Académique Documents
Professionnel Documents
Culture Documents
FTP
Transféré par
Jennifer Rodriguez0 évaluation0% ont trouvé ce document utile (0 vote)
11 vues3 pagestes
jurnal
reading
Titre original
2820601236_ftp
Copyright
© © All Rights Reserved
Formats disponibles
PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documenttes
jurnal
reading
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
11 vues3 pagesFTP
Transféré par
Jennifer Rodrigueztes
jurnal
reading
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 3
Female Patients With Meningioma of the Sphenoid Ridge and
Additional Primary Neoplasms of the Breast and Genital Tract
DANIEL H. J ACOBS, MD, MICHAEL J . MCFARLANE, MD. AND FREDERICK F. HOLMES. MD
Of 283 meningioma patients seen at the University of Kansas from 1948 to 1984, eight women acquired
two primary extraneural cancers in addition to their meningiomas. Of these eight patients, six (75%)
had sphenoid ridge meningiomas compared with 15% of meningioma patients overall (P <0.001). Seven
(87.5%) had at least one breast or genital cancer ( P <0.001). Of the six with sphenoid ridge menin-
giomas, five (83.3%) had both of their additional tumors in these two organ systems, and the sixth had
one such tumor. It is proposed that this grouping of sphenoid ridge meningioma, breast cancer, and
genital cancer represents a unique constellation of neoplasms in women.
Cancer 60:3080-3082, 1987.
ENINGIOMA and breast cancer have been asso-
M ciated in several studies.'-5 Like breast cancers,
meningiomas often contain progesterone receptor pro-
tein and may also contain estrogen receptor pr~tei n. ~- ~
Because meningioma has long been known to be more
common in women than men, it is appropriate to study
the associations between meningiomas and other neo-
plasms in women. In this study we analyzed the syn-
chronous and metachronous occurrence of cancers in
meningioma patients, focusing particularly on breast
and female genital cancers and the distribution of men-
ingiomas among various subsites.
Methods
The records of 283 intracranial meningioma patients
were reviewed. These cases include 177 women and 106
men diagnosed with meningiomas at the University of
Kansas Medical Center from 1948 to 1984. The diag-
noses were confirmed from the hospital records and the
pathology reports contained therein, the Kansas Univer-
sity Medical Center Tumor Registry, and the Cancer
Data Service (the regional cancer registry). Data on the
occurrence of second or third tumors in these menin-
gioma patients were obtained from existing records.
Both metachronous and synchronous second and third
neoplasms were identified. I n order to test the possibility
From the Department of Medicine, University of Kansas Medical
Center, Kansas City, Kansas.
Supported by the Kansas University Cancer Center, the Kansas
State Department of Health, and the Kansas University Medical
Center Hospital.
The authors thank Dr. J ohn Kepes for his thoughtful review and
encouragement.
Address for reprints: Frederick F. Holmes, MD, Department of
Medicine, University of Kansas Medical Center. Kansas City. KS
66 103.
Accepted for publication J uly 7, 1987.
of chance occurrence of sphenoid ridge meningiomas
with multiple malignancies involving the breast or fe-
male genital tract, chi-square tests were performed.
Results
Of the 283 patients with meningiomas, 42 had 50
additional malignant tumors (Table 1). These included
12 breast cancers, five uterine corpus cancers, three
uterine cervix cancers, and one vaginal cancer. Forty-
three patients ( 15%) had meningiomas on the sphenoid
ridge; this group included 29 women and 14 men.
Forty-nine individuals had meningiomas on the con-
vexity, 35 in the parasagittal area, I8 in multiple sites, 17
in the parasellar region, 16 in the falx, and the re-
mainder in other sites (Table 2).
Eight women (19% of those with additional tumors)
had two cancers in addition to their meningiomas
(Table 3). Breast cancers were reported in five of these
eight patients, uterine corpus cancers in three, and uter-
ine cervix cancers in two. Altogether, seven of these
eight women had at least one lesion in the breast or
genital organs and five had lesions in both sites. No
patient had more than three tumors.
In six of the eight women with two additional cancers
(75%) the meningiomas were found on the sphenoid
ridge. A seventh patient had a parasellar meningioma,
and the eighth had an olfactory groove meningioma. Of
these six sphenoid ridge meningiomas, five occurred on
the medial or middle third, and one occurred on the
lateral third, the pterion. Compared with all menin-
gioma patients, those with two additional tumors were
more likely to have sphenoid ridge meningiomas than
meningiomas at other sites ( P <0.001; they were also
more likely to be women ( P <0.05). Compared with
patients with meningioma and one additional tumor,
those with two additional tumors were more likely to
3080
No. I2 MENINGIOMA
Jacobs el al. 308 1
TABLE 1. Sites of 50 Malignant Primary Tumors Occumng
Synchronously or Metachronously in Association With Meningioma
Breast 12
Female genital 10
Gastrointestinal 10
Brain 6
Thyroid 3
Lung 3
Hematopoietic 2
Melanoma 2
Prostate I
Unknown 1
Total 50
have an associated breast or genital cancer than cancer
with a different primary focus (P c 0.00 1).
Of the eight patients with two additional cancers, the
subgroup of six with sphenoid ridge meningiomas in-
cluded the five patients whose additional tumors were
breast cancer(s) (P c 0.05) and the three whose lesions
were uterine corpus cancer (not significant). This sub-
group of six with sphenoid ridge meningiomas also in-
cluded the five patients who developed both of their
additional extraneural neoplasms in the breast and gen-
ital tract ( P c 0.05). Table 3 lists the neoplasms and ages
at diagnosis in these eight patients.
The eight meningioma patients were categorized by
the histologic subtype of the meningioma if available.
Three meningiomas were classified as meningothelial,
two as fibroblastic, and one as transitional. The remain-
ing two meningiomas were not classified. Five of the
eight patients had family histories of cancer. Two pa-
tients had four first-degree relatives with malignancies,
two had three such relatives, and one had two affected
relatives.
The eight patients developed a total of 16 tumors in
addition to their meningiomas; nine of these neoplasms
were diagnosed before the meningioma, three after, and
four synchronously. The earliest neoplasm was discov-
ered 29 years before the meningioma, and the latest one
was found 20 years after the development of the menin-
gioma.
Discussion
We have described a subset of female meningioma
patients at high risk for acquiring additional neoplasms.
Seven of 17 patients (41%) with meningioma and either
breast or female genital cancer developed a third tumor
compared with one of 25 with meningioma and a sec-
ond lesion in a site other than the breast or genitals (P
-=0.00 1). Moreover, sphenoid ridge meningiomas oc-
curred more frequently in patients with three tumors (P
c 0.00 1 ). Because the associated tumors can precede or
follow the meningiomas by 20 or more years, affected
women remain at risk throughout their adult lives.
TABLE 2. Sites of Occurrence of 283 Intracranial Meningiomas,
Universitv of Kansas Medical Center. 1948-1984
Men Women Site Total
Convexity
Sphenoid ridge
Parasagittal
Multiple sites
Parasellar
Falx cerebri
Olfactory groove
Other
Total
49
43
35
18
17
16
1 1
94
283
27
29
23
13
12
13
9
51
177
22
14
12
5
5
3
2
43
106
Endocrine factors may be operative in the occurrence
of this unusual pattern of three neoplasms. Three lines
of evidence support the idea that the sphenoid ridge may
be more susceptible to the effects of endogenous female
sex steroids than other sites of occurrence of menin-
gioma. First, intracranial meningiomas have a two-to-
TABLE 3. Female Patients With Multiple Primary
Malignancies Plus Meningioma
Ageat
Patient diagnosis Site of tumors* Comments
79
79
81
71
66
79
79
79
67
57
59
30, 38
43
50
58
45
34
32
68
39
51
51
58
58
Sphenoid ridge
(pterion)?
Breast
Corpus uteri
Sphenoid ridget
Breast
Corpus uteri
Olfactory groove1
Gall bladder
Hodgkin's disease
Sphenoid ridget
Uterine cervix
Breast
Sphenoid ridget
Corpus uteri
Lung
Parasellart
Thyroid
Cervix
Sphenoid ridget
Breast
Breast
Sphenoid ridget
Breast
Cystadenoid
basal cell
carcinoma of
breast
(different
locus) with
metastasis to
meningioma
Brain tumor in
daughter and brother;
breast cancer in two
sisters
Cancer of unknown
primary site in four
siblings
mother and two sisters
Meningioma recurred at
age 38; corpus uteri
cancer in two sisters;
breast cancer in
mother
Cervical cancer in
Cancer of unknown site
in 2 brothers
~
* Combinations including basal cell and squamous cell carcinoma of
f Designates meningioma: sites with no dagger are where other ma-
the skin are not included.
lignancies occurred.
3082 CANCER December I5 1987 Vol. 60
one predilection for women, but meningiomas en
plaque of the sphenoid ridge occur almost exclusively in
women. l o Second, meningiomas have been reported to
enlarge with pregnancy, regress subsequently, and recur
with subsequent pregnancies. These meningiomas tend
to occur on the medial aspect of the sphenoid wing"-'3
and in the parasellar area contiguous to the sphenoid
ridge.'"'7 Third, investigators have correlated clinical
findings from meningioma patients with studies of the
intensity and incidence of progestin binding to receptors
on the t~mor.',~.'~ They found an increase in the inten-
sity of progestin binding in meningiomas of the sphe-
noid wing and olfactory groove as compared with me-
ningiomas at other sites. The same is true for meningo-
thelial meningiomas as compared with those of other
histologic classifications. '' However, incidence of posi-
tivity in progestin receptor assays could not be corre-
lated with the site of meningioma despite the presence of
positivity in a majority of sphenoid wing menin-
Genetic factors may also play a role in the occurrence
of these tumors. The patients we described developed
multiple neoplasms at various unrelated sites through-
out their adult lives. The family histories showed that
similar neoplasms occurred in at least two first-degree
relatives in a majority of these patients. These features
typify family cancer syndrome^.'^-*^However, these
family cancer syndromes have not been previously re-
ported for meningiomas.
Because the numbers of tumors are small, the tumors
are relatively common, and survival after diagnosis
varies widely among patients affected by these several
tumors, we cannot absolutely exclude the possibility
that the association of meningiomas, breast, and genital
cancers has occurred only by chance. The fact that six of
the 29 women with sphenoid ridge meningiomas had
two additional neoplasms-quite separate from the as-
sociation with breast and genital tract tumors-makes
the association by chance quite unlikely when only two
of the 148 women with meningioma at sites other than
the splenoid ridge had two additional neoplasms (P
<0.001). Further studies should be done with a much
larger data base, preferably a population-based registry
such as one of the SEER registries, comparing the actual
incidence of second and third tumors in women with
sphenoid ridge meningiomas and women with menin-
giomas of the other intracranial sites.
The clinical ramifications of these findings are two-
fold. First, women with a history of multiple tumors
involving the breast, genital tract, and sphenoid menin-
ges may benefit from serial screening for additional ma-
lignancies. Second, patients who have had breast or en-
dometrial cancer and who present with lesions of the
sphenoid ridge may have meningiomas that are opera-
gi ~mas.~.~
ble, rather than metastases of their primary neoplasms
that are probably not operable.
That breast and genital malignancies occur with sphe-
noid ridge meningiomas suggests the possibility that
tumors are responsive to female sex steroids. However,
the clinical importance of the presence of estrogen and
progesterone receptor protein in meningiomas is at
present moot. This, along with evidence that supports a
genetic basis for the tumors, indicates the need for fur-
ther investigation into the etiology of this combination
of lesions.
REFERENCES
1 . Schoenberg BS, Christine BW, Whisnant J P. Nervous system
neoplasms and primary malignancies of other sites: The unique associ-
ation between meningiomas and breast cancer. Neurology 1975;
2. Smith Fp, Slavik M, MacDonald J S. Association of breast cancer
with meningioma: Report of two cases and review of the literature.
Cancer 1978; 42:1992-1994.
3. Mehta D, Khatib R, Patel S. Carcinoma of the breast and me-
ningioma: Association and management. Cancer 1983; 51:1937-1940.
4. Fenyes G, Kepes J J . Uber des gemeinsame Vorkommen von
Meningomen und Geschwulsten anderen Typs in Gehirn. Zeniralbl
5. Burns PE, Naresh J HA, Bain GO. Association of breast cancer
with meningioma: A report of five cases. Cancer 1986; 58: 1537-1539.
6. Tilzer LL, Plapp FV, Evans J P, Stone D, Alward K. Steroid
receptor proteins in human meningiomas. Cancer 1982; 49:4:633-
636.
7. Markwalder TM, Zava DT, Goldhirsch A, Markwalder RV. Es-
trogen and progesterone receptors in meningiomas in relation to clini-
cal and pathologic features. Surg Neurol 1983; 20:42-47.
8. Magdenalat H, Pertuiset BF, Poisson M et al. Progestin and es-
trogen receptors in meningiomas: Biochemical characterization, clini-
cal and pathologic correlations in 42 cases. Acta Neurochir 1982;
64: 199-2 13.
9. Poisson M. Sex steroid receptors in human meningiomas: Re-
view. Clin Neuropharmacol 1984; 74:320-324.
10. Kepes J J . Meningiomas: Biology, Pathology and Differential
Diagnosis. New York: Masson, 1982; 17.
1 I . Bickerstaff ER, Small J M, Guest IA. The relapsing course of
certain meningiomas in relation to pregnancy and menstruation. J
Neurol Neurosurg Psychialry 1958; 2 I :89-9 I .
12. Rand CW, Andler M. Tumors of the brain complicating preg-
nancy. Arch Neurol Psychiat 1950 63:1-41.
13. Walsh FB. Clinical Neuro-Ophthalmology. Baltimore: Williams
and Wilkins, 1947; 416.
14. Sandyk R. Meningioma presenting with recurrent retrobulbar
neuritis. SAfr Med J 1982; 61:857-858.
15. Weyand RD, MacCarty CS, Wilson RB. The effect of pregnancy
on intracranial Meningiomas occurring about the optic chiasm. Surg
CIin Norlh Am 1951; 31:1225-1233.
16. Rucker CW, Kearns TP. Mistaken diagnosis in some cases of
meningioma. Am JOphthalmol 1961; 51:15-19.
17. Hagedoorn A. The chiasmal syndrome and retrobulbar neuritis
in pregnancy. Am J Ophrhalmol 1937; 20690-699.
18. Markwalder TM, Markwalder CV, Zava DT. Estrogen and pro-
gestin receptors in meningiomas: Clinicopathologic correlations. Cl i n
Neuropharmacol 1984; 7:368-374.
19. Lynch HT, Krush AJ. Differential diagnosis of the cancer fam-
ily syndrome. Surg Gynecol Ohsrer 1973; 136:22 1-224.
20. Lynch HT. Familial cancer prevalence spanning eight years:
Family N. Arch Intern Med 1974; 134:931-938.
2 1 . Li FP, Fraumeni J F. Soft tissue sarcomas, breast cancer, and
other neoplasms: A familial syndrome? Ann fnrern hfed 1969;
7 1~747-752.
22. Li FP, Fraumeni J F. Prospective study of a family cancer syn-
drome. JAMA 1982; 247:2692-2694.
25~705-712.
Narochir 1956; 16~25 1-260.
Vous aimerez peut-être aussi
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Venous SinusesDocument15 pagesVenous SinusesJennifer RodriguezPas encore d'évaluation
- Case Study-Breast CADocument11 pagesCase Study-Breast CAJoanna Cabildo83% (6)
- The 5th Edition of The Atlas For GI EndosDocument186 pagesThe 5th Edition of The Atlas For GI EndosNguyễn Văn Cần100% (5)
- The Unseen Side of Pregnancy: Non-Communicable Diseases and Maternal HealthDocument28 pagesThe Unseen Side of Pregnancy: Non-Communicable Diseases and Maternal HealthThe Wilson Center100% (2)
- Can You Identify The Midbrain, Pons and Medulla On This Mid-Sagittal Sequence. Pons MedullaDocument22 pagesCan You Identify The Midbrain, Pons and Medulla On This Mid-Sagittal Sequence. Pons MedullaJennifer RodriguezPas encore d'évaluation
- Case Report PrintDocument38 pagesCase Report PrintJennifer RodriguezPas encore d'évaluation
- A Pop To SisDocument6 pagesA Pop To SisRegiane Miranda OlerPas encore d'évaluation
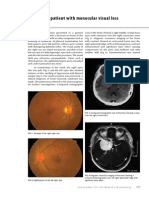
- A Patient With Monocular Visual Loss: Pictorial MedicineDocument2 pagesA Patient With Monocular Visual Loss: Pictorial MedicineJennifer RodriguezPas encore d'évaluation
- T&J No.122Document1 pageT&J No.122Jennifer RodriguezPas encore d'évaluation
- Orbital Meningiomas Clinical ObservationDocument6 pagesOrbital Meningiomas Clinical ObservationJennifer RodriguezPas encore d'évaluation
- Monika 4Document9 pagesMonika 4Jennifer RodriguezPas encore d'évaluation
- Anatomic Moment: Optic Canal Forms An Angle of AboutDocument7 pagesAnatomic Moment: Optic Canal Forms An Angle of AboutJennifer RodriguezPas encore d'évaluation
- Surgical Results of Parasagittal and Falx Meningioma: Case ReportDocument6 pagesSurgical Results of Parasagittal and Falx Meningioma: Case ReportJennifer RodriguezPas encore d'évaluation
- Healthmedicinet I 2016 11Document369 pagesHealthmedicinet I 2016 11tuni santePas encore d'évaluation
- 9.lecturer 18 Biochemistry Effect On Tumor and Tumor MarkersDocument19 pages9.lecturer 18 Biochemistry Effect On Tumor and Tumor MarkersAbdulRahman MuthannaPas encore d'évaluation
- BCP-ALL-MRD Cytognos WhitepaperDocument4 pagesBCP-ALL-MRD Cytognos Whitepaperjonathan andre mora quimbayoPas encore d'évaluation
- G.R. No. 176832 May 21, 2009 Government Service Insurance System, Petitioner, MARIAN T. VICENCIO RespondentDocument4 pagesG.R. No. 176832 May 21, 2009 Government Service Insurance System, Petitioner, MARIAN T. VICENCIO RespondentChristopher AdvinculaPas encore d'évaluation
- Internal RadiationDocument9 pagesInternal RadiationJM SonidoPas encore d'évaluation
- Using Blended-Learning Approach To Improve Education On Clinical Pathways For Breast Cancer Management in Nigeria: A Research ProtocolDocument5 pagesUsing Blended-Learning Approach To Improve Education On Clinical Pathways For Breast Cancer Management in Nigeria: A Research ProtocolasclepiuspdfsPas encore d'évaluation
- Philippine Primary Care Studies: Pilot Study at The UP Health ServiceDocument60 pagesPhilippine Primary Care Studies: Pilot Study at The UP Health ServiceBryan SalvaPas encore d'évaluation
- Toledo, John Carlo - Colon CancerDocument13 pagesToledo, John Carlo - Colon CancerKristine YoungPas encore d'évaluation
- Management and Prevention of Complications During Initial Treatment of Head and Neck Cancer - UpToDateDocument19 pagesManagement and Prevention of Complications During Initial Treatment of Head and Neck Cancer - UpToDateAchmad MusaPas encore d'évaluation
- HealingHabit15-Avoid Milk and Dairy Products PDFDocument4 pagesHealingHabit15-Avoid Milk and Dairy Products PDFJyles SirabPas encore d'évaluation
- Article OralDocument36 pagesArticle Oralamina-fakirproPas encore d'évaluation
- Fall 2023 Health Trends ReportDocument17 pagesFall 2023 Health Trends ReportLaura LizarazoPas encore d'évaluation
- Role of Triple Phase Computed Tomography Findings For Evaluation of Hepatic LesionsDocument8 pagesRole of Triple Phase Computed Tomography Findings For Evaluation of Hepatic LesionsGordana PuzovicPas encore d'évaluation
- Journal Club: Dr. Preethi.S DNB Resident Ent 31/03/23Document27 pagesJournal Club: Dr. Preethi.S DNB Resident Ent 31/03/23PreethiPas encore d'évaluation
- Breast Cancer Prevention: Saint Louis University School of Nursing Research JournalDocument3 pagesBreast Cancer Prevention: Saint Louis University School of Nursing Research JournalDale DeocaresPas encore d'évaluation
- Tumour Inhibitors From PlantsDocument59 pagesTumour Inhibitors From PlantsAlishba Mushtaq100% (1)
- LumpectomyDocument4 pagesLumpectomyvicenteturasPas encore d'évaluation
- Apoptosis & Its Relation To CancerDocument16 pagesApoptosis & Its Relation To CancerRohan DuttaPas encore d'évaluation
- Oncologic NursingDocument16 pagesOncologic Nursinglushxene84Pas encore d'évaluation
- Liam 1 ADocument1 pageLiam 1 ASelina MaycockPas encore d'évaluation
- Blue Book PDFDocument126 pagesBlue Book PDFgojo_11Pas encore d'évaluation
- 1986 7992 1 PBDocument8 pages1986 7992 1 PBSapna thakurPas encore d'évaluation
- Module # 3 Physiological Changes in Aging Affecting Various SystemsDocument30 pagesModule # 3 Physiological Changes in Aging Affecting Various SystemsJann ericka JaoPas encore d'évaluation
- Full Dataset of Papers FormattedDocument234 pagesFull Dataset of Papers FormattedoafsPas encore d'évaluation
- Prostate - TURP 4.1.0.0.REL CAPCPDocument12 pagesProstate - TURP 4.1.0.0.REL CAPCPkarimahihdaPas encore d'évaluation
- Spot Skin Cancer Fact SheetDocument2 pagesSpot Skin Cancer Fact SheetThad WarrenPas encore d'évaluation
- Benevity-Goodness-Calendar-2024 - Goodness Calendar 2024Document3 pagesBenevity-Goodness-Calendar-2024 - Goodness Calendar 2024Russell TorresPas encore d'évaluation