Académique Documents
Professionnel Documents
Culture Documents
Refractory PPH Case
Transféré par
SUSPADescription originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Refractory PPH Case
Transféré par
SUSPADroits d'auteur :
Formats disponibles
370
Journal of Clinical and Biomedical Sciences
Journal homepage: www.jcbsonline.ac.in
Case Report
Refractory Postpartum Haemorrhage - A Case Report
Ratna Bulusu*1, Prathibha S D2, Maheshwari2, Vijay Kumar C R2, Homeira Nishat2
1. Department Obstetrics and Gynaecology, MVJ Medical College and Research Hospital, Dandupalya, Hoskote, Bangalore.
2. Dept Of Obstetrics and Gynaecology, Dr B R Ambedkar Medical College and Hospital, Kadugondanahalli, Bangalore.
Received: 14th October 2014 Accepted: 5th December-2014 Published: 31st-December 2014
Abstract
A case of uterine haemorrhage in the puerperium where conventional treatment failed with the final diagnosis of
arteriovenous malformations which required uterine tamponade, and GnRH agonists. A refractory case of PPH.
Key words: Secondary postpartum haemorrhage, Arterio-venous malformations .
Introduction
Uterine arteriovenous malformations (AVM) are
rare lesions with a considerable risk potential. Clinical
presentation varies from no signs over various degrees of menorrhagia to massive life-threatening vaginal bleeding. Clinical suspicion is essential for a
prompt diagnosis and treatment. Recent reports have
mentioned successful conservative management such
as surgical removal of AVM, laparoscopic bipolar coagulation of the uterine arteries and long term medical
therapy1. Uterine artery embolization is one effective
management for controlling hemorrhage 2.
Case History
A 20 years old lady, married for 1 years, was admitted in the department of Gynaecology and Obstetrics in Dr.B.R. Ambedkar Medical College and Hospital,
Bangalore, with excessive bleeding per vagina since
two months. Obstetric history revealed that she is P1
L1, Last child birth - 2 months back. Patient underwent emergency Caesarean delivery two months ago,
in a private institution for IUGR with PROM with Oligohydraminos. Post operative period was uneventful.
Twenty four days after surgery, she had excessive vaginal bleeding for one day. She changed about 15 pads
in one day.
Bleeding was associated with abdomen pain and
passing of clots. She was admitted to another private
hospital where 2 units of blood were transfused.
Bleeding stopped following symptomatic Rx and patient discharged. Four days later, patient had one
more episode of excessive vaginal bleeding which
was managed conservatively in another hospital. She
had a total of four episodes of heavy vaginal bleeding following which she went to a Govt., hospital
where 3 units of blood was transfused and D &C was
done. Her serum hCG values were normal for non
pregnant condition (< 0.1units /ml).
Episodic bleeding per vagina still persisted for
20 days following which patient reported to Dr B R
Ambedkar Hospital (02 months from the LSCS). On
admission, Hb% was 7.4 gm%. 02 units of blood
were transfused. USG with Doppler study: Dilated
and tortuous arteries in the anterior wall of lower
body of uterus with involvement of left lateral wall- ?
Vascular malformation. Diagnostic hysteroscopy
showed FLIMSY COBWEB LIKE adhesions in the
uterine cavity with multiple big and medium size
blood vessels traversing through them. (Fig 1, 2,).
Ball cautery at the bases of the vessels was not possible as it was very difficult to visualise the bases of
several vessels due to cotton wool adhesions and
highly intertwining anastomotic vessels all over in
the uterine cavity.
*Corresponding Author
Dr Ratna Bulusu, Professor and HOD Department Obstetrics and Gynaecology, MVJ Medical College and Research
Hospital, Dandupalya , Hoskote, Bangalore, India.
E mail : ratna_bulusu@yahoo.co.in; ratnabulusu@gmail.com
J Clin Biomed Sci 2014; 4(4):370-72
2014 Journal of Clinical and Biomedical Sciences. All rights reserved.
Quick access Code
Refractory Postpartum Haemorrhage
On POD 3 of diagnostic hysteroscopy, Inj
Leuproliide Depot 3.75mg SC was given. --- bleeding
apparently stopped. On POD 5, patient had sudden
episode of heavy bleeding P/V with passage of clots.
Uterine cavity balloon tamponade was done
with Foleys catheter No. 16 with bulb inflated with 30
ml of distilled water. The Catheter was removed on
POD 8 (after three days). No fresh episodes of bleeding
PV or pain abdomen. Patient was asymptomatic and
was discharged on D16 following admission.
Follow up - Patient has regular cycles. No further episodes of excessive bleeding.
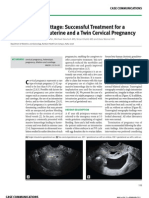
Figure 1&2: Diagnostic hysteroscopy showed FLIMSY COBWEB LIKE adhesions in the uterine cavity with multiple big
and medium size blood vessels traversing through them.
Discussion
The first case of AVM was reported in 1926 by
Dubreuil and Loubat 3. It consists of proliferation of
arterial and venous channels with fistula formation
and admixture of small capillary like channels. In
many cases, distinction between artery and vein becomes blurred due to secondary intimal thickening in
the veins as a result of increased intraluminal pressure.
371
Uterine AVM may be congenital or acquired.
Congenital uterine AVM may be isolated or may occur in association with AVM in other organs. Acquired AVMs may be due to previous uterine trauma
(such as uterine curettage), gestational trophoblastic
disease, caesarean section, intrauterine contraceptive devices, and necrotic chorionic villi invading
venous sinuses. 4 In our case, uterine AVM was acquired in nature as it started after caesarean section.
Though angiography remains the gold standard imaging technique for diagnosis of uterine AVM5
our case was diagnosed by colour doppler sonography. Wiebe and Switzer reported seven cases of AVM
diagnosed by colour Doppler sonography. 6Management depends on the age of the patient, her desire
for future fertility and severity of bleeding. In the
past, treatment had been confined to hysterectomy.
In the last decade, an increasing number of women
have been treated conservatively with success and
hysterectomy is no longer considered essential.
Acute management includes measures to stabilize the patient, uterine tamponade withFoley's
catheter or rolled gauze packing, and medical therapies like estrogens, progestins, methyl-ergonovine,
danazol, and 15-methyl-prostaglandin F2alpha. In
stable women, expectant management, surgical removal of an AVM, laparoscopic bipolar coagulation
of the uterine blood vessels, and long-term medical
therapy with combined oral contraceptive pills are
reported1. Recent reports have described successful
treatment of uterine artery embolization with different materials used singly or in combination such as
autologous blood clot, gel foam, microfibrillar collagen, polyvinyl alcohol, isobutyl cyanoacrylate and
steel coil spring occluders7.
Gonadotropin-releasing hormone agonists
have been used as an adjunct to embolization and
6months of therapy reduced the size of a uterine
AVM from 5.1 x 3.8 cm to 1.4 x 1.0 cm 8. Subsequent
uterine artery embolization resulted in complete
disappearance of the AVM, and normal cycles were
resumed 3 months later. The authors concluded that
gonadotropin-releasing hormone agonist therapy
may be useful in situations where embolization procedures are not available or can be postponed.
J Clin Biomed Sci 2014; 4(4):370-72
Refractory Postpartum Haemorrhage
Conclusions
Uterine AVMs though rare are potentially life
threatening lesions. Though hysterectomy was the
only treatment in the past, uterine artery embolization
and GnRH agonists are safe and effective method of
treatment when uterine function is to be preserved.
References
1. Bagga R, Verma P, Agarwal N, Suri V, Bapuraj JR.
Failed angiographic embolization in uterine arterio venous malformation: a case report and review
of literature. The Medscape Journal of Medicine.
2008; 10(1)12 ( www.medscape.com ).
2. Nicholson AA, Turnbull LW, Coady AM, Guthrie K.
Diagnosis and management of uterine arteriovenous malformations. Clin Radiol1999; 54(4)26569.
372
3.
Dubreuil G, Loubat E, Aneurysme crisoide de l
uterus and Ann Anat Patho. 1926; 3:697- 718
4.
Ghosh TK. Arteriovenous malformation of the
uterus and pelvis. Obstet Gynecol. 1986; 68:40-3
5.
Bottomoley JP, Whitehouse GH. Congenital arteriovenous
malformation
of
the
uterus
demonstrated by angiography. Acta Radiological
Diagnostica 1975; 16:43-48.
6.
Wiebe, ER Switzer P. Arteriovenous malformation
of uterus associated with medical abortion. Int J
obstet Gynecol.2007; 71: 155-8
7.
Fleming H, Ostor AQ, Pickel H, Forune DW. Artiovenous malformations of the uterus. Obstet gyneccol 1989; 73(2):209-14 .
8.
Morikawa M, Yamada T, Yamada H, Minakami H.
Effect of gonadotropin-releasing hormone agonist on a uterine arteriovenous malformation.
Obstet Gynecol. 2006; 108:751-753
How to cite this article: Ratna Bulusu, Prathibha S
D, Maheshwari, Vijay Kumar C R, Homeira Nishat.
Refractory Postpartum Haemorrhage - A Case Report.
J Clin Biomed Sci 2014; 4(4):370-72.
Conflict of interest: The authors claim to have no
conflict of interests in the context of this work.
J Clin Biomed Sci 2014; 4(4):370-72
Vous aimerez peut-être aussi
- Case Report: Postpartum Uterine Wound Dehiscence Leading To Secondary PPH: Unusual SequelaeDocument4 pagesCase Report: Postpartum Uterine Wound Dehiscence Leading To Secondary PPH: Unusual SequelaemelisaberlianPas encore d'évaluation
- Minakshi S. Neglected Puerperal Inversion of The Uterus Ignorance Makes Acute A Chronic FormDocument4 pagesMinakshi S. Neglected Puerperal Inversion of The Uterus Ignorance Makes Acute A Chronic FormJulius Albert SPas encore d'évaluation
- Failure of Coil Embolization in Secondary Postpartum Hemorrhage A Case ReportDocument7 pagesFailure of Coil Embolization in Secondary Postpartum Hemorrhage A Case ReportInternational Journal of Innovative Science and Research TechnologyPas encore d'évaluation
- Medip, IJRCOG-10243 CDocument4 pagesMedip, IJRCOG-10243 CRizki FebriyaniPas encore d'évaluation
- Uterine Inversion: A Life-Threatening Obstetric Emergency: Dawn R. Hostetler, MD, and Michael Bosworth, DODocument4 pagesUterine Inversion: A Life-Threatening Obstetric Emergency: Dawn R. Hostetler, MD, and Michael Bosworth, DOAndi Farras WatyPas encore d'évaluation
- A Rare Case of Abnormal Uterine Bleeding Caused by Cavernous Hemangioma: A Case ReportDocument3 pagesA Rare Case of Abnormal Uterine Bleeding Caused by Cavernous Hemangioma: A Case ReportprincessismaPas encore d'évaluation
- What Is The Recurrence Rate of Postmenopausal Bleeding in Women Who Have A Thin Endometrium During A First Episode of Postmenopausal Bleeding?Document6 pagesWhat Is The Recurrence Rate of Postmenopausal Bleeding in Women Who Have A Thin Endometrium During A First Episode of Postmenopausal Bleeding?dwiagusyuliantoPas encore d'évaluation
- Conservative Management of Placenta Accreta in A Multiparous WomanDocument10 pagesConservative Management of Placenta Accreta in A Multiparous WomanRobel Mae Lagos MontañoPas encore d'évaluation
- Cme Reviewarticle: Cesarean Scar Ectopic Pregnancy: Current Management StrategiesDocument10 pagesCme Reviewarticle: Cesarean Scar Ectopic Pregnancy: Current Management StrategiesDinorah MarcelaPas encore d'évaluation
- Barel 2019Document3 pagesBarel 2019Mariana González DíazPas encore d'évaluation
- Ectopic Pregnancy in Uncommon SitesDocument10 pagesEctopic Pregnancy in Uncommon SitesrezachandraPas encore d'évaluation
- Management of Severe Postpartum Haemorrhage by Uterine Artery EmbolizationDocument4 pagesManagement of Severe Postpartum Haemorrhage by Uterine Artery EmbolizationAndi Tri SutrisnoPas encore d'évaluation
- Retroperitoneal Hemorrhage Following Ultrasound-Guided Transvaginal Oocyte Retrieval: A Case ReportDocument4 pagesRetroperitoneal Hemorrhage Following Ultrasound-Guided Transvaginal Oocyte Retrieval: A Case ReportasclepiuspdfsPas encore d'évaluation
- Ectopic Abdominal Pregnancies: About 2 CasesDocument10 pagesEctopic Abdominal Pregnancies: About 2 CasesIJAR JOURNALPas encore d'évaluation
- Acquired Hemophilia As A Cause of Primary Postpartum HemorrhageDocument4 pagesAcquired Hemophilia As A Cause of Primary Postpartum HemorrhagedrpiratheepanPas encore d'évaluation
- Transvaginal Sonography Versus Hysteroscopy in Evaluation of Abnormal Uterine BleedingDocument6 pagesTransvaginal Sonography Versus Hysteroscopy in Evaluation of Abnormal Uterine BleedingKoko AgungPas encore d'évaluation
- Successful Medical Management of Uterine ArterioveDocument4 pagesSuccessful Medical Management of Uterine ArterioveRizki FebriyaniPas encore d'évaluation
- Leong Et Al-2004-BJOG: An International Journal of Obstetrics & GynaecologyDocument2 pagesLeong Et Al-2004-BJOG: An International Journal of Obstetrics & GynaecologyAngie MandeoyaPas encore d'évaluation
- Abnormal Uterine BleedingDocument22 pagesAbnormal Uterine BleedingAde JuandaPas encore d'évaluation
- Surgical Outcome of Genito Urinary Fistula - RayazDocument3 pagesSurgical Outcome of Genito Urinary Fistula - RayazRiaz Ahmed ChaudhryPas encore d'évaluation
- UC Irvine: Clinical Practice and Cases in Emergency MedicineDocument6 pagesUC Irvine: Clinical Practice and Cases in Emergency MedicinePatrick NunsioPas encore d'évaluation
- Circ PlacentDocument7 pagesCirc PlacentnicoavilaPas encore d'évaluation
- Spontaneous Rupture of Choledochal Cyst During Pregnancy: A Case ReportDocument3 pagesSpontaneous Rupture of Choledochal Cyst During Pregnancy: A Case ReportInternational Organization of Scientific Research (IOSR)Pas encore d'évaluation
- Management of AUB in A Bicornuate Uterus - Endometrial Ablation in A CompDocument1 pageManagement of AUB in A Bicornuate Uterus - Endometrial Ablation in A Comptipu42Pas encore d'évaluation
- History: Chief Complaint: History of Present Illness: Patient Is A 59 Year Old G6 P1051 Woman Who Is An Inmate That WasDocument9 pagesHistory: Chief Complaint: History of Present Illness: Patient Is A 59 Year Old G6 P1051 Woman Who Is An Inmate That WasRoberto RamosPas encore d'évaluation
- Transvaginal Removal of Ectopic Pregnancy Tissue and Repair of Uterine Defect For Caesarean Scar PregnancyDocument4 pagesTransvaginal Removal of Ectopic Pregnancy Tissue and Repair of Uterine Defect For Caesarean Scar PregnancyGladstone AsadPas encore d'évaluation
- Cesarean Scar Ectopic Pregnancy Case ReportDocument6 pagesCesarean Scar Ectopic Pregnancy Case ReportMominah MayamPas encore d'évaluation
- A Reading On HEMATOMA: Delivery Room Nursing RotationDocument7 pagesA Reading On HEMATOMA: Delivery Room Nursing RotationJulianePas encore d'évaluation
- Uterine Fibroid EmbolizationDocument8 pagesUterine Fibroid EmbolizationAlexandre Campos Moraes AmatoPas encore d'évaluation
- Uterine AtonyDocument4 pagesUterine AtonyJohn Cenas100% (1)
- Preservational Procedure of Cervical Pregnancy - 201Document1 pagePreservational Procedure of Cervical Pregnancy - 201online videoPas encore d'évaluation
- Hematometra in Uterus Didelphys With Right Hemivagina and Right Renal AgenesisDocument3 pagesHematometra in Uterus Didelphys With Right Hemivagina and Right Renal AgenesisDexter BluesPas encore d'évaluation
- PlasentaDocument4 pagesPlasentaLois YunikePas encore d'évaluation
- Management Dilemma in Case of Abdominal Pregnancy: A Case ReportDocument5 pagesManagement Dilemma in Case of Abdominal Pregnancy: A Case ReportDivika ShilvanaPas encore d'évaluation
- Anesthetic Management of Hepatitis C Positive Patient With Portal Hypertension For Cesarean Section - A Case ReportDocument5 pagesAnesthetic Management of Hepatitis C Positive Patient With Portal Hypertension For Cesarean Section - A Case ReportFendy PrasetyoPas encore d'évaluation
- Blighted Ovum: A Case ReportDocument2 pagesBlighted Ovum: A Case Reportakhmad ikhwanPas encore d'évaluation
- CORDOCENTESISDocument4 pagesCORDOCENTESISDaily DosePas encore d'évaluation
- Post Hysteroscopic Progesterone Hormone Therapy in The Treatment of Endometrial PolypsDocument5 pagesPost Hysteroscopic Progesterone Hormone Therapy in The Treatment of Endometrial PolypsherryPas encore d'évaluation
- Three-Dimensional Sonographic Findings of A Cervical PregnancyDocument4 pagesThree-Dimensional Sonographic Findings of A Cervical PregnancyEdwin AtencioPas encore d'évaluation
- A Case Study On Successful Ayurvedic Management of Heamorrhagic Ovarian CystDocument4 pagesA Case Study On Successful Ayurvedic Management of Heamorrhagic Ovarian CystEditor IJTSRDPas encore d'évaluation
- Rare Peritoneal Tumour Presenting As Uterine Fibroid: Janu Mangala Kanthi, Sarala Sreedhar, Indu R. NairDocument3 pagesRare Peritoneal Tumour Presenting As Uterine Fibroid: Janu Mangala Kanthi, Sarala Sreedhar, Indu R. NairRezki WidiansyahPas encore d'évaluation
- Van Wyk Grumbach Syndrome The Importance of Thyroi 2024 International JournDocument5 pagesVan Wyk Grumbach Syndrome The Importance of Thyroi 2024 International JournRonald QuezadaPas encore d'évaluation
- Surgical Treatment of Cesarean Scar Ectopic PregnancyDocument7 pagesSurgical Treatment of Cesarean Scar Ectopic PregnancyIndRa KaBhuomPas encore d'évaluation
- OGIJ 06 00208hematometra PDFDocument4 pagesOGIJ 06 00208hematometra PDFMarthin ArdoPas encore d'évaluation
- Medicine: Intrauterine Device Found in An Ovarian TumorDocument5 pagesMedicine: Intrauterine Device Found in An Ovarian TumorRezky amalia basirPas encore d'évaluation
- Placenta Increta Causing Um in The 26th Week of Pregnancy 2Document3 pagesPlacenta Increta Causing Um in The 26th Week of Pregnancy 2Kester ApostolPas encore d'évaluation
- Uterine Rupture in Nulliparous Woman Without Risk Factors: A Case Report and Literature ReviewDocument6 pagesUterine Rupture in Nulliparous Woman Without Risk Factors: A Case Report and Literature ReviewBOHR International Journal on GynaecologyPas encore d'évaluation
- Artigo 2 Sexta 31 MarDocument9 pagesArtigo 2 Sexta 31 MarabigailgomesdefrancaPas encore d'évaluation
- Yan 2007Document3 pagesYan 2007Agustin LindaPas encore d'évaluation
- P ('t':3) Var B Location Settimeout (Function (If (Typeof Window - Iframe 'Undefined') (B.href B.href ) ), 15000)Document4 pagesP ('t':3) Var B Location Settimeout (Function (If (Typeof Window - Iframe 'Undefined') (B.href B.href ) ), 15000)Fhiserra Kusuma PrimadhaniPas encore d'évaluation
- Imafuku 2019Document5 pagesImafuku 2019Rizki FebriyaniPas encore d'évaluation
- A Rare Case of Puerperal Uterine Inversion and Literature ReviewDocument3 pagesA Rare Case of Puerperal Uterine Inversion and Literature ReviewIJAR JOURNALPas encore d'évaluation
- 1 Sttri 3Document6 pages1 Sttri 3parkfishyPas encore d'évaluation
- Uterine VaricesDocument3 pagesUterine VaricesCindy AuliaPas encore d'évaluation
- Omental Pregnancy: Report Case and Literature ReviewDocument5 pagesOmental Pregnancy: Report Case and Literature ReviewIJAR JOURNALPas encore d'évaluation
- Use of Anti-D Immunoglobulin in The Treatment of Threatened Miscarriage in The Accident and Emergency DepartmentDocument4 pagesUse of Anti-D Immunoglobulin in The Treatment of Threatened Miscarriage in The Accident and Emergency DepartmentSabrine DwigintPas encore d'évaluation
- Ar11feb 13Document2 pagesAr11feb 13Jenny ConsignadoPas encore d'évaluation
- Evidence-Based Obstetric AnesthesiaD'EverandEvidence-Based Obstetric AnesthesiaStephen H. HalpernPas encore d'évaluation
- Pituitary Tumors: A Clinical CasebookD'EverandPituitary Tumors: A Clinical CasebookLisa B. NachtigallPas encore d'évaluation
- Management of Occult GI Bleeding: A Clinical GuideD'EverandManagement of Occult GI Bleeding: A Clinical GuideMicheal TadrosPas encore d'évaluation
- Nefroithiasis BilateralDocument3 pagesNefroithiasis BilateralSUSPAPas encore d'évaluation
- Wa000Document6 pagesWa000SUSPAPas encore d'évaluation
- ITC Nephrolithiasis - FullDocument16 pagesITC Nephrolithiasis - FullSUSPAPas encore d'évaluation
- Fundamentals ofDocument23 pagesFundamentals ofSUSPAPas encore d'évaluation
- 10 1 1 322 7265Document7 pages10 1 1 322 7265SUSPAPas encore d'évaluation
- 197.fullDocument13 pages197.fullSUSPAPas encore d'évaluation
- Nephrotic SyndromeDocument15 pagesNephrotic SyndromeSUSPAPas encore d'évaluation
- Tuberculous Spondylitis: What Every Radiologist Should Know: Poster No.: Congress: Type: Authors: KeywordsDocument15 pagesTuberculous Spondylitis: What Every Radiologist Should Know: Poster No.: Congress: Type: Authors: KeywordsArief RachmanPas encore d'évaluation
- Opth 8 015Document7 pagesOpth 8 015SUSPAPas encore d'évaluation
- Buku Bedah UmumDocument126 pagesBuku Bedah UmumSilvia Kamal100% (7)
- Journal Mata SuspaDocument6 pagesJournal Mata SuspaSUSPAPas encore d'évaluation
- 2015 Article 36Document8 pages2015 Article 36SUSPAPas encore d'évaluation
- 2015 Article 35Document4 pages2015 Article 35SUSPAPas encore d'évaluation
- PowerPoint Maxillofacial Trauma EnglishDocument67 pagesPowerPoint Maxillofacial Trauma EnglishRizki Octo Kurniawan100% (1)
- Quick Start Guide for SanDisk SecureAccessDocument21 pagesQuick Start Guide for SanDisk SecureAccessbijan034567Pas encore d'évaluation
- Role of Fats in Periodontal DiseaseDocument9 pagesRole of Fats in Periodontal DiseaseandrealezamaPas encore d'évaluation
- Table of Contents:: Mariam Tariq L1F07BBAM0060 Nabeela Sattar L1F07BBAM2159 Sana Akbar L1F07BBAM2085Document9 pagesTable of Contents:: Mariam Tariq L1F07BBAM0060 Nabeela Sattar L1F07BBAM2159 Sana Akbar L1F07BBAM2085Raheem AhmedPas encore d'évaluation
- Isak 1 2 ViennaDocument6 pagesIsak 1 2 Viennanifej15595Pas encore d'évaluation
- Stunting in IndonesiaDocument218 pagesStunting in IndonesiaPratamaOktaRickyPas encore d'évaluation
- AyurvasthraDocument7 pagesAyurvasthraVineesha VikramPas encore d'évaluation
- Board 4-CHNDocument30 pagesBoard 4-CHNKira100% (22)
- Vogt Koyanagi Harada SyndromeDocument9 pagesVogt Koyanagi Harada SyndromeBianca PavelPas encore d'évaluation
- 2015 EHS Challanges Enablon Reportv9Document15 pages2015 EHS Challanges Enablon Reportv9Anonymous sfY8T3q0100% (1)
- Mynvax PDF File Contained StandardsDocument1 pageMynvax PDF File Contained StandardsSelvabala904260Pas encore d'évaluation
- Interpretation: L23 - FPSC Malviya Nagar1 A-88 Shivanand Marg, Malviyanagar JaipurDocument4 pagesInterpretation: L23 - FPSC Malviya Nagar1 A-88 Shivanand Marg, Malviyanagar Jaipurmahima goyalPas encore d'évaluation
- Interpreting PDX Dot BlotsDocument2 pagesInterpreting PDX Dot BlotsSpy CameraPas encore d'évaluation
- DelegationDocument24 pagesDelegationJP FernandezPas encore d'évaluation
- Infectious DiseasesDocument4 pagesInfectious Diseasesapi-484776271Pas encore d'évaluation
- Ohsas 18001Document36 pagesOhsas 18001santhurkc67% (3)
- 1 PBDocument6 pages1 PBmutiakusumaPas encore d'évaluation
- Lecture No 03 Functional Foods NutraceuticalDocument15 pagesLecture No 03 Functional Foods Nutraceuticalmaryam khanPas encore d'évaluation
- Hemodialysis Prescription and TreatmentDocument12 pagesHemodialysis Prescription and TreatmentkidneymastersPas encore d'évaluation
- NEWCROSS Site Survey - Rev1Document37 pagesNEWCROSS Site Survey - Rev1eke23Pas encore d'évaluation
- Brady J. - Environmental Management in Organizations. The IEMA Handbook (2005)Document459 pagesBrady J. - Environmental Management in Organizations. The IEMA Handbook (2005)Wan Naqib Hamidon100% (5)
- Minitek Indore Profile 2Document9 pagesMinitek Indore Profile 2kunal agiwalePas encore d'évaluation
- Health Declaration Form: (Buong Pangalan) (Petsa) (Oras) (Kasa/ukuyang Tirahan) : (Numero NG Telepono)Document1 pageHealth Declaration Form: (Buong Pangalan) (Petsa) (Oras) (Kasa/ukuyang Tirahan) : (Numero NG Telepono)Reichmond LegaspiPas encore d'évaluation
- Massive Transfusion ProtocolDocument5 pagesMassive Transfusion ProtocolArlette Araceli Barbosa IbarraPas encore d'évaluation
- Digestive System Parts PacketDocument2 pagesDigestive System Parts PacketRusherPas encore d'évaluation
- Truvivity by NutriliteDocument10 pagesTruvivity by Nutriliteโยอันนา ยุนอา แคทเธอรีน เอี่ยมสุวรรณPas encore d'évaluation
- Maybank MNC CompleteDocument37 pagesMaybank MNC CompleteRobbie Ravin0% (1)
- Material Safety Data Sheet: Section 1 - Product InformationDocument2 pagesMaterial Safety Data Sheet: Section 1 - Product Informationmohamed AdelPas encore d'évaluation
- Improving Workplace Safety Behavioral Based Safety: ThroughDocument32 pagesImproving Workplace Safety Behavioral Based Safety: ThroughYursPas encore d'évaluation
- Amniotic MembraneDocument8 pagesAmniotic Membraneapi-481789048Pas encore d'évaluation
- Essential workout guideDocument31 pagesEssential workout guidejo nemesisPas encore d'évaluation
- SITXWHS001 Student Assessment v2.1Document16 pagesSITXWHS001 Student Assessment v2.1Sukhpreet KaurPas encore d'évaluation