Académique Documents
Professionnel Documents
Culture Documents
J 1471-0528 2011 03023 X
Transféré par
ronny29Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
J 1471-0528 2011 03023 X
Transféré par
ronny29Droits d'auteur :
Formats disponibles
Systematic review
DOI: 10.1111/j.1471-0528.2011.03023.x
www.bjog.org
Consequences of hyperemesis gravidarum for
offspring: a systematic review and meta-analysis
MVE Veenendaal,a AFM van Abeelen,a RC Painter,b JAM van der Post,b TJ Rosebooma
a
Department of Clinical Epidemiology, Biostatistics and Bioinformatics and b Department of Obstetrics and Gynaecology, Academic Medical
Centre, University of Amsterdam, Amsterdam, the Netherlands
Correspondence: Dr M Veenendaal, Department of Clinical Epidemiology, Biostatistics and Bioinformatics, Academic Medical Centre,
University of Amsterdam, Meibergdreef 9, PO Box 22660, 1100 DD Amsterdam, the Netherlands. Email m.v.veenendaal@amc.uva.nl
Accepted 4 April 2011. Published Online 12 July 2011.
Background There is evidence that hyperemesis gravidarum (HG)
Main results Women with HG during pregnancy were more likely
is associated with a predominance of female fetuses, lower
birthweights and shorter gestational ages at birth. As the adverse
effects of prematurity and low birthweight on disease risk in later
life have become increasingly clear, the repercussions of HG might
not be limited to adverse perinatal outcomes.
to have a female child (OR 1.27; 95% CI 1.211.34). They were
also more likely to have a baby with low birthweight (LBW,
<2500 kg; OR 1.42; 95% CI 1.271.58) that was small for
gestational age (SGA; OR 1.28; 95% CI 1.021.60), and to deliver
prematurely (OR 1.32; 95% CI 1.041.68). There was no
association with Apgar scores, congenital anomalies or perinatal
death. One study described an association between HG and
testicular cancer in the offspring.
Objectives To summarise the evidence on short- and long-term
outcomes of pregnancies with HG.
Search strategy A literature search was conducted in the
neonatal and long-term outcome of pregnancies complicated by
HG.
Authors conclusions There is evidence that HG is associated with
a higher female/male ratio of offspring and a higher incidence of
LBW, SGA and premature babies. Little is known about the longterm health effects of babies born to mothers whose pregnancies
were complicated by HG.
Data collection and analysis Two authors independently selected
Keywords Hyperemesis gravidarum, long-term effects, meta-analy-
studies and extracted data. Meta-analysis was performed using
review manager.
sis, perinatal outcome.
electronic databases Medline and Embase.
Selection criteria Studies were included that reported on the fetal,
Please cite this paper as: Veenendaal M, van Abeelen A, Painter R, van der Post J, Roseboom T. Consequences of hyperemesis gravidarum for offspring: a
systematic review and meta-analysis. BJOG 2011;118:13021313.
Introduction
Many women suffer from nausea and vomiting in early
pregnancy: the incidence has been estimated to be up to
5070% of pregnancies.1 Hyperemesis gravidarum (HG) is
a severe form of nausea and vomiting during pregnancy.
HG is associated with fluid, electrolyte and acidbase
imbalance, nutrition deficiency and weight loss, often
severe enough to require hospital admission. Symptoms
typically start at 48 weeks of gestation, and continue to
1416 weeks of gestation.2,3 HG occurs in 0.32% of pregnancies,4 and is associated with significant maternal morbidity.5
It is unclear whether HG has short- or long-term effects
on the offspring. Most frequently, studies on HG report
1302
the effects as perinatal outcome, including birthweight and
gestational age. The reported effects of HG on birthweight
and gestational age are conflicting, with some studies
reporting shorter gestational ages and lower birthweights
associated with HG pregnancies,4 and with others reporting
no effects.6 A large body of evidence from epidemiologic
and animal studies suggests that under-nutrition during
pregnancy increases the risk of disease in later life.79
HG may thus be hypothesised to have long-term health
effects resulting from suboptimal fetal nutrition.
As the long-term effects of HG are unclear and the
short-term consequences that are reported are inconsistent,
the aim of this review is to summarise the available evidence regarding the fetal outcome and long-term effects of
pregnancies complicated by HG.
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
Consequences of hyperemesis gravidarum for offspring
Methods
Search strategy
We performed an electronic search to identify all studies
that report on the short- and long-term outcomes of HG.
We searched Central, Medline (1953January 2011) and
Embase (1980January 2011) using a search strategy with
the following keywords: hyperemesis gravidarum, pernicious vomiting of pregnancy, neonate, infant, newborn
and long-term effects. Reference lists of review articles
and primary studies were checked to identify cited articles
not captured by the electronic search.
205 potentially eligible studies identified
(database searches and references lists)
163 studies were excluded based on title
and abstract review
2 studies excluded based on language
criterion
40 full text articles reviewed
16 studies excluded for not having the
required exposure/not reporting the
outcome of interest/no control group
Study selection
Studies were selected in a two-stage process. First, two
reviewers (MV and TR) scrutinised titles and abstracts.
Studies were selected if they reported on the neonatal
outcome of pregnancies complicated by HG and were
written in English. Full articles were obtained of all
selected studies. Second, inclusion and exclusion decisions
were made after an independent examination of the full
articles of selected references by two reviewers (MV and
AA). Inclusion criteria were: (1) patients diagnosed with
and/or admitted for HG; (2) reported neonatal outcomes,
including low birthweight (LBW), small for gestational
age (SGA), sex of the offspring, perinatal death, prematurity, congenital anomalies and long-term health outcomes.
Studies that reported on single and multiple pregnancies
were included. Studies that did not report a control group
were excluded. Any disagreements were resolved by
consensus.
Two independent reviewers (MV and AA) extracted the
data. Meta-analyses were conducted (review manager 5.0;
The Cochrane Collaboration, 2008.). All outcomes were
evaluated with a random-effects model. Dichotomous outcomes were pooled as an odds ratio (OR) with 95% confidence interval (95% CI). Data were plotted in forest plots.
The I2 test was used to assess statistical heterogeneity.
Subgroup analyses were performed for case control and
cohort studies separately. The meta-analysis of observational studies in epidemiology (MOOSE) guidelines were
followed.10
Results
The search resulted in 205 studies. After screening titles
and abstracts, 163 studies were excluded because they did
not report on neonatal outcome of pregnancies complicated by HG. Another two studies were excluded because
of the language criterion. In total, 40 papers were retrieved
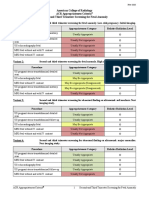
for complete assessment (Figure 1); 24 articles reported on
short- and long-term outcomes, as described above
(Table 1).4,6,1132 The quality of reporting was limited: a
24 studies were included in the
systematic review
Figure 1. Study selection process.
clear definition of the reference group was not always
given. Most studies reported singleton pregnancies only.
In some studies, it was not stated whether twin pregnancies
were included. There were ten cohort studies, 13 case
control studies and one cross-sectional study. Four studies
were conducted prospectively; all others were retrospective.
Meta-analysis was conducted for studies that provided
dichotomous data.
Sex of child
Thirteen studies reported the gender of the offspring.1113,16,18,21,24,2629,31,32 All studies confirmed the
higher female/male ratio in pregnancies complicated by HG:
overall, 55% of the offspring in the HG pregnancies were
female, compared with 49% in the control group, with a
pooled odds ratio of 1.27 (95% CI 1.211.34) and with
moderate heterogeneity (I2 = 54%; P = 0.01) (Figure 2A).
Low birthweight
Five studies reported on delivering an LBW baby
(<2500 g).4,6,18,26,31 Having an LBW baby with a birthweight of <2500 g occurred in 6.4% of HG pregnancies,
compared with 5.0% in control pregnancies (OR 1.42;
95% CI 1.271.58). There was no significant heterogeneity
in results across the different studies (I2 = 0%; P = 0.42)
(Figure 2B).
Small for gestational age
The percentage of SGA infants was reported in four studies.4,18,31,32 Women with HG during pregnancy were more
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
1303
Veenendaal et al.
Table 1. Characteristics of studies included in the review of short- and long-term outcomes of pregnancies complicated by hyperemesis
gravidarum
Study
Askling et al.11
Study design
Definition
Admitted/
diagnosed
Birth cohort
retrospective
Birth cohort
retrospective
ICD9
Admitted
ICD9
Admitted
Bashiri et al.12
Casecontrol
retrospective
Fairweather
criteria2
Admitted
164 HG/209
control
Basso et al.13
Casecontrol
retrospective
Casecontrol
Discharge
diagnoses
Fairweather
criteria2
ICD9
Admitted
6084 HG/76
804 control
46 severe HG/8802
control
ICD8
Admitted &
diagnosed
Diagnosed
4126 HG/127
647 total
419 HG/836
control
Admitted
1270 HG/154
821 control
138 HG/12
335 control
Bailit4
Chin et al.14
Czeizel et al.15
del Mar
Melero et al.16
Depue et al.17
Casecontrol
nonsyndromic
cleft patients
retrospective
Cohort
retrospective
Casecontrol
prospective
Admitted
5926 HG/1 027
213 total
2466 HG/520
739 total
ns
Dodds et al.18
Cohort
retrospective
Diagnosis
criteria varied
per centre
Fairweather
criteria2
Hallak et al.19
Casecontrol
retrospective
Fairweather
criteria2
Admitted
Henderson et al.20
Casecontrol
testicular
cancer patients
Casecontrol
retrospective
Cohort
retrospective
Cross sectional
Excessive
nausea
ns
Severe HG
Admitted
ICD8
Diagnosed
66 HG/20
798 control
3068 HG cases
Clinical
diagnosis
Fairweather
criteria2
Diagnosed
12 HG/34 control
Admitted
45 HG/306 control
Clinical
diagnosis
ns
42 HG/336 total
Hsu et al.21
Kallen22
Kaul et al.23
Paauw et al.24
Cohort
prospective
Roberts25
Cohort
1304
Outcome
Sex of child
BW
Gestational age
SGA
Perinatal death
BW
Gestational age
Sex of child
Perinatal death
Congenital anomalies
Sex of child
BW
Gestational age
HG
Sex of child
BW
Perinatal death
CNS malformations
BW
SGA
Prematurity
Apgar
Sex of child
Perinatal death
BW
Prematurity
Apgar
Congenital
anomalies
HG
Sex of child
BW
Sex of child
BW
BW
Gestational age
Apgar
Prematurity
Sex of child
Neurological and
developmental scores
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
Consequences of hyperemesis gravidarum for offspring
Table 1. (Continued)
Study
Study design
Definition
Admitted/
diagnosed
Outcome
Roseboom et al.32
Birth cohort
retrospective
Clinical
diagnosis
Diagnosed
2190 HG/1 197
028 control
Schiff et al.26
Casecontrol
retrospective
ICD9
Admitted
2110 HG/9783
control
Sorensen et al.27
Cohort
retrospective
Casecontrol
retrospective
Casecontrol
retrospective
ICD8 & 10
Admitted
Clinical
diagnosis
Clinical
diagnosis
Admitted
650 HG/47
931 total
166 HG/4761
control
166 HG/498
control
BW
SGA
Prematurity
Apgar
Sex of child
Perinatal death
BW
Prematurity
Sex of child
Sex of child
Tsang et al.29
Casecontrol
Retrospective
Clinical
diagnosis
Admitted &
diagnosed
193 HG/13
053 total
Vilming et al.30
Casecontrol
retrospective
ICD9
Admitted
120 HG/115
control
Zhang et al.31
Cohort
retrospective
Clinical
diagnosis
severe
vomiting
ns
201 HG/1666
control
Tan et al.28
Tan et al.6
Admitted
Sex of child
BW
Gestational age
Prematurity
Apgar
Prematurity
Apgar
Sex of child
Perinatal death
Congenital
anomalies
BW
Sex of child
Gestational age
BW
Prematurity
SGA
Sex of child
ns, not specified.
likely to have an SGA baby: this occurred in 17.9% of HG
pregnancies, compared with 12.7% in control pregnancies
(OR 1.28; 95% CI 1.021.60). There was significant heterogeneity across the different studies for SGA (I2 = 87%;
P < 0.0001) (Figure 2C).
Preterm delivery
Eight studies reported on preterm delivery.6,18,19,24,26,29,31,32
Premature delivery occurred in 7.4% of HG pregnancies,
compared with 5.8% in control pregnancies. HG during
pregnancy was associated with an increased risk of delivering before 37 weeks of gestation (OR 1.32; 95% CI 1.04
1.68). There was significant heterogeneity in the results
(I2 = 74%; P = 0.0003) (Figure 2D).
Perinatal deaths
Seven studies reported on perinatal deaths.4,6,12,17,18,29,32
Perinatal deaths occurred in 0.7% of HG pregnancies, and
in 0.6% of control pregnancies (OR 0.92; 95% CI 0.61
1.41). Heterogeneity was moderate (I2 = 42%; P = 0.11)
(Figure 2E).
Apgar scores
Apgar scores of <7 at 5 minutes were reported in four
studies.6,18,19,32 No difference was found in the incidence of
5-minute Apgar scores of <7: this occurred in 1.9% of HG
pregnancies and 2.3% of control pregnancies (OR 1.01;
95% CI 0.781.32). Heterogeneity was not significant
(I2 = 7%; P = 0.36) (Figure 2F).
Congenital anomalies
Six studies compared the number of congenital anomalies
in children born to HG mothers with those of control offspring.12,15,17,19,22,29 Three studies provided data suitable
for pooling. There was no difference in the number of congenital anomalies in HG pregnancies (3.1%) compared
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
1305
Veenendaal et al.
A Sex of offspring
HG
Study or subgroup
Events
Control
Total Events
Odds ratio
Total Weight
Odds ratio
M-H, random, 95% CI
5926 496345 1021287
16.6%
1.33 [1.26, 1.40]
164
105
209
1.4%
1.01 [0.67, 1.53]
3337
6227
38138
77719
16.5%
1.20 [1.14, 1.26]
del Mar 2001 (16)
1739
3249
60081
123521
14.5%
1.22 [1.13, 1.30]
Dodds 2006 (18)
692
1270
75506
154821
10.2%
1.26 [1.13, 1.41]
Hsu 1993 (21)
44
66
10145
20798
0.9%
2.10 [1.26, 3.51]
Paauw 2005 (24)
24
45
156
306
0.6%
1.10 [0.59, 2.06]
Askling 1999 (11)
3299
Bashiri 1995 (12)
83
Basso 2001 (13)
Roseboom 2011 (32)
1176
2190 584150 1197028
12.9%
1.22 [1.12, 1.32]
Schiff 2004 (26)
1214
2110
4717
9783
11.7%
1.46 [1.32, 1.60]
Sorensen 2000 (27)
348
650
23026
47281
7.0%
1.21 [1.04, 1.42]
Tan 2006 (28)
100
166
2311
4761
2.3%
1.61 [1.17, 2.20]
Tsang 1996 (29)
102
193
6430
12860
2.7%
1.12 [0.84, 1.49]
Zhang 1991 (31)
109
201
811
1666
2.6%
1.25 [0.93, 1.68]
2672040
100.0%
1.27 [1.21, 1.34]
22457
Total (95% CI)
Total events
M-H, random, 95% CI
1301921
12267
Heterogeneity: t = 0.00; c = 26.29, df = 12 (P = 0.010); I = 54%
0.5 0.7
1
1.5 2
Less female fetuses More female fetuses
Test for overall effect: Z = 9.24 (P < 0.00001)
B Low birth weight
HG
Study or subgroup
Odds ratio
Control
Events Total Events
Total Weight
M-H, random, 95% CI
177 2270
24812 486505
49.3%
1.57 [1.35, 1.84]
Dodds 2006 (18)
72 1270
7143 154821
20.5%
1.24 [0.98, 1.58]
Schiff 2004 (26)
106 2110
Bailit 2005 (4)
386
9783
24.1%
1.29 [1.03, 1.60]
Tan 2007 (6)
18
166
44
498
3.5%
1.25 [0.70, 2.24]
Zhang 1991 (31)
11
201
62
1666
2.7%
1.50 [0.78, 2.89]
653273
100.0%
1.42 [1.27, 1.58]
Total (95% CI)
Total events
6017
384
Odds ratio
M-H, random, 95% CI
32447
Heterogeneity: t = 0.00; c = 3.88, df = 4 (P = 0.42); I = 0%
0.1 0.2
0.5 1
2
5
Less in HG More in HG
Test for overall effect: Z = 6.30 (P < 0.00001)
10
C Small for gestational age
HG
Study or subgroup
Odds ratio
Control
Events Total Events
Total Weight
M-H, random, 95% CI
Bailit 2005 (4)
663 2270 101193
486505
30.4%
1.57 [1.43, 1.72]
Dodds 2006 (18)
137 1270
15217
154821
26.7%
1.11 [0.93, 1.33]
Roseboom 2011 (32)
237 2190 117309 1197028
28.7%
1.12 [0.98, 1.28]
1666
14.1%
1.40 [0.90, 2.20]
1840020
100.0%
1.28 [1.02, 1.60]
Zhang 1991 (31)
25
5931
Total (95% CI)
Total events
153
201
1062
Odds ratio
M-H, random, 95% CI
233872
Heterogeneity: t = 0.04; c = 22.95, df = 3 (P < 0.0001); I = 87%
Test for overall effect: Z = 2.12 (P = 0.03)
0.2
0.5
1
2
5
Less in HG More in HG
Figure 2. Perinatal outcome: sex of offspring, A; low birthweight (<2500 g), B; small for gestational age, C; preterm (<37 weeks of gestation), D;
perinatal death, E; Apgar score <7, F; and congenital anomalies, G.
with controls (3.2%) (OR 1.17; 95% CI 0.682.03). There
was no significant heterogeneity in results across the different studies (I2 = 0%; P = 0.87) (Figure 2G).
Three other studies reported on specific congenital
anomalies. A cohort study reported several congenital
1306
malformations associated with HG, including undescended
testicles, hip dysplasia and trisomy 21.22 A casecontrol
study of children born with an oral cleft showed an association between early-onset HG and a reduced risk of giving
birth to a child with an oral cleft.15 Another casecontrol
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
Consequences of hyperemesis gravidarum for offspring
D Preterm delivery
HG
Study or subgroup
Control
Events Total Events
Odds ratio
Total Weight
Dodds 2006 (18)
82 1270
8233
154821
18.0%
Hallak 1996 (19)
11
98
1320
12335
8.7%
1.06 [0.56, 1.98]
Paauw 2005 (24)
14
45
15
306
6.2%
8.76 [3.87, 19.83]
68231 1197028
Roseboom 2011 (32)
166 2190
Schiff 2004 (26)
132 2110
Tan 2007 (6)
19.5%
1.36 [1.16, 1.59]
445
9783
18.6%
1.40 [1.15, 1.71]
166
36
498
6.5%
0.65 [0.30, 1.43]
Tsang 1996 (29)
44
193
2829
12860
15.0%
1.05 [0.75, 1.47]
Zhang 1991 (31)
201
72
1666
7.5%
1.04 [0.51, 2.11]
1389297
100.0%
1.32 [1.04, 1.68]
Total events
6273
466
M-H, random, 95% CI
1.23 [0.98, 1.54]
Total (95% CI)
Odds ratio
M-H, random, 95% CI
81181
Heterogeneity: t = 0.07; c = 27.32, df = 7 (P = 0.0003); I = 74%
0.05
Test for overall effect: Z = 2.27 (P = 0.02)
0.2
1
5
Less in HG More in HG
20
E Perinatal death
HG
Study or subgroup
Control
Events Total Events
Bailit 2005 (4)
16 2270
Odds ratio
Total Weight
2092
486505
24.4%
1.64 [1.00, 2.69]
Bashiri 1995 (12)
164
209
6.4%
0.95 [0.21, 4.33]
Depue 1987 (17)
419
24
836
13.6%
0.49 [0.20, 1.21]
Dodds 2006 (18)
6 1270
939
154821
15.6%
0.78 [0.35, 1.74]
Roseboom 2011 (32)
7 2190
7182 1197028
17.1%
0.53 [0.25, 1.12]
Tan 2007 (6)
166
498
3.1%
1.00 [0.10, 9.68]
10
193
530
12860
19.8%
1.27 [0.67, 2.42]
1852757
100.0%
0.92 [0.61, 1.41]
Tsang 1996 (29)
Total (95% CI)
6672
Total events
49
Odds ratio
M-H, random, 95% CI
M-H, random, 95% CI
10774
Heterogeneity: t = 0.12; c = 10.38, df = 6 (P = 0.11); I = 42%
0.05
Test for overall effect: Z = 0.37 (P = 0.71)
0.2
1
5
20
Less in HG More in HG
F Apgar score <7
HG
Study or subgroup
Control
Events Total Events
Dodds 2006 (18)
19 1270
Hallak 1996 (19)
Roseboom 2011 (32)
198
50 2186
Tan 2007 (6)
Total (95% CI)
166
154821
29.8%
1.22 [0.78, 1.93]
259
12335
1.8%
0.24 [0.03, 1.70]
28596 1191519
66.1%
0.95 [0.72, 1.26]
498
2.4%
1.51 [0.27, 8.30]
1359173
100.0%
1.01 [0.78, 1.32]
72
Odds ratio
M-H, random, 95% CI
1898
3820
Total events
Odds ratio
Total Weight
M-H, random, 95% CI
30757
Heterogeneity: t = 0.01; c = 3.21, df = 3 (P = 0.36); I = 7%
0.05
Test for overall effect: Z = 0.09 (P = 0.93)
0.2
1
5
20
Less in HG More in HG
G Congenital anomalies
HG
Study or subgroup
Control
Events Total Events
Odds ratio
Total Weight
Bashiri 1995 (12)
164
209
5.2%
0.63 [0.06, 7.06]
Hallak 1996 (19)
98
192 12335
15.2%
1.32 [0.32, 5.38]
Tsang 1996 (29)
11
193
621 12860
79.7%
1.19 [0.64, 2.20]
25404 100.0%
1.17 [0.68, 2.03]
Total (95% CI)
Total events
455
14
Odds ratio
M-H, random, 95% CI
M-H, random, 95% CI
815
Heterogeneity: t = 0.00; c = 0.28, df = 2 (P = 0.87); I = 0%
Test for overall effect: Z = 0.56 (P = 0.57)
0.05
0.2
1
5
20
Less in HG More in HG
Figure 2. (Continued)
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
1307
Veenendaal et al.
A Sex of child
HG
Study or subgroup
Odds ratio
Control
Total Weight
Total Events
Events
Odds ratio
M-H, random, 95% CI
M-H, random, 95% CI
1.1.1 Cohort studies
Askling 1999 (11)
3299
5926 496345 1021287
16.6%
1.33 [1.26, 1.40]
del Mar 2001 (16)
1739
3249
60081
123521
14.5%
1.22 [1.13, 1.30]
Dodds 2006 (18)
692
1270
75506
154821
10.2%
1.26 [1.13, 1.41]
Paauw 2005 (24)
24
45
156
306
0.6%
1.10 [0.59, 2.06]
2190 584150 1197028
12.9%
1.22 [1.12, 1.32]
Roseboom 2011 (32)
1176
Sorensen 2000 (27)
348
650
23026
47281
7.0%
1.21 [1.04, 1.42]
Zhang 1991 (31)
Subtotal (95% CI)
109
201
13531
811
1666
2545910
2.6%
64.3%
1.25 [0.93, 1.68]
1.27 [1.23, 1.31]
Total events
1240075
7387
Heterogeneity: t = 0.00; c = 5.96, df = 6 (P = 0.43); I = 0%
Test for overall effect: Z = 13.67 (P < 0.00001)
1.1.2 Case control studies
Bashiri 1995 (12)
83
164
105
209
1.4%
1.01 [0.67, 1.53]
Basso 2001 (13)
3337
6227
38138
77719
16.5%
1.20 [1.14, 1.26]
44
66
10145
20798
0.9%
2.10 [1.26, 3.51]
1214
2110
4717
9783
11.7%
1.46 [1.32, 1.60]
Tan 2006 (28)
100
166
2311
4761
2.3%
1.61 [1.17, 2.20]
Tsang 1996 (29)
Subtotal (95% CI)
102
193
8926
6430
12860
126130
2.7%
35.7%
1.12 [0.84, 1.49]
1.33 [1.15, 1.54]
Hsu 1993 (21)
Schiff 2004 (26)
Total events
61846
4880
Heterogeneity: t = 0.02; c = 20.24, df = 5 (P = 0.001); I = 75%
Test for overall effect: Z = 3.80 (P = 0.0001)
Total (95% CI)
Total events
2672040
22457
12267
100.0%
1.27 [1.21, 1.34]
1301921
Heterogeneity: t = 0.00; c = 26.29, df = 12 (P = 0.010); I = 54%
0.5
0.7
1
1.5
2
Less female fetuses More female fetuses
Test for overall effect: Z = 9.24 (P < 0.00001)
Test for subgroup differences: c = 0.35, df = 1 (P = 0.55), I = 0%
B Low birth weight
HG
Study or subgroup
Odds ratio
Control
Events Total Events
Total Weight
M-H, random, 95% CI
Odds ratio
M-H, random, 95% CI
4.1.1 Cohort studies
177 2270
24812 486505
49.3%
1.57 [1.35, 1.84]
Dodds 2006 (18)
72 1270
7143 154821
20.5%
1.24 [0.98, 1.58]
Zhang 1991 (31)
Subtotal (95% CI)
11
1666
642992
2.7%
72.4%
1.50 [0.78, 2.89]
1.45 [1.22, 1.71]
Bailit 2005 (4)
Total events
62
201
3741
32017
260
Heterogeneity: t = 0.01; c = 2.66, df = 2 (P = 0.26); I = 25%
Test for overall effect: Z = 4.32 (P < 0.0001)
4.1.2 Case control studies
Schiff 2004 (26)
Tan 2007 (6)
Subtotal (95% CI)
Total events
106 2110
386
9783
24.1%
1.29 [1.03, 1.60]
166
2276
44
498
10281
3.5%
27.6%
1.25 [0.70, 2.24]
1.28 [1.04, 1.58]
100.0%
1.42 [1.27, 1.58]
18
430
124
Heterogeneity: t = 0.00; c = 0.01, df = 1 (P = 0.93); I = 0%
Test for overall effect: Z = 2.38 (P = 0.02)
Total events
653273
6017
Total (95% CI)
384
32447
Heterogeneity: t = 0.00; c = 3.88, df = 4 (P = 0.42); I = 0%
Test for overall effect: Z = 6.30 (P < 0.00001)
Test for subgroup differences: c = 0.77, df = 1 (P = 0.38), I = 0%
0.5 0.7 1 1.5 2
Less in HG More in HG
Figure 3. Perinatal outcome, subanalyses based on study design and overall summary estimates: sex of offspring, A; low birthweight (<2500 g), B;
preterm (<37 weeks of gestation), C; perinatal death, D; and Apgar score <7, E.
1308
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
Consequences of hyperemesis gravidarum for offspring
C Preterm delivery
HG
Study or subgroup
Control
Odds ratio
Total Weight
Events Total Events
Odds ratio
M-H, random, 95% CI
M-H, random, 95% CI
6.1.1 Cohort studies
Dodds 2006 (18)
82 1270
8233
154821
18.0%
1.23 [0.98, 1.54]
Paauw 2005 (24)
14
45
15
306
6.2%
8.76 [3.87, 19.83]
68231 1197028
19.5%
1.36 [1.16, 1.59]
1666
1353821
7.5%
51.2%
1.04 [0.51, 2.11]
1.69 [1.08, 2.65]
Roseboom 2011 (32)
166 2190
Zhang 1991 (31)
Subtotal (95% CI)
Total events
201
3706
72
76551
271
Heterogeneity: t = 0.15; c = 21.32, df = 3 (P < 0.0001); I = 86%
Test for overall effect: Z = 2.29 (P = 0.02)
6.1.2 Case control studies
Hallak 1996 (19)
98
1320
12335
8.7%
1.06 [0.56, 1.98]
132 2110
445
9783
18.6%
1.40 [1.15, 1.71]
166
36
498
6.5%
0.65 [0.30, 1.43]
44
193
2567
2829
12860
35476
15.0%
48.8%
1.05 [0.75, 1.47]
1.14 [0.87, 1.49]
100.0%
1.32 [1.04, 1.68]
11
Schiff 2004 (26)
Tan 2007 (6)
Tsang 1996 (29)
Subtotal (95% CI)
Total events
4630
195
Heterogeneity: t = 0.03; c = 5.23, df = 3 (P = 0.16); I = 43%
Test for overall effect: Z = 0.98 (P = 0.33)
Total (95% CI)
1389297
6273
Total events
81181
466
Heterogeneity: t = 0.07; c = 27.32, df = 7 (P = 0.0003); I = 74%
0.05
Test for overall effect: Z = 2.27 (P = 0.02)
Test for subgroup differences: c = 2.16, df = 1 (P = 0.14), I = 53.7%
0.2
1
5
Less in HG More in HG
20
D Perinatal death
HG
Study or subgroup
Odds ratio
Control
Events Total Events
Total Weight
Odds ratio
M-H, random, 95% CI
M-H, random, 95% CI
7.1.1 Cohort studies
16 2270
2092
486505
24.4%
1.64 [1.00, 2.69]
Dodds 2006 (18)
6 1270
939
154821
15.6%
0.78 [0.35, 1.74]
Roseboom 2011 (32)
Subtotal (95% CI)
7 2190
5730
7182 1197028
1838354
17.1%
57.1%
0.53 [0.25, 1.12]
0.92 [0.44, 1.94]
Bailit 2005 (4)
Total events
10213
29
Heterogeneity: t = 0.31; c = 7.35, df = 2 (P = 0.03); I = 73%
Test for overall effect: Z = 0.22 (P = 0.82)
7.1.2 Case control studies
Bashiri 1995 (12)
164
209
6.4%
0.95 [0.21, 4.33]
Depue 1987 (17)
419
24
836
13.6%
0.49 [0.20, 1.21]
Tan 2007 (6)
166
498
3.1%
1.00 [0.10, 9.68]
Tsang 1996 (29)
Subtotal (95% CI)
10
193
942
530
12860
14403
19.8%
42.9%
1.27 [0.67, 2.42]
0.93 [0.57, 1.51]
Total events
20
100.0%
0.92 [0.61, 1.41]
561
Heterogeneity: t = 0.00; c = 2.88, df = 3 (P = 0.41); I = 0%
Test for overall effect: Z = 0.29 (P = 0.77)
Total events
1852757
6672
Total (95% CI)
49
10774
Heterogeneity: t = 0.12; c = 10.38, df = 6 (P = 0.11); I = 42%
Test for overall effect: Z = 0.37 (P = 0.71)
Test for subgroup differences: c = 0.00, df = 1 (P = 0.98), I = 0%
0.05
0.2
1
5
20
Less in HG More in HG
Figure 3. (Continued)
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
1309
Veenendaal et al.
E Apgar score <7
HG
Study or subgroup
Control
Events Total Events
Odds ratio
Total Weight
Odds ratio
M-H, random, 95% CI
M-H, random, 95% CI
8.1.1 Cohort studies
Dodds 2006 (18)
19 1270
154821
29.8%
1.22 [0.78, 1.93]
Roseboom 2011 (32)
Subtotal (95% CI)
50 2186
3456
28596 1191519
1346340
66.1%
95.8%
0.95 [0.72, 1.26]
1.02 [0.80, 1.30]
Total events
69
30494
1898
Heterogeneity: t = 0.00; c = 0.85, df = 1 (P = 0.36); I = 0%
Test for overall effect: Z = 0.16 (P = 0.87)
8.1.2 Case control studies
Hallak 1996 (19)
198
259
12335
1.8%
0.24 [0.03, 1.70]
Tan 2007 (6)
Subtotal (95% CI)
166
364
498
12833
2.4%
4.2%
1.51 [0.27, 8.30]
0.63 [0.09, 4.37]
Total events
100.0%
1.01 [0.78, 1.32]
263
Heterogeneity: t = 1.06; c = 2.21, df = 1 (P = 0.14); I = 55%
Test for overall effect: Z = 0.46 (P = 0.64)
Total (95% CI)
Total events
1359173
3820
72
30757
Heterogeneity: t = 0.01; c = 3.21, df = 3 (P = 0.36); I = 7%
0.02
Test for overall effect: Z = 0.09 (P = 0.93)
Test for subgroup differences: c = 0.23, df = 1 (P = 0.63), I = 0%
0.1
1
10
50
Less in HG More in HG
Figure 3. (Continued)
study reported an increase in central nervous system and
related skeletal malformations in offspring of mothers that
experienced HG (OR 4.0).17
Long-term effects
No studies were found that were conducted specifically
with the purpose of following up the children born after a
pregnancy complicated by HG in the long term. One
study reported the neurological development of children
at 1 year of age and the obstetric history of their mothers.
There was no observed difference in outcome associated
with HG.25
The only long-term effect was an association of HG and
testicular cancer. In a casecontrol study of men under the
age of 40 years with testicular cancer, eight of the patients
mothers reported excessive nausea as a complication of the
index pregnancy, compared with two of the controls
mothers. The risk was greatest for nausea requiring hospital
treatment.20
Subgroup analyses
Figure 3 shows the summary estimates for the different
study types, as well as the combined summary estimates.
For the outcome SGA and congenital anomalies this analysis was not possible because these studies were all of the
same type. The subgroup analyses show that the observed
heterogeneity was not consistently caused by one type of
study.
1310
Discussion
This systematic review evaluates the outcome of pregnancies complicated by HG. HG during pregnancy is associated with a higher female/male ratio of the offspring, and
with a higher incidence of SGA babies with birthweights of
<2500 g and with preterm delivery. The search retrieved
only two studies reporting long-term effects. Neurological
development at the age of 1 year was not affected by HG
during pregnancy.25 There was an association of HG and
the development of testicular cancer in later life.20 There
was no statistically significant difference in Apgar scores,
congenital anomalies or perinatal death between HG pregnancies, compared with control pregnancies. However, heterogeneity was significant.
The mechanism underlying the higher prevalence of
female offspring after pregnancies complicated by HG is
thought to be hormonal. Serum human chorionic gonadotrophin (hCG) is often stated as the most likely cause of
HG. The highest incidences of HG occur at the time at
which hCG levels peak.33 Furthermore, HG has an increased
incidence in multiple gestation and molar pregnancies, both
conditions associated with elevated hCG levels.34,35 The fact
that hCG is higher in women bearing a female child might
explain the association between a female fetus and HG.36
Although meta-analysis showed an increased risk of
LBW and SGA babies, and prematurity, the effects are
modest. The most clinically relevant effect is probably for
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
Consequences of hyperemesis gravidarum for offspring
SGA babies: 17.9% in HG pregnancies compared with
12.7% in control pregnancies. The increased risk of LBW
could possibly be linked to prematurity, but this cannot be
concluded with certainty because different studies were
included in the three different meta-analyses, as not all
studies provided data for all outcomes.
Three studies investigated whether the effects of HG
were mediated through maternal weight gain during pregnancy.18,24,30 All found an association of lower weight gain
or weight loss during pregnancy and adverse neonatal outcomes, such as LBW. In one study, no difference in SGA
was reported when comparing HG pregnancies with controls, but when comparing HG women with <7 kg of
weight gain during pregnancy with HG women with 7 kg
or more weight gain, the risk of an SGA infant was
increased (OR 1.5; 95% CI 1.02.2).18 This study also compared Apgar scores of babies from women with HG with
7 kg weight gain or more with those of babies from women
with <7 kg of weight gain. Babies of women with <7 kg of
weight gain had an increased risk of having a 5-minute
Apgar score of <7 (OR 5.0; 95% CI 2.69.6) compared
with babies from women without HG.18 The authors
concluded that HG itself is not a risk factor for adverse
outcomes, but these outcomes are the consequence of the
low weight gain associated with HG. These findings are in
correspondence with findings from a retrospective cohort
study investigating weight gain during pregnancy. In this
study low maternal weight gain during pregnancy, defined
as <0.27 kg/week, was associated with LBW, preterm
labour and preterm delivery.37 Accordingly, a populationbased cohort study investigating the effects of low weight
gain in women with normal prepregnancy body mass
indices (BMIs) found an increased odds ratio for SGA
infants in women that gained <25 lb (11.34 kg) during
pregnancy.38 These studies stress the importance of appropriate maternal weight gain during pregnancy in order to
achieve healthy birth outcomes in women.
As mentioned earlier, the search retrieved only two studies reporting on long-term health effects.20,25 The reported
association of HG and testicular cancer in later life is proposed to be the result of hormonal imbalance. Apart from
higher levels of hCG, estradiol is elevated in HG pregnancies compared with controls. Exposure to higher levels of
estrogen in utero might be a cause of undescended testes,
thereby leading to a higher risk of testicular cancer in later
life.17,20,39
Other long-term health effects, such as cardiovascular
and metabolic disease, have not been studied, even though
there is ample evidence from human and animal studies
that under-nutrition during gestation increases the risk of
developing chronic diseases.79 Also, meta-analyses have
shown that birthweight was inversely related to a risk of
raised systolic blood pressure and type-II diabetes mell-
itus.40,41 Moreover, not all long-term effects of prenatal
environmental influences act via birthweight. Studies of
babies born after the Dutch famine show that exposure to
the famine in early gestation had no effect on birthweight,
but was associated with adverse health effects.42 Therefore,
follow-up of children born after an HG pregnancy seems
to be warranted.
The substantial heterogeneity between the studies could
result from both clinical and methodological heterogeneity.
Clinical heterogeneity is partly caused by the difficulty in
defining the condition. In most studies, Fairweathers definition for HG is used. This defines HG as a condition of
intractable vomiting during pregnancy, leading to fluid,
electrolyte and acidbase imbalance, nutrition deficiency
and weight loss, often severe enough to require hospital
admission.2 A weakness of this definition is the fact that it
does not include an estimate of the severity of the condition, apart from the need for hospital admission. Different
hospitals may have different admission policies, and it is
also possible that what is regarded as severe vomiting in one
population may be taken as normal vomiting in another.
The threshold for hospitalisation is highly individual. This
decision can be influenced by psychological and practical
matters, which contribute to the variability in the diagnosis.
The included studies were conducted in a variety of
countries, with different demographic profiles. The incidence of HG is thought to vary across different cultures,43
which will have contributed to the clinical heterogeneity.
Not every study specified the demographic profile of their
study population. As a recent study has shown, adverse
pregnancy outcomes after HG might be largely explained
by maternal characteristics, including ethnicity.32
Methodological heterogeneity can result from the fact
that more than 50% of the studies included are casecontrol studies, of which most are retrospective. Because of
these matters of study design the reported effects may be
overestimated. Subgroup analyses according to the different
study types gave no consistent explanation of the observed
heterogeneity; we cannot conclude that the heterogeneity
was caused by one type of study. In all cases, separately
analysing the study types would not have led to different
conclusions. A consequence of retrospective study design is
the possibility of recall bias, with regard to reported nausea
and prepregnancy weight.
Future research on HG and consequences for the offspring should include a clear definition of HG and complete documentation of maternal characteristics such as
ethnicity, prepregnancy weight and weight gain during
pregnancy, allowing for comparison between studies and
populations. Moreover, not only should the outcome be
documented directly postpartum, but a long-term followup of these babies, focusing on cardiovascular and metabolic functioning, should also be conducted.
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
1311
Veenendaal et al.
In conclusion, this meta-analysis reports that women
with HG during pregnancy are more likely to give birth to
a girl, and have a higher risk of giving birth to an LBW or
SGA child and of delivering prematurely. As little is known
about the long-term health consequences of these children,
there is a need for follow-up.
Disclosure of interests
None of the authors report any conflicts of interest.
Contribution to authorship
JP conceived the idea. MV, AA and TR conducted the literature search; MV and AA extracted the data. MV performed the statistical analysis and wrote the first and final
version of the article. All authors took part in revisions of
the article.
Details of ethics approval
Approval was not required.
Funding
MV is funded by the Netherlands Heart Foundation (grant
number 2007B083).
Acknowledgements
We would like to thank Mrs F. van Etten-Jamaludin for
her help in conducting the literature search. j
References
1 Jarnfelt-Samsioe A. Nausea and vomiting in pregnancy: a review.
Obstet Gynecol Surv 1987;42:4227.
2 Fairweather DV. Nausea and vomiting in pregnancy. Am J Obstet
Gynecol 1968;102:13575.
3 Niebyl JR. Clinical practice. Nausea and vomiting in pregnancy. N
Engl J Med 2010;363:154450.
4 Bailit JL. Hyperemesis gravidarium: epidemiologic findings from a
large cohort. Am J Obstet Gynecol 2005;193:8114.
5 Broussard CN, Richter JE. Nausea and vomiting of pregnancy.
Gastroenterol Clin North Am 1998;27:12351.
6 Tan PC, Jacob R, Quek KF, Omar SZ. Pregnancy outcome in hyperemesis gravidarum and the effect of laboratory clinical indicators of hyperemesis severity. J Obstet Gynaecol Res 2007;33:457
64.
7 Harding J. The nutritional basis of the fetal origins of adult disease.
Int J Epidemiol 2001;30:1523.
8 Nijland MJ, Ford SP, Nathanielsz PW. Prenatal origins of adult disease. Curr Opin Obstet Gynecol 2008;20:1328.
9 Gluckman PD, Hanson MA, Cooper C, Thornburg KL. Effect of in
utero and early-life conditions on adult health and disease. N Engl J
Med 2008;359:6173.
10 Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D,
et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 2000;283:200812.
11 Askling J, Erlandsson G, Kaijser M, Akre O, Ekbom A. Sickness in
pregnancy and sex of child. Lancet 1999;354:2053.
1312
12 Bashiri A, Neumann L, Maymon E, Katz M. Hyperemesis gravidarum:
epidemiologic features, complications and outcome. Eur J Obstet
Gynecol Reprod Biol 1995;63:1358.
13 Basso O, Olsen J. Sex ratio and twinning in women with hyperemesis or pre-eclampsia. Epidemiology 2001;12:7479.
14 Chin RK, Lao TT. Low birth weight and hyperemesis gravidarum. Eur
J Obstet Gynecol Reprod Biol 1988;28:17983.
15 Czeizel AE, Sarkozi A, Wyszynski DF. Protective effect of hyperemesis gravidarum for nonsyndromic oral clefts. Obstet Gynecol
2003;101:73744.
16 del Mar Melero-Montes M, Jick H. Hyperemesis gravidarum and the
sex of the offspring. Epidemiology 2001;12:1234.
17 Depue RH, Bernstein L, Ross RK. Hyperemesis gravidarum in relation
to estradiol levels, pregnancy outcome, and other maternal factors:
a seroepidemiologic study. Am J of Obstet Gynecol 1987;156:1137
41.
18 Dodds L, Fell DB, Joseph KS, Allen VM, Butler B. Outcomes of pregnancies complicated by hyperemesis gravidarum. Obstet Gynecol
2006;107:28592.
19 Hallak M, Tsalamandris K, Dombrowski MP, Isada NB, Pryde PG,
Evans MI. Hyperemesis gravidarum. Effects on fetal outcome. J Reprod Med 1996;41:8714.
20 Henderson BE, Benton B, Jing J, Yu MC, Pike MC. Risk factors for
cancer of the testis in young men. Int J Cancer 1979;23:598602.
21 Hsu CD, Witter FR. Fetal sex and severe hyperemesis gravidarum. Int
J Gynaecol Obstet 1993;40:634.
22 Kallen B. Hyperemesis during pregnancy and delivery outcome: a
registry study. Eur J Obstet Gynecol Reprod Biol 1987;26:291302.
23 Kaul PP, Srivastava R, Srivastava SP, Kamboj M, Chand S. Relationships of maternal blood lead and disorders of pregnancy to neonatal
birthweight. Vet Hum Toxicol 2002;44:3213.
24 Paauw JD, Bierling S, Cook CR, Davis AT. Hyperemesis gravidarum
and fetal outcome. JPEN J Parenter Enteral Nutr 2005;29:936.
25 Roberts CJ. Developmental and neurological sequelae of the common complications of pregnancy and birth. Br J Prev Soc Med
1970;24:338.
26 Schiff MA, Reed SD, Daling JR. The sex ratio of pregnancies complicated by hospitalisation for hyperemesis gravidarum. BJOG
2004;111:2730.
27 Sorensen HT, Thulstrup AM, Mortensen JT, Larsen H, Pedersen L,
James WH. Hyperemesis gravidarum and sex of child. Lancet
2000;355:407.
28 Tan PC, Jacob R, Quek KF, Omar SZ. The fetal sex ratio and metabolic, biochemical, haematological and clinical indicators of severity
of hyperemesis gravidarum. BJOG 2006;113:7337.
29 Tsang IS, Katz VL, Wells SD. Maternal and fetal outcomes in hyperemesis gravidarum. Int J Gynaecol Obstet 1996;55:2315.
30 Vilming B, Nesheim B-I. Hyperemesis gravidarum in a contemporary
population in Oslo. Acta Obstet Gynecol Scand 2000;79:6403.
31 Zhang J, Cai WW. Severe vomiting during pregnancy: antenatal correlates and fetal outcomes. Epidemiology 1991;2:4547.
32 Roseboom TJ, Ravelli AC, van der Post JA, Painter RC. Maternal
characteristics largely explain poor pregnancy outcome after hyperemesis gravidarum. Eur J Obstet Gynecol Reprod Biol 2011;156:569.
33 Kauppila A, Jouppila P, Koivisto M, Moilanen I, Ylikorkala O. Twin
pregnancy. A clinical study of 335 cases. Acta Obstet Gynecol Scand
Suppl 1975;44:512.
34 Saxena BB, Landesman R. Diagnosis and management of pregnancy
by the radioreceptorassay of human chorionic gonadotropin. Am J
Obstet Gynecol 1978;131:97107.
35 Landesman R, Coutinho EM, Saxena BB. Detection of human chorionic gonadotropin in blood of regularly bleeding women using copper intrauterine contraceptive devices. Fertil Steril 1976;27:10626.
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
Consequences of hyperemesis gravidarum for offspring
36 Danzer H, Braustein GD, Rasor J, Forsythe A, Wade ME. Maternal
serum human chorionic gonadotropin concentrations and fetal sex
prediction. Fertil Steril 1980;34:33640.
37 Ehrenberg HM, Dierker L, Milluzzi C, Mercer BM. Low maternal
weight, failure to thrive in pregnancy, and adverse pregnancy outcomes. Am J Obstet Gynecol 2003;189:172630.
38 DeVader SR, Neeley HL, Myles TD, Leet TL. Evaluation of gestational
weight gain guidelines for women with normal prepregnancy body
mass index. Obstet Gynecol 2007;110:74551.
39 Bernstein L, Depue RH, Ross RK, Judd HL, Pike MC, Henderson BE.
Higher maternal levels of free estradiol in first compared to second
pregnancy: early gestational differences. J Natl Cancer Inst
1986;76:10359.
40 Huxley R, Shiell A, Law C. The role of size at birth and postnatal
catch-up growth in determining systolic blood pressure: a systematic
review of the literature. J Hypertens 2000;18:81531.
41 Whincup PH, Kaye SJ, Owen CG, Huxley R, Cook DG, Anazawa S,
et al. Birth weight and risk of type 2 diabetes: a systematic review.
JAMA 2008;300:288697.
42 Painter RC, Roseboom TJ, Bleker OP. Prenatal exposure to the Dutch
famine and disease in later life: an overview. Reprod Toxicol
2005;20:34552.
43 Verberg MF, Gillott DJ, Al-Fardan N, Grudzinskas JG. Hyperemesis
gravidarum, a literature review. Hum Reprod Update 2005;11:527
39.
2011 The Authors BJOG An International Journal of Obstetrics and Gynaecology 2011 RCOG
1313
Vous aimerez peut-être aussi
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (890)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (587)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (119)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2219)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- KAPS Exam Guide and Sample Papers - Australian Pharmacy Council PDFDocument10 pagesKAPS Exam Guide and Sample Papers - Australian Pharmacy Council PDFShoaib BiradarPas encore d'évaluation
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- SDMS - Code of EthicsDocument2 pagesSDMS - Code of Ethicsdgina8800Pas encore d'évaluation
- 1 s2.0 S0002937814003366 MainDocument8 pages1 s2.0 S0002937814003366 Mainronny29Pas encore d'évaluation
- Gelatin Sponge Plug To Seal Fetoscopy Port Sites: Technique in Ovine and Primate ModelsDocument2 pagesGelatin Sponge Plug To Seal Fetoscopy Port Sites: Technique in Ovine and Primate Modelsronny29Pas encore d'évaluation
- Azmil RahmanDocument4 pagesAzmil Rahmanronny29Pas encore d'évaluation
- Chorioamnionitis and Prognosis For Term Infants-13Document5 pagesChorioamnionitis and Prognosis For Term Infants-13ronny29Pas encore d'évaluation
- 1 s2.0 S0002937800250552 MainDocument6 pages1 s2.0 S0002937800250552 Mainronny29Pas encore d'évaluation
- Jurnal Feto NZFDocument3 pagesJurnal Feto NZFronny29Pas encore d'évaluation
- Jurnal HegDocument7 pagesJurnal HegAmanda Mahendra SastranegaraPas encore d'évaluation
- 1.4 Sarcoma Botryoids of The Vagina. S. Cywes and J.H. LouwDocument7 pages1.4 Sarcoma Botryoids of The Vagina. S. Cywes and J.H. Louwronny29Pas encore d'évaluation
- Hyperemesis Gravidarum Associated with Placental Weight Ratio (39Document14 pagesHyperemesis Gravidarum Associated with Placental Weight Ratio (39ronny29Pas encore d'évaluation
- 1 s2.0 S0002937801474217 MainDocument6 pages1 s2.0 S0002937801474217 Mainronny29Pas encore d'évaluation
- 1 s2.0 S0002937800250552 MainDocument6 pages1 s2.0 S0002937800250552 Mainronny29Pas encore d'évaluation
- 1 s2.0 S0002937813013859 MainDocument1 page1 s2.0 S0002937813013859 Mainronny29Pas encore d'évaluation
- NICHD Consecutive StudiesDocument8 pagesNICHD Consecutive Studiesronny29Pas encore d'évaluation
- Dual CatheterDocument6 pagesDual Catheterronny29Pas encore d'évaluation
- Dual CatheterDocument6 pagesDual Catheterronny29Pas encore d'évaluation
- Relationship between vitamin D deficiency, inflammation and preeclampsiaDocument7 pagesRelationship between vitamin D deficiency, inflammation and preeclampsiaronny29Pas encore d'évaluation
- Pamela Grace B. Demaisip: Employment RecordDocument4 pagesPamela Grace B. Demaisip: Employment RecordPearl Demaisip-NinonuevoPas encore d'évaluation
- Unit 5 Bioethics BSNDocument25 pagesUnit 5 Bioethics BSNTamara Kate HalicanPas encore d'évaluation
- Useful Vocabs For OET Writing & Speaking PDFDocument2 pagesUseful Vocabs For OET Writing & Speaking PDFLiju K OommenPas encore d'évaluation
- Literature Review Final DraftDocument21 pagesLiterature Review Final DraftJared AugensteinPas encore d'évaluation
- Apremilast PI Europe Aug 2019Document14 pagesApremilast PI Europe Aug 2019Wei Sheng ChongPas encore d'évaluation
- Second and Third Trimester Screening For Fetal AnomalyDocument12 pagesSecond and Third Trimester Screening For Fetal AnomalyIqra NazPas encore d'évaluation
- Romano Lingual OrthodonticsDocument202 pagesRomano Lingual OrthodonticsAnonymous c6dYwQsrzT75% (4)
- The Federal Emergency Agency (FEMA)Document3 pagesThe Federal Emergency Agency (FEMA)oguturonniePas encore d'évaluation
- Qai 86 200Document8 pagesQai 86 200RishabhPas encore d'évaluation
- Differentiate Between The Four Basic Types of DepartmentalizationDocument3 pagesDifferentiate Between The Four Basic Types of DepartmentalizationVikram Kumar100% (1)
- Grafik Absensi KaryawanDocument3 pagesGrafik Absensi KaryawansolichunPas encore d'évaluation
- Assess Appropriateness For Clinical Condition. Heart Rate Typically 50/min If BradyarrhythmiaDocument1 pageAssess Appropriateness For Clinical Condition. Heart Rate Typically 50/min If BradyarrhythmiaatikaPas encore d'évaluation
- Addressing The Leadership Gap in HealthcareDocument21 pagesAddressing The Leadership Gap in Healthcareinfoninja0Pas encore d'évaluation
- Obesity Obesity Management in AdultsDocument12 pagesObesity Obesity Management in AdultsLorena IbarrolaPas encore d'évaluation
- State School Immunization Requirements and Vaccine Exemption LawsDocument18 pagesState School Immunization Requirements and Vaccine Exemption LawsBen CulpepperPas encore d'évaluation
- Original PDF Pharmacology For Pharmacy Technicians 2nd Edition PDFDocument41 pagesOriginal PDF Pharmacology For Pharmacy Technicians 2nd Edition PDFnoe.simons469100% (32)
- SEBC Merit List PDFDocument184 pagesSEBC Merit List PDFNeel GajjarPas encore d'évaluation
- Study Abroad in Your Favorite Country - SantamonicaDocument11 pagesStudy Abroad in Your Favorite Country - SantamonicaSantamonica Study AbroadPas encore d'évaluation
- The Gazette March 2009Document7 pagesThe Gazette March 2009St George's Healthcare NHS TrustPas encore d'évaluation
- Efic Core NursingDocument52 pagesEfic Core NursingAgron BytyqiPas encore d'évaluation
- Safina Usman T-PDocument23 pagesSafina Usman T-PUsman Ahmad TijjaniPas encore d'évaluation
- Chlorhexidine The Gold Standard in Chemical PlaqueDocument6 pagesChlorhexidine The Gold Standard in Chemical PlaquePhuong ThaoPas encore d'évaluation
- Medical Case Report, HarisDocument13 pagesMedical Case Report, HarisHarlan Putra WPas encore d'évaluation
- Iv Therapy: ProceduresDocument2 pagesIv Therapy: ProceduresMakagago And BruskoPas encore d'évaluation
- Housekeeping ManualDocument22 pagesHousekeeping ManualWe Care Facility Management ServicesPas encore d'évaluation
- BME Közép Szóbeli TémákDocument6 pagesBME Közép Szóbeli TémákKrisztina Kurucz100% (1)
- Thesis Topics For MD PharmacologyDocument6 pagesThesis Topics For MD Pharmacologykatyallenrochester100% (1)
- Physiological and Psychosocial Alterations: Nursing Practice 3A: Nursing Care of Client WithDocument9 pagesPhysiological and Psychosocial Alterations: Nursing Practice 3A: Nursing Care of Client WithSepjho M. Nojepse0% (1)