Académique Documents
Professionnel Documents
Culture Documents
1 s2.0 S1388198114001036 Main
Transféré par
kasabeTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
1 s2.0 S1388198114001036 Main
Transféré par
kasabeDroits d'auteur :
Formats disponibles
Biochimica et Biophysica Acta 1841 (2014) 12921300
Contents lists available at ScienceDirect
Biochimica et Biophysica Acta
journal homepage: www.elsevier.com/locate/bbalip
Review
Role of free fatty acid receptors in the regulation of energy metabolism
Takafumi Hara a,, Daiji Kashihara a, Atsuhiko Ichimura c, Ikuo Kimura a,b, Gozoh Tsujimoto a, Akira Hirasawa a
a
b
c
Department of Pharmacogenomics, Graduate School of Pharmaceutical Sciences, Kyoto University, 46-29 Yoshida-Shimoadachi-cho, Sakyo-ku, Kyoto 606-8501, Japan
Department of Applied Biological Science, Graduate School of Agriculture, Tokyo University of Agriculture and Technology, Fuchu-Shi, Tokyo 183-5381, Japan
Department of Molecular Medicine and Therapy, Tohoku University Graduate School of Medicine, 2-1 Seiryo-cho, Aoba-ku, Sendai 980-8575, Japan
a r t i c l e
i n f o
Article history:
Received 5 November 2013
Received in revised form 26 May 2014
Accepted 2 June 2014
Available online 10 June 2014
Keywords:
G protein-coupled receptor
Free fatty acid receptor
Fatty acid
Energy metabolism
a b s t r a c t
Free fatty acids (FFAs) are energy-generating nutrients that act as signaling molecules in various cellular processes. Several orphan G protein-coupled receptors (GPCRs) that act as FFA receptors (FFARs) have been identied
and play important physiological roles in various diseases. FFA ligands are obtained from food sources and metabolites produced during digestion and lipase degradation of triglyceride stores. FFARs can be grouped according
to ligand proles, depending on the length of carbon chains of the FFAs. Medium- and long-chain FFAs activate
FFA1/GPR40 and FFA4/GPR120. Short-chain FFAs activate FFA2/GPR43 and FFA3/GPR41. However, only
medium-chain FFAs, and not long-chain FFAs, activate GPR84 receptor. A number of pharmacological and physiological studies have shown that these receptors are expressed in various tissues and are primarily involved in
energy metabolism. Because an impairment of these processes is a part of the pathology of obesity and type 2 diabetes, FFARs are considered as key therapeutic targets. Here, we reviewed recently published studies on the
physiological functions of these receptors, primarily focusing on energy homeostasis.
2014 Elsevier B.V. All rights reserved.
1. Introduction
Free fatty acids (FFAs) are essential nutrients that contribute to various cellular functions. Several epidemiological and physiological studies have examined the benecial or harmful effects of FFAs [1,2]. FFAs
exert biological effects through several signaling pathways; however,
the precise mechanisms remain unclear. FFAs are associated with intracellular and nuclear proteins such as FA-binding proteins and peroxisome proliferator-activated receptors (PPARs) [3,4]. Activation of G
protein-coupled receptors (GPCRs) by FFAs has been predicted because
some physiological functions of FFAs are difcult to describe. During the
past decade, several FFA receptors (FFARs) have been identied. Ligand
proles of FFARs depend on the length of the carbon chain of FFAs. Thus,
FFA2 and FFA3 receptors are activated by short-chain FFAs, whereas
FFA1 and FFA4 are activated by medium- and long-chain FFAs. In contrast, GPR84 is activated by medium-chain FFAs but not by long carbon
chains. Expression and functional studies of FFARs have shown that these
receptors are strongly associated with energy metabolism (Table 1).
Therefore, FFARs have received considerable attention as potential therapeutic targets for energy metabolism disorders such as obesity and type
2 diabetes. However, the ligand proles of short-chain and medium- to
long-chain FFA receptors are similar to each other, and the expression
proles of these receptors in pancreas, intestine, and immune cells partly
overlap. Therefore, the development of selective ligands (Fig. 1) and gene
Corresponding author at: Department of Pathology, Stanford University School of
Medicine, 300 Pasteur Drive, Lane 235, Stanford, CA 94305-5324, USA.
E-mail address: thara@stanford.edu (T. Hara).
http://dx.doi.org/10.1016/j.bbalip.2014.06.002
1388-1981/ 2014 Elsevier B.V. All rights reserved.
knockout studies would be essential to reveal the precise physiological
functions of these receptors. Particularly, in addition to the basic properties such as distribution, signaling pathways, and ligands, it is important
to focus on how these receptors are orchestrated in the whole body and
systemically contribute to the pathogenesis of disease, which in turn
might provide novel insights into therapeutic options. This review summarizes the crucial and basic properties previously reported, as well as
the recent advances in FFAR functions in relation to energy metabolism.
2. Short-chain FFAs (SCFAs)
SCFAs consisting of chains less than 6 carbons have various physiological functions. Acetate (C2), propionate (C3), and butyrate (C4) are
major products in the bacterial fermentation of dietary ber with gut
microbiota and are used as an energy source in epithelial cells of the intestinal tract and in the liver [5,6]. SCFAs are therefore considered as endogenous ligands for SCFA receptors expressed in the intestines. In
addition, the increase in the plasma levels of SCFAs from micromolar
to millimolar levels activates the expression of SCFA receptors in leukocytes and sympathetic nerves.
3. FFA3 (GPR41)
3.1. Ligands and signal transduction
Several research groups have characterized the pharmacology of
FFA3. Ligand screening showed that FFA3 is activated by SCFAs such as
propionate (C3), butyrate (C4), and valerate (C5) [7,8]. FFA3 activates
T. Hara et al. / Biochimica et Biophysica Acta 1841 (2014) 12921300
Table 1
Expression and functional proles of FFARs.
Expression
FFARs
Physiological functions of each FFAR
Pancreas
FFA1, FFA4
Intestine
FFA1, FFA2, FFA3,
FFA4
Adipocyte
FFA2, GPR84, FFA4
Sympathetic nerve
system
Immune cells
FFA3
Insulin secretion (FFA1), glucagon
secretion (FFA1)
GLP-1 and GIP secretion (FFA1,
FFA2, FFA3)
Intestinal motility (FFA2)
GLP-1 secretion (FFA4)
Adipogenesis, lipolysis (FFA2)
Adiponectin expression (GPR84)
Differentiation (FFA4)
Sympathetic activation
FFA2, GPR84, FFA4
Anti-inammatory
Neutrophil, eosinophil (FFA2)
Cytokine production
Monocyte, macrophage (GPR84)
Anti-inammatory
Macrophage (FFA4)
the [Ca2+]i response and the phosphorylation of extracellular signalregulated kinase (ERK)1/2, but inhibits cAMP production. Furthermore,
these responses are inhibited by pertussis toxin (PTX) treatment, suggesting that the regulation system is coupled to G(i/o) [9]. On the
other hand, several synthetic compounds have been also reported as
FFA3 agonists or antagonists. Arena Pharmaceuticals have described
the selective agonist (Compound 1) and antagonist (Compound 2) for
FFA3 [10]. Schmidt et al. also reported small carboxylic acids, including
the bulky structure of cyclopropane in the structure (Compound 3) that
showed a 100-fold selectivity for FFA3 against FFA2 [11].
3.2. Physiological functions
3.2.1. Intestine
FFA3 expression has been conrmed in several types of cells in the
intestines [1214]. Intestinal L-cells typically secrete peptides YY (PYY)
and GLP-1, which are gut hormones involved in energy homeostasis,
whereas the neurotensin-positive cells of the proximal colon express
FFA3 mRNA. PYY and GLP-1 secretion is reduced in the primary culture
of cells derived from FFA3 knockout (KO) mice [14]. The effects of another
synthetic compound designated as AR420626, that has the similar basic
structure of compound 1, on GLP-1 secretion from colonic crypt cultures
was conrmed by stimulation of FFA3 or FFA2 using specic synthetic ligands. AR420626 also showed the IP3 accumulation in COS-7 cells transiently expressing FFA3 [10,15]. FFA3 KO mice showed signicantly
lower body and fat pad weight and lower plasma leptin concentrations
than wild-type (WT) mice [16]. In contrast, the intestinal transit rate
and SCFA content in the feces of KO mice were higher than those in the
feces of WT mice. However, these differences between WT and FFA3 KO
mice have not been conrmed under germ-free conditions. Furthermore,
germ-free WT mice, but not FFA3 KO mice, were colonized by specic microbes and showed an increase in PYY levels. These results indicate that
the production of SCFAs by bacterial fermentation is essential for the activation of FFA3 function and that PYY modulation of gut motility is important for the absorption of SCFAs. Bellahcene et al. earlier conrmed the
phenotypic differences between male and female FFA3 KO mice [17].
The rate of energy expenditure and lean body mass in male KO mice supplemented with high-fat diet was lower than those in similarly treated
female KO mice. In addition, compared to female KO mice, body fat
mass and the plasma leptin and glucose levels were elevated in male
KO mice. These differences could be explained by the effect of sex hormones on the metabolic regulation in the central or peripheral nervous
systems and on the distribution of adipose tissues. Furthermore, chemokine and cytokine levels were increased by stimulation of intestinal
epithelial cells with SCFAs, and the recruitment of leukocytes and activation of effector T cells were induced [18]. In addition, the inammatory responses of KO mice were reduced compared to those of WT mice. The
1293
administration of 2,4,6-trinitrobenzene sulfonic acid (TNBS) in KO mice,
which induces acute inammatory responses, showed lower levels of cytokines such as IL-6 and IL-12, and lower levels of neutrophil inltration in
the colon. In a Citrobacter rodentium infection model that evaluates immune responses to bacterial pathogens, the clearance of pathogens from
the intestines was slower in FFA2 and FFA3 KO mice. The levels of IL-6
and neutrophil recruitment, as well as the frequencies of Th1 and Th17
cells were also reduced in the KO mice. These results indicate that SCFA
receptors are important for the regulation of the immune system of the
intestines such as the recruitment of leukocytes and cytokine production
via T-cell activation [18].
3.2.2. Nervous system
We have previously reported that the sympathetic ganglia abundantly express FFA3 mRNA in FFA3 WT [19]. Furthermore, because
tyrosine hydroxylase protein, which is the enzyme for catecholamine
production, and sympathetic nerve innervation were signicantly
lower in FFA3 KO mice than WT mice, FFA3 could be a critical molecule
for sympathetic nerve growth.
Propionate-induced elevation of heart rate and oxygen consumption
was blocked by propranolol (a -adrenergic receptor blocker) treatment but not by hexamethonium (a nicotinic acetylcholine receptor
blocker) treatment. These ndings suggested that propionate affects
sympathetic nerve system activity through FFA3 at the ganglion level.
In vitro studies of precise signaling mechanisms for sympathetic
nerve system activation through FFA3 have demonstrated that FFA3 activates GPLC -3ERK1/2 pathways, leading to the phosphorylation
of synapsin 2- at serine 426. Synapsins are a family of synaptic vesicleassociated proteins implicated in the secretion of neurotransmitters.
Therefore, propionate-activated FFA3 may promote noradrenalin release from sympathetic neurons and regulate energy expenditure.
However, FFA3 contributes to the suppression of energy expenditure
under fasting conditions. -hydroxybutyrate (-HB), a ketone body
produced in the liver during food deprivation, exhibits an inhibitory effect on ERK1/2 phosphorylation and cAMP production through FFA3.
This antagonistic effect has been conrmed in cultured sympathetic
neurons and in mice in vivo. Hence SCFAs produced by bacterial fermentation under fed conditions activate FFA3, leading to an increase
in energy expenditure. In contrast, the ketone body -HB produced
under fasting conditions inhibits FFA3 signaling, suppressing energy expenditure [19,20].
Recently, a transgenic mouse study using monomeric red uorescent protein as the reporter for FFA3 revealed that FFA3 is expressed
in neuronal cells of the submucosal and myenteric ganglia [15]. Pluznick
et al. reported that Olfr78 and FFA3 are expressed in smooth muscle
cells of small resistance vessels. Interestingly, modulation of blood pressure was observed in both Olfr78 and FFA3 KO mice under antibiotic
treatment that causes the reduction of SCFAs derived from the gut microbiota fermentation. Thus, we should consider Olfr78 as the novel
type of SCFAR with the therapeutic potential for and on the novel mechanisms for blood pressure modulation via SCFARs including Olfr78 [21].
To elucidate the precise mechanism of FFA3 in the nerve, conditional KO
mice or specic ligands to discriminate FFA3 expressed in the nerve and
other tissues are required.
4. FFA2 (GPR43)
4.1. Ligands and signal transduction
In 2003, FFA2 was identied as a receptor for SCFAs. During the ligand screening using bioactive compounds in Ca2+ assays, the authors
reported that FFA2 was activated by acetate in transfected cells [8,22].
In vitro, FFA2 is also activated by other SCFAs such as formate (C1), propionate (C3), butyrate (C4), and pentanoate (C5). The potencies of FFA2
activation can range in the following order: C2 = C3 N C4 N other SCFAs
[7,8]. In G protein signaling, FFA2 displays dual coupling through the
1294
T. Hara et al. / Biochimica et Biophysica Acta 1841 (2014) 12921300
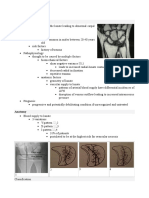
Fig. 1. Chemical structures of synthetic FFARs ligands.
T. Hara et al. / Biochimica et Biophysica Acta 1841 (2014) 12921300
pertussis toxin-sensitive Gi/o and Gq/11 protein [5]. The stimulation of
FFA2 by SCFAs results in the inhibition of cAMP production and activation of the ERK cascade by interactions with the Gi/o family of G proteins
and causes the elevation of [Ca2+]i and activation of the ERK cascade by
interactions with the G q family of G proteins. However, the physiological signicance of this dual-coupled signaling mechanism
through FFA2 remains unclear. On the other hand, the recruitment
of -arrestin 2 induced with the agonist stimulation was conrmed
by bioluminescence resonance energy transfer (BRET)-based approach
using HEK293 cells co-transfected with eYFP-tagged FFA2 and
-arrestin 2-Renilla luciferase [23,24].
Structure-activity relationship (SAR) of FFA2 and FFA3 ligands
was examined in detail and several selective ligands that showed a
10100-fold selectivity for FFA2 compared to FFA3 were characterized
based on the results of the analysis. The SAR analysis successfully provided a general rule to predict the selectivity of ligands to either FFA2
or FFA3. The ligand that has small carboxylic acid with sp2-hybridized
-carbon showed selectivity for FFA2. On the other hand, the small carboxylic acid with sp3-hybridized -carbon showed selectivity for FFA3
[11,25]. In addition, several selective agonists and antagonists have
been reported as patent compounds [10,2528]. Lee et al. reported
that phenylacetamide 1 and 2 are allosteric agonists of FFA2. Compounds 4 and 5 that showed agonistic activity increased glucose uptake
in 3T3-L1 and GLP-1 secretion in NCI-H716 cells, respectively. On the
other hand, Compounds 6 and 7 showed inhibitory effects to FFA2.
The IC 50 values of these two compounds were 20 and 100 nM,
respectively.
4.2. Physiological functions
The evidence of FFA2 expression in adipose and gastrointestinal
tissues suggests that FFA2 may be involved in energy regulation [29].
RT-PCR analysis of mouse tissues has shown that FFA2 is expressed in
the white adipose tissues (WATs) and gastrointestinal tissues [30]. In
the intestine, FFA2 may be implicated in appetite regulation because
FFA2 mRNA is expressed in both rat and human ileum and colon [31,
32]. In contrast, in adipose tissues, FFA2 may be associated with obesity
and energy accumulation because FFA2 mRNA is expressed in WATs
such as subcutaneous, perirenal, and epididymal tissues in 3T3-L1derived adipocytes, and in mature adipocytes [30]. Furthermore, FFA2
is abundantly expressed in immune-related tissues such as the spleen
and bone marrow [32].
4.2.1. Intestine
The intestines are very important in energy homeostasis because it is associated with the secretion of gut hormones, appetite
control, and absorption of nutrients [3337]. Karaki et al. reported that
FFA2-expressing cells completely co-localize with PYY-expressing
enteroendocrine L-cells of the rat gastrointestinal tract by immunohistochemistry analysis using FFA2 antibody. Enteroendocrine L-cells are
also one of the major cell groups expressing the proglucagon gene,
producing GLP-1 and GLP-2. GLP-1 and GLP-2 are co-stored and cosecreted with PYY by enteroendocrine L-cells [38]. It has been reported
that SCFAs, through FFA2, trigger the secretion of GLP-1 from mixed colonic cultures in vitro [39]. FFA2-mediated GLP-1 secretion in STC-1
cells that endogenously express FFA2 was also demonstrated by using
an FFA2 selective agonist [23]. FFA2 or FFA3 KO mice show reduced
SCFAs-triggered GLP-1 secretion in vitro and in vivo and impaired glucose tolerance. A qRT-PCR study has shown that FFA2 and FFA3 are
abundantly expressed in GLP-1-secreting L-cells, and SCFAs elevate cytosolic Ca2+ levels through G q signaling pathways in L-cells in primary culture. Therefore, these receptors have a substantial potential for
dietary or pharmacological manipulation to increase satiety and could
help in the treatment of obesity. In addition, these molecules may be
useful to potentiate insulin secretion by using incretins such as GLP-1
in patients with type 2 diabetes. The anorexigenic neural circuits
1295
working through PYY and GLP-1 could be activated to reduce food intake, increase energy expenditure, and restore the neutral energy
balance. Hence, regulation of PYY and GLP-1 secretion through FFA2
controls energy intake and may be therefore utilized in the treatment
of metabolic disorders such as obesity and metabolic syndrome.
4.2.2. Adipose tissues
Adipose tissues are also related to energy homeostasis and energy
accumulation. Based on the FFA2 expression in adipose tissues and adipocytes, Hong et al. performed a series of studies to elucidate the role of
FFA2 in adipocytes [30]. They showed that the level of expression of
FFA2 in WATs of obesity-induced mice fed on a high-fat diet was significantly higher than that in WAT of normal chow-fed mice. In 3T3-L1
cells, after adipogenesis, FFA2 and Pparg2 (a marker of mature adipocytes) mRNA expression levels increased with SCFA treatment. Suppression of FFA2 mRNA by RNA interference inhibited adipogenesis in
3T3-L1 cells. Moreover, in 3T3-L1-derived adipocytes, SCFAs suppressed
isoproterenol-induced lipolysis in a dose-dependent manner [30]. Using
FFA2 KO mice, Ge et al. demonstrated that these effects are mediated
by FFA2 [40]. Moreover, it has been reported that acetate dosedependently suppresses lipolysis and release of glycerol in adipocytes isolated from WT mice in vitro, and activation of FFA2 by intraperitoneal injection of sodium acetate instantly reduces plasma fatty
acid in vivo, whereas these effects are abolished in FFA2 KO mice [40].
Recent evidence suggests that the gut microbiota affects host nutrient
acquisition and energy regulation and is related to obesity, insulin resistance, and diabetes in the host [4146]. During feeding, SCFAs, ligands
for FFA2, are produced by gut microbial fermentation of dietary ber.
Hence, the relation between gut microbiota and systemic energy regulation by adipose FFA2 using FFA2-modied and germ-free mice was examined [47]. A series of in vitro and in vivo studies with FFA2 KO mice
and mice overexpressing adipose-specic FFA2 showed that acetate potently inhibits fat accumulation by suppressing insulin signaling in
WATs. Furthermore, in germ-free and antibiotic-treated mice, SCFAs
provided by gut microbiota primarily act as activator ligands of FFA2.
FFA2-mediated suppression of insulin signaling in adipocytes is not mediated by cAMP inhibition, rather it involves G of Gi/o protein family
but not Gq. As SCFA levels reect the nutrients supplied under normal
feeding conditions, they appear to control energy balance by modulating fat accumulation. This may be achieved by regulating FFA2mediated insulin signaling in the adipose tissue. The FFA2insulin
pathway in the adipose tissue may be one of the important physiological mechanisms for these metabolic fuels to regulate the body
energy balance.
4.2.3. Immune cells
In 2009, Maslowski et al. reported that FFA2 stimulated with SCFAs
regulated immune responses [32]. The expression of FFA2 in neutrophils and eosinophils was observed. FFA2 KO mice exhibited the deterioration of inammatory condition in arthritis, colitis, and asthma
models. In addition, germ-free mice with almost abolished SCFAs derived
from gut fermentation showed an impairment of inammatory responses. The increase in the recruitment of immune cells and of inammatory mediators was also observed in the KO mice with inammatory
conditions. Masui et al. showed that dextran sulfate sodium treatmentinduced colitis model in FFA2 KO mice showed a potent inammatory
condition compared to that in WT mice. The acetate treatment of this colitis model showed an improvement of disease activity in WT mice but
not in FFA2KO mice [48]. Sina et al. also showed the importance of
FFA2 on leukocyte migration and cytokine secretion in an inammatory
model. FFA2 KO mice exhibited reduced migration of leukocytes in the
intestines compared to WT mice. However, this effect was abolished in
sterile model mice that produced less SCFAs [49]. Hence, these reports
indicate that FFA2 has a potential therapeutic relevance for the treatment
of metabolic and inammatory disorders in obesity and type 2 diabetes.
1296
T. Hara et al. / Biochimica et Biophysica Acta 1841 (2014) 12921300
5. Medium- to long-chain fatty acids
Medium- to long-chain fatty acids impart a wide range of physiological effects. Medium-chain and long-chain fatty acids have 612 carbons
and N12 carbons, respectively. As the energy source, these fatty acids
are supplied primarily by food intake, biosynthesis, and lipolysis from
adipose tissues. However, as unsaturated fatty acids such as linoleic
acid, linolenic acid, and DHA that have more than 2 double bonds in
the structures were not provided by biosynthesis in humans, we need
to derive these macromolecules from food. Medium- to long-chain
fatty acids are metabolized by -oxidation and used as an energy source
in various tissues. On the other hand, fatty acid receptors that are activated by these fatty acids provided the novel possibility of the biological
functions of fatty acids for signaling molecules and the insight for the
importance of dietary habits.
6. Medium- to long-chain fatty acid receptors
6.1. GPR84
6.1.1. Ligands and signal transduction
GPR84 has been identied as a physiological receptor for mediumchain FFAs (C9C14; MCFAs) [50]. A synthetic agonist, diindolylmethane,
has been also developed, and the potency of this compound is greater
than that of MCFA ligands. It has been reported that MCFAs with the hydroxyl group at the 2- or 3-position in the structure potently affect the
chemotaxis of human polymorphonuclear leukocytes (PMNs) compared
with MCFAs without the hydroxyl group [51]. This chemotaxis effect is
inhibited by treatment with PTX, suggesting that GPR84 is coupled to
the Gi/o protein. Galapagos NV developed the synthetic GPR84 antagonist
dihydropyrimidinoisoquinolinone derivatives. These compounds might
be useful for the further characterization of GPR84 and for the treatment
of inammatory diseases [52].
6.1.2. Physiological function
GPR84 is highly expressed in leukocytes and adipocytes. In LPStreated mice, the expression level of GPR84 is signicantly elevated in
monocytes and macrophages (including glial cells). GPR84 stimulation
increases LPS-induced IL12p40 levels and enhances IL-8 and TNF- production in monocytes/macrophages and PMNs, respectively [50,52]. Although GPR84 KO mice do not exhibit any change in the proliferation of
B and T cells, Th2 cytokine production in the KO mice is increased [53].
In 3T3-L1 adipocytes, the expression level of GPR84 increases when the
cells are cultured with macrophages. The expression level of adiponectin
mRNA was also reduced by the stimulation with MCFAs in the presence of
TNF- [54]. In obesity and type 2 diabetes, concomitant with inammatory responses, immune cells such as macrophages and dendritic cells
inltrate the adipocytes and promote inammation by increasing the
secretion of cytokines. Considering that GPR84 binds to MCFAs and
that GPR84 is specically expressed in leukocytes, GPR84 might have
a function that links fatty acid metabolism and the immune system.
7. FFA4 (GPR120)
7.1. Ligands and signal transduction
We have previously isolated the FFA4 gene from genomic DNA.
Using a receptor internalization assay, we identied medium- to longchain FFAs (including saturated FFAs (C1418) and polyunsaturated
FFAs (PUFAs; C1622)) as the endogenous ligands of FFA4 [55]. The ligand proles were similar to those for FFA1; however, the amino acid
homology between FFA4 and FFA1 was only 10%. To identify other natural ligands of FFA4, we screened a series of natural compounds derived
from fruiting bodies of Albatrellus ovinus and found a selective partial
agonist grifolic acid [56]. In addition, we synthesized a series of compounds containing carboxylic acids on the basis of the structure of
PPAR-agonist thiazolidinediones and developed a selective agonist,
NCG21, using a homology model of FFA4 [51,57]. These compounds
might be useful for monitoring the physiological effects of FFA4. Furthermore, they may help in the development of novel drug candidates
for the treatment of type 2 diabetes, obesity, and metabolic diseases.
The synthetic agonist TUG-891 was developed, which showed a
nanomolar order potency to FFA4. TUG-891 activates calcium and
ERK1/2 responses and -arrestin recruitment. In addition, the biological
effect of TUG-891 on glucose uptake in 3T3-L1 derived adipocytes, GLP1 secretion in STC-1 cells, and anti-inammatory effects in macrophages
have also been conrmed [58,59]. On the other hand, Banyu Pharmaceutical Co., Ltd. developed the Isoindolin-1-one series and Phenylisoxazol-3-ol series, which showed nanomole order potency for FFA4,
but not for FFA1 [60,61]. Metabolex was developed as selective agonist
of FFA4 and the pharmacological properties were examined not only in
cultured cells but also in animal models [62]. PUFAs and synthetic ligands induce a rise in cytosolic free Ca2+ levels in HEK293 cells overexpressing FFA4, suggesting that FFA4 is coupled with the G q protein
family. FFA4 can also activate ERK1/2 under certain conditions and activates PI3-kinase and the serine/threonine protein kinase Akt in FFA4expressing cells [56,63]. Recently, Shah et al. showed that PUFAinduced depolarization induced by monovalent cation-specic transient
receptor potential channel type M5 (TRPM5) is related to intracellular
calcium increase and cholecystokinin (CCK) secretion in STC-1 cells
[64]. These observations suggest that TRPM5 plays a crucial role
in FFA4 signaling in STC-1 cells. Oh et al. reported that -3 FFAs,
docosahexaenoic acid (DHA), and eicosapentaenoic acid (EPA) inhibit
the phosphorylation of TGF--activated kinase 1 (TAK1). This kinase
is associated with toll-like receptor (TLR), tumor necrosis factor-
(TNF-), and inammatory pathways through FFA4--arrestin signaling [65]. The long (L) and short (S) form of FFA4 were identied as
splice variants of an insertion of 16 amino acids. Watson et al. examined
the differences in the signaling pathway of these two isoforms. The
FFA4S form showed calcium response and -arrestin 2 recruitment
with agonist stimulation; however, the FFA4L form showed only
-arrestin 2 recruitment and not calcium response [66].
7.2. Physiological function
We recently reported that dysfunctional FFA4 leads to obesity in
both mice and humans [67]. We found that FFA4-decient mice fed on
a high-fat diet develop obesity, glucose intolerance, and fatty liver
with decreased adipocyte differentiation and lipogenesis and enhanced
hepatic lipogenesis. Insulin resistance in these mice is associated with
reduced insulin signaling and enhanced inammation in adipose tissue.
FFA4 exon sequencing in obese subjects revealed a deleterious nonsynonymous mutation (p.R270H) that inhibits FFA4 signaling activity.
Furthermore, the p.R270H variant increases the risk of obesity in
European populations. In the FFA4S form, this variant would be identical
to the p.R254H. However, the effect of this variant on FFA4 signaling has
not been examined in detail yet. Oh et al. showed that the FFA4 agonist
exerts anti-inammatory effects through -arrestin signaling in monocytic RAW264.7 cells and primary macrophages [65]. In addition, DHAmodulated, LPS-induced cyclooxygenase-2 (COX-2) in RAW164.7 cells
is mediated by FFA4 signaling. The effect of DHA on COX-2 expression
is inhibited by siRNA for FFA4 and -arrestin but not for G q/11 and
the treatment of inhibitors of eicosanoid metabolism [68]. Endogenous
expression of FFA4 has also been found in the intestines of humans
and mice. Our previous study showed that FFA4-expressing cells are located in GLP-1-expressing enteroendocrine cells in the large intestine
[69]. These reports persuaded us to speculate the physiological effect
of FFA4 on incretin secretion in vivo.
Endogenous expression of FFA4 also occurs in other cells and tissues.
Oh et al. reported on the endogenous expression of FFA4 in monocytic
RAW 264.7 cells and in primary proinammatory M1-like macrophages
[56]. Matsumura et al. determined the expression of FFA4 in taste buds
T. Hara et al. / Biochimica et Biophysica Acta 1841 (2014) 12921300
[70]. We found that in the lungs, FFA4 protein is co-localized with the
Clara cell, which is a 10-kDa marker [71]. Further studies are needed
to determine the physiological function of FFA4 in the lungs. In 2012,
Taneera et al. used a systems genomics approach to identify genes for
type 2 diabetes, and FFA4 was placed in the top 20 of the ranked list
[72]. In this report, FFA4 expression levels in human pancreatic islets
were found to be positively correlated with insulin secretion, insulin
content, and lower HbA1c levels, suggesting that FFA4 may protect
human pancreatic islets from lipotoxicity.
8. FFA1 (GPR40)
8.1. Ligands and signal transduction
Three independent groups almost simultaneously deorphanized and
characterized FFA1 as a receptor for medium- to long-chain FFAs, but
not for SCFAs [7375]. These reports demonstrated that various FFAs activate FFA1 at the micromolar concentration range and promote insulin
secretion in pancreatic -cells. FFA1 stimulation promotes the release of
[Ca2+]i and ERK1/2 phosphorylation in transiently and stably expressing FFA1 cells and in MIN6 and primary pancreatic -cells [76]. Thus,
FFA1 could be coupled to a G-protein -subunit of the G q family
[77]. We have previously mentioned a potential discrepancy between
agonist-induced intracellular signaling (ERK1/2 or [Ca2+]i responses)
and the effects on insulin secretion. The selective agonists NCG75,
GW9508, and TAK-875 have been described as potent agonists compared to the endogenous ligands of FFA1. However, the effects of these
synthetic compounds on insulin secretion in INS-1 and MIN6 cells are
similar to those of endogenous ligands [7880]. Several studies have
shown that multiple pathways ([Ca2+]i and ERK) contribute to insulin
secretion [8183]. Therefore, FFAs could promote insulin secretion
through FFA1 and other signaling pathways. In 2012, oleate-induced
GSIS was shown to be mediated in a FFA1-dependent manner and
caused rapid F-actin remodeling. Protein kinase D (PKD) phosphorylation was also observed in WT but not in FFA1-null mice. Hence, these
results demonstrate that the signaling pathways leading to insulin secretion in pancreatic islets could be involved in F-actin depolymerization
and PKD1 activation [84].
Lin et al. reported that there are three allosterically linked binding
sites on FFA1 and their synthetic compounds could have different activation mechanisms interacting with these different binding sites. The
full and partial agonists (AMG1638 and AMG837, respectively) were
considered to exhibit positive functional cooperativity. In addition, the
synthetic agonists showed either negative or neutral cooperativity to
endogenous ligands [85]. These ndings might be important for further
ligand development of FFA1.
8.2. Physiological function
8.2.1. Pancreatic -cells
A number of studies have demonstrated the important physiological
roles of FFA1 in the pancreas. FFA-induced acute and chronic effects on
the pancreas are partly mediated by FFA1 and are considered to be associated with the increase in GSIS and -cell dysfunction, respectively
[86]. The FFA-induced GSIS that is considered as an acute effect of FFA
on pancreatic -cells was signicantly decreased by FFA1 loss of function. The chronic exposure of -cell to elevated FFAs resulted in -cell
dysfunction known as glucolipotoxicity. Transgenic overexpression of
the human FFA1 gene in mouse pancreatic -cells under the control of
mouse insulin II promoter prevented the development of hyperglycemia in high fat diet-fed mice and improved insulin secretion and glucose
tolerance in genetically diabetic mice [87]. The FFA1-mediated acute
and chronic effects of palmitate on insulin secretion have also been conrmed [88]. In contrast, transgenic overexpression of FFA1 under the
promoter of PDX-1 showed impairment of -cell function. Therefore,
the precise mechanisms of FFA1 on glucolipotoxicity of pancreatic
1297
-cell remain controversial. As the expression level of FFA1 on -cells
was reduced in type 2 diabetes patients and the administration of
FFA1 synthetic compounds to diabetic rats showed improvement of
the disease condition [89], chronic activation of FFA1 might provide
benecial effects on glucose metabolism. In addition, Jain et al., reported
the effect of chronic activation of Gq signaling selectively in mice pancreatic -cells using Gq coupled designer GPCR. The mice showed
lower blood glucose level, increased insulin content and prevented diabetes in sutoreptozotosin-induced diabetic symptoms [90]. On the
other hand, the result of the clinical trial of synthetic FFA1 agonist
TAK-875 showed the concerns about liver safety. Although it still remains unclear whether this phenomena is related to the FFA1 or other
signaling pathways, and to the physiological function of other tissues
that express FFA1 such as the intestine and stomach, we should carefully examine the chronic effect of FFA1 stimulation not only in pancreatic
-cells but also in other tissues in detail.
8.2.2. Pancreatic -cells
Flodgren et al. previously described the colocalization of glucagon
and FFA1. Furthermore, overexpression of FFA1 in a glucagon-secreting
cell line has been shown to promote FFA-induced glucagon production
[91]. Conversely, knockdown of FFA1 in mouse islets abolishes glucagon
secretion in response to FFAs. Another group reported that FFA1dependent FFA-induced secretion of glucagon from isolated islets requires PLC-mediated [Ca2+]i [92]. Consistent with these in vitro studies,
gene deletion of FFA1 in mice showed signicantly less glucagon secretion in response to increased circulating FFA levels compared to WT
mice [93]. However, FFA1 expression in glucagon-positive pancreatic
cells has been under intense debate.
8.2.3. Intestine
FFA1 is expressed in intestinal enteroendocrine cells and possibly
also in glucagon-producing cells, which are associated with glucose homeostasis [9496]. It may be important to investigate the precise physiological functions of FFA1 in these tissues to predict potential side
effects of FFA1-based drugs. Edfalk et al. reported that intestinal L and
K cells expressing incretin hormones GLP-1 and GIP, respectively, express FFA1 [96]. In addition, FFA1 expression has been detected in intestinal I cells secreting CCK. Hence, FFAs appear to mediate insulin
secretion directly (by activating FFA1 expression in -cells) and indirectly (by releasing incretin) because FFA1 mediates FFA-induced
incretin secretion.
9. Conclusion
Several metabolic response pathways in relation to nutrient sensing
systems have been reported. Among these reports, the recent researches provide the evidences that FFARs expressed on both metabolic
tissues and immune cells act as dietary sensors regulating not only energy metabolism but also inammatory responses. In terms of the inammatory response in metabolic disorders such as obesity and type
2 diabetes, chronic inammatory responses are considered crucial
mechanisms related to the disease progression. Particularly, cytokine
production that was partly regulated by FFA2 and FFA4 expressed in
leukocytes and macrophages, respectively, might be involved in insulin
resistance and further immune response such as migration of immune
cells. In addition, several reports have shown that the production and
secretion of several incretin hormones are denitely regulated by
FFARs. Therefore, to understand the precise mechanisms of FFARs not
only in metabolic tissues but also in immune cells provides the novel aspects of the therapeutic treatment of metabolic disorders. On the other
hand, a number of questions remain unanswered: i) What is the relative
contribution of each FFAR to energy metabolism both in healthy and
disease conditions? A systems biological approach might be useful in
quantifying the contribution of each FFAR to energy metabolism of the
entire body. ii) What is the relationship between signaling pathways
1298
T. Hara et al. / Biochimica et Biophysica Acta 1841 (2014) 12921300
and physiological functions? The G-protein- or -arrestin-dependent
pathways have been reported; however, which signals are connected
to specic physiological functions of FFARs remains unclear. iii) Does
chronic stimulation of FFARs cause any adverse effect? In obesity or
type 2 diabetes, the level of FFAs in plasma might be constantly high.
These conditions might cause the down-regulation of FFARs not only
in the mRNA but also at the protein level. A similar situation might
occur when the selective agonist or antagonist for FFARs is repeatedly
administered. iv) The synthetic ligands that can activate or inhibit the
specic signal pathways, termed biased ligands, should be developed
for further pharmacological characterization. As the common physiological functions of FFARs are conclusively related to the regulation of
energy metabolism, it is important to consider the function of each
FFAR as an integrated metabolic system. Further extensive investigations will answer these questions and signicantly enhance the potential of FFARs in therapeutics.
Acknowledgment
This work was supported by JSPS KAKENHI grant numbers 24790249
and 26860054.
References
[1] E.P. Haber, H.M.A. Ximenes, J. Procpio, C.R.O. Carvalho, R. Curi, A.R. Carpinelli, Pleiotropic effects of fatty acids on pancreatic beta-cells, J. Cell. Physiol. 194 (2003) 112.
[2] E.A. Nunez, Biological complexity is under the strange attraction of non-esteried
fatty acids, Prostaglandins Leukot. Essent. Fatty Acids 57 (1997) 107110.
[3] J.F. Glatz, G.J. van der Vusse, Cellular fatty acid-binding proteins: their function and
physiological signicance, Prog. Lipid Res. 35 (1996) 243282.
[4] A. Chawla, J.J. Repa, R.M. Evans, D.J. Mangelsdorf, Nuclear receptors and lipid
physiology: opening the X-les, Science 294 (2001) 18661870.
[5] A. Andoh, T. Tsujikawa, Y. Fujiyama, Role of dietary ber and short-chain fatty acids
in the colon, Curr. Pharm. Des. 9 (2003) 347358.
[6] J.M.W. Wong, R. de Souza, C.W.C. Kendall, A. Emam, D.J.A. Jenkins, Colonic
health: fermentation and short chain fatty acids, J. Clin. Gastroenterol. 40
(2006) 235243.
[7] E. Le Poul, C. Loison, S. Struyf, J.-Y. Springael, V. Lannoy, M.-E. Decobecq, S. Brezillon,
V. Dupriez, G. Vassart, J. Van Damme, M. Parmentier, M. Detheux, Functional characterization of human receptors for short chain fatty acids and their role in polymorphonuclear cell activation, J. Biol. Chem. 278 (2003) 2548125489.
[8] A.J. Brown, S.M. Goldsworthy, A.A. Barnes, M.M. Eilert, L. Tcheang, D. Daniels, A.I.
Muir, M.J. Wigglesworth, I. Kinghorn, N.J. Fraser, N.B. Pike, J.C. Strum, K.M.
Steplewski, P.R. Murdock, J.C. Holder, F.H. Marshall, P.G. Szekeres, S. Wilson, D.M.
Ignar, S.M. Foord, et al., The Orphan G protein-coupled receptors GPR41 and
GPR43 are activated by propionate and other short chain carboxylic acids, J. Biol.
Chem. 278 (2003) 1131211319.
[9] Y. Xiong, N. Miyamoto, K. Shibata, M.A. Valasek, T. Motoike, R.M. Kedzierski, M.
Yanagisawa, Short-chain fatty acids stimulate leptin production in adipocytes
through the G protein-coupled receptor GPR41, Proc. Natl. Acad. Sci. U. S. A. 101
(2004) 10451050.
[10] Leonard, Gpr41 and modulators thereof for the treatment of insulin-related disorders, 2008.
[11] J. Schmidt, N.J. Smith, E. Christiansen, I.G. Tikhonova, M. Grundmann, B.D. Hudson, R.
J. Ward, C. Drewke, G. Milligan, E. Kostenis, T. Ulven, Selective orthosteric free fatty
acid receptor 2 (FFA2) agonists: identication of the structural and chemical requirements for selective activation of FFA2 versus FFA3, J. Biol. Chem. 286 (2011)
1062810640.
[12] H. Tazoe, Y. Otomo, I. Kaji, R. Tanaka, S.-I. Karaki, A. Kuwahara, Roles of short-chain
fatty acids receptors, GPR41 and GPR43 on colonic functions, J. Physiol. Pharmacol.
59 (Suppl. 2) (2008) 251262.
[13] H. Tazoe, Y. Otomo, S.-I. Karaki, I. Kato, Y. Fukami, M. Terasaki, A. Kuwahara, Expression of short-chain fatty acid receptor GPR41 in the human colon, Biomed. Res. 30
(2009) 149156.
[14] B.S. Samuel, A. Shaito, T. Motoike, F.E. Rey, F. Backhed, J.K. Manchester, R.E.
Hammer, S.C. Williams, J. Crowley, M. Yanagisawa, J.I. Gordon, Effects of the
gut microbiota on host adiposity are modulated by the short-chain fatty-acid
binding G protein-coupled receptor, Gpr41, Proc. Natl. Acad. Sci. U. S. A. 105
(2008) 1676716772.
[15] M.K. Nhr, M.H. Pedersen, A. Gille, K.L. Egerod, M.S. Engelstoft, A.S. Husted, R.M.
Sichlau, K.V. Grunddal, S. Seier Poulsen, S. Han, R.M. Jones, S. Offermanns, T.W.
Schwartz, GPR41/FFAR3 and GPR43/FFAR2 as cosensors for short-chain fatty acids
in enteroendocrine cells vs FFAR3 in enteric neurons and FFAR2 in enteric leukocytes, Endocrinology 154 (2013) 35523564.
[16] M.S. Zaibi, C.J. Stocker, J. O'Dowd, A. Davies, M. Bellahcene, M.A. Cawthorne, A.J.H.
Brown, D.M. Smith, J.R.S. Arch, Roles of GPR41 and GPR43 in leptin secretory responses of murine adipocytes to short chain fatty acids, FEBS Lett. 584 (2010)
23812386.
[17] M. Bellahcene, J.F. O'Dowd, E.T. Wargent, M.S. Zaibi, D.C. Hislop, R.A. Ngala, D.M.
Smith, M.A. Cawthorne, C.J. Stocker, J.R.S. Arch, Male mice that lack the G-proteincoupled receptor GPR41 have low energy expenditure and increased body fat content, Br. J. Nutr. 109 (2013) 17551764.
[18] M.H. Kim, S.G. Kang, J.H. Park, M. Yanagisawa, C.H. Kim, Short-chain fatty acids activate GPR41 and GPR43 on intestinal epithelial cells to promote inammatory responses in mice, Gastroenterology 145 (2013) 396406.
[19] I. Kimura, D. Inoue, T. Maeda, T. Hara, A. Ichimura, S. Miyauchi, M. Kobayashi, A.
Hirasawa, G. Tsujimoto, Short-chain fatty acids and ketones directly regulate sympathetic nervous system via G protein-coupled receptor 41 (GPR41), Proc. Natl.
Acad. Sci. U. S. A. 108 (2011) 80308035.
[20] D. Inoue, I. Kimura, M. Wakabayashi, H. Tsumoto, K. Ozawa, T. Hara, Y. Takei, A.
Hirasawa, Y. Ishihama, G. Tsujimoto, Short-chain fatty acid receptor GPR41mediated activation of sympathetic neurons involves synapsin 2b phosphorylation,
FEBS Lett. 586 (2012) 15471554.
[21] J.L. Pluznick, R.J. Protzko, H. Gevorgyan, Z. Peterlin, A. Sipos, J. Han, I. Brunet, L.-X.
Wan, F. Rey, T. Wang, S.J. Firestein, M. Yanagisawa, J.I. Gordon, A. Eichmann, J.
Peti-Peterdi, M.J. Caplan, Olfactory receptor responding to gut microbiota-derived
signals plays a role in renin secretion and blood pressure regulation, Proc. Natl.
Acad. Sci. U. S. A. 110 (2013) 44104415.
[22] T. Nakamura, S. Shiojima, Y. Hirai, T. Iwama, N. Tsuruzoe, A. Hirasawa, S. Katsuma, G.
Tsujimoto, Temporal gene expression changes during adipogenesis in human mesenchymal stem cells, Biochem. Biophys. Res. Commun. (2003) 306312.
[23] B.D. Hudson, M.E. Due-Hansen, E. Christiansen, A.M. Hansen, A.E. Mackenzie, H.
Murdoch, S.K. Pandey, R.J. Ward, R. Marquez, I.G. Tikhonova, T. Ulven, G. Milligan,
Dening the molecular basis for the rst potent and selective orthosteric agonists
of the FFA2 free fatty acid receptor, J. Biol. Chem. 288 (2013) 1729617312.
[24] B.D. Hudson, E. Christiansen, I.G. Tikhonova, M. Grundmann, E. Kostenis, D.R. Adams,
T. Ulven, G. Milligan, Chemically engineering ligand selectivity at the free fatty acid
receptor 2 based on pharmacological variation between species orthologs, FASEB J.
26 (2012) 49514965.
[25] T. Lee, R. Schwandner, G. Swaminath, J. Weiszmann, M. Cardozo, J. Greenberg, P.
Jaeckel, H. Ge, Y. Wang, X. Jiao, J. Liu, F. Kayser, H. Tian, Y. Li, Identication and functional characterization of allosteric agonists for the G protein-coupled receptor
FFA2, Mol. Pharmacol. 74 (2008) 15991609.
[26] T. Ulven, Short-chain free fatty acid receptors FFA2/GPR43 and FFA3/GPR41 as new
potential therapeutic targets, Front. Endocrinol. 3 (2012) 111.
[27] L. Sanire, M. Pizzonero, N. Triballeau, N. Vandeghinste, S. De Vos, R. Brys, C.
Pourbaix-L'ebraly, Azetidine Derivatives Useful for the Treatment of Metabolic and
Inammatory Diseases, 2012. (WO/2012/098033).
[28] H. Hoveyda, C.E. Brantis, G. Dutheuil, L. Zoute, D. Schils, J. Bernard, Compounds,
Pharmaceutical Composition and Methods for Use in Treating Metabolic Disorders,
2010. (WO/2010/066682).
[29] M.L. Sleeth, E.L. Thompson, H.E. Ford, S.E.K. Zac-Varghese, G. Frost, Free fatty acid receptor 2 and nutrient sensing: a proposed role for bre, fermentable carbohydrates
and short-chain fatty acids in appetite regulation, Nutr. Res. Rev. 23 (2010)
135145.
[30] Y.-H. Hong, Y. Nishimura, D. Hishikawa, H. Tsuzuki, H. Miyahara, C. Gotoh, K.-C. Choi,
D.D. Feng, C. Chen, H.-G. Lee, K. Katoh, S.-G. Roh, S. Sasaki, Acetate and propionate
short chain fatty acids stimulate adipogenesis via GPCR43, Endocrinology 146
(2005) 50925099.
[31] S. Karaki, R. Mitsui, H. Hayashi, I. Kato, H. Sugiya, T. Iwanaga, J.B. Furness, A.
Kuwahara, Short-chain fatty acid receptor, GPR43, is expressed by enteroendocrine
cells and mucosal mast cells in rat intestine, Cell Tissue Res. 324 (2006) 353360.
[32] K.M. Maslowski, A.T. Vieira, A. Ng, J. Kranich, F. Sierro, D. Yu, H.C. Schilter, M.S. Rolph,
F. Mackay, D. Artis, R.J. Xavier, M.M. Teixeira, C.R. Mackay, Regulation of inammatory responses by gut microbiota and chemoattractant receptor GPR43, Nature 461
(2009) 12821286.
[33] R.L. Batterham, M.A. Cowley, C.J. Small, H. Herzog, M.A. Cohen, C.L. Dakin, A.M.
Wren, A.E. Brynes, M.J. Low, M.A. Ghatei, R.D. Cone, S.R. Bloom, Gut hormone
PYY(336) physiologically inhibits food intake, Nature 418 (2002) 650654.
[34] P.K. Chelikani, A.C. Haver, R.D. Reidelberger, Intravenous infusion of peptide
YY(336) potently inhibits food intake in rats, Endocrinology 146 (2005) 879888.
[35] H.R. Davis Jr., D.E. Mullins, J.M. Pines, L.M. Hoos, C.F. France, D.S. Compton, M.P.
Graziano, E.J. Sybertz, C.D. Strader, M. Van Heek, Effect of chronic central administration of glucagon-like peptide-1 (736) amide on food consumption and body
weight in normal and obese rats, Obes. Res. 6 (1998) 147156.
[36] S. Koda, Y. Date, N. Murakami, T. Shimbara, T. Hanada, K. Toshinai, A. Niijima, M.
Furuya, N. Inomata, K. Osuye, M. Nakazato, The role of the vagal nerve in peripheral
PYY3-36-induced feeding reduction in rats, Endocrinology 146 (2005) 23692375.
[37] M.D. Turton, D. O'Shea, I. Gunn, S.A. Beak, C.M. Edwards, K. Meeran, S.J. Choi, G.M.
Taylor, M.M. Heath, P.D. Lambert, J.P. Wilding, D.M. Smith, M.A. Ghatei, J. Herbert,
S.R. Bloom, A role for glucagon-like peptide-1 in the central regulation of feeding,
Nature 379 (1996) 6972.
[38] B.-J. Kim, O.D. Carlson, H.-J. Jang, D. Elahi, C. Berry, J.M. Egan, Peptide YY is secreted
after oral glucose administration in a gender-specic manner, J. Clin. Endocrinol.
Metab. 90 (2005) 66656671.
[39] G. Tolhurst, H. Heffron, Y.S. Lam, H.E. Parker, A.M. Habib, E. Diakogiannaki, J.
Cameron, J. Grosse, F. Reimann, F.M. Gribble, Short-chain fatty acids stimulate
glucagon-like peptide-1 secretion via the G-protein-coupled receptor FFAR2, Diabetes 61 (2012) 364371.
[40] H. Ge, X. Li, J. Weiszmann, P. Wang, H. Baribault, J.-L. Chen, H. Tian, Y. Li, Activation of
G protein-coupled receptor 43 in adipocytes leads to inhibition of lipolysis and suppression of plasma free fatty acids, Endocrinology 149 (2008) 45194526.
[41] N.M. Delzenne, A.M. Neyrinck, F. Bckhed, P.D. Cani, Targeting gut microbiota in
obesity: effects of prebiotics and probiotics, Nat. Rev. Endocrinol. 7 (2011) 639646.
T. Hara et al. / Biochimica et Biophysica Acta 1841 (2014) 12921300
[42] T. Greiner, F. Bckhed, Effects of the gut microbiota on obesity and glucose homeostasis, Trends Endocrinol. Metab. 22 (2011) 117123.
[43] J. Henao-Mejia, E. Elinav, C. Jin, L. Hao, W.Z. Mehal, T. Strowig, C.A. Thaiss, A.L. Kau,
S.C. Eisenbarth, M.J. Jurczak, J.-P. Camporez, G.I. Shulman, J.I. Gordon, H.M.
Hoffman, R.A. Flavell, Inammasome-mediated dysbiosis regulates progression of
NAFLD and obesity, Nature 482 (2012) 179185.
[44] A.L. Kau, P.P. Ahern, N.W. Grifn, A.L. Goodman, J.I. Gordon, Human nutrition, the
gut microbiome and the immune system, Nature 474 (2011) 327336.
[45] P.J. Turnbaugh, M. Hamady, T. Yatsunenko, B.L. Cantarel, A. Duncan, R.E. Ley, M.L.
Sogin, W.J. Jones, B.A. Roe, J.P. Affourtit, M. Egholm, B. Henrissat, A.C. Heath, R.
Knight, J.I. Gordon, A core gut microbiome in obese and lean twins, Nature 457
(2009) 480484.
[46] P.J. Turnbaugh, R.E. Ley, M.A. Mahowald, V. Magrini, E.R. Mardis, J.I. Gordon, An
obesity-associated gut microbiome with increased capacity for energy harvest, Nature 444 (2006) 10271031.
[47] I. Kimura, K. Ozawa, D. Inoue, T. Imamura, K. Kimura, T. Maeda, K. Terasawa, D.
Kashihara, K. Hirano, T. Tani, T. Takahashi, S. Miyauchi, G. Shioi, H. Inoue, G.
Tsujimoto, The gut microbiota suppresses insulin-mediated fat accumulation via
the short-chain fatty acid receptor GPR43, Nat. Commun. 4 (2013) 1829.
[48] R. Masui, M. Sasaki, Y. Funaki, N. Ogasawara, M. Mizuno, A. Iida, S. Izawa, Y. Kondo,
Y. Ito, Y. Tamura, K. Yanamoto, H. Noda, A. Tanabe, N. Okaniwa, Y. Yamaguchi, T.
Iwamoto, K. Kasugai, G protein-coupled receptor 43 moderates gut inammation
through cytokine regulation from mononuclear cells, Inamm. Bowel Dis. 19
(2013) 28482856.
[49] C. Sina, O. Gavrilova, M. Frster, A. Till, S. Derer, F. Hildebrand, B. Raabe, A. Chalaris, J.
Scheller, A. Rehmann, A. Franke, S. Ott, R. Hsler, S. Nikolaus, U.R. Flsch, S. RoseJohn, H.-P. Jiang, J. Li, S. Schreiber, P. Rosenstiel, G protein-coupled receptor 43 is essential for neutrophil recruitment during intestinal inammation, J. Immunol. 1950
(183) (2009) 75147522.
[50] J. Wang, X. Wu, N. Simonavicius, H. Tian, L. Ling, Medium-chain fatty acids as ligands for orphan G protein-coupled receptor GPR84, J. Biol. Chem. 281 (2006)
3445734464.
[51] T. Suzuki, S.-I. Igari, A. Hirasawa, M. Hata, M. Ishiguro, H. Fujieda, Y. Itoh, T. Hirano, H.
Nakagawa, M. Ogura, M. Makishima, G. Tsujimoto, N. Miyata, Identication of G
protein-coupled receptor 120-selective agonists derived from PPARgamma agonists,
J. Med. Chem. 51 (2008) 76407644.
[52] C. Bouchard, J. Pag, A. Bdard, P. Tremblay, L. Vallires, G protein-coupled receptor
84, a microglia-associated protein expressed in neuroinammatory conditions, Glia
55 (2007) 790800.
[53] C. Venkataraman, F. Kuo, The G-protein coupled receptor, GPR84 regulates IL-4 production by T lymphocytes in response to CD3 crosslinking, Immunol. Lett. 101
(2005) 144153.
[54] H. Nagasaki, T. Kondo, M. Fuchigami, H. Hashimoto, Y. Sugimura, N. Ozaki, H. Arima,
A. Ota, Y. Oiso, Y. Hamada, Inammatory changes in adipose tissue enhance expression of GPR84, a medium-chain fatty acid receptor: TNF enhances GPR84 expression in adipocytes, FEBS Lett. 586 (2012) 368372.
[55] S. Fukunaga, S. Setoguchi, A. Hirasawa, G. Tsujimoto, Monitoring ligand-mediated
internalization of G protein-coupled receptor as a novel pharmacological approach,
Life Sci. 80 (2006) 1723.
[56] T. Hara, A. Hirasawa, Q. Sun, K. Sadakane, C. Itsubo, T. Iga, T. Adachi, T. Koshimizu, T.
Hashimoto, Y. Asakawa, G. Tsujimoto, Novel selective ligands for free fatty acid receptors GPR120 and GPR40, Naunyn Schmiedebergs Arch. Pharmacol. 380 (2009)
247255.
[57] Q. Sun, A. Hirasawa, T. Hara, I. Kimura, T. Adachi, T. Awaji, M. Ishiguro, T. Suzuki, N.
Miyata, G. Tsujimoto, Structureactivity relationships of GPR120 agonists based on a
docking simulation, Mol. Pharmacol. 78 (2010) 804810.
[58] B.D. Hudson, B. Shimpukade, A.E. Mackenzie, A.J. Butcher, J.D. Pediani, E. Christiansen, H.
Heathcote, A.B. Tobin, T. Ulven, G. Milligan, The pharmacology of TUG-891, a potent and
selective agonist of the free fatty acid receptor 4 (FFA4/GPR120), demonstrates both potential opportunity and possible challenges to therapeutic agonism, Mol. Pharmacol. 84
(2013) 710725.
[59] B. Shimpukade, B.D. Hudson, C.K. Hovgaard, G. Milligan, T. Ulven, Discovery of a potent and selective GPR120 agonist, J. Med. Chem. 55 (2012) 45114515.
[60] N. Hashimoto, Y. Sasaki, C. Nakama, M. Ishikawa, Novel phenyl-isoxazol-3-ol derivative, US20100130559 A1, 2010.
[61] K. Arakawa, T. Nishimura, Y. Sugimoto, H. Takahashi, T. Shimamura, Novel
Isoindolin-1-One Derivative, 2010. (WO/2010/104195).
[62] J. Ma, A. Novack, I. Nashashibi, P. Pham, C.J. Rabbat, J. Song, D.F. Shi, Z. Zhao, Y.-J.
Choi, X. Chen, Aryl Gpr120 Receptor Agonists and Uses Thereof, 2010. (WO/2010/
048207).
[63] S. Katsuma, N. Hatae, T. Yano, Y. Ruike, M. Kimura, A. Hirasawa, G. Tsujimoto, Free
fatty acids inhibit serum deprivation-induced apoptosis through GPR120 in a murine enteroendocrine cell line STC-1, J. Biol. Chem. 280 (2005) 1950719515.
[64] B.P. Shah, P. Liu, T. Yu, D.R. Hansen, T.A. Gilbertson, TRPM5 is critical for linoleic acidinduced CCK secretion from the enteroendocrine cell line, STC-1, Am. J. Physiol. Cell
Physiol. 302 (2012) C210C219.
[65] D.Y. Oh, S. Talukdar, E.J. Bae, T. Imamura, H. Morinaga, W. Fan, P. Li, W.J. Lu, S.M.
Watkins, J.M. Olefsky, GPR120 is an omega-3 fatty acid receptor mediating potent
anti-inammatory and insulin-sensitizing effects, Cell 142 (2010) 687698.
[66] S.-J. Watson, A.J.H. Brown, N.D. Holliday, Differential signaling by splice variants of
the human free fatty acid receptor GPR120, Mol. Pharmacol. 81 (2012) 631642.
[67] A. Ichimura, A. Hirasawa, O. Poulain-Godefroy, A. Bonnefond, T. Hara, L. Yengo, I.
Kimura, A. Leloire, N. Liu, K. Iida, H. Choquet, P. Besnard, C. Lecoeur, S. Vivequin, K.
Ayukawa, M. Takeuchi, K. Ozawa, M. Tauber, C. Maffeis, A. Morandi, et al., Dysfunction of lipid sensor GPR120 leads to obesity in both mouse and human, Nature 483
(2012) 350354.
1299
[68] X. Li, Y. Yu, C.D. Funk, Cyclooxygenase-2 induction in macrophages is modulated by
docosahexaenoic acid via interactions with free fatty acid receptor 4 (FFA4), FASEB J.
(2013).
[69] A. Hirasawa, K. Tsumaya, T. Awaji, S. Katsuma, T. Adachi, M. Yamada, Y. Sugimoto, S.
Miyazaki, G. Tsujimoto, Free fatty acids regulate gut incretin glucagon-like peptide-1
secretion through GPR120, Nat. Med. 11 (2005) 9094.
[70] S. Matsumura, A. Eguchi, T. Mizushige, N. Kitabayashi, S. Tsuzuki, K. Inoue, T. Fushiki,
Colocalization of GPR120 with phospholipase-Cbeta2 and alpha-gustducin in the
taste bud cells in mice, Neurosci. Lett. 450 (2009) 186190.
[71] S. Miyauchi, A. Hirasawa, T. Iga, N. Liu, C. Itsubo, K. Sadakane, T. Hara, G. Tsujimoto,
Distribution and regulation of protein expression of the free fatty acid receptor
GPR120, Naunyn Schmiedebergs Arch. Pharmacol. 379 (2009) 427434.
[72] J. Taneera, S. Lang, A. Sharma, J. Fadista, Y. Zhou, E. Ahlqvist, A. Jonsson, V. Lyssenko,
P. Vikman, O. Hansson, H. Parikh, O. Korsgren, A. Soni, U. Krus, E. Zhang, X.-J. Jing, J.L.
S. Esguerra, C.B. Wollheim, A. Salehi, A. Rosengren, et al., A systems genetics approach identies genes and pathways for type 2 diabetes in human islets, Cell
Metab. 16 (2012) 122134.
[73] C.P. Briscoe, M. Tadayyon, J.L. Andrews, W.G. Benson, J.K. Chambers, M.M. Eilert, C.
Ellis, N.A. Elshourbagy, A.S. Goetz, D.T. Minnick, P.R. Murdock, H.R. Sauls Jr., U.
Shabon, L.D. Spinage, J.C. Strum, P.G. Szekeres, K.B. Tan, J.M. Way, D.M. Ignar, S.
Wilson, et al., The orphan G protein-coupled receptor GPR40 is activated by medium
and long chain fatty acids, J. Biol. Chem. 278 (2003) 1130311311.
[74] Y. Itoh, Y. Kawamata, M. Harada, M. Kobayashi, R. Fujii, S. Fukusumi, K. Ogi, M.
Hosoya, Y. Tanaka, H. Uejima, H. Tanaka, M. Maruyama, R. Satoh, S. Okubo, H.
Kizawa, H. Komatsu, F. Matsumura, Y. Noguchi, T. Shinohara, S. Hinuma, et al.,
Free fatty acids regulate insulin secretion from pancreatic beta cells through
GPR40, Nature 422 (2003) 173176.
[75] K. Kotarsky, N.E. Nilsson, B. Olde, C. Owman, Progress in methodology Improved reporter gene assays used to identify ligands acting on orphan seven-transmembrane
receptors, Pharmacol. Toxicol. 93 (2003) 249258.
[76] T. Hara, A. Hirasawa, Q. Sun, T. Koshimizu, C. Itsubo, K. Sadakane, T. Awaji, G.
Tsujimoto, Flow cytometry-based binding assay for GPR40 (FFAR1; free fatty acid
receptor 1), Mol. Pharmacol. 75 (2009) 8591.
[77] A. Salehi, E. Flodgren, N.E. Nilsson, J. Jimenez-Feltstrom, J. Miyazaki, C. Owman, B.
Olde, Free fatty acid receptor 1 (FFA(1)R/GPR40) and its involvement in fattyacid-stimulated insulin secretion, Cell Tissue Res. 322 (2005) 207215.
[78] C.P. Briscoe, A.J. Peat, S.C. McKeown, D.F. Corbett, A.S. Goetz, T.R. Littleton, D.C.
McCoy, T.P. Kenakin, J.L. Andrews, C. Ammala, J.A. Fornwald, D.M. Ignar, S.
Jenkinson, Pharmacological regulation of insulin secretion in MIN6 cells through
the fatty acid receptor GPR40: identication of agonist and antagonist small molecules, Br. J. Pharmacol. 148 (2006) 619628.
[79] M. Takeuchi, A. Hirasawa, T. Hara, I. Kimura, T. Hirano, T. Suzuki, N. Miyata, T. Awaji,
M. Ishiguro, G. Tsujimoto, FFA1-selective agonistic activity based on docking simulation using FFA1 and GPR120 homology models, Br. J. Pharmacol. 168 (2013)
15701583.
[80] Y. Tsujihata, R. Ito, M. Suzuki, A. Harada, N. Negoro, T. Yasuma, Y. Momose, K.
Takeuchi, TAK-875, an orally available G protein-coupled receptor 40/free fatty
acid receptor 1 agonist, enhances glucose-dependent insulin secretion and improves both postprandial and fasting hyperglycemia in type 2 diabetic rats, J.
Pharmacol. Exp. Ther. 339 (2011) 228237.
[81] C. Longuet, C. Broca, S. Costes, E.H. Hani, D. Bataille, S. Dalle, Extracellularly regulated
kinases 1/2 (p44/42 mitogen-activated protein kinases) phosphorylate synapsin I
and regulate insulin secretion in the MIN6 beta-cell line and islets of Langerhans,
Endocrinology 146 (2005) 643654.
[82] J. Selway, R. Rigatti, N. Storey, J. Lu, G.B. Willars, T.P. Herbert, Evidence that Ca2+
within the microdomain of the L-type voltage gated Ca2+ channel activates ERK
in MIN6 cells in response to glucagon-like peptide-1, PLoS One 7 (2012) e33004.
[83] J.L. Selway, C.E. Moore, R. Mistry, R.A. John Challiss, T.P. Herbert, Molecular mechanisms of muscarinic acetylcholine receptor-stimulated increase in cytosolic free
Ca(2 +) concentration and ERK1/2 activation in the MIN6 pancreatic -cell line,
Acta Diabetol. 49 (2012) 277289.
[84] M. Ferdaoussi, V. Bergeron, B. Zarrouki, J. Kolic, J. Cantley, J. Fielitz, E.N. Olson, M.
Prentki, T. Biden, P.E. MacDonald, V. Poitout, G protein-coupled receptor (GPR)40dependent potentiation of insulin secretion in mouse islets is mediated by protein
kinase D1, Diabetologia 55 (2012) 26822692.
[85] D.C.-H. Lin, Q. Guo, J. Luo, J. Zhang, K. Nguyen, M. Chen, T. Tran, P.J. Dranseld, S.P.
Brown, J. Houze, M. Vimolratana, X.Y. Jiao, Y. Wang, N.J.M. Birdsall, G. Swaminath,
Identication and pharmacological characterization of multiple allosteric binding
sites on the free fatty acid 1 receptor, Mol. Pharmacol. 82 (2012) 843859.
[86] A.D. Mancini, V. Poitout, The fatty acid receptor FFA1/GPR40 a decade later: how
much do we know? Trends Endocrinol. Metab. 24 (2013) 398407.
[87] K. Nagasumi, R. Esaki, K. Iwachidow, Y. Yasuhara, K. Ogi, H. Tanaka, M. Nakata, T.
Yano, K. Shimakawa, S. Taketomi, K. Takeuchi, H. Odaka, Y. Kaisho, Overexpression
of GPR40 in pancreatic beta-cells augments glucose-stimulated insulin secretion
and improves glucose tolerance in normal and diabetic mice, Diabetes 58 (2009)
10671076.
[88] H. Kristinsson, D.M. Smith, P. Bergsten, E. Sargsyan, FFAR1 is involved in both the
acute and chronic effects of palmitate on insulin secretion, Endocrinology 154
(2013) 40784088.
[89] S. Meidute Abaraviciene, S.J. Muhammed, S. Amisten, I. Lundquist, A. Salehi, GPR40
protein levels are crucial to the regulation of stimulated hormone secretion in pancreatic islets. Lessons from spontaneous obesity-prone and non-obese type 2 diabetes in rats, Mol. Cell. Endocrinol. 381 (2013) 150159.
[90] S. Jain, I. Ruiz de Azua, H. Lu, M.F. White, J.-M. Guettier, J. Wess, Chronic activation of
a designer G(q)-coupled receptor improves cell function, J. Clin. Invest. 123 (2013)
17501762.
1300
T. Hara et al. / Biochimica et Biophysica Acta 1841 (2014) 12921300
[91] E. Flodgren, B. Olde, S. Meidute-Abaraviciene, M.S. Winzell, B. Ahrn, A. Salehi,
GPR40 is expressed in glucagon producing cells and affects glucagon secretion,
Biochem. Biophys. Res. Commun. 354 (2007) 240245.
[92] L. Wang, Y. Zhao, B. Gui, R. Fu, F. Ma, J. Yu, P. Qu, L. Dong, C. Chen, Acute stimulation
of glucagon secretion by linoleic acid results from GPR40 activation and [Ca2+]i increase in pancreatic islet {alpha}-cells, J. Endocrinol. 210 (2011) 173179.
[93] H. Lan, L.M. Hoos, L. Liu, G. Tetzloff, W. Hu, S.J. Abbondanzo, G. Vassileva, E.L.
Gustafson, J.A. Hedrick, H.R. Davis, Lack of FFAR1/GPR40 does not protect mice
from high-fat diet-induced metabolic disease, Diabetes 57 (2008) 29993006.
[94] M.G. Latour, T. Alquier, E. Oseid, C. Tremblay, T.L. Jetton, J. Luo, D.C.-H. Lin, V. Poitout,
GPR40 is necessary but not sufcient for fatty acid stimulation of insulin secretion
in vivo, Diabetes 56 (2007) 10871094.
[95] A.P. Liou, X. Lu, Y. Sei, X. Zhao, S. Pechhold, R.J. Carrero, H.E. Raybould, S. Wank, The
G-protein-coupled receptor GPR40 directly mediates long-chain fatty acid-induced
secretion of cholecystokinin, Gastroenterology 140 (2011) 903912.
[96] S. Edfalk, P. Steneberg, H. Edlund, Gpr40 is expressed in enteroendocrine cells and
mediates free fatty acid stimulation of incretin secretion, Diabetes 57 (2008)
22802287.
Vous aimerez peut-être aussi
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- The DNA Way - Kashif KhanDocument268 pagesThe DNA Way - Kashif Khancepa100% (1)
- Pharm Calcium Channel Blockers (Bahar&Amy) "Vera Dialed The Calcium Channel To Buy A Knife" Verapramil, Diltizaem, NifedipineDocument7 pagesPharm Calcium Channel Blockers (Bahar&Amy) "Vera Dialed The Calcium Channel To Buy A Knife" Verapramil, Diltizaem, Nifedipinecherrybombaz100% (4)
- PATHOLOGY Board Exam ANsWERSDocument22 pagesPATHOLOGY Board Exam ANsWERSchristinejoan100% (1)
- Burnout Syndrome - Stress in Health Care Professionals Working To Fight Covid-19 in Public HospitalsDocument14 pagesBurnout Syndrome - Stress in Health Care Professionals Working To Fight Covid-19 in Public HospitalsIJAERS JOURNALPas encore d'évaluation
- Health TipsDocument102 pagesHealth Tipsgurkirt100% (1)
- Patterns of Paragraph DevelopmentDocument3 pagesPatterns of Paragraph Developmentyacht_69Pas encore d'évaluation
- Notes On History Taking in The Cardiovascular SystemDocument9 pagesNotes On History Taking in The Cardiovascular Systemmdjohar72100% (1)
- Kansas Foodborne Illness ManualDocument186 pagesKansas Foodborne Illness ManualLeo M. Pedro Jr.Pas encore d'évaluation
- SuctioningDocument23 pagesSuctioningrnrmmanphd100% (2)
- Ats Menjawab Soal Gin Nov21 Final 50Document14 pagesAts Menjawab Soal Gin Nov21 Final 50anton suponoPas encore d'évaluation
- TofacitinibDocument23 pagesTofacitinibShubham SenguptaPas encore d'évaluation
- AUBF QUiZDocument12 pagesAUBF QUiZGene Narune GaronitaPas encore d'évaluation
- RSA Regulation 429 Food LabellingDocument106 pagesRSA Regulation 429 Food LabellinggeoffhunterPas encore d'évaluation
- bph0171 1156 (1) 1Document11 pagesbph0171 1156 (1) 1kasabePas encore d'évaluation
- Am J Clin Nutr 2016 Valsesia Ajcn.116.137646Document10 pagesAm J Clin Nutr 2016 Valsesia Ajcn.116.137646kasabePas encore d'évaluation
- Jia Yin, Haiying Li, Chengjie Meng, Dongdong Chen, Zhouqing Chen, Yibin Wang, Zhong Wang, Gang ChenDocument12 pagesJia Yin, Haiying Li, Chengjie Meng, Dongdong Chen, Zhouqing Chen, Yibin Wang, Zhong Wang, Gang ChenkasabePas encore d'évaluation
- Microrna 375 Mediates Palmitate-Induced Enteric Neuronal Damage and High-Fat Diet-Induced Delayed Intestinal Transit in MiceDocument14 pagesMicrorna 375 Mediates Palmitate-Induced Enteric Neuronal Damage and High-Fat Diet-Induced Delayed Intestinal Transit in MicekasabePas encore d'évaluation
- 2014 Article 9408Document10 pages2014 Article 9408kasabePas encore d'évaluation
- 1 s2.0 S0006295216001842 MainDocument11 pages1 s2.0 S0006295216001842 MainkasabePas encore d'évaluation
- 00043Document6 pages00043kasabePas encore d'évaluation
- Am J Clin Nutr 2016 Valsesia Ajcn.116.137646Document10 pagesAm J Clin Nutr 2016 Valsesia Ajcn.116.137646kasabePas encore d'évaluation
- 61 10 09 s3 ArticleDocument6 pages61 10 09 s3 ArticlekasabePas encore d'évaluation
- Nutrition: Basic Nutritional InvestigationDocument8 pagesNutrition: Basic Nutritional InvestigationkasabePas encore d'évaluation
- WJG 21 3085Document9 pagesWJG 21 3085kasabePas encore d'évaluation
- Nutrition: Basic Nutritional InvestigationDocument8 pagesNutrition: Basic Nutritional InvestigationkasabePas encore d'évaluation
- WJG 15 1690Document12 pagesWJG 15 1690kasabePas encore d'évaluation
- Investigation of Relationships Among Gastroesophageal Reflux Disease Subtypes Using Narrow Band Imaging Magnifying EndosDocument8 pagesInvestigation of Relationships Among Gastroesophageal Reflux Disease Subtypes Using Narrow Band Imaging Magnifying EndoskasabePas encore d'évaluation
- JNM 18 78Document8 pagesJNM 18 78kasabePas encore d'évaluation
- Pone 0048602Document7 pagesPone 0048602kasabePas encore d'évaluation
- Interleukin 1B Proinflammatory Genotypes Protect Against Gastro-Oesophageal Reflux Disease Through Induction of Corpus AtrophyDocument8 pagesInterleukin 1B Proinflammatory Genotypes Protect Against Gastro-Oesophageal Reflux Disease Through Induction of Corpus AtrophykasabePas encore d'évaluation
- Associations of Circulating Gut Hormone and Adipocytokine Levels With The Spectrum of Gastroesophageal Reflux DiseaseDocument12 pagesAssociations of Circulating Gut Hormone and Adipocytokine Levels With The Spectrum of Gastroesophageal Reflux DiseasekasabePas encore d'évaluation
- Genetic Influences in GerdDocument6 pagesGenetic Influences in GerdkasabePas encore d'évaluation
- Impact of Self-Reported Gastroesophageal Reflux Disease in Subjects From Copdgene CohortDocument9 pagesImpact of Self-Reported Gastroesophageal Reflux Disease in Subjects From Copdgene CohortkasabePas encore d'évaluation
- DDV 512Document8 pagesDDV 512kasabePas encore d'évaluation
- Interleukin 1B Proinflammatory Genotypes Protect Against Gastro-Oesophageal Reflux Disease Through Induction of Corpus AtrophyDocument8 pagesInterleukin 1B Proinflammatory Genotypes Protect Against Gastro-Oesophageal Reflux Disease Through Induction of Corpus AtrophykasabePas encore d'évaluation
- A61g Polimorfismo and GerdDocument5 pagesA61g Polimorfismo and GerdkasabePas encore d'évaluation
- A61g Polimorfismo and GerdDocument5 pagesA61g Polimorfismo and GerdkasabePas encore d'évaluation
- AsmefDocument35 pagesAsmef.Pas encore d'évaluation
- WC BPR - Prevention and Management of Diabetic Foot Ulcers 1573r4e FinalDocument68 pagesWC BPR - Prevention and Management of Diabetic Foot Ulcers 1573r4e FinalArumDesiPratiwiPas encore d'évaluation
- Fixed Drug EruptionsDocument6 pagesFixed Drug EruptionsArif OktavianPas encore d'évaluation
- Alzheimers Disease,,syringoyeloma by VineethaDocument42 pagesAlzheimers Disease,,syringoyeloma by VineethaDR. KUMARASWAMI HEALTH CENTRE COLLEGE OF NURSING KANYAKUMARIPas encore d'évaluation
- Esophagus: DrzaiterDocument37 pagesEsophagus: DrzaiterdrynwhylPas encore d'évaluation
- Preventative Care Assignment 3 (1) ADocument9 pagesPreventative Care Assignment 3 (1) AOdia OaikhenaPas encore d'évaluation
- Prostatic Abscess - StatPearls - NCBI BookshelfDocument14 pagesProstatic Abscess - StatPearls - NCBI BookshelfSheshang KamathPas encore d'évaluation
- Animal Health and Welfare Module 1Document127 pagesAnimal Health and Welfare Module 1prevosterfuturemwampwePas encore d'évaluation
- AEF2e TB4 VP 2Document2 pagesAEF2e TB4 VP 2Minji LeePas encore d'évaluation
- A Balanced Diet Is One That Provides An Adequate Intake of Energy and Nutrients For Maintenance of The Body and Therefore Good HealthDocument1 pageA Balanced Diet Is One That Provides An Adequate Intake of Energy and Nutrients For Maintenance of The Body and Therefore Good HealthSnigdha SarkarPas encore d'évaluation
- Osteoarthritis of HipDocument3 pagesOsteoarthritis of Hipjcachica21Pas encore d'évaluation
- Media, Merchandise and All Issues Fully On Line atDocument32 pagesMedia, Merchandise and All Issues Fully On Line atlordhavok33Pas encore d'évaluation
- Neurological Disorders Key NotesDocument31 pagesNeurological Disorders Key NotesHannah aswiniPas encore d'évaluation
- Kienbock's DiseaseDocument12 pagesKienbock's DiseaseVirtues GracesPas encore d'évaluation
- Special Populations PDFDocument4 pagesSpecial Populations PDFLouis TrầnPas encore d'évaluation
- 2021 The Enigma of Persistent Symptoms in Hypothyroid PatientsDocument8 pages2021 The Enigma of Persistent Symptoms in Hypothyroid PatientsPeter Albeiro Falla CortesPas encore d'évaluation
- Neuro-Ophthalmology ICD-10 Quick Reference GuideDocument4 pagesNeuro-Ophthalmology ICD-10 Quick Reference GuideFaisal ApendixPas encore d'évaluation