Académique Documents
Professionnel Documents
Culture Documents
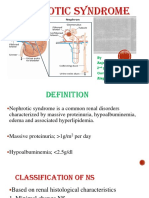
Nephrotic Syndrome I
Transféré par
Robert MontgomeryCopyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Nephrotic Syndrome I
Transféré par
Robert MontgomeryDroits d'auteur :
Formats disponibles
GUIDELINES FOR PRACTICE
INTRODUCTION
Management of Steroid Sensitive
Nephrotic Syndrome:
Revised Guidelines
Nephrotic syndrome is an important chronic disease
in children. About 80% children with idiopathic
nephrotic syndrome show remission of proteinuria
following treatment with corticosteroids, and are
classified as steroid sensitive. Most patients have
multiple relapses, placing them at risk for steroid
toxicity, systemic infections and other complications. A small proportion of patients who are not
steroid sensitive (steroid resistant) are also at risk for
similar complications and renal insufficiency.
INDIAN PEDIATRIC NEPHROLOGY GROUP,
INDIAN ACADEMY OF PEDIATRICS
ABSTRACT
Justification: In 2001, the Indian Pediatric Nephrology
Group formulated guidelines for management of patients
with steroid sensitive nephrotic syndrome. In view of
emerging scientific evidence, it was felt necessary to
review the existing recommendations. Process:
Following a preliminary meeting in March 2007, a draft
statement was prepared and circulated among pediatric
nephrologists in the country to arrive at a consensus on
the evaluation and management of these patients.
Objectives: To revise and formulate recommendations
for management of steroid sensitive nephrotic syndrome.
Recommendations: The need for adequate corticosteroid therapy at the initial episode is emphasized.
Guidelines regarding the initial evaluation, indications
for renal biopsy and referral to a pediatric nephrologist
are updated. It is proposed that patients with frequently
relapsing nephrotic syndrome should, at the first
instance, be treated with long-term, alternate-day
prednisolone. The indications for use of alternative
immunosuppressive agents, including levamisole,
cyclophosphamide, mycophenolate mofetil and
cyclosporin are outlined. The principles of dietary
therapy, management of edema, and prevention and
management of complications related to nephrotic
syndrome are described. These guidelines, formulated on
basis of current best practice, are aimed to familiarize
physicians regarding management of children with
steroid sensitive nephrotic syndrome.
Most pediatricians would encounter few patients
with nephrotic syndrome in their practice. They
should be familiar with management of these
patients and be aware of situations in which referral
to a pediatric nephrologist is required. Long-term
management of these patients should thereafter be a
joint effort between the pediatrician and the pediatric
nephrologist.
OBJECTIVES
Guidelines on the management of children with
nephrotic syndrome were first formulated by the
Indian Pediatric Nephrology Group in 2001(1).
Since a number of studies on management of these
patients have been published during the last 7 years,
it was felt desirable to review the existing
recommendations. Therefore, following a preliminary meeting in New Delhi (7 March 2007), a draft
statement was prepared, circulated and reviewed
by pediatric nephrologists across the country
(Annexure I). The present document reflects the
current opinion on management of patients with
steroid sensitive nephrotic syndrome.
RECOMMENDATIONS
Key words: Nephrotic syndrome, Practice guidelines,
Recommendations.
Important revisions in this document are listed in
Table I.
Correspondence to: Dr. Arvind Bagga, Department of
Pediatrics, All India Institute of Medical Sciences, Ansari
Nagar, New Delhi 110 029, India.
E-mail: arvindbagga@hotmail.com
INDIAN PEDIATRICS
Definitions
Nephrotic syndrome is characterized by heavy
proteinuria, hypoalbuminemia (serum albumin
203
VOLUME 45__MARCH 17, 2008
IAP NEPHROLOGY GROUP
TABLE I IMPORTANT REVISIONS IN THIS DOCUMENT
Investigations necessary at initial and subsequent evaluation are described.
While updating the literature, the Group endorses the existing guidelines on therapy for the initial episode of nephrotic
syndrome.
The role of alternative medications, including mycophenolate mofetil, cyclosporin and tacrolimus in patients with
frequent relapses and steroid dependence is discussed and therapeutic choices further clarified.
Details on dose and duration of therapy with corticosteroids, when co-administered with other agents are included.
Guidelines on immunization, isoniazid prophylaxis and hypertension updated in conformity with recommendations of
the Indian Academy of Pediatrics.
Management of complications updated.
<2.5 g/dL), hyperlipidemia (serum cholesterol >200
mg/dL) and edema(1,2). Nephrotic range proteinuria
is present if early morning urine protein is 3+/4+ (on
dipstick or boiling test), spot protein/creatinine ratio
>2 mg/mg, or urine albumin excretion >40 mg/m2
per hr (on a timed-sample). Precise quantitative
assessment of proteinuria, including 24-hr urine
protein measurement is seldom necessary.
Definitions for clarifying the course of nephrotic
syndrome are shown in Table II.
creatinine. Estimation of blood levels of antistreptolysin O and C3 is required in patients
with gross or persistent microscopic hematuria.
Appropriate tests are performed, if necessary, for
associated conditions (e.g., chest X-ray and tuberculin test, hepatitis B surface antigen, antinuclear
antibodies). Urine culture is not necessary unless the
patient has clinical features suggestive of a urinary
tract infection.
Treatment of the Initial Episode
Initial Evaluation
Adequate treatment of the initial episode, both in
terms of dose and duration of corticosteroids, is
important. Evidence from multiple studies suggests
that appropriate therapy at the first episode of
nephrotic syndrome is an important determinant of
the long-term course of the disease(3).
A detailed evaluation is necessary before starting
treatment with corticosteroids. The height, weight
and blood pressure should be recorded. Regular
weight record helps monitor the decrease or increase
of edema. Physical examination is done to detect
infections and underlying systemic disorder, e.g.,
systemic lupus erythematosus, Henoch Schonlein
purpura, etc. Infections should be treated before
starting therapy with corticosteroids.
Medication: The standard medication for treatment
is prednisolone or prednisone. The medication is
administered after meals to reduce its gastrointestinal side effects. The use of methylprednisolone, dexamethasone, betamethasone, triamcinolone or hydrocortisone is not recommended.
There is also limited evidence on the efficacy or
Investigations recommended at the initial
episode include: (i) urinalysis; (ii) complete blood
count, blood levels of albumin, cholesterol, urea and
TABLE II DEFINITIONS RELATED TO NEPHROTIC SYNDROME
Remission
Urine albumin nil or trace (or proteinuria <4 mg/m2/h) for 3 consecutive early morning specimens.
Relapse
Urine albumin 3+ or 4+ (or proteinuria >40 mg/m2/h) for 3 consecutive early morning specimens,
having been in remission previously.
Frequent relapses
Two or more relapses in initial six months or more than three relapses in any twelve months.
Steroid dependence
Two consecutive relapses when on alternate day steroids or within 14 days of its discontinuation.
Steroid resistance
Absence of remission despite therapy with daily prednisolone at a dose of 2 mg/kg per day for 4 weeks.
INDIAN PEDIATRICS
204
VOLUME 45__MARCH 17, 2008
GUIDELINES: NEPHROTIC SYNDROME
benefits of therapy with deflazocort for nephrotic
syndrome.
rarely result in spontaneous remission, thereby
avoiding the need for treatment with corticosteroids.
Treatment regimen: Various treatment regimens
have been used for the treatment of the initial episode
of nephrotic syndrome. The International Study
for Kidney Diseases in Children had originally
recommended a regimen comprising of four-weeks
each of daily and alternate day steroid therapy(4),
which was used for almost three decades. Controlled
studies later suggested that prolongation of initial
steroid therapy for 12 weeks or longer is associated
with significantly reduced risk for subsequent
relapses. However, prolonged treatment with
steroids is associated with a higher frequency of
adverse events(3,5,6).
Prednisolone is administered at a dose of
2 mg/kg/day (single or divided doses) until urine
protein is trace or nil for three consecutive days.
Subsequently, prednisolone is given in a single
morning dose of 1.5 mg/kg on alternate days for
4 weeks, and then discontinued(1,5). The usual
duration of treatment for a relapse is thus 5-6 weeks.
Prolongation of therapy is not necessary for patients
with infrequent relapses (see below).
In case the patient is not in remission despite two
weeks treatment with daily prednisolone, the
treatment is extended for 2 more weeks. Patients
showing no remission despite 4 weeks treatment
with daily prednisolone should be referred for
evaluation.
The Cochrane Renal Group(3), on systematic
analysis of the literature, recommends that the
duration of initial prednisolone therapy should be for
a minimum of 12 weeks. It further suggests that the
benefits of sustained remission and reduction in
relapse rates are superior if alternate-day treatment is
not stopped abruptly at 12 weeks, but tapered over
the next 2-4 months. It is emphasized that none of the
studies included in this analysis was placebocontrolled, most lacked allocation concealment and
were not powered to evaluate side effects of
prolonged treatment(3). The debate regarding
appropriate dose and duration of steroid treatment is
not resolved. Other regimens are being examined
that reduce the risk of relapse without increased side
effects.
Infrequent Relapsers
Patients who have three or less relapses a year and
respond promptly to prednisolone are managed
using the aforementioned regimen for each relapse.
Such children are at a low risk for developing steroid
toxicity.
Frequent Relapsers and Steroid Dependence
Patients with frequent relapses or steroid
dependence should be managed in consultation with
a pediatric nephrologist.
Based on current evidence and opinion, the
Group recommends that the initial episode of
nephrotic syndrome be treated with prednisolone at a
dose of 2 mg/kg per day (maximum 60 mg in single
or divided doses) for 6 weeks, followed by 1.5 mg/kg
(maximum 40 mg) as a single morning dose on
alternate days for the next 6 weeks; therapy is then
discontinued. The benefits and safety of prolonged
initial steroid therapy, beyond 12 weeks, require
confirmation from further studies.
It is usually not necessary to perform a renal
biopsy in these cases. Following treatment of a
relapse, prednisolone is gradually tapered to
maintain the patient in remission on alternate day
dose of 0.5-0.7 mg/kg, which is administered for 918 months. A close monitoring of growth and blood
pressure, and evaluation for features of steroid
toxicity is essential. If the prednisolone threshold,
to maintain remission, is higher or if features of
corticosteroid toxicity are seen, additional use of the
following immuno-modulators is suggested.
Treatment of Relapse
(a)
The patient should be examined for infections,
which should be treated before initiating steroid
therapy. Appropriate therapy of an infection might
INDIAN PEDIATRICS
205
Levamisole is administered at a dose of
2-2.5 mg/kg on alternate days for 12-24
months(7-9). Co-treatment with prednisolone
at a dose of 1.5 mg/kg on alternate days is given
for 2-4 weeks; its dose is gradually reduced
VOLUME 45__MARCH 17, 2008
IAP NEPHROLOGY GROUP
by 0.15-0.25 mg/kg every 4 weeks to a maintenance dose of 0.25-0.5 mg/kg that is continued
for six or more months. Occasionally, it might
be possible to discontinue treatment with
corticosteroids. The chief side effect of
levamisole is leukopenia; flu-like symptoms,
liver toxicity, convulsions and skin rash are
rare. The leukocyte count should be monitored
every 12-16 weeks.
(b)
nephrotoxicity (increase in serum creatinine by
30% or more from the baseline)(12). Trough
(12-hr) CsA levels should be kept between 80120 ng/mL(12). Side effects of CsA therapy
include hypertension, cosmetic symptoms
(gum hypertrophy, hirsutism) and nephrotoxicity; hypercholesterolemia and elevated
transaminases may occur. Estimation of blood
levels of creatinine is required every 2-3
months and a lipid profile annually. A repeat
kidney biopsy, to examine for histological
evidence of nephrotoxicity, should be done if
therapy with calcineurin inhibitors is extended
beyond 2 years(12).
Cyclophosphamide is administered at a
dose of 2-2.5 mg/kg/day for 12 weeks(10).
Prednisolone is co-administered at a dose of
1.5 mg/kg on alternate days for 4 weeks,
followed by 1 mg/kg for the next 8 weeks;
steroid therapy is tapered and stopped over the
next 2-3 months. Therapy with cyclophosphamide should be instituted preferably
following remission of proteinuria.
Tacrolimus is an alternative agent, administered at a dose of 0.1-0.2 mg/kg daily for 12-24
months. Side effects include hyperglycemia,
diarrhea and rarely neurotoxicity (headache,
seizures). The use of tacrolimus is preferred
especially in adolescents, because of lack of
cosmetic side effects(13). Blood levels of
creatinine and glucose should be estimated
every 2-3 months.
Total leukocyte counts are monitored every
2 weeks; treatment with cyclophosphamide is
temporarily discontinued if the count falls
below 4000/mm3. An increased oral fluid
intake and frequent voiding prevents the
complication of hemorrhagic cystitis; other
side effects are alopecia, nausea and vomiting.
The risk of gonadal toxicity is limited with
a single (12 weeks) course of cyclophosphamide(7,10,11). The use of more than
one course of this agent should preferably be
avoided.
(d)
In view of its toxicity, the use of
chlorambucil, unless under close supervision,
is not recommended.
(c)
Choice of agent: The advantages of using these
drugs should be balanced against their potential
toxicity. There are few studies comparing one agent
with another, but evidence for efficacy is strongest
for cyclophosphamide and CsA. Levamisole has a
modest steroid sparing effect and is a satisfactory
initial choice for patients with frequent relapses or
steroid dependence. Treatment with cyclophosphamide is preferred in patients showing: (i) significant
steroid toxicity, (ii) severe relapses with episodes
of hypovolemia or thrombosis, and (iii) poor
compliance or difficult follow up, where 12 weeks
therapy might be possible to ensure than long-term
compliance.
Calcineurin inhibitors: Cyclosporin (CsA) is
given at a dose of 4-5 mg/kg daily for 12-24
months. Prednisolone is co-administered at a
dose of 1.5 mg/kg on alternate days for 2-4
weeks; its dose is gradually reduced by 0.150.25 mg/kg every 4 weeks to a maintenance
dose of 0.25-0.5 mg/kg that is continued for six
or more months. Occasionally, treatment with
corticosteroids may be discontinued.
Estimation of trough blood levels of CsA is
required in patients with suspected noncompliance, unsatisfactory response or
INDIAN PEDIATRICS
Mycophenolate mofetil (MMF) is given at a
dose of 800-1200 mg/m2 along with tapering
doses of prednisolone for 12-24 months(7,14).
The principal side effects include gastrointestinal discomfort, diarrhea and leukopenia.
Leukocyte counts should be monitored every
1-2 months; treatment is withheld if count falls
below 4000/mm3.
Treatment
206
with
CsA
or
tacrolimus
is
VOLUME 45__MARCH 17, 2008
GUIDELINES: NEPHROTIC SYNDROME
corticosteroids stimulates appetite, parents should be
advised regarding ensuring physical activity and
preventing excessive weight gain.
recommended for patients who continue to show
steroid dependence or frequent relapses despite
treatment with the above medications(12). Either of
these agents is effective in maintaining remission in
most patients with steroid sensitive nephrotic
syndrome. The chief concern with their use is
nephrotoxicity, but with careful assessment of renal
function, minimizing the maintenance dose and
utilizing renal biopsies in those receiving prolonged
therapy, this risk can be minimized. Recent case
series(14) and a controlled trial(15) support the use
of MMF as a steroid sparing agent. The lack of renal,
hemodynamic and metabolic toxicity with this agent
makes it an attractive alternative to calcineurin
inhibitors.
Edema: Control of edema is an integral part of
supportive care. Since treatment with corticosteroids
usually leads to diuresis within 5-10 days, diuretics
are avoided unless edema is significant. Diuretics
should also not be given to patients with diarrhea,
vomiting or hypovolemia.
Patients with persistent edema and weight gain of
7-10% are treated with oral frusemide (1-3 mg/kg
daily). Additional treatment with potassium sparing
diuretics is not required if frusemide is used at this
dose for less than one week. Patients requiring
higher doses and prolonged duration of treatment
with frusemide should receive potassium sparing
diuretics, e.g., spironolactone (2-4 mg/kg daily).
Blood pressure should be monitored frequently. A
gradual reduction of edema, over one week, is
preferred(16,17).
In some patients receiving therapy with
levamisole, MMF and calcineurin inhibitors,
treatment with prednisolone might be tapered and
discontinued after 6-12 months. Some patients who
respond to therapy with levamisole, MMF and
calcineurin inhibitors may relapse once these
medications are discontinued. Relapses during or
following therapy with these agents are treated with
prednisolone as described above.
Edema not responding to the above therapy
should be managed in a hospital. A combination of a
loop and thiazide diuretic, and/or a potassium
sparing agent is occasionally necessary. For patients
with refractory edema, a combination of diuretics
and albumin infusion is used. Albumin (20%) is
given as an infusion at a dose of 0.5-1 g/kg over 2-4
hr, followed by administration of frusemide (1-2 mg/
kg intravenously). While infusion of albumin results
in increased urine output, the effect is not sustained
and repeated administration might be necessary.
Albumin should be administered very cautiously in
patients with renal failure, pneumonia or pulmonary
edema due to its potential to increase the plasma
volume. Patients receiving albumin should be
observed for respiratory distress, hypertension
and congestive heart failure. Refractory ascites
interfering with respiration or associated with breaks
in the skin may be removed by cautious paracentesis.
A protocol for treatment of edema is shown in Fig. 2.
Failure of alternative medication: If a patient has
two or more relapses over 6 months while on
treatment with any of the above agents, its
replacement with an alternative medication should
be considered. A protocol summarizing the
management of patients with steroid sensitive
nephrotic syndrome is shown in Fig. 1.
Supportive Care
This forms an important aspect of managing children
with nephrotic syndrome.
Diet: A balanced diet, adequate in protein (1.5-2 g/
kg) and calories is recommended. Patients with
persistent proteinuria should receive 2-2.5 g/kg of
protein daily(16). Not more than 30% calories
should be derived from fat and saturated fats
avoided. While salt restriction is not necessary in
most patients with steroid sensitive nephrotic
syndrome, reduction of salt intake (1-2 g per day) is
advised for those with persistent edema. Salt should
not be added to salads and fruits, and snacks
containing high salt avoided. Since treatment with
INDIAN PEDIATRICS
Patient and parent education: Long-term outcome of
children with steroid sensitive nephrotic syndrome is
satisfactory, with the majority in sustained remission
and with normal renal functions by adolescence. A
proportion of patients, especially those (i) with early
onset of nephrotic syndrome, (ii) with a frequently
207
VOLUME 45__MARCH 17, 2008
IAP NEPHROLOGY GROUP
First Episode of Nephrotic Syndrome
Absence of hypertension, hematuria, azotemia
Prednisolone 2 mg/kg daily for 6 weeks, followed by 1.5 mg/kg on alternate days for 6 weeks
Infrequent
relapses
Frequent relapses
Steroid dependence
Prednisolone 2 mg/kg daily
until remission, then 1.5 mg/kg
on alternate days for 4 weeks
Refer for evaluation
Alternate day prednisolone to
maintain remission; assess
steroid threshold
Refer for evaluation
Therapy based on renal
biopsy findings
Steroid
resistance
Threshold >0.5-0.7 mg/kg on alternate
days or steroid toxicity
Threshold <0.5-0.7 mg/kg on alternate days
Alternate day
prednisolone for
9-18 months
Levamisole
Cyclophosphamide, Tacrolimus,
Mycophenolate mofetil,
Cyclosporin
FIG. 1. Management of patients with steroid sensitive nephrotic syndrome.
relapsing course, and (iii) requiring treatment with
alkylating agents or CsA may continue to show
relapses beyond adolescence(18). Parents should be
reassured that despite a relapsing course, progression
to end stage renal failure necessitating dialysis or
transplantation is extremely rare.
expected course and risk of complications. The
following are emphasized:
(a)
Parental motivation and involvement is essential
in the long-term management of these children. They
should be provided information about the disease, its
INDIAN PEDIATRICS
208
Urine examination for protein at home using
dipstick, sulfosalicylic acid or boiling test. The
examination should be done every morning
during a relapse, during intercurrent infections
or if there is even mild periorbital puffiness.
The frequency of urine examination is
reduced, to once or twice a week, during
VOLUME 45__MARCH 17, 2008
GUIDELINES: NEPHROTIC SYNDROME
Examine for hypovolemia
remission. The importance of detecting relapse
before development of significant edema is
stressed.
Yes*
No
Frusemide 1-3 mg/kg/day
May add spironolactone 2-4 mg/kg/day
No response
` (no weight loss or diuresis
in 48 h)
Double dose of frusemide until diuresis
or maximum daily dose of frusemide
(4-6 mg/kg/day) is reached
No response
No response
Frusemide IV bolus 1-3 mg/kg/dose
or infusion 0.1-1 mg/kg/h
(c)
Ensure normal activity and school attendance;
the child should continue to participate in all
activities and sports.
(d)
Since infections are an important cause of
morbidity, patients should receive appropriate
immunization and other measures for
protection.
Immunization: Parents should be advised regarding
the need for completing the primary immunization.
Administration of some vaccines, e.g., hepatitis B,
measles-mumps-rubella or meningococcal vaccines
may rarely precipitate a relapse.
No response
Patients receiving prednisolone at a dose of 2 mg/
kg/day or greater, or total 20 mg/day or greater (for
patients weighing >10 kg) for more than 14 days are
considered immunocompromised(20). Such patients
should not receive live attenuated vaccines;
inactivated or killed vaccines are safe(20). Live
vaccines are administered once the child is off
immunosuppressive medications for at least 4
weeks. If there is a pressing need, these vaccines may
be given to patients receiving alternate day
prednisolone at a dose less than 0.5 mg/kg.
20% Albumin 1 g/kg IV
followed by IV frusemide
FIG. 2. Management of edema in patients with nephrotic
syndrome. Patients requiring high-dose frusemide or
addition of other diuretics should be under close
supervision, preferably in a hospital. Monitoring of
serum electrolytes is necessary in all patients
receiving diuretics. Patients showing hypokalemia
require potassium supplements or co-administration
of spironolactone. The medications are reduced
stepwise once diuresis ensues.
* Management of hypovolemia consists of rapid infusion of
normal saline at a dose of 15-20 mL/kg over 20-30 minutes;
this may be repeated if clinical features of hypovolemia
persist. Infusion of 5% albumin (10-15 mL/kg) or 20%
albumin (0.5-1 g/kg) may be used in subjects who do not
respond despite two boluses of saline.
INDIAN PEDIATRICS
Maintain a diary showing results of urine
protein examination, medications received and
intercurrent infections.
Other medications: The use of antacids or histamine
receptor antagonists (e.g., ranitidine) is not
necessary, unless there are symptoms of upper
gastrointestinal discomfort. Long-term calcium
supplementation (calcium carbonate, 250-500 mg) is
necessary if the patient receives more than 3 months
treatment with prednisolone(19). Patients with
steroid sensitive nephrotic syndrome do not usually
require medications for hyperlipidemia, since lipids
normalize following remission.
Add hydrochlorthiazide 1-2 mg/kg/day
or metolazone 0.1-0.3 mg/kg/day
(b)
All children with nephrotic syndrome should
receive immunization against pneumococcal
infections(21). It is important to note that not all
pneumococcal serotypes are included in the vaccines
and that antibody levels may decline during a
209
VOLUME 45__MARCH 17, 2008
IAP NEPHROLOGY GROUP
TABLE III INDICATIONS FOR KIDNEY BIOPSY
relapse. Previously vaccinated children may, therefore, develop pneumococcal peritonitis and sepsis.
The Expert Group endorses the recommendations of
the Immunization Committee of the Indian Academy
of Pediatrics(22). The Committee recommends 2-4
doses of the heptavalent conjugate pneumococcal
vaccine for children below 2 yr of age. For
previously unimmunized children between 2-5 yr
old, a priming dose of the conjugate vaccine should
be followed 8 weeks later, by a dose of the 23-valent
polysaccharide vaccine. Children older than 5 yr
require only a single dose of the polysaccharide
vaccine. The vaccine should be given during
remission, preferably when the child is not receiving
daily prednisolone. Revaccination after 5 yr is
considered for children (<10-yr-old) with active
nephrotic syndrome.
At Onset
Age of onset <1 year.
Gross hematuria, persistent microscopic hematuria or
low serum C3.
Sustained hypertension.
Renal failure not attributable to hypovolemia.
Suspected secondary causes of nephrotic syndrome.
After Initial Treatment
Proteinuria persisting despite 4-weeks of daily
corticosteroid therapy.
Before treatment with cyclosporin A or tacrolimus.
Complications
Patients with steroid sensitive nephrotic syndrome
are at risk for certain complications, early detection
of which is necessary.
Patients in remission and not on immunosuppressive therapy should receive the varicella
vaccine. One dose is recommended for children
between 12 months and 12 yr of age, and 2 doses
separated by an interval of at least 4 weeks for
children 13 yr or older(23).
Infections: Children with nephrotic syndrome are
susceptible to severe infections, which need prompt
treatment. Common infections include peritonitis,
cellulitis and pneumonia. Viral and bacterial infections may occasionally precipitate relapses in
patients previously in remission. The clinical
features and management of common serious
infections are summarized in Table V.
Kidney Biopsy
Children with idiopathic nephrotic syndrome not
having hematuria, hypertension or impaired renal
function are treated with corticosteroids without
requiring a kidney biopsy. A biopsy is usually not
necessary in patients with frequent relapses or
steroid dependence before starting treatment with
levamisole, cyclophosphamide or MMF, but should
be performed before therapy with calcineurin
inhibitors. A biopsy is required to identify the
underlying renal disease in certain cases
(Table III).
Varicella may be a severe illness in patients with
nephrotic syndrome receiving corticosteroids or
other immunosuppressive drugs. Susceptible
patients (those unimmunized or with no history of
varicella) who are exposed to a case of chickenpox
TABLE IV INDICATIONS FOR REFERRAL
NEPHROLOGIST
Kidney biopsies must be performed by experts
with experience in the procedure. Centers that
perform kidney biopsies should have facilities for
evaluation of the specimens by light and immunofluorescence microscopy.
Referral to Pediatric Nephrologist
Indications for referral of patients are given in
Table IV. The care of these patients should be a joint
collaboration between the pediatrician and pediatric
nephrologist.
INDIAN PEDIATRICS
210
TO A
PEDIATRIC
Onset below 1-year of age; family history of nephrotic
syndrome.
Nephrotic syndrome with hypertension, gross/persistent
microscopic hematuria, impaired renal function, or
extrarenal features (e.g., arthritis, serositis, rash).
Complications: refractory edema, thrombosis, severe
infections, steroid toxicity.
Resistance to steroid therapy.
Frequently relapsing or steroid dependent nephrotic
syndrome.
VOLUME 45__MARCH 17, 2008
GUIDELINES: NEPHROTIC SYNDROME
should therefore receive a single dose of varicella
zoster immunoglobulin, within 96 hr of exposure to
prevent or lessen the severity of the disease(17).
Since, this preparation is expensive and not easily
available, a single dose of intravenous immunoglobulin (400 mg/kg) may be used instead(23).
However, no clinical data showing the effectiveness
of the latter strategy are available.
immobilization, indwelling vascular catheters,
aggressive diuretic use and puncture of deep vessels
predispose to thrombus formation. Renal vein
thrombosis is suspected in a patient with oligoanuria,
hematuria or flank pain, especially following an
episode of dehydration. Femoral and mesenteric
arterial thrombosis may occasionally occur. Deep
vein thrombosis of calf veins is less common in
children but may lead to pulmonary embolism.
Saggital sinus and cortical venous thrombosis may
follow episodes of diarrhea and present with
convulsions, vomiting, altered sensorium and
neurological deficits. Ultrasonography, Doppler
studies and cranial MRI are useful in confirming the
diagnosis.
Patients who develop varicella should receive
intravenous acyclovir (1500 mg/m2/day in 3 doses)
or oral acyclovir (80 mg/kg/day in 4 doses) for
7-10 days(23). The dose of prednisolone should be
tapered to 0.5 mg/kg/day or lower during the
infection.
Patients with nephrotic syndrome who are
Mantoux positive but show no evidence of
tuberculosis should receive prophylaxis with INH
for six months(24). Those showing evidence of
active tuberculosis should receive standard therapy
with anti-tubercular drugs.
Patients with thrombotic complications require
urgent treatment. The treatment includes correction
of dehydration and other complications, and
use of heparin (IV) or low-molecular-weight
heparin (subcutaneously) initially, followed by oral
anti-coagulants on the long-term(16,17). There
is no role for prophylactic treatment with
anticoagulants in patients with hypoalbuminemia
and edema.
Thrombosis: Children with nephrotic syndrome
are at risk for venous and, rarely, arterial
thrombosis(16,17). Reduced intravascular volume,
TABLE V CLINICAL FEATURES AND MANAGEMENT OF INFECTIONS*
Infection
Clinical features
Common organisms
Antibiotics, duration of
treatment
Peritonitis
Abdominal pain, tenderness,
distension; diarrhea, vomiting;
ascitic fluid >100 leukocytes/mm3;
>50% neutrophils
S. pneumoniae,
S. pyogenes,
E. coli
Cefotaxime or ceftriaxone
for 7-10 days;
ampicillin and an aminoglycoside
for 7-10 days
Pneumonia
Fever, cough, tachypnea, intercostal,
recessions, crepitations
S. pneumoniae,
H. influenzae,
S. aureus
Oral: amoxicillin, co-amoxiclav,
erythromycin
Parenteral: ampicillin and
aminoglycoside; or
cefotaxime/ceftriaxone
for 7-10 days
Cellulitis
Cutaneous erythema, induration,
tenderness
Staphylococci,
Group A streptococci,
H. influenzae
Cloxacillin and ceftriaxone
for 7-10 days
Co-amoxiclav
Fungal
infections
Pulmonary infiltrates, persistent
fever unresponsive to antibiotics,
sputum/urine showing septate hyphae
Candida, Aspergillus spp.
Skin, mucosa: fluconazole
for 10 days
Systemic: Amphotericin
for 14-21 days
*Supplemental stress doses of hydrocortisone or prednisolone are usually necessary
INDIAN PEDIATRICS
211
VOLUME 45__MARCH 17, 2008
IAP NEPHROLOGY GROUP
Hypertension: This may be detected at the onset of
nephrotic syndrome or later due to steroid toxicity.
Therapy is initiated with ACE inhibitors, calcium
channel blockers or adrenergic antagonists,
keeping the blood pressure at less than the 90th
percentile(25).
and revised based on systematic reviews, published
studies and expert opinion of the members of the
Indian Pediatric Nephrology Group. These
guidelines are intended to familiarize physicians
with principles of management of children with
steroid sensitive nephrotic syndrome. Therapy needs
to be individualized for each patient and optimal care
will be achieved by combined inputs of the primary
pediatrician and pediatric nephrologist. Further
revisions of these guidelines, indicating best current
practice, shall be periodically necessary.
Hypovolemic shock: This complication can occur
due to unsupervised use of diuretics especially if
accompanied by septicemia, diarrhea or vomiting.
The diagnosis is suggested by moderate to severe
abdominal pain, hypotension, tachycardia, cold
extremities and poor capillary refill; hematocrit and
blood levels of urea and uric acid are elevated.
Management consists of rapid infusion of normal
saline at a dose of 15-20 mL/kg over 20-30 minutes;
this is repeated if clinical features of hypovolemia
persist. Infusion of 5% albumin (10-15 mL/kg) or
20% albumin (0.5-1 g/kg) may be used in subjects
who do not respond despite two boluses of saline.
Annexure I
Members of the Review Committee
Kamran Afzal, Jawaharlal Nehru Medical College,
Aligarh; Indira Agarwal, Christian Medical College
Hospital, Vellore; Vinay Agarwal, Max Hospital,
New Delhi; Uma Ali, Bai Jerbai Wadia Hospital for
Children, Mumbai; Sanjeev Bagai, Rockland
Hospital, New Delhi; Arvind Bagga, All India
Institute of Medical Sciences, New Delhi
(Convenor); Sushmita Banerjee, Calcutta Medical
Research Institute, Kolkata; Ashima Gulati, All India
Institute of Medical Sciences, Delhi; Sanjeev Gulati,
Fortis Hospital, New Delhi; Pankaj Hari, All India
Institute of Medical Sciences, New Delhi
(Secretary); Arpana Iyengar, St. Johns Medical
College, Bangalore; OP Jaiswal, Sunder Lal Jain
Hospital, New Delhi; Rupesh Jain, Ekta Hospital for
Children, Raipur; M Kanitkar, Armed Forces
Medical College, Poona; Mukta Mantan, Maulana
Azad Medical College, New Delhi; Kamini Mehta,
Lilavati Hospital & Research Center, Mumbai;
Kumud Mehta, Jaslok Hospital & Research Center &
Bai Jerbai Wadia Hospital for Children, Mumbai; BR
Nammalwar, Kanchi Kamakoti CHILDS Trust
Hospital, Chennai; Amitava Pahari, Apollo
Hospital, Kolkata; Saroj K Patnaik, No.12 Air Force
Hospital, Gorakhpur; KD Phadke, St. Johns
Medical College, Bangalore; PK Pruthi, Sir
Gangaram Hospital, New Delhi; Abhijeet Saha,
Government Medical College, Chandigarh; VK
Sairam, Sri Ramchandra Medical College, Chennai;
Jayati Sengupta, AMRI Hospital, Kolkata; Prabha
Senguttuvan, Institute of Child Health, Chennai
(Chairperson); Sidharth K Sethi, All India Institute of
Medical Sciences, New Delhi; Mehul Shah, Apollo
Corticosteroid side effects: Prolonged steroid
therapy may be associated with significant side effects. Patients (if they can understand) and the parents should be explained about the side effects of the
medications, including increased appetite, impaired
growth, behavioral changes, risk of infections, salt
and water retention, hypertension and bone demineralization. All patients should be monitored for
cushingoid features and blood pressure; six-monthly
record of height and weight, and yearly evaluation
for cataract should be done. Patients on prolonged
(>3 months) treatment with steroids should receive
daily supplements of oral calcium (250-500 mg
daily) and vitamin D (125-250 IU)(19).
Steroids during stress: Patients who have received
high-dose steroids for more than 2 weeks in the past
year are at risk of suppression of the hypothalamopituitary-adrenal axis. These children require
supplementation of steroids during surgery,
anesthesia or serious infections(26). Corticosteroids
are supplemented, as parenteral hydrocortisone
at a dose of 2-4 mg/kg/day, followed by oral
prednisolone at 0.3-1 mg/kg/day. This is given for the
duration of stress and then tapered rapidly.
CONCLUSIONS
Recommendations on management of nephrotic
syndrome, proposed in 2001, have been reexamined
INDIAN PEDIATRICS
212
VOLUME 45__MARCH 17, 2008
GUIDELINES: NEPHROTIC SYNDROME
9.
Davin JC, Merkus MP. Levamisole in steroidsensitive nephrotic syndrome of childhood: the lost
paradise? Pediatr Nephrol 2005; 20: 10-14.
10.
Latta K, von Schnakenburg C, Ehrich JHH. A metaanalysis of cytotoxic treatment for frequently
relapsing nephrotic syndrome in children. Pediatr
Nephrol 2001; 16: 271-282.
11.
Kyrieleis HA, Levtchenko EN, Wetzels JF. Longterm outcome after cyclophosphamide treatment in
children with steroid-dependent and frequently
relapsing minimal change nephrotic syndrome. Am
J Kidney Dis 2007; 49: 592-597.
12.
Cattran DC, Alexopoulos E, Heering P, Hoyer PF,
Johnston A, Meyrier A, et al. Cyclosporin in
idiopathic glomerular disease associated with the
nephrotic syndrome: Workshop recommendations.
Kidney Int 2007; 72: 1429-1447.
13.
Hodson EM, Willis NS, Craig JC. Corticosteroid
therapy for nephrotic syndrome in children.
Cochrane Database System Rev 2007; CD001533.
Westhoff TH, Schmidt S, Zidek W, Beige J, van der
Giet M. Tacrolimus in steroid-resistant and steroiddependent nephrotic syndrome. Clin Nephrol 2006;
65: 393-400.
14.
Primary nephrotic syndrome in children: clinical
significance of histopathologic variants of minimal
change and of diffuse mesangial hypercellularity. A
Report of the International Study of Kidney Disease
in Children. Kidney Int 1981; 20: 765-771.
Afzal K, Bagga A, Menon S, Hari P, Jordan SC.
Treatment with mycophenolate mofetil and
prednisolone for steroid-dependent nephrotic
syndrome. Pediatr Nephrol 2007; 22: 20592065.
15.
Dorresteijn E, Kist-van Holthe J, Levtchenko E,
Nauta J, Hop W, Van der Hejden A. Randomized
controlled trial of mycophenolate mofetil versus
cyclosporine A in children with frequently
relapsing nephrotic syndrome. Pediatr Nephrol
2007; 22: 1442 (28 FC)
16.
Srivastava RN, Bagga A. Nephrotic syndrome. In:
Pediatric Nephrology. 4th edition. New Delhi:
Jaypee Brothers; 2005. p. 161-200.
17.
Vogt AB, Avner ED. Nephrotic syndrome. In:
Nelson Textbook of Pediatrics. 18th edition.
Kliegman RM, Behrman RE, Jenson HB, Stanton
BF, editors. Philadelphia: WB Saunders; 2007. p
2190-2195.
Hospital, Hyderabad; Jyoti Sharma, Bharti
Vidyapeeth Medical College, Poona; RN Srivastava,
Indraprastha Apollo Hospital, New Delhi; AS
Vasudev, Indraprastha Apollo Hospital, New Delhi;
Anil Vasudevan, St. Johns Medical College,
Bangalore; and M Vijayakumar, Mehta Childrens
Hospital, Chennai.
REFERENCES
1.
2.
3.
4.
5.
Consensus Statement on Management of Steroid
Sensitive Nephrotic Syndrome. Indian Pediatric
Nephrology Group, Indian Academy of Pediatrics.
Indian Pediatr 2001; 38: 975-986.
Consensus Statement on Management and Audit
Potential for Steroid Responsive Nephrotic
Syndrome. Report of a Workshop by the British
Association for Paediatric Nephrology and
Research Unit, Royal College of Physicians. Arch
Dis Child 1994; 70: 151-157.
Hogg R, Portman RJ, Milliner D, Lemley KV, Eddy
A, Ingelfinger J. Evaluation and management of
proteinuria and nephrotic syndrome in children:
Recommendations from a pediatric nephrology
panel established at the National Kidney
Foundation
Conference
on
proteinuria,
albuminuria, risk, assessment, detection and
elimination (PARADE). Pediatrics 2000; 106:
1242-1249.
6.
Bagga A, Hari P, Srivastava RN. Prolonged versus
standard initial prednisolone treatment for
idiopathic nephrotic syndrome. Pediatr Nephrol
1999; 13: 824-827.
7.
Durkan A, Hodson EM, Willis NS, Craig JC. Noncorticosteroid treatment for nephrotic syndrome in
children. Cochrane Database System Rev 2005;
CD002290.
18.
Ruth EM, Kemper MJ, Leumann EP, Laube GF,
Neuhaus TJ. Children with steroid-sensitive
nephrotic syndrome come of age: long-term
outcome. J Pediatr 2005; 147: 202-207.
8.
Bagga A, Sharma A, Srivastava RN. Levamisole
therapy in corticosteroid dependent nephrotic syndrome. Pediatr Nephrol 1997; 11:
415-417.
19.
Gulati S, Sharma RK, Gulati K, Singh U, Srivastava
A. Longitudinal followup of bone mineral density
in children with idiopathic nephrotic syndrome.
Nephrol Dial Transpl 2005; 20: 1598-1603.
INDIAN PEDIATRICS
213
VOLUME 45__MARCH 17, 2008
IAP NEPHROLOGY GROUP
20.
21.
22.
23.
American Academy of Pediatrics. Immunization in
special clinical circumstances. In: Pickering LK,
Baker CJ, Long SS, McMillan JA. Red Book:
2006 Report of the Committee on Infectious
Diseases, 27th edn. Elk Grove Village,
IL: American Academy of Pediatrics; 2006. p. 67104.
Committee on Infectious Diseases, 27th edn. Elk
Grove Village, IL: American Academy of
Pediatrics; 2006. p. 711-725.
American Academy of Pediatrics, Committee on
Infectious Diseases. Recommendations for the
prevention of pneumococcal infections, including
the use of pneumococcal conjugate vaccine
(Prevnar), pneumococcal polysaccharide vaccine
and antibiotic prophylaxis. Pediatrics 2000; 106:
362-366.
Shah RC, Shah NK, Kukreja S. Pneumococcal
vaccines. In: Shah RC, Shah NK, Kukreja S,
editors. IAP Guide Book on Immunization.
Mumbai: 2007. p. 35-36.
Chauhan LS, Arora VK. Management of pediatric
tuberculosis under the Revised National
Tuberculosis Control Program (RNTCP). Indian
Pediatr 2004; 41: 901-905.
25.
Indian Pediatric Nephrology Group. Evaluation
and management of hypertension. Indian Pediatr
2007; 44: 103-121.
26.
Axelrod L. Glucocorticoid therapy. In: Endocrinology. 5th edition. DeGroot LJ, Jameson JL.
Philadelphia: Elsevier Saunders; 2006. p. 23292342.
Writing Committee
Uma Ali, Arvind Bagga, Sushmita Banerjee,
Madhuri Kanitkar, Kishore D Phadke, Prabha
Senguttuvan, Sidharth Sethi and Mehul Shah, on
behalf of the Indian Pediatric Nephrology Group.
American Academy of Pediatrics. Varicella-zoster
infections. In: Pickering LK, Baker CJ, Long SS,
McMillan JA. Red Book: 2006 Report of the
INDIAN PEDIATRICS
24.
214
VOLUME 45__MARCH 17, 2008
Vous aimerez peut-être aussi
- SRNS 2021Document44 pagesSRNS 2021Varun KotaPas encore d'évaluation
- Steroid Sensitive Nephrotic Syndrome - Indian Guidelines-1Document55 pagesSteroid Sensitive Nephrotic Syndrome - Indian Guidelines-1Tushar AmbedarePas encore d'évaluation
- Sinha2021 Article SteroidSensitiveNephroticSyndrDocument21 pagesSinha2021 Article SteroidSensitiveNephroticSyndrMrinmayeeDeshmukhPas encore d'évaluation
- SSNS CompressedDocument78 pagesSSNS CompressedVarun KotaPas encore d'évaluation
- slide_set_eular_lupus_nephritis_recommendations (1)Document16 pagesslide_set_eular_lupus_nephritis_recommendations (1)JackelineYampufeCananiPas encore d'évaluation
- Approach ConsiderationsDocument12 pagesApproach ConsiderationsTyna Mew-mewPas encore d'évaluation
- Nephrotic Syndrome Treatment & Management - Approach Considerations, Acute NephroDocument5 pagesNephrotic Syndrome Treatment & Management - Approach Considerations, Acute NephroErvirson Jair Cañon AbrilPas encore d'évaluation
- Managing Complications of Nephrotic SyndromeDocument6 pagesManaging Complications of Nephrotic SyndromeRagabi RezaPas encore d'évaluation
- Practice Essentials: Essential Update: New Guidelines From KDIGODocument13 pagesPractice Essentials: Essential Update: New Guidelines From KDIGOPratama Aditya BiantoroPas encore d'évaluation
- Intravenous Cyclophosphamide in Steroid-Resistant Nephrotic SyndromeDocument6 pagesIntravenous Cyclophosphamide in Steroid-Resistant Nephrotic SyndromeRicho WijayaPas encore d'évaluation
- Oftal Case StudyDocument11 pagesOftal Case StudyMohamad RaisPas encore d'évaluation
- 60 TeneligliptinDocument9 pages60 Teneligliptinankit AcharyaPas encore d'évaluation
- Nephrotic SyndromeDocument14 pagesNephrotic SyndromeAnna Michael AbdullahPas encore d'évaluation
- Total Parenteral Nutrition Guideline-4 - 2Document38 pagesTotal Parenteral Nutrition Guideline-4 - 2FirnandaPas encore d'évaluation
- Total Parenteral Nutrition Guideline-4 - 2Document38 pagesTotal Parenteral Nutrition Guideline-4 - 2Henry M. BarberenaPas encore d'évaluation
- Nephrotic Syndrome: BackgroundDocument7 pagesNephrotic Syndrome: BackgroundRiko JumattullahPas encore d'évaluation
- Two Cases of Recurrent ADIH in ChildrenDocument6 pagesTwo Cases of Recurrent ADIH in ChildrenTry Ahmad MirzaPas encore d'évaluation
- Management of Idiopathic Nephrotic Syndrome in ChildhoodDocument14 pagesManagement of Idiopathic Nephrotic Syndrome in ChildhoodpoerbaantonPas encore d'évaluation
- Research Article: Preemptive Treatment of Nausea and Vomiting of Pregnancy: Results of A Randomized Controlled TrialDocument8 pagesResearch Article: Preemptive Treatment of Nausea and Vomiting of Pregnancy: Results of A Randomized Controlled TrialdarianezulPas encore d'évaluation
- Impacto Clínico de La Rehidratación Intravenosa Rápida Con Dextrosa en Niños Con Gastroenteritis AgudaDocument5 pagesImpacto Clínico de La Rehidratación Intravenosa Rápida Con Dextrosa en Niños Con Gastroenteritis AgudaMarina Escobar NievesPas encore d'évaluation
- Strategies For Acute Metabolic DisordersDocument14 pagesStrategies For Acute Metabolic DisordersAhmed AnwarPas encore d'évaluation
- A New Approach To The Prophylaxis of Cyclic Vomiting TopiramateDocument5 pagesA New Approach To The Prophylaxis of Cyclic Vomiting TopiramateVianPas encore d'évaluation
- J Clin Endocrinol Metab. 2012 97 16 38Document23 pagesJ Clin Endocrinol Metab. 2012 97 16 38rizwan234Pas encore d'évaluation
- Prescribing Info for Dostinex TabletsDocument9 pagesPrescribing Info for Dostinex TabletsasdwasdPas encore d'évaluation
- Efficacy of Higher-Dose Levamisole in Maintaining Remission in Steroid-Dependant Nephrotic SyndromeDocument6 pagesEfficacy of Higher-Dose Levamisole in Maintaining Remission in Steroid-Dependant Nephrotic Syndromechandra maslikhaPas encore d'évaluation
- Rebif Europa EnglishDocument223 pagesRebif Europa EnglishMiguel Antonio Armas RivasPas encore d'évaluation
- Use of A LowDocument8 pagesUse of A Lowirma suwandi sadikinPas encore d'évaluation
- Intraperitoneal Vancomycin Concentrations During Peritoneal Dialysis-Associated Peritonitis: Correlation With Serum LevelsDocument23 pagesIntraperitoneal Vancomycin Concentrations During Peritoneal Dialysis-Associated Peritonitis: Correlation With Serum LevelsHera HeraPas encore d'évaluation
- GentDocument2 pagesGentOxford666Pas encore d'évaluation
- Spontaneous Bacterial Peritonitis Organism-Specific Therapy - Specific Organisms and Therapeutic RegimensDocument2 pagesSpontaneous Bacterial Peritonitis Organism-Specific Therapy - Specific Organisms and Therapeutic RegimensDung TranPas encore d'évaluation
- Clinical Data Zeftrax-SDocument37 pagesClinical Data Zeftrax-SSem.Jb Tan0% (1)
- Hypertension in PregnancyDocument15 pagesHypertension in PregnancyLaura María Salamanca Ternera0% (1)
- Ten-Year Single-Center Experience of The Ketogenic Diet: Factors in Uencing Efficacy, Tolerability, and ComplianceDocument8 pagesTen-Year Single-Center Experience of The Ketogenic Diet: Factors in Uencing Efficacy, Tolerability, and ComplianceMarcin CiekalskiPas encore d'évaluation
- The Ceylon Medical Journal: Paracetamol Overdose: Relevance of Recent Evidence For Managing Patients in Sri LankaDocument5 pagesThe Ceylon Medical Journal: Paracetamol Overdose: Relevance of Recent Evidence For Managing Patients in Sri LankaARaniPas encore d'évaluation
- CPG - Use of Corticosteroids in General Practice Dec 2006Document131 pagesCPG - Use of Corticosteroids in General Practice Dec 2006MUHAMMAD HAEKALPas encore d'évaluation
- Vesanoid (Tretinoin) Capsules R Only Warnings 1. Experienced Physician and InstitutionDocument14 pagesVesanoid (Tretinoin) Capsules R Only Warnings 1. Experienced Physician and InstitutionArun GargPas encore d'évaluation
- Nutritional Status Among Peritoneal Dialysis Patients After Oral Supplement With ONCE Dialyze FormulaDocument7 pagesNutritional Status Among Peritoneal Dialysis Patients After Oral Supplement With ONCE Dialyze FormulanuvitaPas encore d'évaluation
- Challenges Diuretics CasebasedDocument13 pagesChallenges Diuretics CasebasedDaniel MelendezPas encore d'évaluation
- RespDocument2 pagesRespNicolaeDincaPas encore d'évaluation
- Pi Is 0025619611601213Document5 pagesPi Is 0025619611601213FarmaIndasurPas encore d'évaluation
- Nephrotic Syndrome in ChildhoodDocument5 pagesNephrotic Syndrome in ChildhoodJessica SilaenPas encore d'évaluation
- Clinical Course of Steroid Sensitive Nephrotic Syndrome in Children: Outcome and OutlookDocument11 pagesClinical Course of Steroid Sensitive Nephrotic Syndrome in Children: Outcome and OutlookIkhbar FalahPas encore d'évaluation
- Nephrotic Syndrome 5th Year Lecture 2011Document7 pagesNephrotic Syndrome 5th Year Lecture 2011Gutierrez MarinellPas encore d'évaluation
- Pancreatitis GuidelineDocument26 pagesPancreatitis GuidelineShalltear BloodfallenPas encore d'évaluation
- Childhood Membranoproliferative Glomerulonephritis Type I: Limited Steroid TherapyDocument7 pagesChildhood Membranoproliferative Glomerulonephritis Type I: Limited Steroid TherapyKiki Celiana TiffanyPas encore d'évaluation
- Urinary Tract Infection PDFDocument9 pagesUrinary Tract Infection PDFTigerEyzPas encore d'évaluation
- Line e Guida Glo Me Rul One FriteDocument143 pagesLine e Guida Glo Me Rul One FriteAnprtma kaunangPas encore d'évaluation
- Nephrotic Syndrome ExplainedDocument30 pagesNephrotic Syndrome ExplainedAlana KuruvillaPas encore d'évaluation
- NCMB316 Rle 2-10-7addison's DiseaseDocument4 pagesNCMB316 Rle 2-10-7addison's DiseaseMaica LectanaPas encore d'évaluation
- Anaesthetic AwarenessDocument21 pagesAnaesthetic AwarenessPeter KamPas encore d'évaluation
- IndianJOphthalmol54168-4547556 123755Document2 pagesIndianJOphthalmol54168-4547556 123755Gusti Ari SetyawanPas encore d'évaluation
- Fatty Hepatosis in DiabetesDocument3 pagesFatty Hepatosis in DiabetesCentral Asian StudiesPas encore d'évaluation
- 06 Insulin InitiationDocument6 pages06 Insulin InitiationamalPas encore d'évaluation
- Antiemetics in ChildrenDocument14 pagesAntiemetics in ChildrenntnquynhproPas encore d'évaluation
- Nephroticsyndrome 171015133308Document52 pagesNephroticsyndrome 171015133308shravaniPas encore d'évaluation
- Complementary and Alternative Medical Lab Testing Part 8: UrologyD'EverandComplementary and Alternative Medical Lab Testing Part 8: UrologyÉvaluation : 3 sur 5 étoiles3/5 (1)
- Top Trials in Gastroenterology & HepatologyD'EverandTop Trials in Gastroenterology & HepatologyÉvaluation : 4.5 sur 5 étoiles4.5/5 (7)
- Naplex Complete Study Outline A Topic-Wise Approach DiabetesD'EverandNaplex Complete Study Outline A Topic-Wise Approach DiabetesÉvaluation : 4 sur 5 étoiles4/5 (2)
- Top Trials in Gastroenterology & Hepatology, 2nd EditionD'EverandTop Trials in Gastroenterology & Hepatology, 2nd EditionPas encore d'évaluation
- Emerging Nanomedicines for Diabetes Mellitus TheranosticsD'EverandEmerging Nanomedicines for Diabetes Mellitus TheranosticsPas encore d'évaluation
- Multidrug-Resistant Tuberculosis (MDR-TB) : 2012 UpdateDocument2 pagesMultidrug-Resistant Tuberculosis (MDR-TB) : 2012 UpdateRobert MontgomeryPas encore d'évaluation
- Northern California Emergency Ultrasound Course ObjectivesDocument16 pagesNorthern California Emergency Ultrasound Course ObjectivesRobert MontgomeryPas encore d'évaluation
- Sio Jurnal Pertemuan 1Document9 pagesSio Jurnal Pertemuan 1raudatul jannahPas encore d'évaluation
- New York Heart Association (NYHA) ClassificationDocument1 pageNew York Heart Association (NYHA) ClassificationBayu PratamaPas encore d'évaluation
- Asphyxia: Forensic Medicine Rs Bhayangkara Porong Fakultas Kedokteran Universitas Muhammadiyah MalangDocument7 pagesAsphyxia: Forensic Medicine Rs Bhayangkara Porong Fakultas Kedokteran Universitas Muhammadiyah MalangRobert MontgomeryPas encore d'évaluation
- Interprofessional Education PDFDocument3 pagesInterprofessional Education PDFRobert MontgomeryPas encore d'évaluation
- Efast1 PDFDocument1 pageEfast1 PDFRobert MontgomeryPas encore d'évaluation
- 0314 ShockDocument24 pages0314 ShockJose HdzPas encore d'évaluation
- QT Interval Variability in Body Surface ECGDocument20 pagesQT Interval Variability in Body Surface ECGRobert MontgomeryPas encore d'évaluation
- Pediatric FractureDocument22 pagesPediatric FractureRobert MontgomeryPas encore d'évaluation
- Guidance Antenatal CareDocument58 pagesGuidance Antenatal CareRobert MontgomeryPas encore d'évaluation
- Sio Jurnal Pertemuan 1Document9 pagesSio Jurnal Pertemuan 1raudatul jannahPas encore d'évaluation
- ArrhythmiasDocument53 pagesArrhythmiasRobert MontgomeryPas encore d'évaluation
- Diabetic Foot Ulcer ReviewDocument7 pagesDiabetic Foot Ulcer Reviewintan_eklePas encore d'évaluation
- 07 - 1-2 - 83-95 (GAAP) (Upadhyaya Et Al, 2007Document14 pages07 - 1-2 - 83-95 (GAAP) (Upadhyaya Et Al, 2007hrishikesh08Pas encore d'évaluation
- Nonallergic Rhinitis, With A Focus On Vasomotor RhinitisDocument6 pagesNonallergic Rhinitis, With A Focus On Vasomotor RhinitisRaga ManduaruPas encore d'évaluation
- 2012 Article 4Document15 pages2012 Article 4Andriawan BramPas encore d'évaluation
- Daftar Pustaka EdiarDocument1 pageDaftar Pustaka EdiarRobert MontgomeryPas encore d'évaluation
- I1544 581X 73 3Document74 pagesI1544 581X 73 3Ajie WitamaPas encore d'évaluation
- EAST PMG Blunt Abdominal 2001Document14 pagesEAST PMG Blunt Abdominal 2001Adolfo Rfael Gomez EspinosaPas encore d'évaluation
- GERD Pathophysiology Cleveland ClinicDocument16 pagesGERD Pathophysiology Cleveland ClinicMonica Lauretta SembiringPas encore d'évaluation
- Daftar Pustaka EdiarDocument1 pageDaftar Pustaka EdiarRobert MontgomeryPas encore d'évaluation
- 10 Ways To Prepare For RamadanDocument21 pages10 Ways To Prepare For RamadanRobert MontgomeryPas encore d'évaluation
- Powell and Renner Article To Analize DataDocument12 pagesPowell and Renner Article To Analize DataJudith AlbarracinPas encore d'évaluation
- AbawiDocument14 pagesAbawiYizhou WuPas encore d'évaluation
- Bis. Research MethodsDocument136 pagesBis. Research Methodsnebiloo1Pas encore d'évaluation
- Declaration of MontrealDocument2 pagesDeclaration of MontrealLjiljana LjiljaPas encore d'évaluation
- Organization Chart and Services of Acworth Municipal HospitalDocument6 pagesOrganization Chart and Services of Acworth Municipal Hospitaltops123Pas encore d'évaluation
- Psychiatric NursingDocument4 pagesPsychiatric NursingMarj MagundayaoPas encore d'évaluation
- Thornwaldt Cyst - A Disease or AnomalyDocument4 pagesThornwaldt Cyst - A Disease or AnomalyresearchparksPas encore d'évaluation
- V. AzapironesDocument2 pagesV. AzapironesChristine Pialan SalimbagatPas encore d'évaluation
- PneumoniaDocument41 pagesPneumoniapaanar100% (2)
- Pg36 37 of Pneumothorax Case StudyDocument2 pagesPg36 37 of Pneumothorax Case StudyCharles Dean Ugalde100% (2)
- YÖKDİL Health Question Types Relative & Noun ClausesDocument6 pagesYÖKDİL Health Question Types Relative & Noun ClausesİrePas encore d'évaluation
- Neuropsychiatric Symptoms of Multiple Sclerosis - State of The ArtDocument12 pagesNeuropsychiatric Symptoms of Multiple Sclerosis - State of The ArtRenato GuedesPas encore d'évaluation
- Mewbook Final Print Version 2014Document177 pagesMewbook Final Print Version 2014Eduardo BarrazaPas encore d'évaluation
- Sofia Mubarika 180522Document42 pagesSofia Mubarika 180522Nanik AndianiPas encore d'évaluation
- Clinical Feature of MiliariaDocument3 pagesClinical Feature of MiliariaPuteri Diah RahtiniPas encore d'évaluation
- Protonix (Pantoprazole)Document1 pageProtonix (Pantoprazole)EPas encore d'évaluation
- AsthmaDocument142 pagesAsthmaAmirah Mohamad Saidi100% (1)
- الجرب 14مستند بلا عنوانDocument8 pagesالجرب 14مستند بلا عنوانKhadijah HassanPas encore d'évaluation
- Merged PDF 2021 11 16T12 - 01 - 01Document15 pagesMerged PDF 2021 11 16T12 - 01 - 01Ericsson CarabbacanPas encore d'évaluation
- AV CPG 2016 Ed 1.1Document377 pagesAV CPG 2016 Ed 1.1Fatality FatalityPas encore d'évaluation
- Investigative DHHS Report - Horizon Health and RehabDocument29 pagesInvestigative DHHS Report - Horizon Health and RehabLas Vegas Review-JournalPas encore d'évaluation
- Of Diagnosa ICD X SelectedDocument512 pagesOf Diagnosa ICD X Selectedadhisam22_913576642Pas encore d'évaluation
- Mice Rats in Biomedical Research FBRDocument2 pagesMice Rats in Biomedical Research FBRChikondi TemboPas encore d'évaluation
- (2365242X - Pharmaceutical Technology in Hospital Pharmacy) Avoid Drug Incompatibilities Clinical Context in Neonatal Intensive Care Unit (NICU)Document8 pages(2365242X - Pharmaceutical Technology in Hospital Pharmacy) Avoid Drug Incompatibilities Clinical Context in Neonatal Intensive Care Unit (NICU)JoaoPas encore d'évaluation
- Anesthesia For Patients With Mediastinal MassesDocument10 pagesAnesthesia For Patients With Mediastinal MassesFityan Aulia RahmanPas encore d'évaluation
- Minimally Invasive Aortic Valve ReplacementDocument11 pagesMinimally Invasive Aortic Valve ReplacementDm LdPas encore d'évaluation
- Diabetic Coma in Type 2 DiabetesDocument4 pagesDiabetic Coma in Type 2 DiabetesGilda Ditya AsmaraPas encore d'évaluation
- Neuralink PRIME Study BrochureDocument2 pagesNeuralink PRIME Study BrochureSimon AlvarezPas encore d'évaluation
- Advances in Diagnostic Aids / Orthodontic Courses by Indian Dental AcademyDocument25 pagesAdvances in Diagnostic Aids / Orthodontic Courses by Indian Dental Academyindian dental academyPas encore d'évaluation
- Progessence Phyto Plus: Essential Oil BlendDocument2 pagesProgessence Phyto Plus: Essential Oil BlendJesh GranadoPas encore d'évaluation
- Clinical Assessment and Diagnosis of Hypovolemia (Dehydration) in Children - UpToDateDocument12 pagesClinical Assessment and Diagnosis of Hypovolemia (Dehydration) in Children - UpToDateNedelcu MirunaPas encore d'évaluation
- Textbook of Medical Parasitology Protozoology HelmDocument2 pagesTextbook of Medical Parasitology Protozoology HelmAnge OuedraogoPas encore d'évaluation
- Robotics in Medical ScienceDocument45 pagesRobotics in Medical SciencePushkar Singh100% (2)
- The Adult Chain of Survival Module1Document1 pageThe Adult Chain of Survival Module1Mariam E.Pas encore d'évaluation