Académique Documents
Professionnel Documents
Culture Documents
Bases Neurales de La Empatia
Transféré par
Gonzalo GVCopyright
Formats disponibles
Partager ce document
Partager ou intégrer le document
Avez-vous trouvé ce document utile ?
Ce contenu est-il inapproprié ?
Signaler ce documentDroits d'auteur :
Formats disponibles
Bases Neurales de La Empatia
Transféré par
Gonzalo GVDroits d'auteur :
Formats disponibles
ORIGINAL CONTRIBUTION
Cognitive Profiles of Autopsy-Confirmed Lewy Body
Variant vs Pure Alzheimer Disease
Donald J. Connor, PhD; David P. Salmon, PhD; Teresa J. Sandy, BS; Douglas Galasko, MD;
Lawrence A. Hansen, MD; Leon J. Thal, MD
Objective: To compare the cognitive profiles of pa- Initiation/Perseveration subscale (P,.02). The groups did
tients with autopsy-confirmed Alzheimer disease (AD), not differ significantly on the Attention, Construction, or
with or without concomitant Lewy bodies, on 2 demen- Conceptualization subscales. The same overall pattern of
tia screening measures. results was obtained when subgroups with mild to mod-
erate and moderate to severe dementia were examined sepa-
Methods: Profiles on subtests of the Mattis Dementia rately, with the additional finding that in the mild-to-
Rating Scale (range, 105-125) and of component items moderate range patients with dementia and LBV performed
of the Mini-Mental State Examination were compared be- worse than patients with pure AD on the Construction
tween 23 patients with uncomplicated AD and 23 pa- subscale.
tients with concomitant AD and Lewy body pathology
(Lewy body variant [LBV]). Conclusions: The difference in pattern of cognitive defi-
cits among patients with pure AD vs those with LBV is
Results: Although the groups did not differ significantly similar to that seen between AD and more subcortical/
regarding age, years of education, total Mini-Mental State frontal dementias (eg, Huntington disease). This sug-
Examination score, or total Mattis Dementia Rating Scale gests that the concomitant Lewy body pathology signifi-
score, the AD group performed significantly worse than the cantly contributes to the presentation of the cognitive
LBV group on the Mattis Dementia Rating Scale Memory dysfunction in individuals with LBV.
subscale (P,.005). In contrast, the LBV group demon-
strated poorer performance than the pure AD group on the Arch Neurol. 1998;55:994-1000
D
EMENTIA WITH Lewy bod- pure AD. Lewy bodies in LBV occur both
ies 1 is a recently de- neocortically and in the more common
scribed condition in subcortical distribution (substantia ni-
which autopsy examina- gra, locus ceruleus, substantia innomi-
tion of the brain of pa- nata, and dorsal vagus nucleus) typically
tients with dementia reveals diffusely dis- associated with Parkinson disease.4-8 Clini-
tributed cortical and subcortical Lewy cally, both patients with dementia with
bodies. While some of these patients are Lewy bodies and LBV present with a pro-
found to possess only Lewy body pathol- gressive dementia and often develop mild
ogy, most have concomitant Alzheimer dis- extrapyramidal motor dysfunction (eg,
ease (AD) pathologic features. Those pa- bradykinesia, rigidity, or masked facies)
tients with dementia and Lewy bodies who and hallucinations4,8,9 early in the course
also manifest sufficient AD pathologic fea- of the disease. The pattern of cognitive defi-
tures to satisfy the National Institute on cits engendered by LBV is similar to that
Aging autopsy criteria for AD2 and crite- of AD in some respects, but a number of
ria from the Consortium to Establish a Reg- specific features distinguish the 2 groups.
istry for Alzheimer’s Disease for either Although patients with LBV and AD ex-
“definite” or “probable” AD3 are referred hibit similar deficits in memory and con-
to as having the Lewy body variant (LBV) frontation naming, preliminary stud-
of AD.4 While senile plaque distribution ies10-12 have indicated that patients with
From the Department of in LBV is similar to that in pure AD, neo- prominent Lewy body burden display dis-
Neurosciences, University of cortical neurofibrillary tangles are absent proportionately severe deficits in atten-
California, San Diego, La Jolla, or rare, and entorhinal and hippocampal tion, fluency, and visuospatial process-
and the Alzheimer’s Disease tangle counts are intermediate between ing. As Hansen and colleagues4 suggest,
Research Center, San Diego. those of elderly controls and patients with patients with LBV appear to exhibit a com-
ARCH NEUROL / VOL 55, JULY 1998
994
Downloaded from www.archneurol.com on June 22, 2010
©1998 American Medical Association. All rights reserved.
PATIENTS AND METHODS Only data from the patients’ initial ADRC evaluation were
used in the analysis.
PATIENTS The MDRS is a standardized, 144-point mental status
examination that consists of 5 subscales that assess Atten-
Twenty-three patients with autopsy-confirmed LBV and 23 tion (37 points), Initiation/Perseveration (37 points), Con-
patients with autopsy-confirmed AD, all of whom were di- struction (6 points), Conceptualization (39 points), and
agnosed as having dementia at the time of their initial clini- Memory (25 points). The MDRS was administered accord-
cal evaluation, were included in the current study. All pa- ing to the standard procedures24 with the exception that
tients had been participants in the University of California, all items were administered to all patients.
San Diego Alzheimer’s Disease Research Center (UCSD/ The MMSE is a standardized, 30-point scale that
ADRC) in San Diego through which they received yearly encompasses 11 component items: orientation to time (5
physical, neurologic, and neuropsychological assessments. points), orientation to place (5 points), word registration
Written informed consent for participation in the UCSD/ (3 points), serial subtraction or backward spelling (5
ADRC longitudinal study was obtained from all patients (or points), word recall (3 points), naming (2 points), repeti-
their conservators) after the procedures of the study had been tion (1 point), following commands (3 points), reading (1
fully explained. Informed consent for autopsy was obtained point), writing (1 point), and copying a figure (1 point).
from the next of kin immediately after the patient’s death. Both the backward spelling of world and serial subtraction
Three of 23 patients with LBV and 1 of the patients with AD (7’s from 100) were administered to all patients and the
were from the original study by Hansen et al.4 best performance of the 2 items was included in the total
The procedures that were used to prepare and histo- MMSE score.
logically analyze the brains of the patients have been de-
scribed in detail previously.4 The neuropathologic diagnosis STATISTICAL ANALYSIS
was made according to both the criteria suggested by the Na-
tional Institute on Aging and the Consortium to Establish a The scores achieved by the patients with AD and LBV on
Registry for Alzheimer’s Disease criteria for definite or prob- the subscales of the MDRS were compared using multi-
able AD. The neuropathologic diagnosis of LBV required sat- variate analysis of variance with planned post hoc com-
isfaction of the National Institute on Aging and the Consor- parisons using the Fisher least significant difference test.
tium to Establish a Registry for Alzheimer’s Disease criteria Subscales demonstrating significant differences between
for AD, as well as the presence of subcortical and cortical Lewy patients with AD and LBV were submitted for individual
bodies (see Hansen and Samuel26 for detailed diagnostic and item analysis using the Mann-Whitney U test. Since this
nosologic review of LBV). Braak stage was established by de- group represents a broad range of cognitive impairment,
gree and spread of neurofibrillary tangle formation.27 additional exploratory analyses using multivariate analy-
The patients with LBV and AD selected for our study sis of variance were performed separately for patients
were pair matched in terms of level of dementia (MDRS to- with mild to moderate (MDRS score, 106-125) and mod-
tal score), age, and years of education at the time of their ini- erate to severe (MDRS score, 80-105) dementia (ie,
tial ADRC evaluation. The MDRS scores of the patients with SD < − 2.0 to 4.5 and SD < − 4.6 to 8.3, respectively,
LBV and AD ranged from 80 to 125 of a possible 144 points. from the mean normal control score as reported in the
Matching on the MDRS total score was performed to ensure MDRS manual).28
that any differences in group subtest profiles could be attrib- The MDRS subscale scores of the patients with LBV
uted to differences in the underlying nature of the 2 disor- and AD were submitted to a discriminate function equa-
ders, rather than to differences in global level of dementia. tion that has been shown to effectively discriminate be-
The MDRS total score is a more refined staging measure of tween patients with AD and patients with HD.14 Correctly
dementia than the MMSE score, and matching on MMSE score and incorrectly classified patients were compared on de-
can result in significant differences in the total MDRS score mographic variables, time from assessment to death, and
that would confound interpretation of the MDRS subscale pro- Braak stage of AD pathologic progression post mortem. A
files. While this matching causes some interdependence be- new discriminant function analysis using the MDRS sub-
tween the subscales, it does not preclude examination of dif- scale scores of patients with AD and LBV was also con-
ferent subscale profiles at equivalent levels of dementia. ducted to derive an equation that might optimally differ-
However, caution must be used in interpreting what spe- entiate between patients with AD and LBV. The latter
cific cognitive abilities are differentially affected by the pres- analysis should be considered exploratory because of the
ence of the additional cortical and subcortical Lewy body bur- small sample size and ultimately must be validated with a
den (see the “Comment” section). larger sample.
The scores achieved by patients with LBV and AD on
PROCEDURE the 11 component items of the MMSE were compared us-
ing the nonparametric Mann-Whitney U test for continu-
The MDRS24 and the MMSE25 were administered to each ous measures or the x2 test for dichotomous measures as
patient as part of a larger neuropsychological evaluation. appropriate.
bination of cortical and subcortical neuropsychological evaluation.13-15 Typically, patients with AD, a prototypi-
dysfunction. cal cortical dementia, present with severe memory im-
Progressive dementing disorders that involve pre- pairment with additional deficits in language (ie, ano-
dominantly cortical (eg, AD) or subcortical (eg, Hunting- mia), verbal fluency, abstract reasoning, and visuospatial
ton disease [HD]) neurodegeneration manifest distinct pat- abilities.15-17 In contrast, patients with HD, a typical sub-
terns of cognitive deficits on detailed neuropsychological cortical dementia, usually demonstrate impaired atten-
ARCH NEUROL / VOL 55, JULY 1998
995
Downloaded from www.archneurol.com on June 22, 2010
©1998 American Medical Association. All rights reserved.
100
Table 1. Demographics and Level of Dementia* AD
LBV
AD LBV
80
Percent of Maximum Subscale Score
(n = 23) (n = 23) P
∗ ∗∗
Age, y 76.7 (5.7) 75.9 (5.2) .61
Education, y 13.4 (3.0) 12.7 (2.7) .43
60
Mattis Dementia Rating Scale score 104.5 (13.3) 104.7 (13.0) .90
Mini-Mental State Examination score 18.6 (4.2) 19.5 (4.0) .46
Time from cognitive evaluation to death, y 3.88 (1.6) 3.37 (1.7) .30
40
*Values are mean (SD). AD indicates Alzheimer disease; LBV; Lewy body
variant.
20
tion, slowed cognitive processes, severe verbal fluency
deficits, and a relatively moderate memory impair-
ment.18-20 These distinct patterns of cognitive deficits are 0
Attention Initiation/ Construction Conceptualization Memory
robust and have been detected even on brief, standard- Perseveration
Subscale
ized mental status examinations.21-23 In view of the some-
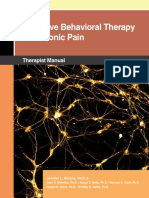
what disparate nature of the cognitive deficits exhibited Figure 1. Mean (SEM) percentage of the maximum possible score on each
subtest of the Mattis Dementia Rating Scale for patients with Alzheimer
by patients with AD and LBV on detailed neuropsycho- disease (AD) or the Lewy body variant (LBV). The groups differed
logical testing, it may be the case that these groups could significantly only on the Initiation/Perseveration and Memory subscales.
be distinguished by their patterns of performance on men- Asterisk indicates P,.05; double asterisk, P,.01.
tal status examinations that have been shown to discrimi-
nate between patients with cortical and subcortical de- cal interview. A significantly higher proportion of pa-
mentia syndromes. That is, since patients with LBV appear tients with AD (18 of 20) than with LBV (8 of 20) achieved
to have a significant subcortical component to their cog- a Braak stage of 4 or higher, indicative of notable corti-
nitive dysfunction, aspects of their performance on men- cal neurofibrillary tangles formation.
tal status tests may resemble those of patients with HD
or Parkinson disease. MATTIS DEMENTIA RATING SCALE
To address this issue, our study compared the per-
formances of patients with autopsy-confirmed LBV and Multivariate analysis of variance revealed that the pat-
pure AD on the Mattis Dementia Rating Scale24 (MDRS) terns of performance of the LBV and AD groups on the
and the Mini-Mental State Examination25 (MMSE). Pa- subscales of the MDRS were significantly different
tients with LBV and AD were matched on overall level (P,.002). Post hoc comparisons of performance on the
of dementia, and their patterns of performance on the 5 individual subscales (Fisher least significant difference
MDRS subscales were compared. To determine whether test) showed that patients with LBV scored significantly
the subcortical component of the cognitive dysfunction higher than patients with AD on the Memory subscale
of patients with LBV is prominent enough to affect their (mean ± SD scores: AD, 10.8 ± 4.2; LBV, 15.3 ± 4.4;
classification as “cortical” or “subcortical,” the MDRS sub- P,.001) but significantly lower on the Initiation/
scale scores of both groups were submitted to discrimi- Perseveration subscale (mean ± SD scores: AD, 25.2 ± 5.0;
nant equations that have been shown to effectively dif- LBV, 21.0 ± 5.9; P,.02). The groups did not differ sig-
ferentiate between patients with AD and HD.22 Since these nificantly on the Attention, Construction, or Conceptu-
groups represent a broad range of cognitive impair- alization measures. The different patterns of perfor-
ment, the MDRS profiles of patients with AD and LBV mance produced by the 2 patient groups are presented
were also analyzed over a mild-moderate and a moderate- in Figure 1. To facilitate comparison across the subs-
severe range of dementia. Finally, the performance of pa- cales, the scores are presented as a percentage of each sub-
tients with LBV and AD was compared on the compo- scale’s maximum possible score.
nents of the MMSE. This comparison was limited to The performance of patients with LBV and pure AD
patients with MMSE scores of 14 to 25, since this range on the individual items of the MDRS Memory subscale
of dementia has been shown to be most conducive to dis- is shown in Table 2. Patients with AD scored signifi-
criminating between patients with AD and HD with this cantly lower than patients with LBV on the orientation
task.21 items (P,.01), on 1 of the free recall measures (sen-
tence 1; P,.001), and marginally lower on the second
RESULTS recall measure (self-generated sentence; P,.06). The
groups did not differ significantly on the word or design
Mean age, years of education, MDRS score, MMSE score, recognition items.
and time from evaluation to death for the 2 patient groups Table 2 also presents the performance of patients with
are presented in Table 1. As expected from the match- LBV and AD on the individual items of the Initiation/
ing procedure, the LBV and AD groups did not differ sig- Perseveration subscale. Although the mean scores of pa-
nificantly on any of the demographic features or overall tients with LBV were lower than those of patients with
level of dementia. Three patients with AD and 3 with LBV AD on each item, the groups differed significantly only
demonstrated significant depressive symptoms on clini- on the clothing-naming item (P,.01) that required gen-
ARCH NEUROL / VOL 55, JULY 1998
996
Downloaded from www.archneurol.com on June 22, 2010
©1998 American Medical Association. All rights reserved.
AD
Table 2. Individual Items of the Memory and
Initiation/Perseveration Subscales* 100 ∗ LBV
Possible ∗ ∗∗
Subscale Item AD LBV P Scale Range 80
Memory Subscale
Dog sentence 0.3 (0.56) 1.7 (1.43) ,.001 0-4
Own sentence 0.5 (1.08) 1.2 (1.37) .06 0-3 60
Orientation 3.0 (2.22) 4.8 (2.15) .01 0-9
Word recognition 4.0 (1.13) 4.1 (1.24) .70 0-5
Design recognition 3.5 (0.85) 3.6 (0.66) .70 0-4 40
Initiation/Perseveration Subscale
Supermarket 10.2 (3.89) 8.2 (4.89) .12 0-20
Percent of Maximum Subscale Score
Clothing 7.2 (1.30) 5.9 (1.89) .01 0-8 20
Repetition 1.9 (0.29) 1.7 (0.56) .10 0-2
Alternating 2.6 (0.78) 2.2 (0.81) .15 0-3
Graphomotor 3.3 (1.02) 2.9 (1.04) .20 0-4
0
Attention Initiation/ Construction Conceptualization Memory
*Values are mean (SD). AD indicates Alzheimer disease; LBV; Lewy body Perseveration
100
variant.
80
erating the names of articles of clothing, including those
that the patient was wearing. Although performance on ∗
∗
the graphomotor component of the Initiation/ 60
Perseveration subscale was not different for the 2 pa-
tient groups, a greater proportion of patients with LBV
than with AD failed the most difficult item of that com- 40
ponent (65% vs 30%, respectively; x2 = 5.6; P,.02), copy-
ing alternating figures presented in a ramparts or saw-
tooth design. 20
Subgroup With Mild to Moderate Dementia
0
The performances of patients with mild to moderate de- Attention Initiation/ Construction Conceptualization Memory
Perseveration
mentia (LBV score, mean ± SD MDRS, 116 ± 5.5; n = 11; Subscale
and AD score, mean ± SD MDRS, 115 ± 7.5; n = 11) on Figure 2. Mean (SEM) percentage of the maximum possible score on each
the subscales of the MDRS are presented in Figure 2 subtest of the Mattis Dementia Rating Scale for patients with Alzheimer
(top). The scores are presented in terms of the percent- disease (AD) or the Lewy body variant (LBV) with mild dementia (top) and
moderate dementia (bottom). Asterisk indicates P,.05; double asterisk,
age of the maximum possible score that could be achieved P,.01.
on each subscale. Overall multivariate analysis of vari-
ance revealed that the patterns of performance of the 2
groups were not significantly different (P..10). How- post hoc comparisons revealed that patients with LBV
ever, planned post hoc comparisons showed that pa- scored significantly lower than patients with AD on the
tients with LBV scored significantly worse than patients Initiation/Perseveration subscale (mean ± SD scores: AD,
with AD on the Initiation/Perseveration (mean ± SD scores: 22.1 ± 4.0; LBV, 17.8 ± 5.3; P,.04), but significantly
AD, 28.5 ± 3.8; LBV, 24.5 ± 4.4; P,.04) and Construc- higher on the Memory subscale (mean ± SD scores: AD,
tion (mean ± SD scores: AD, 5.5 ± 0.7; LBV, 4.3 ± 1.4; 9.2 ± 2.3; LBV, 13.2 ± 4.7; P,.02). The groups did not dif-
P,.02) subscales. In contrast, patients with AD scored fer significantly on any other of the MDRS subscales.
significantly lower than patients with LBV on the Memory
subscale (mean ± SD scores: AD, 12.5 ± 5.1; LBV, DISCRIMINANT FUNCTION ANALYSIS
17.6 ± 2.7; P,.01). The groups did not differ signifi-
cantly on the Attention or Conceptualization subscales. To determine if the MDRS subscale profiles of patients
with LBV and AD in this study were more typical of a
Subgroup With Moderate to Severe Dementia cortical or subcortical dementia, their subscale scores were
submitted to a discriminant equation using coefficients
Figure 2 (bottom) also shows the performances of pa- previously derived from a linear discriminant function
tients with moderate to severe dementia (LBV, mean ± SD analysis comparing the MDRS subscale scores of pa-
MDRS score, 95 ± 9.0; n = 12; and AD, mean ± SD MDRS tients with AD vs HD.22 Seventeen (74%) of 23 patients
score, 95 ± 9.1; n = 12) on the MDRS subscales. As with the with AD were correctly classified as having cortical de-
full group data, multivariate analysis of variance showed mentia by the discriminant equation, whereas only 9
that the groups produced significantly different patterns (40%) of 23 patients with LBV were classified as having
of performance on the MDRS subscales (P,.02). Planned cortical dementia.
ARCH NEUROL / VOL 55, JULY 1998
997
Downloaded from www.archneurol.com on June 22, 2010
©1998 American Medical Association. All rights reserved.
100 ability of group membership, the resulting equation,
AD ∗ ∗
LBV Classification = 0.154 (Attention) − 0.101 (Construction)
+ 0.040 (Conceptualization) − 0.162 (Initiation) + 0.191
80
Percent of Maximum Component Score
(Memory) − 4.75
∗∗
correctly classified 82% of patients with LBV and 78%
60 of patients with AD (canonical r = 0.64; P,.001; overall
classification rate, 80%). When the 5 subscales were en-
tered in a stepwise fashion, only the Memory and Initia-
40 tion/Perseveration subscales were maintained in the sig-
∗ nificant discriminant function,
Classification = 0.212 (Memory Score) − 0.137
20
(Initiation/Perseveration Score) + 0.391
These 2 variables alone were able to correctly classify 78%
0 of the autopsy-verified patients with LBV and 74% of pa-
Date Place Register World Recall Name Repeat Commands Read Write Copy
tients with pure AD (canonical r = 0.61; P,.001; overall
Component
classification rate, 76%).
Figure 3. Mean (SEM) percentage of the maximum possible score obtained
on individual components of the Mini-Mental State Examination for the MINI-MENTAL STATE EXAMINATION
patients with Alzheimer disease (AD) or the Lewy body variant (LBV).
Asterisk indicates P,.05; double asterisk, P,.01.
The performances of patients with LBV (n = 13) and AD
(n = 13) (MMSE scores, 14-25) on the individual com-
Patients with AD classified as having subcortical de- ponents of the MMSE are presented in Figure 3. Scores
mentia (eg, HD-like) and patients with LBV classified as are presented in terms of the percentage of the total pos-
having cortical dementia (eg, AD-like) were not signifi- sible points achieved for each item. Patients with LBV
cantly different regarding demographics (age, education, scored significantly lower than patients with AD on the
or sex distribution) or level of dementia (as assessed by memory registration (P,.05) and writing (P,.05) com-
MMSE and MDRS total scores) from the correctly classi- ponents, whereas patients with AD scored significantly
fied patients in their respective neuropathologically de- lower than patients with LBV on the temporal orienta-
fined groups. However, patients with LBV classified as hav- tion (date; P,.005) and free recall (3 words; P,.02) items.
ing an AD-like or cortical-like dementia had greater cortical
AD-type neurofibrillary tangle pathologic features (Braak COMMENT
stage $4; x2 = 4.4; P,.04) than patients with LBV classi-
fied as having subcortical dementia. That is, those pa- In this study, patients with autopsy-confirmed LBV and
tients with LBV with significant cortical infiltration of neu- pure AD were differentiated by their performance on a
rofibrillary tangles were more often classified as having AD simple dementia screening instrument (MDRS). Al-
than those with tangles largely confined to the medial tem- though matched for overall level of dementia, patients
poral lobe. This greater degree of AD pathologic features with AD performed worse than patients with LBV on the
in patients with LBV who were classified as having corti- Memory subscale, whereas patients with LBV per-
cal dementia is not simply a reflection of their having been formed relatively worse than patients with AD on the Ini-
tested at a more advanced stage of the disease than the other tiation/Perseveration subscale. This pattern is similar to
patients with LBV, since time from neuropsychological as- that found in previous studies22,23 comparing patients with
sessment to death was not different for the 2 subgroups AD and HD, in which patients with AD were more im-
(analysis of variance, P..30). Conversely, patients with AD paired than patients with HD on the Memory subscale
misclassified as having subcortical dementia did not differ of the MDRS, but less impaired on the Initiation/
in Braak stage (x2 = −0.95; P..30) from the correctly clas- Perseveration subscale. Rosser and Hodges29 recently rep-
sified patients with AD. The ability of the original AD vs licated this finding and demonstrated that patients with
HD discriminant function to differentiate patients with AD progressive supranuclear palsy exhibit a pattern of defi-
vs LBV was improved by adjusting the constant (from 8.2 cits on the MDRS subscales identical to that of patients
to 7.02), a procedure that shifts the cutoff point to com- with HD. Similarly, patients with Parkinson disease who
pensate for differences in degree of separation while keep- were equated to patients with AD in total MDRS score
ing the relative pattern of variables that define the groups performed better than the patients with AD on the
intact. This optimally adjusted discriminant function cor- Memory subscale, but worse on the Construction subs-
rectly classified 70% of patients with AD as having corti- cale.30 Therefore, the cognitive deficits of patients with
cal dementia and 87% of patients with LBV as having sub- LBV appear to express characteristics of both subcorti-
cortical dementia. cal and cortical dysfunction.
A new linear discriminant function analysis was per- The possible subcortical contribution to the cogni-
formed to explore the maximal classification rate using tive deficits of patients with LBV was further demon-
the results of the MDRS profile in the present sample. strated by the finding that 60% of these patients were clas-
As in previous studies, all 5 subscales were forced into sified as having subcortical dementia when their MDRS
the discriminant function analysis. With equal prior prob- subscale scores were submitted to a discriminant func-
ARCH NEUROL / VOL 55, JULY 1998
998
Downloaded from www.archneurol.com on June 22, 2010
©1998 American Medical Association. All rights reserved.
tion that had been previously used to differentiate be- mild to moderate dementia range, patients with LBV were
tween patients with AD (cortical) vs HD (subcortical).22 more impaired than patients with AD on the Construc-
In contrast, only 26% of patients with AD in our study tion subscale. This latter finding is consistent with the
were classified as having the HD-like pattern using these finding of poorer Construction subscale performance in
same discriminant equations. The significant improve- patients with Parkinson disease than in patients with AD,30
ment in LBV group classification (from 60% to 87%) with and with studies4,11 that have demonstrated visuospatial
only a minimal loss in correct AD classification (from 74% and constructional deficits in patients with LBV. The ab-
to 70%) following adjustment of the coefficient is con- sence of this difference in the group with moderate to
sistent with the proposition that patients with LBV are severe dementia appears to be due to the increased con-
more likely to manifest an HD-like frontal/subcortical pat- structional deficits of the more impaired patients with
tern on the MDRS compared to patients with AD. Al- AD. Interestingly, one of the most difficult items from
though the observed degree of classification is far from the Initiation/Perseveration subscale that taps both con-
perfect, it is impressive considering that the brains of in- structional and executive abilities (ie, copying the ram-
dividuals with LBV contain significant AD pathologic fea- parts figure) was significantly more impaired in pa-
tures, and in light of the fact that the original AD vs HD tients with LBV than with pure AD across the full MDRS
discriminant function was based on a sample clinically range.
diagnosed as having AD, which most likely included some Comparison of the performance of patients with
patients with LBV (since about 15%-20% of patients clini- AD vs LBV on a more abbreviated screening instrument
cally diagnosed as having AD are found at autopsy to have (MMSE) yielded results that were similar to those re-
had LBV). This possible contamination in the AD vs HD ported for patients with AD and HD matched on total
discriminant function may have contributed to the MMSE score.21 In the study by Brandt et al,21 patients
poorer classification of the patients with pure AD in our with AD were more impaired than those with HD in free
study compared with the AD vs HD study (AD correct, recall (recalling 3 words after a 5-minute delay) and ori-
74% vs 82%).22 entation (date), whereas patients with HD were more
impaired than patients with AD in counting backward
from 100 by 7’s and (in the MMSE total score, 15-19
A
NEW DISCRIMINANT function analysis also range) memory registration and writing items. In our
effectively distinguished patients with AD study, patients with AD performed worse than patients
and LBV in this study. Despite the high with LBV on the free recall and orientation items,
degree of shared neuropathologic fea- whereas patients with LBV performed worse than pa-
tures in the 2 disorders, 78% of patients tients with AD on the memory registration and writing
with AD and 82% of patients with LBV were correctly items. Despite these significant differences between pa-
classified with this discriminant function equation. As tients with AD and LBV, there are several factors that
would be expected from the multivariate analysis of vari- limit the significance of the results. The difference
ance, most of the power of this equation came from the found on the recall item, for example, is confounded by
Initiation/Perseveration and Memory subscales, which by the fact that none of the patients with AD, and only 5 of
themselves were able to correctly classify approxi- the 13 patients with LBV were able to recall any of the 3
mately 76% of all patients. However, these results must words. In addition, our study failed to find the differ-
remain tentative until the equation can be validated with ence between groups on the serial subtraction item that
larger, independent, autopsy-verified groups of patients was noted previously in the AD vs HD study. This may
with AD and LBV. be due to a procedural difference, since our study ac-
Although analysis of individual items within a sub- cepted the highest score from either the serial subtrac-
scale must be approached with caution since they may tion or backward spelling items, while the AD vs HD
represent divergent qualities, exploratory analyses indi- study21 only used the serial subtraction item. Finally,
cated that patients with AD were relatively more im- the small sample size in our study (n = 13 per group),
paired than patients with LBV on the Memory subs- and the restricted range of scores for the instrument,
cale’s orientation and free recall items, but not on the precludes any definitive conclusion about differences
recognition task. That patients with LBV did not show between patients with LBV and AD on the individual
the disproportionate improvement with recognition test- components of the MMSE. Despite these limitations,
ing often observed in patients with a purely subcortical the pattern of results obtained with the MMSE is con-
dementia syndrome31,32 is not surprising, since both groups sistent with the hypothesis that subcortical disfunction
performed near maximum on the recognition test (ceil- significantly influences the cognitive performance of
ing effect). Performance on the individual items of the patients with LBV.
Initiation/Perseveration subscale revealed few consis- In conclusion, the different patterns of perfor-
tent or theoretically interpretable differences between pa- mance on 2 different standardized screening devices for
tients with AD and LBV. dementia (MDRS and MMSE) produced by patients with
Analyses examining the pattern of MDRS perfor- autopsy-verified AD and LBV are consistent with find-
mance in patients with LBV and AD with mild to mod- ings from preliminary studies using a more extensive bat-
erate dementia and moderate to severe dementia dem- tery of neuropsychological tests,4 and similar to the pat-
onstrated that the dissociation between the groups on the tern of differences that have been observed between
Memory and Initiation/Perseveration subscales was main- patients with AD and HD. That is, despite the fact that
tained across both ranges of severity. In addition, in the patients with LBV share much of the same underlying
ARCH NEUROL / VOL 55, JULY 1998
999
Downloaded from www.archneurol.com on June 22, 2010
©1998 American Medical Association. All rights reserved.
neuropathologic features as patients with pure AD, the 10. Galloway PH, Sahgal A, McKeith IG, et al. Visual pattern recognition memory and
learning deficits in senile dementias of Alzheimer and Lewy body types. Demen-
Lewy body burden can influence the pattern of cogni-
tia. 1992;3:101-107.
tive deficits observed, especially in the early stages of the 11. Sahgal A, McKeith IG, Galloway PH, Tasker N, Steckler T. Do differences in vi-
disease before the AD neuropathologic damage be- suospatial ability between senile dementias of the Alzheimer and Lewy body types
comes predominant. While these differences in subs- reflect differences solely in mnemonic function? J Clin Exp Neuropsychol. 1995;
cale profiles were significant, they were also relatively 17:35-43.
12. Salmon DP, Galasko D. Neuropsychological aspects of Lewy body dementia. In:
small and may be of limited clinical utility when applied
Perry EK, Perry RH, McKeith I, eds. Lewy Body Dementia. New York, NY: Cam-
to individual patients. Furthermore, these results need bridge University Press; 1996:99-113.
to be replicated with larger, independent, autopsy- 13. Albert ML, Feldman RG, Willis AL. The “subcortical dementia” of progressive su-
verified cohorts to establish their validity and reliabil- pranuclear palsy. J Neurol Neurosurg Psychiatry. 1974;37:121-130.
ity. Despite these limitations, the results indicate that re- 14. Cummings JL. Subcortical Dementia. New York, NY: Oxford University Press Inc;
1990.
search investigating the nature of the cognitive deficits
15. Bondi MW, Salmon DP, Butters N. Neuropsychological features of memory dis-
in patients with AD and other dementing disorders should orders in dementia of the Alzheimer type. In: Terry RD, Katzman R, Bick KL, eds.
take the existence of concomitant Lewy body patho- Alzheimer’s Disease. New York, NY: Raven Press; 1994:41-63.
logic features into account. 16. Corkin S, David KL, Growdon JH, Usdin E, Wurtman RJ. Alzheimer’s Disease: A
Report of Progress in Research. Vol 19. New York, NY: Raven Press; 1982.
17. Bayles KA, Kaszniak AW. Communication and Cognition in Normal Aging and
Accepted for publication January 6, 1998.
Dementia. Boston, Mass: Little Brown & Co Inc; 1987.
This study was supported in part by a National Re- 18. Brandt J, Butters N. The neuropsychology of Huntington’s disease. Trends Neu-
search Service Award (NS-09515) from the National Insti- rosci. 1986;9:118-120.
tute of Neurological Disorders and Stroke (Dr Connor), 19. Butters N, Sax DS, Montgomery K, Tarlow S. Comparison of the neuropsycho-
grants AG-12963 and AG-05131 from the National Insti- logical deficits associated with early and advanced Huntington’s disease. Arch
Neurol. 1978;35:585-589.
tute on Aging, Bethesda, Md, and a grant from the state of
20. Folstein SE, Brandt J, Folstein MF. Huntington’s disease. In: Cummings JL, ed.
California (Alzheimer’s Disease Diagnostic and Treat- Subcortical Dementia. New York, NY: Oxford University Press Inc; 1990:87-
ment Center). 107.
We gratefully acknowledge our colleague Nelson 21. Brandt J, Folstein SE, Folstein MF. Differential cognitive impairment in Alzhei-
Butters, PhD, for his participation in the conceptualization mer’s disease and Huntington’s disease. Ann Neurol. 1988;23:555-561.
22. Salmon DP, Kwo-on-Yuen PF, Heindel WC, Butters N, Thal LJ. Differentiation of
of the study and the interpretation of the results.
Alzheimer’s disease and Huntington’s disease with the Dementia Rating Scale.
Reprints: Donald J. Connor, PhD, Alzheimer’s Dis- Arch Neurol. 1989;46:1204-1208.
ease Research Center (0948), 9500 Gilman Dr, University 23. Paulsen JS, Butters N, Sadek JR, et al. Distinct cognitive profiles of cortical and
of California, San Diego, La Jolla, CA 92093-0948. subcortical dementia in advanced illness. Neurology. 1995;45:951-956.
24. Mattis S. Mental status examination for organic mental syndrome in the elderly
patient. In: Bellak L, Karasu TB, eds. Geriatric Psychiatry: A Handbook for Psy-
REFERENCES chiatrists and Primary Care Physicians. New York, NY: Grune & Stratton Inc; 1976:
77-121.
1. McKeith IG, Galasko D, Kosaka K, et al. Consensus guidelines for the clinical and 25. Folstein MF, Folstein SE, McHugh, PR. “Mini-Mental State”: a practical method
pathologic diagnosis of dementia with Lewy bodies (DLB). Neurology. 1996;47: for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;
1113-1124. 12:189-198.
2. Khachaturian ZS. Diagnosis of Alzheimer’s disease. Arch Neurol. 1985;42:1097- 26. Hansen LA, Samuel W. Criteria for Alzheimer’s disease and the nosology of de-
1105. mentia with Lewy bodies. Neurology. 1997;48:126-132.
3. Mirra SS, Hart MN, Terry RD. Making the diagnosis of Alzheimer’s disease: a 27. Braak H, Braak E. Neuropathological staging of Alzheimer related changes. Acta
primer for practicing pathologists. Arch Pathol Lab Med. 1993;117:132-144. Neuropathol. 1991;82:239-259.
4. Hansen L, Salmon DP, Galasko D, et al. The Lewy body variant of Alzheimer’s 28. Mattis S. Dementia Rating Scale: Profession Manual. Odessa, Fla: Psychologi-
disease: a clinical and pathologic entity. Neurology. 1990;40:1-8. cal Assessment Resources Inc; 1988.
5. Gibb WRG, Esiri MM, Lees AJ. Clinical and pathological features of diffuse cor- 29. Rosser AE, Hodges JR. The Dementia Rating Scale in Alzheimer disease, Hun-
tical Lewy body disease (Lewy body dementia). Brain. 1985;110:1131-1153. tington’s disease and progressive supranuclear palsy. J Neurol. 1994;241:531-
6. Byrne EJ, Lennox G, Lowe J, Godwin-Austen RB. Diffuse Lewy body disease: 536.
clinical features in 15 cases. J Neurol Neurosurg Psychiatry. 1989;52:709-717. 30. Paolo AM, Troster AI, Glatt S, Hubble JP, Koller WC. Differentiation of the de-
7. Hansen LA, Galasko D. Lewy body disease. Curr Opin Neurol Neurosurg. 1992; mentias of Alzheimer’s and Parkinson’s disease with the Dementia Rating Scale.
5:889-894. J Geriatr Psychiatry Neurol. 1995;8:184-188.
8. Perry RH, Irving D, Blessed G, Fairbairn A, Perry EK. Senile dementia of the Lewy 31. Butters N, Wolfe J, Martone M, Granholm E, Cermak LS. Memory disorders as-
body type: a clinically and neuropathologically distinct form of Lewy body de- sociated with Huntington’s disease: verbal recall, verbal recognition and proce-
mentia in the elderly. J Neurol Sci. 1990;95:119-139. dural memory. Neuropsychologia. 1985;23:729-744.
9. Galasko D, Katzman R, Salmon DP, Thal LJ, Hansen LA. Clinical and neuropatho- 32. Butters N, Wolfe J, Granholm E, Martone M. An assessment of verbal recall, rec-
logical findings in Lewy body dementias. Brain Cogn. 1996;31:166-175. ognition and fluency abilities in Huntington’s disease. Cortex. 1986;22:11-32.
ARCH NEUROL / VOL 55, JULY 1998
1000
Downloaded from www.archneurol.com on June 22, 2010
©1998 American Medical Association. All rights reserved.
calcium channel is ubiquitous in the brain, the channel REFERENCES
is expressed most abundantly in the regions where pa-
tients who currently had SCA6 showed atrophy.
1. Zhuchenko O, Bailey J, Bonnen P, et al. Autosomal dominant cerebellar ataxia
In conclusion, our results suggest that SCA6 af- (SCA6) associated with small polyglutamine expansions in the a1A-voltage-
fects the cerebellum and its afferent and efferent sys- dependent calcium channel. Nat Genet. 1997;15:62-69.
tems. Further study with larger numbers of subjects is 2. Matsuyama Z, Kawakami H, Maruyama H, et al. Molecular features of the
necessary to elucidate the relationship between the CAG CAG repeats of spinocerebellar ataxia 6 (SCA6). Hum Mol Genet. 1997;6:
1283-1288.
repeat length and atrophy or duration of illness.
3. Subramony SH, Fratkin JD, Manyam BV, Currier RD. Dominantly inherited cer-
ebello-olivary atrophy is not due to a mutation at the spinocerebellar ataxia-I,
Accepted for publication January 30, 1998. Machado-Joseph disease, or dentato-rubro-pallido-luysian atrophy locus. Mov
This work was supported by a grant-in-aid from the Re- Disord. 1996;11:174-180.
search Committee of Central Nervous System Degenerative 4. Murata Y, Yamaguchi S, Kawakami H, et al. Characteristic magnetic resonance
imaging findings in Machado-Joseph disease. Arch Neurol. 1998;55:33-37.
Diseases, Ministry of Health and Welfare of Japan, Tokyo. 5. Hillman D, Chen S, Aung TT, Cherksey B, Sugimori M, Llinas RR. Localization of
We thank Takahiko Saida, MD, National Utano Hos- P-type calcium channels in the central nervous system. Proc Natl Acad Sci
pital, Kyoto, for the referral of patients, and Kaori Kata- U S A. 1991;88:7076-7080.
yama, Third Department of Internal Medicine, Hiroshima 6. Starr TVB, Prystay W, Snutch TP. Primary structure of a calcium channel that is
University School of Medicine, for photography. highly expressed in the rat cerebellum. Proc Natl Acad Sci U S A. 1991;88:5621-
5625.
Reprints: Yoshio Murata, MD, Third Department of In- 7. Llinas R, Sugimori M, Hillman DE, Cherksey B. Distribution and functional sig-
ternal Medicine, Hiroshima University School of Medicine, nificance of the P-type, voltage-dependent Ca2+ channels in the mammalian cen-
1-2-3 Kasumi, Minami-ku, Hiroshima 734-8551, Japan. tral nervous system. Trends Neurosci. 1992;15:351-355.
Correction
Incorrect Equation. In the July 1998 issue of the
ARCHIVES (1998;55:994-1000) in the first equation on
page 998 the coefficient value for conceptualization
should have been + 0.040 and not + 040 as printed. Thus,
the correct equation is: Classification = 0.154 (Atten-
tion) − 0.101 (Construction) + 0.040 (Conceptualiza-
tion) − 0.162 (Initiation) + 0.191 (Memory) − 4.75.
ARCH NEUROL / VOL 55, OCT 1998
1352
Downloaded from www.archneurol.com on June 22, 2010
©1998 American Medical Association. All rights reserved.
Vous aimerez peut-être aussi
- Scanned With CamscannerDocument6 pagesScanned With CamscannerGonzalo GVPas encore d'évaluation
- Patterns of Post-Traumatic Stress Symptoms in Families After Paediatric Intensive CareDocument9 pagesPatterns of Post-Traumatic Stress Symptoms in Families After Paediatric Intensive CareGonzalo GVPas encore d'évaluation
- Scas AdministraciónDocument2 pagesScas AdministraciónGonzalo GVPas encore d'évaluation
- 2014 Batería III Woodcock-Muñoz NU Order Form: Payment InformationDocument2 pages2014 Batería III Woodcock-Muñoz NU Order Form: Payment InformationGonzalo GV100% (1)
- Adult Attachment InterviewDocument11 pagesAdult Attachment InterviewAndreea Serpisor100% (1)
- MADRSDocument4 pagesMADRSGonzalo GVPas encore d'évaluation
- Bdi Ii AdolescentesDocument6 pagesBdi Ii AdolescentesGonzalo GVPas encore d'évaluation
- Scas AdministraciónDocument2 pagesScas AdministraciónGonzalo GVPas encore d'évaluation
- SCAS Boys 8-11 FinalJune2018Document1 pageSCAS Boys 8-11 FinalJune2018Gonzalo GVPas encore d'évaluation
- SCAS Boys 8-11 FinalJune2018Document1 pageSCAS Boys 8-11 FinalJune2018Gonzalo GVPas encore d'évaluation
- SCAS Girls 8-11 FinalJune2018Document1 pageSCAS Girls 8-11 FinalJune2018Gonzalo GVPas encore d'évaluation
- SCAS Girls 12-15 FinalJune2018Document1 pageSCAS Girls 12-15 FinalJune2018Gonzalo GVPas encore d'évaluation
- SCAS Boys 8-11 FinalJune2018Document1 pageSCAS Boys 8-11 FinalJune2018Gonzalo GVPas encore d'évaluation
- Utilidad de Los Fármacos Dopaminérgicos en El Daño Cerebral TraumáticoDocument5 pagesUtilidad de Los Fármacos Dopaminérgicos en El Daño Cerebral TraumáticoGonzalo GVPas encore d'évaluation
- Kornish PDFDocument6 pagesKornish PDFEileenGreyPas encore d'évaluation
- Australian Clinical Guidelines For Early Psychosis PDFDocument138 pagesAustralian Clinical Guidelines For Early Psychosis PDFBernardo Linares100% (1)
- Residual Cognitive Effects of Uncomplicated Idiopathic and Cryptogenic Epilepsy PDFDocument6 pagesResidual Cognitive Effects of Uncomplicated Idiopathic and Cryptogenic Epilepsy PDFGonzalo GVPas encore d'évaluation
- Orientation Agnosia in Pentagon PDFDocument2 pagesOrientation Agnosia in Pentagon PDFGonzalo GVPas encore d'évaluation
- Core Assessment Program For Surgical IntDocument13 pagesCore Assessment Program For Surgical IntGonzalo GVPas encore d'évaluation
- Sindromes AtencionalesDocument5 pagesSindromes AtencionalesAida Chelita Santillan MejíaPas encore d'évaluation
- Neuropathologic Diagnostic and Nosologic CriteriaDocument18 pagesNeuropathologic Diagnostic and Nosologic CriteriaiwanPas encore d'évaluation
- Bases Neurales de La EmpatiaDocument8 pagesBases Neurales de La EmpatiaGonzalo GVPas encore d'évaluation
- EpiTrack Tracking Cognitive Side Effects of Medication On AttentionDocument7 pagesEpiTrack Tracking Cognitive Side Effects of Medication On AttentionGonzalo GVPas encore d'évaluation
- Dichotic Listening in Patients With Situs Inversus) Brain AsymmetryDocument6 pagesDichotic Listening in Patients With Situs Inversus) Brain AsymmetryGonzalo GVPas encore d'évaluation
- CBT-CP Therapist Manual PDFDocument124 pagesCBT-CP Therapist Manual PDFGonzalo GVPas encore d'évaluation
- CBT-CP Therapist Manual PDFDocument124 pagesCBT-CP Therapist Manual PDFGonzalo GVPas encore d'évaluation
- CBT-CP Therapist Manual PDFDocument124 pagesCBT-CP Therapist Manual PDFGonzalo GVPas encore d'évaluation
- CBT-CP Therapist Manual PDFDocument124 pagesCBT-CP Therapist Manual PDFGonzalo GVPas encore d'évaluation
- CBT-CP Therapist Manual PDFDocument124 pagesCBT-CP Therapist Manual PDFGonzalo GVPas encore d'évaluation
- MADRSDocument4 pagesMADRSGonzalo GVPas encore d'évaluation
- The Yellow House: A Memoir (2019 National Book Award Winner)D'EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Évaluation : 4 sur 5 étoiles4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceD'EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceÉvaluation : 4 sur 5 étoiles4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeD'EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeÉvaluation : 4 sur 5 étoiles4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingD'EverandThe Little Book of Hygge: Danish Secrets to Happy LivingÉvaluation : 3.5 sur 5 étoiles3.5/5 (399)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaD'EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaÉvaluation : 4.5 sur 5 étoiles4.5/5 (266)
- Shoe Dog: A Memoir by the Creator of NikeD'EverandShoe Dog: A Memoir by the Creator of NikeÉvaluation : 4.5 sur 5 étoiles4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureD'EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureÉvaluation : 4.5 sur 5 étoiles4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItD'EverandNever Split the Difference: Negotiating As If Your Life Depended On ItÉvaluation : 4.5 sur 5 étoiles4.5/5 (838)
- Grit: The Power of Passion and PerseveranceD'EverandGrit: The Power of Passion and PerseveranceÉvaluation : 4 sur 5 étoiles4/5 (588)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryD'EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryÉvaluation : 3.5 sur 5 étoiles3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerD'EverandThe Emperor of All Maladies: A Biography of CancerÉvaluation : 4.5 sur 5 étoiles4.5/5 (271)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyD'EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyÉvaluation : 3.5 sur 5 étoiles3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealD'EverandOn Fire: The (Burning) Case for a Green New DealÉvaluation : 4 sur 5 étoiles4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersD'EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersÉvaluation : 4.5 sur 5 étoiles4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnD'EverandTeam of Rivals: The Political Genius of Abraham LincolnÉvaluation : 4.5 sur 5 étoiles4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaD'EverandThe Unwinding: An Inner History of the New AmericaÉvaluation : 4 sur 5 étoiles4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreD'EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreÉvaluation : 4 sur 5 étoiles4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)D'EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Évaluation : 4.5 sur 5 étoiles4.5/5 (121)
- Her Body and Other Parties: StoriesD'EverandHer Body and Other Parties: StoriesÉvaluation : 4 sur 5 étoiles4/5 (821)
- Lesson Plan-Grade 3-MathDocument4 pagesLesson Plan-Grade 3-Mathtimothy castillo100% (1)
- Type Conditions and StyleDocument18 pagesType Conditions and StyleAmir ChohanPas encore d'évaluation
- Role of Pragmatism in Education: GC University FaisalabadDocument20 pagesRole of Pragmatism in Education: GC University FaisalabadShahid JappaPas encore d'évaluation
- Participate in Workplace CommunicationDocument50 pagesParticipate in Workplace CommunicationJeff LacasandilePas encore d'évaluation
- GTKK 6 Boo Jin Park Patriarchy in Korean SocietyDocument13 pagesGTKK 6 Boo Jin Park Patriarchy in Korean SocietyIleana CosanzeanaPas encore d'évaluation
- Criminal Sociology Q&a Part IiiDocument10 pagesCriminal Sociology Q&a Part IiiDonita BernardinoPas encore d'évaluation
- Song Outline Worksheet Using Figurative LanguageDocument5 pagesSong Outline Worksheet Using Figurative LanguageCathPang-MakPas encore d'évaluation
- HPI GuidelinesDocument5 pagesHPI GuidelinesHani NadiahPas encore d'évaluation
- Impact of Motivation On Organizational PerformanceDocument6 pagesImpact of Motivation On Organizational Performancetewodros gashaw0% (1)
- Facial Expression Recognition Using Convolutional Neural Networks: State of The ArtDocument6 pagesFacial Expression Recognition Using Convolutional Neural Networks: State of The Arttrương xuân thànhPas encore d'évaluation
- Types of Speeches According To PurposeDocument9 pagesTypes of Speeches According To PurposeKamsa HamniPas encore d'évaluation
- Psychology Project 2016-2017: The Indian Community School, KuwaitDocument21 pagesPsychology Project 2016-2017: The Indian Community School, KuwaitnadirkadhijaPas encore d'évaluation
- Retrograde PlanetsDocument2 pagesRetrograde PlanetsthavaPas encore d'évaluation
- Toefl Exercise (Problem With Pronoun)Document2 pagesToefl Exercise (Problem With Pronoun)Waode Zuldiani Nilam CahyaPas encore d'évaluation
- Imam Nur AkbarDocument4 pagesImam Nur AkbarImam Nur akbarPas encore d'évaluation
- Ten FramesDocument5 pagesTen Framesapi-334723488Pas encore d'évaluation
- Active Learning MethodDocument32 pagesActive Learning MethodPatimah Indri RaspatiPas encore d'évaluation
- Jealousy and The Threatened SelfDocument16 pagesJealousy and The Threatened Selfმარი ლელუაშვილიPas encore d'évaluation
- Part B: Session Plan 4 Completed With Details and AttachedDocument2 pagesPart B: Session Plan 4 Completed With Details and AttachedAAditya Shaujan PaudelPas encore d'évaluation
- Introduction To Research Methods 3Document15 pagesIntroduction To Research Methods 311Co sarahPas encore d'évaluation
- Marketing Communications - Module 3 NotesDocument10 pagesMarketing Communications - Module 3 NotesadamPas encore d'évaluation
- Chapter 13 Managing in A Unionized EnvironmentDocument10 pagesChapter 13 Managing in A Unionized EnvironmentLuke Thomas100% (1)
- Why I Think Students Should Cheat AnalysisDocument3 pagesWhy I Think Students Should Cheat AnalysisH.MPas encore d'évaluation
- Unit 1 - Lesson 4Document7 pagesUnit 1 - Lesson 4Diana Fe C. FilpinoPas encore d'évaluation
- Speech & Language Therapy in Practice, Spring 2009Document32 pagesSpeech & Language Therapy in Practice, Spring 2009Speech & Language Therapy in PracticePas encore d'évaluation
- DepEd-NCR Self-Paced Learners ProgramDocument10 pagesDepEd-NCR Self-Paced Learners ProgramCherilyn SaagundoPas encore d'évaluation
- Making Their Voices Heard: The Experiences of Children Born Outside of MarriageDocument9 pagesMaking Their Voices Heard: The Experiences of Children Born Outside of MarriageAriel E SJPas encore d'évaluation
- Key Assessment 2 Documentation Rubric p65-68Document6 pagesKey Assessment 2 Documentation Rubric p65-68api-215636357Pas encore d'évaluation
- Ethics and AccountabilityDocument46 pagesEthics and Accountabilityboniglai50% (1)
- Emotional or Transactional Engagement CIPD 2012Document36 pagesEmotional or Transactional Engagement CIPD 2012Maya Camarasu100% (1)