Académique Documents
Professionnel Documents
Culture Documents
1 High Risk Newborn
Transféré par
myer pasandalan0 évaluation0% ont trouvé ce document utile (0 vote)
27 vues5 pagesbj
Copyright
© © All Rights Reserved
Formats disponibles
DOCX, PDF, TXT ou lisez en ligne sur Scribd
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentbj
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
0 évaluation0% ont trouvé ce document utile (0 vote)
27 vues5 pages1 High Risk Newborn
Transféré par
myer pasandalanbj
Droits d'auteur :
© All Rights Reserved
Formats disponibles
Téléchargez comme DOCX, PDF, TXT ou lisez en ligne sur Scribd
Vous êtes sur la page 1sur 5
1
HIGH RISK NEWBORNS Increased respiratory rate to better use the
surface available
PRETERM INFANT
Predisposing factors:
o A live infant born before the end of
37th week of pregnancy o Cesarean birth (thoracic cavity not
o Weighs less than 2,500 grams at birth compressed thus less lung fluid is
o The earlier the infant is born, the expelled)
greater the chance of complications. o Mother received extensive fluid
administration during labor
Etiology o Prematurity
o Maternal risk factors: smoking, poor Complications:
nutrition, placental problems,
incompetent cervix. o Tiring effort
o Other risk factors: Low socioeconomic o Mild retractions
status, environmental exposure to o Mild hypoxia
harmful substance. o Difficult feeding
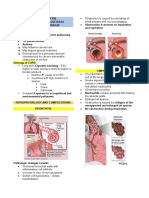
Respiratory Distress Syndrome (RDS) Interventions:
Etiology: 1. Close observation:
o Lack of surfactant o See to it that increased effort is not
o Insufficient surfactant allows alveoli to tiring
collapse with each expiration o Watch out for more serious disorder
o Respiratory failure is most common (respiratory obstruction)
cause of death in preterm infants within 2. Oxygen administration
the first 72 hours of life
o Peaks in intensity at 36 hours of life &
Assessment: then begins to fade
o Tachypnea o By 72 hours, spontaneously fades (lung
o Tachycardia fluid is absorbed)
o Cyanosis Apnea
o Grunting
o Nasal flaring o Pause in respiration longer than 20sec.
o Chest wall retractions o Apnea of 15 seconds or less is normal at
any age
Interventions: o Can be a sign of sepsis, seizures, upper
1. Put the patient on NPO to decrease risk airway abnormalities, gastro-
for aspiration esophageal reflux, hypoglycemia, or
2. Administer Oxygen therapy impaired regulation of sleep or feeding.
3. Assist physician in inserting o Usually presents as an apparent life-
endotracheal tube threatening event.
4. Instill artificial surfactant via the ET tube o Associated with cyanosis, marked
5. Maintain respirations 30-60/min pallor, hypotonia or bradycardia
6. 6. Assess every 1-2 hrs and prn Causes:
Transient tachypnea in newborn o Fatigue
o Rapid respiratory rate up to 80 o Immaturity of respiratory mechanisms
breaths/minute when crying o Secondary stresses:
o Within 1 hour, slows to 30-60 bpm o Infection
o Hyperbilirubinemia
Causes: o Hypoglycemia
Slow absorption of lung fluid --- Slight decrease o Hypothermia
in mature surfactant production --- decreased
alveolar surface area for oxygen exchange ---
2
Interventions: o Assess for abdominal distention and
emesis (neonate is not tolerating the
1. Stimulate the baby to breathe again
feedings)
o Shake the baby gently
Infection (Sepsis Neonatorum)
o Flick the sole of the foot
o Theophylline (bronchodilator) ETIOLOGY:
2. Resuscitation o Immature immune system
o Lack of immunoglobulin from the
Prevention:
mother
o Maintain a neutral thermal
ASSESSMENT:
environment
o Avoid excessive fatigue (gentle o Redness
handling) o Hypoactivity
o Always suction gently o Poor sucking
o Burp after feeding
INTERVENTIONS:
Hypothermia
o Provide antibiotic therapy
ETIOLOGY: o Adhere to ASEPTIC PROTOCOL
o Administer O2 therapy
o Lack of subcutaneous fat to insulate
o Monitor v/s, activity level.
body
o Small muscle mass Hemorrhage
o Absent sweat or shiver mechanisms
ETIOLOGY:
ASSESSMENT:
o Rupture of thin fragile capillaries within
Mottling the ventricles of the brain
o Immature production of clotting factors
o Tachypnea
o Increased activity ASSESSMENT:
o Increased crying
1. Lethargy - degree of inactivity &
INTERVENTIONS: unresponsiveness nearing
unconsciousness
1. Place infant under radiant warmer or in
2. Bulging fontanels
double-wall isolette.
3. Bradycardia
2. Assess infant’s temp q 2-3 hours and
prn INTERVENTIONS:
3. Warm equipment and linen before in
1. Monitor for signs of hemorrhage.
contact with infant.
2. Administer Vitamin K
Aspiration
Hyperbilirubinemia
Etiology:
o Excessive amounts of bile pigment
o Weak suck/swallow reflexes until 33 to bilirubin in the blood.
34 weeks gestation
ETIOLOGY:
o Poor gag/cough reflexes increase risk of
aspiration o Related to immature liver
o Difficulty in eliminating bilirubin
INTERVENTIONS:
released by normal breakdown of red
o Monitor suck/swallow reflex to assess blood cells
the risk of aspiration; if poor, gavage
ASSESSMENT:
feed as indicated
o Use “preemie” nipple if bottle feeding o Jaundice
o Burp frequently o Dark/Tea colored
3
INTERVENTIONS: o Care for neonate receiving
phototherapy:
1. Provide for phototherapy (bili light
o Protect eyes from light
exposure) – 18” from the baby (Protect
o Monitor for signs of dehydration
eyes & the genitals)
2. Regular turning to the side every 2 2. Exchange transfusions
hours
o done on severely affected infants to
3. Promote feeding and hydration and
decrease the antibody level & increase
give water in between feedings
infant RBC & hemoglobin levels.
Abo incompatibility
Retinopathy of Prematurity
o Maternal blood is O and the fetal blood
o Disorder of the retina resulting to
is either A, B, AB
impairment or loss of vision.
Pathophysiology:
ETIOLOGY:
o The mother’s body forms an antibody
Prolonged exposure to high O2 conc. ---
against such particular blood group
Hemorrhage within the retina --- Retinal
antigen and hemolysis (destruction of
detachment --- Loss of vision
RBC) begins.
o The process of antibody formation is Intervention:
maternal sensitization.
o The antibodies are of large class & do 1. Cautious administration of oxygen
not cross the placenta o Administer the minimum amount of
o Hemolysis of blood begins at birth oxygen to maintain PaO2 (partial
during the mixing of maternal & fetal pressure of oxygen in arterial blood) of
blood as the placenta is loosened. 50-70 mmHg
Complications: POSTMATURE INFANTS
o Fetal anemia o Born after completion of 42 weeks of
o Jaundice pregnancy
o Kernicterus (excessively high bilirubin
levels) Etiology:
ASSESSMENT: o Problems are caused by progressively
less efficient actions of placenta.
o Blood incompatibility between mother
& fetus ASSESSMENT
o Jaundice & increasing bilirubin levels o Absence of vernix and minimal lanugo
during first 24 hrs o Minimal subcutaneous fats
o Decreased hematocrit & hemoglobin o OLD MAN’s face – leather like skin; long
o Lethargy & irritability fingernails
o Poor feeding pattern; vomiting o Skin and cord yellow/green
o Enlargement of the liver & spleen
o Signs of kernicterus: Hypoglycemia
- Absence of Moro reflex
ETIOLOGY:
- Apnea
- High pitched cry o Inadequate glucose stores
- Opisthotonos - o Placental insufficiency
- Tremors
ASSESSMENT:
- Seizures
o High-pitched cry
Management:
o Jittery movements (jerky/rapid jumpy
1. Phototherapy - to reduce mild to moderate movements)
kernicterus o Convulsions
4
INTERVENTIONS: Fetal factors:
o Provide glucose infusion (10 – 25 % IV o Normal genetically small infant
glucose) o Chromosomal abnormality
o Monitor patient closely o Malformations
o Provide milk feedings o Congenital infections (rubella &
o Decrease stimuli to prevent seizures cytomegalovirus)
Meconium Aspiration Syndrome (MAS) Clinical manifestations
ETIOLOGY: o Soft tissue wasting and dysmaturity
o Loose, dry and scaling skin
o Occurs when infants take meconium
o Perinatal asphyxia
into their lungs during or before
o Polycythemia (increase hgb conc.),
delivery.
respiratory distress, and CNS
ASSESSMENT: aberrations and persistent acrocyanosis
o Congenital anomalies
o Greenish or yellowish appearance of
the amniotic fluid Lab. & diagnostic study findings
o Infant's skin, umbilical cord, or nail beds
o Glucose testing will reveal decreased
may be stained
glycogen stores (increases the potential
INTERVENTIONS: for hypothermia & hypoglycemia)
o Hematocrit level may be increased
o Adequate suctioning
o Oxygen administration Nursing management
Small-for-gestational-age infant 1. Provide adequate fluid and electrolytes and
nutrition.
o A baby who is smaller than the usual
amount for the number of weeks of o High calorie formula for feeding
pregnancy.
2. Decrease metabolic demands when possible
o Usually has birth weight below the 10th
percentile for babies of the same o Small frequent feedings
gestational age (they are smaller than o Gavage feedings (if no steady weight
90 percent of all other babies of the gain)
same GA) o Neutral thermal environment
o May appear physically and o Decrease iatrogenic stimuli
neurologically mature but is smaller
3. Prevent hypoglycemia
than other babies of the same GA.
o May be preterm, term or post term o Monitor glucose
o Provide early feedings
ETIOLOGY
o Frequent feedings (q 2 to 3 hrs)
Maternal causes: o IV glucose if glucose level does not
normalize with oral feedings
o Hypertension
o Cardiac, pulmonary or renal disease 4. Maintain a neutral thermal environment
o Diabetes Mellitus
5. Monitor serum hematocrit
o Poor nutrition
o Use of alcohol, tobacco or drugs 6. Provide education and emotional support
o Age
o Multiple gestation Large-for-gestational age infant
o Placental insufficiency o Is one who weighs more than 4,000
o Placental fetal abnormalities grams
o Pregnancy that occurred at high o Is above the 90th percentile of the
altitudes normal variation for gestational age.
5
Predisposing factors: o Assess for adduction of affected arm
with internal rotation & elbow
o Genetic predisposition
extension
o Excessive maternal weight gain during
o Moro reflex is absent on the affected
pregnancy
side
o Poorly controlled maternal diabetes
o Grasp reflex is intact
o Pathophysiology:
o Overproduction of growth hormone in Klumpke paralysis
utero
- Affects lower trunk from nerve roots C7 and
o Multiparous pregnancies
T1
Manifestations:
o Assess for absent grasp on the affected
Birth injuries: side
o The hand appears as claw-shaped
o Fractured clavicle
o Facial nerve injury Erb – Duchenne palsy & Klumpke paralysis
o Erb – Duchenne palsy or brachial plexus
Management:
paralysis
o Klumpke paralysis o X-ray of shoulder & upper arm
o Phrenic nerve palsy o Delay passive movement of affected
o Possible skull fracture joints until nerve edema resolves (7-10
days)
Management:
o Possible splinting to prevent wrist &
Fractured clavicle digit contractures on the affected side
o X-ray Phrenic nerve palsy (phrenic nerve - supplies the
o Assess for crepitus, hematoma, or muscles of the diaphragm)
deformity over the clavicle; decreased
Management:
movement of arm on the affected side;
absent Moro reflex o Assess for respiratory distress with
o Limit motion diminished breath sounds
o Pain reliever o X-ray usually shows elevation of the
diaphragm on the affected side
Facial nerve injury
o Avoid pneumonia during the recovery
o Assess for asymmetry of mouth while phase (1-3 months)
crying
Skull fracture
o Wrinkles are deeper on the unaffected
side Manifestations:
o The paralyzed side is smooth, with a
swollen appearance. o Soft tissue swelling over fracture site
o If the eye is affected, protect it with o Visible indentation in scalp
patches and artificial tears o Cephalhematoma
o Positive skull x-rays
Erb – Duchenne palsy o CNS signs & symptoms with intracranial
hemorrhage:
A paralysis of the arm caused by injury
Lethargy
to the upper group of the arm's main
Seizures
nerves, specifically, spinal roots C5-C7.
Apnea
Hypotonia
Vous aimerez peut-être aussi
- Snoring, A Simple Guide To The Condition, Treatment And Related ConditionsD'EverandSnoring, A Simple Guide To The Condition, Treatment And Related ConditionsPas encore d'évaluation
- PediatricsDocument321 pagesPediatricsJulian GalindoPas encore d'évaluation
- A Simple Guide to Skin Polyp and Other PolypsD'EverandA Simple Guide to Skin Polyp and Other PolypsÉvaluation : 5 sur 5 étoiles5/5 (2)
- Care of NeonatesDocument7 pagesCare of NeonatesJankaruroPas encore d'évaluation
- The Psychology of Hysteria - A Selection of Classic Articles on the Analysis and Symptoms of HysteriaD'EverandThe Psychology of Hysteria - A Selection of Classic Articles on the Analysis and Symptoms of HysteriaPas encore d'évaluation
- PediatricsDocument321 pagesPediatricsAlenaPas encore d'évaluation
- Laryngopharyngeal Reflux, A Simple Guide to the Condition, Treatment and Related DiseasesD'EverandLaryngopharyngeal Reflux, A Simple Guide to the Condition, Treatment and Related DiseasesÉvaluation : 3.5 sur 5 étoiles3.5/5 (2)
- General AnaesthesiaDocument5 pagesGeneral Anaesthesiayogesh.sontakke4487Pas encore d'évaluation
- Status AsthmaticusDocument6 pagesStatus AsthmaticusMae Azores100% (1)
- Askep Sdki, SikiDocument4 pagesAskep Sdki, SikiYurmadesi DesiPas encore d'évaluation
- Acute Biologic CrisisDocument7 pagesAcute Biologic CrisisRefeoj Allidañac AyartPas encore d'évaluation
- Neonatal ResuscitationDocument19 pagesNeonatal ResuscitationDavina DakapPas encore d'évaluation
- Pediatrics NCM 109Document26 pagesPediatrics NCM 109Gezabelle SalvePas encore d'évaluation
- AsthmaDocument15 pagesAsthmaDiana HuañecPas encore d'évaluation
- Topic: Bronchitis: PathophysiologyDocument3 pagesTopic: Bronchitis: PathophysiologyEdson John DemayoPas encore d'évaluation
- Nursing Care of at RiskDocument7 pagesNursing Care of at RiskdominicjimenezPas encore d'évaluation
- ANAK (Full Permission)Document167 pagesANAK (Full Permission)anggyPas encore d'évaluation
- Newborn PediaDocument11 pagesNewborn PediaRehanPas encore d'évaluation
- Ob2 Sas 17Document9 pagesOb2 Sas 17Ralph Louie ManagoPas encore d'évaluation
- Pediatri 2Document165 pagesPediatri 2YUYUM100% (2)
- Newbornassessment EDITED FOR LECTUREDocument37 pagesNewbornassessment EDITED FOR LECTUREAllen Caine TaabbilPas encore d'évaluation
- PEDIATRICS DISORDER PART 2 LECTURE MergedDocument33 pagesPEDIATRICS DISORDER PART 2 LECTURE MergedErika CadawanPas encore d'évaluation
- Edward - Intubation CovidDocument23 pagesEdward - Intubation CovidM Ivan Pratama ZebuaPas encore d'évaluation
- Pre-Mature FetusDocument8 pagesPre-Mature FetusCarl Andre ReyesPas encore d'évaluation
- (PESERTA) PEDIATRI 2 - MANTAP Februari 2017 PDFDocument157 pages(PESERTA) PEDIATRI 2 - MANTAP Februari 2017 PDFmarcelinaPas encore d'évaluation
- Textbook & Discussion: DefinitionDocument5 pagesTextbook & Discussion: DefinitionJay VillasotoPas encore d'évaluation
- Flowchart 1 Immediate Management of An Asphyxiated NewbornDocument3 pagesFlowchart 1 Immediate Management of An Asphyxiated Newborndessy pratiwiPas encore d'évaluation
- Acute Conditions of The NewbornDocument5 pagesAcute Conditions of The NewbornCamille Joy BaliliPas encore d'évaluation
- BreathlessnessDocument55 pagesBreathlessnessHanahigaPas encore d'évaluation
- CORNELL NOTE High Risk New BornDocument3 pagesCORNELL NOTE High Risk New BornMargareth DandanPas encore d'évaluation
- Newborn ResuscitationDocument6 pagesNewborn ResuscitationMartina MedranoPas encore d'évaluation
- Immediate Care of The NewbornDocument4 pagesImmediate Care of The Newbornmelinda100% (1)
- Acute Conditions of The NeonatesDocument4 pagesAcute Conditions of The NeonatesShermina JalaniPas encore d'évaluation
- Flowchart 1 Immediate Management of An AsphyxiatednewbornDocument3 pagesFlowchart 1 Immediate Management of An Asphyxiatednewborndessy pratiwiPas encore d'évaluation
- Nursing Care For Child With Autoimmune Diseases & GI DisordersDocument4 pagesNursing Care For Child With Autoimmune Diseases & GI Disordersbunso padillaPas encore d'évaluation
- Chronic Obstructive Pulmonary DiseaseDocument6 pagesChronic Obstructive Pulmonary Diseaseshamae justinianoPas encore d'évaluation
- Pathophysiology: Risk FactorsDocument4 pagesPathophysiology: Risk FactorsEdson John DemayoPas encore d'évaluation
- Basic Skills For Clients With Oxygenation ProblemsDocument3 pagesBasic Skills For Clients With Oxygenation ProblemsAlec Xavier MirandaPas encore d'évaluation
- Management of Extremely Low Birth Weight BabiesDocument57 pagesManagement of Extremely Low Birth Weight BabiesAmit AnandPas encore d'évaluation
- Ina Pedia1Document14 pagesIna Pedia1Kristil ChavezPas encore d'évaluation
- Safe Drugs During Pregnancy & Lactation: Category Pregnancy Breast-FeedingDocument16 pagesSafe Drugs During Pregnancy & Lactation: Category Pregnancy Breast-FeedingJo ckerPas encore d'évaluation
- Medical and Nursing Management Nursing Care PlanDocument7 pagesMedical and Nursing Management Nursing Care PlanPau-pau BasiPas encore d'évaluation
- Arciaga, FG - SGDMicroAnaerobesDocument7 pagesArciaga, FG - SGDMicroAnaerobesFG ArciagaPas encore d'évaluation
- Acute Conditions of The NewbornDocument6 pagesAcute Conditions of The NewbornCamille Joy BaliliPas encore d'évaluation
- Paediatrics SbaDocument34 pagesPaediatrics SbaAhmad Syahmi YZ100% (1)
- Week 13 NCMB 312 Lect NotesDocument18 pagesWeek 13 NCMB 312 Lect NotesAngie BaylonPas encore d'évaluation
- Intussusception TransDocument4 pagesIntussusception TransJames Maravillas100% (1)
- Respiratory - Distress (1) 2 PDFDocument8 pagesRespiratory - Distress (1) 2 PDFSatya Prakash TiwariPas encore d'évaluation
- Lecture NotesDocument56 pagesLecture NotesLalaine April E. Ortiola100% (13)
- Covid Home CareDocument23 pagesCovid Home Careangel_sagun_1Pas encore d'évaluation
- HYPERTHYROIDISMDocument6 pagesHYPERTHYROIDISMSJane FeriaPas encore d'évaluation
- Review NTS..NCM 109Document11 pagesReview NTS..NCM 109Celline Isabelle ReyesPas encore d'évaluation
- (Surg3b) Pediatric Surgery (Resurreccion) - PauzkiDocument13 pages(Surg3b) Pediatric Surgery (Resurreccion) - PauzkiAra CasalsPas encore d'évaluation
- Advanced CaseDocument13 pagesAdvanced CaseÀndrew SsenkosiPas encore d'évaluation
- ND RD TH THDocument18 pagesND RD TH THbarangaynaparingbhsPas encore d'évaluation
- FundamentalsDocument4 pagesFundamentalsKayla CicciaPas encore d'évaluation
- Pneumonia Study GuideDocument5 pagesPneumonia Study GuideMartha Marty BalintPas encore d'évaluation
- AGN 3B FinalDocument37 pagesAGN 3B FinalKristine Dela CruzPas encore d'évaluation
- Care of The NewbornDocument5 pagesCare of The Newbornbuzz Q100% (2)
- ENT Lecture FinalDocument65 pagesENT Lecture FinalNejib M/AminPas encore d'évaluation
- Anatomy of The Urinary System: Patient's Name / Room No. - 1Document2 pagesAnatomy of The Urinary System: Patient's Name / Room No. - 1myer pasandalanPas encore d'évaluation
- Risperidine: Disturbed Thought Process Related To Neurological DisturbancesDocument3 pagesRisperidine: Disturbed Thought Process Related To Neurological Disturbancesmyer pasandalanPas encore d'évaluation
- Complaint For Damages SampleDocument4 pagesComplaint For Damages Samplemyer pasandalanPas encore d'évaluation
- Nursing Care Plan: Cues Nursing Diagnosis Objective Intervention Rationale EvaluationDocument2 pagesNursing Care Plan: Cues Nursing Diagnosis Objective Intervention Rationale Evaluationmyer pasandalanPas encore d'évaluation
- Nursing Care Plan: Cues Nursing Diagnosis Objective Intervention Rationale EvaluationDocument3 pagesNursing Care Plan: Cues Nursing Diagnosis Objective Intervention Rationale Evaluationmyer pasandalanPas encore d'évaluation
- Nursing Assessment IIDocument5 pagesNursing Assessment IImyer pasandalanPas encore d'évaluation
- Nursing Care Plan: Cues Nursing Diagnosis Objective Intervention Rationale EvaluationDocument3 pagesNursing Care Plan: Cues Nursing Diagnosis Objective Intervention Rationale Evaluationmyer pasandalanPas encore d'évaluation
- ConstipationDocument3 pagesConstipationmyer pasandalanPas encore d'évaluation
- Narrative PathophysiologyDocument5 pagesNarrative Pathophysiologymyer pasandalanPas encore d'évaluation
- Diagnostic and Laboratory ProceduresDocument6 pagesDiagnostic and Laboratory Proceduresmyer pasandalanPas encore d'évaluation
- Personality DisordersDocument2 pagesPersonality Disordersmyer pasandalanPas encore d'évaluation
- Discharge Plan: Drug/S Indication/S Dosage Route FrequencyDocument3 pagesDischarge Plan: Drug/S Indication/S Dosage Route Frequencymyer pasandalanPas encore d'évaluation
- Schizophrenia: I. IdentificationDocument3 pagesSchizophrenia: I. Identificationmyer pasandalanPas encore d'évaluation
- Neurobiologic Theories and PsychopharmacologyDocument2 pagesNeurobiologic Theories and Psychopharmacologymyer pasandalanPas encore d'évaluation
- Chapter 16 - SchizophreniaDocument13 pagesChapter 16 - Schizophreniamyer pasandalanPas encore d'évaluation
- Chapter 17 Mood Disorders and SuicideDocument13 pagesChapter 17 Mood Disorders and Suicidemyer pasandalanPas encore d'évaluation
- Group F DXDocument2 pagesGroup F DXmyer pasandalanPas encore d'évaluation
- Eating DisordersDocument1 pageEating Disordersmyer pasandalanPas encore d'évaluation
- Hospital DietsDocument5 pagesHospital Dietsmyer pasandalan100% (2)
- HIV in South AfricaDocument17 pagesHIV in South AfricaMadelinePas encore d'évaluation
- Chapter 6 The Circulatory System of MammalsDocument30 pagesChapter 6 The Circulatory System of MammalsRethenaPas encore d'évaluation
- Dyslipidemia: Darmono SSDocument35 pagesDyslipidemia: Darmono SSLa Ode Rinaldi0% (1)
- 24.18.00 - Chikungunya2 DR RAGADocument48 pages24.18.00 - Chikungunya2 DR RAGAjcvh24Pas encore d'évaluation
- Bach Flowers CombinationsDocument20 pagesBach Flowers Combinationsraghavan remidicharla100% (3)
- Norsyahira Binti Abdullah - hs245 4cDocument8 pagesNorsyahira Binti Abdullah - hs245 4cMOHD MU'IZZ BIN MOHD SHUKRIPas encore d'évaluation
- Chromosome Walking: and David S. Hogness in The Early 1980'sDocument4 pagesChromosome Walking: and David S. Hogness in The Early 1980'sprakash singhPas encore d'évaluation
- Drug StudyDocument14 pagesDrug StudyCj LowryPas encore d'évaluation
- AUB - Physical Examination of UrineDocument3 pagesAUB - Physical Examination of UrineJeanne RodiñoPas encore d'évaluation
- Classification of Psychiatric DisordersDocument64 pagesClassification of Psychiatric Disordersdrkadiyala2100% (1)
- Revalida 1Document3 pagesRevalida 1herrabiel solisPas encore d'évaluation
- Beta Blocker TitrationDocument2 pagesBeta Blocker TitrationAwalunisa IstiqomahPas encore d'évaluation
- Stroke:: What Should Nurses Need To Know About Stroke?Document68 pagesStroke:: What Should Nurses Need To Know About Stroke?Suci Aning TPas encore d'évaluation
- Bakar CD RobiwijayaDocument60 pagesBakar CD RobiwijayaAsep Ribbat MPas encore d'évaluation
- AFA ReviwerDocument21 pagesAFA ReviwerLovely day ybanezPas encore d'évaluation
- Recent Advances in The Management of Hypoxic-Ischemic Encephalopathy-IJPPDocument6 pagesRecent Advances in The Management of Hypoxic-Ischemic Encephalopathy-IJPPdrtgodePas encore d'évaluation
- IPME Research PaperDocument13 pagesIPME Research Papermarina abanPas encore d'évaluation
- Metabolic Acidosis FinalDocument29 pagesMetabolic Acidosis FinalTera SurbaktiPas encore d'évaluation
- Genitourinary SystemDocument27 pagesGenitourinary SystemDanica FrancoPas encore d'évaluation
- HypothesisDocument4 pagesHypothesisSunny Boy Ng SinadjanPas encore d'évaluation
- Challenges Faced by Families of Autistic Children-153Document5 pagesChallenges Faced by Families of Autistic Children-153Zahoor Ahmad100% (1)
- TaxonomyDocument71 pagesTaxonomyNabeel Uddin100% (1)
- Santosh DevDocument45 pagesSantosh Devdevdsantosh100% (1)
- 02 - Recalibrating Gavi 5.0 in Light of COVID-19 and Successful Replenis..Document19 pages02 - Recalibrating Gavi 5.0 in Light of COVID-19 and Successful Replenis..aman_sasanPas encore d'évaluation
- Netically Modified Crops Their Development, Uses, and Risks by G.H. LiangDocument416 pagesNetically Modified Crops Their Development, Uses, and Risks by G.H. LiangbiokanagasundarPas encore d'évaluation
- VITAMINS-Carol Jane Lorenzo, RMTDocument8 pagesVITAMINS-Carol Jane Lorenzo, RMTREYES, JAN MERCK M.Pas encore d'évaluation
- Review - Spinal Cord Injury - 2Document1 pageReview - Spinal Cord Injury - 2Sarah MendozaPas encore d'évaluation
- Pet Food 2Document73 pagesPet Food 2AB100% (1)
- Daily Practice Sheet - 105 Molecular Basis of Inheritance: Biomentors Classes Online, Mumbai Date - 27 September 2018Document6 pagesDaily Practice Sheet - 105 Molecular Basis of Inheritance: Biomentors Classes Online, Mumbai Date - 27 September 2018Sushree DeepaliPas encore d'évaluation
- Endocrine: QuestionsDocument14 pagesEndocrine: QuestionsMuhammad Abubakar100% (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionD'EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionÉvaluation : 4 sur 5 étoiles4/5 (404)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDD'EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDÉvaluation : 5 sur 5 étoiles5/5 (3)
- The Age of Magical Overthinking: Notes on Modern IrrationalityD'EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityÉvaluation : 4 sur 5 étoiles4/5 (29)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeD'EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeÉvaluation : 2 sur 5 étoiles2/5 (1)
- The Obesity Code: Unlocking the Secrets of Weight LossD'EverandThe Obesity Code: Unlocking the Secrets of Weight LossÉvaluation : 4 sur 5 étoiles4/5 (6)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)D'EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Évaluation : 3 sur 5 étoiles3/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisD'EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisÉvaluation : 4.5 sur 5 étoiles4.5/5 (42)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedD'EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedÉvaluation : 5 sur 5 étoiles5/5 (81)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsD'EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsPas encore d'évaluation
- The Comfort of Crows: A Backyard YearD'EverandThe Comfort of Crows: A Backyard YearÉvaluation : 4.5 sur 5 étoiles4.5/5 (23)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.D'EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Évaluation : 4.5 sur 5 étoiles4.5/5 (110)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsD'EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsÉvaluation : 5 sur 5 étoiles5/5 (1)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessD'EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessÉvaluation : 4.5 sur 5 étoiles4.5/5 (328)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaD'EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- To Explain the World: The Discovery of Modern ScienceD'EverandTo Explain the World: The Discovery of Modern ScienceÉvaluation : 3.5 sur 5 étoiles3.5/5 (51)
- Why We Die: The New Science of Aging and the Quest for ImmortalityD'EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityÉvaluation : 4 sur 5 étoiles4/5 (5)
- Troubled: A Memoir of Foster Care, Family, and Social ClassD'EverandTroubled: A Memoir of Foster Care, Family, and Social ClassÉvaluation : 4.5 sur 5 étoiles4.5/5 (27)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeD'EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeÉvaluation : 4.5 sur 5 étoiles4.5/5 (253)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisD'EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisÉvaluation : 4 sur 5 étoiles4/5 (1)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisD'EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisÉvaluation : 3.5 sur 5 étoiles3.5/5 (2)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsD'EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsÉvaluation : 4 sur 5 étoiles4/5 (4)
- The Marshmallow Test: Mastering Self-ControlD'EverandThe Marshmallow Test: Mastering Self-ControlÉvaluation : 4.5 sur 5 étoiles4.5/5 (59)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsD'EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsÉvaluation : 4.5 sur 5 étoiles4.5/5 (170)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryD'EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryÉvaluation : 4 sur 5 étoiles4/5 (45)