Académique Documents
Professionnel Documents
Culture Documents
Postneoadj Reporting
Transféré par
PorterCopyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Postneoadj Reporting
Transféré par
PorterDroits d'auteur :
Formats disponibles
Anatomic Pathology / ESOPHAGEAL CARCINOMAS AFTER CHEMORADIATION
Histopathologic Examination and Reporting of Esophageal
Carcinomas Following Preoperative Neoadjuvant Therapy
Practical Guidelines and Current Issues
Fuju Chang, MD, PhD, Harriet Deere, MBBS, MRCPath, Ula Mahadeva, MBBS, MRCPath,
and Simi George, MBBS, MRCPath
Key Words: Esophagus; Residual carcinoma; Neoadjuvant chemoradiotherapy; Tumor regression grading; Histopathology
DOI: 10.1309/CCR3QN4874YJDJJ7
Abstract
Neoadjuvant chemoradiotherapy is being
increasingly offered to patients with invasive
esophageal carcinoma in an effort to downstage the
tumor and consequently increase the rate of curative
resection. A substantial amount of data has suggested
that pathologic tumor regression following neoadjuvant
therapy is an important predictor of local recurrence
and long-term survival in esophageal cancer. Therefore,
it is important that these posttreatment resection
specimens are handled in a standardized manner and a
reproducible method of tumor regression grading is
used. Pathologic examination of such specimens is not
straightforward, and, in fact, it presents a particular
challenge to pathologists, especially when a good
response to neoadjuvant therapy has been achieved and
little or no residual tumor remains. We provide some
guidelines for handling and reporting such specimens
and outline the commonly used tumor regression
grading systems for posttreatment esophagectomy
specimens.
252
252
Am J Clin Pathol 2008;129:252-262
DOI: 10.1309/CCR3QN4874YJDJJ7
Esophageal carcinoma ranks among the 10 most frequent
malignancies worldwide.1,2 The 5-year survival rate from diagnosis for these patients is low, about 10%.2-5 In the past decade,
the incidence of adenocarcinoma of the lower esophagus and
gastroesophageal junction has risen markedly, and it is now
more common than squamous cell carcinoma in the United
Kingdom and United States.6,7 Attempts have been made to use
preoperative chemoradiotherapy to downstage the primary
tumor and destroy occult lymph node metastases to increase the
possibility of a successful complete resection and to decrease
the rate of tumor recurrence.8-18 Meta-analyses of randomized
trials of neoadjuvant treatment in patients with esophageal cancer to date have shown that the degree of benefit is substantial
and highly comparable with the benefits of neoadjuvant treatment in other cancers, such as breast, colorectal, and lung.19-21
At present, there is no clinical imaging modality that can
accurately gauge tumor response to chemoradiation, and
pathologic examination of the posttreatment resection specimen remains the gold standard for evaluation of tumor
response.22 There has been accumulating evidence to suggest
that pathologic responses in the tumor to primary therapy are
important predictors of local recurrence and long-term survival.23-29 Therefore, preoperative neoadjuvant therapy has
been used increasingly in the management of this group of
patients, and many esophageal carcinoma resection specimens
arrive at the laboratory already modified by chemoradiation.
Pathologic examination of such specimens may be difficult,
particularly if there has been a good response to preoperative
neoadjuvant therapy; even the site of the cancer may be difficult to identify macroscopically and microscopically.
We present a brief review of the literature on morphologic changes associated with preoperative neoadjuvant therapy
American Society for Clinical Pathology
Anatomic Pathology / REVIEW ARTICLE
and outline the most commonly used tumor regression grading (TRG) systems. Special issues regarding specimen processing and histopathologic examination of posttreatment
esophagectomy specimens are also discussed.
Chemoradiotherapy-Induced Morphologic
Changes
It is well known that chemoradiotherapy causes a number
of histopathologic changes in the tumor and its adjacent tissue
Table 1.23-30
Changes in Tumor Cells
Marked cytoplasmic eosinophilia and vacuolation are
commonly seen Image 1. There is often associated nuclear
atypia without apparent mitotic activity.30 When little residual
tumor remains, carcinoma cells are often dissociated and
arranged singly, in short lines or tubules in a fibrotic stroma.
Carcinoma cells may have very large nuclei, often bizarrely
shaped and multilobated. Nuclear chromatin in tumor cells
tends to be vesicular with large eosinophilic single or multiple
nucleoli. The culmination of these changes is often upgrading
of the tumor to a poorly differentiated carcinoma.
The percentage of tumor cells with neuroendocrine differentiation seems to increase in posttreatment resection specimens Image 2. Morphologically, this can encompass the full
range of the neuroendocrine spectrum, from large cells with
abundant granular eosinophilic cytoplasm to poorly differentiated small round carcinoma cells resembling small cell carcinoma, but immunophenotypic expression of neuroendocrine markers is required for confirmation. Neuroendocrine change was
found in 52% of residual adenocarcinomas after preoperative
Table 1
Neoadjuvant TherapyInduced Morphologic Changes in Tumor Cells and Nonneoplastic Tissue
Morphologic Changes
In tumor cells
Architecture
Nucleus
Cytoplasm
In nonneoplastic tissue
Blood vessels
Stroma
Epithelial changes
Description
Dissociated tubules, short lines, or single cells in a fibrotic stroma; discohesive cells, often suspended in pools
of mucin in mucinous tumors
Nuclear membrane irregularities; chromatin clumping, including pyknosis, karyorrhexis, and formation of
apoptotic bodies; may have large and bizarrely shaped nuclei with multiple lobes and popcorn-like
appearance; fewer mitotic figures; large, often multiple nucleoli
Dense, granular and eosinophilic, or vacuolated; may have merging of cytoplasm of adjacent cells
Intimal proliferation, telangiectasia, organizing thrombi and endarteritis obliterans; atypical endothelial
proliferation also possibly present
Transmural fibrosis and elastosis with a lymphoplasmacytic chronic inflammatory cell infiltrate, bizarre
fibroblasts, foreign body reaction
Esophageal mucosa: may show squamous metaplasia and atrophy of submucosal glands; villiform change
of squamous mucosa; gastric mucosa: may show atrophy of specialized glands and increased numbers
of apoptotic bodies
Image 1 Chemoradiotherapy-induced morphologic changes. Scattered pyknotic carcinoma cells are present in an inflammatory
fibrous stroma. Carcinoma cells show cytoplasmic eosinophilia and vacuolization (H&E, A, 200; B, 400).
Am J Clin Pathol 2008;129:252-262
American Society for Clinical Pathology
253
DOI: 10.1309/CCR3QN4874YJDJJ7
253
253
Chang et al / ESOPHAGEAL CARCINOMAS AFTER CHEMORADIATION
neoadjuvant therapy, whereas such change was seen in only
38% of the paired pretreatment biopsy specimens.31 Notably,
the neuroendocrine component seems to be more resistant to
preoperative neoadjuvant therapy than tumors without such
differentiation, and the presence of neuroendocrine differentiation in residual esophageal carcinomas has been associated
with a worse clinical outcome.31
Stromal and Vascular Changes
Tumor regression in posttreatment specimens seems to be
mostly in the form of fibrosis or fibroinflammatory changes
replacing tumor cells (Image 1).30 Mucinous substance in
fibrotic areas should not be considered as vital residual tumor
but rather a sign of therapeutic success. Bizarre stromal
fibroblasts are often present. There are large, atypical endothelial cells in granulation tissue underlying ulcerated tumor.
Vascular changes such as telangiectasia, organizing thrombi,
myxohyaline intimal proliferation of vessels, and endarteritis
obliterans are common. Giant cell reaction around ghost cells
and keratin may be seen in squamous cell carcinoma.
Nonneoplastic Epithelial Changes
Chemoradiotherapy does not exclusively target the tumor
cells; it also has some effect on nonneoplastic tissues. The morphologic alterations seen, such as an increase in nuclear/cytoplasmic ratio, nuclear pleomorphism, clumping of chromatin,
and the presence of prominent, multiple, and irregular nucleoli,
may cause confusion with dysplasia and carcinoma.
Acanthosis of squamous epithelium away from tumor,
with exaggeration of surface folds giving a serrated appearance, may be present. Esophageal submucosal mucous glands
show acinar atrophy and squamous metaplasia. Squamous
epithelium adjacent to tumor may show spongiosis, focal
acantholysis, ballooning, and cystic degeneration of keratinocytes. Specialized gastric mucosa shows focal gland
atrophy, flattening of epithelium, and nuclear atypia.
Apoptotic bodies may be seen in the parietal and chief cells.
Gland lumina frequently contain neutrophils and cell debris.
There is often a pronounced lymphoplasmacytic infiltrate in
the adjacent esophageal and gastric mucosa.
Tumor Regression Grading
On gross examination, posttreatment resection specimens
can be roughly divided into 3 macroscopic groups. In the first
group, there is bulky residual tumor with no evidence of gross
response to preoperative neoadjuvant therapy. In the second
group, apparent tumor regression is present. No macroscopic
residual tumor is seen but a scar (tumor bed) is found instead.
The third group includes partial-response cases in which
fibrosis and a variable amount of residual tumor are grossly
present. However, accurate TRG relies on the microscopic
assessment. So far, several classification systems have been
used to assess the pathologic response to preoperative neoadjuvant therapy Table 2,30,32-37 none of which has become universally accepted.
The TRG system described by Mandard et al30 seems to
be the most widely used. This system estimates the percentage
of residual carcinoma in relation to the total tumor area,
including the amount of radiation-induced tissue injury. This
method distinguishes 5 tumor regression grades. TRG1 is
defined as the absence of residual tumor and fibrosis extending through the different layers of the esophageal wall. TRG2
Image 2 Neuroendocrine differentiation in residual esophageal carcinoma. A, Poorly differentiated carcinoma cells arranged in
cords and nests showing hyperchromatic nuclei and nuclear molding (H&E, 200). B, Tumor cells are positive for CD56 (400).
254
254
Am J Clin Pathol 2008;129:252-262
DOI: 10.1309/CCR3QN4874YJDJJ7
American Society for Clinical Pathology
Anatomic Pathology / REVIEW ARTICLE
Table 2
Tumor Regression Grading (TRG) Systems Commonly Used
in Gastroesophageal Carcinomas
5-tiered grading system proposed by Mandard et al30
TRG 1, absence of residual cancer and extensive fibrosis
TRG 2, rare residual cancer cells scattered through the fibrosis
TRG 3, increased residual cancer cells but fibrosis still predominating
TRG 4, residual cancer outgrowing fibrosis
TRG 5, absence of regressive changes
4-tiered grading system advocated by Chirieac et al,32 Brucher et
al,25 Swisher et al,33 and Wu et al34
TRG 1, no residual carcinoma
TRG 2, 1%-10% residual carcinoma
TRG 3, 11%-50% residual carcinoma
TRG 4, >50% residual carcinoma
3-tiered grading system advocated by Swisher et al,33 Malaisrie et
al,27 and Wu et al34
P0, 0% residual tumor
P1, 1%-50% residual tumor
P2, >50% residual tumor
is characterized by rare residual cancer cells scattered
throughout the fibrosis. TRG3 has more residual tumor cells,
but fibrosis still predominates. In TRG4, residual cancer cells
predominate in the fibrosis, and in TRG5, the tumor shows no
signs of regression.
This TRG system has been shown to be reproducible by
several authors.23,37 Esophagectomy specimens histologically
graded as TRG1 or TRG2 have been associated with a statistically significant survival benefit compared with other regression classes. However, no statistically significant difference
could be detected between pathologic complete remission
(TRG1) and microscopic residual disease (TRG2) in patients
with esophageal cancer.30 Because the separation of TRG1
from TRG2 tumors is dependent on the diligence of the
pathologist in searching for scanty residual tumor cells, this
statistical nonsignificance may be false.
In a large retrospective review of 235 cases carried out by
Chirieac et al,32 a 4-tiered classification scheme Image 3 for
extent of residual carcinoma was used: 0% residual carcinoma, 1% to 10% residual carcinoma, 11% to 50% residual carcinoma, and more than 50% (gross residual carcinoma).
Overall survival was best for patients with no residual carcinoma and worst for patients with more than 50% residual carcinoma, but there was no statistical difference in survival
between patients with 1% to 10% and 11% to 50% residual
carcinoma, who were in an intermediate prognostic category.
On the basis of these results, Wu et al34 proposed a 3tiered classification as P0 (0% residual carcinoma), P1 (1%50% residual carcinoma), and P2 (>50% residual carcinoma)
to reflect the status of tumor response to chemoradiation. The
4- and 3-tiered grading systems were tested in 60 coded cases
of esophageal adenocarcinomas treated with preoperative
chemoradiation followed by esophagectomy. The cases were
reviewed by 6 pathologists from 4 institutions for extent of
residual carcinoma and pathologic TNM stage. Their results
suggested that the interobserver agreement for extent of residual carcinoma is excellent when using a 3-tiered classification
scheme (all scores >0.75). Patients with 0% residual carcinoma (P0) had significantly better overall survival than
patients with 1% to 50% residual carcinoma (P1) and patients
with more than 50% residual carcinoma (P2). Further subdividing the pathologic response in the P1 group into 1% to 10%
residual carcinoma and 11% to 50% residual carcinoma was
not highly reproducible and could achieve at best only good
agreement among pathologists ( = 0.62 for 1%-10% residual
carcinoma; = 0.50 for 11%-50% residual carcinoma).
Therefore, this 3-tiered grading system seems to be more easily implemented and more reproducible and yields similar
quality prognostic information.
Pathologic complete response rates have been reported in up
to 30% of patients.23-37 Most patients experience at least a partial
response after preoperative neoadjuvant therapy. Although different neoadjuvant therapy regimens have been used for preoperative treatment of different carcinoma types, data have suggested
that the TRG classifications could be equally applicable to squamous cell carcinoma and adenocarcinoma.26
Special Issues in Specimen Examination
and Reporting
As for conventional cancer resection specimens, all posttreatment esophagectomy specimens should be examined by
experienced surgical pathologists according to standardized
protocols (eg, College of American Pathologists Cancer
Protocols and the Royal College of Pathologists Minimum
Dataset) that include World Health Organization tumor classification, tumor differentiation, lymph node involvement,
resection margin status, and TNM staging. The y symbol
should be used for staging following neoadjuvant chemoradiotherapy.38 The ypTNM categorizes the extent of residual
tumor in posttreatment resection specimens; it is not an estimate of tumor before initiation of neoadjuvant therapy.38
Macroscopic Examination
Specimens should be sent immediately to the pathology
laboratory, ideally in the fresh state. If this is not possible, the
specimen should be fixed in formalin of a volume at least
twice that of the specimen. The specimen should be accompanied by full clinical information, including the tumor site; the
tumor type and grade if biopsied before neoadjuvant therapy;
the type of neoadjuvant therapy; and the radiologic and clinical
assessments of the response to neoadjuvant therapy. Owing to
neoadjuvant therapyinduced fibrosis, the esophagectomy
specimens may be of suboptimal quality and any tears or
defects in the esophageal adventitia or muscularis propria
need to be carefully documented.
Am J Clin Pathol 2008;129:252-262
American Society for Clinical Pathology
255
DOI: 10.1309/CCR3QN4874YJDJJ7
255
255
Chang et al / ESOPHAGEAL CARCINOMAS AFTER CHEMORADIATION
Specimens should be well fixed. The issue of whether the
esophagus should be opened longitudinally and pinned or left
intact in the region of the tumor and the lumen stuffed with a
3-Tiered
4-Tiered
P0
(0%)
TRG1
(0%)
tissue paper wick is a contentious one.39 It is our opinion that
as long as the circumferential resection margin is inked before
cutting through it, a flexible approach should be adopted, with
TRG2
(1-10%)
P1
(1-50%)
TRG3
(11-50%)
P2
(>50%)
TRG4
(>50%)
Image 3 Schematic diagram and representative illustrations for assessment of residual esophageal carcinoma in
posttreatment resection specimens. In the 4-tiered tumor regression grading (TRG) system, the extent of residual carcinoma is
classified as 0% residual carcinoma (TRG1), 1% to 10% residual carcinoma (TRG2) (arrows), 11% to 50% residual carcinoma
(TRG3), and >50% residual carcinoma (TRG4). The modified 3-tiered system is devised by combining TRG2 and TRG3 to form a
single category. (Modified from Wu et al.34)
256
256
Am J Clin Pathol 2008;129:252-262
DOI: 10.1309/CCR3QN4874YJDJJ7
American Society for Clinical Pathology
Anatomic Pathology / REVIEW ARTICLE
noncircumferential and impalpable tumors best pinned and
bulky circumferential tumors best left intact.
The sampling technique and the number of blocks taken
are clearly dependent on the size of the residual tumor. In many
institutions, including ours, the fixed specimen is cut into complete transverse slices encompassing the entire area of tumor
Image 4. Orientation of the sliced sections can be achieved by
inking the quadrants of circumferential resection margin in different colors. If the lesion remains macroscopically visible, the
specimen can be handled as a specimen not having received
preoperative therapy. A minimum of 4 paraffin blocks should
be taken from the tumor, including samples from its closest
point to the nearest margin to enable microscopic assessment.
In approximately one third of cases, the tumors may have complete or near complete response to preoperative therapy.
Macroscopic assessment of these specimens can be difficult.
The tumor may be ill-defined and impossible to distinguish
from fibrous stromal tissue. In these cases, it is important to
identify the tumor bed. Characteristically, this is a central,
sometimes somewhat edematous-appearing area of fibrosis
Image 5. Pathologic complete response is the gold standard
for many of the ongoing clinical trials and is recognized to be a
good prognostic factor for patients; pathologists must, therefore, sample widely to confirm that there is indeed no pathologically detectable disease. If the tumor bed cannot be identified
macroscopically, the entire area of macroscopic abnormality
may need to be blocked.
The Siewert classification of junctional adenocarcinoma
is used, as for tumors resected without previous neoadjuvant
therapy.40,41 Accordingly, adenocarcinoma of the distal esophagus with the center of the tumor lying 1 to 5 cm above the
gastroesophageal junction is designated as Siewert type 1,
with the center of the tumor lying between 1 cm above and 2
cm below the gastroesophageal junction is designated as
Siewert type 2, and with the center of the tumor lying between
2 and 5 cm below the gastroesophageal junction is designated
as Siewert type 3. This classification determines which
ypTNM system should be used: Siewert type 1 adenocarcinomas are considered as esophageal primary tumors, whereas
type 2 and type 3 adenocarcinomas are regarded as gastric primary tumors. Notably, carcinomas of the squamous, small
cell, and undifferentiated types located at the gastroesophageal junction (topographically equivalent to Siewert
type 2 tumors) are classified as esophageal primary tumors. In
cases with complete pathologic response, the location of the
tumor bed determines the Siewert typing.
The use of large (mega) blocks Image 6, if available, can
be valuable in determining the distribution of residual tumor
foci, when present. If only patchy residual disease is present
and tumor is no longer contiguous, this can be identified particularly clearly in such large blocks.
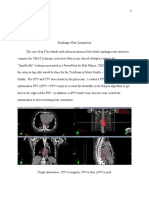
The documentation of the size, location, and gross
appearance of the tumor as digital images is often useful in the
reporting of the specimen and discussion of the case in correlation with radiologic images at multidisciplinary meetings.
Microscopic Examination
A histologic complete pathologic response is defined by
the inability of the pathologist to demonstrate any viable (nonnecrotic) tumor cells within the specimen. Microscopic evidence of a tumor bed must be identified, and this is mandatory for assessment of complete response. Histologically, the
Image 4 A, An example of macroscopic examination of partial esophagogastrectomy specimen containing a Siewert type 2
tumor at the gastroesophageal junction. B, After fixation, the specimen is transversely sectioned and the slices are laid out for
inspection and blocking.
Am J Clin Pathol 2008;129:252-262
American Society for Clinical Pathology
257
DOI: 10.1309/CCR3QN4874YJDJJ7
257
257
Chang et al / ESOPHAGEAL CARCINOMAS AFTER CHEMORADIATION
Image 5 Complete pathologic response. A, A tumor bed
(arrow) with surface ulceration and transmural fibrosis is
present, but no visible tumor is seen on macroscopic
examination. B, This area is composed of fibrous tissue
infiltrated by inflammatory cells (H&E, 100). C, Note the blood
vessels showing intimal hyperplasia (H&E, 200).
Image 6 An example of a mega block section of esophageal carcinoma. A, A transversely sectioned slice revealing bulky
residual tumor on macroscopic examination. B, The tumor apparently infiltrates into esophageal adventitial fibrofatty tissue and
lies very close to the circumferential resection margin.
258
258
Am J Clin Pathol 2008;129:252-262
DOI: 10.1309/CCR3QN4874YJDJJ7
American Society for Clinical Pathology
Anatomic Pathology / REVIEW ARTICLE
tumor bed is characterized by abnormal fibroblastic stroma
that is devoid of the normal layers of the esophageal wall and
contains foamy macrophages and a moderate number of
fibroblasts and mononuclear inflammatory cells (Image 5). In
these areas, there may be edema or mucinous or myxoid
change of the stroma or even areas of necrosis.
The presence of mucin lakes without associated malignant cells should be defined as a pathologic complete response
Image 7. Similarly, necrotic areas (Image 7) and keratin
flakes without identifiable viable cancer cells should be
defined as a pathologic complete response.
When there is diagnostic uncertainty, step-sections and
further staining procedures such as mucin staining (alcian
blueperiodic acidSchiff) and immunohistochemical analysis for pancytokeratin (MNF116 or AE1/AE3) may be helpful
in distinguishing individual tumor cells from treatment-related bizarre fibroblasts and foreign body giant cells Image 8.
Lymph Node Handling
The use of chemoradiotherapy seems to cause lymph
nodes to undergo regression and atrophy to such an extent that
they may become impalpable macroscopically. Therefore, the
Image 7 The presence of necrotic areas (A, H&E, 200) and mucin lakes (B, H&E, 400) without identifiable viable carcinoma
cells should be defined as a pathologic complete response.
A
Image 8 Good response to preoperative treatment is evident in this specimen. A, Only occasional residual carcinoma cells are
seen, and a confident diagnosis is obscured by the presence of chemoradiation-induced bizarre fibroblasts and histiocytic
multinucleated giant cells (H&E, 400). B, Immunohistochemical analysis for pancytokeratin (MNF116) highlights the residual
carcinoma cells (400).
Am J Clin Pathol 2008;129:252-262
American Society for Clinical Pathology
259
DOI: 10.1309/CCR3QN4874YJDJJ7
259
259
Chang et al / ESOPHAGEAL CARCINOMAS AFTER CHEMORADIATION
number of lymph nodes found following preoperative therapy
is generally low. Careful searching for lymph nodes is essential. In addition, random sampling of adventitial fat often
yields only microscopically identifiable lymph nodes.
On microscopic examination, the lymph nodes usually
display considerable lymphoid depletion, sinus histiocytosis, accumulation of hemosiderin-laden macrophages, fibrosis, hyalinization, and acellular mucin lakes. As for the primary tumor, these changes are regarded as negative for
residual tumor unless viable cancer cells can be demonstrated. The residual metastatic carcinoma cells may show cytologic changes similar to those seen in the primary tumor.
When little residual tumor remains, it may be impossible to
demonstrate carcinoma cells in H&E-stained slides. The use
of immunohistochemical analysis for broad-spectrum
cytokeratins, such as MNF116 and AE1/AE3, may be helpful in these cases Image 9. However, false-positive results
may occur, and assessment must be based on the correlation
of such immunohistochemical findings with morphologic
features.
involvement of the resection margins, vascular and perineural invasion, and lymph node involvement.
Preoperatively treated esophageal tumors are graded
using the same criteria as nontreated carcinomas.20-30 It is
important to note that histologic grading of these treated
tumors may be affected by therapy-induced morphologic
changes. As discussed in the preceding sections, preoperative
neoadjuvant therapy causes a number of architectural and
cytologic changes. These include increased percentage of
tumor cells with neuroendocrine differentiation and increased
nuclear atypia of residual cancer cells.30,31 The culmination of
these changes could lead to upgrading of the tumor to a poorly differentiated carcinoma. Further evaluation of neoadjuvant
therapyinduced tumor morphologic changes and their possible effects on tumor differentiation would be helpful in defining more accurate tumor grading systems for preoperatively
treated esophageal carcinomas.
Pathology Report
In addition to comment on the pathologic response to preoperative neoadjuvant therapy (ie, tumor regression grade),
the histopathology report for posttreatment esophagectomy
specimens should also include the principal prognostic factors
already being used for nontreated esophageal cancer specimens. These have been detailed in the CAP Cancer Protocols
(available at http://www.cap.org) and the Royal College of
Pathologists Minimum Dataset (available at http://www.
rcpath.org). Briefly, a report should include comments on the
type and differentiation of the tumor, depth of invasion, TRG,
A substantial amount of data has been accumulated to
suggest that TRG and pathologic ypTNM staging are important prognostic factors in esophageal cancer.23-37 Although
response to therapy has been evaluated using various radiologic imaging techniques, currently, there is no clinical imaging
modality that can accurately gauge tumor response to
chemoradiation,22,42 and pathologic examination of the resected specimen remains the gold standard for tumor response
assessment.23-37 Therefore, it is important that these posttreatment resection specimens are handled in a standardized manner, and a reproducible TRG method must be used.
Conclusions and Future Direction
Image 9 A, A lymph node shows extensive fibrosis (H&E, 100). B, Scattered carcinoma cells are identified by
immunostaining for pancytokeratin (MNF116) (100).
260
260
Am J Clin Pathol 2008;129:252-262
DOI: 10.1309/CCR3QN4874YJDJJ7
American Society for Clinical Pathology
Anatomic Pathology / REVIEW ARTICLE
There is significant variability in the histopathologic
response of tumors to neoadjuvant chemotherapy. Approximately
15% to 30% of patients experience a complete response,
whereas up to 70% of patients have an incomplete or no
response to the neoadjuvant regimen. The identification of
factors that predict a response would be of considerable clinical benefit. The underlying mechanism for this variability is
unknown, and, currently, there are no reliable predictors of
response based on standard pathologic assessment and
immunohistochemical analysis of biopsy specimens.43
Contributing factors may include the diverse genetic
alterations involved in growth factor receptors, chemokines of
angiogenesis, tumor suppressor genes, cell cycle regulators
and enzymes involved in the DNA repair system, apoptosis,
and the degradation of extracellular matrix.43-48 Preliminary
reports indicate that gene expression profiles and polymorphisms seem to allow prediction of sensitivity to specific
chemotherapy and radiotherapy regimens44,48 and, thus, may
allow rational and individualized treatment approaches for
gastroesophageal carcinomas.
From the Department of Histopathology, St Thomas Hospital,
Guys and St Thomas NHS Foundation Trust, London, England.
Address correspondence to Dr Chang: Dept of
Histopathology, St Thomas Hospital, Guys and St Thomas NHS
Foundation Trust, Lambeth Palace Rd, London SE1 7EH, England.
Acknowledgment: The skillful technical assistance of K.
Marsden, FIBMS, and R. Cumming, FIBMS, is gratefully
acknowledged.
References
1. Jemal A, Murray T, Ward W, et al. Cancer statistics. CA
Cancer J Clin. 2005;55:10-30.
2. Enzinger PC, Mayer RJ. Esophageal cancer. N Engl J Med.
2003;349:2241-2252.
3. Hofstetter W, Swisher SG, Correa AM, et al. Treatment
outcomes of resected esophageal cancer. Ann Surg.
2002;236:376-385.
4. Hagen JA, DeMeester SR, Peters JH, et al. Curative resection
for esophageal adenocarcinoma: analysis of 100 en bloc
esophagectomies. Ann Surg. 2001;234:520-530.
5. Muller JM, Erasmi H, Stelzner M, et al. Surgical therapy of
oesophageal carcinoma. Br J Surg. 1990;77:845-857.
6. Devesa SS, Blot WJ, Fraumeni JF. Changing patterns in the
incidence of esophageal and gastric carcinoma in the United
States. Cancer. 1998;83:2049-2053.
7. DeMeester SR. Adenocarcinoma of the esophagus and cardia:
a review of the disease and its treatment. Ann Surg Oncol.
2006;13:12-30.
8. Leichman L, Steiger Z, Seydel HG, et al. Preoperative
chemotherapy and radiation therapy for patients with cancer
of the esophagus: a potentially curative approach. J Clin Oncol.
1984;2:75-79.
9. Forastiere AA, Orringer MB, Perez-Tamayo C, et al.
Preoperative chemoradiation followed by transhiatal
esophagectomy for carcinoma of the esophagus: final report.
J Clin Oncol. 1993;11:1118-1123.
10. Bosset JF, Gignoux M, Triboulet JP, et al. Chemoradiotherapy
followed by surgery compared with surgery alone in squamouscell cancer of the esophagus. N Engl J Med. 1997;337:161-167.
11. Kelsen DP, Ginsberg R, Pajak TF, et al. Chemotherapy
followed by surgery compared with surgery alone for localized
esophageal cancer. N Engl J Med. 1998;339:1979-1984.
12. Coia LR, Minsky BD, Berkey BA, et al. Outcome of patients
receiving radiation for cancer of the esophagus: results of the
1992-1994 Patterns of Care Study. J Clin Oncol. 2000;18:455462.
13. Stein H, Sendler A, Ulrich F, et al. Multidisciplinary approach
to esophageal and gastric cancer. Surg Clin North Am.
2000;80:659-682.
14. Heath EI, Burtness BA, Heitmiller RF, et al. Phase II evaluation
of preoperative chemoradiation and postoperative adjuvant
chemotherapy for squamous cell and adenocarcinoma of the
esophagus. J Clin Oncol. 2000;18:868-876.
15. Urba SG, Orringer MB, Turrisi A, et al. Randomized trial of
preoperative chemoradiation versus surgery alone in patients
with locoregional esophageal carcinoma. J Clin Oncol.
2001;19:305-313.
16. Ancona E, Ruol A, Santi S, et al. Only pathologic complete
response to neoadjuvant chemotherapy improves significantly
the long term survival of patients with resectable esophageal
squamous cell carcinoma. Cancer. 2001;91:2165-2174.
17. Medical Research Council Oesophageal Cancer Working
Group. Surgical resection with or without preoperative
chemotherapy in oesophageal cancer: a randomised controlled
trial. Lancet. 2002;359:1727-1734.
18. Meluch AA, Greco FA, Gray JR, et al. Preoperative therapy
with concurrent paclitaxel/carboplatin/infusional 5-FU and
radiation therapy in locoregional esophageal cancer; final
results of a Minnie Pearl Cancer Research Network phase II
trial. Cancer J. 2003;9:251-260.
19. Gebski V, Burmeister B, Smithers BM, at el. Survival benefits
from neoadjuvant chemoradiotherapy or chemotherapy in
oesophageal carcinoma: a meta-analysis. Lancet Oncol.
2007;8:226-234.
20. Greil R, Stein HJ. Is it time to consider neoadjuvant treatment
as the standard of care in oesophageal cancer [letter]? Lancet
Oncol. 2007;8:189-190.
21. Schneider BJ, Urba SG. Preoperative chemoradiation for the
treatment of locoregional esophageal cancer: the standard of
care? Semin Radiat Oncol. 2007;17:45-52.
22. Westerterp M, van Westreenen HL, Reitsma JB, et al.
Esophageal cancer: CT, endoscopic US, and FDG PET for
assessment of response to neoadjuvant therapy: systematic
review. Radiology. 2005;236:841-851.
23. Dunne B, Reynolds JV, Mulligan E, et al. A pathological study of
tumour regression in oesophageal adenocarcinoma treated with
preoperative chemoradiotherapy. J Clin Pathol. 2001;54:841-845.
24. Brucher BL, Stein HJ, Zimmermann F, et al. Responders
benefit from neoadjuvant radiochemotherapy in esophageal
squamous cell carcinoma: results of a prospective phase-II trial.
Eur J Surg Oncol. 2004;30:963-971.
25. Brucher BL, Becker K, Lordick F, et al. The clinical impact
of histopathologic response assessment by residual tumor cell
quantification in esophageal squamous cell carcinomas.
Cancer. 2006;106:2119-2127.
26. Schneider PM, Baldus SE, Metzger R, et al. Histomorphologic
tumor regression and lymph node metastases determine
prognosis following neoadjuvant radiochemotherapy for
esophageal cancer: implications for response classification.
Ann Surg. 2005;242:684-692.
Am J Clin Pathol 2008;129:252-262
American Society for Clinical Pathology
261
DOI: 10.1309/CCR3QN4874YJDJJ7
261
261
Chang et al / ESOPHAGEAL CARCINOMAS AFTER CHEMORADIATION
27. Malaisrie SC, Hofstetter WL, Correa AM, et al. The addition
of induction chemotherapy to preoperative, concurrent
chemoradiotherapy improves tumor response in patients with
esophageal adenocarcinoma. Cancer. 2006;107:967-974.
28. Korst RJ, Kansler AL, Port JL, et al. Downstaging of T or N
predicts long-term survival after preoperative chemotherapy
and radical resection for esophageal carcinoma. Ann Thorac
Surg. 2006;82:480-485.
29. de Manzoni G, Pedrazzani C, Pasini F, et al.
Chemoradiotherapy followed by surgery for squamous cell
carcinoma of the thoracic esophagus with clinical evidence
of adjacent organ invasion. J Surg Oncol. 2007;95:261-266.
30. Mandard AM, Dalibard F, Mandard JC, et al. Pathologic
assessment of tumor regression after preoperative
chemoradiotherapy of esophageal carcinoma;
clinicopathologic correlations. Cancer. 1994;73:2680-2686.
31. Hornick JL, Farraye FA, Odze RD. Prevalence and significance
of prominent mucin pools in the esophagus post neoadjuvant
chemoradiotherapy for Barretts-associated adenocarcinoma.
Am J Surg Pathol. 2006;30:28-35.
32. Chirieac LR, Swisher SG, Ajani JA, et al. Posttherapy
pathologic stage predicts survival in patients with esophageal
carcinoma receiving preoperative chemoradiation. Cancer.
2005;103:1347-1355.
33. Swisher SG, Hofstetter W, Wu TT, et al. Proposed revision of
the esophageal cancer staging system to accommodate
pathologic response (pP) following preoperative
chemoradiation (CRT). Ann Surg. 2005;241:810-820.
34. Wu TT, Chirieac LR, Abraham SC, et al. Excellent
interobserver agreement on grading the extent of residual
carcinoma after preoperative chemoradiation in esophageal
and esophagogastric junction carcinoma: a reliable predictor
for patient outcome. Am J Surg Pathol. 2007;31:58-64.
35. Wang KL, Yang Q, Cleary KR, et al. The significance of
neuroendocrine differentiation in adenocarcinoma of the
esophagus and esophagogastric junction after preoperative
chemoradiation. Cancer. 2006;107:1467-1474.
36. Hermann RM, Horstmann O, Haller F, et al.
Histomorphological tumor regression grading of esophageal
carcinoma after neoadjuvant radiochemotherapy: which score
to use? Dis Esophagus. 2006;19:329-334.
262
262
Am J Clin Pathol 2008;129:252-262
DOI: 10.1309/CCR3QN4874YJDJJ7
37. MacGuill M, Mulligan E, Ravi N, et al. Clinicopathologic
factors predicting complete pathological response to
neoadjuvant chemoradiotherapy in esophageal cancer. Dis
Esophagus. 2006;19:273-276.
38. Sobin LH, Wittekind CH, International Union Against
Cancer, eds. TNM Classification of Malignant Tumours. 5th ed.
Baltimore, MD: Wiley-Liss, 1997.
39. Ibrahim NB. Guidelines for handling oesophageal biopsies
and resection specimens and their reporting. J Clin Pathol.
2000;53:89-94.
40. Stein HJ, Feith M, Siewert JR. Cancer of the esophagogastric
junction. Surg Oncol. 2000;9:35-41.
41. Siewert JR, Stein HJ. Classification of adenocarcinoma of
the oesophagogastric junction. Br J Surg. 1998;85:1457-1459.
42. Forshaw MJ, Gossage JA, Mason RC. Neoadjuvant
chemotherapy for oesophageal cancer: the need for accurate
response prediction and evaluation. Surgeon. 2005;3:373-382,
422.
43. Vallbohmer D, Lenz HJ. Predictive and prognostic molecular
markers in outcome of esophageal cancer. Dis Esophagus.
2006;19:425-432.
44. Wieder HA, Brcher BL, Zimmermann F, et al. Time course
of tumor metabolic activity during chemoradiotherapy of
esophageal squamous cell carcinoma and response to
treatment. J Clin Oncol. 2004;22:900-908.
45. Heeren PA, Kloppenberg FW, Hollema H, et al. Predictive
effect of p53 and p21 alteration on chemotherapy response
and survival in locally advanced adenocarcinoma of the
esophagus. Anticancer Res. 2004;24:2579-2583.
46. Schneider S, Uchida K, Brabender J, et al. Downregulation of
TS, DPD, ERCC1, GST-Pi, EGFR, and HER2 gene expression
after neoadjuvant three-modality treatment in patients with
esophageal cancer. J Am Coll Surg. 2005;200:336-344.
47. Kaur T, Khanduja KL, Kaushik T, et al. P53, COX-2, iNOS
protein expression changes and their relationship with antioxidant enzymes in surgically and multi-modality treated
esophageal carcinoma patients. J Chemother. 2006;18:74-84.
48. Wu X, Gu J, Wu TT, et al. Genetic variations in radiation and
chemotherapy drug action pathways predict clinical outcomes
in esophageal cancer. J Clin Oncol. 2006;24:3789-3798.
American Society for Clinical Pathology
Vous aimerez peut-être aussi
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (74)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Globocan 2020Document2 pagesGlobocan 2020Dicky keyPas encore d'évaluation
- Mastectomy OutlineDocument6 pagesMastectomy OutlineHope SerquiñaPas encore d'évaluation
- Target Delineation. CTV in Magenta, PTV in Red, ZPTV in PinkDocument11 pagesTarget Delineation. CTV in Magenta, PTV in Red, ZPTV in Pinkapi-540888060Pas encore d'évaluation
- Prostate Cancer Imaging July, 2020 - ICI 01Document42 pagesProstate Cancer Imaging July, 2020 - ICI 01madvincyPas encore d'évaluation
- Men's Health Poster UK A4Document1 pageMen's Health Poster UK A4Charlie WeirPas encore d'évaluation
- Fight Club - Beat SheetDocument28 pagesFight Club - Beat Sheetthegreatseachange5933Pas encore d'évaluation
- Ovarian Cancer Case StudyDocument46 pagesOvarian Cancer Case StudyAmriati100% (3)
- Phyllodes Tumors of The Breast UpToDateDocument22 pagesPhyllodes Tumors of The Breast UpToDateSean SialanaPas encore d'évaluation
- 702 1383 1 PB PDFDocument7 pages702 1383 1 PB PDFEko RistiyantoPas encore d'évaluation
- Soft Tissue TumorsDocument570 pagesSoft Tissue TumorsGeo GrigorePas encore d'évaluation
- Article On Human Papilloma VirusDocument5 pagesArticle On Human Papilloma VirusHafiz SabghatullahPas encore d'évaluation
- Unknown Primary Cancer of The Head and Neck - A MultidisciplinaryDocument10 pagesUnknown Primary Cancer of The Head and Neck - A MultidisciplinaryFreddy Eduardo Navarro BautistaPas encore d'évaluation
- Asbestos AwarenessDocument14 pagesAsbestos AwarenessSAQIBPas encore d'évaluation
- Calendar YejsoDocument2 pagesCalendar YejsoTJ LapuzPas encore d'évaluation
- People Also Ask: Scribd Gave Me Cancer TwiceDocument2 pagesPeople Also Ask: Scribd Gave Me Cancer TwiceRobert Burke0% (1)
- Tumori Stromale GastrointestinaleDocument20 pagesTumori Stromale GastrointestinaleVasui AlexandraPas encore d'évaluation
- Mastectomy: Presenter: DR Janardhan T Post GraduateDocument49 pagesMastectomy: Presenter: DR Janardhan T Post GraduateASHUTOSH KUMARPas encore d'évaluation
- Prostate CancerDocument45 pagesProstate CancerNeethiselvam Devadoss100% (2)
- Intl Journal of Cancer - 2014 - Lakritz - Beneficial Bacteria Stimulate Host Immune Cells To Counteract Dietary and GeneticDocument12 pagesIntl Journal of Cancer - 2014 - Lakritz - Beneficial Bacteria Stimulate Host Immune Cells To Counteract Dietary and GeneticTrang MốcPas encore d'évaluation
- Uk Guidelines SarcomaDocument21 pagesUk Guidelines Sarcomachu_chiang_3Pas encore d'évaluation
- Jama Sharma 2022 RV 220013 1660585212.14221Document9 pagesJama Sharma 2022 RV 220013 1660585212.14221Jatin YegurlaPas encore d'évaluation
- Esophagus Plan Comparison-Supafirefly Vs ImrtDocument17 pagesEsophagus Plan Comparison-Supafirefly Vs Imrtapi-602263051Pas encore d'évaluation
- Breast LumpDocument17 pagesBreast LumpgaganPas encore d'évaluation
- Oncologic Imaging: Bone TumorsDocument379 pagesOncologic Imaging: Bone TumorsRuben Figueroa100% (1)
- Cancer Is A Functional Repair TissueDocument6 pagesCancer Is A Functional Repair TissueFilipos ConstantinPas encore d'évaluation
- Sarcoma de EwingDocument5 pagesSarcoma de EwingLEANDRO GARCIA FILHOPas encore d'évaluation
- Curs Colon RectDocument96 pagesCurs Colon RectIoanaPas encore d'évaluation
- 2009 - Distribusi Gambaran Klinik Laring Pada Penderita Dengan Suara Serak Di THT-KL USU Medan PDFDocument8 pages2009 - Distribusi Gambaran Klinik Laring Pada Penderita Dengan Suara Serak Di THT-KL USU Medan PDFelFadhlyPas encore d'évaluation
- Bezig Met E-Mailen AK-Forbidden - Health-Prostate - CancerDocument3 pagesBezig Met E-Mailen AK-Forbidden - Health-Prostate - CanceravdpoortPas encore d'évaluation
- BI-RADS For UltrasonographyDocument11 pagesBI-RADS For UltrasonographyLucas GuadaPas encore d'évaluation