Académique Documents
Professionnel Documents
Culture Documents
07.gordon Health Assessment and ROS
Transféré par
Keith Wesley Ybut0 évaluation0% ont trouvé ce document utile (0 vote)
69 vues9 pageshfyfufhjg
Titre original
07.Gordon Health Assessment and ROS
Copyright
© © All Rights Reserved
Formats disponibles
DOCX, PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documenthfyfufhjg
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
69 vues9 pages07.gordon Health Assessment and ROS
Transféré par
Keith Wesley Ybuthfyfufhjg
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 9
Psychosocial Profile (Gordons Functional Pattern)
Description Assessment
Initial Ongoing Ongoing Appraisal
(Sept. 22, 2017) (October 21, 2017) (November 08, 2017)
Health Perceived level on health Patient has no recent surgery. Patient still has no recent Patient still has Rheumatic
Perception and and well-being and Patient doesnt have any vices. surgery. Reco Ibarra heart disease without any
Health practices for maintaining He doesnt use cigarettes and Verbalized that his major surgery. Patient is exposed to
Management health. Habits that may be doesnt drink alcohol. During illness is rheumatic heart his uncle who uses cigarettes,
detrimental to health are our first visit, Gikan sa pag- disease. During assessment, dust from the surroundings and
also evaluated, including anak sa akoa, naa nakoy sakit we asked Reco Ibarra what smoke from their dirty kitchen,
smoking, and use of sa heart as verbalized by the are his usual health he does not perceive it as a
alcohol or other drugs. patient. He was admitted last management and he verbalized high risk for developing
April 2017 at St. Joseph that he monthly visits his another cause of diseases. Still
Southern Hospital with his doctor, Dr. Abrena, a his usual blood pressure is
chief complaint of dizziness cardiologist at Don Carlos, 140/100 if antihypertensive
and fainting. His usual blood Maramag, Bukidnon. Still his medication is not taken.
pressure is 140/100 if usual blood pressure is
antihypertensive medication is 140/100 if antihypertensive
not taken. medication is not taken.
Nutrition and Pattern of food and fluid Reco Ibarra Patient is still underweight No appetite changes. Able to
Metabolism intake relative to metabolic Verbalized that he has good with the BMI of 17.3604. No eat average daily food but
needs. The adequacy of eating appetite. He usually food allergies but restricted to restricted to eat chocolates,
local nutrients supplies is consumes vegetables, fish, eat chocolates and drinking green leafy vegetables,
evaluated. rice and fruits and he limits to coffee. He only drinks water drinking coffee, and advised to
consume foods like chocolates not more than 6 glasses per drink only 6 glasses of water
and coffee. And he also day as ordered by his Doctor per day.
verbalized that he eats
everything what is served on
the table. He is underweight as
evidence by his body mass
index is 17.3604.
Elimination Excretory pattern (GI, GU, Reco Ibarra verbalized that Patient urinates 3-4 times a Patient feels no discomfort in
Pattern and skin). Incontinence, he has no any family history of day with yellowish in color his elimination pattern.
constipation, diarrhea and kidney diseases/failure. He with no presence of blood. Urgency to defecate usually
urinary retention. stated that he usually defecates Early in the morning, he early in the morning. No used
once a day with a brownish- usually defecates once a day of laxatives. Patient able to
yellow coloured and formed with no presence of blood. urinate 6 times a day without
stool. In terms of voiding, Sometimes, he experienced any discomfort feels. No
Reco Ibarra usually urinates constipation or diarrhea. problem with bladder control.
3-4 times a day, with a Sometimes, he experienced
yellowish coloured urine. diarrhea and constipation.
Activity- Activities of daily living Nara man ko sa balay sa Patient used to stay in the Patient is still exposed to dust
Exercise Pattern requiring energy akong uncle permi maam, waiting shed near the highway and smokes. The patient is
expenditure including self- usahay maglakaw-lakaw uban to sell some bananas and is advised to avoid heavy
care activities. Assess sa barkada ug gabantay pud ko exposed to dust and smoke workloads and extraneous
major body system diri sa baligya namo nga from the cars passing by. activities. Reco still felt
involved with the activity saging as Reco verbalized. Patient has limited daily joint pain during some of his
and exercise including activities such as walking, activities.
respiratory, cardiovascular Sometimes Reco felt joint
and musculoskeletal pain during some of his
systems. activities.
Sleep-Rest Sleep, rest and relaxation Reco verbalized that he The patient sleep routine is Patient sleeps 7-9 hours
Pattern practices. Dysfunctional usually sleeps at 10:00 pm and 7:00 pm to 5:00 am. No soundly. Still with episodes of
sleep pattern and fatigue wakes up by 7:00 in the symptoms of sleep apnea. waking up because of
may be identified. morning. He also stated that he Sometimes, his sleep is disturbance due to urination at
gets 30 minutes to 1 hour of disturbed due to urination at night.
nap on the afternoon. Sleep night.
disturbance rarely occurs for
Reco and this was
associated to urination at
night.
Cognitive- Ability to comprehend and Reco is a high school Patient was able to understand Patient still has no problems on
Perceptual use information. Assess graduate. Able to hear, see, the questions being asked to his sensory functions, and is
Pattern sensory function. Sensory speak without difficulties. him but sometimes there are able to comprehend. Already
experience such as pain some deviations on his able to answer questions
and altered and altered answers. No problems on his without deviations.
sensory input may be sensory function.
identified and evaluated.
Self-Perception Ability to perceive concept Kulbaan ko usahay sa akong Still fears about his current Patient is conscious and
and Health of self and perception condition, labi na katong nag- health conditions. Patient is coherent, even he fears about
Concept Pattern towards current situation ingon ang doctor nga calm and able to answer his condition, he still shows
and scale of perception. kinahanglan ko operahan he questions being asked to him. being happy to live his life.
verbalized as we asked him
about his condition.
Role- Roles in the world and Reco is currently living with Patient still lived with his Still separated with his mother
Relationship other relationships. his uncle since the day that his uncle while his mother is and lived with his uncle and
Pattern Satisfaction with roles, father died due to an accident. separated from them having a grandmother. Patient still
role strain or dysfunctional He was separated to his mother new family. He helped with assumes the responsibilities of
relationship may be further since that day, as his mother his uncle and grandmother. He taking care of their pigpens
evaluated. found a new partner in life. is the one who takes care for and stall helping his uncle and
Wala namay pakialam ang their pigpen and their stall. grandmother especially in
iyang inahan ni Reco sa doing household chores.
iyaha bisan naa siyay sakit, dili
na daw siya magpasilabot sa
iyaha as verbalized by Recos
uncle.
Sexuality- Satisfaction/dissatisfaction Reco is single and not Patient still is single and not Still with no sexual activities
Reproductive with sexual partners and sexually active. sexually active. done
Pattern production functions.
Concerns with sexuality
may be identified.
Coping Stress General coping pattern and Patient sometimes has Patient still keep his personal Patient is already able to share
Tolerance effectiveness in terms of problems in coping skills problems inside of him, and some of his problems with his
Pattern handling stress. because he will just keep it sometimes he listens music as friends, and still listens to
inside in him, there is no one a way of coping his stress. some music for coping stress.
he can tell his problem on even
his friends.
Value-Belief Values, belief and goals Family belongs to a Cebuano Patient is a Roman Catholic in There are no significant effects
Pattern that may guide choices or ethnicity and a Roman religion of religious beliefs to the
decision. Catholic. patients current situation.
Patient is a Roman Catholic in
religion.
GENERAL HEALTH SURVEY
AREA/SYSTEM PHYSICAL ASSESSMENT
INSPECTION PALPATION PERCUSSION AUSCULTATIO NURSING
N DIAGNOSIS &
PROBLEMS
1. INTEGUMENTARY Skin was brown Cold humid Impaired Skin
and even skin Integrity
Cold humid skin Poor skin
Nails were turgor Hypothermia
untrimmed and
appear pale
Lesion was seen in
lower extremities ------------------------ ----------------------
No redness noted
Body temperature
of 35.3 degree
Celsius
2. HEAD and NECK Skull is No Fluid Volume
normocephalic tenderness Deficit
Hair is black and upon
evenly distributed palpation
Pupils equally
round and reactive
to light and
accommodation
from 4 mm to 2 -------------------------- ----------------------
mm.
Yellowish sclera
observed on both
eye
Lips appeared dry
and pale
3. RESPIRATORY Thorax is Respiratory Lungs/Thorax Crackles Ineffective
symmetric depths are are resonant sound Breathing
Respiratory rate is irregular during heard upon Pattern
25 cycle per minute percussion auscultatio
n
4. CARDIOVASULAR Jugular distention Radial pulse Murmurs Decrease
noted was strong, heard upon Cardiac Output
Extremities were bounding auscultatio
mostly cold to and irregular n Ineffective
touch, pale and in terms of Irregulariti Tissue
humid pattern es in apical Perfusion
140/100 blood Pulse rate of pulse in
pressure 62 beats per terms of
minute rate
Brachial ------------------------- Heart rate
pulse of 65 of 53 beats
beats per per minute
minute
Capillary
refill time is
4 seconds
indicating
delay
5. GASTROINTESTINAL Lesions are noted Firm Dullness on Heartbeat Impaired Skin
The client had a abdominal four quadrants was heard Integrity
history of muscles heard on the
constipation and No upper left Risk for
diarrhea tenderness quadrant Constipation
Eliminates waste felt upon Bowel and Diarrhea
twice a day; palpation sound
heard with
17 clicks
per 5
minutes
6. MUSCULOSKELETAL Symmetrical No nodules Altered ability
bodily structures or any mass to continue
and is able to palpated on previous
mobilize any joint of activities
Normal gait muscle site
No muscle wasting -------------------------- ----------------------
No inflammation,
swelling or wound
noted
Sometimes he felt
joint pain
7. NEUROLOGIC Responsive and Risk for
able to answer Trauma
questions
Oriented to time,
place and event ------------------------ --------------------------- ----------------------
He has history of
fainting and
dizziness.
8. GENITOURINARY Voids 3-4 times a No bladder
day with a distention
yellowish coloured
urine
No pain felt upon
urination -------------------------- ---------------------- -------------------
REVIEW OF SYSTEMS
General: The patient 20 years old. The patient is calm, responsive, cooperative, clean, no foul odor. Body proportions are normal. He has a traumatic
life event when his father died five years ago and when he was separated to his mother. The patient has rheumatic heart disease since birth. He
was recently admitted last April 2017 at St. Joseph Southern Hospital with his chief complaint of dizziness and fainting. The patient is single. He
is satisfied with the way his life has been developing despite of his illness and no religious restriction to care.
HEENT: The patient experiences no visual changes but the sclera is yellowish in colour, no hearing loss, and no impaired sense of taste and smell.
With history of headache, fever, cough, dizziness and faint.
Respiratory: The patient had experience dyspnea and does use accessory muscle to assist breathing. Has symmetric chest expansion. The patient
do not smoke.
Cardiovascular and Hematologic: The patient had family history of heart disease and hypertension. The patient experiences chest pain and have
visible pulsations at the neck.
Gastrointestinal: The client had a history of constipation and diarrhea. The client usually eliminates his waste twice a day. Lesions are noted on
the abdomen. Heartbeat was heard on the upper left quadrant. Bowel sound heard with 17 clicks per 5 minutes.
Genitourinary: The patient didnt experience painful urination. He usually urinates 3 to 4 times a day and in a total amount of 800 cc. he usually
voids with yellowish colour.
Reproductive: The patient is not sexually active and no history of sexually transmitted disease.
Musculoskeletal: Symmetrical bodily structures and is able to mobilize with normal gait. No muscle inflammation, swelling or wound noted. No
nodules or any mass palpated on any joint of muscle site. But sometimes he feels joint pain.
Neurological: The client doesnt have any problems in smelling, vision, taste, touch and hearing. The patient has coordinated movement, proper
orientation of date and place. The client has no history of loss of consciousness convulsions, trauma and loss of memory. He has history of fainting
and dizziness.
Endocrine: No unexplained weight loss. No polyphagia, no polyuria and no polydipsia.
Vous aimerez peut-être aussi
- Final GORDON'SDocument9 pagesFinal GORDON'Svanilla_frappe95% (21)
- Gordon's Functional Pattern PneumoniaDocument6 pagesGordon's Functional Pattern PneumoniaLei Ortega86% (14)
- Case Study PedroDocument13 pagesCase Study PedroAbaba, NicolePas encore d'évaluation
- Gordons Cva 1Document5 pagesGordons Cva 1Ronalyn GasparPas encore d'évaluation
- Nursing Case Study of Pulmonary Congestion and MRSA PatientDocument12 pagesNursing Case Study of Pulmonary Congestion and MRSA PatientJude Remso LabajoPas encore d'évaluation
- Gordon'S Functional Health PatternDocument3 pagesGordon'S Functional Health PatternSheril Sularte CasanesPas encore d'évaluation
- Iv. Gordon'S Functional Health Pattern Table 1: Gordon's Functional Health Pattern in Patient WithDocument6 pagesIv. Gordon'S Functional Health Pattern Table 1: Gordon's Functional Health Pattern in Patient WithZmiaPas encore d'évaluation
- Group 3 Case Presentation FinalDocument45 pagesGroup 3 Case Presentation FinalKurt Zion QuinesPas encore d'évaluation
- PUD GordonsDocument13 pagesPUD GordonsMarielle CabanbanPas encore d'évaluation
- Case Study SJH First SemDocument10 pagesCase Study SJH First SemKathleen VargasPas encore d'évaluation
- Be Your Own Doctor: Alternative Therapies For Conventional PrescriptionsD'EverandBe Your Own Doctor: Alternative Therapies For Conventional PrescriptionsÉvaluation : 5 sur 5 étoiles5/5 (1)
- Gordon'S Functional Pattern Before Hospitalization During Hospitalization 1. Health Perception-Health Management PatternDocument5 pagesGordon'S Functional Pattern Before Hospitalization During Hospitalization 1. Health Perception-Health Management PatternJisel-Apple BulanPas encore d'évaluation
- 1 PPT Liver CirrhosisDocument65 pages1 PPT Liver CirrhosisDannaMae CastroPas encore d'évaluation
- College Nursing Student's ACL Injury Care PlanDocument5 pagesCollege Nursing Student's ACL Injury Care PlanFrancesca Margarita GoñiPas encore d'évaluation
- Chief ComplaintDocument4 pagesChief ComplaintJen GatchalianPas encore d'évaluation
- Case Study On Chronic Kidney Disease Probably To Secondary HypertensionDocument18 pagesCase Study On Chronic Kidney Disease Probably To Secondary Hypertensionkyeria77% (26)
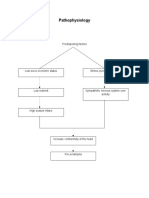
- Pathophysiology: Predisposing FactorsDocument11 pagesPathophysiology: Predisposing FactorsEmerlita ReyesPas encore d'évaluation
- Case StudyDocument25 pagesCase StudybomcorPas encore d'évaluation
- Review of SystemsDocument8 pagesReview of SystemsDendenPas encore d'évaluation
- FINAL PPT of Grand Case Presentation About CKDDocument66 pagesFINAL PPT of Grand Case Presentation About CKDmaria erika94% (16)
- Nursing Assessment IIDocument4 pagesNursing Assessment IIMeg QuidlatPas encore d'évaluation
- Gordons2 CHECK Nyo Nlng..Document7 pagesGordons2 CHECK Nyo Nlng..ackela15Pas encore d'évaluation
- Gordons Threatened AbortionDocument2 pagesGordons Threatened AbortionRobel_Saoi_2309Pas encore d'évaluation
- Hyperthermia and wound infectionDocument10 pagesHyperthermia and wound infectionCleo Joyce C. CristalPas encore d'évaluation
- Group 3 Case Presentation FinalDocument34 pagesGroup 3 Case Presentation FinalKurt Zion QuinesPas encore d'évaluation
- Presented By:: GlomerulonephritisDocument72 pagesPresented By:: GlomerulonephritisRose DaclesPas encore d'évaluation
- Dengue Gordons OnlyDocument5 pagesDengue Gordons OnlyKelvin Pantaleon Ramasta100% (1)
- GORDON-RAMSEY PatternDocument3 pagesGORDON-RAMSEY PatternMarie Ashley CasiaPas encore d'évaluation
- GordonDocument1 pageGordonEzra Miguel DarundayPas encore d'évaluation
- Cadisal MW 1ST Week RequiementsDocument36 pagesCadisal MW 1ST Week RequiementsJonathan GonzalesPas encore d'évaluation
- Case Study FormatDocument15 pagesCase Study Formatpay tinapayPas encore d'évaluation
- Case Report Osteogenesis ImperfectaDocument52 pagesCase Report Osteogenesis ImperfectaFedelis Danii PurnawanPas encore d'évaluation
- Dr. Sebi Food and Herbs List: Potent Dr. Sebi’s Food List and Herbs You Should eat to Cleanse and Revitalize Your Body by Following dr. Sebi’s Alkaline DietD'EverandDr. Sebi Food and Herbs List: Potent Dr. Sebi’s Food List and Herbs You Should eat to Cleanse and Revitalize Your Body by Following dr. Sebi’s Alkaline DietÉvaluation : 5 sur 5 étoiles5/5 (36)
- I. Gordon'S Typology of 11 Health PatternsDocument5 pagesI. Gordon'S Typology of 11 Health PatternsDan Ataniel EnsaladaPas encore d'évaluation
- PersonDocument3 pagesPersonNimrodPas encore d'évaluation
- CHOLEDocument23 pagesCHOLEJun Rennan Sibal PurgananPas encore d'évaluation
- Sample Health HistoryDocument8 pagesSample Health HistoryVal FielPas encore d'évaluation
- Optic-Neuritis GordonsDocument5 pagesOptic-Neuritis GordonsHydie Mae AlcabedosPas encore d'évaluation
- Physical Assessment - TodayDocument5 pagesPhysical Assessment - Todaynoreen.cameros.21Pas encore d'évaluation
- IBS Irritable Bowel Syndrome A Gastroenterologist Answers Your Questions: What Is It? Why Do I Have It? How Can I Get Well?D'EverandIBS Irritable Bowel Syndrome A Gastroenterologist Answers Your Questions: What Is It? Why Do I Have It? How Can I Get Well?Pas encore d'évaluation
- Rumination Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsD'EverandRumination Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsPas encore d'évaluation
- Acute Gastroenteritis (Age)Document37 pagesAcute Gastroenteritis (Age)Jay Ar SantiagoPas encore d'évaluation
- Beating GERD Naturally: A Complete Guide to Managing and Eliminating GerdD'EverandBeating GERD Naturally: A Complete Guide to Managing and Eliminating GerdÉvaluation : 3.5 sur 5 étoiles3.5/5 (3)
- 'S 11 Functional Health Pattern 1. Health Management PatternDocument7 pages'S 11 Functional Health Pattern 1. Health Management PatternYasminGianneDeOcampoBarizoPas encore d'évaluation
- Gordons Finalize After 10yrsDocument4 pagesGordons Finalize After 10yrsShanelli GaviolaPas encore d'évaluation
- Gordon's Functional Health PatternDocument8 pagesGordon's Functional Health PatternDanica NuevaexcijaPas encore d'évaluation
- drug studyDocument7 pagesdrug studyYahiko PainPas encore d'évaluation
- Gordon's Functional Health PatternsDocument4 pagesGordon's Functional Health PatternsDiana JeanPas encore d'évaluation
- Influenza Nausea and Vomiting FeverDocument20 pagesInfluenza Nausea and Vomiting FevercarmaxetaPas encore d'évaluation
- Acute Gastroenteritis: Our Lady of Fatima UniversityDocument24 pagesAcute Gastroenteritis: Our Lady of Fatima UniversityAriaPas encore d'évaluation
- Rahma Safitri (201911027) Nursing Care AngioedemaDocument15 pagesRahma Safitri (201911027) Nursing Care AngioedemaRahma SafitriPas encore d'évaluation
- Health Maintenance and PracticesDocument5 pagesHealth Maintenance and PracticesMrLarry DolorPas encore d'évaluation
- Your kitchen is your clinic: no need going to the hospital when you have a kitchenD'EverandYour kitchen is your clinic: no need going to the hospital when you have a kitchenPas encore d'évaluation
- Ros and PeDocument7 pagesRos and Pedeo_gratias14Pas encore d'évaluation
- Physical Exam Reveals Nutrition and Gallstone Issues in FamilyDocument15 pagesPhysical Exam Reveals Nutrition and Gallstone Issues in Familyriya haryaniPas encore d'évaluation
- Chronic Renal Failure: Prepared by Melrose Virtudazo Christilyn CagasDocument60 pagesChronic Renal Failure: Prepared by Melrose Virtudazo Christilyn CagasJG RNPas encore d'évaluation
- G. Psychosocial Profile (Gordon's Functional Pattern)Document7 pagesG. Psychosocial Profile (Gordon's Functional Pattern)ampalPas encore d'évaluation
- Central Mindanao UniversityDocument1 pageCentral Mindanao UniversityKeith Wesley YbutPas encore d'évaluation
- HypertensionDocument3 pagesHypertensionKeith Wesley YbutPas encore d'évaluation
- Cover Page NovelDocument1 pageCover Page NovelKeith Wesley YbutPas encore d'évaluation
- Charles Dickens: The Quintessential Victorian AuthorDocument2 pagesCharles Dickens: The Quintessential Victorian AuthorKeith Wesley YbutPas encore d'évaluation
- Jomar IsDocument3 pagesJomar IsKeith Wesley YbutPas encore d'évaluation
- Anatomy and PhysiologyDocument12 pagesAnatomy and PhysiologykeithPas encore d'évaluation
- Non Viral HepatitisDocument8 pagesNon Viral HepatitisKeith Wesley YbutPas encore d'évaluation
- Keith Wesley Ybut BSN IIIDocument3 pagesKeith Wesley Ybut BSN IIIKeith Wesley YbutPas encore d'évaluation
- Venice Gween M. Monel BSN III SeptemberDocument3 pagesVenice Gween M. Monel BSN III SeptemberKeith Wesley YbutPas encore d'évaluation
- RHD GenogramDocument1 pageRHD GenogramKeith Wesley YbutPas encore d'évaluation
- Student Nurse Objectives for Family Case Study ExposureDocument1 pageStudent Nurse Objectives for Family Case Study ExposureKeith Wesley YbutPas encore d'évaluation
- Humanities ReactionDocument3 pagesHumanities ReactionKeith Wesley YbutPas encore d'évaluation
- Ward FinalDocument18 pagesWard FinalKeith Wesley YbutPas encore d'évaluation
- RHD IntroDocument3 pagesRHD IntroKeith Wesley YbutPas encore d'évaluation
- Nikol Kolko Lko LDocument3 pagesNikol Kolko Lko LKeith Wesley YbutPas encore d'évaluation
- Anatomy Part 2Document5 pagesAnatomy Part 2keithPas encore d'évaluation
- IoajfsDocument1 pageIoajfsKeith Wesley YbutPas encore d'évaluation
- Thesis Statement ActivityDocument4 pagesThesis Statement ActivityJudy SoonPas encore d'évaluation
- Assessment TOOL 1Document5 pagesAssessment TOOL 1Keith Wesley YbutPas encore d'évaluation
- For UniformsDocument2 pagesFor UniformsKeith Wesley YbutPas encore d'évaluation
- Nicole Hope I. Luza BSN3 10/9/17Document3 pagesNicole Hope I. Luza BSN3 10/9/17Keith Wesley YbutPas encore d'évaluation
- Head To Toe Physical Assessment Systems FindingsDocument5 pagesHead To Toe Physical Assessment Systems FindingsKeith Wesley YbutPas encore d'évaluation
- SportsDocument1 pageSportsKeith Wesley YbutPas encore d'évaluation
- NCP For HypertensionDocument4 pagesNCP For HypertensionKeith Wesley YbutPas encore d'évaluation
- SportsDocument1 pageSportsKeith Wesley YbutPas encore d'évaluation
- OBE Trainining Program VisayasDocument5 pagesOBE Trainining Program VisayasKeith Wesley YbutPas encore d'évaluation
- Bistek PinoyDocument2 pagesBistek PinoyKeith Wesley YbutPas encore d'évaluation
- Till Dusk Painting by Paul HilarioDocument1 pageTill Dusk Painting by Paul HilarioKeith Wesley YbutPas encore d'évaluation
- Course Learning Outcomes No. of Minutes No. of Points Rememb Ering Explain Ing Applyi NG Analyzi NG Evaluati NG Creatin G Type of QuestionDocument2 pagesCourse Learning Outcomes No. of Minutes No. of Points Rememb Ering Explain Ing Applyi NG Analyzi NG Evaluati NG Creatin G Type of QuestionKeith Wesley YbutPas encore d'évaluation
- Affidavit of DesistanceDocument6 pagesAffidavit of Desistancesalasvictor319Pas encore d'évaluation
- Radio Journalism GuideDocument13 pagesRadio Journalism GuideMark June B. GonzagaPas encore d'évaluation
- Yu-Gi-Oh Nightmare Troubadour InfoDocument12 pagesYu-Gi-Oh Nightmare Troubadour InfoBrandon Bradley0% (1)
- VV Siddipet Merit ListDocument81 pagesVV Siddipet Merit ListSubashPas encore d'évaluation
- Accenture 2014 Celent Claims ABCD Acn Duck Creek Dec14Document28 pagesAccenture 2014 Celent Claims ABCD Acn Duck Creek Dec14Ainia Putri Ayu KusumaPas encore d'évaluation
- Pope Francis' Call to Protect Human Dignity and the EnvironmentDocument5 pagesPope Francis' Call to Protect Human Dignity and the EnvironmentJulie Ann BorneoPas encore d'évaluation
- About Meat Eating in Sikh DharmDocument4 pagesAbout Meat Eating in Sikh Dharmvijay123inPas encore d'évaluation
- Bio 140 Exam 4 ReviewDocument7 pagesBio 140 Exam 4 Reviewlp_blackoutPas encore d'évaluation
- Internship Report On Nundhyar Engineering & Construction BattagramDocument65 pagesInternship Report On Nundhyar Engineering & Construction BattagramFaisal AwanPas encore d'évaluation
- Compulsive Buying Tendency As A Predictor of Attitudes and PerceptionsDocument4 pagesCompulsive Buying Tendency As A Predictor of Attitudes and PerceptionsvsharanyaPas encore d'évaluation
- 'Relentless' Poems by Jeff BezosDocument32 pages'Relentless' Poems by Jeff BezosromanlujanPas encore d'évaluation
- Business English Syllabus GuideDocument48 pagesBusiness English Syllabus Guidenicoler1110% (1)
- ECO 201 Sample Midterm Exam (Paulo GuimaraesDocument14 pagesECO 201 Sample Midterm Exam (Paulo GuimaraesAhmed NegmPas encore d'évaluation
- Unit 01 Who Is A Contributor PDFDocument28 pagesUnit 01 Who Is A Contributor PDFKumpavatJayarajsinhPas encore d'évaluation
- Assignment 03Document2 pagesAssignment 03Molto falsoPas encore d'évaluation
- Professional Teaching ResumeDocument2 pagesProfessional Teaching Resumeapi-535361896Pas encore d'évaluation
- CSE Qualifications and PointersDocument9 pagesCSE Qualifications and PointersChristopher de LeonPas encore d'évaluation
- Holy Trinity University: Puerto Princesa City Basic Education DepartmentDocument2 pagesHoly Trinity University: Puerto Princesa City Basic Education DepartmentBrian Reyes GangcaPas encore d'évaluation
- Work Breakdown StructureDocument3 pagesWork Breakdown StructureEllie Annelle LazaroPas encore d'évaluation
- Important Tips On The Law On SalesDocument34 pagesImportant Tips On The Law On SalesJanetGraceDalisayFabreroPas encore d'évaluation
- Antenna & Wave Propagation - Course OutlineDocument2 pagesAntenna & Wave Propagation - Course OutlineSabuj AhmedPas encore d'évaluation
- My Experience With DreamsDocument7 pagesMy Experience With DreamsPamela Rivera SantosPas encore d'évaluation
- English Proficiency Test (EPT) Reviewer With Answers - Part 1 - Online E LearnDocument4 pagesEnglish Proficiency Test (EPT) Reviewer With Answers - Part 1 - Online E LearnMary Joy OlitoquitPas encore d'évaluation
- TO B.inggris Dzakiy Bag 2Document21 pagesTO B.inggris Dzakiy Bag 2Ayu RatnaPas encore d'évaluation
- Phonology BibliogrDocument6 pagesPhonology BibliogrSnapeSnapePas encore d'évaluation
- Two Sides of Effective Oral CommunicationDocument17 pagesTwo Sides of Effective Oral CommunicationSharath KumarPas encore d'évaluation
- Homemade Water PurifierDocument13 pagesHomemade Water PurifierSherazPas encore d'évaluation
- O'laco Vs Cocho ChitDocument16 pagesO'laco Vs Cocho ChitAngel Pagaran AmarPas encore d'évaluation
- Wildlife Ecology - Unit 14 - Week (12) - RevisionDocument1 pageWildlife Ecology - Unit 14 - Week (12) - RevisionAdityaPas encore d'évaluation
- RepigmentationDocument4 pagesRepigmentationMariyaPas encore d'évaluation