Académique Documents
Professionnel Documents
Culture Documents
Placebo Controlled Trial For Myelofibrosis
Transféré par
Anonymous V5l8nmcSxbTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Placebo Controlled Trial For Myelofibrosis
Transféré par
Anonymous V5l8nmcSxbDroits d'auteur :
Formats disponibles
The n e w e ng l a n d j o u r na l of m e dic i n e
original article
A Double-Blind, Placebo-Controlled Trial
of Ruxolitinib for Myelofibrosis
Srdan Verstovsek, M.D., Ph.D., Ruben A. Mesa, M.D., Jason Gotlib, M.D.,
Richard S. Levy, M.D., Vikas Gupta, M.D., John F. DiPersio, M.D., Ph.D.,
John V. Catalano, M.D., Michael Deininger, M.D., Ph.D., Carole Miller, M.D.,
Richard T. Silver, M.D., Moshe Talpaz, M.D., Elliott F. Winton, M.D.,
Jimmie H. Harvey, Jr., M.D., Murat O. Arcasoy, M.D., Elizabeth Hexner, M.D.,
Roger M. Lyons, M.D., Ronald Paquette, M.D., Azra Raza, M.D.,
Kris Vaddi, Ph.D., Susan Erickson-Viitanen, Ph.D., Iphigenia L. Koumenis, M.S.,
William Sun, Ph.D., Victor Sandor, M.D., and Hagop M. Kantarjian, M.D.
A BS T R AC T
background
Ruxolitinib, a selective inhibitor of Janus kinase (JAK) 1 and 2, has clinically signifi- From the University of Texas M.D. Ander-
cant activity in myelofibrosis. son Cancer Center, Houston (S.V., H.M.K.);
Mayo Clinic, Scottsdale, AZ (R.A.M.);
methodS Stanford Cancer Institute, Stanford, CA
(J.G.); Incyte, Wilmington, DE (R.S.L.,
In this double-blind trial, we randomly assigned patients with intermediate-2 or high- K.V., S.E.-V., I.L.K., W.S., V.S.); Princess
risk myelofibrosis to twice-daily oral ruxolitinib (155 patients) or placebo (154 patients). Margaret Hospital, University of Toronto,
The primary end point was the proportion of patients with a reduction in spleen vol- Toronto (V.G.); Washington University
School of Medicine, St. Louis (J.F.D.);
ume of 35% or more at 24 weeks, assessed by means of magnetic resonance imaging. Frankston Hospital and Monash Univer-
Secondary end points included the durability of response, changes in symptom bur- sity, Frankston, VIC, Australia (J.V.C.);
den (assessed by the total symptom score), and overall survival. Oregon Health and Science University,
Portland (M.D.); Huntsman Cancer Insti-
resulTS tute, University of Utah, Salt Lake City
(M.D.); Saint Agnes Cancer Institute,
The primary end point was reached in 41.9% of patients in the ruxolitinib group as Baltimore (C.M.); Weill Cornell Medical
compared with 0.7% in the placebo group (P<0.001). A reduction in spleen volume was Center (R.T.S.) and Columbia Presbyteri-
maintained in patients who received ruxolitinib; 67.0% of the patients with a response an Medical Center (A.R.) — both in New
York; University of Michigan, Ann Arbor
had the response for 48 weeks or more. There was an improvement of 50% or more in (M.T.); Emory University School of Medi-
the total symptom score at 24 weeks in 45.9% of patients who received ruxolitinib as cine, Atlanta (E.F.W.); Birmingham Hema-
compared with 5.3% of patients who received placebo (P<0.001). Thirteen deaths oc- tology and Oncology, Birmingham, AL
(J.H.H.); Duke University Health System,
curred in the ruxolitinib group as compared with 24 deaths in the placebo group Durham, NC (M.O.A.); Abramson Cancer
(hazard ratio, 0.50; 95% confidence interval, 0.25 to 0.98; P = 0.04). The rate of discon- Center at the University of Pennsylvania,
tinuation of the study drug because of adverse events was 11.0% in the ruxolitinib Philadelphia (E.H.); Cancer Care Centers
of South Texas and US Oncology, San
group and 10.6% in the placebo group. Among patients who received ruxolitinib, ane- Antonio (R.M.L.); and UCLA Division of
mia and thrombocytopenia were the most common adverse events, but they rarely led Hematology and Oncology, Los Angeles
to discontinuation of the drug (in one patient for each event). Two patients had trans- (R.P.). Address reprint requests to Dr.
Verstovsek at the Leukemia Department,
formation to acute myeloid leukemia; both were in the ruxolitinib group. M.D. Anderson Cancer Center, Unit 428,
1515 Holcombe Blvd., Houston, TX 77030,
conclusionS or at sverstov@mdanderson.org.
Ruxolitinib, as compared with placebo, provided significant clinical benefits in Investigators and participating centers in
patients with myelofibrosis by reducing spleen size, ameliorating debilitating the Controlled Myelofibrosis Study with
myelofibrosis-related symptoms, and improving overall survival. These benefits Oral JAK Inhibitor Treatment I (COMFORT-I)
are listed in the Supplementary Appendix,
came at the cost of more frequent anemia and thrombocytopenia in the early part available at NEJM.org.
of the treatment period. (Funded by Incyte; COMFORT-I ClinicalTrials.gov number, N Engl J Med 2012;366:799-807.
NCT00952289.) Copyright © 2012 Massachusetts Medical Society.
n engl j med 366;9 nejm.org march 1, 2012 799
The New England Journal of Medicine
Downloaded from nejm.org on March 23, 2018. For personal use only. No other uses without permission.
Copyright © 2012 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
M
yelofibrosis, a myeloproliferative NEJM.org) of 2 (intermediate-2 risk) or 3 or more
neoplasm, is manifested by abnormal (high risk), an Eastern Cooperative Oncology Group
blood counts (anemia, thrombocytosis performance status9 of 3 or less (on a scale from
or thrombocytopenia, and leukocytosis or leuko- 0 to 5, with higher scores indicating greater dis-
penia), splenomegaly, and debilitating symptoms ability; see the Supplementary Appendix for further
(e.g., fatigue, weakness, abdominal pain, cachexia, details), less than 10% peripheral-blood blasts,
weight loss, pruritus, night sweats, and bone pain), an absolute peripheral-blood CD34+ cell count of
which are thought to be caused by the combined more than 20×106 per liter, a platelet count of
effects of massive splenomegaly and elevated levels 100×109 per liter or more, and palpable spleno-
of proinflammatory cytokines.1 Survival ranges megaly (≥5 cm below the left costal margin). Pa-
from approximately 2 to 11 years, depending on tients had disease that was refractory to available
defined prognostic factors.2 Traditional therapeutic therapies, had side effects requiring their discon-
options, including splenectomy, have limited bene- tinuation, or were not candidates for available ther-
fit.3 Although allogeneic stem-cell transplantation apies and had disease requiring treatment. The trial
may cure myelofibrosis, few patients are eligible for protocol, which describes in detail the inclusion
this treatment. and exclusion criteria and other information about
Although the gain-of-function mutation in the the trial design, as well as the statistical analysis
gene encoding Janus kinase (JAK) 2 (JAK2 V617F) plan, is available at NEJM.org.
is present in approximately 50% of patients with
primary myelofibrosis, other mechanisms of direct Study Oversight
or indirect activation of the intracellular JAK– The protocol was approved by the institutional re-
signal transducer and activator of transcription view board at each participating site. The study was
(STAT) pathway are known,4 suggesting that dys- conducted in accordance with the International
regulation of this pathway is a central pathogenic Conference on Harmonization guidelines for Good
component in myelofibrosis, regardless of the mu- Clinical Practice. All patients provided written in-
tational status of JAK2. Also, proinflammatory formed consent.
cytokines that play an important role in myelo- Data were collected by the academic investi-
fibrosis signal through JAK 1 (JAK1) and JAK2.5 gators and analyzed by the sponsor of the study,
In a phase 1–2 trial of ruxolitinib (INCB018424, Incyte. The sponsor, in collaboration with the aca-
Incyte), a potent inhibitor of JAK1 and JAK2,6,7 demic investigators, interpreted the data. The first
patients with myelofibrosis had durable reductions author and an author who was an employee of the
in splenomegaly and improvements in myelofi- sponsor wrote the initial draft of the manuscript,
brosis-related symptoms, regardless of their status with assistance from a medical writer who was
with respect to the JAK2 V617F mutation. To fur- paid by the sponsor. All the authors contributed to
ther evaluate the efficacy and safety of ruxoli- subsequent drafts and made the decision to submit
tinib, we conducted the Controlled Myelofibro- the article for publication. All the authors vouch for
sis Study with Oral JAK Inhibitor Treatment I the accuracy and completeness of the reported data
(COMFORT-I), a randomized, double-blind, pla- and for the fidelity of this report to the protocol.
cebo-controlled trial involving patients with inter-
mediate-2 or high-risk myelofibrosis. STUDY DESIGN AND TREATMENT
This randomized, double-blind, placebo-controlled,
Me thods phase 3 trial was conducted at 89 sites in the Unit-
ed States, Australia, and Canada. Patients were
PATIENTS randomly assigned in a 1:1 ratio to receive oral
Patients were eligible for the study if they were ruxolitinib phosphate tablets or matched placebo.
18 years of age or older and had primary myelo- The starting dose of ruxolitinib depended on the
fibrosis, post–polycythemia vera myelofibrosis, or baseline platelet count: 15 mg twice daily for a
post–essential thrombocythemia myelofibrosis ac- platelet count of 100×109 to 200×109 per liter and
cording to 2008 World Health Organization crite- 20 mg twice daily for a count that exceeded
ria,8 with a life expectancy of 6 months or longer, 200×109 per liter. The dose was adjusted for lack of
an International Prognostic Scoring System (IPSS) efficacy or excess toxicity as specified in the proto-
score2 (see Table S1 in the Supplementary Appen- col (see the Supplementary Appendix). Unblinding
dix, available with the full text of this article at of the study-drug assignments and crossover from
800 n engl j med 366;9 nejm.org march 1, 2012
The New England Journal of Medicine
Downloaded from nejm.org on March 23, 2018. For personal use only. No other uses without permission.
Copyright © 2012 Massachusetts Medical Society. All rights reserved.
Ruxolitinib for Myelofibrosis
placebo to ruxolitinib were permitted for protocol- tients who discontinued the study drug or crossed
defined worsening splenomegaly (see the Supple- over before week 24 were counted as not having a
mentary Appendix). The prospectively defined cut- response (for response measures of a reduction in
off point for data analysis occurred when half the spleen volume and symptom improvement). Sec-
patients remaining in the study had completed the ondary efficacy variables were tested in a fixed-
week 36 visit and when all the patients had com- sequence testing procedure at an alpha level of
pleted the week 24 evaluation or discontinued treat- 0.05. The durability of spleen response and sur-
ment. After crossover, data for patients who were vival were analyzed with the use of the Kaplan–
initially assigned to placebo were not included in Meier method.
the analyses, except for the intention-to-treat analy-
sis of overall survival. R e sult s
The primary end point was the proportion of
patients with a reduction of 35% or more in spleen PATIENTS
volume from baseline to week 24, measured by From September 2009 through April 2010, a total
means of magnetic resonance imaging or com- of 309 patients were enrolled: 155 were random-
puted tomography. Secondary end points included ly assigned to ruxolitinib, and 154 were randomly
the duration of the reduction in spleen volume; the assigned to placebo. Baseline characteristics were
proportion of patients with a reduction in the total similar in the two groups (Table 1). The median
symptom score of 50% or more from baseline to spleen volume was more than 2500 cm3 (>10 times
week 24, as assessed with the modified Myelofi- the median normal spleen volume of 200 cm3).13-15
brosis Symptom Assessment Form (MFSAF), ver- A total of 38.2% of the patients had IPSS inter-
sion 2.0 (see the Supplementary Appendix)10,11; mediate-2–risk disease, and 61.2% had high-risk
the change in the total symptom score from base- disease.
line to week 24; and overall survival. The analysis At the time of the prospectively defined data
of overall survival was updated at the time of a cutoff (median follow-up, 32 weeks), 134 patients
planned data-collection cutoff 4 months after the in the ruxolitinib group (86.5%) and 78 in the pla-
primary analysis. Patients completed the MFSAF cebo group (50.6%) were receiving the randomly
every night; this electronic diary was used to evalu- assigned study drug. Thirty-six patients in the pla-
ate symptoms of night sweats, itching, abdominal cebo group (23.4%) crossed over to ruxolitinib
discomfort, pain under the ribs on the left side, a (16 before and 20 after week 24; see the Supple-
feeling of fullness (early satiety), muscle or bone mentary Appendix.)
pain, and inactivity. Scores ranged from 0 (“ab-
sent” symptoms) to 10 (“worst imaginable” symp- EFFICACY
toms), and the total symptom score was the sum Spleen Size
of the individual scores, excluding inactivity. Ex- The proportion of patients with a reduction of
ploratory end points included changes in body 35% or more in spleen volume at week 24 (primary
weight and the JAK2 V617F allele burden, achieve- end point) was 41.9% in the ruxolitinib group as
ment of independence from transfusions,12 and compared with 0.7% in the placebo group (odds
additional patient-reported outcomes (see the Sup- ratio, 134.4; 95% confidence interval [CI], 18.0 to
plementary Appendix). 1004.9; P<0.001) (Fig. 1A). Additional prespeci-
fied analyses showed that among the patients for
Statistical Analysis whom baseline and week 24 data were available,
The study was designed to enroll 240 patients, pro- the 139 patients receiving ruxolitinib had a mean
viding 97% power to detect a treatment difference reduction in spleen volume of 31.6% (median,
in spleen-volume response at a two-sided alpha 33.0%) at week 24; the 106 patients receiving
level of 0.05, assuming a response rate of 30% or placebo had a mean increase of 8.1% (median,
more for ruxolitinib and a response rate of 10% or 8.5%). Almost all patients receiving ruxolitinib had
less for placebo. Analyses were conducted in accor- some degree of reduction in spleen volume (Fig.
dance with the intention-to-treat principle. For all 1B). The majority of patients receiving placebo
applicable variables, however, patients with missing had spleen growth. Changes in palpable spleen
baseline values were excluded from the analyses of length in the ruxolitinib and placebo groups mir-
change and percent change from baseline. In the rored the changes in spleen volume. The reduc-
analyses of change from baseline to week 24, pa- tion in spleen volume was durable with continued
n engl j med 366;9 nejm.org march 1, 2012 801
The New England Journal of Medicine
Downloaded from nejm.org on March 23, 2018. For personal use only. No other uses without permission.
Copyright © 2012 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
Table 1. Baseline Characteristics of the Patients.*
Variable Ruxolitinib (N = 155) Placebo (N = 154)
Median age (range) — yr 66 (43–91) 70 (40–86)
Male sex — % of patients 51.0 57.1
Myelofibrosis subtype — % of patients
Primary myelofibrosis 45.2 54.5
Post–polycythemia vera myelofibrosis 32.3 30.5
Post–essential thrombocythemia myelofibrosis 22.6 14.3
IPSS risk status — % of patients
High 58.1 64.3
Intermediate 2 41.3 35.1
Previous hydroxyurea use — % of patients 67.1 56.5
Median platelet count (range) — ×10−9/liter 262 (81–984) 238 (100–887)
Median hemoglobin (range) — g/liter 105 (66–170) 105 (35–173)
Median palpable spleen length (range) — cm 16 (0–33)† 16 (5–34)
Median spleen volume (range) — cm3 2598 (478–7462) 2566 (521–8881)
JAK2 V617F–positive — % of patients 72.9 79.9
* There were no significant differences between the two groups with the exception of age (P<0.05). IPSS denotes
International Prognostic Scoring System.
† One patient had a baseline spleen length recorded as nonpalpable in error but had a prior measurement of 16 cm and
a baseline spleen volume of 2450 cm3.
therapy (Fig. 1C). For this secondary end point, A post hoc analysis showed that patients who
among patients who had a reduction of 35% or received ruxolitinib had improvement in each in-
more in spleen volume, 67.0% (95% CI, 46.4 to dividual symptom assessed on the MFSAF (Fig.
81.1) had a reduction in spleen volume that was 2C), whereas symptoms worsened in the placebo
maintained for 48 weeks or more (loss of response group (P<0.01 for all comparisons with placebo).
was defined as a reduction of <35% from base- Prespecified analyses were conducted to cross-
line and an increase of ≥25% from the nadir). validate the modified MFSAF, version 2.0. The
Patient Global Impression of Change and other
Symptoms and Other Patient-Reported Outcomes patient-reported outcomes mirrored changes in
The proportion of patients with a reduction of 50% symptom scores (Fig. S3A, S3B, and S3C in the
or more in the total symptom score from baseline Supplementary Appendix). Patients who received
to week 24, a prespecified secondary end point, ruxolitinib had weight gain, whereas those receiv-
was significantly higher in the ruxolitinib group ing placebo had weight loss (Fig. S4 in the Supple-
than in the placebo group (45.9% vs. 5.3%; odds mentary Appendix). In the ruxolitinib group, 62.7%
ratio, 15.3; 95% CI, 6.9 to 33.7; P<0.001). Addi- of patients with a reduction in spleen volume of
tional prespecified analyses showed that among 35% or more had improvement of 50% or more in
the patients for whom baseline and week 24 data spleen-related symptoms (as indicated by the sum
were available, the 129 patients receiving ruxoli- of MFSAF scores for abdominal discomfort, pain
tinib had a mean improvement of 46.1% (median, under the ribs on the left side, and a feeling of
56.2%) in the total symptom score at week 24; fullness [early satiety]); however, this level of im-
the 103 patients receiving placebo had a mean provement also occurred in 46.9% of patients with
worsening of 41.8% (median, 14.6%) in the score a reduction in spleen volume of less than 35%. An
(P<0.001). The improvement was rapid and was additional post hoc analysis showed an improve-
maintained over the 24-week period during which ment of 50% or more in nonabdominal symptoms
symptom data were collected (Fig. 2A). Most pa- (night sweats, bone or muscle pain, and pruritus)
tients who received ruxolitinib had improvement in 58.6% of patients with reductions in spleen
in symptoms; the majority of patients who received volume of 35% or more and in 54.1% of patients
placebo had worsening of symptoms (Fig. 2B). with reductions in spleen volume of less than 35%.
802 n engl j med 366;9 nejm.org march 1, 2012
The New England Journal of Medicine
Downloaded from nejm.org on March 23, 2018. For personal use only. No other uses without permission.
Copyright © 2012 Massachusetts Medical Society. All rights reserved.
Ruxolitinib for Myelofibrosis
Figure 1. Change in Spleen Volume. A
Panel A shows the results of the intention-to-treat anal- 60 Odds ratio, 134.4 (95% CI, 18.0–1004.9)
ysis of the percentage of patients in each study group P<0.001
41.9
Patients with ≥35% Reduction
who reached the primary end point of a reduction of 50
35% or more in spleen volume as assessed by means
in Spleen Volume (%)
of magnetic resonance imaging (MRI) or computed 40
tomography (CT). Patients who discontinued the study
drug before week 24 or crossed over before week 24 were 30
counted as not having had a response. Only patients
with baseline data were included in this analysis. I bars 20
denote 95% confidence intervals. CI denotes confidence
interval. Panel B shows the percent change from base- 10
0.7
line in spleen volume at week 24 (in 139 patients in the
ruxolitinib group and 106 in the placebo group) or at 0
Ruxolitinib Placebo
the last evaluation before week 24 (in 16 patients in the (N = 155) (N = 153)
ruxolitinib group and 47 in the placebo group). Data for
1 patient with a missing baseline value are not included B
on the graph. Most patients in the ruxolitinib group
80
(150 of 155) had a reduction in spleen volume, where- Ruxolitinib (N=155)
as most patients in the placebo group had either an in- 60 Placebo (N=153)
Change in Spleen Volume
crease in spleen volume (102 of 153 patients) or no change
40
from Baseline (%)
(15 of 153 patients). Panel C shows the median percent
change in spleen volume as assessed by means of MRI 20
or CT over time. Reductions in spleen volume were ap-
parent at the first on-study measurement at 12 weeks 0
and were maintained over the course of the study. The −20
upper edge of each I bar corresponds to the 75th per- 35% Decrease
centile, and the lower edge to the 25th percentile. −40
−60
Subgroups −80
In a post hoc analysis of subgroups, mean changes Individual Patients
in spleen volume among patients with the JAK2 C
V617F mutation were −34.6% in the ruxolitinib 40
group and 8.1% in the placebo group; the corre-
Median Change in Spleen Volume
sponding changes among patients without the mu- 20 Placebo
tation were −23.8% and 8.4% (P value for interac-
from Baseline (%)
0
tion, 0.07). The changes in the total symptom score
among patients with the JAK2 V617F mutation were −20
−52.6% (improvement) in the ruxolitinib group and
−40
42.8% (worsening) in the placebo group, and the
changes among those without the mutation were −60 Ruxolitinib
−28.1% and 37.2%, respectively (P = 0.11 for inter-
action). Across myelofibrosis subtypes (primary −80
Baseline 12 24 36 48
myelofibrosis, post–polycythemia vera myelofibro-
Weeks
sis, and post–essential thrombocythemia myelo-
No. of Patients
fibrosis), patients who received ruxolitinib had a Ruxolitinib 148 139 69 16
decrease in spleen volume and improvement in the Placebo 132 106 46 13
total symptom score; patients receiving placebo
had increases in spleen volume (P = 0.52 for inter-and 21.5% at week 48; patients who received pla-
action) and worsening of the total symptom score cebo had a mean increase of 3.5% at week 24 and
(P = 0.46 for interaction) (Fig. S5A and S5B in the6.3% at week 48 (Fig. S6 in the Supplementary
Supplementary Appendix). Appendix). Furthermore, patients receiving ruxoli-
tinib had reductions in plasma levels of C-reactive
Biomarkers protein and the proinflammatory cytokines tumor
In a prespecified analysis of biomarkers, patients necrosis factor α and interleukin-6, and they had
who received ruxolitinib had mean reductions in increases in levels of plasma leptin and erythro-
the JAK2 V617F allele burden of 10.9% at week 24 poietin (Fig. S7 in the Supplementary Appendix).
n engl j med 366;9 nejm.org march 1, 2012 803
The New England Journal of Medicine
Downloaded from nejm.org on March 23, 2018. For personal use only. No other uses without permission.
Copyright © 2012 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
A Figure 2. Change in Symptom Scores.
60 Panel A shows the results of an intention-to-treat analysis
of the proportion of patients with at least a 50% reduction
Ruxolitinib (N=149) in the total symptom score over time (each value plotted
50 represents the moving average for the previous 7 days).
Patients with ≥50% Reduction
Patients who discontinued the study drug or for whom
in Total Symptom Score (%)
data were missing were considered not to have had a re-
40
sponse. The majority of responses occurred rapidly, with-
in the first 4 weeks after treatment. Only patients with
30 baseline data were included in this analysis. Panel B
shows the percent change from baseline in the total
symptom score at week 24 (in 129 patients in the ruxoli-
20 tinib group and 103 patients in the placebo group) and
at the last evaluation during receipt of the randomly as-
Placebo (N=152) signed study drug (in 16 patients in the ruxolitinib group
10
and 42 patients in the placebo group). Five patients with
a baseline score of 0, 8 patients with missing baseline val-
0 ues, and 6 patients with insufficient data after baseline
0 4 8 12 16 20 24 are not included. Whereas most patients who received
Weeks ruxolitinib had a reduction in the total symptom score,
the majority of patients who received placebo had a wors-
B ening of symptoms (worsening in the total symptom
150 score of ≥150% is shown as 150%). Panel C shows the
Ruxolitinib (N=145)
mean percent change in the score for each symptom in
125 Placebo(N=145)
Change in Total Symptom Score
the modified Myelofibrosis Symptom Assessment Form,
100 version 2.0. All symptoms improved in the ruxolitinib
75 group and worsened in the placebo group (P<0.01 for all
from Baseline (%)
50 comparisons with placebo). T bars denote standard errors.
25
0
−25
14 deaths in the placebo group (9.1%) (hazard ratio,
−50
50% Decrease 0.67; 95% CI, 0.30 to 1.50; P = 0.33). Subsequently, a
−75
survival analysis based on a planned data cutoff
with 4 additional months of follow-up (median
−100
Individual Patients follow-up, 51 weeks) revealed a significant survival
advantage for patients who received ruxolitinib,
C
111.9 with 13 deaths in the ruxolitinib group (8.4%) and
200 Ruxolitinib
24 deaths in the placebo group (15.6%) (hazard
Mean Change in Individual Symptom
(N=77)
Placebo
150 ratio, 0.50; 95% CI, 0.25 to 0.98; P = 0.04) (Fig. 3).
Score from Baseline (%)
70.3
62.8 (N=96) 60.0
100 55.7 (N=86)
(N=100)
51.0 (N=97) Safety
Worsening Improvement
(N=90) 37.7
50 A total of 155 patients in the ruxolitinib group and
(N=89)
151 in the placebo group received at least one
0 dose of the study medication and were included
−50 –29.4 –21.2 –32.1
in the analysis of safety. The number of patient-
(N=124) –46.9 –43.0 –42.1 –42.8 (N=108) (N=119) years of exposure was 105 in the ruxolitinib group
(N=109) (N=122) (N=103) (N=98)
−100 and 87 in the placebo group; study discontinuation
and crossover to ruxolitinib accounted for lower
s
ty
ts
ng
in
ity
t r
ib
fo
tie
ea
Pa
iv
hi
tR
om
Sw
t
Sa
Itc
ac
cle
exposure in the placebo group. Seventeen patients
ef
isc
In
rly
rL
ht
us
D
Ea
ig
de
who received ruxolitinib (11.0%) and 16 patients
N
al
un
or
in
m
in
ne
who received placebo (10.6%) discontinued the
do
Pa
Bo
Ab
study treatment because of adverse events (of any
grade). Twenty deaths occurred during the study or
Overall Survival within 28 days after the last dose was administered
For the secondary end point of overall survival, at (9 deaths in the ruxolitinib group and 11 deaths in
the time of data cutoff, 10 deaths were reported the placebo group, including 1 death after cross-
in the ruxolitinib group (6.5%) as compared with over) (see the Supplementary Appendix for more
804 n engl j med 366;9 nejm.org march 1, 2012
The New England Journal of Medicine
Downloaded from nejm.org on March 23, 2018. For personal use only. No other uses without permission.
Copyright © 2012 Massachusetts Medical Society. All rights reserved.
Ruxolitinib for Myelofibrosis
1.0
Ruxolitinib
0.8
Probability of Survival Placebo
0.6
0.4
0.2
Hazard ratio, 0.50 (95% CI, 0.25–0.98)
P=0.04 by log-rank test
0.0
0 4 8 12 16 20 24 28 32 36 40 44 48 52 56 60 64 68 72 76
Weeks
No. at Risk
Ruxolitinib 155 155 155 154 153 152 148 144 143 143 140 134 102 68 52 37 18 8 3
Placebo 154 152 151 148 147 147 142 139 132 131 123 115 83 58 45 35 20 9 3
Figure 3. Overall Survival.
Kaplan–Meier estimates of overall survival, including 4 months of additional follow-up after the primary analysis,
are shown. There were 13 deaths in the ruxolitinib group (8.4%) and 24 deaths in the placebo group (15.6%) during
a median follow-up period of 51 weeks. Tick marks indicate censoring times for individual patients.
detailed information). Principal causes of death in with an increase by week 24 to a new steady state
the ruxolitinib group were muscle weakness and (101 g per liter). The monthly prevalence of grade
general deterioration, subdural hematoma, renal 3 or 4 anemia and the proportion of patients re-
failure, non–small-cell lung cancer, acute myeloid quiring transfusions (1 or more units of red cells)
leukemia (AML), pneumonia (in 2 patients), and also followed a pattern that was consistent with
sepsis (in 2 patients). Principal causes of death in changes in the hemoglobin level over time (Fig.
the placebo group were staphylococcal infection, S9A and S9B in the Supplementary Appendix). Ac-
gastrointestinal hemorrhage, intestinal perfora- cording to the response criteria of the Interna-
tion, multiorgan failure, pneumonia, sepsis (in tional Working Group for Myelofibrosis Research
2 patients), and disease progression (in 4 patients). and Treatment, 41.2% of patients in the ruxolitinib
Overall, nonhematologic adverse events oc- group and 46.9% of patients in the placebo group
curred at a similar rate in the two groups. Events who were dependent on transfusions at baseline
that occurred more frequently in the ruxolitinib were classified as transfusion-independent during
group were ecchymosis, dizziness, and headache the study (Table S4 in the Supplementary Appen-
(predominantly grade 1 or 2) (Table 2). The most dix). In the ruxolitinib group, patients with new-
common grade 3 or 4 nonhematologic adverse onset grade 3 or 4 anemia had improvements in
events (abdominal pain, fatigue, and dyspnea) oc- symptoms and reductions in spleen volume that
curred more frequently in the placebo group. were similar to those in patients without anemia
Anemia and thrombocytopenia were the most (Fig. 9C and 9D in the Supplementary Appendix).
frequent hematologic adverse events (overall and Approximately half the grade 3 or 4 thrombo-
grade 3 or 4 events) (Table 2) and a reason for cytopenia events (11 of 20) occurred during the
treatment discontinuation in one patient in each first 8 weeks of treatment (Fig. S10 in the Supple-
study-drug group for each event. About half of all mentary Appendix) and led to dose adjustments or
grade 3 or 4 adverse events of anemia in the rux- brief treatment interruptions. Five patients had
olitinib group occurred during the first 8 weeks more than one episode of grade 3 or 4 thrombo-
of therapy. The mean hemoglobin level in patients cytopenia. Grade 3 episodes of bleeding (terms for
who received ruxolitinib reached a nadir of 95 g bleeding events are described in the Supplementary
per liter after approximately 8 to 12 weeks of Appendix) occurred in 2.6% of patients who re-
therapy (Fig. S8 in the Supplementary Appendix), ceived ruxolitinib and in 2.0% of patients who
n engl j med 366;9 nejm.org march 1, 2012 805
The New England Journal of Medicine
Downloaded from nejm.org on March 23, 2018. For personal use only. No other uses without permission.
Copyright © 2012 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
There was no clear pattern in these events to sug-
Table 2. Adverse Events Observed in 10% or More of Patients Who Received
Ruxolitinib. gest a specific withdrawal effect (Tables S5 and S6
in the Supplementary Appendix).
Event Ruxolitinib (N = 155) Placebo (N = 151) Two patients in the ruxolitinib group had a
All Grade All Grade transformation to AML during the study: one pa-
Grades 3 or 4 Grades 3 or 4
tient with 7% bone marrow blasts at baseline and
percent of patients
a history of breast cancer had AML transformation
Nonhematologic
after 8 months in the study; the second patient
Fatigue 25.2 5.2 33.8 6.6 entered the study with 2% bone marrow blasts and
Diarrhea 23.2 1.9 21.2 0 a trisomy 8 chromosomal abnormality at baseline
Peripheral edema 18.7 0 22.5 1.3 and had AML transformation after 5 months in the
Ecchymosis 18.7 0 9.3 0 study. There were no transformations in the pla-
Dyspnea 17.4 1.3 17.2 4.0 cebo group.
Dizziness 14.8 0.6 6.6 0
Nausea 14.8 0 19.2 0.7 Discussion
Headache 14.8 0 5.3 0
Constipation 12.9 0 11.9 0 In this study, ruxolitinib therapy was significantly
Vomiting 12.3 0.6 9.9 0.7 more effective than placebo with respect to all pri-
Pain in extremity 12.3 1.3 9.9 0 mary and secondary efficacy end points, as well as
Insomnia 11.6 0 9.9 0 in an updated analysis of overall survival. In the
Arthralgia 11.0 1.9 8.6 0.7 ruxolitinib group, 41.9% of patients met the de-
Pyrexia 11.0 0.6 7.3 0.7 fined response threshold of a reduction of 35% or
Abdominal pain 10.3 2.6 41.1 11.3 more in spleen volume, and nearly all the patients
Hematologic abnormalities* had some reduction in spleen volume. Reductions
Anemia 96.1 45.2 86.8 19.2 in spleen volume were durable; 67.0% of patients
Thrombocytopenia 69.7 12.9 30.5 1.3 with a response had this response for 48 weeks or
Neutropenia 18.7 7.1 4.0 2.0 longer with continued therapy.
Improvements in symptoms were measured
* Hematologic abnormalities are based on laboratory values. The data shown with the use of the modified MFSAF, version 2.0,
are for events of the worst grade during the study, regardless of whether this
grade was a change from the baseline grade.
diary, a tool designed specifically to assess symp-
toms of myelofibrosis. The majority of patients
had improvements in symptoms, which occurred
received placebo. Grade 4 episodes of bleeding even in patients who did not have a reduction in
occurred in 1.3% of patients who received ruxoli- spleen volume of 35% or more. In contrast, most
tinib and in 1.3% of patients who received place- patients who received placebo had progressive
bo. Bruising (bleeding events related to skin and splenomegaly and worsening of myelofibrosis-
subcutaneous tissue) (see the Supplementary Ap- related symptoms. Changes in symptoms record-
pendix) was assessed separately. A total of 23.2% ed with the MFSAF were directionally consistent
of patients who received ruxolitinib and 14.6% of with the assessments made with other validated
patients who received placebo had bruising; all and common patient-reported outcome instru-
events were grade 1 or 2 except for one grade ments used in this study.
3 event in the ruxolitinib group. Anemia and thrombocytopenia were more
Among patients in whom the study drug was common in patients who received ruxolitinib than
interrupted, symptoms (assessed by means of the in patients who received placebo. These adverse
total symptom score) returned to baseline levels events were manageable, as evidenced by the low
over a period of approximately 1 week (Fig. S11 in discontinuation rate (one patient in each group for
the Supplementary Appendix). Adverse events of each event). Thrombocytopenia rarely recurred at
grade 3 or higher developed in 8 of 49 patients in a grade 3 or 4 level after appropriate dose modi-
the ruxolitinib group (16.3%) and in 7 of 54 pa- fications and was not associated with an increase
tients in the placebo group (13.0%) after interrup- in bleeding events, although bruising was more
tion of the study drug and in 12 of 21 patients in common in the ruxolitinib group. The prevalence
the ruxolitinib group (57.1%) and 17 of 37 patients of grade 3 or 4 anemia peaked after approximately
in the placebo group (45.9%) after discontinuation. 8 to 12 weeks of ruxolitinib therapy, subsequently
806 n engl j med 366;9 nejm.org march 1, 2012
The New England Journal of Medicine
Downloaded from nejm.org on March 23, 2018. For personal use only. No other uses without permission.
Copyright © 2012 Massachusetts Medical Society. All rights reserved.
Ruxolitinib for Myelofibrosis
decreasing to levels similar to those in patients managed with dose modification. These findings
who received placebo. In the ruxolitinib group, show that ruxolitinib is an effective therapy for
patients with new-onset grade 3 or 4 anemia had myelofibrosis.
symptomatic improvement similar to that in pa- Supported by Incyte.
Dr. Verstovsek reports receiving grant support through his in-
tients without anemia. In the placebo group, pa- stitution from Incyte, Exelixis, Celgene, NS Pharma, Infinity Phar-
tients with and those without grade 3 or 4 anemia maceuticals, SBIO, Lilly Oncology, AstraZeneca, Geron, Bristol-
had worsening of symptoms, which was greater in Myers Squibb, YM BioSciences, Gilead, and Roche; Dr. Levy, being
an employee of Incyte and receiving stock options as part of his
patients with anemia. compensation; Dr. Gupta, receiving grant support through his
Transformation to AML occurred in 2 patients institution from Incyte and Novartis, consulting fees from Incyte
in this study; both patients received ruxolitinib and and Novartis, and lecture fees from Novartis; Dr. Catalano, receiv-
ing consulting fees from Incyte; Dr. Deininger, receiving consult-
had baseline characteristics that placed them at ing fees from Bristol-Myers Squibb, Novartis, and Ariad, and grant
increased risk for transformation. In a separate support through his institution from Bristol-Myers Squibb; Dr.
phase 3 trial with a median follow-up of 61 weeks, Miller, receiving grant support through her institution, consulting
fees, and lecture fees from Novartis, and payments for develop-
there were no transformations to AML in 146 pa- ment of educational presentations from Incyte and Novartis; Dr.
tients who received ruxolitinib and two transforma- Silver, receiving grant support through his institution from Incyte
tions in 73 patients who received the best available and lecture fees from Incyte, and holding stock in Incyte both
individually and through his institution; Dr. Lyons, receiving
16
therapy. Longer-term follow-up will be required grant support through his institution from Incyte; Dr. Paquette,
to better define rates of AML transformation. receiving consulting fees paid through his institution from Incyte;
After interruption of ruxolitinib therapy, myelo- Dr. Vaddi, being an employee of Incyte and receiving stock or stock
options as a part of his compensation; Dr. Erickson-Viitanen, be-
fibrosis-related symptoms gradually returned to ing an employee of Incyte and receiving stock or stock options as
baseline levels. A between-group comparison of part of her compensation; Dr. Sun, being an employee of Incyte
adverse events reported after interruption or per- and receiving stock options as part of his compensation; Dr. San-
dor, being an employee of Incyte and receiving stock or stock op-
manent discontinuation of the study drug showed tions as part of his compensation; and Dr. Kantarjian, receiving
no clear pattern of a specific withdrawal effect. grant support through his institution from Incyte. No other po-
tential conflict of interest relevant to this article was reported.
In conclusion, ruxolitinib was associated with Disclosure forms provided by the authors are available with
reductions in splenomegaly and symptoms that are the full text of this article at NEJM.org.
prominent manifestations of myelofibrosis and We thank Kelly Reith of Incyte for editorial assistance with an
earlier version of the manuscript and Daniel Hutta, Ph.D., of
appeared to be associated with an improvement Articulate Science for medical writing assistance with an early
in overall survival. Toxic effects were generally draft of the manuscript.
References
1. Tefferi A, Vaidya R, Caramazza D, apeutic implications for the treatment of Blood 2009;114(22):3917. abstract.
Finke C, Lasho T, Pardanani A. Circulat- myeloproliferative neoplasms. Blood 2010; 12. Tefferi A, Barosi G, Mesa RA, et al. Inter
ing interleukin (IL)-8, IL-2R, IL-12, and 115:3109-17. national Working Group (IWG) consensus
IL-15 levels are independently prognostic 7. Verstovsek S, Kantarjian H, Mesa RA, criteria for treatment response in myelofi-
in primary myelofibrosis: a comprehen- et al. Safety and efficacy of INCB018424, brosis with myeloid metaplasia, for the IWG
sive cytokine profiling study. J Clin Oncol a JAK1 and JAK2 inhibitor, in myelofibro- for Myelofibrosis Research and Treatment
2011;29:1356-63. sis. N Engl J Med 2010;363:1117-27. (IWG-MRT). Blood 2006;108:1497-503.
2. Cervantes F, Dupriez B, Pereira A, et al. 8. Tefferi A, Vardiman JW. Classification 13. Harris A, Kamishima T, Hao HY, et al.
New prognostic scoring system for pri- and diagnosis of myeloproliferative neo- Splenic volume measurements on comput-
mary myelofibrosis based on a study of plasms: the 2008 World Health Organiza- ed tomography utilizing automatically con-
the International Working Group for Myelo- tion criteria and point-of-care diagnostic touring software and its relationship with
fibrosis Research and Treatment. Blood algorithms. Leukemia 2008;22:14-22. age, gender, and anthropometric parame-
2009;113:2895-901. 9. Oken MM, Creech RH, Tormey DC, et ters. Eur J Radiol 2010;75(1):e97-e101.
3. Abdel-Wahab OI, Levine RL. Primary al. Toxicity and response criteria of the 14. Mazonakis M, Damilakis J, Maris T,
myelofibrosis: update on definition, patho- Eastern Cooperative Oncology Group. Am Prassopoulos P, Gourtsoyiannis N. Esti-
genesis, and treatment. Annu Rev Med J Clin Oncol 1982;5:649-55. mation of spleen volume using MR imag-
2009;60:233-45. 10. Mesa RA, Kantarjian H, Tefferi A, et al. ing and a random marking technique. Eur
4. Delhommeau F, Jeziorowska D, Marzac Evaluating the serial use of the Myelofi- Radiol 2000;10:1899-903.
C, Casadevall N. Molecular aspects of my- brosis Symptom Assessment Form for mea- 15. Prassopoulos P, Daskalogiannaki M,
eloproliferative neoplasms. Int J Hematol suring symptomatic improvement: perfor- Raissaki M, Hatjidakis A, Gourtsoyiannis
2010;91:165-73. mance in 87 myelofibrosis patients on a N. Determination of normal splenic vol-
5. Vainchenker W, Dusa A, Constanti- JAK1 and JAK2 inhibitor (INCB018424) ume on computed tomography in relation
nescu SN. JAKs in pathology: role of Janus clinical trial. Cancer 2011;117:4869-77. to age, gender and body habitus. Eur Ra-
kinases in hematopoietic malignancies 11. Mesa RA, Kantarjian H, Tefferi A, et al. diol 1997;7:246-8.
and immunodeficiencies. Semin Cell Dev Validation of the serial use of the Myelo- 16. Harrison C, Kiladjian J-J, Al-Ali HK, et
Biol 2008;19:385-93. fibrosis Symptom Assessment Form al. JAK inhibition with ruxolitinib versus
6. Quintás-Cardama A, Vaddi K, Liu P, et (MF-SAF) for measuring symptomatic im- best available therapy for myelofibrosis.
al. Preclinical characterization of the se- provement: performance in 86 myelofibro- N Engl J Med 2012;366:787-98.
lective JAK1/2 inhibitor INCB018424: ther- sis patients on INCB018424 clinical trial. Copyright © 2012 Massachusetts Medical Society.
n engl j med 366;9 nejm.org march 1, 2012 807
The New England Journal of Medicine
Downloaded from nejm.org on March 23, 2018. For personal use only. No other uses without permission.
Copyright © 2012 Massachusetts Medical Society. All rights reserved.
Vous aimerez peut-être aussi
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (119)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (587)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2219)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (894)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- Vanders Human Physiology The Mechanisms of Body Function 15th Edition Widmaier Test BankDocument29 pagesVanders Human Physiology The Mechanisms of Body Function 15th Edition Widmaier Test BankDavidWardrcobi100% (15)
- Cooling Tower Operation - 030129Document8 pagesCooling Tower Operation - 030129Sekar CmPas encore d'évaluation
- Poultry Science MCQDocument12 pagesPoultry Science MCQelanthamizhmaran83% (6)
- Turbidimetry and Nephelometry1Document3 pagesTurbidimetry and Nephelometry1maxim_crank6101100% (1)
- Warlock of The Magus World - Arc 2Document808 pagesWarlock of The Magus World - Arc 2Hitsuin MoviesPas encore d'évaluation
- Microbiological Test of Medical DevicesDocument5 pagesMicrobiological Test of Medical Devicesbijendra_sinhaPas encore d'évaluation
- Ashish RunthalaDocument10 pagesAshish RunthalaAnonymous V5l8nmcSxbPas encore d'évaluation
- Comparison of A New Sensitive Skin Questionnaire and Baumanns Sensitiveskin Questionnaire in Chengdu ChinaDocument4 pagesComparison of A New Sensitive Skin Questionnaire and Baumanns Sensitiveskin Questionnaire in Chengdu ChinaAnonymous V5l8nmcSxbPas encore d'évaluation
- Cardiovascular and Metabolic Comorbidities of Psoriasis DMCR 1000106Document9 pagesCardiovascular and Metabolic Comorbidities of Psoriasis DMCR 1000106Anonymous V5l8nmcSxbPas encore d'évaluation
- Editorial: Secondary Osteoporosis: Endocrine and Metabolic Causes of Bone Mass DeteriorationDocument2 pagesEditorial: Secondary Osteoporosis: Endocrine and Metabolic Causes of Bone Mass DeteriorationAnonymous V5l8nmcSxbPas encore d'évaluation
- OMICS International ArticlesDocument3 pagesOMICS International ArticlesAnonymous V5l8nmcSxbPas encore d'évaluation
- Research Article: Osteoporosis Knowledge of Students in Relevant Healthcare Academic ProgramsDocument4 pagesResearch Article: Osteoporosis Knowledge of Students in Relevant Healthcare Academic ProgramsAnonymous V5l8nmcSxbPas encore d'évaluation
- Demodex Follicullorum Mimicking Fungal Infection A Case ReportDocument2 pagesDemodex Follicullorum Mimicking Fungal Infection A Case ReportAnonymous V5l8nmcSxb100% (1)
- Clinical Characteristics and Etiologic Analysis of Scabiesassociatedglomerulonephritis 2165 8048 1000198Document5 pagesClinical Characteristics and Etiologic Analysis of Scabiesassociatedglomerulonephritis 2165 8048 1000198Anonymous V5l8nmcSxbPas encore d'évaluation
- Dermatophytosis Due To Trichophyton Verrucosum and T Mentagrophytes DMCR 1000101Document1 pageDermatophytosis Due To Trichophyton Verrucosum and T Mentagrophytes DMCR 1000101Anonymous V5l8nmcSxbPas encore d'évaluation
- Niru Khatiwada Kathmandu University NepalDocument43 pagesNiru Khatiwada Kathmandu University NepalAnonymous V5l8nmcSxbPas encore d'évaluation
- F 12Document5 pagesF 12Anonymous V5l8nmcSxbPas encore d'évaluation
- OMICS Journals Are Welcoming Submissions: For More Details Please Visit Our WebsiteDocument9 pagesOMICS Journals Are Welcoming Submissions: For More Details Please Visit Our WebsiteAnonymous V5l8nmcSxbPas encore d'évaluation
- Research Article: Bone Mineral Density of Adolescent Female Tennis Players and Nontennis PlayersDocument5 pagesResearch Article: Bone Mineral Density of Adolescent Female Tennis Players and Nontennis PlayersAnonymous V5l8nmcSxbPas encore d'évaluation
- Editorial: Secondary Osteoporosis: Endocrine and Metabolic Causes of Bone Mass DeteriorationDocument2 pagesEditorial: Secondary Osteoporosis: Endocrine and Metabolic Causes of Bone Mass DeteriorationAnonymous V5l8nmcSxbPas encore d'évaluation
- Research Article: Potential Extensions of The US FRAX AlgorithmDocument8 pagesResearch Article: Potential Extensions of The US FRAX AlgorithmAnonymous V5l8nmcSxbPas encore d'évaluation
- Research ArticleDocument10 pagesResearch ArticleAnonymous V5l8nmcSxbPas encore d'évaluation
- Research Article: Potential Extensions of The US FRAX AlgorithmDocument8 pagesResearch Article: Potential Extensions of The US FRAX AlgorithmAnonymous V5l8nmcSxbPas encore d'évaluation
- Research Article: Bone Mineral Density of Adolescent Female Tennis Players and Nontennis PlayersDocument5 pagesResearch Article: Bone Mineral Density of Adolescent Female Tennis Players and Nontennis PlayersAnonymous V5l8nmcSxbPas encore d'évaluation
- Research Article: Normative Data For Bone Mass in Healthy Term Infants From Birth To 1 Year of AgeDocument8 pagesResearch Article: Normative Data For Bone Mass in Healthy Term Infants From Birth To 1 Year of AgeAnonymous V5l8nmcSxbPas encore d'évaluation
- Review Article: Are Selective Serotonin Reuptake Inhibitors A Secondary Cause of Low Bone Density?Document7 pagesReview Article: Are Selective Serotonin Reuptake Inhibitors A Secondary Cause of Low Bone Density?Anonymous V5l8nmcSxbPas encore d'évaluation
- Journalusagehalflife PDFDocument5 pagesJournalusagehalflife PDFSanti ParambangPas encore d'évaluation
- j13 PDFDocument11 pagesj13 PDFAnonymous V5l8nmcSxbPas encore d'évaluation
- Evidence-Based Guideline: Clinical Evaluation and Treatment of Transverse MyelitisDocument8 pagesEvidence-Based Guideline: Clinical Evaluation and Treatment of Transverse MyelitisAnonymous V5l8nmcSxbPas encore d'évaluation
- Author and User Rights: Authors Scholarly Rights Institution With A Journal SubscriptionDocument11 pagesAuthor and User Rights: Authors Scholarly Rights Institution With A Journal SubscriptionPoohzain PuspaPas encore d'évaluation
- J Child Neurol 2012 Wolf 1426 36Document12 pagesJ Child Neurol 2012 Wolf 1426 36Elga ElaskiaPas encore d'évaluation
- AppDocument8 pagesAppAnonymous V5l8nmcSxbPas encore d'évaluation
- J 9Document2 pagesJ 9Anonymous V5l8nmcSxbPas encore d'évaluation
- Evidence-Based Guideline: Clinical Evaluation and Treatment of Transverse MyelitisDocument8 pagesEvidence-Based Guideline: Clinical Evaluation and Treatment of Transverse MyelitisAnonymous V5l8nmcSxbPas encore d'évaluation
- Acute Apendicitis LancetDocument10 pagesAcute Apendicitis LancetJeisson Castillo ChauxPas encore d'évaluation
- The Introduction of Adult Appendicitis Score Reduced Negative Appendectomy RateDocument6 pagesThe Introduction of Adult Appendicitis Score Reduced Negative Appendectomy RateAnonymous V5l8nmcSxbPas encore d'évaluation
- Structure of Tooth m121Document13 pagesStructure of Tooth m121amirhossein vaeziPas encore d'évaluation
- Part 8 Biological ScienceDocument5 pagesPart 8 Biological ScienceSteven CentenoPas encore d'évaluation
- Pecutan Akhir Science 2021Document29 pagesPecutan Akhir Science 2021Azween SabtuPas encore d'évaluation
- Hemostatic Effects of Peperomia PellucidDocument41 pagesHemostatic Effects of Peperomia PellucidGina Rose De GuzmanPas encore d'évaluation
- Cellular RespirationDocument20 pagesCellular RespirationAlessiaPas encore d'évaluation
- Explaining Butterfly MetamorphosisDocument13 pagesExplaining Butterfly MetamorphosisCipe drPas encore d'évaluation
- Sickle Cell AnemiaDocument7 pagesSickle Cell AnemiaJuma AwarPas encore d'évaluation
- Human Contact May Reduce Stress in Shelter DogsDocument5 pagesHuman Contact May Reduce Stress in Shelter DogsFlorina AnichitoaePas encore d'évaluation
- A Review of The Environmental Fate, Effects, and Exposures of Bisphenol A PDFDocument25 pagesA Review of The Environmental Fate, Effects, and Exposures of Bisphenol A PDFTiago TorresPas encore d'évaluation
- Full Essay Academic SkillsDocument3 pagesFull Essay Academic SkillsNurl AinaPas encore d'évaluation
- Introduction To Bioinformatics: Database Search (FASTA)Document35 pagesIntroduction To Bioinformatics: Database Search (FASTA)mahedi hasanPas encore d'évaluation
- Analisis Kualitatif Dan Kuantitatif Kandungan Kimia Dari Ekstrak Heksan, Aseton, Etanol Dan Air Dari Umbi Bawang Putih (Allium Sativum Linn.)Document11 pagesAnalisis Kualitatif Dan Kuantitatif Kandungan Kimia Dari Ekstrak Heksan, Aseton, Etanol Dan Air Dari Umbi Bawang Putih (Allium Sativum Linn.)Tari PratiwiPas encore d'évaluation
- Kingdom Protista: Diverse Eukaryotic MicroorganismsDocument79 pagesKingdom Protista: Diverse Eukaryotic MicroorganismsMeah PachecoPas encore d'évaluation
- Cell Division GizmoDocument3 pagesCell Division Gizmoapi-522847737Pas encore d'évaluation
- Daftar PustakaDocument3 pagesDaftar PustakaAdnanPas encore d'évaluation
- 2 Part 1Document99 pages2 Part 1m_luchianPas encore d'évaluation
- Organizing A TextDocument3 pagesOrganizing A TextMercedes Jimenez RomanPas encore d'évaluation
- NSABB Final Report Recommendations Evaluation Oversight Proposed Gain of Function Research May 2016Document109 pagesNSABB Final Report Recommendations Evaluation Oversight Proposed Gain of Function Research May 2016Jim Hoft100% (1)
- The Vulcanization of BrainDocument30 pagesThe Vulcanization of BrainJohnny FragosoPas encore d'évaluation
- Adlerian Psychotherapy: Prioritizing RelationshipsDocument24 pagesAdlerian Psychotherapy: Prioritizing RelationshipsJayanth MamundiPas encore d'évaluation
- Cell Membrane: A Selective BarrierDocument23 pagesCell Membrane: A Selective BarrierHama JamalPas encore d'évaluation
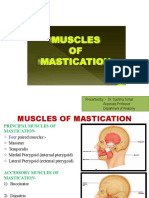
- Presented By:-Dr. Sushma Tomar Associate Professor Department of AnatomyDocument20 pagesPresented By:-Dr. Sushma Tomar Associate Professor Department of AnatomyCristine EchavePas encore d'évaluation
- Molecular Genetics of Colorectal Cancer - UpToDateDocument41 pagesMolecular Genetics of Colorectal Cancer - UpToDateToweran ToweranePas encore d'évaluation
- Effects of Different Fermentation Temperatures On Metabolites of KimchiDocument7 pagesEffects of Different Fermentation Temperatures On Metabolites of KimchiAngela ValdiviesoPas encore d'évaluation