Académique Documents
Professionnel Documents
Culture Documents
Jurnal 2
Transféré par
Arina HusnaTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Jurnal 2
Transféré par
Arina HusnaDroits d'auteur :
Formats disponibles
Journal of Cosmetics, Dermatological Sciences and Applications, 2012, 2, 83-87 83
http://dx.doi.org/10.4236/jcdsa.2012.22019 Published Online June 2012 (http://www.SciRP.org/journal/jcdsa)
Efficacy of Nd:YAG Laser for the Treatment of
Hidradenitis Suppurativa
Neda Nosrati*, Lindsey Hunter, Erica Kelly
Department of Dermatology, University of Texas Medical Branch, Galveston, USA.
Email: *nenosrat@utmb.edu
Received March 21st, 2012; revised April 25th, 2012; accepted May 6th, 2012
ABSTRACT
Hidradenitis suppurativa (HS) is an inflammatory skin disease that involves sebaceous glands and hair follicles of inter-
triginous areas, including axillary and inguinal regions. It is often chronic, painful, disabling, and can worsen over time.
Besides surgically excising affected areas, effective treatments are currently lacking. The long-pulsed neodymium:yt-
trium-aluminium-garnet (Nd:YAG) laser is a device that has traditionally been used for hair removal, but has recently
shown promise in clearing old lesions of HS and preventing new eruptions. In accordance with studies in the current
literature, we hypothesize that the Nd:YAG laser will significantly improve subjects with hidradenitis suppurativa
compared to standard, uninvasive treatment with topical antibiotics [1,2]. Study aims include: to treat subjects with
hidradenitis suppurativa with Nd:YAG laser therapy once monthly for 3 consecutive months, with a one month follow-
up; to compare the effectiveness of Nd:YAG treatment on one side of the subject (e.g., right) to treatment with topical
antibiotics on the subject’s other side (e.g., left); to assess treatment response using a visual analogue scale; to assess
subject satisfaction with treatment using a questionnaire; and to photodocument treatment response at each visit.
Keywords: Hidradenitis Suppurativa; Nd:YAG Laser; Acne Inverse; Follicular Disease
1. Introduction mized controlled trials have not been extensively per-
formed. Current treatment options include topical or sys-
Hidradenitis Suppurativa (HS) is a recurrent and chronic
inflammatory disease which can be disfiguring to pa- temic antibiotics, isotretinoin, dapsone, biological agents,
tients. Usually patients present with tender inflammatory and surgical interventions. Increasing interest in the use
abscesses of the flexures, including the axillary, infra- of biologics has led to several recent studies, albeit with
mammary, and inguinal areas. Scarring and tract forma- only limited numbers of patients. Infliximab was shown
tion are prominent features. Females seem to be more to be effective in small studies; however, its use is lim-
often affected than males. Patients are usually post pu- ited by both adverse effects and cost. Adalimumab, ac-
bertal. The chronic and scarring nature of the disease cording to a recent review, has not shown consistent re-
often leads to significant impacts on the quality of life in sults supporting its use despite its growing popularity
these patients [1,2]. although it has been well tolerated with no serious side
HS was first described by Velpeau, a French physician, effects reported in any of the studies. Traditional surgical
in 1839. He was also the first to hypothesize that the di- intervention has been excision of the affected areas with
sease was related to purulent inflammation of the sweat variable recurrence rates and high associated morbidity.
glands, later thought to be mainly inflammation of apo- Newer approaches include the CO2 and Nd:YAG lasers
crine [2]. More recent data however, supports the theory both with promising results [4].
of follicular occlusion as the predominant feature with A study performed by Tierney et al in HS patients with
apocrine involvement a secondary feature. Bacterial co- moderate disease showed a 65.3% improvement in sever-
lonization is also likely a secondary event which may ity of disease after 4 monthly treatments with Nd:YAG
exacerbate disease. Other factors which may be associ-
laser. They theorized that the hair follicle was the nidus
ated, but not etiologic, include smoking and obesity [2].
for inflammation and that destruction of the follicle
The prevalence of HS is estimated at about 1% of the
would lead to improvement. They were able to support
population, but unfortunately there are limited effective
treatment options [3]. Furthermore, large-scale rando- this theory with histopathologic evidence that the laser
worked through selective photothermolysis of the fol-
*
Corresponding author. licular unit with a reduction in inflammatory lesions [1].
Copyright © 2012 SciRes. JCDSA
84 Efficacy of Nd:YAG Laser for the Treatment of Hidradenitis Suppurativa
Based on the success of this study and others like it re- was used on both the control and treatment sides. After
cently in the literature, we decided to further explore the the study period of 4 months, patients were allowed to
efficacy of the Nd:YAG laser in treatment of patients continue receiving treatment to the treatment side and
with HS. Our study was unique in that we recruited pa- initiate treatment to the control side at no cost if they so
tients even with minimal disease as the Nd:YAG laser desired.
has a very high safety profile with essentially no risk to Patients were contacted within 48 hours of treatment
the patients; therefore, justifying its use in even minimal to assess for adverse events. Patients were also evaluated
disease to prevent scarring and tract formation. Our goals at the follow up visits by the treating physician for any
were to treat patients with HS with Nd:YAG laser ther- development of adverse events, including pigmentary
apy once monthly for 3 consecutive months and reevalu- alterations.
ate after one month, to compare the effectiveness on one Photos were taken of treated and untreated sides with
side (treatment side) of the patient to the other side (con- and without flash prior to each session and at the one
trol side), to assess treatment response using a visual month follow up. Photographs were then evaluated by
analogue scale, to assess subject satisfaction with a sub- both a blinded physician and resident. Initially the modi-
ject questionnaire, and to photodocument treatment re- fied HS LASI score designed by Sartorius et al. [6] was
sponse at each visit. to be the evaluation tool; however, it was difficult to use
this scoring system with the photographs, and a new
2. Methods modified score was created by our center based on the
Sartorius score (Table 1).
Six patients (5 women and 1 man) ages 19 to 54 carrying In addition, patients were asked to fill out a subject
a clinical diagnosis of hidradenitis suppurativa were en-
assessment questionnaire after each treatment visit. The
rolled initially in this study, performed at the University
questionnaires assessed the patients’ overall satisfaction
of Texas Medical Branch in Galveston, Texas from Fe-
with the treatment and their subjective improvement as
bruary 2011 through February 2012. The study was ap-
well as assessing for any side effects of therapy.
proved by the UTMB institutional review board and was
A paired t-test was done to compare the mean per-
in accordance with the Declaration of Helsinki. A sample
centage of change for both treated and control sites for
size of 5 was calculated to have 80% power to detect a
each patient from baseline to the fourth month. Of note
difference in means of 23.400 (e.g. a First condition
the scores between the physician scorer and resident
mean, µ1, of 31.000 and a Second condition mean, µ2, of
scorer were not different based on t tests; therefore, we
7.600), assuming a standard deviation of differences of
averaged across scorers. The p value was calculated for
12.000, using a paired t-test with a 0.050 two-sided sig-
the mean percentage of change and a value of less than
nificance level.
0.05 indicates statistical significance for the study.
Patients were included if they had at least Hurley stage
I disease of their axilla (abscess formation without sinus
3. Results
tracts and cicatrization) [5]. Patients were excluded for
the following reasons: pregnancy, previous surgical A total of 5 patients completed this 4 month study. One
treatment to affected areas, or any concomitant systemic patient (19 year old female) withdrew prior to beginning
therapy. Patients on systemic therapy were allowed to the study secondary to scheduling conflicts. The mean
enter the study as long as they discontinued the therapy age was 37.6 years, with 80% females (n = 4) and 20%
at least 2 weeks prior to the initiation of the study laser males (n = 1). Fitzpatrick skin types ranged from II to V,
protocol. with 3 patients having type II-III, and one patient each
First the treatment side (right vs. left axilla) was cho- having type IV and type V. Only axillary disease was
sen using a computerized randomization tool. Three treated in this study.
monthly laser treatments were then performed using a
single pass of the long pulsed 1064-nm Nd:YAG laser Table 1. Modified scoring system based on Sartorius et al.
(Cutera Inc., Brisbane, California) with a one month fol-
Abscess/Nodule Tract Scar
low up after completion of the three treatments, for a
Formation Formation Formation
total study period of four months. A topical cooling gel
was employed using the standard laser treatment protocol, 0-not present 0-not present 0-not present
but no anesthetics were used. A contact metal-tipped 1-mild activity 1-mild activity 1-mild activity
cooling device was used on the treatment areas immedi- 2-moderate activity 2-moderate activity 2-moderate activity
ately before and after irradiation. The laser settings were 3-severe activity 3-severe activity 3-severe activity
chosen based on the patient’s Ftizpatrick skin type per
Based on 3 factors, including abscess/nodule formation, tract formation, and
Cutera’s recommendations. Patients were given an after- presence of scarring. Highest possible score is 9 indicating more severe
care instructions handout. Topical 1% Clindamycin gel disease, while a score of 0 indicates no active disease.
Copyright © 2012 SciRes. JCDSA
Efficacy of Nd:YAG Laser for the Treatment of Hidradenitis Suppurativa 85
The mean score at baseline for the treatment sites was recent evidence actually suggests that involvement of the
2.4 (SD: 0.33) which increased to 2.75 (SD: 2.56) at the follicle and thus the pilosebaceous unit is the primary
end of the 4 months compared to the mean score at base- event and apocrine gland involvement is a secondary
line for the control sites which was 3.05 (SD: 1.89) and phenomenon. Studies based on histopathology describe a
increased to 3.15 (SD: 2.77) at the end of the 4 months series of events similar to the pathogenesis of acne with
(Figure 1). There was no statistical significance in the hyperkeratinization of the follicle leading to dilation and
percentage of change in the scores after 4 months of rupture causing dermal inflammation and bacterial colo-
treatment (P = 0.41). This is likely related to the fact that nization, sinus tract formation, and eventually scarring
the power to detect statistical significance was very li- [7]. These similarities between the two disorders have led
mited due to the small sample size of 5 patients. to the suggestion of acne inversa as a more appropriate
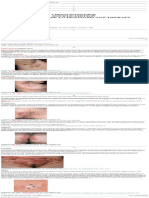
Before and after photographs are demonstrated in description than HS [8]. Furthermore, studies have shown
Figure 2. None of the patients reported experiencing any that similar to acne toll-like receptor 2 expression is in-
side effects when they were contacted shortly after each creased in macrophages and dendritic cells of patients
treatment. All patients opted to continue laser treatments with HS [9]. However, there are several differences
after the 4 month study period was completed. which exist between acne and HS including microbiol-
The subject assessment questionnaire was distributed ogy, clinical presentation, and response to treatment [7].
to the patients at the end of each treatment session and at Overall, there is still no absolute consensus as to the eti-
the end of the study. Overall, 80% of patients (n = 4) ology of HS, but the hair follicle likely plays an integral
rated their overall level satisfaction with the laser treat- role. Localization to intertriginous areas may be ex-
ment as very satisfied. Only one patient (20%) rated their plained by shear forces in these areas leading to micro
level of satisfaction as unsatisfied. None of the patients tears in the hair follicle, which is exacerbated by larger
reported having any pain associated with treatment or skin folds in the obese [10].
any other side effects including redness, swelling, crust- The long pulsed Nd:YAG laser is a device that has
ing or changes in skin pigmentation. Patients were also been traditionally used for hair removal. This treatment
encouraged to leave comments which included the fol- has the advantage of being strictly local and devoid of
lowing: “less outbreaks and leaking from boils” and “no systemic side effects such as those encountered with ad-
new breakouts,” “the [treatment] side had no problems at ministration of systemic steroids, antibiotics, retinoids,
the beginning of the study and remains so. The [control] and biologics. Furthermore, the long pulsed Nd:YAG is
side has developed a new nodule.” safe even in darker skin types due to its longer wave-
length and greater depth of penetration with less effects
4. Discussion on the epidermis leading to pigmentary alterations [11].
Although it appears logical to assume that inflammation As discussed previously, the treatment options for HS
of apocrine glands is the primary event in HS as the le- are limited and none have proven to be dramatically ef-
sions are distributed mainly in apocrine rich locations, fective [4]. Few of the biologics and surgery have shown
Figure 1. Mean scores across treatment periods from baseline to final visit at 4 months.
Copyright © 2012 SciRes. JCDSA
86 Efficacy of Nd:YAG Laser for the Treatment of Hidradenitis Suppurativa
tive as a treatment of HS.
Unfortunately, our results did not show a significant
difference in the treatment side versus the patients’ un-
treated side (control) after 3 consecutive monthly treat-
ments with the Nd:YAG laser. This is likely due to the
very small sample size of only 5 patients. There was a
limited time period allowed for the completion of this
study after IRB approval was finally obtained, which did
not allow for ample recruitment time. Had the sample
size been larger, there may have been a demonstrable
response to the laser as has been seen in several other
similar studies evaluating the Nd:YAG in HS [1,3].
Another factor which likely influenced the non sig-
nificant results was the scoring system used. Initially the
Sartorius Score was to be the visual analog scale used to
score the photographs. It was decided to use photographs
rather than actually evaluating the patient in person to
allow for blinding of the evaluator. However, the physi-
cian scorers found it very difficult to adequately judge
distances between two relevant lesions which was re-
quired by the Sartorius score; therefore, the scoring sys-
(a) tem had to be adjusted. This new scoring system may
have led to poor scoring data and thus nonsignificant
results.
Despite the fact that the results were not significant,
the patients seemed overall pleased with the results with
80% rating their satisfaction level as very satisfied. Fur-
thermore, the one patient who rated their experience as
unsatisfied, chose to drive over 4 hours round trip to our
clinic once a month for continued treatment with the la-
ser. Actually, all the patients chose to continue laser
treatment after the study period for several months with
many of the patients driving very long distances. No side
effects were noted by any of the patients during the entire
study period with most of the patients tolerating very
high fluences up to 70 J/cm2.
In conclusion, patients were overall satisfied with
Nd:YAG laser treatment for HS and continued to request
therapy even though no statistical difference between
treatment and control sites was objectively observed.
Furthermore, Nd:YAG laser was found to be completely
safe with no side effects encountered throughout the
study even when using high fluences. Therefore, laser is
(b) a safe alternative in patients with even mild disease in
HS, although we cannot prove that it is more effective
Figure 2. (a) Immediately before initial treatment showing
than topical antibiotics alone.
small abscesses and mild scarring; (b) One month follow up
after 3 consecutive monthly treatments shows decreased in-
flammatory lesions. REFERENCES
some improvement, but are associated with a high rate of [1] L. Y. Xu, D. R. Wright, B. H. Mahmoud, D. M. Ozog, D.
A. Mehregan and I. H. Hamzavi, “Histopathologic Study
adverse events. Nd:YAG laser is safe and effective for
of Hidradenitis Suppurativa Following Long-Pulsed 1064
hair epilation and as recent scientific evidence points to nm Nd:YAG Laser Treatment,” Archives of Dermatology,
the hair follicle as the primary abnormality in HS; it Vol. 147, No. 1, 2011, pp. 21-28.
seems logical to assume that Nd:YAG should be effec- doi:10.1001/archdermatol.2010.245
Copyright © 2012 SciRes. JCDSA
Efficacy of Nd:YAG Laser for the Treatment of Hidradenitis Suppurativa 87
[2] A. Alikhan, P. J. Lynch and D. B. Eisen, “Hidradenitis Are Significantly Reduced in Uninvolved Hair Follicles
Suppurativa: A Comprehensive Review,” Journal of the from Patients with Hidradenitis Suppurativa,” British
American Academy of Dermatology, Vol. 62, No. 4, 2009, Journal of Dermatology, Vol. 164, No. 5, 2011, pp. 1017-
pp. 706-708. 1022. doi:10.1111/j.1365-2133.2011.10224.x
[3] B. H. Mahmoud, E. Tierney, C. L. Hexsel, J. Pui, D. M. [8] J. Boer and E. F. Weltevreden, “Hidradenitis Suppurativa
Ozog and I. H. Hamzavi, “Prospective Controlled Clinical or Acne Inversa: A Clinicopathologic Study of Early Le-
and Histopathologic Study of Hidradenitis Suppurativa sions,” British Journal of Dermatology, Vol. 135, No. 5,
Treated with the Long Pulsed Neodymium: Yttrium- 1996, pp. 721-725.
Aluminium-Garnet Laser,” Journal of the American Aca- doi:10.1111/j.1365-2133.1996.tb03880.x
demy of Dermatology, Vol. 62, No. 4, 2010, pp. 637-645. [9] R. E. Hunger, A. M. Surovy, A. S. Hassan, L. R.
doi:10.1016/j.jaad.2009.07.048 Braathen and N. Yawalkar, “Toll-Like Receptor 2 Is
[4] P. V. Rambhatla, H. W. Lim and I. Hamzavi, “A System- Highly Expressed in Lesions of Acne Inversa and Colo-
atic Review of Treatments for Hidradenitis Suppurativa,” calizes with C-Type Lectin Receptor,” British Journal of
Archives of Dermatology, Vol. 148, No. 4, 2011, pp. 439- Dermatology, Vol. 158, No. 4, 2008, pp. 691-697.
446. doi:10.1001/archdermatol.2011.1950 doi:10.1111/j.1365-2133.2007.08425.x
[5] H. Hurley, “Dermatologic Surgery, Principles and Prac- [10] H. Kurzen, I. Kurokawa, G. B. Jemec, L. Emtestam, K.
tice,” Marcel Dekker, New York, 1989. Sellhever, E. J. Giamarellos-Bourboulis, I. Nagy, F. G.
[6] K. Sartorius, J. Lapins, L. Emtestam and G. B. Jemec, Bechara, K. Sartorius, J. Lapins, D. Krahl, P. Altmeyer, J.
“Suggestions for Uniform Outcome Variables When Re- Revuz and C. C. Zouboulis, “What Causes Hidradenitis
porting Treatment Effects in Hidradenitis Suppurativa,” Suppurativa?” Experimental Dermatology, Vol. 17, No. 5,
British Journal of Dermatology, Vol. 149, No. 1, 2003, 2008, pp. 455-456.
pp. 211-213. doi:10.1046/j.1365-2133.2003.05390.x doi:10.1111/j.1600-0625.2008.00712.x
[7] S. Kamp, A. M. Fiehn, K. Stenderup, C. Rosada, B. [11] T. S. Alster, H. Bryan and C. M. William, “Long Pulsed
Parkkenberg, K. Kemp, T. N. Dam and G. B. Jemec, Nd:Yag Laser-Assisted Hair Removal in Pigmented Skin:
“Hidradenitis Suppurativa: A Disease of the Absent Se- Clinical and Histological Evaluation,” Archives of Der-
baceous Gland? Sebaceous Gland Number and Volume matology, Vol. 13, No. 7, 2001, pp. 885-889.
Copyright © 2012 SciRes. JCDSA
Vous aimerez peut-être aussi
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (890)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (587)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (119)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2219)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (265)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Fast Hidradenitis Suppurativa CureDocument2 pagesFast Hidradenitis Suppurativa CureIbitoye Ayodeji AlexandriaPas encore d'évaluation
- Jural Arina BedahDocument7 pagesJural Arina BedahArina HusnaPas encore d'évaluation
- Insidensi Dan FR Pada Insisional HerniaDocument9 pagesInsidensi Dan FR Pada Insisional HerniatarietarooPas encore d'évaluation
- Jurnal 2Document5 pagesJurnal 2Arina HusnaPas encore d'évaluation
- Terjemahan Artikel Tugas JurnalDocument41 pagesTerjemahan Artikel Tugas JurnalArina Husna0% (1)
- Obesity GuideDocument94 pagesObesity GuideAbhishek RaghuvanshiPas encore d'évaluation
- BPPV NciDocument4 pagesBPPV NciArina HusnaPas encore d'évaluation
- Guideline For NSTEMI UAPDocument72 pagesGuideline For NSTEMI UAPArina HusnaPas encore d'évaluation
- Jurnal Organ InderaDocument7 pagesJurnal Organ InderaAnggana Faza NazharaPas encore d'évaluation
- Created By: Arina Husna 30101306884 SGD 3Document11 pagesCreated By: Arina Husna 30101306884 SGD 3Arina HusnaPas encore d'évaluation
- Terjemahan Artikel Tugas JurnalDocument41 pagesTerjemahan Artikel Tugas JurnalArina Husna0% (1)
- 395 1628 1 SP - 2 PDFDocument7 pages395 1628 1 SP - 2 PDFArina HusnaPas encore d'évaluation
- InggrisDocument17 pagesInggrisArina HusnaPas encore d'évaluation
- HB LSHBB WLDTRBT DHT LLQDocument62 pagesHB LSHBB WLDTRBT DHT LLQtricia isabellaPas encore d'évaluation
- 0251 Dermabrasion, Chemical Peels and Acne SurgeryDocument31 pages0251 Dermabrasion, Chemical Peels and Acne SurgeryMarian MorenoPas encore d'évaluation
- Natural Herbs For Hidradenitis SuppurativaDocument2 pagesNatural Herbs For Hidradenitis SuppurativaJohn SmithPas encore d'évaluation
- CNG 23-Full-ProgrammeDocument175 pagesCNG 23-Full-ProgrammeJelena BajagicPas encore d'évaluation
- Surgery 8th Se Skin Subcu Compiled TransbooksnotestpreviewersDocument237 pagesSurgery 8th Se Skin Subcu Compiled TransbooksnotestpreviewersMildred DagaleaPas encore d'évaluation
- 2004 HS Habif Clinical Dermatology BOOK EXCERPT PDFDocument1 page2004 HS Habif Clinical Dermatology BOOK EXCERPT PDFindahPas encore d'évaluation
- Hidradenitis SuppurativaDocument35 pagesHidradenitis SuppurativavereriPas encore d'évaluation
- Listening Sample Test 3 Audio ScriptDocument14 pagesListening Sample Test 3 Audio ScriptEliz AchhamiPas encore d'évaluation
- JournalDocument21 pagesJournaltifa adaPas encore d'évaluation
- Care of Clients with Hidradenitis Suppurativa (Acne InversaDocument15 pagesCare of Clients with Hidradenitis Suppurativa (Acne InversaJm OpolintoPas encore d'évaluation
- Hidradenitis SuppurativaDocument5 pagesHidradenitis SuppurativanurulPas encore d'évaluation
- HS Surgical Excision Case SeriesDocument16 pagesHS Surgical Excision Case SeriesMarina StosicPas encore d'évaluation
- Evaluation of Bee Venom and Propolis in Treatment of PsoriasisDocument1 pageEvaluation of Bee Venom and Propolis in Treatment of PsoriasiscsandrasPas encore d'évaluation
- Sweat Glands DisDocument5 pagesSweat Glands DisShahbaz DarPas encore d'évaluation
- Pash Syndrome Co-Existing With Rheumatic Heart Disease and Severe Mitral Valve Regurgitation: A Rare Case ReportDocument3 pagesPash Syndrome Co-Existing With Rheumatic Heart Disease and Severe Mitral Valve Regurgitation: A Rare Case ReportIJAR JOURNALPas encore d'évaluation
- Hidradenitis Suppurativa - Treatment - UpToDate PDFDocument24 pagesHidradenitis Suppurativa - Treatment - UpToDate PDFjandroPas encore d'évaluation
- Original Article Surgical Management of Acne InversaDocument5 pagesOriginal Article Surgical Management of Acne InversaNomi AkramPas encore d'évaluation
- DFGDFG: Why Is My Period Late: 8 Possible ReasonsDocument6 pagesDFGDFG: Why Is My Period Late: 8 Possible ReasonspeepeepoopooPas encore d'évaluation
- Hidradenitis SuppurativaDocument11 pagesHidradenitis SuppurativapologroPas encore d'évaluation
- Acne Fulminans Explosive Systemic Form of Acne PDFDocument8 pagesAcne Fulminans Explosive Systemic Form of Acne PDFPaulus SidhartaPas encore d'évaluation
- Hidradenitis Suppurativa - A Disease Primer. Alexa B. Kimball, Gregor B.E. Jemec. 2017. Adis, ChamDocument59 pagesHidradenitis Suppurativa - A Disease Primer. Alexa B. Kimball, Gregor B.E. Jemec. 2017. Adis, ChammeliaPas encore d'évaluation
- Vulvovaginal DisordersDocument62 pagesVulvovaginal DisordersMabruk MansoorPas encore d'évaluation
- Boils and Carbuncles: (Mayo Clinic)Document15 pagesBoils and Carbuncles: (Mayo Clinic)Jimmy ThomasPas encore d'évaluation
- Profound Disturbances of Sexual Health in Patients With Acne InversaDocument8 pagesProfound Disturbances of Sexual Health in Patients With Acne InversaYasser AlghrafyPas encore d'évaluation
- Hidradenitis SuppurativaDocument12 pagesHidradenitis SuppurativamikezPas encore d'évaluation
- Wa0017.Document9 pagesWa0017.CHAMBI MAMANI JESSICA BETTYPas encore d'évaluation
- Hidradenitis Suppurativa DietDocument3 pagesHidradenitis Suppurativa DietJosse RiverPas encore d'évaluation
- Daftar Pustaka Emedicine MedscapeDocument7 pagesDaftar Pustaka Emedicine MedscapeAyesha Nabilla Putri0% (1)
- Guia 10553Document9 pagesGuia 10553Carolina Fernandez QuirogaPas encore d'évaluation