Académique Documents
Professionnel Documents
Culture Documents
7 Respiration
Transféré par
CLEMENTTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
7 Respiration
Transféré par
CLEMENTDroits d'auteur :
Formats disponibles
Guyton & Hall: Textbook of Medical Physiology, 11th Edition
UNIT VII: Respiration
MULTIPLE CHOICE
1. Patients with emphysema have lungs with reduced elastic recoil, leading to an
increase in resting lung volume or functional residual capacity (FRC). FRC consists
of two subvolumes called
a. Tidal volume and residual volume
b. Inspiratory reserve volume and expiratory reserve volume
c. Tidal volume and expiratory reserve volume
d. Expiratory reserve volume and residual volume
ANS: D
FRC is the volume of air that remains in the lungs at the end of normal expiration. FRC
includes the expiratory reserve volume and the residual volume (i.e., the volume
remaining in the lungs after forced expiration).
2. Which one of the following spirometric terms best represents the total volume of gas
that can be inspired after a normal, quiet expiration?
a. Inspiratory capacity
b. Functional residual capacity
c. Inspiratory reserve volume
d. Vital capacity
ANS: A
Inspiratory capacity represents the maximum volume of air that can be expired,
beginning at the normal resting volume of the chest, achieved at the end of a quiet
expiration. Inspiratory capacity represents full use of the inspiratory reserve volume that
remains after a normal, resting tidal volume.
3. Which one of the following best represents all of the regions of the respiratory system
that are ventilated but that do not participate in gas exchange?
a. Anatomical dead space
b. Anatomical shunts
c. Physiological dead space
d. Physiological shunts
ANS: C
Copyright 2006 by Elsevier, Inc.
Additional Test Bank 2
Physiological dead space includes the anatomical dead space (i.e., conducting system that
consists of the nose, mouth, throat, trachea, and bronchi down to the terminal
bronchioles) and the alveolar dead space (i.e., any alveoli that are ventilated but not
perfused). Shunts are produced when gas exchange areas of the lung are perfused with
blood but are not ventilated.
4. Which one of the following spirometric terms best represents the largest tidal volume
that an individual can generate?
a. Inspiratory reserve volume
b. Inspiratory capacity
c. Vital capacity
d. Total lung capacity
ANS: C
The tidal volume represents the volume of air breathed in or out with a single breath. The
largest tidal volume occurs during a maximum expiratory effort that follows a maximum
inspiratory effort (often called the forced vital capacity [FVC]), using the individual's full
inspiratory capacity and expiratory reserve volume.
5. Which one of the following spirometric terms represents the additional volume of air
that can be expired after a normal, quiet expiration?
a. Residual volume
b. Functional residual capacity
c. Expiratory reserve volume
d. Tidal volume
ANS: C
A normal, quiet, passive expiration returns the chest to its resting volume, equivalent to
the spirometric designation of functional residual capacity (FRC). Active contraction of
the accessory muscles of expiration can decrease lung volume even further, down to the
residual volume (RV). This additional volume of air that can be expired after a quiet
expiration is called the expiratory reserve volume (ERV).
6. Two students, Martha and George, are at rest and breathing normally. Martha decides
to double her tidal volume and decrease her respiratory rate to one half of its resting
value. George decides to double his respiratory rate and reduce his tidal volume to
one half of its resting value. Which student will most likely have an increase in
alveolar ventilation?
a. Martha only
b. George only
c. Both Martha and George
d. Neither Martha nor George
ANS: A
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 3
By doubling her tidal volume, Martha will not increase her dead space and will therefore
more than double the amount of air going to her alveoli. Even if she decreases her
respiratory rate to one half of its resting value, she will still have an overall increase in
alveolar ventilation. George, by reducing his tidal volume to one half of its resting value,
will not decrease his dead space but will reduce the amount of air going to his alveoli by
more than one half. Even if he doubles his respiratory frequency, he will still have an
overall decrease in alveolar ventilation.
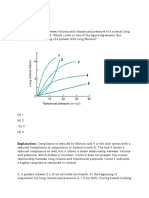
7. Individuals with asthma have increased resistance to airflow due to
bronchoconstriction. Consequently, the work of breathing is increased as higher
pressures become necessary to produce an adequate flow of air. In contrast, airflow
during quiet breathing in normal subjects is produced by a pressure gradient of only
a. 1 cm H2O
b. 5 cm H2O
c. 10 cm H2O
d. 15 cm H2O
ANS: A
Under normal conditions, the flow of air occurs so easily that a pressure of only 1 cm
H2O or less is needed to produce the flow.
8. Burn patients may have collapsed lungs (i.e., atelectasis) because of damage to
surfactant. Treatment with aerosolized synthetic surfactant is often useful. This would
most likely contain the following components:
a. Magnesium ions and sulfate compounds
b. Phospholipids, apoproteins, and calcium ions
c. Dehydrogenated flax oil and phosphorous ions
d. Sulfonic agents
ANS: B
Phospholipids, apoproteins, and calcium ions are the active ingredients of normal
surfactant.
9. In patients with severe asthma, the work of breathing may be 25% or more of the total
energy expended by the body. In contrast, the amount of energy expended for
breathing in normal subjects at rest, as a percentage of total energy expended, is about
a. 1% to 2%
b. 3% to 5%
c. 6% to 8%
d. 10% to 12%
ANS: B
Normal, quiet respiration uses only about 3% to 5% of the total energy expended by the
body.
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 4
10. Patients in respiratory failure are usually put on mechanical ventilators set to deliver
an appropriate tidal volume and frequency. If the tubing connecting the ventilator to
the patient has a volume of 200 ml, appropriate ventilator settings to provide alveolar
ventilation of 4200 ml/min for a 70-kg adult would be approximately
a. Volume = 700 ml; frequency = 12
b. Volume = 500 ml; frequency = 14
c. Volume = 500 ml; frequency = 12
d. Volume = 600 ml; frequency = 10
ANS: A
Alveolar ventilation is described by this equation: (tidal volume dead space)
frequency. The volume of anatomical dead space in adults is about 150 ml. With the extra
200 ml of dead space due to ventilator tubing, the volume should be set at 700 ml to
produce the following result: (700 350) 12 = 4200 ml/min.
11. An elderly patient with emphysema was admitted to the emergency room after he was
found comatose and cyanotic. He was placed on a ventilator with the following
settings: ventilator rate = 10 strokes per minute; volume = 800 ml per stroke; positive
end expiratory pressure = 5 cm H2O; volume of ventilator tubing going to patient =
300 ml. The minute volume (milliliters of air per minute) provided to the patient's
lungs is
a. 5000 ml/min
b. Cannot be calculated from these data
c. 8000 ml/min
d. 800 ml/min
ANS: C
Minute volume is defined as breathing frequency tidal volume. In this case, the
ventilator provides a frequency of 10 strokes per minute and a volume of 800 ml per
stroke. This provides a minute volume of 8000 ml/min. The volume of the tubing (300
ml) increases the dead space, but it does not change the minute volume.
12. In congestive heart failure, pulmonary blood vessels often become distended, leading
to an increase in pulmonary blood volume, including capillary blood volume. Normal
values of total pulmonary blood volume and capillary blood volume are about
a. Total = 700 ml; capillary = 100 ml
b. Total = 450 ml; capillary = 70 ml
c. Total = 1500 ml; capillary = 500 ml
d. Total = 2500 ml; capillary = 300 ml
ANS: B
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 5
Blood volume of the lungs is about 450 ml, which is about 9% of total blood volume of
the circulatory system. About 70 ml of this volume resides in the pulmonary capillaries,
and the remainder is divided about equally between the arteries and veins.
13. In a patient with chronic bronchitis who has regions of her lungs that are poorly
ventilated and have a low value for alveolar PO2, which one of the following
physiological compensatory mechanisms would help redistribute blood to other areas
of her lungs that are better ventilated?
a. Reflex bronchoconstriction
b. Local metabolic vasodilation
c. Hypoxic vasoconstriction
d. Increased dead space ventilation
ANS: C
Hypoxic vasoconstriction, a phenomenon restricted to the pulmonary vasculature, diverts
blood away from areas of low PO2 within the lung and toward regions with higher PO2
values, which helps to maintain ventilation-perfusion ratios. This pattern is opposite that
of the metabolic vasodilation that occurs in other tissues when tissue PO2 falls.
14. A patient suffering from anxiety disorder is admitted to the emergency room
complaining of severe headache and dyspnea. She is breathing room air at sea level
(inspired PO2 = 149 mm Hg) and has a respiratory exchange ratio of 1.0. The arterial
blood gas values are a PaO2 of 90 mm Hg, PaCO2 of 20 mm Hg, and pH of 7.30.
These values indicate which of the following circumstances?
a. Alveolar-arterial PO2 difference exceeds 20 mm Hg.
b. Plasma bicarbonate concentration is elevated.
c. Patient is hypoventilating.
d. Patient probably has partially compensated metabolic alkalosis.
ANS: A
The alveolar PO2 is found from the alveolar gas equation:
PaO2 = PIO2 -PaCO2/R. We can assume that the inspired PO2 is the sea-level normal
value of 149 mm Hg. Neglecting the small correction factor, the alveolar PO2 is 149-20/1
= 129 mm Hg. The alveolar-arterial PO2 diffusion is 12 - 90 = 39 mm Hg. The PCO2 of
20 mm Hg means that the patient is hyperventilating. The combination of the low PCO2
and low pH means that the plasma bicarbonate concentration is reduced. The Henderson-
Hasselbalch equation states that pH = pK + log [HCO3-]/(PCO2 0.03).
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 6
15. A patient with congestive heart failure is evaluated in the cardiac catheterization
laboratory. A balloon-tipped, multilumen Swan-Ganz catheter is advanced from a
peripheral vein into the right atrium, moved into the right ventricle, and then
positioned within a branch of the pulmonary artery. The distal port measures
pulmonary artery pressure, and the proximal port measures right atrial pressure. The
balloon is then inflated, occluding the branch of the pulmonary artery. The pressure in
the distal port, called wedge pressure, rapidly falls to a value close to left atrial
pressure. Expected pressures in the right atrium (RA); pulmonary artery, systolic
(PAS) and diastolic (PAD); and left atrium (LA) are approximately
a. 2 (RA), 120 (PAS), 80 (PAD), 25 (LA)
b. 5 (RA), 45 (PAS), 8 (PAD), 15 (LA)
c. 4 (RA), 32 (PAS), 25 (PAD), 15 (LA)
d. 2 (RA), 25 (PAS), 8 (PAD), 5 (LA)
ANS: D
D is correct because these pressures are normal in the pulmonary circulation. A left atrial
pressure exceeding 15 mm Hg suggests mitral stenosis, mitral insufficiency, severe aortic
stenosis, aortic regurgitation, ventricular failure, or other pathologic conditions. When the
left atrial pressure exceeds 20 mm Hg, it increases pulmonary capillary hydrostatic
pressure, which can lead to pulmonary edema.
16. Patients with heart failure may have a 100% increase in pulmonary blood volume and
pulmonary vascular pressures. Normal pulmonary blood volume is approximately
a. 450 ml
b. 700 ml
c. 200 ml
d. 70 ml
ANS: A
Normal pulmonary blood volume is about 450 ml. Approximately 70 ml of this volume is
located in the pulmonary capillaries (because this is roughly equal to stroke volume, the
entire pulmonary capillary volume is replaced with each heart beat), with the remainder
divided equally between pulmonary arteries and veins.
17. A patient was referred to the pulmonary clinic after complaining of shortness of
breath, cough, and chest pain. Thoracentesis was performed; the procedure removes
fluid from the space between the lining of the outside of the lungs (pleura) and the
wall of the chest. A large volume of fluid was removed, and the fluid contained more
than 30 g/dl of protein. The most likely diagnosis for this patient is
a. Pneumothorax
b. Emphysema
c. Pleural effusion
d. Heroin overdose
ANS: C
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 7
Pleural effusion is the collection of large amounts of free fluid in the pleural space,
analogous to edema fluid in tissues. Common causes of pleural effusion are cardiac
failure, tuberculosis, pulmonary embolism (i.e., blocked pulmonary artery), metastatic
disease (i.e., cancer that has spread to the pleural tissues), lymphoma (i.e., cancer in
lymphoid tissue), and trauma.
18. A swimming pool worker who was accidentally exposed to chlorine gas was taken to
the emergency room after complaining of cough and shortness of breath. A chest
radiograph showed diffuse interstitial pulmonary edema. The mechanism of edema in
this case is probably
a. Hypertension due to heart failure
b. Mitral valve disease
c. Severe pleuritis
d. Damage to pulmonary capillaries
ANS: D
Common causes of pulmonary edema include left-sided heart failure and mitral valve
disease, with both leading to increased pulmonary capillary hydrostatic pressure.
Pulmonary edema also is caused by damage to pulmonary capillaries from infections
such as pneumonia or by breathing noxious substances such as chlorine gas or sulfur
dioxide gas. Damage causes rapid leakage of plasma proteins and fluid out of the
capillaries and into the interstitial space and the alveoli.
19. An elderly, male patient is found to have a lung tumor that blocks airflow to the lower
lobe of his right lung. In this patient, which one of the following most likely is
increased?
a. Residual volume
b. Physiological shunt flow
c. Physiological dead space
d. Pulmonary compliance
ANS: B
The airways distal to the point of obstruction in the patient's right lower lobe cannot be
ventilated. The pulmonary capillary blood leaving the nonventilated alveoli in this region
would retain a low PO2 and high PCO2, would mix with normally oxygenated blood from
normally ventilated regions of the patient's lungs, and would therefore constitute an
increased physiological shunt.
20. A healthy human subject can generate a large increase in the rate of carbon dioxide
production during vigorous exercise without experiencing increases in alveolar or
arterial PCO2. Which one of the following best represents the mechanism by which
alveolar and arterial PCO2 values are maintained in an exercising subject?
a. Decreased diffusion capacity
b. Chloride shift
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 8
c. Decreased dead space ventilation
d. Increased alveolar ventilation
ANS: D
Alveolar and arterial partial pressures of carbon dioxide are determined by the ratio of the
rate of CO2 production to the rate of alveolar ventilation (VCO2/VA). During exercise,
the increased rate of CO2 production is matched by a corresponding increase in alveolar
ventilation, and alveolar and arterial PCO2 values remain essentially unchanged.
21. A hospitalized patient with respiratory disease is given a ventilation-perfusion ( A/
) scan and is found to have some lung regions with very low A/ ratios. Compared
with normal pulmonary venous blood, the pulmonary venous blood draining these
low A/ regions would have a ____ PO2 and a ____ PCO2.
a. Higher higher
b. Higher lower
c. Lower higher
d. Lower lower
ANS: C
Regions of the lung with low ventilation-perfusion ratios have alveolar gas partial
pressures more like those of mixed venous bloodlow PO2 and high PCO2and this is
reflected in the pulmonary venous blood leaving these low A/ regions. Regions of the
lung with high A/ ratios would have alveolar gas partial pressures more like those of
inspired airhigh PO2 and low PCO2which would be reflected in the pulmonary blood
leaving these high A/ regions.
22. A patient complains of severe exercise limitation. Physical examination and
pulmonary function testing reveal normal lung function. Echocardiography reveals no
impairment of heart function. The resulting hypothesis is impairment of oxygen
delivery to working muscles. Which one of the following would have the greatest
effect on the reduction in O2 delivery (arterial O2 concentration cardiac output)?
a. Halving alveolar ventilation
b. A 50% right-to-left shunt
c. Doubling inspired O2
d. Hemoglobin reduced to 50% of normal
ANS: D
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 9
Halving alveolar ventilation would double alveolar PCO2 and therefore reduce alveolar
and arterial PO2, but not enough to halve arterial O2 content. Hypoxia would stimulate
cardiac output by sympathetic stimulation of the heart rate. A 50% right-to-left shunt
would also lower arterial O2 content but not by 50% because the shunted venous blood
has a significant amount of oxygen (normally about 75% saturated). Doubling inspired O2
would, if anything, increase oxygen delivery. D is correct because reducing hemoglobin
concentration to one-half normal would reduce the arterial O2 content (at any saturation)
to one half of its normal level.
23. A patient with iron deficiency anemia is examined for pulmonary function, including
arterial blood gas determinations. If her lung function, metabolic rate, and cardiac
output are normal, you may expect to find which of the following?
a. Arterial PO2 is reduced.
b. Arterial-venous O2 concentration difference is increased.
c. Arterial O2 saturation is reduced.
d. PO2 of mixed venous blood is reduced.
ANS: D
A is incorrect because a patient with anemia and normal lungs typically has a normal
arterial PO2. C is incorrect because the position of the oxygen dissociation curve is
typically normal, and the arterial oxygen saturation level is normal. The Fick principle
holds that O2 = ( T) (CaO2 C O2); total body consumption of oxygen ( O2) is
equal to the product of cardiac output ( T) times the amount of oxygen extracted by
tissues, which is the difference in the arterial oxygen content (CaO2) and mixed venous
oxygen content (C O2). If the oxygen consumption and cardiac output are normal, the
arterial-venous O2 concentration difference will also be normal, and B is therefore
incorrect. Cardiac output is sometimes reflexly increased in anemia, and if this occurs,
the arterial-venous O2 concentration difference will be decreased. Choice D is correct
because, although the arterial PO2 is typically normal, the PO2 of mixed venous blood
must fall. The arterial oxygen content (CaO2) is reduced because there is less
hemoglobin; therefore, venous oxygen content also is reduced, and the venous PO2 is
reduced.
24. Which one of the following best describes the arterial PO2 of a patient suffering from
primary polycythemia (i.e., polycythemia vera) who has a higher than normal
hemoglobin concentration but normal pulmonary gas exchange and normal alveolar
PO2?
a. Significantly higher than normal
b. Essentially normal
c. Significantly lower than normal
ANS: C
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 10
The arterial PO2 represents only the activity of oxygen molecules dissolved in plasma and
not the oxygen molecules bound to hemoglobin. With normal alveolar PO2 and normal
gas exchange, arterial PO2 remains essentially normal over a wide range of hemoglobin
concentrations. Arterial oxygen content, representing both the small amount of dissolved
oxygen and the much larger amount of oxygen bound to hemoglobin, is significantly
increased in a patient with polycythemia.
25. Which one of the following is the most likely mechanism underlying the harmful and
potentially fatal acute effects of carbon monoxide poisoning?
a. Decreased arterial PO2
b. Decreased blood oxygen-carrying capacity
c. Increased hematocrit and blood viscosity
d. Increased red blood cell destruction
ANS: B
The high-affinity binding of carbon monoxide to heme iron decreases the maximum
amount of oxygen that the blood can carry. Because the low concentrations of carbon
monoxide that cause carbon monoxide poisoning do not significantly affect the partial
pressures of oxygen, carbon dioxide, or nitrogen in alveolar gas and arterial blood,
arterial PO2 is relatively normal. Carbon monoxide poisoning does not acutely affect
hematocrit or hemoglobin concentration or affect the rate of red cell destruction.
26. Prolonged exposure of a healthy human subject to high altitude is most likely
accompanied by which of the following?
a. A decrease in intra-erythrocytic 2,3-biphosphoglycerate concentration
b. An increase in arterial PCO2
c. A decrease in alveolar ventilation
d. An increase in hemoglobin concentration
ANS: D
The normal compensations for chronic exposure to high altitude (i.e., ambient hypoxia)
are increases in hemoglobin concentration (to increase arterial oxygen content) and 2,3-
biphosphoglycerate (to decrease oxygen affinity and facilitate oxygen delivery in the
tissue). The ambient hypoxia stimulates an increase in alveolar ventilation, reducing
arterial PCO2.
27. One form of carbon dioxide transport in the blood involves the reversible binding of
carbon dioxide to hemoglobin chains, forming which of the following compounds?
a. Carboxyhemoglobin
b. Bicarbonate
c. Methemoglobin
d. Carbaminohemoglobin
ANS: D
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 11
Carbon dioxide binds in a reversible fashion with amine groups on the globin chains of
hemoglobin, and the carbaminohemoglobin formed accounts for about 30% of the total
carbon dioxide transport from the tissues to the lungs.
28. Arterial blood gas values obtained from a hospitalized patient breathing room air
include the following: PO2, 60 mm Hg; PCO2, 54 mm Hg; hemoglobin concentration,
14 g/dl; and arterial oxygen content, 15.95 ml of O2/dl. What is this patient's
calculated arterial percent saturation?
a. 96%
b. 85%
c. 54%
d. 27%
ANS: B
The maximum oxygen-carrying capacity of this patient's blood can be calculated as the
hemoglobin concentration in g/dl times 1.34 ml of O2 per gram of hemoglobin. For this
patient, the maximum oxygen carrying capacity is 14 1.34, or 18.76 ml of O2/dl.
Because the actual arterial oxygen content is 15.95 ml of O2/dl, the arterial percent
saturation is 15.95/18.76, or 0.85 (85%).
29. Which one of the following would most likely be normal in a patient with severe
anemia but with normal pulmonary gas exchange?
a. Arterial PO2
b. Blood viscosity
c. Arterial oxygen content
d. Hematocrit
ANS: A
In an anemic patient with normal gas exchange, arterial PO2 would be normal, because
PO2 depends only on the dissolved oxygen in the arterial blood and not on the amount of
oxygen bound to hemoglobin. Total arterial oxygen content would be reduced, and both
hematocrit and blood viscosity would be reduced in a patient with anemia.
30. Compared with normal arterial blood, normal mixed venous blood of a healthy
human subject has a ____ PCO2 and a ____ bicarbonate concentration.
a. Higher higher
b. Higher lower
c. Lower higher
d. Lower lower
ANS: A
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 12
The mixed venous blood carries carbon dioxide from the tissues to the lungs in the form
of dissolved CO2, bicarbonate, and carbaminohemoglobin, and the concentrations of all
three forms are higher in mixed venous blood than in arterial blood. An increase in the
PCO2 of the mixed venous blood increases the mixed venous bicarbonate concentration
through the action of red blood cell carbonic anhydrase.
31. A patient with chronic obstructive pulmonary disease is admitted to the emergency
room after complaining of dyspnea. He was placed on high-flow nasal oxygen and
went into respiratory arrest. A likely explanation for this result is
a. Severe metabolic acidosis causing depression of the medulla
b. Paralysis of the diaphragm due to lactic acid
c. Inhibition of hypoxic drive to breath
d. Stimulation of j receptors in the lung
ANS: C
In patients with chronic hypercapnia, the arterial pH and cerebrospinal fluid (CSF) pH are
often within the normal range due to renal retention and CSF regulation, and the main
ventilatory drive comes from hypoxemia. If this hypoxic drive is abolished because of
oxygen therapy and the work of breathing is abnormally high, patients may develop fatal
hypoventilation and severe CO2 retention. Discontinuing the oxygen therapy makes the
subsequent hypoxemia more severe; recall that alveolar PO2 = PIO2 (PaCO2/R).
Problems are normally avoided by not using 100% O2. The reduction in ventilation with
lower levels of oxygen may be beneficial in reducing breathing, which has a high
metabolic cost in these patients.
32. On arriving at high altitude, a healthy, normally sea-level native would immediately
experience an increase in resting minute ventilation that is caused by ____ and that
would result in an ____.
a. Increased arterial PCO2 acidosis
b. Decreased arterial PO2 acidosis
c. Increased arterial PCO2 alkalosis
d. Decreased arterial PO2 alkalosis
ANS: D
The decreased atmospheric PO2 at high altitude stimulates an increase in alveolar
ventilation, which decreases arterial PCO2. This results in respiratory alkalosis.
33. A normal, quiet inspiration is most likely initiated by neurons in which of the
following locations?
a. Central chemoreceptor region
b. Dorsal respiratory group
c. Pneumotaxic center
d. Ventral respiratory group
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 13
ANS: B
The basic rhythm of inspiration is generated mainly by the dorsal respiratory group of
neurons. The central chemoreceptor region helps regulate the overall level of ventilation,
but it does not contribute to the genesis of the respiratory rhythm. The pneumotaxic
center functions to limit inspiration, not stimulate inspiration. The ventral respiratory
group of neurons is relatively inactive during quiet respiration.
34. The ventilatory response to a sudden decrease in arterial PO2 is mediated primarily by
the ____ chemoreceptors, and the ventilatory response to a sudden increase in arterial
PCO2 is mediated primarily by the ____ chemoreceptors.
a. Central central
b. Central peripheral
c. Peripheral central
d. Peripheral peripheral
ANS: C
The peripheral chemoreceptors are responsible for detecting changes in the arterial PO2,
and they send afferent signals to the respiratory center that increase alveolar ventilation.
The central chemoreceptors respond to changes in the hydrogen ion concentrations within
the CNS, caused primarily by changes in the PCO2 of the arterial blood perfusing the
brain, resulting in an increase in ventilation when arterial PCO2 rises.
35. Which one of the following regions of the respiratory center functions to inhibit
inspiration by terminating the activity of the inspiratory neurons?
a. Apneustic center
b. Central chemoreceptors
c. Pneumotaxic center
d. Ventral respiratory group
ANS: C
Increased pneumotaxic center activity switches off the inspiratory neuron activity in the
dorsal respiratory group of neurons, shortening inspiration and secondarily increasing
respiratory frequency. The apneustic center, in the absence of afferent input, stimulates
inspiration; the ventral respiratory group functions to enhance inspiratory and expiratory
activity; and the central chemoreceptor region helps regulate overall levels of ventilation.
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 14
36. A 23-year-old male suffers from a stomach ailment that produces prolonged vomiting
and precipitates a metabolic (nonrespiratory) alkalosis. The respiratory response to
this alkalosis would most likely be a ____ in alveolar ventilation, which would ____
arterial PCO2.
a. Decrease decrease
b. Decrease increase
c. Increase decrease
d. Increase increase
ANS: B
Alkalosis caused by a nonrespiratory problem would lead to a compensatory decrease in
alveolar ventilation, a response mediated by the peripheral chemoreceptors. The decrease
in alveolar ventilation would lead to increased PCO2 and would thereby increase
hydrogen ion concentration back toward normal.
37. After 3 to 4 days of exposure to high altitude, the level of total minute ventilation is
significantly higher than the level seen during the first day of exposure. This
respiratory acclimatization to high altitude primarily results from which one of the
following?
a. Hypertrophy of the inspiratory and expiratory ventilatory musculature
b. Decreased intra-erythrocytic 2,3-biphosphoglycerate concentration
c. Increased hemoglobin concentration
d. Correction of the alkalosis that initially inhibited the ventilatory response to low
oxygen
ANS: D
Acute exposure to high altitude increases ventilation through the response of the
peripheral chemoreceptors to the low oxygen levels. This initial ventilatory response is
limited, however, by the respiratory alkalosis that quickly develops, which inhibits
ventilation by a decrease in the hydrogen ion concentration in the vicinity of the central
chemoreceptors. Gradual restoration of hydrogen ion concentrations toward normal over
3 to 4 days of exposure to high altitude removes the inhibition of ventilation due to
alkalosis, and the ventilatory response to the low oxygen can be fully manifested.
38. The sensation of dyspnea that is frequently experienced by patients with pulmonary
edema is primarily caused by which one of the following?
a. Stimulation of irritant receptors in the airways
b. Increased central chemoreceptor sensitivity to carbon dioxide
c. Stimulation of "J" receptors in alveolar walls near pulmonary capillaries
d. Decreased peripheral chemoreceptor sensitivity to oxygen
ANS: C
Copyright 2005 by Elsevier, Inc.
Additional Test Bank 15
Sensory nerve endings in alveolar walls in juxtaposition to the pulmonary capillaries are
stimulated when the pulmonary capillaries are engorged with blood or when pulmonary
edema occurs. Irritant receptors are responsible for the cough and sneeze reflexes, and
changes in chemoreceptor sensitivities do not play a role in the dyspnea associated with
pulmonary edema.
39. A 76-year-old, retired shipyard worker presents complaining of difficult breathing,
persistent cough, and chest pain. Pulmonary function testing on this patient reveals
decreased total lung capacity, vital capacity, and residual volume and finds a normal
value for the FEV1/FVC ratio. This spirometric pattern is most consistent with which
one of the following?
a. Obstructive lung disease
b. Atelectasis
c. Constrictive (or restrictive) lung disease
d. Hypoxic vasoconstriction
ANS: C
Constrictive, or restrictive, lung disease is characterized by decreased pulmonary
compliance, in which reduces total lung capacity, vital capacity, and residual volume.
Obstructive lung disease manifests primarily as a decrease in the rate at which air can
move out of the lung (i.e., a decrease in the FEV1/FVC ratio), and it is not necessarily
associated with decreases in lung volumes. Atelectasis refers to collapse of portions of the
lung, and hypoxic vasoconstriction is a vascular phenomenon.
40. Even a healthy human subject has a maximum expiratory flow rate that cannot be
exceeded despite greatly increased expiratory force. This phenomenon most likely
results from which of the following?
a. Limited strength of the expiratory musculature
b. Compression of the bronchioles and increased airway resistance
c. High resistance to airflow through the larynx
d. Excessive negative intrapleural pressure
ANS: B
With intense expiratory effort, the increased pressure gradient promoting airflow out of
the lung is matched by an increase in airway resistance due to compression of the
bronchioles. Further increases in expiratory effort increase the pressure gradient
promoting expiratory airflow and the airway resistance, preventing further increases in
flow. The strength of the expiratory musculature is not a critical factor in a healthy human
subject. Likewise, in a healthy human subject, resistance at the larynx does not limit
airflow, and intrapleural pressure is less negative (or even positive) during expiratory
efforts.
Copyright 2005 by Elsevier, Inc.
Vous aimerez peut-être aussi
- Anatomy and PhysiologyDocument3 pagesAnatomy and PhysiologyGichana ElvisPas encore d'évaluation
- CVS Embryology Questions and Study Guide - Quizlet Flashcards by Hugo - OxfordDocument5 pagesCVS Embryology Questions and Study Guide - Quizlet Flashcards by Hugo - OxfordAzizPas encore d'évaluation
- Respiratory System Study GuideDocument13 pagesRespiratory System Study GuidebisnumPas encore d'évaluation
- Section-I Mcqs and SeqsDocument3 pagesSection-I Mcqs and SeqsSadia NasirPas encore d'évaluation
- 2 K 23 Mbbs CurriculumDocument300 pages2 K 23 Mbbs CurriculumAbdullah Nayyar100% (1)
- CVS MCQsDocument1 pageCVS MCQsManisha JindalPas encore d'évaluation
- MCQs On CVS Pharmacology by Medical Study CenterDocument47 pagesMCQs On CVS Pharmacology by Medical Study CenterLin YunPas encore d'évaluation
- U Michigan Written Practice Quiz Brain and MeningesDocument3 pagesU Michigan Written Practice Quiz Brain and MeningesJublant JimmiyahPas encore d'évaluation
- Mbbs Question BankDocument38 pagesMbbs Question BankHappy MukherjeePas encore d'évaluation
- Respiratory QuestionsDocument116 pagesRespiratory QuestionsNatukunda Dianah100% (1)
- MCI Screening Test 2005Document46 pagesMCI Screening Test 2005Iboyaima SinghPas encore d'évaluation
- Anatomy QBank Volume Two ThoraxDocument57 pagesAnatomy QBank Volume Two ThoraxDan Mupenzi100% (1)
- PHYSIO MCQsDocument10 pagesPHYSIO MCQsarwa fawzy100% (1)
- Physiology Mcqs August 2011Document13 pagesPhysiology Mcqs August 2011banje746Pas encore d'évaluation
- Quiz On The Chest WallDocument10 pagesQuiz On The Chest WallNajah Hanim100% (2)
- Hemodynamics Practice QuestionsDocument2 pagesHemodynamics Practice QuestionsMax HocksteinPas encore d'évaluation
- 2nd MB Resit 2019 Respiration QuestionsDocument5 pages2nd MB Resit 2019 Respiration Questionsada100% (1)
- 054 Physiology MCQ ACEM Primary RenalDocument1 page054 Physiology MCQ ACEM Primary RenalYasif AbbasPas encore d'évaluation
- MCQ Anatomy-thorax-Abdo-PelvisDocument100 pagesMCQ Anatomy-thorax-Abdo-PelvisMatt McCannPas encore d'évaluation
- Ganong Physiology 21eDocument1 pageGanong Physiology 21eprasun_v0% (1)
- Biochem Practical QuestionsDocument13 pagesBiochem Practical QuestionsBurhan HameedPas encore d'évaluation
- Skeletal System ExamDocument9 pagesSkeletal System ExamBijay Kumar Mahato100% (1)
- Quiz - Development of Human Cardiovascular SystemDocument7 pagesQuiz - Development of Human Cardiovascular Systemlucky mbaselaPas encore d'évaluation
- Bone McqsDocument4 pagesBone McqsAwan1994100% (2)
- Wiley Edition 13 ch26Document54 pagesWiley Edition 13 ch26philip100% (1)
- MCQ CVS AnswersDocument4 pagesMCQ CVS AnswersDEOGRATIAS NDAYISABAPas encore d'évaluation
- (K) Gastroenteritis and Fluid VolumeDocument1 page(K) Gastroenteritis and Fluid Volumeapi-3769252Pas encore d'évaluation
- First Part Exam - March 2021Document28 pagesFirst Part Exam - March 2021hassan mohamedPas encore d'évaluation
- 47 MCQs On GI and Nutrition PhysiologyDocument14 pages47 MCQs On GI and Nutrition Physiologyrazsubedi100% (1)
- Respiratory Module TestDocument14 pagesRespiratory Module TestMuhammad AhmadPas encore d'évaluation
- Cerebellum MCQ'S: A) Posterior LobeDocument2 pagesCerebellum MCQ'S: A) Posterior LobeTahir AzizPas encore d'évaluation
- Physiology 3RD Test Steeplechase Revision 2023Document3 pagesPhysiology 3RD Test Steeplechase Revision 2023NewtonPas encore d'évaluation
- Cardiovascular SystemDocument9 pagesCardiovascular SystemShan ShaniPas encore d'évaluation
- Class Notes On Questionnaires For Pharmacology in The Gastrointestinal TractDocument12 pagesClass Notes On Questionnaires For Pharmacology in The Gastrointestinal TractMarqxczPas encore d'évaluation
- MCQs On GITDocument3 pagesMCQs On GITsamuel waiswaPas encore d'évaluation
- Shams Pulmonary Quiz 1Document9 pagesShams Pulmonary Quiz 1tylermedPas encore d'évaluation
- Anatomy Abdomen MCQs For DNBDocument62 pagesAnatomy Abdomen MCQs For DNBPG Aspirant100% (2)
- Physiology Final Exams JULY 8, 2020Document17 pagesPhysiology Final Exams JULY 8, 2020Ndor BariboloPas encore d'évaluation
- Second Year ExamDocument4 pagesSecond Year ExamSyamil AzharPas encore d'évaluation
- DocxDocument22 pagesDocxmuryum100% (1)
- Cvs MCQDocument52 pagesCvs MCQMiracle For NursesPas encore d'évaluation
- Physiology Magdy Sabry GITDocument84 pagesPhysiology Magdy Sabry GITallswell addoPas encore d'évaluation
- Compiled MSPC 235 Past Questions Volume IIIDocument15 pagesCompiled MSPC 235 Past Questions Volume IIIPaapaErnestPas encore d'évaluation
- CVS MCQDocument11 pagesCVS MCQمصطفى حسن هاديPas encore d'évaluation
- Histology Final ExamDocument8 pagesHistology Final Examliz gamezPas encore d'évaluation
- Anatomy and Physiology of The ThoraxDocument6 pagesAnatomy and Physiology of The ThoraxdocaliPas encore d'évaluation
- MCQ ChoDocument31 pagesMCQ Choامجد حسين جواد كاظمPas encore d'évaluation
- Past Questions - AnatomyDocument17 pagesPast Questions - AnatomyInnocent L NdambakuwaPas encore d'évaluation
- C. Common Cardinal VeinsDocument6 pagesC. Common Cardinal VeinsTofik MohammedPas encore d'évaluation
- Important Seqs of Biochemistry For 1st Year Mbbs StudentsDocument7 pagesImportant Seqs of Biochemistry For 1st Year Mbbs Studentsdr saadia anjum0% (1)
- A and P II: Test I Review Questions On Cardiovascular SystemDocument50 pagesA and P II: Test I Review Questions On Cardiovascular SystemMartina MicicPas encore d'évaluation
- Lymphoid System MCQDocument8 pagesLymphoid System MCQAbduladheemPas encore d'évaluation
- Zanki Respiratory PhysiologyDocument19 pagesZanki Respiratory Physiologysmian08Pas encore d'évaluation
- Sense OrgansDocument8 pagesSense OrgansKeelah BennPas encore d'évaluation
- MCQ 23 Physio AnswersDocument8 pagesMCQ 23 Physio AnswersJulyhathul Kuraishi100% (1)
- MCQ On Biochemistr2Document3 pagesMCQ On Biochemistr2BassamSheryanPas encore d'évaluation
- Depa SGDDocument40 pagesDepa SGDEhrli CuaresmaPas encore d'évaluation
- Explaination To Answers of Respiration Test Date: 16.08.2020Document1 pageExplaination To Answers of Respiration Test Date: 16.08.2020Shubham SsPas encore d'évaluation
- Pulmonary Function TestsDocument38 pagesPulmonary Function TestsMohamedSalahPas encore d'évaluation
- 8.aviation, Space and Deep Sea Diving PhysiologyDocument5 pages8.aviation, Space and Deep Sea Diving PhysiologyCLEMENTPas encore d'évaluation
- 2.membrane Physiology, Nerve and MuscleDocument6 pages2.membrane Physiology, Nerve and MuscleCLEMENT100% (1)
- History Taking and Physical Examination, Level 5Document48 pagesHistory Taking and Physical Examination, Level 5CLEMENTPas encore d'évaluation
- 1.introduction To Physiology, The Cell and General PhysiologDocument3 pages1.introduction To Physiology, The Cell and General PhysiologCLEMENT100% (1)
- Sports PhysiologyDocument3 pagesSports PhysiologyCLEMENTPas encore d'évaluation
- Synthesis of Eicosanoids and SignalingDocument10 pagesSynthesis of Eicosanoids and SignalingCLEMENTPas encore d'évaluation
- Aqueous SolutionsDocument57 pagesAqueous SolutionsCLEMENTPas encore d'évaluation
- Pathological Response To Infectious and Parasitic DiseasesDocument36 pagesPathological Response To Infectious and Parasitic DiseasesCLEMENTPas encore d'évaluation
- Pathogenesis and Classification of NeoplasiaDocument36 pagesPathogenesis and Classification of NeoplasiaCLEMENT0% (1)
- The HeartDocument15 pagesThe HeartCLEMENTPas encore d'évaluation
- Genetics: Definition: Branch of Biologic Science That Deals With Transmission of Characters From Parents To OffspringsDocument22 pagesGenetics: Definition: Branch of Biologic Science That Deals With Transmission of Characters From Parents To OffspringsCLEMENTPas encore d'évaluation
- Development of A Research ProposalDocument25 pagesDevelopment of A Research ProposalCLEMENTPas encore d'évaluation
- Pain Sensation and Pathophysiology of Headache: Presenter: DR William Ramadhan.A FACILITATOR: DR M A. NjelekelaDocument34 pagesPain Sensation and Pathophysiology of Headache: Presenter: DR William Ramadhan.A FACILITATOR: DR M A. NjelekelaCLEMENTPas encore d'évaluation
- Clinical Epidemiology of The Leading Causes of MorbidityDocument22 pagesClinical Epidemiology of The Leading Causes of MorbidityCLEMENTPas encore d'évaluation
- Nutritional and Nutritional RequirementsDocument25 pagesNutritional and Nutritional RequirementsCLEMENTPas encore d'évaluation
- Growth and Development in Children by Dr. Rafia. IqbalDocument34 pagesGrowth and Development in Children by Dr. Rafia. IqbalCLEMENTPas encore d'évaluation
- Malaria: Definition: Infection Due To PlasmodiumDocument17 pagesMalaria: Definition: Infection Due To PlasmodiumCLEMENTPas encore d'évaluation
- Clinical Use of Antimicrobial AgentsDocument24 pagesClinical Use of Antimicrobial AgentsCLEMENTPas encore d'évaluation
- DicDocument17 pagesDicCLEMENT0% (1)
- Basic PathologyDocument37 pagesBasic PathologyCLEMENTPas encore d'évaluation
- Antigens, Hapteins, Immunogens Lectures 10.1.06Document32 pagesAntigens, Hapteins, Immunogens Lectures 10.1.06CLEMENTPas encore d'évaluation
- Gas Transport in Blood PPT 1Document34 pagesGas Transport in Blood PPT 1CLEMENTPas encore d'évaluation
- Disorders of Skeletal, Cardiac and Smooth Muscle Cells-Myasthenia Gravis, Muscular Dystrophy and MyotoniaDocument51 pagesDisorders of Skeletal, Cardiac and Smooth Muscle Cells-Myasthenia Gravis, Muscular Dystrophy and MyotoniaCLEMENTPas encore d'évaluation
- Protein Energy Malnutrition (PEM)Document39 pagesProtein Energy Malnutrition (PEM)CLEMENT100% (3)
- Cellular Growth, Injury and Adaptation: DR Kasonda Pediatrician 17/5/2017Document3 pagesCellular Growth, Injury and Adaptation: DR Kasonda Pediatrician 17/5/2017CLEMENTPas encore d'évaluation
- Genital UlcersDocument17 pagesGenital UlcersCLEMENTPas encore d'évaluation
- Hypertension: Definition: BP 95% Percentile Incidence: 1% of All AdolescentsDocument15 pagesHypertension: Definition: BP 95% Percentile Incidence: 1% of All AdolescentsCLEMENTPas encore d'évaluation
- CICM First Part Syllabus 2017 - FINAL 10 07 2017Document33 pagesCICM First Part Syllabus 2017 - FINAL 10 07 2017drewantaPas encore d'évaluation
- Respiratory Physiology NOTESDocument3 pagesRespiratory Physiology NOTESJulienne Sanchez-Salazar100% (1)
- Basics of Mechanical VentilationDocument63 pagesBasics of Mechanical VentilationDiem KhuePas encore d'évaluation
- Monitoring Solutions SA For Respiratory catalogJB25824XX10Nov7 PDFDocument15 pagesMonitoring Solutions SA For Respiratory catalogJB25824XX10Nov7 PDFdcgPas encore d'évaluation
- Pathophysiology Nr.5 Final S.F.ADocument34 pagesPathophysiology Nr.5 Final S.F.AСергей МалайPas encore d'évaluation
- BERNARDI Slow BreathingDocument68 pagesBERNARDI Slow BreathingMiklós BalatinczPas encore d'évaluation
- Test Bank For Clinical Application of Mechanical Ventilation 4th Edition ChangDocument6 pagesTest Bank For Clinical Application of Mechanical Ventilation 4th Edition ChangKevin Jackson100% (38)
- Mechanical Ventilation Basic ModesDocument37 pagesMechanical Ventilation Basic ModesAmr El TaherPas encore d'évaluation
- GVS EngDocument84 pagesGVS EngDaria SergeevnaPas encore d'évaluation
- Guruji Pranayama SadhanaDocument9 pagesGuruji Pranayama Sadhanadr.sush01Pas encore d'évaluation
- Vpap - Sta St-A - iVAPS - User ManualDocument55 pagesVpap - Sta St-A - iVAPS - User ManualDiabestes-stuffPas encore d'évaluation
- Bio 122 Chapter 22Document155 pagesBio 122 Chapter 22Eyvan EvanPas encore d'évaluation
- High-Frequency Oscillatory Ventilation: Theory and Practical Applications Jane PillowDocument39 pagesHigh-Frequency Oscillatory Ventilation: Theory and Practical Applications Jane PillowJimmy PinoPas encore d'évaluation
- Respiratory Physiology NoteDocument19 pagesRespiratory Physiology NotePeter Wong0% (1)
- Diffusion, Exchange & Transport of O2 & Co2Document79 pagesDiffusion, Exchange & Transport of O2 & Co2Darshika Vyas MohanPas encore d'évaluation
- Arterial Blood Gas InterpretationDocument69 pagesArterial Blood Gas InterpretationostuffePas encore d'évaluation
- 43 Adaptive Support Ventilation As VDocument5 pages43 Adaptive Support Ventilation As Vnanang criztaPas encore d'évaluation
- ANP1105B Topic 6B Respiratory Physiology 2014Document42 pagesANP1105B Topic 6B Respiratory Physiology 2014mdhPas encore d'évaluation
- Dead Space The Physiology of Wasted Ventilation ERJ 2015Document13 pagesDead Space The Physiology of Wasted Ventilation ERJ 2015Javier SegoviaPas encore d'évaluation
- Quiz RespiratoryDocument123 pagesQuiz RespiratoryMedShare100% (23)
- KZ-103-EN149-test-report For SURGICAL MASKDocument12 pagesKZ-103-EN149-test-report For SURGICAL MASKMd. Moniruzzaman Precision GroupPas encore d'évaluation
- Respiration Physiology SEQs With KeyDocument12 pagesRespiration Physiology SEQs With KeyMudassar Roomi100% (1)
- Eng Hamilton t1 SpecsDocument6 pagesEng Hamilton t1 SpecsArbjan RusiPas encore d'évaluation
- USMLE Step 1 EquationsDocument1 pageUSMLE Step 1 EquationsDina Nadeem100% (2)
- Pulmonary Physiology of The NewbornDocument39 pagesPulmonary Physiology of The NewbornADPas encore d'évaluation
- Lab 6 Respiratory PrelabDocument23 pagesLab 6 Respiratory Prelabkkk13whyPas encore d'évaluation
- Department of Mechanical & Industrial Engineering MIE458: Biofluid MechanicsDocument20 pagesDepartment of Mechanical & Industrial Engineering MIE458: Biofluid Mechanicsrhea100% (1)
- The Structured Oral Examination in AnaesthesiaDocument287 pagesThe Structured Oral Examination in AnaesthesiaGerman Yakushkin100% (8)
- Inspiration 7i Ventilator BrochureDocument6 pagesInspiration 7i Ventilator BrochureAgung WicaksanaPas encore d'évaluation
- Spiro ScoutDocument2 pagesSpiro ScoutskyperxPas encore d'évaluation