Académique Documents
Professionnel Documents
Culture Documents
Doctor
Transféré par
Ajeng Diastika WatiTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Doctor
Transféré par
Ajeng Diastika WatiDroits d'auteur :
Formats disponibles
Original Investigation
Experiences of Care Among Medicare Beneciaries With ESRD:
Medicare Consumer Assessment of Healthcare Providers and
Systems (CAHPS) Survey Results
Charlotte A.M. Paddison, PhD,
1
Marc N. Elliott, PhD,
2
Amelia M. Haviland, PhD,
3,4
Donna O. Farley, PhD,
3
Georgios Lyratzopoulos, MD,
1
Katrin Hambarsoomian, MS,
2
Jacob W. Dembosky, MPM,
3
and Martin O. Roland, DM
1
Background: Patients with end-stage renal disease (ESRD) have special health needs; little is known about
their care experiences.
Study Design: Secondary analysis of 2009-2010 Medicare Consumer Assessment of Healthcare Providers
and Systems (CAHPS) data, using representative random samples of Medicare beneciaries. Description of
Medicare beneciaries with ESRDand investigation of differences in patient experiences by sociodemographic
characteristics and coverage type.
Setting & Participants: Data were collected from 823,564 Medicare beneciaries (3,794 with ESRD) as
part of the Medicare CAHPS survey, administered by mail with telephone follow-up of nonrespondents.
Predictor: ESRD status, age, education, self-reported general and mental health status, race/ethnicity, sex,
Medicare coverage type, state of residence, and other demographic measures.
Outcomes: 6 composite measures of patient experience in 4 care domains (access to care, physician
communication, customer service, and access to prescription drugs and drug information) and 4 ratings
(overall care, personal physician, specialist physician, and prescription drug plan).
Results: Patients with ESRD reported better care experiences than non-ESRD beneciaries for 7 of 10
measures (P 0.05) after adjustment for patient characteristics, geography, and coverage type, although to
only a small extent (adjusted mean difference, 3 points [scale, 0-100]). Black patients with ESRD and less
educated patients were more likely than other patients with ESRD to report poor experiences.
Limitations: Inability to distinguish patient experiences of care for different treatment modalities.
Conclusions: On average, beneciaries with ESRD report patient experiences that are at least as positive
as non-ESRD beneciaries. However, black and less educated patients with ESRD reported worse experi-
ences than other ESRD patients. Stratied reporting of patient experience by race/ethnicity or education in
patients with ESRD can be used to monitor this disparity. Physician choice and condence and trust in
physicians may be particularly important for patients with ESRD.
Am J Kidney Dis. 61(3):440-449. 2013 by the National Kidney Foundation, Inc. Published by Elsevier Inc. All
rights reserved.
INDEX WORDS: End-stage renal disease; patient experience; race/ethnicity; Medicare; Consumer Assess-
ment of Healthcare Providers and Systems (CAHPS).
Editorial, p. 366
P
eople with end-stage renal disease (ESRD) have
complete or nearly complete kidney failure and
typically require dialysis or kidney transplantation. In
the United States, they are eligible for Medicare cover-
age regardless of age if they have worked the required
amount of time under Social Security.
1
There has been
little previous research describing the care experiences
of Medicare beneciaries with this serious chronic con-
dition.
Providing good quality of care for people with ESRD
is challenging given the cost and complexity of treat-
ment. Quality is understood best as a multidimensional
construct
2-4
informed by evidence of clinical effective-
ness, patient safety, and patient experiences. Information
for patient experiences, as measured by the Consumer
Assessment of Healthcare Providers and Systems
(CAHPS) family of surveys and other instruments, can
be used to drive improvements in quality of care,
5,6
and
as such, forms a useful complement to assessments of
clinical quality.
Pay-for-performance schemes are being used in-
creasingly to incentivize improvements in health care
quality. Under the Patient Protection and Affordable
From the
1
Cambridge Centre for Health Services Research,
Institute of Public Health, University of Cambridge, Forvie Site,
Cambridge, United Kingdom;
2
RANDCorporation, Santa Monica,
CA;
3
RAND Corporation; and
4
Heinz College, Carnegie Mellon
University, Pittsburgh, PA.
Received April 12, 2012. Accepted in revised form October 6,
2012. Originally published online November 23, 2012.
Address correspondence to Marc N. Elliott, PhD, RAND Corpo-
ration, 1776 Main St, Santa Monica, CA 90401-3208. E-mail:
marc_elliott@rand.org
2013by the National Kidney Foundation, Inc. Publishedby Elsevier
Inc. All rights reserved.
0272-6386/$36.00
http://dx.doi.org/10.1053/j.ajkd.2012.10.009
Am J Kidney Dis. 2013;61(3):440-449 440
Care Act (2010), patient experience scores will affect
quality bonuses received by Medicare Advantage
plans. These scores are derived from the Medicare
CAHPS survey, annually administered by the Centers
for Medicare & Medicaid Services (CMS) to a nation-
ally representative sample of Medicare beneciaries,
and will have nancial implications for US providers.
In contrast to the extensive research examining the
clinical quality of care provided to patients with
ESRD (eg,
7,8
), there is relatively little research exam-
ining patient-reported experiences in patients with
ESRD, most of it based on the US Renal Data System
(USRDS).
The aim of this research is to describe Medicare
beneciaries with ESRD (representing 78% of all
571,414 US individuals with ESRD in 2009
9-11
) and
their care experiences, including self-reported charac-
teristics and experiences that otherwise are not avail-
able. Our specic objectives were to investigate differ-
ences in patient experiences between Medicare
beneciaries with and without ESRD, and in those
with ESRD, to examine variation in patient experi-
ences reported by sociodemographic group and cover-
age type.
METHODS
Data Collection
Data were collected as part of the Medicare CAHPS survey,
12
which assesses patients health care experiences in a representative
random sample of 1.5% of the approximately 47 million Medi-
care beneciaries and is a mail survey with telephone follow-up of
nonrespondents. We used pooled data from the 2009-2010 Medi-
care CAHPS surveys of Medicare Advantage beneciaries and for
fee-for-service (FFS) beneciaries, with and without a free-
standing prescription drug plan. Surveys from 823,564 benecia-
ries were analyzed (FFS, 327,246; Medicare Advantage, 496,318),
including 3,794 (0.5%) with ESRD (these respondents represent
1% of all Medicare beneciaries with ESRD). The overall
response rates were 50.8% for beneciaries with ESRD and 60.9%
for others.
Patient Experience Measures
Ten measures of patients health care constitute the primary
outcomes of interest: 4 global ratings of care and 6 composite
measures. All Medicare CAHPS measures were linearly rescaled
to a possible range of 0-100 for comparability and ease of interpre-
tation, so that the transformed score y 100 (x-a)/(b-a), where
the original score x was on a scale from a to b.
Global Ratings of Care
The 4 global items were rated on a scale from 0 (worst possible
care) to 10 (best possible care). Patients were asked to rate the
health care they had received in the last 6 months. Additionally,
patients with personal physicians, Medicare prescription drug
coverage, or specialist visits in the past 6 months were asked to rate
their personal physician, prescription drug plan, or specialist,
respectively. Many patients with ESRD may consider their neph-
rologist to be their personal physician as opposed to a specialist
because 20% may have a family physician, and nephrologists
estimate they spend as much as one-third of their time with patients
with ESRD for primary care.
13-17
CompositeMeasures of Specic CareDomains
Six composite scores measured patient experiences in 4 care
domains: access, physician communication, customer services,
and prescription plan. All responses were given on a Likert scale
with options of always, usually, sometimes, or never. Each compos-
ite is the sum of its transformed constituent items.
18
Further detail
for the 6 composite measures can be found in Item S1 (provided as
online supplementary material).
Sociodemographic Characteristics, Self-rated
Health, andCoverage
The following data were obtained from the Medicare CAHPS
survey (see rst table): sex, race/ethnicity, age, education, self-
rated overall and mental health status, and proxy status. The
following information was obtained from CMS administrative
les: ESRD status, beneciarys coverage type (including Medi-
care Advantage and Special Needs Plans [for beneciaries with
certain chronic conditions or who are dually eligible for Medicare
and Medicaid] in particular), and a low income subsidy indicator
(income 150% of the federal poverty line). It was not possible to
obtain data for ESRD treatment modality (eg, whether a patient
had nondialysis-dependent chronic kidney disease, was receiving
peritoneal dialysis or hemodialysis, or was posttransplantation) or
care setting (eg, large or small hospital or clinic or patients own
home).
To assess the generalizability of the ESRD Medicare CAHPS
sample, we compared it to the distribution of characteristics of the
USRDS ESRD patient population. Since 1988, in a joint effort
with the CMS and the National Institute of Diabetes and Digestive
and Kidney Diseases, the USRDS annually collects data for the
ESRD patient population and publishes their ndings in the
Annual Data Report. We report on USRDS data from 2009, which
became available as of the 2011 USRDS Annual Data Report.
19
Analyses
To compare demographic characteristics of patients with ESRD
with those of other Medicare beneciaries, a series of bivariate
logistic regression models predicted ESRD status (present or
absent) from each of the demographic case-mix adjustors. Stan-
dard case-mix Medicare CAHPS adjustment variables include age,
education level, general and mental health status, low income
subsidy, and proxy status.
18
We additionally evaluated the associa-
tion of ESRD status with sex, race/ethnicity, and enrollment in
Medicare Advantage and Special Needs plans. For reference, a
3-point increase in some CAHPS measures on a 0-100 scale has
been associated with a 30% reduction in disenrollment from plans;
thus, one might consider differences of this magnitude to be
moderately large.
20
Next, we compared the experiences of patients with ESRD with
those of patients without ESRD, adjusting for patient characteris-
tics to control for demographic differences between the 2 groups.
First, for each of the 10 outcome measures separately, a mixed-
effects linear regression model was estimated, with ESRD status,
survey year, and each of the case-mix adjustors as independent
variables (xed effects). Random effects for state of residence and
Medicare Advantage contract (treating FFS as an additional con-
tract) controlled for location and health plan. We then estimated a
second series of identical models restricted to ESRD beneciaries
to compare the experiences of patients with ESRD with different
characteristics.
Am J Kidney Dis. 2013;61(3):440-449 441
ESRD Patient Experience
Sensitivity Analyses
We repeated the mentioned analyses in 3 ways as sensitivity
analyses: (1) substituting patients who had been told by a physician
that they had diabetes for patients with ESRD (to assess the extent to
which patterns for patients with ESRD might be typical of patients
with other chronic conditions), (2) restricting to ages 65 years and
older (because Medicare eligibility for younger than 65 years is
restricted to the disabled), and (3) using 1-to-1 matching of ESRD to
non-ESRDpatients (using the full set of covariates described).
Plan-level weights accounting for survey design and nonre-
sponse were used in all analyses, performed in SAS, version 9.2
(SAS Institute Inc), which corrected for the design effects of these
weights using the linearization method implemented by SAS
survey procedures.
21,22
RESULTS
Demographic Characteristics andSelf-ratedHealth
Table 1 lists demographic characteristics and self-
reported health for Medicare beneciaries with and
without ESRD, which are consistent with expecta-
tions. (See Item S2 for characteristics of USRDS
patients.) Respondents with ESRDincluded a substan-
tially smaller proportion of women (44% vs 56%),
white individuals (41%vs 70%), and Medicare Advan-
tage beneciaries (12% vs 23%) in comparison to
respondents without ESRD.
Beneciaries with ESRD were much more likely to
be younger than 65 years (49% vs 15% of other
beneciaries), as might be expected from eligibility
criteria that generally restrict Medicare coverage to
those 65 years and older, but provide coverage for
people meeting entitlement denitions for ESRD or
disability regardless of age. Beneciaries with ESRD
were more likely to receive a low income subsidy
(44% vs 20% of others).
Beneciaries with ESRD tended to have much worse
self-rated general health status. Almost two-thirds of those
with ESRD (64%) reported fair or poor health status com-
pared with only 32%of those without ESRD.
Similarly, 43% of USRDS patients are women. The
USRDS patient population is more likely to be white
(61%) and younger than 65 years (63%) than the
Medicare CAHPS ESRD population.
Differences inPatient Experiences by ESRDStatus
Adjusted analyses in Table 2 compare patient expe-
riences of Medicare beneciaries with ESRD with
those of other beneciaries with similar case-mix
characteristics, in similar areas, and with similar cov-
erage type. A positive estimate of the adjusted mean
difference in patient experiences of care (Medicare
CAHPS score) indicates better experiences of care for
those with ESRD than their non-ESRD counterparts.
We observed better experiences for patients with
ESRD for rating of care (0.68 point on the 0-100
scale; P 0.01), rating of physician (0.77 point; P
0.001), rating of prescription drug plan (0.98 point;
P 0.002), getting prescription drugs (0.86 point; P
0.01), getting needed care (1.05 points; P 0.001),
customer service (2.74 points; P 0.001), and getting
care quickly (2.39 points; P 0.001). These results
show that beneciaries with ESRD reported better
experiences than their non-ESRD counterparts for 7
of 10 measures, although the magnitude of these
differences between ESRD and non-ESRD benecia-
ries is small (3 points difference on a scale of
0-100). Beneciaries with ESRD did not have poorer
experiences of care than non-ESRD beneciaries on
any of the 10 experience measures considered here.
VariationinPatient Experiences by
Sociodemographics andCoverage Type
Table 3 lists adjusted mean values from the second
series of mixed-effects regressions including only
patients with ESRD and shows differences in patient
experiences of care by sociodemographics, self-rated
health, and coverage type within the ESRD group.
The most notable differences relate to race/ethnicity
and education. Black patients with ESRD reported
worse experiences versus white patients with ESRD
on rating of care (79.2 vs 81.6 points; difference,
2.4; P 0.007), rating of physician (87.1 vs 88.7
points; difference, 1.6; P 0.03), rating of special-
ist (84.6 vs 86.9 points; difference, 2.4; P 0.02),
rating of prescription drug plan (79.8 vs 81.8 points;
difference, 2.0; P 0.04), getting prescription
drugs (83.6 vs 86.3 points; difference, 2.7; P
0.008), and physician communication (86.5 vs 89.0
points; difference, 2.6; P 0.002). Patients with
ESRD who did not attend high school reported worse
experiences versus high school graduates on rating of
care (77.1 vs 81.9 points; difference, 4.7; P
0.001), getting needed care (77.2 vs 85.3 points;
difference, 8.1; P 0.001), and physician commu-
nication (85.5 vs 89.8 points; difference, 4.3; P
0.001).
Analysis of mean differences for the 3 physician
measures show that on average, black patients with
ESRD reported less positive experiences with physi-
cians than white patients (mean difference for rating
of physician, 1.6 points; for ratings of specialist, 2.4
points; and for physician communication, 2.6 points),
although the magnitude of these differences is modest
(3 points on a 0-100 scale). Black patients with
ESRD also reported more difculty getting needed
prescription drugs than white patients with ESRD
(mean difference, 2.7 points). Differences between
patients with ESRD who had not attended high school
and high school graduates are somewhat larger, rang-
ing from 4.3-8.1 points (the latter for getting needed
care). There are some differences in the experience of
Am J Kidney Dis. 2013;61(3):440-449 442
Paddison et al
Table 1. Demographic Characteristics and Health of Medicare Beneciaries With and Without ESRD, 2009-2010
Weighted Percentage
a
Unweighted No.
ESRD No ESRD P
b
ESRD No ESRD
Total (N 823,564) 3,794 819,770
Female sex 44 56 0.001 1,747 479,227
Race/ethnicity
White 41 70 0.001 1,593 560,615
Hispanic 14 7 0.001 580 76,732
Black 27 8 0.001 984 69,372
Asian/Pacic Islander 3 3 0.02 127 21,561
Native American 1 1 0.001 33 3,306
Multiracial 4 3 0.3 102 19,074
Unknown race/ethnicity 10 9 0.1 375 69,110
Care plan
Medicare Advantage 12 23 0.001 1,529 494,789
Special Needs Plans 2 3 0.07 553 95,124
Age
c
18-24 y 0 0 0.03 7 385
25-34 y 3 1 0.001 73 3,625
35-44 y 9 2 0.001 243 10,753
45-54 y 15 4 0.001 485 31,937
55-64 y 22 8 0.001 704 60,184
65-74 y 25 43 0.001 1,105 360,615
75-79 y 11 17 0.001 492 144,452
80-84 y 7 13 0.001 360 105,105
85 y 5 11 0.001 210 79,715
Educational attainment
8th grade 11 9 0.003 518 87,009
Some high school but no diploma 15 12 0.001 609 106,361
High school diploma 34 34 0.6 1,264 280,769
Some college, but no 4-y degree 27 24 0.009 904 194,302
4-y college degree only 7 9 0.005 262 68,510
4-y college degree 7 12 0.001 237 82,813
Self-rated general health status
Excellent 3 8 0.001 98 64,236
Very good 8 25 0.001 321 203,904
Good 26 36 0.001 924 294,414
Fair 40 24 0.001 1,541 199,591
Poor 24 8 0.001 910 57,625
Self-rated mental health status
Excellent 24 29 0.001 902 237,991
Very good 28 32 0.001 1,015 258,563
Good 30 26 0.001 1,160 215,413
Fair 15 11 0.001 589 87,120
Poor 3 3 0.2 128 20,682
Proxy status
Proxy respondent 5 4 0.001 212 29,194
Assistance from proxy 14 9 0.001 579 70,755
Received low-income subsidy status
d
44 20 0.001 1765 192,346
Note: Data are from 2009-2010 (N 823,564).
Abbreviation: ESRD, end-stage renal disease.
a
Individual-level weights were used to calculate weighted percentages.
b
P values correspond to logistic regressions predicting each nonimputed case-mix or characteristic indicator from an ESRD indicator.
c
Beneciaries with ESRD are shown to be younger (65 years; 49%) than non-ESRD beneciaries (65 years; 15%), and this likely is a consequence
of Medicare eligibility criteria that generally restrict coverage to those 65 years and older, but provide coverage for all people with ESRD or legal disability
regardless of age.
d
Income 150% of federal poverty line.
Am J Kidney Dis. 2013;61(3):440-449 443
ESRD Patient Experience
patients with ESRD by self-reported health, with
those in better health typically having reported better
experiences. Table 3 shows little evidence of differ-
ences in the experience of patients with ESRD by age,
sex, or coverage type.
Sensitivity Tests
Table a of Item S3 shows that patients with diabetes
generally have slightly more positive experiences
than those without diabetes (5 positive and 1 negative
difference were statistically signicant; all differences
were 1 point), smaller differences than were seen
for patients with ESRD. As is the case for ESRD,
patients with diabetes who are black and those with-
out a high school degree reported generally worse
experiences than other patients with diabetes (Table b
of Item S3). As seen in Tables c and d of Item S3,
ndings are similar when we restrict to patients 65
years and older. Finally, matching ESRD with non-
ESRD patients produces results similar to those re-
ported here.
DISCUSSION
In this study, we nd that Medicare beneciaries
with ESRD (N 3,794) report patient experiences,
on average, at least as good as experiences reported by
Medicare beneciaries without ESRD. We nd that
these Medicare patients are similar to the USRDS
population for some characteristics, although the Medi-
care ESRD sample is less likely to be white and is
more likely to be older than 65 years.
When comparing Medicare beneciaries with ESRD
with other beneciaries with similar case-mix charac-
teristics, in similar areas, and with similar coverage
type, we nd that patients with ESRD reported some-
what more positive experiences of care. Although the
magnitude of effect was small, it was directionally
consistent and was observed for 7 of the 10 measures.
There are a number of possible explanations for this
nding. We outline 2 possibilities: differences in ex-
pectations and the role of chronic conditions more
generally. First, beneciaries with and without ESRD
may have different expectations resulting from pre-
Medicare health care and health insurance experi-
ences. Beneciaries with ESRD are especially likely
to have low educational attainment. As such, a dispro-
portionate number may have had limited health insur-
ance prior to kidney failure making them eligible for
Medicare by classifying them as patients with ESRD.
Thus, Medicare coverage may represent a dramatic
improvement in coverage and care for some ESRD
beneciaries. However, ndings that in patients with
ESRD, the least educated had the worst Medicare
experiences, may cast doubt on this explanation.
Second, the positive experiences of care in Medi-
care beneciaries with ESRD may reect in part a
general pattern in patients with life-threatening non-
acute illnesses (eg, patients with cancer) to report high
satisfaction and better patient experiences than pa-
tients without such conditions.
23
Frequent contact
with the same providers over a prolonged period may
contribute to the positive experiences reported by
ESRD beneciaries. For example, many patients re-
ceiving dialysis in hospital-based outpatient centers
meet with their nephrology team 3 or more times
weekly; similarly, care after kidney transplantation
involves frequent follow-up care interactions with the
patients nephrology team. Nephrologists also have a
Table 2. Differences in Patient Experiences in Medicare Beneciaries With and Without ESRD, 2009-2010
ESRD Non-ESRD Difference (95% CI) P
Rating of care 84.89 84.20 0.68 (0.15 to 1.21) 0.01
Rating of physician 90.52 89.76 0.77 (0.29 to 1.24) 0.001
Rating of specialist 88.32 88.23 0.09 (0.48 to 0.66) 0.8
Rating of PDP 83.17 82.19 0.98 (0.36 to 1.61) 0.002
Getting prescription drugs 88.96 88.10 0.86 (0.21 to 1.51) 0.01
Getting information for drugs 79.58 79.44 0.13 (1.26 to 1.52) 0.9
Getting needed care 85.71 84.66 1.05 (0.41 to 1.69) 0.001
Customer service 81.68 78.94 2.74 (1.51 to 3.96) 0.001
Getting care quickly 71.90 69.51 2.39 (1.68 to 3.09) 0.001
Physician communication 89.75 89.51 0.24 (0.29 to 0.76) 0.4
Note: Patient experiences quantied as adjusted mean Medicare CAHPS scores. Results for ESRD indicator from linear regression
model that includes xed effects for sex, race/ethnicity (black, Hispanic, and white plus all others), indicator for 2010 survey year, and
standard Medicare CAHPS case-mix adjustors (age, education, general health status, mental health status, low income supplement,
and proxy assistance). Models include random effects for state and Medicare Advantage contract. Medicare CAHPS measures are
linearly rescaled to 0-100. Higher scores correspond to better patient experience.
Abbreviations: CAHPS, Consumer Assessment of Healthcare Providers and Systems; CI, condence interval; ESRD, end-stage
renal disease; PDP, prescription drug plan.
Am J Kidney Dis. 2013;61(3):440-449 444
Paddison et al
Table 3. Patient Experiences of Care by Sociodemographic Group in Medicare Beneciaries With ESRD
Race/Ethnicity Age (y) Education Self-rated Health Sex Coverage Type
Hispanic Black White/Other
a
55-64 65-74
a
80-84 <8th Grade
HS Grad/
GED
a
4-y College
Grad Excellent Good
a
Poor M
a
F FFS
a
MA
Rating of care
Adjusted mean 82.6 79.2 81.6 82.8 81.0 81.6 77.1 81.9 81.1 91.3 82.9 78.5 81.4 80.9 81.5 80.6
Adjusted difference 1.0 2.4 1.8 0.6 4.7 0.7 8.4 4.4 0.5 0.9
P 0.4 0.007 0.07 0.7 0.001 0.6 0.002 0.001 0.5 0.4
Rating of physician
Adjusted mean 91.1 87.1 88.7 89.4 89.1 89.1 88.8 89.7 87.1 93.1 89.3 87.2 88.5 88.9 89.4 87.6
Adjusted difference 2.4 1.6 0.2 0.0 0.9 2.6 3.9 2.1 0.4 1.8
P 0.01 0.03 0.8 0.9 0.5 0.04 0.07 0.02 0.5 0.06
Rating of specialist
Adjusted mean 88.3 84.6 86.9 87.1 87.1 87.9 84.6 87.4 86.0 84.2 87.0 86.5 86.4 86.9 87.3 85.6
Adjusted difference 1.3 2.4 0.0 0.8 2.8 1.4 2.8 0.6 0.6 1.7
P 0.3 0.02 0.9 0.7 0.08 0.3 0.4 0.6 0.4 0.2
Rating of PDP
Adjusted mean 86.8 79.8 81.8 81.2 82.4 85.7 83.0 82.1 80.2 91.7 83.1 80.8 80.7 83.6 80.6 84.0
Adjusted difference 5.0 2.0 1.2 3.4 0.9 1.9 8.6 2.3 2.9 3.4
P 0.001 0.04 0.3 0.07 0.5 0.3 0.002 0.05 0.001 0.2
Getting prescription drugs
Adjusted mean 84.1 83.6 86.3 85.5 86.2 85.1 83.8 86.1 84.5 83.3 85.6 85.5 85.0 85.4 84.5 86.0
Adjusted difference 2.1 2.7 0.7 1.1 2.2 1.6 2.3 0.0 0.4 1.4
P 0.1 0.008 0.6 0.6 0.1 0.4 0.4 0.9 0.7 0.3
Getting information for drugs
Adjusted mean 80.9 78.9 74.6 77.7 76.5 73.9 72.6 76.9 70.8 75.0 77.2 75.8 76.8 76.8 75.0 79.6
Adjusted difference 6.3 4.3 1.2 2.6 4.3 6.1 2.2 1.4 0.0 4.6
P 0.02 0.05 0.6 0.6 0.2 0.1 0.7 0.6 0.9 0.1
Getting needed care
Adjusted mean 83.9 81.5 83.1 83.3 83.7 85.9 77.2 85.3 83.4 86.6 84.1 81.9 83.0 82.7 83.3 82.1
Adjusted difference 0.8 1.6 0.4 2.2 8.1 1.9 2.5 2.2 0.3 1.2
P 0.5 0.1 0.8 0.2 0.001 0.3 0.4 0.06 0.7 0.4
Customer service
Adjusted mean 82.8 76.0 76.4 81.2 78.0 75.8 76.7 78.8 76.3 80.6 74.6 77.5 77.6 77.4 74.7 80.5
Adjusted difference 6.3 0.4 3.2 2.1 2.1 2.4 6.0 2.9 0.2 5.8
P 0.01 0.8 0.1 0.6 0.5 0.4 0.2 0.2 0.9 0.008
Getting care quickly
Adjusted mean 70.3 67.2 68.4 69.3 68.4 65.4 66.4 68.2 72.2 72.2 67.7 70.5 69.6 67.1 69.1 67.2
Adjusted difference 1.9 1.2 0.9 3.0 1.8 4.0 4.5 2.8 2.4 1.9
P 0.2 0.3 0.5 0.1 0.3 0.02 0.2 0.02 0.004 0.4
(Continued)
A
m
J
K
i
d
n
e
y
D
i
s
.
2
0
1
3
;
6
1
(
3
)
:
4
4
0
-
4
4
9
4
4
5
E
S
R
D
P
a
t
i
e
n
t
E
x
p
e
r
i
e
n
c
e
role in providing primary care for patients with ESRD,
including preventative general medical care, care for
minor acute illnesses, and care for comorbid condi-
tions (diabetes mellitus, cardiac disease, and gastroin-
testinal disease).
16
This explanation is supported in
part by a similar but weaker nding of more positive
experiences in patients with diabetes than those with-
out diabetes, given that diabetes is a chronic condition
with somewhat less intense contact with the health
care system.
We found that black ESRD beneciaries were more
likely than white beneciaries to report poor patient
experiences, a pattern that may be particular to condi-
tions such as ESRD because it does not hold consis-
tently for blacks compared with whites for the Medi-
care population as a whole.
24
Previous research
suggests racial/ethnic disparities also exist in renal
replacement therapy, including differences in referral
and initiation of dialysis therapy, adequacy of dialy-
sis, and anemia management.
25,26
There is evidence
that racial disparities persist for important clinical
outcomes, even within integrated delivery systems
such as the Veterans Administration.
27
In particular, we noted that black beneciaries
reported less positive experiences with physicians
(both personal physicians and specialists). These dif-
ferences may reect worse access to care and lower
clinical quality of care for black patients with ESRD
compared with white patients with ESRD.
28-34
In
addition, previous literature
35-37
suggests that con-
dence in ones physician is a salient issue for black
patients, and that black patients in general often may
express a preference for black physicians. Poorer
reported experiences for black patients with ESRD
may reect difculty locating a desired ethnically
concordant specialist nearby, a possibility than could
be examined in further research. Relatedly, there may
be differences by patient race/ethnicity in ease of
obtaining referrals to a specialist.
38,39
Finding a policy strategy to address the discrepan-
cies between black and nonblack patients care expe-
riences is a difcult issue, in part because of the
limited choice of nephrologists for patients with ESRD.
As noted by others, improving cross-cultural patient-
physician communication and facilitating access to a
diverse group of physicians may increase patient
involvement in care and satisfaction and improve
outcomes.
40
Adapting this principle to the ESRD
population could involve nephrologists, dialysis clin-
ics, and larger aspects of the health care system. One
key action would be implementation of regular report-
ing of differences in patient experiences of care by
race/ethnicity in Medicare beneciaries with ESRD.
Such reporting has been advocated previously
41
and
now is required at the health plan level by the Medi-
T
a
b
l
e
3
(
C
o
n
t
d
)
.
P
a
t
i
e
n
t
E
x
p
e
r
i
e
n
c
e
s
o
f
C
a
r
e
b
y
S
o
c
i
o
d
e
m
o
g
r
a
p
h
i
c
G
r
o
u
p
i
n
M
e
d
i
c
a
r
e
B
e
n
e
c
i
a
r
i
e
s
W
i
t
h
E
S
R
D
R
a
c
e
/
E
t
h
n
i
c
i
t
y
A
g
e
(
y
)
E
d
u
c
a
t
i
o
n
S
e
l
f
-
r
a
t
e
d
H
e
a
l
t
h
S
e
x
C
o
v
e
r
a
g
e
T
y
p
e
H
i
s
p
a
n
i
c
B
l
a
c
k
W
h
i
t
e
/
O
t
h
e
r
a
5
5
-
6
4
6
5
-
7
4
a
8
0
-
8
4
<
8
t
h
G
r
a
d
e
H
S
G
r
a
d
/
G
E
D
a
4
-
y
C
o
l
l
e
g
e
G
r
a
d
E
x
c
e
l
l
e
n
t
G
o
o
d
a
P
o
o
r
M
a
F
F
F
S
a
M
A
P
h
y
s
i
c
i
a
n
c
o
m
m
u
n
i
c
a
t
i
o
n
A
d
j
u
s
t
e
d
m
e
a
n
8
9
.
5
8
6
.
5
8
9
.
0
8
9
.
7
8
9
.
3
8
7
.
5
8
5
.
5
8
9
.
8
8
9
.
3
8
6
.
1
8
9
.
3
8
7
.
6
8
7
.
9
8
9
.
0
8
8
.
7
8
8
.
0
A
d
j
u
s
t
e
d
d
i
f
f
e
r
e
n
c
e
0
.
4
2
.
6
0
.
4
1
.
8
4
.
3
0
.
6
3
.
1
1
.
7
1
.
2
0
.
7
P
0
.
7
0
.
0
0
2
0
.
6
0
.
2
0
.
0
0
1
0
.
7
0
.
2
0
.
0
8
0
.
0
8
0
.
6
N
o
t
e
:
D
a
t
a
s
h
o
w
a
d
j
u
s
t
e
d
m
e
a
n
v
a
l
u
e
s
o
f
M
e
d
i
c
a
a
r
e
C
A
H
P
S
s
c
o
r
e
s
f
r
o
m
m
i
x
e
d
-
e
f
f
e
c
t
s
m
o
d
e
l
s
a
p
p
l
i
e
d
t
o
E
S
R
D
g
r
o
u
p
o
n
l
y
.
A
b
b
r
e
v
i
a
t
i
o
n
s
:
C
A
H
P
S
,
C
o
n
s
u
m
e
r
A
s
s
e
s
s
m
e
n
t
o
f
H
e
a
l
t
h
c
a
r
e
P
r
o
v
i
d
e
r
s
a
n
d
S
y
s
t
e
m
s
;
E
S
R
D
,
e
n
d
-
s
t
a
g
e
r
e
n
a
l
d
i
s
e
a
s
e
;
F
,
f
e
m
a
l
e
;
F
F
S
,
f
e
e
-
f
o
r
-
s
e
r
v
i
c
e
;
G
E
D
,
G
e
n
e
r
a
l
E
d
u
c
a
t
i
o
n
D
e
v
e
l
o
p
m
e
n
t
c
e
r
t
i
c
a
t
e
;
g
r
a
d
,
g
r
a
d
u
a
t
e
;
H
S
,
h
i
g
h
s
c
h
o
o
l
;
M
,
m
a
l
e
;
M
A
,
M
e
d
i
c
a
r
e
A
d
v
a
n
t
a
g
e
;
P
D
P
,
p
r
e
s
c
r
i
p
t
i
o
n
d
r
u
g
p
l
a
n
.
a
R
e
f
e
r
e
n
c
e
g
r
o
u
p
.
Am J Kidney Dis. 2013;61(3):440-449 446
Paddison et al
care Improvements for Patients and Providers Act of
2008.
In addition, the least educated ESRD beneciaries
reported poorer physician communication and care,
also a pattern that may be particular to ESRD and
other chronic conditions and may reect the complex-
ity of ESRD care. Although it also holds for patients
with diabetes, it does not hold consistently for the
Medicare population as a whole.
42
Because lowhealth
literacy is most common in those with low educa-
tional attainment,
43
this nding may point to the need
to improve health literacy in ESRD beneciaries and
make the process of care and physician interactions
more accommodating of patients with ESRD with low
health literacy.
Consistent with previous studies of non-ESRD pa-
tient populations,
44,45
we found that ESRD benecia-
ries in better self-reported health are more likely to
report positive experiences of care. Previous research
also has indicated some differences in patient-
reported experiences of care by coverage type.
Ratings of physicians tend to be higher in FFS than
Medicare Advantage in general, perhaps because of
the greater ability to see a physician of ones
choosing in FFS, whereas prescription drug and
customer service typically are more positive in Medi-
care Advantage than in FFS.
24,46,47
However, in ESRD
beneciaries in this study, we found no consistent
tendency for more positive experiences in Medicare
Advantage or FFS, perhaps reecting that provisions
for the care of patients with ESRD are relatively
uniform and independent of coverage type.
Strengths of this study include data from a large
nationally representative survey of patient experi-
ences (Medicare CAHPS), which enable us to de-
scribe the characteristics of Medicare beneciaries
with ESRD and their experiences of care and also to
compare Medicare beneciaries with and without
ESRD. Although response rates were 51% for ESRD
and 61% for non-ESRD beneciaries, recent analyses
of these and other CAHPS data have not found
evidence of nonresponse bias when case-mix adjust-
ment is used.
44,48
There also are some limitations. The Medicare
ESRD beneciary group is not perfectly representa-
tive of the USRDS patient population: in particular,
the ESRD beneciary group is older and more likely
to be white than all USRDS patients. Despite being
one of the largest surveys of ESRD patients experi-
ences (N 3,794), the study may still have been
underpowered to detect small between-group differ-
ences within the ESRD beneciary group. We were
unable to obtain data to distinguish between patient
experiences for subgroups of ESRD patients differ-
ent treatment (eg, patients with advanced kidney dis-
ease who were not yet receiving renal replacement
therapy, those treated with peritoneal dialysis or hemo-
dialysis, and patients with a functioning kidney trans-
plant) or between patients treated in different settings
(eg, home, small regional hospital, or large teaching
hospital). It is possible that there is sociodemographic
variation in the experience of patients with ESRD
treated by different modalities or in different settings.
Finally, patients with ESRD have less access to Medi-
care Advantage plans than non-ESRD patients; only a
limited number of ESRD-specic Special Needs Plans
are available to those with pre-existing ESRD, whereas
other Medicare beneciaries may choose from a large
number of general Medicare Advantage plans. Further
research is needed to distinguish among several com-
peting explanations for this studys results; the CMS-
sponsored In-Center Hemodialysis CAHPS Survey,
which began implementation as of late 2012, may
provide such an opportunity.
In conclusion, it is encouraging to learn from our
study that on average, beneciaries with ESRD report
patient experiences at least comparable with non-
ESRD beneciaries. However, we also found some
evidence of sociodemographic differences in patient
care experiences, with black and less educated ESRD
Medicare beneciaries reporting poorer experiences
of care than other beneciaries with ESRD. Educa-
tional outreach, efforts targeting physician supply and
patient choice, and measurement of patient experi-
ences according to sociodemographic subgroups may
reduce these differences.
ACKNOWLEDGEMENTS
The authors thank Aneetha Ramadas, AB, and Daisy Montfort,
AB, of the RAND Corporation for assistance with manuscript
preparation as part of compensated employment and Roberto
Vargas, MD, for comments on an earlier version of this manu-
script.
Support: This study was funded by CMS contract HHSM-500-
2005-00028I to RAND Corporation. Dr Elliott and Dr Farley were
supported in part by a cooperative agreement from the Agency for
Healthcare Research and Quality U18 HS016980.
Financial Disclosure: The authors declare that they have no
other relevant nancial interests.
SUPPLEMENTARY MATERIAL
Item S1. Detail on 6 composite measures assessing patient
experiences in 4 specic domains of care.
Item S2. Treatment modalities and characteristics of USRDS
ESRD patients.
Item S3. Additional analyses for diabetic subgroups and bene-
ciaries 65 years and older.
Note: The supplementary material accompanying this article
(http://dx.doi.org/10.1053/j.ajkd.2012.10.009) is available at
www.ajkd.org.
Am J Kidney Dis. 2013;61(3):440-449 447
ESRD Patient Experience
REFERENCES
1. Centers for Medicare & Medicaid Services. Medicare Cover-
age of Kidney Dialysis and Kidney Transplant Services. Baltimore,
MD: Centers for Medicare & Medicaid Services; 2011.
2. Campbell SM, Roland MO, Buetow SA. Dening quality of
care. Soc Sci Med. 2000;51(11):1611-1625.
3. Cleary PD, Edgman-Levitan S. Health care quality. JAMA.
1997;278(19):1608-1612.
4. Donabedian A. The quality of care. JAMA. 1988;260(12):
1743-1748.
5. Browne K, Roseman D, Shaller D, Edgman-Levitan S.
Measuring patient experience as a strategy for improving primary
care. Health Aff (Millwood). 2010;29(5):921-925.
6. Picker Institute Europe. Improving patient experience. 2011.
http://www.pickereurope.org/improvingpatientexperience. Ac-
cessed April 1, 2011.
7. Lacson E Jr, Wang W, DeVries C, et al. Effects of a nation-
wide predialysis educational program on modality choice, vascular
access, and patient outcomes. Am J Kidney Dis. 2011;58(2):235-
246.
8. Zhang Y, Cotter DJ, Thamer M. The effect of dialysis chains
on mortality among patients receiving hemodialysis. Health Serv
Res. 2011;46(3):747-767.
9. Centers for Medicare & Medicaid Services. Data Compen-
dium: 2010 Edition. Baltimore, MD: Centers for Medicare &
Medicaid Services; 2010.
10. Charnow JA. ESRD population continues to rise. Ren Urol
News. 2011. http://www.renalandurologynews.com/esrd-population-
continues-to-rise/article/214930/. Accessed June 15, 2012.
11. Centers for Medicare & Medicaid Services. Data Compen-
dium: 2011 Edition Baltimore, MD: Centers for Medicare &
Medicaid Services; 2011.
12. Centers for Medicare & Medicaid Services. Consumer
Assessment of Health Providers & Systems (CAHPS): Overview.
Baltimore, MD: Centers for Medicare & Medicaid Services; 2011.
13. Nespor SL, Holley JL. Patients on hemodialysis rely on
nephrologists and dialysis units for maintenance health care.
ASAIO J. 1992;38(3):M279-M281.
14. Holley JL, Nespor SL. Nephrologist-directed primary health
care in chronic dialysis patients. Am J Kidney Dis. 1993;21(6):628-
631.
15. Shah N, Dahl NV, Kapoian T, Sherman RA, Walker JA. The
nephrologist as a primary care provider for the hemodialysis
patient. Int Urol Nephrol. 2005;37(1):113-117.
16. Bender FH, Holley JL. Most nephrologists are primary care
providers for chronic dialysis patients: results of a national survey.
Am J Kidney Dis. 1996;28(1):67-71.
17. Zimmerman DL, Selick A, Singh R, Mendelssohn DC.
Attitudes of Canadian nephrologists, family physicians and pa-
tients with kidney failure toward primary care delivery for chronic
dialysis patients. Nephrol Dial Transplant. 2003;18(2):305-309.
18. Martino SC, Elliott MN, Cleary PD, et al. Psychometric
properties of an instrument to assess Medicare beneciaries
prescription drug plan experiences. Health Care Financ Rev.
2009;30(3):41-53.
19. US Renal Data System. USRDS 2011 Annual Data Report:
Atlas of Chronic Kidney Disease and End-Stage Renal Disease in
the United States. Am J Kidney Dis. 2012;59(1)(suppl 1):e1-e420.
20. Lied TR, Sheingold SH, Landon BE, Shaul JA, Cleary
PD. Beneciary reported experience and voluntary disenroll-
ment in Medicare managed care. Health Care Financ Rev.
2003;25(1):55-66.
21. Graubard B, Korn E. Modeling the sampling design in the
analysis of health surveys. Stat Methods Med Res. 1996;5:263-
281.
22. Woolridge JM. Econometric Analysis of Cross Section and
Panel Data. Cambridge, MA: MIT Press; 2002.
23. Department of Health (UK). National Cancer Patient Expe-
rience Survey Programme: 2010 National Survey Report. London,
England: Department of Health; 2010.
24. Elliott MN, Haviland AM, Orr N, Hambarsoomian K,
Cleary PD. How do the experiences of Medicare beneciary
subgroups differ between managed care and original Medicare.
Health Serv Res. 2011;46(4):1039-1058.
25. Gadegbeku C, Freeman M, Agodoa L. Racial disparities in
renal replacement therapy. J Natl Med Assoc. 2002;94(8 suppl):45S-
54S.
26. Klassen AC, Hall AG, Saksvig B, Curbow B, Klassen DK.
Relationship between patients perceptions of disadvantage and
discrimination and listing for kidney transplantation. Am J Public
Health. 2002;92(5):811-817.
27. Trivedi AN, Grebla RC, Wright SM, Washington DL.
Despite improved quality of care in the Veterans Affairs health
system, racial disparitiy persists for important clinical outcomes.
Health Aff (Millwood). 2011;30(4):707-714.
28. Churak JM. Racial and ethnic disparities in renal transplan-
tation. J Natl Med Assoc. 2005;97(2):153-160.
29. Chakkera HA, OHare AM, Johansen KL, et al. Inuence of
race on kidney transplant outcomes within and outside the Depart-
ment of Veterans Affairs. J Am Soc Nephrol. 2005;16(1):269-277.
30. Owen WF, Szczech LA, Frankeneld DL. Healthcare sys-
teminterventions for inequality in quality: corrective action through
evidence-based medicine. J Natl Med Assoc. 2002;94(8):83s-91s.
31. Leonard MB, Stablein DM, Ho M, Jabs K, Feldman HI.
Racial and center differences in hemodialysis adequacy in children
treated at pediatric centers: a North American Pediatric Renal
Transplant Cooperative Study (NAPRTCS) report. J Am Soc
Nephrol. 2004;15(11):2923-2932.
32. Weisbord SD, Fried LF, Mor MK, et al. Associations of race
and ethnicity with anemia management among patients initiating
renal replacement therapy. J Natl Med Assoc. 2007;99(11):1218-
1226.
33. Stolzmann KL, Bautista LE, Gangnon RE, McElroy JA,
Becker BN, Remington PL. Trends in kidney transplantation rates
and disparities. J Natl Med Assoc. 2007;99(8):923-932.
34. Omoloja A, Stol A, Mitsnefes M. Racial differences in
pediatric renal transplantation24-year single center experience.
J Natl Med Assoc. 2006;98(2):154-157.
35. Keating NL, Gandhi TK, Orav EJ, Bates DW, Ayanian JZ.
Patient characteristics and experiences associated with trust in
specialist physicians. Arch Intern Med. 2004;164(9):1015-1020.
36. Saha S, Komaromy M, Koepsell TD, Bindman AB. Patient-
physician racial concordance and the perceived quality and use of
health care. Arch Intern Med. 1999;159(9):997-1004.
37. Barr DA. Race/ethnicity and patient satisfaction. J Gen
Intern Med. 2004;19(9):937-943.
38. Rettig R, Vargas R, Norris K, Nissenson AR. A quiet
revolution in nephrology. Nephrol News Issues. 2010;24(12):18-
19, 23.
39. Nguyen GC, LaVeist TA, Harris ML, Wang MH, Datta LW,
Brant SR. Racial disparities in utilization of specialist care and
medications in inammatory bowel disease. Am J Gastroenterol.
2010;105(10):2202-2208.
40. Cooper-Patrick L, Gallo JJ, Gonzales JJ, et al. Race, gender,
and partnership in the patient-physician relationship. JAMA. 1999;
282(6):583-589.
41. Fiscella K, Franks P, Gold MR, Clancy CM. Inequality in
quality: addressing socioeconomic, racial, and ethnic disparities in
health care. JAMA. 2000;282(19):2579-2053.
42. Elliott MN, Haviland AM, Kanouse DE, Hambarsoomian
K, Hays RD. Adjusting for subgroup differences in extreme
Am J Kidney Dis. 2013;61(3):440-449 448
Paddison et al
response tendency in ratings of health care: impact on disparity
estimates. Health Serv Res. 2009;44(2, pt 1):542-561.
43. Martin LT, Ruder T, Escarce JJ, et al. Developing predictive
models of health literacy. J Gen Intern Med. 2009;24(11):1211-1216.
44. Elliott MN, Zaslavsky AM, Goldstein E, et al. Effects of
survey mode, patient mix, and nonresponse on CAHPS
Hospital
Survey scores. Health Serv Res. 2009;44:501-518.
45. OMalley AJ, Zaslavsky AM, Elliott MN, Zaborski L,
Cleary PD. Case-mix adjustment of the CAHPS Hospital Survey.
Health Serv Res. 2005;40(6):2163-2181.
46. Keenan PS, Elliott MN, Cleary PD, Zaslavsky AM, Landon
BE. Quality assessments by sick and health beneciaries in tradi-
tional Medicare and Medicare managed care. Med Care. 2009;47(8):
882-888.
47. Landon BE, Zaslavsky AM, Bernard SL, Ciof MJ,
Cleary PD. Comparison of performance of traditional Medicare
vs. Medicare managed care. JAMA. 2004;291(14):1744-1752.
48. Klein DJ, Elliott MN, Haviland AM, et al. Understanding
nonresponse to the 2007 Medicare CAHPS Survey. Gerontologist.
2011;51(6):843-855.
Am J Kidney Dis. 2013;61(3):440-449 449
ESRD Patient Experience
Vous aimerez peut-être aussi
- Textbook of Urgent Care Management: Chapter 42, Evaluation and Management of Coding and DocumentationD'EverandTextbook of Urgent Care Management: Chapter 42, Evaluation and Management of Coding and DocumentationPas encore d'évaluation
- Fenton (2012) - The Cost of Satisfaction - A National Study of Patient Satisfaction, Health Care Utilization, Expenditures, and MortalityDocument7 pagesFenton (2012) - The Cost of Satisfaction - A National Study of Patient Satisfaction, Health Care Utilization, Expenditures, and Mortalityghcabsb87Pas encore d'évaluation
- Precision Medicine Oncology: A PrimerD'EverandPrecision Medicine Oncology: A PrimerLorna Rodriguez-RodriguezPas encore d'évaluation
- Savs SdvawfaDocument9 pagesSavs SdvawfakennydimitraPas encore d'évaluation
- Meeting the Needs of Older Adults with Serious Illness: Challenges and Opportunities in the Age of Health Care ReformD'EverandMeeting the Needs of Older Adults with Serious Illness: Challenges and Opportunities in the Age of Health Care ReformAmy S. KelleyPas encore d'évaluation
- 464 FullDocument7 pages464 FullLorand RusPas encore d'évaluation
- RoleDocument8 pagesRolePutra EkaPas encore d'évaluation
- Monica Vansuch, James M Naessens, Robert J Stroebel, Jeanne M Huddleston, and Arthur R WilliamsDocument10 pagesMonica Vansuch, James M Naessens, Robert J Stroebel, Jeanne M Huddleston, and Arthur R WilliamsLuigi Prada GuzmanPas encore d'évaluation
- Screening Elders For Risk of Hospital Admission (1993)Document7 pagesScreening Elders For Risk of Hospital Admission (1993)Timothy TanPas encore d'évaluation
- J Aem 2007 06 035Document8 pagesJ Aem 2007 06 035kingkinresmytaPas encore d'évaluation
- Expectations of Multiple Sclerosis Patients and Their Families: A Qualitative Study in IranDocument7 pagesExpectations of Multiple Sclerosis Patients and Their Families: A Qualitative Study in IranpipitingesPas encore d'évaluation
- Nursing HealthcareDocument8 pagesNursing HealthcareBrobafettPas encore d'évaluation
- Kim2013 Article Self-reportedMedicalMorbidityA OJODocument8 pagesKim2013 Article Self-reportedMedicalMorbidityA OJOMariaLisseth MoralesPas encore d'évaluation
- HCM 340 7-2Document11 pagesHCM 340 7-2Robin McFaddenPas encore d'évaluation
- Journal Review Final PaperDocument10 pagesJournal Review Final Paperapi-464793486Pas encore d'évaluation
- Nej Ms A 0804116Document11 pagesNej Ms A 0804116FazaKhilwanAmnaPas encore d'évaluation
- Predictive Analytics in Health CareDocument8 pagesPredictive Analytics in Health Carezarcone7Pas encore d'évaluation
- Choosing Between Hospitals: The Influence of The Experiences of Other PatientsDocument15 pagesChoosing Between Hospitals: The Influence of The Experiences of Other PatientsYonathan ArdhanaPas encore d'évaluation
- Exploration of The Relationship Between Continuity, Trust in Regular Doctors and Patient Satisfaction With Consultations With Family DoctorsDocument7 pagesExploration of The Relationship Between Continuity, Trust in Regular Doctors and Patient Satisfaction With Consultations With Family DoctorsBently JohnsonPas encore d'évaluation
- Health Affairs: For Reprints, Links & Permissions: E-Mail Alerts: To SubscribeDocument11 pagesHealth Affairs: For Reprints, Links & Permissions: E-Mail Alerts: To SubscribeDesak ErnaPas encore d'évaluation
- Low-Patient-Social-SupportDocument9 pagesLow-Patient-Social-SupportshegawPas encore d'évaluation
- Emergency Department Waiting Room: Many Requests, Many Insured and Many Primary Care Physician ReferralsDocument7 pagesEmergency Department Waiting Room: Many Requests, Many Insured and Many Primary Care Physician ReferralsSyed ShahPas encore d'évaluation
- Comparing Unmet Needs To Optimize Quality Characterizing Inpatient and Outpatient Palliative Care PopulationsDocument10 pagesComparing Unmet Needs To Optimize Quality Characterizing Inpatient and Outpatient Palliative Care PopulationsAdams MaltaPas encore d'évaluation
- Characteristics of Frequent Attenders at A Community Health CenterDocument11 pagesCharacteristics of Frequent Attenders at A Community Health CenterjlventiganPas encore d'évaluation
- The Economic Burden of Fragile X Syndrome:: Healthcare Resource Utilization in The United StatesDocument11 pagesThe Economic Burden of Fragile X Syndrome:: Healthcare Resource Utilization in The United StatesUzyPas encore d'évaluation
- Pi Is 0741521414007095Document12 pagesPi Is 0741521414007095Irina NeamtuPas encore d'évaluation
- Clinical Practice Guidelines and Quality of Care For Older Patients With Multiple Comorbid DiseasesDocument9 pagesClinical Practice Guidelines and Quality of Care For Older Patients With Multiple Comorbid DiseasesBiblioteca Centro Médico De Mar del PlataPas encore d'évaluation
- Medical Conditions and Medication Use in A US Dental School Clinic PopulationDocument6 pagesMedical Conditions and Medication Use in A US Dental School Clinic PopulationLina Marcela LuceroPas encore d'évaluation
- Hayward EvaluationGenericScreens 1993Document10 pagesHayward EvaluationGenericScreens 1993Dauna Apriansa Anggoro PutriPas encore d'évaluation
- End of Life Care For Lung CancerDocument7 pagesEnd of Life Care For Lung CancerPhilip R. MarallagPas encore d'évaluation
- Physician-Patient Colorectal Cancer Screening Discussions by Physicians' Screening RatesDocument5 pagesPhysician-Patient Colorectal Cancer Screening Discussions by Physicians' Screening RatesRizki YaniesPas encore d'évaluation
- Prognosis Pneumonia PDFDocument18 pagesPrognosis Pneumonia PDFamania jeumpa nur alamPas encore d'évaluation
- Nurse and Physician Barriers To Spiritual CareDocument11 pagesNurse and Physician Barriers To Spiritual CareacbcarolPas encore d'évaluation
- 10 1016@j Jclinepi 2004 04 005Document8 pages10 1016@j Jclinepi 2004 04 005ari_julian94Pas encore d'évaluation
- Gade 2008Document11 pagesGade 2008Agustina IturriPas encore d'évaluation
- Management Arteriosclerosis and ClaudicationDocument41 pagesManagement Arteriosclerosis and ClaudicationLuqman AlwiPas encore d'évaluation
- Short ReportDocument2 pagesShort Reportscribdnotes123Pas encore d'évaluation
- HR Action ResearchDocument7 pagesHR Action ResearchChristel DilleraPas encore d'évaluation
- Teunis Sen 2016Document19 pagesTeunis Sen 2016Ekfatil MardiyahPas encore d'évaluation
- 1365-Article Text-8141-1-4-20210610Document16 pages1365-Article Text-8141-1-4-20210610Maabena AsantePas encore d'évaluation
- MCWK 1Document5 pagesMCWK 1ANDREWPas encore d'évaluation
- Preferences of Iranians To Select The Emergency Department Physician at The Time of Service Delivery - Nargesi Et Al. 2021Document7 pagesPreferences of Iranians To Select The Emergency Department Physician at The Time of Service Delivery - Nargesi Et Al. 2021LuciaPas encore d'évaluation
- Submitted 30 July 2021, Accepted 18 October 2022 AbstractDocument7 pagesSubmitted 30 July 2021, Accepted 18 October 2022 Abstractfahrunsiddik5Pas encore d'évaluation
- AtingaDocument6 pagesAtingaBudi Syamsul ArifinPas encore d'évaluation
- 281 FullDocument9 pages281 FullReRe DomilaPas encore d'évaluation
- Special Article: The Care of Hiv-Infected Adults in The United StatesDocument8 pagesSpecial Article: The Care of Hiv-Infected Adults in The United StatesByaruhanga EmmanuelPas encore d'évaluation
- 2010 - The Association of Health Literacy and Socio-Demographic Factors With Medication KnowledgeDocument5 pages2010 - The Association of Health Literacy and Socio-Demographic Factors With Medication KnowledgeGONDHES CHANNELPas encore d'évaluation
- JCO 2006 Koroukian 2304 10Document7 pagesJCO 2006 Koroukian 2304 10Yuliana Eka SintaPas encore d'évaluation
- Bekele ChakaDocument74 pagesBekele ChakaDoods QuemadaPas encore d'évaluation
- Study ProposalDocument4 pagesStudy Proposalarchana jhaPas encore d'évaluation
- Patient and Clinician Perceptions of Precision Cardiology Care: Findings From The HeartCare StudyDocument10 pagesPatient and Clinician Perceptions of Precision Cardiology Care: Findings From The HeartCare StudyJoban PhulkaPas encore d'évaluation
- Preprint Not Peer ReviewedDocument18 pagesPreprint Not Peer Reviewedinno semuPas encore d'évaluation
- Academic Emergency Medicine - 2008 - Hobgood - Medical Errors What and When What Do Patients Want To KnowDocument8 pagesAcademic Emergency Medicine - 2008 - Hobgood - Medical Errors What and When What Do Patients Want To Knowqualitymalak660Pas encore d'évaluation
- Perfil Sociodemográfico e Padrão de Utilização de Serviços de Saúde para Usuários e Não-Usuários Do SUS - PNAD 2003Document12 pagesPerfil Sociodemográfico e Padrão de Utilização de Serviços de Saúde para Usuários e Não-Usuários Do SUS - PNAD 2003Joao BonfimPas encore d'évaluation
- Future ImplicationsDocument2 pagesFuture ImplicationsConsuelo MolinaPas encore d'évaluation
- USRDS 2019 ES FinalDocument64 pagesUSRDS 2019 ES FinalEdi HidayatPas encore d'évaluation
- Primary Care Consultations About Medically Unexplained Symptoms How Do Patients Indicate What They WantDocument7 pagesPrimary Care Consultations About Medically Unexplained Symptoms How Do Patients Indicate What They WantrenatavescoviPas encore d'évaluation
- Pharmaceutical CareDocument22 pagesPharmaceutical CarefikebatuPas encore d'évaluation
- Burden and Quality of Life of Caregivers For Hemodialysis PatientsDocument8 pagesBurden and Quality of Life of Caregivers For Hemodialysis PatientsAsim EisaPas encore d'évaluation
- Annals of General PsychiatryDocument9 pagesAnnals of General PsychiatryPutu Agus GrantikaPas encore d'évaluation
- Learning Logs 2Document9 pagesLearning Logs 2api-240988800Pas encore d'évaluation
- Extrapyramidal System DisordersDocument41 pagesExtrapyramidal System DisordersAyshe SlocumPas encore d'évaluation
- Drug Study Magnesium SulfateDocument3 pagesDrug Study Magnesium SulfateSchyna Marielle VitalePas encore d'évaluation
- GeneXpert PosterDocument1 pageGeneXpert PosterRisqon Anjahiranda AdiputraPas encore d'évaluation
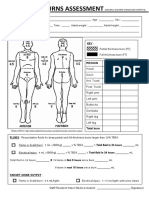
- Burn Assessment CMU PDFDocument2 pagesBurn Assessment CMU PDFmegamindPas encore d'évaluation
- T2 Sains KSSM (Section B &C)Document15 pagesT2 Sains KSSM (Section B &C)Azreen Syazwani Azmi100% (1)
- Ocular Trauma - BantaDocument211 pagesOcular Trauma - BantaLuisa Fernanda Arboleda100% (1)
- Megan Fobar - Case Study AbstractDocument2 pagesMegan Fobar - Case Study Abstractapi-288109471Pas encore d'évaluation
- Journal of Chronic PainDocument8 pagesJournal of Chronic PainRirin TriyaniPas encore d'évaluation
- Lesson Plan BrochodilatorsDocument14 pagesLesson Plan BrochodilatorsVaishali SinghPas encore d'évaluation
- Public Health ModelDocument10 pagesPublic Health ModelSurendra SanapPas encore d'évaluation
- Toxicology-Handbook PDFDocument2 pagesToxicology-Handbook PDFssb channelPas encore d'évaluation
- Biosafety and Bioethics of Biotechnology ABS-832: DR Attya Bhatti Assistant Professor Head of Department Asab-NustDocument25 pagesBiosafety and Bioethics of Biotechnology ABS-832: DR Attya Bhatti Assistant Professor Head of Department Asab-NustAviation MedicinePas encore d'évaluation
- Literature Review Low Birth WeightDocument4 pagesLiterature Review Low Birth Weightc5qx9hq5100% (1)
- Self Care Management and Puberty Health IssuesDocument10 pagesSelf Care Management and Puberty Health IssuesIan Atienza0% (1)
- Quisted en P Menopausicas Guias GTG - 34 PDFDocument32 pagesQuisted en P Menopausicas Guias GTG - 34 PDFAdela Marìa P LPas encore d'évaluation
- New England Journal Medicine: The ofDocument11 pagesNew England Journal Medicine: The ofahmadto80Pas encore d'évaluation
- HR Policy ManualDocument34 pagesHR Policy Manualshamna AbdullaPas encore d'évaluation
- Bpac CRP Vs Esr Poem 2005 WVDocument14 pagesBpac CRP Vs Esr Poem 2005 WVTanveerPas encore d'évaluation
- Mathis Et. Al. Intraoperative MV & PPCDocument17 pagesMathis Et. Al. Intraoperative MV & PPCJun HungPas encore d'évaluation
- A New Approach To Treating Pain With: Comra TherapyDocument16 pagesA New Approach To Treating Pain With: Comra Therapygbg@polka.co.zaPas encore d'évaluation
- Dental BiofilmsDocument44 pagesDental BiofilmsRamona MateiPas encore d'évaluation
- Short Increment Sensitivity Index Test (SISI)Document2 pagesShort Increment Sensitivity Index Test (SISI)Anish RajPas encore d'évaluation
- I. Objectives: GeneralDocument36 pagesI. Objectives: GeneralSharlaine CabanayanPas encore d'évaluation
- Applied Pharmacology For The Dental Hygienist 7th Edition Haveles Solutions ManualDocument24 pagesApplied Pharmacology For The Dental Hygienist 7th Edition Haveles Solutions ManualJosephCraiggmax100% (50)
- 1 CervixDocument12 pages1 Cervixzianab aliPas encore d'évaluation
- Nursing Care Plan Ineffective Breathing Pattern Hepatic MassDocument2 pagesNursing Care Plan Ineffective Breathing Pattern Hepatic MassRheegell Ellar-Fuertes100% (3)
- 3 PBDocument9 pages3 PBSusana Tito LuceroPas encore d'évaluation
- Biodiversity of Micro-OrganismsDocument32 pagesBiodiversity of Micro-Organismsapi-20234922250% (2)
- Ok Urologi Maret 2021 Minggu IDocument25 pagesOk Urologi Maret 2021 Minggu ILittle DevPas encore d'évaluation
- The Obesity Code: Unlocking the Secrets of Weight LossD'EverandThe Obesity Code: Unlocking the Secrets of Weight LossÉvaluation : 4 sur 5 étoiles4/5 (6)
- The Age of Magical Overthinking: Notes on Modern IrrationalityD'EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityÉvaluation : 4 sur 5 étoiles4/5 (28)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsD'EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsPas encore d'évaluation
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeD'EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeÉvaluation : 2 sur 5 étoiles2/5 (1)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDD'EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDÉvaluation : 5 sur 5 étoiles5/5 (2)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionD'EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionÉvaluation : 4 sur 5 étoiles4/5 (404)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsD'EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsÉvaluation : 5 sur 5 étoiles5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisD'EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisÉvaluation : 4.5 sur 5 étoiles4.5/5 (42)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedD'EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedÉvaluation : 5 sur 5 étoiles5/5 (81)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsD'EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsÉvaluation : 3.5 sur 5 étoiles3.5/5 (3)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisD'EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisÉvaluation : 4 sur 5 étoiles4/5 (1)
- Why We Die: The New Science of Aging and the Quest for ImmortalityD'EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityÉvaluation : 4 sur 5 étoiles4/5 (3)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaD'EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- The Comfort of Crows: A Backyard YearD'EverandThe Comfort of Crows: A Backyard YearÉvaluation : 4.5 sur 5 étoiles4.5/5 (23)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningD'EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningÉvaluation : 4 sur 5 étoiles4/5 (3)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)D'EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Pas encore d'évaluation
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisD'EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisÉvaluation : 3.5 sur 5 étoiles3.5/5 (2)
- Gut: the new and revised Sunday Times bestsellerD'EverandGut: the new and revised Sunday Times bestsellerÉvaluation : 4 sur 5 étoiles4/5 (392)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryD'EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryÉvaluation : 4 sur 5 étoiles4/5 (44)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.D'EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Évaluation : 4.5 sur 5 étoiles4.5/5 (110)
- The Marshmallow Test: Mastering Self-ControlD'EverandThe Marshmallow Test: Mastering Self-ControlÉvaluation : 4.5 sur 5 étoiles4.5/5 (58)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessD'EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessÉvaluation : 4.5 sur 5 étoiles4.5/5 (328)
- Dark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingD'EverandDark Psychology: Learn To Influence Anyone Using Mind Control, Manipulation And Deception With Secret Techniques Of Dark Persuasion, Undetected Mind Control, Mind Games, Hypnotism And BrainwashingÉvaluation : 4 sur 5 étoiles4/5 (1138)
- Troubled: A Memoir of Foster Care, Family, and Social ClassD'EverandTroubled: A Memoir of Foster Care, Family, and Social ClassÉvaluation : 4.5 sur 5 étoiles4.5/5 (27)