Académique Documents
Professionnel Documents
Culture Documents
Peptic Ulcer Disease
Transféré par
Chino Paolo SamsonDescription originale:
Titre original
Copyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Peptic Ulcer Disease
Transféré par
Chino Paolo SamsonDroits d'auteur :
Formats disponibles
GROUP
C2
Physiology Laboratory
Small Group Discussion
Output
March 9, 2016
[PEPTIC ULCER DISEASE]
By: ASUBARIO, Olufunmilola Omonike; BALADAD, Alvin Byron; DE JESUS, Chrislou; GURUNG, Man
Bahadur; KALANYEG, Kristie; MAHALEE, Naphitcharak; MONTHATHONG, Thanapol; PANLASIGUI,
Rikkimae Maria; SAMSON, Chino Paolo; SOLONIO, Natalie Keith; VALDEZ, Gregorio
PEPTIC ULCER DISEASE
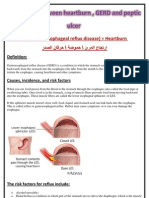
Peptic ulcer disease (PUD), also known
as a peptic ulcer or stomach ulcer, is a break in
the lining of the stomach, first part of the small
intestine, or occasionally the lower esophagus. An
ulcer in the stomach is known as a gastric
ulcer while that in the first part of the intestines is
known as a duodenal ulcer. The most common
symptoms are waking at night with upper
abdominal pain or upper abdominal pain that
improves with eating. The pain is often described
as a burning or dull ache. Other symptoms include
Deep gastric ulcer belching, vomiting, weight loss, or poor appetite.
About a third of older people have no symptoms.
Complications may include bleeding, perforation,
and blockage of the stomach. Bleeding occurs in
as many as 15% of people.
EPIDEMIOLOGY
In the United States, PUD affects approximately 4.5 million people annually.
Approximately 10% of the US population has evidence of a duodenal ulcer at some
time. Of those infected with H pylori, the lifetime prevalence is approximately 20%. Only
about 10% of young persons have H pylori infection; the proportion of people with the
infection increases steadily with age.
Overall, the incidence of duodenal ulcers has been decreasing over the past 3-4
decades. Although the rate of simple gastric ulcer is in decline, the incidence of
complicated gastric ulcer and hospitalization has remained stable, partly due to the
concomitant use of aspirin in an aging population. The hospitalization rate for PUD is
approximately 30 patients per 100,000 cases.
The prevalence of PUD has shifted from predominance in males to similar
occurrences in males and females. Lifetime prevalence is approximately 11-14% in men
and 8-11% in women. Age trends for ulcer occurrence reveal declining rates in younger
men, particularly for duodenal ulcer, and increasing rates in older women. Trends reflect
complex changes in risk factors for PUD, including age-cohort phenomena with the
prevalence of H pylori infection and the use of NSAIDs in older populations.
Physiology Laboratory Small Group Discussion Output | Peptic Ulcer Disease 1
International statistics
The frequency of PUD in other countries is variable and is determined primarily
by association with the major causes of PUD: H pylori and NSAIDs
SIGNS & SYMPTOMS
An ulcer may or may not have symptoms. When symptoms occur, they may include:
A gnawing or burning pain in the middle or upper stomach between meals or at
night
Bloating
Heartburn
Nausea or vomiting
In severe cases, symptoms can include:
Dark or black stool (due to bleeding)
Vomiting blood (that can look like "coffee-grounds")
Weight loss
Severe pain in the mid to upper abdomen
CAUSES
Different factors can cause the lining of the stomach, the esophagus, and the small
intestine to break down. These include:
Helicobacter pylori (H. pylori): a bacteria that can cause a stomach infection and
inflammation
frequent use of aspirin, ibuprofen, and other anti-inflammatory drugs (risk associated
with this behavior increases in women and people over the age of 60)
smoking
drinking too much alcohol
radiation therapy
stomach cancer
PATHOPHYSIOLOGY
Peptic ulcers result from an imbalance between factors that can damage the
gastroduodenal mucosal lining and defense mechanisms that normally limit the injury.
Aggressive factors include gastric juice (including hydrochloric acid, pepsin, and bile
salts refluxed from the duodenum), H pylori, and NSAIDs.
Physiology Laboratory Small Group Discussion Output | Peptic Ulcer Disease 2
Mucosal defenses comprise a mucus bicarbonate layer secreted by surface
mucus cells forming a viscous gel over the gastric mucosa; the integrity of tight
junctions between adjacent epithelial cells; and the process of restitution, whereby any
break in the epithelial lining is rapidly filled by adjacent epithelial and mucosal stromal
cells migrating and flattening to fill the gap. Mucosal defenses depend on an adequate
blood supply and on formation within the gastric mucosa.
In general, duodenal ulcers are the result of hypersecretion of gastric acid related
to H pylori infection (the majority of cases), whereas secretion is normal or low in
patients with gastric ulcers.
In duodenal ulcers, chronic H pylori infection confined mainly to the gastric
antrum leads to impaired secretion of somatostatin and consequently increased gastrin
release, resulting in gastric acid hypersecretion. In Zollinger-Ellison syndrome, a
gastrin-secreting neuro-endocrine tumour is the stimulus for high rates of gastric acid
secretion.
In gastric ulcers, longstanding H pylori infection throughout the stomach
accompanied by severe inflammation results in gastric mucin degradation, disruption of
tight junctions between gastric epithelial cells, and the induction of gastric epithelial cell
death. NSAIDs cause injury directly (involving trapping hydrogen ions) and indirectly (a
systemic effect involving the inhibition of cyclo-oxygenases, especially COX-1) and
increase bleeding risk through anti-platelet actions. Chronic gastric ischaemia underlies
the stress ulcers of patients in intensive care.
DIAGNOSIS:
Tests for H. pylori- Your doctor may recommend tests to determine whether the
bacterium H. pylori is present in your body. Tests can test for H. pylori using:
> Blood
> Breath
> Stool
Endoscopy- using a scope to examine your upper digestive system.During
endoscopy, your doctor passes a hollow tube equipped with a lens (endoscope)
down your throat and into your esophagus, stomach and small intestine. Using
the endoscope, your doctor looks for ulcers. If your doctor detects an ulcer, small
tissue samples (biopsy) may be removed for examination in a lab. A biopsy can
also identify the presence of H. pylori in your stomach lining. Your doctor is more
likely to recommend endoscopy if you are older, have signs of bleeding, or have
experienced recent weight loss or difficulty eating and swallowing
Physiology Laboratory Small Group Discussion Output | Peptic Ulcer Disease 3
X-ray of your upper digestive system- sometimes called a barium swallow or
upper gastrointestinal series, this series of X-rays creates images of your
esophagus, stomach and small intestine. During the X-ray, you swallow a white
liquid (containing barium) that coats your digestive tract and makes an ulcer
more visible.
TREATMENT & MANAGEMENT:
Treatment for peptic ulcers depends on the cause. Treatments can include:
Antibiotic medications to kill H. pylori. If H. pylori is found in your digestive tract, your
doctor may recommend a combination of antibiotics to kill the bacterium.
Proton pump inhibitors reduce stomach acid by blocking the action of the parts of
cells that produce acid. These drugs include the prescription and over-the-counter
medications omeprazole (Prilosec), lansoprazole (Prevacid), rabeprazole (Aciphex),
esomeprazole (Nexium) and pantoprazole (Protonix).
Acid blockers — also called histamine (H-2) blockers — reduce the amount of
stomach acid released into your digestive tract, which relieves ulcer pain and
encourages healing.
Antacids that neutralize stomach acid. Antacids neutralize existing stomach acid and
can provide rapid pain relief. Side effects can include constipation or diarrhea,
depending on the main ingredients.
In some cases, your doctor may prescribe medications called cytoprotective agents
that help protect the tissues that line your stomach and small intestine. Options
include the prescription medications sucralfate (Carafate) and misoprostol (Cytotec).
Another nonprescription cytoprotective agent is bismuth subsalicylate (Pepto-
Bismol).
PROGNOSIS
When the underlying cause is addressed, the prognosis is excellent. Most
patients are treated successfully with eradication of H pylori infection, avoidance of
NSAIDs, and the appropriate use of antisecretory therapy. Eradication of H
pyloriinfection changes the natural history of the disease, with a decrease in the ulcer
recurrence rate from 60-90% to approximately 10-20%. However, this is a higher
recurrence rate than previously reported, suggesting an increased number of ulcers not
caused by H pylori infection.
Physiology Laboratory Small Group Discussion Output | Peptic Ulcer Disease 4
With regard to NSAID-related ulcers, the incidence of perforation is
approximately 0.3% per patient year, and the incidence of obstruction is approximately
0.1% per patient year. Combining both duodenal ulcers and gastric ulcers, the rate of
any complication in all age groups combined is approximately 1-2% per ulcer per year.
The mortality rate for PUD, which has decreased modestly in the last few
decades, is approximately 1 death per 100,000 cases. If one considers all patients with
duodenal ulcers, the mortality rate due to ulcer hemorrhage is approximately 5%. Over
the last 20 years, the mortality rate in the setting of ulcer hemorrhage has not changed
appreciably despite the advent of histamine-2 receptor antagonists (H2RAs) and proton
pump inhibitors (PPIs). However, evidence from meta-analyses and other studies has
shown a decreased mortality rate from bleeding peptic ulcers when intravenous PPIs
are used after successful endoscopic therapy.[19, 20, 21, 22]
Emergency operations for peptic ulcer perforation carry a mortality risk of 6-30%.
Factors associated with higher mortality in this setting include the following:
Shock at the time of admission
Renal insufficiency
Delaying the initiation of surgery for more than 12 hours after presentation
Concurrent medical illness (eg, cardiovascular disease, diabetes mellitus
Age older than 70 years
Cirrhosis
Immunocompromised state
Location of ulcer (mortality associated with perforated gastric ulcer is twice that
associated with perforated
References:
1. Guyton, AC; Hall, JE: Textbook of Medical Physiology, 11th edition. Elsevier Inc.
2006.
2. Koeppen, BM; Stanton, BA: Berne and Levy Physiology, 6 th edition. Elsevier Inc.
2010.
3. en.wikipedia.org
4. http://www.webmd.com/digestive-disorders/digestive-diseases-peptic-ulcer-disease
Physiology Laboratory Small Group Discussion Output | Peptic Ulcer Disease 5
Vous aimerez peut-être aussi
- Stomach Ulcers (Peptic Ulcers)Document25 pagesStomach Ulcers (Peptic Ulcers)Irtza MajeedPas encore d'évaluation
- "Peptic Ulcer": Presented By, Archana Devi M.Sc. (N) 1 Year EconDocument27 pages"Peptic Ulcer": Presented By, Archana Devi M.Sc. (N) 1 Year EconArchana VermaPas encore d'évaluation
- Peptic Ulcer Disease Peptic Ulcer Disease Peptic Ulcer Disease Peptic Ulcer Disease Peptic Ulcer DiseaseDocument9 pagesPeptic Ulcer Disease Peptic Ulcer Disease Peptic Ulcer Disease Peptic Ulcer Disease Peptic Ulcer DiseaseRhesky Noer FhadillahPas encore d'évaluation
- Peptic Ulcer Disease: "Something Is Eating at Me"Document37 pagesPeptic Ulcer Disease: "Something Is Eating at Me"bobtaguba100% (1)
- Perforated Gastric UlcerDocument15 pagesPerforated Gastric UlcerNorshahidah IedaPas encore d'évaluation
- Ulkus PeptikumDocument9 pagesUlkus PeptikumRandi AnugerahPas encore d'évaluation
- By Amente J. (B.Pharm, MSC) : For Clinical Pharmacy Students (4 Year)Document38 pagesBy Amente J. (B.Pharm, MSC) : For Clinical Pharmacy Students (4 Year)Mohamed IsmaelPas encore d'évaluation
- Peptic Ulcer Disease - EMEDICINE.2020Document47 pagesPeptic Ulcer Disease - EMEDICINE.2020qayyum consultantfpsc100% (1)
- Dysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsD'EverandDysphagia, A Simple Guide To The Condition, Treatment And Related ConditionsÉvaluation : 5 sur 5 étoiles5/5 (1)
- Gastrointestinal Health: The Self-Help Nutritional Program That Can Change the Lives of 80 Million AmericansD'EverandGastrointestinal Health: The Self-Help Nutritional Program That Can Change the Lives of 80 Million AmericansPas encore d'évaluation
- Some Causes of Upper Midline Abdominal PainDocument2 pagesSome Causes of Upper Midline Abdominal PainChris RayPas encore d'évaluation
- Comprehensive Resume On Hepatitis ADocument9 pagesComprehensive Resume On Hepatitis AGeoffrey MasyhurPas encore d'évaluation
- Pud 2Document5 pagesPud 2Jake MillerPas encore d'évaluation
- Ulkus PeptikDocument26 pagesUlkus PeptikKang MunirPas encore d'évaluation
- Peptic Ulcer Disease - Need PicturesDocument5 pagesPeptic Ulcer Disease - Need PicturesAriana ValenciaPas encore d'évaluation
- Symptoms: Dyspepsia. The Most Common Symptoms of Peptic Ulcer Are Known Collectively As Dyspepsia. However, PepticDocument10 pagesSymptoms: Dyspepsia. The Most Common Symptoms of Peptic Ulcer Are Known Collectively As Dyspepsia. However, Pepticmiz uPas encore d'évaluation
- Ulcers, Peptic (Gastric, Duodenal)Document14 pagesUlcers, Peptic (Gastric, Duodenal)lagas_ralphPas encore d'évaluation
- Complication of Peptic Ulcer: Department of Surgery S. S. Medical College Rewa and Associate GMH and SGMH RewaDocument76 pagesComplication of Peptic Ulcer: Department of Surgery S. S. Medical College Rewa and Associate GMH and SGMH RewaBrajesh MouryaPas encore d'évaluation
- Peptic UlcerDocument7 pagesPeptic UlcerMarielle Adey Magcawas RNPas encore d'évaluation
- Helicobacter Pylori: Gastric and Duodenal Ulcers: A Gastric Ulcer Would GiveDocument5 pagesHelicobacter Pylori: Gastric and Duodenal Ulcers: A Gastric Ulcer Would Giveleslie_08Pas encore d'évaluation
- Definition, Etiology, Epidemiology PepticDocument3 pagesDefinition, Etiology, Epidemiology Pepticalfira andiniPas encore d'évaluation
- Definition, Etiology, Epidemiology PepticDocument4 pagesDefinition, Etiology, Epidemiology Pepticalfira andiniPas encore d'évaluation
- Tugas Ppdi + TerjemahanDocument14 pagesTugas Ppdi + TerjemahanAnggii WidyPas encore d'évaluation
- Peptic Ulcer DiseaseDocument3 pagesPeptic Ulcer DiseaseleahraizaPas encore d'évaluation
- Rami Dwairi, MD: Internal Medicine, HSDocument27 pagesRami Dwairi, MD: Internal Medicine, HSraed faisalPas encore d'évaluation
- Gastrointestinal Diseases - Part 1Document27 pagesGastrointestinal Diseases - Part 1glenn johnstonPas encore d'évaluation
- Brief History of The DiseaseDocument17 pagesBrief History of The DiseaseJon Corpuz AggasidPas encore d'évaluation
- Peptic Ulcer 2Document38 pagesPeptic Ulcer 2tarekPas encore d'évaluation
- Gastro-Oesophageal Reflux Disease: EpidemiologyDocument6 pagesGastro-Oesophageal Reflux Disease: EpidemiologyRehan RiyazPas encore d'évaluation
- Part 1 Introduction ADocument6 pagesPart 1 Introduction Ajay5ar5jamorabon5torPas encore d'évaluation
- Peptic Ulcer InfoDocument8 pagesPeptic Ulcer InfoSyazmin KhairuddinPas encore d'évaluation
- Gastric UlcerDocument2 pagesGastric Ulcersaby abbyPas encore d'évaluation
- Seminar ON Peptic Ulcer: Presented By: Ms. Sweta SinghDocument26 pagesSeminar ON Peptic Ulcer: Presented By: Ms. Sweta Singhshweta singhPas encore d'évaluation
- Hematemesis Melena Due To Helicobacter Pylori Infection in Duodenal Ulcer: A Case Report and Literature ReviewDocument6 pagesHematemesis Melena Due To Helicobacter Pylori Infection in Duodenal Ulcer: A Case Report and Literature ReviewWahyu Agung PribadiPas encore d'évaluation
- Peptic Ulcer HDocument6 pagesPeptic Ulcer HIlyes FerenczPas encore d'évaluation
- Brief Summary of Peptic UlcersDocument3 pagesBrief Summary of Peptic UlcersruguPas encore d'évaluation
- 01 Gastritis & PUDxxDocument51 pages01 Gastritis & PUDxxTor Koang ThorPas encore d'évaluation
- Peptis Ulcer-Bs TâmDocument27 pagesPeptis Ulcer-Bs TâmÁnh PhạmPas encore d'évaluation
- Peptic Ulcer DiseaseDocument7 pagesPeptic Ulcer DiseaseDiriba FedasaPas encore d'évaluation
- Part 1 Introduction ADocument6 pagesPart 1 Introduction AGeevee Naganag VentulaPas encore d'évaluation
- Nursing Management OF Git Problems Gastric and Duodenal DisordersDocument109 pagesNursing Management OF Git Problems Gastric and Duodenal DisorderstantanbaragoPas encore d'évaluation
- A Simple Guide to Gastritis and Related ConditionsD'EverandA Simple Guide to Gastritis and Related ConditionsÉvaluation : 4.5 sur 5 étoiles4.5/5 (3)
- Presentation On Gastric Ulcer-1Document37 pagesPresentation On Gastric Ulcer-1Roshan GhimirePas encore d'évaluation
- Part 1 Introduction ADocument6 pagesPart 1 Introduction AGeevee Naganag VentulaPas encore d'évaluation
- Duodenum Esophagus Stomach Meckel's Diverticulum: Pylori. Infection Usually Persists For ManyDocument3 pagesDuodenum Esophagus Stomach Meckel's Diverticulum: Pylori. Infection Usually Persists For ManyKim Andrew SantosPas encore d'évaluation
- GastritisDocument18 pagesGastritisBeatrice Sandra ChelaruPas encore d'évaluation
- Peptic Ulcer PresentationDocument46 pagesPeptic Ulcer Presentationmaryam ijazPas encore d'évaluation
- Medscape GastritisDocument13 pagesMedscape GastritisFalaudin LaksanaPas encore d'évaluation
- A Peptic UlcerDocument7 pagesA Peptic UlcerjenilyndchavezPas encore d'évaluation
- Unit 3 Gastrointestinal Disorders P2 Peptic UlcerDocument43 pagesUnit 3 Gastrointestinal Disorders P2 Peptic UlcerShashidharan MenonPas encore d'évaluation
- Peptic UlcermazherDocument49 pagesPeptic UlcermazherjawaidakramPas encore d'évaluation
- Peptic UlcerDocument2 pagesPeptic UlcerluvvemullePas encore d'évaluation
- 2 NCM+116n+Lecture+Care+of+the+Clients+with+Problems+GI+Function+and+NutritionDocument11 pages2 NCM+116n+Lecture+Care+of+the+Clients+with+Problems+GI+Function+and+NutritionKylle AlimosaPas encore d'évaluation
- Peptic Ulcer DiseaseDocument5 pagesPeptic Ulcer DiseasecookiePas encore d'évaluation
- Patho AssignmentDocument17 pagesPatho AssignmentKevser UnalPas encore d'évaluation
- Etiology: Peptic Ulcer Disease (PUD)Document4 pagesEtiology: Peptic Ulcer Disease (PUD)Chiki CacaPas encore d'évaluation
- Case Presentation On (Pud) Peptic Ulcer Disease: Presented by Pharm D InternDocument28 pagesCase Presentation On (Pud) Peptic Ulcer Disease: Presented by Pharm D InternAntoPas encore d'évaluation
- Dyspepsiapud 151124152422 Lva1 App6892Document16 pagesDyspepsiapud 151124152422 Lva1 App6892Tabada NickyPas encore d'évaluation
- 9 Annual Review in Internal Medicine: GastroenterologyDocument26 pages9 Annual Review in Internal Medicine: GastroenterologyChino Paolo SamsonPas encore d'évaluation
- Protein-Calories, Malnutrition & Nutritional DeficienciesDocument14 pagesProtein-Calories, Malnutrition & Nutritional DeficienciesChino Paolo SamsonPas encore d'évaluation
- Female Physiology Before PregnancyDocument81 pagesFemale Physiology Before PregnancyChino Paolo SamsonPas encore d'évaluation
- BIOENERGETICS Trans - IncDocument3 pagesBIOENERGETICS Trans - IncChino Paolo SamsonPas encore d'évaluation
- Protein-Calories, Malnutrition & Nutritional DeficienciesDocument15 pagesProtein-Calories, Malnutrition & Nutritional DeficienciesChino Paolo SamsonPas encore d'évaluation
- Adrenal Insufficiency & Addison'S Disease: April 13, 2016Document6 pagesAdrenal Insufficiency & Addison'S Disease: April 13, 2016Chino Paolo SamsonPas encore d'évaluation
- Hemolytic DiseaseDocument10 pagesHemolytic DiseaseChino Paolo SamsonPas encore d'évaluation
- The Depth of Christ's LoveDocument14 pagesThe Depth of Christ's LoveChino Paolo SamsonPas encore d'évaluation
- Cardiac ArrhythmiasDocument11 pagesCardiac ArrhythmiasChino Paolo SamsonPas encore d'évaluation
- Where Will We Hold OnDocument1 pageWhere Will We Hold OnChino Paolo SamsonPas encore d'évaluation
- Examination in Hematology: NameDocument1 pageExamination in Hematology: NameChino Paolo SamsonPas encore d'évaluation
- Long Term Safety AnalysesDocument3 pagesLong Term Safety AnalysesChino Paolo SamsonPas encore d'évaluation
- Fluid Blance SGDDocument11 pagesFluid Blance SGDChino Paolo SamsonPas encore d'évaluation
- Osce FormDocument2 pagesOsce FormChino Paolo SamsonPas encore d'évaluation
- Reproductive Endocrinology FinalDocument98 pagesReproductive Endocrinology FinalChino Paolo SamsonPas encore d'évaluation
- OB Chap 22 - Normal LaborDocument4 pagesOB Chap 22 - Normal LaborChino Paolo SamsonPas encore d'évaluation
- If I Am To Change A Negative Attitude of Mine, I Would Like To Change My Being - Why?Document3 pagesIf I Am To Change A Negative Attitude of Mine, I Would Like To Change My Being - Why?Chino Paolo SamsonPas encore d'évaluation
- What Is Hemolysis of Sample?Document3 pagesWhat Is Hemolysis of Sample?Chino Paolo Samson100% (1)
- Dr. Arif Gunawan Teguh WDocument64 pagesDr. Arif Gunawan Teguh WarifgteguhPas encore d'évaluation
- A Review On Extraction Isolation Characterization and Some Biological Activities of Essential Oils From Various PlantsDocument32 pagesA Review On Extraction Isolation Characterization and Some Biological Activities of Essential Oils From Various PlantsMisganaw KerebhPas encore d'évaluation
- Final Test Session 2 Professional BSN, 4 Year Programme Subject: Adult Health Nursing I Topic: Unit I (Gastrointestinal System)Document8 pagesFinal Test Session 2 Professional BSN, 4 Year Programme Subject: Adult Health Nursing I Topic: Unit I (Gastrointestinal System)You TuberPas encore d'évaluation
- 1 Surgery McqsDocument29 pages1 Surgery McqsSherlockHolmesSez50% (6)
- Overcoming Helicobacter Pylori NaturallyDocument130 pagesOvercoming Helicobacter Pylori NaturallyZaid AbdulqadirPas encore d'évaluation
- World Gastroenterology Organisation Global.5Document12 pagesWorld Gastroenterology Organisation Global.5kiki rizkiPas encore d'évaluation
- Tratament Helicobacter PyloriDocument9 pagesTratament Helicobacter PyloriFlavia ElenaPas encore d'évaluation
- Stomach Cancer Concept MapDocument1 pageStomach Cancer Concept MapNikkaDablio0% (1)
- Clinical Practice From Bench To Bedside - Is There A Great Divide by DR Marceliano T Aquino JRDocument25 pagesClinical Practice From Bench To Bedside - Is There A Great Divide by DR Marceliano T Aquino JRChristian ErelPas encore d'évaluation
- Lecture-PPI 20230226Document25 pagesLecture-PPI 20230226Mahadi Hasan KhanPas encore d'évaluation
- Molecules 25 05342 v2Document14 pagesMolecules 25 05342 v2CristianFrancoPas encore d'évaluation
- Care of Adults 27 Gastrointestinal ManagementDocument33 pagesCare of Adults 27 Gastrointestinal ManagementGaras AnnaBernicePas encore d'évaluation
- GastritisDocument3 pagesGastritisalicePas encore d'évaluation
- 02 Bont GastricDocument8 pages02 Bont GastricGabriela MilitaruPas encore d'évaluation
- NCMB316 Lec PrelimDocument25 pagesNCMB316 Lec PrelimErickson V. LibutPas encore d'évaluation
- Peptic Ulcer - Causes, Treatment, and PreventionDocument24 pagesPeptic Ulcer - Causes, Treatment, and PreventionAmfo Baffoe FrederickPas encore d'évaluation
- BiofilmDocument97 pagesBiofilmAshwin SinghPas encore d'évaluation
- Storage Mite Abstract EAACI-s552Document161 pagesStorage Mite Abstract EAACI-s552Özle SünmezPas encore d'évaluation
- GI 2007 Exam QuestionsDocument47 pagesGI 2007 Exam QuestionsRoh JitenPas encore d'évaluation
- Standard Guideline 2010 PDFDocument479 pagesStandard Guideline 2010 PDFLuvita Fitri KarinaPas encore d'évaluation
- GI Review For USMLE Step 1Document3 pagesGI Review For USMLE Step 1mojdaPas encore d'évaluation
- Helicobacter Pylori Infection and TreatmentDocument3 pagesHelicobacter Pylori Infection and Treatmentto van quyenPas encore d'évaluation
- Ue Gen PathologyDocument287 pagesUe Gen PathologyReza RastgooPas encore d'évaluation
- How To Describe Research Contribution For WebsiteDocument2 pagesHow To Describe Research Contribution For WebsiteHumayun KhalidPas encore d'évaluation
- Chapter One: Helicobacter Pylori, Previously Named Campylobacter Pyloridis, Is A Gram-NegativeDocument24 pagesChapter One: Helicobacter Pylori, Previously Named Campylobacter Pyloridis, Is A Gram-NegativeDaniel GarbaPas encore d'évaluation
- Peptic Ulcer DiseaseDocument3 pagesPeptic Ulcer DiseaseleahraizaPas encore d'évaluation
- Treatment of Iron Deficiency Anemia in Adults - UpToDateDocument82 pagesTreatment of Iron Deficiency Anemia in Adults - UpToDateSantiago MayorPas encore d'évaluation
- Difference Between GERD and PUDDocument7 pagesDifference Between GERD and PUDOla Adel ShabeebPas encore d'évaluation
- Peptic Ulcer Nursing Case StudyDocument50 pagesPeptic Ulcer Nursing Case Studygideon A. owusu100% (1)
- Moringa OleiferaDocument25 pagesMoringa OleiferaGeramy JavierPas encore d'évaluation