Académique Documents
Professionnel Documents
Culture Documents
2012 PROF 174 Ophthalmic Instrument Decontamination PDF
Transféré par
mochkurniawanDescription originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
2012 PROF 174 Ophthalmic Instrument Decontamination PDF
Transféré par
mochkurniawanDroits d'auteur :
Formats disponibles
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
Ophthalmic Instrument Decontamination
1 Decontamination
Decontamination is the term used to describe a combination of processes, including cleaning,
disinfection and/or sterilization, used to render a re-usable item safe for further use on
patients and handling by staff.
The effective decontamination of re-usable surgical instruments (or other clinical devices
used in direct contact with tissues) is essential in minimising the risk of infectious agents.
Ineffective decontamination can result in problems via four main pathways:
Foreign protein transfer, leading to risk of adverse reaction, or even risk of
transmission of prion material.
Infection, via transfer of microorganisms.
Particulate material.
Bacterial endotoxins.
Effective Decontamination:
Life-cycle of re-usable surgical instruments
Acquisition
(loan/purchase)
Cleaning
Transportation
Disinfection
Inspection
Use
Packaging
Disposal
Storage
Sterilization
Transport
General Principles - see MRHA MAC Manual
1
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
1.1 Acquisition
Manufacturers of re-usable surgical instruments are required to supply information on the
appropriate decontamination process to allow reuse, including cleaning, disinfection and
where appropriate the method of sterilization. Theatre staff should ensure that such
information is provided and is available for those involved at all stages of the
decontamination life-cycle.
All devices should be CE marked. Exceptions may occur for specific custom-made
instruments, or those undergoing investigation, but should only be used with local
authorisation and monitoring agreed by the hospital or trust decontamination lead.
1.1.1 Single-use instruments (SUI) v Re-useable
Single use is an advisable option for certain instruments used in many ophthalmic
procedures: instruments that can be difficult or costly to decontaminate safely (e.g. those with
a lumen), or those dependent on a cutting edge (e.g. scalpel blades or phako needles). It is
also a means by which risk of transmission of CJD/vCJD can be reduced. (see below).
Instruments marked by the manufacturer for single use only should never be reused for a
number of reasons:
Inadequate cleaning and decontamination of instrument occurs with reuse. This can
be due to instrument construction (e.g. small bore), or surface damage occurring,
preventing removal of all debris or organisms.
Component materials can become damaged or brittle. This leads to the risk of loose
fragments entering the eye during surgery.
Some materials can adsorb or absorb certain chemicals, potentially causing harm.
MHRA Device Bulletin Single-use Medical Devices: Implications and Consequences of
Reuse DB2006(04) v2.0 December 2011
http://www.mhra.gov.uk/home/groups/dts-iac/documents/publication/con2025021.pdf
2
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
1.2 Cleaning
Due to the high volume of operations in ophthalmology, particularly for cataract surgery, there
is a need to ensure that sufficient instruments exist to allow for adequate cleaning and resterilization of instruments, even if the reprocessing facility is some distance from the
ophthalmic unit. (Where there is transition to a centralised unit, it is important that service
contracts and provision of sufficient tray sets reflect the expected local demands).
Cleaning is the most important stage in the decontamination process. A Guide to the
decontamination of reusable surgical instruments NHS Estates 2003 states that effective
cleaning of surgical instruments is of the utmost importance in reducing the risk of
transmission of infectious agents.
Immediately after use, the dirty instruments must be taken via a specially dedicated theatre
hatch, separate from the "clean" hatch, to an adjacent area. Separation of clean and
contaminated instruments is of paramount importance. Complex instruments such as phaco
hand-pieces and Aspiration/Irrigation sets should be disassembled following manufacturers
recommendations. It is usual practice (and probably particularly appropriate for phaco handpieces) for ophthalmic theatre staff to begin this process in theatre immediately as these are
deemed difficult to clean items. Appropriate personal protection should be worn. Any
instrument with a lumen should be flushed with pure water. Instruments ready for transfer to
the Decontamination facility should be kept moist, as drying could cause any residual debris
to harden, making further removal difficult. Liaison between theatre staff and HSDU regarding
specialised equipment requirements is advisable, even when the HSDU provider is at a
distance.
Manual cleaning of some instruments can be performed using an immersion method with a
specifically designed detergent (possibly with enzymes). However, such manual cleaning
should normally only take place if the manufacturer has made this a specific requirement.
Instruments are dismantled and, whilst immersed, are brushed, irrigated, sprayed and
agitated to remove dirt. They are then rinsed and then dried with non-linting cloth or
mechanical drying. Instruments that should not be soaked, including those with electronic
components (e.g. phaco hand-pieces), can be cleaned using a non-immersion method using
detergent-soaked cloth, and then dried as above. The manufacturer guidance should always
be followed.
Automated cleaning is possible using either properly validated and maintained washerdisinfectors or ultrasonic cleaners, or possibly a combination of both. Some cleaners also
incorporate a disinfection stage. The instruments must be adequately packed so as to
prevent damage during the washing cycle.
3
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
It is important that only recommended detergents are used. Ideally, manufacturers should
have tested them on ophthalmic instruments as it is preferable to know if such products have
toxic effects on the eye and if they can be removed adequately from ophthalmic instruments.
1.3 Disinfection
Disinfection is usually achieved by the use of liquid chemicals or by moist heat. Moist heat is
the first choice method except for devices unable to withstand high temperatures.
Disinfection aims to reduce the number of viable organisms, but cannot be relied upon to
inactivate all organisms, particularly viruses and bacterial spores. The process is more
effective if air bubbles are dislodged by agitation.
Manufacturers guidance must always be provided and followed.
1.4 Inspection
Inspection of devices should be performed by staff members in the decontamination facility
other than those responsible for cleaning them. For fine ophthalmic instruments, it is useful
for magnification to be used, using a loupe system or microscope. Instruments that are
damaged can be identified, as can those that have been inadequately cleaned. Damaged
instruments are removed for repair or disposal after decontaminated in accordance with,
MHRA DB2006(05) and inadequately cleaned items are returned to the decontamination
cycle for further cleaning.
The final visual inspection should be made by the operating surgeon before using any
instrument.
1.5 Packaging
The packaging of instruments will depend on its size, planned use, and chosen sterilization
method. Some instruments will form part of a multiple package and be packed in suitable
trays. Others will be individually packed in sealed peel-apart pouches.
All instruments should be traceable. The use of coloured adhesive marking tapes is not
recommended and should be discouraged, as this leads to inadequate decontamination and
gradual break-down of the applied material. Ideally, all instruments should be etched with a
unique identifying code. Retrograde marking using etching is unlikely to be feasible for all
existing instruments, apart from high-value items (such as phaco hand-pieces), so at least all
trays should be coded in such a way that they, and their contents, are traceable.
4
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
1.6 Sterilization
The preferred method for instruments in the clinical setting is the use of saturated steam
under pressure, at the highest temperature compatible with the instruments being processed.
Solid items can be sterilized in Bowl and Instrument Sterilizers that do not have an active airremoval stage. Non-solid items, including those with lumen, or wrapped goods, require
sterilization in Porous-Load Sterilizers (Autoclaves), and are not suitable for sterilization in
non-vacuum sterilizers.
The use of stand-alone bench-top units in the operating theatre or clinic is discouraged as
their maintenance and validation can be difficult. Health care organisations, and indeed
individual professionals, could be held liable if guidance is not followed.
1.7 Transport
Transportation of instruments between clinical areas and decontamination facilities will rise
as the latter are increasingly centralised. It is essential that transit containers fully protect
their contents and individuals handling them. They must be secure, tamper-proof, waterproof,
and clearly labelled.
In order to avoid damage, clean instruments must be packed by speciality-trained personnel
in trays designed for eye instruments.
1.8 Storage
Ideally, once ready for use, these trays should then be stored in the Eye Theatre (or clinic)
suite. The storage area should be safe, dry, above floor level and away from sunlight and
water. It is vital that packs are handled carefully in order to prevent damage and loss of
sterility.
1.9 Use
Before use, packages should be checked to ensure that:
The package is intact
The sterilization indicator confirms sterilization
Expiry date has not passed
Theatre or clinic staff must notify the decontamination unit staff about any concerns regarding
problems with instrument or device availability, or the instruments themselves.
5
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
2 CJD
2.1 High Risk or Low Risk Surgical Procedures
Ophthalmic procedures regarded as high-risk are given in Transmissible spongiform
encephalopathy agents: safe working and the prevention of infection, Annex L Managing
CJD/vCJD Risk in Ophthalmology Appendix 1.
"High Risk category includes ophthalmic procedures on the Posterior eye, specifically the
posterior hyaloid face, retina, retinal pigment epithelium, choroid, subretinal fluid and optic
nerve. Procedures on cranial nerves are also high risk.
Appendix 2 covers all anterior segment surgery (including corneal surgery and complicated
cataract surgery) which is now considered low risk for infectivity.
High risk procedures are also listed as HES codes in NICE interventional procedure
guidance 196 Appendix C:
C01 Excision of eye
C79 Operations on vitreous body
C81 Photocoagulation of retina for detachment (only when the retina is handled
directly)
C82 Destruction of lesion of retina
C84 Other operations on retina
The inclusion of C79 Operations on vitreous body here refers to posterior approach surgery.
N.B. Anterior vitrectomy is considered low risk and warrants no specific variation from
normal practice in instrumentation, or in decontamination of instruments and equipment.
As single-use instrumentation has improved and is more readily available, disposable
equipment can be considered for High Risk procedures. It is no longer a requirement that
such procedures are undertaken with disposable instruments. The costs involved may
preclude this approach, as recognised by NICE. Referring to high-risk surgical procedures,
including eye surgery, NICE interventional procedure guidance 196 (para 1.4) states: the
evidence on cost effectiveness related to the possible transmission of CJD does not support
a change to single-use instruments based on current costs.
If SUIs are used, it is essential that they are of consistent and suitable quality.
If re-usable instruments are used, they must not migrate between sets, and should be fully
traceable. There should be a separate pool of instruments for patients born after 1 January
1997.
6
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
2.2 The Patient with, or at increased risk of, CJD or vCJD
2.2.1 Identification of the patient with, or at increased risk of CJD or vCJD
Transmissible spongiform encephalopathy agents: safe working and the prevention of
infection, Annex J advises that ALL patients undergoing ANY surgical procedure should be
asked:
Have you ever been notified that you are at increased risk of CJD or vCJD for public
health purposes?
The patients response should be recorded in the notes. A positive response requires further
questioning and consultation with local infection control team.
For patients undergoing High Risk (posterior segment) surgery, in addition to checking
patient records and observing any clinic signs of CJD/vCJD, a series of questions should be
asked, as outlined in Table J1 of Annex J above. These questions relate to family history,
growth hormone treatment, previous neurosurgery and exposure to multiple blood
transfusions.
(N.B. Annex J is continually under review, and changes may occur with any new evidence).
2.2.2 Low risk surgery in a patient with, or at increased risk of CJD/vCJD
For routine Anterior Segment surgery and other Low Risk ophthalmic procedures, no
change to routine instrumentation or decontamination is required. Avoiding instrument
migration between trays and instrument sets remains good practice. Anterior Segment
surgery that becomes complicated, involving instrument contact with optic nerve or retina,
should then be considered High Risk. (see para L39-44 of Annex L Transmissible
spongiform encephalopathy agents: safe working and the prevention of infection).
2.2.3 High risk surgery in a patient with, or at increased risk of CJD/vCJD
For High Risk ophthalmic surgery (Posterior Segment), if a patient is suspected to be
suffering from any form of CJD, a further opinion may be considered. If surgery is deemed
urgent, then consideration should be given to the operation being carried out entirely with
single-use instruments. If this is not possible, at the end of the procedure then quarantining
instruments should be considered (see Annex E of Transmissible spongiform
encephalopathy agents: safe working and the prevention of infection).
Single-Use Instrument (SUI) use as an option to reduce risk of CJD/vCDJ transmission in
ophthalmic surgery is also covered in more detail in Appendix 4 of Annex L Managing
CJD/vCJD Risk in Ophthalmology from the ACDP TSE Risk Management Subgroup. SUIs
should be of equivalent standard to re-usable instruments.
7
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
After washing, instruments (single-use or re-usable) should be placed on a disposable
instrument tray and allowed to air-dry. They should then be placed in an impervious rigid
plastic container with a close-fitting lid. The lid should be sealed with heavy-duty tape (e.g.
autoclave tape) and labelled with the patients identification details (i.e. name, date of birth
and hospital number). The label should also state the surgical procedure in which the
instruments were used and the name of the responsible person (e.g. theatre superintendent).
The original instrument tray should be disposed of by incineration.
The sealed box can be stored indefinitely in a suitable designated place until the outcomes of
any further investigations are known. If the patient is confirmed as suffering from CJD or
vCJD, the box and its contents should be incinerated without any further examination. The
instruments could alternatively be donated to the DH sponsored research store organized by
the Health Protection Agency. (This is in order to retain for decontamination experiments).
Guidance from ACDP TSE Risk Management Subgroup (Part 4 of 'Transmissible Spongiform
Encephalopathy Agents: Safe Working and the Prevention of Infection) is that for all patients
with, or at increased risk of, CJD or vCJD, single-use should be used where possible, and
subsequently destroyed by incineration or sent to the instrument store. It is possible for
instruments to be segregated and processed using standard decontamination process, for
use again on the same patient.
If an alternative diagnosis is confirmed, the instruments may be removed from the box by the
responsible person (or a named deputy) and any re-usable instruments reprocessed
according to best practice and returned to use. Additional decontamination procedures are
not required.
Records must be kept of all decisions, and the Sterile Service Department (SSD) must be
informed about the decision before the instruments are sent for routine reprocessing
In summary: for any High Risk surgery performed on patients with, or at risk of CJD/vCJD,
the instruments should be either single-use (and destroyed post-operatively), or re-usable, in
which case they should be destroyed or kept for re-use solely on the individual patient.
8
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
From Annex J of Transmissible spongiform encephalopathy agents: safe working and the
prevention of infection:
9
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
3 Devices used in Clinic
Numerous instruments are used in eye clinics that come into contact with the surface of the
eye or the mucous membrane surface of the conjunctiva. Whilst some are available as
single-use items, it is necessary to re-use others.
For items such as diagnostic contact lenses, ultrasound probes or pachymetry that cannot be
replaced after each use, it is essential that departments have a policy for ensuring the risk of
transmission of infection is reduced to the minimum practical level.
3.1 General Principles
The greatest risk for transmission of infection is likely to be poor hand hygiene in the clinic
environment. Other infections can be transmitted during ophthalmic examinations, particularly
those involving direct contact with mucous membranes and tears. Whereas the transmission
of prions is an unlikely and theoretical risk, albeit one that cannot be ignored, many other
infections (such as adenovirus outbreaks) pose well-recognised and significant risks. It is
possible to disinfect the contaminated surface of an instrument, but without attention to work
surface (including slit-lamp) decontamination, hand washing and glove wearing when
appropriate, transmission of infections remains a risk.
The APDS TSE Risk Management Subgroup in Appendix 3 of Managing CJD/vCJD Risk in
Ophthalmology has addressed the issue of possible CJD/vCJD in the context of the eye
clinic.
A solution containing 10,000 parts per million of available chlorine (sodium hypochlorite) is
effective in reducing Transmissible Spongiform Encephalopathies, including vCJD. It is also
effective against most organisms likely to be encountered within the environment of the Eye
Clinic. Rutala & Weber.
Soaking in 1% hypochlorite solution (e.g. Milton) for 10 minutes between patients as part of a
decontamination procedure is therefore recommended as best decontamination practice
against the risk of CJD/vCJD. The compatibility of such solutions with various devices has yet
to be determined, although it is widely used for tonometer prisms. Clinicians must make their
own risk-assessments for their own practice within their own departments, based on the
available knowledge, including data from equipment manufacturers. (In considering a
balance of risk versus cost-effectiveness, it may be useful to compare the approach taken by
NICE on the subject of single-use items in surgical procedures: Referring to surgical
procedures, including all eye surgery, NICE interventional procedure guidance 1966 para 1.4
states the evidence on cost effectiveness related to the possible transmission of CJD does
not support a change to single-use instruments based on current costs). This will
10
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
undoubtedly apply also to many devices used in an ophthalmic outpatient setting.
http://www.nice.org.uk/guidance/index.jsp?action=download&o=31754
The use of alcohol wipes alone is insufficient for safe decontamination, and if used before the
cleaning stage there is a theoretical risk of binding any prion protein to the instrument
surface. 70% alcohol wipes have been shown to be insufficient to inactivate Adenovirus and
other viruses.
3.2 Tonometry
Single-use disposable tonometer heads or tonometer shields are an option for use with
patients known to have, or under suspicion of having, CJD. This could include neurological
diseases such as dementia of unknown aetiology. These devices should be available in all
departments, and single-use options used whenever possible for these potential risk cases.
It is unnecessary to use disposable tonometry for all routine cases. There is no evidence that
using single-use devices for all routine is cost-effective in reducing infection risk. It is
acceptable to use reusable tonometer prisms provided that they are decontaminated
correctly between patients. Cellular and proteinaceous debris can be present on tonometers
after use, although the cornea is now regarded as low risk for prion infectivity. After each use,
and before being allowed to dry, re-usable prisms should ideally be rinsed in water, washed
with soap/detergent and rinsed again, then immersed in 1% sodium hypochlorite solution for
at least 10 minutes; after which they should be rinsed (using sterile water) and dried.
Tonometer prisms can become damaged with time. Regular inspection at the slit-lamp is
recommended, with replacement of any prism with significant damage. Neubauer S et al
3.3 Diagnostic Contact Lenses
These lenses should be decontaminated as for tonometer prisms. They should also be
checked on a regular basis for evidence of damage; cracks could not only abrade the cornea
but could also harbour debris or hold disinfectant, both possibly leading to further ocular
irritation.
3.4 Contact Lenses
The vast majority of contact lenses are for single patient use only. There are some
exceptions, such as Trial Contact Lenses or Special Complex Diagnostic Contact Lenses,
which may need to be re-used. The College of Optometrist recommend in their document
A03 Infection Control para A3.57 that in these circumstances:
a) The lenses should be used solely within the clinicians premises and under the control of
the clinician at all times;
11
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
b) The clinician should ensure that decontamination is carried out to the highest possible
standards;
c) The clinician should keep full records to show the usage of each lens;
d) The clinician should inform the patient of all the relevant risks and benefits associated
with contact lens fitting.
Guidance in the British Standards Draft for Development: Ophthalmic optics - Contact lenses
- Hygienic management of multipatient use trial contact lenses BSi DD ISO/TS 19979:2004
includes a decontamination method that has been superseded by that suggested by ACDP
TSE Risk Management Subgroup, which is in line with current College of Optometrist advice.
3.5 Surgical instruments
Where possible, any instrument used in the clinic should be processed for decontamination
just as for use in theatres, except for single-use instruments, which should be disposed of
after use. In the event of any instrument that has touched the eye or adnexae, where that
instrument needs to be re-used in the clinic setting for any reason, the general principles
above should apply.
12
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
4 Summary for Clinic Devices Decontamination:
The guidance given in Annex L is a distillation of the views of a multidisciplinary expert
advisory group to address the issue of prion transmission. The guidance presented in this
document reflects a pragmatic approach to decontamination of most instruments used in an
ophthalmic clinic and should enable ophthalmic units to minimise infection risk to patients,
staff and to equipment in a cost-effective and practical way. In offering a slightly simplified
recommended regime, it is expected that compliance with the recommendations should be
both readily achievable and can be easily audited on a regular basis in any department.
This guidance, like the guidance in Annex L, remains advisory. Should individual units have
particular concerns regarding any recommended measures, they are strongly advised to
seek the advice of their Infection Control Advisors and draw up a written local policy that is
both practical and likely to be effective.
Good Hand Hygiene is essential
Clean device immediately after use, or keep moist until decontaminated
Wash with clean running tap water with soap or detergent (as for hand-washing).
o TSE guidance recommends sterile water at every stage of cleaning, but for frequently
used items with hard surfaces, such tonometer prisms, the above is a practical
approach in a clinic setting. Concerns regarding water contamination with
acanthamoeba exist; general guidance for standard contact lens management is that
tap water should be avoided. The above cleaning technique however would reduce the
risk of contamination to equal that of a clean hand holding the device in normal use,
and following this immediately with disinfection will reduce any risk of contamination to
a negligible level.
o Further guidance on water quality is the responsibility of local infection control and
estates.
Soak for min. 10 minutes in sodium hypochlorite solution (10,000ppm chlorine)
o Ensure staff are familiar with potential hazards of storing, preparing and handling
solutions
o Label solutions and containers clearly
o Solutions should be fresh
o Avoid prolonged soaking
o Check with instrument manufacture for advice if in doubt regarding use of this method
Rinse thoroughly with Sterile Water
Dry using paper tissues
Store to prevent contamination prior to next use
Note: Alcohol Swabs
o Alcohol used prior to decontamination risks of fixing any existing prions to the surface.
o 70% alcohol is inadequate to inactive all virus particles.
13
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
5 Bibliography
5.1 Decontamination - General Resources
5.1.1 MHRA http://www.mhra.gov.uk
The MAC Manual Sterilization, Disinfection and Cleaning of Medical Equipment:
Guidance on Decontamination from the Microbiology Advisory Committee (MAC) to
the Department of Health Medical Devices Directorate.
Part 1 (2nd Ed 2002) PRINCIPLES of the processes that are available for
decontamination.
Part 2 (2nd Ed April 2005) PROTOCOLS for decontamination using cleaning,
disinfection and sterilization processes.
Part 3 PROCEDURES
o
Section 1 (Feb 1999) General advice regarding European Directives for
medical devices
o
Section 2 (Oct 2000) Provides general procedures for groups of equipment
including ophthalmology.
http://www.mhra.gov.uk/Publications/Safetyguidance/Otherdevicesafetyguidance/CON007438
Other Publications available via MHRA Website:
http://www.mhra.gov.uk/index.htm
DB 2006(04) Single-use Medical Devices: Implications and Consequences of Reuse
http://www.mhra.gov.uk/Publications/Safetyguidance/DeviceBulletins/CON2024995
5.1.2 Department of Health
NHS Decontamination Programme : DH Managing your organisation:
http://www.dh.gov.uk/en/Managingyourorganisation/Leadershipandmanagement/Healt
hcareenvironment/NHSDecontaminationProgramme/index.htm
Guide to the decontamination of reusable surgical instruments (DH 2003)
http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAnd
Guidance/DH_4120906
5.1.3 Scotland:
Health Protection Scotland Decontamination website:
http://www.hps.scot.nhs.uk/haiic/decontamination/index.aspx
The Glennie report: http://www.scotland.gov.uk/Publications/2001/10/10106/File-1
5.1.4 Wales
Public Health Wales http://www.wales.nhs.uk/sitesplus/888/page/43949
14
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
5.1.5 U.S.A.
Healthcare Infection Control Practices Advisory Committee (HICPAC)
Guideline for Disinfection and Sterilization in Healthcare Facilities, 2008.
http://www.cdc.gov/hicpac/pdf/guidelines/Disinfection_Nov_2008.pdf
http://www.cdc.gov/hicpac/Disinfection_Sterilization/acknowledg.html
Hellinger WC, Bacalis LP, Edelhauser HF, Mamalis N, Milstein B, Masket S; ASCRS
Ad Hoc Task Force on Cleaning and Sterilization of Intraocular Instruments.
Recommended practices for cleaning and sterilizing intraocular surgical instruments. J
Cataract Refract Surg. 2007 Jun;33(6):1095-100.
5.2 CJD Information and Resources:
5.2.1 Guidance from the Advisory Committee on Dangerous Pathogens and the
Spongiform Encephalopathy Advisory Committee/ Dept. of Health.
Transmissible spongiform encephalopathy agents: Safe working and the prevention
of infection: (2007)
http://www.dh.gov.uk/PolicyAndGuidance/HealthAndSocialCareTopics/CJD/CJDGener
alInformation/CJDGeneralArticle/fs/en?CONTENT_ID=4031067&chk=4gOe2r
NHS Estates, Health Service Circular HSC 1999/178 Variant Creutzfeldt-Jakob
Disease (vCJD): Minimising the Risk of Transmission. DH 1999
http://www.dh.gov.uk/en/PublicationsAndStatistics/LettersAndCirculars/HealthService
Circulars/DH_4004969
5.2.2 Guidance from the ACDP TSE Risk Management Subgroup (formerly TSE
Working Group) http://www.dh.gov.uk/ab/ACDP/TSEguidance/index.htm
Transmissible Spongiform Encephalopathy Agents: Safe Working and the Prevention
of Infection: Annex A1, Distribution of TSE infectivity in human tissues and body fluids
http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@ab/documents/
digitalasset/dh_132095.pdf
Transmissible Spongiform Encephalopathy Agents: Safe Working and the Prevention
of Infection: Annex C, General Principles of decontamination TSE.
http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@ab/documents/
digitalasset/dh_108602.pdf
Transmissible Spongiform Encephalopathy Agents: Safe Working and the Prevention
of Infection: Annex J, Pre-operative Assessment.
http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@ab/documents/
digitalasset/dh_123586.pdf
Transmissible Spongiform Encephalopathy Agents: Safe Working and the Prevention
of Infection: Annex L, Managing CJD/vCJD Risk in Ophthalmology.
http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@ab/documents/
digitalasset/dh_123585.pdf
15
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
5.2.3 RCOphth / Dept. Health
Creutzfeldt-Jakob Disease (CJD) and Ophthalmology
http://www.rcophth.ac.uk/page.asp?section=169§ionTitle=Decontamination+and+
Creutzfeld%2DJacob+Disease+%28CJD%29+Advice
http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@ab/documents/
digitalasset/dh_123910.pdf
5.2.4 NICE
NICE interventional procedure guidance 196 Nov. 2006. Patient safety and reduction
of risk of transmission of CreutzfeldtJakob disease (CJD) via interventional
procedures.
http://www.nice.org.uk/guidance/index.jsp?action=download&o=31754
5.3 Infection Control - General Principles
National electronic Library of Infection
http://www.neli.org.uk/IntegratedCRD.nsf/NeLI_Home1?OpenForm
National Resource for Infection Control (NRIC) decontamination policy
http://www.nric.org.uk/IntegratedCRD.nsf/d4714c229facb1148025701a0039d34e/f384
8d4fd889cbc18025701a0039f8d5?OpenDocument
5.3.1 Health Protection Scotland & Welsh Healthcare Associated Infection Programme
(WHAIP)
Environmental Cleanliness
http://www.wales.nhs.uk/sites3/page.cfm?orgid=379&pid=38961
Hand Hygiene http://www.wales.nhs.uk/sites3/page.cfm?orgid=379&pid=38962
Hand Hygiene Literature Review:
http://www.wales.nhs.uk/sites3/Documents/379/PHW%5FHHallLitR%5F200910%5FV
1.pdf
5.3.2 College of Optometrists:
A03 Infection Control
http://www.college-optometrists.org/en/utilities/documentsummary.cfm/docid/EBEDBDAB-AD05-404C-8850B2E9D5A2EE37
5.3.3 Healthcare Infection Control Practices Advisory Committee (HICPAC)
Guideline for Isolation Precautions: Preventing Transmission of Infectious Agents in
Healthcare Settings (2007).
http://www.cdc.gov/hicpac/2007IP/2007isolationPrecautions.html
Herwaldt LA. Smith SD. Carter CD. Infection control in the outpatient setting. Infection
Control & Hospital Epidemiology. 19(1):41-74, 1998 Jan.
16
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
5.4 Devices in Clinic
College of Optometrists: A03 Infection Control
http://www.college-optometrists.org/en/utilities/documentsummary.cfm/docid/EBEDBDAB-AD05-404C-8850B2E9D5A2EE37
Amin SZ, Smith L, Luthert PJ, Cheetham ME, Buckley RJ. Minimizing the risk of prion
transmission by contact tonometry. Br J Ophthalmol. 2003 Nov;87(11):1360-2.
Austin MW, Clark DI, Moreton C. Disinfection of tonometer prisms and examination
contact lenses in ophthalmic departments. Eye 1992 (6), 115-116
Bell NP, Anand A, Wanger A, Prager TC. Microbial contamination of ultrasound
biomicroscopy probes: Evaluation of cross-infection risk. Journal of Cataract &
Refractive Surgery. 2012;38,(1) 174-175.
British Standards Institution. Ophthalmic optics - Contact lenses - Hygienic
management of multipatient use trial contact lenses BSi DD ISO/TS 19979:2004.
Buckley R Decontamination Optom in Practice 2010 11(1) 25-29
Cillino S, Casuccio A, Giammanco GM, Mammina C, Morreale D, Di Pace F, Lodato
G. Tonometers and infectious risk: myth or reality? Efficacy of different disinfection
regimens on tonometer tips. Eye 2007 Apr;21(4):541-6.
http://www.nature.com/eye/journal/v21/n4/full/6702269a.html
Comoy E, Bonnevalle C, Mtais A, et al. Dsinfection de lentilles de contact rigides
permables vis--vis des prions. J Fr Ophtalmol 2003;3:233-9
Desai SP, Sivakumar S, Fryers PT. Evaluation of a disposable prism for tonometry.
Eye 2001;15: 279-282
Herwaldt LA. Smith SD. Carter CD. Infection control in the outpatient setting. Infection
Control & Hospital Epidemiology. 19(1):41-74, 1998 Jan.
Hillier RJ, Kumar N. Tonometer disinfection practice in the United Kingdom: A national
survey. Eye 2008;22(8)1029-33
http://www.nature.com/eye/journal/v22/n8/full/6702831a.html
Jernigan JA, Lowry BS, Hayden FG, et al. Adenovirus type 8 epidemic
keratoconjunctivitis in an eye
clinic: r
1993;167:1307-13.
Kniestedt C, Strmer J, Stamper R. Clinical alert: damage to Goldmann applanation
tonometer tips. Acta Ophthalmologica Scandinavica Volume 83, Issue 1, pages 129
130,
February
2005
http://onlinelibrary.wiley.com/doi/10.1111/j.16000420.2005.00360.x/pdf
Koo D, Bouvier B, Wesley M, Courtright P, Reingold A. Epidemic keratoconjunctivitis
in a university
medical center
-evaluation
of the
ophthalmo
-Infect. Co
design and disinfection of instruments.
52.
17
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
The Royal College of Ophthalmologists
Ophthalmic Services Guidance
Lim R, Dhillon B, Kurian KM, Aspinall PA, Fernie K, Ironside JW. Retention of corneal
epithelial cells following Goldmann tonometry: implications for CJD. Br J Ophthalmol.
2003;87:583-6.
Neubauer S, Heeg P, Kampik A, Hirneiss C. Disinfecting Contact Tonometers - a
Systematic Review. Klin Monatsbl Augenheilkd 2009; 226(5): 396-403
Rutala WA, Peacock JE, Gergen MF, Sobsey MD, Weber DJ. Efficacy of hospital
germicides against
a
denovi
in health care facilities. Antimicrob. Agents Chemother. 2006;50:1419-24.
Rutala WA, Weber DJ. Uses of Inorganic Hypochlorite (Bleach) in Health-Care
Facilities. Clinical Microbiology Reviews, Oct. 1997; 597610.
Sattar SA, Springthorpe VS, Karim Y, Loro P. Chemical disinfection of non-porous
inanimate surfaces
experim
viruses. Epidemiol. Infect. 1989;102:493-505
Segal WA, Pirnazar JR, Arens M, Pepose JS. Disinfection of Goldmann tonometers
after contamination with hepatitis C virus. Am. J Ophthalmology 2001; (131) 184-187
Weber DJ, Rutala WA. Nosocomial ocular infections. In: Mayhall CG, ed. Infect.
Control and Hosp.
l.E pidemio
Philadelphia: Lippincott Williams & Wilkins, 1999:28799
18
Author: Mr Nick Hawksworth
2012/PROF/174
Review Date June 2015
The Royal College of Ophthalmologists 2012 All rights reserved For permission to reproduce any of the content contained
herein please contact beth.barnes@rcophth.ac.uk
Vous aimerez peut-être aussi
- 2013 - BestPractices For HLDDocument53 pages2013 - BestPractices For HLDDaniela Cirnatu100% (1)
- Vitalograph - Hygiene Considerations For SpirometryDocument4 pagesVitalograph - Hygiene Considerations For SpirometryEileenYingYeePas encore d'évaluation
- Operating Theater ManagementDocument5 pagesOperating Theater Managementtummalapalli venkateswara raoPas encore d'évaluation
- TASS Prevention: CIS Self-Study Lesson PlanDocument5 pagesTASS Prevention: CIS Self-Study Lesson Planjerimiah_manzonPas encore d'évaluation
- Infection Control - MicrobiologyDocument9 pagesInfection Control - MicrobiologySarah KahilPas encore d'évaluation
- 6 Reprocessing of EndosDocument28 pages6 Reprocessing of Endoshananshosha743Pas encore d'évaluation
- BSG Guidelines Decontamination of Equipment For Gastrointestinal EndosDocument25 pagesBSG Guidelines Decontamination of Equipment For Gastrointestinal Endoshani1986yePas encore d'évaluation
- Sterlization and DisinfectionDocument20 pagesSterlization and Disinfectionshagun singh100% (1)
- Infection Control in The Dental Practice Through Proper SterilizationDocument5 pagesInfection Control in The Dental Practice Through Proper SterilizationDental ArtPas encore d'évaluation
- IFU-Ortho - Reusable Surgical Instruments GB-Rev 6 - 240205 - 151904Document6 pagesIFU-Ortho - Reusable Surgical Instruments GB-Rev 6 - 240205 - 151904Lukas WijayantoPas encore d'évaluation
- Levofloksasin Hemihidrat MsdsDocument6 pagesLevofloksasin Hemihidrat MsdsEsin KahramanPas encore d'évaluation
- Laboratory Safety Laboratory Analysis #1: Rubrics: Content (50%)Document7 pagesLaboratory Safety Laboratory Analysis #1: Rubrics: Content (50%)Nicole Edelweiss Liza100% (2)
- Module 5-Laboratory SafetyDocument5 pagesModule 5-Laboratory SafetyAllyah Ross DuquePas encore d'évaluation
- Hospital Hazards PresentationDocument30 pagesHospital Hazards Presentationkhizgaming worldPas encore d'évaluation
- Proper DecontaminationDocument38 pagesProper DecontaminationLyza RodriguezPas encore d'évaluation
- ملازم د.عليDocument141 pagesملازم د.عليbbnnnPas encore d'évaluation
- Standard Operating Procedure for Hydrochloric AcidDocument10 pagesStandard Operating Procedure for Hydrochloric AcidArunkumar ChandaranPas encore d'évaluation
- MSDS Engine Oil TitleDocument4 pagesMSDS Engine Oil TitleBiju_PottayilPas encore d'évaluation
- Aorn 12784Document10 pagesAorn 12784Yahia HassaanPas encore d'évaluation
- ResultDocument8 pagesResultAzmeer YusufPas encore d'évaluation
- Processing of Re-UsableDocument10 pagesProcessing of Re-UsableliuslinoPas encore d'évaluation
- Nitric Acid SOPDocument7 pagesNitric Acid SOPnlmiPas encore d'évaluation
- Infection PreventionDocument3 pagesInfection PreventionDentalLearningPas encore d'évaluation
- Standard - Decontamination - Surgical - Instruments - PDFDocument27 pagesStandard - Decontamination - Surgical - Instruments - PDFsugiartoPas encore d'évaluation
- SiD 4.3.3.3 at 7 June 2011Document4 pagesSiD 4.3.3.3 at 7 June 2011Dr-Mohamed KandeelPas encore d'évaluation
- Study Guide For The Dental Technician ExaminationDocument64 pagesStudy Guide For The Dental Technician ExaminationAurora100% (1)
- Clinical Lab Safety GuideDocument4 pagesClinical Lab Safety GuidejelenaPas encore d'évaluation
- OpthalmicDocument6 pagesOpthalmicminhajuljim2000Pas encore d'évaluation
- Endoscope DisinfectionDocument14 pagesEndoscope Disinfectioneliasox123Pas encore d'évaluation
- Standard Operating Procedure: Potassium HydroxideDocument7 pagesStandard Operating Procedure: Potassium HydroxideSHRINIVASPas encore d'évaluation
- HPS Endoscope Decontamination 2004 PDFDocument190 pagesHPS Endoscope Decontamination 2004 PDFHong-Nam Kim100% (1)
- Industrial Hygiene Hazard Communication and Chemical SafetyDocument19 pagesIndustrial Hygiene Hazard Communication and Chemical SafetyJayChristian QuimsonPas encore d'évaluation
- Here are the words from the box that complete the sentences:1. Reduction 2. Airborne3. Reduction4. Clear5. Slips6. Illness7. Burns 8. HealthDocument39 pagesHere are the words from the box that complete the sentences:1. Reduction 2. Airborne3. Reduction4. Clear5. Slips6. Illness7. Burns 8. Healthnerissa dollentePas encore d'évaluation
- Tandex 285 SDSDocument10 pagesTandex 285 SDSHarnani NanikPas encore d'évaluation
- Laboratory SafetyDocument30 pagesLaboratory SafetyEliana Nicole IbongPas encore d'évaluation
- Histo Histopath Safety ManualDocument14 pagesHisto Histopath Safety ManualJanielle Medina FajardoPas encore d'évaluation
- T3 Lab Safety and RegulationsDocument3 pagesT3 Lab Safety and RegulationsZeian Jacob BaylaPas encore d'évaluation
- QLD Health Sterilisation-Section - 2Document13 pagesQLD Health Sterilisation-Section - 2LisaPas encore d'évaluation
- 1250 White Sds PDFDocument4 pages1250 White Sds PDFkwerwaPas encore d'évaluation
- Sop BSL IiDocument7 pagesSop BSL IiBridget HaleyPas encore d'évaluation
- Standard Operating Procedure: Glacial Acetic AcidDocument6 pagesStandard Operating Procedure: Glacial Acetic AcidNikita PedamkarPas encore d'évaluation
- Sterilization of Ophthalmic Surgical Instruments and EquipmentDocument27 pagesSterilization of Ophthalmic Surgical Instruments and EquipmentMohammad Abdullah BawtagPas encore d'évaluation
- Standard Operating Procedure: AmmoniaDocument6 pagesStandard Operating Procedure: AmmoniaRASHEED YUSUFPas encore d'évaluation
- Caustinerf ForteDocument5 pagesCaustinerf Fortefadli_nugraha6109Pas encore d'évaluation
- Endoscope Reprocessing Risk and Current Risk PracticeDocument65 pagesEndoscope Reprocessing Risk and Current Risk PracticeHosam GomaaPas encore d'évaluation
- Wynn's Ultra Synthet Hi-Temp Universal Grease (MSDS)Document6 pagesWynn's Ultra Synthet Hi-Temp Universal Grease (MSDS)Anibal Rios0% (1)
- Tandex 245Document10 pagesTandex 245Harnani NanikPas encore d'évaluation
- My SeminarDocument52 pagesMy SeminarvinnycoolbuddyPas encore d'évaluation
- Sterilization and Disinfection Protocol in Dentistry - Review 1Document7 pagesSterilization and Disinfection Protocol in Dentistry - Review 1alexPas encore d'évaluation
- Module-5 Chemical Safety and Other Safety Checks: Some Most Common Features of High Cost AccidentsDocument17 pagesModule-5 Chemical Safety and Other Safety Checks: Some Most Common Features of High Cost AccidentsBuddies Da Neeghe PuroPas encore d'évaluation
- 059617castrol MXD 153Document4 pages059617castrol MXD 153Musab Ömer KarabulutPas encore d'évaluation
- Infection Control in Surgical PracticeDocument41 pagesInfection Control in Surgical PracticeMuhammad Azeem KhanPas encore d'évaluation
- Biological Toxin SafetyDocument10 pagesBiological Toxin SafetySimon SPas encore d'évaluation
- Sulfuric Acid Sarpong FinalDocument10 pagesSulfuric Acid Sarpong FinalHussain RizviPas encore d'évaluation
- Endoscope ReprocessingDocument34 pagesEndoscope Reprocessingmonir61100% (1)
- Fundamentals of Aseptic Pharmaceutical Engineering: Pdhonline Course K112 (4 PDH)Document16 pagesFundamentals of Aseptic Pharmaceutical Engineering: Pdhonline Course K112 (4 PDH)asfdadfasdfPas encore d'évaluation
- Offices Safety Program: Infection ControlDocument7 pagesOffices Safety Program: Infection Controlفراس الموسويPas encore d'évaluation
- Basic Guide to Dental InstrumentsD'EverandBasic Guide to Dental InstrumentsÉvaluation : 2.5 sur 5 étoiles2.5/5 (3)
- Distillation: Operation and ApplicationsD'EverandDistillation: Operation and ApplicationsAndrzej GorakÉvaluation : 4 sur 5 étoiles4/5 (10)
- Good Manufacturing Practices (GMP) Modules for Pharmaceutical ProductsD'EverandGood Manufacturing Practices (GMP) Modules for Pharmaceutical ProductsPas encore d'évaluation
- Ripe For InvestmentDocument76 pagesRipe For InvestmentFaris ImanPas encore d'évaluation
- Id LSHC Aec Impact Indonesia LSHC IndustryDocument24 pagesId LSHC Aec Impact Indonesia LSHC IndustrymochkurniawanPas encore d'évaluation
- Who PhlebotomiDocument125 pagesWho PhlebotomiFariha FirdausPas encore d'évaluation
- Nursing Best Practice Guidelines Program RNAODocument98 pagesNursing Best Practice Guidelines Program RNAOAlmeiliana Arruanpasau'0% (1)
- ASEANDocument84 pagesASEANmochkurniawanPas encore d'évaluation
- Brochure Transducer SingleDocument2 pagesBrochure Transducer SinglemochkurniawanPas encore d'évaluation
- 102 Article 143 1 10 20180817Document4 pages102 Article 143 1 10 20180817mochkurniawanPas encore d'évaluation
- Blind Spots Video Discussion GuideDocument13 pagesBlind Spots Video Discussion GuidemochkurniawanPas encore d'évaluation
- UICC WorldCancerDeclaration Progress Report 2016 BookDocument146 pagesUICC WorldCancerDeclaration Progress Report 2016 BookmochkurniawanPas encore d'évaluation
- The Next Wave of Consumer MA Searching For GrowthDocument7 pagesThe Next Wave of Consumer MA Searching For GrowthPatricia GarciaPas encore d'évaluation
- Managing Pain in the CommunityDocument11 pagesManaging Pain in the CommunitymochkurniawanPas encore d'évaluation
- Opleidingsprogramma ENG - MarnixDocument81 pagesOpleidingsprogramma ENG - MarnixmochkurniawanPas encore d'évaluation
- IMPACTDocument20 pagesIMPACTmochkurniawanPas encore d'évaluation
- AsepticDocument39 pagesAsepticmochkurniawanPas encore d'évaluation
- WEF TheGlobalCompetitivenessReport2019Document666 pagesWEF TheGlobalCompetitivenessReport2019Marco Mares RedacciónPas encore d'évaluation
- Moving Towards Universal Health Access in Indonesia: Dr. Nafsiah Mboi, Sp.A, MPH Minister of Health Republic of IndonesiaDocument32 pagesMoving Towards Universal Health Access in Indonesia: Dr. Nafsiah Mboi, Sp.A, MPH Minister of Health Republic of IndonesiamochkurniawanPas encore d'évaluation
- Medical Device Guidance DocumentDocument1 pageMedical Device Guidance DocumentmochkurniawanPas encore d'évaluation
- Session 01.5 Induced Hypothermia-The Nursing CareDocument13 pagesSession 01.5 Induced Hypothermia-The Nursing CaremochkurniawanPas encore d'évaluation
- Hadaway Resource Needlessconnectors PDFDocument11 pagesHadaway Resource Needlessconnectors PDFmochkurniawanPas encore d'évaluation
- The Rise and Rise of Medtech in AsiaDocument12 pagesThe Rise and Rise of Medtech in AsiamochkurniawanPas encore d'évaluation
- Endotracheal Tube ETT Insertion IntubationDocument3 pagesEndotracheal Tube ETT Insertion IntubationmochkurniawanPas encore d'évaluation
- Duodopa Intestinal Gel ENG SMPC - 09001be68007fc9a PDFDocument16 pagesDuodopa Intestinal Gel ENG SMPC - 09001be68007fc9a PDFmochkurniawanPas encore d'évaluation
- Medical Devices MPI Insights and Rankings 2017Document15 pagesMedical Devices MPI Insights and Rankings 2017mochkurniawanPas encore d'évaluation
- System: Total Solution For Value-Based Healthcare PurchasingDocument17 pagesSystem: Total Solution For Value-Based Healthcare PurchasingmochkurniawanPas encore d'évaluation
- Jan 2014 Nadine Nakazawa RNDocument70 pagesJan 2014 Nadine Nakazawa RNmochkurniawanPas encore d'évaluation
- SOP - Reducing CVL Related Blood - Stream Infections - Paediatrics Oncology PTDocument4 pagesSOP - Reducing CVL Related Blood - Stream Infections - Paediatrics Oncology PTmochkurniawanPas encore d'évaluation
- Neonatal Exposure To DEHPDocument24 pagesNeonatal Exposure To DEHPmochkurniawanPas encore d'évaluation
- Endotracheal Tube Cuffs:: Design and FunctionDocument8 pagesEndotracheal Tube Cuffs:: Design and FunctionmochkurniawanPas encore d'évaluation
- Philippines Meddev05Document10 pagesPhilippines Meddev05rein_iceePas encore d'évaluation
- Investing in IndonesiaDocument60 pagesInvesting in IndonesiaJustice SeekerPas encore d'évaluation
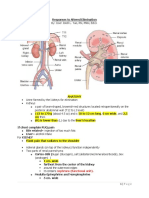
- Nephrons (Functional Unit)Document44 pagesNephrons (Functional Unit)Nur SanaaniPas encore d'évaluation
- It 18 - Neonatal Seizure - HerDocument35 pagesIt 18 - Neonatal Seizure - HerRurie Awalia SuhardiPas encore d'évaluation
- Primary school teachers lack knowledge of autism disordersDocument7 pagesPrimary school teachers lack knowledge of autism disordersArunasis AdhikariPas encore d'évaluation
- Anticestodal Drugs for Tapeworm TreatmentDocument3 pagesAnticestodal Drugs for Tapeworm TreatmentAbiHa YousaufPas encore d'évaluation
- Advances in Extraction TechniquesDocument13 pagesAdvances in Extraction TechniquesashajangamPas encore d'évaluation
- Clinical Biochemistry ReviewDocument10 pagesClinical Biochemistry Reviewyaykatai100% (2)
- 17-6 eJDD FinalDocument100 pages17-6 eJDD FinalMohamed GamalPas encore d'évaluation
- Blood and Tissue Coccidian GuideDocument40 pagesBlood and Tissue Coccidian GuideMichael DawitPas encore d'évaluation
- Total Leukocyte Count by HemocytometerDocument4 pagesTotal Leukocyte Count by HemocytometerMalkish RajkumarPas encore d'évaluation
- Rapid Pathogen Detection by Metagenomic Next-Generation Sequencing of Infected Body FluidsDocument26 pagesRapid Pathogen Detection by Metagenomic Next-Generation Sequencing of Infected Body FluidsLuisPas encore d'évaluation
- PrimaquineDocument3 pagesPrimaquineVijayakumar NsPas encore d'évaluation
- Past PapaersDocument515 pagesPast PapaersShariq ShaPas encore d'évaluation
- Urolithiasis Overview: Classification, Pathogenesis and Treatment ModalitiesDocument38 pagesUrolithiasis Overview: Classification, Pathogenesis and Treatment Modalitiesraed ganmPas encore d'évaluation
- Erectile DysfunctionDocument145 pagesErectile Dysfunctionluna palitoPas encore d'évaluation
- Prostaglandins: An Overview of Structure and FunctionDocument33 pagesProstaglandins: An Overview of Structure and FunctionMuhammad JamalPas encore d'évaluation
- Typhoid Fever NCPDocument46 pagesTyphoid Fever NCPLyra Lustre RN67% (3)
- Femur and Pelvis Fracture (Trauma)Document20 pagesFemur and Pelvis Fracture (Trauma)Ree YahPas encore d'évaluation
- Asthma Attack Nursing Care Plan for Married Female PatientDocument5 pagesAsthma Attack Nursing Care Plan for Married Female PatientMarivic Yuson MalagarPas encore d'évaluation
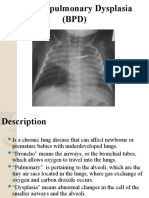
- Bronchopulmonary Dysplasia (BPD)Document13 pagesBronchopulmonary Dysplasia (BPD)Joan BuiPas encore d'évaluation
- Vaksin HexaximDocument50 pagesVaksin HexaximApeliaPas encore d'évaluation
- Mini-implant molar intrusion caseDocument1 pageMini-implant molar intrusion caseVesna AndreevskaPas encore d'évaluation
- Interpretting ABG SuccessfullyDocument15 pagesInterpretting ABG Successfullyanimathz100% (1)
- ACLS NotesDocument3 pagesACLS Notessaxmanwrv0% (1)
- ShineDocument37 pagesShineMohd SaifPas encore d'évaluation
- Global Tuberculosis Report 2018 PDFDocument243 pagesGlobal Tuberculosis Report 2018 PDFDudungPas encore d'évaluation
- TimeWise Miracle Set 3D Fact Sheet MYSG ENGDocument2 pagesTimeWise Miracle Set 3D Fact Sheet MYSG ENGKilinSilinPas encore d'évaluation
- Auditory Brainstem Response - ABR - in Clinical Practice PDFDocument9 pagesAuditory Brainstem Response - ABR - in Clinical Practice PDFary wisma dewiPas encore d'évaluation
- Retrograde Intubation Using Epidural Catheter - A Safe and Cost Effective Technique - A Case ReportDocument2 pagesRetrograde Intubation Using Epidural Catheter - A Safe and Cost Effective Technique - A Case ReportIOSRjournalPas encore d'évaluation
- Rheumatic Fever For All For DR Wilfredo Stokes B. Guatemala Nov 2,009Document9 pagesRheumatic Fever For All For DR Wilfredo Stokes B. Guatemala Nov 2,009drwstokes100% (1)
- ACTIVIDAD INGLES Reading ComprehensionDocument3 pagesACTIVIDAD INGLES Reading Comprehensionyulis mesaPas encore d'évaluation