Académique Documents
Professionnel Documents
Culture Documents
Tiroid Tiroid
Transféré par
naotonaoiTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Tiroid Tiroid
Transféré par
naotonaoiDroits d'auteur :
Formats disponibles
CANADIAN ASSOCIATION OF GENERAL SURGEONS AND ACS,
EVIDENCE-BASED REVIEWS IN SURGERY
Treatment Options for Graves Disease
Prosanto K Chaudhury, MD, FACS, Peter Angelos, MD, FACS, Janice L Pasieka, MD, FACS; for Members of
the Evidence-Based Reviews in Surgery Group
The term evidence-based medicine was first coined by Sackett and colleagues1 as the conscientious, explicit and judicious use of current best evidence in making decisions
about the care of individual patients. The key to practicing
evidence-based medicine is applying the best current
knowledge to decisions in individual patients. Medical
knowledge is continually and rapidly expanding, and it is
impossible for an individual clinician to read all the medical literature. For clinicians to practice evidence-based
medicine, they must have the skills to read and interpret the
medical literature so that they can determine the validity,
reliability, credibility, and utility of individual articles.
These skills are known as critical appraisal skills. Generally,
critical appraisal requires that the clinician have some
knowledge of biostatistics, clinical epidemiology, decision
analysis, and economics as well as clinical knowledge.
The Canadian Association of General Surgeons (CAGS)
and the American College of Surgeons (ACS) jointly sponsor a program titled Evidence-Based Reviews in Surgery
(EBRS), supported by an educational grant from Ethicon
Inc and Ethicon Endo Surgery Inc. The primary objective
of this initiative is to help practicing surgeons improve their
critical appraisal skills. During the academic year, 8 clinical
articles are chosen for review and discussion. They are selected not only for their clinical relevance to general surgeons, but also because they cover a spectrum of issues
important to surgeons; for example, causation or risk factors for disease, natural history or prognosis of disease, how
to quantify disease (measurement issues), diagnostic tests
and the diagnosis of disease, and the effectiveness of treatment. Both methodologic and clinical reviews of the article
are performed by experts in the relevant areas and posted
on the EBRS Web site. A listserve discussion is held where
participants can discuss the monthly article. Fellows and
candidates of the College can access Evidence Based Reviews in Surgery through the American College of Surgeons Web site (www.facs.org). All journal articles and reviews are available electronically through the Web site.
Currently we have a library of 50 articles and reviews,
which can be accessed at any time. Each October, a new set
of articles will be available each month until May. Surgeons
who participate in the current (modules) packages can receive CME credits by completing a series of multiple choice
questions. Additional information about EBRS is on the
ACS Web site or by email to the administrator, Marg McKenzie at mmckenzie@mtsinai.on.ca.
In addition to making the reviews available through the
ACS and CAGS Web sites, 4 of the reviews are published in
condensed versions in the Canadian Journal of Surgery, 4
in the Journal of the American College of Surgeons, and 4 in
Diseases of Colon and Rectum each year.
REFERENCE
1. Evidence-Based Medicine Working Group. Evidence-based medicine. JAMA 1992;268:24202425.
roid medication, radioactive iodine [RAI], and total
thyroidectomy).
SELECTED ARTICLE
Treatment Options for Graves Disease:
A Cost-Effectiveness Analysis
Haejin I, Pearce EN, Wong AK, et al. J Am Coll Surg
2009;209:170179.
Setting: Treatment efficacy and complication data were
derived from a literature review. Costs were examined from
a health care system perspective using actual Medicare reimbursement rates to an urban university hospital.
ABSTRACT
Objective: To determine the most cost effective option
for treating Graves disease after 18 months of antithyroid
medication (ATM).
Base case: Thirty-year-old nonpregnant woman without a large goiter, ophthalmopathy, or palpable nodules,
who has failed to remain euthyroid after completion of 18
months of ATM.
Design: A decision tree model was used to examine the
cost effectiveness of 3 treatment options (lifelong antithy-
Interventions: Each treatment option incorporated all
associated events, their probabilities, and costs including
2011 by the American College of Surgeons
Published by Elsevier Inc.
806
ISSN 1072-7515/11/$36.00
doi:10.1016/j.jamcollsurg.2011.09.015
Vol. 213, No. 6, December 2011
medications, laboratory tests, clinic visits, treatment costs,
costs associated with adverse events, such as agranulocytosis and recurrent laryngeal nerve damage; and costs associated with change in treatment for failed intervention.
Main outcomes: Outcomes were measured in qualityadjusted life-years (QALY).
Results: Total thyroidectomy was the most costeffective strategy, resulting in a gain of 1.32 QALYs compared with RAI (at an additional cost of $9,594) and an
incremental cost-effectiveness ratio of $7,240/QALY. RAI
was the least costly option at $23,600, but provided the
least QALY (25.08). Once the cost of total thyroidectomy
exceeds $19,300, the incremental cost-effectiveness ratio of lifelong ATM and total thyroidectomy reverse,
and lifelong ATM becomes the more cost-effective strategy at $15,000/QALY.
Conclusions: The findings demonstrate that total thyroidectomy is more cost effective than RAI or lifelong
ATM in these patients; this continues until the cost of total
thyroidectomy becomes greater than $19,300.
Commentary: Graves disease is an autoimmune disorder that affects approximately 0.5% of the North American
population. Graves disease is the most common cause of
primary hyperthyroidism. Treatment of hyperthyroidism is
essential because overt manifestations of the condition can
lead to long-term effects on the heart, bones, and psychological well being of the patient. Immediate control of
symptoms is obtained with the use of beta-blockers; the
antithyroidial drugs take effect and block further syntheses
of thyroxin production. The goals of therapy are to control symptoms and restore the patient to a euthyroid
state. There are 3 modes of therapy for the treatment of
Graves disease: antithyroidal medication, RAI, and total thyroidectomy.
Typically, patients with Graves disease are treated with
ATM for a period of time in hopes that the disease will
resolve spontaneously. Remission, depending on the size of
the gland, can occur in 30% to 50% of patients after a 12to 18-month course of the drugs. After 12 to 18 months,
most patients are faced with 3 possible treatment choices:
continue the ATM for an indefinite period of time; receive
RAI; or have a total thyroidectomy. The authors have correctly assumed that the best surgical option is a total thyroidectomy, and yet some surgeons continue to offer the
option of a subtotal thyroidectomy to their patients. In
contrast to a subtotal thyroidectomy, patients undergoing a
total thyroidectomy will predictably require thyroid hormone replacement but will have a significantly lower risk of
recurrence.
Evidence-Based Reviews in Surgery
807
In counseling such patients with Graves disease, the
total thyroidectomy option is the one that has the most
readily identifiable risks. As a result, many surgeons look at
total thyroidectomy as something that should be strongly
considered by patients only if there is a reason why ATM or
RAI is not a safe option. For example, if the patient is
pregnant or has suspicious nodules, RAI is not a safe option, or if a patient has had a bad reaction to the ATM,
continuing medication is not a good option. Surgeons in
the US are not commonly sent patients for total thyroidectomy for Graves disease unless there is some other reason
why RAI or continuing ATMs for long periods of time is
not safe.
Total thyroidectomy, when done by experienced surgeons, is safe and provides an immediate and permanent
solution to the hyperthyroid state. Surgery should continue
to be used in all patients who fail to become euthyroid with
other treatments, patients with very large goiters, in whom
RAI would likely fail or is contraindicated, and those with
significant Graves ophthalmopathy. This analysis provides
further evidence that thyroidectomy should also be considered the first line treatment option in patients with refractory Graves disease because the long-term benefits and
cost-effectiveness of this treatment are superior to lifelong
medication and RAI. Although thyroidectomy is more
costly up front, the benefit is realized in the long-term. It is
important, however, to recognize that this benefit is realized only when the thyroidectomy is done by an experienced surgeon who has a low risk profile and understands
the complexity of operating on a patient with Graves disease. This study provides a rational basis for a physician to
recommend a total thyroidectomy to patients even if they
have no contraindication to ATM or RAI. Namely, total
thyroidectomy is the most cost-effective strategy as long as
the cost of total thyroidectomy does not exceed $19,300.
The authors also report the results of sensitivity analyses for
key variables that would influence medical decisions or
have substantial medical consequences. The cost of thyroidectomy had the greatest influence on the results. As
long as the cost of total thyroidectomy remained less than
$19,300, total thyroidectomy remained the most costeffective strategy. Other variables, including cost of medication, cost of RAI, patient age, probability of cancer with
medication or RAI, success rate of RAI, rate of hypothyroidism with RAI, and complication rates of total thyroidectomy, did not influence the results. The sensitivity analyses are included as an online supplement (Appendix: 2).
This study has several limitations. It was based on retrospective nonexperimental data supplemented by expert
opinion to generate probabilities and quality-of-life adjustment factors. In addition, utilities were not derived based
808
Evidence-Based Reviews in Surgery
on patient opinions. So, it is possible that patient assessments of the utility or disutility of different disease states
might differ considerably from those that were assigned by
the authors. In addition, costs were based on the reimbursement structure for Medicare as representative of US
payors. Actual 2007 Medicare reimbursements to a large
urban university hospital were used to calculate the cost of
treatment. Medication costs were obtained from average
US wholesale prices. Future health care costs were computed using an inflation rate of 5%. A standard discount
rate of 3% was applied to both cost and effectiveness, as
recommended by the Panel on Cost-Effectiveness in
Health and Medicine. However, although this methodology is the easiest, there are some concerns about it. The first
limitation of this method is that the price is not always
the same as the actual cost of delivering the service or
product. These variances may occur because the price was
established some time previously and does not reflect current costs; it may be due to the bargaining power of health
care institutions, third-party payers, and the profit margin
of for-profit health care systems. The second limitation is
that the results of the analysis may not be generalizable to
other systems. Because the cost of each resource is not
explicitly stated, it is not possible to substitute the cost that
may be incurred in another system in the analysis to determine if the results of the analysis are robust. Having said
that, Medicare reimbursement is not a bad way of estimating cost in the US setting because these rates are established
centrally and are not subject to bargaining and volume
discounts.
In summary, the analysis by Haejin and colleagues is a
timely article. This review brings to light the role that thyroidectomy can have in the treatment of Graves disease. It
is likely that the surgeons role will expand in the years to
come, with the increasing awareness and concerns about
the long-term impact of RAI and the increasing emphasis
J Am Coll Surg
on cost-effective therapies. Surgeons need to be more involved in the first line decision process when it comes to
treatment of Graves disease. Thyroidectomy is a valid
treatment option and it is only the surgeon who can accurately explain the surgical risk vs benefit of this modality to
the patient.
The Evidence-Based Reviews in Surgery Group
Comprises:
Members of the EBRS Steering Committee
Nancy N Baxter, MD, FACS, Toronto, ON Canada
Karen J Brasel, MD, FACS, Milwaukee, WI
Carl J Brown, MD, Vancouver, BC Canada
Prosanto K Chaudhury, MD, Montreal, QC Canada
C Suzanne Cutter, MD, Los Angeles, CA
Celia M Divino, MD, FACS, New York, NY
Elijah Dixon, MD, FACS, Calgary AB, Canada
Luc Dubois, MD, London, ON Canada
G William N Fitzgerald, MD, St. Anthony, NL Canada
S Morad Hameed, MD, FACS, Vancouver, BC Canada
Harry J Henteleff, MD, FACS, Halifax, NS Canada
Andrew W Kirkpatrick, MD, FACS, Calgary, AB Canada
Steven Latosinsky, MD, London, ON Canada
Tara M Mastracci, MD, Cleveland, OH
Robin S McLeod, MD, FACS, Toronto, ON Canada
Arden M Morris, MD, FACS, Ann Arbor, MI
Leigh A Neumayer, MD, FACS, Salt Lake City, UT
Larissa K Temple, MD, FACS, New York, NY
Marg McKenzie, RN, Toronto, ON Canada
Vous aimerez peut-être aussi
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5795)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (74)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (400)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Hypocalcemia in NewbornsDocument2 pagesHypocalcemia in NewbornsEunice Lan ArdientePas encore d'évaluation
- Pathology Supplement Handout Nov 2018Document25 pagesPathology Supplement Handout Nov 2018Zak Kaz100% (2)
- Case 4 Reproductive Block PBLDocument9 pagesCase 4 Reproductive Block PBLFarisPas encore d'évaluation
- Psychosis and Memory Loss by Dr. Shivan MahabirDocument41 pagesPsychosis and Memory Loss by Dr. Shivan MahabirShivan A.C.Pas encore d'évaluation
- Drug Study FluimucilDocument2 pagesDrug Study FluimucilJemina Rafanan Racadio0% (1)
- Capstone ProjectDocument11 pagesCapstone ProjectDave Matthew LibiranPas encore d'évaluation
- RX Protocol by DR - Anwarul Azim PDFDocument120 pagesRX Protocol by DR - Anwarul Azim PDFGB Majumder100% (1)
- Current Status of Health and Disease Burden in IndiaDocument23 pagesCurrent Status of Health and Disease Burden in IndiaKavi rajput100% (1)
- XN-1500 10p ENDocument5 pagesXN-1500 10p ENHarika PutraPas encore d'évaluation
- Acute Limb Ischemia Acute Limb Ischemia N SuddenDocument43 pagesAcute Limb Ischemia Acute Limb Ischemia N SuddenSWETHAPas encore d'évaluation
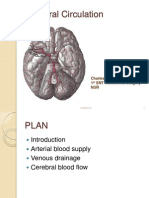
- Cerebral CirculationDocument85 pagesCerebral CirculationCharles Nkurunziza100% (2)
- Presentation On Health AssessmentDocument12 pagesPresentation On Health AssessmentSimran ChauhanPas encore d'évaluation
- Information Text by DR Ali EvliceDocument5 pagesInformation Text by DR Ali Evlicehitler88Pas encore d'évaluation
- National Integrated Emergency Medicine TrainingDocument274 pagesNational Integrated Emergency Medicine TrainingAddisu AdanePas encore d'évaluation
- Status EpilepticusDocument17 pagesStatus EpilepticusXavier AbrilPas encore d'évaluation
- Aerobic and Anaerobic ExercisesDocument3 pagesAerobic and Anaerobic ExercisesBonak na BataPas encore d'évaluation
- Drug Analysis: Submitted By: GALICINAO, Gretta Shalou GDocument9 pagesDrug Analysis: Submitted By: GALICINAO, Gretta Shalou GggalicinaoPas encore d'évaluation
- Multi-Frequency and Multi-Component TympanometryDocument8 pagesMulti-Frequency and Multi-Component TympanometryEstudiantede FonoaudiologíaPas encore d'évaluation
- Practical Guide To Insulin Therapy in Type 2 Diabetes: January 2011Document91 pagesPractical Guide To Insulin Therapy in Type 2 Diabetes: January 2011leeyie22Pas encore d'évaluation
- Vaccines and Vaccination History and Emerging IssuesDocument15 pagesVaccines and Vaccination History and Emerging IssuesMěđ SimoPas encore d'évaluation
- Imaging of Solitary and Multiple Pulmonary NodulesDocument75 pagesImaging of Solitary and Multiple Pulmonary NodulesAnshulVarshneyPas encore d'évaluation
- Sophia Guy ResumeDocument3 pagesSophia Guy Resumeapi-677670066Pas encore d'évaluation
- Mirikizumab As Induction and Maintenance Therapy For UlcerativeDocument15 pagesMirikizumab As Induction and Maintenance Therapy For Ulcerativesreebhahun satishPas encore d'évaluation
- Crisis Management Covid 19Document22 pagesCrisis Management Covid 19jon ellePas encore d'évaluation
- Comparative Study of Posterior Stabilizing VS Cruciate Retaining Prosthesis in Total Knee ReplacementDocument15 pagesComparative Study of Posterior Stabilizing VS Cruciate Retaining Prosthesis in Total Knee ReplacementIJAR JOURNALPas encore d'évaluation
- Homeostasis and The Excretory SystemDocument21 pagesHomeostasis and The Excretory Systemmark smithPas encore d'évaluation
- ER Nurse: NMC Speciality Hospital Al Salam / Riyahd, Kingdom of Saudi Arabia / October 2018 To October 2020Document5 pagesER Nurse: NMC Speciality Hospital Al Salam / Riyahd, Kingdom of Saudi Arabia / October 2018 To October 2020Alman MacasindilPas encore d'évaluation
- Indices MeasuringDocument27 pagesIndices Measuringdinesh11rPas encore d'évaluation
- Introduction History Examination (Prosthodontics)Document37 pagesIntroduction History Examination (Prosthodontics)sarah0% (1)