Académique Documents
Professionnel Documents
Culture Documents
Copd 3 319
Transféré par
Romi AndriyanaTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Copd 3 319
Transféré par
Romi AndriyanaDroits d'auteur :
Formats disponibles
ORIGINAL RESEARCH
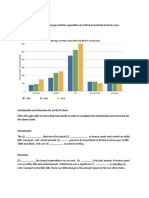
Antibiotics used in the ambulatory management
of acute COPD exacerbations
Marie-France
Beauchesne 1,2,3
Marcel Julien 2,4
Louis-Andr Julien 2,4
Dominique Piquette 4
Amlie Forget 2
Manon Labrecque 2,4
Lucie Blais 1,2,3
Faculty of Pharmacy, 4Faculty of
Medicine, University of Montral,
Montral, Qubec, Canada; 2 Hpital
du Sacr-Coeur de Montral, Gouin
Ouest, Montral, Qubec, Canada;
3
Endowment Pharmaceutical Chair
AstraZeneca in Respiratory Health,
Montral, Qubec, Canada
1
Study objectives: This study was conducted to describe the different antibiotics that are used
in the home management of chronic obstructive pulmonary disease (COPD) exacerbations and
to estimate the failure rates following the initiation of the antibiotic.
Methods: A cohort study was conducted. Patients enrolled in a COPD home management
program were included in the analysis. Failure rates were dened as an additional prescription
of an antibiotic, an emergency room visit, or a hospitalization for a COPD exacerbation in the
30 days following the initiation of the antibiotic.
Results: A total of 1180 episodes of antibiotic treatment were analyzed. Overall, 348 episodes
led to a failure (29.5%). The most frequently used antibiotics were cefuroxime (45.9%) and
ciprooxacin (21.1%).
Conclusion: This project demonstrates that a wide range of antibiotics were prescribed to our
population of COPD patients with a moderate to severe form of the disease. Many treatment
failures (about 30%) occurred in the 30-day period following the initiation of the home therapy
with an antibiotic. Clinicians should be aware of this high failure rate when managing mild
exacerbations of COPD at home.
Keywords: acute exacerbation of COPD, antibiotics, COPD
Introduction
Correspondence: Marie-France
Beauchesne
Pharmacy, Hpital du Sacr-Cur
de Montral, 5400 boul. Gouin ouest,
Montreal, Quebec, H4J 1C5, Canada
Tel +1 514 338 2222 2666
Fax +1 514 338 3200
Email marie-france.
beauchesne@umontreal.ca
Several trials have demonstrated that antibiotics are benecial over placebo for the
treatment of acute exacerbations of chronic obstructive pulmonary disease (COPD)
(Anthonisen et al 1987; Saint et al 1995; Ram et al 2006). COPD guidelines recommend the use of antibiotics when clinical signs of infection are apparent; for example,
increased sputum volume and purulence, and/or fever (GOLD 2007). Antimicrobial
choices can be based upon the local patterns of antibiotic sensitivity among the
most common responsible pathogens (GOLD 2007). Canadian guidelines recommend the use of amoxicillin, doxycycline, trimethoprim/sulfamethoxazole, second
or third-generation cephalosporins, or extended spectrum macrolides in the absence
of risk factors, whereas uoroquinolones or beta-lactam/beta-lactamase inhibitor
(amoxicillin/clavulanic acid) are suggested for patients who have an forced expiratory
volume in one second (FEV1) lower than 50% of the predicted, four or more COPD
exacerbations per year, ischemic heart disease, home oxygen use, chronic use of oral
corticosteroids, and/or antibiotherapy taken in the previous three months (ODonnell
et al 2007). The authors do however, specify that this is a level 3c recommendation
(consensus from expert groups based on clinical experience and poor evidence to
support a recommendation for or against use). Furthermore, it is also specied that
antibiotics for patients with no risk factors when combined with prednisone may sufce (ODonnell et al 2007).
Most patients included in our COPD home management program have the risk
factors associated with the use of second line antimicrobial agents (ie, for patients with
International Journal of COPD 2008:3(2) 319322
319
2008 Beauchesne et al, publisher and licensee Dove Medical Press Ltd. This is an Open Access
article which permits unrestricted noncommercial use, provided the original work is properly cited.
Beauchesne et al
risk factors), specied in the Canadian COPD guidelines,
but various antibiotics, including rst-line agents, are used.
Therefore, we sought to describe the type of antibiotics that
are used by COPD patients included in our home management program and to estimate the failure rate associated
with this therapy.
Methods
We conducted a retrospective cohort study to describe the
different antibiotics that are used for COPD patients included
in our home management program, and estimate the treatment failure rates. All patients participating in the COPD
home-management program of lHpital du Sacr-Coeur de
Montral (HSCM) were included in the analysis if they had
follow-up data for at least 12 months. This program follows
patients for whom COPD represents a chronic disease that
has an important impact on their quality of life and who are at
risk of severe exacerbations; for example, have had previous
exacerbations requiring acute care. Patient charts updated
at least every month by doctors, nurses, and pharmacists
were used for data collection. Cohort entry corresponded
to inclusion in the program (started in 1995) and follow-up
until exclusion from the program, death, or November 31st,
2004, whichever occurred rst. Antibiotics were initiated at
home for these patients when they reported at least two of
the following criteria: dyspnea, increased sputum production, increased sputum volume (Anthonisen et al 1987). The
selection of an appropriate antibiotic for the patients action
plan is at the physicians discretion and is not based upon
prespecied criteria with the exception of drug allergy or
intolerance. Usually, the action plan (antibiotic) is prescribed
for a year and rotation from one antibiotic to another over
the course of the year to treat subsequent exacerbations is
not done unless treatment fails. Microbiologic data is not
usually available to select the antibiotic; patients who begin
an exacerbation are managed by telephone communication
between the nurse and the patient. Usual treatment duration
is of 10 days (with the exception of azithromycin which in
most cases is prescribed for 5 days). An intravenous antibiotic regimen and a concomitant use of two antibiotics were
excluded from the analysis, since these cases are managed
differently (usual protocol is not followed for these cases at
our program). Patients included in this program are followed
by one of the respiratory physicians at HSCM with meetings
once or twice a year at the outpatient clinic.
Data collected included antibiotic treatments (number
and agents used), number of emergency room visits for
a COPD exacerbation, number of hospitalizations for a
320
COPD exacerbation, use of oral and inhaled corticosteroids,
use of bronchodilators (inhaled short and long-acting
bronchodilators, theophylline), FEV1, level of dyspnea
(based on the cardiac rhythm management dyspnea index;
scale 15, a higher score implies a higher level of dyspnea),
co-morbidities, age, sex, smoking status, home oxygen use,
hypercapnia, and level of autonomy (scale 16, a higher score
implies a better level of autonomy).
The main outcome was the type of antimicrobial agents
prescribed to the patients in the cohort. The secondary
outcome was treatment failure in the 30 days following the
initiation of the antibiotic. Treatment failure was considered
if one of the following events occurred in the 30-day period
following the initiation of the antibiotic: prescription of
the same antibiotic for home management once the initial
treatment has been completed; use of a different antimicrobial agent for home management of a COPD exacerbation
(change in the antibiotic initially prescribed before treatment
completion or upon treatment completion); emergency room
visit for a COPD exacerbation (as soon as 1 day following
treatment initiation); and hospitalization for a COPD exacerbation (as soon as 1 day following treatment initiation).
These were described separately and then, treatment failure
was assessed based on the occurrence of one of these four
events; if more than one occurred in the 30-day period, only
one treatment failure was calculated. Furthermore, a delay
of at least 30 days between two exacerbations in the same
patient was mandatory to consider the occurrence of a new
COPD exacerbation requiring antibiotic therapy. The conduct of this project was approved by the ethics committee
of our institution.
Statistical analysis
Descriptive statistics proportions and standard deviation
were calculated to describe the type of antibiotics
prescribed.
Results
The initial cohort included 2288 episodes of oral antibiotic
treatments received by 152 COPD patients included in the
home management program between 1995 and 2004. We
excluded 972 antibiotic treatments that were preceded in the
30 days by a COPD exacerbation (hospitalization, emergency
room visit, another antibiotic therapy), and 136 episodes
for which complete clinical data of the patients were not
available. Therefore, a total of 1180 episodes of antibiotic
treatment received by 152 patients were analyzed. The distribution of the characteristics of the patients at cohort entry
International Journal of COPD 2008:3(2)
Antibiotics in AECOPD
and antibiotic choices are found in Table 1 and Table 2. All
patients included in our cohort had an FEV1 lower than 50%
at cohort entry, and therefore were in the category with
risk factors based on the Canadian guidelines. The most
frequently used antibiotics were cefuroxime (45.9%) and
ciprooxacin (21.1%). A total 473 of the 1180 antibiotic
treatments (40.0%) were combined with prednisone.
Overall, 348 of the 1180 episodes led to a treatment failure (29.5%), including 103 hospitalizations for a COPD exacerbation, 29 emergency room visits, 44 repeated treatments
with the same antibiotic, and 172 repeated treatments with
a different antibiotic (Table 3). The average time between
Table 1 Characteristics of the patients at their entry in the COPD
home management program
Characteristics (n = 152)
N (%)
Gender: Male
Mean age:
4964 years old
6574 years old
75 years old
BMI:
20
2029
30
Smoking status:
Past history of smoking
Smoker
No history of smoking
Number of co-morbiditites:
2
2
Dyspnea index (scale of 1-5)
12
3
45
Level of autonomy (scale 16)
13
46
Home oxygen
Use of a short-acting bronchodilator
(albuterol and ipratropium)
Use of a long-acting beta-2 agonist
Use of an inhaled corticosteroid
Use of theophylline
Continuous use of oral corticosteroids
FEV1
76 (50.0)
Annual rate of exacerbations
31 (20.4)
60 (39.5)
61 (40.1)
37 (24.3)
92 (60.5)
23 (15.1)
120 (79.0)
26 (17.1)
6 (4.0)
88 (57.9)
64 (42.1)
19 (12.5)
29 (19.1)
104 (68.4)
78 (55.3)
63 (44.7)
70 (46.4)
152 (100)
87 (57.2)
132 (86.8)
56 (36.8)
22 (14.6)
Mean ( SD)
32.3% predicted (9.1)
2.9 (2.3)
Notes: The mean number of pack-years of smoking was unknown; Based on the CRM
dyspnea index: a higher score implies a higher level of dyspnea; Questionnaire developed
for our program (not validated): a higher score implies a better level of autonomy. The
six-minute walk distance is unknown.
Abbreviations: BMI, body mass index; FEV1, forced expiratory volume in one second;
SD, standard deviation.
International Journal of COPD 2008:3(2)
Table 2 Antibiotics used to treat acute exacerbations of COPD
at home
Antibiotics used (n = 1180 treatments)
N (%)
Cefuroxime
Ciprofloxacin
Levofloxacin
Azithromycin
Amoxicillin
Moxifloxacin
Trimethoprim-sulfamethoxazole
Gatifloxacin
Amoxicillin-clavulanic acid
Others (ampicillin, cephalexin, cefaclor, cefixime,
cefprozil, clindamycin, cloxacillin,
erythromycin, ofloxacin, penicillin,
pivampicillin, trovafloxacin)
542 (45.9)
249 (21.1)
73 (6.2)
56 (4.8)
49 (4.2)
48 (4.1)
41 (3.5)
24 (2.0)
20 (1.7)
37 (3.1)
the initiation of the antibiotic and the treatment failure was
15.3 days (median of 14 days).
A total of 418 of the 1180 treatments prescribed (35.4%)
were antibiotics recommended for patients with risk factors
according to the Canadian COPD guidelines (ie, amoxicillin/clavulanic acid or uroquinolones). The failure rates
associated with the use of an antibiotic for patients with risk
factors was of 32.8% while it was of 27.7% for antibiotics
in the category of patients without risk factors. The risk of
having a treatment failure was slightly higher when an antibiotic for patients with risk factors was prescribed (data not
shown, available upon request).
Discussion
Overall, our failure rate was greater than the ones reported
in the literature that vary from 12% to 21% (Adams et al
2000; Dewan et al 2000; Miravitlles et al 2001). Potential
explanations for this difference are our studys inclusion of
patients with a more severe form of the disease, and the use
of a different denition of failure (Adams et al 2000; Dewan
et al 2000; Miravitlles et al 2001). Furthermore, about 65%
of patients received an antibiotic for patients with no risk
factors, while they were considered at risk based on their
characteristics (such as FEV1). A deciency in guideline
conformity and under use with regard to COPD treatment has
been previously reported (Jans et al 1998; Roche et al 2001;
Choi et al 2004; Brand et al 2005; Fritsch et al 2005; Boulet
et al 2006; Glaab et al 2006a, 2006b). However, antibiotic
treatment recommendations in the Canadian COPD guidelines are not based on a high level of evidence.
The main strength of our study is that we collected
data from a real clinical setting. But our results cannot be
generalized to all COPD patients since the patients included
321
Beauchesne et al
Table 3 Description of treatment failure (N = 348 failures for 1180
episodes of treatment)
Type of failure
N (%)
Emergency room visit
Hospitalization
Re-prescription of the same antibiotic
Re-prescription of the same antibiotic followed
by a hospitalization
Prescription of a different antibiotic
Prescription of a different antibiotic followed
by a hospitalization
29 (8.3)
100 (28.7)
44 (12.6)
1 (0.3)
172 (49.4)
2 (0.6)
in our program have a severe form of the disease. We
attempted to compare failure rates between different classes
of antibiotic (data not shown) by performing a Chi-square test
and a Poisson regression analysis, but our study design had
many limitations such as lack of power and the absence of
randomization. In fact, patients who received large spectrum
antibiotics had a higher risk of failure even after adjusting our
results for confounding variables. This suggests that patients
who received large spectrum of antibiotics were the ones with
the most severe disease (ie, higher risk of failure) and we could
not completely exclude the possibility of residual confounding
of disease severity in the analysis of our results.
In conclusion, a wide range of antibiotics are prescribed
to our patients with moderate to severe COPD to treat mild
exacerbations at home. Overall, the initiation at home of
an antibiotic for an acute exacerbation of COPD failed to
prevent the use of another antibiotic treatment, an emergency
room visit, or a hospitalization in 30% of the cases. Results
of this study should alert the clinician to the high risk of
treatment failure when managing mild exacerbations of
COPD at home in patients with severe disease. Furthermore,
our results support the implementation of strategies to better
promote the application of clinical practice guidelines for the
management of chronic diseases.
Disclosure
This study was funded by Bayer Canada Inc. Marie-France
Beauchesne has participated in continuing education programs sponsored by the pharmaceutical industry, such as
GSK, BI, Pzer, and AstraZeneca. She has also received
grants from Merck Frosst, GSK, and AstraZeneca for some
of her research projects. Lucie Blais is a recipient of a New
Investigator Salary Support Grant from the Canadian Institutes
322
for Health Research (CIHR). She has received support from
AstraZeneca, GSK, and Amgen for some of her research
projects. Manon Labrecque has participated in CE programs
or advisory boards for AstraZeneca, AltanaPharma, and GSK.
She has also received grants from Merck Frosst, GSK, and
AstraZeneca for some of her research projects. Marcel Julien
has participated in an advisory board sponsored by BI.
References
Adams SG, Melo J, Luther M, et al. 2000. Antibiotics are associated with
lower relapse rates in outpatients with acute exacerbations of COPD.
Chest, 117:134552.
Anthonisen NR, Manfreda J, Waren CPW, et al. 1987. Antibiotic therapy
of acute exacerbations of chronic obstructive pulmonary disease.
Ann Intern Med, 106:196204.
Boulet L, Becker A, Bowie D, et al. 2006. Implementing practice guidelines:
a workshop on guidelines dissemination and implementation with a
focus on asthma and COPD. Can Respir J, 13(Suppl A):547.
Brand C, Landgren F, Hutchinson A, et al. 2005. Clinical practice guidelines: barriers to durability after effective early implementation. Intern
Med J, 35:1629.
Choi PP, Day A, Etchells E. 2004. Gaps in the care of patients admitted to
hospital with an exacerbation of chronic obstructive pulmonary disease.
CMAJ, 170:140913.
Dewan NA, Raque S, Kanwar B, et al. 2000. Acute exacerbation of COPD.
Factors associated with poor treatment outcome. Chest, 117:66271.
Fritsch K, Jacot ML, Klarer A, et al. 2005. Adherence to the Swiss guidelines
for management of COPD: experience of a Swiss teaching hospital.
Swiss Med Wkly, 135:11621.
Glaab T, Banik N, Trautmann M, et al. 2006. Guideline-conformity of
outpatient COPD management by pneumologists. Pneumologie,
60:395400.
Glaab T, Banik N, Singer C, et al. 2006. Guideline conformance for outpatient management of COPD in Germany. Dtsch Med Wochenschr,
21:12038.
[GOLD] Rabe KF, Hurd S, Anzueto A, et al; Global Initiative for Chronic
Obstructive Lung Disease. 2007. Global strategy for the diagnosis,
management, and prevention of chronic obstructive pulmonary
disease: GOLD executive summary. Am J Respir Crit Care Med,
176:53255.
Jans MP, Schellevis FG, van Hensbergen W, et al. 1998. Management of
asthma and COPD patients: feasibility of the application of guidelines
in general practice. Int J Qual Health Care, 10:2734.
Miravitlles M, Murio C, Guerrero T, et al. 2001. Factors associated with
relapse after ambulatory treatment of acute exacerbations of chronic
bronchitis. Eur Respir J, 17:92833.
ODonnell DE, Aaron S, Bourbeau J, et al. 2007. Canadian Thoracic Society
recommendations for management of chronic obstructive pulmonary
disease2007 update. Can Respir J, 14:5B32B.
Ram FSF, Rodriguez-Roisin R, Granados-Navarrete A, et al. 2006. Antibiotics for exacerbations of chronic obstructive pulmonary disease.
Cochrane Database Syst Rev, 2:CD004403.
Roche N, Lepage T, Bourcereau J, et al. 2001. Guidelines versus clinical
practice in the treatment of chronic obstructive pulmonary disease.
Eur Respir J, 18:9038.
Saint S, Bent S, Vittinghoff E, et al. 1995. Antibiotics in chronic obstructive pulmonary disease exacerbations: a meta-analysis. JAMA,
273:95760.
International Journal of COPD 2008:3(2)
Vous aimerez peut-être aussi
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Case VertigoDocument30 pagesCase VertigoRomi AndriyanaPas encore d'évaluation
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Clinical Pathology and Medical Laboratory: Indonesian Journal ofDocument5 pagesClinical Pathology and Medical Laboratory: Indonesian Journal ofRomi AndriyanaPas encore d'évaluation
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Cover Blok 20Document1 pageCover Blok 20Romi AndriyanaPas encore d'évaluation
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- NkljnrlknlfnrleajngfaejkgnvakejnvdnkvfbkejjDocument1 pageNkljnrlknlfnrleajngfaejkgnvakejnvdnkvfbkejjRomi AndriyanaPas encore d'évaluation
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- KJB KJBDKJBKDDocument1 pageKJB KJBDKJBKDRomi AndriyanaPas encore d'évaluation
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- KJB KJBDKJBKDDocument1 pageKJB KJBDKJBKDRomi AndriyanaPas encore d'évaluation
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- KJB KJBDKJBKDDocument1 pageKJB KJBDKJBKDRomi AndriyanaPas encore d'évaluation
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- JbjbdabDocument1 pageJbjbdabRomi AndriyanaPas encore d'évaluation
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- (AC-S07) Week 07 - Pre-Task - Quiz - Weekly Quiz (PA) - INGLES IV (7573)Document5 pages(AC-S07) Week 07 - Pre-Task - Quiz - Weekly Quiz (PA) - INGLES IV (7573)Lucero JimenezPas encore d'évaluation
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- LeasingDocument18 pagesLeasingsunithakravi0% (1)
- Effect of Educational Environment On Personality and Adjustment of Female Students Studying in Colleges of UttarakhandDocument5 pagesEffect of Educational Environment On Personality and Adjustment of Female Students Studying in Colleges of UttarakhandESSENCE - International Journal for Environmental Rehabilitation and ConservaionPas encore d'évaluation
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- Early Theories On The Origin of Life On Earth: Creation TheoryDocument1 pageEarly Theories On The Origin of Life On Earth: Creation TheoryAngel Elizaga IIPas encore d'évaluation
- SECTION 02892 Traffic Signals Rev 0Document65 pagesSECTION 02892 Traffic Signals Rev 0Abdul HannanPas encore d'évaluation
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- "Mode One" Author & Dating Coach Alan Roger Currie Releases Criticism of Alleged Harvey Weinstein BehaviorDocument3 pages"Mode One" Author & Dating Coach Alan Roger Currie Releases Criticism of Alleged Harvey Weinstein BehaviorPR.com100% (1)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- Plumbing Specifications: Catch Basin PlanDocument1 pagePlumbing Specifications: Catch Basin PlanMark Allan RojoPas encore d'évaluation
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- 004 Torillo v. LeogardoDocument2 pages004 Torillo v. LeogardoylessinPas encore d'évaluation
- Ielts TASK 1 ExerciseDocument3 pagesIelts TASK 1 Exerciseanitha nathenPas encore d'évaluation
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Industrialisation by InvitationDocument10 pagesIndustrialisation by InvitationkimberlyPas encore d'évaluation
- Kim Lighting Landscape Lighting Catalog 1988Document28 pagesKim Lighting Landscape Lighting Catalog 1988Alan MastersPas encore d'évaluation
- Cessna 206 Chapter 24 Illustrated Parts CatalogueDocument33 pagesCessna 206 Chapter 24 Illustrated Parts Cataloguekanwar100% (1)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Selection and Ranking of Rail Vehicle Components For Optimal Lightweighting Using Composite MaterialsDocument14 pagesSelection and Ranking of Rail Vehicle Components For Optimal Lightweighting Using Composite MaterialsAwan AJaPas encore d'évaluation
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Model CV QLDocument6 pagesModel CV QLMircea GiugleaPas encore d'évaluation
- Trump ReportDocument237 pagesTrump ReportAaron Nobel100% (1)
- Cleaning Disinfecting School ClassroomsDocument2 pagesCleaning Disinfecting School ClassroomsFitz JaminitPas encore d'évaluation
- Kevin Coleman's Sentencing MemoDocument26 pagesKevin Coleman's Sentencing MemoThe Valley IndyPas encore d'évaluation
- Index: General Notices (1) Apply To All Monographs and Other TextsDocument36 pagesIndex: General Notices (1) Apply To All Monographs and Other TextsGhenaPas encore d'évaluation
- Homeopathic Colour RemediesDocument23 pagesHomeopathic Colour Remediesisadore100% (42)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- C783 - Intake Manifold 1 Temperature-Abnormal Rate of ChangeDocument4 pagesC783 - Intake Manifold 1 Temperature-Abnormal Rate of ChangeLucas CamposPas encore d'évaluation
- Acute GastroenteritisDocument7 pagesAcute GastroenteritisCherr NollPas encore d'évaluation
- Green Rating System - Ritik JainDocument6 pagesGreen Rating System - Ritik Jainmayuresh barbarwarPas encore d'évaluation
- Chest and Triceps ExercisesDocument6 pagesChest and Triceps ExercisesTess WilliamsPas encore d'évaluation
- CHEQUERED PLATE - Engineer DiaryDocument9 pagesCHEQUERED PLATE - Engineer DiaryAnonymous imkwF8N7TePas encore d'évaluation
- Barista Coffee Company LTDDocument3 pagesBarista Coffee Company LTDGanesh AnandPas encore d'évaluation
- Why Is ICS Important For Schools?Document8 pagesWhy Is ICS Important For Schools?Spit FirePas encore d'évaluation
- DSE8620 MKII Operator ManualDocument224 pagesDSE8620 MKII Operator Manualhenrygrados44Pas encore d'évaluation
- Uas Semt Genap Fix BING XIDocument12 pagesUas Semt Genap Fix BING XISaepulloh KurniaPas encore d'évaluation
- Program Thành TrungDocument3 pagesProgram Thành TrungQuốc HuyPas encore d'évaluation
- Aqa Chm6w W QP Jun02Document18 pagesAqa Chm6w W QP Jun02Diksha KoossoolPas encore d'évaluation
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)