Académique Documents
Professionnel Documents
Culture Documents
Associations Between Practice-Reported Medical Homeness and Health Care Utilization Among Publicly Insured Children
Transféré par
Anonymous ceYk4p4Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Associations Between Practice-Reported Medical Homeness and Health Care Utilization Among Publicly Insured Children
Transféré par
Anonymous ceYk4p4Droits d'auteur :
Formats disponibles
Associations Between Practice-Reported Medical
Homeness and Health Care Utilization Among
Publicly Insured Children
Anna L. Christensen, PhD; Joseph S. Zickafoose, MD, MS; Brenda Natzke, MPP;
Stacey McMorrow, PhD; Henry T. Ireys, PhD
From the Mathematica Policy Research, Washington, DC (Dr Christensen, Ms Natzke, and Dr Ireys); Mathematica Policy Research, Ann
Arbor, Mich (Dr Zickafoose); and The Urban Institute, Washington, DC (Dr McMorrow)
The authors declare that they have no conflict of interest.
Address correspondence to Anna L. Christensen, PhD, Mathematica Policy Research, 1100 1st St NE, 12th Floor, Washington, DC 20002
(e-mail: achristensen@mathematica-mpr.com).
Received for publication June 12, 2014; accepted December 8, 2014.
ABSTRACT
BACKGROUND: The patient-centered medical home (PCMH)
is widely promoted as a model to improve the quality of
primary care and lead to more efficient use of health care
services. Few studies have examined the relationship between
PCMH implementation at the practice level and health care utilization by children. Existing studies show mixed results.
METHODS: Using practice-reported PCMH assessments and
Medicaid claims from child-serving practices in 3 states participating in the Childrens Health Insurance Program Reauthorization Act of 2009 Quality Demonstration Grant Program, this
study estimates the association between medical homeness (tertiles) and receipt of well-child care and nonurgent, preventable,
or avoidable emergency department (ED) use. Multilevel logistic regression models are estimated on data from 32 practices in
Illinois (IL) completing the National Committee for Quality Assurances (NCQA) medical home self-assessment and 32 practices in North Carolina (NC) and South Carolina (SC)
completing the Medical Home Index (MHI) or Medical Home
IndexRevised Short Form (MHI-RSF).
RESULTS: Medical homeness was not associated with receipt of
age-appropriate well-child visits in either sample. Associations be-
tween nonurgent, preventable, or avoidable ED visits and medical
homeness varied. No association was seen among practices in NC
and SC that completed the MHI/MHI-RSF. Children in practices
in IL with the highest tertile NCQA self-assessment scores were
less likely to have a nonurgent, preventable, or avoidable ED visit
than children in practices with low (odds ratio 0.65; 95% confidence
interval 0.470.92; P <.05) and marginally less likely to have such a
visit compared with children in practices with medium tertile scores
(odds ratio 0.72, 95% confidence interval 0.521.01; P .06).
CONCLUSIONS: Higher levels of medical homeness may be
associated with lower nonurgent, preventable, or avoidable
ED use by publicly insured children. Robust longitudinal
studies using multiple measures of medical homeness are
needed to confirm this observation.
KEYWORDS: child health services; health care quality, access,
and evaluation; medical home; patient-centered care; primary
health care
ACADEMIC PEDIATRICS 2015;15:267274
WHATS NEW
Committee for Quality Assurances (NCQA) PCMH recognition program4 and the Medical Home Index (MHI), often
used for internal quality improvement and practice transformation.5 However, little research has examined the relationship between PCMH implementation, as reflected in
these practice-level PCMH measures, and childrens use
of health services. Studies that examine parent-reported
medical homeness and health care utilization are more
common and are often based on data from a few large national surveys.6 These studies have had mixed findings. In
the general pediatric population, parent-reported care in a
medical home has been associated with increased receipt
of well-child care,79 decreased emergency department
(ED) use,7,8 and no differences in hospitalizations.8 In children with chronic conditions, parent-reported care in a
medical home has been associated with no differences in
receipt of preventive care,10,11 mixed results for ED
visits,10,12,13 and no differences in hospitalizations.10
Children in practices with high medical homeness were
less likely to have a nonurgent, preventable, or avoidable emergency department visit than those with low
or medium medical homeness, but only among practices in Illinois scored using the NCQA selfassessment, not among a second sample.
THE PATIENT-CENTERED MEDICAL home (PCMH) is
widely promoted as a model to improve quality of primary
care and lead to more efficient use of health care services.1
3
Programs promoting PCMH adoption typically measure
fidelity to the model, or medical homeness, through
primary care practices responses to inventories of
practice infrastructure and care processes.
In pediatric primary care, some of the most commonly
used practice-level PCMH measures include the National
ACADEMIC PEDIATRICS
Copyright 2015 by Academic Pediatric Association
267
Volume 15, Number 3
MayJune 2015
268
CHRISTENSEN ET AL
Two published studies that have examined the relationship between practice-reported PCMH measures and
health care utilization by children also show mixed results.
In a study of children with chronic conditions in 43 primary
care practices in multiple states, Cooley et al14 found that
children were less likely to be hospitalized if their primary
care practice scored higher on the MHI, but there was no
reduction in ED use, a key target of many PCMH efforts.5
In a study of 296 primary care practices in Michigan, Paustian et al15 found that children were more likely to receive
preventive services but had no differences in overall costs
when receiving care in practices that scored higher on an
insurer-specific practice-level PCMH measure.
The aim of the present analysis was to assess the relationship between practice-reported medical homeness
and health service use by children enrolled in Medicaid
in 3 states. We hypothesized that children would be more
likely to attend preventive care visits and less likely to
use the ED for nonurgent, potentially avoidable, and primary caretreatable conditions when receiving care in primary care practices with higher levels of medical
homeness. A secondary aim was to assess whether the association between medical homeness and health care use
differed for children with chronic conditions and disabilities versus all other children. Given the widespread promotion and implementation of the PCMH model, more
information is needed to understand the association between practice-level measures of the PCMH and health
care utilization for children in a variety of populations.
This analysis helps fill the gap in the current literature.
METHODS
DATA
We performed a cross-sectional analysis assessing the
relationship between practice-reported medical homeness
and health service use by children enrolled in Medicaid
in 64 practices in 3 states participating in the Childrens
Health Insurance Program Reauthorization Act (CHIPRA)
Quality Demonstration Grant Program: Illinois (IL), North
Carolina (NC), and South Carolina (SC).16 The 2009 CHIPRA legislation authorized $100 million in grants to states
to test various approaches to improve the quality of health
care for children in the United States, particularly publicly
insured children. As part of this effort, several states pursued projects to promote the implementation of the
PCMH model in primary care practices serving children.
The 3 states in this analysis have varied histories with primary care transformation and represent different state
Medicaid contexts, including managed care penetration.
Intervention practices in all 3 states volunteered to participate with the aim of primary care practice transformation.
NC and SC also recruited comparison practices. This analysis uses baseline data that were collected for the national
evaluation of the program, funded by the Agency for
Healthcare Research and Quality (AHRQ).16
Medical homeness was assessed via standardized
practice-reported surveys. Each state selected the medical
home assessment that was most appropriate for its demon-
ACADEMIC PEDIATRICS
stration project.17 NCs practices completed the MHI, and
SCs completed the Medical Home IndexRevised Short
Form (MHI-RSF).5,17 We have shown that the MHI and
MHI-RSF rank practices similarly17; consequently, we
combined data from NC and SC. NC practices were surveyed in mid- to late 2011, at the beginning of the intervention. SC practices were surveyed in early 2012, more than 1
year after the intervention began. Practices in IL completed
the NCQA 2011 medical home self-assessment in late
2011 to early 2012, less than a year before the intervention
began.4 The self-assessment does not require practices to
submit documentation to NCQA.
Patient characteristics and health care utilization were
assessed via Medicaid enrollment and claims data from
the calendar year before medical home assessment: 2010
in NC and IL, and 2011 in SC. Because the SC PCMH
intervention began in 2011, we were concerned that the
MHI-RSF score collected in early 2012 would not reflect
the level of medical homeness corresponding to utilization.
Thus, we exclude the SC intervention practices and include
only the comparison practices in this baseline analysis. Utilization data included fee for service (FFS) or primary care
case management (PCCM) claims only and excluded traditional managed care encounters. Depending on the state,
managed care encounters were not available to researchers
or could not be linked to practices participating in the
demonstration due to the variation in provider identification variables across managed care organizations.
The New England institutional review board deemed
this phase of the evaluation as exempt from review because
it used existing administrative data and practice-level data
(45 CFR 46.101(b)(4)).
STUDY POPULATION
The study population included children aged 0 to 18
years continuously enrolled for 12 months (with no more
than a 1-month gap in coverage) in FFS or PCCM
Medicaid who were attributed to primary care practices
enrolled in the demonstration in the 3 states. Children
were excluded if they received partial Medicaid benefits;
received benefits through a Medicaid waiver program;
had any other source of insurance coverage; or were institutionalized. Children were attributed to a primary care
practice using a staged, claims-based approach. First, children were attributed to the practice where they received the
majority of their well-child visits (WCV) in the calendar
year (of children who could be attributed, 72% of children
in IL, 67% of children in NC, and 43% of children in SC
were attributed in this stage). Children without a WCV
were attributed to the practice where they received the majority of their other ambulatory care visits (24% of children
in IL, 30% of children in NC, and 50% of children in SC
were attributed in this stage). In the remaining cases where
there was no majority practice for WCV or other ambulatory visits (4% of children in IL, 3% of children in NC,
and 7% of children in SC), children were attributed to
the practice they attended most recently.
Practices participating in the demonstration were identified by billing and/or service provider identification
ACADEMIC PEDIATRICS
numbers supplied by the states. There is no variable to link
children to their primary care provider other than the billing
provider on a claim, so children without any WCVor ambulatory claims could not be attributed to a primary care
practice and were excluded from this analysis. Further information on our attribution algorithm may be obtained
upon request. Practices with fewer than 30 Medicaid
children attributed to them were excluded from the analysis
(6 practices in IL; no practices in NC or SC) to ensure a
sufficient sample size to estimate within-practice variation.
MEASURES
Medical homeness was measured using the MHI/MHIRSF or the NCQA self-assessment. We used the NCQA
self-assessment total score rather than recognition level
because we were interested in the overall relationship between medical homeness and service use and because no
practices were NCQA certified. Scores for all tools range
from 0 to 100; practices were categorized into tertiles, representing low, medium, and high levels of medical homeness. Tertile cutoffs were set separately for practices
completing the MHI/MHI-RSF (NC, SC) and the NCQA
2011 self-assessment (IL).
We generated 2 measures of health care utilization:
receipt of the age-appropriate number of WCV, and use
of ED services for nonurgent, potentially avoidable, or primary caretreatable conditions. The WCV outcome is a binary measure of whether the child received at least 75% of
the recommended number of WCV for their age during the
measurement year, based on Bright Futures, the American
Academy of Pediatrics guideline and generally recognized
standard for preventive care of children.18 For children under 36 months of age, the number of recommended visits
was determined for their age in months. All children 36
months and older are recommended to have one WCV
per year. We identified WCV using procedure codes from
the Centers for Medicare and Medicaid Services Core Set
of Childrens Health Care Quality Measures.19
The ED use outcome is a binary measure of whether the
child had any nonurgent, primary caretreatable, or potentially avoidable ED visits in the measurement year. These
are ED visits that could hypothetically be reduced or
avoided when children receive continuous and appropriate
care in a medical home. The measure uses ED procedure
and diagnosis codes aligned with the Centers for Medicare
and Medicaid Services Core Set of Childrens Health Care
Quality Measures.19 We then categorized ED visits using a
modified version of the NYU algorithm, a claims-based
method for classifying the severity of ED visits based on
ICD-9 diagnosis codes.2022 In the present study, visits
were considered to be nonurgent, primary caretreatable,
or potentially avoidable if 1) the NYU algorithm
classified them as having a 0.75 or higher probability of
being nonemergent plus emergent but primary care
treatable plus emergent but preventable or avoidable, or
2) if they contain a diagnosis code consistent with a
pediatric-specific nonurgent ED visit, as identified by an
expert panel in a prior study.23 We refer to this group
PRACTICE-REPORTED MEDICAL HOMENESS
269
of visits as nonurgent, preventable, or avoidable ED visits.
We elected not to assess primary caresensitive hospitalizations because they were rare in this sample (0.4% prevalence), with limited variation across practices.
Covariates included in the multivariate analyses come
from the Medicaid enrollment files in all states (child age,
race/ethnicity) and a practice-level survey in NC/SC (practice geography and number of providers, including physicians, nurse practitioners, and physician assistants), which
was not available for practices in IL. Additionally, children
were classified as having a chronic condition or disability
if the claims-based Pediatric Medical Complexity Algorithm
identified them has having a complex chronic condition or a
noncomplex chronic condition,24 or if their Medicaid eligibility category indicated they are disabled. We refer to the remaining group as healthy children.
ANALYSES
We examined the number and characteristics of children
attributed to practices in each state overall and by medical
homeness level. We also summarized practice-level characteristics. To measure the association between medical
homeness and childrens health care utilization, we estimated multilevel logistic regression models using SAS/
STAT software, version 9.3, PROC GLIMMIX (SAS Institute, Cary, NC). The models account for clustering of childrens outcomes within practices. Separate models were
estimated for practices using the MHI/MHI-RSF in NC/
SC and those using the NCQA 2011 self-assessment in
IL. Adjusted models include covariates that are thought
to be associated with medical home level and health care
utilization, based on theory or prior literature. All models
control for child age, race/ethnicity, and chronic conditions/disability status. For NC/SC analyses, where
practice-level characteristics were available, models also
control for number of providers in the practice and practice
geography (urban/suburban, rural). We also include a
dummy variable for state.
To assess whether associations between medical homeness and service use differ for children with and without
chronic conditions or disabilities (ie, effect modification),
we tested stratified models and models with an interaction
term between medical homeness and health status.
Additionally, for sensitivity testing of the medical home
variable, we estimated the final models for each sample using the continuous medical home score, as well as with categorical cutoffs at the 25th and 75th percentile (rather than
33rd and 66th percentile) for medical home level; these
models resulted in similar inferences as the final models
presented in the results section.
RESULTS
The IL sample included 33,895 publicly insured children
attributed to 32 practices (Table 1). The NC/SC sample
included 57,553 children in 32 practices, primarily in
NC. In both samples, the number of children in FFS or
PCCM Medicaid per practice ranged widely, from 34 to
over 10,700. Over half of the children in both samples
CHRISTENSEN ET AL
270
ACADEMIC PEDIATRICS
Table 1. Sample Selection, Sample Size, and Attribution of Children to Practices
State
No. of Children
(018 y)
in Medicaid
No. of Children
Attributed to
Demonstration
Practices
No. of Children
in Analytic
Sample*
No. of Demonstration
Practices With
Complete Data
Sample Size per
Demonstration Practice,
Median (Range)
1,599,800
1,632,819
40,353
92,882
33,895
57,553
32
32
469 (349,803)
846 (3610,714)
1,055,162
577,657
73,715
19,167
46,632
10,921
18
14
1,819 (26110,714)
583 (362,596)
Illinois
North Carolina/
South Carolina
North Carolina
South Carolina
*Children were included in the sample if they were continuously enrolled in fee for service or primary care case management Medicaid, had
no other source of coverage, had full benefits not through a waiver program, were not institutionalized, and the practice they were attributed to
completed a medical home assessment.
were age 5 or younger (Table 2). About 31% of the sample
in IL and 34% of the sample in NC/SC had a chronic condition or disability.
Seventy-six percent of the sample in IL and 64% in
NC/SC received the appropriate number of WCV. More
than one-quarter of each sample had a nonurgent, preventable, or avoidable ED visit (30% in IL; 28% in
NC/SC). By design, practices were equally distributed
into categories of medical homeness (tertiles; Table 3).
Table 4 shows how sample characteristics vary by medical homeness level. In the IL sample, a higher proportion
of children in the high medical homeness group were
black compared with children in the other medical
home levels. The percentage of children with a chronic
condition/disability was similar across medical home
levels (range 29%31%). In the NC/SC sample, a higher
proportion of children in the high medical homeness
group were from practices in NC and in rural practices.
Again, the percentage of children with a chronic condition/disability was fairly similar across medical home
levels (range 31%37%).
In multilevel logistic regression models, the estimated
associations between medical home level and childrens
health care utilization differed for practices completing
the NCQA 2011 self-assessment in IL and the MHI/
MHI-RSF in NC/SC. Inferences about the association between medical homeness and outcomes were the same in
the unadjusted and adjusted models; here we present results from adjusted models (Table 5).
For practices completing the NCQA tool in IL, there was
no statistically significant association between medical
homeness and receipt of WCV. However, children who
received care in practices with high medical homeness
were less likely to have a nonurgent, preventable, or avoidable ED visit than children in practices with low medical
homeness (odds ratio 0.65; 95% confidence interval
0.470.92). They were marginally less likely to have a
nonurgent, preventable, or avoidable ED visit than children
in practices with medium medical homeness (odds ratio
0.72, 95% confidence interval 0.521.01; P .06; not
shown in Table 5). There was no difference in nonurgent,
preventable, or avoidable ED use between the middle and
low medical home tertiles (odds ratio 0.90; 95% confidence
interval 0.651.27). Among practices completing the MHI/
MHI-RSF in NC/SC, there was no statistically significant
association between medical homeness and receipt of
WCV or nonurgent, preventable, or avoidable ED visits
(Table 5).
Table 2. Child-Level Sample Characteristics
Illinois
North Carolina/South Carolina
North Carolina
South Carolina
Characteristic
Total
Age group
05 y
612 y
1318 y
Sex
Male
Female
Race/ethnicity
Black
White
Other
Chronic condition or disability (yes)
Health care utilization
Appropriate receipt of well-child
visits
Any nonurgent, preventable, or
avoidable ED visit
33,895
100
57,553
100
46,632
100
10,921
100
18,081
10,498
5,316
53
31
16
32,510
17,362
7,681
56
30
14
26,810
13,936
5,886
57
30
13
5,700
3,426
1,795
52
31
16
17,197
16,698
51
49
29,584
27,969
51
49
23,943
22,689
51
49
5,641
5,280
52
48
15,204
10,644
8,047
10,384
45
31
24
31
18,886
26,059
12,608
19,360
33
45
22
34
14,316
21,643
10,673
15,695
31
46
23
34
4,570
4,416
1,935
3,665
42
40
18
34
25,659
76
36,455
64
29,831
65
6,624
62
10,103
30
15,914
28
12,808
27
3,106
28
ED indicates emergency department.
ACADEMIC PEDIATRICS
PRACTICE-REPORTED MEDICAL HOMENESS
Table 3. Practice-Level Sample Characteristics and Medical
Homeness
Characteristic
Illinois (NCQA self-assessment)
Total
32
NCQA 2011 self-assessment medical home tertile
High (score range: 66.8 to 83.3)
11
Medium (score range: 29.0 to 64.0)
11
Low (score range: 10.3 to 27.8)
10
North Carolina/South Carolina (MHI/MHI-RSF)
Total
32
Median (range) no. of providers*
4.5 (121)
Geography*
Urban/suburban
11
Rural
21
MHI/MHI-RSF medical home tertile
High (score range: 59.6 to 89.3)
10
Medium (score range: 49.1 to 58.9)
11
Low (score range: 24.1 to 46.4)
11
%
100
34
34
31
100
NA
34
66
31
34
34
NCQA indicates National Committee for Quality Assurance; MHI/
MHI-RSF, Medical Home Index/Medical Home IndexRevised
Short Form; NA, not applicable.
*Numbers of providers and geography were not available for
practices in Illinois.
An interaction term between medical home level and
chronic condition/disability status was not statistically significant in the NC/SC or IL analyses for either outcome,
indicating that the association between medical homeness
and outcomes did not vary significantly by health status.
Cross-tabulations and regression models stratified by
chronic condition/disability status confirmed the interpretation of the interaction term. This term was excluded
from final models presented in Table 5.
DISCUSSION
This study contributes to the small but growing body of
evidence on the association between medical homeness
and childrens health care utilization. In this crosssectional baseline analysis of practices participating in
the CHIPRA Quality Demonstration Grant Program, medical home level was not associated with age-appropriate
receipt of WCV among practices completing either the
MHI/MHI-RSF or the NCQA self-assessment. These results differ from findings by Paustian et al.15 There may
be a methodological explanation for null results: children
are only included in the sample if they had a well-child
or other ambulatory visit during the measurement year.
Although we are able to attribute approximately 70% to
80% of children in FFS or PCCM Medicaid, depending
on the state, it is possible that if we were able to attribute
children with no visits to practices there might be significant variation across medical home levels.
The association between nonurgent, preventable, or
avoidable ED visits and medical homeness varied depending on the sample and PCMH measure. Among practices in
IL that completed the NCQA 2011 medical home selfassessment, children who received care in practices with
high medical home scores were less likely to have a nonurgent, preventable, or avoidable ED visit than practices with
271
Table 4. Child-Level Sample Characteristics by Level of MH
Column % for:
Characteristic
Low MH
Medium MH
High MH
Illinois (NCQA
Self-Assessment)
n 7,507
n 8,917
n 17,471
58
30
12
53
30
16
51
32
17
52
48
51
49
50
50
27
49
24
29
21
50
29
30
65
14
21
31
n 10,687
n 15,055
n 31,811
53
31
15
55
31
14
58
29
12
52
48
51
49
51
49
34
40
26
37
27
57
16
31
35
42
23
34
53
47
14
86
23
77
40
60
82
18
95
5
Age group
05 y
612 y
1318 y
Sex
Male
Female
Race/ethnicity
Black
White
Other
Chronic condition or
disability (yes)
North Carolina/South
Carolina (MHI/MHI-RSF)
Age group
05 y
612 y
1318 y
Sex
Male
Female
Race/ethnicity
Black
White
Other
Chronic condition or
disability (yes)
Practice geography*
Urban/suburban
Rural
State
North Carolina
South Carolina
MH indicates medical homeness; NCQA, National Committee for
Quality Assurance; MHI/MHI-RSF, Medical Home Index/Medical
Home IndexRevised Short Form.
*Practice geography was not available for practices in Illinois.
low and medium medical home scores. Among practices
that completed the MHI/MHI-RSF in NC/SC, there was
no association with nonurgent, preventable, or avoidable
ED visits, a finding similar to that reported by Cooley
et al,14 who examined medical claims for children in practices that completed the MHI.
Several factors could explain the variation in our ED
visit results. First, the differences between the 2 PCMH
tools may explain the variation in results. Previous unpublished research has shown that scores on the MHI and the
NCQA self-assessment are not highly correlated.25,26 It is
plausible that the NCQA self-assessment better captures
domains of medical homeness that could be expected to
prevent nonurgent, preventable, or avoidable ED visits.
For example, access to primary care has been linked to
decreased ED use among children.2730 The NCQA selfassessment contains 7 items that measure Access and
Continuity, including access during office hours, afterhours access, and electronic access, whereas the
272
CHRISTENSEN ET AL
ACADEMIC PEDIATRICS
Table 5. Effect of Medical Homeness on Health Care Utilization
Appropriate Receipt of
Well-Child Visits
Characteristic
Unadjusted
%
Illinois (NCQA self-assessment)
MH tertile
High
75
Medium
78
Low
74
North/South Carolina (MHI/MHI-RSF)
MH tertile (pooled)
High
64
Medium
66
Low
64
MH tertile (NC)
High
64
Medium
66
Low
70
MH tertile (SC)
High
72
Medium
63
Low
59
Regression
Adjusted %
Adjusted
OR
77
74
76
1.02
0.91
(ref)
63
69
69
Any Nonurgent, Preventable, or Avoidable
Emergency Department Visit
Unadjusted
%
Regression
Adjusted %
Adjusted
OR
0.711.46
0.641.30
30
27
31
23
26
29
0.65*
0.90
(ref)
0.470.92
0.651.27
0.77
1.03
(ref)
0.471.26
0.681.55
25
31
29
27
29
29
0.92
0.99
(ref)
0.701.20
0.791.25
63
73
73
0.62
0.99
(ref)
0.341.15
0.511.91
25
33
29
28
29
31
0.86
0.91
(ref)
0.591.25
0.611.36
75
60
61
1.88
0.95
(ref)
0.754.74
0.581.57
27
26
30
25
26
26
0.96
1.04
(ref)
0.551.66
0.771.41
95% CI
95% CI
OR indicates odds ratio; CI, confidence interval; NCQA, National Committee for Quality Assurance; MH, medical home; MHI/MHI-RSF,
Medical Home Index/Medical Home IndexRevised Short Form.
*P < .05.
All models adjusted for: child age, race/ethnicity, and chronic conditions/disability status. NC/SC models further adjusted for number of
providers in the practice, practice geography (urban/suburban, rural), and state.
MHI-RSF includes only one item for Communication/Access, which does not specifically reference after-hours access or electronic access. It is possible that variation in
access to care was not well measured in the NC/SC sample.
Alternatively, given that these tools were used in
different states, the state Medicaid context and prior incentives for medical home implementation may also explain
the differences. For example, the racial composition of
children in the high medical homeness group varies across
the NC/SC and the IL samples. Although we controlled for
race in our models, these differences may be indicative of
other unobserved variations that could contribute to our results.
Variations in regression modeling across samples are unlikely to account for the difference in inferences. Although
we controlled for practice characteristics in the NC/SC
model but not the IL model (due to lack of data), the inferences regarding medical homeness did not change when we
removed practice characteristics from the NC/SC model in
sensitivity testing.
Several limitations of our study are important to note.
Medical homeness scores were self-reported by practices
and not verified against documentation. Practices volunteered to participate in the demonstration program and
may not be representative of child-serving practices statewide. Like many studies of Medicaid service use, our findings might not be generalizable to publicly insured children
who are enrolled in managed care (other than PCCM)
because we were unable to include those children in our analyses. In 2010, 71% of children with Medicaid in SC were
enrolled in traditional managed care (vs 0% of children in
NC and 9% of children in IL), making generalizability
more of a concern in SC than other states.31 However,
SC represents less than a fifth of the NC/SC sample, minimizing this limitation.
Like Cooley et al,14 we analyzed Medicaid claims from
the calendar year before the year medical homeness was assessed. If practices were increasing their medical homeness
during the claims year and quality of care improved after
the claims year, our models may attenuate any existing associations between higher medical home level and higherquality service use patterns. We have no information on
practices medical homeness or transformation activities
before the baseline data collection for the demonstration;
however, we know that practices began participating in
PCMH practice transformation activities under the CHIPRA Quality Demonstration Grant program immediately
after the baseline data collection, so we did not use claims
from the calendar year after medical homeness was assessed.
Finally, the NYU algorithm assigns each ED visit a probability of falling into the nonurgent, preventable, and primary caretreatable categories and was not designed to
classify individual visits into mutually exclusive categories. Thus, there is likely to be measurement error in
our indicator for nonurgent, preventable, or avoidable ED
use. However, that error is unlikely to systematically
vary by medical homeness tertile and therefore is unlikely
to bias our estimates of the association between medical
homeness and ED utilization.
Despite these limitations, this study contributes to the
narrow knowledge base on the associations between pediatric PCMH implementation and health service use in
several ways. First, it uses standardized, practice-reported
ACADEMIC PEDIATRICS
PCMH assessment tools and medical claims rather than
parent reports of medical homeness and service use. We
are aware of only 2 other published studies that use these
types of data to examine the relationship between medical
homeness and childrens health care utilization. As noted,
these studies yield mixed findings. Second, the multilevel
models account for the clustering of patients within practices, which has not been done in most other studies
(including adult studies) of PCMH outcomes. Failing to account for clustering can result in biased estimates.32
Finally, by presenting results using 2 different PCMH
tools, this study also suggests that differences in the definition and measurement of medical homeness may
contribute to the mixed findings in the existing literature.
Continued emphasis by insurers and states on PCMH interventions underscores the value of determining whether
medical homes in fact improve care for children. The
mixed findings to date reflect the complexity of this issue.
To determine the effects in various populations and policy
contexts with different measures, researchers must design
studies that can identify whether mixed medical home outcomes are due to variations in the measures of medical
homeness used, actual variations in medical home implementation fidelity, or variations in other factors not yet
measured. Longitudinal studies that examine changes in
multiple measures of medical homeness and health care
service use within practices over time would contribute
greatly to the evidence base.
CONCLUSIONS
With the CHIPRA Quality Demonstration Grant Program and other PCMH demonstrations currently underway, the evidence base on pediatric PCMH impacts will
expand over the next several years. Although our findings
suggest a potential association between medical homeness
and nonurgent, preventable, or avoidable ED use, the
mixed results of this and previous studies imply a need to
recognize the effects that differences in PCMH measurement tools and state policy context may have on the
research findings.
ACKNOWLEDGMENTS
All phases of this study were supported by a contract with the US
Department
of
Health
and
Human
Services,
AHRQ
(HHSA290200900019I/HHSA29032004T). The authors wish to
acknowledge Carl Cooley, MD, co-chair of the National Center for Medical Home Implementation; Sarah Scholle, PhD, of the National Committee for Quality Assurance; Genevieve Kenney, PhD, of the Urban Institute;
Catherine McLaughlin, PhD, of Mathematica Policy Research; and Cindy
Brach, MPP, and Linda Bergofsky, MSW, MBA, of the AHRQ for
providing valuable comments. We also thank the demonstration project
staff and state Medicaid agency staff who provided data and guidance.
Preliminary results from this study were presented at the Academy Health
Annual Research Meeting, June 23, 2013, in Baltimore, Md.
REFERENCES
1. Patient-Centered Primary Care Collaborative. Joint principles of
the patient-centered medical home. Available at: http://www.aafp.
org/dam/AAFP/documents/practice_management/pcmh/initiatives/
PCMHJoint.pdf. Accessed October 14, 2013.
PRACTICE-REPORTED MEDICAL HOMENESS
273
2. Bitton A, Martin C, Landon BE. A nationwide survey of patient
centered medical home demonstration projects. J Gen Intern Med.
2010;25:584592.
3. Grundy P, Hagan KR, Hansen JC, et al. The multi-stakeholder movement for primary care renewal and reform. Health Aff (Millwood).
2010;29:791798.
4. National Committee for Quality Assurance. Standards and guidelines
for NCQAs patient-centered medical home (PCMH). Available at:
http://www.ncqa.org/PublicationsProducts/RecognitionProducts/
PCMHPublications.aspx; 2011. Accessed October 14, 2013.
5. Cooley WC, McAllister JW, Sherrieb K, et al. The Medical Home Index: development and validation of a new practice-level measure of
implementation of the medical home model. Ambul Pediatr. 2003;3:
173180.
6. Hadland SE, Long WE. A systematic review of the medical home for
children without special health care needs. Matern Child Health J.
2014;18:891898.
7. Long WE, Bauchner H, Sege RD, et al. The value of the medical home
for children without special health care needs. Pediatrics. 2012;129:
8798.
8. Romaire MA, Bell JF, Grossman DC. Health care use and expenditures associated with access to the medical home for children and
youth. Med Care. 2012;50:262269.
9. Strickland BB, Jones JR, Ghandour RM, et al. The medical home:
health care access and impact for children and youth in the United
States. Pediatrics. 2011;127:604611.
10. Kieckhefer GM, Greek AA, Joesch JM, et al. Presence and characteristics of medical home and health services utilization among children
with asthma. J Pediatr Health Care. 2005;19:285292.
11. Knapp CA, Hinojosa M, Baron-Lee J, et al. Factors associated with a
medical home among children with attention-deficit hyperactivity
disorder. Matern Child Health J. 2012;16:17711778.
12. Diedhiou A, Probst JC, Hardin JW, et al. Relationship between presence of a reported medical home and emergency department use
among children with asthma. Med Care Res Rev. 2010;67:450475.
13. Romaire MA, Bell JF, Grossman DC. Medical home access and health
care use and expenditures among children with special health care
needs. Arch Pediatr Adolesc Med. 2012;166:323330.
14. Cooley WC, McAllister JW, Sherrieb K, et al. Improved outcomes
associated with medical home implementation in pediatric primary
care. Pediatrics. 2009;124:358364.
15. Paustian ML, Alexander JA, El Reda DK, et al. Partial and incremental PCMH practice transformation: implications for quality and costs.
Health Serv Res. 2014;49:5274.
16. Agency for Healthcare Research and Quality. National evaluation of
the CHIPRA quality demonstration grant program. Available at:
http://www.ahrq.gov/policymakers/chipra/demoeval/index.html. Accessed October 14, 2013.
17. McMorrow S, Christensen A, Natzke B, et al. How are states and evaluators measuring medical homeness in the CHIPRA Quality Demonstration Grant Program? Available at: http://www.ahrq.gov/policymakers/
chipra/demoeval/what-we-learned/highlight02.pdf; 2013. Accessed
January 9, 2015.
18. American Academy of Pediatrics. Recommendations for preventive
pediatric health care. Available at: http://brightfutures.aap.org/pdfs/
AAP%20Bright%20Futures%20Periodicity%20Sched%20101107.
pdf. Accessed October 15, 2013.
19. Centers for Medicare and Medicaid Services. Core set of childrens
health care quality measures for Medicaid and CHIP (child core
set): technical specifications and resource manual for federal fiscal
year 2013 reporting. Available at: http://www.medicaid.gov/
Medicaid-CHIP-Program-Information/By-Topics/Quality-of-Care/
Downloads/Medicaid-and-CHIP-Child-Core-Set-Manual.pdf. Accessed October 16, 2013.
20. Ballard DW, Price M, Fung V, et al. Validation of an algorithm for categorizing the severity of hospital emergency department visits. Med
Care. 2010;48:5863.
21. New York University. NYU ED background. Available at: http://
wagner.nyu.edu/faculty/billings/nyued-background.
Accessed
October 15, 2013.
274
CHRISTENSEN ET AL
22. Billings J, Parikh N, Mijanovich T. Emergency Department Use: The
New York Story. New York, NY: Commonwealth Fund. Available at:
http://www.commonwealthfund.org/usr_doc/billings_nystory.pdf;
2010. Accessed September 24, 2014.
23. Ben-Isaac E, Schrager SM, Keefer M, et al. National profile of nonemergent pediatric emergency department visits. Pediatrics. 2010;
125:454459.
24. Simon TD, Cawthon ML, Stanford S, et al. Pediatric medical
complexity algorithm: a new method to stratify children by medical
complexity. Pediatrics. 2014;133:e1647e1654.
25. Swigonski N, Nutakki K, Eckert G, et al. What is the measure of a
medical home? A comparison of the two leading instruments. Paper
presented at: Pediatric Academic Societies Annual Meeting; May
47, 2013; Washington, DC.
26. Reutland CP, Gallia C, Laurie A, et al. Becoming better medical
homes: improving systems and processes in the Tri-state Childrens
Health Improvement Consortium (T-CHIC). Poster presented at:
Academy Health Child Health Services Research Meeting; June 22,
2013; Baltimore, Md.
27. Brousseau DC, Gorelick MH, Hoffmann RG, et al. Primary care quality and subsequent emergency department utilization for children in
Wisconsin Medicaid. Acad Pediatr. 2009;9:3339.
ACADEMIC PEDIATRICS
28. Johnson WG, Rimsza ME. The effects of access to pediatric care and
insurance coverage on emergency department utilization. Pediatrics.
2004;113:483487.
29. Zickafoose JS, DeCamp LR, Prosser LA. Association between
enhanced access services in pediatric primary care and utilization
of emergency departments: a national parent survey. J Pediatr.
2013;163:13891395.
30. Wang C, Villar ME, Mulligan DA, et al. Cost and utilization analysis
of a pediatric emergency department diversion project. Pediatrics.
2005;116:10751079.
31. Centers for Medicare and Medicaid Services. Medicaid Statistical Information System (MSIS) state summary datamarts, 2010. Available at:
http://www.cms.gov/Research-Statistics-Data-and-Systems/ComputerData-and-Systems/MedicaidDataSourcesGenInfo/MSIS-Mart-Home.
html. Accessed October 16, 2013.
32. Peikes D, Dale S, Lundquist E, et al. Building the Evidence Base for
the Medical Home: What Sample and Sample Size Do Studies Need?.
Rockville, Md: Agency for Healthcare Research and Quality; 2011.
AHRQ Publication No. 11-0100-EF. White paper prepared by Mathematica Policy Research under contract HHSA290200900019I TO2.
Vous aimerez peut-être aussi
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (894)
- 9 To 5 Props PresetsDocument4 pages9 To 5 Props Presetsapi-300450266100% (1)
- HierbasDocument25 pagesHierbasrincón de la iohPas encore d'évaluation
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- RUKUS March 2010Document32 pagesRUKUS March 2010RUKUS Magazine29% (14)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- QRF HD785-7Document2 pagesQRF HD785-7Ralf MaurerPas encore d'évaluation
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- Wastewater Treatment Plant Design PDFDocument68 pagesWastewater Treatment Plant Design PDFmostafa1alaahobaPas encore d'évaluation
- Experiment Vii To Prepare A Temporary Mount of Onion Root Tip To Study MitosisDocument4 pagesExperiment Vii To Prepare A Temporary Mount of Onion Root Tip To Study MitosisAnonymous ceYk4p4100% (12)
- Post Insertion Complaints in CD For Dental Students For Final Year For Their Seminar.Document31 pagesPost Insertion Complaints in CD For Dental Students For Final Year For Their Seminar.Anonymous ceYk4p4Pas encore d'évaluation
- BDS First Professional Exam Question Paper 2008-2009 - Teerthanker Mahaveer Dental CollegeDocument21 pagesBDS First Professional Exam Question Paper 2008-2009 - Teerthanker Mahaveer Dental CollegeAnonymous ceYk4p4Pas encore d'évaluation
- Benefits and Limitations of Vojta ApproachDocument50 pagesBenefits and Limitations of Vojta ApproachAlice Teodorescu100% (3)
- HTM 2025 2 (New) Ventilation in HospitalsDocument123 pagesHTM 2025 2 (New) Ventilation in HospitalsArvish RamseebaluckPas encore d'évaluation
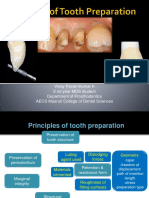
- Tooth Preparation Design and PrinciplesDocument80 pagesTooth Preparation Design and PrinciplesAnonymous ceYk4p4100% (2)
- A. Kumar Aswamy Job Offer LetterDocument1 pageA. Kumar Aswamy Job Offer LetterHimanshu PatelPas encore d'évaluation
- 3-Step Mindset Reset: Overcome Self-Doubt with Mel Robbins' TrainingDocument11 pages3-Step Mindset Reset: Overcome Self-Doubt with Mel Robbins' TrainingBožana RadošPas encore d'évaluation
- NCMA 217 - Newborn Assessment Ma'am JhalDocument5 pagesNCMA 217 - Newborn Assessment Ma'am JhalMariah Blez BognotPas encore d'évaluation
- Abstract - Tropen Tag 2011 PDFDocument634 pagesAbstract - Tropen Tag 2011 PDFzmoghesPas encore d'évaluation
- Family MedicineDocument156 pagesFamily MedicinedtriggPas encore d'évaluation
- Naugachiya To Agra Fort 22 August 2019Document2 pagesNaugachiya To Agra Fort 22 August 2019Anonymous ceYk4p4Pas encore d'évaluation
- Experiment III - To Study Soil TexturesDocument2 pagesExperiment III - To Study Soil TexturesAnonymous ceYk4p4Pas encore d'évaluation
- PV in India Good ArticleDocument8 pagesPV in India Good ArticleAnonymous ceYk4p4Pas encore d'évaluation
- Boss Si Pay ReceiptDocument1 pageBoss Si Pay ReceiptAnonymous ceYk4p4Pas encore d'évaluation
- Application For Replacement of Faulty RefrigeratorDocument1 pageApplication For Replacement of Faulty RefrigeratorAnonymous ceYk4p4Pas encore d'évaluation
- Bhbhi Pan Application AcknloDocument2 pagesBhbhi Pan Application AcknloAnonymous ceYk4p4Pas encore d'évaluation
- BSc Nursing ProspectusDocument32 pagesBSc Nursing ProspectusAnonymous ceYk4p4Pas encore d'évaluation
- BPSSC Online Recruitment for Bihar Police JobsDocument1 pageBPSSC Online Recruitment for Bihar Police JobsAnonymous ceYk4p4Pas encore d'évaluation
- Volunteer Guidebook For Unknown ExpeditionDocument65 pagesVolunteer Guidebook For Unknown ExpeditionAnonymous ceYk4p4Pas encore d'évaluation
- Application For Replacement of Faulty LPG RegulatorDocument1 pageApplication For Replacement of Faulty LPG RegulatorAnonymous ceYk4p40% (1)
- JR Valmiki Hospital 2018Document2 pagesJR Valmiki Hospital 2018Anonymous ceYk4p4Pas encore d'évaluation
- List of Eligible Candidates and Rejected Applications For Interview For Short Term Paid Clinical Assistantship 2017Document2 pagesList of Eligible Candidates and Rejected Applications For Interview For Short Term Paid Clinical Assistantship 2017Anonymous ceYk4p4Pas encore d'évaluation
- Advertisement For The Post of Dentist in Indian Air Force Station, DalhousieDocument1 pageAdvertisement For The Post of Dentist in Indian Air Force Station, DalhousieAnonymous ceYk4p4Pas encore d'évaluation
- Vis Checks in CPDocument7 pagesVis Checks in CPAnonymous ceYk4p4Pas encore d'évaluation
- Entomology Question Paper 2005Document6 pagesEntomology Question Paper 2005Anonymous ceYk4p4Pas encore d'évaluation
- Instrs For Isg Detailed To Cover Prac CampDocument22 pagesInstrs For Isg Detailed To Cover Prac CampAnonymous ceYk4p4Pas encore d'évaluation
- National Eligibility Entrance Test 2102 PDFDocument1 pageNational Eligibility Entrance Test 2102 PDFAnonymous ceYk4p4Pas encore d'évaluation
- Objective of Impression Making - SupportDocument8 pagesObjective of Impression Making - SupportAnonymous ceYk4p4Pas encore d'évaluation
- श्रीमद् भगवत गीता अध्याय-2 ,Shree Mad Bhagwat Geeta Chapter 2Document42 pagesश्रीमद् भगवत गीता अध्याय-2 ,Shree Mad Bhagwat Geeta Chapter 2vikalpsewa100% (1)
- Alimentary Canal 3rd Year2Document19 pagesAlimentary Canal 3rd Year2slOwpOke13Pas encore d'évaluation
- Common Snakes of IndiaDocument19 pagesCommon Snakes of IndiaHemant KarandikarPas encore d'évaluation
- Admission Notice 2013 - English PDFDocument1 pageAdmission Notice 2013 - English PDFchatuusumitavaPas encore d'évaluation
- MediCAL AND DENTAL COURSE DETAIL IN ALIGARH MUSLIM UNIVERSITY 2013Document2 pagesMediCAL AND DENTAL COURSE DETAIL IN ALIGARH MUSLIM UNIVERSITY 2013Anonymous ceYk4p4Pas encore d'évaluation
- Glass Ionomer Cement and Its Application in Advance DentistryDocument20 pagesGlass Ionomer Cement and Its Application in Advance DentistryAnonymous ceYk4p4Pas encore d'évaluation
- Basic Computer For Small BusinessDocument21 pagesBasic Computer For Small Businessashiq_a99Pas encore d'évaluation
- BDS First Professional Exam 2009-2010, Teerthanker Mahaveer Dental College, MoradabadDocument8 pagesBDS First Professional Exam 2009-2010, Teerthanker Mahaveer Dental College, MoradabadAnonymous ceYk4p4Pas encore d'évaluation
- Dr. Namrata Misra Head of Bioinnovations at KIIT UniversityDocument1 pageDr. Namrata Misra Head of Bioinnovations at KIIT Universitymanisha maniPas encore d'évaluation
- Practice of Epidemiology Performance of Floating Absolute RisksDocument4 pagesPractice of Epidemiology Performance of Floating Absolute RisksShreyaswi M KarthikPas encore d'évaluation
- EEDMATH1 - Teaching Mathematics in The Primary Grades Beed 2E Learning Activity PlanDocument3 pagesEEDMATH1 - Teaching Mathematics in The Primary Grades Beed 2E Learning Activity PlanBELJUNE MARK GALANANPas encore d'évaluation
- Pack Alimentacion Clin in Perin 14Document194 pagesPack Alimentacion Clin in Perin 14Paz BustosPas encore d'évaluation
- English III Module 2 Simple Present Job and Job VerbsDocument4 pagesEnglish III Module 2 Simple Present Job and Job VerbsAdrian CortesPas encore d'évaluation
- Model Fs CatalogDocument4 pagesModel Fs CatalogThomas StempienPas encore d'évaluation
- Solcon Catalog WebDocument12 pagesSolcon Catalog Webquocviet612Pas encore d'évaluation
- EP Series User Manual PDFDocument40 pagesEP Series User Manual PDFa.elwahabPas encore d'évaluation
- Chapter 21Document39 pagesChapter 21Hamza ElmoubarikPas encore d'évaluation
- Comm Part For A320Document1 pageComm Part For A320ODOSPas encore d'évaluation
- Jairo Garzon 1016001932 G900003 1580 Task4Document12 pagesJairo Garzon 1016001932 G900003 1580 Task4Jairo Garzon santanaPas encore d'évaluation
- Position paper-MUNUCCLE 2022: Refugees) Des États !Document2 pagesPosition paper-MUNUCCLE 2022: Refugees) Des États !matPas encore d'évaluation
- ABSCESSDocument35 pagesABSCESSlax prajapatiPas encore d'évaluation
- The Impact of StressDocument3 pagesThe Impact of StressACabalIronedKryptonPas encore d'évaluation
- MLS 321 Aubf M6u2 Other Metabolic Diseases V2122Document7 pagesMLS 321 Aubf M6u2 Other Metabolic Diseases V2122proximusPas encore d'évaluation
- Lesson 1 CA 3Document13 pagesLesson 1 CA 3myndlePas encore d'évaluation
- OC - PlumberDocument6 pagesOC - Plumbertakuva03Pas encore d'évaluation
- Grab Go Porter S 5 ForcesDocument2 pagesGrab Go Porter S 5 ForcesUtkarsh SharmaPas encore d'évaluation