Académique Documents
Professionnel Documents
Culture Documents
Understanding acid-base balance: Interpret values and steady a disturbed equilibrium
Transféré par
YuniParaditaDjunaidiDescription originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Understanding acid-base balance: Interpret values and steady a disturbed equilibrium
Transféré par
YuniParaditaDjunaidiDroits d'auteur :
Formats disponibles
Understanding
acid-base balance
Find out how to interpret values and steady a disturbed equilibrium in an acutely ill patient.
By Susan J. Appel, APRN,BC, CCRN, PhD, and Charles A. Downs, APRN,BC, CCRN, MSN
Many critical illnesses can upset a patients acid-base balance, and a disturbance in acid-base equilibrium may indicate other underlying diseases or organ damage. Accurately
interpreting acid-base balance requires simultaneous measurements of arterial pH and plasma electrolytes, as well as
knowledge of compensatory physiologic mechanisms.
In this article, well review normal acid-base physiology, acid-base disturbances, and lab techniques and mathematical calculations used to identify the cause of acid-base
derangements. Lastly, well discuss potential treatments for
acid-base disturbances.
generates 50 to 100 mEq/day of acid from metabolism of
carbohydrates, proteins, and fats. In addition, the body
loses base in the stool. In order to maintain acid-base
homeostasis, acid production must balance the neutralization or excretion. The lungs and kidneys are the main regulators of acid-base homeostasis. The lungs release CO2, an
end product of carbonic acid (H2CO3). The renal tubules,
with the regulation of bicarbonate (HCO3-), excrete other
acids produced from the metabolism of proteins, carbohydrates, and fats.1
Compensating for changes
Whats normal?
The body has three compensatory mechanisms to handle
changes in serum pH:
Physiologic buffers, consisting of a weak acid (which
can easily be broken down) and its base salt or of a weak
base and its acid salt. These buffers are the bicarbonatecarbonic acid buffering system, intracellular protein
buffers, and phosphate buffers in the bone.
Pulmonary compensation, in which changes in ventilation work to change the partial pressure of arterial carbon
dioxide (PaCO2) and drive the pH toward the normal
range. A drop in pH, for example, results in increased ventilation to blow off excess CO2. An increase in pH decreases ventilatory effort, which increases PaCO2 and lowers
the pH back toward normal.
Renal compensation, which kicks in when the other
mechanisms have been ineffective, generally after about
6 hours of sustained acidosis or alkalosis. While respira-
A normal range for arterial pH is 7.35 to 7.45. Acidosis is
a pH less than 7.35; alkalosis is a pH greater than 7.45.
Because pH is measured in terms of hydrogen (H+) ion
concentration, an increase in H+ ion concentration decreases pH and vice versa. Changes in H+ ion concentration can be stabilized through several buffering systems:
bicarbonate-carbonic acid, proteins, hemoglobin, and
phosphates.
Acidosis, therefore, can be described as a physiologic
condition caused by the bodys inability to buffer excess H+
ions. At the other end, alkalosis results from a deficiency in
H+ ion concentration. Acidemia and alkalemia refer to the
process of acidosis or alkalosis, respectively, occurring in
arterial blood.
Body acids are formed as end products of cellular metabolism. Under normal physiologic conditions, a person
Fall 2008
ED Insider
Metabolic alkalosis
tory compensation occurs almost immediately, renal
mechanisms can take hours to days to make a difference.
In acidosis the kidneys excrete H+ in urine and retain
HCO3-. In alkalosis, the kidneys excrete bicarbonate and
retain H+ in the form of organic acids, resulting in nearnormalization of pH.2,3 Lastly, bone may also serve as a
buffer because it contains a large reservoir of bicarbonate
and phosphate and can buffer a significant acute acid
load. Patients who have low albumin levels and bone
density due to malnutrition or chronic disease, and anemic patients, have an ineffective buffering capability.4
Metabolic alkalosis occurs when HCO3- is increased, usually as the result of excessive loss of metabolic acids. Causes
of metabolic alkalosis include diuretics, secretory adenoma
of the colon, emesis, hyperaldosteronism, Cushings syndrome, and exogenous steroids.
Some causes of metabolic alkalosis respond to treatment with 0.9% sodium chloride solution. If the patients
urine chloride concentration is less than 15 mmol/L, his
metabolic alkalosis is saline-responsive; urine chloride
levels above 25 mmol/L indicate nonsaline-responsive
metabolic alkalosis.2,7 The mechanisms resulting in salineresponsive metabolic alkalosis include GI loss, diuresis, or
renal compensation from hypercapnia. Nonsaline responsivemetabolic alkalosis results from mineralocorticoid excess or potassium depletion.
Fluid administration is the foundation for treatment
for saline-responsivemetabolic alkalosis.8 In cases of extreme alkalosis, the patient may be given dilute hydrochloric acid. Saline-resistant alkalosis is treated by addressing
the underlying etiology.
Common acid-base upsets
Generally, if your patient has changes in acid-base homeostasis, youd look for the cause first before intervening to
normalize the pH. But because some acid-base disturbances have a limited number of causes, you can systematically eliminate some potential causes.
Start by looking at the patients arterial blood gas
analysis. Many disorders are mild and dont require treatment, and in some cases, too-hasty treatment can do more
harm than the imbalance itself. Also, critically ill patients
may have more than one acid-base imbalance simultaneously.
The most common acid-base derangements can be divided into four categories: metabolic acidosis, metabolic
alkalosis, respiratory acidosis, and respiratory alkalosis.
Lets look at each and how youd respond.
Respiratory acidosis
In respiratory acidosis, the patients pH is less than 7.35
and his PaCO2 is above 45 mm Hg (the upper limit of normal). Alveolar hypoventilation is the only mechanism that
causes hypercarbia, or a PaCO2 above the upper limit of
normal. The amount of alveolar ventilation necessary to
maintain normal PaCO2 varies depending upon CO2 produced.
The relationship between PaCO2 and plasma HCO3determines arterial pH. Generally, acute increases in PaCO2
are accompanied by only minimal changes in serum
HCO3-. However, over a period of 1 to 3 days, renal conservation of HCO3- results in an increase in pH.9
Chronic respiratory acidosis occurs secondary to a
chronic reduction in alveolar ventilationfor example, in
chronic lung diseases such as chronic obstructive pulmonary disease (COPD). Acute respiratory acidosis is
caused by an acute change in alveolar ventilation; respiratory depression from acute opioid ingestion is one cause.
Treatment for respiratory acidosis is largely supportive, but
if opioid ingestion is suspected, I.V. naloxone may be given
as an antidote.
Metabolic acidosis
Metabolic acidosis is an increase in the amount of absolute
body acid, either from excess production of acids or excessive loss of bicarbonate, sodium, and potassium. Causes of
metabolic acidosis include lactic acidosis, diabetic ketoacidosis, and loss of bicarbonate through severe diarrhea or
bicarbonate wasting through the kidneys or gastrointestinal (GI) tract.
In general, the kidneys attempt to preserve sodium by
exchanging it for excreted H+ or potassium. In the presence
of an H+ load, H+ ions move from the extracellular fluid
into the intracellular fluid.2 For this process to occur,
potassium moves outside the cell into the extracellular
fluid to maintain electroneutrality. In severe acidosis, significant overall depletion of total body potassium stores
can occur despite serum hyperkalemia. This is why I.V.
potassium is given to patients with diabetic ketoacidosis
early in treatment, despite the often-elevated serum potassium level.5,6 External and internal potassium balances are
regulated to maintain an extracellular fluid concentration
of 3.5 to 5.5 mEq/L and a total body content of about 50
mEq/kg (40 mEq/kg in females).6
ED Insider
Respiratory alkalosis
Common in critical care, respiratory alkalosis occurs
when PaCO2 is reduced, causing an increase in pH.
The most common cause of respiratory alkalosis is
increased alveolar ventilation, which can happen in
hyperventilation, mechanical overventilation, hepatic
10
Fall 2008
disease, pregnancy, and septicemia.
Comparing acid-base imbalances
Determining appropriate compensatory
changes in HCO3- is key to determining if the
patient also has a concomitant metabolic disCondition
pH
PaCO2
HCO3order. In chronic respiratory alkalosis, the
Pure respiratory alkalosis
High
Low
Normal
compensatory mechanisms result in mild rePure respiratory acidosis
Low
High
Normal
duction in plasma HCO3- levels to maintain a
near normal or normal pH. This causes a
Pure metabolic alkalosis
High
Normal
High
mixed acid-base disorder, which will be disPure metabolic acidosis
Low
Normal
Low
cussed later.
Treatment of respiratory alkalosis is diMetabolic alkalosis with partial
High
High
High
rected at discovering and correcting the unrespiratory compensation
derlying etiology. For example, if a patient is
Metabolic acidosis with partial
Low
Low
Low
hyperventilating from anxiety, have him
respiratory compensation
breathe into a paper bag. In mechanically ventilated patients with mechanical overventilation, reducing the minute ventilation or tidal volume will
anion gap, then a non-anion gap metabolic acidosis is conincrease PaCO2 and reduce pH. Monitor the patient
sidered to be present and is worsening the anion gap aciclosely, because a rapid reduction of PaCO2 in a patient
dosis. For more examples, see Comparing acid-base
with chronic respiratory alkalosis may cause acute metaimbalances.
bolic acidosis.10
Caring for the critically ill
Mixed acid-base imbalances
Acid-base imbalances are common in critically ill patients.
By understanding the basic physiology of acid-base balance
and what can go wrong, you can help your patient get back
in balance.
When a patient has two or three acid-base imbalances simultaneously, hes said to have a mixed acid-base imbalance.7 Examples include:
respiratory alkalosis or acidosis that shrouds a metabolic
acidosis or alkalosis
metabolic alkalosis or acidosis that shrouds another
metabolic alkalosis acidosis.
Combined respiratory and metabolic imbalances may
occur when the respiratory system compensates inappropriately for metabolic imbalances. Look at the difference
between the patients observed PaCO2 and the calculated
changes in PaCO2, or the observed or expected change in
HCO3-.2,11 If the observed PaCO2 is higher than the calculated PaCO2, the patient has respiratory acidosis with a
mixed metabolic disturbance. If the observed PaCO2 is
lower than the calculated PaCO2, the patient has respiratory
alkalosis mixed with a metabolic imbalance. Generally, the
PaCO2 should be similar to the two last digits of the patients pH. For example, if the patients pH is 7.25, youd
expect his PaCO2 to be about 25 mm Hg.1
Mixed metabolic acidosis and alkalosis can be identified by calculating the anion gap.11 The anion gap is an approximate measure of the additional amount of acid in the
body; the HCO3- should decrease by about an amount
equaling the increase in the anion gap. If the HCO3- is
higher than the calculated increase of the anion gap, a chief
metabolic alkalosis is mixed with the metabolic acidosis.
Conversely, if the HCO3- is lower than the increase of the
Fall 2008
REFERENCES
1. Marino PL, Sutin KM. Acid-base interpretations. In Marino PL (ed). The ICU
Book, 3rd edition. Lippincott Williams & Wilkins, 2006.
2. Disney JD. Acid-base disorders. In Marx JA, et al. (eds). Rosens Emergency
Medicine: Concepts and Clinical Practice, 5th edition. Mosby, Inc., 2002.
3. Docherty B, Foudy C. Homeostasis. Part 4: fluid balance. Nursing Times.
102(17):22-23, April 25-May 1, 2006.
4. Lemann J, et al. Bone buffering of acid and base in humans. American Journal of
Physiology. Renal Physiology. 285(5):F811-F832, November 2003.
5. Hurlock-Chorostecki C. Managing diabetic ketoacidosis: the role of the ICU
nurse in an endocrine emergency. Dynamics. 15(1):18-22, Spring 2004.
6. White NH. Management of diabetic ketoacidosis. Reviews in Endocrine and
Metabolic Disorders. 4(4):343-353, December 2003.
7. Adrogue HJ. Mixed acid-base disturbances. Journal of Nephrology. 19(Suppl
9):S97-S103, March-April 2006.
8. Funk GC, Doberer D, Heinze G, et al. Changes of serum chloride and metabolic
acid-base state in critical illness. Anaesthesia. 59(11):1111-1115, November 2004.
9. Frank JA, et al. General principles of managing the patient with respiratory failure. In George RB (ed). Chest Medicine: Essentials of Pulmonary and Critical Care
Medicine, 4th edition. Lippincott Williams & Wilkins, 2000.
10. McPhee SJ, Tierney LM. Fluid and electrolyte disorders. In McPhee SJ, et al.
(eds). Current Medical Diagnosis and Treatment, 46th edition. McGraw-Hill Cos.,
2007.
11. Story DA. Bench-to-bedside review: A brief history of clinical acid-base.
Critical Care. 8(4):253-258, August 2004.
At the University of Alabama at Birmingham, Susan Appel is an associate professor, and Charles A. Downs is an instructor.
Adapted from Appel SJ, Downs CA, Steady a disturbed equilibrium: Accurately
interpret the acid-base balance of acutely ill patients. Nursing2007 Critical
Care, July 2007.
11
ED Insider
Vous aimerez peut-être aussi
- What Is Respiratory Alkalosis?Document3 pagesWhat Is Respiratory Alkalosis?Lorenn AdarnaPas encore d'évaluation
- Pharmacology TMCExam TipsDocument14 pagesPharmacology TMCExam TipsRyn Shadow100% (1)
- Respiratory MedicationsDocument18 pagesRespiratory Medicationsapi-338095748Pas encore d'évaluation
- 6 - Hemodynamic Disorders PDFDocument69 pages6 - Hemodynamic Disorders PDFJames Chua0% (1)
- ABG Analysis: 6-Step ApproachDocument22 pagesABG Analysis: 6-Step Approachrajan40dmcPas encore d'évaluation
- Respiratory PathophysiologiesDocument1 pageRespiratory PathophysiologiesTori IkeharaPas encore d'évaluation
- Implications For Secretion ClearanceDocument27 pagesImplications For Secretion ClearancearbazPas encore d'évaluation
- Introduction To Wireless Communication - Radio CommunicationDocument21 pagesIntroduction To Wireless Communication - Radio CommunicationYas773Pas encore d'évaluation
- Resp Medicine NotesDocument95 pagesResp Medicine Noteshugolucas182100% (1)
- C27 and C32 Generator With EMCP4.2 Electrical SystemDocument2 pagesC27 and C32 Generator With EMCP4.2 Electrical SystemAngel BernacheaPas encore d'évaluation
- Management of Acute Metabolic Acidosis in The ICU Sodium BicarbonateDocument6 pagesManagement of Acute Metabolic Acidosis in The ICU Sodium Bicarbonatecastillojess100% (1)
- Pulmonary Auscultation PDFDocument5 pagesPulmonary Auscultation PDFThatikala AbhilashPas encore d'évaluation
- Acid Base Disorders JAPIDocument5 pagesAcid Base Disorders JAPIVitrag_Shah_1067Pas encore d'évaluation
- PFT Reveals Lung FunctionDocument35 pagesPFT Reveals Lung FunctionMartha ChasePas encore d'évaluation
- Understanding Acid Base Balance.3Document3 pagesUnderstanding Acid Base Balance.3Hazel Vivian Soliz AlconzPas encore d'évaluation
- 0bbamechanical VentilationDocument85 pages0bbamechanical VentilationKamal MohamedPas encore d'évaluation
- Basics of Ventilatory SupportDocument43 pagesBasics of Ventilatory SupportAdhithya BhatPas encore d'évaluation
- Ledger - Problems and SolutionsDocument1 pageLedger - Problems and SolutionsDjamal SalimPas encore d'évaluation
- Ventilation, Perfusion and Ventilation-Perfusion RelationshipsDocument14 pagesVentilation, Perfusion and Ventilation-Perfusion RelationshipspuchioPas encore d'évaluation
- Acid Base ImbalanceDocument50 pagesAcid Base ImbalanceDian Pratiwi BurnamaPas encore d'évaluation
- How To Read Arterial Blood Gas .PTDocument36 pagesHow To Read Arterial Blood Gas .PTMohd Erham bin JonohPas encore d'évaluation
- Guidelines For Sedation and Anesthesia in GI Endos PDFDocument11 pagesGuidelines For Sedation and Anesthesia in GI Endos PDFHernan RuedaPas encore d'évaluation
- ABG InterpretationDocument10 pagesABG InterpretationNisha MathewPas encore d'évaluation
- ClubbingDocument44 pagesClubbingAkshat Srivastava100% (1)
- Acid-Base Disorders NotesDocument10 pagesAcid-Base Disorders NotesLovely100% (1)
- Basic Ventilator y ModesDocument47 pagesBasic Ventilator y ModesAlina VanceaPas encore d'évaluation
- Aprv Power PointDocument96 pagesAprv Power PointAndi HidayatPas encore d'évaluation
- Human Anatomy and Physiology II: Biology 1414 Unit 8 Metabolism and NutritionDocument103 pagesHuman Anatomy and Physiology II: Biology 1414 Unit 8 Metabolism and Nutritionciroj25Pas encore d'évaluation
- Assessment of Fluid Responsiveness Recent Advances. OkDocument6 pagesAssessment of Fluid Responsiveness Recent Advances. OkLeiniker Navarro Rey100% (1)
- Acid Base TutorialDocument47 pagesAcid Base TutorialDiah Puspita Rini100% (2)
- Acid-Base Homeostasis: Dr. Abeer KhurshidDocument42 pagesAcid-Base Homeostasis: Dr. Abeer Khurshidسلة فواكة100% (2)
- Assessment of Metabolic AcidosisDocument34 pagesAssessment of Metabolic Acidosisfatha100% (1)
- APRVDocument20 pagesAPRVivanrom100% (1)
- Module 5A: Dental Management of Patients With Asthma: Prepared By: Dr. Maria Luisa Ramos - ClementeDocument27 pagesModule 5A: Dental Management of Patients With Asthma: Prepared By: Dr. Maria Luisa Ramos - Clementeelaine100% (1)
- Concentration of Urine: Maj DR Shavana R.L RanaDocument22 pagesConcentration of Urine: Maj DR Shavana R.L RanaChandan Sah100% (1)
- Acid Base DisordersDocument11 pagesAcid Base DisordersS100% (1)
- Financial Modeling Interview Questions AnsweredDocument6 pagesFinancial Modeling Interview Questions AnsweredBHAVEN ASHOK SINGHPas encore d'évaluation
- Acid Base HomeostasisDocument11 pagesAcid Base HomeostasisOrion JohnPas encore d'évaluation
- Approach To The Child With Metabolic Acidosis - UDocument3 pagesApproach To The Child With Metabolic Acidosis - URishi Shrestha100% (1)
- VFTO DocumentationDocument119 pagesVFTO DocumentationSheri Abhishek ReddyPas encore d'évaluation
- Back to Basics: Understanding Acids and BasesDocument45 pagesBack to Basics: Understanding Acids and BasesJosepPas encore d'évaluation
- Physiology of RespirationDocument2 pagesPhysiology of RespirationIOSRjournalPas encore d'évaluation
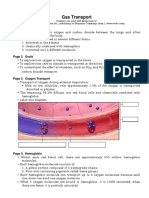
- Gas Transport in the BloodDocument19 pagesGas Transport in the BloodMarilia BonorinoPas encore d'évaluation
- Pathophysiology of Septic Encephalopathy A ReviewDocument6 pagesPathophysiology of Septic Encephalopathy A ReviewFerdila Putri A DilaPas encore d'évaluation
- Foot Drop - CBLDocument16 pagesFoot Drop - CBLbpt2100% (1)
- Anesthesia Cheat Sheet: Dogs CatsDocument3 pagesAnesthesia Cheat Sheet: Dogs CatsJoão Pedro Pereira100% (1)
- Lactic Acidosis: An Update: Jansen Seheult, Gerard Fitzpatrick and Gerard BoranDocument12 pagesLactic Acidosis: An Update: Jansen Seheult, Gerard Fitzpatrick and Gerard Borangasman2003Pas encore d'évaluation
- NEJM 2014 Fundamentals of Lung AuscultationDocument7 pagesNEJM 2014 Fundamentals of Lung AuscultationFelipe CeaPas encore d'évaluation
- Regional AnesthesiaDocument54 pagesRegional AnesthesiaIdza Fariha AfriPas encore d'évaluation
- Sport Diving-CompletedDocument66 pagesSport Diving-CompletedMuthu KumarPas encore d'évaluation
- Renal Regulation of Acid-Base BalanceDocument10 pagesRenal Regulation of Acid-Base BalanceMarianela Vásquez ArayaPas encore d'évaluation
- Lung AuscultationDocument62 pagesLung AuscultationOlea CroitorPas encore d'évaluation
- Lecture notes on human respiratory system physiologyDocument33 pagesLecture notes on human respiratory system physiologyMiles HuiPas encore d'évaluation
- Arterial Blood Gas Analysis GuideDocument43 pagesArterial Blood Gas Analysis GuideKresna Dharma SuryanaPas encore d'évaluation
- Impaired Gas ExchangeDocument4 pagesImpaired Gas ExchangeNuraini Hamzah100% (1)
- Surviving Sepsis Campaign 2016 Guidelines Presentation Final RevisiedDocument32 pagesSurviving Sepsis Campaign 2016 Guidelines Presentation Final RevisiedAdli Wafi Jabbar100% (1)
- Uptake and Distribution of Volatile AnestheticsDocument22 pagesUptake and Distribution of Volatile AnestheticsSuresh Kumar100% (3)
- How To Take A Set of Arterial Blood Gases (Abgs) : Think Lemon Juice in A Salted Paper Cut ..It Does Smart A Little!Document48 pagesHow To Take A Set of Arterial Blood Gases (Abgs) : Think Lemon Juice in A Salted Paper Cut ..It Does Smart A Little!shiv dattaPas encore d'évaluation
- Copd HandoutDocument6 pagesCopd Handoutapi-272951876Pas encore d'évaluation
- Describe The Factors Affecting Cardiac OutputDocument6 pagesDescribe The Factors Affecting Cardiac OutputSis SukarnoPas encore d'évaluation
- Physiology MnemonicsDocument1 pagePhysiology MnemonicsSadeesh Niroshan KodikaraPas encore d'évaluation
- Complications of General Anesthesia (Summary)Document19 pagesComplications of General Anesthesia (Summary)Hassan.shehri100% (2)
- Vascular Responses to PathogensD'EverandVascular Responses to PathogensFelicity N.E. GavinsPas encore d'évaluation
- Understanding Acid-Base BalanceDocument3 pagesUnderstanding Acid-Base Balanceabxaz100% (1)
- Effect of HPV vaccine in women with cervical and vulvar diseaseDocument1 pageEffect of HPV vaccine in women with cervical and vulvar diseaseYuniParaditaDjunaidiPas encore d'évaluation
- Bitemporal Hemianopia from Pituitary AdenomasDocument1 pageBitemporal Hemianopia from Pituitary AdenomasYuniParaditaDjunaidiPas encore d'évaluation
- JURNALDocument20 pagesJURNALYuniParaditaDjunaidiPas encore d'évaluation
- Anatomy, Physiology, and Immunology of The Nose, Paranasal Sinuses, and FaceDocument1 pageAnatomy, Physiology, and Immunology of The Nose, Paranasal Sinuses, and FaceYuniParaditaDjunaidiPas encore d'évaluation
- Otolaryngologist Guide to Diagnosing Common Headaches and Facial PainDocument15 pagesOtolaryngologist Guide to Diagnosing Common Headaches and Facial PainYuniParaditaDjunaidiPas encore d'évaluation
- Ballenger Chapter 25Document2 pagesBallenger Chapter 25YuniParaditaDjunaidiPas encore d'évaluation
- Manual of Otorhinolaryngology Head and Neck Surgery: Ballenger'sDocument9 pagesManual of Otorhinolaryngology Head and Neck Surgery: Ballenger'sYuniParaditaDjunaidiPas encore d'évaluation
- ABC of ENT RSADocument2 pagesABC of ENT RSAYuniParaditaDjunaidiPas encore d'évaluation
- Acids-Bases Theory ExplainedDocument7 pagesAcids-Bases Theory ExplainedYuniParaditaDjunaidiPas encore d'évaluation
- Nej MR A 1503102Document12 pagesNej MR A 1503102YuniParaditaDjunaidiPas encore d'évaluation
- AcidDocument5 pagesAcidYuniParaditaDjunaidiPas encore d'évaluation
- Nej MR A 1503102Document12 pagesNej MR A 1503102YuniParaditaDjunaidiPas encore d'évaluation
- Acids-Bases Theory ExplainedDocument7 pagesAcids-Bases Theory ExplainedYuniParaditaDjunaidiPas encore d'évaluation
- Tugas TranslateDocument9 pagesTugas TranslateYuniParaditaDjunaidiPas encore d'évaluation
- Tectonics, Vol. 8, NO. 5, PAGES 1015-1036, October 1989Document22 pagesTectonics, Vol. 8, NO. 5, PAGES 1015-1036, October 1989atoinsepePas encore d'évaluation
- Idioma IV Cycle Q1 Exam (2021-1) - STUDENTS ANSWERDocument9 pagesIdioma IV Cycle Q1 Exam (2021-1) - STUDENTS ANSWEREdward SlaterPas encore d'évaluation
- Galen and The Antonine Plague - Littman (1973)Document14 pagesGalen and The Antonine Plague - Littman (1973)Jörgen Zackborg100% (1)
- Handout Week10.1Document7 pagesHandout Week10.1Antoniette Niña YusonPas encore d'évaluation
- TK17 V10 ReadmeDocument72 pagesTK17 V10 ReadmePaula PérezPas encore d'évaluation
- Analyzing Visual TextsDocument4 pagesAnalyzing Visual Textsapi-582845240Pas encore d'évaluation
- 8th Edition of The AJCC - TNM Staging System of Thyroid Cancer - What To Expect (ITCO#2)Document5 pages8th Edition of The AJCC - TNM Staging System of Thyroid Cancer - What To Expect (ITCO#2)Valentina IndahPas encore d'évaluation
- Grade 9 SyllabusDocument23 pagesGrade 9 SyllabusClopzPas encore d'évaluation
- Prayer of SubmissionDocument3 pagesPrayer of SubmissionLindaLindyPas encore d'évaluation
- PHY3 BJune 2004Document1 pagePHY3 BJune 2004api-3726022Pas encore d'évaluation
- 1 Session1 DRR ConceptsDocument43 pages1 Session1 DRR ConceptsHoneylet Ü FerolPas encore d'évaluation
- Mahabharata Book 9 Shalya ParvaDocument413 pagesMahabharata Book 9 Shalya Parvaavacdis1969Pas encore d'évaluation
- Dslam Commissioning Steps Punjab For 960 PortDocument8 pagesDslam Commissioning Steps Punjab For 960 Portanl_bhn100% (1)
- RTL8185 Windows7 FixDocument2 pagesRTL8185 Windows7 FixJamesHackPas encore d'évaluation
- Durgah Ajmer Sharif 1961Document19 pagesDurgah Ajmer Sharif 1961Deepanshu JharkhandePas encore d'évaluation
- VR 2200 CatalogueDocument4 pagesVR 2200 Catalogueh.torabyPas encore d'évaluation
- Lab No.7: Measurement of Coupling Coefficient, Directivity and Insertion Loss of A Directional CouplerDocument3 pagesLab No.7: Measurement of Coupling Coefficient, Directivity and Insertion Loss of A Directional CouplerM. Ahmad RazaPas encore d'évaluation
- Che 430 Fa21 - HW#5Document2 pagesChe 430 Fa21 - HW#5Charity QuinnPas encore d'évaluation
- Indian Standard: Hexagon Head Bolts, Screws and Nuts of Product Grades A and BDocument11 pagesIndian Standard: Hexagon Head Bolts, Screws and Nuts of Product Grades A and BJignesh TrivediPas encore d'évaluation
- Celene Stained Glass ColoursDocument4 pagesCelene Stained Glass ColoursRathna ChalamPas encore d'évaluation
- Justification: Justification: Doctrine of Council of TrentDocument4 pagesJustification: Justification: Doctrine of Council of TrentMihai SarbuPas encore d'évaluation
- HavellsDocument4 pagesHavellsanurag_iiitmPas encore d'évaluation
- WEEK 1 Materi-EM101-M01-The Foundation of Business 2Document48 pagesWEEK 1 Materi-EM101-M01-The Foundation of Business 2ddhani299Pas encore d'évaluation
- Apostolic Faith: Beginn NG of World REV VALDocument4 pagesApostolic Faith: Beginn NG of World REV VALMichael HerringPas encore d'évaluation
- Climate Change ReactionDocument2 pagesClimate Change ReactionAngelika CotejoPas encore d'évaluation