Académique Documents
Professionnel Documents
Culture Documents
Bio 132 Chapter 23 Notes
Transféré par
gilissaDescription originale:
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Bio 132 Chapter 23 Notes
Transféré par
gilissaDroits d'auteur :
Formats disponibles
Respiratory System Respiratory System Functions:
(Chapter 23) 1. External respiration (gas exchange)
2. Pulmonary ventilation (move air)
Lecture Materials
3. Protect respiratory surfaces from:
for -dehydration
-temp changes
Amy Warenda Czura, Ph.D.
-invasion by pathogens
Suffolk County Community College 4. Produce sound (communication)
5. Provide olfactory sensation (smell)
Eastern Campus
Primary Sources for figures and content:
Marieb, E. N. Human Anatomy & Physiology 6th ed. San Francisco: Pearson Benjamin
Cummings, 2004.
Martini, F. H. Fundamentals of Anatomy & Physiology 6th ed. San Francisco: Pearson
Benjamin Cummings, 2004.
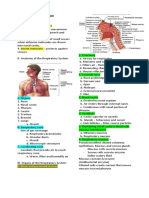
Anatomy of Respiratory System: Respiratory Mucosa (mucus membrane)
1. Upper respiratory system: -lines conduction portions
-functions to warm and humidify air -pseudostratified columnar epithelium
-nose, nasal cavity, sinuses, pharynx -usually ciliated
2. Lower respiratory system: -scattered goblet cells (mucin production)
A. Conducting portion:
-bring air to respiratory surfaces
-larynx, trachea, bronchi, bronchioles
B. Respiratory portion:
-gas exchange
-alveoli
-lamina propria = areolar CT with
-mucus glands (mucin) and
-serous glands (lysozyme)
Glands produce ~1 quart mucus fluid /day
-cilia move mucus to pharynx to be swallowed
(cilia beat slow in cold)
Amy Warenda Czura, Ph.D. 1 SCCC BIO132 Chapter 23 Lecture Notes
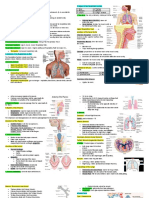
Respiratory Defense Systems: The Upper Respiratory System
1. Mucus: from goblet cells and glands in
lamina propria, traps foreign objects
2. Cilia: mucus escalator: move carpet of
mucus with trapped debris out of
respiratory tract
3. Alveolar macrophages: phagocytose
particles that reach alveoli
1. Nose: only external feature
Cystic fibrosis = failure of mucus escalator: Functions:
produce thick mucus which blocks airways 1. Opening to airway for respiration
and encourages bacteria growth 2. Moisten and warm entering air
3. Filter and clean inspired air
Smoking ! destroys cilia 4. Resonating chamber for speech
5. Houses olfactory receptors
Inhalation of irritants ! chronic inflammation Features:
! cancer e.g. squamous cell carcinoma -external nares conduct air into vestibule
-vestibule = space in flexible part, lined with
hairs to filter particles, leads to nasal cavity
2. Nasal Cavity -nasal conchae cause air to swirl:
-divided into right and left by nasal septum 1. Increase likelihood of trapping foreign
-superior portion has olfactory epithelium material in mucus
-nasal conchae (superior, middle, inferior 2. Provide time for smell detection
project into cavity on both sides 3. Provide time and contact to warm and
humidify air
-hard and soft palate form floor
-internal nares open to nasopharynx
-mucosa has large superficial blood supply
(warm, moisten air) Epistaxis = nose bleed
-paranasal sinuses in frontal, sphenoid,
ethmoid and maxillay bones; lined with
respiratory mucosa, connected to nasal
cavity, aid in warming/moistening air
Amy Warenda Czura, Ph.D. 2 SCCC BIO132 Chapter 23 Lecture Notes
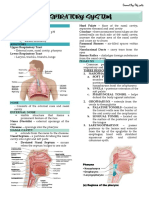
Rhinitis = inflammation of nasal mucosa ! A. Nasopharynx : air only
" mucus production. -posterior to nasal cavity
Infection ! blockage of sinuses: headache -pseudostratified columnar epithelium
from negative pressure -closed off by soft palate and uvula during
3. Pharynx: swallowing
-chamber between internal nares and entrances -pharyngeal tonsil located on posterior wall
to larynx and esophagus (inflammation can block airway)
-Three parts -auditory tubes open here
B. Oropharynx: food and air
-posterior to oral cavity
-stratified squamous epithelium
-palatine and lingual tonsils in mucosa
C. Laryngopharynx: food and air
-lower portion
-stratified squamous epithelium
-continuous with esophagus
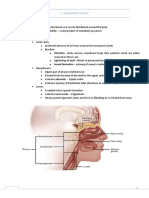
Lower Respiratory System -folds of epithelium over ligaments of elastic
4. Larynx (voice box) fibers create vocal folds/cords.
-hyaline cartilages around glottis = opening
from laryngopharynx to trachea
-vocal cords project into glottis
-air passing through glottis vibrates folds
producing sound
Pitch controlled by tensing/relaxing cords:
tense & narrow = high pitch
Volume controlled by amount of air
Functions of larynx:
Sound production = phonation
1. Provide continuous airway
Speech = formation of sound using mouth and
2. Act as switch to route food and air properly
tongue with resonance in pharynx,
3. Voice production
mouth, sinuses and nose
Laryngitis = inflammation of vocal folds due
-contains epiglottis = elastic cartilage flap,
to infection or overuse, can inhibit
covers glottis during swallowing
phonation
Amy Warenda Czura, Ph.D. 3 SCCC BIO132 Chapter 23 Lecture Notes
5. Trachea -trachea branches into
-attached inferior to larynx right and left
-walls composed of three layers: primary bronchi
1. Mucosa: pseudostratified columnar
epithelium, goblet cells, lamina propria 6. Primary bronchi
with smooth muscle & glands -similar structure as
2. Submucosa: CT with additional mucus trachea (no
glands trachealis muscle)
3. Adventitia: CT with hyaline cartilage -right: steeper angle
rings (keep airway open): 15-20 C- -enter lungs at hilum
shaped, have opening toward esophagus (along with blood
(allow expansion), ends connected by and lymphatic
trachealis muscle vessels, nerves)
Inside lungs bronchi
branch, get smaller in
diameter:
branch ~23 times
creating the bronchial
tree
As bronchi get smaller, structure changes: Asthma = strong bronchoconstriction
1. less cartilage in adventitia activated by inflammatory chemicals
2. more smooth muscle in lamina propria (histamine), reduces airflow. Epinephrine
3. epithelium thinner, less cilia, less mucus inhaler mimics sympathetic (bronchodilate)
7. Terminal bronchiole -each terminal bronchiole delivers air to one
-smallest bronchi of pulmonary lobule (separated by CT)
respiratory tree -inside lobule, terminal bronchiole branches
-no cartilage into respiratory bronchioles: no cilia or
-last part of mucus
conducting portion -each respiratory bronchiole connects to
alveolar sac made up of many alveoli
Trachea, Bronchi and
Bronchioles innervated by
ANS to control airflow to
lungs:
Sympathetic = bronchodilation
Parasympathetic =
bronchoconstriction
Amy Warenda Czura, Ph.D. 4 SCCC BIO132 Chapter 23 Lecture Notes
8. Alveoli -alveoli connected to neighbors by alveolar
-wrapped in capillaries pores (equalize pressure)
-held in place by elastic fibers -Gas exchange occurs across the
respiratory membrane (0.5m thick):
1. Type I cells of alveolus
2. Thin basal lamina (fusion)
3. Endothelial cells of capillary
-three cell types:
1. Type I cells: simple squamous epithelium,
lines inside , gas exchange
2. Type II cells: cuboidal epithelial cells,
produce surfactant
(phospholipids +
proteins), prevent
alveolar collapse
3. Alveolar Pneumonia = inflammation of lungs from
macrophages: infection or injury, fluid in alveoli
phagocytosis of prevents gas exchange
particles Pulmonary embolism = block in branch of
pulmonary artery, reduced blood flow
causes alveolar collapse
Gross Anatomy of Lungs Respiratory Physiology
3 steps of respiration:
1. Pulmonary ventilation
2. Gas Diffusion/Exchange
3. Gas Transport to/from tissues
1. Pulmonary Ventilation
= movement of air into/out of alveoli
-visceral pleura adheres to parietal pleura via
surface tension: altering size of pleural
-concave base, rests on diaphragm cavity will alter size of lungs
-right: 3 lobes Pneumothorax = injury of thoracic cavity, air
-left: 2 lobes (accommodates heart) breaks surface tension, lungs recoil =
-housed in pleural cavity atelectasis (collapsed lung)
-cavity lined with parietal pleura
-lungs covered by visceral pleura Mechanics of breathing:
-both pleura produce serous pleural fluid to -Boyles Law: gas pressure is inversely
reduce friction during expansion proportional to volume
Pleurisy = inflammation of pleura, can restrict -Air flows from area of high pressure to low
movement of lungs causing breathing
difficulty
Amy Warenda Czura, Ph.D. 5 SCCC BIO132 Chapter 23 Lecture Notes
Contraction of Factors influencing pulmonary ventilation:
diaphragm pulls it 1. Airway resistance
toward abdomen: -diameter of bronchi
-lung volume " -obstructions
-air pressure # 2. Alveolar surface tension
-air flows in -surfactant (Type II cells) reduces alveoli
surface tension to allow inflation
Respiratory distress syndrome = too little
Relaxation causes surfactant, requires great force to open
diaphragm to rise in alveoli to inhale
dome shape: 3. Compliance
-lung volume # = effort required to expand lungs and chest
-air pressure " High compliance = expand easily (normal)
-air flows out Low compliance = resist expansion
Compliance affected by:
A. CT structure: loss of elastin/replacement
by fibrous tissue = # compliance
Emphysema = respiratory surface replaced by
Rib cage movements can also contribute: scars, # elasticity # compliance, and
-superior = bigger, air in have loss of surface for gas exchange
-inferior = smaller, air out
B. Alveolar expandability (vs. collapse) Respiratory Volumes and Capacities:
-"surface tension(#surfact.) = #compliance -a breath = one respiratory cycle
-fluid (edema) = # compliance (go to handout)
C. Mobility of thoracic cage
-less mobility = # compliance
Inspiration
-inhalation involves contraction of muscles to
increase thoracic volume
A. Quiet breathing = eupnea
-diaphragm: moves 75% of air
-external intercostals: elevate ribs, 25% more
B. Forced breathing = hyperpnea
-maximum rib elevation increases respiratory
volume 6X: serratus anterior, pectoralis Respiratory rate = breaths/min ~18-20 at rest
minor, scalenes, sternocleidomastoid Respiratory Minute Volume (RMV/MRV) =
Expiration respiratory rate X tidal volume ~ 6 L
A. Eupnea: passive, muscles relax, thoracic Not all reaches alveoli, some air remains in
volume decrease conducting portions = anatomic dead
B. Hyperpnea: abdominal muscles (obliques, space (~1ml / lb body weight)
transversus, rectus) contract forcing diaphragm Alveolar ventilation = air reaching alveoli /
up, thoracic volume further decreases min at rest ~ 4.2 L
Amy Warenda Czura, Ph.D. 6 SCCC BIO132 Chapter 23 Lecture Notes
Both tidal volume and respiratory rate are Diffusion at respiratory membrane efficient:
adjusted to meet oxygen demands of body 1. Substantial differences in PP across the
membrane
2. Gas Exchange 2. Distance is small
-Air = 79% N2, 21% O2, 0.5% H2O, 3. Gasses are lipid soluble
0.04% CO2, trace inert gasses 4. Large surface area for diffusion
-Partial pressure of gas = concentration in air 5. Coordination of blood and air flow: " blood
-Gasses follow diffusion gradients to diffuse to alveoli with " O2
into liquid: rate depends on partial In Lung:
pressure and temperature -PP O2 " in alveoli,
High Altitude Sickness = #PP O2 at high # in capillary:
altitude causes # diffusion into blood diffuse into capillary
Decompression Sickness = PP of air gasses -PP CO2 # in alveoli,
high underwater, high amounts of N2 " in capillary:
diffuse into blood. If pressure suddenly diffuse into alveoli
decreases, N2 leaves blood as gas In Tissues:
causing bubbles (damage, pain), Pressures and flow reversed:
Hyperbaric chambers used to treat O2 into tissues
CO2 into capillary
3. Gas Transport Hypoxia = inadequate O2 delivery to tissues
A. Transport of Oxygen B. Transport of Carbon Dioxide
-1.5 % dissolved in plasma 1. ~ 70% as Carbonic acid
-most bound to iron ions on heme of -in RBCs and plasma
hemoglobin in erythrocytes: 4 O2/Hb, -carbonic anhydrase in RBCs catalyze
~280million Hb/RBC = 1 billion O2/RBC reaction with water:
Hemoglobin saturation = %hemes bound to O2 CO2 + H2O $ H2CO3 $ H+ + HCO3-
~ 97.5% at alveoli -reaction reversed at lungs
@"PP O2 hemoglobin binds O2 2. ~23% as carbaminohemoglobin
@#PP O2 hemoglobin drops O2 -CO2 bound to amino groups of Hb
Carbon Monoxide Poisoning: CO out- 3. ~7% dissolved in plasma as CO2
competes O2 for binding to Hb, even at Regulation of Respiration
low PP CO, causes suffocation (no O2) (handout)
Other factors that affect Hb saturation:
1. Bohr effect: Hb releases O2 in acidic pH
(high CO2 creates carbonic acid)
2. Temperature: Hb releases O2 in " temp
3. BPG (2,3bisphosphoglycerate): produced
by healthy RBC during glycolysis,
"BPG = "O2 release
4. Pregnancy: fetal Hb = "O2 binding
Amy Warenda Czura, Ph.D. 7 SCCC BIO132 Chapter 23 Lecture Notes
Age Related Changes
1. Elastic tissue deteriorates:
# compliance, # VC
2. Arthritic changes in rib cage:
# mobility, # RMV
3. Emphysema, some degree
# gas exchange
Higher risk for smokers, dusty job, etc.
Amy Warenda Czura, Ph.D. 8 SCCC BIO132 Chapter 23 Lecture Notes
Vous aimerez peut-être aussi
- External Respiration: Angiotensin-Converting EnzymeDocument4 pagesExternal Respiration: Angiotensin-Converting EnzymeEllä PabustanPas encore d'évaluation
- Respiratory PhysiologyDocument16 pagesRespiratory PhysiologyYsabel Salvador DychincoPas encore d'évaluation
- Respiratory SystemDocument5 pagesRespiratory SystemChloe Mae PastranaPas encore d'évaluation
- Respiratory SystemDocument6 pagesRespiratory Systemjenryl100% (1)
- Respiratory SystemDocument6 pagesRespiratory SystemChelsie NicolePas encore d'évaluation
- Micro - Respiratory SystemDocument3 pagesMicro - Respiratory SystemKaren ValdezPas encore d'évaluation
- Respiratory System TransesDocument5 pagesRespiratory System Transesadrielvamos28Pas encore d'évaluation
- NCM 112 LEC Topic 1 Respiratory System Anatomy PhysiologyDocument7 pagesNCM 112 LEC Topic 1 Respiratory System Anatomy PhysiologyViviene Faye FombuenaPas encore d'évaluation
- 2 - Respiratory SystemDocument9 pages2 - Respiratory SystemHannah Grace CorveraPas encore d'évaluation
- Respiratory SystemDocument6 pagesRespiratory SystemCharlie CharlesPas encore d'évaluation
- UNIT 1 (MS 1) Care of Clients With Problems in OxygenationDocument10 pagesUNIT 1 (MS 1) Care of Clients With Problems in OxygenationElle MirandaPas encore d'évaluation
- Respiratory SystemDocument13 pagesRespiratory SystemEllePas encore d'évaluation
- Anatomy Final pt.2Document8 pagesAnatomy Final pt.2Gladys Mae S. BañesPas encore d'évaluation
- Airway Mngt. Module 1.Document11 pagesAirway Mngt. Module 1.marc gorospePas encore d'évaluation
- Respiratory SystemDocument12 pagesRespiratory SystemCUESCANO, CRISTEL G. BSMT 2-APas encore d'évaluation
- 2 - Respiratory SystemDocument9 pages2 - Respiratory SystemHannah Grace CorveraPas encore d'évaluation
- Chapter 15 Respiratory SystemDocument3 pagesChapter 15 Respiratory SystemRayumaaa100% (1)
- Pre-Finals Topic 1 AnaphyDocument5 pagesPre-Finals Topic 1 AnaphyGlenice Joy SenocPas encore d'évaluation
- Respiratory PDFDocument9 pagesRespiratory PDFJoydee Liza MarcoPas encore d'évaluation
- Respiratory SystemDocument4 pagesRespiratory SystemAlloiza CaguiclaPas encore d'évaluation
- Nose and Paranasal SinusesDocument2 pagesNose and Paranasal SinusesCarlo BarriosPas encore d'évaluation
- The Respiratory SystemDocument4 pagesThe Respiratory SysteminitaygracileshaynePas encore d'évaluation
- OXYGENATIONDocument10 pagesOXYGENATIONnicolePas encore d'évaluation
- Anaphy - Chapter 23 - Respiratory SystemDocument9 pagesAnaphy - Chapter 23 - Respiratory SystemAileen DemaguilaPas encore d'évaluation
- Functions of The Respiratory System: Inside-RestDocument7 pagesFunctions of The Respiratory System: Inside-RestRaven LacsonPas encore d'évaluation
- Catatan Koas THT 1Document5 pagesCatatan Koas THT 1MEDS easyPas encore d'évaluation
- Respiratory System: LarynxDocument4 pagesRespiratory System: LarynxLouise GermainePas encore d'évaluation
- Anaphy Chapter 23 Respiratory System Doran MLS 1 FDocument9 pagesAnaphy Chapter 23 Respiratory System Doran MLS 1 FayenaPas encore d'évaluation
- Repiratory System Concept Rna NotesDocument21 pagesRepiratory System Concept Rna NotesArpan BhadrawalPas encore d'évaluation
- Respiratory SystemDocument7 pagesRespiratory SystemChristiane with an EPas encore d'évaluation
- MCN KweenDocument4 pagesMCN KweenAngelo SiguePas encore d'évaluation
- Respiratory SystemDocument38 pagesRespiratory Systemjsreyes.402Pas encore d'évaluation
- Medical Surgical Nursing Lecture 234 Pages Pg. 333 566Document189 pagesMedical Surgical Nursing Lecture 234 Pages Pg. 333 566Crystal Ann TadiamonPas encore d'évaluation
- Chapter 15: Respiratory System MC 1Document6 pagesChapter 15: Respiratory System MC 1guadalupedeamargaretPas encore d'évaluation
- Sistem RespirasiDocument39 pagesSistem RespirasiBestariayuPas encore d'évaluation
- Respiratory System - NotesDocument4 pagesRespiratory System - NotessPas encore d'évaluation
- Anaphy Reviiewer - RabeDocument16 pagesAnaphy Reviiewer - RabeAyessa Marie BarbosaPas encore d'évaluation
- Respiratory SystemDocument15 pagesRespiratory SystemMichelle Gambol100% (2)
- Lec 1 Respiratory SystemDocument3 pagesLec 1 Respiratory SystemfaiPas encore d'évaluation
- Respiratory SystemDocument3 pagesRespiratory Systemydnic alykPPas encore d'évaluation
- O CO O CO O CO: Chapter 15: Respiratory SystemDocument3 pagesO CO O CO O CO: Chapter 15: Respiratory SystemPrecious Faith RodriguezPas encore d'évaluation
- Anatomy CHP 13 NotesDocument5 pagesAnatomy CHP 13 NotesIsland RaePas encore d'évaluation
- Week 3 Respiratory SystemDocument10 pagesWeek 3 Respiratory SystemangeliaPas encore d'évaluation
- AnatomyDocument8 pagesAnatomyAnna NanaPas encore d'évaluation
- Lecture 1structure & Function of Respiratory System Nose & Paranasal SinusesDocument7 pagesLecture 1structure & Function of Respiratory System Nose & Paranasal Sinusesadham bani younesPas encore d'évaluation
- ANAPHY Lec Session #18 - SAS (Agdana, Nicole Ken)Document7 pagesANAPHY Lec Session #18 - SAS (Agdana, Nicole Ken)Nicole Ken AgdanaPas encore d'évaluation
- MTHISTO100 Lesson 2 Respiratory SystemDocument7 pagesMTHISTO100 Lesson 2 Respiratory SystemJaeri HuangPas encore d'évaluation
- Review On Respiratory SystemDocument4 pagesReview On Respiratory Systemsecondacvalo123Pas encore d'évaluation
- The Respiratory System and Its DisordersDocument16 pagesThe Respiratory System and Its DisordersZea Leyan J. LopezPas encore d'évaluation
- Upper Nasal Cavity and Chest WallDocument18 pagesUpper Nasal Cavity and Chest WallHessa AlamiraPas encore d'évaluation
- Anaphy ReviewerDocument10 pagesAnaphy ReviewerTsukishima RinPas encore d'évaluation
- CHAP13Document8 pagesCHAP13Crystal ARIETAPas encore d'évaluation
- Respiratory SystemDocument8 pagesRespiratory SystemHenry BuñagPas encore d'évaluation
- M7 RespiratoryDocument6 pagesM7 RespiratoryNel joy PaurilloPas encore d'évaluation
- Respiratory System-2cgf2Document42 pagesRespiratory System-2cgf2Nzenwa Jedidiah KimizuPas encore d'évaluation
- Lesson 1 Overview of The Respiratory SystemDocument3 pagesLesson 1 Overview of The Respiratory SystemJacqueline S. PunoPas encore d'évaluation
- Respiratory SystemDocument13 pagesRespiratory SystemAly HannahPas encore d'évaluation
- Gen BioDocument15 pagesGen BioCAMILLE JELLA ALZOLAPas encore d'évaluation
- NCM 112 N LECTURE MidtermDocument42 pagesNCM 112 N LECTURE MidtermVivien IgnacioPas encore d'évaluation
- Treatise on the Anatomy and Physiology of the Mucous Membranes: With Illustrative Pathological ObservationsD'EverandTreatise on the Anatomy and Physiology of the Mucous Membranes: With Illustrative Pathological ObservationsPas encore d'évaluation
- Benedict's and Heat and Acetic Acid TestDocument2 pagesBenedict's and Heat and Acetic Acid Testgilissa100% (1)
- Linen Inventory FormsDocument5 pagesLinen Inventory FormsgilissaPas encore d'évaluation
- Bac 3 - Practice Career Professionalism NotesDocument13 pagesBac 3 - Practice Career Professionalism Notesgilissa0% (1)
- Asepsis and Infection ControlDocument10 pagesAsepsis and Infection ControlgilissaPas encore d'évaluation
- Changing An Unoccupied Bed - ChecklistDocument5 pagesChanging An Unoccupied Bed - ChecklistgilissaPas encore d'évaluation
- Human Anatomy and Physiology KNR 182: Lecture Packet For Unit V Respiratory SystemDocument19 pagesHuman Anatomy and Physiology KNR 182: Lecture Packet For Unit V Respiratory SystemgilissaPas encore d'évaluation
- Chapter 1: Introduction To Human Anatomy and Physiology: Characteristics of LifeDocument3 pagesChapter 1: Introduction To Human Anatomy and Physiology: Characteristics of LifegilissaPas encore d'évaluation
- Anatomy & Physiology Notes Ch. 16: The Reproductive SystemDocument11 pagesAnatomy & Physiology Notes Ch. 16: The Reproductive SystemgilissaPas encore d'évaluation
- The Reproductive System - EDITEDDocument6 pagesThe Reproductive System - EDITEDgilissaPas encore d'évaluation
- The Tissues: The Four Primary Tissue TypesDocument10 pagesThe Tissues: The Four Primary Tissue TypesgilissaPas encore d'évaluation
- Nursing BulletsDocument83 pagesNursing BulletsgilissaPas encore d'évaluation
- Unit 12: - Reproductive SystemDocument18 pagesUnit 12: - Reproductive SystemgilissaPas encore d'évaluation
- Bio 130 Chapter 4 NotesDocument12 pagesBio 130 Chapter 4 Notesgilissa100% (1)
- Management of Status Asthmatic Us in ChildrenDocument7 pagesManagement of Status Asthmatic Us in Childrenjshq1971Pas encore d'évaluation
- Modifying The Body: Motivations For Getting Tattooed and PiercedDocument9 pagesModifying The Body: Motivations For Getting Tattooed and PiercedKrzysztof NowosielskiPas encore d'évaluation
- Pediatricflatfoot: Pearls and PitfallsDocument14 pagesPediatricflatfoot: Pearls and PitfallsSuplementos Fit CarvajalPas encore d'évaluation
- Kentucky CBD OverviewDocument1 pageKentucky CBD OverviewMPP100% (1)
- Pediatric NotesDocument12 pagesPediatric Noteslanie_jecielPas encore d'évaluation
- Claim IntimationDocument2 pagesClaim IntimationSyed's Way PoolPas encore d'évaluation
- Antenatal and Intrapartum Prediction Dystocia ShoulderDocument7 pagesAntenatal and Intrapartum Prediction Dystocia ShoulderDewiDwipayantiGiriPas encore d'évaluation
- Dental Health and Management For Children With Congenital Heart DiseaseDocument6 pagesDental Health and Management For Children With Congenital Heart DiseaseJavier Farias VeraPas encore d'évaluation
- Project ReportDocument13 pagesProject ReportRenjan Kuruvilla100% (5)
- Mock CodeDocument4 pagesMock CodeKrezielDulosEscobarPas encore d'évaluation
- New York State PCRDocument3 pagesNew York State PCRdandude505Pas encore d'évaluation
- ResumeDocument2 pagesResumeJune TorrionPas encore d'évaluation
- 2011 - IJCHP - The Leyton Obsessional Inventory-Child VersionDocument16 pages2011 - IJCHP - The Leyton Obsessional Inventory-Child VersionEsteysi Villarroel BernalesPas encore d'évaluation
- Formula Selection OPNPGDocument2 pagesFormula Selection OPNPGRina PratiwiPas encore d'évaluation
- Isosorbide DinitrateDocument4 pagesIsosorbide DinitrateManelle Singzon100% (1)
- MRI Findings in Susac SyndromeDocument6 pagesMRI Findings in Susac SyndromeLeonardoBubackPas encore d'évaluation
- NA-0201 Application For Driving Licence and Certificate of Professional Competence (In English)Document2 pagesNA-0201 Application For Driving Licence and Certificate of Professional Competence (In English)Del MabelPas encore d'évaluation
- Krzywosinski PBLsDocument24 pagesKrzywosinski PBLsleahbayPas encore d'évaluation
- Key Topics in Orthopaedic Trauma SurguryDocument318 pagesKey Topics in Orthopaedic Trauma SurguryMaria Claudia Bercea80% (10)
- Cardiac Diseases in PregnancyDocument27 pagesCardiac Diseases in PregnancyHoney May Rollan Vicente50% (2)
- OP - Department Frequently Asked Question PDFDocument29 pagesOP - Department Frequently Asked Question PDFMSA AvGeekPas encore d'évaluation
- Optimal Size Selection of The Classic Laryngeal Mask Airway by Tongue Width-Based Method in Male AdultsDocument4 pagesOptimal Size Selection of The Classic Laryngeal Mask Airway by Tongue Width-Based Method in Male AdultsDefayudina Dafilianty RosatariaPas encore d'évaluation
- Bonicas Management of Pain 5th Edition Ebook PDFDocument61 pagesBonicas Management of Pain 5th Edition Ebook PDFpaul.tucker16998% (42)
- Stock Alkes IcuDocument6 pagesStock Alkes IcuDoni PurwantoPas encore d'évaluation
- New Post Grad ProgramDocument8 pagesNew Post Grad ProgramPradeep KumarPas encore d'évaluation
- Dermatomycological Profile of Patients in A Tertiary Care Hospital of Western MaharashtraDocument2 pagesDermatomycological Profile of Patients in A Tertiary Care Hospital of Western MaharashtraApple IdeaPas encore d'évaluation
- AmfepramoneDocument3 pagesAmfepramone18.10.1986Pas encore d'évaluation
- HospitalDocument20 pagesHospitalSparsh SharmaPas encore d'évaluation
- Terapi Oksigen KPPIKDocument42 pagesTerapi Oksigen KPPIKAtikah PurnamasariPas encore d'évaluation
- Abdominal Pain in ChildrenDocument48 pagesAbdominal Pain in ChildrenSurin Jayawardene100% (1)