Académique Documents
Professionnel Documents
Culture Documents
Jurnal Bedah Saraf
Transféré par
Nurul Ramadhaniaty PutriDescription originale:
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Jurnal Bedah Saraf
Transféré par
Nurul Ramadhaniaty PutriDroits d'auteur :
Formats disponibles
Journal of Medicine and Life Vol. 8, Issue 3, July-September 2015, pp.
278-284
Current diagnosis and treatment of chronic
subdural haematomas
Iliescu IA
Department of Neurosurgery, University Hospital Bucharest, Romania
Correspondence to: Iliescu IA, MD, PhD student
Department of Neurosurgery, University Hospital Bucharest
159 Splaiul Independentei Street, District 5, Bucharest, Romania
Mobile phone: +40722 345 684, E-mail: iliescu.aurel@gmail.com
Received: February 25th, 2015 Accepted: May 26th, 2015
Abstract
A developed society is usually also characterized by an elderly population, which has a continuous percentage growth. This
population frequently presents a cumulus of medical pathologies. With the development of the medication and surgical treatment of
different affections, the life span has increased and the pathology of an old patient has diversified as far as the cumulus of various
pathological diseases in the same person is concerned. Chronic subdural pathologies represent an affection frequently met in
neurosurgery practice. Any neurosurgeon, neurologist and not only, has to be aware of the possibility of the existence of a chronic
subdural haematoma, especially when the patient is old and is subjected to an anticoagulant or antiaggregant treatment, these 2
causes being by far the etiological factors most frequently met in chronic subdural haematomas. With an adequate diagnosis and
treatment, usually surgical, the prognosis is favorable. Although the surgical treatment presents a categorical indication in most of
the cases, the fact that there are many surgical techniques, a great relapse rate, as well as the numerous studies, which try to
highlight the efficiency of a technique as compared to another, demonstrate that the treatment of these haematomas is far from
reaching a consensus among the neurosurgeons. The latest conservatory treatment directions are still being studied and need many
years to be confirmed.
Keywords: chronic subdural haematoma, diagnostic, treatment
Abbreviations
CT = computerized tomography, MRI = magnetic resonance imaging
Definition
Subdural
haematoma
represents
an
extracerebral blood collection, which can be met as a clot
or in liquid form, located between the dura mater and the
middle layer of the meninges (arachnoid) and, which does
not expand in the subarachnoid area or in the basal
cisterns (interpeduncular cisterns). Usually, this collection
has a traumatic etiology (the acute and subacute ones are
always traumatic) and a compressive effect on the brain,
producing localization neurological signs, increased
intracranial pressure signs and various alterations of the
consciousness.
According to the time passed from the trauma to
the one of the manifestation, they can be classified into
the following groups:
Acute subdural hematoma the manifestations
appear during the first 3 days
Subacute subdural hematoma clinically
manifests between 4 and 21 days
Chronic subdural hematoma the clinical
manifestations appear after 21 days
It was first described by Virchow, in 1857, as an
internal hemorrhagic pachymeningitis. Later, in 1914,
Trotter launched the theory of traumatic brain injury and
the consecutive lesion of the bridging veins, as being the
cause of what he called hemorrhagic subdural cyst.
Epidemiology
With an approximate incidence of 2-3%
presence in the neurosurgery clinics, subdural
haematomas usually have a traumatic etiology and are
most often produced due to falls from the same or from
another level. The trauma is usually minor, with an
anteroposterior direction and it causes the rupture of the
emissary veins to the superior saggital sinus. In traumatic
brain injury, between the acceleration and deceleration of
the skull and the encephala there is a short interval, the
brain following in a short time the movement or the
stopping of the skull. The moment the skull stops, the
brain, which has inertia, continues its movement while
determining the stretching and subsequently the rupture
of the bridging veins in the subdural space. If the traumas
have a lateral direction, the subdural haematoma can
Journal of Medicine and Life Vol. 8, Issue 3, July-September 2015
form rarely, in which case besides the subdural
haematoma there are also brain contusions or brain
dilacerations.
The incidence of chronic subdural hematomas is
estimated at 1,7-18/ 100.000 inhabitants of the entire
population and it raises to 58/ 100.000 inhabitants in the
group of patients over 65 years old. The medium age of
patients with chronic subdural haematoma is of 63 years
old. Due to the fact that the population continues to get
old, it is expected that in 2030, its incidence will double [14]. Moreover, the prevalence of chronic subdural
haematoma is of 69% vs. 31% in the age group of over 65
years old compared to the rest of the age groups. The
incidence on sex highlights the fact that only the male
population is more frequently affected 64% vs. 33%
according to some studies, 71,8% vs. 28,2% according to
other studies, etc.
As far as the localization of chronic subdural
haematomas are concerned, the studies have
demonstrated a higher frequency of chronic subdural
haematomas of left brain hemisphere (52%) compared to
the ones of right brain hemisphere (30%), in 18% of the
cases being bilateral.
What is interesting to mention is the medium
thickness of chronic subdural haematomas, which was of
approximately 20,5mm +/- 5mm in unilateral haematomas
and of approximately 29,6mm +/- 9mm in bilateral
haematomas.
In 77% of the cases, the patients have suffered a
trauma by falling and 41% of them were under oral
anticoagulant treatment or antiplatelets.
The relapses of chronic subdural haematomas
are reported between 2,3% and 33%, in 25% of the
cases, haematomas being bilateral.
Considered for a long time a risk factor and not
an etiological factor, the treatment with anticoagulants
and antiplatelets has become an important subject to be
discussed in the last couple of years, having a major
complication in the appearance of subdural haematomas,
especially the chronic ones. In addition, in the last 10
years, all the studies and statistics have shown it as a
main etiologic factor in chronic spontaneous subdural
haematomas or better said in non-traumatic haematomas
and in their relapse, the anticoagulant and antiplatelet
treatment. The statistics show that in non-traumatic
subdural haematomas in 71% of the cases, there was an
anticoagulant or antiplatelets treatment as compared to
only 18% in the traumatic group, and the relapse was of
17% in this group of patients.
injury, which can pass unobserved and may frequently be
ignored, the chronic subdural haematoma has a latent
period until the appearance of the clinical symptoms, the
diagnosis presenting many errors.
Therefore, the main element that can lead to the
diagnosis of chronic subdural haematoma is the minor
brain injury; however, it should not be forgotten that it is
seriously taken into account only by some of the patients
or their families. Besides the trauma, there are 3 elements
that can contribute to the clinical diagnosis of a chronic
subdural haematoma [5]: the signs of hemispheric brain
damage or the foci (mainly the motor deficits and the
speech disorders), psychical disorders which are most
often met (chronic subdural haematoma being one of the
causes of evolutive dementia in elders) and the
symptomatic fluctuation. Besides these 3 elements, other
relevant clinical signs have also been described in cases
of haematoma: headache, drowsiness, signs of
intracranial hypertension [6].
Generally, the clinical stage of chronic subdural
haematoma orients towards an injury at the level of the
brain hemisphere but does not help in the differential
diagnosis of other brain injuries.
Usually, a progressive slow expansive
intracranial process or an ischemic stroke is suspected.
The suspicion of expansive intracranial injury makes us
perform a paraclinical investigation (CT or MRI), which
makes the diagnosis clearer by evidencing the iso- or
hypodense subdural collection.
If the CT examination is currently very easily
accessible, the diagnosis of chronic subdural haematoma
has become quite simple, the main condition being that
you only have to think about such a diagnosis. This is
valid mostly in cases of elders, who progressively develop
psychic disorders, representing the group of patients with
chronic subdural haematoma.
Regarding the differential diagnosis, it should not
be forgotten that the clinical signs of a haematoma mimic
an intracranial neoformation or an ischemic stroke. In
youngsters, chronic subdural haematomas often manifest
with epilepsy crises and behavior disorders, which are
due to alcohol consumption.
Paraclinical diagnosis
The diagnosis of chronic subdural haematoma
has evolved in the last 20-30 years together with the
introduction of the CT scan, the MRI and the access of
the patients to this type of explorations.
The CT scan
It was introduced in 1972, based on the researches
of Hounsfield. By using the densitometry differences at the
level of the serial sections of the skull and its contents, it
created the possibility of evidencing different injuries, the
injured structure and the movement of the brain structures
the mass effect. It represents an investigation, which is
currently very often used, it is rapid and it can also be applied
in comatose patients, which has led to the precocious
Clinical diagnosis
The diagnosis of a chronic subdural haematoma
can present many difficulties taking into account the fact
that it frequently appears in elders, who anyway have a
higher or a lower degree of psychical disorders due to
brain involution. Moreover, in the context of a usual brain
279
Journal of Medicine and Life Vol. 8, Issue 3, July-September 2015
screening of many brain injuries. Being an extremely
accessible investigation at present, which offers important
information for the neurosurgeon in many cases of brain
injuries, the CT scan is an essential tool in emergency brain
injuries traumas. Currently, no emergency room of an
emergency hospital can be conceived without having a CT
scan (Fig. 1,2).
MRI
It was introduced in 1982 and it is based on the
movement of the hydrogen atoms, which are included in
different tissues in a magnetic field. In addition, each
structure, even in the same organ, presents the specific
T1 and T2 relaxation times, determining particular aspects
of the whole MRI image. The intensity of the signal from
different structures is captured and translated to an image
with white shades, which means strong signal, or black
shades, which means lack of signal.
This way the cerebrospinal fluid, the bone, the
rapid blood flow and the air, appear as being black or in
different shades of black in T1. The cerebral gray matter
and the white substance appear in T1 in different shades
of gray. The fat and the recent blood effusions emit a
strong signal, these being white in T1. In T2, the images
are clearer, reflecting the modifications in the water
content. In addition, the structures that contain a large
amount of water appear with a strong signal, being white,
as for example the cerebrospinal fluid (CSF), cerebral
edema, demyelinated areas, tumors with a content
characterized by a large amount of water. Due to the fact
that the bone does not contain water, it appears as being
black and its anatomical details are visualized harder than
in a CT scan or in the images of an MRI in T1 (Fig. 3,4).
Although it is an exceptional investigation tool, the MRI
has its limitations which are given by the presence of
some metallic structures in the organism as well as by the
long process of images acquisition, which, in some cases,
can make the examination impossible (for example the
claustrophobic patients or the medico-surgical
emergencies).
As far as the traumatic brain injuries are
concerned, the CT and the MRI have advantages and
disadvantages when being compared.
In addition, the CT examination is fast, more
accessible than the MRI examination and brings essential
information for the neurosurgeon in a short time. What
should also be taken into account is that in a CT scan, a
bone injury is easily and correctly appreciated. The MRI
image presents a higher fidelity than the CT scan as far
as the images and the injuries are concerned. It can also
highlight the so-called diffuse axonal injuries of the brain
(DAI); practically these could be described and studied
closely only after the introduction of MRI examination.
This type of injuries is predominantly located in the
parasagittal cortical white-matter, the corpus callosum
and the pontomesencephalic junction adjacent to the
superior cerebellar peduncle. The microscopic aspect of
this type of injuries corresponds to the Wallerian axonal
degeneration so that the axon practically disintegrates.
There are studies concerning the chronic
subdural haematomas, which also demonstrate the
superiority of the MRI examination in comparison with the
CT [7]. The MRI examination better shows the location of
the chronic subdural haematoma and evidences its
dimensions much clearer together with the mass effect of
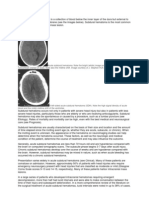
Fig. 1 Chronic subdural haematoma of right brain
hemisphere (CT scan); what should be noted is the
hypodense aspect of the haematoma and the mass effect it
has on the structures of the median line
Fig. 2 Chronic subdural haematoma with a recent bleeding of
right brain hemisphere (CT scan); what should be noted is the
mixed, hypo- hyperdense aspect of the haematoma and the
erase of the circle movements of the right brain hemisphere as
an effect of the compression due to the haematoma
280
Journal of Medicine and Life Vol. 8, Issue 3, July-September 2015
minimal craniotomy (under 3cm diameter)
technique single burr hole with a closed
vacuum drainage system
minimal craniotomy (under 3cm diameter)
technique with a closed drainage system and
irrigation with sodium chloride solution (physiologic
serum), which is a variant of the first technique
twist drill trephination technique together with
a closed drainage system
2 minimal craniotomies technique with a
drainage system (a variant of the previous
technique)
craniotomy (the diameter of the craniotomy being
of over 3cm), together with a vacuum closed
drainage system usually used in cases of old,
septated chronic subdural haematomas
The 3 main surgical techniques used the
treatment of chronic subdural haematomas consisted of
the following:
1. Craniotomy most often used in the past, it has the
advantage of exposing an important part of the brain. It is
usually practiced under general anesthesia and it is the
most invasive of the treatment options of chronic subdural
haematomas because it takes a lot of time and it
presupposes a lot of intraoperatory blood loss. However,
it remains the chosen option in cases of old, organized,
multiseptated subdural haematomas. In Markwalders
study (1981) on chronic subdural haematomas,
craniotomy, which was considered a radical approach,
was reserved to cases in which: a) the subdural
haematoma relapsed; b) the haematoma seemed to be
very well organized in the CT examination and having
solid consistency; c) the brain did not re-expansion and
obliterated the subdural area [8].
2. Minimal craniotomy (trephination) - is one of the most
often used surgical techniques in cases of current chronic
subdural haematomas. According to a national Canadian
study in 2005, 85% of the respondents have indicated this
technique as the most commonly used as initial surgical
treatment. However, in cases of relapses, 43,1%
preferred the craniotomy and only 35,1% the trephination
[9]. It is usually done under general anesthesia, some
surgeons preferring only one trephination, others two.
Nevertheless, none of the 2 variants represents a clear
choice although in a study it was shown that patients
whom were applied only one trephination presented a
high relapse rate, a longer hospitalization period and a
high rate of infection of the wound [10].
3. Single twist drill trephination presents the great
advantage that it can be performed in the hospital bed
while using local anesthesia or in the surgery room under
local or general anesthesia. It is considered useful in
cases of patients with multiple comorbidities, who are very
old and in whom the risks of a complex surgery are very
high. It is efficient only in cases in which the subdural
haematoma is completely liquefied and, usually a
Jackson-Pratt vacuum drainage system is also used.
What should also be mentioned is that most of the studies
highlight that the relapse rate in the case of a surgical
the adjacent structures. Moreover, it is more useful in
cases of bilateral and isodense chronic subdural
haematomas. The MRI examination is superior to the CT
examination as far as the membranes dimensions of the
chronic subdural haematoma and the presence of the
septa inside the haematoma are concerned, in these
conditions the surgical approach could be modified.
Fig. 3 Bilateral chronic subdural haematoma; what should
be taken into account is the absence of the mass effect on
the structures of the median line, and the presence of the
compressive effect on the noble brain structures MRI
image, T1
Fig. 4 FLAIR, T1, T2 MRI images of an acute subdural
haematoma of a left brain hemisphere which determines an
important mass effect on the structures of the median line
as well as the concomitant presence of an area of left
frontal lobe laceration; complex brain injury
Treatment
Over the years, together with the development of
the diagnosis methods and the surgical techniques, the
treatment of chronic subdural haematomas has evolved;
currently there are also studies of conservative treatment
beside the various surgical techniques, which however
have not been applied very often.
In addition, as far as the surgical treatment is
concerned, some techniques have been described:
281
Journal of Medicine and Life Vol. 8, Issue 3, July-September 2015
treatment is between 5 and 33%. The relapse in cases of
chronic subdural haematomas means the symptomatic
relapse of the subdural haematoma in the area which was
already operated on. The risk factors of relapses are the
following: tendency of bleeding, intracranial hypotension,
recurrent neomembrane hemorrhages. Moreover, the
persistence of the subdural area due to the insufficient
expansion of the brain is considered a risk factor for the
recurrence of a haematoma. In case it is not symptomatic,
it is not regarded as a recurrence. As far as the brain reexpansion is concerned, it is considered that its
mechanical properties, such as the elasticity, can explain
the tendency of its re-expansion. The factors of brain
elasticity have been considered the compression the
cerebrovascular volume, meningeal membranes and the
subpial transection test [11]. Some studies highlight that
the existence of neomembranes and the volume of
primary brain expansion that precedes decompression, is
not considered a predictor for the clinical aspect of the
patient postoperatory.
According to a very thorough and on a long
period of time study done in India, on a period of 30
years, which consisted of 2300 cases, the best technique
was considered temporal craniotomy with the dura mater
left open and the subdural area communicating with the
subtemporal area. According to this study, the
membranectomy was not necessary, the relapse rate
diminished and the mortality rate was of only 0,5% [12].
In spite of these published results, the treatment
of chronic subdural haematomas remains a controversy!
Many neurosurgeons recommend a minimal craniotomy
followed by an irrigation of the subdural area with sodium
chloride solution and the use of a vacuum drainage
system. Some studies even raise controversies regarding
the utility of a drainage system.
Other
neurosurgeons
recommend
the
endoscopic treatment of chronic subdural haematomas,
especially the septated ones [13,14].
It was also proposed that the universal technique
should be the single twist drill trephination, followed by the
use of a subdural catheter, instead of a minimal
craniotomy, on a group of 66 patients. In this study, the
reintervention rate was of 18,1% in the group of patients
with a single twist drill trephination and of 33,3% in the
one with minimal craniotomy [15].
A study that was recently published showed that
in the absence of a clear evidence of the superiority of a
certain type of surgical intervention, it is the
neurosurgeons job to choose the technique to use:
craniotomy or minimal craniotomy followed by drainage.
The study was centered on the costs of each procedure,
the relapse rate and reintervention, mortality and
postoperatory morbidity. The conclusions of the study
done on 119 patients, of whom 61 underwent minimal
craniotomy and 58 craniotomy, are surprising: the percent
of reintervention was lower in minimal craniotomy in
comparison with craniotomy which had a 6,6% as
compared with 24,1%, and the percent of postoperatory
complications (infections, acute hemorrhages and stroke),
was higher in patients with craniotomies. Regarding the
medium hospitalization period, the medium period spent
in the surgery room and the medium cost of the treatment,
the minimal craniotomy followed by drainage also proved
superior to craniotomy. Another conclusion of the authors,
who have taken into consideration the costs of each type
of intervention (craniotomy and minimal craniotomy), was
that due to the fact that the health state of the population
has a raising cost, the surgeons who choose to perform
surgeries which are more expensive when there are
others which are cheaper and more efficient, should be
more careful when choosing the type of intervention to
perform [16].
Another special category in the treatment of
chronic subdural haematomas is the patients with
anticoagulant treatment. This category is continually
growing because a high proportion of the elder population
undergoes a daily treatment with oral anticoagulants. A
recent study has shown that the anticoagulant treatment
raises to 42,5 times the risk of developing a chronic
subdural haematoma [17], and another study done in
Switzerland showed that 41% of the patients with chronic
subdural haematomas undergo a daily anticoagulant
treatment.
Besides the raise of the risk of developing a
chronic subdural haematoma, coagulopathy also
complicates the neurosurgical treatment. A study done in
the U.S.A. showed that the patients undergoing an
anticoagulant treatment present a medium hospitalization
period higher than the others 11 vs. 7,5 days. There is a
consensus as far as the patients with anticoagulant
medication who present symptomatic chronic subdural
haematomas are concerned: they have to be readjusted
from the point of view of coagulopathy in order to prevent
the development of a haematoma and also to facilitate the
neurosurgery. The initial treatment of coagulopathy is
necessary even in patients with severe cardiac pathology
with a specific indication of anticoagulants, as for example
the patients with valvular prostheses.
The ones undergoing antiplatelets therapy
represent another category of patients at risk. Also in their
case, stopping the antiplatelets medication is the first step
before any decision of performing a neurosurgery. The
reintroduction of antiplatelets therapy can be done similar
as in the case of anticoagulant therapy.
As far as the prophylactic anticonvulsive
treatment is concerned, there are numerous pro and con
opinions; the studies indicate rates between 2 and 19% of
the patients who present epileptic crises pre- or post
surgical intervention. The majoritys opinion is that the
prophylactic administration of anticonvulsants is
reasonable, mostly because the patients with chronic
subdural haematomas frequently present other traumatic
brain injuries, which are a well-known risk factor in crises
appearance. However, what should be taken into account
282
Journal of Medicine and Life Vol. 8, Issue 3, July-September 2015
is the fact that the anticonvulsant medication represents
an additional risk factor of falling from the same level in
the population over 65 years old, also representing the
main age group who presents chronic subdural
haematomas.
Two studies report there is no significant
difference in the appearance rate of convulsive crises in
patients who have received prophylactic antiepileptic
treatment as compared to the ones who have not.
However, both studies underline the fact that the benefit
of administering prophylactic antiepileptic treatment is
overtaken by the risks of their administration except for
the patients with a high risk of presenting crises, such as
the chronic alcohol consumers [18,19].
Besides the surgical techniques, conservative
methods of treatment have been described and are still
being studied:
tranexamic acid administration
oral administration of corticosteroids
The oral administration of tranexamic acid in a
daily dose of 750mg has as basis the studies which
indicate that fibrinolysis and the kinin-kallikrein
inflammatory system have an important role in the growth
of chronic subdural haematoma. These studies have led
to the idea that the antifibrinolytic and anti-inflammatory
treatment administration, basically tranexamic acid, can
lead to the complete resection of the subdural
haematoma. The study involving the tranexamic acid was
conducted on a period of 4 years, the clinical follow up
and the imagistic analysis of the patients in the study
being on average of 58 days and the medium volume of
the chronic subdural haematoma being reduced to
55,6ml. After the treatment with tranexamic acid, the
volume of the haematoma was reduced to a medium size
of 3,7ml, without its reoccurring or growing in size [20].
Another conservative treatment method is
represented by the oral administration of corticosteroids
(a double-blind multicentric randomized study, in
Montpellier University Hospital, started in 2011), such as
Prednisone in a dose of 1mg/ kg body/ day for 1 week,
and then the dose is reduced with 10 mg/ week, until a
dose of 5-10mg/ day is reached, a moment when the
treatment can be stopped; the medium duration of the
treatment being of 2 months. This treatment also has as a
main idea the anti-inflammatory role medication
administration with the purpose of counteracting the local
inflammatory reaction at the level of the parietal
membrane and consecutively the determination of the
reduction in size of the haematoma. This study also
proposed the administration of corticosteroids after
surgery, with the purpose of preventing the relapses and
a new reintervention, knowing the fact that the relapses in
chronic subdural haematomas can reach to 30%. The
study is still ongoing, no preliminary conclusions being
drawn yet.
However, in a study done on 496 patients with
chronic subdural haematoma, the administration of
corticoids preoperatively has been associated with a
decrease in the rate of relapses. The preoperatory use of
corticoids did not determine a growth of complications or
of mortality and morbidity rates in patients [21].
Conclusion
Although the surgical treatment has a categorical
indication in most of the cases, the fact that there are
many surgical techniques, a higher relapse rate, as well
as the multiple studies that try to highlight the efficiency of
a technique over another, it demonstrates that the
treatment of these haematomas is far from reaching a
consensus among the neurosurgeons. However, it is
obvious that the purpose of the treatment is to be
minimally invasive and, in the same time, to diminish the
rate of relapses. The new non-surgical treatment
directions are still at the beginning and they need time to
prove their efficiency.
References
1.
2.
3.
4.
McArthur DL. Traumatic Brain Injury:
Some history and some epidemiology. In:
Levin H, Shum D, Chan R. Understanding 5.
Traumatic Brain Injury: Current Research
and Future Directions. Feb 2014, Oxford
University Press, 8-25.
Markwalder TM. Chronic subdural
hematomas: a review. Journal of 6.
Neurosurgery. May 1981; 54, 5, 637-645.
Fogelholm R, Waltimo O. Epidemiology
of chronic subdural haematoma. Acta
7.
Neurochirurgica. 1975; 32, 247-250.
Chen JC, Levy ML. Causes,
epidemiology, and risk factors of chronic
subdural hematoma. Neurosurgery Clinics
of North America. 2000; 11(3), 399-406.
Arseni C, Danaila L. Hematoamele durei 8.
mater. In Arseni C, Danaila L, Arseni A.
Bolile vasculare ale creierului si maduvei
spinarii. 1985, Bucuresti, Ed. Academiei
Republicii Socialiste Romania, 113-392.
Arseni C, Ciurea AV.
Revarsate
sanguine
intracraniene
traumatice. 9.
Consfatuirea Nationala de Medicina
Legala. Sept 1988, Targoviste, 46-99.
Senturk S, Guzel A, Bilici A et al. CT
and MR imaging of chronic subdural
haematomas: a comparative study. Swiss
283
Medical Weekly. 2010; 140(2324), 335
340.
Cenica A, Bhandaria M, Reddya K.
Management of Chronic Subdural
Hematoma: A National Survey and
Literature Review. The Canadian Journal
of Neurological Sciences. Nov 2005; 32,
501-506.
Taussky P, Fandino J, Landolt H.
Number of burr holes as independent
predictor of postoperative relapse in
chronic subdural haematoma. British
Journal of Neurosurgery. 2008; 22, 2,
279-282.
Journal of Medicine and Life Vol. 8, Issue 3, July-September 2015
10. Fukuhara T, Gotoh M, Asari S et al. The
relationship between brain surface
elastance and brain re-expansion after
evacuation
of
chronic
subdural
hematoma. Surgical Neurology. June
1996; 45, 570574.
11. Sambasivan M. An overview of chronic
subdural hematoma: Experience with
2300 cases. Surgical Neurology. May
1997; 47, 418422.
12. Hellwig D, Kuhna TJ, Bauera BL, ListHellwig E. Endoscopic treatment of
septated chronic subdural hematoma.
Surgical Neurology. March 1996; 45,
272277.
13. Rodziewicz
GS,
Chuang
WC.
Endoscopic removal of organized chronic
subdural hematoma. Surgical Neurology.
June 1995; 43, 569573.
14. Smely C, Madlinger A, Scheremet R.
preventing seizures in patients with
Chronic subdural haematoma a
chronic subdural haematoma. The
comparison of two different treatment
Cochrane Library. June 2013.
modalities. Acta Neurochirurgica. 1997; 19. Kageyama H, Toyooka T, Tsuzuki N,
139, 818-826.
Oka K. Nonsurgical treatment of chronic
15. Regan JM, Worley E, Shelburne C et al.
subdural hematoma with tranexamic acid.
Burr Hole Washout versus Craniotomy for
Journal of Neurosurgery. Aug 2013; 119,
Chronic Subdural Hematoma: Patient
2, 332-337.
Outcome and Cost Analysis. PLoS One. 20. Berghauser P, Dammers R, Schouten
2015 January; 10(1), e0115085.
JW et al. Clinical Factors Associated With
16. Rust T, Kiemer N, Erasmus A. Chronic
Outcome in Chronic Subdural Hematoma:
subdural
haematomas
and
A Retrospective Cohort Study of Patients
anticoagulation
or
anti-thrombotic
on Preoperative Corticosteroid Therapy.
therapy. Journal of Clinical Neuroscience.
Neurosurgery. April 2012; 70, 873880.
October 2006; 13 (8), 823827.
21. Amirjamshidi A, Abouzari M, Eftekhar
17. Rubin G, Rappaport ZH. Epilepsy in
B et al. Outcomes and relapse rates in
chronic subdural haematoma. Acta
chronic subdural haematoma. British
Neurochirurgica. 1993; 123, 39-42.
Journal of Neurosurgery. 2007; 21, 3,
18. Ratilal BO, Pappamikail L, Costa J,
272-275.
Sampaio C. Anticonvulsants for
284
Vous aimerez peut-être aussi
- Intracerebral Haemorrhage: Disease PrimersDocument18 pagesIntracerebral Haemorrhage: Disease PrimersMarlon VillanuevaPas encore d'évaluation
- Ronny Yusyanto. SUBDURAL HEMATOMADocument20 pagesRonny Yusyanto. SUBDURAL HEMATOMAFerdy100% (1)
- Mandibular Overdenture PDFDocument103 pagesMandibular Overdenture PDFIbrahim Ahmed Dahab100% (1)
- OM 15407 GE MAC5500 Operator ManualDocument178 pagesOM 15407 GE MAC5500 Operator ManualArmanPas encore d'évaluation
- Sumber Referat 4 PDFDocument7 pagesSumber Referat 4 PDFAkhdan AufaPas encore d'évaluation
- Hematoma SubduralDocument27 pagesHematoma SubduralRoeder Max Pangramuyen100% (4)
- Subdural Hematomas in The ElderlyDocument19 pagesSubdural Hematomas in The ElderlyRegina PhilyriaPas encore d'évaluation
- Syncope in Adults - Epidemiology, Pathogenesis, and EtiologiesDocument28 pagesSyncope in Adults - Epidemiology, Pathogenesis, and EtiologiesRaúl MartínezPas encore d'évaluation
- Journal NeuroDocument6 pagesJournal NeuroBetari DhiraPas encore d'évaluation
- Bod CerebrovasculardiseasestrokeDocument67 pagesBod CerebrovasculardiseasestrokeErlin IrawatiPas encore d'évaluation
- Bod - Cerebrovascular Disease Stroke BurdenDocument67 pagesBod - Cerebrovascular Disease Stroke BurdenderiPas encore d'évaluation
- Surgical Treatment of Chronic Subdural Hematoma CLDocument12 pagesSurgical Treatment of Chronic Subdural Hematoma CLNikola StevanovicPas encore d'évaluation
- A Subdural HematomaDocument2 pagesA Subdural HematomaMohammadAwitPas encore d'évaluation
- Bod Cerebrovasculardiseasestroke PDFDocument67 pagesBod Cerebrovasculardiseasestroke PDFMax Laban SeminarioPas encore d'évaluation
- S TrokeDocument12 pagesS Trokenersimelda dutyPas encore d'évaluation
- Ischemic StrokeDocument13 pagesIschemic StrokearthurbaidoodouglasPas encore d'évaluation
- A Subdural HematomaDocument2 pagesA Subdural HematomaMohammadAwitPas encore d'évaluation
- Epidural Hematoma: Continuing Education ActivityDocument16 pagesEpidural Hematoma: Continuing Education ActivityIka AriandanaPas encore d'évaluation
- EN07 Sindrom CushingDocument8 pagesEN07 Sindrom CushingAryanto AntoPas encore d'évaluation
- Cerebral Venous Sinus ThrombosisDocument34 pagesCerebral Venous Sinus ThrombosisNeurologia homicPas encore d'évaluation
- Article Acute Stroke PDFDocument10 pagesArticle Acute Stroke PDFHeather PorterPas encore d'évaluation
- Case Study Cva Gr1Document72 pagesCase Study Cva Gr1Divina Gracia Fabicon Arana100% (1)
- A Subdural HematomaDocument12 pagesA Subdural HematomaGina Irene IshakPas encore d'évaluation
- Enabeel, 173-176Document4 pagesEnabeel, 173-176keerthi.sakthi0794Pas encore d'évaluation
- Final Case Study (Group3)Document58 pagesFinal Case Study (Group3)Juvelyn Ranuco BalagosaPas encore d'évaluation
- Stroke ThesisDocument7 pagesStroke Thesisnavysavchenkobellevue100% (1)
- Moyamoya Epidemiology, Presentation, and DiagnosisDocument9 pagesMoyamoya Epidemiology, Presentation, and DiagnosisshiloinPas encore d'évaluation
- Meningitis EskemikDocument17 pagesMeningitis Eskemikakbar011512Pas encore d'évaluation
- Review Article: Ischemic Stroke in Infants and Children: Practical Management in EmergencyDocument8 pagesReview Article: Ischemic Stroke in Infants and Children: Practical Management in EmergencyEstela MachadoPas encore d'évaluation
- SNCDocument8 pagesSNCAdrian PetrosPas encore d'évaluation
- Acute Stroke ArticleDocument10 pagesAcute Stroke ArticlenesredePas encore d'évaluation
- Stroke: BackgroundDocument10 pagesStroke: Backgroundjhay-r reyesPas encore d'évaluation
- Otogenic Brain Abscess Our ExperienceDocument5 pagesOtogenic Brain Abscess Our ExperienceNeysaAzaliaEfrimaisaPas encore d'évaluation
- Subdural HematomaDocument8 pagesSubdural HematomaaaronmanullangPas encore d'évaluation
- Cerebral Venous ThrombosisDocument15 pagesCerebral Venous ThrombosisValentina RobuPas encore d'évaluation
- Subdural HematomaDocument20 pagesSubdural HematomaArief Zamir100% (1)
- Management of Ischaemic Stroke2000Document29 pagesManagement of Ischaemic Stroke2000FEllis LEoPas encore d'évaluation
- Nervous SystemDocument62 pagesNervous Systemmyat252Pas encore d'évaluation
- Art 3A10.1007 2Fs00415 016 8189 XDocument7 pagesArt 3A10.1007 2Fs00415 016 8189 XIrmagian PaleonPas encore d'évaluation
- Understanding and Treating Moyamoya Disease in ChildrenDocument11 pagesUnderstanding and Treating Moyamoya Disease in ChildrenFitriyana WinarnoPas encore d'évaluation
- Ischemic Stroke in A Young Male Patient in Rural Uganda, Case Report.Document3 pagesIschemic Stroke in A Young Male Patient in Rural Uganda, Case Report.International Journal of Innovative Science and Research TechnologyPas encore d'évaluation
- Epidural Haematoma: DR - Karan R RawatDocument65 pagesEpidural Haematoma: DR - Karan R RawatSitha ChristinePas encore d'évaluation
- Chronic Subdural HematomaDocument21 pagesChronic Subdural Hematomamarc_caronan100% (2)
- Epidural Hematoma in Emergency Medicine: BackgroundDocument3 pagesEpidural Hematoma in Emergency Medicine: BackgroundMercy HasanPas encore d'évaluation
- STROKE: Handbook with activities, exercises and mental challengesD'EverandSTROKE: Handbook with activities, exercises and mental challengesPas encore d'évaluation
- Cerebrovascular Diseases Risk Factors:: o o o o oDocument4 pagesCerebrovascular Diseases Risk Factors:: o o o o otrinaPas encore d'évaluation
- Non-Pharmacological Measures: PacemakerDocument11 pagesNon-Pharmacological Measures: PacemakerAlmendra Olenka LSPas encore d'évaluation
- Schimmel 2017Document31 pagesSchimmel 2017yalocim666Pas encore d'évaluation
- Overview of The Clinical Features and Diagnosis of Brain Tumors in AdultsDocument37 pagesOverview of The Clinical Features and Diagnosis of Brain Tumors in AdultsFSHB-A&APas encore d'évaluation
- Brainstem StrokeDocument22 pagesBrainstem StrokeAlin CiubotaruPas encore d'évaluation
- Rehabilitation in Cerebrovascular AccidentDocument19 pagesRehabilitation in Cerebrovascular AccidentIsaac OmwengaPas encore d'évaluation
- Dementia Vaskular CinaDocument16 pagesDementia Vaskular CinaGuntur AntonPas encore d'évaluation
- Iht Nejm 2014Document10 pagesIht Nejm 2014Ademir Ruiz EcheverríaPas encore d'évaluation
- Overview of The Evaluation of Stroke - UpToDateDocument57 pagesOverview of The Evaluation of Stroke - UpToDateclarissa suryaPas encore d'évaluation
- Caso Acv4 PDFDocument7 pagesCaso Acv4 PDFVianny PossoPas encore d'évaluation
- Clinical Manifestations, Prevention and Treatment of Stroke in WomenDocument6 pagesClinical Manifestations, Prevention and Treatment of Stroke in WomenCentral Asian StudiesPas encore d'évaluation
- Sensors 22 04670Document13 pagesSensors 22 04670hiimamanenuPas encore d'évaluation
- Case Study On Subacute Subdural HematomaDocument33 pagesCase Study On Subacute Subdural Hematomajarelle bondoc100% (15)
- Review of Related LiteratureDocument23 pagesReview of Related LiteratureMark Alden PaduaPas encore d'évaluation
- Noninvasive Radiologic Diagnosis of Extracranial Vascular PathologiesD'EverandNoninvasive Radiologic Diagnosis of Extracranial Vascular PathologiesPas encore d'évaluation
- Vascular Compression Syndromes - What You Need to KnowD'EverandVascular Compression Syndromes - What You Need to KnowPas encore d'évaluation
- NEUROPrelims - History Taking in NeurologyDocument4 pagesNEUROPrelims - History Taking in NeurologyRenatoCosmeGalvanJuniorPas encore d'évaluation
- Dept of Orthopaedics Brochure 2017 EnglishDocument2 pagesDept of Orthopaedics Brochure 2017 EnglishsharikasureshssPas encore d'évaluation
- Stroke PamphletDocument12 pagesStroke Pamphletapi-232971337Pas encore d'évaluation
- CH9 PhlebDocument2 pagesCH9 PhlebBSMT1ANANGIT, DYRELPas encore d'évaluation
- Vestibular MigrainDocument50 pagesVestibular MigrainMindi Widayani100% (1)
- CMS Neuro Form Number 4 Query Answer Req? - USMLE Forum: Jun 30, 2016 - 7 PostsDocument3 pagesCMS Neuro Form Number 4 Query Answer Req? - USMLE Forum: Jun 30, 2016 - 7 Postsbob0% (1)
- Guideline Hypoglycemia PDFDocument13 pagesGuideline Hypoglycemia PDFleslyjanet100% (1)
- All About Physiotherapy Student PresentationDocument17 pagesAll About Physiotherapy Student Presentationvida konadu AgyemanPas encore d'évaluation
- Bladder PDFDocument22 pagesBladder PDFSuci Mega SariPas encore d'évaluation
- HEYER VizOR - Product List - en 0314 2Document7 pagesHEYER VizOR - Product List - en 0314 2kalandorka92Pas encore d'évaluation
- Self Study Intraoral Anatomy RadiologyDocument80 pagesSelf Study Intraoral Anatomy RadiologydeenmPas encore d'évaluation
- Hospital MedicineDocument36 pagesHospital MedicineCarlos HernándezPas encore d'évaluation
- Application LetterDocument3 pagesApplication LetterElisya KharuniawatiPas encore d'évaluation
- SALVO Newsletter Apr 15Document2 pagesSALVO Newsletter Apr 15Women's Health Research UnitPas encore d'évaluation
- Persistent Pulmonary Hypertension of The NewbornDocument4 pagesPersistent Pulmonary Hypertension of The NewbornMarwa Adly100% (1)
- Otitis MediaDocument7 pagesOtitis MediaNorminaKiramAkmadPas encore d'évaluation
- TSCUH Trachy Bed Head PDFDocument4 pagesTSCUH Trachy Bed Head PDFTudistef Analize SanatatePas encore d'évaluation
- Management of Neonatal Seizures: AIIMS-NICU Protocols 2010Document18 pagesManagement of Neonatal Seizures: AIIMS-NICU Protocols 2010gitphillipPas encore d'évaluation
- EM Case Write UpDocument11 pagesEM Case Write UpRaihana Rafi100% (2)
- Organistional Study: at V.S.M HospitalDocument10 pagesOrganistional Study: at V.S.M HospitalBinsa ThomasPas encore d'évaluation
- Neurosurgery Direct 6 Yrs PDFDocument31 pagesNeurosurgery Direct 6 Yrs PDFSoumitraPas encore d'évaluation
- Nelson MCQ PDFDocument595 pagesNelson MCQ PDFPavan Kumar100% (5)
- Trinity Health v. Anesthesia Associates of Ann ArborDocument53 pagesTrinity Health v. Anesthesia Associates of Ann ArborAlex KacikPas encore d'évaluation
- Acne Vulgaris PDFDocument8 pagesAcne Vulgaris PDFsmackooooooPas encore d'évaluation
- Journal Club: Surfactant Therapy in Premature InfantsDocument44 pagesJournal Club: Surfactant Therapy in Premature InfantsSubash PaudealPas encore d'évaluation
- Basal Cell Carcinoma: CausesDocument5 pagesBasal Cell Carcinoma: CausesRini LianingsihPas encore d'évaluation
- NCM 33 Framework For Maternal and Child Health Nursing: ST ST RD ND TH TH RD TH TH THDocument5 pagesNCM 33 Framework For Maternal and Child Health Nursing: ST ST RD ND TH TH RD TH TH THSherika Mariz Moreno GuarinPas encore d'évaluation
- Dpco Norms 2011Document25 pagesDpco Norms 2011NAVNEET BAGGAPas encore d'évaluation