Académique Documents
Professionnel Documents
Culture Documents
PrEP Fact Sheet Final PDF
Transféré par
Shiv ChopraTitre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
PrEP Fact Sheet Final PDF
Transféré par
Shiv ChopraDroits d'auteur :
Formats disponibles
Pre-exposure Prophylaxis (PrEP) May 2014
for HIV Prevention
Fast Facts
• Pre-exposure prophylaxis, or PrEP, is a way to help prevent HIV by taking a pill every day.
• People who are at substantial risk for HIV should talk to their doctor about PrEP.
• PrEP must be taken every day to be most effective.
Pre-exposure prophylaxis, or PrEP, is a way for people who do not have HIV to help prevent HIV infection by taking a pill every day.
The pill contains two medicines that are also used, in combination with other medicines, to treat HIV. When someone is exposed
to HIV through sex or injection drug use, PrEP can help stop the virus from establishing a permanent infection.
When used consistently, PrEP has been shown to greatly reduce the risk of HIV infection in people who are at substantial risk.
PrEP is much less effective when it is not taken consistently.
PrEP is a powerful HIV prevention tool, and can be combined with condoms and other prevention methods to provide even
greater protection than when used alone. People who use PrEP must commit to taking the drug daily and seeing their health
care provider every 3 months for HIV testing and other follow-up.
PrEP Medicines
Most PrEP clinical trials have tested a combination of two antiretroviral drugs, tenofovir disoproxil fumarate (also called TDF,
or tenofovir) and emtricitabine (also called FTC), taken in a single pill daily for HIV prevention. This combination pill (brand name
Truvada) was approved by the US Food and Drug Administration (FDA) for use as an HIV treatment in 2004, and was approved
as PrEP in July 2012. Some clinical studies have also evaluated the use of tenofovir on its own as a preventive drug, but this drug
alone is not FDA-approved for PrEP.
Research Supporting PrEP Use
On May 14, 2014, the US Public Health Service released the first comprehensive clinical practice guidelines for PrEP
(www.cdc.gov/hiv/pdf/guidelines/PrEPguidelines2014.pdf ). This follows the earlier publication of brief interim guidelines that
were based on findings from several large national and international clinical trials. These trials evaluated PrEP among gay and
bisexual men, heterosexual men and women, and injection drug users. All participants in these trials received pills containing
either PrEP or placebo, along with intensive counseling on safe-sex behavior, regular testing for sexually transmitted diseases
(STDs), and a regular supply of condoms.
In all of these studies, the risk of getting HIV infection was lower—up to 92% lower—for participants who took the medicines
consistently than for those who did not take the medicines. (See our PrEP web page at www.cdc.gov/hiv/prevention/research/prep/
for a brief description of the clinical trials, with links to the published studies.)
Guidelines for PrEP Use
The new federal guidelines for health care providers recommend that PrEP be considered for people who are HIV-negative and
at substantial risk for HIV infection.
For sexual transmission, this includes anyone who is in an ongoing relationship with an HIV-positive partner. It also includes
anyone who 1) is not in a mutually monogamous relationship with a partner who recently tested HIV-negative, and 2) is a
• gay or bisexual man who has had anal sex without a condom or been diagnosed with an STD in the past 6 months; or
• heterosexual man or woman who does not regularly use condoms during sex with partners of unknown HIV status who are
at substantial risk of HIV infection (e.g., people who inject drugs or have bisexual male partners).
For people who inject drugs, this includes those who have injected illicit drugs in past 6 months and who have shared injection
equipment or been in drug treatment for injection drug use in the past 6 months.
Health care providers should also discuss PrEP with heterosexual couples in which one partner is HIV-positive and the other
is HIV-negative as one of several options to protect the partner who is HIV-negative during conception and pregnancy.
For a summary of clinical indications and treatment recommendations for PrEP, see the Table on the
next page.
National Center for HIV/AIDS, Viral Hepatitis, STD, and TB Prevention
Division of HIV/AIDS Prevention
Summary of Guidance for PrEP Use
Men Who Have Sex With Men Heterosexual Women and Men Injection Drug Users
Detecting substantial risk • Sexual partner with HIV • Sexual partner with HIV • HIV-positive injecting
of acquiring HIV infection: • Recent bacterial STD • Recent bacterial STD partner
• High number of sex • High number of sex • Sharing injection
partners partners equipment
• History of inconsistent or • History of inconsistent or • Recent drug treatment
no condom use no condom use (but currently injecting)
• Commercial sex work • Commercial sex work
• Lives in high-prevalence
area or network
Clinically eligible: • Documented negative HIV test before prescribing PrEP
• No signs/symptoms of acute HIV infection
• Normal renal function, no contraindicated medications
• Documented hepatitis B virus infection and vaccination status
Prescription Daily, continuing, oral doeses of TDF/FTC (Truvada), ≤90 day supply
Other services: • Follow-up visits at least every 3 months to provide:
• HIV test, medication adherence counseling, behavioral risk reduction support,
side effect assessment, STD symptom assessment
• At 3 months and every 6 months after, assess renal function
• Every 6 months test for bacterial STDs
• Do oral/rectal STD testing • Assess pregnancy intent • Access to clean needles/
• Pregnancy test every 3 syringes and drug
months treatment services
Source: US Public Health Service. Preexposure prophylaxis for the prevention of HIV infection in the United States —2014: a clinical practice guideline.
Because no prevention strategy for sexually active people is 100% effective, patients taking PrEP are encouraged to use other
effective prevention strategies to maximally reduce their risk, including:
• Using condoms consistently and correctly.
• Getting HIV testing with partners.
• Choosing less risky sexual behaviors, such as oral sex.
• For people who inject drugs, getting into drug treatment programs and using sterile equipment.
The more prevention options patients choose, the greater their protection. Some HIV prevention strategies, such as using
condoms, can also provide protection against other STDs, which PrEP does not prevent.
PrEP is only for people who are at ongoing substantial risk of HIV infection. For people who need to prevent HIV after a single
high-risk event of potential HIV exposure—such as unprotected sex, needle-sharing injection drug use, or sexual assault
—there is another option called postexposure prophylaxis, or PEP. PEP must begin within 72 hours of exposure.
See our PEP Q&A (www.cdc.gov/hiv/basics/pep.html) for more information.
Supporting PrEP Uptake
To support the new guidelines and provider’s supplement, CDC is leading efforts on multiple fronts to improve PrEP awareness
and delivery in community settings. For example, the agency is implementing a pilot study examining practical requirements,
costs, and impact of PrEP delivered at four federally qualified health centers, and will support state and local health departments
by providing webinars and program guidance on using CDC funds to support PrEP implementation.
Many other groups will also play a vital role in achieving the full promise of PrEP. Health care providers can prescribe PrEP to
those patients with indications for its use and increase awareness and uptake of PrEP for their patients who are at substantial risk.
Advocates can raise PrEP awareness in at-risk populations, and groups implementing HIV prevention efforts can integrate PrEP
education into existing programs.
Additional Resources
Resources CDC-INFO
• Basic PrEP Q&As (www.cdc.gov/hiv/basics/prep.html) 1-800-CDC-INFO (232-4636)
www.cdc.gov/info
• Clinical Practice Guidelines (www.cdc.gov/hiv/pdf/guidelines/PrEPguidelines2014.pdf ) CDC HIV Website
www.cdc.gov/hiv
• Clinical Practice Guidelines—Providers’ Supplement
CDC Act Against AIDS
(www.cdc.gov/hiv/pdf/guidelines/PrEPProviderSupplement2014.pdf ) Campaign
www.cdc.gov/actagainstaids
• Basic PEP Q&As (www.cdc.gov/hiv/basics/pep.html)
Page 2 of 2
Vous aimerez peut-être aussi
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (74)
- Mental and Emotional Health PowerpointDocument36 pagesMental and Emotional Health PowerpointYen Aduana86% (7)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- Ansi+asse+z359 13-2013Document54 pagesAnsi+asse+z359 13-2013Oscar Casso100% (1)
- N Vent Code ENDocument28 pagesN Vent Code ENGwenn LecturaPas encore d'évaluation
- Drug Study (FINAL)Document31 pagesDrug Study (FINAL)iamjenivicPas encore d'évaluation
- GOVERNMENT Leave - Form - Complete2Document2 pagesGOVERNMENT Leave - Form - Complete2Marc CaurelPas encore d'évaluation
- TUM CoursesDocument3 pagesTUM CoursesJoao N Da SilvaPas encore d'évaluation
- Clinical Efficacy of Anodized Dental Implants For Implantsupported Prostheses After Different Loading Protocols - A Systematic Review and Meta-Analysis (2021)Document20 pagesClinical Efficacy of Anodized Dental Implants For Implantsupported Prostheses After Different Loading Protocols - A Systematic Review and Meta-Analysis (2021)Andy LeePas encore d'évaluation
- Filipino Research Paper Kabanata 4Document8 pagesFilipino Research Paper Kabanata 4nynodok1pup3100% (1)
- Relationship of Chronic Disease With Psychososial Problems in Patients in Gunung Jati Hospital CirebonDocument7 pagesRelationship of Chronic Disease With Psychososial Problems in Patients in Gunung Jati Hospital CirebonSitti AuraPas encore d'évaluation
- EnSURE Touch - F&BDocument6 pagesEnSURE Touch - F&BfaradillafattaPas encore d'évaluation
- American Soc. of Addiction Medicine Naloxone StatementDocument5 pagesAmerican Soc. of Addiction Medicine Naloxone Statementwebmaster@drugpolicy.orgPas encore d'évaluation
- Your Wellness Profile: Laboratory ActivitiesDocument4 pagesYour Wellness Profile: Laboratory Activitiesdusty kawiPas encore d'évaluation
- HPMC CapsulesDocument15 pagesHPMC Capsuleskunalprabhu148Pas encore d'évaluation
- Magellan Code ChangesDocument15 pagesMagellan Code ChangesdaringdreuPas encore d'évaluation
- Government Policies and Interventions For Development in Various Sectors and Issues Arising Out of Their Design and ImplementationDocument30 pagesGovernment Policies and Interventions For Development in Various Sectors and Issues Arising Out of Their Design and ImplementationHasnu MohdPas encore d'évaluation
- Edicted PG, StanDocument69 pagesEdicted PG, StanNwakpa Stanley OgbonnayaPas encore d'évaluation
- Body Parts Lesson PlanDocument3 pagesBody Parts Lesson Planapi-372758719Pas encore d'évaluation
- Magnetis Polus AmboDocument4 pagesMagnetis Polus Amboadi.mititean1585Pas encore d'évaluation
- Chest Drains Al-WPS OfficeDocument16 pagesChest Drains Al-WPS OfficeisnainiviaPas encore d'évaluation
- Mia Deal or No Deal 2.3.7.A1Document2 pagesMia Deal or No Deal 2.3.7.A1bxnds. zay0% (1)
- Imci Drug StudyDocument4 pagesImci Drug StudyDea Sabelle CastroPas encore d'évaluation
- Id ProofDocument3 pagesId ProofSagar MittaPas encore d'évaluation
- M5D BRT Ascending, Trav & RappelingDocument83 pagesM5D BRT Ascending, Trav & RappelingFallucky Santiago100% (1)
- A. Differential Diagnosis:: Bone MetastasisDocument3 pagesA. Differential Diagnosis:: Bone MetastasisDonna DumaliangPas encore d'évaluation
- Emergency Response Procedures Manual - PT. Saberindo Pacific - 2011Document15 pagesEmergency Response Procedures Manual - PT. Saberindo Pacific - 2011Indah Rida Afriyanti100% (1)
- Respiration 16 Respiratory FailureDocument31 pagesRespiration 16 Respiratory Failureapi-19641337Pas encore d'évaluation
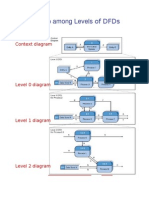
- Relationship Among Levels of DFDsDocument8 pagesRelationship Among Levels of DFDssunny_242574Pas encore d'évaluation
- Mental Health Resources - OrganizedDocument39 pagesMental Health Resources - OrganizedGabrielle Costello-GuerraPas encore d'évaluation
- HgedgergtDocument84 pagesHgedgergtWRGWSRPas encore d'évaluation
- Slu Brochure Ay 2014-2015Document2 pagesSlu Brochure Ay 2014-2015Michael BermudoPas encore d'évaluation