Académique Documents
Professionnel Documents
Culture Documents
Engineering Renal
Transféré par
Ayesha RalliyaCopyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Engineering Renal
Transféré par
Ayesha RalliyaDroits d'auteur :
Formats disponibles
Regeneration of Renal Tissues
T. Aboushwareb, J.J. Yoo, A. Atala
Contents
60.1
Introduction . . . . . . . . . . . . . . . . . . . . . . . . 869
60.2
Basic Components . . . . . . . . . . . . . . . . . . . 869
60.3
Approaches for Renal Tissue Regeneration 870
60.3.1 Developmental Approaches . . . . . . . . . . . . 870
60.3.2 Tissue Engineering Approaches . . . . . . . . . 871
60.4
Regeneration of Functional Tissue In Vivo 872
60.5
Summary . . . . . . . . . . . . . . . . . . . . . . . . . . 874
References . . . . . . . . . . . . . . . . . . . . . . . . . 874
60.1
Introduction
The kidney is a vital and complex organ that performs many critical functions [13]. It is responsible
for filtering the bodys wastes, such as urea, from the
blood and excreting them as urine. In addition to the
excretory function, the kidney maintains the bodys
homeostasis by regulating acid-base balance, blood
pressure, and plasma volume. Moreover, it synthesizes 1, 25 vitamin D3, erythropoietin, glutathione,
and free radical scavenging enzymes. It is also known
that the kidney participates in the catabolism of low
molecular weight proteins and in the production and
regulation of cytokines [46].
There are many conditions where the kidney
functions are diminished and these lead to renal
failure. End stage renal failure is a devastating condition which involves multiple organs in affected
60
individuals. Although dialysis can prolong survival
via filtration, other kidney functions are not replaced,
leading to long-term consequences such as anemia
and malnutrition [2, 3, 7]. Currently, renal transplantation is the only definitive treatment that can restore
full kidney function. However, transplantation has
several limitations, such as critical donor shortage,
complications due to chronic immunosuppressive
therapy and graft failure [2, 3, 7].
The limitations of current therapies for renal
failure have led investigators to explore the development of alternative therapeutic modalities that
could improve, restore, or replace renal function.
The emergence of cell-based therapies using tissue
engineering and regenerative medicine strategies has
presented alternative possibilities for the management of pathologic renal conditions [1, 713]. The
concept of kidney cell expansion followed by cell
transplantation using tissue engineering and regenerative medicine techniques has been proposed as a
method to augment either isolated or total renal function. Despite the fact that the kidney is considered to
be one of the more challenging organs to regenerate
and/or reconstruct, investigative advances made to
date have been promising [8, 1012].
60.2
Basic Components
The unique structural and cellular heterogeneity
present within the kidney creates many challenges
for tissue regeneration. The system of nephrons and
870
collecting ducts within the kidney is composed of
multiple functionally and morphologically distinct
segments. For this reason, appropriate conditions
need to be provided for the long-term survival, differentiation, and growth of many types of cells. Recent efforts in the area of kidney tissue regeneration
have focused on the development of a reliable cell
source [1419]. In addition, optimal growth conditions have been extensively investigated to provide
an adequate enrichment to achieve stable renal cell
expansion systems [2024].
Isolation of particular cell types that produce specific factors, such as erythropoietin, may be a good
approach for selective cell therapies. However, total renal function would not be achieved using this
approach. To create kidney tissue that would deliver
full renal function, a culture containing all of the cell
types comprising the functional nephron units should
be used. Optimal culture conditions to nurture renal
cells have been extensively studied and the cells
grown under these conditions have been reported
to maintain their cellular characteristics [25]. Furthermore, renal cells placed in a three-dimensional
culture environment are able to reconstitute renal
structures.
Recent investigative efforts in the search for a reliable cell source have been expanded to stem and
progenitor cells. The use of these cells for tissue regeneration is attractive due to their ability to differentiate and mature into specific cell types required for
regeneration. This is particularly useful in instances
where primary renal cells are unavailable due to extensive tissue damage. Bone marrow-derived human
mesenchymal stem cells have been shown to be a potential source because they can differentiate into several cell lineages [14, 15, 18]. These cells have been
shown to participate in kidney development when
they are placed in a rat embryonic niche that allows
for continued exposure to a repertoire of nephrogenic
signals [19]. These cells, however, were found to
contribute mainly to regeneration of damaged glomerular endothelial cells after injury. In addition, the
major cell source of kidney regeneration was found
to originate from intrarenal cells in an ischemic renal
injury model [14, 17]. Another potential cell source
for kidney regeneration is circulating stem cells,
which have been shown to transform into tubular and
glomerular epithelial cells, podocytes, mesangial
cells, and interstitial cells after renal injury [15, 16,
T. Aboushwareb, J.J. Yoo, A. Atala
2630]. These observations suggest that controlling
stem and progenitor cell differentiation may lead to
successful regeneration of kidney tissues.
Although isolated renal cells are able to retain
their phenotypic and functional characteristics in
culture, transplantation of these cells in vivo may not
result in structural remodeling that is appropriate for
kidney tissue. In addition, cell or tissue components
cannot be implanted in large volumes as diffusion
of oxygen and nutrients is limited [31]. Thus, a cellsupport matrix, preferably one that encourages angiogenesis, is necessary to allow diffusion across the
entire implant. A variety of synthetic and naturally
derived materials have been examined in order to determine the ideal support structures for regeneration
[9, 3235]. Biodegradable synthetic materials, such
as poly-lactic and poly-glycolic acid polymers, have
been used to provide structural support for cells.
Synthetic materials can be easily fabricated and configured in a controlled manner, which make them attractive options for tissue engineering. However, naturally derived materials, such as collagen, laminin,
and fibronectin, are much more biocompatible and
provide a similar extracellular matrix environment to
normal tissue. For this reason, collagen-based scaffolds have been used in many applications [3639].
60.3
Approaches for Renal
Tissue Regeneration
60.3.1
Developmental Approaches
Transplantation of a kidney precursor, such as the
metanephros, into a diseased kidney has been proposed as a possible method for achieving functional
restoration. In an animal study, human embryonic
metanephroi, transplanted into the kidneys of an immune deficient mouse model, developed into mature
kidneys [40]. The transplanted metanephroi produced urine-like fluid but failed to develop ureters.
This study suggests that development of an in vitro
system in which metanephroi could be grown may
lead to transplant techniques that could produce a
Chapter 60 Regeneration of Renal Tissues
small replacement kidney within the host. In another
study, the metanephros was divided into mesenchymal tissue and ureteral buds, and each of the tissue
segments was cultured in vitro [41]. After 8days in
culture, each portion of the mesenchymal tissues had
grown to the original size. A similar method was
used for ureteral buds, which also propagated. These
results indicate that if the mesenchyme and ureteral
buds were placed together and cultured in vitro, a
metanephros-like structure would develop. This suggests that the metanephros could be propagated under optimal conditions.
In another study, transplantation of metanephroi
into a nonimmunosuppressed rat omentum showed
that the implanted metanephroi are able to undergo
differentiation and growth that is not confined by a
tight organ capsule [42]. When the metanephroi with
an intact ureteric bud were implanted, the metanephroi
were able to enlarge and become kidney-shaped tissue within 3 weeks. The metanephroi transplanted
into the omentum were able to develop into kidney
tissue structures with a well-defined cortex and medulla. Mature nephrons and collecting system structures are shown to be indistinguishable from those of
normal kidneys by light or electron microscopy [43].
Moreover, these structures become vascularized via
arteries that originate at the superior mesenteric artery of the host [43]. It has been demonstrated that
the metanephroi transplanted into the omentum survive for up to 32weeks post implantation [44]. These
studies show that the developmental approach may
be a viable option for regenerating renal tissue for
functional restoration.
60.3.2
Tissue Engineering Approaches
The ability to grow and expand cells is one of the
essential requirements in engineering tissues. The
feasibility of achieving renal cell growth, expansion,
and in vivo reconstitution using tissue engineering
techniques was investigated [9]. Donor rabbit kidneys were removed and perfused with a nonoxide
solution which promoted iron particle entrapment in
the glomeruli. Homogenization of the renal cortex
and fractionation in 83 and 210 micron sieves with
871
subsequent magnetic extraction yielded three separate purified suspensions of distal tubules, glomeruli,
and proximal tubules. The cells were plated separately in vitro and after expansion, were seeded onto
biodegradable polyglycolic acid scaffolds and implanted subcutaneously into host athymic mice. This
included implants of proximal tubular cells, glomeruli, distal tubular cells, and a mixture of all three cell
types. Animals were sacrificed at 1 week, 2 weeks,
and 1month after implantation and the retrieved implants were analyzed. An acute inflammatory phase
and a chronic foreign body reaction were seen, accompanied by vascular ingrowth by 7days after implantation. Histologic examination demonstrated progressive formation and organization of the nephron
segments within the polymer fibers with time. Renal
cell proliferation in the cell-polymer scaffolds was
detected by in vivo labeling of replicating cells with
the thymidine analog bromodeoxyuridine [17]. BrdU
incorporation into renal cell DNA was confirmed using monoclonal anti-BrdU antibodies. These results
demonstrated that renal specific cells can be successfully harvested and cultured, and can subsequently
attach to artificial biodegradable polymers. The renal
cell-polymer scaffolds can be implanted into host
animals where the cells replicate and organize into
nephron segments, as the polymer, which serves as a
cell delivery vehicle, undergoes biodegradation.
Initial experiments showed that implanted cellpolymer scaffolds gave rise to renal tubular structures. However, it was unclear whether the tubular
structures reconstituted de novo from dispersed
renal elements, or if they merely represented fragments of donor tubules which survived the original
dissociation and culture processes intact. Further investigation was conducted in order to examine the
process [45]. Mouse renal cells were harvested and
expanded in culture. Subsequently, single isolated
cells were seeded on biodegradable polymers and
implanted into immune competent syngeneic hosts.
Renal epithelial cells were observed to reconstitute
into tubular structures in vivo. Sequential analyses
of the retrieved implants over time demonstrated that
renal epithelial cells first organized into a cord-like
structure with a solid center. Subsequent canalization
into a hollow tube could be seen by 2 weeks. Histologic examination with nephron-segment-specific
lactins showed successful reconstitution of proximal tubules, distal tubules, loop of Henle, collecting
872
tubules, and collecting ducts. These results showed
that single suspended cells are capable of reconstituting into tubular structures, with homogeneous cell
types within each tubule.
60.4
Regeneration of Functional
Tissue In Vivo
The kidneys are critical to body homeostasis because
of their excretory, regulatory, and endocrine functions. The excretory function is initiated by filtration
of blood at the glomerulus, and the regulatory function is provided by the tubular segments. Although
our prior studies demonstrated that renal cells seeded
on biodegradable polymer scaffolds are able to
form some renal structures in vivo, complete renal
function could not be achieved in these studies. In
a subsequent study we sought to create a functional
artificial renal unit which could produce urine [46].
Mouse renal cells were harvested, expanded in culture, and seeded onto a tubular device constructed
from polycarbonate [39]. The tubular device was
connected at one end to a silastic catheter which terminated into a reservoir. The device was implanted
subcutaneously in athymic mice. The implanted
devices were retrieved and examined histologically
and immunocytochemically at 1, 2, 3, 4 and 8weeks
after implantation. Fluid was collected from inside
the implant, and uric acid and creatinine levels were
determined.
T. Aboushwareb, J.J. Yoo, A. Atala
Histological examination of the implanted device demonstrated extensive vascularization as well
as formation of glomeruli and highly organized
tubule-like structures. Immunocytochemical staining with antiosteopontin antibody, which is secreted
by proximal and distal tubular cells and the cells of
the thin ascending loop of Henle, stained the tubular
sections. Immunohistochemical staining for alkaline
phosphatase stained proximal tubule-like structures.
Uniform staining for fibronectin in the extracellular
matrix of newly formed tubes was observed. The
fluid collected from the reservoir was yellow and
contained 66mg/dl uric acid (as compared to 2mg/dl
in plasma) suggesting that these tubules are capable
of unidirectional secretion and concentration of uric
acid. The creatinine assay performed on the collected
fluid showed an 8.2-fold increase in concentration, as
compared to serum. These results demonstrated that
single cells from multicellular structures can become
organized into functional renal units that are able to
excrete high levels of solutes through a urine-like
fluid [46].
To determine whether renal tissue could be formed
using an alternative cell source, nuclear transplantation (therapeutic cloning) was performed to generate
histocompatible tissues, and the feasibility of engineering syngeneic renal tissues in vivo using these
cloned cells was investigated [25]. Nuclear material
from bovine dermal fibroblasts was transferred into
unfertilized enucleated donor bovine eggs. Renal
cells from the cloned embryos were harvested, expanded in vitro, and seeded onto three-dimensional
renal devices (Fig. 60.1a). The devices were implanted into the back of the same steer from which
Fig.60.1ac Formation of functional renal tissue in vivo. a Renal device. b Tissue-engineered renal unit shows the accumulation of urine-like fluid. c There was a clear unidirectional continuity between the mature glomeruli, their tubules, and the
polycarbonate membrane
Chapter 60 Regeneration of Renal Tissues
the cells were cloned, and were retrieved 12weeks
later. This process produced functioning renal units.
Urine production and viability were demonstrated
after transplantation back into the nuclear donor
animal (Fig. 60.1b). Chemical analysis suggested
unidirectional secretion and concentration of urea
nitrogen and creatinine. Microscopic analysis revealed formation of organized glomeruli and tubular
structures (Fig. 60.1c). Immunohistochemical and
RT-PCR analysis confirmed the expression of renal
mRNA and proteins, whereas delayed-type hypersensitivity testing and in vitro proliferative assays
showed that there was no rejection response to the
cloned cells. This study indicates that the cloned renal cells are able to form and organize into functional
tissue structures which are genetically the same as
the host. Generating immune-compatible cells using
therapeutic cloning techniques is feasible and may be
useful for the engineering of renal tissues for autologous applications.
In our previous study, we showed that renal cells
seeded on synthetic renal devices attached to a collecting system are able to form functional renal units
that produce urine-like fluid. However, a naturally
derived tissue matrix with existing three-dimensional
kidney architecture would be preferable, because it
would allow for transplantation of a larger number
of cells, resulting in greater renal tissue volumes.
Thus, we developed an acellular collagen-based
kidney matrix, which is identical to the native renal
architecture. In a subsequent study we investigated
whether these collagen-based matrices could accommodate large volumes of renal cells and form kidney
structures in vivo [47].
Acellular collagen matrices, derived from porcine kidneys, were obtained through a multistep decellularization process. During this process, serial
evaluation of the matrix for cellular remnants was
performed using histochemistry, scanning electron
microscopy (SEM) and RT-PCR. Mouse renal cells
were harvested, grown, and seeded on 80 of the decellularized collagen matrices at a concentration of
30106 cells/ml. Forty cell-matrix constructs grown
in vitro were analyzed 3days, 1, 2, 4, and 6weeks after seeding. The remaining 40 cell-containing matrices were implanted in the subcutaneous space of 20
athymic mice. The animals were sacrificed 3days, 1,
2, 4, 8, and 24weeks after implantation for analyses.
873
Gross, SEM, histochemical, immunocytochemical,
and biochemical analyses were performed.
Scanning electron microscopy and histologic examination confirmed the acellularity of the processed
matrix. RT-PCR performed on the kidney matrices
demonstrated the absence of any RNA residues. Renal cells seeded on the matrix adhered to the inner
surface and proliferated to confluency 7 days after
seeding, as demonstrated by SEM. Histochemical
and immunocytochemical analyses performed using
H & E, periodic acid Schiff, alkaline phosphatase,
antiosteopontin and anti-CD-31 identified stromal,
endothelial, and tubular epithelial cell phenotypes
within the matrix. Renal tubular and glomerulus-like
structures were observed 8weeks after implantation.
MTT proliferation and titrated thymidine incorporation assays performed 6 weeks after cell seeding
demonstrated a population increase of 116% and
92%, respectively, as compared to the 2-week time
points. This study demonstrates that renal cells are
able to adhere to and proliferate on the collagenbased kidney matrices. The renal cells reconstitute
renal tubular and glomeruli-like structures in the
kidney-shaped matrix. The collagen-based kidney
matrix system seeded with renal cells may be useful
in the future for augmenting renal function.
However, creation of renal structures without the
use of an artificial device system would be preferable, as implantation procedures are invasive and may
result in unnecessary complications. We also investigated the feasibility of creating three-dimensional
renal structures for in situ implantation within the native kidney tissue. Primary renal cells from 4-weekold mice were grown and expanded in culture. These
renal cells were labeled with fluorescent markers and
injected into mouse kidneys in a collagen gel for in
vivo formation of renal tissues. Collagen injection
without cells and sham-operated animals served as
controls. In vitro reconstituted renal structures and
in vivo implanted cells were retrieved and analyzed.
The implanted renal cells formed tubular and glomerular structures within the kidney tissue, as confirmed by the fluorescent markers. There was no
evidence of renal tissue formation in the control and
the sham-operated groups. These results demonstrate
that single renal cells are able to reconstitute kidney
structures when placed in a collagen-based scaffolding system. The implanted renal cells are able to
874
T. Aboushwareb, J.J. Yoo, A. Atala
Fig.60.2a,b Reconstitution of kidney structures. The implanted renal cells self assembled into (a) glomerular and (b) tubular
structures within the kidney tissue
self assemble into tubular and glomerular structures
within the kidney tissue (Fig. 60.2). These findings
suggest that this system may be the preferred approach to engineer functional kidney tissues for the
treatment of end stage renal disease.
60.5
Summary
The increasing demand for renal transplantation,
combined with the critical shortage of donor organs,
has ignited intense interest in seeking alternative
treatment modalities. Cell-based approaches have
been proposed as a viable method for kidney tissue
regeneration. Various tissue engineering and regenerative medicine approaches that aim to achieve
functional intra- and extracorporeal kidney support
were presented in this chapter. Although the progress
in this area has been somewhat successful toward
regeneration of functional kidney tissue, clinical application of this technology is still distant.
The concept of renal cell transplantation has been
demonstrated on multiple occasions. It has been
shown that renal cells are able to reconstitute into
functional kidney tissues in vivo, but numerous challenges must be addressed and solved in order for
these techniques to be applied clinically. Some of
these challenges include the generation of a large tissue mass that could augment systemic renal function,
the formation of adequate vascularization in the engineered renal tissue, and the development of a reliable renal failure model system for testing cell-based
technologies.
References
1. Amiel, G. E., Yoo, J. J., Atala, A.: Renal therapy using
tissue-engineered constructs and gene delivery. World J
Urol, 18: 71, 2000
2. Chazan, J. A., Libbey, N. P., London, M. R. et al.: The
clinical spectrum of renal osteodystrophy in 57 chronic
hemodialysis patients: a correlation between biochemical parameters and bone pathology findings. Clin Nephrol, 35: 78, 1991
3. Cohen, J., Hopkin, J., Kurtz, J.: Infectious complications
after renal transplantation Philadelphia, WB Saunders,
1994
4. Frank, J., Engler-Blum, G., Rodemann, H. P. et al.: Human renal tubular cells as a cytokine source: PDGF-B,
GM-CSF and IL-6 mRNA expression in vitro. Exp Nephrol, 1: 26, 1993
5. Maack, T.: Renal handling of low molecular weight proteins. Am J Med, 58: 57, 1975
6. Stadnyk, A. W.: Cytokine production by epithelial cells.
Faseb J, 8: 1041, 1994
7. Amiel, G. E., Yoo, J. J. and Atala, A.: Renal tissue engineering using a collagen-based kidney matrix. Tissue
Engineering suppl, 2000
8. Amiel, G. E., Atala, A.: Current and future modalities for
functional renal replacement. Urol Clin North Am, 26:
235, 1999
9. Atala, A., Schlussel, R. N., Retik, A. B: Renal cell growth
in vivo after attachment to biodegradable polymer scaffolds. J Urol, 153, 1995
Chapter 60 Regeneration of Renal Tissues
10. Atala, A.: Tissue engineering in the genitourinary system. Vol chap 8, 1997
11. Atala, A.: Future perspectives in reconstructive surgery
using tissue engineering. Urol Clin North Am, 26: 157,
1999
12. Humes, H. D., Buffington, D. A., MacKay, S. M. et al.:
Replacement of renal function in uremic animals with a
tissue-engineered kidney. Nat Biotechnol, 17: 451, 1999
13. Humes, H. D., Fissell, W. H., Weitzel, W. F. et al.: Metabolic replacement of kidney function in uremic animals
with a bioartificial kidney containing human cells. Am J
Kidney Dis, 39: 1078, 2002
14. Ikarashi, K., Li, B., Suwa, M. et al.: Bone marrow cells
contribute to regeneration of damaged glomerular endothelial cells. Kidney Int, 67: 1925, 2005
15. Kale, S., Karihaloo, A., Clark, P. R. et al.: Bone marrow
stem cells contribute to repair of the ischemically injured
renal tubule. J Clin Invest, 112: 42, 2003
16. Lin, F., Cordes, K., Li, L. et al.: Hematopoietic stem cells
contribute to the regeneration of renal tubules after renal
ischemia-reperfusion injury in mice. J Am Soc Nephrol,
14: 1188, 2003
17. Lin, F., Moran, A., Igarashi, P.: Intrarenal cells, not bone
marrow-derived cells, are the major source for regeneration in postischemic kidney. J Clin Invest, 115: 1756,
2005
18. Prockop, D. J.: Marrow stromal cells as stem cells for
nonhematopoietic tissues. Science, 276: 71, 1997
19. Yokoo, T., Ohashi, T., Shen, J. S. et al.: Human mesenchymal stem cells in rodent whole-embryo culture are
reprogrammed to contribute to kidney tissues. Proc Natl
Acad Sci U S A, 102: 3296, 2005
20. Carley, W. W., Milici, A. J., Madri, J. A.: Extracellular
matrix specificity for the differentiation of capillary endothelial cells. Exp Cell Res, 178: 426, 1988
21. Horikoshi, S., Koide, H., Shirai, T.: Monoclonal antibodies against laminin A chain and B chain in the human and
mouse kidneys. Lab Invest, 58: 532, 1988
22. Humes, H. D., Cieslinski, D. A.: Interaction between
growth factors and retinoic acid in the induction of kidney tubulogenesis in tissue culture. Exp Cell Res, 201: 8,
1992
23. Milici, A. J., Furie, M. B., Carley, W. W.: The formation
of fenestrations and channels by capillary endothelium in
vitro. Proc Natl Acad Sci U S A, 82: 6181, 1985
24. Schena, F. P.: Role of growth factors in acute renal failure. Kidney Int Suppl, 66: S11, 1998
25. Lanza, R. P., Chung, H. Y., Yoo, J. J. et al.: Generation
of histocompatible tissues using nuclear transplantation.
Nat Biotechnol, 20: 689, 2002
26. Gupta, S., Verfaillie, C., Chmielewski, D. et al.: A role
for extrarenal cells in the regeneration following acute
renal failure. Kidney Int, 62: 1285, 2002
27. Ito, T., Suzuki, A., Imai, E. et al.: Bone marrow is a reservoir of repopulating mesangial cells during glomerular
remodeling. J Am Soc Nephrol, 12: 2625, 2001
28. Iwano, M., Plieth, D., Danoff, T. M. et al.: Evidence that
fibroblasts derive from epithelium during tissue fibrosis.
J Clin Invest, 110: 341, 2002
875
29. Poulsom, R., Forbes, S. J., Hodivala-Dilke, K. et al.:
Bone marrow contributes to renal parenchymal turnover
and regeneration. J Pathol, 195: 229, 2001
30. Rookmaaker, M. B., Smits, A. M., Tolboom, H. et al.:
Bone-marrow-derived cells contribute to glomerular endothelial repair in experimental glomerulonephritis. Am
J Pathol, 163: 553, 2003
31. Folkman, J., Hochberg, M.: Self-regulation of growth in
three dimensions. J Exp Med, 138: 745, 1973
32. Atala, A., Bauer, S. B., Soker, S. et al.: Tissue-engineered
autologous bladders for patients needing cystoplasty.
Lancet, 367: 1241, 2006
33. El-Kassaby, A. W., Retik, A. B., Yoo, J. J. et al.: Urethral
stricture repair with an off-the-shelf collagen matrix. J
Urol, 169: 170, 2003
34. Oberpenning, F., Meng, J., Yoo, J. J. et al.: De novo reconstitution of a functional mammalian urinary bladder
by tissue engineering. Nat Biotechnol, 17: 149, 1999
35. Tachibana, M., Nagamatsu, G. R., Addonizio, J. C.: Ureteral replacement using collagen sponge tube grafts. J
Urol, 133: 866, 1985
36. Freed, L. E., Vunjak-Novakovic, G., Biron, R. J. et al.:
Biodegradable polymer scaffolds for tissue engineering.
Biotechnology (N Y), 12: 689, 1994
37. Hubbell, J. A., Massia, S. P., Desai, N. P. et al.: Endothelial cell-selective materials for tissue engineering in the
vascular graft via a new receptor. Biotechnology (N Y),
9: 568, 1991
38. Mooney, D. J., Mazzoni, C. L., Breuer, C. et al.: Stabilized polyglycolic acid fibre-based tubes for tissue engineering. Biomaterials, 17: 115, 1996
39. Wald, H. L., Sarakinos, G., Lyman, M. D. et al.: Cell
seeding in porous transplantation devices. Biomaterials,
14: 270, 1993
40. Dekel, B., Burakova, T., Arditti, F. D. et al.: Human
and porcine early kidney precursors as a new source for
transplantation. Nat Med, 9: 53, 2003
41. Steer, D. L., Bush, K. T., Meyer, T. N. et al.: A strategy
for in vitro propagation of rat nephrons. Kidney Int, 62:
1958, 2002
42. Rogers, S. A., Lowell, J. A., Hammerman, N. A. et al.:
Transplantation of developing metanephroi into adult
rats. Kidney Int, 54: 27, 1998
43. Hammerman, M. R.: Transplantation of embryonic kidneys. Clin Sci (Lond), 103: 599, 2002
44. Rogers, S. A., Powell-Braxton, L., Hammerman, M. R.:
Insulin-like growth factor I regulates renal development
in rodents. Dev Genet, 24: 293, 1999
45. Fung, L. C. T., Elenius, K., Freeman, M., Donovan, M.
J., Atala, A.: Reconstitution of poor EGFr-poor renal
epithelial cells into tubular structures on biodegradable
polymer scaffold. Pediatrics, 98 (Suppl): S631, 1996
46. Yoo, J. J., Ashkar, S., Atala, A.: Creation of functional
kidney structures with excretion of kidney-like fluid in
vivo. Pediatrics, 98S: 605, 1996
47. Yoo, J. J., Atala, A.: A novel gene delivery system using urothelial tissue engineered neo-organs. J Urol, 158:
1066, 1997
Vous aimerez peut-être aussi
- Regenerative Medicine Applications in Organ TransplantationD'EverandRegenerative Medicine Applications in Organ TransplantationPas encore d'évaluation
- Kidney Repair and Stem Cells: A Complex and Controversial ProcessDocument8 pagesKidney Repair and Stem Cells: A Complex and Controversial ProcessTara SanderPas encore d'évaluation
- 1 B. Teknologi Sel Punca Terapi HatiDocument12 pages1 B. Teknologi Sel Punca Terapi HatiarisPas encore d'évaluation
- Materials: Scaffold Characteristics For Functional Hollow Organ RegenerationDocument23 pagesMaterials: Scaffold Characteristics For Functional Hollow Organ RegenerationroyPas encore d'évaluation
- Liver RegenerationDocument262 pagesLiver RegenerationJosé Ramírez100% (1)
- Technical ReportsDocument8 pagesTechnical ReportsalecssterPas encore d'évaluation
- Tissue EngineeringDocument12 pagesTissue EngineeringDevanand GuptaPas encore d'évaluation
- Organ Reconstruction: Dream or Reality For The Future: J.-F. Stoltz, L. Zhang, J.S. Ye and N. de IslaDocument7 pagesOrgan Reconstruction: Dream or Reality For The Future: J.-F. Stoltz, L. Zhang, J.S. Ye and N. de IslaRuxandra BadiuPas encore d'évaluation
- Regen EndoDocument88 pagesRegen EndoJitender ReddyPas encore d'évaluation
- Tissue Engineering: From Wikipedia, The Free EncyclopediaDocument12 pagesTissue Engineering: From Wikipedia, The Free EncyclopediaAnonymous ytZsBOVPas encore d'évaluation
- Tissue EngineeringDocument9 pagesTissue EngineeringbogdanotiPas encore d'évaluation
- Tissue Engineering - Wikipedia, The Free EncyclopediaDocument10 pagesTissue Engineering - Wikipedia, The Free EncyclopediaBenni WewokPas encore d'évaluation
- Tissue Engineered Urinary ConduitsDocument9 pagesTissue Engineered Urinary ConduitsNajwa PortofPas encore d'évaluation
- Anatomy (2Document25 pagesAnatomy (2Zohaib AmjadPas encore d'évaluation
- HemodialysisDocument3 pagesHemodialysisgabxyzPas encore d'évaluation
- StocumDocument5 pagesStocumLucía Carolina VidalPas encore d'évaluation
- d6e449ece855f3bbdd4ac6b61cadd242Document12 pagesd6e449ece855f3bbdd4ac6b61cadd242B VeerendrasaiPas encore d'évaluation
- Sabetkish 2020Document9 pagesSabetkish 2020asparaginaaacPas encore d'évaluation
- (Re) Building A KidneyDocument9 pages(Re) Building A KidneyUlisesPas encore d'évaluation
- Comparing the Therapeutic Potential of Stem CellsDocument30 pagesComparing the Therapeutic Potential of Stem CellsAnaaya SinghaniaPas encore d'évaluation
- Tissue EngineeringDocument8 pagesTissue EngineeringJimsPas encore d'évaluation
- Advances in Tissue EngineeringDocument10 pagesAdvances in Tissue EngineeringarisPas encore d'évaluation
- Cell Transplantation-Based Regenerative Medicine in Liver DiseasesDocument18 pagesCell Transplantation-Based Regenerative Medicine in Liver DiseasesalumnogustaPas encore d'évaluation
- Application of Tissue EngineeringDocument3 pagesApplication of Tissue Engineeringtahomag44Pas encore d'évaluation
- 2016 - Zhou Et AlDocument14 pages2016 - Zhou Et AlAfranio Cogo DestefaniPas encore d'évaluation
- J Cellular Molecular Medi - 2014 - Liu - The Multiple Functional Roles of Mesenchymal Stem Cells in Participating inDocument10 pagesJ Cellular Molecular Medi - 2014 - Liu - The Multiple Functional Roles of Mesenchymal Stem Cells in Participating indr. RiyanPas encore d'évaluation
- NIH Public Access: Author ManuscriptDocument13 pagesNIH Public Access: Author Manuscriptbdvd1007092Pas encore d'évaluation
- Liver Regeneration by Hematopoietic Stem Cells: Have We Reached The End of The Road?Document23 pagesLiver Regeneration by Hematopoietic Stem Cells: Have We Reached The End of The Road?Morana JaganjacPas encore d'évaluation
- Ryan Agsunod Undergraduate Honors ThesisDocument51 pagesRyan Agsunod Undergraduate Honors Thesisapi-496617876Pas encore d'évaluation
- Knee Stem CellsDocument25 pagesKnee Stem CellsKN TMPas encore d'évaluation
- 2017-Ozougwuj C 2017Document13 pages2017-Ozougwuj C 2017DebPas encore d'évaluation
- Ureteral ReconstructionDocument6 pagesUreteral ReconstructiongumPas encore d'évaluation
- Metabolic Status of Pluripotent Cells Andexploitation For Growth in Stirred SuspensionbioreactorsDocument8 pagesMetabolic Status of Pluripotent Cells Andexploitation For Growth in Stirred SuspensionbioreactorsArianna CastroPas encore d'évaluation
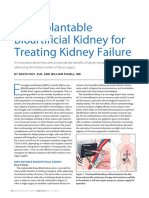
- An Implantable Bioartificial Kidney For Treating Kidney FailureDocument2 pagesAn Implantable Bioartificial Kidney For Treating Kidney FailureAnugrah Pangeran100% (1)
- CARDIOVASCULAR TISSUE ENGINEERINGDocument10 pagesCARDIOVASCULAR TISSUE ENGINEERINGArpit MaheshwariPas encore d'évaluation
- Research Article in Vitro and in VivoDocument14 pagesResearch Article in Vitro and in VivoVILEOLAGOLDPas encore d'évaluation
- Bio-artificial liver systems support acute liver failure patientsDocument8 pagesBio-artificial liver systems support acute liver failure patientsRijy LorancePas encore d'évaluation
- Basic PathologyDocument35 pagesBasic Pathologyshinichi kudoPas encore d'évaluation
- The Comprehensive Review On The Approach of Kidney Regeneration Using Stem CellsDocument10 pagesThe Comprehensive Review On The Approach of Kidney Regeneration Using Stem CellsIJRASETPublicationsPas encore d'évaluation
- 383 2018 Article 4373Document6 pages383 2018 Article 4373Anjas HappyprayogaPas encore d'évaluation
- Artículo Semana 03 InglesDocument12 pagesArtículo Semana 03 InglesSofia :DPas encore d'évaluation
- TMP AED3Document13 pagesTMP AED3FrontiersPas encore d'évaluation
- jurnal toxicDocument47 pagesjurnal toxicMuh ImranPas encore d'évaluation
- Regeneration Endodontics (1) - 1Document29 pagesRegeneration Endodontics (1) - 1شامخ شموخ الجبالPas encore d'évaluation
- J Tissue Eng Regen Med - 2016 - Stefani - A double chamber rotating bioreactor for enhanced tubular tissue generation fromDocument11 pagesJ Tissue Eng Regen Med - 2016 - Stefani - A double chamber rotating bioreactor for enhanced tubular tissue generation fromjielingPas encore d'évaluation
- @@@ Regenerating Tubular Epithelial Cells of The KidneyDocument8 pages@@@ Regenerating Tubular Epithelial Cells of The KidneyeullobaPas encore d'évaluation
- Gholobova Et Al. - Biofabrication - 2020 - Functional Evaluation of Prevascularization in One-Stage Versus Two-Stage Tissue EngineeriDocument19 pagesGholobova Et Al. - Biofabrication - 2020 - Functional Evaluation of Prevascularization in One-Stage Versus Two-Stage Tissue EngineeriLievenPas encore d'évaluation
- TherapeuticsDocument11 pagesTherapeuticsFilipa LagoaPas encore d'évaluation
- 04 Ijpscr 121 23Document7 pages04 Ijpscr 121 23BRNSS Publication Hub InfoPas encore d'évaluation
- Liver Regeneration (PDFDrive)Document261 pagesLiver Regeneration (PDFDrive)Kapetan AhavPas encore d'évaluation
- Bmri2014 473536Document10 pagesBmri2014 473536Lê HằngPas encore d'évaluation
- Tissue Engineering: Kavya Thilakan MSC Biotechnology - Semester IIIDocument23 pagesTissue Engineering: Kavya Thilakan MSC Biotechnology - Semester IIIRahul PillaiPas encore d'évaluation
- Technological Institute of The Philippines - Manila: 363 P. Casal ST., Quiapo, ManilaDocument4 pagesTechnological Institute of The Philippines - Manila: 363 P. Casal ST., Quiapo, ManilaZeny NaranjoPas encore d'évaluation
- Desenvolvimento Do FígadoDocument15 pagesDesenvolvimento Do Fígadocopiasmed semvirusPas encore d'évaluation
- Bio-Electrospraying and Cell Electrospinning: Progress and Opportunities For Basic Biology and Clinical SciencesDocument8 pagesBio-Electrospraying and Cell Electrospinning: Progress and Opportunities For Basic Biology and Clinical SciencesMarcos Vinicios Borges GaldinoPas encore d'évaluation
- The Kidneys Matter: Johannes Loffing Francois Verrey Carsten A. WagnerDocument3 pagesThe Kidneys Matter: Johannes Loffing Francois Verrey Carsten A. WagnerRania T. SabriPas encore d'évaluation
- Hemostatic factors promote liver regenerationDocument16 pagesHemostatic factors promote liver regenerationSiti Azra Khairiah LubisPas encore d'évaluation
- 74.burglary - Policy WordingDocument18 pages74.burglary - Policy WordingAyesha RalliyaPas encore d'évaluation
- AIG41313 - FINAL 3 (ENG-Single PG) - tcm4009-638392Document92 pagesAIG41313 - FINAL 3 (ENG-Single PG) - tcm4009-638392Ayesha RalliyaPas encore d'évaluation
- Administration of The Act: LegislationDocument6 pagesAdministration of The Act: LegislationAyesha RalliyaPas encore d'évaluation
- Artificial EngineeringDocument12 pagesArtificial EngineeringAyesha RalliyaPas encore d'évaluation
- SN P&P 2013 PDFDocument188 pagesSN P&P 2013 PDFMixxmixouPas encore d'évaluation
- Food Waste MalaysiaDocument4 pagesFood Waste MalaysiaAyesha RalliyaPas encore d'évaluation
- Cell Delivery Using Cell SheetDocument11 pagesCell Delivery Using Cell SheetAyesha RalliyaPas encore d'évaluation
- Presentation AyeshaDocument28 pagesPresentation AyeshaAyesha RalliyaPas encore d'évaluation
- Cell Disruption by Homogenization 3006 01-06-2008 USDocument20 pagesCell Disruption by Homogenization 3006 01-06-2008 USPrathi_Pal_8304Pas encore d'évaluation
- An Introduction To Takaful - An AlternativeDocument3 pagesAn Introduction To Takaful - An Alternativealvis2entPas encore d'évaluation
- Plant Location Factors Under 40 CharactersDocument16 pagesPlant Location Factors Under 40 CharactersAyesha RalliyaPas encore d'évaluation
- Course Outline: International Islamic University MalaysiaDocument5 pagesCourse Outline: International Islamic University MalaysiaAyesha RalliyaPas encore d'évaluation
- Safety and Loss PreventionDocument65 pagesSafety and Loss PreventionAyesha RalliyaPas encore d'évaluation
- Recycled Organic Waste As Animal Feed PFPDocument4 pagesRecycled Organic Waste As Animal Feed PFPAyesha RalliyaPas encore d'évaluation
- Animal FeedDocument106 pagesAnimal FeedAyesha Ralliya100% (2)
- Bioreactor Monitoring & Control GuideDocument51 pagesBioreactor Monitoring & Control GuideAyesha RalliyaPas encore d'évaluation
- Ideal Bioreactor EngineeringDocument60 pagesIdeal Bioreactor EngineeringAyesha RalliyaPas encore d'évaluation
- Course Outline: International Islamic University MalaysiaDocument5 pagesCourse Outline: International Islamic University MalaysiaAyesha RalliyaPas encore d'évaluation
- Eng Econ - Inv An N BEP - L9Document31 pagesEng Econ - Inv An N BEP - L9Ayesha RalliyaPas encore d'évaluation
- Eng Econ - Cash - Flow - L3 - MME 4272Document55 pagesEng Econ - Cash - Flow - L3 - MME 4272Ayesha RalliyaPas encore d'évaluation
- Eng Econ - Cash - Flow - L3 - MME 4272Document55 pagesEng Econ - Cash - Flow - L3 - MME 4272Ayesha RalliyaPas encore d'évaluation
- Eng Econ MGT Ratios L2 - MME 4272Document41 pagesEng Econ MGT Ratios L2 - MME 4272Ayesha RalliyaPas encore d'évaluation
- Organizational Structure: Ref. Contemporary Management, 3 Ed Gareth R. Jones Jennifer M. George Mcgraw-HillDocument39 pagesOrganizational Structure: Ref. Contemporary Management, 3 Ed Gareth R. Jones Jennifer M. George Mcgraw-HillAyesha RalliyaPas encore d'évaluation
- Eng Econ Deprec L10Document29 pagesEng Econ Deprec L10Ayesha RalliyaPas encore d'évaluation
- Eng Econ Deprec L10Document29 pagesEng Econ Deprec L10Ayesha RalliyaPas encore d'évaluation
- Eng Econ - Inv An N BEP - L9Document31 pagesEng Econ - Inv An N BEP - L9Ayesha RalliyaPas encore d'évaluation
- Chap 2 Polymer & CompositesDocument18 pagesChap 2 Polymer & CompositesAyesha RalliyaPas encore d'évaluation
- Revised Chemical KineticsDocument36 pagesRevised Chemical KineticsAyesha RalliyaPas encore d'évaluation
- Eng Econ Cash Flow L4 - MME 4272Document43 pagesEng Econ Cash Flow L4 - MME 4272Ayesha RalliyaPas encore d'évaluation
- National Mediclaim Policy: BrochureDocument3 pagesNational Mediclaim Policy: Brochureshukla8Pas encore d'évaluation
- Pressure Ulcers and Wound CareDocument52 pagesPressure Ulcers and Wound CareKarina Mega WPas encore d'évaluation
- Synergy CementlessDocument32 pagesSynergy CementlessSergiu Plesca100% (1)
- Minimally Invasive Shoulder and Elbow Surgery - W. Levine, Et Al., (Informa, 2007) WWDocument408 pagesMinimally Invasive Shoulder and Elbow Surgery - W. Levine, Et Al., (Informa, 2007) WWGeo SanchezPas encore d'évaluation
- Family Coping IndexDocument5 pagesFamily Coping IndexDarcey NicholePas encore d'évaluation
- Gram Negative RodsDocument23 pagesGram Negative RodsYasir KareemPas encore d'évaluation
- AntacidsDocument2 pagesAntacidsMa Corazon MelecioPas encore d'évaluation
- Pain47, 295Document4 pagesPain47, 295Ezel RitmoPas encore d'évaluation
- Bacillus Pumilus - MicrobewikiDocument4 pagesBacillus Pumilus - MicrobewikiAleivi PérezPas encore d'évaluation
- Safety and Efficacy of Vinyl Bags in Prevention of Hypothermia of Preterm Neonates at BirthDocument3 pagesSafety and Efficacy of Vinyl Bags in Prevention of Hypothermia of Preterm Neonates at BirthArgadia YuniriyadiPas encore d'évaluation
- 2.0 Classification of Mental DisordersDocument3 pages2.0 Classification of Mental DisordersJohnBenedictRazPas encore d'évaluation
- Neurofeedback ResearchDocument50 pagesNeurofeedback Researchdocs1234567Pas encore d'évaluation
- Research Proposal Power Point PresentationDocument24 pagesResearch Proposal Power Point PresentationSithara JayatungaPas encore d'évaluation
- 10 1097@CCM 0b013e31818b35f2Document7 pages10 1097@CCM 0b013e31818b35f2omarihuanoPas encore d'évaluation
- Peritoneum 2022Document86 pagesPeritoneum 2022Tayyib KhanPas encore d'évaluation
- PE.4 - BPEd2NUÑEZ, MYRADocument25 pagesPE.4 - BPEd2NUÑEZ, MYRANuñez MyraPas encore d'évaluation
- Paper For Enzyme ActivityDocument7 pagesPaper For Enzyme ActivityFar hatPas encore d'évaluation
- NCM 116 Course SyllabusDocument21 pagesNCM 116 Course SyllabusMagne CharliePas encore d'évaluation
- What Is Bronchitis 2Document3 pagesWhat Is Bronchitis 2lea jumawanPas encore d'évaluation
- FACTORS AFFECTING THE PUBLIC SPEAKING FA - OdtDocument16 pagesFACTORS AFFECTING THE PUBLIC SPEAKING FA - OdtKenneth BitunPas encore d'évaluation
- Antisense Oligonucleotide Biotechnology, Applications and FutureDocument29 pagesAntisense Oligonucleotide Biotechnology, Applications and FuturesurojitarpitaPas encore d'évaluation
- NLE 2015 Questions SampleDocument8 pagesNLE 2015 Questions SampleJona Suarez100% (4)
- 2004 2005 Magnetom Flash 2 2Document64 pages2004 2005 Magnetom Flash 2 2Herick SavionePas encore d'évaluation
- Salicylates Tca ToxicityDocument54 pagesSalicylates Tca Toxicityapi-298936498Pas encore d'évaluation
- Seminar Presentation On Management of Diabetic Ketoacidosis BY:Kelil Kedir (CII)Document34 pagesSeminar Presentation On Management of Diabetic Ketoacidosis BY:Kelil Kedir (CII)Meraol HusseinPas encore d'évaluation
- 21 Top Orthopedic Tests PDFDocument27 pages21 Top Orthopedic Tests PDFLaraib Mirza100% (1)
- 1577un 2026-01Document79 pages1577un 2026-01ngovantienPas encore d'évaluation
- Parents of Episcopal School of Jacksonville Students File Lawsuit Over Mask MandateDocument32 pagesParents of Episcopal School of Jacksonville Students File Lawsuit Over Mask MandateActionNewsJaxPas encore d'évaluation
- Module 8 - Diversity of Microbial World: Lecture 1-Microbial Taxonomy and PhylogenyDocument27 pagesModule 8 - Diversity of Microbial World: Lecture 1-Microbial Taxonomy and PhylogenyDr. P.V.Kamala KumariPas encore d'évaluation
- 3.blood Pressure and Its RegulationDocument44 pages3.blood Pressure and Its RegulationNatasha Grace NtembwaPas encore d'évaluation