Académique Documents
Professionnel Documents
Culture Documents
Epiderm Bulosa
Transféré par
Anonymous hTivgzixVNTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Epiderm Bulosa
Transféré par
Anonymous hTivgzixVNDroits d'auteur :
Formats disponibles
Tampoia et al.
Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
RESEARCH
Open Access
Prevalence of specific anti-skin autoantibodies
in a cohort of patients with inherited
epidermolysis bullosa
Marilina Tampoia1*, Domenico Bonamonte2, Angela Filoni2, Lucrezia Garofalo2, Maria Grazia Morgese3,
Luigia Brunetti4, Chiara Di Giorgio5 and Giuseppina Annicchiarico6
Abstract
Background: Inherited epidermolysis bullosa (EB) is a group of skin diseases characterized by blistering of the skin
and mucous membranes.
There are four major types of EB (EB simplex, junctional EB, dystrophic EB and Kindler syndrome) caused by
different gene mutations. Dystrophic EB is derived from mutations in the type VII collagen gene (COL7A1),
encoding a protein which is the predominant component of the anchoring fibrils at the dermal-epidermal junction.
For the first time in literature, we have evaluated the presence of anti-skin autoantibodies in a wider cohort of
patients suffering from inherited EB and ascertained whether they may be a marker of disease activity.
Methods: Sera from patients with inherited EB, 17 with recessive dystrophic EB (RDEB), 10 with EB simplex (EBS)
were analysed. As much as 20 patients with pemphigus vulgaris, 21 patients with bullous pemphigoid and 20
healthy subjects were used as controls.
Anti-skin autoantibodies were tested in all samples with the Indirect Immunofluorescence (IIF) method and the
currently available ELISA method in order to detect anti-type VII collagen, anti-BP180 and anti-BP230 autoantibodies.
Results: The mean concentrations of anti-type VII collagen autoantibodies titres, anti-BP180 and anti-BP230
autoantibodies were statistically higher in RDEB patients than in EBS patients.
The sensitivity and specificity of the anti-type VII collagen ELISA test were 88.2% and 96.7%. The Birmingham
Epidermolysis Bullosa Severity score, which is used to evaluate the severity of the disease, correlated with anti-skin
autoantibodies titres.
Conclusions: The precise pathogenic role of circulating anti-skin autoantibodies in RDEB is unclear. There is a
higher prevalence of both anti-type VII collagen and other autoantibodies in patients with RDEB, but their presence
can be interpreted as an epiphenomenon.
Keywords: Inherited epidermolysis bullosa, Dystrophic epidermolysis bullosa, Anti-skin autoantibodies, Type VII
collagen, BP180, BP230, ELISA, Birmingham Epidermolysis Bullosa Severity score
* Correspondence: mtampoia@libero.it
1
Laboratory of Clinical Pathology, University Hospital of Bari, Piazza Giulio
Cesare 11, Bari 70124, Italy
Full list of author information is available at the end of the article
2013 Tampoia et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative
Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use, distribution, and
reproduction in any medium, provided the original work is properly cited.
Tampoia et al. Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
Background
Epidermolysis bullosa (EB) is a group of both acquired
and inherited diseases characterized by blistering of the
skin and mucous membranes, in response to little or no
apparent trauma [1].
In inherited EB, the phenotypic manifestations of this
disease can be very different; in the milder forms, there
is a lifelong blistering tendency with no impact on the
overall longevity of the affected subject, while in the
most severe forms children die during the early postnatal period from metabolic perturbations, dehydration,
and sepsis [2].
Inherited EB has typically been classified into four
main subtypes; these differ not only phenotypically and
genotypically but, more importantly, by the site of ultrastructural distruption or cleavage. Tissue separation occurs within the intraepidermal keratinocyte cytoplasm in
EB simplex (EBS), through the lamina lucida in junctional EB (JEB) or in the sublamina densa in dystrophic
EB (DEB) [3]; in Kindler syndrome, multiple cleavage
planes may be seen within the same sample of skin [4].
Inherited EB is now known to result from more than
1100 mutations, encompassing more than 14 distinct
structural genes expressed within the cutaneous basement membrane zone (BMZ) at the dermoepidermal
junction [5,6]. After the initial clinical evaluation, based
on careful examination of cutaneous and extracutaneous
manifestations and inheritance pattern, the diagnosis is
confirmed by the use of three main techniques: immunofluorescence mapping (IFM), transmission electron
microscopy (TEM), which can both be used to identify
the level of skin cleavage, and mutation analysis [7]. TEM
is considered the gold standard laboratory test for differentiation between the various forms of EB. The primary
advantage is that it can visualize ultra-structural abnormalities and may be particularly useful in patients with
mild DEB or EBS. However, TEM is time-consuming and
expensive, and the results are, to a high degree, operatordependent and sometimes inaccurate [8]. The diagnostic
precision of IFM is similar to that of TEM, with the advantage that it is simpler and faster both to perform and
to interpret. A previous study has shown that IFM is more
sensitive (97% vs. 71%) and specific (100% vs. 81%) than
TEM [9].
Mutation analysis is an excellent technique to confirm
the diagnosis for the various subtypes of EB as well as to
provide information that might be useful for prenatal
diagnosis and someday for genetic therapy [10].
Dystrophic EB and type VII collagen
Dystrophic EB (DEB) forms, also known as dermolytic
forms, are characterized by tense blisters and erosions
that heal with extensive, either atrophic or hypertrophic,
scarring. The scarring tendency reflects the fact that
Page 2 of 10
blister formation occurs below the level of the lamina
densa of the BMZ of the papillary derma. The spectrum of
clinical severity in DEB is, however, highly variable, with
milder forms of the disease showing a limited tendency to
blistering or nail involvement and severe forms where the
gastrointestinal tract, particularly the oesophagus, is affected by blistering and scarring. All forms result from
mutations within type VII collagen gene, COL7A1 [10].
The type VII collagen, the main constituent of the
anchoring fibrils, is composed of a triple-helical domain
flanked by a large 145 kDa non-collagenous aminoterminal (NC-1) domain and a small 34 kDa noncollagenous carboxyl-terminal (NC-2) domain [11,12]. In
patients with DEB, ultrastructural analysis of skin demonstrates the presence of altered anchoring fibrils, reduced in number or completely absent in the different
forms [13].
Autoantibodies against type VII collagen
In addition to inherited forms of EB, there is an acquired
form of epidermolysis bullosa (EBA), which is caused by
an auto-reactive response against collagen VII. Patients
with EBA have both tissue-bound and circulating IgG
autoantibodies against type VII collagen [14,15]. Specifically, circulating autoantibodies recognize epitopes
within the amino-terminal NC-1 domain of type VII collagen [16,17]; only a small number of EBA patients have
been described with autoantibodies reactivity against the
NC-2 domain [18]. The routine screening tests for the
diagnosis of EBA are: direct and indirect immunofluorescence microscopy; in particular, the salt-split skin method.
Patients with EBA have immune deposits on the dermal
side of salt-split skin, whereas in bullous pemphigoid (BP)
deposits are on the epidermal side. However, this method
does not distinguish EBA from anti-laminin 332 mucous
membrane pemphigoid (MMP) or anti-laminin c1 pemphigoid as these diseases also show immune deposition on
the dermal side of salt-split skin. EBA sera recognize the
290 kDa type VII collagen protein in immunoblotting
studies; in fact, this reactivity confirms the diagnosis of
EBA. However, immunoblotting studies are difficult to
carry out because they are time-consuming and technically demanding. Advances in the identification of target
antigens and the subsequent development of an increasing
number of sensitive and specific assays for the detection
of circulating autoantibodies, including recombinant
forms of the target antigens and ELISA, allow serological
diagnosis in patients with autoimmune skin disorders.
Several ELISA systems using recombinant fragments of
BP180, BP230, desmoglein1, desmoglein3, have become
commercially available and are highly valuable diagnostic
tools [19]. ELISAs were also developed to detect autoantibodies in EBA using different recombinant proteins of
the NC-1 domain of type VII collagen [20,21]. Previous
Tampoia et al. Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
reports demonstrate that these tests showed high sensitivity and specificity, and in some clinical studies serial titres
of anti-type collagen VII from each patient with EBA
reflected the disease activity [22-24]. Experimental studies
provided evidence that autoantibodies against type VII
collagen are pathogenic. When rabbit and human antibodies were passively transferred into mice, they induced
subepidermal blister formation and nail dystrophy [25,26].
The active mouse model of EBA was also established by
immunizing mice with the recombinant NC-1 domain of
murine type VII collagen [27].
Although DEB has been shown to result from mutations in COL7A1, relatively little is known about the
mechanistic consequences of the mutations in relation
to blistering. To facilitate our understanding of DEB, we
have evaluated the presence of anti-skin autoantibodies
in a wider cohort of patients suffering from DEB and
ascertained whether they correlated with the disease
severity.
Methods
Patients
Serum samples were obtained from 27 patients with
inherited forms of EB, seen at the Dermatological
Department of the University Hospital in Bari between
January 2010 and December 2012. All patients examined had typical clinical features of EB with a variable
phenotype as well as immunofluorescence mapping and
transmission electron microscopy findings consistent
with EB.
As many as 17 patients had recessive dystrophic EB
(RDEB), mean age 21.2 years, range 2-50, 4 male and 13
female; 10 patients had EB simplex (EBS), mean age
17 years, range 1-56, 3 male and 7 female. In all patients,
disease severity was evaluated through the Birmingham
Epidermolysis Bullosa Severity score (BEBS), which includes 11 items: area of damaged skin, involvement of
nails, mouth, eyes, larynx and oesophagus, scarring of
hands, skin cancer, chronic wounds, alopecia and nutritional compromise. Area was allocated 50 points, and
the 10 other items 5 points each, giving a maximum
score of 100 [28]. The BEBS score was performed by a
dermatology specialist at blood sample collection.
Diseases control sera were obtained from 41 patients,
including 20 patients with pemphigus vulgaris (PV) (mean
age 59 years, range 37-85, 6 males, 14 females) and from
21 patients with bullous pemphigoid (BP) (mean age
74 years, range 61-90, 9 males, 12 females).
Control sera were obtained from 20 healthy subjects
(mean age 47 years, range 36-65, 6 males and 14 females).
All sera were stored at -20C until assayed.
Patients and control subjects gave written consent to
participate in this study, and the Ethics Committee of
the hospital approved this study.
Page 3 of 10
Methods
The detection of circulating anti-skin autoantibodies was
performed in all samples with an Indirect Immunofluorescence (IIF) method (Euroimmun, Lubeck, Germany) and
with the currently commercially available ELISA methods
(MBL, Nagoya, Japan). Anti-type VII collagen ELISA kits
were provided free of charge by the manufacturer. All
assays were performed at the Laboratory of Clinical
Pathology in the University Hospital of Bari.
IIF method
Slides were made of frozen primate oesophagus section.
IIF assays were performed at a serum dilution of 1:10 in
phosphate buffered saline (pH 7.3).
Two different fluorescence patterns can be observed
on primate esophagus sections: a) anti-intercellular substance (ICS) and anti-basal membrane zone (BMZ). ICS
antibodies, which are specific for pemphigus, are directed against prickle cell desmosomes and react with
surface antigens of keratinocytes; on tissue sections
they display a granular fluorescence of the intercellular matter in the whole stratum spinosum. BMZ autoantibodies, which are specific for pemphigoid diseases
or epidermolysis bullosa acquisita, are directed against
epidermal basal membrane and generate a fine linear
colouring between the stratum basale and the connective
tissue.
Samples were scored positive if a fluorescence reaction
was observed at 1:10 sample dilution.
ELISA methods
Autoantibodies detection was performed in all samples
with the ELISA systems, each one employing different
antigenic proteins coated on the wells of microplates.
Assays were run according to the manufacturers
instructions.
Patients and control sera, diluted 1:100, were added to
each well of a microwell plate. For detection of anti-type
VII collagen autoantibodies the microplates were coated
with human recombinant NC-1 and NC-2 proteins;
for detection of anti-BP180 and anti-BP230 autoantibodies, the microplates were coated with recombinant
purified BP180-NC16A antigen and recombinant purified
BP230-N and BP230-C antigens, respectively. Sera were
incubated for 1 hour at RT. After washing to remove
any unbound serum proteins, horseradish peroxidiseconjugated anti-human IgG was added and incubated
for 1 hour at RT. After another washing step, the peroxidise
substrate was added and incubated for 30 min at RT.
The acid solution was then added to each well to terminate the enzyme reaction and stabilize the colour
development. The value in each sample was obtained
by comparing the optical density (OD) of the sample
with the OD of the calibrator.
Tampoia et al. Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
Statistical analysis
To assess the relationship between clinical features and
autoantibodies titres, we divided inherited EB patients into
EB simplex (EBS) patients and EB recessive dystrophic
(RDEB) patients.
The Kruskal Wallis test was used to compare the titres
of each autoantibody assayed by the ELISA methods in
patients and in the control group.
A P-value below 0.05 was considered statistically significant. The Unpaired T test was used to compare the
mean autoantibodies titres between EBS patients and
RDEB patients.
The diagnostic sensitivity of ELISA for anti-type VII
collagen autoantibodies was calculated in 17 patients
with RDEB, and the specificity was calculated in 10
patients with EBS, in 41 control patients with other
diseases and in 20 healthy subjects. The cut-off value
for positivity was validated and optimised by Receiver
Operating Characteristics (ROC).
Correlation analyses were performed by using the
Pearson test.
MedCalc software (Mariakerke, Belgium) was used for
statistical and ROC curve analysis.
Results
Analytical measurements
In patients with EB, the IIF method did not show an
anti-basal membrane zone (BMZ) pattern, as expected.
In the present study, all samples were tested at 1:10, in
accordance to the recommendations for qualitative IIF
given by the manufacturer. However, as the use of only a
single dilution may lead to blocking or masking effects
in high-titered sera, thus causing false-negative results, sera
were retested at 1:100 dilution. At this dilution, no prozone
effects were noted, confirming that those sera were true
negatives. Detection of antibodies by ELISA test allowed
quantitative measurements of autoantibodies serum titres.
Figure 1 shows that the mean concentration of anti-type
VII collagen autoantibodies titres was statistically higher in
patients with RDEB than in patients with EBS, in controls
with other diseases and in healthy subjects (test Kruskal
Wallis, P < 0.0001). Clinical and serological findings of patients with two different inherited types of EB are reported
in Table 1.
The mean concentrations of anti-type VII collagen autoantibodies titres were statistically higher in patients with
RDEB than in patients with EBS (P =0.0014). The mean
concentrations of anti-BP180 and anti-BP230 autoantibodies were also statistically higher in patients with RDEB
than in patients with EBS (P = 0.0028 and P = 0.0023,
respectively).
The area under the curve (AUC) for anti-type VII
collagen ELISA test was 0.931(CI, 0.850-0.976) and ROC
analysis showed that anti-type VII collagen autoantibodies
Page 4 of 10
had a sensitivity of 88.2% (CI, 63.5 -98.2) and a specificity of 96.7% (CI, 88.6-99.5), using a cut-off value of
5 UA/mL (Figure 2). The prevalence of anti-type VII
collagen autoantibodies was 88% in patients with
RDEB and 10% in patients with EBS. The combined
prevalence of anti-BP180 and anti-BP230 autoantibodies
was 88% in patients with RDEB and 50% in patients
with EBS.
Thus, in RDEB forms there was a higher prevalence
of both anti-type VII collagen autoantibodies and
autoantibodies against BMZ antigens, in particular
BP180 and BP230 (chi-square, P < 0.0001; OR 79.95%
IC 4.01-1575).
Analytical and clinical correlations
ELISA results for each autoantibody and BEBS score for
each patient are reported in Table 2.
In all patients with RDEB, anti-type VII collagen
autoantibodies titres significantly correlated with both
anti-BP180 (slope < 0.0009, R2 0.53) (Figure 3A) and
anti-BP230 (slope < 0.0001, R2 0.83) autoantibodies titres
(Figure 3B).
Birmingham Epidermolysis Bullosa Severity score (BEBS)
correlated with anti-type VII collagen autoantibodies
titres (P = 0.0190) (Figure 4A) and also with anti-BP180
and anti-BP230, P = 0.0119 and P = 0.0097, respectively
(Figure 4B and 4C).
Discussion
Over the last years, the great worldwide interest in inherited EB has led to the publication of studies concerning
EB clinical features and its genetic correlation, which are
important for the disease classification and the prediction
of organ involvement. However, no studies about serological features of patients with different subtypes of
inherited EB are available. Recently, recombinant proteins
have been used as antigenic targets in ELISA methods for
detection of anti-skin autoantibodies. These methods have
also confirmed that the sensitivity and the specificity are
analogous to those of the method of reference.
In our study, we analysed for the first time in the literature the presence of circulating anti-skin autoantibodies in patients suffering from RDEB and EBS. In other
autoimmune blistering skin diseases (as pemphigus and
pemphigoid), it has been shown that anti-skin specific
autoantibodies can take part in the formation process of
the bullous lesion [19]. Regarding EBA, the cross-reacting
autoantibodies are responsible for the incorrect assembly
of type VII collagen into anchoring fibrils, thus altering
both the natural maintenance and turnover of fibrils or
interfering with the ability of the anchoring fibrils to attach to the basement membrane at dermal level [29].
The pathogenic role of these autoantibodies has been
demonstrated in experimental models [30].
Tampoia et al. Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
RDEB
Page 5 of 10
EBS
PV
BP
HS
Figure 1 Distribution of anti-type VII collagen autoantibodies titres. Distribution of anti-type VII collagen autoantibodies titres, expressed in
Units/mL in patients with recessive dystrophic epidermolysis bullosa (RDEB), epidermolysis bullosa simplex (EBS), pemphigus vulgaris (PV), bullous
pemphigoid (BP) and healthy subjects (HS). Kruskal Wallis test, P < 0.0001.
As for DEB, relatively little is known about the mechanistic consequences of the mutations in relation to blistering, which has led us to look for autoantibodies directed
against cutaneous structures also in these patients. Some
very interesting data have emerged from our study about
the prevalence of anti-skin positivity in patients with
RDEB.
The relationship between a monogenic disease and
autoimmunity is difficult to clarify; we tried to explain it
through different hypothesis.
In RDEB patients, a possible explanation for the development of autoantibodies recognizing type VII collagen epitopes could be based on an altered immunologic
recognition of "self" consequence of altered proteins synthesis due to genetic mutation.
We know that autoimmune diseases are characterized
by aberrant immune responses against healthy cells and
tissues, in which a given individual's genetic susceptibility may play a central role. However, the exact mechanisms underlying the development of these conditions
remain for the most part unknown. In recent years, growing evidence has demonstrated that, in addition to
100
80
Patients
with RDEB
Patients
with EBS
Patients, no.
17
10
Mean Age
21
17
Range years
2-50
1-56
Males/Females
4/13
3/7
Birmingham severity score, mean
55
5.4
Birmingham severity score, range
5-90
2-36
Sensitivity
Table 1 Clinical and serological findings in patients with
recessive dystrophic epidermolysis bullosa (RDEB) and
with epidermolysis bullosa simplex (EBS)
60
40
20
Birmingham severity score
Autoantibodies titres, mean concentrations
0
0
P*
-Anti-type VII collagen (U/mL)
27.8
2.5
0.0014
-Anti-BP180 (U/mL)
59.4
8.3
0.0028
-Anti-BP230 (U/mL)
51.2
6.6
0.0023
* Unpaired T Test, P-value < 0.05 was considered statistically significant.
20
40
60
80
100
100-Specificity
Figure 2 ROC analysis of anti-type VII collagen IgG. Receiveroperating-characteristic (ROC) plot analysis of anti-type VII collagen
IgG autoantibodies. AUC, area under the curve, was 0.931. The
continuous line refers to the ELISA method used.
Tampoia et al. Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
Page 6 of 10
Table 2 ELISA data for each autoantibody and BEBS score for each patient with recessive dystrophic epidermolysis
bullosa (RDEB) and with epidermolysis bullosa simplex (EBS)
Autoantibodies anti-skin
n. pt
Sex
Age years
tipe EB
Anti-BP180
Anti-BP230
Anti-coll VII
BEBS score
20
RDEB
68,8
45,2
27,9
65
12
RDEB
36
26,7
20,1
67
RDEB
23,5
20,3
8,5
56
EBS
14,7
13,8
2,1
19
RDEB
37,5
37,8
14,9
63
45
RDEB
6,8
3,3
1,1
39
34
RDEB
93
53,4
24,5
79
34
EBS
2,9
3,2
1,3
10
EBS
3,5
3,5
1,2
10
27
RDEB
1,4
110
53,5
89
11
15
RDEB
77,8
69,8
44,4
60
12
29
RDEB
151,8
144,5
48,6
82
13
29
RDEB
34,5
18,2
5,9
53
14
RDEB
16,8
13,9
5,8
55
15
RDEB
76,7
57,9
29,9
53
16
EBS
13,4
3,5
1,4
17
EBS
10,1
6,3
1,9
18
33
RDEB
107,6
65,9
45,3
90
19
19
EBS
2,7
4,1
1,2
20
56
EBS
15,1
13,1
10,8
36
21
50
RDEB
2,8
3,3
1,2
11
22
16
RDEB
161
120,7
76,7
71
23
10
RDEB
58,2
52,8
36,6
52
24
17
EBS
4,5
8,9
2,1
25
13
EBS
15,1
8,4
2,2
26
RDEB
56
27,1
12,4
34
27
EBS
1,2
1,4
Figure 3 Correlation between anti-type VII collagen autoantibodies titres and the other two anti-skin autoantibodies. (A) Correlation
between anti-type VII collagen autoantibodies titres and anti-BP180 autoantibodies. Pearson test, P < 0.0009, R2 0.53. (B) Correlation between antitype VII collagen autoantibodies titres and anti-BP230 autoantibodies. Pearson test, P < 0.0001, R2 0.83.
Tampoia et al. Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
Anti-type VII collagen autoantibodies
titres (U/mL)
Page 7 of 10
90
80
70
P=0.0190
60
50
40
30
20
10
0
10
20
30
50
60
70
80
90
100
BEBS score
B
Anti-type BP 180 autoantibodies titres
(U/mL)
40
180
160
P=0.0119
140
120
100
80
60
40
20
0
0
Anti-type BP 230 autoantibodies titres
(U/mL)
10
20
30
40
50
60
70
80
90
100
BEBS score
160
140
120
P=0.0097
100
80
60
40
20
0
0
10
20
30
40
50
60
70
80
90
100
BEBS score
Figure 4 Correlation between anti-skin autoantibodies and Birmingham Epidermolysis Bullosa Severity score. (A) Correlation between
anti-type VII collagen autoantibodies titres and BEBS score. (B) Correlation between anti- anti-BP180 autoantibodies titres and BEBS score.
(C) Correlation between anti-BP230 autoantibodies titres and BEBS score. Red points indicate EBS patients; black points indicate RDEB patients.
Tampoia et al. Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
genetics, other complementary mechanisms are involved
in the pathogenesis of autoimmunity; in particular, epigenetics. Epigenetics is defined as stable and heritable patterns of gene expression that do not entail any alterations
to the original DNA sequence. Epigenetic mechanisms
primarily consist of DNA methylation, histone modifications and small non-coding RNA transcripts [31].
Another hypothesis for this autoimmune condition
may relate to the "molecular mimicry", based on the assumption that a foreign antigen holds similar sequence
or structure with self-antigens. Molecular mimicry has
typically been characterized at antibody or T cell level.
Moreover, the exposure to antigen protein derived from
bacterial and viral infection can induce this phenomenon
with the activation of T and B cells [32]. RDEB patients,
as a consequence of chronic wound formation, are often
exposed to bacterial infection; therefore, molecular mimicry is likely to occur. However, it is possible that the
initial insult to the anchoring fibrils, mediated by an antibody recognizing a single epitope, could lead to the exposure of additional epitopes and subsequent development of
polyvalent antisera.
However, it has recently been shown that the reactivity
versus the NC-1 and NC-2 domains of type VII collagen
protein is more predictive of an inflammatory rather
than an autoimmune disease. This hypothesis is supported by the presence of anti-type VII collagen autoantibodies in inflammatory diseases involving the
intestine, where the presence of this protein has been
demonstrated but not featured by skin blistering such as
Crohns disease and inflammatory bowel disease. However, the correlation between the presence of those antibodies and their pathogenic significance in that illness
remains elusive [33,34]. It has recently been reported
that the major determinant of autoantibody pathogenicity relies on the different IgG subclass, and within the
anti-type VII collagen autoantibodies the IgG4 sub-class
was the most represented. IgG4 may induce inflammation and tissue damage by activating leukocytes with a
non-complement fixing pattern or just binding collagen
VII in a Fc-independent fashion leading to dermalepidermal separation [35]. Although in our study we
have not identified the subclass of IgG-autoantibodies,
we observed very high levels of IgG4 among patients
with RDEB; this observation might explain the dissimilar
clinical evolution not only relative to skin manifestation,
but also in relation to extracutaneous complication, such
as organ damage.
In this study, we have also found autoantibodies against
NC-16A domain of BP180 and C- and N-terminal domains of BP230. Another current model of chronic autoimmune skin diseases predicts that dominant self
epitopes induce the inflammatory cascade and tissue damage in the target organ. Recruitment and activation of
Page 8 of 10
autoreactive T lymphocytes specific for secondary epitopes of the nominal autoantigen or non distinct selfproteins subsequently contribute to the disease course.
This phenomenon is called epitope spreading (ES). There
is growing evidence that inter- and intramolecular ES
events are not simply an epiphenomenon but are critical
in the evolution and progression of diseases [36]. Our data
confirm this hypothesis and demonstrate that anti-type
VII collagen autoantibodies strictly correlate with BP180
and BP230 autoantibodies.
Our study could be limited by the lack of Direct
Immunofluorescence (DIF) data on skin biopsies for
detection of tissue-bound autoantibodies. We believe that
this detection, which is very important to define the role
of these autoantibodies, should be carried out by more
specific epitope-related methods rather than by fluorescence pattern observed with DIF.
Our opinion is that the most significant finding can
be seen in the correlation between antibodies titres and
the skin disease activity score. However, we also think
that this finding should be confirmed on a wider number of DEB patients, considering the natural history of
the disease. These correlations can also be assessed by
means of other clinical scores [37-39]. On the other
hand, the determination of anti-skin autoantibodies by
means of the ELISA method has many advantages: it
can be easily introduced in the clinical routine, it is
little traumatic for the patient, therefore repeatable,
and quantitative.
Conclusions
In this study, we have reported the presence of skin autoantibodies in EB patients. In particular, we revealed a high
prevalence of autoantibodies in RDEB patients. Unless the
pathogenic role of antiskin autoantibodies in patients with
DEB is demonstrated by ex vivo and experimental animals
using antibody passive transfer model, their presence can
be simply interpreted as an epiphenomenon.
Experimental models can be very useful not only to investigate the mechanism underlying pathogenetic autoantibody production and autoantibodies mediated tissue
injury, but also for the development of more effective
therapeutic strategies for this disease.
Abbreviations
EB: Epidermolysis bullosa; RDEB: Recessive dystrophic epidermolysis bullosa;
EBS: Epidermolysis bullosa simplex; IIF: Indirect immunofluorescence;
ELISA: Enzyme linked immunosorbant assay; BP: Bullous pemphigoid;
JEB: Junctional epidermolysis bullosa; DEB: Dystrophic epidermolysis bullosa;
BMZ: Basement membrane zone; IFM: Immunofluorescence mapping;
TEM: Transmission electron microscopy; NC: Non-collagenous;
EBA: Epidermolysis bullosa acquisita; IgG: Immunoglobulin G; MMP: Mucous
membrane pemphigoid; BEBS: Birmingham epidermolysis bullosa severity
score; PV: Pemphigus vulgaris; ICS: Intercellular substance; RT: Room
temperature; OD: Optical density; ROC: Receiver operating characteristics;
AUC: Area under the curve; CI: Confidence interval; OR: Odds ratio;
ES: Epitope spreading.
Tampoia et al. Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
Competing interests
The authors declare that they have no financial and no-financial competing
interests.
Authors contributions
MT and GA conceived and designed the study; MT performed the assays
and carried out the statistical analysis; LG, GA and AF obtained the clinical
data; GA, DB and LB interpreted the data; MT, AF and MGM wrote the paper;
CDG made the linguistic revision. All authors read and approved the final
manuscript.
Author details
1
Laboratory of Clinical Pathology, University Hospital of Bari, Piazza Giulio
Cesare 11, Bari 70124, Italy. 2Department of Biomedical Sciences and Human
Oncology, Dermatology Department, University Hospital of Bari, Bari, Italy.
3
Department of Clinical and Experimental Medicine, University of Foggia,
Foggia, Italy. 4Pediatric Department B. Trambusti, University Hospital of Bari,
Bari, Italy. 5Department of Emergency and Organ Transplantation, University
of Bari, Bari, Italy. 6Regional Coordination for Rare Diseases-Ares Puglia, Bari,
Italy.
Received: 26 April 2013 Accepted: 16 August 2013
Published: 4 September 2013
References
1. Fine JD, Eady RA, Bauer EA, Bauer JW, Bruckner-Tuderman L, Heagerty A,
Hintner H, Hovnanian A, Jonkman MF, Leigh I, McGrath JA, Mellerio JE,
Murrell DF, Shimizu H, Uitto J, Vahlquist A, Woodley D, Zambruno G: The
classification of inherited epidermolysis bullosa (EB): report of the Third
International Consensus Meeting on Diagnosis and Classification of EB.
J Am Acad Dermatol 2008, 58:931950.
2. Fine JD: Inherited epidermolysis bullosa. Orphanet J Rare Dis 2010,
28:512.
3. Uitto J, Richard G: Progress in epidermolysis bullosa: from eponyms to
molecular genetic classification. Clin Dermatol 2005, 23:3340.
4. Shimizu H, Sato M, Ban M, Kitajima Y, Ishizaki S, Harada T, BrucknerTuderman L, Fine JD, Burgeson R, Kon A, McGrath JA, Christiano AM, Uitto J,
Nishikawa T: Immunohistochemical, ultrastructural, and molecular
features of Kindler syndrome distinguish it from dystrophic
epidermolysis bullosa. Arch Dermatol 1997, 133:11111117.
5. Has C: Molecular genetic assays for inherited epidermolysis bullosa.
Clin Dermatol 2011, 29:420426.
6. Wertheim-Tysarowska K, Sobczyska-Tomaszewska A, Kowalewski C, Skroski
M, Swikowski G, Kutkowska-Kamierczak A, Woniak K, Bal J: The COL7A1
mutation database. Hum Mutat 2012, 33:327331.
7. Intong LR, Murrell DF: Inherited epidermolysis bullosa: new diagnostic
criteria and classification. Clin Dermatol 2012, 30:7077.
8. Pohla-Gubo G, Cepeda-Valdes R, Hintner H: Immunofluorescence mapping
for epidermolysis bullosa. Dermatol Clin 2010, 28:201210.
9. Yiasemides E, Walton J, Marr P, Villanueva EV, Murrell DF: A comparative
study between transmission electron microscopy and
immunofluorescence mapping in the diagnosis of epidermolysis bullosa.
Am J Dermatopathol 2006, 28:387394.
10. Uitto J, Christiano AM: Molecular basis for the dystrophic forms of
epidermolysis bullosa: mutations in the type VII collagen gene.
Arch Dermatol Res 1994, 287:1622.
11. Christiano AM, Rosenbaum LM, Chung-Honet LC, Parente MG, Woodley DT,
Pan TC, Zhang RZ, Chu ML, Burgeson RE, Uitto J: The large noncollagenous domain (NC-1) of type VII collagen is amino-terminal and
chimeric: homology to cartilage matrix protein, the type III domains of
fibronectin and the A domains of von Willebrand factor. Hum Mol Genet
1992, 1:475481.
12. Greenspan DS: The carboxyl-terminal half of type VII collagen, including
the non-collagenous NC-2 domain and intronexon organization of
the corresponding region of the COL7A1 gene. Hum Mol Genet 1993,
2:273278.
13. Chung HJ, Uitto J: Type VII collagen: the anchoring fibril protein at fault
in dystrophic epidermolysis bullosa. Dermatol Clin 2010, 28:93105.
14. Gupta R, Woodley DT, Chen M: Epidermolysis bullosa acquisita. Clin Dermatol
2012, 30:6069.
Page 9 of 10
15. Sitaru AG, Sesarman A, Mihai S, Chiriac MT, Zillikens D, Hultman P, Solbach
W, Sitaru C: T cells are required for the production of blister-inducing
autoantibodies in experimental epidermolysis bullosa acquisita.
J Immunol 2010, 184:15961603.
16. Woodley DT, Briggaman RA, O'Keefe EJ, Inman AO, Queen LL, Gammon WR:
Identification of the skin basement-membrane autoantigen in
epidermolysis bullosa acquisita. N Engl J Med 1984, 310:10071013.
17. Tanaka H, Ishida-Yamamoto A, Hashimoto T, Hiramoto K, Harada T, Kawachi
Y, Shimizu H, Tanaka T, Kishiyama K, Hpfner B, Takahashi H, Iizuka H,
Bruckner-Tuderman L: A novel variant of acquired epidermolysis bullosa
with autoantibodies against the central triple-helical domain of type VII
collagen. Lab Invest 1997, 77:623632.
18. Mller R, Dahler C, Mbs C, Wenzel E, Eming R, Messer G, Niedermeier A,
Hertl M: T and B cells target identical regions of the non-collagenous
domain 1 of type VII collagen in epidermolysis bullosa acquisita.
Clin Immunol 2010, 135:99107.
19. Schmidt E, Zillikens D: Modern diagnosis of autoimmune blistering skin
diseases. Autoimmun Rev 2010, 10:8489.
20. Saleh MA, Ishii K, Kim YJ, Murakami A, Ishii N, Hashimoto T, Schmidt E,
Zillikens D, Shirakata Y, Hashimoto K, Kitajima Y, Amagai M: Development
of NC-1 and NC-2 domains of Type VII collagen ELISA for the diagnosis
and analysis of the time course of epidermolysis bullosa acquisita
patients. J Dermatol Sci 2011, 62:169175.
21. Komorowski L, Mller R, Vorobyev A, Probst C, Recke A, Jonkman MF,
Hashimoto T, Kim SC, Groves R, Ludwig RJ, Zillikens D, Stcker W, Schmidt
E: Sensitive and specific assays for routine serological diagnosis of
epidermolysis bullosa acquisita. J Am Acad Dermatol 2013, 68:e89e95.
22. Sato M, Ishitsuka A, Shibuya Y, Kanoh H, Koga H, Hashimoto T, Seishima M:
Time-course of the change in titre of antibodies against type VII
collagen in a patient with epidermolysis bullosa acquisita. Acta Derm
Venereol 2012, 92:693694.
23. Marzano AV, Cozzani E, Fanoni D, De Pit O, Vassallo C, Berti E, Parodi
A, Crosti C, Cugno M: Diagnosis and disease severity assessment of
epidermolysis bullosa acquisita by ELISA for anti-type VII collagen
autoantibodies: an Italian multicentre study. Br J Dermatol 2013,
168:8084.
24. Kim JH, Kim YH, Kim S, Noh EB, Kim SE, Vorobyev A, Schmidt E, Zillikens D,
Kim SC: Serum levels of anti-type VII collagen antibodies detected by
enzyme-linked immunosorbent assay in patients with epidermolysis
bullosa acquisita are correlated with the severity of skin lesions.
J Eur Acad Dermatol Venereol 2013, 27:e224e230.
25. Sitaru C, Mihai S, Otto C, Chiriac MT, Hausser I, Dotterweich B, Saito H, Rose
C, Ishiko A, Zillikens D: Induction of dermal-epidermal separation in mice
by passive transfer of antibodies specific to type VII collagen. J Clin Invest
2005, 115:870878.
26. Woodley DT, Ram R, Doostan A, Bandyopadhyay P, Huang Y, Remington J,
Hou Y, Keene DR, Liu Z, Chen M: Induction of epidermolysis bullosa
acquisita in mice by passive transfer of autoantibodies from patients.
J Invest Dermatol 2006, 126:13231330.
27. Ludwig RJ, Recke A, Bieber K, Mller S, Marques Ade C, Banczyk D, Hirose M,
Kasperkiewicz M, Ishii N, Schmidt E, Westermann J, Zillikens D, Ibrahim SM:
Generation of antibodies of distinct subclasses and specificity is linked
to H2s in an active mouse model of epidermolysis bullosa acquisita.
J Invest Dermatol 2011, 131:167176.
28. Moss C, Wong A, Davies P: The Birmingham Epidermolysis Bullosa
Severity score: development and validation. Br J Dermatol 2009,
160:10571065.
29. Chen M, Kim GH, Prakash L, Woodley DT: Epidermolysis bullosa acquisita:
autoimmunity to anchoring fibril collagen. Autoimmunity 2012, 45:91101.
30. Sesarman A, Sitaru C: Induction of experimental epidermolysis bullosa
acquisita by immunization with murine collagen VII. Meth Mol Biol 2013,
961:371387.
31. Lu Q: The critical importance of epigenetics in autoimmunity. J Autoimmun
2013, 41:15.
32. Cusick MF, Libbey JE, Fujinami RS: Molecular mimicry as a mechanism of
autoimmune disease. Clin Rev Allergy Immunol 2012, 42:102111.
33. Hundorfean G, Neurath MF, Sitaru C: Autoimmunity against type VII
collagen in inflammatory bowel disease. J Cell Mol Med 2010,
14:23932403.
34. Licarete E, Ganz S, Recknagel MJ, Di Zenzo G, Hashimoto T, Hertl M,
Zambruno G, Hundorfean G, Mudter J, Neurath MF, Bruckner-Tuderman L,
Tampoia et al. Orphanet Journal of Rare Diseases 2013, 8:132
http://www.ojrd.com/content/8/1/132
35.
36.
37.
38.
39.
Page 10 of 10
Sitaru C: Prevalence of collagen VII-specific autoantibodies in patients
with autoimmune and inflammatory diseases. BMC Immunol 2012, 13:16.
Mihai S, Chiriac MT, Herrero-Gonzlez JE, Goodall M, Jefferis R, Savage CO,
Zillikens D, Sitaru C: IgG4 autoantibodies induce dermal-epidermal
separation. J Cell Mol Med 2007, 11:11171128.
Di Zenzo G, Thoma-Uszynski S, Calabresi V, Fontao L, Hofmann SC, Lacour
JP, Sera F, Bruckner-Tuderman L, Zambruno G, Borradori L, Hertl M:
Demonstration of epitope e-spreading phenomena in bullous
pemphigoid: results of a prospective multicenter study. J Invest Dermatol
2011, 131:22712280.
Tamai K, Hashimoto I, Hanada K, Ikeda S, Imamura S, Ogawa H: Japanese
Study Group for Rare Intractable Skin Diseases: Japanese guidelines for
diagnosis and treatment of junctional and dystrophic epidermolysis
bullosa. Arch Dermatol Res 2003, 295:S24S28.
Fortuna G, Chainani-Wu N, Lozada-Nur F, Aria M, Cepeda-Valdes R, Pollio A,
Marinkovich MP, Martinez-Salazar AE, Mignogna MD, Bruckner AL, Salas-Alan
s JC: Epidermolysis Bullosa Oropharyngeal Severity (EBOS) score: a
multicenter development and reliability assessment. J Am Acad Dermatol
2013, 68:8392.
Loh CH, Kim J, Su JC, Daniel BS, Venugopal SS, Rhodes LM, Intong L, Law M,
Murrell DF: Excellent reliability and validity of a novel Epidermolysis
Bullosa Disease Activity and Scarring Index (EBDASI) compared to two
other outcome measures. J Investig Dermatol 2013, 133(S1):518.
doi:10.1186/1750-1172-8-132
Cite this article as: Tampoia et al.: Prevalence of specific anti-skin
autoantibodies in a cohort of patients with inherited epidermolysis
bullosa. Orphanet Journal of Rare Diseases 2013 8:132.
Submit your next manuscript to BioMed Central
and take full advantage of:
Convenient online submission
Thorough peer review
No space constraints or color gure charges
Immediate publication on acceptance
Inclusion in PubMed, CAS, Scopus and Google Scholar
Research which is freely available for redistribution
Submit your manuscript at
www.biomedcentral.com/submit
Vous aimerez peut-être aussi
- 68th AACC Annual Scientific Meeting Abstract eBookD'Everand68th AACC Annual Scientific Meeting Abstract eBookPas encore d'évaluation
- 10 1016@j Autrev 2019 06 007Document10 pages10 1016@j Autrev 2019 06 007Castle SkyPas encore d'évaluation
- Isrn Dermatology2013-812029Document25 pagesIsrn Dermatology2013-812029Anonymous hTivgzixVNPas encore d'évaluation
- NIH Public Access: Author ManuscriptDocument17 pagesNIH Public Access: Author ManuscriptAnonymous hTivgzixVNPas encore d'évaluation
- Direct Immmuno Flourescence Study in Auto Immune Bullous DisordersDocument3 pagesDirect Immmuno Flourescence Study in Auto Immune Bullous DisordersInternational Organization of Scientific Research (IOSR)Pas encore d'évaluation
- DescargaDocument19 pagesDescargaGianlucca GiardelliPas encore d'évaluation
- 13.autoimmune Basement AbreuVelezAMDocument16 pages13.autoimmune Basement AbreuVelezAMJulie Payne-KingPas encore d'évaluation
- Vesicubullous Diseases & Mucocutaneous DisordersDocument23 pagesVesicubullous Diseases & Mucocutaneous Disordersshahlaraib001Pas encore d'évaluation
- Diagnosis of Autoimmune BullousDocument15 pagesDiagnosis of Autoimmune BullousNadim SalejeePas encore d'évaluation
- Lupus Band Test in SLE, DLEDocument3 pagesLupus Band Test in SLE, DLEKuldeepSinghBanaPas encore d'évaluation
- Seminar: Enno Schmidt, Detlef ZillikensDocument13 pagesSeminar: Enno Schmidt, Detlef ZillikensUssiy RachmanPas encore d'évaluation
- Pemphigus: by Demetris Ioannides, MD Associate Professor of DermatologyDocument43 pagesPemphigus: by Demetris Ioannides, MD Associate Professor of DermatologyYulita PurbaPas encore d'évaluation
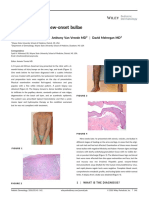
- Itchy Bumps With New-Onset Bullae: Syed H. Mahmood BS - Anthony Van Vreede MD - David Mehregan MDDocument2 pagesItchy Bumps With New-Onset Bullae: Syed H. Mahmood BS - Anthony Van Vreede MD - David Mehregan MDAna MariaPas encore d'évaluation
- Jcad 6 8 23Document6 pagesJcad 6 8 23Hadi FirmansyahPas encore d'évaluation
- Direct Immunofluorescence and Histopathology in Chronic Discoid Lupus ErythematosusDocument4 pagesDirect Immunofluorescence and Histopathology in Chronic Discoid Lupus ErythematosusdesiPas encore d'évaluation
- Pemphigus vulgarisPPTDocument23 pagesPemphigus vulgarisPPTSiti HanisaPas encore d'évaluation
- Diagnosing New Autoimmune Blistering Skin Diseases of Dogs and CatsDocument5 pagesDiagnosing New Autoimmune Blistering Skin Diseases of Dogs and CatsLauPas encore d'évaluation
- A Comparative Study Between Transmission ElectronDocument8 pagesA Comparative Study Between Transmission ElectronYuyan DuanPas encore d'évaluation
- Anetodermic Lupus Panniculitis and Antiphospholipid Antibodies: Report of Three CasesDocument4 pagesAnetodermic Lupus Panniculitis and Antiphospholipid Antibodies: Report of Three CasesDermatologie VenerologiePas encore d'évaluation
- MortalDocument6 pagesMortalazhar naufaldiPas encore d'évaluation
- BP InggrisDocument5 pagesBP InggrisJe'ii PadillaPas encore d'évaluation
- This Article: Natural Gene Therapy in Dystrophic Epidermolysis BullosaDocument10 pagesThis Article: Natural Gene Therapy in Dystrophic Epidermolysis BullosaNadzira KarimaPas encore d'évaluation
- Diagnosis of Autoimmune Blistering DiseasesDocument14 pagesDiagnosis of Autoimmune Blistering DiseasesElisa CarreraPas encore d'évaluation
- Ashy Dermatosis and Lichen PlanusDocument27 pagesAshy Dermatosis and Lichen PlanusAthenaeum Scientific PublishersPas encore d'évaluation
- 1471 5945 10 10Document3 pages1471 5945 10 10TheQueensafa90Pas encore d'évaluation
- Cryptococcal Cellulitis in A Patient With Myelodysplastic SyndromeDocument2 pagesCryptococcal Cellulitis in A Patient With Myelodysplastic SyndromeSan Maria SitompulPas encore d'évaluation
- EBV-induced Erythema Multiforme: A CaseDocument3 pagesEBV-induced Erythema Multiforme: A CaseNicco MarantsonPas encore d'évaluation
- Epidermolysis Bullosa Acquisita The 2019 Update PDFDocument28 pagesEpidermolysis Bullosa Acquisita The 2019 Update PDFindriPas encore d'évaluation
- Bullous PemphigoidDocument13 pagesBullous PemphigoidSharifah HanimPas encore d'évaluation
- Epidermolysis Bullosa Simplex: Case Report: Ernawati HidayatDocument5 pagesEpidermolysis Bullosa Simplex: Case Report: Ernawati HidayatliyaPas encore d'évaluation
- 13 DH-OrtizBDocument4 pages13 DH-OrtizBD U N I A A N I M EPas encore d'évaluation
- Immunofluorescence in Dermatology: Review ArticleDocument16 pagesImmunofluorescence in Dermatology: Review ArticlefeliciaPas encore d'évaluation
- 2 5456181012360856193Document70 pages2 5456181012360856193Maha KhalidPas encore d'évaluation
- Biomedicines 10 01197 v2Document10 pagesBiomedicines 10 01197 v2Silvia Montejo FareloPas encore d'évaluation
- Paraneoplastic Pemphigus With Clinical Features of Lichen Planus Associated With Low-Grade B Cell LymphomaDocument7 pagesParaneoplastic Pemphigus With Clinical Features of Lichen Planus Associated With Low-Grade B Cell LymphomalizasilvianaPas encore d'évaluation
- IT 14 - ANT Kornea Dan KeratitisDocument36 pagesIT 14 - ANT Kornea Dan KeratitisVhandy RamadhanPas encore d'évaluation
- 2020 - Pemphigus Vulgaris and Bullous Pemphigoid Update On Diagnosis and TreatmentDocument12 pages2020 - Pemphigus Vulgaris and Bullous Pemphigoid Update On Diagnosis and TreatmentnancyerlenPas encore d'évaluation
- Main 1Document10 pagesMain 1Adianto Jaya Nagara, drPas encore d'évaluation
- Immunopathogenesis of Pemphigus Vulgaris: A Brief ReviewDocument3 pagesImmunopathogenesis of Pemphigus Vulgaris: A Brief ReviewAnonymous SPrI0gbTr0Pas encore d'évaluation
- Oleogel-S10 Phase 3 Study "EASE" For Epidermolysis Bullosa: Study Design and RationaleDocument13 pagesOleogel-S10 Phase 3 Study "EASE" For Epidermolysis Bullosa: Study Design and RationalePaola PassarielloPas encore d'évaluation
- 1 s2.0 S1578219020300792 MainDocument2 pages1 s2.0 S1578219020300792 MainFeyzullah TokgözPas encore d'évaluation
- Jurnal 1Document5 pagesJurnal 1Dzaenap UlfahPas encore d'évaluation
- 575 1273 0 Immunofluorescence in Dermatology-MutasimDocument22 pages575 1273 0 Immunofluorescence in Dermatology-MutasimLeandro QuitoPas encore d'évaluation
- Out 3Document9 pagesOut 3Musthafa Afif WardhanaPas encore d'évaluation
- Pityriasis Alba: A Condition With Possibly Multiple EtiologiesDocument2 pagesPityriasis Alba: A Condition With Possibly Multiple EtiologiesAndana Haris R.Pas encore d'évaluation
- Review On Pathogenesis of Pemphigus: Dr. P. T. Chan Social Hygiene Service (Dermatology), Department of Health, Hong KongDocument7 pagesReview On Pathogenesis of Pemphigus: Dr. P. T. Chan Social Hygiene Service (Dermatology), Department of Health, Hong KongMeuthia AlamsyahPas encore d'évaluation
- Microbiology - Inicet Nov 2022Document19 pagesMicrobiology - Inicet Nov 2022Kuldeep SinghPas encore d'évaluation
- Boeira2013 Détails de L'ep Et Les TypesDocument14 pagesBoeira2013 Détails de L'ep Et Les Typesislem fekiPas encore d'évaluation
- Joost Schalkwijk., 2010 PDFDocument11 pagesJoost Schalkwijk., 2010 PDFInna LiashenkoPas encore d'évaluation
- Autoimmune Diseases of The Oral CavityDocument143 pagesAutoimmune Diseases of The Oral CavityMohammed ShaikhPas encore d'évaluation
- Diagnosisandclinical Featuresofpemphigus Vulgaris: Supriya S. Venugopal,, Dédée F. MurrellDocument1 pageDiagnosisandclinical Featuresofpemphigus Vulgaris: Supriya S. Venugopal,, Dédée F. MurrellDwiKamaswariPas encore d'évaluation
- Erythema MultiformeDocument5 pagesErythema MultiformeNicco MarantsonPas encore d'évaluation
- Distrophic EBDocument29 pagesDistrophic EBcyntia arumPas encore d'évaluation
- Clinical Spectrum of Skin Manifestations of Lyme Borreliosis in 204 Children in AustriaDocument7 pagesClinical Spectrum of Skin Manifestations of Lyme Borreliosis in 204 Children in Austriadanucj.2009Pas encore d'évaluation
- Chronic Spontaneous Urticaria-Status Quo and Future: Susanne Melchers Jan P. NicolayDocument11 pagesChronic Spontaneous Urticaria-Status Quo and Future: Susanne Melchers Jan P. NicolayRizka ZulaikhaPas encore d'évaluation
- Clinical and Microscopic Features of Generalized Discois LupusDocument14 pagesClinical and Microscopic Features of Generalized Discois LupusPatrícia StancuPas encore d'évaluation
- JCM 10 01040Document15 pagesJCM 10 01040Luminita HutanuPas encore d'évaluation
- Clinical and Experimental AllergyDocument11 pagesClinical and Experimental AllergyrobbyPas encore d'évaluation
- Single Nucleotide Polymorphism-Based Genome-Wide Linkage Analysis in Japanese Atopic Dermatitis FamiliesDocument8 pagesSingle Nucleotide Polymorphism-Based Genome-Wide Linkage Analysis in Japanese Atopic Dermatitis FamiliesdermRounds Dermatology NetworkPas encore d'évaluation
- Dystrophic Epidermolysis Bullosa:Pathogenesis AndclinicalfeaturesDocument8 pagesDystrophic Epidermolysis Bullosa:Pathogenesis AndclinicalfeaturesRiefka Ananda ZulfaPas encore d'évaluation
- YaniiiDocument24 pagesYaniiiAnonymous hTivgzixVNPas encore d'évaluation
- Chronic OpioidDocument19 pagesChronic OpioidAnonymous hTivgzixVNPas encore d'évaluation
- Femur Leg FracturesDocument78 pagesFemur Leg FracturesAnonymous hTivgzixVNPas encore d'évaluation
- Prof. Dr. Dr. Syarifuddin Rauf, Spa (K)Document9 pagesProf. Dr. Dr. Syarifuddin Rauf, Spa (K)Anonymous hTivgzixVNPas encore d'évaluation
- Eb SimplexDocument10 pagesEb SimplexAnonymous hTivgzixVNPas encore d'évaluation
- Bacterial Food IntoxicationDocument46 pagesBacterial Food IntoxicationAnonymous hTivgzixVNPas encore d'évaluation
- Presentation SurgionDocument16 pagesPresentation SurgionAnonymous hTivgzixVNPas encore d'évaluation
- Serum Protein PDFDocument5 pagesSerum Protein PDFAnonymous hTivgzixVNPas encore d'évaluation
- Biochemistry of Urine: Biomedic 2Document29 pagesBiochemistry of Urine: Biomedic 2Anonymous hTivgzixVNPas encore d'évaluation
- VitiligoDocument24 pagesVitiligoAnonymous hTivgzixVNPas encore d'évaluation
- 1 - Kuliah Pengenalan OrganDocument155 pages1 - Kuliah Pengenalan OrganAan KhaerismanPas encore d'évaluation
- Thromb 1Document7 pagesThromb 1AlisPas encore d'évaluation
- Autoimmunity and Autoimmune DiseasesDocument89 pagesAutoimmunity and Autoimmune DiseasesImmas Wahyu FajariniPas encore d'évaluation
- Dr. Jean Dodds Responding Exp. Report (Plaintiff)Document24 pagesDr. Jean Dodds Responding Exp. Report (Plaintiff)Osiris-KhentamentiuPas encore d'évaluation
- Autoimmune Disease MechanismsDocument6 pagesAutoimmune Disease MechanismsHaliunaa BattulgaPas encore d'évaluation
- Overview of Autoimmune Hepatitis - UpToDateDocument33 pagesOverview of Autoimmune Hepatitis - UpToDatebagir_dm10Pas encore d'évaluation
- Coombs TestDocument13 pagesCoombs TestPatNoppadolPas encore d'évaluation
- 2014 - SLE LectureDocument96 pages2014 - SLE LectureDon CaprettoPas encore d'évaluation
- Approach To The Patient With Rheumatic DiseaseDocument11 pagesApproach To The Patient With Rheumatic DiseasetedplushPas encore d'évaluation
- Autoimmune Diseases and Types PDFDocument24 pagesAutoimmune Diseases and Types PDFBaqar ZaidiPas encore d'évaluation
- The Autoimmune Disease MythDocument20 pagesThe Autoimmune Disease MythMark Sloan100% (5)
- Clinical Significance of Antinuclear Antibody Staining Patterns and Associated Autoantibodies - UpToDateDocument13 pagesClinical Significance of Antinuclear Antibody Staining Patterns and Associated Autoantibodies - UpToDateMelanie NgPas encore d'évaluation
- Vaccination and Autoimmune Disease: What Is The Evidence?: ReviewDocument8 pagesVaccination and Autoimmune Disease: What Is The Evidence?: Reviewtito7227Pas encore d'évaluation
- Connective Tissue DisorderDocument51 pagesConnective Tissue DisorderKathleenZunigaPas encore d'évaluation
- 0239Document7 pages0239vishnupgiPas encore d'évaluation
- An Update On The Pathogenesis of Hashimoto's Thyroiditis: A. P. WeetmanDocument8 pagesAn Update On The Pathogenesis of Hashimoto's Thyroiditis: A. P. WeetmanMauricio VidalPas encore d'évaluation
- UntitledDocument66 pagesUntitledPhilip Edward OsbornePas encore d'évaluation
- Diagnosis of Pyrexia of Unknown Origin - in PracticeDocument10 pagesDiagnosis of Pyrexia of Unknown Origin - in PracticeVioletPas encore d'évaluation
- 44 - 75 - Detection of Autoantibodies Against Platelet Glycoproteins in ... HeDocument21 pages44 - 75 - Detection of Autoantibodies Against Platelet Glycoproteins in ... HevishnupgiPas encore d'évaluation
- Systemic Lupus ErythemathosusDocument23 pagesSystemic Lupus ErythemathosusFransisca HardimartaPas encore d'évaluation
- Autoimmune Disease-Associated HypertensionDocument9 pagesAutoimmune Disease-Associated HypertensiondennPas encore d'évaluation
- ACVIM Consensus Statement On The Diagnosis and TreatmentDocument28 pagesACVIM Consensus Statement On The Diagnosis and TreatmentBê LagoPas encore d'évaluation
- LP2 MAJOR EXAM 4 Files Merged 2 Files MergedDocument285 pagesLP2 MAJOR EXAM 4 Files Merged 2 Files MergedBianca ArcePas encore d'évaluation
- Anti-TG ARCDocument7 pagesAnti-TG ARCMariaPas encore d'évaluation
- Associação Da Ingestão de Glúten Nos Primeiros 5 Anos de Vida e A Incidencia de Doença CeliacaDocument10 pagesAssociação Da Ingestão de Glúten Nos Primeiros 5 Anos de Vida e A Incidencia de Doença CeliacaAna Beatriz SpagollaPas encore d'évaluation
- Autoimmune DisordersDocument6 pagesAutoimmune DisordersMaquille Ann CervalesPas encore d'évaluation
- LECTURE 7 AUTOIMMUNITY AND AUTOIMMUNE DISEASE Part1 PDFDocument20 pagesLECTURE 7 AUTOIMMUNITY AND AUTOIMMUNE DISEASE Part1 PDFMAYAPas encore d'évaluation
- Disorders of The Immune System: Allergic DiseasesDocument2 pagesDisorders of The Immune System: Allergic DiseasesElisha RosalynPas encore d'évaluation
- Plabable-Gems-16. Rheumatology Plabable GemsDocument28 pagesPlabable-Gems-16. Rheumatology Plabable GemsThuraPas encore d'évaluation
- Euroline Ana Profile 23 (Igg) Test Instruction: Modifications To The Former Version Are Marked in GreyDocument16 pagesEuroline Ana Profile 23 (Igg) Test Instruction: Modifications To The Former Version Are Marked in GreyRiskullah MakmurPas encore d'évaluation
- Autoimmune Diseases - MMSDocument37 pagesAutoimmune Diseases - MMSmulatumelesePas encore d'évaluation
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)D'EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Évaluation : 3 sur 5 étoiles3/5 (1)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedD'EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedÉvaluation : 4.5 sur 5 étoiles4.5/5 (82)
- The Age of Magical Overthinking: Notes on Modern IrrationalityD'EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityÉvaluation : 4 sur 5 étoiles4/5 (32)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionD'EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionÉvaluation : 4 sur 5 étoiles4/5 (404)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDD'EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDÉvaluation : 5 sur 5 étoiles5/5 (3)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsD'EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsPas encore d'évaluation
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsD'EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsÉvaluation : 5 sur 5 étoiles5/5 (1)
- The Comfort of Crows: A Backyard YearD'EverandThe Comfort of Crows: A Backyard YearÉvaluation : 4.5 sur 5 étoiles4.5/5 (23)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsD'EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsÉvaluation : 4 sur 5 étoiles4/5 (4)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisD'EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisÉvaluation : 3.5 sur 5 étoiles3.5/5 (2)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeD'EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeÉvaluation : 2 sur 5 étoiles2/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisD'EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisÉvaluation : 4.5 sur 5 étoiles4.5/5 (42)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.D'EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Évaluation : 4.5 sur 5 étoiles4.5/5 (110)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeD'EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeÉvaluation : 4.5 sur 5 étoiles4.5/5 (254)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsD'EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsÉvaluation : 4.5 sur 5 étoiles4.5/5 (170)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesD'EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesÉvaluation : 4.5 sur 5 étoiles4.5/5 (1412)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaD'EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- To Explain the World: The Discovery of Modern ScienceD'EverandTo Explain the World: The Discovery of Modern ScienceÉvaluation : 3.5 sur 5 étoiles3.5/5 (51)
- The Obesity Code: Unlocking the Secrets of Weight LossD'EverandThe Obesity Code: Unlocking the Secrets of Weight LossÉvaluation : 4 sur 5 étoiles4/5 (6)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryD'EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryÉvaluation : 4 sur 5 étoiles4/5 (46)
- The Marshmallow Test: Mastering Self-ControlD'EverandThe Marshmallow Test: Mastering Self-ControlÉvaluation : 4.5 sur 5 étoiles4.5/5 (60)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessD'EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessÉvaluation : 4.5 sur 5 étoiles4.5/5 (328)
- Why We Die: The New Science of Aging and the Quest for ImmortalityD'EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityÉvaluation : 4.5 sur 5 étoiles4.5/5 (6)
- How to ADHD: The Ultimate Guide and Strategies for Productivity and Well-BeingD'EverandHow to ADHD: The Ultimate Guide and Strategies for Productivity and Well-BeingÉvaluation : 1 sur 5 étoiles1/5 (1)