Académique Documents
Professionnel Documents
Culture Documents
Traumatic Ulcers
Transféré par
rdindamyrna0 évaluation0% ont trouvé ce document utile (0 vote)
44 vues7 pagestraumatic ulcers
Titre original
traumatic ulcers
Copyright
© © All Rights Reserved
Formats disponibles
PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documenttraumatic ulcers
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
44 vues7 pagesTraumatic Ulcers
Transféré par
rdindamyrnatraumatic ulcers
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 7
Journal of Clinical Periodontology 1982: 9: 178-183
Key words: Gingivai lesion - Tooth brushing.
Accepted for publicaEion March 30, 1981
Traumatic ulcerative gingivai iesion
TONY AxfeLL AND GORAN KOCH
Department of Oral Surgery, Faculty of Odontology, University of Lund, Malmo and Department of
Pedodontics, Institute for Postgraduate Dental Education, Jonkoping, Sweden
Abstract. Gingival ulcers caused by tooth brushing in 13 patients with an average age of 29.9 years are
presented. The lesions show characteristic clinical features not compatible with simple traumatic ulcers,
e. g. running a more chronical course, the duration averaging 6.5 months. Repeated trauma and, in some
cases, infection might explain the chronicity. The lesion is suggested to be designated traumatic
ulcerative gingival lesion. As treatment, cessation of tooth brushing for 2 weeks and concomitant
mouthrinses with chlorhexidine are recommended.
Traumatization of gingival tissues caused by
mechanical oral hygiene procedures is not in-
frequent. The subject has been reviewed by
Sangnes (1976). Laceration or ulceration ofthe
gingival tissues are considered as acute lesions.
Similar lesions, probably also connected with
tooth brushing trauma but of a more chronic
nature, have been mentioned by Ainamo (1977)
and described by Axell (1979). !n a recent
article, Schiadt et al. (1979) gave a thorough
description of "traumatic lesions of the gingiva
provoked by tooth brushing" in a material
comprising 38 patients. They also dealt with the
treatment of the lesion.
The purpose of the present paper was to
describe tbe lesion, discuss its etiology and to
suggest treatment.
Material and Methods
The report is based on findings in 13 patients,
five males and eight females (Table 1), treated
between 1973 and !979. Four of them were
treated in a pedodontic clinic and nine in an oral
surgery clinic. The median age of these two
groups of patients was 13.5 and 33 years.
respectively. The overall median age was 21
years and the average age 29.9 years.
Ctinical characteristics
Well-circumscribed ulcers were seen in all pa-
tients on the free gingival margin, usually
leaving the top of the interdental papillae
undamaged (Figs. 1 and 4). The ulcers, which
were covered by a thin yellowish or sometimes a
greyish, greasy exudate, showed a marked,
somewhat bow-shaped border against the
healthy gingiva. There were some exceptions in
which the lesion extended to the vestibular
mucosa (Figs. 2a, b).
The most frequent location was the canine
region and surrounding areas ofthe upper jaws
(Table 1 and Fig. 3), and out of a tota! of 23
ulcers 21 (91 %) were found on the buccal or
labial surfaces of the gingiva.
AU patients complained of a smarting sensa-
tion or a dull pain making tooth brushing
difficult to carry out. Nevertheless, they all
exhibited excellent orai hygiene with a mini-
mum of dental plaque and gingivitis. No patient
showed more general symptoms such as a sore
throat or increased temperature, nor was there
0303-6979/82/030178-06 SO2.5O/0 1982 Munksgaard, Copenhagen
TRAUMATIC ULCERATIVE GINGIVAL LESION 179
Table 1. Clinical data on 13 pauenis showing giogivai oicers provoked by tooth brushing
Klinisehe Daten von 13 Patienten mit durch Zcihnebursten verursachtcn ZahnjleLschiasionen
Donnees cliniques provenant de 13 patients ayant des ulceres gingivaux provoques par le brassage
Patiejit
LJ*
IM*
GS*
PS*
MA
RA
AB
LB
GH
EJ
EP
TR
VW
Sex
F
M
M
M
F
F
M
F
M
F
F
F
F
Age
years
12
15
14
13
53
36
19
2i
69
17
23
33
64
Gingival location
2 1 , ,
13, ,
11, ,
12, .
, , 26
, , 26, 33, .
, . 26, 43. .
. . 22
13, 23, 37
12, .
23, ,
13. ,
14.,
23. ,
11. .
45
12,,
, . I 3 , 22. .
, . 24
, , 44
,.46
.,23**
. . 15, 24, 33, . . . 34
. , 24, 33, ,
. . 27, 47**
. .14, 23, ,
, , I 3
..34
27
Duration
months
<1
<1
3
9
7
3
<1
25
<1
15
10
<1
8
* Patients treated at the Pedodontic Clinic
** Lingoal or palatal location
* In der Klinik fiir Kinderzahnheiikunde behandelte Faiienten
** Linguale oder palatinale Lage
* Patients traites a la Clinique de Pedodontie
** Localisation linguale ou palatine
any general inflammation of the gingiva. Only
occasionally slightly tender submandibular
lymph nodes could be palpated.
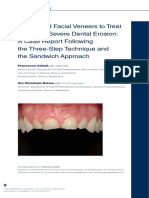
Fig. I. Patient EJ showing lesion on the ;ii;ccal
attached gingiva in the upper left jaw. The top of the
interdental papillae left undamaged.
Patient EJ mit Lasion der Gingiva propria im linken
Oberkiefer. Die Spitze der Interdentalpapilie ist un-
verletzt,
Patient EJ ayant une iesion situee sur ia gencive
atlachee vestibulaire au niveau du maxilaire superieur
gauche, Le sommet despapiltes interdentaires n'est pas
endommage.
The lesions seemed to run an intertnittent and
chronic course unless they were given proper
treatment. The duration averaged 6.5 months.
One patient revealed a past history of the lesion
of more than 2 years (LB, Table 1), verified by
her dentist.
Samples for bacteriologic cultivation were
secured frotn five patients, Frotn two of them,
material was also taken from a clinically
healthy, contralateral gingiva. ID these two
cases there was no difference in bacterial flora
between ulcerated and healthy gingiva and in
four of the five cases the flora was considered
normal. The one exception showed an increased
presence of Klebsiella pneutnoniae. Fungi were
not found in any specimen,
Treattnent
Initially various treatments were tried including
intensified oral hygiene procedures. More fre-
quent and careful tooth brushing was supple.-
metited in some cases with daily mouthrinses
with a 0,2% chlorhexidine solution. Local
180 AXELL AND KOCH
^. 2. Patient GS showing extensive gingival lesions also extending to the vestibular mucosa in the upperjaw (a)
aod lower jaw (b).
Patient GS mit umfassenden Zahnfleischlasianen, welche sicii bis zu der vestibularett Mukosa im Obet'kteferfa} und
Unterkiefer (b) erstrecken.
Patient GS ayani des lesions gingivales importantess'etendant egaiement a la muqueuse vestibuiaire des machoires
superieure (a) et inferieure (b).
application of corticosteroids as well as anti-
biotic and antitnycotic drugs was also tried in a
few patients. None of these remedies proved
effective and produced only slight, temporary
improvement in a couple of cases. On the other
hand, intensified tooth brushing seemed to
make matters worse (Fig. 5). This latter fact
gave rise to a course of action based on
cessation of tooth brushing for 1-2 weeks. To
Right side
Fig. 4 Patient AB. Initial iesn
Leftside Patient AB. Initiale Lasion.
Patient AB. Lesion initiale.
A
7 6 5 4 3 2 1 1 2 3 4 5 6 7
upper i
Lower jaw
Number
Fig. 3. Location of giogival ulcers provoked by tooth Fig. 5. Patient PS. Extensive lesioB that developed
brushing in 13 patients. after instruction on intensifying tooth brushing.
Lage der von Zahneburslen verursachten Zahnjleiseh- Patient PS. Umfassende Lasion, die nach Instruktion in
lasionen bei )3 Patienten. intensiviertem ZahnebUrsten entstanden ist.
Localisation duiceres gingivaux provoques par le bros- Patient PS. Lesion etendues'etan! developpee apres une
sage chez 13 patients. intensive instruction en hygiene buccale.
TRAUMATIC ULCERATIVE GINGIVAL LESION 181
maintain plaque control the patients were in-
structed to use a 0.1 or 0.2% chlorhexidine
solution for mouthrinses twice daily. After 1 or
2 weeks, tooth brushitig was started. The pa-
tients were then shown how to employ a gentle
and proper brushing technique.
The treatment resulted in rapid healing (Figs.
6a. b) in all but one patient. This patient, a 23-
year-old woman (EP, Table 1) was referred by
her dentist because of extensive ulcers in her
upper left and right gingiva (Fig. 7a). The
lesions were aggravated by intensified tooth
brtishing. She used barbiturates daily against
epilepsy, but apart from that she was healthy.
Her blood values were all within normal limits.
Gentle tooth brushing supplemented with daily
mouthriosing with 0.2% chlorhexidine pro-
duced only slight improvement and cessation of
tooth brushing for 1 week failed to make the
lesions heal completely. A bacteriological
Fi^. 6. Patient LJ. Typical lesion (a) which healed (b) promptly after cessauon of tooth brushing.
Patient IJ. Typisehe Lasiou (a): (b) Sofortige Heilung nach Ein.stellen des Zahnebiirstens.
Patient LJ. Lesion typique (a) rapidement guerie apres arret de tout brossagc (bj.
Fig. 7. PL;tiL:Eii l-.P Very extensive lesion which developed after nv.i;::sirietl KHT.:: hrushing. The ulcer is covered
by a greasy exudate (a) indicating infection. Healing after topical application of antibiotics and cessation of
tooth brushing (b).
Patient EP. Sehr umfassende. nach intensiviertem ZUlmebUrsten entstandene Lasion. Diese Ldsion ist von
.ichmierigem Exsudat bedeekt (a), was auf eine Infekiion deutet. Heilung nach Lokalapplikation von Antibiotika
und Einstellen des Zahnebiirstens (bj.
Patient EP. Lesion tres imporiante s'etant developpee apres I'intensification des mesures de brossage. Uulcere est
recouveri par un exudai graisseux (aj indiquant I'infection. Cicairisation apres application topique d'antibiotiques
et arrei de tout brossage (bj.
182 AXELL AND KOCH
sample taken from the ulcers revealed the
presence of Ktebsiella pneumoniae. Local treat-
ment with Gentamycin, to which the bacteria
proved sensible in vitro, resulted in prompt
relief and complete healing within 2 weeks (Fig.
7b). During these 2 weeks the patient did not
brush her teeth but rinsed her mouth twice daily
with a 0.1 % solution of chlorhexidine. Shallow
clefts persisted in the gingiva even after healing.
Such persistent clefts were also seen in a few
other patients, especially in those who had
suffered from their lesions for several months.
Discussion
Ulceration of the gingival tissues may be seen in
connection with many different conditions such
as general diseases, local infections and trau-
matic injuries. Among the 13 patients presented
in this report, none was suffering from any
general disease that could possibly give rise to
the gingivai ulcers present.
Among local infections acute specific entities
like acute necrotizing ulcerating gingivitis
(ANUG), herpetic gingivostomatitis and strep-
tococcal gingivostomatitis (Pindborg 1980)
may be considered from a differential diag-
nostic point of view. In contrast to the lesion
presented here, ANUG often shows necrosis at
the top of the interdental papillae and there is
usually a lot of dental bacterial plaque present.
Furthermore, ANUG, as opposed to the present
lesion, has a more generalized gingival distribu-
tion and is accompanied by a characteristic oral
fetor.
Acute herpetic gingivostomatitis may present
gingival ulcers with characteristics similar to
those presented here but the gingiva is most
often generally edematous and tender and there
is usttally general malaise and an increased
temperature. Streptococcal gingivostomatitis
may also show similar gingival necrotic ulcers
but there is always a diffuse, almost generalized
reddening of the gingiva, where occasionally
abscesses may be found. A sore throat and/or
tonsillitis and an increased temperature usually
precede the gingival manifestations. Strepto-
coccal gingivostomatitis as well as acute herpe-
tic gingivostomatitis are self-limiting and usual-
ly resolve spontaneously within 2 weeks.
The lesions presented here are obviously
connected with tooth brushing. Thus, the ulcers
were consistently found in patients with excel-
lent oral hygiene and most often located in
regions where tooth brushing is easiest to
perform viz. the maxillary buccal gingiva and
especially the canine region. This location has
previously been considered as one of predilec-
tion for ulcers caused by tooth brushing
(Sangnes 1976). However, a simple traumatic
ulcer of the gingival tissues should heal within
1-2 weeks in a healthy individual. In the light of
this it is astonishing, as Schiedt et al. (1979)
pointed out, that the healing time for the lesions
discussed here should be so considerably pro-
longed; in their material it averaged over 5
weeks and in this material over 6 months.
According to Schiadt et al. (1979), the expla-
nation for the delayed healing was probably
repeated trauma. Intensified oral hygiene pro-
cedures commonly instituted during recent
years would then account for the fact that these
lesions have lately been found more frequently.
Repeated trauma is the most plausible etioiogie
factor but perhaps, in a few cases, infection
could be a supplementary factor disturbing
healing. Thus, occasionally, a somewhat greasy,
greyish exudate, not typical of the simple trau-
matic ulcer covering, was noted. Infection could
be caused by microorganisms within the normal
mixed flora of the oral cavity but occasionally
bacteria normally not harbored in the mouth
might cause an infection demanding special
attention. This suggestion is based on the fact
that one of the present patients did not show
definite improvement until local antibiotic
treatment was initiated against a bacteria, Kteb-
sietta pneumoniae, which is not regularly found
in the mouth but in the intestines.
The lesion described by Axell (1979) and
Schiedt et al. (1979) and confirmed in this
article seems to constitute a clinical entity. We
TRAUMATIC ULCERATIVE GINGIVAL LESION
t83
suggest it to be designated traumatic ulcerative
girtgival lesion with reference to the etiology of a
traumatic nature, the appearance of well-
marked ulcers and to the fact that it is oniy
exceptionally located outside the gingiva.
As treatment we suggest cessation of tooth
brushing for 1-2 weeks during which time the
patient should use a mouthrinse with a 0. 1-
0,2% aqueous solution of chlorhexidine glu-
conate twice daily. If heahng is not completed
after 2 weeks, the regimen should be prolonged
for a further 2-week period. If healing is still not
completed after this period, bacterial cultiva-
tion should be undertaken and a proper local
antibiotic tried. After healing, the patient
should be instructed to use as gentle a tooth-
brushing technique as possible.
Gingivalasion" zu benennen. Als Behandlung wird
zweiwochentliches Einstellen des Zahneputzens und
gleichzeitige Mundspulungen rait Chlorhexidin emp-
fohlen.
Resume
Lesions gingivales ulcereuses d'origine traumatique
Les ulceres gingivaux provoques par le brossage chez
13 patients d'un age moyen de 29,9 ans ont ete
examines, Les lesions montrent un aspect clinique
caracteristique incompatible avec ceiui des ulcJres
traumatiques simples, Elles sont en cffet plus chro-
niques et remontent en moyenne a 6 mois et demi, Le
traumatisme repete et, dans certains cas, Tinfcction,
peuvent expliquer Ia chronicite. On propose de de-
signer cette lesion par le terme "lesion gingivale
uicereuse d'origine traumatique". Le traitement con-
siste a supprimer tout brossage pendant 2 seraaines et
a utiliser des bains de bouche a la chlorhexidine.
Acknowledgment
For aid with the microbiological analyses, the
authors express their sincere gratitude to pro-
fessor Stig Edwardsson, Department of Oral
Microbiology, Faculty of Odontology, Univer-
sity of Lund, Maltno,
Zusammeniassung
Traumatisch - ulzerose Gingivalasion
Durch das Zahneputzen entstandene gingivale Ulze-
rationen bei 13 Patienten im Durchschnittsalter von
29,9 Jahren werden hier beschrieben, Klinisch haben
solche Lasionen ein typisches Aussehen das mit dera
klinischen Bilde der einfachen traumatischen Lasion
nicht vergleichbar ist - wie z.B, der ausgesprochen
chronische Verlauf mit einer durchschnittlichen
Dauer von 6,5 Monaten. Wiederholtes Trauma und in
einigen Fallen eine Infektion konnen moglicherweise
der chronischen Verlauf erklaren. Es wird vorge-
schlagen, diese Lasionsform "traumatisch-ulzerose
References
Ainamo, J. (1977) Control of plaque by chemical
agents. Journal of Ciinicai Periodontology 4,23-35.
Axell, T, (1979) Bacterial gingivo-stomatitis. Work-
ing paper, Scandinavian Association of Oral Sur-
geons, XIII annual meeting, Elsinore.
Pindborg, J, J. (19S0) Atlas of diseases ofthe oral
mucosa, 3rd ed. Copenhagen: Munksgaard,
Sangnes, G. (1976) Traumatization of teeth and
gingiva related to habitual tooth-cleaning proce-
dures . Journal of Clinical Periodontology 3,94-103.
Schiadt, M., Worsaae, N , Holmstrup, P., Bay, L.,
Andreasen, J. & Besserman, M. (1979) Gingivale
sar som fsige af tandbarstning. Tandlaegebladet
83, 743-747.
Address:
J}r, Tony Axell
Department of Oral Surgery
School of Dentistry
Carl Gustavs vag S4
S-214 21 Malmo
Sweden
Vous aimerez peut-être aussi
- Endoscopy Handbook Amended 2nd Edition 2016 GESADocument242 pagesEndoscopy Handbook Amended 2nd Edition 2016 GESAblackurlz4111100% (1)
- Rehabilitation Summary ProjectDocument3 pagesRehabilitation Summary ProjectKENNEDY KAUKAPas encore d'évaluation
- Cardiovascular Disease Nursing Diagnosis - Causes - FactsDocument3 pagesCardiovascular Disease Nursing Diagnosis - Causes - Factsfeirri0% (1)
- Severe High Angle Class II Division 1 Malocclusion With Vertical Maxillary Excess and Gummy Smile: A Case ReportDocument4 pagesSevere High Angle Class II Division 1 Malocclusion With Vertical Maxillary Excess and Gummy Smile: A Case ReportElla GolikPas encore d'évaluation
- Sinus 2 IOSR JDMS PDFDocument3 pagesSinus 2 IOSR JDMS PDFbhupendraPas encore d'évaluation
- A Rare Case Report Along With Surgical Management of Bilateral Maxillary Buccal Exostosis in A Patient of Polydactyly and Distomol.Document3 pagesA Rare Case Report Along With Surgical Management of Bilateral Maxillary Buccal Exostosis in A Patient of Polydactyly and Distomol.Fransiski HoPas encore d'évaluation
- Jurnal Paper 4Document6 pagesJurnal Paper 4asa0411 behiraPas encore d'évaluation
- Oroantral FistulaDocument4 pagesOroantral FistulaMahesh AgrawalPas encore d'évaluation
- Lase Report: Infection From An Exfoliating Primary Tooth in A Child With Severe Neutropenia: A CaseDocument4 pagesLase Report: Infection From An Exfoliating Primary Tooth in A Child With Severe Neutropenia: A CaseangelpazcalPas encore d'évaluation
- Management of Extra Oral Sinus Tract Associated With Large Periapical Lesion - A Case ReportDocument1 pageManagement of Extra Oral Sinus Tract Associated With Large Periapical Lesion - A Case ReportNgân PhạmPas encore d'évaluation
- Jurnal Resesi Gingiva 6Document6 pagesJurnal Resesi Gingiva 6Muhammad KholisPas encore d'évaluation
- Perio GingivektomiDocument5 pagesPerio GingivektomiSafiraMaulidaPas encore d'évaluation
- Treatment of A Large Maxillary Cyst With MarsupializationDocument8 pagesTreatment of A Large Maxillary Cyst With MarsupializationDinesh SolankiPas encore d'évaluation
- Dens Evaginatus and Type V Canal Configuration: A Case ReportDocument4 pagesDens Evaginatus and Type V Canal Configuration: A Case ReportAmee PatelPas encore d'évaluation
- Case Report: Dentigerous Cyst and Canine Impaction at The Orbital FloorDocument5 pagesCase Report: Dentigerous Cyst and Canine Impaction at The Orbital FloorAmira NaufallPas encore d'évaluation
- Odontogenic Cutaneous Sinus Tract Associated With A Mandibular Second Molar Having A Rare Distolingual Root: A Case ReportDocument6 pagesOdontogenic Cutaneous Sinus Tract Associated With A Mandibular Second Molar Having A Rare Distolingual Root: A Case ReportMa NelPas encore d'évaluation
- Nasopalatine Duct Cyst - A Delayed Complication To Successful Dental Implant Placement - Diagnosis and Surgical Management - As Published in The JOIDocument6 pagesNasopalatine Duct Cyst - A Delayed Complication To Successful Dental Implant Placement - Diagnosis and Surgical Management - As Published in The JOIHashem Motahir Ali Al-ShamiriPas encore d'évaluation
- Treatment of Gummy Smile of Multifactorial Etiology: A Case ReportDocument16 pagesTreatment of Gummy Smile of Multifactorial Etiology: A Case ReportMed-Amine TouloutPas encore d'évaluation
- Exostosis MandibularDocument6 pagesExostosis MandibularCOne Gomez LinartePas encore d'évaluation
- Torus InglesDocument5 pagesTorus InglespaolaPas encore d'évaluation
- Openbite CamouflageDocument8 pagesOpenbite CamouflageRakesh RaveendranPas encore d'évaluation
- Severe Extrusion From An Apical Abscess - A Case ReportDocument4 pagesSevere Extrusion From An Apical Abscess - A Case ReportSaca AnastasiaPas encore d'évaluation
- Gummy Smile and Optimization of Dentofacial Esthetics: Muhamad Abu-Hussein Nezar Watted Azzaldeen AbdulganiDocument5 pagesGummy Smile and Optimization of Dentofacial Esthetics: Muhamad Abu-Hussein Nezar Watted Azzaldeen AbdulganiIOSRjournalPas encore d'évaluation
- Gak Jadi CaseDocument3 pagesGak Jadi CaseZahra HayunaPas encore d'évaluation
- A Case Report Using Regenerative Therapy For Generalized Aggressive PeriodontitisDocument9 pagesA Case Report Using Regenerative Therapy For Generalized Aggressive PeriodontitisripadiPas encore d'évaluation
- Dens Invaginate..Document4 pagesDens Invaginate..Hawzheen SaeedPas encore d'évaluation
- 15 D16 298 Popovska MirjanaDocument5 pages15 D16 298 Popovska MirjanaVera Radojkova NikolovskaPas encore d'évaluation
- Rehabilitation of A Complete Maxillectomy Patient: A Case Report of Osteomyelitis of MaxillaDocument6 pagesRehabilitation of A Complete Maxillectomy Patient: A Case Report of Osteomyelitis of MaxillajoephinPas encore d'évaluation
- 2.2 Valproate-Induced Gingival Overgrowth - A Case ReportDocument5 pages2.2 Valproate-Induced Gingival Overgrowth - A Case ReportRaluca ElenaPas encore d'évaluation
- A Complex Facial Trauma Case With Multiple MandibuDocument6 pagesA Complex Facial Trauma Case With Multiple MandibuIndra D KristionoPas encore d'évaluation
- Peripheral Cemento-Ossifying Fibroma - A Case Report With A Glimpse On The Differential DiagnosisDocument5 pagesPeripheral Cemento-Ossifying Fibroma - A Case Report With A Glimpse On The Differential DiagnosisnjmdrPas encore d'évaluation
- Orbital Cellulitis As A Complication of Odontogenic InfectionDocument5 pagesOrbital Cellulitis As A Complication of Odontogenic InfectionCikal Abyan Nur 1417Pas encore d'évaluation
- Benign Cementoblastoma Associated With Primary Mandibular Second MolarDocument9 pagesBenign Cementoblastoma Associated With Primary Mandibular Second Molarcahya satriaPas encore d'évaluation
- Block 2017Document10 pagesBlock 2017AngiePas encore d'évaluation
- 10866-Article Text-52118-1-10-20220425Document10 pages10866-Article Text-52118-1-10-20220425Trianita DivaPas encore d'évaluation
- Migratory and Misleading AbscessDocument4 pagesMigratory and Misleading AbscessRodrigoSolisPas encore d'évaluation
- Capstone Project PDFDocument38 pagesCapstone Project PDFapi-461805331Pas encore d'évaluation
- Benign Cementoblastoma Associated With Primary Mandibular Second MolarDocument9 pagesBenign Cementoblastoma Associated With Primary Mandibular Second Molarcahya satriaPas encore d'évaluation
- Case Report: Osteomyelitis of The Mandible After Dental Implants in An Immunocompetent PatientDocument6 pagesCase Report: Osteomyelitis of The Mandible After Dental Implants in An Immunocompetent PatientDha Dina SevofrationPas encore d'évaluation
- 243 674 1 PB PDFDocument2 pages243 674 1 PB PDFsurgaPas encore d'évaluation
- Ramsay Hunt Syndrome With Oral Findings - A Rare Case - CASE REPORT KEDUA BAGUSDocument7 pagesRamsay Hunt Syndrome With Oral Findings - A Rare Case - CASE REPORT KEDUA BAGUSfoto pasienPas encore d'évaluation
- Lichen Planus Article PDFDocument3 pagesLichen Planus Article PDFSuresh KumarPas encore d'évaluation
- Treatment of Large Thyroglossal Duct Cyst PDFDocument2 pagesTreatment of Large Thyroglossal Duct Cyst PDFNadia SalsabilaPas encore d'évaluation
- JCM 09 00576Document9 pagesJCM 09 00576GABRIELA MOLANO MEZAPas encore d'évaluation
- Css Perio IdolaDocument6 pagesCss Perio IdolanadyapuPas encore d'évaluation
- 10 1016@j Joms 2013 10 016Document11 pages10 1016@j Joms 2013 10 016Wayan Sutresna YasaPas encore d'évaluation
- Palatal and Facial Veneers To TreatDocument11 pagesPalatal and Facial Veneers To TreatSabrina Antonella Zeballos ClarosPas encore d'évaluation
- Guo Et Al 2011: Full-Mouth Rehabilitation of A Patient With Gastroesophageal Reflux Disease: A Clinical ReportDocument5 pagesGuo Et Al 2011: Full-Mouth Rehabilitation of A Patient With Gastroesophageal Reflux Disease: A Clinical Reportmoji_puiPas encore d'évaluation
- Cases Journal: Gingival Health in Relation To Clinical Crown Length: A Case ReportDocument3 pagesCases Journal: Gingival Health in Relation To Clinical Crown Length: A Case ReportBruno Adiputra Patut IIPas encore d'évaluation
- Vol06 b2 37-40strDocument4 pagesVol06 b2 37-40strDentist HerePas encore d'évaluation
- Gingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleDocument5 pagesGingival Epulis: Report of Two Cases.: Dr. Praful Choudhari, Dr. Praneeta KambleAnandPas encore d'évaluation
- Periodontal Plastic SurgeryDocument5 pagesPeriodontal Plastic Surgeryudhai170819Pas encore d'évaluation
- Periapical GranulomaDocument6 pagesPeriapical GranulomaEzza RiezaPas encore d'évaluation
- Journal Case Study ExampleDocument7 pagesJournal Case Study ExampleMAYORMITA SHEBERLYN KYEPas encore d'évaluation
- Angle Class II Malocclusion Treated Without Extractions and With Growth ControlDocument11 pagesAngle Class II Malocclusion Treated Without Extractions and With Growth ControlishtiiiPas encore d'évaluation
- Orbital Abscess During Endodontic Treatment: A Case ReportDocument3 pagesOrbital Abscess During Endodontic Treatment: A Case ReportJing XuePas encore d'évaluation
- Agenesia de Incisivo Lateral MaxilarDocument10 pagesAgenesia de Incisivo Lateral MaxilarharpsychordPas encore d'évaluation
- Dentj 38 2 02Document4 pagesDentj 38 2 02Alfonsius JeriPas encore d'évaluation
- Dental Anomaly 1Document6 pagesDental Anomaly 1Fachriza AfriPas encore d'évaluation
- GINGIVEKTOMIDocument6 pagesGINGIVEKTOMIAstrid ChrisanditaPas encore d'évaluation
- Gingival Abscess Case ReportDocument4 pagesGingival Abscess Case ReportKrishan GuliaPas encore d'évaluation
- Avoiding and Treating Dental Complications: Best Practices in DentistryD'EverandAvoiding and Treating Dental Complications: Best Practices in DentistryDeborah A. TermeiePas encore d'évaluation
- Tricuspid Atresia VivekDocument66 pagesTricuspid Atresia Vivekmihalcea alin100% (1)
- The Role of The Gut Microbiota in SepsisDocument9 pagesThe Role of The Gut Microbiota in SepsisSyahrul HamidPas encore d'évaluation
- Ankle-Brachial Index For Assessment of Peripheral Arterial DiseaseDocument5 pagesAnkle-Brachial Index For Assessment of Peripheral Arterial DiseaseindrawepePas encore d'évaluation
- Catalog Tracoe 2014 PDFDocument94 pagesCatalog Tracoe 2014 PDFLiudmila RailescuPas encore d'évaluation
- Energy Pen: MeridianDocument11 pagesEnergy Pen: Meridianjose luis lamadrid armasPas encore d'évaluation
- Camp NotesDocument17 pagesCamp NotesTeOmbre GarciaPas encore d'évaluation
- Concept MapDocument1 pageConcept MapYalante BellPas encore d'évaluation
- BESOKKKDocument5 pagesBESOKKKpt. maha rendra utamaPas encore d'évaluation
- Rogelio Ramos Vs CADocument28 pagesRogelio Ramos Vs CAAnonymous FBDGfUqHEPas encore d'évaluation
- CPG On CTGDocument5 pagesCPG On CTGТони ДиасPas encore d'évaluation
- Research Study Designs: Non-ExperimentalDocument5 pagesResearch Study Designs: Non-ExperimentalDiego TorresPas encore d'évaluation
- Veterinary Medicine: 1 HistoryDocument8 pagesVeterinary Medicine: 1 HistoryAbdalmoedAlaiashyPas encore d'évaluation
- Vanessa Hoos ResumeDocument3 pagesVanessa Hoos Resumeapi-533753716Pas encore d'évaluation
- DM - JournalDocument3 pagesDM - JournalMara Jon Ocden CasibenPas encore d'évaluation
- Haemodynamic Monitoring Learning Package: Hornsby Ku-Ring-Gai Hospital Intensive Care UnitDocument41 pagesHaemodynamic Monitoring Learning Package: Hornsby Ku-Ring-Gai Hospital Intensive Care UnitPoldo ReinaldoPas encore d'évaluation
- Congenital Postero-Medial Bowing of The Tibia and Fibula: Is Early Surgery Worthwhile?Document8 pagesCongenital Postero-Medial Bowing of The Tibia and Fibula: Is Early Surgery Worthwhile?Kaustubh KeskarPas encore d'évaluation
- Community Medicine Term 1 QBankDocument9 pagesCommunity Medicine Term 1 QBankFaiza TasneemPas encore d'évaluation
- Animal Testing: Pros and ConsDocument11 pagesAnimal Testing: Pros and ConsabhishekjainitPas encore d'évaluation
- Interview Guide QuestionsDocument3 pagesInterview Guide QuestionsYam KayePas encore d'évaluation
- Verminous Arteritis HandoutDocument1 pageVerminous Arteritis HandoutmarceeseamansPas encore d'évaluation
- Guia de Productos PDFDocument32 pagesGuia de Productos PDFJulio Cesar Ramirez OlavePas encore d'évaluation
- Kulit Emergency in DermatologyDocument47 pagesKulit Emergency in DermatologyAulia Shabrina SyukharialPas encore d'évaluation
- Vitamin D3Document29 pagesVitamin D3Ambreen AmirPas encore d'évaluation
- Chenhua Yan, MD: ChinaDocument34 pagesChenhua Yan, MD: ChinaaymenPas encore d'évaluation
- Inflammatory Breast CancerDocument6 pagesInflammatory Breast CancerHafsa ShafiquePas encore d'évaluation
- Gambaran Penggunaan Antibiotik Pada Pasien Pediatri Infeksi Saluran Pernapasan Akut (Ispa) Di Klinik Sint. Carolus BengkuluDocument8 pagesGambaran Penggunaan Antibiotik Pada Pasien Pediatri Infeksi Saluran Pernapasan Akut (Ispa) Di Klinik Sint. Carolus BengkuluLuli Corvelo SarmentoPas encore d'évaluation
- Orthostatic ToleranceDocument3 pagesOrthostatic Tolerancehajar ahmadPas encore d'évaluation