Académique Documents
Professionnel Documents
Culture Documents
Ajopht 1977 Rush
Transféré par
remotmCopyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Ajopht 1977 Rush
Transféré par
remotmDroits d'auteur :
Formats disponibles
ACUTE MACULAR NEURORETINOPATHY
J A M E S A. R U S H , M . D .
Charlottesville,
Virginia
acuity was 6/6 (20/20) in each eye. Both anterior
segments were normal. Direct and indirect ophthalmoscopy demonstrated pertinent findings restricted
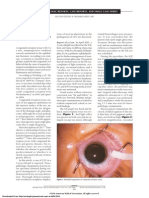
to the macula of the left eye. In the fovea, there were
three discrete, although faint, reddish-brown lesions
that had an arrowhead or a wedge shape, pointing
toward a normal foveolar light reflex (Fig. 1). Biomicroscopy through a Goldmann contact lens showed
three superficial, vague areas of dusty, dusky deposits that merged imperceptibly with normal retina.
There were no deep areas of altered pigmentation or
exudative deposits in the retina. No commonly identifiable changes in retinal structure were noted.
Fluorescein angiograms were normal (Fig. 2),
confirming the integrity of the retinal pigment epithelium and retinal vasculature, and substantiating the
gossamer-like quality of the observed lesions. The
patient was able to reproduce scotomas on an
Amsler grid (Fig. 3). Goldmann perimetry revealed
no abnormality other than that on the Amsler grid,
although the varying illuminance and size of the test
objects corresponded well with both the densities of
the ophthalmoscopically observed lesions and the
subjective appreciation described by the patient.
No change in the visual acuity, and no change in
the subjective scotomas, occurred in six months of
follow-up observation. The lesions neither coalesced nor regressed. The patient still finds the
scotomas most bothersome, but has refused to consider cessation of the oral contraceptive hormone.
Recently, B o s and D e u t m a n examined
four patients with an unusual macular
affliction characterized by minimal depression of vision and scotomas that corresponded to peculiar foveal lesions situated in the superficial retina. T h e y termed
this illness acute macular neuroretinopathy.
1
Their four patients were women, aged
2 4 to 3 3 years, and all were taking oral
contraceptives. T w o of the four patients
had experienced a mild, apparently infectious illness: one had an acute "enteritis,"
and the other, " a bout of influenza."
T h r e e of the four patients had bilateral
involvement, although one of these did
not manifest simultaneous bilateral involvement. F u n d i and visual fields were
abnormal, but fluorescein angiograms in
all four, and electroretinograms with
electro-oculograms ( E O G ) in both patients tested, were normal.
Recently, I observed a woman with a
remarkably
similar malady. T o my
knowledge, this is the first case reported
in the United States.
CASE REPORT
A 24-year-old white woman complained of "seeing spots in her left eye." She had been healthy until
late in December 1975, when she contracted "a
cold." Six weeks later, she developed an acute
pharyngitis, that, although culture-negative, was
treated with erythromycin. When her symptoms
resolved two weeks later, she noted three tearshaped spots in front of her left eye. They were
constant, and always appeared where she "focused."
At an ocular examination two days later, without
cessation of symptoms, she admitted to having had
"migraine" in high school. She had been taking oral
contraceptives for many years. Her general history
was otherwise unremarkable.
At that visit on March 10, 1976, her best corrected
From the University of Virginia Medical Center,
Eye Clinic, Charlottesville, Virginia.
Reprint requests to James A. Rush, M.D., 1404
Hazel St., Charlottesville, VA 22901.
490
Fig. 1 (Rush). Fovea of the left eye. Normal light
reflex is surrounded by one temporal and two nasal
wedges or teardrops, pointing to the foveola (arrows).
VOL. 83, NO. 4
ACUTE MACULAR NEURORETINOPATHY
491
pigment epitheliopathy were female, but
only three of them were known to be
taking oral contraceptives. All patients
recovered and only one patient had a
recurrence. Despite speculation concerning the causea viral infection or its
sequelae etiology and pathogenesis
are unknown. Whether it is primarily a
disease of choriocapillaris or retinal pigment epithelium is still being debated.
Clinically distinct, acute retinal pigment epitheliitis was described in 1 9 7 2 .
Only four cases have been reported
since.
T h e lesions were ophthalmoscopically distinct, and restricted to the
macula. They were multiple, and resembled gray to black pigment spots, surrounded by halo zones. T h e y were usually monocular, asymptomatic, and caused
a moderate visual lossmost cases better
than 6/22 (20/70) and only one had 6/30
(20/100)although recovery was the rule.
Fluorescein angiography showed hypofluorescence in the central dark areas and
9
10
11
1 2 , 1 3
14
1 5 , 1 6
Fig. 2 (Rush). Left eye. Late phase fluorescein
angiogram showing absence of window defects,
blocked transmission, or capillary leakage.
DISCUSSION
Several idiopathic acute posterior pole
lesions have been described recently. In
1968, G a s s first described three young
women with moderately severe loss of
central vision bilaterally, in whose posterior pole areas were seen multiple
cream-colored lesions, apparently located
at the pigment epithelial level. He termed
this entity acute posterior multifocal placoid pigment epitheliopathy, and noted
that these lesions did not extend beyond
the equator and generally were less than 1
disk diameter in size. Despite a superficial resemblance to choroiditis, no inciting agent was ascertained, and his patients recovered normal, or nearly normal,
acuity in several months.
Later reports documented that this condition was not benign, being associated
with papillitis and retinovasculitis. It
has been associated with bilateral serous
detachments in two patients, and erythema nodosum in two o t h e r s .
Several
patients developed this after an acute
viral i l l n e s s .
Twenty-seven of the 51 p a t i e n t s
with acute posterior multifocal placoid
2
->
r \
5,6
7,8
2 - 1 3
Fig. 3 (Rush). Amsler grid demonstrates the teardrop or wedge shapes of parafoveal scotomas pointing toward fixation. Large horizontal scotoma was
most prominent, followed by inferonasal scotoma
whose corresponding lesion was closest to the foveola.
492
AMERICAN JOURNAL O F OPHTHALMOLOGY
hyperfluorescence in the halo zones.
Leakage was not demonstrated. Thes e lesions did not look like those of acute
posterior multifocal placoid pigment epitheliopathy, being considerably smaller,
and healing without scar formation.
However, the retinal pigment epithelium
is implicated because the E O G s , when
they have been recorded, have been baseline or subnormal. Like acute posterior
multifocal placoid pigment epitheliopathy, the illness is idiopathic, and recovery
is common. Only one of the ten reported
cases occurred after an acute viral illness.
Acute macular neuroretinopathy was
first described in 1 9 7 5 , when four detailed and two supplemental cases from
Europe were reported. Typically, acute
macular neuroretinopathy manifests three
to five reddish-brown foveal lesions, occurs predominantly in women and often
after mild viral illnesses. T h e s e lesions
assume a peculiar wedge-shaped or teardrop configuration, pointing to the umbo,
and characteristically do not cause a decline in visual acuity (Snellen). Yet, they
are bothersome, as they infringe upon
the foveola and produce small central
scotomas. T h e lesions are subtle, and
are best seen with the direct ophthalmoscope by using red-free light and motion
parallax.
1
Our case is typical of acute macular
neuroretinopathy: a young woman recovering from a viral upper respiratory infection noted the onset of three central scotomas corresponding to parafoveal deposits
of the unusual shape and coloration previously described. Visual acuity, peripheral fields, and fluorescein angiograms
were normal. Central fields, as depicted
on Amsler grid, showed scotomas corresponding to the fundus lesions.
O f seven patients, six women including
my patient with acute macular neuroretinopathy were taking oral contraceptives.
None of the other women had a remission, but no knowledge of discontin-
APRIL, 1977
uation of the hormone is available. My
patient was bothered by disruptive scotomas, but declined to consider longterm cessation of the pill. Therefore,
whether the association is causal or casual
is speculative.
There is some overlapping in these
three different conditions (Table). T h e y
are more common in women, but are
increasingly being diagnosed in m e n .
They may occur after viral illnesses. T h e y
may be related to oral hormones. T h e y
occur primarily, yet not exclusively, in
younger people. T h e y affect the posterior
pole.
These lesions, although superficially
similar, differ in appearance, and differ on
fluorescein
angiography. Furthermore,
acute macular neuroretinopathy is a disease of the more superficial sensory layers
of the retina, whereas the other two entities have involved the retinal pigment
epithelium.
Although acute macular neuroretinopathy is associated with the least decline in
visual acuity, it is the one disease that
undergoes the least amount of amelioration of symptoms. Whereas acute posterior multifocal placoid pigment epitheliopathy is associated with an initial dramatic decline in acuity, and the acute retinal
epitheliitis is manifested by a moderate to
severe loss of vision, recovery, although
slow, ultimately occurs. On the other
hand, in acute macular neuroretinopathy,
the paracentral scotomas have never been
documented to regress.
Finally, all three illnesses are idiopathic. As the number of cases of acute posterior multifocal placoid pigment epitheliopathy mounts, the association with viral
illness is becoming a potential source of
research. Although most cases of acute
macular neuroretinopathy occurred after
a viral illness, a relationship to viral infection has not yet been proven. Furthermore, although all six women with acute
macular neuroretinopathy had been re1
VOL. 83, NO. 4
ACUTE MACULAR NEURORETINOPATHY
493
TABLE
D I F F E R E N T I A L DIAGNOSIS O F M A C U L A R L E S I O N S *
APMPPE "
2
Sex
Appearance
13
24 M , 2 7 F
Cream-colored plaques
Location
Posterior pole
to equator
Systemic infection Common
Associated ocular Common
inflammation
Laterality
Usually bilateral
Diminished acuity Marked
Fluorescein study Abnormal
Recovery
Months to years
Cause
Possibly
infection-related
Pathology
Choriocapillaris
and RPE
Pigment
Epitheliitis "
14
16
Acute Macular
Neuroretinopathy
4 M, 6 F
Gray-black spots
with halo
Macula
1 M, 5 F
Red-brown wedge
Rare
None
4 of 6
None
Usually monocular
Moderate
Abnormal
Weeks to months
Unknown
Either
Mild
Normal
None
Possibly infection
or hormone
Sensory retina
RPE
Fovea
*M indicates male; F , female; RPE, retinal pigment epithelium; and APMPPE, acute posterior multifocal
placoid pigment epitheliopathy.
ceiving oral contraceptives, this avenue of
research may be restricted because one
other patient was a man.
Further awareness of the existence of,
and the differentiation among, these three
illnesses, and the accumulation of more
clinical experience, will necessarily lead
to a further delineation of pathophysiology.
1
scopic findings. Fluorescein angiograms
were normal. She had been taking oral
contraceptives for many years. Although
viral illness and oral contraceptives have
been associated with acute macular neuroretinopathy, no etiology was proven, and
no treatment is known. T h e patient remains symptomatic after a six-month
follow-up.
SUMMARY
A 24-year-old white woman convalescing from a viral upper respiratory infection suddenly developed three positive
scotomas around the fixation point in her
left eye. T h e fundus had three corresponding lesions that appeared to be
characteristic of acute macular neuroretinopathy. Situated in the fovea, subtle,
reddish-brown, wedge- or tear-shaped lesions were best seen with the direct ophthalmoscope using red-free light. Visual
acuity was 6/6 (20/20), and peripheral
fields were normal. T h e patient's reproduction of the scotomas on an Amsler grid
sheet mirrored the observed ophthalmo-
REFERENCES
1. Bos, P. J. M., and Deutman, A. F.; Acute
macular neuroretinopathy. Am. J . Ophthalmol. 80:
573, 1975.
2. Gass, J. D. M.: Acute posterior multifocal placoid pigment epitheliopathy. Arch. Ophthalmol. 80:
177, 1968.
3. Kirkham, T. H., Ffytche, T. J., and Sanders,
M. D.: Placoid pigment epitheliopathy with retinal
vasculitis and papillitis. Br. J. Ophthalmol. 56:875,
1972.
4. Bird, A. C , and Hamilton, A. M.: Placoid
pigment epitheliopathy. Br. J. Ophthalmol. 56:881,
1972.
5. Deutman, A. F., Oosterhuis, J. A., Boen-tan, T.
N., and Aan de Kerk, A. L.: Acute posterior multifocal placoid pigment epitheliopathy. Br. J. Ophthalmol. 56:863, 1972.
6. Van Buskirk, E . M., Lessei, S., and Friedman,
494
AMERICAN JOURNAL O F OPHTHALMOLOGY
E.: Pigmentary epitheliopathy and erythema nodosum. Arch. Ophthalmol. 85:369, 1971.
7. Ryan, S. J., and Maumenee, A. E.: Acute posterior multifocal placoid pigment epitheliopathy.
Am. J. Ophthalmol. 74:1066, 1972.
8. Annesley, W. H., Tomer, T. L., and Shields, J.
A.: Multifocal placoid pigment epitheliopathy. Am.
J. Ophthalmol. 76:511, 1973.
9. Lewis, R. A.: Acute posterior multifocal placoid pigment epitheliopathy. Arch. Ophthalmol. 93:
235, 1975.
10. Azar, P. Jr., Gohd, R. S., Waltman, D., and
Gitter, K. A.: Acute multifocal placoid pigment
epitheliopathy associated with an adenovirus type 5
infection. Am. J. Ophthalmol. 80:1003, 1975.
11. Holt, W. S., Regan, C. D. S., and Trempe, C :
APRIL, 1977
Acute posterior multifocal placoid pigment epitheliopathy. Am. J. Ophthalmol. 81:403, 1976.
12. Savino, P. J., Weinberg, R. J., Yassin, J. G.,
and Pilkerton, A. R.: Diverse manifestations of acute
posterior multifocal placoid pigment epitheliopathy. Am. J. Ophthalmol. 77:659, 1974.
13. Fishman, G. A., Rabb, M. F., and Kaplan, J.:
Acute posterior multifocal placoid pigment epitheliopathy. Arch. Ophthalmol. 92:173, 1974.
14. Krill, A. E., and Deutman, A. F.: Acute retinal
epitheliitis. Am. J. Ophthalmol. 74:193, 1972.
15. Deutman, A. F.: Acute retinal epitheliitis. Am.
J. Ophthalmol. 78:571, 1974.
16. Friedman, M. W.: Bilateral recurrent acute
retinal pigment epitheliitis. Am. J. Ophthalmol. 79:
567, 1975.
OPHTHALMIC MINIATURE
But suddenly the Mirror went altogether dark, as dark as i f a hole
had opened in the world o f sight, and F r o d o looked into emptiness.
In the black abyss there appeared a single E y e that slowly grew,
until it filled nearly all the Mirror. S o terrible was it that F r o d o stood
rooted, unable to cry out or to withdraw his gaze. T h e E y e was
rimmed with fire, but was itself glazed, yellow as a cat's, watchful
and intent, and the black slit o f its pupil opened on a pit, a window
into nothing.
J . R. R. T o l k i e n , The Lord of the Rings,
Part 1. The Fellowship
of the Ring
New York, Ballantin e Books
Vous aimerez peut-être aussi
- JNC8 HTNDocument2 pagesJNC8 HTNTaradifaNurInsi0% (1)
- KMKP 2 BookDocument499 pagesKMKP 2 BookgigaslayerxPas encore d'évaluation
- Neurosurgery Review (PDF) (UnitedVRG) PDFDocument377 pagesNeurosurgery Review (PDF) (UnitedVRG) PDFHo Hoang Vu80% (5)
- Enema PresentationDocument34 pagesEnema PresentationVishalni Menon Returnz100% (2)
- AETCOMDocument11 pagesAETCOMFree FirePas encore d'évaluation
- Generic Name Brand Name Classification/ Indication Mechanism of Action Adverse Effects Nursing ResponsibilitiesDocument3 pagesGeneric Name Brand Name Classification/ Indication Mechanism of Action Adverse Effects Nursing ResponsibilitiesRia Nicole100% (1)
- The Code of Ethics For NursesDocument8 pagesThe Code of Ethics For NursesZulkifli PomalangoPas encore d'évaluation
- Retinitis Pigmentosa: Causes, Tests, and Treatment OptionsD'EverandRetinitis Pigmentosa: Causes, Tests, and Treatment OptionsÉvaluation : 4 sur 5 étoiles4/5 (1)
- P2010/0509-001 Management of EclampsiaDocument7 pagesP2010/0509-001 Management of EclampsiaYwagar YwagarPas encore d'évaluation
- Theories - Thesis ProposalDocument12 pagesTheories - Thesis ProposalJordan Cruz100% (2)
- Role of Child Health NurseDocument7 pagesRole of Child Health NurseBinal Joshi100% (1)
- Dafpus 10 Sympathetic - Opthalmia-2Document7 pagesDafpus 10 Sympathetic - Opthalmia-2Anonymous jh87ryPas encore d'évaluation
- AJOPHT 1978 PriluckDocument4 pagesAJOPHT 1978 PriluckremotmPas encore d'évaluation
- X-Linked Incontinentia Pigmenti or Bloch-Sulzberger Syndrome: A Case ReportDocument4 pagesX-Linked Incontinentia Pigmenti or Bloch-Sulzberger Syndrome: A Case ReportOman ArifPas encore d'évaluation
- 40 Odogu EtalDocument4 pages40 Odogu EtaleditorijmrhsPas encore d'évaluation
- Herpes Zoster OphthalmicusDocument12 pagesHerpes Zoster OphthalmicusGio Vano NaihonamPas encore d'évaluation
- Phthisis Bulbi: Clinical and Pathologic Findings in RetinoblastomaDocument6 pagesPhthisis Bulbi: Clinical and Pathologic Findings in RetinoblastomaEstmar ValentinoPas encore d'évaluation
- 4 Epilepsy in A PatientDocument4 pages4 Epilepsy in A Patientarturschander3614Pas encore d'évaluation
- Ophthal Notes PGDocument6 pagesOphthal Notes PGSwati TyagiPas encore d'évaluation
- Ocular Histoplasmosis SyndromeDocument17 pagesOcular Histoplasmosis SyndromeDiana PSPas encore d'évaluation
- Tubercular ScleritisDocument5 pagesTubercular Scleritismutya yulindaPas encore d'évaluation
- Iridocorneal Endothelial Syndrome in A 16-Year-OldDocument4 pagesIridocorneal Endothelial Syndrome in A 16-Year-OldCamiCasasPas encore d'évaluation
- Exudative Retinopathy of Adults A Late S PDFDocument5 pagesExudative Retinopathy of Adults A Late S PDFInna BujorPas encore d'évaluation
- Sawyer 1976Document8 pagesSawyer 1976FrancescFranquesaPas encore d'évaluation
- Herpes Ophthalmicus: Review: ZosterDocument4 pagesHerpes Ophthalmicus: Review: ZosterAndika Wahyu UtomoPas encore d'évaluation
- Orbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusDocument4 pagesOrbital Apex Syndrome Secondary To Herpes Zoster OphthalmicusYosiita KartinaaPas encore d'évaluation
- Sarcoidosis (Heerfordt Syndrome) : A Case Report: Tiia Tamme, Edvitar Leibur, Andres KullaDocument4 pagesSarcoidosis (Heerfordt Syndrome) : A Case Report: Tiia Tamme, Edvitar Leibur, Andres KullajaquelineartPas encore d'évaluation
- Ocular Adnexal and Orbital Amyloidosis: A Case Series and Literature ReviewDocument18 pagesOcular Adnexal and Orbital Amyloidosis: A Case Series and Literature ReviewMariela LezamaPas encore d'évaluation
- tmp874C TMPDocument9 pagestmp874C TMPFrontiersPas encore d'évaluation
- Neuromyelitis Optica: Mark J. Morrow, MD, Dean Wingerchuk, MD, MSC, FRCP (C)Document13 pagesNeuromyelitis Optica: Mark J. Morrow, MD, Dean Wingerchuk, MD, MSC, FRCP (C)sidogra100% (1)
- Clinicopathologic Reports, Case Reports, and Small Case SeriesDocument3 pagesClinicopathologic Reports, Case Reports, and Small Case SeriesDiaz RandanilPas encore d'évaluation
- Glaucoma, Pseudoexfoliation: Emedicine Specialtiesophthalmologyintraocular PressureDocument9 pagesGlaucoma, Pseudoexfoliation: Emedicine Specialtiesophthalmologyintraocular PressureChintya Dwi PutriPas encore d'évaluation
- Associations of High Hypermetropia in Childhood JE Marr Et AlDocument2 pagesAssociations of High Hypermetropia in Childhood JE Marr Et AlArisa RosyadaPas encore d'évaluation
- Infantile Glaucoma in Down's Syndrome (Trisomy 21) : Case ReportsDocument6 pagesInfantile Glaucoma in Down's Syndrome (Trisomy 21) : Case ReportsJOHNATAN ANDREWS CARMONA SÁNCHEZPas encore d'évaluation
- Retroorbital PainDocument1 pageRetroorbital PainDang CuevasPas encore d'évaluation
- Subhyaloid Hemorrhage in Cerebral Malaria: Case ReportDocument4 pagesSubhyaloid Hemorrhage in Cerebral Malaria: Case ReportFaza KahfiPas encore d'évaluation
- Prabhakaran 2006Document2 pagesPrabhakaran 2006Milutin MelkaPas encore d'évaluation
- Clinical Profile and Ophthalmologic Manifestations of Herpes Zoster OphthalmicusDocument5 pagesClinical Profile and Ophthalmologic Manifestations of Herpes Zoster OphthalmicusNgakan WisnuPas encore d'évaluation
- An Old Friend Revisited: Chloramphenicol Optic Neuropathy: Case ReportDocument3 pagesAn Old Friend Revisited: Chloramphenicol Optic Neuropathy: Case ReportckeshavaPas encore d'évaluation
- Optic Neuritis in Leprosy - 231215 - 030338Document2 pagesOptic Neuritis in Leprosy - 231215 - 030338dr samyPas encore d'évaluation
- Review: Ocular Toxoplasmosis II: Clinical Features, Pathology and ManagementDocument14 pagesReview: Ocular Toxoplasmosis II: Clinical Features, Pathology and Managementhidrisdmnk_747467972Pas encore d'évaluation
- MedscapeDocument12 pagesMedscapeRissa WatlolyPas encore d'évaluation
- Masquerade SyndromesDocument10 pagesMasquerade Syndromestony_chrisPas encore d'évaluation
- Reversible Ocular Toxicity Related To Tamoxifen Therapy: DE) Also of ofDocument3 pagesReversible Ocular Toxicity Related To Tamoxifen Therapy: DE) Also of ofsafasayedPas encore d'évaluation
- Canine Lobular Orbital Adenoma Headrick2004Document5 pagesCanine Lobular Orbital Adenoma Headrick2004MicheleBerselliPas encore d'évaluation
- Spontaneous Resolution of Ophthalmologic Symptoms Following Bilateral Traumatic Carotid Cavernous FistulaeDocument6 pagesSpontaneous Resolution of Ophthalmologic Symptoms Following Bilateral Traumatic Carotid Cavernous FistulaeMaria Angelina BunawanPas encore d'évaluation
- Case Report Mata 2Document4 pagesCase Report Mata 2Hanung PujanggaPas encore d'évaluation
- Subluksasi Lensa Dengan Marfan SindromDocument3 pagesSubluksasi Lensa Dengan Marfan SindrommiftahulrauhanPas encore d'évaluation
- Hemorrhagic Unilateral RetinopathyDocument7 pagesHemorrhagic Unilateral RetinopathyHanna_RPas encore d'évaluation
- Visual Field Defects in Vascular Lesions The Lateral GeniculateDocument4 pagesVisual Field Defects in Vascular Lesions The Lateral GeniculateMarion FernandaPas encore d'évaluation
- Issue Apr2012 Pdffiles CasereportDocument5 pagesIssue Apr2012 Pdffiles CasereportyunjaealwaysPas encore d'évaluation
- EyesDocument42 pagesEyesKrittin NaravejsakulPas encore d'évaluation
- Case Discussion SLEDocument4 pagesCase Discussion SLERanjeetha SivaPas encore d'évaluation
- Secondary Buphthalmos: A Case SeriesDocument2 pagesSecondary Buphthalmos: A Case SeriesdrheriPas encore d'évaluation
- Bells PalsyDocument6 pagesBells PalsyCastay GuerraPas encore d'évaluation
- 1 s2.0 S245199361730395X MainDocument4 pages1 s2.0 S245199361730395X MainFadhli Muhammad KurniaPas encore d'évaluation
- Wang.2008.Central Serous ChorioretinopathyDocument20 pagesWang.2008.Central Serous ChorioretinopathyRohit GuptaPas encore d'évaluation
- Abstract 5Document7 pagesAbstract 5rluiknagwa lingPas encore d'évaluation
- Management of Bell's Palsy and Ramsay Hunt Syndrome - ClinicalKeyDocument33 pagesManagement of Bell's Palsy and Ramsay Hunt Syndrome - ClinicalKeyWaterfloPas encore d'évaluation
- Case Report: A Case of Type II Bilateral Sturge - Weber SyndromeDocument3 pagesCase Report: A Case of Type II Bilateral Sturge - Weber SyndromeIOSRjournalPas encore d'évaluation
- Leung (2008) - Familial Melanonychia StriataDocument4 pagesLeung (2008) - Familial Melanonychia StriataxtraqrkyPas encore d'évaluation
- Of Optic Gliomas: ManagementDocument8 pagesOf Optic Gliomas: ManagementUtama Hadiputra SurbaktiPas encore d'évaluation
- Ophthalmoplegic Migraine: Avery H. Weiss, MD, and James O. Phillips, PHDDocument3 pagesOphthalmoplegic Migraine: Avery H. Weiss, MD, and James O. Phillips, PHDAsriyani Ahmad DiniPas encore d'évaluation
- Upper Eyelid Ptosis RevisitedDocument14 pagesUpper Eyelid Ptosis RevisitedLia Noor AnggrainiPas encore d'évaluation
- Damasio 1985Document4 pagesDamasio 1985Gabriel Vargas MondacaPas encore d'évaluation
- Retinoschisis - A Teaching Case ReportDocument12 pagesRetinoschisis - A Teaching Case ReportGabriela Paz Mengoya CidPas encore d'évaluation
- Am J Ophthalmol 2015 ChenDocument10 pagesAm J Ophthalmol 2015 ChenremotmPas encore d'évaluation
- Arch Ophthalmol 2011 YehDocument4 pagesArch Ophthalmol 2011 YehremotmPas encore d'évaluation
- Am J Ophthalmol 2015 SridharDocument12 pagesAm J Ophthalmol 2015 SridharremotmPas encore d'évaluation
- Arch Ophthalmol 1991 YannuzziDocument6 pagesArch Ophthalmol 1991 YannuzziremotmPas encore d'évaluation
- Am J Ophthalmol 2014 YuDocument13 pagesAm J Ophthalmol 2014 YuremotmPas encore d'évaluation
- Am J Ophthalmol 2015 DansinganiDocument5 pagesAm J Ophthalmol 2015 DansinganiremotmPas encore d'évaluation
- Choroidal Granulomas in Sistemic SarcoidosisDocument8 pagesChoroidal Granulomas in Sistemic SarcoidosisremotmPas encore d'évaluation
- Am J Ophthalmol 2014 Rahimy-3Document10 pagesAm J Ophthalmol 2014 Rahimy-3remotmPas encore d'évaluation
- Acta Ophthalmol Scand 2000 Feigl-1Document4 pagesActa Ophthalmol Scand 2000 Feigl-1remotmPas encore d'évaluation
- Oral Mifepristone For Chronic Central Serous.26Document9 pagesOral Mifepristone For Chronic Central Serous.26remotmPas encore d'évaluation
- Brief Reports Out - 2001Document39 pagesBrief Reports Out - 2001remotmPas encore d'évaluation
- Squisis MacularDocument8 pagesSquisis MacularremotmPas encore d'évaluation
- Katarak Penyebab KebutaanDocument96 pagesKatarak Penyebab KebutaanIhsan HaidarPas encore d'évaluation
- AntioxidantDocument8 pagesAntioxidantremotmPas encore d'évaluation
- Brief Reports Fev - .2001pdfDocument30 pagesBrief Reports Fev - .2001pdfremotmPas encore d'évaluation
- A Randomized, Double-Masked Trial of Topical Ketorolac VersusDocument6 pagesA Randomized, Double-Masked Trial of Topical Ketorolac VersusremotmPas encore d'évaluation
- Acute Multifocal Placoid Pigment EpitheliopathyDocument8 pagesAcute Multifocal Placoid Pigment EpitheliopathyremotmPas encore d'évaluation
- An Analysis of Lesion Size and Location in Newly Diagnosed CyDocument7 pagesAn Analysis of Lesion Size and Location in Newly Diagnosed CyremotmPas encore d'évaluation
- Artigo 02 1-S2.0-S0161642012003545-MainDocument6 pagesArtigo 02 1-S2.0-S0161642012003545-MainremotmPas encore d'évaluation
- Artigo 03 Eye201122aDocument5 pagesArtigo 03 Eye201122aremotmPas encore d'évaluation
- Spaide PDFDocument11 pagesSpaide PDFremotmPas encore d'évaluation
- Artigo01 10 - 3928 - 1081597X - 20120921 - 07Document11 pagesArtigo01 10 - 3928 - 1081597X - 20120921 - 07remotmPas encore d'évaluation
- C CCCCCCCCCCCC C C C CDocument20 pagesC CCCCCCCCCCCC C C C CZandra Kiamco MillezaPas encore d'évaluation
- New Freedom Commission - BushDocument39 pagesNew Freedom Commission - BushKaren Crawford SimmsPas encore d'évaluation
- Alzehimer GuiaDocument9 pagesAlzehimer GuiaAlejandro PiscitelliPas encore d'évaluation
- Clinical Instrumentation, MLT 2760, BCC, Assessment Test 2Document9 pagesClinical Instrumentation, MLT 2760, BCC, Assessment Test 2alphacetaPas encore d'évaluation
- Pancreatic PseudocystDocument3 pagesPancreatic PseudocystViorel BudacPas encore d'évaluation
- Genetic Dis & AnaesthDocument19 pagesGenetic Dis & AnaesthaksinuPas encore d'évaluation
- Differential Diagnosis of The Scalp Hair FolliculitisDocument8 pagesDifferential Diagnosis of The Scalp Hair FolliculitisandreinaviconPas encore d'évaluation
- AclsDocument5 pagesAclsAnonymous vUl83IptiSPas encore d'évaluation
- Secondary HemostasisDocument24 pagesSecondary Hemostasisalibayaty1Pas encore d'évaluation
- 93 M Deatials PDFDocument5 pages93 M Deatials PDFRatna RoesardhyatiPas encore d'évaluation
- Case Analysis SchizoDocument4 pagesCase Analysis SchizoiamELHIZAPas encore d'évaluation
- MS 21Document10 pagesMS 21karenkaren09Pas encore d'évaluation
- Complications of Peptic Ulcer Disease: Surgical ManagementDocument57 pagesComplications of Peptic Ulcer Disease: Surgical ManagementJoan LuisPas encore d'évaluation
- Medication History Interview Form Demographic DataDocument3 pagesMedication History Interview Form Demographic Datakim jongin100% (1)
- ATPDDocument11 pagesATPDsagar189Pas encore d'évaluation
- Revision MCQsDocument6 pagesRevision MCQswiamPas encore d'évaluation
- Insomnia: Management of Underlying ProblemsDocument6 pagesInsomnia: Management of Underlying Problems7OrangesPas encore d'évaluation
- Orbit Key ArticlesDocument37 pagesOrbit Key ArticlesArjun MUPas encore d'évaluation
- Stress and Pregnancy: What Are The Effects?: Can Crying Cause Complications of Pregnancy?Document2 pagesStress and Pregnancy: What Are The Effects?: Can Crying Cause Complications of Pregnancy?Florin TudosePas encore d'évaluation
- Tka Inservice HandoutDocument2 pagesTka Inservice Handoutapi-317395769Pas encore d'évaluation
- FMConsensusDocumentbk 1Document105 pagesFMConsensusDocumentbk 1Cheryl BensonPas encore d'évaluation