Académique Documents
Professionnel Documents
Culture Documents
Antiarrhythmic Drugs
Transféré par
Uma Mouna0 évaluation0% ont trouvé ce document utile (0 vote)
103 vues10 pagespharmac
Copyright
© © All Rights Reserved
Formats disponibles
DOCX, PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentpharmac
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
103 vues10 pagesAntiarrhythmic Drugs
Transféré par
Uma Mounapharmac
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 10
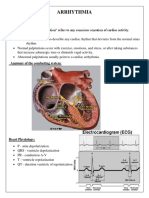
ANTIARRHYTHMIC DRUGS and propagates to the rest of
(AADs) the heart-PACEMAKER
CONTENT v. Other automatic fibers
Physiology of normal cardiac have slower phase-4
rhythm depolarization- receive
Definition and mechanisms impulse from SAN.
of arrhythmias vi. Latent pacemakers
Classification of drugs to BASIC CARDIAC
treat arrhythmias ELECTROPHYSIOLOGY
Important anti-arrhythmic 2. Conduction
drugs (mechanism and A more completely
pharmacological polarized membrane
characteristics) depolarizes faster because
more Na+ channels have
BASIC CARDIAC recovered (voltage
ELECTROPHYSIOLOGY -dependent reactivation):
1. Impulse generation seen in atrial, ventricular
Nonautomatic myocardial and Purkinje fibers
fibers cannot generate an SAN and AVN remain
impulse on their own. refractory for sometime:
Resting membrane potential Ca2+ channel reactivation is
(RMP) is -90mv time-dependent
Automatic fibers in SA and Purkinje fibers have highest
nodes, His-Purkinje system. conduction velocity
Phase-4 or slow diastolic BASIC CARDIAC
depolarization: Sudden ELECTROPHYSIOLOGY
depolarization occurs 3. Excitability: strength of
spontaneously. stimulus required to produce an
BASIC CARDIAC action potential (AP)
ELECTROPHYSIOLOGY Hyperpolarization decreases
iv. SA node (SAN) has the excitability
steepest phase-4 Decrease in RMP increases
depolarization, self-excitatory excitability
BASIC CARDIAC to spread across the
ELECTROPHYSIOLOGY myocardium
4. Refractory period.
Effective refractory period PHASES OF ACTION
(ERP): Minimum interval POTENTIAL OF CARDIAC
between two APs. CELLS
ERP is closely related to Phase 0 rapid depolarisation
APD (inflow of Na+)
ERP/APD is <1 in fast Phase 1 partial repolarisation
channel fibers (Na+ (inward Na+ current
channels) deactivated, outflow of K+)
ERP/APD is > in slow Phase 2 plateau (slow inward
channel fibers (Ca2+ calcium current)
channels Phase 3 repolarisation (calcium
Most antiarrhythmic drugs current inactivates, K+ outflow)
increase ERP/APD ratio Phase 4 pacemaker potential
(Slow Na+ inflow, slowing of K+
outflow) autorhythmicity
Refractory period (phases 1-3)
045 The Pacemaker Potential of
PHYSIOLOGY OF CARDIAC the SA Node and the AV
RATE AND RHYTHM Node.mp4
Cardiac myocytes are
electrically excitable SINUS RHYTHM
Resting intracellular voltage of
myocardial cells is negative Sinoatrial rate controlled by
-90mV (SA node is -40mV) autonomic nervous system
Resting state - K+ inside and Parasympathetic system
Na+ outside cell (Na+/K+ pump) predominates (M2 muscarinic
Action potential occurs when receptors)
Na+ enters the cell and sets up a Sympathetic system (1 receptors)
depolarising current Increased heart rate (positive
Stimulation of a single muscle chronotropic effect)
fibre causes electrical activity Increased automaticity
Facilitation of conduction of
AV node Mechanisms of dysrhythmias
DEFINITION OF Increased/ectopic pacemaker
ARRHYTHMIA activity
Cardiac arrhythmia is an After-depolarizations: Early
abnormality of the heart rhythm after-depolarization (EAD)
Bradycardia heart rate slow Delayed after-depolarization
(<55-60 beats/min) (DAD)
Tachycardia heart rate fast (>100 3. Reentry
beats/min) Circus movement reentry
CLINICAL CLASSIFICATION Functional reentry
OF ARRHYTHMIAS Fractionation of impulse
Heart rate (increased/decreased) MECHANISMS OF
Heart rhythm (regular/irregular) ARRHYTHMIA PRODUCTION
Site of origin (supraventricular / Re-entry (refractory tissue
ventricular) reactivated due to conduction
Complexes on ECG block, causes abnormal continuous
(narrow/broad) circuit; eg accessory pathways
ANTIARRHYTHMIC DRUGS linking atria and ventricles in
Antiarrhythmic drugs are Wolff-Parkinson-White syndrome)
used to prevent or treat Abnormal pacemaker activity in
abnormal cardiac rhythms. non-conducting/conducting tissue
Abnormal automaticity, (eg ischemia)
impaired conduction or both Delayed after-depolarisation
cause cardiac dysrhythmias. (automatic depolarisation of
Cardiac dysrhythmias cardiac cell triggers ectopic beats,
Causes: can be caused by drugs; eg
Ischemia digoxin)
Electrolyte & pH imbalance
Mechanical injury Important cardiac dysrhythmias
Stretching (CHF) Extrasystoles [ES]:
Neurogenic premature ectopic beats from
Drugs, including AADs an ectopic focus in atrium,
AV node or ventricle
PSVT: atrial tachycardia Third degree: Complete
(150-200/min) heart block. Ventricle
Atrial flutter: 200-350/min. generates own impulses
AV node cannot transmit Cardiac Dysrhythmia
impulses faster than 200/min Heartbeat Dances.mp4
Atrial fibrillation: 350-550/ Classification of AADs: Based on
min, asynchronous their effects on AP (Singh &
Ventricular tachycardia: 4 Williams)
or more consecutive Class I (membrane
ventricular extrasystoles stabilizers):Na+ channel blockers
Important cardiac dysrhythmias These AADs slow the rate of
6. Torsades de pointes: raise of phase 0
Polymorphic ventricular of AP by inhibiting fast sodium
tachycardia, asynchronous channels.
complexes The class is subdivided
7. Ventricular fibrillation: according to the
Uncoordinated contraction of effects of drugs on the duration of
ventricular fibers with loss of AP.
pumping function. Indications: SV and
Death within 2-5 mins. Most ventricular arrhythmias.
common cause of sudden
cardiac death Class I (membrane stabilizers)
Important cardiac dysrhythmias
8. A-V block: Depressed impulse Quinidine Lignocaine
conduction through AVN and Flecainide
bundle of His. Procainamide Phenytoin
First degree: Prolonged P- Propafenone
R interval Disopyramide Mexilitine
Second degree: Some Tocainide
supraventricular complexes
are not conducted: drop Class II (-adrenoceptor
beats antagonists)
Reduce the rate
of spontaneous depo-
larization of sinus Class II: -adrenoceptor
and AV nodal tissue antagonists (atenolol, sotalol)
Indications: SV and Class III: prolong action
ventricular arrhythmias. potential and prolong refractory
period (suppress re-entrant
Propranolol, sotalol, rhythms) (amiodarone,
esmolol dronedarone, sotalol)
Class IV: Calcium channel
Class III antagonists. Impair impulse
propagation in nodal and
These AADs prolong
damaged areas (verapamil)
the duration of the AP
Mechanism of Action of
and increase the abso-
Antiarrhythmic Drugs.mp4
lute refractory period.
This is the result of
block of K+ channels
Other drugs used in
Ind: SV and ventri- tachyarrhythmias
Amiodarnone, dronedarnone,
cular arrhythmias. Adenosine inhibits AV conduction.
dofetilide, ibutilide The duration of effect is less than
60 s.Used as an i.v. bolus in SV
Class IV (CCBs) tachycardia with narrow QRS
complex.
SINGH &WILLIAMS ADRs: bradycardia, AV
CLASSIFICATION OF block.
ANTIARRHYTHMIC DRUGS Digoxin reduces conduction
Class I: block sodium channels through the AV node and is useful
Ia (quinidine, in the control of atrial flutter, atrial
procainamide, fibrillation and PSVT
disopyramide) AP AADs used in bradyarrhythmias
Ib (lidocaine, mexiletine, Atropine is given by bolus
phenytoin) AP i.v. inj. in sinus brady-
Ic (flecainide, propafenone) cardia and AV block. It blocks
AP M2-receptors and
increases conduction through the No effect on AP of atrial
AV node. fibers (short duration of
Isoprenaline is used in AV block inactive Na+ channels).
Class IA:Procainamide No effective in treating
Orally active amide form of atrial and SVTs
procaine PKE: Orally ineffective,
MOA: given IV, action lasts for 10-
Blocks open Na+ channels 20 mins
Reduces automaticity Class IB:Lignocaine
Slows phase 0 depolarization ADRs
Prolongs APD, ERP, QRS CNS: Drowsiness,
complex and Q-T interval parasthesias, disorientation,
PKE: Oral, IV. Acetylation in nystagmus, twitchings and
liver. convulsions
Rapid and slow acetylators CVS: Hypotension and
Class IA:Procainamide cardiac depression
ADRs: Uses:
Cardiac: Hypotension, VT
torsades de pointes Prevent VF
Rash, fever, angioedema Selected cases of MI to
SLE with long term use, prevent VF
especially in slow Digitalis-induced VTs
acetylators Difference between
Uses: Occasionally to lignocaine for VT and LA
terminate VT and SVT.
Class IB:Lignocaine Class IC: Propafenone
MOA: MOA:
Blocks inactive Na+ channels Blocks Na+ channels
( use-dependent)Voltage Depresses impulse
Gated Channels.flv transmission in HP and
Suppresses automaticity of accessory pathways (WPW)
ectopic foci Prolongs APD
Decreases APD in PF and blocking property
ventricular muscle PKE: Oral
ADRs: Blurred vision, bitter IV to terminate torsades de
taste, nausea, vomiting, pointes
constipation, CHF & Sotalol
bronchospasm MOA:Non-selective -
Propafenone blocker, with Class III
Uses actions: Blocks inward
Prophylaxis and treatment of rectifier K+ channels
VTs Delays A-V conduction,
Reentrant tachycardias prolongs ERP
To maintain sinus rhythm in ADRs
AF Uses:
Class II Propranolol Polymorphic VTs
MOA: Non-selective - WPW arrhythmias
blocker with membrane To maintain sinus rhythm in
stabilizing activity. No ISA AF/AFl
Decreases slope of phase-4
depolarization and
automaticity in SAN, PF and Esmolol
ectopic foci, when due to MOA: Ultrashort acting
increased sympathetic cardioselective -blocker
activity without ISA/MSA
Prolongs ERP of AVN Given IV, t1/2 < 10 mins
Reentrant impulses through Uses:
AVN are abolished To terminate SVTs
ECG: prolongs PR interval Episodic AF/Afl
Propranolol Arrhythmia during anesthesia
ADRs: Early treatment of MI
Uses: During and after cardiac
Sinus tachycardia surgery- to reduce HR and
Atrial and nodal ESs BP
Prevent PSVT Class III
Pheochromocytoma Prolong phase-3
Halothane induced Widen AP
dysrhythmias Increases ERP
Terminates reentrant Hypotension, bradycardia,
arrhythmias myocardial depression
Class III: Amiodarone (Iodine Photosensitization
containing) Corneal microdeposits-
MOA: reversible o discontinuation
Blocks delayed rectifier K+ Pulmonary fibrosis &
channels : APD and Q-T alveolitis
prolonged Peripheral neuropathy
Blocks inactive Na+ Inhibits peripheral T4 to T3
channels: conversion
Partial L-type CCB activity Hypo/ hyperthyroidism
Partial -blocker activity
I.V injection causes Dronedarone
myocardial depression and Noniodinated congener of
hypotension amiodarone
Amiodarone MOA: Similar to amiodarone
PKE: Action is delayed on Uses: To maintain sinus
oral administration: rhythm in
Accumulation in muscle and SVTs, PSVT
fat AF/ Afl
t1/2: 3-8 weeks ADRs: Bradycardia,
Uses: weakness, cough, skin
VTs, SVTs, PSVT reactions,
AF, AFl No risk of Pulmonary fibrosis
Resistant & recurrent VF & alveolitis
WPW tachyarrhythmia Neuropathy, hypo/
Broad spectrum , long hyperthyroidism
duration & less
prodysrhythmogenic
potential
Dofetilide
Pure Class III
Amiodarone
ADRs:
MOA: Blocks delayed MOA
rectifier K+ channels : APD Effects
and ERP prolonged Uses:
No action on other receptors To control ventricular rate in
Uses: TO maintain sinus AF/AFl: Given I.V
rhythm in converted patients Preferred to verapamil: Less
of AF & AFl hypotension, cardiac
ADRs: Headache, dizziness, depression, better dose
nausea, rarely allergic skin titration, can be used in
reactions presence of mild-to-
Class IV: CCBs moderate CHF
Verapamil ADRs:
MOA: Blocks L-type Ca2+ Drugs used in tachyarrhythmias
channels Adenosine
Negative inotropic MOA:
SAN automaticity is reduced: Via A1 receptors it activates
Bradycardia ACh sensitive K+ channels on
AV nodal ERP is prolonged: SAN, AVN and atrium
reentry terminated Depresses SAN activity,
Given I.V., oral slows AV conduction and
ADRs: Bradycardia, nausea, atrial excitability
constipation, heart block. Also reduces Ca2+ current in
D/I: -blockers, digoxin AVN
Reduced AVN conduction is
Class IV: CCBs responsible for terminating
Verapamil PSVTs
Uses: Adenosine
AF/AFl
PSVT Given rapid I.V
Taken up by RBCs and
endothelial cells
t1/2: 10 secs
Class IV: CCBs Advantages in PSVT
Diltiazem 1. Efficacy verapamil
2. Duration of action < 1 min-
ADRs transient Drugs for AV block
3. Can be given in CHF, Implanted cardiac pacemaker
hypotension and with -blockers Atropine:
4. Safe in wide QRS tachycardia When block is due to vagal
(verapamil is C/I) overactivity/ some cases of
5. Effective in patients refractory MI
to verapamil Atropine reduces AV node
ERP and increases
conduction velocity in bundle
Adenosine of His
ADRs: Dyspnoea, chest pain, Atropine I.M
hypotension, flushing, Drugs for AV block
cardiac arrest, bronchospasm Adrenaline, isoprenaline
Other uses: Increase AV conduction and
Diagnosis of AVN shorten ERP in conducting
tachycardia tissues
To induce brief coronary Used temporarily in partial
vasodilatation during and complete heart block till
diagnostic/interventional pacemaker can be implanted
procedures Any questions?
Controlled hypotension
THANK YOU
Vous aimerez peut-être aussi
- Core V - Cardiovascular CoreDocument35 pagesCore V - Cardiovascular CoreMatthew LeiPas encore d'évaluation
- Arrhythmia: PalpitationDocument36 pagesArrhythmia: PalpitationHala BahaaPas encore d'évaluation
- Essential Cardiac Electrophysiology: The Self-Assessment ApproachD'EverandEssential Cardiac Electrophysiology: The Self-Assessment ApproachPas encore d'évaluation
- EKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookD'EverandEKG Interpretation Basics Guide: Electrocardiogram Heart Rate Determination, Arrhythmia, Cardiac Dysrhythmia, Heart Block Causes, Symptoms, Identification and Medical Treatment Nursing HandbookPas encore d'évaluation
- Essential Guide to Antihypertensive DrugsDocument46 pagesEssential Guide to Antihypertensive DrugsClarencePas encore d'évaluation
- Focal Atrial Tachycardia I: Clinical Features, DiagnosisDocument10 pagesFocal Atrial Tachycardia I: Clinical Features, Diagnosisapi-26166949Pas encore d'évaluation
- Basic EP IntervalsDocument13 pagesBasic EP IntervalsdrharoonmohdPas encore d'évaluation
- Mitral RegurgitationDocument10 pagesMitral RegurgitationWalter Saavedra YarlequePas encore d'évaluation
- Mechanisms of Cardiac Arrhythmias From Automatici+Document24 pagesMechanisms of Cardiac Arrhythmias From Automatici+Malar MannanPas encore d'évaluation
- MVR CabgDocument57 pagesMVR CabgRoshani sharmaPas encore d'évaluation
- 4.03 Anti-Arrhythmic Drugs PDFDocument8 pages4.03 Anti-Arrhythmic Drugs PDFKarl ChavezPas encore d'évaluation
- Journal of Arrhythmia - 2022 - Ono - JCS JHRS 2020 Guideline On Pharmacotherapy of Cardiac ArrhythmiasDocument141 pagesJournal of Arrhythmia - 2022 - Ono - JCS JHRS 2020 Guideline On Pharmacotherapy of Cardiac ArrhythmiastochtliPas encore d'évaluation
- CARDIAC ELECTROPHYSIOLOGY AND THE ELECTROCARDIOGRAM - ClinicalKey PDFDocument40 pagesCARDIAC ELECTROPHYSIOLOGY AND THE ELECTROCARDIOGRAM - ClinicalKey PDFMelanie DascăluPas encore d'évaluation
- The Heart: A Dual Pump and Rhythmic MuscleDocument10 pagesThe Heart: A Dual Pump and Rhythmic Muscle22194Pas encore d'évaluation
- CH17 Cardiovascular Assessment - Nk07Document69 pagesCH17 Cardiovascular Assessment - Nk07Abdiel Tobii SanchezPas encore d'évaluation
- Difficult Weaning From Cardiopulmonary Bypass Final Edit LiaDocument41 pagesDifficult Weaning From Cardiopulmonary Bypass Final Edit LiaYuri SadewoPas encore d'évaluation
- Νευρολογία σύνολο απαντήσεωνDocument38 pagesΝευρολογία σύνολο απαντήσεωνCheng Kuao HengPas encore d'évaluation
- Cardiac Action PotentialDocument41 pagesCardiac Action PotentialRadijska Postaja KoprivnicaPas encore d'évaluation
- Heart Failure 2022-2023 First Semester - FinalDocument69 pagesHeart Failure 2022-2023 First Semester - FinalAlaa zayadnehPas encore d'évaluation
- Electrophysiological Foundations of Cardiac Arrhythmias - A Bridge Between Basic Mechanisms and Clinical Electrophysiology (PDFDrive)Document689 pagesElectrophysiological Foundations of Cardiac Arrhythmias - A Bridge Between Basic Mechanisms and Clinical Electrophysiology (PDFDrive)drdpkrimsPas encore d'évaluation
- Plante PacemakersDocument57 pagesPlante Pacemakersdragon66Pas encore d'évaluation
- HUTTDocument25 pagesHUTTdrdj14100% (1)
- DELNIDODocument32 pagesDELNIDOsarwansyahPas encore d'évaluation
- Surgical Aspects of Pulmonary Infections: Kibrom Gebreselassie, MD, FCS-ECSA Cardiovascular and Thoracic SurgeonDocument60 pagesSurgical Aspects of Pulmonary Infections: Kibrom Gebreselassie, MD, FCS-ECSA Cardiovascular and Thoracic SurgeonVincent SerPas encore d'évaluation
- Cardiac Mechanics: With Thad WilsonDocument26 pagesCardiac Mechanics: With Thad WilsonpasambalyrradjohndarPas encore d'évaluation
- Cardiac Output and Hemodynamic MeasurementDocument29 pagesCardiac Output and Hemodynamic Measurementdeepa100% (1)
- Cardiac ElectrophysiologyDocument6 pagesCardiac Electrophysiologyareznik3007Pas encore d'évaluation
- Heart Valve DiseaseDocument67 pagesHeart Valve DiseaseSaba SivaPas encore d'évaluation
- Design and Analysis of A Dual Chamber Cardiac Pacemaker Using VHDL in Biomedical ApplicationDocument3 pagesDesign and Analysis of A Dual Chamber Cardiac Pacemaker Using VHDL in Biomedical ApplicationEditor IJRITCCPas encore d'évaluation
- Pericarditis 65 SlidesDocument65 pagesPericarditis 65 SlidesAtifBhorePas encore d'évaluation
- Cardiac Cycle: Mechanical Event and Their Electrical and Clinical CorrelationDocument28 pagesCardiac Cycle: Mechanical Event and Their Electrical and Clinical Correlationhawas muhammed100% (1)
- ECG InterpretationDocument82 pagesECG InterpretationIin Widya Sari SiregarPas encore d'évaluation
- Neurohormonal Activation in Heart FailureDocument4 pagesNeurohormonal Activation in Heart Failurekunalprabhu148Pas encore d'évaluation
- PTMC: A Guide to Percutaneous Transmitral CommissurotomyDocument42 pagesPTMC: A Guide to Percutaneous Transmitral CommissurotomyNavojit Chowdhury100% (1)
- DRUG THERAPY FOR HEART FAILUREDocument40 pagesDRUG THERAPY FOR HEART FAILURENiteesh Kumar SharmaPas encore d'évaluation
- 5.10 Cardiac AuscultationDocument47 pages5.10 Cardiac AuscultationDenisseRangelPas encore d'évaluation
- Ch-13 Drugs Used in Heart FailureDocument49 pagesCh-13 Drugs Used in Heart FailureShabrin SadikhPas encore d'évaluation
- Echocardiographic Assessment of Valve Stenosis: Heart Circulation Ultrasound SpecialistsDocument1 pageEchocardiographic Assessment of Valve Stenosis: Heart Circulation Ultrasound SpecialistsWayan GunawanPas encore d'évaluation
- VALVULAR HEART DISEASE GUIDEDocument69 pagesVALVULAR HEART DISEASE GUIDEAbanoub AwadallaPas encore d'évaluation
- Pericardial EffusionDocument3 pagesPericardial EffusionNita Hurek100% (1)
- Mitral Valve Disease QuizDocument5 pagesMitral Valve Disease QuizReda SoPas encore d'évaluation
- An Introduction To Cardiac ElectrophysiologyDocument342 pagesAn Introduction To Cardiac ElectrophysiologyBinod KumarPas encore d'évaluation
- Inotropes, Excellent Article, With DosingDocument47 pagesInotropes, Excellent Article, With DosingNavojit ChowdhuryPas encore d'évaluation
- Arrhythmia 2Document31 pagesArrhythmia 2rittvedPas encore d'évaluation
- Life Threatening Arrhythmia and ManagementDocument40 pagesLife Threatening Arrhythmia and ManagementRuki HartawanPas encore d'évaluation
- 1 The Electrical Activity of The HeartDocument2 pages1 The Electrical Activity of The HeartRickertsPas encore d'évaluation
- Aortic Root & Ascending Aortic Aneurysm Surgery OptionsTITLEDocument82 pagesAortic Root & Ascending Aortic Aneurysm Surgery OptionsTITLEMustafa KamalPas encore d'évaluation
- Contrast Agents, Cath Lab & Anaphylatic Shock-ParamedDocument29 pagesContrast Agents, Cath Lab & Anaphylatic Shock-ParamedManikanta GupthaPas encore d'évaluation
- Contrast EchocardiographyDocument54 pagesContrast EchocardiographySruthiPas encore d'évaluation
- Mitral RegurgitationDocument6 pagesMitral RegurgitationMelfi Triani SiskaPas encore d'évaluation
- Principles of EchocardiographyDocument3 pagesPrinciples of Echocardiographys336336anl100% (1)
- Heartbeat Irregularities ExplainedDocument5 pagesHeartbeat Irregularities ExplainedKayelyn-Rose Combate100% (1)
- Acute Respiratory Failure 2010Document87 pagesAcute Respiratory Failure 2010bassist5217100% (1)
- Holter Analysis Software FeaturesDocument27 pagesHolter Analysis Software FeaturesSuciu FlorinPas encore d'évaluation
- Simple Office SpirometryDocument42 pagesSimple Office SpirometryRoberto Merza III100% (4)
- Ecg Pathology 02Document95 pagesEcg Pathology 02Andi MP Manurung100% (1)
- Mitral RegurgitationDocument11 pagesMitral RegurgitationAbdur RaqibPas encore d'évaluation
- NHS Greater Glasgow & Clyde Medical Staffing Guide To Clinical AttachmentsDocument3 pagesNHS Greater Glasgow & Clyde Medical Staffing Guide To Clinical AttachmentsUma MounaPas encore d'évaluation
- BasicPharmacologySlides PDFDocument101 pagesBasicPharmacologySlides PDFCabdi WaliPas encore d'évaluation
- CVS-System Wise 1700 document team contribution guideDocument158 pagesCVS-System Wise 1700 document team contribution guideBio DataPas encore d'évaluation
- Outstanding Student LetterDocument3 pagesOutstanding Student LettersagarshirolePas encore d'évaluation
- Bacterial Corneal UlcerDocument5 pagesBacterial Corneal UlcerUma MounaPas encore d'évaluation
- Step 1 Study PlanDocument3 pagesStep 1 Study PlanUma MounaPas encore d'évaluation
- Ramayana by C. RajagopalachariDocument204 pagesRamayana by C. RajagopalacharikaumaaramPas encore d'évaluation
- Sample Strong Eras Lor 5-05Document1 pageSample Strong Eras Lor 5-05Raiyan KhanPas encore d'évaluation
- Application Form Student Elective 2014-15Document5 pagesApplication Form Student Elective 2014-15Uma MounaPas encore d'évaluation
- Writing Letters of RecommendationDocument4 pagesWriting Letters of Recommendationwenskyrose1100% (1)
- Methods of Airway ManagementDocument10 pagesMethods of Airway ManagementUma MounaPas encore d'évaluation
- Ramayana by C. RajagopalachariDocument204 pagesRamayana by C. RajagopalacharikaumaaramPas encore d'évaluation
- Suspended AnimationDocument7 pagesSuspended AnimationUma MounaPas encore d'évaluation
- Concepts of Disease OccurrenceDocument24 pagesConcepts of Disease OccurrenceUma Mouna100% (1)
- Prevention of HTNDocument6 pagesPrevention of HTNUma MounaPas encore d'évaluation
- Identification of SexDocument24 pagesIdentification of SexUma MounaPas encore d'évaluation
- GeriatricsDocument8 pagesGeriatricsUma MounaPas encore d'évaluation
- Adrenergic Receptor Blockers JPDocument17 pagesAdrenergic Receptor Blockers JPUma MounaPas encore d'évaluation
- PM ChangesDocument49 pagesPM ChangesUma MounaPas encore d'évaluation
- Acid Peptic Disease (APD)Document73 pagesAcid Peptic Disease (APD)Uma MounaPas encore d'évaluation
- Bacterial Cell Wall Differential Staining VMCDocument26 pagesBacterial Cell Wall Differential Staining VMCUma MounaPas encore d'évaluation
- P Harm Co KineticsDocument86 pagesP Harm Co KineticsUma MounaPas encore d'évaluation
- Pharmaco DynamicsDocument51 pagesPharmaco DynamicsUma MounaPas encore d'évaluation
- Injury: Clinically Its Defined As Solution or Disruption of The Anatomical Continuity of Any Tissues of The BodyDocument83 pagesInjury: Clinically Its Defined As Solution or Disruption of The Anatomical Continuity of Any Tissues of The BodyMelitta SetyaraniPas encore d'évaluation
- Adrenergicsystem 110126105226 Phpapp02Document73 pagesAdrenergicsystem 110126105226 Phpapp02Uma Mouna100% (1)
- Pharmaco DynamicsDocument51 pagesPharmaco DynamicsUma MounaPas encore d'évaluation
- Injury: Clinically Its Defined As Solution or Disruption of The Anatomical Continuity of Any Tissues of The BodyDocument83 pagesInjury: Clinically Its Defined As Solution or Disruption of The Anatomical Continuity of Any Tissues of The BodyMelitta SetyaraniPas encore d'évaluation
- Adrenergic Receptor Blockers JPDocument17 pagesAdrenergic Receptor Blockers JPUma MounaPas encore d'évaluation
- Ch4 HemodynDocument113 pagesCh4 HemodynUma MounaPas encore d'évaluation
- Atrioventricular Nodal Reentrant Tachycardia: AvnrtDocument13 pagesAtrioventricular Nodal Reentrant Tachycardia: AvnrthiPas encore d'évaluation
- Supraventricular Tachycardia PresentationDocument31 pagesSupraventricular Tachycardia PresentationAkbar IskandarPas encore d'évaluation
- Show Questions One by OneDocument12 pagesShow Questions One by OneCharlie Cheng-Ying HsiehPas encore d'évaluation
- FLASHCARD CardiovascularDocument40 pagesFLASHCARD CardiovascularsnehaPas encore d'évaluation
- Acute Medicine 4th EdDocument660 pagesAcute Medicine 4th EdEmmanuel Ortiz100% (4)
- Catheter Ablation Superior to Drug Therapy for VT Storm in ICMDocument41 pagesCatheter Ablation Superior to Drug Therapy for VT Storm in ICMSilp SatjawattanavimolPas encore d'évaluation
- SVT With Aberrancy Versus VTDocument5 pagesSVT With Aberrancy Versus VTEdwin MayaPas encore d'évaluation
- Nursing Care PlanDocument2 pagesNursing Care Plansyfi56Pas encore d'évaluation
- Rhythm Recognition - ACLS Medical Training 1Document9 pagesRhythm Recognition - ACLS Medical Training 1Catalina BorquezPas encore d'évaluation
- ArrhythmiaDocument55 pagesArrhythmiaDonjeta AbaziPas encore d'évaluation
- Cardiac Arrhythmias Guide - Causes, Symptoms and Treatment OptionsDocument5 pagesCardiac Arrhythmias Guide - Causes, Symptoms and Treatment OptionsaksinuPas encore d'évaluation
- MBBS Antiarrhythmics 2014 Class II (Antiarrhythmic Drugs)Document23 pagesMBBS Antiarrhythmics 2014 Class II (Antiarrhythmic Drugs)Dr.U.P.Rathnakar.MD.DIH.PGDHM100% (1)
- Alawiya, Jamal Tango P.Document18 pagesAlawiya, Jamal Tango P.Jamal P. AlawiyaPas encore d'évaluation
- Avnrt VS AvrtDocument79 pagesAvnrt VS AvrtDwi Nugroho PrastowoPas encore d'évaluation
- Sinus Rhythm DisturbancesDocument3 pagesSinus Rhythm DisturbancesMarcus Philip GonzalesPas encore d'évaluation
- Pacing ManualDocument76 pagesPacing ManualMirela Sfaraiala LuculescuPas encore d'évaluation
- Regular Sinus Rhythm (RSR)Document3 pagesRegular Sinus Rhythm (RSR)ISABEL REGASPIPas encore d'évaluation
- Emp SyncopeDocument20 pagesEmp SyncopeWilmer JimenezPas encore d'évaluation
- Mi (Case # 1) : 1. How Would You Classify Mr. Smith's Chest Pain?Document11 pagesMi (Case # 1) : 1. How Would You Classify Mr. Smith's Chest Pain?Faizan MazharPas encore d'évaluation
- Bradycardia and TachycardiaDocument50 pagesBradycardia and Tachycardialiu_owen17Pas encore d'évaluation
- PracticeExam 2 AnsDocument51 pagesPracticeExam 2 AnsBehrouz YariPas encore d'évaluation
- Acls EcgDocument4 pagesAcls EcgScribdTranslationsPas encore d'évaluation
- Healthmedicinet I 2016 5Document282 pagesHealthmedicinet I 2016 5tuni santePas encore d'évaluation
- Fundamentalof Ventilation & PacemakerDocument22 pagesFundamentalof Ventilation & PacemakerLucila Lugo100% (1)
- The Six Second ECGDocument9 pagesThe Six Second ECGAC0RNPas encore d'évaluation
- Onlinemeded Notes CardioDocument1 pageOnlinemeded Notes CardioCourtney HolbrookPas encore d'évaluation
- History of Palpitation: Editing LinkDocument6 pagesHistory of Palpitation: Editing LinkTouseef Ur RehmanPas encore d'évaluation
- Arrhythmia in Emergency 111Document21 pagesArrhythmia in Emergency 111Iyas JehadPas encore d'évaluation
- Systematic Approach To ECGDocument12 pagesSystematic Approach To ECGAmr El TaherPas encore d'évaluation
- Rhythm Diagnostics SystemsDocument30 pagesRhythm Diagnostics SystemswwinterPas encore d'évaluation