Académique Documents
Professionnel Documents
Culture Documents
Horner SYndrome
Transféré par
Hendri Wijaya Wang0 évaluation0% ont trouvé ce document utile (0 vote)
92 vues3 pagesHorner's syndrome is caused by a lesion along the sympathetic pathway that controls the iris and sweat glands. This pathway runs from the brainstem and spinal cord through the neck. Lesions can be central in the brain/spinal cord, preganglionic in the neck, or postganglionic in the eye area. Signs include ptosis, miosis, anisocoria that worsens in dim light, and reduced sweating on the affected side of the face. The location of the lesion determines whether sweating is affected. Central lesions may be due to brainstem issues while preganglionic can arise from lung tumors or neck injuries. Testing distinguishes between lesion locations and rules out other causes of
Description originale:
aaaaaaaaaa mataaaa
Copyright
© © All Rights Reserved
Formats disponibles
DOCX, PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentHorner's syndrome is caused by a lesion along the sympathetic pathway that controls the iris and sweat glands. This pathway runs from the brainstem and spinal cord through the neck. Lesions can be central in the brain/spinal cord, preganglionic in the neck, or postganglionic in the eye area. Signs include ptosis, miosis, anisocoria that worsens in dim light, and reduced sweating on the affected side of the face. The location of the lesion determines whether sweating is affected. Central lesions may be due to brainstem issues while preganglionic can arise from lung tumors or neck injuries. Testing distinguishes between lesion locations and rules out other causes of
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
92 vues3 pagesHorner SYndrome
Transféré par
Hendri Wijaya WangHorner's syndrome is caused by a lesion along the sympathetic pathway that controls the iris and sweat glands. This pathway runs from the brainstem and spinal cord through the neck. Lesions can be central in the brain/spinal cord, preganglionic in the neck, or postganglionic in the eye area. Signs include ptosis, miosis, anisocoria that worsens in dim light, and reduced sweating on the affected side of the face. The location of the lesion determines whether sweating is affected. Central lesions may be due to brainstem issues while preganglionic can arise from lung tumors or neck injuries. Testing distinguishes between lesion locations and rules out other causes of
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 3
Right preganglionic Horner syndrome
Central (first-order neurone)
brain stem disease (tumours. vascular. demyelination)
syringomyelia
lateral medullary (Wallenberg) syndrome
spinal cord tumours
1. Preganglionic (second-order neurone)
Pancoast tumour
carotid and aortic aneurysms and dissection
neck lesions (glands. trauma. postsurgical)
J. Postganglionic (third~order neurone)
duster headaches (migrainous neuralgia)
internal carotid artery dissection
nasopharyngeal tumours
otitis media
cavernous sinus mass
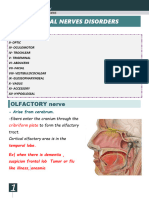
Mild ptosis (usually 1-2 mm) as a result of weakness of
Miillermuscle (Fig. 18.67).
Slight elevation of the inferior eyelid as a result of weakness of the inferior
tarsal muscle.
Miosis resnlting from the unopposed acUon of the
sphincter pupillae. with resultant anisocoria which is
accentnated in dim light. since the Horner pupil will not
dUate. like its fellow.
i\ormal reactions to light and near
Reduced ipsilateral sweating, but only if thc lesion is
below the superior cervical ganglion because the fibres
~upplying the skin of the face run along the cxternal
carotid artery.
Hypochromic heterochromia (irides of different colourHorner is lighter) may
be seen if the lesion is congenital or
long-standing.
The pupil is slow to dilate.
Less important signs include hyperactive accommodation.
ocular hypotony and conjunctival hyperaemia
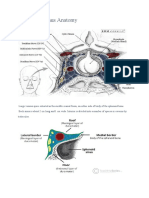
Horner's syndrome is caused by a lesion of the sympathetic pathway either (1) in
its central portion, which extends from the posterior hypothalamus through the
brainstem to the upper spinal cord (C8T2); or (2) in its preganglionic portion,
which exits the spinal cord and synapses in the superior cervical (stellate)
ganglion; or (3) in its postganglionic portion, from the superior cervical ganglion
via the carotid plexus and the ophthalmic division of the trigeminal nerve, by
which it enters the orbit. The sympathetic fibers then follow the nasociliary branch
of the ophthalmic division of the trigeminal nerve and the long ciliary nerves to
the iris and innervate Mller's muscle and the iris dilator. Iris dilator muscle
paresis causes miosis, which is more evident in dim light. Melanocyte maturation
in the iris of a neonate depends on sympathetic innervation; thus, less pigmented
(bluer) irides occur if a congenital sympathetic lesion is present. Paresis of
Mller's muscle produces ptosis. Unilateral miosis, ptosis, and absence of
sweating on the ipsilateral face and neck make up the complete syndrome.
Sweating on the face is normal in postganglionic lesions because postganglionic
fibers to the face for sweating follow the external rather than the internal carotid
artery.
Central Horner's syndrome may be due to brainstem infarction, particularly lateral
medullary infarction (Wallenberg's syndrome), syringomyelia, or cervical cord
tumor. Preganglionic Horner's syndrome may be due to cervical rib, cervical
vertebral fractures, apical pulmonary lesionsparticularly bronchogenic
carcinoma (Pancoast's syndrome)or brachial plexus injuries. Postganglionic
Horner's syndrome may be due to carotid artery dissection, skull base tumors, or
cluster headache. The localization of central and preganglionic Horner's syndrome
is often apparent from the associated clinical features. Sudden-onset isolated
painful Horner's syndrome, particularly with a recent history of neck trauma or
associated with pain in the neck or jaw, necessitates urgent investigation for
carotid dissection, which may lead to thrombotic or embolic stroke. Horner's
syndrome associated with chronic facial pain, particularly if associated with fifth,
sixth, third, fourth, or second cranial nerve palsy, requires investigation for skullbase tumor.
Pharmacologic testing with topical cocaine in the conjunctival sac differentiates
Horner's syndrome, in which the pupil does not dilate, from physiologic
anisocoria. Topical apraclonidine, which causes dilation of the affected but not the
normal pupil, can also be used. Testing with hydroxyamphetamine drops
differentiates central and preganglionic from postganglionic lesions, but they are
difficult to obtain.
Figure 24.15. Appearance of Horner syndrome in four patients. A, Congenital
right Horner syndrome. Note associated heterochromia iridis and minimal ptosis.
B, Left Horner syndrome after neck trauma. C, Left Horner syndrome associated
with apical lung (Pancoast) tumor. D, Left Horner syndrome in a patient with
Raeder's paratrigeminal neuralgia.
Vous aimerez peut-être aussi
- Right Preganglionic Horner Syndrome Dfagmn Akjdg Amg 'Lakg'lakg'lakg'alkg'akg'ag'akg Akg A Kgakg'agkaDocument5 pagesRight Preganglionic Horner Syndrome Dfagmn Akjdg Amg 'Lakg'lakg'lakg'alkg'akg'ag'akg Akg A Kgakg'agkaHendri Wijaya WangPas encore d'évaluation
- Slide MusculoDocument19 pagesSlide MusculoStefan CandraPas encore d'évaluation
- Sindrom HornerDocument15 pagesSindrom HornervivinPas encore d'évaluation
- Horner Syndrome - StatPearls - NCBI BookshelfDocument9 pagesHorner Syndrome - StatPearls - NCBI BookshelfShweh Fern LooPas encore d'évaluation
- 28-Cranial Nerves and MusclesDocument26 pages28-Cranial Nerves and Musclesrodrigocorcino899959Pas encore d'évaluation
- FACIAL NERVE ParalysisDocument35 pagesFACIAL NERVE ParalysisIgnasPas encore d'évaluation
- Mandatory at First Presentation With: Meningitis, in An Obviously IllDocument13 pagesMandatory at First Presentation With: Meningitis, in An Obviously IllkughaprianPas encore d'évaluation
- Mrcs NeurosurgeryDocument28 pagesMrcs NeurosurgeryAdebisiPas encore d'évaluation
- HornerDocument7 pagesHornerpriyaPas encore d'évaluation
- CN DisordersDocument15 pagesCN DisordersMogtaba M HilalPas encore d'évaluation
- Horner's Syndrome FinalDocument11 pagesHorner's Syndrome Finalpriya0% (1)
- 3RD CN - SeminarDocument49 pages3RD CN - Seminarabhishek tPas encore d'évaluation
- Horner's SyndromeDocument7 pagesHorner's SyndromeNastiti WidyariniPas encore d'évaluation
- Acoustic NeuromaDocument31 pagesAcoustic NeuromaHreem FarrakhPas encore d'évaluation
- Draw It To Know It NotesDocument13 pagesDraw It To Know It Noteskat9210Pas encore d'évaluation
- Neurological Disturbances of FaceDocument33 pagesNeurological Disturbances of FaceDrMuskan AroraPas encore d'évaluation
- Brainstem II: Eye Movements and Pupillary ControlDocument34 pagesBrainstem II: Eye Movements and Pupillary ControlhemendrePas encore d'évaluation
- Brain TumorsDocument54 pagesBrain Tumorssrushtideokar0537Pas encore d'évaluation
- Trigeminal NerveDocument11 pagesTrigeminal NerveluckyPas encore d'évaluation
- Collection Tricks: Ramsay-Hunt SyndromeDocument7 pagesCollection Tricks: Ramsay-Hunt SyndromeMarc GriffinPas encore d'évaluation
- Articulo PDFDocument6 pagesArticulo PDFLuisa Vanessa CueroPas encore d'évaluation
- The Pupil and It's Abnormalities: Presented By: Dr. Gloria George Moderator: Dr. Ajay KamathDocument25 pagesThe Pupil and It's Abnormalities: Presented By: Dr. Gloria George Moderator: Dr. Ajay KamathNinaPas encore d'évaluation
- 2 OverviewIII Iaat12i5p621Document4 pages2 OverviewIII Iaat12i5p621FadhilAfifPas encore d'évaluation
- Horner Syndrome: by Shubham GargDocument11 pagesHorner Syndrome: by Shubham GargShubham GargPas encore d'évaluation
- Neuro-Ophthalmology: DR Jusuf Wijaya, SPM FK - Uki CawangDocument65 pagesNeuro-Ophthalmology: DR Jusuf Wijaya, SPM FK - Uki CawanggeorgyPas encore d'évaluation
- 2 5307975357561833113Document8 pages2 5307975357561833113sherani999Pas encore d'évaluation
- Neurology ReviewDocument42 pagesNeurology ReviewShahnaaz Shah50% (2)
- Gangguan Saraf KranialDocument30 pagesGangguan Saraf KranialWisnu Surya WardhanaPas encore d'évaluation
- Spinal CordDocument15 pagesSpinal Cordsimi y100% (1)
- Orbital Fractures:: Orbit Applied AspectsDocument4 pagesOrbital Fractures:: Orbit Applied AspectsTaimoor QadeerPas encore d'évaluation
- Cavernous Sinus SyndromeDocument8 pagesCavernous Sinus SyndromeMuresan Ioana Catalina100% (1)
- Lecture Head & Neck Anatomy RTMDocument75 pagesLecture Head & Neck Anatomy RTMbadhon48Pas encore d'évaluation
- 8-Complications of Suppurative Otitis MediaDocument2 pages8-Complications of Suppurative Otitis MediaAnmarPas encore d'évaluation
- Head and Spinal Cord Injury (Ci)Document111 pagesHead and Spinal Cord Injury (Ci)azmerawPas encore d'évaluation
- Spinal cord lesion (Transverse myelitis) د.رشاد عبدالغنيDocument33 pagesSpinal cord lesion (Transverse myelitis) د.رشاد عبدالغنيMohammad BelbahaithPas encore d'évaluation
- Neuro SBA3Document3 pagesNeuro SBA3Mehdi Hasan MazumderPas encore d'évaluation
- 19 Spinal CordDocument8 pages19 Spinal Cordkarar AhmedPas encore d'évaluation
- Facial PalsyDocument33 pagesFacial PalsyArista SPas encore d'évaluation
- Bells PalsyDocument66 pagesBells PalsyanshikaPas encore d'évaluation
- Head InjuryDocument30 pagesHead InjuryAngel MakinPas encore d'évaluation
- Cavernous Sinus AnatomyDocument8 pagesCavernous Sinus AnatomyPrashant TiwariPas encore d'évaluation
- Ptosis and Lid RetractionDocument40 pagesPtosis and Lid Retractionsarath chandranPas encore d'évaluation
- CNS Congenital AnomaliesDocument74 pagesCNS Congenital AnomaliesMoh DrhusseinyPas encore d'évaluation
- Brain TumorsDocument24 pagesBrain TumorsStevina TanuwijayaPas encore d'évaluation
- Clinical Approach To Brainstem LesionsDocument10 pagesClinical Approach To Brainstem LesionsJosé SánchezPas encore d'évaluation
- Head InjuryDocument6 pagesHead InjuryHurrinazilla AwaliaPas encore d'évaluation
- Central Vertigo PDFDocument6 pagesCentral Vertigo PDFarliniePas encore d'évaluation
- Surgery of PeripheralDocument31 pagesSurgery of PeripheralMircea JunbeiPas encore d'évaluation
- Horner, S Syndrome &Document39 pagesHorner, S Syndrome &Shahzada KhanPas encore d'évaluation
- Facial Nerve ParalysisDocument66 pagesFacial Nerve ParalysisELIA RICHARDPas encore d'évaluation
- Spinal Cord Chest Sympathetic Nervous System AutonomicDocument1 pageSpinal Cord Chest Sympathetic Nervous System AutonomicPutzz AriPas encore d'évaluation
- ParaplegiaDocument56 pagesParaplegiarashid38Pas encore d'évaluation
- Clinical Notes of Cranial NervesDocument6 pagesClinical Notes of Cranial Nerveseducation HubPas encore d'évaluation
- Spinal Cord Injury and CompressionDocument10 pagesSpinal Cord Injury and CompressionAdeputhPas encore d'évaluation
- UWorld Notes NeurologyDocument6 pagesUWorld Notes NeurologysarahPas encore d'évaluation
- Seminar: Facial Nerve PalsyDocument166 pagesSeminar: Facial Nerve PalsyShouvik ChowdhuryPas encore d'évaluation
- Horner Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsD'EverandHorner Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsPas encore d'évaluation
- Intralipid infusion for Myelin Sheath Repair in Multiple Sclerosis and Trigeminal Neuralgia?D'EverandIntralipid infusion for Myelin Sheath Repair in Multiple Sclerosis and Trigeminal Neuralgia?Pas encore d'évaluation
- Neuromodulation in Headache and Facial Pain Management: Principles, Rationale and Clinical DataD'EverandNeuromodulation in Headache and Facial Pain Management: Principles, Rationale and Clinical DataGiorgio LambruPas encore d'évaluation
- Neurology Equations Made Simple: Differential Diagnosis and NeuroemergenciesD'EverandNeurology Equations Made Simple: Differential Diagnosis and NeuroemergenciesPas encore d'évaluation
- Daftar Pustaka LPR - Hendri WijayaDocument2 pagesDaftar Pustaka LPR - Hendri WijayaHendri Wijaya WangPas encore d'évaluation
- Chastre J, Fagon JY. Ventilator-Associated Pneumonia. Am J Respir Crit Care Med 2002 165:867-903Document2 pagesChastre J, Fagon JY. Ventilator-Associated Pneumonia. Am J Respir Crit Care Med 2002 165:867-903Hendri Wijaya WangPas encore d'évaluation
- Daffdaadfgddhgf 222 Ahdfj KLJLHLDocument2 pagesDaffdaadfgddhgf 222 Ahdfj KLJLHLHendri Wijaya WangPas encore d'évaluation
- Ssssssssssssssssssssssssssssssssssssss Fafdfghklj Kjhgfddafafafaga Qjwfhqwoghqwoghoqw HgoqwDocument2 pagesSsssssssssssssssssssssssssssssssssssss Fafdfghklj Kjhgfddafafafaga Qjwfhqwoghqwoghoqw HgoqwHendri Wijaya WangPas encore d'évaluation
- Milestone Umur (BLN) Developmental ImplicationsDocument2 pagesMilestone Umur (BLN) Developmental ImplicationsHendri Wijaya WangPas encore d'évaluation
- Batu Ginjal (Kidney Stone)Document11 pagesBatu Ginjal (Kidney Stone)Qorry AmandaPas encore d'évaluation
- Polar Bear (Report Text)Document14 pagesPolar Bear (Report Text)Adeb Wahyu100% (1)
- The Vitamin C Treatment of Whooping CoughDocument14 pagesThe Vitamin C Treatment of Whooping CoughoneclickgroupPas encore d'évaluation
- Prepared by D.sirag Al-Hamadi Tripoli University Dental FacultyDocument59 pagesPrepared by D.sirag Al-Hamadi Tripoli University Dental Facultypepe_074Pas encore d'évaluation
- Gibberish WordsDocument4 pagesGibberish WordsDaniel PopaPas encore d'évaluation
- SDOFM Viscerosomatic Reflex Pocket ChartDocument2 pagesSDOFM Viscerosomatic Reflex Pocket ChartRohit NalamasuPas encore d'évaluation
- All Questions PhysiologyDocument25 pagesAll Questions Physiologyfilchibuff100% (6)
- CN 9-12Document6 pagesCN 9-12The Real UploaderPas encore d'évaluation
- Modic Type 1 Vs Tuberculous SpondylitisDocument5 pagesModic Type 1 Vs Tuberculous SpondylitisAgnes JauwPas encore d'évaluation
- Case Study About Cervical CancerDocument11 pagesCase Study About Cervical CancerJisel-Apple Bulan100% (1)
- Interpretasi Foto DadaDocument137 pagesInterpretasi Foto DadaRofi Irman100% (1)
- MUST To KNOW in HematologyDocument40 pagesMUST To KNOW in HematologyPatricia Yutuc90% (10)
- Anatomical LandmarksDocument32 pagesAnatomical Landmarksdrhari_omrdPas encore d'évaluation
- Biology Project PDFDocument18 pagesBiology Project PDFSuyash Baghel86% (7)
- Shampoo Condition and Treat The Hair and Scalp: Unit Gh8Document31 pagesShampoo Condition and Treat The Hair and Scalp: Unit Gh8Em JayPas encore d'évaluation
- TerminologiesDocument65 pagesTerminologiesErika Mae PascuaPas encore d'évaluation
- Phobia ListsDocument5 pagesPhobia Listskatts4uPas encore d'évaluation
- LFS 001 Module 1 PPT 2016-17 - 2Document23 pagesLFS 001 Module 1 PPT 2016-17 - 2Hussain AliPas encore d'évaluation
- Animales en La Cultura YorubaDocument9 pagesAnimales en La Cultura Yorubaaganju999Pas encore d'évaluation
- The Ordog Effect DeadworldDocument59 pagesThe Ordog Effect DeadworldJw SqPas encore d'évaluation
- Possession 'SDocument2 pagesPossession 'SazlinPas encore d'évaluation
- Nephrolithiasis - NCPDocument9 pagesNephrolithiasis - NCPAia Javier83% (6)
- Hi-Yield Notes in Im & PediaDocument20 pagesHi-Yield Notes in Im & PediaJohn Christopher LucesPas encore d'évaluation
- L1 - BB LecDocument11 pagesL1 - BB LecJUDEA WILCH ORJEPas encore d'évaluation
- Pregnancy 1Document70 pagesPregnancy 1Annapurna DangetiPas encore d'évaluation
- PoultryDocument2 pagesPoultryDineshkumar NdkPas encore d'évaluation
- Nervous System Endocrine System and Reproductive SystemDocument5 pagesNervous System Endocrine System and Reproductive SystemMcdaryl Inmenzo Lleno50% (2)
- Oh No, It's A Big Fat Bitch SpayDocument8 pagesOh No, It's A Big Fat Bitch SpayWilliam Chandler100% (1)
- Animal AbuseDocument21 pagesAnimal AbuseLiza BDPas encore d'évaluation
- Formation of Faeces and DefecationDocument11 pagesFormation of Faeces and Defecationbiologi88Pas encore d'évaluation