Académique Documents
Professionnel Documents
Culture Documents
Id
Transféré par
api-278913876Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Id
Transféré par
api-278913876Droits d'auteur :
Formats disponibles
904 SECTION VIII Chemotherapeutic Drugs
TABLE 51–1 Empiric antimicrobial therapy based on microbiologic etiology.
Suspected or Proven Disease or Pathogen Drugs of First Choice Alternative Drugs
Gram-negative cocci (aerobic)
1 3 4
Moraxella (Branhamella) catarrhalis TMP-SMZ, cephalosporin Quinolone, macrolide
2
(second- or third-generation)
Neisseria gonorrhoeae Ceftriaxone, cefixime Spectinomycin, azithromycin
Neisseria meningitides Penicillin G Chloramphenicol, ceftriaxone, cefotaxime
Gram-negative rods (aerobic)
E coli, Klebsiella, Proteus Cephalosporin (first- or second- Quinolone,3 aminoglycoside5
2 1
generation), TMP-SMZ
1 3 7 5
Enterobacter, Citrobacter, Serratia TMP-SMZ, quinolone, Antipseudomonal penicillin, aminoglycoside, cefepime
6
carbapenem
3 1
Shigella Quinolone TMP-SMZ, ampicillin, azithromycin, ceftriaxone
3
Salmonella Quinolone, ceftriaxone Chloramphenicol, ampicillin, TMP-SMZ1
Campylobacter jejuni Erythromycin or azithromycin Tetracycline, quinolone3
Brucella species Doxycycline + rifampin or Chloramphenicol + aminoglycoside5 or TMP-SMZ1
aminoglycoside5
Helicobacter pylori Proton pump inhibitor + amoxi- Bismuth + metronidazole + tetracycline + proton pump
cillin + clarithromycin inhibitor
Vibrio species Tetracycline Quinolone,3 TMP-SMZ1
3
Pseudomonas aeruginosa Antipseudomonal penicillin ± Antipseudomonal penicillin ± quinolone, cefepime,
aminoglycoside5 6
ceftazidime, antipseudomonal carbapenem, or aztreonam
5
± aminoglycoside
Burkholderia cepacia (formerly Pseudomonas TMP-SMZ1 Ceftazidime, chloramphenicol
cepacia)
Stenotrophomonas maltophilia (formerly TMP-SMZ1 Minocycline, ticarcillin-clavulanate, tigecycline,
3
Xanthomonas maltophilia) ceftazidime, quinolone
Legionella species Azithromycin or quinolone3 Clarithromycin, erythromycin
Gram-positive cocci (aerobic)
Streptococcus pneumoniae Penicillin8 Doxycycline, ceftriaxone, antipneumococcal quinolone,3
macrolide,4 linezolid
2
Streptococcus pyogenes (group A) Penicillin, clindamycin Erythromycin, cephalosporin (first-generation)
5
Streptococcus agalactiae (group B) Penicillin (± aminoglycoside ) Vancomycin
2
Viridans streptococci Penicillin Cephalosporin (first- or third-generation), vancomycin
Staphylococcus aureus
β-Lactamase negative Penicillin Cephalosporin (first-generation),2 vancomycin
9
β-Lactamase positive Penicillinase-resistant penicillin As above
Methicillin-resistant Vancomycin TMP-SMZ,1 minocycline, linezolid, daptomycin, tigecycline
10 5 5
Enterococcus species Penicillin ± aminoglycoside Vancomycin ± aminoglycoside
Gram-positive rods (aerobic)
3
Bacillus species (non-anthracis) Vancomycin Imipenem, quinolone, clindamycin
1
Listeria species Ampicillin (± aminoglycoside5) TMP-SMZ
1
Nocardia species Sulfadiazine, TMP-SMZ Minocycline, imipenem, amikacin, linezolid
Anaerobic bacteria
6
Gram-positive (clostridia, Peptococcus, Penicillin, clindamycin Vancomycin, carbapenem, chloramphenicol
Actinomyces, Peptostreptococcus)
Clostridium difficile Metronidazole Vancomycin, bacitracin
Bacteroides fragilis Metronidazole Chloramphenicol, carbapenem,6 β-lactam–β-lactamase-
inhibitor combinations, clindamycin
(continued )
CHAPTER 51 Clinical Use of Antimicrobial Agents 905
TABLE 51–1 Empiric antimicrobial therapy based on microbiologic etiology. (Continued)
Suspected or Proven Disease or Pathogen Drugs of First Choice Alternative Drugs
Fusobacterium, Prevotella, Porphyromonas Metronidazole, clindamycin, As for B fragilis
penicillin
Mycobacteria
Mycobacterium tuberculosis Isoniazid + rifampin + Streptomycin, moxifloxacin, amikacin, ethionamide,
ethambutol + pyrazinamide cycloserine, PAS, linezolid
Mycobacterium leprae
Multibacillary Dapsone + rifampin +
clofazimine
Paucibacillary Dapsone + rifampin
Mycoplasma pneumoniae Tetracycline, erythromycin Azithromycin, clarithromycin, quinolone3
Chlamydia
C trachomatis Tetracycline, azithromycin Clindamycin, ofloxacin
C pneumoniae Tetracycline, erythromycin Clarithromycin, azithromycin
C psittaci Tetracycline Chloramphenicol
Spirochetes
Borrelia recurrentis Doxycycline Erythromycin, chloramphenicol, penicillin
Borrelia burgdorferi
Early Doxycycline, amoxicillin Cefuroxime axetil, penicillin
Late Ceftriaxone
Leptospira species Penicillin Tetracycline
Treponema species Penicillin Tetracycline, azithromycin, ceftriaxone
Fungi
Aspergillus species Voriconazole Amphotericin B, itraconazole, caspofungin
Blastomyces species Amphotericin B Itraconazole, fluconazole
11
Candida species Amphotericin B, echinocandin Fluconazole, itraconazole, voriconazole
Cryptococcus Amphotericin B ± flucytosine Fluconazole, voriconazole
(5-FC)
Coccidioides immitis Amphotericin B Fluconazole, itraconazole, voriconazole, posaconazole
Histoplasma capsulatum Amphotericin B Itraconazole
Mucoraceae (Rhizopus, Absidia) Amphotericin B Posaconazole
Sporothrix schenckii Amphotericin B Itraconazole
1
Trimethoprim-sulfamethoxazole (TMP-SMZ) is a mixture of one part trimethoprim plus five parts sulfamethoxazole.
2
First-generation cephalosporins: cefazolin for parenteral administration; cefadroxil or cephalexin for oral administration. Second-generation cephalosporins: cefuroxime for
parenteral administration; cefaclor, cefuroxime axetil, cefprozil for oral administration. Third-generation cephalosporins: ceftazidime, cefotaxime, ceftriaxone for parenteral
administration; cefixime, cefpodoxime, ceftibuten, cefdinir, cefditoren for oral administration. Fourth-generation cephalosporin: cefepime for parenteral administration.
Cephamycins: cefoxitin and cefotetan for parenteral administration.
3
Quinolones: ciprofloxacin, gemifloxacin, levofloxacin, moxifloxacin, norfloxacin, ofloxacin. Norfloxacin is not effective for the treatment of systemic infections. Gemifloxacin,
levofloxacin, and moxifloxacin have excellent activity against pneumococci. Ciprofloxacin and levofloxacin have good activity against Pseudomonas aeruginosa.
4
Macrolides: azithromycin, clarithromycin, dirithromycin, erythromycin.
5
Generally, streptomycin and gentamicin are used to treat infections with gram-positive organisms, whereas gentamicin, tobramycin, and amikacin are used to treat infections
with gram-negatives.
6
Carbapenems: doripenem, ertapenem, imipenem, meropenem. Ertapenem lacks activity against enterococci, Acinetobacter, and P aeruginosa.
7
Antipseudomonal penicillin: piperacillin, piperacillin/tazobactam, ticarcillin/clavulanic acid.
8
See footnote 3 in Table 51–2 for guidelines on the treatment of penicillin-resistant pneumococcal meningitis.
9
Parenteral nafcillin or oxacillin; oral dicloxacillin.
10
There is no regimen that is reliably bactericidal for vancomycin-resistant enterococcus for which there is extensive clinical experience; daptomycin has bactericidal activity in
vitro. Regimens that have been reported to be efficacious include nitrofurantoin (for urinary tract infection); potential regimens for bacteremia include daptomycin, linezolid,
and dalfopristin/quinupristin.
11
Echinocandins: anidulafungin, caspofungin, micafungin.
906 SECTION VIII Chemotherapeutic Drugs
TABLE 51–2 Empiric antimicrobial therapy based on site of infection.
Presumed Site of Infection Common Pathogens Drugs of First Choice Alternative Drugs
Bacterial endocarditis
Acute Staphylococcus aureus Vancomycin + gentamicin Penicillinase-resistant
1
penicillin + gentamicin
Subacute Viridans streptococci, enterococci Penicillin + gentamicin Vancomycin + gentamicin
Septic arthritis
Child H influenzae, S aureus, β-hemolytic Ceftriaxone Ampicillin-sulbactam
streptococci
Adult S aureus, Enterobacteriaceae Cefazolin Vancomycin, quinolone
Acute otitis media, H influenzae, S pneumoniae, Amoxicillin Amoxicillin-clavulanate,
sinusitis M catarrhalis cefuroxime axetil, TMP-SMZ
Cellulitis S aureus, group A streptococcus Penicillinase-resistant penicillin, Vancomycin, clindamycin,
cephalosporin (first-generation)2 linezolid, daptomycin
Meningitis
Neonate Group B streptococcus, E coli, Listeria Ampicillin + cephalosporin (third- Ampicillin + aminoglycoside,
generation) chloramphenicol, meropenem
Child H influenzae, pneumococcus, Ceftriaxone or cefotaxime ± Chloramphenicol, meropenem
meningococcus vancomycin3
Adult Pneumococcus, meningococcus Ceftriaxone, cefotaxime Vancomycin + ceftriaxone or
cefotaxime3
Peritonitis due to Coliforms, B fragilis Metronidazole + cephalosporin Carbapenem, tigecycline
ruptured viscus (third-generation), piperacillin/
tazobactam
Pneumonia
Neonate As in neonatal meningitis
Child Pneumococcus, S aureus, H influenzae Ceftriaxone, cefuroxime, cefotaxime Ampicillin-sulbactam
Adult (community- Pneumococcus, Mycoplasma, Outpatient: Macrolide,4 amoxicillin, Outpatient: Quinolone
acquired) Legionella, H influenzae, S aureus, tetracycline
C pneumonia, coliforms
Inpatient: Macrolide4 + cefotaxime, Inpatient: Doxycycline +
ceftriaxone, ertapenem, or ampicillin cefotaxime, ceftriaxone,
ertapenem, or ampicillin;
5
respiratory quinolone
Septicemia6 Any Vancomycin + cephalosporin (third-generation) or piperacillin/
tazobactam or imipenem or meropenem
Septicemia with Any Antipseudomonal penicillin + aminoglycoside; ceftazidime; cefepime;
granulocytopenia imipenem or meropenem; consider addition of systemic antifungal therapy
if fever persists beyond 5 days of empiric therapy
1
See footnote 9, Table 51–1.
2
See footnote 2, Table 51–1.
3
When meningitis with penicillin-resistant pneumococcus is suspected, empiric therapy with this regimen is recommended.
4
Erythromycin, clarithromycin, or azithromycin (an azalide) may be used.
5
Quinolones used to treat pneumonococcal infections include levofloxacin, moxifloxacin, and gemifloxacin.
6
Adjunctive immunomodulatory drugs such as drotrecogin-alfa can also be considered for patients with severe sepsis.
done to maximize it. For example, are adequate numbers of ANTIMICROBIAL PHARMACODYNAMICS
granulocytes present and are HIV infection, malnutrition, or
underlying malignancy present? The presence of abscesses or for- The time course of drug concentration is closely related to the anti-
eign bodies should also be considered. Finally, culture and suscep- microbial effect at the site of infection and to any toxic effects.
tibility testing should be repeated to determine whether Pharmacodynamic factors include pathogen susceptibility testing,
superinfection has occurred with another organism or whether the drug bactericidal versus bacteriostatic activity, drug synergism, antag-
original pathogen has developed drug resistance. onism, and postantibiotic effects. Together with pharmacokinetics,
Vous aimerez peut-être aussi
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- BIOLOGY CONCEPT MAPS XI and XII PDFDocument37 pagesBIOLOGY CONCEPT MAPS XI and XII PDFSatish Science100% (3)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Bacteria QuizDocument10 pagesBacteria QuizMark Abion ValladolidPas encore d'évaluation
- Importance of Self Healing ConcreteDocument19 pagesImportance of Self Healing ConcreteAnonymous gA8TMWG1pw86% (7)
- Use of Bioflocs in Shrimp Farming: July 2014Document6 pagesUse of Bioflocs in Shrimp Farming: July 2014Kresimir Sedak-BencicPas encore d'évaluation
- Contoh Rencana Studi LPDPDocument3 pagesContoh Rencana Studi LPDPZahid ZainPas encore d'évaluation
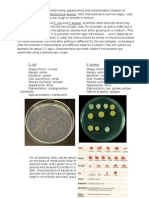
- Bacteria Colony Appearance MorphologyDocument2 pagesBacteria Colony Appearance MorphologyMonique Lopes da SilvaPas encore d'évaluation
- NCERT BookDocument10 pagesNCERT Bookkaushikray06Pas encore d'évaluation
- 2021 Issue 3 IPPTA Article 01Document3 pages2021 Issue 3 IPPTA Article 01jasvinder kumarPas encore d'évaluation
- 9th-Cell Coloring - ProkaryoteDocument2 pages9th-Cell Coloring - ProkaryoteMaritza ZapataPas encore d'évaluation
- MOTILITYDocument3 pagesMOTILITYPersonnel LaboratoryPas encore d'évaluation
- Urine Preservatives - SLUDocument2 pagesUrine Preservatives - SLUShana Flame Haze0% (1)
- JenicaDocument9 pagesJenicaChian-xhian LandichoPas encore d'évaluation
- Final Istb 2016Document192 pagesFinal Istb 2016yudhaputraPas encore d'évaluation
- Flashcards - 1b Variety of Living Organisms - Edexcel Biology IGCSEDocument23 pagesFlashcards - 1b Variety of Living Organisms - Edexcel Biology IGCSEsohaila ibrahimPas encore d'évaluation
- International Journal of Medical MicrobiologyDocument10 pagesInternational Journal of Medical MicrobiologyArthur Zanetti Nunes FernandesPas encore d'évaluation
- Anexa CORECTA UbisoftDocument19 pagesAnexa CORECTA UbisoftClaudia DumitriuPas encore d'évaluation
- Bacterial ReproductionDocument12 pagesBacterial Reproductionchann.maahiPas encore d'évaluation
- Tools For Systematic Study of BacteriaDocument33 pagesTools For Systematic Study of Bacteriaanjana josephPas encore d'évaluation
- Vahling-Armstrong Et Al-2016-Plant PathologyDocument9 pagesVahling-Armstrong Et Al-2016-Plant PathologyJhon ReyesPas encore d'évaluation
- Colilert - 18 E-Coli Detection ManualDocument8 pagesColilert - 18 E-Coli Detection Manuallgunterc7202Pas encore d'évaluation
- Chapter 18Document10 pagesChapter 18nehallakdawalaPas encore d'évaluation
- 4 Types of Food HazardsDocument3 pages4 Types of Food HazardsDenver De CastilloPas encore d'évaluation
- Garlic and Its Antibacterial PropertiesDocument29 pagesGarlic and Its Antibacterial PropertiesLikhith Vardhan SRPas encore d'évaluation
- Infectious DiseaseDocument151 pagesInfectious Diseasebolt boltPas encore d'évaluation
- Annotated BibliographyDocument2 pagesAnnotated BibliographyKevin JohnsenPas encore d'évaluation
- Kondisi Pencemaran Lingkungan Berdasarkan Parameter Mikrobiologis Di Sekitar Muara Sungai Cimandiri, Teluk Pelabuhan Ratu, Jawa BaratDocument6 pagesKondisi Pencemaran Lingkungan Berdasarkan Parameter Mikrobiologis Di Sekitar Muara Sungai Cimandiri, Teluk Pelabuhan Ratu, Jawa BaratNurulPas encore d'évaluation
- Natural Antimicrobial and Bioactive Compounds From Ludwigia Parviflora RoxbDocument6 pagesNatural Antimicrobial and Bioactive Compounds From Ludwigia Parviflora Roxbnguyen ba trungPas encore d'évaluation
- Microbiology Chapter 1 2Document69 pagesMicrobiology Chapter 1 2joshPas encore d'évaluation
- FHH Forest PathologyDocument10 pagesFHH Forest PathologyMahiMehtabPas encore d'évaluation
- Handcare Type1Document2 pagesHandcare Type1Habib BerishaPas encore d'évaluation