Académique Documents
Professionnel Documents
Culture Documents
Traumatic Sex
Transféré par
Fitri Nur Dini0 évaluation0% ont trouvé ce document utile (0 vote)
86 vues2 pagesTraumatic Sex
Titre original
11. Traumatic Sex
Copyright
© © All Rights Reserved
Formats disponibles
PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentTraumatic Sex
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
86 vues2 pagesTraumatic Sex
Transféré par
Fitri Nur DiniTraumatic Sex
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 2
Case Report
Traumatic sex with vulval haematoma formation: case report and review of
literature
Ngatia JW
Consultant Obstetrician/ Abstract later, she noticed a painful vulval swelling.
The swelling progressively increased in
Gynecologist, Lecturer The rich vascular supply to the vulva size for about 2 hours and subsequently,
Kenyatta University places it at risk for bleeding from trauma. she noticed per vaginal bleeding. She
P.O. Box 43844-00100, Vulval haematomas are the most common was changing approximately 1 pad every
Nairobi, Kenya. Email: sequelae. In adult women, the labia 2 hours. She had been managed for
ngatia_j@yahoo.com majora are comprised of large fat pads, pulmonary tuberculosis in 2013.
which act to protect the vulva against On examination, she was in pain and
injury. In contrast, children lack well- was walking with a waddling gait. She
developed fat pads in this area and often was not pale and the blood pressure was
engage in play activities predisposing normal. She had no lymphadenopathy.
them to vulval trauma; thus, they are She had very tender left vulval swelling
more likely to sustain vulval injuries approximately 7x4cm (Figure 1). There
than adults eg “Straddle injuries” [1-4]. was a bleeding site on the surface of the
The case presented was of traumatic sex swelling. The impression was vulval
with vulval haemorhage and haematoma haematoma. Her haemogram, urea and
formation. It was successfully managed electrolytes, urinalysis, random blood
by surgical evacuation, ligation of the sugar were normal. HIV test, VDRL and
bleeding sites, and use of antibiotics and pregnancy tests were negative.
analgesics. She was prepared for operation.
Under epidural anaesthesia, vulvo-
Key words: Coitus, Vulval haematoma, vaginal toilet was done and she was
Lacerations catheterized. An incision was made on
the mucocutaneous junction, haematoma
was drained and bleeding sites singularly
Introduction ligated using absorbable monocryl
2/0 suture. Obliteration of the cavity
Any female with a complaint of vulvo- was done using the same suture. She
vaginal pain, bleeding or swelling should was put on Betapyn, Augmentin and
undergo a careful examination to look for Clindamycin (Dalacin C). Sitz bath was
vulval or vaginal trauma or laceration. done twice daily. She was discharged
Patients may not be forthcoming with on 1st post-operative day. Subsequent
details of the events that caused the follow-up revealed complete recovery.
trauma. Therefore, identifying those at
risk is a crucial step in management. The
possibility of sexual abuse or assault must
always be considered. A case of a young
lady who had “quick” coitus on her way
home with subsequent vulval haematoma
is presented.
Case Report
On 13th September 2014, a 19 year old
para 0+0 single lady presented at St
Francis Community Hospital at Nairobi
with vulval pain, swelling and bleeding
for 8 hours. On her way home, she had
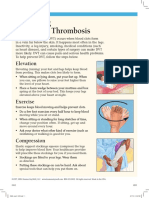
passed through her boyfriend’s house and Figure 1: Left vulval haematoma and
had coitus for a few minutes. One hour associated blood clots in the vulva
104 East and Central Africa Medical Journal 2015; 2: 104-105
Discussion analgesics. Sitz bath helped to reduce the discomfort and
accelerated the healing process.
The highly vascular nature of the vulva places it at risk
for bleeding from trauma. Haematoma of the vulva is a Conclusion and Recommendation
possible sequelae [5]. In adult women, the labia majora
are comprised of large fat pads, which act to protect the A case of vulval haematoma due to traumatic sex was
vulva against injury. Among the adult women, obstetric presented as one of the injuries that may be a consequence
injuries are the commonest causes of vulval haematomas. of violent coitus (consensual and non-consensual). In
In contrast, children lack well-developed fat pads in this view of rich vascular supply to the perineum, patients
area and often engage in play activities predisposing them should be encouraged to seek medical attention when
to vulvar trauma; thus, they are more likely to sustain they sustain vulval injuries. It is recommended that there
vulval injuries than adults eg Straddle injuries [3,4]. should be modest approach to sexual intercourse with
In most cases direct vulvo-vaginal trauma is caused sufficient foreplay to encourage lubrication of the female
by direct blunt trauma to an area containing a rich vascular external genitalia. This may not be accomplished when
net-work. Such injuries usually result from coitus. either of the parties is in extreme hurry.
Suggested predisposing factors that may result in such
injuries include virginity, insertion of foreign bodies, self Acknowledgement
mutilation, disproportion of male and female genitalia,
atrophic vagina in postmenopausal women, congenital To the administration of St Francis Community Hospital.
abnormalities stenosis and scarring of the vagina because Written consent was obtained from the patient.
of previous surgery, or pelvic radiation therapy. Other
factors include rough and violent thrusting of the penis References
during intercourse (consensual and non-consensual).
This traumatic sex may result from hastily performed 1. Ian SCJ and Alan O. Non-obstetric vaginal trauma.
coitus [1,2,3,6]. This case is presented to highlight one of Open J Obstet Gynecol. 2013; (3): 21-23.(http://
the injuries that may be a consequence of such. www.script.org/journal/ojog)
Non-obstetric injuries of the female genital tract 2. Singhal V, Bhargava S, Saxena N. et al. Case Report
constitute up to 0.8% of all gynaecologic admissions. – Traumatic vulval injury : A rare case. Intern J
Approximately 40% of such admissions are due to Gynae Plastic Surg. 2014; 4 (1): 30-32.
coital injuries [2,7]. Non-obstetric vulva/vaginal trauma 3. Odawa FXO. Post-coital vulval haematoma: Case
can span a continuum of severity from minor trauma report and review of literature J Obstet Gynaecol
resulting from normal sexual intercourse to major East Central Afr. 2012; 24(2): 55-56.
vaginal lacerations. The true incidences of such injuries 4. Propst AM and Thorp JM Jr. Traumatic vulvar
are difficult to ascertain, especially because the nature of hematomas: conservative versus surgical
vulvo-vaginal injury usually remains undisclosed (8). management. South Med J. 1998; 91(2):144-146.
Diagnosis is usually not a problem when there is 5. Dash S, Verghese J and Nizami DJ. Severe
proper co-relation with the history, but sometimes, the haematoma of the vulva: A report of two cases and a
vulval swelling could be mistaken for a Bartholin’s clinical review. Kathmandu University Med J. 2006;
abscess [5]. In our case, the diagnosis was presumed 4(2): 228-231.
from the clinical picture and confirmed at operation. 6. Jeyalakshmi P. Case report: Postcoital bleeding -
Patients with large haematomas require operative an unusual cause for abdominal apoplexy. J Obstet
management. Incision is made on the inner aspect of the Gynecol India. 2009; 59(4): 360-361.
vulva. Evacuation of the clots and separate ligation of the 7. Rabinerson D, Fradin Z, Zeidman A. et al. Vulvar
individual bleeding points are done. Then the dead space hematoma after cunnilingus in a teenager with
is obliterated with absorbable suture. Small haematomas essential thrombocythemia: a case report. J Reprod
with no active bleeding are managed conservatively with Med. 2007; 52(5):458-459.
ice packs, bed rest and analgesics [1,3-5). In our case, 8. Marvin MS, Mersedeh K and Pedram I. Non obstetric
ligation of the bleeders and obliteration of the cavity lacerations of the vagina. J Amer Osteopath Ass.
was done. In view of the possible infection which could 2006; 106(5): 271-273.
have occurred, the patient was put on antibiotics and
105 East and Central Africa Medical Journal 2015; 2: 104-105
Vous aimerez peut-être aussi
- The Change-Up: Acted By: Ryan Reynolds: Jason BatemanDocument3 pagesThe Change-Up: Acted By: Ryan Reynolds: Jason BatemanYazan AssadPas encore d'évaluation
- @UrFRENZ by Jeff PhillipsDocument198 pages@UrFRENZ by Jeff PhillipsJimStraderPas encore d'évaluation
- Gambia DV FGC Forced Marriage Rape 2013Document28 pagesGambia DV FGC Forced Marriage Rape 2013Elisa Perez-SelskyPas encore d'évaluation
- B Inggris PDFDocument12 pagesB Inggris PDFNisa Amelia Putri PutriPas encore d'évaluation
- Noida Escorts Neha Babe Independent Cal GirlsDocument6 pagesNoida Escorts Neha Babe Independent Cal GirlsAnamika SinghPas encore d'évaluation
- Mycelia Creative PassportDocument17 pagesMycelia Creative PassportJordynCoatsPas encore d'évaluation
- ADDYs 2020 Digital Show Entry GalleryDocument369 pagesADDYs 2020 Digital Show Entry GalleryAaron LattanzioPas encore d'évaluation
- Consensual Sex Injury Revised 3 - 12Document5 pagesConsensual Sex Injury Revised 3 - 12JMarkowitzPas encore d'évaluation
- TramplingDocument2 pagesTramplingMoshe RubinPas encore d'évaluation
- History of A PhantasyDocument49 pagesHistory of A Phantasyjurbina1844Pas encore d'évaluation
- Useful Wild Plants-9Document29 pagesUseful Wild Plants-9hassan_maatoukPas encore d'évaluation
- MMPI-2 Correlates of Sadomasochism in A Sexual Addiction Sample: Contrasting and Men and WomenDocument28 pagesMMPI-2 Correlates of Sadomasochism in A Sexual Addiction Sample: Contrasting and Men and WomenMichael Tavera OsorioPas encore d'évaluation
- Bizarre WorldDocument22 pagesBizarre Worldrich_danaPas encore d'évaluation
- Treatment of Orgasmic DysfunctionDocument10 pagesTreatment of Orgasmic DysfunctionRicardo GarciaPas encore d'évaluation
- Irish - Potato Production in The West Coast Region of The GambiaDocument7 pagesIrish - Potato Production in The West Coast Region of The GambiaTI Journals Publishing100% (1)
- Afterthoughts: Naked AmbitionDocument1 pageAfterthoughts: Naked AmbitionKathryn WagnerPas encore d'évaluation
- Passion, Politics and Politically Incorrect Sex - MA - Thesis - AnnaRobinsonDocument186 pagesPassion, Politics and Politically Incorrect Sex - MA - Thesis - AnnaRobinsonandrew_culpPas encore d'évaluation
- Sex Work and Prostitution For WebDocument3 pagesSex Work and Prostitution For WebArmida Talaugon100% (1)
- UrolagniaDocument4 pagesUrolagniaAzrul Yahaya100% (1)
- Sex - A Buddhist PerspectiveDocument6 pagesSex - A Buddhist PerspectiveDr Edo ShoninPas encore d'évaluation
- Human Sexuality Chapter 15 NotesDocument7 pagesHuman Sexuality Chapter 15 NotesCandice ChengPas encore d'évaluation
- Ko-Lin Chin, James O. Finckenauer - Selling Sex Overseas - Chinese Women and The Realities of Prostitution and Global Sex Trafficking-New York University Press (2016) PDFDocument324 pagesKo-Lin Chin, James O. Finckenauer - Selling Sex Overseas - Chinese Women and The Realities of Prostitution and Global Sex Trafficking-New York University Press (2016) PDFFaizJamilPas encore d'évaluation
- Sexual SelfDocument24 pagesSexual SelfLady of the Light100% (1)
- EurydiceDocument8 pagesEurydiceMeghan Kathleen Van DynePas encore d'évaluation
- Boys and Men Healing Documentary/the Healing Years Documentary ReviewsDocument2 pagesBoys and Men Healing Documentary/the Healing Years Documentary ReviewsbigvoicepicturesPas encore d'évaluation
- 7 LiesDocument42 pages7 LiesMadhav KushwahaPas encore d'évaluation
- Consensual Sadomasochistic Sex (BDSM) : The Roots, The Risks, and The Distinctions Between BDSM and ViolenceDocument9 pagesConsensual Sadomasochistic Sex (BDSM) : The Roots, The Risks, and The Distinctions Between BDSM and ViolenceSmile and LovePas encore d'évaluation
- Influence of Personality Type On Marital and Sexua PDFDocument11 pagesInfluence of Personality Type On Marital and Sexua PDFPeter MissolePas encore d'évaluation
- The Visible VaginaDocument2 pagesThe Visible VaginaHagit Shapir ShafirPas encore d'évaluation
- BOUND TOGETHER - Campbell - Dissertation - 2012 PDFDocument453 pagesBOUND TOGETHER - Campbell - Dissertation - 2012 PDFAllBear FkPas encore d'évaluation
- America MasochismDocument23 pagesAmerica MasochismJESUS AYLLONPas encore d'évaluation
- English Duong - BerkeleyDocument141 pagesEnglish Duong - BerkeleyPyae Sone KyawPas encore d'évaluation
- ABC's "20/20" Interview With Dorothy Hayden, Sex Addiction SpecialistDocument4 pagesABC's "20/20" Interview With Dorothy Hayden, Sex Addiction SpecialistDorothy HaydenPas encore d'évaluation
- Safer Oral Sex BrochureDocument2 pagesSafer Oral Sex BrochureAugustin SekhemAset MureseanuPas encore d'évaluation
- Power and Control Wheel-EnglishDocument1 pagePower and Control Wheel-EnglishRebecca RichardsonPas encore d'évaluation
- Veiled Pornography: Patterns and Consumption of Pornography in The Middle EastDocument10 pagesVeiled Pornography: Patterns and Consumption of Pornography in The Middle EastDr Steven McDermott100% (2)
- MoviesDocument110 pagesMoviesSaki_KinomotoPas encore d'évaluation
- Erotica & Porn EssayDocument15 pagesErotica & Porn EssayvanityinsanityPas encore d'évaluation
- Under The Skin Black Swan PDFDocument11 pagesUnder The Skin Black Swan PDFDig ItyPas encore d'évaluation
- Benefits of Sexting Among Long-Term Monogamous Romantic PartnersDocument10 pagesBenefits of Sexting Among Long-Term Monogamous Romantic PartnersJulia Araya DavilaPas encore d'évaluation
- Simon Z. Weismantel From Sadomasochism To BDSM - Rethinking PDFDocument95 pagesSimon Z. Weismantel From Sadomasochism To BDSM - Rethinking PDFJohn C. YoungPas encore d'évaluation
- Corrigan T - The Elements of Editing, Pp. 155-159Document5 pagesCorrigan T - The Elements of Editing, Pp. 155-159Pasquale CicchettiPas encore d'évaluation
- Preecha's Technique MtF. (The Pioneer in Sex Reassignment Surgery, Thailand) - 1Document7 pagesPreecha's Technique MtF. (The Pioneer in Sex Reassignment Surgery, Thailand) - 1VeroniquePas encore d'évaluation
- Global Sex Sexuality and Sexual Practices Around The WorldDocument12 pagesGlobal Sex Sexuality and Sexual Practices Around The WorldCher LimPas encore d'évaluation
- Where Are The Men? EssayDocument20 pagesWhere Are The Men? Essayjpkirch92Pas encore d'évaluation
- The Stony Brook Press - Volume 33, Issue 12Document44 pagesThe Stony Brook Press - Volume 33, Issue 12The Stony Brook PressPas encore d'évaluation
- Guide To Filming Live Theater: Archival Filming Guidelines and Lessons Learned From The Ctda ProjectDocument46 pagesGuide To Filming Live Theater: Archival Filming Guidelines and Lessons Learned From The Ctda ProjectMario PinedoPas encore d'évaluation
- Human Sexual ActivityDocument11 pagesHuman Sexual ActivitynathanPas encore d'évaluation
- Story Board SampleDocument16 pagesStory Board SampleRiddhi JainPas encore d'évaluation
- Psychology & Sexuality: Click For UpdatesDocument19 pagesPsychology & Sexuality: Click For UpdatesAgustín LiartePas encore d'évaluation
- OBGYN0622 Core GynecologyDocument4 pagesOBGYN0622 Core GynecologyAlex Bernales MartínezPas encore d'évaluation
- A Reading On HEMATOMA: Delivery Room Nursing RotationDocument7 pagesA Reading On HEMATOMA: Delivery Room Nursing RotationJulianePas encore d'évaluation
- Management of Penile Fracture: Ahmad M. El-Taher, Hassan A. Aboul-Ella, Mohamed A. Sayed, and Atef A. GaafarDocument3 pagesManagement of Penile Fracture: Ahmad M. El-Taher, Hassan A. Aboul-Ella, Mohamed A. Sayed, and Atef A. GaafarTeja LaksanaPas encore d'évaluation
- Vesicovaginal Fistula: Diagnosis and Management: Review ArticleDocument6 pagesVesicovaginal Fistula: Diagnosis and Management: Review ArticleDion PratamaPas encore d'évaluation
- The Management of Genitourinary Fistula in The Third MillenniumDocument9 pagesThe Management of Genitourinary Fistula in The Third MillenniumDikiArmaDuhaAlaydrusPas encore d'évaluation
- Rectovaginal Fistulae: Bidhan Das, MD Michael Snyder, MDDocument7 pagesRectovaginal Fistulae: Bidhan Das, MD Michael Snyder, MDNovaPas encore d'évaluation
- Consensual Coital Lacerations A Case SeriesDocument2 pagesConsensual Coital Lacerations A Case SeriesLara PachecoPas encore d'évaluation
- A Rare Case of Abnormal Uterine Bleeding Caused by Cavernous Hemangioma: A Case ReportDocument3 pagesA Rare Case of Abnormal Uterine Bleeding Caused by Cavernous Hemangioma: A Case ReportprincessismaPas encore d'évaluation
- 1 s2.0 S2214911220300904 MainDocument3 pages1 s2.0 S2214911220300904 MainSandra ArellanoPas encore d'évaluation
- Obesitas: Dr. Nanang Miftah F, SPPDDocument26 pagesObesitas: Dr. Nanang Miftah F, SPPDFitri Nur DiniPas encore d'évaluation
- Lewi DizzinessDocument5 pagesLewi DizzinessFitri Nur DiniPas encore d'évaluation
- Laporan Pagi Anestesi Cito 09-10 April 2017Document1 pageLaporan Pagi Anestesi Cito 09-10 April 2017Fitri Nur DiniPas encore d'évaluation
- DR Yudianta - DAAAA LBP MULTIMODAL TREATMENT BJMSNDocument38 pagesDR Yudianta - DAAAA LBP MULTIMODAL TREATMENT BJMSNFitri Nur DiniPas encore d'évaluation
- Hormon Parathyroid: Dr. Nanang Miftah F, SPPDDocument13 pagesHormon Parathyroid: Dr. Nanang Miftah F, SPPDFitri Nur DiniPas encore d'évaluation
- Opioid-Presentasi - Banjar 2016Document87 pagesOpioid-Presentasi - Banjar 2016Fitri Nur DiniPas encore d'évaluation
- Associated Risk Factors of Placenta Previa A Matched Case Control StudyDocument4 pagesAssociated Risk Factors of Placenta Previa A Matched Case Control StudyFitri Nur DiniPas encore d'évaluation
- Phys ResDocument18 pagesPhys ResFitri Nur DiniPas encore d'évaluation
- 6th Central Pay Commission Salary CalculatorDocument15 pages6th Central Pay Commission Salary Calculatorrakhonde100% (436)
- Review Article: Epidemiology, Etiology, Diagnosis, and Management of Placenta AccretaDocument8 pagesReview Article: Epidemiology, Etiology, Diagnosis, and Management of Placenta AccretaFitri Nur DiniPas encore d'évaluation
- Seminar Nasional Sains & Teknologi V Lembaga Penelitian Universitas Lampung 19-20 November 2013Document9 pagesSeminar Nasional Sains & Teknologi V Lembaga Penelitian Universitas Lampung 19-20 November 2013Ariz VmPas encore d'évaluation
- Daftar Pustaka Bells PalsyDocument2 pagesDaftar Pustaka Bells PalsyFitri Nur DiniPas encore d'évaluation
- Temporal Relationship Between Lens Protein Oxidation and Cataract Development in Streptozotocin-Induced Diabetic RatsDocument6 pagesTemporal Relationship Between Lens Protein Oxidation and Cataract Development in Streptozotocin-Induced Diabetic RatsFitri Nur DiniPas encore d'évaluation
- Hypoglycemia in The NewbornDocument7 pagesHypoglycemia in The NewbornFitri Nur DiniPas encore d'évaluation
- High-Flux Versus Low-Flux Membranes For End-Stage Kidney DiseaseDocument1 pageHigh-Flux Versus Low-Flux Membranes For End-Stage Kidney DiseaseFitri Nur DiniPas encore d'évaluation
- Di PDF 2. 3. Di PDF 4. 5. 6. 7. - Ini Emang LinkDocument1 pageDi PDF 2. 3. Di PDF 4. 5. 6. 7. - Ini Emang LinkFitri Nur DiniPas encore d'évaluation
- D013531316 PDFDocument4 pagesD013531316 PDFFitri Nur DiniPas encore d'évaluation
- Dr. Isa - TuberculosisDocument12 pagesDr. Isa - TuberculosisFitri Nur DiniPas encore d'évaluation
- Trali EnglishDocument5 pagesTrali EnglishFitri Nur DiniPas encore d'évaluation
- Trali EnglishDocument5 pagesTrali EnglishFitri Nur DiniPas encore d'évaluation
- CHT Hfa Boys Z 2 5Document1 pageCHT Hfa Boys Z 2 5Sunu RachmatPas encore d'évaluation
- Daftar Pustaka BCB BMK BBLC Ikterus NeonatorumDocument3 pagesDaftar Pustaka BCB BMK BBLC Ikterus NeonatorumFitri Nur DiniPas encore d'évaluation
- Etiology, Diagnosis, and Management of Facial Palsy: 2000 Patients at A Facial Nerve CenterDocument11 pagesEtiology, Diagnosis, and Management of Facial Palsy: 2000 Patients at A Facial Nerve CenterLastaArshintaPas encore d'évaluation
- Transfusion-Related Acute Lung Injury (TRALI) - Blood Transfusion ComplicationDocument4 pagesTransfusion-Related Acute Lung Injury (TRALI) - Blood Transfusion ComplicationFitri Nur DiniPas encore d'évaluation
- Daftar Pustaka HD Pada AnakDocument3 pagesDaftar Pustaka HD Pada AnakFitri Nur DiniPas encore d'évaluation
- Pattern of Non Obstetrics Lower Genital Tract Trauma From Western PDFDocument8 pagesPattern of Non Obstetrics Lower Genital Tract Trauma From Western PDFFitri Nur DiniPas encore d'évaluation
- Daftar Pustaka - EndocarditisDocument4 pagesDaftar Pustaka - EndocarditisFitri Nur DiniPas encore d'évaluation
- Traumatic SexDocument2 pagesTraumatic SexFitri Nur DiniPas encore d'évaluation
- Zat Kimia Yang Digunakan Untuk Merangsang Daya Seksual)Document3 pagesZat Kimia Yang Digunakan Untuk Merangsang Daya Seksual)Fitri Nur DiniPas encore d'évaluation
- Circ Coital Injuries MANUSCRIPT ONLY J Urology 2-5-10 SM DoneDocument16 pagesCirc Coital Injuries MANUSCRIPT ONLY J Urology 2-5-10 SM DoneFitri Nur DiniPas encore d'évaluation
- Framingham Category Risk ScoreDocument1 pageFramingham Category Risk Scoresyaiful rinantoPas encore d'évaluation
- Oral Neoplasma IDocument31 pagesOral Neoplasma INandika 'ndek' DewaraPas encore d'évaluation
- Central Neuraxial Blockade: Major ComplicationsDocument26 pagesCentral Neuraxial Blockade: Major ComplicationsGareth SymonsPas encore d'évaluation
- Preventing Deep Vein Thrombosis: ElevationDocument2 pagesPreventing Deep Vein Thrombosis: ElevationTeuku Ilham AkbarPas encore d'évaluation
- Immediate Care in PostnatalDocument12 pagesImmediate Care in Postnatalvarshasharma05Pas encore d'évaluation
- Poisonplants 140917075435 Phpapp02 PDFDocument42 pagesPoisonplants 140917075435 Phpapp02 PDFNareshPas encore d'évaluation
- EwingDocument10 pagesEwingMd Ahsanuzzaman PinkuPas encore d'évaluation
- Paclitaxel With Dose Dense EC Adjuvant or Neo-Adjuvant Protocol V1.0Document7 pagesPaclitaxel With Dose Dense EC Adjuvant or Neo-Adjuvant Protocol V1.0smokkerPas encore d'évaluation
- J.B. Family Case Presentation Group 1Document67 pagesJ.B. Family Case Presentation Group 1Jeno Luis AcubPas encore d'évaluation
- S974 Abstract Book ESTRO 2022: Variable N (%)Document1 pageS974 Abstract Book ESTRO 2022: Variable N (%)andresPas encore d'évaluation
- Delirium: Continuum Lifelong Learning Neurol 2010 16 (2) :120-134Document15 pagesDelirium: Continuum Lifelong Learning Neurol 2010 16 (2) :120-134Maria Isabel Montañez RestrepoPas encore d'évaluation
- Biperiden HCLDocument2 pagesBiperiden HCLivy_tan_6Pas encore d'évaluation
- Pathognomonic SignsDocument4 pagesPathognomonic SignsJoan Rose Rendon-Hung50% (2)
- Case Conference: Presenter: Dr. Sandesh Hegde Moderator: DR Neela ShenoyDocument51 pagesCase Conference: Presenter: Dr. Sandesh Hegde Moderator: DR Neela ShenoySandesh HegdePas encore d'évaluation
- Counseling Depressed ElderlyDocument4 pagesCounseling Depressed ElderlyLara Sabunod - PalloPas encore d'évaluation
- Example of Completed Blood Safety Indicators FormDocument9 pagesExample of Completed Blood Safety Indicators FormEmhemed Amer TabibPas encore d'évaluation
- Chapter 12 - Drugs Associated With Pregnancy, Labor and Delivery, and LactationDocument4 pagesChapter 12 - Drugs Associated With Pregnancy, Labor and Delivery, and LactationmysPas encore d'évaluation
- Nclex AobyDocument7 pagesNclex Aobyvienny kayePas encore d'évaluation
- Management of Pancreatic Fistulas: Surgical Clinics of North America June 2013Document22 pagesManagement of Pancreatic Fistulas: Surgical Clinics of North America June 2013Shravani ShagapuramPas encore d'évaluation
- Comprehension Activity Story 1: (One Hour Later)Document2 pagesComprehension Activity Story 1: (One Hour Later)mihai cristinaPas encore d'évaluation
- Sleep PowerpointDocument10 pagesSleep PowerpointTravisHarringtonPas encore d'évaluation
- Causes and Risk Factors For Attention-Deficit Hyperactivity DisorderDocument8 pagesCauses and Risk Factors For Attention-Deficit Hyperactivity DisorderFranthesa LayloPas encore d'évaluation
- Managing Feline Diabetes: Current Perspectives: Veterinary Medicine: Research and Reports DoveDocument10 pagesManaging Feline Diabetes: Current Perspectives: Veterinary Medicine: Research and Reports Doveabazanhasan6705Pas encore d'évaluation
- PEDIS Classification in Diabetic Foot Ulcers Patients PDFDocument5 pagesPEDIS Classification in Diabetic Foot Ulcers Patients PDFDeo ValendraPas encore d'évaluation
- Final Ugib Sec To BpudDocument17 pagesFinal Ugib Sec To BpudBaby Kate BONGCARASPas encore d'évaluation
- Prado, Catherine BSN IIB (Activity 2 Term Paper)Document2 pagesPrado, Catherine BSN IIB (Activity 2 Term Paper)Catherine PradoPas encore d'évaluation
- Heirs of Deauna vs. Fil-Star Maritime Corp.Document31 pagesHeirs of Deauna vs. Fil-Star Maritime Corp.Coleen ReyesPas encore d'évaluation
- Icd 10Document401 pagesIcd 10Dewi MajidahPas encore d'évaluation
- Oncocytoma of The Nasal CavityDocument2 pagesOncocytoma of The Nasal CavityInes Camilla PutriPas encore d'évaluation
- Usos de Bite Blocks PDFDocument25 pagesUsos de Bite Blocks PDFNatasha RiveraPas encore d'évaluation
- The Obesity Code: Unlocking the Secrets of Weight LossD'EverandThe Obesity Code: Unlocking the Secrets of Weight LossÉvaluation : 4 sur 5 étoiles4/5 (6)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsD'EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsPas encore d'évaluation
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeD'EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeÉvaluation : 2 sur 5 étoiles2/5 (1)
- The Age of Magical Overthinking: Notes on Modern IrrationalityD'EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityÉvaluation : 4 sur 5 étoiles4/5 (24)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaD'EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisD'EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisÉvaluation : 4.5 sur 5 étoiles4.5/5 (42)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedD'EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedÉvaluation : 5 sur 5 étoiles5/5 (80)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDD'EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDÉvaluation : 5 sur 5 étoiles5/5 (1)
- Self-Care for Autistic People: 100+ Ways to Recharge, De-Stress, and Unmask!D'EverandSelf-Care for Autistic People: 100+ Ways to Recharge, De-Stress, and Unmask!Évaluation : 5 sur 5 étoiles5/5 (1)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsD'EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsÉvaluation : 5 sur 5 étoiles5/5 (1)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisD'EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisÉvaluation : 4 sur 5 étoiles4/5 (1)
- The Comfort of Crows: A Backyard YearD'EverandThe Comfort of Crows: A Backyard YearÉvaluation : 4.5 sur 5 étoiles4.5/5 (23)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.D'EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Évaluation : 4.5 sur 5 étoiles4.5/5 (110)
- Gut: the new and revised Sunday Times bestsellerD'EverandGut: the new and revised Sunday Times bestsellerÉvaluation : 4 sur 5 étoiles4/5 (392)
- Why We Die: The New Science of Aging and the Quest for ImmortalityD'EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityÉvaluation : 4 sur 5 étoiles4/5 (3)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsD'EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsÉvaluation : 4.5 sur 5 étoiles4.5/5 (169)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryD'EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryÉvaluation : 4 sur 5 étoiles4/5 (44)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessD'EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessÉvaluation : 4.5 sur 5 étoiles4.5/5 (328)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsD'EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsÉvaluation : 3.5 sur 5 étoiles3.5/5 (3)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisD'EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisÉvaluation : 3.5 sur 5 étoiles3.5/5 (2)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningD'EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningÉvaluation : 4 sur 5 étoiles4/5 (3)
- Gut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)D'EverandGut: The Inside Story of Our Body's Most Underrated Organ (Revised Edition)Évaluation : 4 sur 5 étoiles4/5 (378)
- To Explain the World: The Discovery of Modern ScienceD'EverandTo Explain the World: The Discovery of Modern ScienceÉvaluation : 3.5 sur 5 étoiles3.5/5 (51)
- The Marshmallow Test: Mastering Self-ControlD'EverandThe Marshmallow Test: Mastering Self-ControlÉvaluation : 4.5 sur 5 étoiles4.5/5 (58)