Académique Documents
Professionnel Documents
Culture Documents
'Leptorapide'-A One-Step Assay For Rapid Diagnosis of Human Leptospirosis
Transféré par
vignesh9489Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
'Leptorapide'-A One-Step Assay For Rapid Diagnosis of Human Leptospirosis
Transféré par
vignesh9489Droits d'auteur :
Formats disponibles
See
discussions, stats, and author profiles for this publication at: http://www.researchgate.net/publication/256764133
'Leptorapide'-A one-step assay for rapid
diagnosis of human leptospirosis
ARTICLE in EPIDEMIOLOGY AND INFECTION SEPTEMBER 2013
Impact Factor: 2.49 DOI: 10.1017/S0950268813002112 Source: PubMed
CITATIONS
9 AUTHORS, INCLUDING:
Owen Kavanagh
Rudy A Hartskeerl
York Saint John University
Royal Tropical Institute
16 PUBLICATIONS 147 CITATIONS
152 PUBLICATIONS 3,113 CITATIONS
SEE PROFILE
SEE PROFILE
Available from: Owen Kavanagh
Retrieved on: 31 August 2015
Epidemiol. Infect., Page 1 of 6. Cambridge University Press 2013
doi:10.1017/S0950268813002112
Leptorapide a one-step assay for rapid diagnosis
of human leptospirosis
T. BROWNLOW 1 *, O. V. KAVANAGH 1 , 2 , E. F. LOGAN 1 , R. A. HARTSKEERL 3 ,
R. SAVAGE 1 , M. F. PALMER 4 , M. KRAHL 5 , D. P. MACKIE 5 A N D W. A. ELLIS 6
1
Linnodee Ltd, Ballyclare, Northern Ireland
Department of Veterinary Science, Faculty of Agriculture & Science, Queens University of Belfast,
Belfast Northern Ireland
3
Department of Biomedical Research, Royal Tropical Institute (KIT), Amsterdam, The Netherlands
4
Leptospirosis Reference Unit, PHLS Laboratory, County Hospital, Hereford, UK
5
Zoonoses Centre, UFPRS, Pelotas, CEP 96010-900, Brazil
6
OIE Leptospira Reference Laboratory, AFBI Veterinary Sciences Division, Belfast Northern Ireland
2
Received 17 April 2013; Final revision 7 August 2013; Accepted 13 August 2013
SUMMARY
Leptospirosis is a globally important zoonotic infection caused by spirochaetes of the genus
Leptospira. It is transmitted to humans by direct contact with infected animals or indirectly via
contaminated water. It is mainly a problem of the resource-poor developing countries of the
tropical and sub-tropical regions of the world but outbreaks due to an increase in travel and
recreational activities have been reported in developed and more industrialized areas of the
world. Current methods of diagnosis are costly, time-consuming and require the use of
specialized laboratory equipment and personnel. The purpose of this paper is to report the
validation of the Leptorapide test (Linnodee Ltd, Northern Ireland) for the diagnosis of
human leptospirosis. It is a simple one-step latex agglutination assay performed using equal
volumes of serum sample and antigen-bound latex beads. Evidence of leptospiral antibodies is
determined within minutes. Agglutination is scored on a scale of 15 and the results interpreted
using a score card provided with the kit. Validation has been performed with a large sample size
obtained from individuals originating from various parts of the world including Brazil and India.
The test has shown sensitivity and specicity values of 971% and 940%, respectively, relative
to the microscopic agglutination test. The results demonstrate that Leptorapide offers a
cost-effective and accurate alternative to the more historical methods of antibody detection.
Key words: Infectious disease, leptospirosis, spirochaetes, tropical diseases, zoonoses.
I N T RO D U C T I O N
Considered the most common zoonosis worldwide,
leptospirosis is a bacterial infection caused by
spirochaetes from the genus Leptospira [14]. The
* Author for correspondence: Mrs T. Brownlow, Linnodee Ltd,
Holestone Road, Ballyclare, BT39 OTJ, Northern Ireland.
(Email: info@linnodee.com)
genus Leptospira includes both saprophytic and
pathogenic species. The pathogenic family consists
of 13 pathogenic species: L. alexanderi, L. alstonii,
L. borgpetersenii, L. inadai, L. interrogans, L. fainei,
L. kirschneri, L. licerasiae, L. noguchi, L. santarosai,
L. terpstrae, L. weilii, and L. wolfi, with more than
250 serovars [5].
Leptospires persist in the kidneys and genital tracts
of carrier wild and domestic animals and are excreted
T. Brownlow and others
in urine and genital uids. Survival outside the host is
favoured by warm moist conditions [6]. Humans are
generally considered to be incidental dead end hosts
who can become infected by any parasitic leptospire,
although recent information would indicate that
under certain circumstances, humans can also maintain infection [7]. Transmission to humans occurs by
direct contact with infected animals or indirectly, via
water contaminated from urine shed by carrier animals such as rodents or domestic animals [1, 8, 9].
The most common route of entry is through abrasions
in the skin or mucous membranes of the nose, eyes or
throat [10].
Infected humans exhibit a wide spectrum of clinical
responses to infection ranging from subclinical, acute
u-like symptoms, pyrexia of unknown origin, haemoptysis, acute renal disease, CNS involvement, to
acute haemorrhagic fever [11, 12] none of which are
pathognomonic for leptospirosis.
In the absence of a clinical diagnosis, there is a
need for rapid supportive laboratory diagnoses
especially in the face of an epidemic. Laboratory
methods are based on the demonstration of the organism in the patient or the presence of an immune
response. Organism detection methods are slow
(culture) and expensive (culture and PCR) and
require access to specialist laboratories [13, 14].
Antibody detection methods are often the only
practical option but have a variety of limitations.
Patients only develop a detectable serological response
1014 days post-infection. The standard serological
test the microscopic agglutination test (MAT) is
not very cross-reactive, thus with the potential for
a person to be infected by such a large number of
serovars, the World Health Organization (WHO) [4]
recommends the use of 19 different live antigens
in the test making it impractical for all but specialist
laboratories. The response to this problem has been
the development of a variety of genus-specic tests
mainly IgM ELISAs, lateral ow tests and MATs.
There are disadvantages inherent in some of these
tests: expense (ELISA, lateral ow tests and whole
cell antigen only MATs) or still the requirement for
an element of laboratory access and expertise
(ELISA tests). MATs, in which antigen is attached
to a carrier matrix, offer the cheapest and simplest
approach to diagnosis. The purpose of this paper is
to describe the validation of a commercial latex
agglutination test (Leptorapide, Linnodee Ltd,
Northern Ireland) for the rapid serological diagnosis
of human leptospirosis.
M AT E R I A L S A N D ME T H O D S
Sera
Fifty-ve human sera samples were collected from
the Leptospira Reference Unit, Hereford, UK.
Twenty-six samples were conrmed positive for leptospirosis and 29 samples were conrmed negative
using MAT. Fifty-two human sera samples were
collected from the WHO/FAO/OIE Leptospira
Reference Unit, KIT Biomedical Research Institute,
The Netherlands (hereafter KIT, The Netherlands).
Of these, nine were identied as positive and 43 identied as negative using MAT. Sera (n = 168) from
patients with clinical presentation suggesting leptospirosis in the southern Brazilian state of Rio
Grande de Sul, was used to test Leptorapide in a
population where the disease is endemic. Sera samples
(n = 406) were obtained from the endemic region of
South Andaman in an independent study sponsored
by the WHO and performed by the Indian Council
of Medical Research (ICMR). Samples were obtained
from patients who had fever along with any of the following symptoms: headache, body ache and muscle
tenderness, jaundice, haemorrhagic tendency, cough
with haemoptysis or breathlessness, oliguria or signs
of meningeal irritation. Cases were identied during
an outbreak in Middle Andaman. Ninety-six sera
samples were obtained from a leptospirosis reference
centre in Poland. All 96 samples were conrmed negative by MAT testing. To determine the efcacy of
Leptorapide as a rapid screening test in relation to
the MAT, 220 sera samples representing patients
with clinical symptoms suggesting leptospirosis were
tested by the Istituto Superiore di Sanita (ISS),
Rome, Italy, and 472 clinically suspected patient
samples were tested by the Centers for Disease
Control and Prevention (CDC, USA).
IgM ELISA
The Panbio IgM ELISA (Panbio Pty Ltd, Australia)
was used according to the manufacturers instructions.
A titre of 51:80 was considered positive for the presence of leptospiral antibody.
MAT
The MAT was performed according to standard
WHO guidelines, described by Wolff [15], Palmer
et al. [16] and Zochowski et al. [17]. The titre was
A one-step assay for diagnosis of human leptospirosis
1
Negative
Inconclusive,
repeat on
second sample
Positive
Fig. 1. [colour online]. Scoring of the Linnodee latex agglutination test. Test serum is mixed with an equal volume (5 l) of
antigen-bound latex beads on a 12-well glass slide. The bead/sera mix is placed on a Gyro rocker to promote drying.
After 5 min the extent of agglutination was scored on a scale of 15 (1, seronegative; 2, inconclusive; 35, seropositive).
taken as the highest dilution giving 50% agglutination
of leptospires.
The serovar ranges of antigens used within each
MAT analysis and cut-off values are given in
Supplementary Table S1 (available online).
for Leptorapide.
Specificity = d/(b + d) 100,
where d is the number of samples testing negative by
Leptorapide and MAT and b is the number of samples
testing negative by MAT, but positive by Leptorapide.
Accuracy = (a + d)/(a + b + c + d) 100.
Linnodee Leptorapide
The Leptorapide assay was performed as described
in the kit instructions. Antigen-bound beads were
re-suspended by gentle swirling or rolling the bottle
immediately before use. Using a new pipette for
each sample, 5 l of test sera/positive control sera
was mixed with 5 l of the antigen-bound latex
beads on a 12-well glass slide. The bead/serum mix
was placed on a Gyro rocker (Sigma-Aldrich, USA)
with gentle rotation to promote drying. The extent
of agglutination was scored on a scale of 15 (according to a score card included with the kit) ranging
from 1 (no agglutination) to 5 (strong positive
agglutination) (see Fig. 1). Four separate tests with
Leptorapide were used for the study in Hereford,
UK and three separate tests with Leptorapide
were used to evaluate the samples in KIT, The
Netherlands. An average of the results was obtained
by determining the majority overall result within the
tests performed.
Statistical methods
The sensitivity and specicity of Leptorapide for the
detection of the of anti-leptospiral antibodies was
determined in comparison with the MAT. The following calculations were used:
Sensitivity = a/(a + c) 100,
where a is the number of samples testing positive
by Leptorapide and MAT and c is the number of
samples testing positive by MAT, but negative
Kappa index = (a + d P)/(1 P),
where P = (a + c)(a + b) + (b + d)(c + d).
R E S ULTS
A total of 107 sera samples (34 MAT positive, 73
MAT negative) collected from Hereford, UK and
KIT, The Netherlands were tested with Leptorapide
and used to determine its sensitivity and specicity
relative to the MAT. Sera was considered positive
for the presence of leptospiral antibody if the MAT
titre >1:40 (Hereford, UK) or 51:160 (KIT, The
Netherlands) and if the Leptorapide score was 35.
Supplementary Table S2 outlines the results obtained
and shows Leptorapide compares well to the MAT;
with a sensitivity of 971% [95% condence interval
(CI) 829998] and specicity of 940% (95% CI
807957). In this analysis, there was very good agreement between Leptorapide and MAT, with a Kappa
index of 835%.
Ninety-six MAT-conrmed negative samples were
obtained from the reference centre in Poland and
used to determine the specicity of Leptorapide in
relation to the MAT. Supplementary Table S6 outlines the results obtained and shows Leptorapide compares well to the MAT; with a specicity of 958%
(95% CI 891987).
To determine the efcacy of Leptorapide as a
screening test for diagnosis of leptospirosis, validation
on diagnostic submissions was performed by the CDC
and the ISS. The MAT was used to diagnose
T. Brownlow and others
leptospirosis in patient samples, with a MAT titre
>1:100 indicative of disease. In total, 172/472 clinically
suspected patient samples from CDC were conrmed
positive for leptospirosis. Of the 172 samples, 11 were
single sera samples obtained from individual patients
and 77 samples were paired sera (71 2, 5 3, 1 4).
Overall specicity for Leptorapide was 93% and overall
sensitivity 71%. Leptorapide performed better with
samples obtained during the convalescent phase of the
disease; with a sensitivity of 814% vs. 616% sensitivity
during the acute phase of the disease. Similar results
were obtained by the ISS; overall specicity for
Leptorapide was 909% and overall sensitivity was
788%. Comparable results were seen with samples
obtained from patients after 1 week and 2 or 3 weeks
from onset of symptoms, with both sets of sera producing a sensitivity of 80% in relation to the MAT and
a high specicity of 90% (930% in week 1 and
864% in weeks 2/3). Weeks 12 are considered the
acute phase of this disease and it can sometimes be difcult regardless of the assay being used to identify the
antibodies at this stage of the disease. To determine
a correct diagnoses any negative results in patients
experiencing acute symptoms should be interrupted
with caution and should be again tested within the
2- to 3-week time period to give a more accurate
diagnoses and conrm the initial negative result.
In total, 168 samples (MAT titre >1:100) obtained
from patients with suspected leptospirosis in Brazil,
were used to validate the efcacy of Leptorapide in
an endemic region. Three different tests with
Leptorapide were performed (tests 1, 2 and 3). The
average of the three tests was determined and used
as a representative result. Supplementary Table S3
outlines the results from testing the samples with
both Leptorapide and the commercially available
Panbio ELISA. Both Leptorapide and the IgM
ELISA detected a similar number of positive samples;
66 testing positive with IgM ELISA and 87 of the
samples testing positive with Leptorapide. When
tested with Leptorapide, 36 samples were deemed
inconclusive requiring a repeat test and 45 samples
tested negative.
An independent study sponsored by the WHO was
performed by the ICMR. Sera samples (n = 406) from
the endemic region of South Andaman were collected
from clinical submissions and the indices of accuracy
were estimated for four rapid tests available for the
diagnosis of leptospirosis: latex agglutination test prepared at the Regional Medical Research Centre, Port
Blair, Leptorapide (Linnodee Ltd, Northern Ireland),
SD Leptospira IgM ELISA (Standard Diagnostics,
Korea) and Leptocheck (Zephyr Biomedicals, India).
Results showed Leptorapide was the most accurate
of the four tests evaluated (Supplementary Tables S4
and S5). In particular, Leptorapide was extremely
efcient at diagnosis of leptospirosis >1 week after
onset of illness, with sensitivity and specicity values
of 900% and 873%, respectively (Supplementary
Table S5).
D I S C U S S IO N
The purpose of this paper is to describe the validation
of the commercially available latex agglutination
test, Leptorapide, for the rapid serological diagnosis
of human leptospirosis. The sensitivity and specicity
of Leptorapide in relation to the MAT was determined using 107 sera samples; 55 obtained from the
Leptospira Reference Unit, Hereford, UK and 52
from KIT, The Netherlands. All samples had
Leptospira antibody titres pre-determined by the
MAT in the respective laboratory of origin. Of the
34 MAT-positive samples, Leptorapide correctly
identied 33 (971%) of these. Leptorapide identied
66 (940%) of the 73 MAT-negative samples. To
further support the specicity of Leptorapide as a
rapid screening test, 96 MAT-conrmed negative
sera were obtained from the reference centre in
Poland, all samples from this reference centre were
negative samples as it was a random selection from
the region and leptospirosis is not a common disease
in developed countries such as Poland, unfortunately
no positive samples were found. Leptorapide correctly
identied 92 (958%) of the 96 sera samples as negative, with the remaining four samples testing positive.
Leptorapide testing with these MAT-conrmed
samples has shown the test to be in agreement with
the current gold-standard test for the detection of leptospirosis. Therefore, the results support the suitability
of Leptorapide as an accurate, rapid screening test for
the diagnosis of leptospirosis.
To further support the use of Leptorapide as a
rapid screening test for the detection of leptospirosis,
the CDC and ISS tested the performance of
Leptorapide on serum samples obtained from patients
presenting with symptoms indicative of leptospirosis.
Although all of these patients were displaying symptoms of leptospirosis not all of the samples tested positive with the gold-standard MAT, this could have
been due to the wide and varied range of symptoms
that occur with leptospiral infections. Leptospirosis
A one-step assay for diagnosis of human leptospirosis
symptoms such as migraine, u-like symptoms and
jaundice are common to other diseases such as dengue
fever and meningitis. MAT testing was used for clinical diagnosis of each sample. Results from CDC show
a high (93%) specicity for Leptorapide in relation
to the MAT, with increased sensitivity of the test
during the convalescent phase of the disease (814%
vs. 616% during the acute phase). Similar ndings
were observed from the validation performed by the
ISS. Again, a high overall specicity (909%) of
Leptorapide was detected in relation to the MAT.
Sensitivity of the test was comparable from samples
obtained within 1 week and 2 or 3 weeks after the
onset of symptoms; 803% and 784%, respectively.
Taken together, these ndings suggest the suitability
of Leptorapide as a rapid screening test for use on
diagnostic submissions. However, as mentioned in
the Results section of this publication, negative
samples regardless of the diagnosing assay should be
treated with caution and a retest should be performed
within 23 weeks of onset of the disease to conrm
any results obtained at this time. Similarly, results
obtained after antibiotic treatment were not considered in this work which could cause false negatives
or antibody titres that were too low to be identied by
MAT for comparison.
To determine the efcacy of Leptorapide as a
rapid screening test in an endemic region, sera was
obtained from patients with pyrexia of unknown
origin submitted to the Centre for Zoonoses, in the
southern Brazilian state of Rio Grande de Sul.
A panel (n = 168) of MAT seropositive samples (titre
51/100) was acquired. Although the MAT is the
current gold-standard test for leptospirosis, it cannot
differentiate between acute, ongoing infection and
previous convalescent infection [18, 19]. Ribeiro
et al. [20] reported that IgM-detecting ELISAs were
more sensitive than MAT in detection of the acute
phase of the disease in humans. Concomitant with
this nding, results show that the IgM ELISA and
Leptorapide detected a similar proportion of positive
samples in the panel; 66/168 samples testing positive
with IgM ELISA and 87/168 samples testing positive
with Leptorapide. With both the IgM ELISA and
Leptorapide detecting a similar degree of positivity
in the samples, this suggests that the MAT cannot
be used to correctly diagnose acute disease. The ability
of Leptorapide to detect a greater proportion of positive samples than the IgM ELISA may indicate a
greater sensitivity inherent in Leptorapide, which
could in turn be due to its dependence on IgM and
high-afnity IgG to work. Forty-ve of 168 of
the MAT-positive sera were deemed negative by
Leptorapide and 36/168 samples produced an
inconclusive result. These samples may represent individuals with a previous convalescent infection containing signicant levels of antibody isotypes other
than IgM, in accord with Brandao et al. [21].
An independent study funded by the WHO and performed by the ICMR further supports the use of
Leptorapide as a screening test in an endemic region.
Leptorapide was deemed the most accurate of four
rapid tests validated (Vijayachari et al., unpublished
data, 2008). In particular, Leptorapide was extremely
efcient at diagnosis after 1 week of onset of symptoms. Taken together, results from validation on clinical submissions suggest the suitability of Leptorapide
as a rapid and accurate screening test during an epidemic. When considering the reduced sensitivity of
the Leptorapide latex agglutination test, especially in
these sub-tropical regions of the world where seronegative samples were conrmed on suspect cases, it
should be noted that leptospirosis symptoms mimic
those of many other infectious disease which would
be common to sub-tropical regions of the world
such as hantavirus, dengue and malaria. The lower
sensitivity of Leptorapide in these areas could be
explained by hantavirus infections where all symptoms of leptospirosis are present except haemoptysis,
thereby resulting in a misdiagnosis of Leptospira infection and failure of antibiotic treatment in these
patients.
We have described the suitability of Leptorapide
as a rapid screening test for diagnosis of leptospirosis.
The assay has been validated with a large sample size
obtained from individuals originating from various
parts of the world; demonstrating the ability of
Leptorapide to detect a wide range of globally distributed serovars. The main advantages of the assay
are that it can be performed without the use of specialized equipment by untrained personnel, results are
obtained within minutes and it corresponds well in
comparison to the MAT in terms of its sensitivity
and specicity. Thus, Leptorapide is a valuable tool
for rapid diagnosis of the disease, particularly in endemic regions that frequently cannot rely on adequate
medical support.
S U P P L E M E N TA RY M AT E R I A L
For supplementary material accompanying this paper
visit http://dx.doi.org/10.1017/S0950268813002112.
T. Brownlow and others
AC KN OWL ED GE MEN T S
The authors thank the staff at the Leptospirosis
Reference Unit, Hereford, UK for providing the
serum samples.
D E C L A R ATI O N O F I N T E R E S T
None.
R E F E RE NC E S
1. Vijayachari P, Sugunan AP, Shriram AN. Leptospirosis:
an emerging global public health problem. Journal of
Biosciences 2008; 33: 557569.
2. Victoriano AF, et al. Leptospirosis in the Asia Pacic
region. BioMed Central Infectious Diseases. Published
online 4 September 2009. doi:10.1186/1471-2334-9-147.
3. Pappas G, et al. The globalization of leptospirosis:
worldwide incidence trends. International Journal of
Infectious Diseases 2008; 12: 351357.
4. WHO. Leptospirosis worldwide. Weekly Epidemiological Record 1999; 74: 237242.
5. Adler B, de la Pena Moctezuma A. Leptospira and leptospirosis. Veterinary Microbiology 2010; 140: 287296.
6. Karaseva EV, Chernukha YG, Piskunova LA. Results of
studying the time of survival of pathogenic leptospira
under natural conditions. Journal of Hygiene, Epidemiology, Microbiology and Immunology 1973; 17:
339345.
7. Ganoza CA, et al. Asymptomatic renal colonization of
humans in the peruvian Amazon by Leptospira. PLoS
Neglected Tropical Diseases 2010; 4: 612.
8. Trueba G, et al. Cell aggregation: a mechanism of
pathogenic Leptospira to survive in fresh water. International Microbiology 2004; 7: 3540.
9. Benschop J, et al. Seroprevalence of leptospirosis
in workers at a New Zealand slaughterhouse. New
Zealand Medical Journal 2009; 122: 3947.
10. Levett PN. Leptospirosis. Clinical Microbiology Reviews
2001; 14: 296326.
11. Dolhnikoff M, et al. Pathology and pathophysiology
of pulmonary manifestations in leptospirosis. Brazilian
Journal of Infectious Diseases 2007; 11: 142148.
12. de Albuquerque Filho AP, et al. Validation of a case
denition for leptospirosis diagnosis in patients with
acute severe febrile disease admitted in reference hospitals at the State of Pernambuco, Brazil. Revista da
Sociedade Brasileira de Medicina Tropical 2011; 44:
735739.
13. Smythe LD, et al. The microscopic agglutination
test (MAT) is an unreliable predictor of infecting
Leptospira serovar in Thailand. American Journal of
Tropical Medicine and Hygiene 2009; 81: 695697.
14. Ahmad SN, Shah S, Ahmad FM. Laboratory diagnosis
of leptospirosis. Journal of Postgraduate Medicine,
2005; 51: 195200.
15. Wolff JW. The Laboratory Diagnosis of Leptospirosis.
The University of Michigan: C. C. Thomas, 1954.
16. Palmer MF, Waitkins SA, Wanyangu SW. A comparison of live and formalised leptospiral microscopic
agglutination test. Zentralblatt fur Bakteriologie,
Mikrobiologie, und Hygiene. Series A, Medical Microbiology, Infectious Diseases, Virology, Parasitology
1987; 265: 151159.
17. Zochowski WJ, Palmer MF, Coleman TJ. An evaluation of three commercial kits for use as screening
methods for the detection of leptospiral antibodies in
the UK. Journal of Clinical Pathology 2001; 54: 2530.
18. Pappas MG, et al. Rapid serodiagnosis of leptospirosis
using the IgM-specic Dot-ELISA: comparison with
the microscopic agglutination test. American Journal
of Tropical Medicine and Hygiene 1985; 34: 346354.
19. Winslow WE, et al. Evaluation of a commercial enzymelinked immunosorbent assay for detection of immunoglobulin M antibody in diagnosis of human leptospiral
infection. Journal of Clinical Microbiology 1997; 35:
19381942.
20. Ribeiro MA, Souza CC, Almeida SH. Dot-ELISA
for human leptospirosis employing immunodominant
antigen. American Journal of Tropical Medicine and
Hygiene 1995; 98: 452456.
21. Brandao AP, et al. Macroscopic agglutination test for
rapid diagnosis of human leptospirosis. Journal of
Clinical Microbiology 1998; 36: 31383142.
Vous aimerez peut-être aussi
- Evaluation of Real-Time PCR and Culturing For The Detection of Leptospires in Canine SamplesDocument9 pagesEvaluation of Real-Time PCR and Culturing For The Detection of Leptospires in Canine SamplesraviggPas encore d'évaluation
- A Quantitative PCR (Taqman) Assay For Pathogenic: Leptospira SPPDocument22 pagesA Quantitative PCR (Taqman) Assay For Pathogenic: Leptospira SPPVigneshwaran RavishankarPas encore d'évaluation
- Evaluation of qPCR-Based Assays For Leprosy Diagnosis Directly in Clinical SpecimensDocument8 pagesEvaluation of qPCR-Based Assays For Leprosy Diagnosis Directly in Clinical SpecimenszemanesilvaPas encore d'évaluation
- Diagnosis and Treatment of Human Salmonellosis inDocument8 pagesDiagnosis and Treatment of Human Salmonellosis inRajihaPas encore d'évaluation
- The Use of Levofloxacin in A Patient With Leptospirosis (#610928) - 793160Document2 pagesThe Use of Levofloxacin in A Patient With Leptospirosis (#610928) - 793160Emmanuel MorilloPas encore d'évaluation
- Streptococcus Pneumoniae Carriage, Resistance and Serotypes Among Jordanian Children From Wadi Al Seer District, JordanDocument8 pagesStreptococcus Pneumoniae Carriage, Resistance and Serotypes Among Jordanian Children From Wadi Al Seer District, JordanInternational Medical PublisherPas encore d'évaluation
- 10126-Article Text-75914-1-10-20181208Document5 pages10126-Article Text-75914-1-10-20181208Odessa EnriquezPas encore d'évaluation
- Clinico - Seroepidemiological Evaluation of Toxocariasis in Asthmatic Pediatric Children in Mansoura City in EgyptDocument5 pagesClinico - Seroepidemiological Evaluation of Toxocariasis in Asthmatic Pediatric Children in Mansoura City in EgyptInternational Medical PublisherPas encore d'évaluation
- Prospective Evaluation of Three Rapid Diagnostic Tests For Diagnosis of Human LeptospirosisDocument21 pagesProspective Evaluation of Three Rapid Diagnostic Tests For Diagnosis of Human LeptospirosisRio Gusta NotarioPas encore d'évaluation
- LeptospirosisDocument8 pagesLeptospirosisSanda Puspa RiniPas encore d'évaluation
- WFVSDCSVSFDocument7 pagesWFVSDCSVSFmuscadomPas encore d'évaluation
- Role of Widal Test in The Diagnosis of Typhoid Fever in Context To Other TestDocument3 pagesRole of Widal Test in The Diagnosis of Typhoid Fever in Context To Other TestDrashua AshuaPas encore d'évaluation
- Comparative Study of Typhidot-M With Widal and Blood Culture in Diagnosis of Enteric FeverDocument4 pagesComparative Study of Typhidot-M With Widal and Blood Culture in Diagnosis of Enteric FeverPranay BhosalePas encore d'évaluation
- Jurnal 2Document16 pagesJurnal 2grace liwantoPas encore d'évaluation
- Detection of Typhoid CarriersDocument6 pagesDetection of Typhoid CarriersClarestaPas encore d'évaluation
- Clinico - Seroepidemiological Evaluation of Toxocariasis in Asthmatic Pediatric Children in Mansoura City in EgyptDocument5 pagesClinico - Seroepidemiological Evaluation of Toxocariasis in Asthmatic Pediatric Children in Mansoura City in EgyptInternational Medical PublisherPas encore d'évaluation
- l36 B Met Syphillis Rapid Plasma Reagin PDFDocument17 pagesl36 B Met Syphillis Rapid Plasma Reagin PDFkath celenriquezPas encore d'évaluation
- Pathogens 12 00135Document12 pagesPathogens 12 00135Isa Andrea Aro TarquiPas encore d'évaluation
- Journal of Infection and Public HealthDocument7 pagesJournal of Infection and Public HealthFajar Cah BumiayuPas encore d'évaluation
- Rapid Test Detects SyphilisDocument17 pagesRapid Test Detects SyphilisMeta ParamitaPas encore d'évaluation
- Salmonellosis Research PaperDocument5 pagesSalmonellosis Research PaperxkcwaaqlgPas encore d'évaluation
- 268 Ijar-3708Document4 pages268 Ijar-3708SHIVA JYOTHIPas encore d'évaluation
- Research ArticleDocument6 pagesResearch ArticleTRI GUMILARPas encore d'évaluation
- Jurnal 2Document12 pagesJurnal 2zingioPas encore d'évaluation
- 3 - Indentify Serotype DengueDocument11 pages3 - Indentify Serotype DengueBùi Thanh TùngPas encore d'évaluation
- Sensitivity and Specificity of Typhoid Fever Rapid Antibody Tests For Laboratory Diagnosis at Two Sub-Saharan African SitesDocument9 pagesSensitivity and Specificity of Typhoid Fever Rapid Antibody Tests For Laboratory Diagnosis at Two Sub-Saharan African SitesAde SupraptoPas encore d'évaluation
- Carraro 2013 RSBMTV 46 N 2 P 161Document5 pagesCarraro 2013 RSBMTV 46 N 2 P 161Emerson CarraroPas encore d'évaluation
- Jurnal HibridisasiDocument12 pagesJurnal HibridisasiNurfanida Natasya mPas encore d'évaluation
- 2 C PDFDocument14 pages2 C PDFAvisena AzisPas encore d'évaluation
- Comparative Analysis of Severe Pediatric and Adult Leptospirosis in Sa o Paulo, BrazilDocument3 pagesComparative Analysis of Severe Pediatric and Adult Leptospirosis in Sa o Paulo, BrazilShofura AzizahPas encore d'évaluation
- Accuracy of A Commercial Igm Elisa For The Diagnosis of Human Leptospirosis in ThailandDocument4 pagesAccuracy of A Commercial Igm Elisa For The Diagnosis of Human Leptospirosis in Thailandrestu anindityaPas encore d'évaluation
- Bulletin of The World Health OrganizationDocument11 pagesBulletin of The World Health OrganizationJohn LewandowskiPas encore d'évaluation
- Molecularapproachesand Biomarkersfordetectionof MycobacteriumtuberculosisDocument14 pagesMolecularapproachesand Biomarkersfordetectionof MycobacteriumtuberculosischiralicPas encore d'évaluation
- Clinical Value of Serology For The Diagnosis of Strongyloidiasis in Travelers and Migrants - A 4-Year Retrospective Study Using The Bordier IVD Strongyloides Ratti ELISA AssayDocument10 pagesClinical Value of Serology For The Diagnosis of Strongyloidiasis in Travelers and Migrants - A 4-Year Retrospective Study Using The Bordier IVD Strongyloides Ratti ELISA Assaygwyneth.green.512Pas encore d'évaluation
- Laboratory Features of Systemic Lupus Erythematosus (SLE)Document6 pagesLaboratory Features of Systemic Lupus Erythematosus (SLE)AmrKamalPas encore d'évaluation
- Review of Literature On Mycobacterium Tuberculosis Test ElisaDocument6 pagesReview of Literature On Mycobacterium Tuberculosis Test ElisajicjtjxgfPas encore d'évaluation
- Toxins: Venomous Arachnid Diagnostic Assays, Lessons From Past AttemptsDocument26 pagesToxins: Venomous Arachnid Diagnostic Assays, Lessons From Past Attemptskamila auliyaPas encore d'évaluation
- Review 01-06 PDFDocument6 pagesReview 01-06 PDFEditor IjprtPas encore d'évaluation
- Faring It IsDocument8 pagesFaring It IsMuhammad sukronPas encore d'évaluation
- Efficiency of Direct Microscopy of Stool Samples Using An Antigen-Specific Adhesin Test For Entamoeba HistolyticaDocument5 pagesEfficiency of Direct Microscopy of Stool Samples Using An Antigen-Specific Adhesin Test For Entamoeba HistolyticaNoraine Princess TabangcoraPas encore d'évaluation
- Validity of CSF Tests for Diagnosing Tuberculous MeningitisDocument5 pagesValidity of CSF Tests for Diagnosing Tuberculous MeningitismelisaberlianPas encore d'évaluation
- High Dose Corticosteroids in Severe LeptospirosisDocument8 pagesHigh Dose Corticosteroids in Severe Leptospirosisdiego antonio ordorica alaminaPas encore d'évaluation
- SeroDocument15 pagesSeroSaid IsaqPas encore d'évaluation
- Modern Techniques in Diagnostic Parasitology 4-2-2015Document62 pagesModern Techniques in Diagnostic Parasitology 4-2-2015dinahzaqoutPas encore d'évaluation
- Leptospirosis JournalDocument5 pagesLeptospirosis JournalNoviana DewiPas encore d'évaluation
- Comparing Widal and ELISA Tests for Diagnosing Typhoid Fever in Iraqi PatientsDocument6 pagesComparing Widal and ELISA Tests for Diagnosing Typhoid Fever in Iraqi PatientsMildred MontPas encore d'évaluation
- Lepto SpirosDocument8 pagesLepto SpirosNisa UcilPas encore d'évaluation
- Jurnal Biologi MolekulerDocument4 pagesJurnal Biologi MolekulerScorpyo Ainun Schulerin'detektive Al-BikelPas encore d'évaluation
- Diagnosis and Treatment of Typhoid Fever and Associated PrevailingDocument7 pagesDiagnosis and Treatment of Typhoid Fever and Associated Prevailing073090Pas encore d'évaluation
- Value of Single Widal Test in Children For Diagnosis of Typhoid FeverDocument5 pagesValue of Single Widal Test in Children For Diagnosis of Typhoid FeverArdita FaradhikaPas encore d'évaluation
- International Journal of Infectious DiseasesDocument7 pagesInternational Journal of Infectious DiseasesyurikaPas encore d'évaluation
- Epidemiology of Plasmodium Infections in Flores Island, Indonesia Using Real-Time PCRDocument9 pagesEpidemiology of Plasmodium Infections in Flores Island, Indonesia Using Real-Time PCRTeuku M Arief YaminPas encore d'évaluation
- 3.evaluation of DFM, Isolation - IJPBS-July 2012Document5 pages3.evaluation of DFM, Isolation - IJPBS-July 2012SHIVA JYOTHIPas encore d'évaluation
- Evaluation of A Blocking ELISA For The Detection of Antibodies Against Lawsonia Intracellularis in Pig SeraDocument6 pagesEvaluation of A Blocking ELISA For The Detection of Antibodies Against Lawsonia Intracellularis in Pig SeraBima Jalu AtmajaPas encore d'évaluation
- Cathelicidin Level in Less in ARDocument6 pagesCathelicidin Level in Less in ARvishdubey777Pas encore d'évaluation
- Persistence and Complex Evolution of Fluoroquinolone-Resistant Streptococcus Pneumoniae CloneDocument7 pagesPersistence and Complex Evolution of Fluoroquinolone-Resistant Streptococcus Pneumoniae CloneMark ReinhardtPas encore d'évaluation
- Quantification of Demodex Folliculorum by PCR in RosaceaDocument6 pagesQuantification of Demodex Folliculorum by PCR in RosaceaRoxana SurliuPas encore d'évaluation
- AsoDocument10 pagesAsoDiah WahyuniPas encore d'évaluation
- Role of Widal Test in The Diagnosis of Typhoid Fever in Context To Other TestDocument3 pagesRole of Widal Test in The Diagnosis of Typhoid Fever in Context To Other TestsimbawulaPas encore d'évaluation
- Fungal Enzymes For Environmental Management: SciencedirectDocument11 pagesFungal Enzymes For Environmental Management: SciencedirectsoultansimamoraPas encore d'évaluation
- GE AnswersDocument1 pageGE Answersvignesh9489Pas encore d'évaluation
- Handbook of COVID-19 Prevention and Treatment (Compressed)Document68 pagesHandbook of COVID-19 Prevention and Treatment (Compressed)Vanessa SánchezPas encore d'évaluation
- Corynebacterium SPP, PDFDocument7 pagesCorynebacterium SPP, PDFanggaririnPas encore d'évaluation
- 4 261650026147611555 PDFDocument9 pages4 261650026147611555 PDFvignesh9489Pas encore d'évaluation
- 4 261650026147611586 PDFDocument19 pages4 261650026147611586 PDFvignesh9489Pas encore d'évaluation
- Haemophilus InfluenzaeDocument20 pagesHaemophilus Influenzaevignesh9489Pas encore d'évaluation
- 4 261650026147611555 PDFDocument9 pages4 261650026147611555 PDFvignesh9489Pas encore d'évaluation
- Erysipelothrix Rhusiopathiae: Molecular Medical Microbiology. DOI: © 2015 Elsevier Ltd. All Rights ReservedDocument14 pagesErysipelothrix Rhusiopathiae: Molecular Medical Microbiology. DOI: © 2015 Elsevier Ltd. All Rights Reservedvignesh9489Pas encore d'évaluation
- Haemophilus Ducreyi: Chancroid: EpidemiologyDocument11 pagesHaemophilus Ducreyi: Chancroid: Epidemiologyvignesh9489Pas encore d'évaluation
- Enterotoxin-Producing Staphylococcus AureusDocument17 pagesEnterotoxin-Producing Staphylococcus Aureusvignesh9489Pas encore d'évaluation
- 4 261650026147611533 PDFDocument15 pages4 261650026147611533 PDFvignesh9489Pas encore d'évaluation
- Lec15 PDFDocument47 pagesLec15 PDFvignesh9489Pas encore d'évaluation
- Bacteriology of Periodontal DiseasesDocument12 pagesBacteriology of Periodontal Diseasesvignesh9489Pas encore d'évaluation
- Bacteriology of Periodontal DiseasesDocument12 pagesBacteriology of Periodontal Diseasesvignesh9489Pas encore d'évaluation
- Phosphate BufferDocument1 pagePhosphate BufferAdeel AltuhishPas encore d'évaluation
- Corynebacterium SPP, PDFDocument7 pagesCorynebacterium SPP, PDFanggaririnPas encore d'évaluation
- 4 261650026147611533 PDFDocument15 pages4 261650026147611533 PDFvignesh9489Pas encore d'évaluation
- Picard Eau 2017Document22 pagesPicard Eau 2017vignesh9489Pas encore d'évaluation
- What Is DiabetesDocument8 pagesWhat Is DiabetesJessica GintingPas encore d'évaluation
- Gate 2018 Answer Key Architecture and PlanningDocument3 pagesGate 2018 Answer Key Architecture and Planningvignesh9489Pas encore d'évaluation
- Candidemia PDFDocument2 pagesCandidemia PDFRavi GulatiPas encore d'évaluation
- Lesson 15Document13 pagesLesson 15Mystical MagicPas encore d'évaluation
- School RepresentativesDocument4 pagesSchool Representativesvignesh9489Pas encore d'évaluation
- E.coli Expression SystemsDocument36 pagesE.coli Expression SystemstarannumPas encore d'évaluation
- Lab Manual For Biochemistry For PTU Students PDFDocument24 pagesLab Manual For Biochemistry For PTU Students PDFvignesh9489Pas encore d'évaluation
- Rummy - RulesDocument3 pagesRummy - RulesvijayPas encore d'évaluation
- Qualitative Test of Lipids IIDocument18 pagesQualitative Test of Lipids IIManohar Pattar75% (4)
- Entrance Test For M.Sc. (Biotechnology) I May 2L, 2oll IDocument41 pagesEntrance Test For M.Sc. (Biotechnology) I May 2L, 2oll Ivignesh9489Pas encore d'évaluation
- Bio - Technology Volume 10 Issue 12 1992 (Doi 10.1038 - nbt1292-1572) Fett-Neto, Arthur G. DiCosmo, Frank Reynolds, W. F. Sakata, K - Cell Culture of Taxus As A Source of The Antineoplastic Drug TaxDocument4 pagesBio - Technology Volume 10 Issue 12 1992 (Doi 10.1038 - nbt1292-1572) Fett-Neto, Arthur G. DiCosmo, Frank Reynolds, W. F. Sakata, K - Cell Culture of Taxus As A Source of The Antineoplastic Drug Taxvignesh9489Pas encore d'évaluation
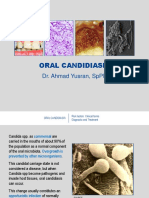
- Oral Candidiasis: Dr. Ahmad Yusran, SPPDDocument87 pagesOral Candidiasis: Dr. Ahmad Yusran, SPPDM Nedi Sevtia BudiPas encore d'évaluation
- Lower Motor Neuron LesionsDocument29 pagesLower Motor Neuron LesionsLoshi ChandrasekarPas encore d'évaluation
- VMD-511 Important PointsDocument11 pagesVMD-511 Important PointsSandeepbissu100% (1)
- A Stag God Is Born Ch6-7Document12 pagesA Stag God Is Born Ch6-7Eka KimPas encore d'évaluation
- Benign Ovarian ConditionsDocument31 pagesBenign Ovarian ConditionsNur Hanani KhanPas encore d'évaluation
- Guide to Therapeutic Plasma ExchangeDocument5 pagesGuide to Therapeutic Plasma ExchangeAnaPas encore d'évaluation
- Spina Bifida: Saba Ramzan Nadia Shoukat Laraib Yasin Anam WarisDocument40 pagesSpina Bifida: Saba Ramzan Nadia Shoukat Laraib Yasin Anam WarislaraibPas encore d'évaluation
- Diagnostic Laboratory TestsDocument6 pagesDiagnostic Laboratory TestsKiana Mae Wong Diwag100% (1)
- Urethral Thickness in DogsDocument9 pagesUrethral Thickness in DogsGabriellaPas encore d'évaluation
- Thoracic Trauma TreatmentDocument77 pagesThoracic Trauma TreatmentAnonymous GsvDOlQuSPas encore d'évaluation
- Blood LecturesDocument128 pagesBlood LecturessrhrenaissancePas encore d'évaluation
- Dexter, Susan - Herding InstinctDocument8 pagesDexter, Susan - Herding InstinctMata Bana Najou0% (1)
- Full Download Test Bank For Comprehensive Radiographic Pathology 6th Edition by Eisenberg PDF Full ChapterDocument36 pagesFull Download Test Bank For Comprehensive Radiographic Pathology 6th Edition by Eisenberg PDF Full Chapterdiesnongolgothatsczx100% (13)
- Commentary On The Hindu System of Medicine 1000273526Document471 pagesCommentary On The Hindu System of Medicine 1000273526adiseifPas encore d'évaluation
- Uterine Blood Flow During Supine Rest and Exercise in Late PregnancyDocument9 pagesUterine Blood Flow During Supine Rest and Exercise in Late PregnancyMD Luthfy LubisPas encore d'évaluation
- Severe of Stenosis Unfavor: Carotid A Stenosis Carotid Angioplasty + StentingDocument14 pagesSevere of Stenosis Unfavor: Carotid A Stenosis Carotid Angioplasty + StentingURo Kku100% (1)
- Rectal ExaminationDocument21 pagesRectal ExaminationAlexandra HornariuPas encore d'évaluation
- Ch.8 - Axial & Appendicular SkeletonDocument72 pagesCh.8 - Axial & Appendicular SkeletonMeganPas encore d'évaluation
- Alteration in Endocrine SystemDocument215 pagesAlteration in Endocrine Systemyen1988100% (1)
- Understanding The Contact Tracing Reporting TemplateDocument51 pagesUnderstanding The Contact Tracing Reporting TemplateAlvin Lee Cucio AsuroPas encore d'évaluation
- FESBE Apresentados - SextaDocument601 pagesFESBE Apresentados - SextaVanessa MirandaPas encore d'évaluation
- One Word PDFDocument15 pagesOne Word PDFneeta chandPas encore d'évaluation
- General Medicine MCQDocument11 pagesGeneral Medicine MCQsami1218100% (3)
- Mtemi Dedan - Poems - : Poetry SeriesDocument35 pagesMtemi Dedan - Poems - : Poetry SeriesNosfe Matingli DiazPas encore d'évaluation
- General Arrangement of The Abdominal ViserasDocument14 pagesGeneral Arrangement of The Abdominal ViserasShimmering MoonPas encore d'évaluation
- 04 Bahas Inggris Paket 4Document9 pages04 Bahas Inggris Paket 4Aji PangestuPas encore d'évaluation
- Anti-FTO Antibody (EPR6894) Ab126605: 6 ImagesDocument4 pagesAnti-FTO Antibody (EPR6894) Ab126605: 6 Imageshorace35Pas encore d'évaluation
- Naval Medical Research Center: 503 Robert Grant Ave. Silver Spring, MDDocument2 pagesNaval Medical Research Center: 503 Robert Grant Ave. Silver Spring, MDthe brainburnerPas encore d'évaluation
- Pubic Health SurvilanceDocument28 pagesPubic Health Survilanceteklay100% (1)
- Chapter 1: Transport: Prepared By: Ling Mei TengDocument21 pagesChapter 1: Transport: Prepared By: Ling Mei TengJuliet LingPas encore d'évaluation