Académique Documents
Professionnel Documents
Culture Documents
Background: This MRI Demonstrates Spinal Epidural Hematoma
Transféré par
A Novita Dewi AryantiTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Background: This MRI Demonstrates Spinal Epidural Hematoma
Transféré par
A Novita Dewi AryantiDroits d'auteur :
Formats disponibles
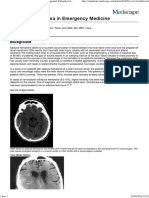
Background
Epidural hematoma (ie, accumulation of blood in the potential space between dura and bone) may be
intracranial (EDH) or spinal (SEDH) (see the image below). Intracranial epidural hematoma occurs in
approximately 2% of patients with head injuries and 5-15% of patients with fatal head injuries. Intracranial
epidural hematoma is considered to be the most serious complication of head injury, requiring immediate
diagnosis and surgical intervention. Intracranial epidural hematoma may be acute (58%), subacute (31%), or
chronic (11%). Spinal epidural hematoma may also be traumatic, though it may occur spontaneously.
This MRI demonstrates spinal epidural hematoma.
Pathophysiology
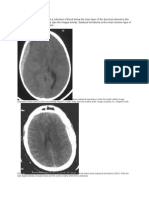
Epidural hematoma usually results from a brief linear contact force to the calvaria that causes separation of the
periosteal dura from bone and disruption of interposed vessels due to shearing stress. Skull fractures occur in
85-95% of adult cases, but they are much less common in children because of the plasticity of the immature
calvaria. Arterial or venous structures may be compromised, causing rapid expansion of the hematoma;
however, chronic or delayed manifestations may occur when venous sources are involved. Extension of the
hematoma usually is limited by suture lines owing to the tight attachment of the dura at these locations. Recent
analyses have revealed that epidural hematomas may actually traverse suture lines in a minority of cases. [1]
The temporoparietal region and the middle meningeal artery are involved most commonly (66%), although the
anterior ethmoidal artery may be involved in frontal injuries, the transverse or sigmoid sinus in occipital injuries,
and the superior sagittal sinus in trauma to the vertex. Bilateral epidural hematomas account for 2-10% of all
acute epidural hematomas in adults but are exceedingly rare in children. Posterior fossa epidural hematomas
represent 5% of all cases of epidural hematomas.
Spinal epidural hematoma may be spontaneous or may follow minor trauma, such as lumbar puncture or
epidural anesthesia. Spontaneous spinal epidural hematoma may be associated with anticoagulation,
thrombolysis, blood dyscrasias, coagulopathies, thrombocytopenia, neoplasms, or vascular malformations. The
peridural venous plexus usually is involved, though arterial sources of hemorrhage also occur. The dorsal
aspect of the thoracic or lumbar region is involved most commonly, with expansion limited to a few vertebral
levels.
Epidemiology
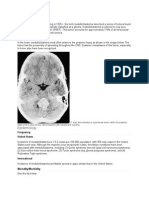
Frequency
United States
Epidural hematoma complicates 2% of cases of head trauma (approximately 40,000 cases per year). Spinal
epidural hematoma affects 1 per 1,000,000 people annually. Alcohol and other forms of intoxication have been
associated with a higher incidence of epidural hematoma.
International
International frequency is unknown, though it is likely to parallel the frequency in the United States.
Mortality/Morbidity
Mortality rate associated with epidural hematoma has been estimated to be 5-50%.
The level of consciousness prior to surgery has been correlated with mortality rate: 0% for awake
patients, 9% for obtunded patients, and 20% for comatose patients.
Bilateral intracranial epidural hematoma has a mortality rate of 15-20%.
Posterior fossa epidural hematoma has a mortality rate of 26%.
Race
No racial predilection has been reported.
Sex
Intracranial and spinal epidural hematomas are more frequent in men, with a male-to-female ratio of 4:1.
Age
Intracranial epidural hematoma is rare in individuals younger than 2 years.
Intracranial epidural hematoma is also rare in individuals older than 60 years because the dura is
tightly adherent to the calvaria.
Spinal epidural hematoma has a bimodal distribution with peaks during childhood and during the fifth
and sixth decades of life. Increasing age has been noted as a risk factor for postoperative spinal epidural
hematoma.
http://emedicine.medscape.com/article/1137065-overview#showall
Vous aimerez peut-être aussi
- Genetics NotesDocument28 pagesGenetics NotesjasPas encore d'évaluation
- Thyroid PathologyDocument9 pagesThyroid PathologyNada MuchPas encore d'évaluation
- A Serum Autoantibody Marker of Neuromyelitis Optica: Distinction From Multiple SclerosisDocument7 pagesA Serum Autoantibody Marker of Neuromyelitis Optica: Distinction From Multiple SclerosistiaraleshaPas encore d'évaluation
- Neuroradiology Head TraumaDocument21 pagesNeuroradiology Head TraumaNyoman Marsel Rama GranditaPas encore d'évaluation
- UW Path NoteDocument218 pagesUW Path NoteSophia Yin100% (4)
- Subdural HematomaDocument8 pagesSubdural HematomaaaronmanullangPas encore d'évaluation
- A Subdural HematomaDocument12 pagesA Subdural HematomaGina Irene IshakPas encore d'évaluation
- Method SujokDocument4 pagesMethod Sujokbhupatin100% (6)
- Epidural Hematoma Case ReportDocument48 pagesEpidural Hematoma Case ReportJansept Bruce Guinto67% (6)
- Intracerebral Haemorrhage: Disease PrimersDocument18 pagesIntracerebral Haemorrhage: Disease PrimersMarlon VillanuevaPas encore d'évaluation
- Hyperemesis Gravidarum: Is An Extreme, Persistent Nausea and Vomiting During PregnancyDocument1 pageHyperemesis Gravidarum: Is An Extreme, Persistent Nausea and Vomiting During PregnancyDarren RobertoPas encore d'évaluation
- Chronic Subdural HematomaDocument21 pagesChronic Subdural Hematomamarc_caronan100% (2)
- CA Coil ClipDocument12 pagesCA Coil ClipArdiansyah P PratamaPas encore d'évaluation
- Management of Unruptured Intracranial Aneurysms: Neurology Clinical PracticeDocument10 pagesManagement of Unruptured Intracranial Aneurysms: Neurology Clinical PracticeEddwwin Varillas ReyesPas encore d'évaluation
- Community Mobilisation and Participation in HealthDocument33 pagesCommunity Mobilisation and Participation in HealthMayom MabuongPas encore d'évaluation
- Stress Level and Coping Strategies of Bs Criminology-1 Students in Perpetual Help College of Pangasinan During PandemicDocument38 pagesStress Level and Coping Strategies of Bs Criminology-1 Students in Perpetual Help College of Pangasinan During PandemicJohn Paul Sarmiento100% (1)
- Euthanasia ArticleDocument12 pagesEuthanasia ArticleLubna Tanweer100% (1)
- EDH TesDocument2 pagesEDH TesAyu SofianaPas encore d'évaluation
- Daniel D Price, MD Director of International Ultrasound, Department ofDocument3 pagesDaniel D Price, MD Director of International Ultrasound, Department ofPutri Swandayani NofendyPas encore d'évaluation
- Index - : Professor Yasser MetwallyDocument11 pagesIndex - : Professor Yasser MetwallyDrhikmatullah SheraniPas encore d'évaluation
- Epidural Hematoma in Emergency Medicine: BackgroundDocument3 pagesEpidural Hematoma in Emergency Medicine: BackgroundMercy HasanPas encore d'évaluation
- Hematoma PathophysiologyDocument1 pageHematoma PathophysiologyRein VillanuevaPas encore d'évaluation
- Epidural Hematoma: Continuing Education ActivityDocument16 pagesEpidural Hematoma: Continuing Education ActivityIka AriandanaPas encore d'évaluation
- Cerebrovascular Disease Residents 2Document29 pagesCerebrovascular Disease Residents 2emilio9fernandez9gatPas encore d'évaluation
- Epidural Hematomas: BackgroundDocument5 pagesEpidural Hematomas: BackgroundDina MaulidaPas encore d'évaluation
- Traumatic Brain InjuryDocument48 pagesTraumatic Brain InjuryAtanasoaei OanaPas encore d'évaluation
- Aneurysmal Subarachnoid Hemorrhage.6Document19 pagesAneurysmal Subarachnoid Hemorrhage.6Aldy Setiawan PutraPas encore d'évaluation
- Frequency: Head TraumaDocument2 pagesFrequency: Head TraumaA Nurfatiha JafarPas encore d'évaluation
- Types of Brain HemorrhageDocument2 pagesTypes of Brain HemorrhageRichie Marie BajaPas encore d'évaluation
- Cerebral Venous Sinus ThrombosisDocument34 pagesCerebral Venous Sinus ThrombosisNeurologia homicPas encore d'évaluation
- Brainstem StrokeDocument22 pagesBrainstem StrokeAlin CiubotaruPas encore d'évaluation
- Acute Flaccid ParalysisDocument4 pagesAcute Flaccid Paralysismadimadi11Pas encore d'évaluation
- Objectives:: Access Free Multiple Choice Questions On This TopicDocument7 pagesObjectives:: Access Free Multiple Choice Questions On This TopicVierynaPas encore d'évaluation
- Critical Care Management of Increased Intracranial PressureDocument8 pagesCritical Care Management of Increased Intracranial Pressurep_sempoiPas encore d'évaluation
- Corelation SDH Brain AtrophyDocument16 pagesCorelation SDH Brain Atrophyselubung linePas encore d'évaluation
- A Subdural HematomaDocument2 pagesA Subdural HematomaMohammadAwitPas encore d'évaluation
- EPIDURAL HEMATOM Kel 3Document15 pagesEPIDURAL HEMATOM Kel 3Rizka Desti AyuniPas encore d'évaluation
- Clinical Manifestations, Prevention and Treatment of Stroke in WomenDocument6 pagesClinical Manifestations, Prevention and Treatment of Stroke in WomenCentral Asian StudiesPas encore d'évaluation
- A Subdural HematomaDocument2 pagesA Subdural HematomaMohammadAwitPas encore d'évaluation
- Ich Magistris, 2013Document8 pagesIch Magistris, 2013ignasachyntiaPas encore d'évaluation
- Cerebrovascular Disease Residents 1Document20 pagesCerebrovascular Disease Residents 1emilio9fernandez9gatPas encore d'évaluation
- Extracranial Carotid Artery Aneurysm - UpToDateDocument25 pagesExtracranial Carotid Artery Aneurysm - UpToDateDiego RodriguesPas encore d'évaluation
- Syncope in Adults - Epidemiology, Pathogenesis, and EtiologiesDocument28 pagesSyncope in Adults - Epidemiology, Pathogenesis, and EtiologiesRaúl MartínezPas encore d'évaluation
- Intracranial Aneurysms and SAH: Philippe Younes MD Neurosurgeon Head of Neuroscience Department BMCDocument37 pagesIntracranial Aneurysms and SAH: Philippe Younes MD Neurosurgeon Head of Neuroscience Department BMCHussein TarhiniPas encore d'évaluation
- Moyamoya Epidemiology, Presentation, and DiagnosisDocument9 pagesMoyamoya Epidemiology, Presentation, and DiagnosisshiloinPas encore d'évaluation
- Birth TraumaDocument8 pagesBirth Traumaسحر احمدPas encore d'évaluation
- Continuing Education Activity: Hemorrhagic StrokeDocument18 pagesContinuing Education Activity: Hemorrhagic StrokeHandayaniPas encore d'évaluation
- Tema 1. - Neurotrauma Aproximación Genral y Estrategias de ResuscitaciónDocument17 pagesTema 1. - Neurotrauma Aproximación Genral y Estrategias de ResuscitaciónaniadPas encore d'évaluation
- Nej M 199701023360106Document13 pagesNej M 199701023360106AriefNugrohoPas encore d'évaluation
- Surgical Treatment of Chronic Subdural Hematoma CLDocument12 pagesSurgical Treatment of Chronic Subdural Hematoma CLNikola StevanovicPas encore d'évaluation
- Arch Dis Child 2008 Pappachan 890 8Document10 pagesArch Dis Child 2008 Pappachan 890 8chinocauPas encore d'évaluation
- Neuroradiology Traumatic HemorrhageDocument21 pagesNeuroradiology Traumatic HemorrhageKoni MamujuPas encore d'évaluation
- Stroke - Disease Management-1-19Document19 pagesStroke - Disease Management-1-19Ahsan kamalPas encore d'évaluation
- Pathophysiology: Subarachnoid HemorrhageDocument15 pagesPathophysiology: Subarachnoid HemorrhageLaura AstridPas encore d'évaluation
- Stroke Prevention and Treatment in Sickle Cell Disease: Robert J. Adams, MS, MDDocument4 pagesStroke Prevention and Treatment in Sickle Cell Disease: Robert J. Adams, MS, MDMeshaki MbarukaPas encore d'évaluation
- Aneurysmal Subarachnoid Hemorrhage: Review ArticleDocument10 pagesAneurysmal Subarachnoid Hemorrhage: Review ArticlekucingkucingPas encore d'évaluation
- Anesth Analg 2010 Elliott 1419 27Document9 pagesAnesth Analg 2010 Elliott 1419 27Darrel Allan MandiasPas encore d'évaluation
- Review Article: Ischemic Stroke in Infants and Children: Practical Management in EmergencyDocument8 pagesReview Article: Ischemic Stroke in Infants and Children: Practical Management in EmergencyEstela MachadoPas encore d'évaluation
- Cerebral Venous ThrombosisDocument19 pagesCerebral Venous ThrombosisgresiaPas encore d'évaluation
- WK II WikiDocument4 pagesWK II Wikiapi-174496267Pas encore d'évaluation
- Lapkas Dian and DamboDocument34 pagesLapkas Dian and DamboDian Primadia PutriPas encore d'évaluation
- Subarachnoid HemorrhageDocument3 pagesSubarachnoid Hemorrhagetenaj_purplePas encore d'évaluation
- Cerebral Venous Thrombosis From UptodateDocument20 pagesCerebral Venous Thrombosis From UptodatewbudyaPas encore d'évaluation
- Stroke ImagingDocument1 pageStroke ImagingRheeza ElhaqPas encore d'évaluation
- Background: Frequency United StatesDocument2 pagesBackground: Frequency United StatesMohammadAwitPas encore d'évaluation
- Heart Valve Disease: State of the ArtD'EverandHeart Valve Disease: State of the ArtJose ZamoranoPas encore d'évaluation
- Risk Factors For Developing Aortic Disease (Second Edition)D'EverandRisk Factors For Developing Aortic Disease (Second Edition)Pas encore d'évaluation
- NSG 461 - Disease Deep DiveDocument5 pagesNSG 461 - Disease Deep Diveapi-641353289100% (1)
- Fall Risk Assessment Form: Total Score - A Total Score of 10 or More Indicates A Resident "At Risk" For FallsDocument1 pageFall Risk Assessment Form: Total Score - A Total Score of 10 or More Indicates A Resident "At Risk" For FallswaheedmohsinPas encore d'évaluation
- Bilateral Atypical Optic Neuritis - Endi Pramudya LaksanaDocument12 pagesBilateral Atypical Optic Neuritis - Endi Pramudya LaksanaGufront MustofaPas encore d'évaluation
- Lexington Medical Center Heart Health InsertDocument12 pagesLexington Medical Center Heart Health InsertLexington Medical CenterPas encore d'évaluation
- Table Of: Insects and ArachnidsDocument9 pagesTable Of: Insects and ArachnidsSamuelPas encore d'évaluation
- Homocysteine and Markers of Coagulation and Endothelial Cell ActivationDocument7 pagesHomocysteine and Markers of Coagulation and Endothelial Cell ActivationMaya RustamPas encore d'évaluation
- Understanding Insomnia - Felson, SDocument4 pagesUnderstanding Insomnia - Felson, SRoxan PacsayPas encore d'évaluation
- Garner 1511222Document17 pagesGarner 1511222Bj LongPas encore d'évaluation
- Drug Study Lab, NCP - Bronchial AsthmaDocument6 pagesDrug Study Lab, NCP - Bronchial AsthmaRichelle Sandriel C. de CastroPas encore d'évaluation
- Gut Probe in A PillDocument12 pagesGut Probe in A PillLaya LastPas encore d'évaluation
- Patient - Carpal Tunnel ReleaseDocument2 pagesPatient - Carpal Tunnel Releaseapi-277825138Pas encore d'évaluation
- Kirsten WeirDocument3 pagesKirsten Weirapi-2819031830% (1)
- Renal Failure Cronic Group 6Document18 pagesRenal Failure Cronic Group 6Wiwi Hardiyanti100% (1)
- Critique PaperDocument3 pagesCritique PaperASHER BETHEL JUMAQUIOPas encore d'évaluation
- DTR Resume 2 0Document2 pagesDTR Resume 2 0api-380987816Pas encore d'évaluation
- Case Study Presentation: Chronic Obstructive Pulmonary Disease CopdDocument5 pagesCase Study Presentation: Chronic Obstructive Pulmonary Disease CopdHusaifah BaliwanPas encore d'évaluation
- Dr. Hasyim Kasim, HipertensiDocument50 pagesDr. Hasyim Kasim, HipertensiImaji Corp MakassarPas encore d'évaluation
- Nejm Pcsk9 StudyDocument10 pagesNejm Pcsk9 Studyherbertgur777Pas encore d'évaluation
- What Is Vitamin B12 Good For: Vitamins Vitamin B Niacin Folic Acid Vitamin B12Document75 pagesWhat Is Vitamin B12 Good For: Vitamins Vitamin B Niacin Folic Acid Vitamin B12Nanda SuchirPas encore d'évaluation
- Scolioza CongenitalaDocument20 pagesScolioza CongenitalaIulia Dulgheru100% (1)
- Vechur CowDocument2 pagesVechur CowkappygasPas encore d'évaluation
- Nail DisordersDocument123 pagesNail DisordersyaraamadoPas encore d'évaluation