Académique Documents
Professionnel Documents
Culture Documents
Coronary Artery Disease (CAD) Angina Pectoris: Chapter 28: Management of Patients With CVD
Transféré par
Lizzy WayDescription originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Coronary Artery Disease (CAD) Angina Pectoris: Chapter 28: Management of Patients With CVD
Transféré par
Lizzy WayDroits d'auteur :
Formats disponibles
Chapter
28:
Management
Patients with CVD
of
e) Silent ischemia ECG changes with
a stress test, no reports of pain
Coronary Artery Disease (CAD)
Angina Pectoris
Most
prevalent
type
of
cardiovascular disease in adults
It is important for nurses to be
familiar with various manifestations
of coronary artery conditions
The need of O2 exceeds that of
what the body has
Characterized by episodes or
paroxysms of pain or pressure in
the anterior chest
Factors causing pain:
Physical exertion
Exposure to cold
Eating a heavy meal
Stress or any emotion-provoking
situation
Mild indigestion to choking or
heavy sensation on upper chest
that ranges from discomfort to
agonizing pain accompanied by
severe apprehension and feeling of
impending death
Pain may radiate to neck, jaw,
shoulders, or inner aspects of
upper arms usually left arm
Weakness or numbness in the
arms, wrists hands, SOB, pallor,
diaphoresis,
dizziness/lightheadedness,
N/V,
anxiety
Increased O2 demand O2 therapy
Nitroglycerin
to
reduce
myocardial
O2
consumption,
decreases ischemia and relieves
pain
adrenergic blocking agents (olol)reduce myocardial O2
consumption by blocking
adrenergic sympathetic stimulation
to the heart
Calcium channel blocking agents
(amlodipine) - decrease workload
of the heart
Anti-platelet and anti-coagulant
meds
prevent
platelet
aggregation
Aspirin
Clopidogrel
Heparin prevents formation of
new blood clots
Glycoprotein 2B/3A agents
bleeding is the major side effects
Coronary Atherosclerosis
Abnormal accumulation of lipid
(fatty substances) and fibrous
tissue in the lining of arterial blood
vessel walls; these block and
narrow the coronary vessels and
reduces
blood
flow
to
the
myocardium
Impediment to blood flow is usually
progressive, causing an inadequate
blood supply that deprives cardiac
muscle cells of O2 (ischemia)
Risk Factors:
Hyperlipidemia
Smoking, tobacco use
HPN
DM
Metabolic Syndrome
Obesity
Physical inactivity
Prevention:
Controlling
cholesterol
abnormalities
Dietary measures
Physical activity
Medications (-statins, nicotinic
acids,
fibrates,
bile
acid
sequestrants,
cholesterol
absorption inhibitor, omega-3acid-ethyl esters)
Promoting cessation of tobacco
use
Managing HPN
Controlling DM
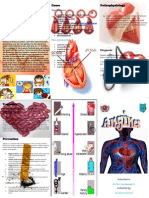
Types of Angina:
a) Stable angina occurs on exertion,
relieved by rest
b) Unstable angina (preinfarction or
crescendo angina) symptoms
increase in intensity and severity,
may not be relieved by rest
c) Intractable or refectory angina
severe incapacitating chest pain
d) Variant
angina
(Prinzmetals
angina) pain at rest, caused by
coronary artery vasospasm
Myocardial Infarction (MI)
Irreversible cardiac damage from
occlusion of one or more arteries
Also
called
coronary
artery
occlusion/thrombosis
Chest pain that occurs suddenly
and continuous despite rest and
meds
SOB, indigestion, nausea, anxiety,
cool, pale, moist skin
Assessment:
Patient
Hx
presenting
symptoms, Hx of previous cardiac
and other illnesses, family Hx
ECG,
2D-Echo,
lab
tests
(creatinine kinase, myoglobin,
troponin)
Analgesics,
ACE-inhibitors,
thrombolytics
Cardiac Rehab
Phase
1
diagnosis
of
atherosclerosis
Phase 2 after patient has been
discharged
Phase 3 long-term outpatient
program, maintaining CV stability
and long-term conditioning
Chapter 32: Assessment
and
Management of Patients with HPN
Primary HPN high BP from an
unknown cause
Secondary HPN high BP r/t
identified cause
Accompanies other risk factors:
atherosclerotic
heart
disease
(dyslipidemia abnormal fat level),
obesity, DM, metabolic syndrome,
sedentary lifestyle
Hemorrhages, exudates, arteriolar
narrowing,
cotton-wool
spots,
papilledema (in severe HPN), left
ventricular hypertrophy, alterations
in vision or speech, dizziness,
weakness, a sudden fall, or
transient or permanent paralysis
on one side (hemiplegia)
Ax: ECG; renal damage maybe
suggested by elevations of BUN
and creatinine levels or by
microalbuminuria
or
macroalbuminuria
Risk factors:
Smoking
Dyslipidemia
DM
Impaired renal fxn
Obesity
Physical inactivity
Age (older than 55 for men, 65
for women)
Family Hx
Management:
Pharmacologic Tx:
Thiazide diuretics
Loop diuretics (-anides)
K-sparing diuretics
Aldosterone receptor blockers
Central 2 agonists and
other centrally acting drugs
-blockers
1-blockers
Combined - and -blockers
Vasodilators
ACE inhibitors
Angiotensin
2
receptor
blockers
CCB
Dihydropyridines
Direct renin inhibitors
Step 1:
S-top smoking
C-ontrol weight
I-nvolve your doctor
E-at right
N-ote your med intake
Cut down your salt
E-xercise
Step 2 continue lifestyle
modification,
single
med
is
prescribed and started at low
dose
Step 3 increase drug dose or
substitute another drug if no
response or side effects become
apparent; add a 2nd drug if
diuretic is not used
Step 4 add a 2nd or 3rd drug
Hypertensive crisis: hypertensive
emergency
and
hypertensive
urgency
Hypertensive emergency BP is
extremely elevated (more than
180/120 mmHg); there is an
actual or developing clinical
dysfunction of the target organ;
acute,
life-threatening
BP
elevations that require prompt Tx
in an ICU because of the serious
target organ damage that may
occur
Hypertensive urgency BP is very
elevated but there is no evidence
of impending or progressive
target organ damage
*LDL: Normal Adult Range: 62 130 mg/dl
Optimal Adult Reading: 81 mg/dl
HDL: Normal Adult Range: 35 - 135 mg/dl
Optimal Adult Reading: +85 mg/dl
Various things that can affect normal HDL
and LDL levels.:
1- Weight
2345-
Physical activity
Diet strategy
Genetic factor
Age and sex
Vous aimerez peut-être aussi
- Angina PectorisDocument36 pagesAngina PectorisBardahWasaLamahPas encore d'évaluation
- IHD. Stable Angina Pectoris Clinical Protocols of The Ministry of Health of THDocument34 pagesIHD. Stable Angina Pectoris Clinical Protocols of The Ministry of Health of THMemories Of j5Pas encore d'évaluation
- Angina (Coronary Artery Disease/Acute Coronary Syndrome) : Care SettingDocument17 pagesAngina (Coronary Artery Disease/Acute Coronary Syndrome) : Care SettingmeghanaPas encore d'évaluation
- Hypertension Concept MapDocument1 pageHypertension Concept Mapgfhbgfhgf71% (7)
- AnginaDocument6 pagesAnginaArslan SaeedPas encore d'évaluation
- PrelimsDocument11 pagesPrelimsJess Fabra100% (1)
- Cardio-Vascular Problems: Group 1Document15 pagesCardio-Vascular Problems: Group 1Reanne Claudine LagunaPas encore d'évaluation
- Angina PectorisDocument30 pagesAngina PectorisTaufik Ramadhan Biya83% (6)
- Atherosclerosis Is The Primary Factor in The Development of CADDocument6 pagesAtherosclerosis Is The Primary Factor in The Development of CADSharlee StonePas encore d'évaluation
- CardiologyDocument9 pagesCardiologyAbi RajasingamPas encore d'évaluation
- Angina PectorisDocument12 pagesAngina Pectorismardsz93% (14)
- Nursing Management Patients W CVD Part2 Myocardial Infarction EnglishDocument43 pagesNursing Management Patients W CVD Part2 Myocardial Infarction EnglishRizka Patria SariPas encore d'évaluation
- Science Time: With Ma'am Melanie!Document28 pagesScience Time: With Ma'am Melanie!Melanie CoronaPas encore d'évaluation
- Angina (Coronary Artery Disease) : Care SettingDocument18 pagesAngina (Coronary Artery Disease) : Care SettingNom NomPas encore d'évaluation
- Presentor: John Hommer E. Dy M.D. Moderator: Joy Marchadesch M.DDocument57 pagesPresentor: John Hommer E. Dy M.D. Moderator: Joy Marchadesch M.DJohn Hommer DyPas encore d'évaluation
- Unstable AnginaDocument5 pagesUnstable AnginaAria AlysisPas encore d'évaluation
- Case Analysis: Medical Surgical NursingDocument7 pagesCase Analysis: Medical Surgical NursingMaria TheresePas encore d'évaluation
- Angina Pectoris: Prepared byDocument30 pagesAngina Pectoris: Prepared byjyothiPas encore d'évaluation
- NCMB 316 Cu14 AdrenalDocument39 pagesNCMB 316 Cu14 AdrenalJanine Dela CruzPas encore d'évaluation
- Angina PectorisDocument12 pagesAngina Pectorisapi-3797941Pas encore d'évaluation
- Angina PectorisDocument8 pagesAngina PectorisPrince DuPas encore d'évaluation
- What Is Angina PectorisDocument2 pagesWhat Is Angina PectorisjesloupayagPas encore d'évaluation
- NCP Angina Coronary Artery DiseaseDocument6 pagesNCP Angina Coronary Artery DiseaseRon Batacan De LeonPas encore d'évaluation
- CV Diet-Fk Modul 4.1 2015Document34 pagesCV Diet-Fk Modul 4.1 2015aryu.kusumastutiPas encore d'évaluation
- NCM Disorders of Myocardial Perfusion-2Document9 pagesNCM Disorders of Myocardial Perfusion-2Jeson Vien GuerraPas encore d'évaluation
- Cardiac Function DisordersDocument8 pagesCardiac Function DisordersAshley MalsonPas encore d'évaluation
- Cardivascular Case Study 4Document57 pagesCardivascular Case Study 4api-302598263Pas encore d'évaluation
- Ischemic Heart Disease, or Coronary Artery Disease: CausesDocument2 pagesIschemic Heart Disease, or Coronary Artery Disease: CausesRandolph AvelinoPas encore d'évaluation
- Stable IHDDocument16 pagesStable IHDDarawan MirzaPas encore d'évaluation
- DR - Datten Bangun MSC - SPFK & DR - Tri Widyawati Msi, PHD Dept - Farmakologi & Therapeutik Fak - Kedokteran Usu MedanDocument50 pagesDR - Datten Bangun MSC - SPFK & DR - Tri Widyawati Msi, PHD Dept - Farmakologi & Therapeutik Fak - Kedokteran Usu MedanHabib Al KahfiPas encore d'évaluation
- Ischemic Heart DiseaseDocument76 pagesIschemic Heart DiseaseNasser AlorfiPas encore d'évaluation
- Drugs For Hypertension 2023Document19 pagesDrugs For Hypertension 2023aguilarjanicaPas encore d'évaluation
- Nclex Study 1Document11 pagesNclex Study 1Katie Shortt100% (4)
- What Symptoms Should Lead The Nurse To Suspect The Pain May Be Angina?Document5 pagesWhat Symptoms Should Lead The Nurse To Suspect The Pain May Be Angina?Dylan Angelo AndresPas encore d'évaluation
- CardioDocument9 pagesCardioVirgilio Reyes ManuelPas encore d'évaluation
- Unstable Angina PectorisDocument28 pagesUnstable Angina PectorisLissaberti AmaliahPas encore d'évaluation
- HypertensionDocument1 pageHypertensionAllyne GavinoPas encore d'évaluation
- Coronary Artery DiseaseDocument15 pagesCoronary Artery DiseaseMuhammad Daha SanusiPas encore d'évaluation
- Cardiovascular SystemDocument205 pagesCardiovascular Systemizuku midoriyaPas encore d'évaluation
- Cardio Ms Hand OutDocument10 pagesCardio Ms Hand OutVictor ShonPas encore d'évaluation
- Asthma:: Case Scenario: DDXDocument10 pagesAsthma:: Case Scenario: DDXFemale calmPas encore d'évaluation
- Chapter 30Document16 pagesChapter 30NurseNancy93Pas encore d'évaluation
- 2myocardial InfarctionDocument29 pages2myocardial Infarctionblessed23Pas encore d'évaluation
- Myocardial InfarctionDocument3 pagesMyocardial Infarctionaja_delPas encore d'évaluation
- Angina PectorisDocument11 pagesAngina Pectorisjialin80% (5)
- Angina Pectoris: Basic InformationDocument3 pagesAngina Pectoris: Basic InformationAsma FerabilPas encore d'évaluation
- ACS (Dr. Thamrin 2015)Document43 pagesACS (Dr. Thamrin 2015)ok sogatenPas encore d'évaluation
- Hypertension (Hypertensive Urgency)Document2 pagesHypertension (Hypertensive Urgency)itsmeayaPas encore d'évaluation
- Pharmacology: Unit VIIIDocument92 pagesPharmacology: Unit VIIIChristian Laraya AlayonPas encore d'évaluation
- Drugs Used To Treat Cardiovascular Diseases: HypertensionDocument35 pagesDrugs Used To Treat Cardiovascular Diseases: HypertensionAyro Business CenterPas encore d'évaluation
- Endocrine Disorders and DrugsDocument149 pagesEndocrine Disorders and DrugsJaypee Fabros Edra100% (1)
- Management & Nursing Care of Patient With Coronary Artery DiseasesDocument49 pagesManagement & Nursing Care of Patient With Coronary Artery DiseaseslouradelPas encore d'évaluation
- Healing Your Heart : The Power of Diet and Homeopathy: Diet, #3D'EverandHealing Your Heart : The Power of Diet and Homeopathy: Diet, #3Pas encore d'évaluation
- Diabetes: Complications of Diabetes: The most important information you need to improve your healthD'EverandDiabetes: Complications of Diabetes: The most important information you need to improve your healthPas encore d'évaluation
- A Simple Guide to Hypertension and Heart DiseasesD'EverandA Simple Guide to Hypertension and Heart DiseasesÉvaluation : 5 sur 5 étoiles5/5 (1)
- How Not To Die From High Blood Pressure - Based On The Teachings Of Michael Greger: Preventing Hypertension And ThrivingD'EverandHow Not To Die From High Blood Pressure - Based On The Teachings Of Michael Greger: Preventing Hypertension And ThrivingPas encore d'évaluation
- Exercise and Diabetes: A Clinician's Guide to Prescribing Physical ActivityD'EverandExercise and Diabetes: A Clinician's Guide to Prescribing Physical ActivityPas encore d'évaluation
- CIR-vs-Isabela-Cultural-CorpDocument1 pageCIR-vs-Isabela-Cultural-CorpLizzy WayPas encore d'évaluation
- Duty Free v. COADocument1 pageDuty Free v. COALizzy Way100% (1)
- Winebrenner Inigo Insurance Brokers Inc vs. CIRDocument1 pageWinebrenner Inigo Insurance Brokers Inc vs. CIRLizzy WayPas encore d'évaluation
- MERALCO, Et Al. Vs LimDocument2 pagesMERALCO, Et Al. Vs LimLizzy WayPas encore d'évaluation
- Arches v. BellosilloDocument1 pageArches v. BellosilloLizzy WayPas encore d'évaluation
- Medicard v. CirDocument1 pageMedicard v. CirLizzy WayPas encore d'évaluation
- 2004 Rules On Notarial PracticeDocument14 pages2004 Rules On Notarial PracticeLizzy Way100% (3)
- Electronic Commerce Act (RA No. 8792)Document2 pagesElectronic Commerce Act (RA No. 8792)Lizzy WayPas encore d'évaluation
- Intellectual Property Code (RA No. 8293)Document8 pagesIntellectual Property Code (RA No. 8293)Lizzy WayPas encore d'évaluation
- Basilan Estates vs. CirDocument1 pageBasilan Estates vs. CirLizzy WayPas encore d'évaluation
- Mendez Vs People 726 SCRA 203 (2014)Document1 pageMendez Vs People 726 SCRA 203 (2014)Lizzy WayPas encore d'évaluation
- Sy Po Vs CTADocument1 pageSy Po Vs CTALizzy WayPas encore d'évaluation
- ABAKADA Guro vs. Ermita, 469 SCRA 14Document2 pagesABAKADA Guro vs. Ermita, 469 SCRA 14Lizzy WayPas encore d'évaluation
- Tan Tiong Bio vs. CIR, G.R. No. L-15778, April 23, 1962Document1 pageTan Tiong Bio vs. CIR, G.R. No. L-15778, April 23, 1962Lizzy WayPas encore d'évaluation
- Abakada Guro Party List Vs Ermita GR 168056Document1 pageAbakada Guro Party List Vs Ermita GR 168056Lizzy WayPas encore d'évaluation
- Data Privacy Act (RA No. 10173)Document4 pagesData Privacy Act (RA No. 10173)Lizzy WayPas encore d'évaluation
- PLDT Vs City of BacolodDocument1 pagePLDT Vs City of BacolodLizzy Way100% (1)
- Lutz Vs AranetaDocument1 pageLutz Vs AranetaLizzy WayPas encore d'évaluation
- Lorenzo vs. Posadas Jr.Document2 pagesLorenzo vs. Posadas Jr.Lizzy Way100% (1)
- Paseo Realty and Development CorpDocument1 pagePaseo Realty and Development CorpLizzy WayPas encore d'évaluation
- CIR Vs Eastern TelecommunicationsDocument1 pageCIR Vs Eastern TelecommunicationsLizzy WayPas encore d'évaluation
- Phantom of The OperaDocument18 pagesPhantom of The OperaLizzy Way100% (1)
- CIR V SantosDocument1 pageCIR V SantosLizzy WayPas encore d'évaluation
- Holy Sonnets - Batter My Heart, Three Person'd GodDocument11 pagesHoly Sonnets - Batter My Heart, Three Person'd GodLizzy WayPas encore d'évaluation
- Sarasola v. Trinidad, 40 Phil. 252Document1 pageSarasola v. Trinidad, 40 Phil. 252Lizzy Way100% (1)
- Treatment of EncopresisDocument2 pagesTreatment of Encopresisapi-324904250Pas encore d'évaluation
- Insulin in DMDocument46 pagesInsulin in DMask1400Pas encore d'évaluation
- AIIMS PG Entrance May 2004 Solved Question Paper With KeyDocument15 pagesAIIMS PG Entrance May 2004 Solved Question Paper With KeySAIFPas encore d'évaluation
- Medical para Health-1Document504 pagesMedical para Health-1Yordanos AsmarePas encore d'évaluation
- Interpretation of Mmpi 2 Clinical ScalesDocument23 pagesInterpretation of Mmpi 2 Clinical ScalesJuan LopezPas encore d'évaluation
- Maria Reinares, Eduard Vieta - Integrative Psychotherapy For Bipolar Disorders-Cambridge University Press (2020)Document133 pagesMaria Reinares, Eduard Vieta - Integrative Psychotherapy For Bipolar Disorders-Cambridge University Press (2020)nohanemillerPas encore d'évaluation
- RLE III - A ENT MED Day 2Document6 pagesRLE III - A ENT MED Day 2Kristian Karl Bautista Kiw-isPas encore d'évaluation
- مدونة كل العرب الطبية Davidson - Mcq - 22 - edition PDFDocument232 pagesمدونة كل العرب الطبية Davidson - Mcq - 22 - edition PDFنورهانعزالدين100% (1)
- "Focal Infection Theory" States That Bacteria FromDocument2 pages"Focal Infection Theory" States That Bacteria FromBea YmsnPas encore d'évaluation
- COMPLETE Medical Disease in PregnancyDocument210 pagesCOMPLETE Medical Disease in PregnancyCHANDREN ARUMUGAMPas encore d'évaluation
- Haematology-Oncology McqsDocument80 pagesHaematology-Oncology McqsKarim MohamedPas encore d'évaluation
- 4 6048890192880730833Document332 pages4 6048890192880730833Rin4lPas encore d'évaluation
- Experimental Pharmacology: Irrational Drug CombinationsDocument5 pagesExperimental Pharmacology: Irrational Drug CombinationsPrabangkara BillyPas encore d'évaluation
- Dr. Lamia El Wakeel, PhD. Lecturer of Clinical Pharmacy Ain Shams UniversityDocument19 pagesDr. Lamia El Wakeel, PhD. Lecturer of Clinical Pharmacy Ain Shams UniversitysamvetPas encore d'évaluation
- MS Review Exam 5Document10 pagesMS Review Exam 5Gian Karlo GarridoPas encore d'évaluation
- Delos Reyes - Grade 12 - EAPPDocument2 pagesDelos Reyes - Grade 12 - EAPPzavriaPas encore d'évaluation
- OCDDocument51 pagesOCDImon Paul100% (1)
- Guideline Rheumatic Disease in Children PDFDocument432 pagesGuideline Rheumatic Disease in Children PDFMada DobosPas encore d'évaluation
- Visi 71Document196 pagesVisi 71Khoa HữuPas encore d'évaluation
- Prevent Platelet Plugs.: Never IMDocument1 pagePrevent Platelet Plugs.: Never IMdekspeerPas encore d'évaluation
- Accident Reporting ProcedureDocument7 pagesAccident Reporting ProcedureDavid J CRPas encore d'évaluation
- Biology Investigatory Project Xii On Drug AddictionDocument18 pagesBiology Investigatory Project Xii On Drug AddictionKhalifa Shameer60% (5)
- Pakistan Journal of Pharmaceutical Sciences, 23 (4), 449-454 (2010)Document7 pagesPakistan Journal of Pharmaceutical Sciences, 23 (4), 449-454 (2010)Sam SonPas encore d'évaluation
- The Effects of Cigarette Smoking To The Health of Automotive Grade 11 and Grade 12 Students in Computer Reseacrh Network, INC Background of The StudyDocument9 pagesThe Effects of Cigarette Smoking To The Health of Automotive Grade 11 and Grade 12 Students in Computer Reseacrh Network, INC Background of The StudyRuel OrculloPas encore d'évaluation
- What Is Mental Health or Emotional HealthDocument5 pagesWhat Is Mental Health or Emotional HealthAl LanPas encore d'évaluation
- Momeopathy MM by TAfelDocument321 pagesMomeopathy MM by TAfelKrishan Kumar GargPas encore d'évaluation
- The Wrong Answer: by Harold D. Foster, PHD © 2003Document6 pagesThe Wrong Answer: by Harold D. Foster, PHD © 2003JOSH USHERPas encore d'évaluation
- The Frequency GenerationDocument67 pagesThe Frequency Generationjayjonbeach100% (5)
- Id MMD 2Document9 pagesId MMD 2Nashrah HusnaPas encore d'évaluation
- Basal GangliaDocument40 pagesBasal GangliaEnkefalos KardiaPas encore d'évaluation