildrenEmmi Valentina PardedePas encore d'évaluation
- DR - Saleh-26 March 2013-Farmakologi (Anti Jamur, Anti Virus, Anti Parasit, DLL)Document72 pagesDR - Saleh-26 March 2013-Farmakologi (Anti Jamur, Anti Virus, Anti Parasit, DLL)jeinpratpong100% (4)
- Gerd PresentationDocument44 pagesGerd PresentationMia Mia MiaPas encore d'évaluation
- DyslipidemiaDocument21 pagesDyslipidemiaBasil HussamPas encore d'évaluation
- Sepsis Power Point Slide Presentation - The Guidelines - Implementation For The FutureDocument25 pagesSepsis Power Point Slide Presentation - The Guidelines - Implementation For The Futuremontie13Pas encore d'évaluation
- Epidemiology of Diarrheal DiseasesDocument36 pagesEpidemiology of Diarrheal DiseasesMuna Hassan MustafaPas encore d'évaluation
- Sepsis Content Concepts MapDocument2 pagesSepsis Content Concepts Mapghodghod1230% (1)
- Snake BiteDocument61 pagesSnake Biteniraj_sdPas encore d'évaluation
- Surfactant PresentationDocument18 pagesSurfactant PresentationMaadaPas encore d'évaluation
- Crohns DiseaseDocument32 pagesCrohns DiseaseMin Chi PakPas encore d'évaluation
- (03nov) Matra Laut - DCS & AGE Dr. GuritnoDocument47 pages(03nov) Matra Laut - DCS & AGE Dr. GuritnodimasahadiantoPas encore d'évaluation
- Decompression Sickness and Gas Embolism: Mohammad Guritno SURYOKUSUMODocument47 pagesDecompression Sickness and Gas Embolism: Mohammad Guritno SURYOKUSUMOarinindyaPas encore d'évaluation
- Uhms DCS Age GuidelinesDocument17 pagesUhms DCS Age GuidelinesMarios PolyzoisPas encore d'évaluation
- JadwalDocument2 pagesJadwalcaptaincandyPas encore d'évaluation
- Unit 37: Should + Have + Past ParticipleDocument1 pageUnit 37: Should + Have + Past ParticiplecaptaincandyPas encore d'évaluation
- Diseases of Children in The Subtropics and TropicsDocument1 092 pagesDiseases of Children in The Subtropics and TropicscaptaincandyPas encore d'évaluation
- Evaluasi Program KeslingDocument9 pagesEvaluasi Program KeslingcaptaincandyPas encore d'évaluation
- Lembar Follow UpDocument2 pagesLembar Follow UpcaptaincandyPas encore d'évaluation
- IdhfOIJ Vjief Joif J'Document1 pageIdhfOIJ Vjief Joif J'captaincandyPas encore d'évaluation
- Skin Graft and Skin FlapDocument4 pagesSkin Graft and Skin FlapcaptaincandyPas encore d'évaluation
- Ventura 4 DLX ManualDocument36 pagesVentura 4 DLX ManualRoland ErdőhegyiPas encore d'évaluation
- Argumentative Essay Research PaperDocument5 pagesArgumentative Essay Research PaperJadPas encore d'évaluation
- Full Test Bank For Health Economics and Policy 7Th Edition Henderson PDF Docx Full Chapter ChapterDocument34 pagesFull Test Bank For Health Economics and Policy 7Th Edition Henderson PDF Docx Full Chapter Chapterpeeepochaq15d100% (9)
- SA 8000 Audit Check List VeeraDocument6 pagesSA 8000 Audit Check List Veeranallasivam v92% (12)
- Business PlanDocument17 pagesBusiness PlanChester Cortez50% (2)
- STR Mpa-MpmDocument8 pagesSTR Mpa-MpmBANGGAPas encore d'évaluation
- L Addison Diehl-IT Training ModelDocument1 pageL Addison Diehl-IT Training ModelL_Addison_DiehlPas encore d'évaluation
- Aakanksha ProjectDocument32 pagesAakanksha ProjectAakash murarkaPas encore d'évaluation
- Onuaguluchi1996 1Document10 pagesOnuaguluchi1996 1IkaSugihartatikPas encore d'évaluation
- LIC Jeevan Labh Plan (836) DetailsDocument12 pagesLIC Jeevan Labh Plan (836) DetailsMuthukrishnan SankaranPas encore d'évaluation
- Đề ANH chuyên 5Document7 pagesĐề ANH chuyên 5Phạm Ngô Hiền MaiPas encore d'évaluation
- EB Research Report 2011Document96 pagesEB Research Report 2011ferlacunaPas encore d'évaluation
- Fundamental Molecular Biology: GenomesDocument45 pagesFundamental Molecular Biology: GenomesMoonHoLeePas encore d'évaluation
- TherabandDocument1 pageTherabandsuviacesoPas encore d'évaluation
- Thorley Amended Complaint (Signed)Document13 pagesThorley Amended Complaint (Signed)Heather ClemenceauPas encore d'évaluation
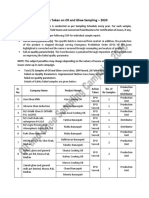
- Action Taken On Oil and Ghee Sampling - 2020Document2 pagesAction Taken On Oil and Ghee Sampling - 2020Khalil BhattiPas encore d'évaluation
- Emission Estimation Technique Manual: For Mining and Processing of Non-Metallic MineralsDocument84 pagesEmission Estimation Technique Manual: For Mining and Processing of Non-Metallic MineralsAbdelaziem mahmoud abdelaalPas encore d'évaluation
- Waste Heat Recovery UnitDocument15 pagesWaste Heat Recovery UnitEDUARDOPas encore d'évaluation
- Практичне 25. Щодений раціонDocument3 pagesПрактичне 25. Щодений раціонAnnaAnnaPas encore d'évaluation
- (Cô Vũ Mai Phương) Tài liệu LIVESTREAM - Chuyên đề thi THPT - Câu hỏi giao tiếp xã hội (Buổi 1)Document4 pages(Cô Vũ Mai Phương) Tài liệu LIVESTREAM - Chuyên đề thi THPT - Câu hỏi giao tiếp xã hội (Buổi 1)nguyen duong trungPas encore d'évaluation
- Overall Summary:: SAP MM Certified Associate & SAP Certification ID: 0019350978Document6 pagesOverall Summary:: SAP MM Certified Associate & SAP Certification ID: 0019350978Ganapathi RajPas encore d'évaluation
- Ecological Imbalance in IndiaDocument4 pagesEcological Imbalance in IndiaabhywaPas encore d'évaluation
- Online Games and Academic AchievementDocument25 pagesOnline Games and Academic AchievementJasmine GamoraPas encore d'évaluation
- Pyq of KTGDocument8 pagesPyq of KTG18A Kashish PatelPas encore d'évaluation
- Nodular Goiter Concept MapDocument5 pagesNodular Goiter Concept MapAllene PaderangaPas encore d'évaluation
- Recommended Standards For Newborn ICU DesignDocument39 pagesRecommended Standards For Newborn ICU DesignAlbert SekarPas encore d'évaluation
- Measurement of Bioreactor K ADocument18 pagesMeasurement of Bioreactor K AAtif MehfoozPas encore d'évaluation
- Tiếng AnhDocument250 pagesTiếng AnhĐinh TrangPas encore d'évaluation
- Missoula County Fairgrounds Phase 2Document10 pagesMissoula County Fairgrounds Phase 2Olivia IversonPas encore d'évaluation
- Paterno Report: Dr. Fred S. Berlin, M.D., PH.D Final Report 2-7-2013Document45 pagesPaterno Report: Dr. Fred S. Berlin, M.D., PH.D Final Report 2-7-2013The Morning CallPas encore d'évaluation