Académique Documents
Professionnel Documents
Culture Documents
Snuff
Transféré par
Anonymous 6koUBmDL0 évaluation0% ont trouvé ce document utile (0 vote)
26 vues4 pages,
Copyright
© © All Rights Reserved
Formats disponibles
DOCX, PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce document,
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
26 vues4 pagesSnuff
Transféré par
Anonymous 6koUBmDL,
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 4
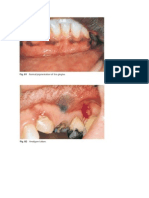
Snuff dippers patch (tobacco chewers esion, snuff keratosis)
A wrinked yellow-white area on the gingibal mucosa flexure and mandibular
buccal or labial mucosa is indicative of intraoral use of unburned tobacco.
Smokeless tobacco may take various forms (snuff, dip, plug, or quid), leaving its
characteristic mark at the preferential site of tobacoo placement. Posterior sites
are commonly utilized for dip, plig, or quid, whereas anterior sites are
preferential for snuff. Individuals who vary intraoral sites have multiple, less
prominent lesions. Male teenagers are most frquently affected, largely because
of intensive marketing efforts by tobacco companies.
Early snuff dippers patches are pale pink in color, with the surface appearing
corrugated and wrinkled. A progression to white, yellow-white, and ye;ow-brown
may ensue as hyperkeratosis and exogenous staining occur.
Chronic smokeless tobacco use is associated with periodontal alterations, caries,
epidermal dysplastic changes, and verrucous carcinoma. To achieve resolution,
cessation of use is recommended,. If normal appearance does not return 14 days
after cessation, biopsy is necessary
There arc marked geographic and gender differences
in tobacco use. In the United Slates there is a relatively
high prevalence of smokeless tobacco users in
the southern and western states. Usage by men in New
York and Rhode Island is less than 1 % of the population,
but in West Virginia it exceeds 20%. Among
teenagers, whites are the predominant users of smokeless
tobacco, with males making up nearly all of this
group. Smokeless tobacco is also used in Sweden, and
in regions such as the Indian subcontinent and Southeast
Asia, usage is even more common and the materials
more destructive in Southeast Asia. The tobacco
preparations are generally of a higher (alkaline) pH
and are often mixed with other ingredients, including
shredded areca (betel) nut, and also containing
lime, camphor, and spices.
The general increase in smokeless tobacco consumption
has been related to both peer pressure and
increased media advertising, which often glamorizes
the use of smokeless tobacco, or snuff dipping. In addition,
individuals who have been intense smokers or
those who wish to avoid smoking may gravitate to this
alternative. The clinical results of long-term exposure
to smokeless tobacco include the development of oral
mucosal white patches with a slightly increased malignant
potential, dependence, alterations of taste, acceleration
of periodontal disease, and significant amounts
of dental abrasion.
Etiology. A causal relationship has been documented
between smokeless tobacco and white tissue changes.
Although all forms of smokeless tobacco may potentially
cause alterations in the oral mucosa, snuff
(paniculate, finely divided, or shredded tobacco)
appears to be much more likely to cause oral lesions
than chewing tobacco. Oral mucosa responds to the
topically induced effects of tobacco with inflammation
and keratosis. Dysplastic changes may follow, with
a low-potential risk of malignant change. Smokeless
tobacco-induced alterations in tissues are thought to
be a response to tobacco constituents and perhaps
other agents that are added for flavoring or moisture
retention. Carcinogens, such as nitrosonornicotine,
an organic component of chewing tobacco and snuff,
have been identified in smokeless tobacco. The pH of
snuff, which ranges between 8.2 and 9.3, may be
another factor that contributes to the alteration of
mucosa.
Duration of exposure to smokeless tobacco that is
necessary to produce mucosal damage is measured in
terms of years. It has been demonstrated that leuko
plakia can be predicted with the use of three tins of
tobacco per week or duration of the habit for more
than 2 years.
Clinical Features. White lesions associated with smokeless
tobacco develop in the immediate area where
the tobacco is habitually placed (Figures 3-9 and
3-10). The most common area of involvement is
the mucobuccal fold of the mandible in either the
incisor or the molar region. The mucosa develops
a granular to wrinkled appearance. In advanced
cases a heavy, folded character may be seen. Less
often, an erythroplakic or red component may be
admixed with the white keratotic component. The
lesions are generally painless and asymptomatic, and]
their discovery is often incidental to routine oral
examination.
Chewing tobacco is an important established risk factor for the
development of oral carcinoma in the United States.52
Habitually chewing tobacco leaves or dipping snuff results in
the development of a well-recognized white mucosal lesion in
the area of tobacco contact, called smokeless tobacco keratosis,
snuff dippers keratosis, or tobacco pouch keratosis.53
90 Diagnosis and Management of Oral and Salivary Gland Diseases
While these lesions are accepted as precancerous, they are significantly
different from true leukoplakia and have a much
lower risk of malignant transformation.54
This habit was once almost universal in the United States
and is very common among certain other populations, most
notably in Sweden, India, and Southeast Asia.52,5560
Smokeless tobacco use among white males in the United
States has shown a recent resurgence.6062 The estimated proportion
of adult men in the United States who regularly use
spit tobacco ranges from 6 to 20%.58,63 This range is attributed
to significant geographic, cultural, and gender variations
in chewing habits.54 The cumulative incidence for
smokeless tobacco use was highest for non-Hispanic white
males.54 Unfortunately, the habit starts relatively early in life,
usually between the ages of 9 and 15 years, and is rarely begun
after 20 years of age. Recent epidemiologic data indicate that
over five million Americans use smokeless tobacco and that
more than 750,000 of these users are adolescents. It is estimated
that each year in the United States, approximately
800,000 young people between the ages of 11 and 19 years
experiment with smokeless tobacco and that about 300,000
become regular users.5559,63
Smokeless tobacco contains several known carcinogens,
including N-nitrosonornicotine (NNN), and these have been
proven to cause mucosal alterations.64 In addition to its established
role as a carcinogen, chewing tobacco may be a risk factor
in the development of root surface caries and, to a lesser
extent, coronal caries. This may be due to its high sugar content
and its association with increased amounts of gingival
recession.58 The duration of exposure is very important in the
production of mucosal damage. Leukoplakia has been
reported to develop with the habitual use of as little as three
cans of snuff per week for longer than 3 years.53 Although all
forms of smokeless tobacco may result in mucosal alterations,
snuff (a finely powdered tobacco) appears to be much more
likely to cause such changes than is chewing tobacco.53,59
Smokeless tobacco is not consistently associated with
increased rates of oral cancer.54Approximately 20% of all adult
Swedish males use moist snuff, yet it has not been possible to
detect any significant increase in the incidence of cancer of the
oral cavity or pharynx in Sweden. By international standards,
the prevalence of oral cancer is low in Sweden.52 This has been
attributed to variations in the composition of snuff, in particular,
the amount of fermented or cured tobacco in the mixture.
The carcinogen NNN is present in much lower concentrations
in Swedish snuff, probably because of a lack of fermentation
of the tobacco. Also, the high level of snuff use might decrease
the amount of cigarette smoking and therefore lead to a lesser
prevalence of oral cancer.52,54
TYPICAL FEATURES
Numerous alterations are found in habitual users of smokeless
tobacco. Most changes associated with the use of smokeless
tobacco are seen in the area contacting the tobacco. The most
common area of involvement is the anterior mandibular vestibule,
followed by the posterior vestibule.53 The surface of the mucosa.
appears white and is granular or wrinkled (Figure 5-9); in some
cases, a folded character may be seen (tobacco pouch keratosis).
Commonly noted is a characteristic area of gingival recession
with periodontal-tissue destruction in the immediate area of contact
(Figure 5-10). This recession involves the facial aspect of the
tooth or teeth and is related to the amount and duration of
tobacco use. The mucosa appears gray or gray-white and almost
translucent. Since the tobacco is not in the mouth during examination,
the usually stretched mucosa appears fissured or rippled,
and a pouch is usually present. This white tobacco pouch may
become leathery or nodular in long-term heavy users (Figure 511). Rarely, an erythroplakic component may be seen.The lesion
is usually asymptomatic and is discovered on routine examination.
Microscopically, the epithelium is hyperkeratotic and thickened.
A characteristic vacuolization or edema may be seen in the
keratin layer and in the superficial epithelium. Frank dysplasia is
uncommon in tobacco pouch keratosis.62
TREATMENT AND PROGNOSIS
Cessation of use almost always leads to a normal mucosal
appearance within 1 to 2 weeks.54,64,65 Biopsy specimens
should be obtained from lesions that remain after 1 month.
Biopsy is particularly indicated for those lesions that appear
clinically atypical and that include such features as surface
ulceration, erythroplakia, intense whiteness, or a verrucoid or
papillary surface.53, 62, 64 The risk of malignant transformation
is increased fourfold for chronic smokeless tobacco users.66
Vous aimerez peut-être aussi
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- Star BurnDocument7 pagesStar BurnAnonymous 6koUBmDLPas encore d'évaluation
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (587)
- Dental ArtDocument20 pagesDental ArtAnonymous 6koUBmDLPas encore d'évaluation
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (890)
- Humanitarian Supply BookDocument189 pagesHumanitarian Supply BookPeby Rajo MangindoPas encore d'évaluation
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Dapus Herpes VirusDocument1 pageDapus Herpes VirusAnonymous 6koUBmDLPas encore d'évaluation
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- Star BurnDocument7 pagesStar BurnAnonymous 6koUBmDLPas encore d'évaluation
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- 551 FullDocument10 pages551 FullAnonymous 6koUBmDLPas encore d'évaluation
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Bikin Variabel: Group StatisticsDocument5 pagesBikin Variabel: Group StatisticsAnonymous 6koUBmDLPas encore d'évaluation
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Amalgam Tattoo With DDDocument5 pagesAmalgam Tattoo With DDAnonymous 6koUBmDLPas encore d'évaluation
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Pattern Identification According To Qi and BloodDocument7 pagesPattern Identification According To Qi and BloodCarleta StanPas encore d'évaluation
- Original Article: Parathyroid Cytology: A Diagnostic DilemmaDocument6 pagesOriginal Article: Parathyroid Cytology: A Diagnostic DilemmaZuzu FinusPas encore d'évaluation
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Role of Teacher in School Health Education: by Rasheeda, Sabana, Raifa, NethraDocument15 pagesRole of Teacher in School Health Education: by Rasheeda, Sabana, Raifa, NethraJaved Abdul JaleelPas encore d'évaluation
- Cholecystitis and Biliary Colic: Learning ObjectivesDocument37 pagesCholecystitis and Biliary Colic: Learning Objectivesapi-19641337Pas encore d'évaluation
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- 2007 Menstrual History QuestionnaireDocument2 pages2007 Menstrual History QuestionnaireAnonymous kieXEbsGePas encore d'évaluation
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Kidney FunctionDocument2 pagesKidney FunctionTanjaPas encore d'évaluation
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2219)
- Ante Sample ExamDocument33 pagesAnte Sample ExamEric Matig-a EbradaPas encore d'évaluation
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Keratinization - Dr. PriyaDocument37 pagesKeratinization - Dr. PriyaDr. Priya Patel75% (4)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Dr. Osamu Mizukami's Health Promotion Clinic in TokyoDocument40 pagesDr. Osamu Mizukami's Health Promotion Clinic in TokyoLuckner Jr. Jean-BaptistePas encore d'évaluation
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (265)
- Essential Cases in Head and Neck OncologyDocument241 pagesEssential Cases in Head and Neck OncologyZuriPas encore d'évaluation
- Photographic Illustrations of Skin DiseasesDocument316 pagesPhotographic Illustrations of Skin DiseasessfranchiniPas encore d'évaluation
- Fever PresentationDocument15 pagesFever PresentationMaira InaamPas encore d'évaluation
- SCH - of - Charges - 2015 1 - 1 01072015Document61 pagesSCH - of - Charges - 2015 1 - 1 01072015Anil PurtyPas encore d'évaluation
- Vnus ClosurefastDocument2 pagesVnus ClosurefastBertha DuránPas encore d'évaluation
- Hpia Version 6.0 PDFDocument48 pagesHpia Version 6.0 PDFAl- ImanuddinPas encore d'évaluation
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Pain in Terminally IllDocument29 pagesPain in Terminally IllAida Tantri100% (1)
- Immunohematology HandoutDocument9 pagesImmunohematology Handoutmarkylopez2383% (6)
- DRUG NAME: Fluorouracil: Synonym (S) : Common Trade Name: ClassificationDocument14 pagesDRUG NAME: Fluorouracil: Synonym (S) : Common Trade Name: ClassificationNurul Kamilah SadliPas encore d'évaluation
- Case Study IN Penile CancerDocument15 pagesCase Study IN Penile CancerPrincess Gutierrez RositaPas encore d'évaluation
- Subjective Refraction Prescribing Glasses JCAHPODocument272 pagesSubjective Refraction Prescribing Glasses JCAHPOAndrei R LupuPas encore d'évaluation
- Lecture 5 Prenatal Genetic CounselingDocument53 pagesLecture 5 Prenatal Genetic Counselingjaish8904Pas encore d'évaluation
- Law360 ArticleDocument2 pagesLaw360 ArticleJohn DurstPas encore d'évaluation
- Surviving Breast CancerDocument55 pagesSurviving Breast CancerSalem NewsPas encore d'évaluation
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (119)
- The Efficacy of Acupuncture in The Treatment of Bell's Palsy SequelaeDocument11 pagesThe Efficacy of Acupuncture in The Treatment of Bell's Palsy Sequelaeseptiani hasibuanPas encore d'évaluation
- Tuberculosis and Lung Damage: From Epidemiology To PathophysiologyDocument20 pagesTuberculosis and Lung Damage: From Epidemiology To PathophysiologyDyan TonyPas encore d'évaluation
- Imaging Presacral MassesDocument102 pagesImaging Presacral Masseskiran_mmc100% (2)
- Daftar Kode Panyakit: Kode Bedah Kode Interna Kode NeuroDocument1 pageDaftar Kode Panyakit: Kode Bedah Kode Interna Kode NeuroMutemjPas encore d'évaluation
- Safe Mercury DetoxDocument6 pagesSafe Mercury DetoxJohn Jensen100% (2)
- Pathogenesis of Tuberculosis (TB) Infection - LabCE - Com, Laboratory Continuing EducationDocument2 pagesPathogenesis of Tuberculosis (TB) Infection - LabCE - Com, Laboratory Continuing Educationshrish chandra pandeyPas encore d'évaluation
- Pediatric Evans Syndrome Is Associated With A High Frequency of PDFDocument41 pagesPediatric Evans Syndrome Is Associated With A High Frequency of PDFJerryEddyaPutraBoerPas encore d'évaluation
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)